Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Hepatitis
Caricato da
Thomas Utomo0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
87 visualizzazioni33 pagineThis document discusses hepatitis, which is an infection affecting the liver. It is predominantly caused by five viruses - Hepatitis A, B, C, D, and E. These viruses present clinically similar illnesses ranging from asymptomatic to fulminant liver failure. Hepatitis A and E are usually self-limiting while Hepatitis B, C and D can lead to chronic liver disease. The document covers the virology, pathogenesis, clinical presentation and diagnosis of each viral hepatitis type.
Descrizione originale:
penyakit dalam
Copyright
© © All Rights Reserved
Formati disponibili
PPTX, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoThis document discusses hepatitis, which is an infection affecting the liver. It is predominantly caused by five viruses - Hepatitis A, B, C, D, and E. These viruses present clinically similar illnesses ranging from asymptomatic to fulminant liver failure. Hepatitis A and E are usually self-limiting while Hepatitis B, C and D can lead to chronic liver disease. The document covers the virology, pathogenesis, clinical presentation and diagnosis of each viral hepatitis type.
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
87 visualizzazioni33 pagineHepatitis
Caricato da
Thomas UtomoThis document discusses hepatitis, which is an infection affecting the liver. It is predominantly caused by five viruses - Hepatitis A, B, C, D, and E. These viruses present clinically similar illnesses ranging from asymptomatic to fulminant liver failure. Hepatitis A and E are usually self-limiting while Hepatitis B, C and D can lead to chronic liver disease. The document covers the virology, pathogenesis, clinical presentation and diagnosis of each viral hepatitis type.
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 33
Hepatitis
Acute viral hepatitis
systemic infection affecting the liver predominantly
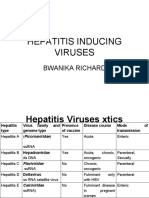
Etiology:
Hepatitis A virus (HAV)
Hepatitis B virus (HBV)
Hepatitis C virus = HBV-associated delta agent (HCV)
Hepatitis D virus (HDV)
Hepatitis E virus (HEV)
All are RNA virus, except HBV DNA virus, replicated like retrovirus.
Although these agents can be distinguished by their molecular and
antigenic properties, all types of viral hepatitis produce clinically similar
illnesses.
These range from asymptomatic and inapparent to fulminant and
fatal acute infections common to all types, on the one hand, and from
subclinical persistent infections to rapidly progressive chronic liver
disease with cirrhosis and even hepatocellular carcinoma, common to
the bloodborne types (berenvelope, rusak dgn pajanan detergen &
empedu, tidak ada di tinja) (HBV, HCV, and HDV), on the other.
Enteric borne HAV, HEV
Virology Hepatitis A
Hepatitis A Virus
Nonenveloped, 27nm, heat-, acid-, and ether resistant
RNA virus in the Hepatovirus genus of the picornavirus family.
Virion contains four capsid polypeptides, designated VP1 to VP4.
Inactivation of viral activity can be achieved by boiling for 1 min, by
contact with formaldehyde and chlorine, or by ultraviolet irradiation.
Pathogenesis-Pathophysiology
Hepatitis A has an incubation period of ~4 weeks.
Its replication is limited to the liver, but the virus is present in the liver,
bile, stools, and blood during the late incubation period and acute
preicteric/ presymptomatic phase of illness.
Despite slightly longer persistence of virus in the liver, fecal shedding,
viremia, and infectivity diminish rapidly once jaundice becomes
apparent.
Antibodies to HAV (anti-HAV) can be detected during acute illness
when serum aminotransferase activity is elevated and fecal HAV
shedding is still occurring.
This early antibody response is predominantly of the IgM class and persists for
several (~3) months, rarely for 612 months.
During convalescence, however, anti-HAV of the IgG classbecomes the
predominant antibody
Therefore, the diagnosis of hepatitis A is made during acute illness by
demonstrating anti-HAV of the IgM class
After acute illness, anti-HAV of the IgG class remains detectable indefinitely, and
patients with serum anti-HAV are immune to reinfection.
Virology Hepatitis B
HBV is a DNA virus with a remarkably compact genomic structure;
despite its small, circular, 3200-bp size, HBV DNA codes for four sets
of viral products with a complex, multiparticle structure.
