Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Urinary Tract Infection
Caricato da
Vittorio Carlino0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
14 visualizzazioni38 pagineUrinary tract infection ppw
Copyright
© © All Rights Reserved
Formati disponibili
PPTX, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoUrinary tract infection ppw
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
14 visualizzazioni38 pagineUrinary Tract Infection
Caricato da
Vittorio CarlinoUrinary tract infection ppw
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 38
Urinary tract infection
PREVALENCE AND ETIOLOGY
Urinary tract infections (UTIs) occur in 1-3% of girls and
1% of boys.
In girls, the first UTI usually occurs by the age of 5 yr,
with peaks during infancy and toilet training.
In boys, most UTIs occur during the 1st yr of life; UTIs
are much more common in uncircumcised boys,
especially in the 1st year of life.
The prevalence of UTIs varies with age. During the 1st
yr of life, the male : female ratio is 2.8-5.4 : 1. Beyond
1-2 yr, there is a female preponderance, with a male :
female ratio of 1 : 10.
PREVALENCE AND ETIOLOGY
UTIs are caused mainly by colonic bacteria.
In girls, 75-90% of all infections are caused by
Escherichia coli , followed by Klebsiella spp
and Proteus spp.
Staphylococcus saprophyticus and
enterococcus are pathogens in both sexes.
Adenovirus and other viral infections also can
occur, especially as a cause of cystitis.
CLINICAL MANIFESTATIONS AND
CLASSIFICATION
The 3 basic forms of UTI are
pyelonephritis,
cystitis, and
asymptomatic bacteriuria.
Focal pyelonephritis (nephronia) and renal
abscesses are less common.
Clinical Pyelonephritis
Clinical pyelonephritis is characterized by
abdominal, back, or flank pain;
fever;
malaise;
nausea;
vomiting;
occasionally, diarrhea.
Fever may be the only manifestation.
Newborns can show nonspecific symptoms such as poor
feeding, irritability, jaundice, and weight loss.
Clinical Pyelonephritis
Pyelonephritis is the most common serious
bacterial infection in infants <24 mo of age who
have fever without an obvious focus.
Involvement of the renal parenchyma is termed
acute pyelonephritis, whereas if there is no
parenchymal involvement, the condition may be
termed pyelitis.
Acute pyelonephritis can result in renal injury,
termed pyelonephritic scarring.
Acute lobar nephronia
is a renal mass caused by acute focal infection
without liquefaction.
It may be an early stage in the development of
a renal abscess.
Manifestations are identical to pyelonephritis;
Renal abscess can occur following a
pyelonephritic infection due to the usual
uropathogens or may be secondary to a primary
bacteremia (S. aureus).
Perinephric abscess can occur secondary to
contiguous infection in the perirenal area (e.g.,
vertebral osteomyelitis, psoas abscess) or
pyelonephritis that dissects to the renal capsule.
Xanthogranulomatous pyelonephritis is a rare
type of renal infection characterized by
granulomatous inflammation with giant cells and
foamy histiocytes.
It can manifest clinically as a renal mass or an
acute or chronic infection.
Renal calculi, obstruction, and infection with
Proteus spp or E. coli contribute to the
development of this lesion, which usually
requires total or partial nephrectomy.
Cystitis
Cystitis indicates that there is bladder
involvement; symptoms include dysuria,
urgency, frequency, suprapubic pain,
incontinence, and malodorous urine.
Cystitis does not cause fever and does not
result in renal injury.
Malodorous urine is not specific for a UTI.
Acute hemorrhagic cystitis
is caused by E. coli; it also has been attributed
to adenovirus types 11 and 21.
Adenovirus cystitis is more common in boys;
it is self-limiting, with hematuria lasting
approximately 4 days.
Eosinophilic cystitis is a rare form of cystitis of obscure
origin that occasionally is found in children.
The usual symptoms are those of cystitis with hematuria,
ureteral dilation with occasional hydronephrosis, and filling
defects in the bladder caused by masses that consist
histologically of inflammatory infiltrates with eosinophils.
Children with eosinophilic cystitis may have been exposed
to an allergen.
Bladder biopsy often is necessary to exclude a neoplastic
process.
Treatment usually includes antihistamines and nonsteroidal
anti-inflammatory agents, but in some cases intravesical
dimethyl sulfoxide instillation is necessary.
