Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Cystic Swellings of The Neck - 2009 - Surgery (Oxford)
Caricato da
Muhammad AdilDescrizione originale:
Titolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Cystic Swellings of The Neck - 2009 - Surgery (Oxford)
Caricato da
Muhammad AdilCopyright:
Formati disponibili
HEAD AND NECK
Cystic swellings of the neck Key aspects of history-taking from patients with neck
lumps
William AE Parker
Andrew J Parker History of presenting complaint
Duration
Onset e sudden, gradual, congenital
Changes in size and exacerbating factors e.g. increasing in size
Abstract
when eating
Cystic neck swellings in the neck arise from a diverse range of tissues and
pathological disorder. The approach to diagnosis relies on a thorough Associated symptoms
history and an appropriate examination including the internal ENT to Pain
exclude an occult primary malignancy. The typical feature of fluctuance is Dysphagia
often not elicited because the contents of the cyst can be under tension Dysphonia
and transillumination is seldom performed these days. Aspiration and ultra- Hypo/hyperthyroid symptoms
sonography are usual but other imaging such as CTand MRI scanning can be Weight loss
indicated. Definitive treatment is usually surgical excision but with benign Night sweats
disease repeat aspiration can be considered. No intervention can be an Any other swellings
option if there is significant co-morbidity, absence of functional or cosmetic
Past medical/surgical/family history
impairment or there is reluctance by the patient to undergo surgery.
Endocrine disorders
Congenital abnormality
Keywords cyst; fine needle biopsy; neck lump; salivary gland; thyroid
Malignancy
Trauma/neck surgery
Drug history
Introduction Social history
Cystic swellings of the neck comprise an important group of head Smoking status
and neck pathologies. They are relatively common and often cause Occupation
alarm in patients presenting with them. Cysts can arise from any
component of the neck and hence thorough knowledge of the
Box 1
embryology, anatomy and pathology is vital for correct diagnosis
and management. Here we consider the main groups of cystic within an epithelialized cavity. A pseudocyst is defined as the
swellings, discussing their origin, clinical features and treatment. presence of fluid within a tissue or tissue space, but without an
Some neck cysts are thought to have a congenital origin. The epithelial boundary. When considered together, cystic lesions of
neck develops in utero from fusion of ectodermal, mesodermal and the neck form a diverse collection of pathological disorders.
endodermal elements. There are five branchial arches containing To evaluate the situation further, the clinician needs to
cartilaginous, muscular, neural and blood vessel elements and undertake history-taking and examination along conventional
corresponding clefts on each side which become fused. Ecto- lines, the latter dividing into inspection, palpation and auscul-
dermal tissue from the second arch then grows down caudally to tation. Investigations may then be needed and are discussed
form the external neck covering and this arrangement is a throw- below.
back to the pattern found in vertebrates with a primitive gill
apparatus. In the midline where the upper arches meet is a small History
elevation known as the tuberculum impar containing a median The history should include ascertaining the nature of the pre-
depression known as the foramen caecum which gives rise to the senting complaint, namely duration, speed of onset, changes in
primordial thyroid tissue, which then descends in the neck taking size since onset, any exacerbating factors (for example when
with it a thyroglossal tract which then becomes obliterated. eating), presence or absence of pain, dysphagia, dysphonia,
hypo/hyperthyroid symptoms, weight loss, night sweats, other
Diagnosis and general considerations swellings, as well as the usual past medical, surgical, drug, social
The management of a patient with a neck lump poses several and family histories, looking particularly at endocrine disorders,
challenges to the clinician. A cyst implies the presence of fluid congenital abnormality, malignancy, trauma and smoking status
(see Box 1).
William AE Parker BA (Hons) is a Clinical Medical Student, Magdalene Examination
College and Addenbrooke’s Hospital, University of Cambridge. Conflicts There are various ways of classifying neck cysts. From the point
of interest: none. of obtaining a diagnosis, probably the best method is as set out
below and in Figure 1.
Andrew J Parker LLM ChM DLO FRCS is a Consultant ENT and Head & Neck 1. Is the lesion fixed to the skin or within subcutaneous tissue?
Surgeon, Senior Lecturer in ENT Surgery, Royal Hallamshire Hospital This implies that the lump can be picked up with the skin and
and Sheffield University. Conflicts of interest: none. moves with it and is not fixed to underlying structures. The
SURGERY 27:12 530 Ó 2009 Published by Elsevier Ltd.
HEAD AND NECK
Algorithm for diagnosis of cystic neck swellings on examination
Cystic swelling in the neck
Fixed to
the skin In/fixed to the Deep
skin or deep?
Epidermal cyst lipoma
Lateral Midline or
lateral?
