Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Treacher Collins
Caricato da
theva_thy0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
102 visualizzazioni26 paginemedical pediatrics
Titolo originale
Treacher collins
Copyright
© © All Rights Reserved
Formati disponibili
PPT, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentomedical pediatrics
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPT, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
102 visualizzazioni26 pagineTreacher Collins
Caricato da
theva_thymedical pediatrics
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPT, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 26
B/O JN
D25 OF LIFE/ SVD @ 40 WEEKS/ BW3.025/AS 14 5 7
MOTHER: 37YO/PARA 3+2/ BG A+VE/VDRL/RT : NR
ANTENATALLY :
1)GDM on diet control
-dx @ 28 weeks
HBA1c :5.4 %
2) Polyhydramnions
-AFI: 27
3) h/o ectopic and abortion in 2012
** other children are healthy
No h/o consanginous marriage
Baby born not vigorous & flat, poor tone, poor cry
RESUSCITATION WAS INTIATED !!!
Given PPV X 3 HR picked up 70-100 dropped < 100 & gasping
Attempted intubation multiple times failed oropharyngeal airway
inserted
HR < 60
CPR x 1 HR < 100
UVC was inserted given adrenaline 0.3 cc X 2 HR still not improving
given bolus NS 35cc X1 HR > 100
ETT was inserted via Right nostril in view of spo 30% improved
Emergency tracheostomy by ENT team
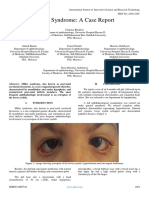
Downward slanting
palpebral fissure
Hypoplastic of
zygomatic bones
Hypoplastic
supraorbital rims
On examination :
Microtia Micrognathia
AFNT, Tone normal
Moros complete & symetrical bilaterally
Lungs : clear
CVS : no murmur DRNM
PA : soft, no hepatomegaly
B/l femoral pulses palpable
Spine normal, hips : stable
Digits were normal
TREACHER COLLINS SYNDROME WITH DIFFICULT
AIRWAY
Cleft palate
ALTE at D20/D23 of life
Presumed sepsis at D9&D22 of life
Seizure at D22 of life
Thrombocytosis
FBC
BG
COAG PROFILE
RP
LFT
BLOOD C&S
CXR
CHROMOSOMAL STUDY - PENDING
Airway Tracheostomy
Feeding Tube feeding
IV antibiotics
ENT/Audiology
Physiotherapy
Dietician
CLAPAM
JKSP
Social support
Rare genetic disorder
This disorder is named Edward Treacher
Collins, a London ophthalmologist medical literature
in 1900
mandibulofacial dysostosis or Treacher Collins-Franceschetti
syndrome
prevalence range between 1 in 40,000 to 1 in
70,000 of live birthsI
features are caused abnormal development of the first and
second branchial archs
Inherited in autosomal dominant pattern
An error in chromosome number 5 at TCOF1 gene treacle plays a
role in craniofacial development.
60% of TSC cases a new mutation without a positive family history of
the disorder.
A parent may be mildly affected & unaware that they have the disorder.
The risk of passing the abnormal gene from affected parent to offspring
is 50% for each pregnancy.
Other modes of inheritance autosomal recessive transmission & a role
for gonadal mosaicism & chromosomal rearrangement in the causation of
this syndrome have also been proposed TCS
Diagnostic clinical features
Diagnostic clinical test
Radiographs and CT for evaluation of
craniofacial abnormality
Audiological evaluation for hearing impairment
DNA diagnosis : Direct sequencing of the coding
and flanking intronics of TCOF1 defects mutations
in about 90-95 % of patients
Prenatal diagnosis
Two dimensional/ three dimesional
sonography
Polyhydramnions
Demonstrations of characteristics facies TCS
Amniocentesis/ CVS
Detect TCOF 1
The disease causing allele of an affected individual
must be identified before prenatal testing can be
performed
The presence of TCOF1 mutation detected by
prenatal diagnosis does not predict the specific
malformation or severity of the disease
The current approach for TCS's clinical deformities seeks functional and
esthetical correction as well as psychosocial support.
Multidisciplinary approach pediatricians, otorhinolarngologists,
craniofacial surgeons , ophthalmologists, speech therapists,
psychologists and pediatric dentists most appropriate way to manage
these patients.