HBV is now recognized as one of a family of animal viruses,
hepadnaviruses (hepatotropic DNA viruses), and is classified as
hepadnavirus type 1.
The envelope protein expressed on the outer surface of the virion and
on the smaller spherical and tubular structures is referred to as
hepatitis B surface antigen (HBsAg)
The antigen expressed on the surface of the nucleocapsid core is
hepatitis B core antigen (HBcAg), and its corresponding antibody is
anti-HBc.
A third HBV antigen is hepatitis B e antigen (HBeAg), a soluble,
nonparticulate, nucleocapsid protein.
HBsAg-positive serum containing HBeAg is more likely to be highly
infectious and to be associated with the presence of hepatitis B
virions (and detectable HBV DNA) than HBeAg-negative or anti-HBe-
positive serum.
Serologic and virologic markers
After a person is infected with HBV, the first virologic marker
detectable in serum within 112 weeks, usually between 8 and 12
weeks, is HBsAg.
Circulating HBsAg precedes elevations of serum aminotransferase
activity and clinical symptoms by 26 weeks and remains detectable
during the entire icteric or symptomatic phase of acute hepatitis B
and beyond.
In typical cases, HBsAg becomes undetectable 12 months after the
onset of jaundice and rarely persists beyond 6 months.
After HBsAg disappears, antibody to HBsAg (anti-HBs) becomes
detectable in serum and remains detectable indefinitely thereafter.
Because HBcAg is intracellular and, when in the serum, sequestered
within an HBsAg coat, naked core particles do not circulate in serum,
and therefore, HBcAg is not detectable routinely in the serum of
patients with HBV infection.
By contrast, anti-HBc is readily demonstrable in serum, beginning
within the first 12 weeks after the appearance of HBsAg and
preceding detectable levels of anti-HBs by weeks to months.
Because variability exists in the time of appearance of anti-HBs after
HBV infection, occasionally a gap of several weeks or longer may
separate the disappearance of HBsAg and the appearance of anti-HBs.
During this gap or window period, anti-HBc may represent the
only serologic evidence of current or recent HBV infection, and blood
containing anti-HBc in the absence of HBsAg and anti-HBs has been
implicated in transfusion-associated hepatitis B
Virology Hepatitis D
The delta hepatitis agent, or HDV, the only member of the genus Deltavirus,
is a defective RNA virus that co-infects with and requires the helper function
of HBV (or other hepadnaviruses) for its replication and expression.
Slightly smaller than HBV, HDV is a formalin-sensitive, 35- to 37-nm virus
with a hybrid structure.
Its nucleocapsid expresses HDV antigen (HDAg), which bears no antigenic
homology with any of the HBV antigens, and contains the virus genome.
The HDV core is encapsidated by an outer envelope of HBsAg,
indistinguishable from that of HBV except in its relative compositions of
major, middle, and large HBsAg component proteins.
HDV can either infect a person simultaneously with HBV (coinfection)
or superinfect a person already infected with HBV (superinfection).
When HDV infection is transmitted from a donor with one HBsAg
subtype to an HBsAg-positive recipient with a different subtype, HDV
assumes the HBsAg subtype of the recipient, rather than the donor.
Because HDV relies absolutely on HBV, the duration of HDV infection
is determined by the duration of (and cannot outlast) HBV infection.
HDV replication tends to suppress HBV replication; therefore, patients
with hepatitis D tend to have lower levels of HBV replication.
HDV antigen is expressed primarily in hepatocyte nuclei and is
occasionally detectable in serum.
During acute HDV infection, anti-HDV of the IgM class predominates,
and 3040 days may elapse after symptoms appear before anti-HDV
can be detected.
In self-limited infection, anti-HDV is low-titer and transient, rarely
remaining detectable beyond the clearance of HBsAg and HDV
antigen.
In chronic HDV infection, anti-HDV circulates in high titer, and both
IgM and IgG anti-HDV can be detected.
HDV antigen in the liver and HDV RNA in serum and liver can be
detected during HDV replication.
Virology Hepatitis C
Hepatitis C virus, which, before its identification was labelled non-A,
non-B hepatitis, is a linear, single-strand, positive-sense, 9600-
nucleotide RNA virus, the genome of which is similar in organization
to that of flaviviruses and pestiviruses.
HCV is the only member of the genus Hepacivirus in the family
Flaviviridae.
