Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Tocolisis
Caricato da
Jorge Luis Nuñez Pizarro0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
141 visualizzazioni12 pagineTitolo originale
Tocolisis.pptx
Copyright
© © All Rights Reserved
Formati disponibili
PPTX, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
141 visualizzazioni12 pagineTocolisis
Caricato da
Jorge Luis Nuñez PizarroCopyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPTX, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 12
Tocolisis
Jorge Luis Nuez Pizarro
Introduccion
La labor pretrmino (LPT) precede el 50% de partos
pretrmino, pero aproximadamente el 30% se resuelve
espontanemente y slo el 10% da a luz en los primeros 7 das
(el 50% de las pacientes hospitalizadas por LPT tiene un parto
a termino). La terapia tocoltica cesa las contracciones
tempralmente, pero no remueve el estimulo causal; por lo que
es util para horas a dias, pero no para semanas o meses.
No partner Systemic infection
Low socioeconomic status Bacteriuria
Anxiety Periodontal disease
Depression Placenta previa
Life events (divorce, separation, death) Placental abruption
Occupational issues
Vaginal bleeding, especially in more than one
trimester
Abdominal surgery during pregnancy Previous preterm delivery
Multiple gestation Substance abuse
Polyhydramnios Smoking
Uterine anomaly Maternal age (<18 or >40)
Uterine leiomyoma African-American race
Diethylstilbestrol-induced changes in uterus Poor nutrition and low body mass index
History of second trimester abortion Inadequate prenatal care
History of cervical surgery Anemia (hemoglobin <10 g/dL)
Premature cervical dilatation or effacement (short
cervical length)
Excessive uterine contractility
Sexually transmitted infections Low level of educational achievement
Pyelonephritis, appendicitis, pneumonia Genotype
Systemic infection Fetal anomaly
Environmental factors (eg, heat, air pollution) Fetal growth restriction
Labor pretrmino
Clnica no especfica (puede presentarse varias horas antes)
Clicos parecidos a menstrual
Contracciones leves e irregulares
Dolor lumbar
Sensacin de presin en la vagina
Secrecin vaginal de moco (claro, rosa o ligr sanguinolento)
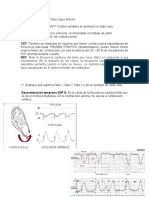
Dx: Clnico. Eco tv es la mejor manera de medir cuello (<30cm
riesgo)
Contracciones: 4 every 20 minutes or 8 every 60 minutes.
Incorporacin 80%; dilatacin >2cm.
Triaje basado en longitud de cuelo (>30cm: bajo riesgo 20cm:
alto riesgo) Fibronectina fetal como predictor. (ayuda a
diferenciar de Braxton Higgs)
Indicaciones
Slo indicado en gestantes con una edad gestacional en la que el
feto se beneficia de un retraso de 48h del parto.
1. Evaluacin inicial
2. Objetivos: 1) Demorar parto al menos 48h para alcanzar efecto
mximo profilctico de corticoides. 2) Dar tiempo para el traslado
de la madre. 3) Si se sospecha de causa transitoria (infecciosa o
ciruga)
3. Contraindicaciones:
Muerte fetal
Anomala fetal letal
Status fetal no reactivo
Preeclampsia o eclampsia severa
Hemorragia materna con inestabilidad hemodinmica
Infeccin intraamnitica
Contraindicacin materna a la droga tocoltica
Tratamiento
Systematic review and network meta-analysis of 95 randomized
trials of tocolytic therapy for preterm labor, all of the commonly
used tocolytic agents (cyclooxygenase inhibitors, beta-adrenergic
receptor agonist, calcium channel blockers, magnesium sulfate,
oxytocin receptor antagonists) were statistically more effective
than placebo/no therapy for delaying delivery for 48 hours (odds
ratios compared toplacebo/no treatment ranged from 1.91 to 5.39)
[18]. Cyclooxygenase inhibitors and calcium channel blockers had
the highest probability of delaying delivery and improving neonatal
and maternal outcomes. However, prolongation of pregnancy was
not associated with a statistically significant reduction in overall
rates of respiratory distress syndrome or neonatal death. This may
be related to the rarity of neonatal death and inconsistency in
definitions and reported outcomes among trials.
Haas DM, Caldwell DM, Kirkpatrick P, et al. Tocolytic therapy for
preterm delivery: systematic review and network meta-analysis. BMJ
2012; 345:e6226.
Atosiban
Inhibidor competitivo de receptores de oxitocina.
FDA no lo aprob. Us en Europa.