Treatment use of hearing aids and multiple reconstructive
surgeries based on the severity to correct the facial
malformations.
1. Respiratory compromise due to
maxillary hypoplasia which results in choanal stenosis/atresia
and tends to constrict the nasal passages
2. Presence of mandibular micrognathia and a retropositioned
tongue obstructing the oropharyngeal and hypopharngeal
spaces
3. Very rarely sleep apnoea and sudden infant death syndrome have
been described in these patients
4. Social stigmata because of severe face deformity
The longevity of survival in patients with TCS is
comparable with that of the normal population.
Individuals with severe form of TCS usually, over a period
of time, undergo multiple major reconstructive surgeries
that are rarely fully corrective.
The majority of these patients are of normal intelligence
early recognition of deafness & its correction using
hearing aids and/or surgery is of great importance to
enable them to lead a near normal life
Prevent its occurrence in the offspring of affected
parents (40% chance of transmitting it).
Genetic counselling, good quality antenatal sonography
with amniocentesis and/or chorionic villus sampling
FACEBOOK -1 in 50,000 blog-Treacher Collins Syndrome, Help Suport Juliana
Wetmore Who Was Born With Rare Treacher Collins Syndrome,microtia and
atresia
Treacher collins family support group ( not in malaysia)
1)Sowmya B Shetty, Ann Thomas, Raghavendrea Pidamale. Treacher Collins Syndrome : A Case Report
and a Brief Review on Diagnostic Aids :International Journal of Clinical Pediatric Dentistry
2011;4(3):235-239.
2) Girish Gopal, Dr. Divya Durga , Dr. S. Prashanth. Treacher Collins Syndrome In The Newborn.
International journal of biological and medical research 2014; 5(2): 4112-4115
3) Prachi Shete, Tupkari JV1, Tabita Benjamin, Aarti Singh. A Case report on TCS. Journal of Oral and
Maxillofacial Pathology 2011 Vol. 15 : 348-351
4) Bowornsilp Chowchuen, Kamonwan Jenwitheesuk ,Prathana Chowchuen ,Palakorn Surakunprapha.
Challenges in Evaluation, Management and Outcome of the Patients with Treacher Collins
Syndrome. J Med Assoc Thai 2011; 94 (Suppl. 6): S85-S90
5) Ranadheer E, Nagaraju, Suresh, Updesh. Eight year follow-up dental treatment in a
patient with Treacher Collins syndrome.J Indian Soc Pedod Prev Dent 2012;30:254-7.
6) http://www.webmedcentral.com
7) http://emedicine.medscape.com/article/946143
8) http://www.rarediseases.org/docs.
Potrebbero piacerti anche
- MRCPCH Clinical The Whole Book PDFDocumento108 pagineMRCPCH Clinical The Whole Book PDFtheva_thy100% (3)
- 2011 - Practical Guide Insulin TherapyDocumento6 pagine2011 - Practical Guide Insulin Therapytheva_thy100% (1)
- Neonatal Hypoglycemia APNECDocumento27 pagineNeonatal Hypoglycemia APNECtheva_thyNessuna valutazione finora
- AACE GuidelinesDocumento23 pagineAACE GuidelinesHatem GamalNessuna valutazione finora
- NSAIDsDocumento37 pagineNSAIDstheva_thyNessuna valutazione finora
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Treacher Collins Syndrome F1705 FINAL Dec19Documento3 pagineTreacher Collins Syndrome F1705 FINAL Dec19zafakwuNessuna valutazione finora
- Treacher Collins Syndrome: A Case StudyDocumento8 pagineTreacher Collins Syndrome: A Case StudyjoeNessuna valutazione finora
- Treachercollinssyndrome: Albaraa Aljerian,, Mirko S. GilardinoDocumento9 pagineTreachercollinssyndrome: Albaraa Aljerian,, Mirko S. GilardinoSai KrupaNessuna valutazione finora
- Wonder: R.J. PalacioDocumento89 pagineWonder: R.J. PalacioSwati RaiNessuna valutazione finora
- Wonder Novel Study Preview PDFDocumento12 pagineWonder Novel Study Preview PDFMouna Mch0% (1)