Virology Hepatitis E
Previously labeled epidemic or enterically transmitted non-A, non-B
hepatitis, HEV is an enterically transmitted virus that causes clinically
apparent hepatitis primarily in India, Asia, Africa, and Central
America; in those geographic areas, HEV is the most common cause
of acute hepatitis.
HEV is a 27- to 34-nm, nonenveloped, HAV-like virus with a 7200-
nucleotide, single-strand, positive-sense RNA genome.
Contributing to the perpetuation of this virus are animal reservoirs,
most notably in swine.
The virus has been detected in stool, bile, and liver and is excreted in
the stool during the late incubation period.
Both IgM anti-HEV during early acute infection and IgG anti-HEV
predominating after the first 3 months can be detected.
Currently, availability and reliability of serologic/virologic testing for
HEV infection is limited but can be done in specialized laboratories.
Gejala Klinik
Fase inkubasi Asimptomatik kondisi fatal gagal
hati akut
Fase prodromal
Malaise, anoreksia, mual, muntah
Fase icterus Gejala flu, faringitis akut, fotofobia,
Fase konvalesen myalgia, sakit kepala
Demam (pd HAV)
Ikterus pd kulit dan mukosa, urin
berwarna gelap, pruritus saat icterus
meningkat
PF: hepatomegaly, nyeri tekan,
splenomegaly, limfadenopati (15-20%)
Terapi non medikamentosa
Rawat jalan kecuali mual dan anorexia berat hingga dehidrasi
Hindari konsumsi alcohol
Hindari aktivitas fisik berat, batasi aktivitas fisik tergantung derajat
malaise
Terapi Medikamentosa
Self-limiting disease HAV
Hepatoprotektors
Hepatitis Kronis
Infeksi hepar yg berlangsung > 6 bulan
Hepatitis B kronis HbsAg positif > 6 bulan, peningkatan persisten
SGOT & SGPT, serum HBV DNA 106 kopi/ml
Hepatitis C kronis anti-HCV positif, HVC RNA positif, SGPT
meningkat min 6 bulan
HBV & HCV
Transmisi: IVDU
Darah Transfusi darah
Saliva Transplantasi dr orang terinfeksi
Semen
Bayi lahir dari ibu yg positif
Sekret vagina
ASI Pasien HD
Multiple sexual partner
Laboratory test for HBV
Medikamentosa
Interferon
Dewasa: 5 MU sehari atau 10 MU 3x seminggu
Anak: 6 MU 3x seminggu max 10 MU
Durasi terapi:
Hepatitis B kronis HbeAg negative 12-24 bulan
Hepatitis B kronis HbeAg positif 16-32 minggu
Diberikan scr SC
Lamivudine
Adenofir
Entecavir
Telbivudine
Tenofovir
Komplikasi
Fullminan hepatitis
Sirosis hepatis
Hepatocellular carcinoma
Potrebbero piacerti anche
- Med Surg Test 4 Study GuideDocumento29 pagineMed Surg Test 4 Study GuideJessNessuna valutazione finora
- Viral HepatitisDocumento51 pagineViral HepatitisIlmiah BagusNessuna valutazione finora
- Viral Hepatitis PC II 2023Documento76 pagineViral Hepatitis PC II 2023Suhayb CumarNessuna valutazione finora
- Viral HepatitisDocumento58 pagineViral HepatitisKathrine SiahaanNessuna valutazione finora
- Viral Hepatitis: Reading AssignmentDocumento51 pagineViral Hepatitis: Reading AssignmentNadya VanessaNessuna valutazione finora
- Infections of The Gastrointestinal TractDocumento32 pagineInfections of The Gastrointestinal Tract180045Nessuna valutazione finora
- 1 HepatitisDocumento62 pagine1 HepatitisKamal AhmedNessuna valutazione finora
- Viral Hepatitis: DR - Abiy F. Nov 2019 Arsi UniversityDocumento67 pagineViral Hepatitis: DR - Abiy F. Nov 2019 Arsi UniversityWakjira NigusuNessuna valutazione finora
- Hepatitis Viruses: Dr. Muna. M. A. Yousif M.D Clinical MicrobiologyDocumento45 pagineHepatitis Viruses: Dr. Muna. M. A. Yousif M.D Clinical MicrobiologyMAxeneNessuna valutazione finora
