Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
AFLP
Caricato da
saryindrianyCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
AFLP
Caricato da
saryindrianyCopyright:
Formati disponibili
ncy an
gna d
re
Nilanchali and Pragati, J Preg Child Health 2015, 2:4
Journal of P
Ch
Journal of Pregnancy and Child Health DOI: 10.4172/2376-127X.1000e118
ISSN: 2376-127X ild Health
Editorial
Research Article OpenAccess
Open Access
Acute Fatty Liver of Pregnancy: A Case Report and Literature Review
Nilanchali Singh* and Pragati Meena
Department of Obstetrics and Gynecology, University College of Medical Sciences and Guru Tegh Bahadur Hospital, Delhi, India
Abstract
Acute Fatty Liver of Pregnancy (AFLP) is a rare, catastrophic disease affecting women in pregnancy. It usually
occurs in the third trimester or post-partum period. It is usually a diagnosis of exclusion and a strong index of suspicion
can lead to timely diagnosis. Delay in diagnosis is associated with morbid complications with high mortality. We report
a case of 22 years old lady with 36 weeks pregnancy presented with malaise, nausea, vomiting and jaundice. A clinical
diagnosis of acute fatty liver of pregnancy was made. Although early Cesarean section was performed, postoperative
course was complicated by acute hepatic encephalopathy with hepatorenal shutdown and coagulopathy. Despite
intensive management in critical care, the patient expired.
Introduction Ultrasound abdomen showed normal liver and other organs.
Acute fatty liver of pregnancy (AFLP) affects 1 in 7000 to 1 in 16000 A differential diagnosis of AFLP, acute hepatitis, HELLP syndrome
deliveries [1,2]. There is predilection for nulliparous women, women was made. Viral markers (HBsAg, Anti-HCV, and Anti HAV) were
with multiple gestation and pregnancies with male fetus [3]. Maternal negative ruling out viral hepatitis. Her blood pressure was normal
mortality rate is estimated to be 12.5-18% with neonatal mortality rate throughout the hospital stay, ruling out gestational hypertension. There
of 7-66% [3]. was no evidence of hemolysis or thrombocytopenia (to rule out HELLP
syndrome). Persistent hypoglycemia despite correction aided towards
Diagnosing the etiology of jaundice is extremely important in diagnosis of AFLP. The patient was started on conservative management
pregnant patients as certain conditions like AFLP, HELLP syndrome with syrup lactulose, high carbohydrate diet and anti-coma regime.
and intra-hepatic cholestasis of pregnancy (ICP) may require early
termination of pregnancy even in the presence of jaundice and or Patient started deteriorating with rising liver enzymes and
coagulation failure [1]. On the contrary, in conditions like acute viral deteriorating coagulation profile despite correction with fresh frozen
hepatitis one must try to prolong pregnancy till the liver has recovered. plasma. She developed grade 1 hepatic encephalopathy. A decision
Thus, the maternal and fetal outcomes of pregnancy can significantly be for induction of labor was taken with informed written high risk
improved by appropriate management. However, differentiating these consent. She was induced with vaginal misoprostol (25 µgm 4 hourly).
conditions is difficult due to unpredictable and similar presentation and Amniotomy was done at 4 cm dilatation of cervix and the liquor was
laboratory investigations. Acute fatty liver of pregnancy is a rare but life blood stained and fetal heart rate showing bradycardia (90-100 bpm).
threatening cause of jaundice in the third trimester of pregnancy and Decision of emergency LSCS was taken after 18 hours of induction
early postpartum period. It has very high maternal and fetal morbidity in view of antepartum hemorrhage and fetal bradycardia. She was
and mortality, especially if it is complicated by coagulation failure. transfused with four units fresh frozen plasma and two units red cell
concentrate preoperatively. Emergency LSCS was done with informed
Case Report high risk consent. A live male child of 2 kg birth weight was delivered.
