Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Giant Cell Tumor
Caricato da
Maxmillian Alexander Kawilarang0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
64 visualizzazioni22 pagineGiant cell tumor of bone is a rare, locally aggressive bone lesion that typically occurs in the epiphyses of long bones in young adults. It appears lytic on x-ray and is composed of multinucleated giant cells and monocyte-macrophage stromal cells. While usually benign, it can rarely metastasize or transform into a high-grade sarcoma. Treatment involves thorough curettage and bone grafting, with possible adjuvants like liquid nitrogen or cement. Recurrence rates can be high depending on location.
Descrizione originale:
ppt GCT
Copyright
© © All Rights Reserved
Formati disponibili
PPTX, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoGiant cell tumor of bone is a rare, locally aggressive bone lesion that typically occurs in the epiphyses of long bones in young adults. It appears lytic on x-ray and is composed of multinucleated giant cells and monocyte-macrophage stromal cells. While usually benign, it can rarely metastasize or transform into a high-grade sarcoma. Treatment involves thorough curettage and bone grafting, with possible adjuvants like liquid nitrogen or cement. Recurrence rates can be high depending on location.
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
64 visualizzazioni22 pagineGiant Cell Tumor
Caricato da
Maxmillian Alexander KawilarangGiant cell tumor of bone is a rare, locally aggressive bone lesion that typically occurs in the epiphyses of long bones in young adults. It appears lytic on x-ray and is composed of multinucleated giant cells and monocyte-macrophage stromal cells. While usually benign, it can rarely metastasize or transform into a high-grade sarcoma. Treatment involves thorough curettage and bone grafting, with possible adjuvants like liquid nitrogen or cement. Recurrence rates can be high depending on location.
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 22
GIANT CELL TUMOR
Giant cell tumour of bone
Rare (12 per million of population
per year)
solitary,
locally aggressive lesion seen at the
epiphyseal ends of long bones
(typically distal femur 25%, proximal
tibia 25% and distal radius 10%)
in the third decade
Giant cell tumour of bone
X-ray shows an aggressive lytic
lesion in the metaphyseal/diaphyseal
part of the bone, usually juxta-
articular.
There is often complete cortical
destruction and an associated soft-
tissue mass
Giant cell tumour of bone
Histologically,
the tumour comprises spindle-
shaped tumour cells and
multinucleated giant cells which are
indistinguishable from osteoclasts.
Giant cell tumour of bone
These are recruited from the
monocytemacrophage population.
Agents which interfere with
osteoclast recruitment (e.g.
bisphosphonates and Rank-ligand
inhibitors) may be helpful in difficult
cases.
Giant cell tumour of bone
This lesion needs to be distinguished
from giant cell-rich osteosarcoma
Treatment is by curettage and
grafting and the use of a surgical
adjuvant (e.g. high-speed burr, liquid
nitrogen, cement).
Local recurrence rates can be high,
particularly in difficult sites such as
the pelvis, spine and distal radius
Giant cell tumour of bone
Malignant transformation and
metastasis is a rare but well
recognized complication.
Locally recurrent tumours are
associated with a higher risk of
metastatic disease.
Pathology
Giant-cell tumour is a lesion of uncertain
origin that appears after the end of bone
growth, most commonly in the distal
femur, proximal tibia, proximal humerus
and distal radius.
The tumour has a reddish, fleshy
appearance; it comes away in pieces
quite easily when curetted but is difficult
to remove completely from the
surrounding bone.
Pathology
Aggressive lesions have a poorly defined
floor and appear to extend into the
surrounding bone.
Histologically the striking feature is an
abundance of multinucleated giant cells
scattered on a background of stromal cells,
with little or no visible intercellular tissue.
About one-third of these tumours remain
truly benign; one-third become locally
invasive and onethird metastasize.
Clinical features
The patient is usually a young adult
who complains of pain at the end of a
long bone; sometimes there is slight
swelling.
Pathological fracture occurs in 1015
per cent of cases.
Imaging
Although this is a solid tumour, it appears
on x-ray as a cystic (i.e. radiolucent)
area situated eccentrically at the end of a
long bone.
Unlike any of the other cystic lesions, it
always extends right up to the
subchondral bone plate.
The endosteal margin is usually clear-cut,
but in invasive lesions it is illdefined.
Imaging
Considering the tumours potential for
aggressive behaviour, detailed staging
procedures are essential.
CT scans and MRI will reveal the extent of
the tumour, both within the bone and
beyond.