- Hepatitis 1 (Viral Hepatitis)Documento47 pagineHepatitis 1 (Viral Hepatitis)Louis TanNessuna valutazione finora
- HepatitisDocumento29 pagineHepatitisRose Anne AbivaNessuna valutazione finora
- Hepatitis VirusesDocumento26 pagineHepatitis VirusesRachel SinghNessuna valutazione finora
- HepatitisDocumento24 pagineHepatitisAnn MariaNessuna valutazione finora
- 8.hepatitis VirusesDocumento33 pagine8.hepatitis VirusesShaibin MuhammadNessuna valutazione finora
- Hepato-Billiary Diseases: Tutor: DR SocdaalDocumento32 pagineHepato-Billiary Diseases: Tutor: DR SocdaalOmar mohamedNessuna valutazione finora
- Acute Liver FailureDocumento29 pagineAcute Liver FailureSamuel kuriaNessuna valutazione finora
- Dr. G. Thiruvenkadam Post Graduate Dept of Pediatric & Preventive DentistryDocumento31 pagineDr. G. Thiruvenkadam Post Graduate Dept of Pediatric & Preventive Dentistryதிருவேங்கடம் கோபாலன்Nessuna valutazione finora
- Infectious Gastrointestinal Diseases: MicrobiologyDocumento37 pagineInfectious Gastrointestinal Diseases: MicrobiologyRakesh KumarNessuna valutazione finora
- Viral Hepatitis: References: Harrisons Infectious Disease 2 Ed., Oxford Handbook of Microbiology and IdDocumento58 pagineViral Hepatitis: References: Harrisons Infectious Disease 2 Ed., Oxford Handbook of Microbiology and IdMohammad Emad Al MadadhaNessuna valutazione finora
- Viral Hepatitis Final PPDocumento66 pagineViral Hepatitis Final PPTESFAYE YIRSAWNessuna valutazione finora
- Muhammad Asaad Maidin Departement Microbiology Faculty of Medicine Hasanuddin University, MakassarDocumento54 pagineMuhammad Asaad Maidin Departement Microbiology Faculty of Medicine Hasanuddin University, MakassarPratiwi PurnamaNessuna valutazione finora
- Hepatitis VirusesDocumento19 pagineHepatitis VirusesFort SalvadorNessuna valutazione finora
- 1010 M Balm - Viral HepatitisDocumento17 pagine1010 M Balm - Viral HepatitisSaad KhanNessuna valutazione finora
- Hepatitis A-E Viruses: An OverviewDocumento49 pagineHepatitis A-E Viruses: An OverviewDeepak VermaNessuna valutazione finora
- HEPATITIS Compilation (From Various Sources)Documento44 pagineHEPATITIS Compilation (From Various Sources)Cathy TajaoNessuna valutazione finora
- Hepatitis A GDocumento23 pagineHepatitis A Gapi-3712326Nessuna valutazione finora
- Viral HepatitisDocumento6 pagineViral HepatitisangelarainNessuna valutazione finora
- Hepatitis: Dr. Amany A. GhazyDocumento44 pagineHepatitis: Dr. Amany A. GhazyJosé Luis García GarcíaNessuna valutazione finora
- Hepatitis A, D, E & GDocumento28 pagineHepatitis A, D, E & GsaleemNessuna valutazione finora
- Hepatitis VirusesDocumento23 pagineHepatitis Viruses4jzbxz64kqNessuna valutazione finora
- Viral HepatitisDocumento73 pagineViral HepatitisDownerofHeadsNessuna valutazione finora
- Hepatitis VirusDocumento83 pagineHepatitis VirusRudresh Shoorashetty ManoharNessuna valutazione finora
- Hepatitis Viruses Combination (Blood Borne Pathogens)Documento51 pagineHepatitis Viruses Combination (Blood Borne Pathogens)Hosam GomaaNessuna valutazione finora
- Hepatitis B - Virology: DNA Virus Class Hepadnaviridae TransmissionDocumento6 pagineHepatitis B - Virology: DNA Virus Class Hepadnaviridae TransmissionDominic Delos SantosNessuna valutazione finora
- HepatitisDocumento19 pagineHepatitisDayana PrasanthNessuna valutazione finora
- Acute & Chronic HepatitisDocumento65 pagineAcute & Chronic HepatitisMahmoud AjinehNessuna valutazione finora
