Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Comparison of The Acute and Long-Term Effects of Exercise On Glucose Control in Type 1 Diabetes CONTINUA A SALVAR NO DRIVE PDF
Caricato da
Elaine CspTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Comparison of The Acute and Long-Term Effects of Exercise On Glucose Control in Type 1 Diabetes CONTINUA A SALVAR NO DRIVE PDF
Caricato da
Elaine CspCopyright:
Formati disponibili
Original Articles
c omparison of the Acute and Long'Term
Effects of Exercise on Glucose Control
in Type I Diabetes
B. ZINMAN, M.D., S. ZUNIGA-GUAJARDO, M.D., AND D. KELLY, M.D.
To determine the long-term effect of exercise training on glucose control, 13 subjects with type I
diabetes and 7 control subjects performed 45 min of cycle exercise three times per wk for 12 wk. The
acute blood glucose response, the long-term effect on glucose control (glycosylated hemoglobin and
fasting plasma glucose), and changes in nutrient intake were assessed. Fitness as measured by VO2 MAX
increased in both control (33.8 ± 1.7 to 43.2 ± 3.5 ml/min/kg) and diabetic (38.7 ± 3.3 to 46.5 ± 3.6
ml/min/kg) (P < 0.05) subjects although body weight remained unchanged. In the diabetic subjects,
an acute glucose-lowering effect occurred with each exercise session throughout the 12-wk training
period (225.8 ± 16.1 to 148.5 ± 16.8 mg/dl, P < 0.001). However, fasting plasma glucose and gly-
cosylated hemoglobin remained essentially unchanged (pretraining, 193.7 ± 27.5 mg/dl and 10.7 ±
0.3%; 6-wk training, 192.5 ± 27.1 mg/dl and 10.7 ± 0.03%; 12-wk training, 202 ± 30.1 mg/dl and
10.3 ± 0.8%). Total caloric intake as assessed by diet history increased significantly on exercising days
(2569-2849 kcal, P < 0.05). Although plasma glucose decreases acutely with exercise, increased caloric
intake on exercising days obviates a long-term effect of training on glucose control. More precise
guidelines and recommendations as to exercise timing and nutrient intake, likely based on self-moni-
toring of blood glucose, are required to achieve a beneficial effect of exercise training on metabolic
control in type I diabetes, DIABETES CARE 1984; 7:515-19.
S
ince the early demonstration of its acute glucose- of the therapeutic benefits of exercise on glucoregulation in
lowering effect,1 exercise has been considered an diabetes. Limited investigations in this regard have shown
important component of the management of dia- that physical training increases insulin sensitivity in obese
betes.2 With the increased interest in fitness and subjects and patients with type II diabetes, although a long-
exercise in general, the role of exercise in the treatment of term effect on improving glucose tolerance was not consis-
diabetes has recently been re-emphasized. However, docu- tently evident. 10~13 A recent study examining the response to
mentation of a beneficial long-term effect on glucose control training of patients with type I diabetes snowed increased
in type I diabetes has been lacking. peripheral insulin sensitivity but unchanged blood glucose
Most recent studies have focused on defining the metabolic control.14 This later study appears to be inconsistent with
responses to acute exercise in type I diabetes as compared the well-documented hypoglycemic effects of acute exercise
with normal controls. 3~7 The effects of insulin deficiency and and the observation that postprandial exercise significantly
insulin excess on glucoregulation and the mobilization of improves meal-related glucose excursions.15 One would ex-
energy stores for exercising muscle have been well defined. pect these acute responses to have a summation effect on
As a result of these studies, specific guidelines on the avoid- overall glucose control in the training patient.
