Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Flap Valved VSD Closure Prasanna
Caricato da
prasannasimhaDescrizione originale:
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Flap Valved VSD Closure Prasanna
Caricato da
prasannasimhaCopyright:
Formati disponibili
Flap valved closure of ventricular septal defects with increased pulmonary
vascular resistance
Prasanna Simha Mohan Rao, Varadaraju Raju and Madhusudana Narayana
Interact CardioVasc Thorac Surg 2010;11:577-580; originally published online Aug 19,
2010;
DOI: 10.1510/icvts.2010.243865
The online version of this article, along with updated information and services, is
located on the World Wide Web at:
http://icvts.ctsnetjournals.org/cgi/content/full/11/5/577
Interactive Cardiovascular and Thoracic Surgery is the official journal of the European Association
for Cardio-thoracic Surgery (EACTS) and the European Society for Cardiovascular Surgery
(ESCVS). Copyright © 2010 by European Association for Cardio-thoracic Surgery. Print ISSN:
1569-9293.
Downloaded from icvts.ctsnetjournals.org by on October 20, 2010
ARTICLE IN PRESS
doi:10.1510/icvts.2010.243865
Editorial
New Ideas
Interactive CardioVascular and Thoracic Surgery 11 (2010) 577–580
www.icvts.org
Institutional report - Congenital
Progress Report
Flap valved closure of ventricular septal defects with increased
Work in
pulmonary vascular resistance
Prasanna Simha Mohan Rao*, Varadaraju Raju, Madhusudana Narayana
Protocol
Sri Jayadeva Institute of Cardiovascular Sciences and Research, Bannerghatta Road, Bangalore, India
Received 21 May 2010; received in revised form 27 July 2010; accepted 29 July 2010
Institutional
Report
Abstract
Closure of ventricular septal defect (VSD) in children with elevated pulmonary vascular resistance (PVR) is associated with significant
morbidity and mortality with pulmonary hypertensive (PH) episodes being a major postoperative problem. Flap valved closure of VSD is
reported to decrease morbidity and mortality. We report our experience of closure of a VSDs in patients with severe PH, using a valved
Article
ESCVS
patch in an effort to reduce the risk of operation. Eighteen consecutive patients with a large VSD with severe PH (mean PVR )8 Wood
units) underwent flap valved closure (as described by Novick et al.) of VSD during a one-year study period. The mean age at surgery was
8.3"3.9 years (range: 3–13 years). Mean PVRI was 13.02"4.05 Wood units. In-hospital 30-day mortality was 5.6% (1y18). Mechanical
Proposal for Bail-
out Procedure
ventilation time averaged 11.6"8.1 hours. Postoperative pulmonary artery pressures were significantly reduced. Four patients had PH crisis
postoperatively. Obvious opening and closing of the flap valve was detected by echocardiography in eight patients. There were no late
deaths due to cardiac causes. Closure of a large VSD in patients with severe pulmonary hypertension could be performed with low morbidity
and mortality when a flap valve patch was used.
䊚 2010 Published by European Association for Cardio-Thoracic Surgery. All rights reserved.
Negative
Results
Keywords: Ventricular septal defect; Pulmonary vascular resistance; Flap valve patch; Cardiopulmonary bypass; Low cardiac output
1. Introduction tively is especially difficult with a high mortality and
Follow-up
morbidity. We report our experience of closure of a VSDs
Paper
Congenital heart disease with septal defects and a large in patients with severe PH, using valved patch in an effort
left to right shunt often causes pulmonary artery (PA) to reduce risk of operation.
