Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
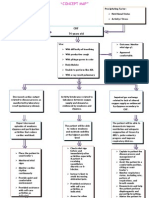
Nursing Care Plan For Glaucoma
Caricato da
Emiey RaraDescrizione originale:
Titolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Nursing Care Plan For Glaucoma
Caricato da
Emiey RaraCopyright:
Formati disponibili
Nursing Care Plan for Glaucoma Nursing Assessment for Glaucoma 1.
History or presence of risk factors : Positive family history (believed to be associated with primary open angle glaucoma). Tumors of the eye Hemorrhage intraocular Inflammatory intraocular uveiti) Eye contusion from trauma. Physical examination based on those in the general assessment of the eye may indicate: For primary open angle Reported a loss of peripheral vision slow (see tunnel) For primary angle closure : Incidence of sudden severe pain in the eye is often accompanied by headache, nausea and vomiting. Complaints halo light, blurred vision, and decreased light perception. The pupils are being fixed with redness due to inflammation of the sclera and cornea looks cloudy. Diagnostic Examination Tonometri used to measure intra-ocular pressure. Glaucoma is suspected when IOP greater than 22 mmHg. Gonioskopi possible to see directly the anterior chamber angle glaucoma to distinguish between closed and open-angle glaucoma. Optalmoskopi allow inspectors to see directly optic disc and internal eye structure. Assess the patient's understanding about the condition and emotional response to the condition and plan of action. Nursing Diagnosis and Nursing Interventions for Glaucoma Pain related to spasm, intra-ocular pressure, glaucoma acute. Which is characterized by :
o o o o o
2.
o o o
3.
o o o
4.
patients express pain in the eye, protect the side of the pain patients, frowned and whimpered. Goal : reduction of discomfort, said pain is gone / reduced, relaxed facial expression, no moaning. Intervention :
o o o o o
Monitor blood pressure, pulse, and respiration every 4 hours. Monitor the degree of eye pain every 30 minutes during the acute phase. Monitor input and output every 8 hours while receiving intravenous osmotic agent. Monitor visual acuity at any time before hatching ophthalmic agents. Give appropriate instructions optalmic agent for glaucoma. Inform your doctor if : hypotension urinary output of less than 240 ml / hour No loss of pain in the eye within 30 minutes of drug therapy Decrease in constant visual acuity. Prepare patients for surgery Maintain bed rest in semi-Fowler position. Prevent increase in IOP : Instruct to avoid coughing, sneezing, straining, or placing the head below the pelvic Provide quiet environment and avoid light. Give anlgetic prescription and evaluation of its effectiveness.
Complications:
Bacterial sinusitis is nearly always harmless (although uncomfortable and sometimes even very painful). If an episode becomes severe, antibiotics generally eliminate further problems. In rare cases, however, sinusitis can be very serious. Osteomyelitis. Adolescent males with acute frontal sinusitis are at particular risk for severe problems. One important complication is
infection of the bones (osteomyelitis) of the forehead and other facial bones. In such cases, the patient usually experiences headache, fever, and a soft swelling over the bone known as Pott's puffy tumor. Infection of the Eye Socket. Infection of the eye socket, or orbital infection, which causes swelling and subsequent drooping of the eyelid, is a rare but serious complication of ethmoid sinusitis. In these cases, the patient loses movement in the eye, and pressure on the optic nerve can lead to vision loss, which is sometimes permanent. Fever and severe illness are usually present. Blood Clot. Blood clots are another danger, although rare, from ethmoid or frontal sinusitis. If a blood clot forms in the sinus area around the front and top of the face, symptoms are similar to orbital infection. In addition, the pupil may be fixed and dilated. Although symptoms usually begin on one side of the head, the process usually spreads to both sides. Brain Infection. The most dangerous complication of sinusitis, particularly frontal and sphenoid sinusitis, is the spread of infection by anaerobic bacteria to the brain, either through the bones or blood vessels. Abscesses, meningitis, and other life-threatening conditions may result. In such cases, the patient may experience mild personality changes, headache, altered consciousness, visual problems, and, finally, seizures, coma, and death.