ance of exercise-induced hypoglycemia have been suggested. To date, few studies have examined both the acute and
In addition, it has been shown that with intravenous insulin long-term effects of exercise in the same population. The
infusion pumps specific insulin infusion waveforms (algo- present study was thus undertaken to document both the
rithms) for exercise both in the fasted and postprandial states acute and long-term effects of 45 min of exercise performed
could be developed, which normalize the metabolic responses three times per wk in type I diabetic individuals as compared
to exercise.8'9 However, these studies do not address the issue with normal controls. Measurements of blood glucose were
DIABETES CARE, VOL. 7 NO. 6, NOVEMBER-DECEMBER 1984 515
EFFECTS OF EXERCISE ON GLUCOSE CONTROL IN TYPE 1 DIABETES/B. ZINMAN AND ASSOCIATES
mg/dl Exercise training program. Maximal oxygen uptake (VO 2
250 MAX) was estimated during steady-state exercise on a bicycle
• Bete>re exercise * p <0.01
O AMe r exercise ** p < 0.05 ergometer (Siemens-Elema Model 380, Stockholm, Sweden)
200 -
I T I at two different workloads measuring oxygen uptake and heart
rate.1617 Respiratory gas concentrations were measured with
*
ill * rapid response CO2 (LB/2) andO 2 (OM/11) analyzers (Beck-
150 -
I I PI
I man Instruments Inc., Palo Alto, California). Once VO2
MAX was assessed and baseline metabolic measurements per-
formed, physical training was initiated 3 times per wk for 12
mm wk under the supervision of a qualified exercise therapist.
100
week 0 to 6
S§j
week 6 to 12
mm
week 0 to 12
Training consisted of 45 min of exercise on a stationary cycle
ergometer with a workload of sufficient intensity to stimulate
an increase in endurance fitness.l8 Heart rate response achieved
during each exercise session was 60-85% of predicted max-
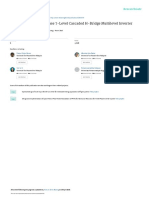
FIG. I. Blood glucose concentrations before {hatched bars) and after
imum. The actual work intensity was individually determined
(open bars) each exercise session during the first 6 wk of training, second
6 wk of training, and over the entire training period. Mean ± SEM are
and adjusted by the results obtained from the fitness assess-
shown for 13 subjects with type I diabetes. ment. Training workloads were reassessed every 2 wk and
appropriate changes made to result in continued stimulation
and cardiorespiratory adaptation. Before and after each ex-
made before and after each exercise session while fitness, ercise session, fingerprick blood samples were taken for glu-
glycosylated hemoglobin, and fasting plasma glucose were cose measurement using glucose-oxidase reagent strips and a
assessed before and after 6 and 12 wk of exercise training. glucometer (Ames, Miles Laboratories, Elkhart, Indiana).
Blood samples were taken before training, at 6 and 12 wk of
training, and in the posttraining period for determination of
MATERIALS AND METHODS glycosylated hemoglobin and fasting plasma glucose. Ten of
Subjects. Thirteen type I diabetic subjects and seven normal the 13 diabetic patients were interviewed by a qualified die-
controls were studied. All were nonobese. The six female titian after the training period in order to assess caloric intake
and seven male diabetic subjects were 30.0 ± 1.8 yr of age, on exercising and nonexercising days by diet history. Diet
97.5% of ideal body weight, with a duration of diabetes of histories were hand-calculated from reference guides (Nu-
14.3 ± 3.2 yr and an average daily insulin dose of 37.6 ± 3.2 trient Values of Some Common Foods, Health and Welfare
U. Eleven of the diabetic subjects were taking a combination Canada, 1979, and the National Heart, Lung and Blood
of intermediate-acting insulin (NPH or lente) and regular Institute Nutrition Coding Centre Food Table Intake,
(crystalline zinc) insulin, and two were being treated with 1977). 19~21 In two patients, caloric intake was assessed from
intermediate-acting insulin alone. Ten of the diabetic sub- 5-day food records.
jects were receiving one insulin injection daily while two Subjects were asked to continue with their daily routines
were on two injections and one was on three injections. The and usual diets. They were instructed to record all hypo-
control group consisted of five women and two men with a glycemic episodes and any adjustments in insulin dosage.