Intraoperative findings were normal and intraoperative period was
A 22 years old primigravida with 36 weeks period of gestation
uneventful. No significant retro-placental clot was noted and liquor
was referred from a peripheral hospital to our tertiary care center
was blood stained. Prophylactic Hayman’s suture with bilateral uterine
with complaints of yellow discoloration of urine and eyes, malaise,
artery ligation was done to prevent postpartum hemorrhage. An intra-
anorexia and vomiting since 3-4 days. She had no complaints of
peritoneal drain was put in. Transfusion with blood components was
pain abdomen, leaking or bleeding per vaginum or decreased fetal
given intra-operatively and postoperatively (4 unit FFP+ 4 unit platelet)
movement. There was no significant past history. On examination she
to correct coagulopathy. Patient was shifted to Intensive Care Unit in
was conscious, oriented to time, place and person, cooperative and
view of hepatic encephalopathy with coagulopathy with hepato-renal
responding appropriately to verbal commands. The patient was well
shut-down. Patient progressively deteriorated in post-operative period.
hydrated and afebrile. Her blood pressure was 120/84 mm Hg and
She became tachypneic and tachycardiac with increased abdominal
pulse rate was 84 per min. She had icterus and mild pedal edema. Her
distension and decreased urine output. She landed in Disseminated
cardiovascular and respiratory systems were normal on examination.
Abdominal examination revealed relaxed uterus of 36 weeks size,
with fetus in cephalic presentation and normal fetal heart rate. On
vaginal examination, it was closed and cervix uneffaced. Investigations *Corresponding author: Nilanchali Singh, Department of Obstetrics and
Gynecology, University College of Medical Sciences and Guru Tegh Bahadur
revealed hemoglobin of 12.4 g/dl, leucocyte count of 17,700/mm3and Hospital, Delhi, India, Tel: 919811343168; E-mail: nilanchalisingh@gmail.com
platelet count 1.5 lac/mm [3]. Her liver function test showed a serum
Received: June 25, 2015; Accepted: June 27, 2015; Published: June 30, 2015
bilirubin of 12.8 mg/dl, alanine aminotransferase 332 IU/l, aspartate
aminotransferase 210 IU/l, alkaline phosphatase 480 U/l, total proteins Citation: Singh N, Meena P (2015) Acute Fatty Liver of Pregnancy: A Case
5.6 g/dl, and albumin 2.4 g/dl. Kidney function tests revealed blood Report and Literature Review. J Preg Child Health 2: e118. doi:10.4172/2376-
127X.1000e118
urea 40 mg/dl, serum creatinine 1.7 mg/dl, random blood sugar 67 mg/
dl. The coagulation profile showed prothrombin time 52 seconds (12), Copyright: © 2015 Nilanchali S, et al. This is an open-access article distributed
under the terms of the Creative Commons Attribution License, which permits
a partial thromboplastintime >1 min (30) with INR 5.7. Random blood unrestricted use, distribution, and reproduction in any medium, provided the
glucose was 52 mg/dl. Blood gas analysis revealed metabolic acidosis. original author and source are credited.
J Preg Child Health
ISSN: 2376-127X JPCH, an open access journal Volume 2 • Issue 4 • 1000e118
Citation: Singh N, Meena P (2015) Acute Fatty Liver of Pregnancy: A Case Report and Literature Review. J Preg Child Health 2: e118. doi:10.4172/2376-
127X.1000e118
Page 2 of 3
Intravascular Coagulation. The drain output increased within first 24 third trimester of pregnancy, (iii) other associated organ derangements,
hour of LSCS (2500 ml). She had to be dialyzed in view of acute renal i.e., renal insufficiency, coagulopathy, hypoglycemia, and hepatic
failure and blood component therapy was given to correct coagulation encephalopathy, along with multiple organ dysfunction. Along with
profile. Patient was intubated and put on inotropes later on. Despite this these, other causes of jaundice need exclusion.
management, she deteriorated progressively and expired on fourth day.
