Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
BB, CCB
Caricato da
Al Hijjah Fadhilah0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
34 visualizzazioni47 paginecardio
Copyright
© © All Rights Reserved
Formati disponibili
PPT, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentocardio
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPT, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
34 visualizzazioni47 pagineBB, CCB
Caricato da
Al Hijjah Fadhilahcardio
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPT, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 47
Beta Blocker
blockers are used for a number of
cardiovascular conditions, including ischemic
heart disease, hypertension, heart failure, and
tachyarrhytmias.
blockers decrease inotropy, slow heart rate, and
decrease conduction velocity.
1-adrenergic receptors are primarily located on
the surface of the myocardium
2-adrenergic receptors are primarily located on
the vascular and bronchial smooth muscle
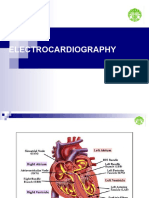
Pathophysiology of the heart
Lionel Opie, Drugs for the heart
1. Ischemic Heart Disease
Blockade is usually started early
Blockers are often combined with nitrate
vasodilators and calcium channel blockers (CCBs)
in the therapy of angina
Chronic Il-blockade increases B-receptor density.
When P-blockers are suddenly withdrawn, angina
may be exacerbated, sometimes resulting in
myocardial infarction.
Printzmetals variant angina B blocker is
ineffective and even harmful
STEMI
Early STEMI
American Heart Association (AHA) guidelines
recommend starting half-dose oral b-blockade
on day 2 (assuming hemodynamic stability)
followed by dose increase to the full or the
maximum tolerated dose, followed by long-
term postinfarct b-blockade
Postinfarction
Administer b-blockade for all postinfarct
patients with an ejection fraction (EF) of 40%
or less unless contraindicated,
Administer b-blockade for 3 years in patients
with normal LV function after AMI or ACS.
the Thrombolysis in Myocardial Infarction (TIMI)-II-
B trial, patients with ACS treated with fibrinolysis
were randomized to receive immediate treatment
with -blockers (metoprolol 5 mg IV) or deferred
treatment. After 6 weeks of follow-up, there was
no difference in the primary outcome of mortality
between the 2 groups. There was, however, a
lower incidence of recurrent chest pain (18.8 vs.
24.1%) and recurrent infarction (2.7 vs. 5.1%) in
the patients that received immediate treatment
with -blockade
These findings were reproduced with atenolol in a
post hoc analysis of the Global Utilization of
Streptokinase and Tissue Plasminogen Activator
for Occluded Coronary Arteries-1 (GUSTO-1)
database. It is important to note that this trial
demonstrated a slightly increased risk of heart
failure.
The most recent randomized trial evaluating the
use of intravenous metoprolol for ACS included
45,852 patients in Asia [Clopidogrel and
Metoprolol in Myocardial Infarction Trial
(COMMIT)]. The majority of this population
presented with ECG evidence of STEMI (93%) and
were randomized to receive immediate treatment
with intravenous -blockers (metoprolol 5 mg IV)
followed by oral metoprolol (200 mg daily) or
placebo.
The primary combined composite end-point of
death, reinfarction, or cardiac arrest was
equivalent between the 2 groups (9.4 vs. 9.9%).
Treatment with -blockers did result, however, in
a reduction in the rate of reinfarction (2.0 vs.
2.5%) as well as an increase in the rate of
cardiogenic shock (5.0 vs. 3.9%). Based on this
data, greater caution is now suggested in the
routine use of intravenous -blockers for ACS. In
particular, these agents should be avoided in
patients with clinical evidence of heart failure or
hemodynamic instability
In the last 10 years, the U.S. carvedilol trials,
Carvedilol Prospective Randomized Cumulative
Survival (COPERNICUS), and Effect of Carvedilol on
Outcome After Myocardial Infarction in Patients with
Left Ventricular Dysfunction (CAPRICORN), all
explored the benefits of the selective beta-blocker,
carvedilol, in the polypharmacy environment of
patients with heart failure. The former two studies
were in heart failure populations with reduced left
ventricular ejection fraction (LVEF); the CAPRICORN
trial studied a post-AMI population with low LVEF
(40%).
The SAVE trial showed that ACE
inhibitors and blockade are additive in
reducing postinfarct mortality, at least
in patients wilh reduced ejection
fractions. The benefit of blockade when
added to cotherapy wilh ACE inhibitors
is a mortality reduction of 23% to 40%
2. Hypertension
B-Blockers are no longer recommended as first-line
treatment for hypertension.
JNC7 lists the following as 'compelling indications
for the use of B-blockers in hypertension: heart
failure, post-MI hypertension, high coronary risk,
and diabetes
Hypertension plus effort angina : risk of new
diabetes.
Older patient : B Blockade reduces the central
aortic pressure
INVEST study, in 6391 patients with
hypertension and coronary artery
disease followed for more than 2 years,
the b-blocker atenolol gave similar
major cardiovascular outcomes to the
nondihydropyridine CCB verapamil, and
yet the b-blocker group had more
anginal episodes, new diabetes, and
psychological depression
3. Heart failure
3. Heart failure
Trials in patients with all classes of clinically stable
heart failure have actually shown a survival benefit
with chronic B-blocker administration using
carvedilol, metoprolol, or bisoprolol.