inflammation or swelling of the tonsils from frequent or ongoing (chronic) tonsillitis can cause complications such as: Difficulty breathing Disrupted breathing during sleep (obstructive sleep apnea) Infection that spreads deep into surrounding tissue (tonsillar cellulitis) Infection that results in a collection of pus behind a tonsil (tonsillar abscess)
Potrebbero piacerti anche
- NCP Alcoholic NeuropathyDocumento5 pagineNCP Alcoholic NeuropathyPeachy Marie Anca100% (1)
- Word Ncp.......... TetanusDocumento6 pagineWord Ncp.......... TetanusaianrNessuna valutazione finora
- PYOMYOSITISDocumento12 paginePYOMYOSITISPaolo VillaNessuna valutazione finora
- Nursing Care Plan: IndependentDocumento1 paginaNursing Care Plan: IndependentJay Mar BabateNessuna valutazione finora
- Nursing Care of Client With Cataract SurgeryDocumento11 pagineNursing Care of Client With Cataract SurgeryFatin Fatihah AzizanNessuna valutazione finora
- Student Nurses' Community: Nursing Care Plan AmputationDocumento3 pagineStudent Nurses' Community: Nursing Care Plan AmputationNur faizah bt azmiNessuna valutazione finora
- Impaired Physical MobilityDocumento2 pagineImpaired Physical MobilityJayson OlileNessuna valutazione finora
- Retinal DetachmentDocumento6 pagineRetinal DetachmentNader Smadi100% (3)
- NCP Impaired Physical MobilityDocumento1 paginaNCP Impaired Physical MobilityCharmaine SolimanNessuna valutazione finora
- Session 8 Ethical Dilemma in Professional PracticeDocumento14 pagineSession 8 Ethical Dilemma in Professional PracticeSyed MaazNessuna valutazione finora
- Assessment and Management of Patients With Hearing and Balance Disorders WebDocumento36 pagineAssessment and Management of Patients With Hearing and Balance Disorders Webmalinda0% (1)
- CP Intestinal Obstruction Nursing Care PlanDocumento7 pagineCP Intestinal Obstruction Nursing Care PlanShiella Heart MalanaNessuna valutazione finora
- Glasgow Coma Scale: Presented by Pankaj Singh Rana Nurse Practitioner in Critical CareDocumento17 pagineGlasgow Coma Scale: Presented by Pankaj Singh Rana Nurse Practitioner in Critical CareAnisya AbabeliaNessuna valutazione finora
- Retinopathy of PrematurityDocumento15 pagineRetinopathy of Prematuritymarissa ulkhairNessuna valutazione finora
- Teaching P UlcersDocumento2 pagineTeaching P UlcersFiona Cheryl Amsterdam100% (1)
- Femur FractureDocumento19 pagineFemur FractureMadx VNessuna valutazione finora
- Word Ncp.......... TetanusDocumento3 pagineWord Ncp.......... TetanusYvounne Ananias Bautista RNNessuna valutazione finora
- NCP Sicu!Documento6 pagineNCP Sicu!joanne190Nessuna valutazione finora
- NCP PTBDocumento6 pagineNCP PTBJay Dela VegaNessuna valutazione finora
- Pathophysiology of FractureDocumento2 paginePathophysiology of Fracturemyer pasandalanNessuna valutazione finora
- Compartment Syndrome NCP (PAIN)Documento2 pagineCompartment Syndrome NCP (PAIN)eunica16Nessuna valutazione finora
- As Needed.: Environmental Stimuli 6Documento4 pagineAs Needed.: Environmental Stimuli 6Nicole GumolonNessuna valutazione finora
- NCP HyperthermiaDocumento1 paginaNCP HyperthermiaPastor James PacadaljenNessuna valutazione finora
- Nursing Care PlanDocumento13 pagineNursing Care PlanCris Solis33% (3)
- Ortho NCPDocumento1 paginaOrtho NCPErjohn Vincent Lim100% (1)
- FractureDocumento1 paginaFractureReechie TeasoonNessuna valutazione finora
- Cues Nursing Diagnosis Rationale Goals and Objectives Nursing Intervention Rationale Evaluation SubjectiveDocumento4 pagineCues Nursing Diagnosis Rationale Goals and Objectives Nursing Intervention Rationale Evaluation SubjectiveFaye Dianne Damian-BuenafeNessuna valutazione finora