Interstitial cystitis is characterized by irritative
voiding symptoms such as urgency, frequency,
and dysuria, and bladder and pelvic pain relieved
by voiding with a negative urine culture.
The disorder is most likely to affect adolescent
girls and is idiopathic.
Diagnosis is made by cystoscopic observation of
mucosal ulcers with bladder distention.
Treatments have included bladder
hydrodistention and laser ablation of ulcerated
areas, but no treatment provides sustained relief.
Asymptomatic Bacteriuria
Asymptomatic bacteriuria refers to a condition in which there is a
positive urine culture without any manifestations of infection.
It is most common in girls.
The incidence is <1% in preschool and school-age girls and is rare in
boys.
The incidence declines with increasing age.
This condition is benign and does not cause renal injury, except in
pregnant women, in whom asymptomatic bacteriuria, if left
untreated, can result in a symptomatic UTI.
Some girls are mistakenly identified as having asymptomatic
bacteriuria, whereas they actually are experiencing day or night
incontinence or perineal discomfort secondary to UTI.
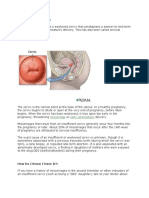
PATHOGENESIS AND PATHOLOGY
Most UTIs are ascending infections.
The bacteria arise from the fecal flora, colonize the
perineum, and enter the bladder via the urethra.
In uncircumcised boys, the bacterial pathogens arise
from the flora beneath the prepuce.
In some cases, the bacteria causing cystitis ascend to
the kidney to cause pyelonephritis.
Rarely, renal infection occurs by hematogenous
spread, as in endocarditis or in some neonates.
PATHOGENESIS AND PATHOLOGY
If bacteria ascend from the bladder to the kidney, acute
pyelonephritis can occur.
Normally the simple and compound papillae in the kidney have an
antireflux mechanism that prevents urine in the renal pelvis from
entering the collecting tubules.
However, some compound papillae, typically in the upper and lower
poles of the kidney, allow intrarenal reflux.
Infected urine then stimulates an immunologic and inflammatory
response. The result can cause renal injury and scarring
Children of any age with a febrile UTI can have acute pyelonephritis
and subsequent renal scarring, but the risk is highest in those <2
years of age.
Vesicoureteral reflux If there is grade III, IV, or V
vesicoureteral reflux and a febrile UTI, 90% have
evidence of acute pyelonephritis on renal scintigraphy
or other imaging studies.
In girls, UTIs often occur at the onset of toilet training
because of voiding dysfunction that occurs at that age.
The child is trying to retain urine to stay dry, yet the
bladder may have uninhibited contractions forcing
urine out.
The result may be high-pressure, turbulent urine flow
or incomplete bladder emptying, both of which
increase the likelihood of bacteriuria.
Voiding dysfunction can occur in the toilet-trained child
who voids infrequently.
Similar problems can arise in school-age children who
refuse to use the school bathroom.
Obstructive uropathy resulting in hydronephrosis
increases the risk of UTI because of urinary stasis.
Urethral catheterization for urine output monitoring or
during a voiding cystourethrogram or nonsterile
catheterization can infect the bladder with a pathogen.
Constipation with fecal impaction can increase the risk
of UTI because it can cause voiding dysfunction.
The pathogenesis of UTI is based in part on the
presence of bacterial pili or fimbriae on the bacterial
surface.
There are two types of fimbriae, type I and type II.
Type I fimbriae are found on most strains of E. coli.
Because attachment to target cells can be blocked by
d-mannose, these fimbriae are referred to as mannose-
sensitive. They have no role in pyelonephritis.
The attachment of type II fimbriae is not inhibited by
mannose, and these are known as mannose-resistant.
These fimbriae are expressed by only certain strains of
E. coli.
The receptor for type II fimbriae is a glycosphingolipid
that is present on both the uroepithelial cell
membrane and red blood cells. The Gal 1-4 Gal
oligosaccharide fraction is the specific receptor.
Because these fimbriae can agglutinate by P blood
group erythrocytes, they are known as P fimbriae.
Bacteria with P fimbriae are more likely to cause
pyelonephritis.
Between 76-94% of pyelonephritogenic strains of E.
coli have P fimbriae, compared with 19-23% of cystitis
strains.
Other host factors for UTI include anatomic abnormalities
precluding normal micturition, such as a labial adhesion.