Midline
No
No
Branchial cyst
Moves on Moves on Cystic
Salivary gland cyst
swallowing? swallowing? hygroma
Cystic hygroma
Yes Yes
No
Moves on tongue Thyroid
Thyroid cyst
protrustion? cyst
Yes
No
Above Thyroglossal
the hyoid? cyst
Yes
Sublingual dermoid
Figure 1
classic example is an epidermal cyst. It is important to remember Other ways of determining a differential diagnosis include
that at body temperature fat can feel fluid and a lipoma can have trying to ascertain the tissue of origin by clinical and anatomical
a cystic quality, although it is not a cyst. Note that these are characteristics, for example a cystic swelling present in the
generalized disorders and can occur anywhere there is skin or parotid area, and some clinicians may find the traditional
fat. ‘surgical sieve’ approach to diagnosis useful, as shown in Box 2.
2. What is the anatomical location? Is it midline or lateral?
Midline neck cysts are generally either thyroid, thyroglossal or
The ‘surgical sieve’ applied to cystic neck swellings
sublingual dermoid. These can however sometimes be lateral.
3. Does it move on swallowing? Congenital Acquired
Any lesion attached to the laryngopharyngeal structures, including Cystic hygroma Traumatic e pseudocyst
the hyoid, would do this including the three examples given in (2). Thyroglossal cysts Inflammatory e branchial cyst, some
4. What is its relation to the hyoid bone? Branchial cysts thyroid and salivary gland cysts
Midline cysts at the level of or below the hyoid that move on Neoplastic e some thyroid and salivary
swallowing are thyroglossal or thyroid in nature and those above gland cysts
represent sublingual dermoids. Degenerative e pseudocyst
5. Does it move on tongue protrusion? Other
This suggests a thyroglossal cyst or, uncommonly, something
attached to the hyoid bone such as a sublingual dermoid. Box 2
SURGERY 27:12 531 Ó 2009 Published by Elsevier Ltd.
HEAD AND NECK
During examination the patient should be seated, be fully with profound consequences. Differential diagnosis should
exposed from the clavicles upwards and be seen in good light. An include haemangiomata and it is useful that any surgeon
internal ENT examination is similarly essential and this should attempting excision should have this diagnosis excluded first.
include at least examination of the oral cavity, oro-pharynx and Aspiration may temporarily relieve the problem, but never in
indirect laryngoscopy or flexible fibreoptic endoscopy in outpatients the long term and surgical excision is the treatment of choice. This
under local anaesthesia. This is necessary to ascertain whether or is potentially difficult because of important anatomical relations,
not the lesion is related to the internal ENT structures and particu- such as the great vessels and lower cranial nerves. Recurrent
larly applies to an occult malignancy, which cannot be excluded lesions are often seen and it is not uncommon to require multiple
otherwise. This is an omission that is potentially negligent. operations throughout the course of a patient’s life.
Clinical characteristics of a cystic swelling are those of fluc- Sclerosant agents have been used to good effect including in
tuancy where the examiner’s fingers on either side of the lesion utero. These include OK-432 (a lyophilized incubation mixture of
are displaced outwards when pressure is applied to the centre of group A Streptococcus pyogenes of human origin), also known as
the cyst and also translucency, although the latter is rarely per- Picibanil3 and the antineoplastic agent bleomycin.4 However,
formed outside the examination hall! these drugs are not licensed for this use.
Investigations Branchial cysts
It is often reasonable practice to aspirate the lesion in clinic with An understanding of the embryology of the neck is essential in
a needle and syringe as it confirms the cystic nature of the lump the appreciation of branchial fistulae and sinuses because of the
and enables cytological, biochemical and microbiological anal- important anatomical relationships which can make excisional
ysis to be undertaken, but this is often performed in association surgery fraught with difficulty. The aetiology of the branchial
with an ultrasound scan. cyst is controversial and most authorities consider that is not in
It is usual to undertake some form of imaging as further fact a congenital disorder, but rather a cystic degeneration within
investigation. Ultrasonography is a very useful technique and a lymph node.5 The branchial cyst is seen in young adults, rather
needle aspiration can be performed at the same time. An elegant than at birth, and typically lies at the junction of the upper and
review of this mode of imaging and its application to cystic neck lower two-thirds of the sternomastoid muscle, either anterior or
swellings is provided by El-Simily and Corney, 1993.1 deep to it. They occur more frequently in males, in their thirties
Other techniques include magnetic resonance imaging (MRI) and and in the anterior triangle of the neck.