- Cerebral Aneurysm Case Analysis and Concept MapDocumento5 pagineCerebral Aneurysm Case Analysis and Concept Mapate NarsNessuna valutazione finora
- San Francisco St. Butuan City 8600, Region XIII Caraga, PhilippinesDocumento3 pagineSan Francisco St. Butuan City 8600, Region XIII Caraga, Philippineskuro hanabusaNessuna valutazione finora
- Nursing Care Plan For Low SelfDocumento3 pagineNursing Care Plan For Low SelfMarissa AsimNessuna valutazione finora
- NCP For Ears Nose ThroatDocumento1 paginaNCP For Ears Nose ThroatMcmac YangoNessuna valutazione finora
- Date and Time Objectives Learning Contents Strategies Target Population Resources Evaluation OutcomeDocumento8 pagineDate and Time Objectives Learning Contents Strategies Target Population Resources Evaluation OutcometrizzlecNessuna valutazione finora
- NCP Impaired Skin IntegrityDocumento4 pagineNCP Impaired Skin IntegrityElgie SantosNessuna valutazione finora
- Ncp-Impaired S.i.-NavidasDocumento4 pagineNcp-Impaired S.i.-NavidasFran LanNessuna valutazione finora
- NCP Epidural HemDocumento32 pagineNCP Epidural HemKatrina PonceNessuna valutazione finora
- CELINDocumento9 pagineCELINaikoestrellaNessuna valutazione finora
- 1 Ineffective Airway ClearanceDocumento8 pagine1 Ineffective Airway ClearanceEsel Mae DinamlingNessuna valutazione finora
- Schizophrenia Nursing ManagementDocumento56 pagineSchizophrenia Nursing ManagementHumphreyNessuna valutazione finora
- NCPDocumento2 pagineNCPAnne De VeraNessuna valutazione finora
- Osteomalacia Care Plan/OthersDocumento11 pagineOsteomalacia Care Plan/OthersJill Jackson, RNNessuna valutazione finora
- Health Teaching PlanDocumento10 pagineHealth Teaching PlanPaolo Vittorio Perdigueros GonzalesNessuna valutazione finora
- Research ProposalDocumento22 pagineResearch ProposalKapil LakhwaraNessuna valutazione finora
- Nursing Care Plan: Nikolai P. Funcion, FSUU-SNDocumento5 pagineNursing Care Plan: Nikolai P. Funcion, FSUU-SNNikolai FuncionNessuna valutazione finora
- Primary HypothyroidismDocumento1 paginaPrimary HypothyroidismChezika Ennail PamplinaNessuna valutazione finora
- Myasthenia Gravis NCPDocumento1 paginaMyasthenia Gravis NCPCzarina0% (1)
- Nursing Care Plan: General: Goals Met GenreralDocumento3 pagineNursing Care Plan: General: Goals Met GenreralRomzy BasañesNessuna valutazione finora
- Ineffective Breathing PatternDocumento7 pagineIneffective Breathing PatternJanmae JivNessuna valutazione finora
- Nursing Care Plan: Determine Cause of Activity - Determining The Cause of A Disease CanDocumento2 pagineNursing Care Plan: Determine Cause of Activity - Determining The Cause of A Disease Canrix07Nessuna valutazione finora
- Concept Map - Abby !Documento2 pagineConcept Map - Abby !Abegail Abaygar100% (3)
- Impetigo PathophysiologyDocumento1 paginaImpetigo PathophysiologyCesar Arada100% (1)
- Nursing Care Plan - Fatigue (Antepartum)Documento3 pagineNursing Care Plan - Fatigue (Antepartum)kaimimiyaNessuna valutazione finora
- NCP Self CaRE DeficitDocumento1 paginaNCP Self CaRE Deficitnicole pageNessuna valutazione finora
- Glaucoma Health Teaching Plan - SuladayDocumento7 pagineGlaucoma Health Teaching Plan - SuladayChris P BaconNessuna valutazione finora
- LARYNGITISDocumento13 pagineLARYNGITIStherese BNessuna valutazione finora
- FHP & NCP - FractureDocumento14 pagineFHP & NCP - FractureFrancis AdrianNessuna valutazione finora
- NCP Icu-CcuDocumento6 pagineNCP Icu-CcuJohn CenasNessuna valutazione finora
- Case Report PresentationDocumento34 pagineCase Report PresentationDwi Permana PutraNessuna valutazione finora