This lesion acts as a barrier and causes vaginal voiding.
A neuropathic bladder can predispose to UTIs if there is
incomplete bladder emptying and/or detrusor-sphincter
dyssynergia.
Sexual activity is associated with UTIs in girls, in part
because of incomplete bladder emptying.
From 4-7% of pregnant women have asymptomatic
bacteriuria, which can develop into a symptomatic UTI.
The incidence of UTI in infants who are breast-fed is lower
than in those fed with formula.
DIAGNOSIS
UTI may be suspected based on symptoms or findings on urinalysis, or
both; a urine culture is necessary for confirmation and appropriate
therapy.
There are several ways to obtain a urine sample; some are more accurate
than others. a midstream urine sample usually is satisfactory
In children who are not toilet trained, a catheterized urine sample should
be obtained.
Alternatively, the application of an adhesive, sealed, sterile collection bag
after disinfection of the skin of the genitals can be useful only if the
culture is negative or if a single uropathogen is identified.
a positive culture can result from skin contamination, particularly in girls
and uncircumcised boys.
A suprapubic aspirate generally is unnecessary.
Pyuria (leukocytes in the urine) suggests infection, but
infection can occur in the absence of pyuria; this
finding is more confirmatory than diagnostic.
Conversely, pyuria can be present without UTI.
Sterile pyuria (positive leukocytes, negative culture)
occurs in partially treated bacterial UTIs, viral
infections, renal tuberculosis, renal abscess, UTI in the
presence of urinary obstruction, urethritis due to a
sexually transmitted infection (STI), inflammation near
the ureter or bladder (appendicitis, Crohn disease), and
interstitial nephritis (eosinophils).
Nitrites and leukocyte esterase usually are positive in
infected urine.
Microscopic hematuria is common in acute cystitis, but
microhematuria alone does not suggest UTI.
White blood cell casts in the urinary sediment suggest
renal involvement, but in practice these are rarely
seen.
If the child is asymptomatic and the urinalysis result is
normal, it is unlikely that there is a UTI.
However, if the child is symptomatic, a UTI is possible,
even if the urinalysis result is negative.
Prompt plating of the urine sample for culture is important,
because if the urine sits at room temperature for more than 60 min,
overgrowth of a minor contaminant can suggest a UTI when the
urine might not be infected. Refrigeration is a reliable method of
storing the urine until it can be cultured.
If the culture shows >100,000 colonies of a single pathogen, or if
there are 10,000 colonies and the child is symptomatic, the child is
considered to have a UTI.
In a bag sample, if the urinalysis result is positive, the patient is
symptomatic, and there is a single organism cultured with a colony
count >100,000, there is a presumed UTI.
If any of these criteria are not met, confirmation of infection with a
catheterized sample is recommended.
With acute renal infection, leukocytosis, neutrophilia,
and elevated serum erythrocyte sedimentation rate
and C-reactive protein are common.
The latter 2 are nonspecific markers of bacterial
infection, and their elevation does not prove that the
child has acute pyelonephritis.
With a renal abscess, the white blood cell count is
markedly elevated to >20,000-25,000/mm3.
Because sepsis is common in pyelonephritis,
particularly in infants and in any child with obstructive
uropathy, blood cultures should be considered before
starting antibiotics if possible.
TREATMENT
Acute cystitis should be treated promptly to
prevent possible progression to pyelonephritis.
If the symptoms are severe, presumptive
treatment is started pending results of the
culture.
If the symptoms are mild or the diagnosis is
doubtful, treatment can be delayed until the
results of culture are known, and the culture can
be repeated if the results are uncertain.
TREATMENT
If treatment is initiated before the results of a culture and
sensitivities are available, a 3- to 5-day course of therapy
with trimethoprim-sulfamethoxazole (TMP-SMX) or
trimethoprim is effective against most strains of E. coli.
Nitrofurantoin (5-7 mg/kg/24 hr in 3-4 divided doses) also
is effective and has the advantage of being active against
Klebsiella and Enterobacter organisms.
Amoxicillin (50 mg/kg/24 hr) also is effective as initial
treatment but has no clear advantages over sulfonamides
or nitrofurantoin.
In acute febrile infections suggesting pyelonephritis, a 10-
to 14-day course of broad-spectrum antibiotics capable of
reaching significant tissue levels is preferable.