The baby expired on fifth day due to birth asphyxia. Diagnosis
The diagnosis of AFLP is challenging and complicated. It is a diagnosis
Discussion
of exclusion. Specific investigations are lacking. The characteristic
It is well known that AFLP is neither inherited nor infectious [1]. diagnostic investigations reveal deranged liver functions, coagulopathy,
The precise etiology of AFLP is not known. It is thought to be due to hypoglycemia, deranged renal function tests, thrombocytopenia and
a mitochondrial dysfunction in the oxidation of fatty acids leading ultrasound imaging showing fatty liver. A specific criterion was devised
to an accumulation in hepatocytes. Fatty acid accumulation leads to diagnose this rare condition. Patients with at least six or more of
to hepatocyte dysfunction. The cause may be underlying fatty acid the Swansea criteria [15] confirm the diagnosis of AFLP: vomiting,
assimilation defects, which may be inherited. Women having AFLP abdominal pain, polydipsia/polyuria, encephalopathy, elevated serum
may have a heterozygous long-chain 3-hydroxyacyl-coenzyme-A- bilirubin level, elevated uric acid, hypoglycemia, leukocytosis, elevated
dehydrogenase (LCHAD) deficiency, which is found on mitochondrial transaminases, ascites or bright liver on ultrasound scan, elevated
membrane and is involved in the beta oxidation of long-chain fatty ammonia, renal impairment, coagulopathy, and microvesicularsteatosis
acids [4-9]. on liver biopsy in addition to metabolic acidosis and occasionally
biochemical pancreatitis.
Pregnancy with jaundice has many differential diagnoses like
cholestasis, viral hepatitis, pre-eclampsia with or without HELLP Management
syndrome, and AFLP. Intrahepatic cholestasis of pregnancy (IHCP) Management of AFLP comprises of rapid delivery of the fetus
usually occurs in the third trimester, is characterized by itching in palms and supportive care. There is no other definitive therapy. In most of
and soles mainly and serum bilirubin is mostly less than 6 mg/dl. Acute the cases, jaundice, liver dysfunction, and DIC improve after two to
viral hepatitis in pregnancy presents as a systemic illness with fever, three days of delivery [14]. Maternal and fetal mortality rates were
nausea, vomiting, fatigue, and jaundice, however, aminotransferase reported to be as high as 85% [16] earlier mostly due to cerebral edema,
concentrations are markedly elevated (>500 U/liter). All these causes gastrointestinal hemorrhage, renal failure, coagulopathy, and sepsis.
were ruled out in our case on the basis of presentation, symptoms, and However, mortality has been lowered now, to less than 10% due to
investigations. improvements in intensive care. Our patient presented rather late to
As discussed earlier, pre-eclampsia with deranged liver enzymes, us after the development of hepatic encephalopathy, acute renal failure,
HELLP syndrome, and AFLP have some distinct characteristics, DIC, and fetal demise. Although we performed an early caesarean
particularly with regard to time of presentation. However, they also have section, we were unable to interrupt the progression of the disease
some similarities in terms of clinical presentation and investigations. and her condition continued to deteriorate with serious complications
This makes differentiating these entities difficult [1,10,11]. The like ARDS, sepsis, and worsening coagulopathy [1]. It is not clear
incidence of HELLP syndrome is much higher (1:5,000) as compared whether ARDS occurred as a complication of acute liver failure (ALF),
to AFLP (1:13,000) [12]. The distinct features of AFLP include severe septicemia, or transfusion of multiple blood products, but it responded
coagulopathy, jaundice, hepatic encephalopathy, ascitis, hypoglycemia, to supportive therapy.
