Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Dr. Irbab Hawari
Caricato da
irbabhmd0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
37 visualizzazioni25 pagineCOPD is characterized by chronic cough, sputum production, and shortness of breath. A diagnosis is made based on spirometry showing reduced airflow. Treatment focuses on smoking cessation, bronchodilators to open airways, and managing infections and inflammation. The goals are improving symptoms and quality of life while preserving lung function and preventing exacerbations.
Descrizione originale:
Lecture about COPD and its management comprehensively
Titolo originale
Copd
Copyright
© © All Rights Reserved
Formati disponibili
PPTX, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCOPD is characterized by chronic cough, sputum production, and shortness of breath. A diagnosis is made based on spirometry showing reduced airflow. Treatment focuses on smoking cessation, bronchodilators to open airways, and managing infections and inflammation. The goals are improving symptoms and quality of life while preserving lung function and preventing exacerbations.
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
37 visualizzazioni25 pagineDr. Irbab Hawari
Caricato da
irbabhmdCOPD is characterized by chronic cough, sputum production, and shortness of breath. A diagnosis is made based on spirometry showing reduced airflow. Treatment focuses on smoking cessation, bronchodilators to open airways, and managing infections and inflammation. The goals are improving symptoms and quality of life while preserving lung function and preventing exacerbations.
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 25
COPD
dr. Irbab Hawari
Symptoms and Signs
• Cough, usually worse in the mornings and
productive of a small amount of colorless
sputum
• Breathlessness: The most significant symptom,
but usually does not occur until the sixth
decade of life
• Wheezing: May occur in some patients,
particularly during exertion and exacerbations
• Hyperinflation (barrel chest)
• Wheezing – Frequently heard on forced and
unforced expiration
• Diffusely decreased breath sounds
• Hyperresonance on percussion
• Prolonged expiration
(in severe disease)
• Tachypnea and respiratory distress with
simple activities
• Use of accessory respiratory muscles and
paradoxical indrawing of lower intercostal
spaces (Hoover sign)
• Cyanosis
• Elevated jugular venous pulse (JVP)
• Peripheral edema
Certain characteristic :
Chronic Bronchitis
• Patients may be obese
• Frequent cough and expectoration are typical
• Use of accessory muscles of respiration is
common
• Coarse rhonchi and wheezing may be heard
on auscultation
• Patients may have signs of right heart failure
(ie, cor pulmonale), such as edema and
cyanosis
Certaim characteristics:
Emphysema
• Patients may be very thin with a barrel chest
• Patients typically have little or no cough or
expectoration
• Breathing may be assisted by pursed lips and
use of accessory respiratory muscles; patients
may adopt the tripod sitting position
• The chest may be hyperresonant, and
wheezing may be heard
• Heart sounds are very distant
Diagnosis
• The formal diagnosis of COPD is made with
spirometry; when the ratio of forced
expiratory volume in 1 second over forced
vital capacity (FEV1/FVC) is less than 70%
• Severity
– Stage I (mild): FEV1 80% or greater of predicted
– Stage II (moderate): FEV1 50-79% of predicted
– Stage III (severe): FEV1 30-49% of predicted
– Stage IV (very severe): FEV1 less than 30% of
predicted or FEV1 less than 50% and chronic
respiratory failu
• Chest radiograph : Emphysema
– Flattening of the diaphragm
– Increased retrosternal air space
– A long, narrow heart shadow
– Rapidly tapering vascular shadows accompanied
by hyperlucency of the lungs
– Radiographs in patients with chronic bronchitis
show increased bronchovascular markings and
cardiomegaly
• Chest Radiograph : Bronchitis
– Chronic bronchitis is associated with increased
bronchovascular markings and cardiomegaly.
Differential Diagnosis
• CHF
• Chronic asthma
Treatment
• The goal of COPD management is to improve a
patient’s functional status and quality of life
by preserving optimal lung function,
improving symptoms, and preventing the
recurrence of exacerbations.