- Viral Hepatitis & HIVDocumento14 pagineViral Hepatitis & HIVaymnhssn2020Nessuna valutazione finora
- 3 Acute Viral HepatitisDocumento52 pagine3 Acute Viral HepatitismusabNessuna valutazione finora
- Viral Hepatitis-Dr. A.M IyagbaDocumento62 pagineViral Hepatitis-Dr. A.M IyagbaDr. Amb. Monday ZaccheausNessuna valutazione finora
- Hepatitis 1Documento40 pagineHepatitis 1Noelle Grace Ulep BaromanNessuna valutazione finora
- By: Hasan Suleiman Artem LorensDocumento35 pagineBy: Hasan Suleiman Artem LorenssgolbariNessuna valutazione finora
- Virus Hepatitis RevDocumento83 pagineVirus Hepatitis RevSukma WinahyuNessuna valutazione finora
- Viral Hepatitis Training Manual: Federal Ministry of Health National Hepatitis Control Program 2017Documento44 pagineViral Hepatitis Training Manual: Federal Ministry of Health National Hepatitis Control Program 2017Eleni HagosNessuna valutazione finora
- Hepatitis Viruses: VIRUS:Hepatitis A, B, CDocumento25 pagineHepatitis Viruses: VIRUS:Hepatitis A, B, Carisita firmanNessuna valutazione finora
- Hepatitis A /BDocumento79 pagineHepatitis A /BnasibdinNessuna valutazione finora
- Hepatitis B & DDocumento40 pagineHepatitis B & DMeena CtNessuna valutazione finora
- Microbiology and Parasitology 100: Trinity University of Asia St. Luke's College of NursingDocumento11 pagineMicrobiology and Parasitology 100: Trinity University of Asia St. Luke's College of NursingFereli Joy SupanNessuna valutazione finora
- Hepatitis B Virus and Hepatitis C Virus Co-Infection With HIVDocumento54 pagineHepatitis B Virus and Hepatitis C Virus Co-Infection With HIVShree Narayan YadavNessuna valutazione finora
- TASH CI HepatitisDocumento47 pagineTASH CI HepatitisBeamlak Getachew WoldeselassieNessuna valutazione finora
- Hepatitis VirusesDocumento35 pagineHepatitis VirusesRaja RuzannaNessuna valutazione finora
- Viral Hepatitis (Virus Hepatitis)Documento75 pagineViral Hepatitis (Virus Hepatitis)Ilmiah Bagus100% (1)
- Hepatitis Virus: Bagian Mikrobiologi FK UnissulaDocumento36 pagineHepatitis Virus: Bagian Mikrobiologi FK UnissulaKarina Mega WNessuna valutazione finora
- Jaundice and Hepatitis in Children: Dr. MwendwaDocumento46 pagineJaundice and Hepatitis in Children: Dr. MwendwaAlvin OmondiNessuna valutazione finora
- Viral InfectionsDocumento59 pagineViral Infectionsrenato renatoNessuna valutazione finora
- Hepatologi 1 (CMP)Documento61 pagineHepatologi 1 (CMP)Yun ZhaNessuna valutazione finora
- Serology of Viral Infections PDFDocumento72 pagineSerology of Viral Infections PDFAffie SaikolNessuna valutazione finora
- 2 Hepatitis VirusDocumento31 pagine2 Hepatitis VirusDr. Md. Abdullah YusufNessuna valutazione finora
- Hepatitis B: Steve HartDocumento36 pagineHepatitis B: Steve HartangelinaNessuna valutazione finora
- Hepatitis VirusesDocumento35 pagineHepatitis Virusesm dawoodNessuna valutazione finora
- Hepatitis B Virus and Liver DiseaseDa EverandHepatitis B Virus and Liver DiseaseJia-Horng KaoNessuna valutazione finora
- Case Presentation: Paediatrics: by Tapan Jyoti Saikia 8 Sem Gauhati Medical CollegeDocumento22 pagineCase Presentation: Paediatrics: by Tapan Jyoti Saikia 8 Sem Gauhati Medical CollegeArpit Mehta100% (1)
- Hepatitis A /BDocumento79 pagineHepatitis A /BnasibdinNessuna valutazione finora
- MLSP Lecture Finals ReviewerDocumento22 pagineMLSP Lecture Finals ReviewerAkira Anne KreyceNessuna valutazione finora