It is important to establish whether the
articular surface has been broached;
arthroscopymay be helpful.
Biopsy is essential.
Treatment
Well-confined, slow-growing lesions
with benign histology can safely be
treated by thorough curettage and
stripping of the cavity with burrs
and gouges, followed by swabbing
with hydrogen peroxide or by the
application of liquid nitrogen; the
cavity is then packed with bone
chips.
Treatment
More aggressive tumours, and
recurrent lesions, should be treated
by excision, followed, if necessary, by
bone-grafting or prosthetic
replacement.
Benign form
Distinctive neoplasm that has poorly
differentiated cells Benign but
aggressive
Confusion in diagnosis results
from the fact that in rare cases
(<2%), this benign tumor
metastasizes to the lungs (benign
metastasizing giant cell tumor).
Most common in the
epiphysis and
metaphysis of long
bones, and about
50% of lesions occur
about the knee; the
vertebra, sacrum,
and distal radius are
involved in about
10% of cases (Figure
9-40).
The sacrum is the most common axial
location of giant cell tumors of bone.
Unlike most bone tumors, which occur
more often in boys and men, giant cell
tumors are more common in girls and
women.
They are uncommon in children with open
physes.
Manifest with pain that is usually
referable to the joint involved
A purely lytic
destructive
lesion in the
metaphysis
that extends
into the
epiphysis and
often borders
the
subchondral
bone (Figure
9-41)
Early in the symptomatic phase, the
radiographs may appear normal; a
small lytic focus is difficult to detect.
Basic proliferating cell has a round
to oval or even spindle-shaped
nucleus (giant cells appear to have
the same nuclei as the
proliferating mononuclear cells).
Mitotic figures may be numerous.
Giant cell tumors may
undergo a number of
secondary
degenerative
changes, such as
aneurysmal bone cyst
formation, necrosis,
fibrous repair, foam
cell formation, and
reactive new bone
(Figure 9-42).
Treatment is aimed at removing the lesion,
with preservation of the involved joint.
Extensive exteriorization (removal of a large
cortical window over the lesion)
Curettage with manual and power instruments
Chemical cauterization with phenol
Area of defect is usually reconstructed with
subchondral bone grafts, methylmethacrylate,
or both.
Local control with this treatment regimen has
a success rate of 85% to 90%.
2. Malignant forms:
Primary and secondary malignant giant cell
tumors
With primary malignant giant cell tumor of
bone, a benign giant cell tumor coexists
with a high-grade sarcoma (occurs with
about 1% of giant cell tumors).
Secondary malignant giant cell tumor
occurs after irradiation to treat a giant cell
tumor or after multiple local recurrences
Potrebbero piacerti anche
- Benign Bone TumoursDocumento106 pagineBenign Bone TumoursBharath NarasimhaNessuna valutazione finora
- Hip Disorders in Children: Postgraduate Orthopaedics SeriesDa EverandHip Disorders in Children: Postgraduate Orthopaedics SeriesValutazione: 3 su 5 stelle3/5 (2)
- Bone Tumours: Natasha Eleena Nor Maghfirah Hani Farhana Nur FadhilaDocumento85 pagineBone Tumours: Natasha Eleena Nor Maghfirah Hani Farhana Nur FadhilaWan Nur AdilahNessuna valutazione finora
- Resource Unit Wound Care EnglishDocumento5 pagineResource Unit Wound Care EnglishPeterOrlinoNessuna valutazione finora
- Fracture of The Talus and Calcaneus NickDocumento43 pagineFracture of The Talus and Calcaneus NickTan Zhi HongNessuna valutazione finora
- Pelvic FractureDocumento31 paginePelvic Fracturepoe3Nessuna valutazione finora
- Adult Isthmic SpondylolisthesisDocumento21 pagineAdult Isthmic SpondylolisthesisNur RahmawatiNessuna valutazione finora