• Diet
Inadequate nutritional status associated with low
body weight in patients with COPD is associated
with impaired pulmonary status, reduced
diaphragmatic mass, lower exercise capacity, and
higher mortality rates.
• Smoking Cessation
• Bronchodilator
Bronchodilators are the backbone of any COPD
treatment regimen. They work by dilating airways,
thereby decreasing airflow resistance. This
increases airflow and decreases dynamic
hyperinflation.
• Beta 2-agonist and cholinergic antagonist
– Beta2-agonist bronchodilators activate specific B2-
adrenergic receptors on the surface of smooth
muscle cells, which increases intracellular cyclic
adenosine monophosphate (cAMP) and smooth
muscle relaxation.
– Anticholinergic drugs compete with acetylcholine
for postganglionic muscarinic receptors, thereby
inhibiting cholinergically mediated bronchomotor
tone, resulting in bronchodilation
• Management of Inflammation
– Steroid is effective in acute exacerbation
– the use of oral steroids in persons with chronic
stable COPD is widely discouraged,
– inhaled corticosteroids should be used only in
conjunction with a long-acting beta agonist.
• Management of infection
– In patients with COPD, chronic infection or
colonization of the lower airways is common from S
pneumoniae, H influenzae, and M catarrhalis. In
patients with chronic severe airway obstruction, P
aeruginosa infection may also be prevalent.
– Empiric antimicrobial therapy is recommended in
patients with an acute exacerbation
– In a study by Daniels et al, the addition to doxycycline
to corticosteroids was found to somewhat improve
treatment for acute exacerbation of COPD (AECOPD).
• Oxygen Therapy and Hypoxemia
Thank You
Potrebbero piacerti anche
- Asthma: Symptoms, Treatments, and Medication for Asthma and BronchitisDa EverandAsthma: Symptoms, Treatments, and Medication for Asthma and BronchitisNessuna valutazione finora
- Zhunussova DDocumento18 pagineZhunussova DAnanth Sai BadetiNessuna valutazione finora
- CopdDocumento41 pagineCopdneelumshaukatNessuna valutazione finora
- 1 - CopdDocumento40 pagine1 - Copdvmj8tyh5dsNessuna valutazione finora
- Chronic Obstructive Pulmonary Disease (COPD) : Assistant Professor:Tong JinDocumento39 pagineChronic Obstructive Pulmonary Disease (COPD) : Assistant Professor:Tong JinEINSTEIN2DNessuna valutazione finora
- COPDDocumento42 pagineCOPDAnoos rabayarabayaNessuna valutazione finora
- Chronic Obstructive Airway Disease: Assoc Professor Dr. VinothiniDocumento29 pagineChronic Obstructive Airway Disease: Assoc Professor Dr. VinothiniVivienneNessuna valutazione finora
- Respi CopdDocumento90 pagineRespi CopdJosephine IsonNessuna valutazione finora
- Chronic Obstructive Pulmonary Disease: Joshi MarmikDocumento27 pagineChronic Obstructive Pulmonary Disease: Joshi MarmikRaj DuraiNessuna valutazione finora
- Chronic Obstructive Lung Disease (COPD) : Is An Obstructive Lung Diseases in Which Irreversible Lung Damage Has OccuredDocumento25 pagineChronic Obstructive Lung Disease (COPD) : Is An Obstructive Lung Diseases in Which Irreversible Lung Damage Has OccuredOmar AbdillahiNessuna valutazione finora
- 13.acute Respiratory FailureDocumento34 pagine13.acute Respiratory Failurekarim hassan100% (1)
