Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
The Tree in Bud Sign
Caricato da
Munish GuleriaDescrizione originale:
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
The Tree in Bud Sign
Caricato da
Munish GuleriaCopyright:
Formati disponibili
Signs in Imaging
Edith Eisenhuber, MD
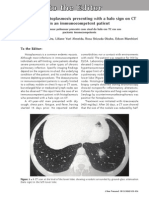
The Tree-in-Bud Sign1
APPEARANCE
The tree-in-bud sign is a nding seen on thin-section computed tomographic (CT) images of the lung (13). Peripheral (within approximately 35 mm of the pleural surface), small (2 4 mm in diameter), centrilobular, and well-dened nodules of soft-tissue attenuation are connected to linear, branching opacities that have more than one contiguous branching site, thus resembling a tree in bud (1 4) (Figs 1, 2). The tree-in-bud pattern is particularly well depicted by thinsection CT. It is not visible on chest radiographs. The appearance of the tree-in-bud sign is closely linked to the anatomy of the secondary pulmonary lobule. Each secondary lobule is supplied by a lobular bronchiole and a lobular artery that are located in the center of the lobule. Under normal circumstances, the intralobular bronchiole is less than 1 mm in diameter and is not normally visible on CT scans (8). However, diseased bronchioles with mucous plugging, wall thickening, or dilatation can be visualized on thin-section CT scans, often displaying the tree-in-bud phenomenon. The tree-in-bud sign has primarily been used as a descriptive term for abnormalities found on CT scans of the lung in patients with endobronchial spread of Mycobacterium tuberculosis (6). In the past several years, however, it has become clear that the nding of a tree-in-bud sign on a CT scan is not specic for a single pulmonary disease entity, but it can be found with a large number of conditions, primarily those of infectious origin, but also with immunologic disorders, congenital disorders, neoplasms, aspiration of irritant substances, and disease entities with idiopathic causes (2,5). Pulmonary infectious disorders involving the small airways are the most common causes of the tree-in-bud sign (2). Any infectious organism, including bacterial, mycobacterial, viral, parasitic, and fungal agents, can involve the small airways and cause a tree-in-bud pattern. In pulmonary infectious disorders, the tree-in-bud sign has most commonly been described in patients with endobronchial spread of M tuberculosis (6,9). In patients with pulmonary tuberculosis, the tree-in-bud pattern is the most characteristic, but not pathognomonic, CT feature of active endobronchial spread and can be found in 72% of patients with active disease (6). At histopathologic examination, the tree-in-bud opacities seen on CT scans were correlated with caseous material in the small airways (6). The terminal tufts of the tree-in-bud pattern may represent inammation with caseous material in the respiratory bronchioles and alveolar ducts, whereas the stalks may represent caseous material within the terminal bronchiole (6). Similarly, bronchogenic dissemination of atypical mycobacterial organisms or pyogenic bacteria can result in tree-inbud opacities (10 12) (Fig 2). Less frequently, the tree-in-bud sign is seen with viral and fungal infections (eg, invasive as-
EXPLANATION
The tree-in-bud pattern represents bronchiolar luminal impaction with mucus, pus, or uid, which demarcates the normally invisible branching course of the peripheral airways (13,5,6). In addition, dilated and thickened walls of the peripheral airways and peribronchiolar inammation can contribute to the visibility of affected bronchioles (1,5,6). In histopathologic studies, the tree-in-bud appearance correlates well with the presence of plugging of the small airways with mucus, pus, or uid; dilated bronchioles; bronchiolar wall thickening; and peribronchiolar inammation (1,6,7).
DISCUSSION
The tree-in-bud sign has become a popular descriptive term for various diseases of the peripheral airways in which mucous plugging, bronchial dilatation, and wall thickening are present (2,5). In addition, indirect signs of bronchiolar disease, such as air trapping or subsegmental consolidation, may be present.