computed tomography (CT) scanning. There is no place for plain Occasionally, because of the tension within the cyst, the lesion
neck X-rays and barium swallow contrast examinations are of limited feels solid. Again, it can dramatically increase in size and become
value in the investigation of a patient thought to have a neck cyst. infected. A detailed internal ENT examination is essential. Aspira-
This review deals with the clinical presentation, diagnosis and tion shows straw-coloured fluid, typically showing degenerate
management of various common cystic lesions specific to the neck. keratinocytes and cholesterol crystals. The diagnosis of a branchial
cyst in those over 40 years of age should be made with trepidation as
Specific lesions it can be cystic degeneration in a lymph node containing metastatic
Epidermal cysts and sebaceous cysts squamous carcinoma from an internal ENT occult primary.6
The clinical characteristic of an epidermal (sebaceous) cyst is one Treatment is usually by surgical excision unless the patient
of a tense swelling within the skin, usually with absence of prefers recurrent aspiration, for example during pregnancy or
fluctuance. Since these arise from the adenexae of hair follicles, simply pursuing an expectant course. When patients are asked to
there is usually an obvious relation or a small punctum although give consent for surgery, it is appropriate to warn about the possi-
this is not inevitable. The usual treatment is surgical excision, bility of cranial nerve deficit. This is predominately to the
which can often be undertaken under local anaesthesia. mandibular division of the facial nerve, especially if the incision is
inadvertently placed too high. In addition, one should warn the
Lipoma patient about the potential for accessory nerve damage since this
Although not a cystic lesion, these can often assume the clinical can occur and can be particularly disabling, leading to destabiliza-
characteristics thereof. They usually move with the skin, but do tion of the ipsilateral shoulder joint with weakness and pain. Divi-
not have a punctum. Since they arise from subcutaneous tissue, sion of the greater auricular nerve is often necessary, particularly
as with the epidermoid cyst, they are not exclusive to the neck. with the larger cysts, and will result in numbness of the ipsilateral
Treatment is usually excision. ear which can be permanent but surprisingly very often recovers.
The accessory nerve, which enters the neck through the internal
Cystic hygroma jugular foramen, can be intimately applied to the posterior aspect
This is a curious swelling usually present at birth, but occasionally of the cyst and so inadvertently divided or traumatized. This is
presents later on. It is thought to result from abnormal fusion of the a particular risk if surgery is undertaken after incision and drainage
lymphoid elements of the neck.2 It usually consists of multiple of an infected branchial cyst when scar tissue can obliterate tissue
grape-like swellings which often interconnect and is obviously planes and make dissection difficult. As a good guide, the surface
cystic on examination. It can affect any part of the neck, but is anatomy of this vulnerable nerve is determined by drawing a line
usually seen laterally. This disorder can be extensive and involve between the junction of the upper third and lower two-thirds of the
other structures such as the mediastinum, and can be associated sternomastoid muscle and the junction of the upper two-thirds and
with other congenital abnormalities. It can progressively increase lower one-third of the anterior border of the trapezius muscle in the
in size, often dramatically so, and can be associated with infection posterior triangle of the neck.
SURGERY 27:12 532 Ó 2009 Published by Elsevier Ltd.
HEAD AND NECK
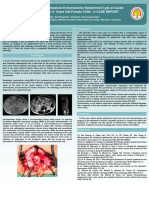
Case study
A 35-year-old male who works as a pie factory operative pre-
sented to the general ENT clinic with a 12-week history of a left-
sided swelling in the neck. On further questioning, there was no
dysphagia, no changes in the voice and there was no significant
past medical history. He was a non-smoker, but drank approxi-
mately 6 units of alcohol per night.
On examination, the internal ENT was normal. External
examination demonstrated a 5 cm swelling just anterior to the
sternomastoid muscle on the left side at the junction of the upper
one-third and lower two-thirds and deep to the subcutaneous
tissues. Periodic aspiration had been performed at the patient’s
request but with recurrence shortly after and was clearly not
a long-term solution. Repeated cytological analysis showed
degenerate keratinocytes and cholesterol crystals. Microbiolog-
ical analysis revealed no detectable infection. An ultrasound scan
showed cystic appearances.
Figure 2 Marking landmarks. The upper line indicates the lower limit of the
The situation was entirely typical for a benign branchial cyst. mandible. The lower line indicates the anterior border of the sternomastoid
The patient was advised to undergo excision to resolve the muscle. The middle line represents the site of the incision, taking care to
problem and obtain precise histology. Informed consent was place it at least two finger-breadths below the mandible to avoid trauma to
obtained and the patient warned pre-operatively about the small the mandibular branch of the facial nerve. Ideally it should be placed in
risks of bleeding, infection, unsightly scarring, recurrence, a natural skin crease but some surgeons prefer an incision running anterior
to and parallel with the upper sternomastoid muscle. The arrow below the
numbness and associated cranial nerve deficit.
lowest line was drawn on whilst the patient was on the ward and indicates
The operation was undertaken and the sequence for excision the side to be operated upon. It forms part of the pre-operative checks
of the cyst are as detailed in Figures 2e6. before the patient leaves for theatre, once again in the anaesthetic room
and then when on the operating table just before commencing excision.