hypertension. The course of the disease is variable and
State-of-the-art
depends on the size of the defect, magnitude of the left
to right shunt, and the pulmonary vascular response to 2. Patients and methods
increased pulmonary blood flow and pressure. PA pressure
is hyperkinetic in the early phase but may eventually
become a fixed elevation due to a fixed increase of 2.1. Patients
Best Evidence
pulmonary vascular resistance (PVR) w1x. They clinically
manifest with decreased exercise tolerance, cyanosis, con- Between August 2008 and July 2009, 18 patients present-
Topic
gestive cardiac failure, often hemoptysis, and finally death ing to our unit with a VSD and increased PVRI (mean PVRI
(Eisenmenger’s syndrome). )8 Wood units) were included in the study. The patients
Closure of a ventricular septal defect (VSD) with increased were evaluated preoperatively by history and physical
Nomenclature
PVR is associated with significant morbidity and mortality examination, chest radiography, electrocardiography,
w2, 3x. Acute congestive heart failure, pulmonary hyperten- transthoracic echocardiography (TTE), and cardiac
sive (PH) crisis, and acute respiratory failure are the catheterization.
principal causes of postoperative death. In some patients Complete hemodynamic data were determined by cardiac
the postoperative increase of PVR may be more marked, catheterization. Pulmonary and systemic flow and resis-
Historical
may regress slowly, may show intermittent spontaneous or tance were measured at rest and 100% oxygen. Color
Pages
precipitated crisis-like exacerbation, and may require pro- M-mode echocardiography was done to assess the direction
longed ventilation and specific strategies to maintain a of shunting across VSD. The decision for surgery was based
lower PVR w4x. on the presence of any augmentation of left to right shunt
Many patients in developing nations come at a stage of or increase in pulmonary vascular blood flow following
Communication
near eisenmengerization and their management periopera- sublingual nitrate administration on preoperative echocar-
Brief
diography even if the patients showed an unfavorable PVR
*Corresponding author. Shri, No 33, 2ndy3rd Cross, Sampige Road, Malles-
waram, Bangalore 560003, Karnataka, India. Tel.: q91 93 41216294. on formal hemodynamic testing in the cardiac catheteri-
E-mail address: prasannasimha@gmail.com (P.S. Mohan Rao). zation laboratory. The study was approved by the Hospital
Case Report
䊚 2010 Published by European Association for Cardio-Thoracic Surgery
Downloaded from icvts.ctsnetjournals.org by on October 20, 2010
ARTICLE IN PRESS
578 P.S. Mohan Rao et al. / Interactive CardioVascular and Thoracic Surgery 11 (2010) 577–580
Research Ethics Committee, and written informed consent 2.5. Follow-up
was obtained from the parents of each child.
All patients were followed-up at regular intervals (every
three months) with clinical examination, and TTE to esti-
2.2. Surgical procedure and cardiopulmonary bypass
mate the PA pressure, assess the right ventricular function
Surgery was performed with standard cardiopulmonary and to demonstrate any right-to-left shunting.
bypass (CPB) with moderate hypothermia and cold blood
cardioplegia was used in all patients. Inj phenoxybenzamine 2.6. Statistical analysis
(0.5 mgykg i.v.) was given prior to CPB. Zero balance ultra
All data are expressed as mean"standard deviation. Con-
filtration was done throughout CPB. The operative approach
tinuous variables at baseline and following surgery were
was transatrial.
compared with unpaired t-test. A P-value of 0.05 or lower
A patch was constructed using the technique described by
on any test was considered to indicate statistical signifi-
Novick et al., using a Gore-Tex patch approximately as
cance. Data were analyzed using SPSS software (SPSS Inc,
large as the defect to be closed. A fenestration that was
Chicago, IL, USA).
half of the expected aortic annulus diameter was made in
the patch. Following this, a separate flap patch at least
3. Results
2 mm larger than the fenestration was constructed and was
sewn onto the superior margin of the fenestration along
one-third of the circumference. A separate tethering stitch 3.1. Patient characteristics
was placed at the inferior apex of the flap valve and tied The mean age at surgery was 8.3"3.9 years (range: 3–
loosely over a Hegar dilator that was the same size as the 13 years) and female to male ratio was 1.25:1. One patient
fenestration. This tethering stitch length approximated the with PVR 13.3 Wood units had Down’s syndrome.
diameter of the fenestration. The VSD patch was sewn into
place orienting the patch in such a way that the flap valve 3.2. Preoperative data
was placed on the left ventricular (LV) side with the flap
opening towards the LV apex to avoid subaortic obstruction. A perimembranous VSD was diagnosed in 80% of patients.