- Fracture of Radius and Ulna 3Documento38 pagineFracture of Radius and Ulna 3Noor Al Zahraa AliNessuna valutazione finora
- Avascular NecrosisDocumento58 pagineAvascular Necrosischatree100% (4)
- Distal End Humerus Fractures: BY:-Dr. Anshu Sharma Guide:-Dr.A.K. MathurDocumento76 pagineDistal End Humerus Fractures: BY:-Dr. Anshu Sharma Guide:-Dr.A.K. MathurToàn Đặng Phan VĩnhNessuna valutazione finora
- Fibrous Dysplasia & Osteofibrous Dysplasia: By: Dian KalistaDocumento35 pagineFibrous Dysplasia & Osteofibrous Dysplasia: By: Dian KalistaFerryzal OkviandaNessuna valutazione finora
- Femoral Neck FracturesDocumento8 pagineFemoral Neck FracturesMorshed Mahbub AbirNessuna valutazione finora
- All Papers Topic WiseDocumento55 pagineAll Papers Topic WiseZ TariqNessuna valutazione finora
- Thoracolumbar FracturesDocumento29 pagineThoracolumbar FracturesFernaldi Anggadha100% (1)
- Kamars RadiologyDocumento135 pagineKamars RadiologyNayantara Nair100% (1)
- B 756 Vertebris GB III10Documento44 pagineB 756 Vertebris GB III10Lukasz Bartochowski100% (1)
- Sem Osteoporosis (Edit)Documento31 pagineSem Osteoporosis (Edit)Rhomizal MazaliNessuna valutazione finora
- Management Tibial Plateau FractureDocumento45 pagineManagement Tibial Plateau FracturePurushothama Rao NalamatiNessuna valutazione finora
- AO Trauma Vol.2Documento100 pagineAO Trauma Vol.2Cujba GheorgheNessuna valutazione finora
- Bone Tumor: Daniel A. (Orthopedic Surgeon)Documento225 pagineBone Tumor: Daniel A. (Orthopedic Surgeon)mebrieNessuna valutazione finora
- 3 Column AnkleDocumento8 pagine3 Column AnkleJosé Eduardo Fernandez RodriguezNessuna valutazione finora
- DR - O. K. A. SamuelsDocumento76 pagineDR - O. K. A. Samuelsgdudex118811Nessuna valutazione finora
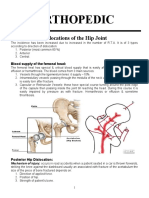
- Orthopedic: Dislocations of The Hip JointDocumento16 pagineOrthopedic: Dislocations of The Hip JointAnmarNessuna valutazione finora
- DislocationDocumento46 pagineDislocationShaa ShawalishaNessuna valutazione finora
- Syllabus Ms OrthoDocumento8 pagineSyllabus Ms OrthoMuthu KumarNessuna valutazione finora
- Benign Bone TumorDocumento42 pagineBenign Bone Tumorsaqrukuraish2187Nessuna valutazione finora
- Lect 8 Lower Extremity Fracture 2Documento22 pagineLect 8 Lower Extremity Fracture 220-221 Crisny Novika Yely Br. HutagaolNessuna valutazione finora
- Classification of Bone TumoursDocumento3 pagineClassification of Bone TumoursMalueth AnguiNessuna valutazione finora
- Spinal Trauma: Causes of Cervical Spinal Injury (UK)Documento16 pagineSpinal Trauma: Causes of Cervical Spinal Injury (UK)Mohamed Farouk El-FaresyNessuna valutazione finora
- X-Ray Rounds: (Plain) Radiographic Evaluation of The ShoulderDocumento58 pagineX-Ray Rounds: (Plain) Radiographic Evaluation of The ShoulderYeonseun KimNessuna valutazione finora
- Classification of Bone Tumors NewDocumento38 pagineClassification of Bone Tumors NewSyed WahajNessuna valutazione finora
- Shoulder Dislocation DraftDocumento26 pagineShoulder Dislocation Drafthusnajihah18Nessuna valutazione finora
- Salter Harris Classification of Growth Plate FracturesDocumento13 pagineSalter Harris Classification of Growth Plate FracturesAarón E. CaríasNessuna valutazione finora
- External Fixation Principles and Applications.5Documento8 pagineExternal Fixation Principles and Applications.5Leonardo Rocha100% (1)
- P.R.I.IN. People Readiness in (First Aid) Intervention: - Bone and Joint InjuriesDocumento35 pagineP.R.I.IN. People Readiness in (First Aid) Intervention: - Bone and Joint InjurieschristopherNessuna valutazione finora