and an elevation of transaminase levels. Some of these features are
Conclusion
common to HELLP syndrome. In our case, the clinical features of
severe liver dysfunction appeared at the gestational age of 36 weeks. AFLP is a rare, life-threatening complication of pregnancy with
The symptoms initially mimicked those of acute hepatitis but clinical variable presentation, mostly in late pregnancy and post-partum
and laboratory evidence of severe coagulopathy, modest elevation of occasionally. The progression is rapid and unpredictable. Prompt
serum transaminase and bilirubin levels, hypoglycemia, an elevated diagnosis and management in the form of early delivery and intensive
ammonia value, and a low albumin level favored the diagnosis of AFLP care support may be life-saving. It is crucial to identify patients with
over HELLP syndrome. nausea, vomiting or epigastric pain and persistent jaundice in the third
trimester, to be suspected for the diagnosis of AFLP. The patients,
“Acute yellow atrophy of the liver,” a rare and fatal complication of who are critically ill at the time of clinical presentation, develop
pregnancy, was first described by Stander and Cadden in 1934 [4,6,13]. complications, or continue to deteriorate despite emergency delivery,
The liver biopsy is diagnostic but is not feasible in pregnant women and require collaborative management in the intensive care unit (ICU).
especially with severe coagulopathy. Moreover, the management Early diagnosis, prompt delivery, adequate supportive care, and a
remains same, hence, an unnecessary intervention. Ultrasound and multidisciplinary approach are the key to a good outcome.
computed tomography may be used to identify liver changes however;
References
these imaging studies too have low sensitivity and specificity [14]. In
our case, presence of coagulopathy did not allow us to perform liver 1. Bacq Y. The liver in pregnancy. In: Schiff ER, Sorrell MF, Schiff L, Maddrey WC,
biopsy. editors. Schiff’s Diseases of the liver (2006). 10th Edn Lippincott: Williams and
Wilkins (LWW) 1281–1304.
AFLP should be suspected in following conditions: (i) severe 2. Ch’ng CL, Morgan M, Hainsworth I, Kingham JG (2002) Prospective study of
gastrointestinal symptoms, i.e., nausea, vomiting, abdominal pain, liver dysfunction in pregnancy in Southwest Wales. Gut 51: 876-880.
polydipsia/polyuria, and persistent jaundice appearing in late pregnancy 3. Rajasri AG, Srestha R, Mitchell J (2007) Acute fatty liver of pregnancy (AFLP)-
(ii) abnormal liver function tests, leukocytosis and thrombocytopenia in An overview. J Obstet Gynaecol 27: 237-240.
J Preg Child Health
2376-127X JPCH, an open access journal Volume 2 • Issue 4 • 1000e118
Citation: Singh N, Meena P (2015) Acute Fatty Liver of Pregnancy: A Case Report and Literature Review. J Preg Child Health 2: e118. doi:10.4172/2376-
127X.1000e118
Page 3 of 3
4. Bhat RA, Kumar PN, Vyas NM (2006) Liver diseases complicating pregnancy. peripartum liver failure: A new perspective on the diagnosis, treatment, and
ObsGynae Today XI 8:437-40. cause of acute fatty liver of pregnancy, based on 28 consecutive cases. Am J
Obstet Gynecol 181: 389-395.
5. Mackillop L, Williamson C (2010) Liver disease in pregnancy. Postgrad Med J
86: 160-164. 11. Riely CA1 (1999) Liver disease in the pregnant patient. American College of
Gastroenterology. Am J Gastroenterol 94: 1728-1732.
6. McNulty J (2005) Acute fatty liver of pregnancy. In: Obst Intensive Care Manual.
Tata McGraw-Hill, New Delhi 207-215. 12. Pereira SP, O’Donohue J, Wendon J, Williams R (1997) Maternal and perinatal
outcome in severe pregnancy-related liver disease. Hepatology 26: 1258-1262.
7. Vora KS, Shah VR, Parikh GP (2009) Acute fatty liver of pregnancy: A case
report of an uncommon disease. Indian J Crit Care Med 13: 34-36. 13. Sheehan HL (1940) The pathology of acute yellow atrophy and delayed
chloroform poisoning. J ObstetGynaecol Br Emp 47: 49-62.