Patent foramen ovale (PFO) was left open in all patients. Muscular VSD was seen in 20% of patients. Cardiac cathe-
Tricuspid valve competence was checked and repaired if terization showed the ratio of systolic pulmonary artery
necessary. pressure to systolic systemic arterial blood pressure ranged
from 0.8 to 0.9 (mean: 0.85). Mean PVR was 13.02"4.05
2.3. Weaning from CPB Wood units (range: 8.5–23 Wood units) and after oxygen
administration was 8.34"2.5 Wood units. PVR was more
Prior to discontinuation of CPB, dobutamine 3 mgykgymin, than 10 Wood units in 11 patients and was )15 Wood units
nitroprusside 0.5–2 mgykgymin, and the phosphodiesterase in four patients. The ratio of pulmonary artery flow to
inhibitor milrinone 0.35 mgykgymin were started. Inj phen- systemic arterial blood flow (QpyQs) ranged from 0.5 to
oxybenzamine 0.5 mgykgyday were given as infusion for 2.0 (mean: 1.44"0.36) and increased to a mean of
48 h followed by oral formulation. Left atrial (LA) line was 1.91"0.34 after oxygen administration, and was -1.5 in
placed if required and systemic vasoconstrictors were start- eight patients. Mean pulmonary artery pressure (MPAP)
ed through it. After weaning from CPB, modified ultrafil- ranged from 57 to 80 mmHg (mean: 68.8"9.7 mmHg) and
tration was used in all the patients. Epicardial echo- was )70 mmHg in nine patients. Arterial oxygen saturation
cardiography was used to assess the degree of shunting ranged from 88 to 99% (mean: 95.2"3.04%). Preoperative
across the fenestration. catheterization data are summarized in Table 1.
2.4. Postoperative management 3.3. Operative data
Pulmonary and systemic artery pressures were monitored Eighteen patients underwent flap valved closure of VSD
continuously. Mild to moderate hypocarbia was maintained out of which four patients could not be weaned-off CPB
during mechanical ventilation. Serial postoperative TTE was initially and required placement of LA line, through which
used to assess the degree of shunting across the fenestra- systemic vasoconstrictors (noradrenaline and vasopressin)
tion. Once the patients are fully awake and hemodynami- were started and then patients could be weaned from CPB.
cally stable, they were extubated. Inhaled nitroprusside
and milrinone nebulisation were given intermittently (every Table 1. Preoperative catheterization data
2 hours) or when PA pressure surges occur. Inotropes were Variables Mean value
weaned-off once patients were hemodynamically stable.
Milrinone infusion was stopped within 36–48 hour provided PVRI 13.02"4.05
QpyQs 1.44"0.37
PA pressure surges stopped or no right to left shunting SpO2 (%) 95.2"3.04
across PFO. Oral phenoxybenzamine was administered at PAsyAos 0.88"0.5
48 hours and sildenafil (1 mgykg 4 hourly) was adminis-
PAsyAos, ratio of pulmonary artery systolic pressure to aortic systolic pres-
tered on the first postoperative day (POD). Patients were sure; PVRI, pulmonary vascular resistance index; QpyQs, ratio of pulmonary
monitored for seven days in ICUyintermediate care for PH blood flow to systemic blood flow; SpO2 , arterial hemoglobin oxygen
crisis. saturation.