mean age of 30.7 ± 2.9 yr. They were 101 ± 5% of ideal They were asked to compensate for exercise as they were
body weight and had no family history of diabetes mellitus, usually instructed to by their physician.
nor were they taking any medication. None of the diabetic All subjects administered their insulin 15-30 min before
patients had clinical evidence of diabetic microvascular or breakfast. Five subjects performed the exercise training 30
macrovascular complications, although two were receiving min after breakfast (0800-0830 h), four subjects exercised
thyroid replacement for primary hypothyroidism. All subjects 90-120 min after breakfast (0930-1000 h), and four subjects
had a normal exercise electrocardiogram and informed con- exercised 30 min after lunch (1230-1300 h). There was no
sent was obtained in compliance with the Human Subjects difference in the observed response in relationship to the
Review Committee of the University of Toronto. time of exercise.
TABLE 1
Effect of exercise training on maximal oxygen uptake (V0 2 MAX) (ml/min/kg)
Training
Pretraining Posttraining
(Owk) 6 wk 12 wk (18 wk)
Control subjects 33.8 ± 1.7 40.0 ± 1.8* 43.2 ±3.5* 40.0 ± 4.0
Diabetic subjects 38.7 ± 3.3 44.6 ± 3.0' 46.5 ±3.6' 43.1 ± 3.3*
'P < 0.05 as compared with pretraining.
516 DIABETES CARE, VOL. 7 NO. 6, NOVEMBER-DECEMBER 1984
EFFECTS OF EXERCISE ON GLUCOSE CONTROL IN TYPE I DIABETES/B. ZINMAN AND ASSOCIATES
TABLE 2
Effect of exercise training on weight (kg)
Training
Pretraining Posttraining
(0 wk) 6 wk 12 wk (18 wk)
Control subjects 65.7 ± 5.2 65.4 ± 5.1 65.1 ± 5. 2 64.9 ± 5.1
Diabetic subjects 64.2 ± 1.1 64.3 ± 1.1 64.2 ± 1. 1 64.5 ± 1.1
Analytic methods. All venous blood samples were obtained values. Body weight was similar in both control and diabetic
in the postabsorptive state after a 10-h fast. Plasma glucose subjects at the start of training and no significant changes
was determined using a glucose analyzer (Beckman Instru- were seen in either group (Table 2).
ments, Inc.) and glycosylated hemoglobin concentrations To determine the effect of exercise on overall glucose con-
(hemoglobin Al) were determined by the microcolumn tech- trol, fasting plasma glucose and hemoglobin Al measure-
nique with preincubation of samples to remove the reversible ments were performed before, during, and after training (Ta-
glycosylated fractions. To compare differences within groups, ble 3). The diabetic subjects had elevated fasting plasma
Student's paired t-test was used, and for differences between glucose (193.7 mg/dl) and hemoglobin Al (10.7%) (P <
groups Student's unpaired t-test was employed. All data are 0.005) as compared with control subjects before training and
given as the mean ± SEM in the tables and figures. neither changed significantly with training. Other clinical
measures of diabetes control were also recorded before and
RESULTS after training. Total insulin dose was unchanged at 37.6 ± 3.2
U before and 40.0 ± 3.1 U after training, and the occurrence
Acute response to exercise. The heart rate response during the of hypoglycemic reactions was similar.
last 10 min of each training session was similar for both The effect of exercise on nutrient intake as assessed by
control and diabetic subjects (156.7 ± 1.9 beats/min and diet history is shown in Table 4. Total caloric intake in-
160 ± 3.2 beats/min). Figure 1 shows the acute blood glu- creased significantly on exercising days and this was primarily
cose response to each exercise session during the first 6 wk in the form of carbohydrate and protein. Two subjects kept
of training (first pair of bars), the second 6 wk of exercise 5-day food records that showed a similar increase in ingested
training (middle bars), and over the entire training period calories on exercising days (520 and 828 kcal, respectively).
