Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Conjunctiva
Caricato da
Muhammad AboAlasaadCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Conjunctiva
Caricato da
Muhammad AboAlasaadCopyright:
Formati disponibili
CONJUNCTIVA
MCQs
Conjunctival injection is characterized by the following except:
Bright red colour. Movable. Not affected by vasoconstrictors. Individual vessels are easily distinguished.
One of these is not manifested by ciliary injection:
Corneal ulcer Viral conjunctivitis. Acute congestive glaucoma. Acute iridocyclitis.
Persistent unilateral conjunctivitis is usually due to:
Purulent conjunctivitis. Chronic dacryocystitis. Mucopurulent conjunctivitis. Foreign body.
In ophthalmia neonatorum, all are true except:
Caused by birth trauma. Frequently caused by gonococcal infection. Maternal infection plays a role. Silver nitrate drops were used as a prophylaxis.
All the following can be caused by chlamydial infection except:
Ophthalmia neonatorum Trachoma. Inclusion Conjunctivitis. Central corneal ulcer.
These organisms can be seen normally in the conjunctiva:
Koch- Weeks bacillus. Pneumococci. Corynobacterium xerosis. Corynobacterium diphtheria.
Most common organism in purulent conjunctivitis is:
Pneumococci. Streptococci. Gonococci. Herpes simplex virus.
Subconjunctival hemorrhage is not caused by:
Trauma. Mucopurulent conjunctivitis. Adenoviral infection. Acute hemorrhagic conjunctivitis.
Which is true about vernal conjunctivitis :
Always unilateral. Usually occurs in young boys. Antibiotic drops are the main therapy. Main symptom is foreign body sensation.
Patient presented with itching, lacrimation, excoriation and macerated outer canthus, the claimed organism is:
Morax Axenfeld diplobacillus. Haemophylus influenza. Pnumococci.. Koch- Weeks diplobacillus.
Old asthmatic hypertensive patient, presented with severe red eye after acute attack of cough, most propably may be due to:
Corneal abrasion. Acute conjunctivitis. Spontaneous subconjunctival hemorrhage. Acute iritis.
All are sure signs of trachoma except:
Arlts line. Papillae of upper tarsal conjunctiva. Herberts Pits. Expressible follicles.
Itching is common with:
Spring catarrh. Trachoma. Mucopurulrnt conjunctivitis. Corneal ulcer.
The secretions of spring catarrh are rich in:
Eosinophils. Neutrophils. Basophils. Lymphocytes.
Pinguecula is:
Fatty degeneration. Hyaline degeneration. Elastoid hyaline degeneration. Elastoid degeneration.
Giant papillary conjunctivitis can be caused by the following except:
Artificial prosthesis. Spring catarrh. Contact lens wear. Acute conjunctivitis.
Topical treatment used for phlyctenular conjunctivitis is:
Antibiotic drops. Vasoconstrictor drops. Corticosteroid drops. Antiviral drops.
These may cause pterygium, except:
Exposure to ultra violet rays. Viral infection. Pinguecula. Living in tropical area.
Patient had a pterygium, excised since one month, and starts to see double vision, this may be due to:
Medial rectus weakness. Lateral rectus paralysis. Symblepharon formation. Recurrence.
These treatments are useful in preventing the recurrence after pterygium excision except:
Topical antibiotics. Topical corticosteroids. Beta irradiation. 5 FU eye drops.
Which of the following is specific for the diagnosis of allergic conjunctivitis?
Eye redness Itching Foreign body sensation Excessive lacrimation
EYE LID
A patient suffered from acute onset of facial palsy, the first line of treatment is:
Frequent ocular lubrication. Lateral tarsorrhaphy Topical corticosteroids. Levator muscle resection.
The levator palpebrae superioris is inserted into the following structures except:
Skin of upper eye lid Upper border of tarsus Bulbar conjunctiva Medial orbital margin & medial palpebral ligament
Rolling in of the lower lid margin can be due to:
Thermal injury of lid skin Facial palsy Trachoma Ophthalmoplegia
The most important examination in case of congenital ptosis is:
The state of extraocular muscles Fundus examination Amount of levator function Pupillary light reflex
Stye is an acute suppurative inflammation of:
Meibomian glands Accessory lacrimal glands Zeiss glands of the lash Lid margin
follicles
A female patient C / O diffuse hyperemic lid margin with multiple grayish yellow crustations covering the lashes. The best treatment is:
Epilation of affected lashes Electrolysis Hot fomentations and local antibiotics Systemic corticosteroids
In recurrent squamous blepharitis you should:
Give long acting corticosteroids Give long acting antibiotics Correct any refractive errors Give maintenance dose of vitamins.