Index terms: Bronchi, abnormalities, 671.265 Bronchiolitis, 671.2191 Lung, infection, 671.203, 671.265, 671.23 Signs in Imaging Published online before print 10.1148/radiol.2223991980 Radiology 2002; 222:771772
1
From the Department of Radiology, University of Vienna, Waehringer Guertel 18-20, A-1090 Vienna, Austria. Received November 11, 1999; revision requested December 10; revision received and accepted May 22, 2000. Address correspondence to the author (email: edith.eisenhuber@univie.ac.at). RSNA, 2002
A trainee (resident or fellow) wishing to submit a manuscript for Signs in Imaging should rst write to the Editor for approval of the sign to be prepared, to avoid duplicate preparation of the same sign.
771
Figure 1. spring.
Photograph of a twig obtained from a budding tree in
pergillosis of the airways) and Pneumocystis carinii pneumonia (2,5). The tree-in-bud sign is also a common nding on thinsection CT scans in patients with diffuse panbronchiolitis (1,7). In histopathologic studies, the centrilobularly distributed nodular and branching linear opacities at CT correspond to thickened and dilated bronchiolar walls with intraluminal mucous plugs (1,7). In addition, various congenital disorders can cause diseases of the small airways that demonstrate a tree-in-bud pattern. In patients with cystic brosis, thick-walled mucus- or pus-lled bronchioles are frequently seen as branching or nodular centrilobular opacities at CT, usually associated with central bronchiectasis (2). Similar ndings can be seen in patients with chronic infections of the small airways due to dyskinetic cilia syndrome, yellow nail syndrome, or congenital immunodeciency states (5,10). Primary pulmonary lymphoma has recently been reported as a rare but important differential diagnosis for the tree-in-bud pattern. Lymphomatous involvement of the lung can simulate the radiologic ndings of bronchiolitis (13). In summary, the tree-in-bud sign is a characteristic and easily detectable CT nding in patients with disease of the small airways. It is a useful sign, which, in the appropriate context of clinical ndings and laboratory features, almost invariably points to inammatory disease of the small airways.
References 1. Akira M, Kitatani F, Lee YS, et al. Diffuse panbronchiolitis: evaluation with high-resolution CT. Radiology 1988; 168:433 438. 2. Aquino SL, Gamsu G, Webb WR, Kee ST. Tree-in-bud pattern: frequency and signicance on thin section CT. J Comput Assist Tomogr 1996; 20:594 599. 3. Gruden JF, Webb WR. Identication and evaluation of centrilobu-
Figure 2. Thin-section CT scan obtained in a 29-year-old man with acute myeloid leukemia after bone marrow transplantation. The patient had a history of fever and cough. Image shows multiple, small, centrilobular nodules of soft-tissue attenuation connected to linear branching opacities (arrows). Note the morphologic similarities to the photograph of the tree in bud (Fig 1). At serologic examination, an infection with Mycoplasma pneumoniae was conrmed.
4. 5. 6. 7. 8. 9. 10. 11. 12. 13.
lar opacities on high-resolution CT. Semin Ultrasound CT MR 1995; 16:435 449. Itoh H, Tokunaga S, Asamoto H, et al. Radiologic-pathologic correlations of small lung nodules with special reference to peribronchiolar nodules. AJR Am J Roentgenol 1978; 130:223231. Collins J, Blankenbaker D, Stern EJ. CT patterns of bronchiolar disease: what is tree-in-bud? AJR Am J Roentgenol 1998; 171: 365370. Im JG, Itoh H, Shim YS, et al. Pulmonary tuberculosis: CT ndings early active disease and sequential change with antituberculous therapy. Radiology 1993; 186:653 660. Fitzgerald JE, King TE Jr, Lynch DA, Tuder RM, Schwarz MI. Diffuse panbronchiolitis in the United States. Am J Respir Crit Care Med 1996; 154:497503. Muller NL, Miller RR. Diseases of the bronchioles: CT and histopathologic ndings. Radiology 1995; 196:312. Hatipoglu ON, Osma E, Manisali M, et al. High resolution computed tomographic ndings in pulmonary tuberculosis. Thorax 1996; 51:397 402. Gruden JF, Webb WR, Warnock M. Centrilobular opacities in the lung on high-resolution CT: diagnostic considerations and pathologic correlation. AJR Am J Roentgenol 1994; 162:569 574. Hartman TE, Swensen SJ, Williams DE. Mycobacterium aviumintracellulare complex: evaluation with CT. Radiology 1993; 187: 2326. Moore EH. Atypical mycobacterial infection in the lung: CT appearance. Radiology 1993; 187:777782. Hwang JH, Kim TS, Han J, Lee KS. Primary lymphoma of the lung simulating bronchiolitis: radiologic ndings. AJR Am J Roentgenol 1998; 170:220 221.
