Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Pps 2
Caricato da
Hendy NurahadiDescrizione originale:
Titolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Pps 2
Caricato da
Hendy NurahadiCopyright:
Formati disponibili
Dental Traumatology 2007; doi: 10.1111/j.1600-9657.2005.00372.
x All rights reserved
Copyright Blackwell Munksgaard 2006 DENTAL TRAUMATOLOGY
Case Report
Segmental osteotomy to reposition multiple osseointegrated dental implants in the anterior maxilla in a trauma patient
Kao S-Y, Fong J-HJ, Chou S-J, Wu J-H, Tu H-F, Yeung T-C. Segmental osteotomy to reposition multiple osseointegrated dental implants in the anterior maxilla in a trauma patient. Blackwell Munksgaard, 2006. Abstract A 16-year-old young man had severe loss of alveolar bone and lost four teeth in the anterior maxilla because of traumatic injury in a trafc accident. To overcome the surgically compromised condition for implant rehabilitation, the decient ridge was augmented by autogenous bone graft from the mandibular symphysis. The augmented ridge had much improvement in width but less in vertical height. Four implants were placed to gain initial osseointegration. Segmental osteotomy was performed to occlusally reposition the implants and bone for 5-mm in the anterior maxilla. After 2 years of clinical follow-up, the rehabilitation outcome is satisfactory and stable. Excessive loss of teeth and bone are frequently seen in the traumatized anterior maxilla. The traumatized area often requires bone augmentation to provide appropriate dental implant support (1). Difculties have been encountered to simultaneously augment the width and height of the decient ridge. Crestal split technique is efcient in lateral widening but not vertical augmentation (2). Onlay bone graft or guided bone regeneration (GBR) technique is especially useful for augmenting the ridge width but, to some extent, has limited advantages in increasing the ridge height (36). The interpositional bone graft procedure also has technical difculty in a limited edentulous ridge (7, 8). The various above bone graft techniques can lead to wound dehiscence, infection, and possibly total failure of bone graft because of lack of appropriate soft tissue coverage in those traumatized areas (29). While seeking for methods to increase the success rate of these technique-sensitive procedures, the success rate differs in various follow-up studies to estimate the benets of the various bone augmen56
Shou-Yen Kao1,2,3, Jenny Hwai-Jen Fong2, Shen-Ju Chou1, Jen-Hsien Wu1, Hsi-Fen Tu4, Tze-Cheung Yeung1
Department of Dentistry, Taipei Veterans General Hospital (VGH); 2School of Dentistry, National Yang-Ming University (NYMU); 3Central Clinic Hospital; 4Department of Dentistry, I-Lan Hospital, Taiwan, Republic of China
1
Key words: bone graft; implant; maxilla; segmental osteotomy; trauma; vestibuloplasty Dr Shou-Yen Kao DDS DMSc, No 201, Sec II, ShihPai Rd., Oral and Maxillofacial Surgery, Department of Dentistry, Taipei-Veterans General Hospital, Taipei, Taiwan, Republic of China Tel.: 886 2 287 57572 Fax: 886 2 287 42375 e-mail: sykao@vghtpe.gov.tw Accepted 29 March, 2005
tation procedures (1). Distraction osteogenesis (DOG) is another recently proposed principle with signicant advantage to increase the bone height but occasional complications and expensiveness of commercial devices sometimes hinder the general acceptance of its clinical use (1012). Soft tissue management is equally as important as bone augmentation. The morphology of the augmented area needs to be improved by vestibuloplasty with skin or mucosa graft. Among the various donor sites, keratinized palatal mucosa (KPM) is the best choice as peri-implant tissue grafting in terms of quality and cosmetics (1315). Here we describe a case of narrow traumatized edentulous ridge in the anterior maxilla which sequentially received bone graft, implant surgery, vestibuloplasty and segmental osteotomy in a comprehensive oral rehabilitation procedure.