- Copd (Chronic Obstructive: Pulmonary Disease)Documento68 pagineCopd (Chronic Obstructive: Pulmonary Disease)sinan kNessuna valutazione finora
- Chronic Obstructive Pulmonary Disease: by Abhinay Sharma Bhugoo Ml-610Documento62 pagineChronic Obstructive Pulmonary Disease: by Abhinay Sharma Bhugoo Ml-610abhinay_1712Nessuna valutazione finora
- 16 Martie - Curs BPOC - SlideDocumento95 pagine16 Martie - Curs BPOC - Slidejonah1024Nessuna valutazione finora
- COPDDocumento41 pagineCOPDsanalcrazy100% (3)
- COPD CaseDocumento73 pagineCOPD CaseTony DawaNessuna valutazione finora
- Chronic Obstructive Pulmonary DiseaseDocumento29 pagineChronic Obstructive Pulmonary DiseasesivaNessuna valutazione finora
- Student Copy of COPD Lecture NotesDocumento8 pagineStudent Copy of COPD Lecture NotesMary MarshNessuna valutazione finora
- C.O.P.D: (Chronic Obstructive Pulmonary Disorder)Documento47 pagineC.O.P.D: (Chronic Obstructive Pulmonary Disorder)KrystelNessuna valutazione finora
- Chronic Obstructive Pulmonary Disease (COPD)Documento23 pagineChronic Obstructive Pulmonary Disease (COPD)akoeljames8543Nessuna valutazione finora
- Asthama & COPDDocumento84 pagineAsthama & COPDAbdullah BhattiNessuna valutazione finora
- It 8 Restrictive Pulmonary Diseases - RouDocumento43 pagineIt 8 Restrictive Pulmonary Diseases - RoududidumNessuna valutazione finora
- COPDDocumento11 pagineCOPDSherree HayesNessuna valutazione finora
- Obstructive Pulmonary DiseasesDocumento42 pagineObstructive Pulmonary Diseasesbessan alfqeatNessuna valutazione finora
- Chronic Obstructive Pulmonary Disease (COPD)Documento51 pagineChronic Obstructive Pulmonary Disease (COPD)api-19641337Nessuna valutazione finora
- Week 5 Respiratory EmergencyDocumento61 pagineWeek 5 Respiratory EmergencyArmand Bong SantiagoNessuna valutazione finora
- Chest AyuDocumento70 pagineChest AyuAbebe GelawNessuna valutazione finora
- Copd by Musa Afridi 17-029Documento6 pagineCopd by Musa Afridi 17-029Essa AfridiNessuna valutazione finora
- Gold and Gina Guideline For Copd and AsthmaDocumento56 pagineGold and Gina Guideline For Copd and AsthmaSomnath Das GuptaNessuna valutazione finora
- Asma Dan Penyakit Paru Obstruktif KronisDocumento34 pagineAsma Dan Penyakit Paru Obstruktif KronisAtikah ArifahNessuna valutazione finora
- Pulmonary EmphysemaDocumento20 paginePulmonary EmphysemaAbigailNessuna valutazione finora
- 4 5850649646552060844Documento29 pagine4 5850649646552060844mosaNessuna valutazione finora
- CopdDocumento47 pagineCopdIsmail AbdulNoorNessuna valutazione finora
- Chapter 4 HTDocumento52 pagineChapter 4 HTtesfamichael mengistuNessuna valutazione finora
- COPDDocumento47 pagineCOPDMegha VadanereNessuna valutazione finora
- Pulmonary Eval Amd LabDocumento58 paginePulmonary Eval Amd LabSara DuranNessuna valutazione finora
- Obstructive Disorders: Dr. Suman SherazDocumento45 pagineObstructive Disorders: Dr. Suman SherazSalman KhanNessuna valutazione finora
- Chronic Obstructive Pulmonary DiseaseDocumento45 pagineChronic Obstructive Pulmonary DiseaseAlexander Santiago ParelNessuna valutazione finora
- Patient Prep: Follow Guidelines On P. 65 of Clinical PacketDocumento4 paginePatient Prep: Follow Guidelines On P. 65 of Clinical PacketKatherine AmbrosiaNessuna valutazione finora
- CopdDocumento89 pagineCopdVijayalaxmi KathareNessuna valutazione finora