The mechanism may relate to blunting of
cardiotoxic effects of excesive circulating
cathecolamines.
The therapy should be started at low dosage,
augmented slowly, and carefully monitored
The first large, prospective, comparative trial of a
beta-blocker vs an angiotensin-converting enzyme
(ACE) inhibitor as initial therapy in patients with
congestive heart failure (CHF), the Cardiac
Insufficiency Bisoprolol Study III (CIBIS III), has
shown that initiating treatment with the selective
beta-1 receptor blocker bisoprolol is as effective
and well tolerated as beginning treatment with the
ACE inhibitor enalapril. Results of CIBIS III,
presented at the European Society of Cardiology
(ESC) Congress 2005[1]and published
simultaneously inCirculation,also suggest that
starting treatment with bisoprolol may reduce the
risk of death, especially in the first year of
treatment.
the COMET trial; carvedilol reduced
mortality more than metoprolol. Thus far
there is no evidence that diastolic heart
failure improves.
For every heart rate reduction of 5
beats/min with b-blockade, there is an
18% reduction (cardiac index, 6%-29%)
in the risk for death as occurred in the
23 b-blocker trials in 19,209 patients, of
whom more than 95% had systolic
dysfunction
4. Antiarrhytmias
B-blocker decreased slope of phase 4
depolarization reduce automaticity
B-blocker increase the effective refractory periode
of the AV node reduce reentry
b-blockade may help in the prophylaxis of SVTs by
inhibiting the initiating atrial ectopic beats and in
the treatment of SVT by slowing the AV node and
lessening the ventricular response rate
In patients with atrial fibrillation, current
management practices often aim at control of
ventricular rate (rate control)
a retrospective analysis of data from the CAST
study shows that B-blockade reduced all cause
mortality and arrhythmia deaths
Other cardiac indication
Hypertrophic obstructive cardiomyopathy
high dose propanolol
Mitral stenosis with sinus rhythm
decreasing resting and exercise heart rates
Mitral valve prolapse for control of
associated arrhythmias
Dissecting aneurysms propanonol IV, but
could be replaced by esmolol.
TOF 2mg/kg twice daily effective against
cyanotic spells
Adverse Effects
1. B-blocker non selective agents (or large doses of
B1 selective blockers) can exacerbate
bronchospasm
2. The impairment of AV nodal conduction by B-
blockade can cause conduction blocks.
3. B-blocker can precipitate arterial vasospasm
worsening PAD
4. Abrubt withdrawal of a B-blocker after chronic
use could precipitate myocardial ischemia in
patients with CAD.
5. Reduce HDL and increase triglyseride
6. B2 blockade may impair recovery from
hypoglycemia in diabetics suffering in insulin
reaction.
Calcium
Channel
Blocker
Calcium channel blockers (CCBs; calcium
antagonists) act chiefly by vasodilation and
reduction of the peripheral vascular resistance
CCBs have ability to impede the influx of calcium
through membrane channels in cardiac and
smooth muscle.
CCBs reduce myocardial contractility resulting in
a reduction in myocardial oxygen demand.
CCBs also dilate the epicardial coronary arteries
resulting in an increase in myocardial oxygen
supply
CCBs are particularly effective in elderly patients.
Major indications
Stable effort angina
Unstable angina verapamil
Coronary spasm
Hypertensionbest for older and black
patients
SVT inhibit the AV node
Postinfact protection verapamil
Verapamil
Oral verapamil takes 2 hours to act and
peaks at 3 hours
The elimination half-life is usually 3 to 7
hours
Dose is 180-360 mg daily
Side effects of verapamil causing
headaches, facial flushing, and
dizziness.
Diltiazem
The onset of action of short-acting diltiazem is
within 15 to 30 minutes (oral), with a peak at 1
to 2 hours. The elimination half-life is 4 to 7
hours.
The dose of diltiazem is 120 to 360 mg, given in
four daily doses of the short-acting formulation
or once or twice a day with slow-release
preparations.
Normally side effects of the standard
preparation are few and limited to headaches,
dizziness, and ankle edema
Amlodipin
Peak blood levels are reached after 6 to
12 hours, the elimination half-life is 35
to 48 hours
In women there is more edema (15%)
than in men (6%). Next in significance
are dizziness (3% to 4%) and flushing
(2% to 3%).
Clinical Trial
The Multicenter Diltiazem Postinfarction
Trial (MDPIT) randomized 2,466 patients
to diltiazem (240 mg daily) or placebo
315 days after presenting with a
myocardial infarction. After over 2 years
of follow-up, the mortality between the
2 groups was identical (13.5%) with a
nonsignificant trend toward fewer
recurrent events in patients treated with
diltiazem (16.4 vs. 18.3%)
The Danish Study Group on Verapamil in
Myocardial Infarction II (DAVIT II) randomized
almost 1,800 patients to verapamil (360 mg
daily) or placebo in the second week after
admission for ACS. Treatment with verapamil had
a nonsignificant reduction in mortality (11.1 vs.