Case report
A 16-year-old boy involved in a motorcycle accident presented facial laceration, mandibular
Dental Traumatology 2007; 23: 5659
Segmental osteotomy to reposition implants in anterior maxilla
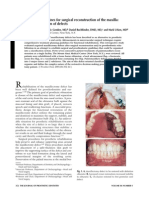
Fig. 1. Panoramic radiographs at different stages of rehabilitation. (a) Four months after open reduction for maxillo-mandibular fractures, bone plates were retained at both jaws. Four anterior teeth in the maxilla were missing. (b) A vague shadow at the symphysis of the mandible represents the donor site of bone graft. The implant is obviously located far above the cervical line of the adjacent teeth. (c) The prosthetic cylinders on the implants show a vertical space longer than needed for the clinical crowns. (d) The implants are repositioned more occlusally when comparing the preoperative level of both apex and top of each implant with postoperative level.
symphysis and Lefort I fracture, and loss of alveolar bone with avulsion of four anterior teeth in the maxilla. Four months after open reduction surgery, he was evaluated for dental rehabilitation. Intra-orally, he had acceptable occlusion but showed severely decient alveolar bone, lack of keratinized gingiva, shallow vestibule with scar, and loss of four anterior teeth in the maxilla. Radiographic examination showed bone plates left from previous open reduction surgery (Fig. 1a). Different treatment plans including necessary surgical procedures, potential outcomes or complications were explained to the patient and his family. They agreed to take the comprehensive approach for implant rehabilitation. Bone graft The anterior maxilla was estimated by tomography and model study. Under general anesthesia, a 1.2 3-cm sized fragment of cortico-cancellous
Dental Traumatology 2007; 23: 5659
bone was harvested from mandibular symphysis via a vestibular approach. In the maxilla, the miniplates at previous fractured sites were removed bilaterally via two separate vestibular approaches. A sub-periosteal tunnel between right and left maxillary canines was prepared to provide the recipient site for the grafted symphysis bone, which was immobilized by a 10-mm-long mini-screw. The wound was tightly closed and covered by a COEPAKTM periodontal dressing material (GC America Inc., ALSIP, IL, USA) for 1 week. A compromised shallow vestibule was seen at this stage. Implant surgery Six months later, the augmented ridge was ready for implant surgery. Under local anesthesia, four OsseotiteTM 3.75 3.75 13 mm implants (3I Implamt Innovations Inc., Palm Beach Gardens, FL, USA), were placed according to the guide of the surgical stent. One month later, a removable partial
57
Kao et al.
denture was relined and delivered. The panoramic lm showed an obvious insufciency of the bone level at the implant site (Fig. 1b). Design of segmental osteotomy and soft tissue management Four months later, the second stage operation to expose implant xtures was performed. Clinically, the insufcient vertical ridge height at the implant site led to an occlusal clearance much longer than needed when prosthetic abutments were tried (Fig. 1c). To overcome the predictable unsatisfactory cosmetics of the prosthesis, another surgery to occlusally reposition osseointegrated implants and bone for 57 mm was planned. Under general anesthesia, a labial ap with supra-periosteal dissection was created from the muco-gingival junction close to the ridge crest, and extended with bilateral buccal releasing incisions. Segmental osteotomy was started via bilateral vertical cuts of anterior maxilla with minimal exposure of bone between teeth and implant xtures. Bilateral
cuts were continued and connected by medial extension to the mid-palatal vault (Fig. 2a). The anterior nasal septum was separated from the palate with an osteotome. The anterior maxillary bone fragment was tracked by orthodontic ligature wires xing at the cervical area of healing abutment of implants and immobilized to a palatal stent. The edge of the labial ap was apically sutured with the periosteum to leave a 15-mm-wide nude supraperiosteal tissue surface spanning between bilateral canines (Fig. 2b). The nude surface was covered by periodontal dressing material for 2 weeks. The vestibular contour at the anterior maxilla was then created. Six weeks later, the primary stability of the downward repositioned maxillary fragment was observed. A permanent xed prosthesis was completed in the following 2 months with a good cosmetic result (Fig. 2c,d). The radiographic image showed a signicant downward repositioning of the bone fragments (Fig. 1d). After 2 years of follow-up, the rehabilitation outcome is stable and satisfactory.
