Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
01 Pathophysiology & MX of Pain
Caricato da
rikarz0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
23 visualizzazioni37 paginepain management vvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvv knnjkjmlk;lkll
Titolo originale
01 Pathophysiology & Mx of Pain
Copyright
© © All Rights Reserved
Formati disponibili
PPT, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentopain management vvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvv knnjkjmlk;lkll
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPT, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
23 visualizzazioni37 pagine01 Pathophysiology & MX of Pain
Caricato da
rikarzpain management vvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvvv knnjkjmlk;lkll
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PPT, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 37
Physiology of Pain and
Principles of Pain Relief
Dr Dushyanthi Perera MD FRCA
Senior Lecturer in Anaesthesiology
Faculty of Medicine
University of Kelaniya
Pain is one of the commonest reason
for a patient visiting a doctor.
Definition of pain
Pain pathway
Post op pain
Analgesia for post op pain
Pain in labour
Chronic Pain
Cancer pain
Non malignant
Ethical issues
DEFINITION
An unpleasant sensory and
emotional experience
associated with potential or
actual tissue damage.
EMOTIONAL
RATIONAL
PHYSICAL
Psychological
Anxiety
Prev. experiences
Insight
Motivation
Factors influencing the pain
experience
Age
Gender
Personality
Culture
Learned behaviour from past
experiences
Beliefs / Attitudes
Religious
Anxiety and fears
Pain is whatever the patient says it is,
existing whenever the patient says it
does.
The patients self reporting of pain is the
single most reliable indicator of pain.
Assessment of Pain
A detailed history
A comprehensive physical examination
An understanding of the pathophysiology
of pain
Methodical documentation
Measurement of Pain
Pain History
Site
Intensity
Duration
Elsewhere radiation
Associated factors
Relieving factors
Management to date
SIDE ARM
Pathophysiology of Pain
Types of pain
Acute ( brief pain that subsides with
healing)
Labour
Post op
Chronic Pain
Cancer
Non malignant pain
Types of pain
Nociceptive pain ( stimuli from somatic
and visceral structures)
Neuropathic (abnormal processing of
the nervous system)
Nociception
Term used to describe how pain becomes
conscious
Transduction
Transmission
Perception
Modulation
Transduction changing of the noxious
stimuli in sensory nerve endings to
impulses
Transmission movement of these
impulses to the brain
Perception recognizing, defining and
responding to the pain
Modulation activation of descending
pathways that exert inhibitory effects on
pain transmission
Peripheral Receptors (somatic
or visceral)
High threshold cutaneous receptors
Silent nociceptors
Peripheral opioid receptors ( anti
nociceptors)
Inflammatory Mediator soup
Neurogenic eg Substance P
Tissue mediated eg Bradykinin
prostoglandins, 5HT,
histamine, K and H ions
Substance P and Prostoglandins further
sensitize the nociceptors including
activating the silent type.
PHYSIOLOGY OF PAIN
TRAUMA
Nociceptors
Skin
Deep tissues
Viscera
Mechanoreceptors
Polymodel Symp and Parasymp
Ad (sharp,localized)
C (dull,poorly localized, aching)
Inflammatory mediators- SP,
Hist, Bradykinin
+
+
+
PHYSIOLOGY OF PAIN
DORSAL HORN
substance P,glutamate,ATP
SPINOTHALAMIC TRACTS
THALAMUS
CORTEX
Descending tracts
Exact location in the brain where pain is
perceived is unclear
Reticular activating system- symp
response
Somatosensory cortex localizes and
characterizes
Limbic system emotional and
behavioural response
Central Spinal Processing
Gate Control Theory
Wind Up phenomenon (AMPA and
NMDA receptors)
Descending inhibitory control
( endogenous opioids, 5HT,
Noradrenaline, GABA)
Higher Centres
T cell
SG
Large fibres
Ab
C fibres
+
-
+ +
-
-
Gate Control Theory of Melzack and Wall
Harmful Effects of Pain
CVS Increased heart rate and BP.
Hypercoagulability
RS inadequate ventilation
Stress response release of multitude
of hormones and hyperglycaemia
GIT nausea and vomiting
GUT fluid and urinary retention
Immune depressed immunity
Muscle spasm
REQUIREMENTS
CONTINUOUS ANALGESIA
ANALGESIA TITRATABLE TO PAIN
AVAILABLE ANALGESIC
TECHNIQUES
OPIODS
Morphine, Pethidine,Codeine
NSAIDS
Paracetamol, Diclofenac sodium
LOCAL ANAESTHETICS
Local infiltration, Epidural, EMLA
OTHERS
Acupuncture, Entonox,
TRAMADOL
OPIOIDS
ROUTES- im, iv, sc,continuous infusion, PCA
SIDE EFFECTS
VENTILATORY DEPRESSION
SEDATION
VASODILATATION
COUGH SUPPRESSION
NAUSEA AND VOMITING
TOLERENCE AND DEPENDENCE
CONSTIPATION
NSAID
OPIOID SPARING
CONTRA INDICATIONS
GASTRIC ULCERS
BLEEDING DIATHESIS
RENAL DYSFUNCTION
HYPOVOLAEMIC, ELDERLY, INADEQ.