Downloaded from icvts.ctsnetjournals.org by on October 20, 2010
ARTICLE IN PRESS
P.S. Mohan Rao et al. / Interactive CardioVascular and Thoracic Surgery 11 (2010) 577–580 579
Editorial
One patient with PVR of 9.3 Wood units had a persistent 3.6. Clinical outcome
rise in PA pressure )70% of systemic pressure, inspite of
maximizing pulmonary vasodilators and had significant LV Thirty-day mortality was 5.6%. One patient with PVR of
New Ideas
dysfunction. She had her chest kept open and was shifted 18.43 Wood units expired after 48 days due to bronchom-
to the ICU. alacia. There have been no subsequent deaths on follow-
up. At a mean follow-up of nine months (range: five to
3.4. Postoperative period 12 months), one patient with PVR of 13.56 Wood units had
Progress Report
TTE evidence of moderate PH at three months, postopera-
Work in
Mechanical ventilation time ranged from 8 to 36 hours tively. Sildenafil and phenoxybenzamine were continued for
(mean: 11.6"8.1 hours). Three patients with a PVR of the next two months and were stopped when follow-up PA
18.43, 8.8 and 15 Wood units had an episode of PH crisis pressure was persistently low. The others were asympto-
on the day of surgery and were managed with administra- matic with normal or near normal PA pressure. Postopera-
Protocol
tion of inhaled pulmonary vasodilators, oxygen administra- tive hemodynamics are given in Table 3.
tion, and support with inotropic and vasodilator drugs. We compared our data to a historical control of 18
One patient with PVR of 9.3 Wood units required splinting patients with PVRI )8 Wood units, where the mortality
open of the sternum. She had persistent elevation of the was 12.6% and the mean ventilation time was 86"12 hours.
Institutional
Report
PA pressure in the postoperative period and developed
repeated episodes of PH crisis on first POD. She developed 4. Discussion and conclusions
intractable supraventricular tachycardia followed by low
cardiac output (LCO) and expired on the second POD. Historically, surgical closure of a large VSD with severe
PH was associated with a high mortality rate w4, 5x. Even
Article
Three patients with a PVR of 18.43, 9.3 and 18.6 Wood
ESCVS
units, respectively went into supraventricular tachycardia in the present era, postoperative PH remains a significant
on the day of surgery and were managed with administra- risk factor for morbidity and mortality.
Acute congestive heart failure, PH crisis, and acute res-
Proposal for Bail-
tion of amiodarone as a bolus followed by infusion. Six
out Procedure
patients developed right lower lobe collapse of which three piratory failure are the principal causes of postoperative
required pleural drain insertion for concomitant effusion death. CPB, infusion of protamine, and other factors that
and two required bronchoscopy. One patient with PVR of could cause the release of vasoactive substances, such as
18.43 Wood units had an episode of PH crisis on the third thromboxane A2 and catecholamines could result in pul-
POD, which was triggered by right lower lobe collapse due monary vasoconstriction and acute PH crisis w6, 7x.
Negative
Creation of an intracardiac shunt to prevent right ventri-
Results
to bronchomalacia requiring reintubation. The patient
underwent tracheostomy on the eighth POD and was in the cular failure has been used with success. Novick and col-
ICU for one month and was later discharged at their leagues used a flap valved double-patch for closure of VSDs
request. She expired after 48 days due to bronchomalacia in children with increased PVR w3, 8x. The double patch
Follow-up
technique provides a simple physiological mechanism for
Paper
which required stenting but her parents refused treatment
for it. The patient with Down’s syndrome could not be unloading the right ventricle during periods of severe PH,
weaned-off the ventilator due to upper airway obstruction whether acute and transient or sustained. The modification
allowed more patients to be extubated within 48 hours and
State-of-the-art
caused by a large tongue. He required a tracheo-
stomy on the second POD. Take down of tracheostomy was with lower operative mortality. The flap valve allows early
done on 10th POD and he was discharged on the 14th POD. extubation and prevents supra-systemic pulmonary pres-
The other patients had an uneventful postoperative course. sures that can be rapidly fatal in the postoperative period
and allows patients to ride through PH crisis without the
need for prolonged intubation and multiple maneuvers
Best Evidence
3.5. Echocardiographic assessment
albeit at the cost of transient desaturation, while main-
Topic
Eight patients had a right-to-left shunt through the valved taining adequate systemic cardiac output which is tolerated
patch as determined by TTE (eight patients up to the well until the PH crisis is resolved.