Thyroid cysts
This article is not intended to provide an exhaustive discussion of enlargement or a sinus tract may be present.7 MRI may be useful in
thyroid disorder, which can be obtained elsewhere. Thyroid cysts recurrent disease as it can help to define the residual fistulous tract
can form part of more generalized thyroid disorder, but pre-operatively, thus aiding accurate excision, although in our
a common presentation is of a solitary and unilateral thyroid experience this investigation is usually not necessary.8
enlargement. Fluctuance is not usually demonstrated. The Small cysts can be left alone, but often patients presenting
swelling moves on swallowing, but not on tongue protrusion. with larger lesions request removal. Recurrence is relatively
The patient usually becomes aware of a painless lump and common following simple cyst excision and it is usual practice to
a history of rapid enlargement may indicate haemorrhage or less remove the body of the hyoid bone in continuity (Sistrunk’s
commonly malignancy. It is important to determine the nature of operation).
a lesion in this situation. Thyroid cysts are usually best investi-
gated with an ultrasound scan and aspiration. Benign cytology
and no further recurrence after aspiration requires no further
attention but a recurrent or progressively enlarging lesion usually
requires surgery, for example hemithyroidectomy.
Thyroglossal duct cysts
The thyroglossal cyst provides an example of how an under-
standing of the embryology of this area can aid diagnosis and
management. The thyroid gland arises from the region of the
base of tongue and then descends through the neck taking with it
a thyroglossal tract. This usually disappears, but occasionally can
either persist or an isolated segment can remain and undergo
cystic change. It is usually seen at the level of or below the hyoid
bone and in the midline, but not exclusively so. It is a relatively
easy clinical diagnosis to make and is a favourite for clinical
examinations. Occasionally it can be confused with an anterior
lymph node or rarely a sublingual dermoid.
On ultrasound, if uncomplicated, a thyroglossal cyst may appear Figure 3 Exposure of the branchial cyst. Once the incision has been made
through skin, the subcutaneous tissue, platysma and deep cervical
dark and well circumscribed or pseudosolid if it contains cholesterol
investing fascia needs to be divided. The sternomastoid muscle can be
or keratinocytes. If complicated by infection or haemorrhage, the divided to assist in the delivery of the larger cyst, but this increases the
cyst may show internal echoes of a complex nature and hetero- risk of haemorrhage and is a more major undertaking leading to a longer
genicity. In the surrounding tissues, oedema, reactive lymph node recovery phase. The lesion is then usually easily identified.
SURGERY 27:12 533 Ó 2009 Published by Elsevier Ltd.
HEAD AND NECK
Figure 4 Dissection. Further dissection around the cyst is then undertaken Figure 6 Preparation for pathological analysis. After delivery the lesion is
bearing in mind that on its posterior aspect lies the internal jugular vein, then examined and placed in formalin for histological analysis. If there is
common carotid artery and bifurcation, and the accessory nerve. Dissection a strong suspicion of an infectious cause e.g. tuberculosis, part of the cyst
can be difficult if there has been previous infection and sometimes the can be removed with a scalpel and sent for microbiology. If lymphoma is
internal jugular vein has to be sacrificed if the lesion is strongly adherent. suspected, some laboratories require fresh material for examination and
This produces no adverse functional problem but is not usually necessary. this should be ascertained beforehand. Often the lesion is associated with
a small cluster of lymph nodes which are typically reactive in nature and
Salivary gland cysts can be removed in continuity. A pre-vacuumed neck drain is inserted
Cysts can occur in salivary tissue and those presenting as through a separate stab incision and the wound closed in two layers with
external swelling usually arise from either the parotid or appropriate sutures.
submandibular glands. Occasionally cystic degeneration can
arise in the sublingual area within the mouth, which then surgery is required, firstly to resolve the problem and secondly to
herniates through or around the mylohyoid muscle when it determine the precise histological characteristic because cystic
becomes known as a ‘plunging’ ranula. This latter swelling is change can be an accompaniment of salivary gland neoplasia.
always accompanied by a swelling in the floor of mouth. Salivary gland surgery often involves meticulous localization and
Diagnosis is usually obtained on the clinical characteristics preservation of various cranial nerves, for example the facial in
and on the anatomical location. A true cyst of the parotid gland relation to the parotid and can be complex and time consuming.
usually occurs in the region overlying the angle of the mandible Salivary gland outlet obstruction can be seen as a result of
and may in fact represent a branchial arch abnormality. As with stone formation or inflammation and this most often affects the
other lesions, aspiration and cytology can be undertaken. Often submandibular gland although this is not necessarily a true cyst.