A recent Cochrane review (Papatsonis et al, 2005) did not
demonstrate any superiority of atosiban over beta-agonists
or placebo in terms of tocolytic efficacy or infant outcomes.
Compared with beta-agonists, there were more atosiban-
exposed infants with birth weights under 1500 gms (RR 1.96;
95% CI 1.15 to 3.35, 2 trials, 575 infants), and no overall clear
benefit on in perinatal or neonatal outcomes
Initial intravenous injection of 6.75mg in 0.9ml slowly
injected over one minute
A continuous infusion at a rate of 24 ml/hr up to 3 hours
A continuous infusion at a rate of 8ml/hr up to 45 hours
Inhibidores Ciclooxigenasa
(indometacina)
Por su eficacia, seguridad y costo-efectividad, se considera de
primera linea hasta las 32ss. (2-A)
Prostaglandinas son esenciales para el labor de parto. Tanto la COX1
como la COX2 son producidas por la placenta, teniendo ms
importantcia la COX2 durante el parto.
Compared to the other drugs, COX inhibitors were associated with a
trend toward reduction of birth within 48 hours of initiation of
treatment (RR 0.59, 95% CI 0.34-1.02) The effect was more robust
when COX inhibition was only compared with beta-adrenergic
receptor agonists (RR 0.27, 95% CI 0.08-0.96).
50 to 100 mg loading dose (may be given per rectum), followed by
25 mg orally every four to six hours
If indomethacin is continued for longer than 48 hours, sonographic
evaluation for oligohydramnios and narrowing of the fetal ductus
arteriosus is warranted at least weekly
Informacin limitada sobre COX2 selectivos.
Bloqueadores de canales de
calcio
Disminuye el ingreso y liberacin por el retculo
sarcoplasmtico de Ca, lo que disminuye la interaccin entre
cadenas de actina y miosina, disminuyendo contractibilidad.
Compare with Beta-agonist, use of nifedipine was also
associated with significant reductions in risk of respiratory
distress syndrome, necrotizing enterocolitis, intraventricular
hemorrhage, neonatal jaundice, and admission to the
neonatal intensive care unit, and had a better side effect
profile.
De primera linea entre las 32 y 34ss. (2-B)
30 mg loading dose and then 10 to 20 mg every four to six
hours
Agonistas beta adrenrgicos
( terbutaline)
Se une al receptor beta-2 e incrementa adenil ciclasa
intracelular, activando a la proteinkinasa y fosforilando
proteinas intracelulares, lo que disminuye el Ca libre y
finalmente, la interaccion entre actina y miosina,
disminuyendo la contractibilidad.
0.25 mg can be administered every 20 to 30 minutes for up to
four doses or until tocolysis is achieved
Monitorizar FC materna (parar si >120xmin), K y glucosa.
Sulfato de Magnesio
Mecanismo de accin no claro. Compite con calcio en
membrana celular.
In 15 comparative trials, magnesium sulfate was neither more
nor less effective than other tocolytics.
Review from 4 meta-analisis evidence there was no evidence
of a clinically important tocolytic effect of magnesium sulfate
Efecto neuroprotector sobre neonato. (We limit magnesium
sulfate for neuroprotection to pregnancies less than 32 weeks
of gestation). Descontinuar tras 24h. Este efecto no debe
condicionar eleccin de tocoltico.
6 g intravenous load over 20 minutes, followed by a
continuous infusion of 2 g/hour. Puede ajustarse de acuerdo a
toxicidad materna y efectividad en contracciones.
Donadores de oxido ntrico
Incrementa el cGMP mediante la interaccin la guanilato
ciclasa. Esto interacciona con la cadena de miosina
produciendo relajacin del musculo liso.
There is insufficient evidence to recommend NO donors for
inhibition of preterm labor
10 mg glyceryl trinitrate patch applied to the skin of the
abdomen. Aumentar otro parche si fuera necesario.
10ug/min en infusin intravenosa.
Referencias
UPTODATE
American College of Obstetricians and Gynecologists, Committee on
Practice BulletinsObstetrics. ACOG practice bulletin no. 127:
Management of preterm labor. Obstet Gynecol 2012; 119:1308.
King JF, Grant A, Keirse MJ, Chalmers I. Beta-mimetics in preterm labour:
an overview of the randomized controlled trials. Br J Obstet Gynaecol
1988; 95:211.
Gazmararian JA, Petersen R, Jamieson DJ, et al. Hospitalizations during
pregnancy among managed care enrollees. Obstet Gynecol 2002;
100:94.
Scott CL, Chavez GF, Atrash HK, et al. Hospitalizations for severe
complications of pregnancy, 1987-1992. Obstet Gynecol 1997; 90:225.