- Presentasi Kasus Glaukoma AkutDocumento24 paginePresentasi Kasus Glaukoma AkutHendrawan Ariwibowo100% (1)
- Angle-Closure Glaucoma - UpToDateDocumento9 pagineAngle-Closure Glaucoma - UpToDateElaine June FielNessuna valutazione finora
- Activity7 (Sympathetic Ophthalmia)Documento4 pagineActivity7 (Sympathetic Ophthalmia)Gabbii CincoNessuna valutazione finora
- Pavement Design1Documento57 paginePavement Design1Mobin AhmadNessuna valutazione finora
- BNF Pos - StockmockDocumento14 pagineBNF Pos - StockmockSatish KumarNessuna valutazione finora
- Working Capital in YamahaDocumento64 pagineWorking Capital in YamahaRenu Jindal50% (2)
- KP Tevta Advertisement 16-09-2019Documento4 pagineKP Tevta Advertisement 16-09-2019Ishaq AminNessuna valutazione finora
- Elements of ArtDocumento1 paginaElements of Artsamson8cindy8louNessuna valutazione finora
- Cisco SDWAN Case Study Large Global WANDocumento174 pagineCisco SDWAN Case Study Large Global WANroniegrokNessuna valutazione finora
- MASONRYDocumento8 pagineMASONRYJowelyn MaderalNessuna valutazione finora
- 3 ALCE Insulators 12R03.1Documento12 pagine3 ALCE Insulators 12R03.1Amílcar Duarte100% (1)
- Tplink Eap110 Qig EngDocumento20 pagineTplink Eap110 Qig EngMaciejNessuna valutazione finora
- DPSD ProjectDocumento30 pagineDPSD ProjectSri NidhiNessuna valutazione finora
- Task 3 - LPDocumento21 pagineTask 3 - LPTan S YeeNessuna valutazione finora
- An Exploration of The Ethno-Medicinal Practices Among Traditional Healers in Southwest Cebu, PhilippinesDocumento7 pagineAn Exploration of The Ethno-Medicinal Practices Among Traditional Healers in Southwest Cebu, PhilippinesleecubongNessuna valutazione finora
- FM 2030Documento18 pagineFM 2030renaissancesamNessuna valutazione finora
- Law of EvidenceDocumento14 pagineLaw of EvidenceIsha ChavanNessuna valutazione finora
- WEB DESIGN WITH AUSTINE-converted-1Documento9 pagineWEB DESIGN WITH AUSTINE-converted-1JayjayNessuna valutazione finora
- AnticyclonesDocumento5 pagineAnticyclonescicileanaNessuna valutazione finora
- Impact of Advertising On Consumers' Buying Behavior Through Persuasiveness, Brand Image, and Celebrity EndorsementDocumento10 pagineImpact of Advertising On Consumers' Buying Behavior Through Persuasiveness, Brand Image, and Celebrity Endorsementvikram singhNessuna valutazione finora
- Pe 03 - Course ModuleDocumento42 paginePe 03 - Course ModuleMARIEL ASINessuna valutazione finora
- Ron Kangas - IoanDocumento11 pagineRon Kangas - IoanBogdan SoptereanNessuna valutazione finora
- Hdfs Default XML ParametersDocumento14 pagineHdfs Default XML ParametersVinod BihalNessuna valutazione finora
- PyhookDocumento23 paginePyhooktuan tuanNessuna valutazione finora
- V737 OverheadDocumento50 pagineV737 OverheadnewahNessuna valutazione finora
- Powerpoint Speaker NotesDocumento4 paginePowerpoint Speaker Notesapi-273554555Nessuna valutazione finora
- Deal Report Feb 14 - Apr 14Documento26 pagineDeal Report Feb 14 - Apr 14BonviNessuna valutazione finora
- DQ Vibro SifterDocumento13 pagineDQ Vibro SifterDhaval Chapla67% (3)
- German Atv-Dvwk Rules and StandardsDocumento25 pagineGerman Atv-Dvwk Rules and StandardsMehmet Emre Bastopcu100% (1)
- Grade 7 ExamDocumento3 pagineGrade 7 ExamMikko GomezNessuna valutazione finora
- Comparitive Study ICICI & HDFCDocumento22 pagineComparitive Study ICICI & HDFCshah faisal100% (1)
- Richardson Heidegger PDFDocumento18 pagineRichardson Heidegger PDFweltfremdheitNessuna valutazione finora
- Countries EXCESS DEATHS All Ages - 15nov2021Documento21 pagineCountries EXCESS DEATHS All Ages - 15nov2021robaksNessuna valutazione finora