Chalazion is defined as:
Acute suppurative inflammation of meibomian glands Chronic suppurative inflammation of meibomian glands Chronic inflammatory lipogranuloma of meibomian glands. Chronic non granulomatous inflammation of meibomian glands
Chalazion can cause the following complications except:
Irrigular astigmatism Mechanical ptosis Anterior uveitis Internal hordeolum
A male patient is C / O chronic eye lid redness and frequent loss of lashes. The most propable diagnosis is
Cicatricial entropion Squamous blepharitis Ulcerative blepharitis Active trachoma
A case presented with hypermic lid margin, matting of eye lashes, yellow crustations. The treatment include all the following except:
Local lid hygeine Rubbing the lid margin by antibiotic ointment Elctrolysis Systemic antibiotic
Epilation of maldirected lashes is indicated in:
When the number is less than four When the lashes are close together In presence of acute corneal ulcer In cases of high refractive error.
Congenital ptosis may be associated with the following congenital anomalies except:
Blepharophimosis Telecanthus Epicanthus Naso lacrimal duct obstruction.
Complications of congenital causes include the following except:
Ocular torticollis. Amblyopia. Complicated cataract. Anbormal head posture.
Lagophthalmos can be caused by the following except:
Hyperthyroidism. Facial palsy. Severe entropion Lid coloboma.
The commonest cause of bilateral ptosis is:
Horner syndrome. Third nerve palsy. Congenital Mechanical.
Lid splitting and everting sutures is an operation used for the correction of:
Pure trichiasis of the upper eye lid. Trichiasis and entropion of the upper eye lid. Ectropion of the lower eye lid. Paralytic entropion of the lower eye lid.
All these are true about ulcerative blepharitis except:
Can cause madarosis. Can be complicated by ulcerative keratitis. Can be caused by Morax Axenfeld bacillus. Can be treated by antibiotics.
A 65 ys old patient had recurrence of chalazion after removal from the same site two times. The best management is:
Systemic antibiotic and steroids. Excision and histopathological evaluation. Excision and curette evacuation. Excision and cautery of the edges.
A patient has about 10 maldirected localized lashes of the upper eye lid. The treatment of choice is:
Snellens operation. Lid splitting and cryo application. Epilation Weiss procedure.
Fasaenella operation for ptosis is carried out in cases with:
Severe ptosis. Levator action less than 5 mm. Moderate ptosis. Levator action 5-8 mm. Mild ptosis. Levator action more than 8 mm. None of above.
Incision and curette of chalazion should be.
Vertical. Horizontal. Any shape. circular.
Grey line indicates a tissue plane between:
Skin muscle layer & tarsus conjunctival layer. Tarsus & canjunctiva. Skin & meibomian glands. Palpebral conjunctiva & meibomian gland orifices.
Ankyloblepharon is :
The adhesion of the lids. The adhesion between palpebral and bulbar canjunctiva. The adhesion of the margins of the two lids. All of the above.
Glands of Zeis are:
Modified sweat glands. Modified sebaceous glands. Modified meibomian glands. None of above.
Levator palpebrae is inserted into:
Upper border of the tarsus. Skin of upper lid. Upper fornix. All of above.
Hordeolum externum is an acute suppurative inflammation of:
Gland of Zeis. Gland of Moll. Gland of Wolfring. Gland of Krause.
All of the following types of entropion are known except:
Spastic entropian. Senile entropion. Paralytic entropion. Cicatricial entropion.
The amount of normal levator function is :
5 mm. 8 mm. 25 mm. 13 mm .
1.
In brow suspension operation of ptosis, the best suspension material is :
Fascia lata. Supramid. Prolene. Silicone.
All of the following are the causes of lagophthalmus except:
Facial nerve palsy. Proptosis. Lid fibrosis. Third nerve paralysis.
OCULAR TRAUMA
A 30 ys old patient was subjected to face burn with strong acid, two months later he presented with watering and inability to close his left eye. The explanation of this may be:
Mechanical ectropion. Cicatricial ectropion. Paralytic ectropion. Corneal ulcer.