- 1.26 (Surgery) Orthopedic Pathology - OncologyDocumento7 pagine1.26 (Surgery) Orthopedic Pathology - OncologyLeo Mari Go LimNessuna valutazione finora
- Medlung Deformity: D D K SDocumento5 pagineMedlung Deformity: D D K SManish MauryaNessuna valutazione finora
- Chapter 25: Trauma: (Also See Chapter 19, Pediatrics)Documento70 pagineChapter 25: Trauma: (Also See Chapter 19, Pediatrics)poddataNessuna valutazione finora
- Trochanteric #Documento20 pagineTrochanteric #Prakash AyyaduraiNessuna valutazione finora
- Distal Femur (Sandeep Sir)Documento22 pagineDistal Femur (Sandeep Sir)Kirubakaran Saraswathy PattabiramanNessuna valutazione finora
- I. X-Ray Image: Hindfoot Fractures By: Jeremy Tan and Sarah HillDocumento8 pagineI. X-Ray Image: Hindfoot Fractures By: Jeremy Tan and Sarah HillSheril MarekNessuna valutazione finora
- Arm:Leg Fracture PDFDocumento11 pagineArm:Leg Fracture PDFHannaNessuna valutazione finora
- DRUJinstabilityreview - PDF 034407Documento15 pagineDRUJinstabilityreview - PDF 034407Oscar Cayetano Herrera RodríguezNessuna valutazione finora
- Coxitis TB Hip KneeDocumento26 pagineCoxitis TB Hip KneefajarvicNessuna valutazione finora
- Lower Limb FracturesDocumento120 pagineLower Limb FracturesAnda Madalina Zaharia100% (1)
- Why Every Spine Fusion Can Be A Deformity?Documento88 pagineWhy Every Spine Fusion Can Be A Deformity?PaulMcAfeeNessuna valutazione finora
- How To Examine The Wrist and HandDocumento7 pagineHow To Examine The Wrist and HandSurgicalgownNessuna valutazione finora
- Ficat and Arlet Staging of Avascular Necrosis of Femoral HeadDocumento6 pagineFicat and Arlet Staging of Avascular Necrosis of Femoral HeadFernando Sugiarto0% (1)
- Gpe - 017.1 - Orthopaedic ExaminationDocumento3 pagineGpe - 017.1 - Orthopaedic ExaminationImiey Eleena HanumNessuna valutazione finora
- OSTEOTOMIES AROUND THE HIP FinalDocumento51 pagineOSTEOTOMIES AROUND THE HIP FinalWasim R. IssaNessuna valutazione finora
- Ankle Fractures: A Literature Review of Current Treatment MethodsDocumento13 pagineAnkle Fractures: A Literature Review of Current Treatment Methodsadrian1989Nessuna valutazione finora
- Basic Principles of Tendon TransferDocumento10 pagineBasic Principles of Tendon TransferyeapdshengNessuna valutazione finora
- Lateral Condyle Fracture Tips and TricksDocumento33 pagineLateral Condyle Fracture Tips and TricksPurushotham NalamatiNessuna valutazione finora
- Management of Avn HipDocumento13 pagineManagement of Avn Hipterencedsza100% (1)
- Treatment of Diaphyseal Femoral Fractures With Ilizarov Frame. Maurizio A. Catagni and Francesco GuerreschiDocumento4 pagineTreatment of Diaphyseal Femoral Fractures With Ilizarov Frame. Maurizio A. Catagni and Francesco GuerreschiNuno Craveiro LopesNessuna valutazione finora
- 1.3 Soft Tissue InjuryDocumento44 pagine1.3 Soft Tissue InjurySylvinho46100% (1)
- Humeral Shaft FractureDocumento82 pagineHumeral Shaft FractureYoga AninditaNessuna valutazione finora
- Transient SynovitisDocumento9 pagineTransient SynovitisMuhammad Taufik AdhyatmaNessuna valutazione finora
- Management of FractureDocumento20 pagineManagement of FractureHitesh RohitNessuna valutazione finora
- Hand FPL Repair PT ProtocolDocumento2 pagineHand FPL Repair PT ProtocolHari25885Nessuna valutazione finora
- Kapandji Vs K-Wires StudyDocumento6 pagineKapandji Vs K-Wires StudymonkeyzergNessuna valutazione finora
- Maternal Pelvis Fetal Skull PDFDocumento13 pagineMaternal Pelvis Fetal Skull PDFAnuradha Maurya100% (2)
- Reconstruction of Posttraumatic Disorders of The ForearmDocumento12 pagineReconstruction of Posttraumatic Disorders of The Forearmsinung bawonoNessuna valutazione finora
- Rosenberg ViewDocumento3 pagineRosenberg ViewdeepakNessuna valutazione finora