Removal of the gland is indicated if the obstructive element
cannot be resolved. A
REFERENCES
1 El-Silimy O, Corney C. The value of sonography in the management of
cystic neck lesions. J Laryngol Otol 1993; 107: 245e51.
2 Bull PD. Lymphangioma. In: Scott Brown’s otorhinolaryngology, head
and neck surgery. 7th edn. Hodder Arnold, 2008.
3 Giguere CM, Bauman NM, Sato Y, et al. Treatment of lymphangiomas
with OK-432 (Picibanil) sclerotherapy. Arch Otolaryngol Head Neck
Surg 2002; 128: 1137e44.
4 Mathur NN, Rana I, Bothra R, Dhawan R, Geeta K, Pradhan T. Bleomycin
sclerotherapy in congential lymphatic and vascular malformations of
head and neck. Int J Pediatr Otorhinolaryngol 2005; 69: 75e80.
5 Golledge J, Ellis H. The aetiology of lateral cervical (branchial) cysts:
past and present theories. J Laryngol Otol 1994; 108: 653e9.
6 Flanagan PM, Roland NJ, Jones AS. Cervical node metastases presenting
Figure 5 Delivering the specimen. Atraumatic tissue-holding forceps, such with features of branchial cysts. J Laryngol Otol 1994; 108: 1068e71.
as those of the Babcock or Allis design, are useful during this phase of the
7 Ahuja AT, Wong KT, King AD, Yuen EHY. Imaging for thyroglossal duct
procedure. As dissection proceeds, often the lesion seems to originate
from a pedicle arising superiorly and this can be ligated and divided. In cyst: the bare essentials. Clin Radiol 2005; 60: 141e8.
some instances a branchial fistula can continue up to the tonsil region 8 Patel NN, Hartley BE, Howard DJ. Management of thyroglossal tract disease
and represents a true first arch abnormality. after failed Sistrunk’s procedure. J Laryngol Otol 2003; 117: 710e2.
SURGERY 27:12 534 Ó 2009 Published by Elsevier Ltd.
Potrebbero piacerti anche
- Kimura Disease, Pott'S Puffy - XXXXXDocumento28 pagineKimura Disease, Pott'S Puffy - XXXXXHossam ThabetNessuna valutazione finora
- Neck Mass ProtocolDocumento8 pagineNeck Mass ProtocolCharlene FernándezNessuna valutazione finora
- Congenital CholesteatomaDocumento3 pagineCongenital CholesteatomazainabNessuna valutazione finora
- Journal Benjolan Di LeherDocumento9 pagineJournal Benjolan Di LeherStase IPD SoedarsoNessuna valutazione finora
- Scott-Brown's Vol 2 Benign Neck Disease - Infections & SwellingDocumento12 pagineScott-Brown's Vol 2 Benign Neck Disease - Infections & SwellingjessNessuna valutazione finora
- Neck LumpDocumento18 pagineNeck LumpJosh BurkeNessuna valutazione finora
- Abd1806-4841 20153078Documento4 pagineAbd1806-4841 20153078Cricelle Rose CobreNessuna valutazione finora
- An Approach To The Neck Masses: BY: Hardi H. QaderDocumento49 pagineAn Approach To The Neck Masses: BY: Hardi H. QaderEmad AlryashiNessuna valutazione finora
- Cervical AuricleDocumento2 pagineCervical AuricleTahir S.MNessuna valutazione finora
- Neck Masses and Lesions in PediatricsDocumento63 pagineNeck Masses and Lesions in PediatricsRanj B. AshrafNessuna valutazione finora
- Homoeopathic Treatment of Complicated Sebaceous Cyst - A Case StudyDocumento5 pagineHomoeopathic Treatment of Complicated Sebaceous Cyst - A Case StudyDr deepakNessuna valutazione finora
- Pyomyositis-Bagra 1Documento11 paginePyomyositis-Bagra 1Monkz Gila-eteNessuna valutazione finora
- Otorhinolaryngology: Fibromatosis Colli or Pseudotumour of Sternocleidomastoid Muscle, A Rare Infantile Neck SwellingDocumento3 pagineOtorhinolaryngology: Fibromatosis Colli or Pseudotumour of Sternocleidomastoid Muscle, A Rare Infantile Neck SwellingMohammedNessuna valutazione finora
- Art 3Documento4 pagineArt 3miguelNessuna valutazione finora
- Case Bezold AbscessDocumento3 pagineCase Bezold AbscessCarimaGhalieNessuna valutazione finora
- Case Reports About An Overlooked Cause of Neck Pain: Calcific Tendinitis of The Longus Colli Case Reports.9Documento5 pagineCase Reports About An Overlooked Cause of Neck Pain: Calcific Tendinitis of The Longus Colli Case Reports.9mikeb92556Nessuna valutazione finora