(third pair of bars). A significant fall in glycemia occurred
with each exercise session and this acute decrease was similar
DISCUSSION
and persisted throughout the entire exercise training period.
A
Effects of exercise training. Maximal oxygen uptake (VO2 lthough exercise is thought to be useful in the
MAX) is shown in Table 1. VO2 MAX increased 28% and treatment of diabetes, there is little evidence to
20% in the control and diabetic groups, respectively, at 12 support a beneficial effect of exercise training in
wk of training. When reassessed at 18 wk, VO2 MAX de- type I diabetes. Indeed, a recent Scandinavian
creased in both groups. However, a significant difference study14 failed to demonstrate a significant change in glycos-
persisted in the diabetic subjects as compared with pretraining ylated hemoglobin in 9 type I diabetic subjects undergoing
TABLE 3
Effect of exercise training on fasting plasma glucose and glycosylated hemoglobin
Training
Pretraining Posttraining
(Owk) 6 wk 12 wk (18 wk)
Fasting plasma glucose,
mg/dl (mmol/L)
Control subjects 87.4 ± 3.6 87.2 ± 6.3 84.6 ± 2.7 81.0 ± 2.5
(4.8 ± 0.2) (4.8 ± 0.4) (4.7 ± 0.2) (4.5 ±0.1)
Diabetic subjects 193.7 ± 27.7* 192.5 ± 27.1* 202 ± 30. T 189.8 ± 29.5*
(10.8 ± 1.5) (10.7 ± 1.5) (11.2 ± 1.7) (10.5 ± 1.6)
Hemoglobin Al (%)t
Control subjects 7.7 ± 0 . 5 7.5 ± 0.4 7.4 ± 0.2 7.0 ± 0.1
Diabetic subjects 10.7 ± 0.3* 10.7 ± 0.3* 10.3 ± 0.8' 10.6 ± 0.3*
'P < 0.005 as compared with control subjects.
tNormal, 6.5-8.5%.
DIABETES CARE, VOL. 7 NO. 6, NOVEMBER-DECEMBER 1984 517
EFFECTS OF EXERCISE ON GLUCOSE CONTROL IN TYPE I DIABETES/B. Z1NMAN AND ASSOCIATES
TABLE 4 of caloric intake to match increased caloric expenditure with
Effect of exercise on nutrient intake the maintenance of body weight has been previously docu-
mented experimentally in rodents.22 Although changes in
Nonexercising day Exercising day
body composition were not precisely assessed in our study,
Total calories (kcal) 2569 ± 273 2849 ± 330' triceps skinfold thickness did not change with training (con-
Carbohydrate (g) 265 ± 30 309 ± 38* trol subjects: 14.3 ± 2.0 versus 14.0 ± 2.3 mm; diabetic
Protein (g) 115 ± 11 125 ± 15* subjects: 15.3 ± 2.3 versus 14-2 ± 2.3 mm, before and after
Fat (g) 115 ± 15 121 ± 17 training, respectively).
In summary, a significant increase in fitness as assessed by
'P < 0.05 as compared with nonexercising day. VO2 MAX can be achieved with 12 wk of exercise training
on a cycle ergometer in type I diabetes. Although plasma
glucose decreased acutely with each exercise session, a long-
16 wk of exercise training despite an increase in peripheral term effect on overall glucose control could not be demon-
insulin sensitivity. However, the patients studied tended to strated. Increased caloric intake primarily as carbohydrate on
be physically fit before training (3.24 ± 0.16 L/min or 42 exercising days likely accounts for the above observations.
ml/min/kg), and only an 8% increase in VO2 MAX was achieved Although exercise training per se does not have a significant
with training. effect on overall glucose control, diabetic patients should be
The failure to demonstrate a beneficial effect of exercise encouraged and have the freedom to exercise for the same
on long-term glucose control appears to be inconsistent with general reasons (primarily cardiovascular and psychological)
the well-known acute hypoglycemic effect of exercise1"7 and that it is recommended for the population at large.23"27 To
the observation that exercise can improve postprandial glu- demonstrate a beneficial metabolic effect of exercise training
cose excursion.15 The present study was undertaken to ex- on diabetes control, more precise guidelines and recommen-
amine the variables that might explain this apparent con- dations as to exercise timing and nutrient intake based on
tradiction. Thus, the acute glucose responses to exercise, the self-monitoring of blood glucose data may be required.