A patient subjected to vertical lid wound, he is unable to to close his eye properly. This condition can lead to:
Corneal scarring Exposure keratopathy. Vascularized corneal scar. Corneal pannus.
The first line of treatment in acid burn of the eye is:
Eye patching. Immediate wash with plain water. Instilling local antibiotic drops. Neutralization of the acid with alkali.
A 10 ys old boy, received blunt ocular trauma by tennis ball to his right eye, you will expect to have:
Hypopion ulcer. Blood staining of the cornea. Hyphema. Tractional retinal detachment.
A patient had penetrating eye injury in the right eye, the first aid management is:
Washing with plain water. Sterile eye bandage. Application of antibiotic ointment. Instilling atropine eye drops.
A patient is C / O monocular diplopia after blunt ocular trauma, the following could cause this except:
Sublaxated lens. Iridodialysis. Traumatic hyphema. Incipient immature cataract.
A patient had blunt ocular trauma, now he is C / O severe visual defect, the cause of this may be due to:
Anteflexion of the pupil. Berlins edema. Conjunctival chemosis. Angle recession.
Blunt ocular trauma commonly results in:
Blue dot cataract. Anterior subcapsular cataract. Posterior subcapsular cataract. Coronary cataract.
A patient with a history of blunt trauma to the left eye C / O double vision that disappears on covering the left eye & persists on covering the right eye. Examination of this patient would reveal:
Miotic pupil. Ectropion uveae. Pupil showing lens equator. Dilated pupil.
Trauma to the eye cannot cause:
Vitreous hemorrhage. Macular edema. Central retinal vein occlusion. Retinal breaks.
A patient had blunt ocular trauma & C / O double vision that disappears on covering either eye. The cause might be:
Orbital hematoma. Corneal edema. Orbital blow out fracture. Iridodialysis.
A aptient had history of blunt ocular trauma 3 months ago, now is C / O severe headache due to increased intraocular pressure.the most important diagnistic tool is:
Automated field of vision . Manual field of vision. Gonioscopic examination. Fundus examination.
A patient with recent history of ocular trauma & C/ O blurry vision.ocular motility was normal, the most needed investigation is:
Ocular ultrasound. Fluorescein angiography. Field of vision. Performing CT brain.
Etiology of sympathetic ophthalmia is:
Viral Allergic Bacterial None
Prodromal symptoms of sympathetic ophthalmia is:
Pain Redness Photophobia lacrimation
Sympathetic ophthalmia is rarely seen in:
Corneo scleral wounds PECCE. Acute suppuration Iris encarceration.
Retained Intra Orbital FB may not be removed if
Sterile & inert Mild visual affection Its removal will affect the vision. All of the above.
Metallic IOFB can be localized by the following methods except
Limbal ring & X ray CT scan US MRI
Pathognomonic sign of IOFB
Corneal wound Root in the iris Traumatic cataract hyphema
In siderosis bulbi, iron gets:
Deposited in membranes Combined with cell proteins Both None
The following iris lesions caused by blunt trauma except:
Aniridia Anteflexion Retroflection Heterochromia iridum
The weakest part of the eye affected by blunt trauma is:
Canal of Schlemm Muscle insertion Equator Lens zonules
Blunt trauma coming down & out, the sclera ruptures:
Down & out. Up & out. Up & in. Down & in.
Worker with arc light is exposed to:
UVR corneal burn. Infra red heat burn. Gamma radiation. X ray radiation.
Which of the following conditions does NOT require emergency ophthalmological management?
Anterior uveitis Acute angle-closure glaucoma Orbital floor fracture Orbital cellulitis
Solar viewing during an eclipse can cause:
Corneal ulcer Orbital cellulitis Macular burn Retinal tear
Patient had right maxillary tumours treated successfully with multiple doses of radiotherapy, after that he noted dramatic decrease of visual acuity of the right eye, the explanation of this may be due to:
Complicated cataract. Anterior uveitis. Central retinal vein thrombosis. Acute congestive glaucoma.
Which of the following is not advised in the early management of a patient with hyphema?
Admission to hospital. Cycloplegics. IOP lowering agents. None of the above.