- CODPDocumento34 pagineCODPNeeraja M SureshNessuna valutazione finora
- Merged 37Documento21 pagineMerged 37abdulkreemsalem4Nessuna valutazione finora
- Chronic Obstructive Pulmonary Disease: Presented byDocumento25 pagineChronic Obstructive Pulmonary Disease: Presented byChinni 12599Nessuna valutazione finora
- Anaesthesia and CopdDocumento7 pagineAnaesthesia and CopdAshish PandeyNessuna valutazione finora
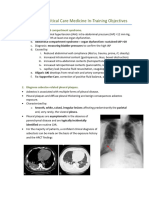
- Pulmonary and Critical Care Medicine In-Training ObjectivesDocumento12 paginePulmonary and Critical Care Medicine In-Training ObjectiveshectorNessuna valutazione finora
- Respiratory Failure Results From Inadequate Gas ExchangeDocumento7 pagineRespiratory Failure Results From Inadequate Gas ExchangeJiezl Abellano AfinidadNessuna valutazione finora
- Pulmonary Vascular Disorders and Respiratory FailureDocumento5 paginePulmonary Vascular Disorders and Respiratory FailureTrishia GuillermoNessuna valutazione finora
- Copd PDFDocumento28 pagineCopd PDFDarawan MirzaNessuna valutazione finora
- COPD Student Lec DR Atef Alkarn 6-2022Documento42 pagineCOPD Student Lec DR Atef Alkarn 6-2022mohamed albnaNessuna valutazione finora
- Asthma and COPDDocumento47 pagineAsthma and COPDSamuelVilbrunNessuna valutazione finora
- Copd CalDocumento30 pagineCopd Calwheeyycoldandhot55Nessuna valutazione finora
- Approach To Chronic CoughDocumento31 pagineApproach To Chronic CoughNoreen Ooi Zhi MinNessuna valutazione finora
- COPD (Chronic Obstructive Pulmonary Disease)Documento16 pagineCOPD (Chronic Obstructive Pulmonary Disease)Maurine OmondiNessuna valutazione finora
- Emphysema Fall 2019Documento3 pagineEmphysema Fall 2019Mary MarshNessuna valutazione finora
- Anaesthesia For Patients With COPD: University College of Medical Sciences & GTB Hospital, DelhiDocumento76 pagineAnaesthesia For Patients With COPD: University College of Medical Sciences & GTB Hospital, DelhiRINI100% (1)
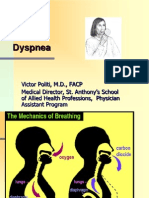
- DyspneaDocumento86 pagineDyspneaJorianditha RamadhanNessuna valutazione finora
- 418-M1-Cu 5 Resp. Emergencies 2Documento12 pagine418-M1-Cu 5 Resp. Emergencies 2Paradillo Regatuna LesterNessuna valutazione finora
- Dyspnea or Breathlessness Is Defined As The Feeling of An Uncomfortable Need To BreatheDocumento33 pagineDyspnea or Breathlessness Is Defined As The Feeling of An Uncomfortable Need To Breatheapi-19641337Nessuna valutazione finora
- 1.chronic Illness Overview and COPDDocumento12 pagine1.chronic Illness Overview and COPDOmar IzzoNessuna valutazione finora
- Update MX of COPDDocumento60 pagineUpdate MX of COPDNusrat JahanNessuna valutazione finora
- Drug StudyDocumento7 pagineDrug StudyMae Navidas DigdiganNessuna valutazione finora
- Ncp-Drug StudyDocumento2 pagineNcp-Drug StudyMark oliver GonzalesNessuna valutazione finora
- Chronic Obstructive Pulmonary Disease (COPD) : Sultan Chaudhry Benny Dua Eric WongDocumento7 pagineChronic Obstructive Pulmonary Disease (COPD) : Sultan Chaudhry Benny Dua Eric Wongjamil aldasriNessuna valutazione finora
- Standards For The Diagnosis and Treatment of Patients With COPDDocumento15 pagineStandards For The Diagnosis and Treatment of Patients With COPDAri KuncoroNessuna valutazione finora