effect of exercise on nutrient intake, and the long-term re-
sponses to exercise training were studied in 13 type I diabetic
ACKNOWLEDGMENTS: We are indebted to Patricia A. McClean
subjects.
and other members of the respiratory research laboratory for
As shown in Table I, a significant increase in fitness as technical support; to Kathy Camelon and Ann Murphy for
measured by VO2 MAX was achieved in both control (33.8 ± the dietary evaluation; to the Tri-Hospital Diabetes Educa-
1.7 to 43.2 ± 3.5 ml/min/kg) and diabetic (38.7 ± 3.3 to tion Centre for administrative support; and to Mae Abucay
46.5 ± 3.6 ml/min/kg) subjects with 12 wk of exercise train- for excellent secretarial assistance in preparation of the man-
ing on a cycle ergometer. The acute glucose-lowering effect uscript.
of exercise was present with each exercise session and the These studies were supported by a grant from the Canadian
magnitude of this effect extended over the entire training Diabetes Association and the Banting and Best Diabetes
period (Figure 1). Since exercise was performed at least 3
Centre.
times per wk, one would expect that the repeated acute
decreases in blood glucose with exercise would be reflected
in a long-term decrease in glycosylated hemoglobin. How- This paper was presented in part in abstract form at the Ca-
ever, this was not the case, and hemoglobin Al remained nadian Society for Clinical Investigation Meeting in September
constant throughout. Since the variable of nutrient intake 1983 (Clin. Invest. Med. 1983; 6:69).
From the Division of Endocrinology and Metabolism, Toronto
clearly plays an important role in overall diabetes control,
General Hospital, Department of Medicine, University of To-
diet histories were obtained by a qualified dietitian to assess ronto, Toronto, Ontario, Canada.
caloric intake on exercising and nonexercising days. As Address reprint requests to Dr. B. Zinman, Toronto General
shown in Table 4, a significant increase in caloric intake Hospital, 101 College Street, Toronto, Ontario M5G 1L7, Can-
was evident during exercising days. A similar increase was ada.
seen in two patients who kept 5-day food records. These
findings are consistent with the common clinical practice of REFERENCES
1
avoiding exercise-induced hypoglycemia by ingesting supple- Lawrence, R. D.: The effect of exercise on insulin action in
mental calories. However, without specific guidelines that diabetes. Br. Med. J. 1926; 1:648-52.
2
could be developed from self-monitoring of blood glucose, Marble, A., and Smith, R. M.: Exercise in diabetes mellitus.
overtreatment commonly occurs. In addition, several pa- Arch. Intern. Med. 1936; 58:577-88.
3
tients clearly indicated that during exercise days they could Vranic, M., and Berger, M.: Exercise in diabetes mellitus. Di-
abetes 1979; 28:147-67.
"liberalize" their diet and considered this one of the advan- 4
Felig, P., and Wahren, J.: Fuel homeostasis in exercise. N. Engl.
tages of regular exercise. The failure to demonstrate a sig- J. Med. 1975; 293:1978-84.
nificant difference in body weight with training is also con- 5
Zinman, B., Vranic, M., Albisser, A. M., and Marliss, E. B.:
sistent with the observations of increased food consumption The role of insulin in metabolic response to exercise in diabetic
on exercising days. Interestingly, this apparent self-regulation man. In Proceedings of the KROC Conference on Exercise and
518 DIABETES CARE, VOL. 7 NO. 6, NOVEMBER-DECEMBER 1984
EFFECTS OF EXERCISE ON GLUCOSE CONTROL IN TYPE I DIABETES/B. ZINMAN AND ASSOCIATES
Diabetes. Vranic, M., Wahren, J., and Horvath, S., Eds. Diabetes effect of postprandial exercise on meal-related glucose intolerance
1979; 28 (Suppl. 1):76-81. in insulin-dependent diabetic individuals. Diabetes Care 1982; 5:364-
6
Zinman, B., Murray, F. T., Vranic, M., Albisser, A. M., and 69.