Fig. 2. Clinical pictures of surgery and prosthetic rehabilitation. (a) The vestibuloplasty was performed together with the segmental osteotomy to reposition the multiple implants retained anterior maxilla. A partial thickness apically positioned ap was prepared. (b) The bone fragment was tracked through the ligature wire of each healing abutment on the implant. A 5 mm downward movement of the bone was achieved by immobilization to a palatal stent. (c) Most of the clinical crowns of the xed prosthesis can be seen with satisfactory cosmetics with the increase of lip strain. (d) Full exposure of prostheses shows acceptable cosmetics with the cervical line in continuation with the adjacent natural teeth.
58 Dental Traumatology 2007; 23: 5659
Segmental osteotomy to reposition implants in anterior maxilla Discussion References
1. Oikarinen KS, Sandor GKB, Kainulainen VT, SalonenKemppi M. Augmentation of the narrow traumatized anterior alveolar ridge to facilitate dental implant placement. Dent Traumatol 2003;19:1929. 2. Palti A. Ridge splitting and implant techniques for the anterior maxilla. Dental Implantol Update 2003;14:2532. 3. Keller EE, Tolman DE, Eckert S. Surgical-prosthodontic reconstruction of advanced maxillary bone compromise with autogenous onlay block bone grafts and osseointegrated endosseous implants: a 12-year study of 32 consecutive patients. Int J Oral Maxillofac Implants 1999;14:197209. 4. Verhoeven JW, Cune MS, Terlou M, Zoon MA, de Putter C. The combined use of endosteal implants and iliac crest onlay grafts in the severely atrophic mandible: a longitudinal study. J Oral Maxillofac Surg 1997;26:3517. 5. Astrand P, Nord PG, Branemark PI. Titanium implants and onlay bone graft to the atrophic edentulous maxilla: a 3year longitudinal study. Int J Oral Maxillofac Surg 1996;25:259. 6. Simion M, Jovanovic SA, Tinti C, Benfenati SP. Long-term evaluation of ossointegrated implants inserted at the time or after vertical ridge augmentation. A retrospective study on 123 implants with 15 year follow-up. Clin Oral Implants Res 2003;12:3545. 7. Nystrum E, Lundgren S, Gunne J, Nilson H. Interpositional bone grafting and Le fort I osteotomy for reconstruction of the atrophic edentulous maxilla. A two stage technique. Int J Oral Maxillofac Surg 1997;26:4237. 8. Kao SY, Yeung TC, Chou IC, Chang CS. Reconstruction of the severely resorbed atrophic edentulous ridge of the maxilla and mandible for implant rehabilitation: report of a case. J Oral Implantol 2002;28:12832. 9. Oikarinen K, Kainulainen V, Kainulainen T. A method harvesting corticocancellous bone chips for reconstructive maxillofacial surgery. Int J Oral Maxillofac Surg 1997;27:1035. 10. Rachmiel A, Srouji S, Peled M. Alveolar ridge augmentation by distraction osteogenesis. Int J Oral Maxillofac Surg 2001;30:5107. 11. Klug CN, Millesi-Schobel GA, Millesi W, Watzinger F, Ewers R. Preprosthetic vertical distraction osteogenesis of the mandible using an L-shaped osteotomy and titanium membranes for guided bone regeneration. J Oral Maxillofac Surg 2001;59:13028. 12. ILizarov GA, Devyatov AA, Kamerin VK. Plastic reconstruction of longitudinal bone defects by means of compression and subsequent distraction. Acta Chir Plast (Prague) 1980;22:3241. 13. Froschl T, Kerscher A. The optimal vestibuloplasty in preprosthetic surgery of the mandible. J Craniomaxillofac Surg 1997;25:8590. 14. Hughes WG, Howard CW III. Simultaneous split-thickness skin grafting and placement of endosteal implants in the edentulous mandible: a preliminary report. J Oral Maxillofac Surg 1992;50:44851. 15. Jennings DE. Treatment of the mandibular compromised ridge: a literature review. J Prosthet Dent 1989;61:5759. 16. Robiony M, Toro C, Stucki-McCormick SU, Zerman N, Costa F, Politi M. The FAD (Floating Alveolar Device): a bidirectional distraction system for distraction osteogenesis of the alveolar process. J Oral Maxillofac Surg 2004;62:13642. 17. Kassolis JD, Baer ML, Reynolds MA. The segmental osteotomy in the management of malposed implants: a case report and literature review. J Periodontol 2003;74:52936.