second POD, one patient on the third POD and no patients In our study, all patients were children with high PVR.
up to the seventh POD). Three patients had right to left Thirty-day mortality was 5.6%. One patient with a PVR 9.3 Nomenclature
shunting across the PFO. Postoperative TTE results are Wood unit died on the second POD with frequent episodes
summarized in Table 2. All patients had preserved right of PH crisis and intractable supra ventricular tachycardia
ventricular function (by visual estimation on echocardio- followed by LCO. Early extubation was possible in most of
graphy) and none of the patients had significant tricuspid our patients thereby diminishing the need for prolonged
regurgitation. mechanical ventilation. In addition, prolonged stay in the
Historical
Pages
Table 2. Postoperative echocardiographic assessment Table 3. Preoperative and postoperative hemodynamic status
Time No right to left shunt Right to left shunt Characteristics Before repair After repair P-value
(cases) (cases)
Communication
MPAP (mmHg) 68.83"9.67 34.4"11.42 0.0001
Day 2 10 8 PAsyAos 0.88"0.5 0.52"0.2 0.013
Brief
Day 7 17 0 SpO2 95.2"3.04 97.9"2.4 0.005
Three months 16 0
Six months 16 0 MPAP, mean pulmonary artery pressure; PAsyAos, ratio of pulmonary artery
Nine months 14 0 systolic pressure to aortic systolic pressure; SpO2 , arterial hemoglobin oxygen
saturation.
Case Report
Downloaded from icvts.ctsnetjournals.org by on October 20, 2010
ARTICLE IN PRESS
580 P.S. Mohan Rao et al. / Interactive CardioVascular and Thoracic Surgery 11 (2010) 577–580
ICU is associated with an increase in septic complications References
w9x and other adverse events. Early extubation reduces the
use of resources that are already limited in a number of w1x Rabinovitch M, Keane JF, Norwood WI, Castaneda AR, Reid L. Vascular
developing countries. structure in lung tissue obtained at biopsy correlated with pulmonary
Severe reactive postoperative PH may occur despite a hemodynamic findings after repair of congenital heart defects. Circu-
technically successful operation and active conventional lation 1984;69:655–667.
w2x Frontera-Izquierdo P, Cabezuelo-Huerta G. Natural and modified history
management, including the administration of high inspired
of isolated ventricular septal defect: a 17-year study. Pediatr Cardiol
oxygen, hyperventilation, sedation, neuromuscular block- 1992;13:193–197.
ade, and support with inotropic and vasodilator drugs w6x. w3x Novick WM, Gurbuz AT, Watson DC, Lazorishinets VV, Perepeka AN,
When these therapies fail, patients can be considered for Malcic I, Marinovic B, Alpert BS, Di Sessa TG. Double patch closure of
inhaled nitric oxide and extracorporeal life support (ECLS) ventricular septal defect with increased pulmonary vascular resistance.