772
Radiology
March 2002
Eisenhuber
Potrebbero piacerti anche
- Equine Board ReviewDocumento34 pagineEquine Board ReviewGurpreet SinghNessuna valutazione finora
- Medical Mnemonic Sketches : Pulmonary DiseasesDa EverandMedical Mnemonic Sketches : Pulmonary DiseasesNessuna valutazione finora
- The Covid Vaccine Linked To CancerDocumento34 pagineThe Covid Vaccine Linked To CancerNoyb Nal100% (4)
- 5.thyroid Gland LectureDocumento96 pagine5.thyroid Gland Lecturesdsher100% (3)
- Radiographic Signs of Pulmonar DiseaseDocumento10 pagineRadiographic Signs of Pulmonar DiseaseMarleeng CáceresNessuna valutazione finora
- Medicated Nail Lacquers - For Effective Treatment of Nail DisordersDocumento12 pagineMedicated Nail Lacquers - For Effective Treatment of Nail DisordersBaru Chandrasekhar RaoNessuna valutazione finora
- Preboards MICRODocumento6 paginePreboards MICROM C100% (1)
- Bronchiolitis A Practical Approach For The General RadiologistDocumento42 pagineBronchiolitis A Practical Approach For The General RadiologistTara NareswariNessuna valutazione finora
- Gentamicin Drug SummDocumento1 paginaGentamicin Drug SummWarren100% (1)
- Medical Surgical Nursing Nclex Questions7Documento7 pagineMedical Surgical Nursing Nclex Questions7dee_day_8Nessuna valutazione finora
- Case Clerking SG SipuuuttDocumento11 pagineCase Clerking SG Sipuuuttsafwan67% (3)
- Immunization Knowledge, Attitude and Practice Among Mothers of Children From 0 To 5 YearsDocumento7 pagineImmunization Knowledge, Attitude and Practice Among Mothers of Children From 0 To 5 YearsUlil Amri Pramadani100% (1)
- Bovine Mastitis PDFDocumento34 pagineBovine Mastitis PDFMamtaNessuna valutazione finora
- Description of DiseaseDocumento10 pagineDescription of DiseaseRajaNessuna valutazione finora
- Interstitial Lung DiseaseDocumento4 pagineInterstitial Lung DiseasedewimarisNessuna valutazione finora
- Infection PulmonaryDocumento14 pagineInfection Pulmonaryvina_vina100% (1)
- PDF To WordDocumento17 paginePDF To Wordanisa ghinaNessuna valutazione finora
- Imaging Pulmonary Infection: Classic Signs and PatternsDocumento18 pagineImaging Pulmonary Infection: Classic Signs and PatternsRizky MaulydaNessuna valutazione finora
- Jurnal Radiologi TBDocumento7 pagineJurnal Radiologi TBrian00019Nessuna valutazione finora
- Jurnal RadiologiDocumento3 pagineJurnal RadiologiKevinBrevianNessuna valutazione finora
- Bronquiolite DiagnosticoDocumento14 pagineBronquiolite DiagnosticoFrederico PóvoaNessuna valutazione finora
- Neu Motor AxDocumento6 pagineNeu Motor AxZay SiagNessuna valutazione finora
- Esti2012 E-0066Documento40 pagineEsti2012 E-0066nistor97Nessuna valutazione finora
- Seminar For Clinicians: Radiographic Differentiation of Advanced Fibrocystic Lung DiseasesDocumento9 pagineSeminar For Clinicians: Radiographic Differentiation of Advanced Fibrocystic Lung DiseasesmandasetwulNessuna valutazione finora
- Tuberculosis From Head To Toe: (CME Available in Print Version and On RSNA Link)Documento22 pagineTuberculosis From Head To Toe: (CME Available in Print Version and On RSNA Link)nayejih371Nessuna valutazione finora