The implant rehabilitation at the narrow traumatized edentulous ridge often needs a stepwise improvement of both soft and hard tissue (1). Although both soft and hard tissue management is of equal importance in the full plan of reconstruction, bone graft at the decient ridge should be considered prior to soft tissue management. The autogenous bone graft can provide the needed bone volume in severe cases. The mandibular symphysis is a reliable bone graft to serve as an accountable implant supporting tissue (9). The ridge width at the anterior maxilla had substantially provided the need for the implant. However, the insufciency in the ridge height could still be observed. Current surgical techniques, for example, onlay bone graft, GBR, bone splitting and bone distraction, may have their respective advantages or disadvantages (13, 6, 10). Ridge splitting technique could have benet of widening the decient area, yet further increase of the ridge height because of insufcient soft tissue coverage for the bone graft (2, 4, 5). DOG theory to generate new bone has also been applied to increase the edentulous ridge by various commercial devices (10). This method succeeds in making new bone grow in the distracted bone gap through a biological process (1012). However, it is difcult to combine bone lengthening simultaneously with bone widening. A two-directioned oating distraction device has recently been advocated. However, the longterm stability still needs to be conrmed (16). As the management of both hard and soft tissue before implant surgery is essential, a multidisciplinary approach for the implant rehabilitation of cases with dento-alveolar trauma is necessary. Instead of using the expensive distraction device to prepare the bone for implant surgery in this case, the segmental osteotomy was selected to further reposition the osseointegrated implants in the anterior maxilla. The segmental osteotomy to immediately correct a single malposed implant has recently been reported (17). The transfer of the multiple implants in the bone has not been reported. The other unique feature for this case is the use of palatal stent for fragment immobilization. The comprehensive rehabilitation procedure of bone graft, implant surgery, segmental osteotomy and vestibuloplasty with a satisfactory and stable result warrants attention. Acknowledgement This article and the case were sponsored by VGH93C230 grant and NSC 933112B075 grant, Taipei, China. The work was administratively helped by Miss Su-Ting Tsai.
Dental Traumatology 2007; 23: 5659
59
Potrebbero piacerti anche
- Orthodontically Driven Corticotomy: Tissue Engineering to Enhance Orthodontic and Multidisciplinary TreatmentDa EverandOrthodontically Driven Corticotomy: Tissue Engineering to Enhance Orthodontic and Multidisciplinary TreatmentFederico BrugnamiNessuna valutazione finora
- Alveolar Segmental Sandwich Osteotomy PDFDocumento7 pagineAlveolar Segmental Sandwich Osteotomy PDFDeepak YadavNessuna valutazione finora
- Short ImplantsDa EverandShort ImplantsBoyd J. TomasettiNessuna valutazione finora
- Oh 2010Documento5 pagineOh 2010gbaez.88Nessuna valutazione finora
- Articulo ProtodonciaDocumento5 pagineArticulo ProtodonciaMilton David Rios SerratoNessuna valutazione finora
- USE OF TEMPORARY ANCHORAGE DEVICES IN INTRUSION OF SUPRAERUPTED MOLARS-case ReportsDocumento9 pagineUSE OF TEMPORARY ANCHORAGE DEVICES IN INTRUSION OF SUPRAERUPTED MOLARS-case ReportsVesna AndreevskaNessuna valutazione finora
- Alveolar Ridge Augmentation by Distraction OsteogenesisDocumento8 pagineAlveolar Ridge Augmentation by Distraction OsteogenesisCarlos Santiago VivenzaNessuna valutazione finora
- 23 03 09 07 03 11 - ExpansionDocumento5 pagine23 03 09 07 03 11 - ExpansionRaed Abu HamadNessuna valutazione finora