16
Marliss, E. B.: Glucoregulation during moderate exercise in insulin Exercise Testing and Training of Apparently Healthy Individ-
treated diabetes. J. Clin. Endocrinol. Metab. 1977; 45:641-52. uals: A Handbook for Physicians. New York, American Heart As-
7
Murray, F. T., Zinman, B., McClean, P. A., Devoga, A., sociation, 1972; 14-15.
17
Albisser, A. M., Leibel, B. S., Nakhooda, A. F., Stokes, E. F, Astrand, P. O.: Aerobic work capacity in men and women
and Marliss, E. B.: The metabolic response to moderate exercise with special reference to age. Acta Physiol. Scand. 1960; 49:169.
18
in diabetic man receiving intravenous and subcutaneous insulin. J. Pollock, M. L.: The quantification of endurance training pro-
Clin. Endocrinol. Metab. 1977; 44:708-20. grammes. Exer. Sport Sci. Rev. 1973; 1.
8 19
Nelson, J. D., Poussier, P., Marliss, E. B., Albisser, A. M., Young, C. M., Hagan, G. C., Tucker, R. E., and Foster,
and Zinman, B.: The metabolic responses of normal and insulin W. D.: A comparison of dietary study methods II. Dietary history
infused diabetics to postprandial exercise. Am. J. Physiol. 1982; vs. seven-day record vs. 24 hour recall. J. Am. Diet. Assoc. 1952;
242:E309. 28:218-21.
9 20
Poussier, P., Zinman, B., Marliss, E. B., Albisser, A. M., Perl- Reed, R. B., and Burke, B. S.: Collection and analysis of
man, K., and Caron, D.: Open loop intravenous insulin waveforms dietary intake data. Am. J. Public Health 1954; 44:1015-26.
21
for postprandial exercise in type I diabetes. Diabetes Care 1983; Young, C. M., and Trulson, M. F: Methodology for dietary
6:129-34. studies in epidemiological surveys II—strengths and weaknesses of
10
Bjorntorp, P., Dejounge, K., Sjostrom, L , and Sullivan, L : existing methods. Am. J. Public Health 1960; 50:803-14.
22
Physical training in human obesity II. Effects of plasma insulin in Mayer, J., Marshall, N. B., Vitale, J. J., Christensen, J. D.,
glucose intolerant obese subjects without marked hyperinsulinemia. Mosha-Gekhi, M. B., and Stare, F. J.: Exercise food intake and
Scand. J. Clin. Lab. Invest. 1973; 32:41-45. body weight in normal rats and genetically obese adult mice. Am.
11
Bjorntorp, P., Holm, G., Jacobson, B., Dejounge, K., Lund- J. Physiol. 1954; 177:544-48.
23
berg, P., Smith, V., and Sullivan, L.: Physical training in human Paffenbarger, R. S., Jr., and Hyde, R. T.: Exercise as protection
hyperplastic obesity IV and effects on the hormonal status. Metab- against heart attack. N. Engl. J. Med. 1980; 302:1026-27.
24
olism 1977; 26:319-28. Peterson, C M . , Jones, R. L , Esterly, J. A., Wantz, G. E.,
12
Ruderman, N. B., Ganda, O. P., and Johnson, K.: The effect and Jackson, R. L.: Changes in basement membrane thickening
of physical training on glucose tolerance and plasma lipids in ma- and pulse volume concomitant with improved glucose control and
turity-onset diabetes. Diabetes 1979; 28 (Suppl. 1):89—92. exercise in patients with insulin-dependent diabetes mellitus. Di-
13
Saltin, B., Lingarde, B. S., Jouston, M., Horlin, R., Nygaard, abetes Care 1980; 3:586-89.