Finally I wish you all
GOOD LUCK
Potrebbero piacerti anche
- Turkey Tail MushroomDocumento10 pagineTurkey Tail Mushroomjuanitos111100% (2)
- Ophthalmology PDFDocumento28 pagineOphthalmology PDFKukuh Rizwido PrasetyoNessuna valutazione finora
- Clinical Ophthalmology for UndergraduatesDa EverandClinical Ophthalmology for UndergraduatesValutazione: 4 su 5 stelle4/5 (5)
- Massage TherapyDocumento79 pagineMassage TherapyMukesh Duryodhan Hirekhan100% (1)
- Case Based Ophthalmology GuideDocumento12 pagineCase Based Ophthalmology GuideGradestack100% (2)
- Ophthalmology NotesDocumento22 pagineOphthalmology NotesdrusmansaleemNessuna valutazione finora
- Lacrimal System and Disorders: DR Asad FrazDocumento30 pagineLacrimal System and Disorders: DR Asad FrazAsad Fraz0% (1)
- Biggs Medicine, SurgeryDocumento19 pagineBiggs Medicine, Surgerymary20149Nessuna valutazione finora
- 2735 Pediatric Cataract Manual - CompressedDocumento66 pagine2735 Pediatric Cataract Manual - CompressedKevin RamsahaiNessuna valutazione finora
- Interpretation of Weld RadiographsDocumento10 pagineInterpretation of Weld RadiographsarianaseriNessuna valutazione finora
- Pediatric OphthalmologyDocumento12 paginePediatric Ophthalmologyapi-3743483Nessuna valutazione finora
- Chalcone Synthesis, Structure DiversityDocumento13 pagineChalcone Synthesis, Structure DiversityDini Elsi ANessuna valutazione finora
- Examination of Eye PT IIDocumento77 pagineExamination of Eye PT IIMihaela TomaNessuna valutazione finora
- I Notes RETINA PDFDocumento251 pagineI Notes RETINA PDFFelipe renquenNessuna valutazione finora
- Past MRCOphth Apri1Documento3 paginePast MRCOphth Apri1Eliza SparkNessuna valutazione finora
- Compile Soal Mata PreklinikDocumento77 pagineCompile Soal Mata PreklinikFika RahmawatiNessuna valutazione finora
- 10Documento19 pagine10Bruno100% (3)
- MCQ 1Documento21 pagineMCQ 1rocky singhNessuna valutazione finora
- Okap Samson Uveitis PDFDocumento12 pagineOkap Samson Uveitis PDFsharu4291Nessuna valutazione finora
- Rana Al-Senawi - Arab Board 2014 Exam ExprinceDocumento5 pagineRana Al-Senawi - Arab Board 2014 Exam ExprinceMuhammed AbdulmajeedNessuna valutazione finora
- Opthamology MnemonicsDocumento103 pagineOpthamology MnemonicsIzaz Khan100% (2)
- KERATOCONUSDocumento22 pagineKERATOCONUSAarush DeoraNessuna valutazione finora
- Optho Diams QDocumento5 pagineOptho Diams QShawn Gaurav JhaNessuna valutazione finora
- Viva and Osce Exams in Ophthalmology A Revision Study Guide 1st Ed 9783030430627 9783030430634 CompressDocumento392 pagineViva and Osce Exams in Ophthalmology A Revision Study Guide 1st Ed 9783030430627 9783030430634 CompressstingbeesparvNessuna valutazione finora
- Guia para Estudiar para IcoDocumento16 pagineGuia para Estudiar para IcoMaria Silvana Sequera LampeNessuna valutazione finora
- Clinical OpticsDocumento88 pagineClinical OpticsKris ArchibaldNessuna valutazione finora
- CNLDO JurnalDocumento6 pagineCNLDO JurnalKhairul FitrahNessuna valutazione finora
- Johnson & Johnson Tylenol CrisisDocumento21 pagineJohnson & Johnson Tylenol CrisisArnab Chatterjee100% (2)
- 1000 Ico Basic MCQDocumento231 pagine1000 Ico Basic MCQNidia M. Quispe Rodríguez100% (3)
- 014 Duke Elder Examination Information For Candidates 2013Documento9 pagine014 Duke Elder Examination Information For Candidates 2013PartialChargeNessuna valutazione finora