- Bachelor of Science in Nursing: Ncmb316 Rle: RLE RLE Unit WeekDocumento4 pagineBachelor of Science in Nursing: Ncmb316 Rle: RLE RLE Unit WeekMaica LectanaNessuna valutazione finora
- Ch. 25 Body Defence MechanismsDocumento34 pagineCh. 25 Body Defence Mechanisms吴昊Nessuna valutazione finora
- Literature Review On Hepatitis B VirusDocumento5 pagineLiterature Review On Hepatitis B Virusafmzeracmdvbfe100% (1)
- GIT and LiverDocumento28 pagineGIT and LiverUsmanNessuna valutazione finora
- Pediatric Hepatocelullar CarcinomaDocumento21 paginePediatric Hepatocelullar Carcinomamoh.ikhsanzNessuna valutazione finora
- Understanding The Serology of Hepatitis B VirusDocumento8 pagineUnderstanding The Serology of Hepatitis B VirusQurat-Ul-Ain tariqNessuna valutazione finora
- MR - Mohankumar ReportDocumento3 pagineMR - Mohankumar ReportJayaprabhu Prabhu0% (1)
- Epidemiology of Infectious DiseasesDocumento69 pagineEpidemiology of Infectious Diseasesmus zaharaNessuna valutazione finora
- HepatitisDocumento39 pagineHepatitisRahmiati LaoNessuna valutazione finora
- Qand ADocumento5 pagineQand AJoshua PascasioNessuna valutazione finora
- Foresight HBsAg I231 1021 English Insert 070115Documento2 pagineForesight HBsAg I231 1021 English Insert 070115Rajkishor YadavNessuna valutazione finora
- Mcqs Ahn PDFDocumento11 pagineMcqs Ahn PDFMhr AliNessuna valutazione finora
- Blood Bank 2Documento21 pagineBlood Bank 2moonfire2009Nessuna valutazione finora
- Hepatitis B (HBV) : 2-Months RegimenDocumento20 pagineHepatitis B (HBV) : 2-Months Regimenulovemusicsodoi7799Nessuna valutazione finora
- Virus Liver Hepatitis: What Is Hepatitis B?Documento2 pagineVirus Liver Hepatitis: What Is Hepatitis B?Victor Iv MirandaNessuna valutazione finora
- Guidelines For The Management of Occupational Exposures To HBV, HCV, and HIV and Recommendations For Postexposure ProphylaxisDocumento58 pagineGuidelines For The Management of Occupational Exposures To HBV, HCV, and HIV and Recommendations For Postexposure ProphylaxisvenkayammaNessuna valutazione finora
- Romeo and Juliet Death EssayDocumento5 pagineRomeo and Juliet Death EssayiygcdknbfNessuna valutazione finora
- Communicable Disease 2 AnswersDocumento14 pagineCommunicable Disease 2 AnswersRika MaeNessuna valutazione finora
- MD Occupational Health ProtocolDocumento6 pagineMD Occupational Health ProtocolGareth GrechNessuna valutazione finora
- Quiz Blood Born Pathogen Refresher Mix Quiz Non ECU Employees and Students and Temporary StaffDocumento4 pagineQuiz Blood Born Pathogen Refresher Mix Quiz Non ECU Employees and Students and Temporary Staffvipin khatriNessuna valutazione finora
- v2 SD BIOLINE Hepatitis Products CatalogueDocumento8 paginev2 SD BIOLINE Hepatitis Products CatalogueBrajhan GrimaldosNessuna valutazione finora
- Hepatitis B - DOLEDocumento23 pagineHepatitis B - DOLEMary Rose VirtucioNessuna valutazione finora
- Acute Viral Hepatitis (Final)Documento5 pagineAcute Viral Hepatitis (Final)Kim LompotNessuna valutazione finora
- Hepati Tac AbstractDocumento296 pagineHepati Tac AbstractMagda MagNessuna valutazione finora
- Lecture 8 - SCI 8007SEF Medical Microbiology & Virology-Virology II - 2023Documento76 pagineLecture 8 - SCI 8007SEF Medical Microbiology & Virology-Virology II - 2023YY CheungNessuna valutazione finora
- Recombinant Vaccine: Neethu AsokanDocumento29 pagineRecombinant Vaccine: Neethu AsokanShivraj JadhavNessuna valutazione finora