- Rehab of Severley Worn Dentition-Using Fixed and RemovableDocumento0 pagineRehab of Severley Worn Dentition-Using Fixed and RemovableFaheemuddin MuhammadNessuna valutazione finora
- Горизонтальная дистракцияDocumento7 pagineГоризонтальная дистракцияIrinaBorodulinaNessuna valutazione finora
- Reconstrução de Severa Reabsorção Maxilar Com Distração OsteogenicaDocumento7 pagineReconstrução de Severa Reabsorção Maxilar Com Distração OsteogenicaNelson UzunNessuna valutazione finora
- Long-Term Changes of The Anterior Palatal Alveolar Bone After Treatment With Bialveolar Protrusion, Evaluated With Computed TomographyDocumento10 pagineLong-Term Changes of The Anterior Palatal Alveolar Bone After Treatment With Bialveolar Protrusion, Evaluated With Computed TomographyMonojit DuttaNessuna valutazione finora
- Bone and Tissue LevelDocumento3 pagineBone and Tissue LevelSaleh AlsadiNessuna valutazione finora
- Cleft PalateDocumento4 pagineCleft PalateShoaib A. KaziNessuna valutazione finora
- Surgical-Orthodontic Expansion of The: MaxillaDocumento12 pagineSurgical-Orthodontic Expansion of The: MaxillaAna LauraNessuna valutazione finora
- Articol Pentru Teme 14-18Documento9 pagineArticol Pentru Teme 14-18Diamanta Yalomit CirsteaNessuna valutazione finora
- The Socket-Shield Technique To Support The Buccofacial Tissues at Immediate Implant Placement PDFDocumento7 pagineThe Socket-Shield Technique To Support The Buccofacial Tissues at Immediate Implant Placement PDFAhmed Mohammed Saaduddin SapriNessuna valutazione finora
- Horizontal Ridge Augmentation Using Particulate BoneDocumento12 pagineHorizontal Ridge Augmentation Using Particulate Bonecmfvaldesr7Nessuna valutazione finora
- Rehabilitation of Severely Resorbed Edentulous Mandible Using The Modified Visor Osteotomy TechniqueDocumento5 pagineRehabilitation of Severely Resorbed Edentulous Mandible Using The Modified Visor Osteotomy TechniqueSaurabh SatheNessuna valutazione finora
- Bone Ring 1Documento6 pagineBone Ring 1Pradusha RevuruNessuna valutazione finora
- 2007 - Intrusion of Overerupted Molars byDocumento7 pagine2007 - Intrusion of Overerupted Molars byTien Li AnNessuna valutazione finora
- Prosthetic Rehabilitation of Maxillectomy Patient With Telescopic DenturesDocumento6 pagineProsthetic Rehabilitation of Maxillectomy Patient With Telescopic DenturesVero AngelNessuna valutazione finora
- Jurnal ProstodonsiaDocumento4 pagineJurnal ProstodonsiaWulan Ambar WatyNessuna valutazione finora
- Chung 2009Documento19 pagineChung 2009Joshua StalinNessuna valutazione finora
- Edéntulo Tota Superior HíbridaDocumento7 pagineEdéntulo Tota Superior HíbridaAlexis BenitesNessuna valutazione finora
- Tooth TtriyionDocumento5 pagineTooth TtriyionDhanasriNessuna valutazione finora
- Split Technique 2Documento8 pagineSplit Technique 2Alejandro RuizNessuna valutazione finora
- Khoury AnteriorDocumento5 pagineKhoury Anterioralessandra camposNessuna valutazione finora
- Biologically Oriented Preparation Technique (BOPT) For Implant-Supported Fixed ProsthesesDocumento5 pagineBiologically Oriented Preparation Technique (BOPT) For Implant-Supported Fixed ProsthesesazazelNessuna valutazione finora
- Materials: A Modified Ridge Splitting Technique Using Autogenous Bone Blocks-A Case SeriesDocumento10 pagineMaterials: A Modified Ridge Splitting Technique Using Autogenous Bone Blocks-A Case SeriesLouis HutahaeanNessuna valutazione finora
- Corticotomia y Canteamiento Plano OclusalDocumento11 pagineCorticotomia y Canteamiento Plano OclusalKarla SolísNessuna valutazione finora
- Jurnal AccDocumento6 pagineJurnal AcchelmysiswantoNessuna valutazione finora
- Tissueengineeringfor Verticalridge Reconstruction: Neel Patel,, Beomjune Kim,, Waleed Zaid,, Daniel SpagnoliDocumento23 pagineTissueengineeringfor Verticalridge Reconstruction: Neel Patel,, Beomjune Kim,, Waleed Zaid,, Daniel SpagnoliAB MISHRANessuna valutazione finora