McPheeters ML, Miller WC, Hartmann KE, et al. The epidemiology of
threatened preterm labor: a prospective cohort study. Am J Obstet
Gynecol 2005; 192:1325.
Fuchs IB, Henrich W, Osthues K, Dudenhausen JW. Sonographic cervical
length in singleton pregnancies with intact membranes presenting with
threatened preterm labor. Ultrasound Obstet Gynecol 2004; 24:554.
Potrebbero piacerti anche
- Oxitocina y PG ModificadoDocumento22 pagineOxitocina y PG ModificadoAnaid CrespoNessuna valutazione finora
- Decálogos y algoritmos en ginecología y obstetriciaDa EverandDecálogos y algoritmos en ginecología y obstetriciaNessuna valutazione finora
- Monitoreo Fetal Intraparto y AntepartoDocumento22 pagineMonitoreo Fetal Intraparto y AntepartoEliixiita GuerreroNessuna valutazione finora
- Anticoncepcion Post PartoDocumento42 pagineAnticoncepcion Post PartoCesar MurgaNessuna valutazione finora
- Amenaza Parto PreterminoDocumento12 pagineAmenaza Parto PreterminoFlorencia Villar LazNessuna valutazione finora
- Trabajo de Parto: Caso ClínicoDocumento35 pagineTrabajo de Parto: Caso ClínicoMarcos BonillaNessuna valutazione finora
- Sindrome de Infección PuerperalDocumento36 pagineSindrome de Infección PuerperalRoger Angulo ToribioNessuna valutazione finora
- DengueDocumento29 pagineDengueGustavo DominguezNessuna valutazione finora
- OxitócicosDocumento24 pagineOxitócicosEduardo Alarcón HernándezNessuna valutazione finora
- Hiperemesis GravidicaDocumento4 pagineHiperemesis GravidicaGA HANessuna valutazione finora
- Resumen de Distocias Uterinas y PresentacionDocumento18 pagineResumen de Distocias Uterinas y Presentacionbelkysc26Nessuna valutazione finora
- Contracción UterinaDocumento42 pagineContracción UterinaWA RA50% (2)
- Amenaza de Parto PreterminoDocumento26 pagineAmenaza de Parto PreterminoMagaly Montoya SolisNessuna valutazione finora
- Hemorragia postparto: causas, diagnóstico y tratamientoDocumento33 pagineHemorragia postparto: causas, diagnóstico y tratamientoEngenharia cotidianannNessuna valutazione finora
- Incompetencia CervicalDocumento19 pagineIncompetencia CervicalMauricio GarcíaNessuna valutazione finora
- Frecuencia Cardiaca Fetal Durante El PartoDocumento12 pagineFrecuencia Cardiaca Fetal Durante El PartoNicole Martinez100% (1)
- Shock hipovolemico obstetrico: definicion, etiologia, cuadro clinico y tratamientoDocumento16 pagineShock hipovolemico obstetrico: definicion, etiologia, cuadro clinico y tratamientoJazmin Brito CastilloNessuna valutazione finora
- Practica Número 1 PreparacionDocumento9 paginePractica Número 1 PreparacionYahaira OvandoNessuna valutazione finora
- Expo Puerperio Patologico para SubirDocumento22 pagineExpo Puerperio Patologico para SubirYenny TorresNessuna valutazione finora
- 2.2 Farmacos Que Modifican La Motilidad Uterina PDFDocumento30 pagine2.2 Farmacos Que Modifican La Motilidad Uterina PDFFernando DiegoNessuna valutazione finora
- TEMA 1. Embarazo Cronologicamente ProlongadoDocumento6 pagineTEMA 1. Embarazo Cronologicamente Prolongadoyolanda3nu3ez-645909Nessuna valutazione finora
- Monitoreo FetalDocumento9 pagineMonitoreo FetalRuby Esmeralda Mendez Hernandez0% (1)
- FOLLETO ANALGESIA EPIDURAL Por EnfermeriaDocumento3 pagineFOLLETO ANALGESIA EPIDURAL Por EnfermeriakalalamirNessuna valutazione finora
- Salud FetalDocumento19 pagineSalud FetalKatherin VlcekNessuna valutazione finora
- Drogas Que Afectan La Motilidad UterinaDocumento23 pagineDrogas Que Afectan La Motilidad UterinaEliana Eulacio AuletNessuna valutazione finora
- Abscesos MamariosDocumento13 pagineAbscesos Mamarioscandy manuela chaca monagoNessuna valutazione finora