8. Bellig LL1 (2004) Maternal acute fatty liver of pregnancy and the associated risk
for long-chain 3-hydroxyacyl-coenzyme a dehydrogenase (LCHAD) deficiency 14. Usta IM, Barton JR, Amon EA, Gonzalez A, Sibai BM (1994) Acute fatty liver of
in infants. Adv Neonatal Care 4: 26-32. pregnancy: An experience in the diagnosis and management of fourteen cases.
Am J Obstet Gynecol 171: 1342-1347.
9. Yang Z, Yamada J, Zhao Y, Strauss AW, Ibdah JA (2002) Prospective screening
for paediatric mitochondrial tri functional protein defects in pregnancies 15. Joshi D, James A, Quaglia A, Westbrook RH, Heneghan MA (2010) Liver
complicated by liver disease. JAMA 288: 2163-2166. disease in pregnancy. Lancet 375: 594-605.
10. Castro MA, Fassett MJ, Reynolds TB, Shaw KJ, Goodwin TM (1999) Reversible 16. Kaplan MM (1985) Acute fatty liver of pregnancy. N Engl J Med 313: 367-370.
J Preg Child Health
2376-127X JPCH, an open access journal Volume 2 • Issue 4 • 1000e118
Potrebbero piacerti anche
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Acute Fatty Liver of Pregnancy: Letter To EditorDocumento2 pagineAcute Fatty Liver of Pregnancy: Letter To EditorsaryindrianyNessuna valutazione finora
- HELLP and AFLP PDFDocumento5 pagineHELLP and AFLP PDFDesyHandayaniNessuna valutazione finora
- ACG Clinical Guideline: Liver Disease and Pregnancy: Practice GuidelinesDocumento19 pagineACG Clinical Guideline: Liver Disease and Pregnancy: Practice GuidelinessaryindrianyNessuna valutazione finora
- Acute Fatty Liver of Pregnancy: Better Understanding of Pathogenesis and Earlier Clinical Recognition Results in Improved Maternal OutcomesDocumento8 pagineAcute Fatty Liver of Pregnancy: Better Understanding of Pathogenesis and Earlier Clinical Recognition Results in Improved Maternal OutcomessaryindrianyNessuna valutazione finora
- Nelson2013 Ajog PDFDocumento7 pagineNelson2013 Ajog PDFsaryindrianyNessuna valutazione finora
- Minakami 2014Documento9 pagineMinakami 2014saryindrianyNessuna valutazione finora
- Pregnancy-Related Liver Disorders: Seminar Journal of Clinical and Experimental HepatologyDocumento12 paginePregnancy-Related Liver Disorders: Seminar Journal of Clinical and Experimental HepatologysaryindrianyNessuna valutazione finora
- Acute Fatty Liver of Pregnancy: Better Understanding of Pathogenesis and Earlier Clinical Recognition Results in Improved Maternal OutcomesDocumento8 pagineAcute Fatty Liver of Pregnancy: Better Understanding of Pathogenesis and Earlier Clinical Recognition Results in Improved Maternal OutcomessaryindrianyNessuna valutazione finora
- Management Prior Cesarean DeliveryDocumento14 pagineManagement Prior Cesarean DeliveryAditya Arya PutraNessuna valutazione finora
- Induction of LaborDocumento124 pagineInduction of LaborFarah DinaNessuna valutazione finora
- Jastrow Et Al-2016-Ultrasound in ObstetricsDocumento6 pagineJastrow Et Al-2016-Ultrasound in ObstetricssaryindrianyNessuna valutazione finora
- Acog PB184 Vbac 2017 PDFDocumento17 pagineAcog PB184 Vbac 2017 PDFdwipaNessuna valutazione finora
- Birth After Previous Caesarean Section (C Obs 38) Re Write July 2015 1Documento27 pagineBirth After Previous Caesarean Section (C Obs 38) Re Write July 2015 1saryindrianyNessuna valutazione finora