- Bookshelf NBK553857Documento12 pagineBookshelf NBK553857Sanda Škrinjarić-CincarNessuna valutazione finora
- Bronchiolitis in Adult: A ReviewDocumento7 pagineBronchiolitis in Adult: A ReviewNamira Firdha KNessuna valutazione finora
- CT Halo SignDocumento4 pagineCT Halo Signmitmat4uNessuna valutazione finora
- Diagnostic Approach To The Adult With Cystic Lung Disease - UpToDateDocumento21 pagineDiagnostic Approach To The Adult With Cystic Lung Disease - UpToDateAnestesio 2022Nessuna valutazione finora
- Journal Radiologi 3Documento14 pagineJournal Radiologi 3WinayNayNessuna valutazione finora
- Challenges in Pulmonary Fibrosis ? 3: Cystic Lung Disease: Review SeriesDocumento11 pagineChallenges in Pulmonary Fibrosis ? 3: Cystic Lung Disease: Review SeriesedelinNessuna valutazione finora
- 1 s2.0 S0140673622010522 MainDocumento18 pagine1 s2.0 S0140673622010522 MainMirella Rugel SocolaNessuna valutazione finora
- 1 s2.0 S0140673622010522 MainDocumento18 pagine1 s2.0 S0140673622010522 MainsilviaNessuna valutazione finora
- Role of Multi-Detector Computed Tomography in Evaluation of Lung AnomaliesDocumento16 pagineRole of Multi-Detector Computed Tomography in Evaluation of Lung AnomaliesIJAR JOURNALNessuna valutazione finora
- Letter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationDocumento3 pagineLetter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationfatimiahmastaNessuna valutazione finora
- Journal ReadingDocumento42 pagineJournal Readingnurza yeyeniNessuna valutazione finora
- Thoracic Manifestations of Connective Tissue DiseasesDocumento50 pagineThoracic Manifestations of Connective Tissue DiseasesAnkita ShahNessuna valutazione finora
- Journal Reading: TuberculosisDocumento44 pagineJournal Reading: Tuberculosisnurza yeyeniNessuna valutazione finora
- Chest X-Ray Manifestations of PneumoniaDocumento3 pagineChest X-Ray Manifestations of PneumoniaVishesh SoodNessuna valutazione finora
- Diagnosis and Treatment of Cystic Lung Disease: Sanghoon Park and Eun Joo LeeDocumento10 pagineDiagnosis and Treatment of Cystic Lung Disease: Sanghoon Park and Eun Joo LeeicaeeeNessuna valutazione finora
- Ultra-Rare Cystic DiseaseDocumento17 pagineUltra-Rare Cystic DiseaseRaul DoctoNessuna valutazione finora
- Gharib2001 Radiologi Pneumonia-DikonversiDocumento31 pagineGharib2001 Radiologi Pneumonia-Dikonversitsamara24_Nessuna valutazione finora
- NeumoniaDocumento14 pagineNeumoniaPedro TumbacoNessuna valutazione finora
- Patrones Tomograficos Epid PDFDocumento28 paginePatrones Tomograficos Epid PDFYony Morales LeonNessuna valutazione finora
- Complications of Pulmonary TuberculosisDocumento18 pagineComplications of Pulmonary TuberculosisedhobiondiNessuna valutazione finora
- Pitfalls of EmphysemaDocumento7 paginePitfalls of EmphysemaWahyu Puspita IrjayantiNessuna valutazione finora
- Pneumo Cist IsDocumento6 paginePneumo Cist IsAlexei RobuNessuna valutazione finora