- 2005 Laster Width Distraction OsteogenesisDocumento7 pagine2005 Laster Width Distraction Osteogenesislisal1saNessuna valutazione finora
- Strategies in Reconstruction of The Atrophic MaxillaDocumento19 pagineStrategies in Reconstruction of The Atrophic MaxillaEmil CorreaNessuna valutazione finora
- Ankylosed Teeth As Abutments For Maxillary Protraction: A Case ReportDocumento5 pagineAnkylosed Teeth As Abutments For Maxillary Protraction: A Case Reportdrgeorgejose7818Nessuna valutazione finora
- Jameson THE USE OF LINER OCCLUSIO PDFDocumento5 pagineJameson THE USE OF LINER OCCLUSIO PDFLucia Lucero Paz OliveraNessuna valutazione finora
- A Fixed Guide Flange Appliance For HemimandibulectomyDocumento4 pagineA Fixed Guide Flange Appliance For HemimandibulectomyRohan GroverNessuna valutazione finora
- Prosthodontic Management of Severely ResorbedDocumento2 pagineProsthodontic Management of Severely ResorbedAamir BugtiNessuna valutazione finora
- 2020 Article 265Documento7 pagine2020 Article 265Fabian BarretoNessuna valutazione finora
- An 2/2 Implant Overdenture: Case ReportDocumento3 pagineAn 2/2 Implant Overdenture: Case ReportasclepiuspdfsNessuna valutazione finora
- Ams 5 108Documento4 pagineAms 5 108Alice EmailsNessuna valutazione finora
- Anterior Implant EstheticsDocumento9 pagineAnterior Implant EstheticsRatih Cynthia100% (1)
- Full Mouth Rehabilitation of The Patient With Severly Worn Out Dentition A Case Report.Documento5 pagineFull Mouth Rehabilitation of The Patient With Severly Worn Out Dentition A Case Report.sivak_198100% (1)
- Bone Ring Autogenous GraftDocumento4 pagineBone Ring Autogenous GraftHub SciNessuna valutazione finora
- An Esthetic Solution For Single-Implant Restorations - Type Porcelain Veneer Bonded To A Screw-Retained Custom Abutment: A Clinical ReportDocumento6 pagineAn Esthetic Solution For Single-Implant Restorations - Type Porcelain Veneer Bonded To A Screw-Retained Custom Abutment: A Clinical ReportKarnatam DinakarNessuna valutazione finora
- Preliminary Report On A Staged Ridge Splitting Technique For Implant Placement in The Mandible: A Technical NoteDocumento5 paginePreliminary Report On A Staged Ridge Splitting Technique For Implant Placement in The Mandible: A Technical NoteSaurabh SatheNessuna valutazione finora
- Mandible Vertical Height Correction Using LingualDocumento5 pagineMandible Vertical Height Correction Using LingualNguyễn Thái AnNessuna valutazione finora
- Bone Ring 3Documento4 pagineBone Ring 3Pradusha RevuruNessuna valutazione finora
- Multidisciplinary Treatment of A Subgingivally Fractured Tooth With Indirect Restoration A Case ReportDocumento5 pagineMultidisciplinary Treatment of A Subgingivally Fractured Tooth With Indirect Restoration A Case ReportEriana 梁虹绢 SutonoNessuna valutazione finora
- Sectional RPDDocumento5 pagineSectional RPDTejas KhaireNessuna valutazione finora
- Aula EduinaDocumento7 pagineAula EduinaJoão S NetoNessuna valutazione finora
- GholamiDocumento4 pagineGholamiLalaNessuna valutazione finora
- Case Report: Rehabilitation of Posterior Maxilla With Zygomatic and Dental Implant After Tumor Resection: A Case ReportDocumento6 pagineCase Report: Rehabilitation of Posterior Maxilla With Zygomatic and Dental Implant After Tumor Resection: A Case ReportManjulika TysgiNessuna valutazione finora
- Osteogenesis InglesDocumento4 pagineOsteogenesis InglesJulio TorresNessuna valutazione finora
- Esthetic Localized Soft Tissue Ridge Augmentation in A Fixed Partial Denture A Case Report PDFDocumento3 pagineEsthetic Localized Soft Tissue Ridge Augmentation in A Fixed Partial Denture A Case Report PDFAmar Bhochhibhoya0% (1)