Children who are dehydrated, are vomiting, are unable to
drink fluids, are 1mo of age, or in whom urosepsis is a
possibility should be admitted to the hospital for IV
rehydration and IV antibiotic therapy.
Parenteral treatment with ceftriaxone (50-75 mg/kg/24
hr, not to exceed 2 g) or cefotaxime (100 mg/kg/24 hr), or
ampicillin (100 mg/ kg/24 hr) with an aminoglycoside
such as gentamicin (3-5 mg/ kg/24 hr in 1-3 divided doses)
is preferable.
The potential ototoxicity and nephrotoxicity of
aminoglycosides should be considered, and
serum creatinine and trough gentamicin levels
must be obtained before initiating treatment, as
well as daily thereafter as long as treatment
continues.
Treatment with aminoglycosides is particularly
effective against Pseudomonas spp, and
alkalinization of urine with sodium bicarbonate
increases its effectiveness in the urinary tract.
Oral 3rd-generation cephalosporins such as cefixime
are as effective as parenteral ceftriaxone against a
variety of gramnegative organisms other than
Pseudomonas, and these medications are considered
by some authorities to be the treatment of choice for
oral outpatient therapy. Nitrofurantoin should not be
used routinely in children with a febrile UTI because it
does not achieve significant renal tissue levels.
The oral fluoroquinolone ciprofloxacin is an
alternative agent for resistant microorganisms,
particularly Pseudomonas, in patients >17 yr
It also has been used on occasion for short-course therapy
in younger children with Pseudomonas UTI. However, the
clinical use of fluoroquinolones in children should be
restricted because of potential cartilage damage.
In some children with a febrile UTI, intramuscular injection
of a loading dose of ceftriaxone followed by oral therapy
with a 3rd-generation cephalosporin is effective.
A urine culture 1 wk after the termination of treatment of a
UTI ensures that the urine is sterile but is not routinely
needed.
A urine culture during treatment almost invariably is
negative.
Children with a renal or perirenal abscess or
with infection in obstructed urinary tracts can
require surgical or percutaneous drainage in
addition to antibiotic therapy and other
supportive measures .
Small abscesses may initially be treated
without drainage.
Prophylaxis against reinfection, using TMPSMX,
trimethoprim, or nitrofurantoin at 30% of the normal
therapeutic dose once a day, is one approach to this
problem.
Prophylaxis with amoxicillin or cephalexin can also be
effective, but the risk of breakthrough UTI may be
higher because bacterial resistance may be induced.
There is controversy about prophylaxis against
recurrent UTIs in children with low-grade or no reflux
because resistant organisms can develop, and the
incidence of recurrent infection might not
consistently be reduced.
Other more high risk conditions for recurrent UTIs that
might need long-term prophylaxis include
neurogenic bladder,
urinary tract stasis and obstruction,
reflux,
and calculi.
There is interest in probiotic therapy, which replaces
pathologic urogenital flora, and cranberry juice, which
prevents bacterial adhesion and biofilm formation, but
these agents have not proved beneficial in preventing UTI
in children.
The main consequences of chronic renal
damage caused by pyelonephritis are arterial
hypertension and end-stage renal
insufficiency; when they are found they
should be treated appropriately.