RESUSC POST OP
HYPERSENSITIVITY
LOCAL ANAESTHETIC
EXPERTISE
MONITORING
Low Tech Topical
Wound infiltration
Peripheral nerve blocks
Plexus blocks
High Tech Spinal , Epidural
Advantages of epidural
Prolong the duration of analgesia by
use of the catheter
Decreases the incidence of DVT
Less sedation therefore early
mobilization and feeding
Early return of bowel function
Disadvantages
Expensive
Expertise
Monitoring
Hypotension, urinary retention
Resp depression with added opioids
If opioids are added they must not be given
by any other route.
Ideally keep on O
2
.
Balanced analgesia
Combination of appropriate analgesics.
Act on different sites in the pain
pathway
Decrease individual doses and thereby
decrease the incidence of side effects
PRE EMPTIVE ANALGESIA
Factors to consider when
choosing analgesics
Appropriateness of the intervention for
the pain
Coexisting illness
Available staff
Available equipment
Risks and side effects
Cost / Benefit ratio
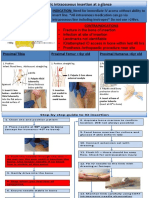
MONITORING
PAIN SCORE
1 NO PAIN AT REST OR MOVEMENT
2 NO PAIN AT REST SLIGHT PAIN ON
MOVEMENT
3 PAIN AT REST. MOD. PAIN ON
MOVEMENT
4 CONTINUOUS PAIN AT REST AND
SEVERE PAIN ON MOVEMENT
Visual Analogue Score
MONITORING
SEDATION
0 NONE
1 DROWSY. EASYY TO ROUSE
2 ASLEEP .EASY TO ROUSE
3 SOMNOLENT AND DIFFCULT TO
ROUSE
MONITORING
RESPIRATORY RATE
NAUSEA AND VOMITING
CVS - HEART RATE AND BP
Steps to Successful
Management of Pain
Regular assessment and recording of pain
and side effects
Protocols for monitoring and treating pain
Protocols for monitoring and treating side
effects
Use a safe and simple balanced analgesic
regime
Appropriate backup by identified personnel
Continuing in service training and education.
Potrebbero piacerti anche
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Andre Tan's Surgery Notes (Ed 1)Documento163 pagineAndre Tan's Surgery Notes (Ed 1)Daniel LimNessuna valutazione finora
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- USC 4-3 Blitz SchemeDocumento13 pagineUSC 4-3 Blitz Schemegambitt43Nessuna valutazione finora
- ROTC Smart CardDocumento4 pagineROTC Smart Cardrjn367Nessuna valutazione finora
- SCIATICA EXERCISES Functional BestDocumento3 pagineSCIATICA EXERCISES Functional BestMellow Moon RecordsNessuna valutazione finora
- Luftwaffe Plot Against GoeringDocumento204 pagineLuftwaffe Plot Against Goeringcheapgary100% (1)
- SLB Cavings Morphology PosterDocumento1 paginaSLB Cavings Morphology PosterMudLogggerAUS100% (3)
- Pre Incident Plan Confine Space Emergency TCOTDocumento1 paginaPre Incident Plan Confine Space Emergency TCOTkamen55Nessuna valutazione finora
- Idetifying School and Community ResourcesDocumento16 pagineIdetifying School and Community ResourcesAmani AbasNessuna valutazione finora
- 2004 AlliantPowderSMDocumento64 pagine2004 AlliantPowderSMscottperkinsusaNessuna valutazione finora
- Musculoskeletal Imaging Oxford HandbookDocumento478 pagineMusculoskeletal Imaging Oxford HandbookJuned A Ansari100% (2)
- Ideas Wts - Mds - Prostho Q&ADocumento18 pagineIdeas Wts - Mds - Prostho Q&AMostafa Fayad100% (1)
- Fall Protection Plan FormDocumento5 pagineFall Protection Plan FormharpreetresearchNessuna valutazione finora
- Postintern15 07 2014letterDocumento2 paginePostintern15 07 2014letterrikarzNessuna valutazione finora
- ABC TraumaDocumento27 pagineABC TraumarikarzNessuna valutazione finora
- Fractures: Dr. Pradeep Fernando MS, FRCSDocumento31 pagineFractures: Dr. Pradeep Fernando MS, FRCSrikarzNessuna valutazione finora
- An Approach To The Problem of Low Back PainDocumento35 pagineAn Approach To The Problem of Low Back PainrikarzNessuna valutazione finora
- Fluid and Electrolyte TherapyDocumento39 pagineFluid and Electrolyte TherapyrikarzNessuna valutazione finora
- 04 Toxic GasesDocumento30 pagine04 Toxic GasesrikarzNessuna valutazione finora