- Implants in MandiblesDocumento81 pagineImplants in MandiblesMoataz Mohamed Barakat100% (1)
- A Classification System of DefectsDocumento12 pagineA Classification System of DefectsPrana SkyaNessuna valutazione finora
- Resective Osseous Surgery: A Tool in Restoring Smile - A Case ReportDocumento3 pagineResective Osseous Surgery: A Tool in Restoring Smile - A Case ReportdoctormallikaNessuna valutazione finora
- Dental CatalogueDocumento28 pagineDental CataloguePaulus LagadanNessuna valutazione finora
- HUSNI ADAM - Jurnal Utama No.3Documento3 pagineHUSNI ADAM - Jurnal Utama No.3Adam HusniNessuna valutazione finora
- Bonegraftingforimplant Surgery: Ladi Doonquah,, Pierre-John Holmes,, Laxman Kumar Ranganathan,, Hughette RobertsonDocumento19 pagineBonegraftingforimplant Surgery: Ladi Doonquah,, Pierre-John Holmes,, Laxman Kumar Ranganathan,, Hughette RobertsonJason LeeNessuna valutazione finora
- Bone and Bone Graft HealingDocumento12 pagineBone and Bone Graft HealingJayanth PerumalNessuna valutazione finora
- DNB Qs 10 Yrs PDFDocumento65 pagineDNB Qs 10 Yrs PDFHaribabu ArumugamNessuna valutazione finora
- 60539b628a2420261a40480b64a41d7aDocumento4 pagine60539b628a2420261a40480b64a41d7aAbdullah özel100% (1)
- Cleft Lip & Palate SurgeryDocumento5 pagineCleft Lip & Palate SurgeryShoaib A. KaziNessuna valutazione finora
- Review Cirugía Preprotésica. ArtículoDocumento9 pagineReview Cirugía Preprotésica. ArtículoAnita Estela Batz MatulNessuna valutazione finora
- Extraction-Site Ridge Preservation: Clinical Techniques in PeriodonticsDocumento5 pagineExtraction-Site Ridge Preservation: Clinical Techniques in PeriodonticsrmarawanNessuna valutazione finora
- Direct vs. Indirect Sinus Lift Procedure: A Comparison: March 2012Documento8 pagineDirect vs. Indirect Sinus Lift Procedure: A Comparison: March 2012Sidhartha KumarNessuna valutazione finora
- Question Paper Preview: 1. Cemento - Enamel JunctionDocumento8 pagineQuestion Paper Preview: 1. Cemento - Enamel Junctionswati agarwalNessuna valutazione finora
- Limitations of Autograft and Allograft New Synthetic Solutions PDFDocumento10 pagineLimitations of Autograft and Allograft New Synthetic Solutions PDFSantiago VázquezNessuna valutazione finora
- Ca. Ca.: - .,.1b1h1tlesDocumento179 pagineCa. Ca.: - .,.1b1h1tleshNessuna valutazione finora
- Proximal Humerus and Humeral Shaft NonunionsDocumento11 pagineProximal Humerus and Humeral Shaft NonunionsRina AlvionitaNessuna valutazione finora
- Inion Freedom Brochure v2 12-2014Documento11 pagineInion Freedom Brochure v2 12-2014Ivo van de KampNessuna valutazione finora
- Exabone PasteDocumento4 pagineExabone PasteExabone GmbHNessuna valutazione finora
- Bukti ACCELERATION OF BONE FRACTURE HEALINGDocumento18 pagineBukti ACCELERATION OF BONE FRACTURE HEALINGsanny silabanNessuna valutazione finora
- Management of Segmental Bone DefectDocumento11 pagineManagement of Segmental Bone DefectZin HtutNessuna valutazione finora
- Implant Dentistry - The Most Promising Discipline of DentistryDocumento488 pagineImplant Dentistry - The Most Promising Discipline of DentistrydrescobedocomfNessuna valutazione finora
- Ijdr 12414Documento5 pagineIjdr 12414Ahmed BadrNessuna valutazione finora
- Principles of Bone GraftingDocumento6 paginePrinciples of Bone GraftingJayanth Perumal100% (2)
- Bicon Catalog 2012Documento68 pagineBicon Catalog 2012Bicon Implant InaNessuna valutazione finora
- Lampiran Bongros 5ccDocumento7 pagineLampiran Bongros 5ccNgurah AndhikaNessuna valutazione finora
- Congenital Pseudoarthrosis of The Clavicle A Rare CaseDocumento5 pagineCongenital Pseudoarthrosis of The Clavicle A Rare CaseInternational Medical PublisherNessuna valutazione finora
- Final PaperDocumento12 pagineFinal PaperKhaled Atef ElhayesNessuna valutazione finora