Ann Thorac Surg 1998;66:1533–1538.
which ensures adequate oxygenation and systemic perfusion
w4x Kirklin JW, Barratt-Boyes BG. Ventricular septal defect. In: Cardiac
in the face of a markedly elevated PVR and may allow time surgery, 3rd edition. Churchill-Livingstone, 2003:851–897.
for the PH crisis to resolve w10x. w5x Kannan BR, Sivasankaran S, Tharakan JA, Titus T, Ajith Kumar VK,
PH after closure of a large VSD continues to cause signif- Francis B, Krishnamoorthy KM, Harikrishnan S, Padmakumar R, Nair K.
icant morbidity and mortality even in industrialized coun- Long-term outcome of patients operated for large ventricular septal
tries. The use of nitric oxide and extra corporeal membrane defects with increased pulmonary vascular resistance. Indian Heart J
2003;55:161–166.
oxygenation rescue has reduced the mortality, but with
w6x Hopkins RA, Bull C, Haworth SG, de Leval MR, Stark J. Pulmonary
significant cost and patient morbidity. These expensive and hypertensive crises following surgery for congenital heart defects in
sophisticated modalities are not available in many countries young children. Eur J Cardiothorac Surg 1991;5:628–634.
throughout the world w10x. w7x De Souza CA, Spyt TJ. Release of vasoactive substance during cardio-
Patients with VSD with severe PH who would otherwise be pulmonary bypass. Ann Thorac Surg 1992;56:397–398.
considered for lung transplantation can undergo conven- w8x Novick WM, Sandoval N, Lazorhysynets VV, Castillo V, Baskevitch A, Mo
X, Reid RW, Marinovic B, Di Sessa TG. Flap valve double patch closure
tional cardiac surgery using flap valve method of VSD
of ventricular septal defects in children with increased pulmonary
closure in a significant subset. Reports show that patients vascular resistance. Ann Thorac Surg 2005;79:21–28.
with PH improved their hemodynamics and exercise capa- w9x Milliken J, Tait GA, Ford Jones EL, Mindorff CM, Gold R, Mullins G.
bility after closure of the septal defect. It implies that Nosocomial infections in a pediatric intensive care unit. Crit Care Med
pulmonary vascular remodeling might take place but 1998;16:233–237.
w10x Dhillon R, Pearson GA, Firmin RK, Chan KC, Leanage R. Extracorporeal
requires long-term follow-up w11x.
membrane oxygenation and the treatment of critical pulmonary hyper-
We conclude that a valved patch in cases of severe PH
tension in congenital heart disease. Eur J Cardiothorac Surg 1995;9:553–
can undergo operation with reasonable morbidity and mor- 556.
tality in the absence of sophisticated pharmacological or w11x Wessel D. Current and future strategies in the treatment of childhood
mechanical intervention. pulmonary hypertension. Progr Pediatr Cardiol 2001;12:289–318.
Downloaded from icvts.ctsnetjournals.org by on October 20, 2010
Flap valved closure of ventricular septal defects with increased pulmonary
vascular resistance
Prasanna Simha Mohan Rao, Varadaraju Raju and Madhusudana Narayana
Interact CardioVasc Thorac Surg 2010;11:577-580; originally published online Aug 19,
2010;
DOI: 10.1510/icvts.2010.243865
This information is current as of October 20, 2010
Updated Information including high-resolution figures, can be found at:
& Services http://icvts.ctsnetjournals.org/cgi/content/full/11/5/577
References This article cites 10 articles, 5 of which you can access for free at:
http://icvts.ctsnetjournals.org/cgi/content/full/11/5/577#BIBL