- PosterDocumento1 paginaPosterRaif RizqullahNessuna valutazione finora
- L R: E C D: Iteratur Eading AR Anal IseaseDocumento19 pagineL R: E C D: Iteratur Eading AR Anal IseaseTitaPuspitasariNessuna valutazione finora
- The Neck - Oral and Maxillofacial Surgery Clinics of North America PDFDocumento224 pagineThe Neck - Oral and Maxillofacial Surgery Clinics of North America PDFDr SS ki VinesNessuna valutazione finora
- Fox 2014Documento3 pagineFox 2014Bookaholic 11Nessuna valutazione finora
- Papillary Thyroid Ca: Group. 1 B Grand CaseDocumento16 paginePapillary Thyroid Ca: Group. 1 B Grand CaseAdora Dela CruzNessuna valutazione finora
- Papillary Thyroid Ca: Group. 1 B Grand CaseDocumento16 paginePapillary Thyroid Ca: Group. 1 B Grand CaseAdora Dela CruzNessuna valutazione finora
- Absesparafaring4 PDFDocumento3 pagineAbsesparafaring4 PDFnataliayobeantoNessuna valutazione finora
- Duplication of The External Auditory Canal Two CasDocumento5 pagineDuplication of The External Auditory Canal Two CasIvana SupitNessuna valutazione finora
- Steatocystoma Multiplex A Case Report of A Rare Disease Diagnosed in A Trauma PatientDocumento5 pagineSteatocystoma Multiplex A Case Report of A Rare Disease Diagnosed in A Trauma Patientma hNessuna valutazione finora
- D.D of Mid-Line Neck SwellingsDocumento21 pagineD.D of Mid-Line Neck Swellingsmhmdalbdyny764Nessuna valutazione finora
- Eagle's Syndrome in An 11-Year-Old PatientDocumento4 pagineEagle's Syndrome in An 11-Year-Old Patientleeperlhan2000Nessuna valutazione finora
- The Treatment of Neck and Upper Back Pain With AcuDocumento6 pagineThe Treatment of Neck and Upper Back Pain With AcuMohmmad Hossein NazariNessuna valutazione finora
- Case Report: A Case of Conservatively Managed Invasive Ceruminoma and A Review of The LiteratureDocumento4 pagineCase Report: A Case of Conservatively Managed Invasive Ceruminoma and A Review of The Literaturesaffrin syedNessuna valutazione finora
- Checklist HEAD and NECKDocumento8 pagineChecklist HEAD and NECKAezyreal Anne MirallesNessuna valutazione finora
- Spiegel 2004Documento5 pagineSpiegel 2004manuel abantoNessuna valutazione finora
- Incidental Reportzaharopoulos2000Documento4 pagineIncidental Reportzaharopoulos2000maglangitmarvincNessuna valutazione finora
- Dr. Erjan Fikri, M. Ked. SPB, Spba (K)Documento60 pagineDr. Erjan Fikri, M. Ked. SPB, Spba (K)ramadhan syah putraNessuna valutazione finora
- Chapter 23the Multiply & Severely Injured PatientDocumento19 pagineChapter 23the Multiply & Severely Injured PatientWahyuNessuna valutazione finora
- Bilateral Sternocleidomastoid Tumor of IDocumento3 pagineBilateral Sternocleidomastoid Tumor of ISuparna Roy VarunNessuna valutazione finora
- An 2014Documento4 pagineAn 2014Jing XueNessuna valutazione finora
- Dic Ing Varios en-USDocumento29 pagineDic Ing Varios en-USSindy Melissa Melendez OrtizNessuna valutazione finora
- Thyroglossal CystsDocumento4 pagineThyroglossal CystsCondurache Ilie-AndreiNessuna valutazione finora
- Ghan em 2005Documento5 pagineGhan em 2005asfwegereNessuna valutazione finora
- DOI: 10.1515/jbcr-2015-0170: Case ReportDocumento4 pagineDOI: 10.1515/jbcr-2015-0170: Case ReporttaufikolingNessuna valutazione finora
- Surgery 1.02 Head and Neck - Dr. BartolomeDocumento11 pagineSurgery 1.02 Head and Neck - Dr. BartolomeJoel SaluNessuna valutazione finora
- Branchial Cleft Cyst: A Case Report and Review of LiteratureDocumento3 pagineBranchial Cleft Cyst: A Case Report and Review of LiteratureValonia IreneNessuna valutazione finora
- Cervical GiaDocumento14 pagineCervical GiaSyamsuryadi AdheNessuna valutazione finora
- 05Documento2 pagine05Ahsan JamilNessuna valutazione finora