- Why Obstetric Patients Are Admitted To Intensive Care Unit A Retrospective StudyDocumento3 pagineWhy Obstetric Patients Are Admitted To Intensive Care Unit A Retrospective StudysaryindrianyNessuna valutazione finora
- Causes and Management of Surgical Wound Dehiscence: Department of General SurgeryDocumento10 pagineCauses and Management of Surgical Wound Dehiscence: Department of General SurgerysaryindrianyNessuna valutazione finora
- VANCOUVER Reference GuideDocumento7 pagineVANCOUVER Reference GuideNoval FarlanNessuna valutazione finora
- 3881825Documento30 pagine3881825saryindrianyNessuna valutazione finora
- Risk Factors For Wound Dehiscence After Laparotomy - Clinical Control TrialDocumento9 pagineRisk Factors For Wound Dehiscence After Laparotomy - Clinical Control TrialsaryindrianyNessuna valutazione finora
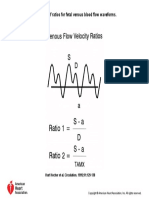
- Calculation of Ratios For Fetal Venous Blood Flow WaveformsDocumento1 paginaCalculation of Ratios For Fetal Venous Blood Flow WaveformssaryindrianyNessuna valutazione finora
- Partograph 1Documento22 paginePartograph 1SIRBENZNessuna valutazione finora
- Hiperemesis Gravidea PDFDocumento7 pagineHiperemesis Gravidea PDFFrank Luis Acosta MendozaNessuna valutazione finora
- Risk Factors For Wound Dehiscence After Laparotomy - Clinical Control TrialDocumento9 pagineRisk Factors For Wound Dehiscence After Laparotomy - Clinical Control TrialsaryindrianyNessuna valutazione finora
- Causes and Management of Surgical Wound Dehiscence: Department of General SurgeryDocumento10 pagineCauses and Management of Surgical Wound Dehiscence: Department of General SurgerysaryindrianyNessuna valutazione finora
- 1 s2.0 S0889854515001163Documento18 pagine1 s2.0 S0889854515001163saryindrianyNessuna valutazione finora
- Post Caesarean Surgical Site Infections 2Documento6 paginePost Caesarean Surgical Site Infections 2saryindrianyNessuna valutazione finora
- Renal Vein Doppler Ultrasound of Maternal KidneysDocumento5 pagineRenal Vein Doppler Ultrasound of Maternal KidneyssaryindrianyNessuna valutazione finora
- Keamanan Obat Bagi Ibu Hamil Berdasarkan Evidence BasedDocumento17 pagineKeamanan Obat Bagi Ibu Hamil Berdasarkan Evidence BasedJasonJejametNessuna valutazione finora
- Diagnosis and Management of Placenta PreviaDocumento6 pagineDiagnosis and Management of Placenta PreviaNoveno Semestre FmuaqNessuna valutazione finora
- Technical Series 2 Using PartographDocumento5 pagineTechnical Series 2 Using PartographsaryindrianyNessuna valutazione finora
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- P3 Chapter 2 End-Of-Chapter (Higher) Mark SchemeDocumento3 pagineP3 Chapter 2 End-Of-Chapter (Higher) Mark SchemePaul LloydNessuna valutazione finora
- Heating Ventilation Air Conditioning Hvac ManualDocumento4 pagineHeating Ventilation Air Conditioning Hvac ManualShabaz KhanNessuna valutazione finora
- Electro Acupuncture TherapyDocumento16 pagineElectro Acupuncture TherapyZA IDNessuna valutazione finora
- Registration of Hindu Marriage: A Project On Family Law-IDocumento22 pagineRegistration of Hindu Marriage: A Project On Family Law-Iamit dipankarNessuna valutazione finora