Subspecialty Collections This article, along with others on similar topics, appears in the
following collection(s):
Congenital - acyanotic
http://icvts.ctsnetjournals.org/cgi/collection/congenital_acyanotic
Permissions & Licensing Requests to reproducing this article in parts (figures, tables) or in
its entirety should be submitted to: icvts@ejcts.ch
Reprints For information about ordering reprints, please email:
icvts@ejcts.ch
Downloaded from icvts.ctsnetjournals.org by on October 20, 2010
Potrebbero piacerti anche
- Sslvd1-Eos2 - Mission BrochureDocumento6 pagineSslvd1-Eos2 - Mission BrochureprasannasimhaNessuna valutazione finora
- SIRT6 PPAR Experssion PIIS2211124721005362Documento20 pagineSIRT6 PPAR Experssion PIIS2211124721005362prasannasimhaNessuna valutazione finora
- Mucosal Immunity in Viral DX Ann Immunol 2016Documento37 pagineMucosal Immunity in Viral DX Ann Immunol 2016prasannasimhaNessuna valutazione finora
- 2lewsi Dexter ASD 09.fullDocumento17 pagine2lewsi Dexter ASD 09.fullprasannasimhaNessuna valutazione finora
- Mask H2O2 Sterilization IPIntJMedMicrobiolTropDis-7-4-232-236Documento5 pagineMask H2O2 Sterilization IPIntJMedMicrobiolTropDis-7-4-232-236prasannasimhaNessuna valutazione finora
- Linear AbridgedDocumento145 pagineLinear AbridgedFrancisco BenítezNessuna valutazione finora
- 02-07-2021 HMB EnglishDocumento36 pagine02-07-2021 HMB EnglishKiran SNNessuna valutazione finora
- Mucosal Immunity in Viral DX Ann Immunol 2016Documento37 pagineMucosal Immunity in Viral DX Ann Immunol 2016prasannasimhaNessuna valutazione finora
- Basics of CPB: Praanna Simha Mohan RaoDocumento35 pagineBasics of CPB: Praanna Simha Mohan Raoprasannasimha0% (1)
- Recent Trials Score 2019Documento21 pagineRecent Trials Score 2019prasannasimhaNessuna valutazione finora
- Mucosal Immunity in Viral DX Ann Immunol 2016Documento37 pagineMucosal Immunity in Viral DX Ann Immunol 2016prasannasimhaNessuna valutazione finora
- Iist Bond Format Undergraduate 2015Documento5 pagineIist Bond Format Undergraduate 2015prasannasimhaNessuna valutazione finora
- Cut Here Cut Here: Assembly InstructionsDocumento1 paginaCut Here Cut Here: Assembly InstructionsprasannasimhaNessuna valutazione finora
- IIST Bond SpecimenDocumento4 pagineIIST Bond SpecimenprasannasimhaNessuna valutazione finora
- Handbook Chapter 7Documento4 pagineHandbook Chapter 7prasannasimhaNessuna valutazione finora
- Geri Radial To Femoral Pressure GradientDocumento5 pagineGeri Radial To Femoral Pressure GradientprasannasimhaNessuna valutazione finora
- Improving Neuroprotection During Dhca, by Vicki Mahan, MD, Instructor in Surgery (PPT Slide Show)Documento79 pagineImproving Neuroprotection During Dhca, by Vicki Mahan, MD, Instructor in Surgery (PPT Slide Show)prasannasimhaNessuna valutazione finora
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- CHN - 1Documento23 pagineCHN - 1Raagul SaravanaKumarNessuna valutazione finora
- DR Bagus Ari - Cardiogenic Shock KuliahDocumento28 pagineDR Bagus Ari - Cardiogenic Shock KuliahrathalosredNessuna valutazione finora
- GMO Pro Arguments (Gen-WPS OfficeDocumento4 pagineGMO Pro Arguments (Gen-WPS OfficeFranchesca RevelloNessuna valutazione finora
- Operator MGC Ultima PFX - English - 142152-001rCDocumento65 pagineOperator MGC Ultima PFX - English - 142152-001rCEvangelosNessuna valutazione finora
- Geria NCPDocumento4 pagineGeria NCPBrylle CapiliNessuna valutazione finora