- Trabajo Clave RojaDocumento9 pagineTrabajo Clave RojaFanny RocioNessuna valutazione finora
- Caso Clinico N 2 - Semana 3Documento10 pagineCaso Clinico N 2 - Semana 3Mario Trasmonte100% (1)
- GinecorragiaDocumento25 pagineGinecorragiaFede DelponteNessuna valutazione finora
- Hemorragias Segunda Mitad Del EmbarazoDocumento34 pagineHemorragias Segunda Mitad Del EmbarazoEralda HushNessuna valutazione finora
- Hemorragia postparto: causas, prevención y tratamientoDocumento51 pagineHemorragia postparto: causas, prevención y tratamientoEstrella LlerenaNessuna valutazione finora
- Monitorización Fetal IntrapartoDocumento17 pagineMonitorización Fetal IntrapartoVolg ZangiefNessuna valutazione finora
- OxitocitosDocumento11 pagineOxitocitosJonathan GarciaNessuna valutazione finora
- Farmacos en Embarazo y LactanciaDocumento13 pagineFarmacos en Embarazo y Lactanciaapi-3745568100% (9)
- Pre EclampsiaDocumento29 paginePre EclampsiaMagaly ArzolaNessuna valutazione finora
- Inducción y conducción del trabajo de parto: Indicaciones, métodos y complicacionesDocumento18 pagineInducción y conducción del trabajo de parto: Indicaciones, métodos y complicacionesFanny VillalobosNessuna valutazione finora
- InducciónDocumento49 pagineInducciónBryan VasledNessuna valutazione finora
- Atención Del PuerperioDocumento20 pagineAtención Del PuerperioPatricia OrregoNessuna valutazione finora
- Farmacos ObstetricosDocumento19 pagineFarmacos ObstetricosL Hopital PerúNessuna valutazione finora
- Ictericia Neonatal: Causas, Clínica y ManejoDocumento8 pagineIctericia Neonatal: Causas, Clínica y ManejoAlexandra FlorNessuna valutazione finora
- RCP SeminarioDocumento48 pagineRCP SeminarioBélice Yupanqui BustamanteNessuna valutazione finora
- Amenaza de Parto Pretermino Diapositiva PDFDocumento38 pagineAmenaza de Parto Pretermino Diapositiva PDFJOSNEILYS100% (1)
- Colestasia IntrahepáticaDocumento20 pagineColestasia IntrahepáticamonsecatalinaNessuna valutazione finora
- Perfil Biofisico FetalDocumento24 paginePerfil Biofisico FetalesmeNessuna valutazione finora
- Embarazo EctopicoDocumento13 pagineEmbarazo Ectopicoanita perez guevaraNessuna valutazione finora
- Casos Clínicos SEM 12 Obst I LaboratorioDocumento17 pagineCasos Clínicos SEM 12 Obst I LaboratorioLUCIA ELIANA OLIVA CUSTODIONessuna valutazione finora
- Analgesia en ObstetriciaDocumento15 pagineAnalgesia en ObstetriciaMiriamQlNessuna valutazione finora
- Atonía UterinaDocumento13 pagineAtonía UterinaJuan Carlos Barajas FloresNessuna valutazione finora
- Cir 5-1Documento19 pagineCir 5-1Cynthi De La Cruz100% (1)
- Cambios fisiológicos en la gestanteDocumento82 pagineCambios fisiológicos en la gestanteRocio Del Pilar Damian Alvarado50% (2)
- CasoClínicoDistociasRoturaUterinaDocumento6 pagineCasoClínicoDistociasRoturaUterinaVictor jesus Siguas garciaNessuna valutazione finora
- Trabajo de PartoDocumento14 pagineTrabajo de PartoAzu Luz CalderónNessuna valutazione finora
- Hemorragias 1er 2do y 3er TrimestreDocumento66 pagineHemorragias 1er 2do y 3er TrimestreMercy Guerrero GuerreroNessuna valutazione finora
- PreguntasDocumento3 paginePreguntasPaola RincónNessuna valutazione finora
- Absceso de MamaDocumento9 pagineAbsceso de MamaYovana Guzman LlanquiNessuna valutazione finora
- DistociasDocumento33 pagineDistociaspavelich_93Nessuna valutazione finora
- Cambios Fisiologicos Del PuerperioDocumento11 pagineCambios Fisiologicos Del PuerperioKAREN ORTIZNessuna valutazione finora
- Shock Hipovolemico Ob NildaDocumento28 pagineShock Hipovolemico Ob NildaFernando OrihuelaNessuna valutazione finora
- Parto PreterminoDocumento27 pagineParto Preterminobla bla bla100% (1)