- Short Answer Questions For The MRCOphth Part 1Documento159 pagineShort Answer Questions For The MRCOphth Part 1Yaman Muhaisen100% (1)
- Eye MCQDocumento1 paginaEye MCQLoveKumarNessuna valutazione finora
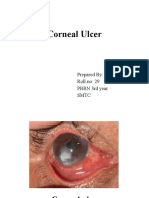
- Corneal Ulcer: Prepared By: Renuka Shrestha Roll No: 29 PBBN 3rd Year SMTCDocumento41 pagineCorneal Ulcer: Prepared By: Renuka Shrestha Roll No: 29 PBBN 3rd Year SMTCsushma shresthaNessuna valutazione finora
- Eye Module ExamDocumento10 pagineEye Module ExamTehniat iqbalNessuna valutazione finora
- First Class Test Topic: GlaucomaDocumento10 pagineFirst Class Test Topic: GlaucomaUkash AkramNessuna valutazione finora
- Evaluation Checklist Case 7 Bronchial AsthmaDocumento7 pagineEvaluation Checklist Case 7 Bronchial AsthmaChristian MendiolaNessuna valutazione finora
- Pediatric OpthDocumento10 paginePediatric OpthZaher Al ObeydNessuna valutazione finora
- BlepharitisDocumento11 pagineBlepharitismohamadNessuna valutazione finora
- Azra Naheed Medical College Departmnt of Ophthalmology Class Test MBBS 4th YearDocumento5 pagineAzra Naheed Medical College Departmnt of Ophthalmology Class Test MBBS 4th YearAhmad ChaudharyNessuna valutazione finora
- Ocular TraumaDocumento67 pagineOcular TraumaRenita Siwi M WNessuna valutazione finora
- Eye Docs GlaucomaDocumento147 pagineEye Docs GlaucomaMuneeb ShahzadNessuna valutazione finora
- Eye Docs RetinaDocumento279 pagineEye Docs RetinaRahul LokhandeNessuna valutazione finora
- Recent Advances in Ophthalmology: Volume 7Da EverandRecent Advances in Ophthalmology: Volume 7S. I. DavidsonValutazione: 5 su 5 stelle5/5 (3)
- 01 OPTICS MCQ - CoNNect AcademyDocumento45 pagine01 OPTICS MCQ - CoNNect AcademyYousef ElnagarNessuna valutazione finora
- Revision Mcqs MCQS: Professor Osama ShalabyDocumento161 pagineRevision Mcqs MCQS: Professor Osama ShalabyAhmed YounisNessuna valutazione finora
- EyeDocumento11 pagineEyeSyed Ali HaiderNessuna valutazione finora
- Glaucoma and LensDocumento4 pagineGlaucoma and Lenssarguss14Nessuna valutazione finora
- Eye To Eye BCQsDocumento23 pagineEye To Eye BCQsLoveKumarNessuna valutazione finora
- Eye Docs UveitisDocumento90 pagineEye Docs UveitisMuneeb ShahzadNessuna valutazione finora
- Ophtha Quiz - PACGDocumento3 pagineOphtha Quiz - PACGAsif MohammedNessuna valutazione finora
- 24 HR IOP Review 2015Documento7 pagine24 HR IOP Review 2015Mape100% (1)
- Qa 1356599084Documento36 pagineQa 1356599084KishoreChandraKoradaNessuna valutazione finora
- DT LeukocoriaDocumento43 pagineDT LeukocoriadeyshieNessuna valutazione finora
- OpthamologyDocumento12 pagineOpthamologyRayyanNessuna valutazione finora
- RetinaDocumento19 pagineRetinaSuze C.Nessuna valutazione finora
- Dams Ophthal TestDocumento76 pagineDams Ophthal TestShrikant Shukla100% (1)
- MCQ Kamal 2021Documento26 pagineMCQ Kamal 2021king darkNessuna valutazione finora
- Direct OphthalmoscopeDocumento16 pagineDirect OphthalmoscopeMuhammed AbdulmajeedNessuna valutazione finora
- Corneal Ulcers in General Practice: Clinical IntelligenceDocumento2 pagineCorneal Ulcers in General Practice: Clinical IntelligenceBenitaNessuna valutazione finora
- Post Cataract EndophthalmitisDocumento55 paginePost Cataract Endophthalmitisdr samreen arifNessuna valutazione finora
- Share Myopia Mcqs'sDocumento4 pagineShare Myopia Mcqs'sshumaila khan50% (2)