- Notes On The Thorax: Anatomy RHS 241Documento71 pagineNotes On The Thorax: Anatomy RHS 241William JonathanNessuna valutazione finora
- STRETCHING EXERCISE NewDocumento7 pagineSTRETCHING EXERCISE NewIkramul Hussain KhanNessuna valutazione finora
- 3-1-Pediatric Trigger ThumbDocumento17 pagine3-1-Pediatric Trigger ThumbProfesseur Christian DumontierNessuna valutazione finora
- Insufficiency Fractures: A Rare Cause of Foot and Ankle Pain in Three Patients With Rheumatoid ArthritisDocumento7 pagineInsufficiency Fractures: A Rare Cause of Foot and Ankle Pain in Three Patients With Rheumatoid ArthritisNovia KurniantiNessuna valutazione finora
- LESSON 3.1 C Human Anatomy Fundamentals C-MUSCLEDocumento24 pagineLESSON 3.1 C Human Anatomy Fundamentals C-MUSCLEJoppy VargasNessuna valutazione finora
- NUR 092 Session 1-2 RationaleDocumento4 pagineNUR 092 Session 1-2 RationaleAnne rose Tabang100% (1)
- Adult Reflexes Bicep ReflexDocumento4 pagineAdult Reflexes Bicep ReflexChris Deinielle Marcoleta SumaoangNessuna valutazione finora
- Pemeriksaan BMDDocumento43 paginePemeriksaan BMDMisael ChristianNessuna valutazione finora
- 18 - 23agni Karma With Guda in Tennis ElbowDocumento6 pagine18 - 23agni Karma With Guda in Tennis ElbowrauolNessuna valutazione finora
- The Origin-Point Therapy - ENDocumento16 pagineThe Origin-Point Therapy - ENChan Justin100% (1)
- 2016 Muscle Activation Comparisons Between Elastic and Isoinertial ResistanceDocumento10 pagine2016 Muscle Activation Comparisons Between Elastic and Isoinertial ResistanceVictor Andrés Olivares IbarraNessuna valutazione finora
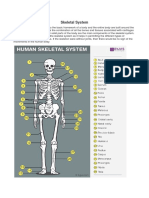
- Skeletal SystemDocumento5 pagineSkeletal SystemSobia KanwalNessuna valutazione finora
- Kinesiology of The Musculoskeletal System 3rd Edition (Donald A. Neumann) Capitulo Ombro ComplexoDocumento57 pagineKinesiology of The Musculoskeletal System 3rd Edition (Donald A. Neumann) Capitulo Ombro ComplexoMurilo PinzNessuna valutazione finora
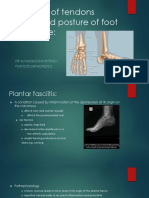
- Tendon Disorders of Foot and Ankle (Autosaved) 2Documento74 pagineTendon Disorders of Foot and Ankle (Autosaved) 2Irfan Ahmad100% (1)
- Rig O MaticDocumento9 pagineRig O MaticrendermanuserNessuna valutazione finora
- Knee Assessement FormDocumento2 pagineKnee Assessement FormLee Woo GuanNessuna valutazione finora
- Gait CycleDocumento1 paginaGait CycleLakshita PrajapatiNessuna valutazione finora
- Manual/Assisted Stretching Techniques: WWW - Fisiokinesiterapia.bizDocumento26 pagineManual/Assisted Stretching Techniques: WWW - Fisiokinesiterapia.bizLuca AnamariaNessuna valutazione finora
- Kalkaneal OsteotomiDocumento11 pagineKalkaneal Osteotomitravma777Nessuna valutazione finora
- RRBN Past Questions For Medical Image Processing X-Ray TechnicianDocumento6 pagineRRBN Past Questions For Medical Image Processing X-Ray TechnicianCharles Obaleagbon100% (2)
- Core Stability Exercise Principles: Spine ConditionsDocumento6 pagineCore Stability Exercise Principles: Spine ConditionsDavid Moreno - ManzanaroNessuna valutazione finora
- Lower Limb Neurological ExamDocumento2 pagineLower Limb Neurological ExamRochelle BaileyNessuna valutazione finora
- Ponseti Management of Clubfoot in Chittagong DisvisionDocumento34 paginePonseti Management of Clubfoot in Chittagong Disvisionmuthia saniNessuna valutazione finora
- Sex Determination From Skeletal RemainsDocumento47 pagineSex Determination From Skeletal Remainsgemini27858734100% (2)
- Exercise and Ankle Sprain Injuries: A Comprehensive ReviewDocumento6 pagineExercise and Ankle Sprain Injuries: A Comprehensive Reviewabraham landaetaNessuna valutazione finora