- 2.BE PathogenesisDocumento7 pagine2.BE PathogenesisJaya Semara PutraNessuna valutazione finora
- FPI Progn TratDocumento13 pagineFPI Progn TratTurcu AndreeaNessuna valutazione finora
- Chronic Airspace DiseasesDocumento31 pagineChronic Airspace DiseasesAnkita ShahNessuna valutazione finora
- Interstitial Pneumonia Seminar PaperDocumento9 pagineInterstitial Pneumonia Seminar PaperLamy SNessuna valutazione finora
- Main Image ©muratseyit/istockphotoDocumento10 pagineMain Image ©muratseyit/istockphotoade_liaNessuna valutazione finora
- Diagnostic Evaluation of BronchiectasisDocumento16 pagineDiagnostic Evaluation of BronchiectasisAinun Jariah MuliadiNessuna valutazione finora
- Pulmonary Histoplasmosis Presenting With A Halo Sign On CT in An Immunocompetent PatientDocumento2 paginePulmonary Histoplasmosis Presenting With A Halo Sign On CT in An Immunocompetent PatientSharom R. AlvarezNessuna valutazione finora
- Journal of Thoracic ImagingDocumento11 pagineJournal of Thoracic Imagingestues2Nessuna valutazione finora
- BRONKIEKTASIS BaruDocumento23 pagineBRONKIEKTASIS BaruRamanda Cahya UmbarraNessuna valutazione finora
- Diagnostic Approach To The Adult With Cystic Lung Disease - UpToDateDocumento20 pagineDiagnostic Approach To The Adult With Cystic Lung Disease - UpToDateTatiana Valencia CastañoNessuna valutazione finora
- The Many Faces of Cryptogenic Organizing Pneumonia (COP)Documento7 pagineThe Many Faces of Cryptogenic Organizing Pneumonia (COP)Miguel Angel GarciaNessuna valutazione finora
- Clinically Relevant Phenotypes in Chronic RhinosinusitisDocumento22 pagineClinically Relevant Phenotypes in Chronic RhinosinusitisA.Nessuna valutazione finora
- Depiction Control: ECG Prognostic Significance of ECG Changes in Acute PneumoniaDocumento5 pagineDepiction Control: ECG Prognostic Significance of ECG Changes in Acute PneumoniaAudrey Martin RañisesNessuna valutazione finora
- Potential Pathogenesis and Clinical Aspects of Pulmonary Fibrosis Associated With Rheumatoid ArthritisDocumento6 paginePotential Pathogenesis and Clinical Aspects of Pulmonary Fibrosis Associated With Rheumatoid ArthritisLiya SuwarniNessuna valutazione finora
- Tree in BudDocumento3 pagineTree in BudChakradhar ChakrreNessuna valutazione finora
- Computed Tomography Findings of Community-Acquired Immunocompetent Patient: A Case ReportDocumento4 pagineComputed Tomography Findings of Community-Acquired Immunocompetent Patient: A Case ReportDenta HaritsaNessuna valutazione finora
- Parasitic Infections of The Lung: A Guide For The Respiratory PhysicianDocumento9 pagineParasitic Infections of The Lung: A Guide For The Respiratory Physicianحسام الدين إسماعيلNessuna valutazione finora
- Case Reporttonsillar Tuberculosis Simulating A Cancer and Revealing Miliary Pulmonary TuberculosisDocumento5 pagineCase Reporttonsillar Tuberculosis Simulating A Cancer and Revealing Miliary Pulmonary TuberculosisIJAR JOURNALNessuna valutazione finora