- 2013 9 1 045 ChuangDocumento8 pagine2013 9 1 045 ChuangRamaMahardikaNessuna valutazione finora
- SMF Orthopaedi Dan Traumatologi RSU DR Saiful Anwar Malang: Thomas Erwin C J HuwaeDocumento58 pagineSMF Orthopaedi Dan Traumatologi RSU DR Saiful Anwar Malang: Thomas Erwin C J Huwaeyulia manaweanNessuna valutazione finora
- CE (Ra1) F (GH) PF1 (ANAK) PFA (AK) PF2 (PAG)Documento2 pagineCE (Ra1) F (GH) PF1 (ANAK) PFA (AK) PF2 (PAG)Diana CantúNessuna valutazione finora
- An Unusual Cause of Stridor: Retropharyngeal Cold Abscess: Pediatric Surgery International April 2002Documento4 pagineAn Unusual Cause of Stridor: Retropharyngeal Cold Abscess: Pediatric Surgery International April 2002akshayajainaNessuna valutazione finora
- The Management of Intracranial AbscessesDocumento3 pagineThe Management of Intracranial AbscessesDio AlexanderNessuna valutazione finora
- Compilation Spinal SsmsDocumento35 pagineCompilation Spinal SsmsPiaRomildaTagaoCayetano100% (1)
- Thanatophoric Dysplasia: A Rare Entity: Oman Medical Journal May 2011Documento3 pagineThanatophoric Dysplasia: A Rare Entity: Oman Medical Journal May 2011Atria DewiNessuna valutazione finora
- CephalhematomaDocumento3 pagineCephalhematomaNazhar FarhanNessuna valutazione finora
- Inguinal Hernia and Hydrocele: Congenital Hydrocele Presents As A Mass in The Scrotum ShortlyDocumento3 pagineInguinal Hernia and Hydrocele: Congenital Hydrocele Presents As A Mass in The Scrotum ShortlyBetão AviãoNessuna valutazione finora
- Liu 2016Documento2 pagineLiu 2016Anonymous l3X3jf0NPNessuna valutazione finora
- Superior Laryngeal Nerve Neuralgia: Case Series and Review of Anterior Neck Pain SyndromesDocumento4 pagineSuperior Laryngeal Nerve Neuralgia: Case Series and Review of Anterior Neck Pain SyndromesjtbattaNessuna valutazione finora
- Abstract: Kimura Disease Is A Rare Form of Chronic Inflammatory Disorder InvolvingDocumento4 pagineAbstract: Kimura Disease Is A Rare Form of Chronic Inflammatory Disorder InvolvingpriyokNessuna valutazione finora
- American Journal of Emergency Medicine: Case ReportDocumento2 pagineAmerican Journal of Emergency Medicine: Case ReportqalbiNessuna valutazione finora
- 10 1002@hed 20358Documento5 pagine10 1002@hed 20358Antania IsyatiraNessuna valutazione finora
- Diagnosis and Treatment of Neurogenic Oropharyngeal DysphagiaDa EverandDiagnosis and Treatment of Neurogenic Oropharyngeal DysphagiaNessuna valutazione finora
- National Ambient Air Quality Standards (Naaqs)Documento2 pagineNational Ambient Air Quality Standards (Naaqs)Muhammad AdilNessuna valutazione finora
- MicrophtalmiaDocumento5 pagineMicrophtalmiaMuhammad AdilNessuna valutazione finora
- BLOK 12 - IT 2 - Farmakogenetik 1 - MISDocumento38 pagineBLOK 12 - IT 2 - Farmakogenetik 1 - MISMuhammad AdilNessuna valutazione finora
- The Following Short Quiz Consists of 4 Questions. This Will Test Your IQ and Tells Whether You Are Qualified To Be A "Professional"Documento13 pagineThe Following Short Quiz Consists of 4 Questions. This Will Test Your IQ and Tells Whether You Are Qualified To Be A "Professional"Muhammad AdilNessuna valutazione finora
- Prehistoric Period: Melaka SultanateDocumento22 paginePrehistoric Period: Melaka SultanateMuhammad AdilNessuna valutazione finora
- Detalyadong Banghay Arralin Sa Filipino 6 May 2, 2023 I. LayuninDocumento4 pagineDetalyadong Banghay Arralin Sa Filipino 6 May 2, 2023 I. LayuninamygailNessuna valutazione finora
- DRUG-STUDY - CelecoxibDocumento3 pagineDRUG-STUDY - Celecoxibamal abdulrahmanNessuna valutazione finora
- Dissertation - CD 2Documento112 pagineDissertation - CD 2pavlov2Nessuna valutazione finora
- Obgyn: History Taking and Examination DR Musa Marena ObgynDocumento94 pagineObgyn: History Taking and Examination DR Musa Marena ObgynnidoNessuna valutazione finora