- Crouzon Syndrome (Craniofacial Dysostosis)Documento41 pagineCrouzon Syndrome (Craniofacial Dysostosis)Dr. Hasna ArshadNessuna valutazione finora
- Chaimae Khodriss Ahmed Bennis Fouad Chraibi Meriem Abdellaoui Idriss Benatiya AndaloussiDocumento3 pagineChaimae Khodriss Ahmed Bennis Fouad Chraibi Meriem Abdellaoui Idriss Benatiya AndaloussiInternational Journal of Innovative Science and Research TechnologyNessuna valutazione finora
- sp104f Es enDocumento5 paginesp104f Es enLyna ZamoraNessuna valutazione finora
- Pron 1993Documento10 paginePron 1993Javiera Paz Rios CarmonaNessuna valutazione finora
- Bilateral Macrostomia: Interesting Case SeriesDocumento4 pagineBilateral Macrostomia: Interesting Case Seriesahmed bouzouidaNessuna valutazione finora
- Ugcs3 v3 Project Attachments WonderDocumento10 pagineUgcs3 v3 Project Attachments WonderDavid KaufmanNessuna valutazione finora
- Treacher Collins Syndrome: A Systematic Review of Evidence-Based Treatment and RecommendationsDocumento14 pagineTreacher Collins Syndrome: A Systematic Review of Evidence-Based Treatment and RecommendationsSai KrupaNessuna valutazione finora
- Imaging Features: Cleidocranial DysplasiaDocumento13 pagineImaging Features: Cleidocranial DysplasiaLevina DermawanNessuna valutazione finora
- Edac225 Assignment 1c - Case StudyDocumento7 pagineEdac225 Assignment 1c - Case Studyapi-319193686Nessuna valutazione finora
- Branchial Arch SyndromesDocumento7 pagineBranchial Arch SyndromesVita Dental PachucaNessuna valutazione finora
- Cleft Lip and PalateDocumento50 pagineCleft Lip and Palatesusanti bulanNessuna valutazione finora
- DENT3002-Oral Histology and Embryology FDocumento146 pagineDENT3002-Oral Histology and Embryology FLorenzini GrantNessuna valutazione finora
- Hearing ImpairmentDocumento7 pagineHearing ImpairmentIrene MendozaNessuna valutazione finora
- The Genetic Basis of Facial Skeletal Characteristics and Its Relation With OrthodonticsDocumento6 pagineThe Genetic Basis of Facial Skeletal Characteristics and Its Relation With OrthodonticssmritiNessuna valutazione finora
- Clinical Diagnosis in Plastic SurgeryDocumento166 pagineClinical Diagnosis in Plastic SurgeryFrancoDaniloRocaLandaveri100% (6)
- Craniofacial AnomaliesDocumento78 pagineCraniofacial AnomaliesAhmad KaramNessuna valutazione finora
- Mohan Et AlDocumento4 pagineMohan Et AlDwi WicaksonoNessuna valutazione finora
- Cleft Lip and Palate - Claniofacial Clefts BookDocumento137 pagineCleft Lip and Palate - Claniofacial Clefts BookAbdulaziz HassenNessuna valutazione finora
- Treacher Collins SyndromeDocumento12 pagineTreacher Collins SyndromeDiego BravoNessuna valutazione finora
- Craniofacial SyndromesDocumento101 pagineCraniofacial SyndromesSaranya MohanNessuna valutazione finora
- Congenital Defect On Maxillofacial Region: Developmental Defects of The Oral and Maxillofacial RegionDocumento134 pagineCongenital Defect On Maxillofacial Region: Developmental Defects of The Oral and Maxillofacial RegionRedy Pristanto PutraNessuna valutazione finora
- David Renz Defense Federal Sentencing MemorandumDocumento13 pagineDavid Renz Defense Federal Sentencing MemorandumAmanda JordanNessuna valutazione finora
- Treacher-Collins Syndrome (TCS), Also Known As Treacher-Collins-Franceschetti Syndrome, Mandibulofacial DysostosisDocumento17 pagineTreacher-Collins Syndrome (TCS), Also Known As Treacher-Collins-Franceschetti Syndrome, Mandibulofacial DysostosisAilyn LoroNessuna valutazione finora
- ABO Master Module 1Documento13 pagineABO Master Module 1PopoNessuna valutazione finora
- Anatomical Classification of Facial, Cranio-Facial and Latero-Facial CleftsDocumento24 pagineAnatomical Classification of Facial, Cranio-Facial and Latero-Facial CleftsAlvaro Jose Uribe TamaraNessuna valutazione finora