- Part Abs SamplesDocumento12 paginePart Abs SamplesgenalinangNessuna valutazione finora
- MCQ Opthalmology For Mbbs 2010 BatchDocumento1 paginaMCQ Opthalmology For Mbbs 2010 Batchcolltfrank100% (1)
- Case Reviews in Ophthalmology Expert Consult - OnlDocumento2 pagineCase Reviews in Ophthalmology Expert Consult - Onldr. mostakNessuna valutazione finora
- Ophthalmology ICTDocumento250 pagineOphthalmology ICTChin Heng Toh100% (1)
- Sistem Pelaporan Dan Pembelajaran Keselamatan Pasien RS Arjaty 2022Documento13 pagineSistem Pelaporan Dan Pembelajaran Keselamatan Pasien RS Arjaty 2022vera kusunyadewiNessuna valutazione finora
- Konversi Insulin IV-sc 2Documento12 pagineKonversi Insulin IV-sc 2Nurul Kamilah SadliNessuna valutazione finora
- Cardiac PoisonsDocumento36 pagineCardiac PoisonsTARIQNessuna valutazione finora
- Impact of School Health Education Program On PersonalDocumento4 pagineImpact of School Health Education Program On Personalaspiah mahmudNessuna valutazione finora
- Parenteral NutritionDocumento8 pagineParenteral NutritionivanNessuna valutazione finora
- Times Leader 07-25-2011Documento27 pagineTimes Leader 07-25-2011The Times LeaderNessuna valutazione finora
- Corpal Nindya Duri IkanDocumento10 pagineCorpal Nindya Duri IkanRadianNasutionNessuna valutazione finora
- What Is Intestinal ObstructionDocumento7 pagineWhat Is Intestinal ObstructionsagerNessuna valutazione finora
- Lactose Intolerance in InfantsDocumento10 pagineLactose Intolerance in InfantsflorenceNessuna valutazione finora
- Fascio LaDocumento20 pagineFascio LaMuhammad NoorNessuna valutazione finora
- Drug InteractionsDocumento21 pagineDrug InteractionsPawan Deshmukh100% (1)
- Effectiveness of A Comprehensive Hand Hygiene Program ForDocumento11 pagineEffectiveness of A Comprehensive Hand Hygiene Program Form1k0eNessuna valutazione finora
- Classification of Drugs Are: Hepatoprotective Drugs E.g.: Silymarin Antibiotics E.G.Documento2 pagineClassification of Drugs Are: Hepatoprotective Drugs E.g.: Silymarin Antibiotics E.G.Navya Sara SanthoshNessuna valutazione finora
- Lesser Metatarsal Osteotomy Complications: Lowell S. Weil and Erin E. KleinDocumento9 pagineLesser Metatarsal Osteotomy Complications: Lowell S. Weil and Erin E. KleinAntonio FloresNessuna valutazione finora
- Outbreak Investigation Part 1 PDFDocumento4 pagineOutbreak Investigation Part 1 PDFashythegreat93Nessuna valutazione finora
- Dabur PresentationDocumento26 pagineDabur PresentationShraddha Khurana100% (1)
- DC145 Cross-Reactivity ChartDocumento2 pagineDC145 Cross-Reactivity ChartRyan BurrNessuna valutazione finora
- Pebc Evaluating Exam Sample QuestionDocumento50 paginePebc Evaluating Exam Sample QuestionZain zanzoonNessuna valutazione finora
- Pain ADocumento19 paginePain Akcc2012Nessuna valutazione finora
- Post-Operative Abdominal Infections: Epidemiology, Operational Definitions, and OutcomesDocumento10 paginePost-Operative Abdominal Infections: Epidemiology, Operational Definitions, and OutcomesJared CossioNessuna valutazione finora
- DR Irza Wahid - Annemia Approach - 139Documento60 pagineDR Irza Wahid - Annemia Approach - 139single_ladyNessuna valutazione finora
- Ais YesDocumento15 pagineAis YesLauriz Dillumas MachonNessuna valutazione finora
- NantesDiagnosticCriteria For Pudendal NeuralgiaDocumento5 pagineNantesDiagnosticCriteria For Pudendal NeuralgiaTeresa BeckNessuna valutazione finora