- Fluid and Electrolyte TherapyDocumento39 pagineFluid and Electrolyte TherapyrikarzNessuna valutazione finora
- Batch 17 Tutorial 1Documento5 pagineBatch 17 Tutorial 1rikarzNessuna valutazione finora
- Acute Renal Failure: DR S. RatnayakeDocumento19 pagineAcute Renal Failure: DR S. RatnayakerikarzNessuna valutazione finora
- Thrombocytopenia: DR Chamilka JayasingheDocumento31 pagineThrombocytopenia: DR Chamilka JayasingherikarzNessuna valutazione finora
- Tute 13Documento24 pagineTute 13rikarzNessuna valutazione finora
- TuteDocumento6 pagineTuterikarzNessuna valutazione finora
- Immunotherapy: Prof Anura WeerasingheDocumento17 pagineImmunotherapy: Prof Anura WeerasingherikarzNessuna valutazione finora
- Tumour Immunology: Prof Anura WeerasingheDocumento18 pagineTumour Immunology: Prof Anura WeerasingherikarzNessuna valutazione finora
- 7 - Spinal Column and Spinal Cord Injuries TestDocumento3 pagine7 - Spinal Column and Spinal Cord Injuries Testkamilkasim262Nessuna valutazione finora
- How To Prevent Musculoskeletal Disorders in The WorkplaceDocumento48 pagineHow To Prevent Musculoskeletal Disorders in The WorkplaceSoarin626Nessuna valutazione finora
- Changes in Musculoskeletal System During AgingDocumento19 pagineChanges in Musculoskeletal System During Agingsonali tushamerNessuna valutazione finora
- Clinical Neurology and NeurosurgeryDocumento4 pagineClinical Neurology and NeurosurgeryGissela AlvaradoNessuna valutazione finora
- MS For Installation - Hypochlorination 23.10.07 HamdyDocumento8 pagineMS For Installation - Hypochlorination 23.10.07 HamdyunnicyriacNessuna valutazione finora
- Case Report: Fracture of Distal of Right Radius Fracture of Styloid of Right UlnaDocumento23 pagineCase Report: Fracture of Distal of Right Radius Fracture of Styloid of Right Ulna-'Rhya Rhyemma James Potter'-Nessuna valutazione finora
- Oag Report - Wardel Davis IIIDocumento61 pagineOag Report - Wardel Davis IIIWGRZ-TVNessuna valutazione finora
- Pulp Revascularization of A Necrotic Infected Immature Permanent Tooth: Case Report and Review of The LiteratureDocumento4 paginePulp Revascularization of A Necrotic Infected Immature Permanent Tooth: Case Report and Review of The LiteratureRiad BachoNessuna valutazione finora
- Bes700 Bes710 en Ru A5 260819Documento36 pagineBes700 Bes710 en Ru A5 260819Евгений МаркеловNessuna valutazione finora
- Bimall vs. Trimall Ankle Fractures: Outcome Study: Chadi Tannoury, MDDocumento22 pagineBimall vs. Trimall Ankle Fractures: Outcome Study: Chadi Tannoury, MDneareastspineNessuna valutazione finora
- Small Fragment Set: - Features and Benefits - Indications - Operative Technique - Ordering InformationDocumento20 pagineSmall Fragment Set: - Features and Benefits - Indications - Operative Technique - Ordering InformationRicardo_CHES1986Nessuna valutazione finora
- AO OTA Fracture and Dislocation ClassificationDocumento10 pagineAO OTA Fracture and Dislocation ClassificationBENEDICTUSNessuna valutazione finora
- Intraosseous IO Insertion GuideDocumento2 pagineIntraosseous IO Insertion GuideYusardi R PradanaNessuna valutazione finora
- (2P2) GROUP 2 - MusclesDocumento5 pagine(2P2) GROUP 2 - MusclesAlexa AurellanoNessuna valutazione finora
- Test 4 (Module 4) : MirrorDocumento2 pagineTest 4 (Module 4) : Mirrorjanuzaj90Nessuna valutazione finora
- Clinical Symptom Score of The Japanese Orthopaedic AssociationDocumento3 pagineClinical Symptom Score of The Japanese Orthopaedic AssociationYap Young SangNessuna valutazione finora
- PEH2 Finals ReviewerDocumento5 paginePEH2 Finals ReviewerPedro HampaslupaNessuna valutazione finora
- Qcs 2010 Section 11 Part 2.3.08 She Procedures - The Report and InvesDocumento39 pagineQcs 2010 Section 11 Part 2.3.08 She Procedures - The Report and Invesbryanpastor106Nessuna valutazione finora