13.8%). A meta-analysis including 19,000
patients derived from 28 independent trials
assessing the utility of calcium channel blockers
has confirmed these findings
In the aforementioned MDPIT, patients with
impaired left ventricular ejection fraction (<40%)
with evidence of pulmonary congestion on chest
radiograph, who were treated with diltiazem, had
an increased number of cardiac events and
worsened mortality. Because of this, CCBs should
be avoided in patients presenting with ACS with
concomitant left ventricular systolic dysfunction
Terima Kasih
InACTION,a large placebo-controlled trial long-
acting nifedipine in SCAD proved to be safe and
reduced the need for coronary angiography and
cardiovascular interventions
Potrebbero piacerti anche
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- JET2Documento8 pagineJET2fufuka fukalifuNessuna valutazione finora
- Morgan 2012Documento5 pagineMorgan 2012aixacamila3Nessuna valutazione finora
- EKG Clep TestDocumento13 pagineEKG Clep TestElissa LafondNessuna valutazione finora
- ECG Interpretations DR RPDocumento109 pagineECG Interpretations DR RPArnis Putri RosyaniNessuna valutazione finora
- 2019 ESC Guidelines For The Management of Patients With Supraventricular TachycardiaDocumento3 pagine2019 ESC Guidelines For The Management of Patients With Supraventricular TachycardiaBuya TaftaNessuna valutazione finora
- 50 Item Medical-Surgical Nursing Practice TestDocumento13 pagine50 Item Medical-Surgical Nursing Practice TestReymund Timog TalarocNessuna valutazione finora
- Atrium FlutterDocumento11 pagineAtrium FlutterSiti Maryam NatadisastraNessuna valutazione finora
- ARRHYTHMIADocumento82 pagineARRHYTHMIAjiluNessuna valutazione finora
- Aconitum NapellusDocumento12 pagineAconitum NapellusMuhammad Mustafa IjazNessuna valutazione finora
- Heart RhythmsDocumento68 pagineHeart Rhythmsyasahswi91Nessuna valutazione finora
- 0905 (1) When Cardiovascular Medications Become ToxinsDocumento20 pagine0905 (1) When Cardiovascular Medications Become ToxinsjojoleroNessuna valutazione finora
- Cardiomyopathy Case StudyDocumento11 pagineCardiomyopathy Case StudyJen Faye Orpilla100% (1)
- Full Report Holter Lorena M 1-23-13Documento36 pagineFull Report Holter Lorena M 1-23-13traja_vlrNessuna valutazione finora
- ECG InterpretationDocumento82 pagineECG InterpretationIin Widya Sari Siregar100% (1)
- Flash CardsDocumento35 pagineFlash CardsMihaela AlexandraNessuna valutazione finora
- ECG Short Note Chula EP PDFDocumento62 pagineECG Short Note Chula EP PDFKhuniok SixcoNessuna valutazione finora
- 2014 CCM Review Notes Jon-Emile S. Kenny M.D, 2014Documento142 pagine2014 CCM Review Notes Jon-Emile S. Kenny M.D, 2014PkernNessuna valutazione finora
- Electrocardiography (ECG) Recording and InterpretationDocumento59 pagineElectrocardiography (ECG) Recording and Interpretationkhushsandhu0% (1)
- Atypical Bypass Tracts 2019Documento21 pagineAtypical Bypass Tracts 2019Võ Từ NhấtNessuna valutazione finora
- 9515-184-51-ENG - REV - B1 HScribe Clinicians Guide V5 - 01Documento48 pagine9515-184-51-ENG - REV - B1 HScribe Clinicians Guide V5 - 01Rodrigo GutierrezNessuna valutazione finora
- Conduction System of HeartDocumento2 pagineConduction System of HeartEINSTEIN2DNessuna valutazione finora
- CVD and HTNDocumento60 pagineCVD and HTNZsazsa100% (1)
- Basic ECG Analysis and Interpretation SkillsDocumento46 pagineBasic ECG Analysis and Interpretation SkillsSumeet TripathiNessuna valutazione finora
- PacemakersDocumento28 paginePacemakersliang2012Nessuna valutazione finora
- Monitor F. Vitales Philips MP40-50 IntelliVueDocumento390 pagineMonitor F. Vitales Philips MP40-50 IntelliVuechejo84100% (1)
- Supraventricular Tachycardia: Arun Umesh Mahtani,, Devi Gopinath NairDocumento17 pagineSupraventricular Tachycardia: Arun Umesh Mahtani,, Devi Gopinath Nairwindar baquero100% (1)
- Cardiac DysrhythmiasDocumento6 pagineCardiac DysrhythmiasJeffrey Viernes100% (1)
- Ecg ReadingDocumento6 pagineEcg ReadingMarianette CainongNessuna valutazione finora
- E - Cart DrugsDocumento18 pagineE - Cart Drugs'SheenMarkReal'100% (2)
- ACLS-Study-Guide-2011 MADE EASYDocumento2 pagineACLS-Study-Guide-2011 MADE EASYFrances Albaña TevesNessuna valutazione finora