- 3 - Alterations in Fluid & Electrolyte BalanceDocumento62 pagine3 - Alterations in Fluid & Electrolyte Balancegeng gengNessuna valutazione finora
- Diabetesand Ramadan Update New Guidelines 2023Documento4 pagineDiabetesand Ramadan Update New Guidelines 2023Taufiqurrokhman RofiiNessuna valutazione finora
- Diagnosis and Treatment of Clostridioides (Clostridium) Difficile Infection in Adults in 2020Documento2 pagineDiagnosis and Treatment of Clostridioides (Clostridium) Difficile Infection in Adults in 2020Alem OrihuelaNessuna valutazione finora
- Spondylosis Information LeafletDocumento3 pagineSpondylosis Information LeafletAnis Azizah MogilNessuna valutazione finora
- Rongga Mulut, Kelenjar Saliva Dan Rahang: No Istilah Terminologi Medis Istilah Arti Sumber ReferensiDocumento30 pagineRongga Mulut, Kelenjar Saliva Dan Rahang: No Istilah Terminologi Medis Istilah Arti Sumber ReferensiAlfi Melinda FNessuna valutazione finora
- Anaphylaxis Guidelines PosterDocumento1 paginaAnaphylaxis Guidelines PosterBabo SanNessuna valutazione finora
- Felocell Felv Helps Prevent Disease Cause by Feline Leukemia Virus (Felv)Documento1 paginaFelocell Felv Helps Prevent Disease Cause by Feline Leukemia Virus (Felv)Reginaldo ParcianelloNessuna valutazione finora
- Achalasia: History & ExamDocumento28 pagineAchalasia: History & ExamMicija CucuNessuna valutazione finora
- Letter To The Editor: DisordersDocumento2 pagineLetter To The Editor: DisordersJoNessuna valutazione finora
- Physio After SurgeryDocumento2 paginePhysio After SurgeryGursangeet KaurNessuna valutazione finora
- The Impact of Increasingly Harmful Obesity Levels inDocumento10 pagineThe Impact of Increasingly Harmful Obesity Levels inEkwebelem GeorgeNessuna valutazione finora
- Tumours of Nasopharynx DhingraDocumento8 pagineTumours of Nasopharynx DhingraIkmal ShahromNessuna valutazione finora
- Copd - NCPDocumento6 pagineCopd - NCPMonique Sacherow BacherNessuna valutazione finora
- Arab Board Exam 2008Documento7 pagineArab Board Exam 2008alaaNessuna valutazione finora
- What Are The Side Effects of StatinsDocumento2 pagineWhat Are The Side Effects of StatinsJeff TeeNessuna valutazione finora
- Module 10Documento5 pagineModule 10Yuki Xairah TunayNessuna valutazione finora
- Rsik of ICH in Anticoagulation Primary Brain Tumor PatientDocumento7 pagineRsik of ICH in Anticoagulation Primary Brain Tumor PatientFithry RahmaNessuna valutazione finora
- Distant Metastases of Nasopharyngeal Carcinoma: Literature ReadingDocumento33 pagineDistant Metastases of Nasopharyngeal Carcinoma: Literature ReadingTeuku Muhammad Rizqi FadhlillahNessuna valutazione finora
- Dermatology - PedsDocumento16 pagineDermatology - PedsbencleeseNessuna valutazione finora
- Prado, Catherine BSN IIB (Activity 1 Case Scenario)Documento52 paginePrado, Catherine BSN IIB (Activity 1 Case Scenario)Catherine PradoNessuna valutazione finora
- Cefixime OS DS PIfinalDocumento10 pagineCefixime OS DS PIfinalfiqrifahruroziaNessuna valutazione finora
- Fast Chicken Pox Cure PDF-eBook, Stefan HallDocumento46 pagineFast Chicken Pox Cure PDF-eBook, Stefan HallCyrusNessuna valutazione finora
- Absent End-Diastolic Velocity in The Umbilical Artery and Its Clinical SignificanceDocumento12 pagineAbsent End-Diastolic Velocity in The Umbilical Artery and Its Clinical Significancejakob_saleanNessuna valutazione finora
- Examination of A Male For Determination of PotencyDocumento4 pagineExamination of A Male For Determination of PotencyHarish AgarwalNessuna valutazione finora
- Definition:: Pleural EffusionDocumento4 pagineDefinition:: Pleural EffusionGetom NgukirNessuna valutazione finora
- The Diagnosis of Organic Brain Syndrome: TfcqtureDocumento4 pagineThe Diagnosis of Organic Brain Syndrome: TfcqtureWonderCatNessuna valutazione finora