- Hypnosis For Irritable Bowel SyndromeDocumento3 pagineHypnosis For Irritable Bowel SyndromeImam Abidin0% (1)
- Bipolar Disorder - A Cognitive Therapy Appr - Cory F. NewmanDocumento283 pagineBipolar Disorder - A Cognitive Therapy Appr - Cory F. NewmanAlex P100% (1)
- Corona Vacsine 2nd DoseDocumento2 pagineCorona Vacsine 2nd Doseavishekbhowmick18Nessuna valutazione finora
- Amazing Facts About Our BrainDocumento4 pagineAmazing Facts About Our BrainUmarul FarooqueNessuna valutazione finora
- 11 Retention of Maxillofacial Prosthesis Fayad PDFDocumento7 pagine11 Retention of Maxillofacial Prosthesis Fayad PDFMostafa Fayad50% (2)
- 2015 JC2 GP H1 Prelim PapersDocumento357 pagine2015 JC2 GP H1 Prelim PapersofficialJCUOLnotes100% (6)
- Malawi Clinical HIV Guidelines 2019 Addendumversion 8.1Documento28 pagineMalawi Clinical HIV Guidelines 2019 Addendumversion 8.1INNOCENT KHULIWANessuna valutazione finora
- Nclex Mnemonics 2020 2Documento9 pagineNclex Mnemonics 2020 2Winnie OkothNessuna valutazione finora
- NUR091 - Session 8Documento6 pagineNUR091 - Session 8aquinoemjay27Nessuna valutazione finora
- Program Implementation With The Health Team: Packages of Essential Services For Primary HealthcareDocumento1 paginaProgram Implementation With The Health Team: Packages of Essential Services For Primary Healthcare2A - Nicole Marrie HonradoNessuna valutazione finora
- NCRP 160 PDFDocumento81 pagineNCRP 160 PDFmarkNessuna valutazione finora
- Infective Endocarditis (IE)Documento76 pagineInfective Endocarditis (IE)Mahesh RathnayakeNessuna valutazione finora
- Punjab Municipal Corporation Act, 1976 PDFDocumento180 paginePunjab Municipal Corporation Act, 1976 PDFSci UpscNessuna valutazione finora
- Parathyroi D HormoneDocumento25 pagineParathyroi D HormoneChatie PipitNessuna valutazione finora
- 12 Psychology - Meeting Life Challenges - Notes & Video LinkDocumento11 pagine12 Psychology - Meeting Life Challenges - Notes & Video LinkRamesh TalukdarNessuna valutazione finora
- 3E - Agustin, Anne Julia - Group 1 - Case 7,8Documento5 pagine3E - Agustin, Anne Julia - Group 1 - Case 7,8Anne Julia AgustinNessuna valutazione finora
- ESC - 2021 - The Growing Role of Genetics in The Understanding of Cardiovascular Diseases - Towards Personalized MedicineDocumento5 pagineESC - 2021 - The Growing Role of Genetics in The Understanding of Cardiovascular Diseases - Towards Personalized MedicineDini SuhardiniNessuna valutazione finora
- Carbon Monoxide PoisoningDocumento31 pagineCarbon Monoxide PoisoningDheerajNessuna valutazione finora
- Written Report Bio 150Documento7 pagineWritten Report Bio 150hyebibieNessuna valutazione finora
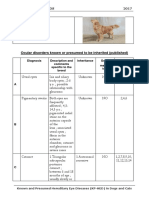
- GoldenretrieverDocumento6 pagineGoldenretrieverTobias-Andreas DietzelNessuna valutazione finora
- Abnormalities Protein Synthesis 2Documento7 pagineAbnormalities Protein Synthesis 2yori rafiadliNessuna valutazione finora
- Test Bank For Microbiology Basic and Clinical Principles 1st Edition Lourdes P Norman MckayDocumento36 pagineTest Bank For Microbiology Basic and Clinical Principles 1st Edition Lourdes P Norman Mckayshriekacericg31u3100% (43)
- BM Procedure and ProcessingDocumento28 pagineBM Procedure and ProcessingNidhi JaisNessuna valutazione finora
- New Study in Candida InfectionsDocumento3 pagineNew Study in Candida InfectionsHenz FreemanNessuna valutazione finora
- DOPR Vision 2030Documento36 pagineDOPR Vision 2030Hendi HendriansyahNessuna valutazione finora