- Bone Graft and Gbr1Documento34 pagineBone Graft and Gbr1Dr. Nachammai NagarajanNessuna valutazione finora
- Craniosynostosis Surgery: The Legacy of Paul Tessier: Historical VignetteDocumento8 pagineCraniosynostosis Surgery: The Legacy of Paul Tessier: Historical VignetteKiky Martha A.Nessuna valutazione finora
- Contemporary Implant Dentistry 3eDocumento5 pagineContemporary Implant Dentistry 3etrivex8825% (4)
- OsteosintesisDocumento15 pagineOsteosintesisNicolásNessuna valutazione finora
- PHD Thesis Guidelines UclDocumento8 paginePHD Thesis Guidelines Ucldnrssvyt100% (2)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Da EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Valutazione: 3 su 5 stelle3/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDa EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedValutazione: 4.5 su 5 stelle4.5/5 (82)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDa EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDValutazione: 5 su 5 stelle5/5 (3)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDa EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionValutazione: 4 su 5 stelle4/5 (404)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDa EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityValutazione: 4 su 5 stelle4/5 (32)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDa EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeValutazione: 2 su 5 stelle2/5 (1)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesDa EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesValutazione: 4.5 su 5 stelle4.5/5 (1412)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsDa EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNessuna valutazione finora
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDa EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsValutazione: 4 su 5 stelle4/5 (4)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDa EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsValutazione: 5 su 5 stelle5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDa EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisValutazione: 4.5 su 5 stelle4.5/5 (42)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDa EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Obesity Code: Unlocking the Secrets of Weight LossDa EverandThe Obesity Code: Unlocking the Secrets of Weight LossValutazione: 4 su 5 stelle4/5 (6)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDa EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityValutazione: 4.5 su 5 stelle4.5/5 (6)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisDa EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisValutazione: 3.5 su 5 stelle3.5/5 (2)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeDa EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeValutazione: 4.5 su 5 stelle4.5/5 (254)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Da EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Valutazione: 4.5 su 5 stelle4.5/5 (110)
- To Explain the World: The Discovery of Modern ScienceDa EverandTo Explain the World: The Discovery of Modern ScienceValutazione: 3.5 su 5 stelle3.5/5 (51)
- Critical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsDa EverandCritical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsValutazione: 4.5 su 5 stelle4.5/5 (39)
- The Marshmallow Test: Mastering Self-ControlDa EverandThe Marshmallow Test: Mastering Self-ControlValutazione: 4.5 su 5 stelle4.5/5 (60)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingDa EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingValutazione: 4 su 5 stelle4/5 (1138)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessDa EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessValutazione: 4.5 su 5 stelle4.5/5 (328)