25
E., and Gad, P.: Physical training and glucose tolerance in middle- Kannel, W. B., and Sorlie, P.: Some health benefits of physical
age men. Diabetes 1979; 28:30-32. activity. Arch. Intern. Med. 1979; 139:857-61.
14 26
Wallberg-Henriksson, H., Gunnarsson, R., Henriksson, J., Froelicher, V. F., and Oberman, A.: Analysis of epidemiologic
DeFronzo, R. A., Felig, P., Ostran, J., and Wahren, J.: Increased studies of physical inactivity as risk factor for coronary artery disease.
peripheral insulin sensitivity and muscle mitochondrial enzymes but In Exercise and Heart Disease. Sonnenblick, E. H., and Lesch, M.,
unchanged blood glucose control in type I diabetics after physical Eds. New York, Grune & Stratton, Inc., 1977:209-27.
27
training. Diabetes 1982; 31:1044-50. Morgan, W. P.: Psychological effects of exercise. Behav. Med.
15
Caron, D., Poussier, P., Marliss, E. B., and Zinman, B.: The Update 1982; 4:25-30.
DIABETES CARE, VOL. 7 NO. 6, NOVEMBER-DECEMBER 1984 519
Potrebbero piacerti anche
- Current Concepts in Muscle Stretching For Exercise and Rehabilitation PDFDocumento11 pagineCurrent Concepts in Muscle Stretching For Exercise and Rehabilitation PDFElaine CspNessuna valutazione finora
- Current Concepts in Shoulder Examination of The Overhead Athlete PDFDocumento25 pagineCurrent Concepts in Shoulder Examination of The Overhead Athlete PDFElaine CspNessuna valutazione finora
- Diaphragmatic Breathing - The Foundation of Core Stability PDFDocumento7 pagineDiaphragmatic Breathing - The Foundation of Core Stability PDFElaine CspNessuna valutazione finora
- Complex Systems Approach For Sports Injuries - Moving From Risk Factor Identification To Injury Pattern Recognition-Narrative Review and New Concept PDFDocumento8 pagineComplex Systems Approach For Sports Injuries - Moving From Risk Factor Identification To Injury Pattern Recognition-Narrative Review and New Concept PDFElaine CspNessuna valutazione finora
- Biotensegrity and Myofascial Chains - A Global Approach To An Integrated Kinectic Chain PDFDocumento7 pagineBiotensegrity and Myofascial Chains - A Global Approach To An Integrated Kinectic Chain PDFElaine CspNessuna valutazione finora
- Adductor Magnus An EMG Investigation Into Proximal and Disctal Portions and Direction Specific ActionDocumento9 pagineAdductor Magnus An EMG Investigation Into Proximal and Disctal Portions and Direction Specific ActionElaine CspNessuna valutazione finora
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5795)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Recommended Practice For Corrosion Management of Pipelines in Oil & Gas Production and TransportationDocumento123 pagineRecommended Practice For Corrosion Management of Pipelines in Oil & Gas Production and Transportationsaifoa100% (2)
- Pineapple PDFDocumento7 paginePineapple PDFDestia AyuNessuna valutazione finora
- Planificare Săptămânală - Clasa A II-a (Fairyland 2)Documento6 paginePlanificare Săptămânală - Clasa A II-a (Fairyland 2)Oxy Oxy100% (1)
- Trane Air Cooled Scroll Chillers Installation Operation MaintenanceDocumento276 pagineTrane Air Cooled Scroll Chillers Installation Operation MaintenanceBay Mưa100% (1)
- Osh e MeerDocumento3 pagineOsh e MeerfatduckNessuna valutazione finora