Potrebbero piacerti anche
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- Barriers To NP Practice That Impact Healthcare RedesignDocumento15 pagineBarriers To NP Practice That Impact Healthcare RedesignMartini ListrikNessuna valutazione finora
- Preterm Birth and ComplicationsDocumento5 paginePreterm Birth and Complicationsandrahlyn100% (1)
- Provisionals in Dentistry - From Past To Recent Advances: Rohitraghavan, Shajahan P A, NeenakunjumonDocumento6 pagineProvisionals in Dentistry - From Past To Recent Advances: Rohitraghavan, Shajahan P A, Neenakunjumonnavdeep100% (1)
- Seminar 1 EXPANDED AND EXTENDED ROLE OF PEDIATRIC NURSEDocumento15 pagineSeminar 1 EXPANDED AND EXTENDED ROLE OF PEDIATRIC NURSESuganthi Parthiban100% (7)
- Antepartum HemorrhageDocumento3 pagineAntepartum Hemorrhagenur1146Nessuna valutazione finora
- Medical Surgical Nursing in Canada 2nd Edition Lewis Test BankDocumento7 pagineMedical Surgical Nursing in Canada 2nd Edition Lewis Test BankTeresa Price100% (37)
- Introduction To Integrative MedicineDocumento7 pagineIntroduction To Integrative MedicinePrincess MendezNessuna valutazione finora
- CBCT Applications in DentistryDocumento75 pagineCBCT Applications in DentistryjoephinNessuna valutazione finora
- Mxillary FractureDocumento14 pagineMxillary FractureVittorio CarlinoNessuna valutazione finora
- Abscesses Maxillo: Vittorio Carlino MGE VIDocumento31 pagineAbscesses Maxillo: Vittorio Carlino MGE VIVittorio CarlinoNessuna valutazione finora
- Pharmacology of Blood Drugs Lp1Documento32 paginePharmacology of Blood Drugs Lp1Vittorio CarlinoNessuna valutazione finora
- Hand Expressing Breast PubmedDocumento15 pagineHand Expressing Breast PubmedAsri HartatiNessuna valutazione finora
- University of Dentistry Medicine .: Department of Dermatology and D VenerologyDocumento4 pagineUniversity of Dentistry Medicine .: Department of Dermatology and D VenerologyEriola FrrokuNessuna valutazione finora
- Virtual-OSCE-Frameworks - Published - Resto PartDocumento12 pagineVirtual-OSCE-Frameworks - Published - Resto PartSaleh El BarasiNessuna valutazione finora
- Student's Handbook 2014Documento52 pagineStudent's Handbook 2014Ahmed MawahibNessuna valutazione finora
- Glycemic Targets 2022Documento14 pagineGlycemic Targets 2022Tom BiusoNessuna valutazione finora
- DR Avijit Bansal-My Experiences at UCMSDocumento6 pagineDR Avijit Bansal-My Experiences at UCMScholesterol200Nessuna valutazione finora
- Telaah Jurnal KGDDocumento17 pagineTelaah Jurnal KGDriska eka fatma HasibuanNessuna valutazione finora
- Kleinth Quinto - Week6 EAPP - Performance ActivityDocumento9 pagineKleinth Quinto - Week6 EAPP - Performance ActivityAehjhae DancelNessuna valutazione finora
- Aerobic Dancing BenefitsDocumento4 pagineAerobic Dancing BenefitsDal.giNessuna valutazione finora
- Literatur A 123Documento5 pagineLiteratur A 123Adis ŠišićNessuna valutazione finora
- Hahn El 2016Documento9 pagineHahn El 2016ka waiiNessuna valutazione finora
- CONCEPTUAL FRAMEWORK CorectedDocumento1 paginaCONCEPTUAL FRAMEWORK Corectedsourabh mehraNessuna valutazione finora
- Ali NewDocumento1 paginaAli NewAdeel AizadNessuna valutazione finora
- Intensive Nursing Practicum: Bachelor of Science in NursingDocumento7 pagineIntensive Nursing Practicum: Bachelor of Science in NursingMichelle Gliselle Guinto MallareNessuna valutazione finora
- Cervical Insufficiency:: Miscarriage Early (Premature)Documento2 pagineCervical Insufficiency:: Miscarriage Early (Premature)Ardelean EmanuelNessuna valutazione finora
- Closing Event For Surrey Perinatal Impact PartnershipDocumento11 pagineClosing Event For Surrey Perinatal Impact Partnershipranjanadas0% (1)
- PhilHealth Hospital Accreditation ChecklistDocumento14 paginePhilHealth Hospital Accreditation Checklistamira_hassan100% (1)
- Sf2 - 2022 - Grade 1 - RoseDocumento3 pagineSf2 - 2022 - Grade 1 - RoseNorlds TacukenNessuna valutazione finora
- Management of Terminal Illness in ChildrenDocumento8 pagineManagement of Terminal Illness in Childrenraneen reazNessuna valutazione finora
- What Vaccines Do BC Adults NeedDocumento2 pagineWhat Vaccines Do BC Adults NeedCatalina VisanNessuna valutazione finora
- 302 RUA - Interview WorksheetDocumento4 pagine302 RUA - Interview WorksheetChristy RobinettNessuna valutazione finora
- P.E 11 Quiz 1Documento3 pagineP.E 11 Quiz 1Gilbert ObingNessuna valutazione finora
- Epiglottitis and LaryngitisDocumento9 pagineEpiglottitis and Laryngitisputri balqisNessuna valutazione finora