- RITS. Bronchial AsthmaDocumento56 pagineRITS. Bronchial AsthmaRita100% (1)
- 1final MCQSDocumento56 pagine1final MCQSahmed100% (4)
- (PULMO) - Asthma PDFDocumento5 pagine(PULMO) - Asthma PDFKeith LajotNessuna valutazione finora
- Clen GuideDocumento19 pagineClen Guidemilad bigdeliNessuna valutazione finora
- Asthma Review PDFDocumento12 pagineAsthma Review PDFdanielc503Nessuna valutazione finora
- Ineffective Airway ClearanceDocumento2 pagineIneffective Airway ClearanceMaria ArregoitiaNessuna valutazione finora
- BronchodilatorsDocumento5 pagineBronchodilatorsLUMAGSAO, Aliah KaraizNessuna valutazione finora
- Asthma: Rochelle M. Nolte, MD CDR Usphs Family MedicineDocumento56 pagineAsthma: Rochelle M. Nolte, MD CDR Usphs Family MedicineJoan Marie Lechado InoviaNessuna valutazione finora
- Emphysema NCPDocumento5 pagineEmphysema NCPAbegail Bautista DoriaNessuna valutazione finora
- Bronchial AsthmaDocumento14 pagineBronchial AsthmaRashmi GoswamiNessuna valutazione finora
- Chapter 14: Acute Respiratory Failure Test Bank: Multiple ChoiceDocumento13 pagineChapter 14: Acute Respiratory Failure Test Bank: Multiple ChoiceMalak AbdullahNessuna valutazione finora
- Bronchodilators and Other Respiratory DrugsDocumento44 pagineBronchodilators and Other Respiratory DrugsastriedamaliaamanatNessuna valutazione finora
- Formulation Development and Evaluations of Pulsatile Drug Delivery of Tiotropium BromideDocumento76 pagineFormulation Development and Evaluations of Pulsatile Drug Delivery of Tiotropium BromideG.MANOHAR BABUNessuna valutazione finora
- COPD Case PresentationDocumento4 pagineCOPD Case PresentationMary Mae Bercacio BuellaNessuna valutazione finora
- Pharmacology Review For NursesDocumento11 paginePharmacology Review For Nursesisabel_avancena100% (4)
- Aspiration Pneumonia in Dogs:: Treatment, Monitoring, and PrognosisDocumento5 pagineAspiration Pneumonia in Dogs:: Treatment, Monitoring, and Prognosisever syNessuna valutazione finora
- Discrete Separation of Patients' Profiles For Chronical Obstructive Pulmonary Disease Context-Aware Healthcare Efficient SystemsDocumento13 pagineDiscrete Separation of Patients' Profiles For Chronical Obstructive Pulmonary Disease Context-Aware Healthcare Efficient SystemsIAES IJAINessuna valutazione finora
- Doxophylline Prescribing InformationDocumento1 paginaDoxophylline Prescribing InformationMohammed shamiul ShahidNessuna valutazione finora
- Lesson 5 - Respiratory DrugsDocumento69 pagineLesson 5 - Respiratory DrugsMarc AndrewNessuna valutazione finora
- AminophyllineDocumento9 pagineAminophyllineZaira BataloNessuna valutazione finora
- Topic: Asthma and Copd: Internal Medicine IiDocumento8 pagineTopic: Asthma and Copd: Internal Medicine IicarlosNessuna valutazione finora
- COPDDocumento30 pagineCOPDAmila SirisingheNessuna valutazione finora
- Generic NameDocumento7 pagineGeneric NameGia Bautista-AmbasingNessuna valutazione finora
- Chapter 29: Nursing Management: Obstructive Pulmonary Diseases Test BankDocumento15 pagineChapter 29: Nursing Management: Obstructive Pulmonary Diseases Test BankBriseidaSolisNessuna valutazione finora
- Bronchial AsthmaDocumento43 pagineBronchial AsthmaAmar BimavarapuNessuna valutazione finora
- Mksap PulmonaryDocumento77 pagineMksap PulmonaryAna Roman100% (4)