- 2021-Congenital Pulmonary Airway MalformationDocumento8 pagine2021-Congenital Pulmonary Airway MalformationAzucena La QuirozNessuna valutazione finora
- TracheitisDocumento7 pagineTracheitisÁlvaro DezaNessuna valutazione finora
- Assessing and Treating Small Airways Disease in Asthma and Chronic Obstructive Pulmonary DiseaseDocumento12 pagineAssessing and Treating Small Airways Disease in Asthma and Chronic Obstructive Pulmonary DiseasePetra ŠalamúnováNessuna valutazione finora
- Lung Disease in Rheumatoid ArthritisDa EverandLung Disease in Rheumatoid ArthritisAryeh FischerNessuna valutazione finora
- Vap Poster WPB VaDocumento1 paginaVap Poster WPB VaJoe ThesecondmonthNessuna valutazione finora
- Clinical Bacteriology Lecture (W01)Documento3 pagineClinical Bacteriology Lecture (W01)nicholehernandez05Nessuna valutazione finora
- Wuchereria Bancrofti Brugia Malayi Loa Loa Onchocerca Volvulus Mansonella Perstans Mansonella Ozzardi Dracunculus MedinensisDocumento4 pagineWuchereria Bancrofti Brugia Malayi Loa Loa Onchocerca Volvulus Mansonella Perstans Mansonella Ozzardi Dracunculus MedinensisJoshua TrinidadNessuna valutazione finora
- CDC February 2014Documento179 pagineCDC February 2014bryan_millan_9100% (1)
- Robert Koch PDFDocumento5 pagineRobert Koch PDFFarzanaShaikNessuna valutazione finora
- BMBL-5th EditionDocumento421 pagineBMBL-5th EditionBryan OngNessuna valutazione finora
- 15 - Chapter 7 PDFDocumento4 pagine15 - Chapter 7 PDFRamNessuna valutazione finora
- Types of MicroorganismsDocumento69 pagineTypes of MicroorganismshyvasNessuna valutazione finora
- Bacteriophage Phix174Documento3 pagineBacteriophage Phix174Arul ManiNessuna valutazione finora
- Soalan Pathology 3Documento425 pagineSoalan Pathology 3muhammadridhwanNessuna valutazione finora
- Parasitology (Pictures)Documento17 pagineParasitology (Pictures)ahmed AhmedNessuna valutazione finora
- Daftar PustakaDocumento3 pagineDaftar Pustakahendri najibNessuna valutazione finora
- Oral Cavity Is The Mirror of Your Own BodyDocumento60 pagineOral Cavity Is The Mirror of Your Own BodyNazia AliNessuna valutazione finora
- Acute Viral Encephalitis in Children Clinical Manifestations and DiagnosisDocumento41 pagineAcute Viral Encephalitis in Children Clinical Manifestations and DiagnosisCRISTOPHER CHAVAR GARCIANessuna valutazione finora
- Approach To The Adult With Fever of Unknown OriginDocumento9 pagineApproach To The Adult With Fever of Unknown OriginsezenitNessuna valutazione finora
- IPC M8 BloodbanksLabs PDFDocumento54 pagineIPC M8 BloodbanksLabs PDFMaryam AimanNessuna valutazione finora
- UntitledDocumento2 pagineUntitledsomaticayurvedaNessuna valutazione finora
- Truth About The Weird PandemicDocumento63 pagineTruth About The Weird PandemicHarshita ShivanagowdaNessuna valutazione finora
- (3)Documento20 pagine(3)Muhammad Hadi ArwaniNessuna valutazione finora
- Radiographic Cardiopulmonary Changes in Dogs With Heartworm DiseaseDocumento8 pagineRadiographic Cardiopulmonary Changes in Dogs With Heartworm DiseaseputriwilujengNessuna valutazione finora