- HDFC Life Insurance (HDFCLIFE) : 2. P/E 58 3. Book Value (RS) 23.57Documento5 pagineHDFC Life Insurance (HDFCLIFE) : 2. P/E 58 3. Book Value (RS) 23.57Srini VasanNessuna valutazione finora
- RIASEC Personality TestDocumento2 pagineRIASEC Personality TestSarah Jane NomoNessuna valutazione finora
- BT HandoutsDocumento4 pagineBT HandoutsNerinel CoronadoNessuna valutazione finora
- Sikadur 42 HSDocumento2 pagineSikadur 42 HSthe pilotNessuna valutazione finora
- Preparing Polymers For The Jar TestDocumento5 paginePreparing Polymers For The Jar Testarvin4dNessuna valutazione finora
- Written Assignment Unit 4 Health ScienceDocumento6 pagineWritten Assignment Unit 4 Health SciencesafsdaNessuna valutazione finora
- W01 M58 6984Documento30 pagineW01 M58 6984MROstop.comNessuna valutazione finora
- Research Activity #2Documento2 pagineResearch Activity #2Shania GualbertoNessuna valutazione finora
- Minerals and Resources of IndiaDocumento11 pagineMinerals and Resources of Indiapartha100% (1)
- Textbook of Dental Anatomy, Physiology and Occlusion, 1E (2014) (PDF) (UnitedVRG)Documento382 pagineTextbook of Dental Anatomy, Physiology and Occlusion, 1E (2014) (PDF) (UnitedVRG)Konstantinos Ster90% (20)
- Toxic RelationshipDocumento1 paginaToxic RelationshipwidyasNessuna valutazione finora
- Cat 880620 R11Documento60 pagineCat 880620 R11pawelprusNessuna valutazione finora
- Low Voltage Fixed and Automatic Power Factor Correction SystemsDocumento6 pagineLow Voltage Fixed and Automatic Power Factor Correction Systemszabiruddin786Nessuna valutazione finora
- OphthalmoplegiaDocumento5 pagineOphthalmoplegiaPatricia Feliani SitohangNessuna valutazione finora
- Plasma Arc Machining (Pam) : Mechanical Engineering Department I.I.T Guwahati-781039 E-Mail: Manasdas@iitg - Ernet.inDocumento15 paginePlasma Arc Machining (Pam) : Mechanical Engineering Department I.I.T Guwahati-781039 E-Mail: Manasdas@iitg - Ernet.inSrinivasanNessuna valutazione finora
- 7 LevelDocumento5 pagine7 LevelACHREF RIHANINessuna valutazione finora
- 48V 100ah LiFePO4 Battery Spec With CommunicationDocumento6 pagine48V 100ah LiFePO4 Battery Spec With CommunicationsoulmuhNessuna valutazione finora
- Precision Medicine Care in ADHD The Case For Neural Excitation and InhibitionDocumento12 paginePrecision Medicine Care in ADHD The Case For Neural Excitation and InhibitionDaria DanielNessuna valutazione finora
- MGMTDocumento19 pagineMGMTMakrant MohanNessuna valutazione finora
- Intraocular Pressure and Aqueous Humor DynamicsDocumento36 pagineIntraocular Pressure and Aqueous Humor DynamicsIntan EkarulitaNessuna valutazione finora
- Plastic As Soil StabilizerDocumento28 paginePlastic As Soil StabilizerKhald Adel KhaldNessuna valutazione finora
- Intellectual Disability: Definition, Classification, Causes and CharacteristicsDocumento12 pagineIntellectual Disability: Definition, Classification, Causes and CharacteristicsRyan RV ViloriaNessuna valutazione finora
- Exam Questions: Exam Title: Chapter MEK 8Documento4 pagineExam Questions: Exam Title: Chapter MEK 8vishnu sharmaNessuna valutazione finora
- Pearls and Pitfalls in Emergency Radiology Variants and Other Difficult Diagnoses 2013Documento389 paginePearls and Pitfalls in Emergency Radiology Variants and Other Difficult Diagnoses 2013mmbire@gmail.comNessuna valutazione finora
- RCMaDocumento18 pagineRCMaAnonymous ffje1rpaNessuna valutazione finora