- Consenso Uso de Uteroinhibidores-AppDocumento15 pagineConsenso Uso de Uteroinhibidores-Applaura_m_eNessuna valutazione finora
- Bienestar Fetal Insatisfactorio PDFDocumento61 pagineBienestar Fetal Insatisfactorio PDFDiego Fernando Hoyos SNessuna valutazione finora
- Farmacos Del EmbarazoDocumento22 pagineFarmacos Del Embarazooliver121Nessuna valutazione finora
- Amenaza de Parto Pre-Termino Y Parto PrematuroDocumento34 pagineAmenaza de Parto Pre-Termino Y Parto PrematuroMario Rosado GarcíaNessuna valutazione finora
- Amenaza de parto prematuroDocumento6 pagineAmenaza de parto prematuroOrlando Ramirez NarvaezNessuna valutazione finora
- Orciprenalina en La Amenaza de Parto Pretermino - RinarodriguezroblesDocumento5 pagineOrciprenalina en La Amenaza de Parto Pretermino - RinarodriguezroblesRina RoblesNessuna valutazione finora
- Drogas Que Afectan La Motilidad UterinaDocumento23 pagineDrogas Que Afectan La Motilidad UterinaEliana Eulacio AuletNessuna valutazione finora
- Trabajo de Aula - S12Documento4 pagineTrabajo de Aula - S12RENATO ALONSO PACHECO ROSALESNessuna valutazione finora
- Amenaza Parto PreterminoDocumento12 pagineAmenaza Parto PreterminoADELMA ORTIZ CUEVANessuna valutazione finora
- Evalatosiban 07Documento7 pagineEvalatosiban 07Diana JimenezNessuna valutazione finora
- AtosibanDocumento8 pagineAtosibanErik GarciaNessuna valutazione finora
- Nifedipino SolucionDocumento8 pagineNifedipino SolucionSaray GutierrezNessuna valutazione finora
- Fármacos UteroinhibidoresDocumento9 pagineFármacos UteroinhibidoresEnrique AlarcónNessuna valutazione finora
- 3 PDF Amenaza de Parto Pretermino21Documento21 pagine3 PDF Amenaza de Parto Pretermino21Maria C OrtizNessuna valutazione finora
- Guía FarmacológicaDocumento20 pagineGuía FarmacológicaMariel OlmosNessuna valutazione finora
- Atosiban vs. Orciprenalina en La Amenaza de Parto PretérminoDocumento6 pagineAtosiban vs. Orciprenalina en La Amenaza de Parto PretérminoAsun alvarezNessuna valutazione finora
- Clase 08Documento59 pagineClase 08Bárbara RubĭlarNessuna valutazione finora
- Parto PreterminoDocumento7 pagineParto Preterminoshadi mNessuna valutazione finora
- Fármacos GinecológicosDocumento11 pagineFármacos GinecológicosFigueredo GimenaNessuna valutazione finora
- Farmacos para La Relajacion y Contraccion UterinaDocumento60 pagineFarmacos para La Relajacion y Contraccion Uterinapoly fpdNessuna valutazione finora
- Expo Fármaco Tocolíticos y OxitócicosDocumento72 pagineExpo Fármaco Tocolíticos y OxitócicosGaby Roca75% (4)
- Nifedipine Frente Atosiban en El Tratamiento de La Amenaza de Parto PretérminoDocumento7 pagineNifedipine Frente Atosiban en El Tratamiento de La Amenaza de Parto PretérminoNilson Bruges MarinNessuna valutazione finora
- Amenaza de Parto Pretérmino: R1Gyo Guzmán Benavides ItzelDocumento39 pagineAmenaza de Parto Pretérmino: R1Gyo Guzmán Benavides ItzelItz GuzmanNessuna valutazione finora
- TocolisisDocumento12 pagineTocolisisJorge Luis Nuñez PizarroNessuna valutazione finora
- Amenaza de parto preterminoDocumento11 pagineAmenaza de parto preterminoGustavo Decelis GordilloNessuna valutazione finora
- Farmacos de Ginecologia CompletoDocumento15 pagineFarmacos de Ginecologia CompletoNoa MuñozNessuna valutazione finora
- DefinicionDocumento14 pagineDefinicionMargarita TorresNessuna valutazione finora
- Practica 4Documento65 paginePractica 4Emociones DetallesNessuna valutazione finora
- Farmacologia MedicamentoDocumento4 pagineFarmacologia MedicamentoMELANY NICOL MULATO HUAMANNessuna valutazione finora
- TOCÓLISISDocumento15 pagineTOCÓLISISMelanie Betteta DíazNessuna valutazione finora