- 084 - ME8073, ME6004 Unconventional Machining Processes - NotesDocumento39 pagine084 - ME8073, ME6004 Unconventional Machining Processes - NotesA. AKASH 4001-UCE-TKNessuna valutazione finora
- Critique PaperDocumento1 paginaCritique PapernicolealerNessuna valutazione finora
- NG Uk RTR 0220 r15 PDFDocumento9 pagineNG Uk RTR 0220 r15 PDFDuong Thai BinhNessuna valutazione finora
- 2021 Physician Compensation Report - Updated 0821Documento24 pagine2021 Physician Compensation Report - Updated 0821Michael Knapp100% (3)
- OSCE Pediatric Dentistry Lecture-AnswersDocumento40 pagineOSCE Pediatric Dentistry Lecture-AnswersR MNessuna valutazione finora
- Beta CaroteneDocumento2 pagineBeta CaroteneValeria MarcuțăNessuna valutazione finora
- Dental Hygienist Learning Outcomes Form v1.2Documento32 pagineDental Hygienist Learning Outcomes Form v1.2Karman Deep Singh100% (1)
- 1635 The Papal Stakes - Eric FlintDocumento1.813 pagine1635 The Papal Stakes - Eric Flintwon100% (2)
- Ship Captain's Medical Guide - 22nd EdDocumento224 pagineShip Captain's Medical Guide - 22nd EdcelmailenesNessuna valutazione finora
- Solved Rail Chapter 1Documento7 pagineSolved Rail Chapter 1spectrum_48Nessuna valutazione finora
- Lesson Plan On Digestion in Stomach and Intestines Grade 4Documento3 pagineLesson Plan On Digestion in Stomach and Intestines Grade 4jaydalene saga macay100% (5)
- Technical Reference For Water Conservation in Cooling TowersDocumento41 pagineTechnical Reference For Water Conservation in Cooling TowersDorn GalamarNessuna valutazione finora
- Matriculation Chemistry Amino Acids-Part-1Documento24 pagineMatriculation Chemistry Amino Acids-Part-1iki292Nessuna valutazione finora
- Lithium Battery Handling RegulationDocumento11 pagineLithium Battery Handling RegulationFan Man ChungNessuna valutazione finora
- Hand-Pallet Truck - NewDocumento2 pagineHand-Pallet Truck - NewAkhilNessuna valutazione finora
- FPSB 2 (1) 56-62oDocumento7 pagineFPSB 2 (1) 56-62ojaouadi adelNessuna valutazione finora
- 5754 Almg3 5754 Almg3 Almg3 Almg3 5754 Almg3 Almg3 Almg3 Almg3Documento3 pagine5754 Almg3 5754 Almg3 Almg3 Almg3 5754 Almg3 Almg3 Almg3 Almg3InfoNessuna valutazione finora
- Elephantgrass Bookchapter PDFDocumento22 pagineElephantgrass Bookchapter PDFMuhammad rifayNessuna valutazione finora
- Cell Organelles 2Documento13 pagineCell Organelles 2Sadeeq ur RahmanNessuna valutazione finora
- Sikament®-4101 NS: Product Data SheetDocumento2 pagineSikament®-4101 NS: Product Data SheetShihab AhamedNessuna valutazione finora
- 50-Article Text-116-1-10-20191113Documento6 pagine50-Article Text-116-1-10-20191113Annisa FauziahNessuna valutazione finora
- Monopoly Tycoon TipsDocumento8 pagineMonopoly Tycoon TipsVictoria SmithNessuna valutazione finora
- PU-133AB - 規格GMXa spc 2022Documento5 paginePU-133AB - 規格GMXa spc 2022Ý TrầnNessuna valutazione finora
- High Voltage - WikipediaDocumento7 pagineHigh Voltage - WikipediaMasudRanaNessuna valutazione finora
- Extubation After Difficult IntubationDocumento3 pagineExtubation After Difficult Intubationramanrajesh83Nessuna valutazione finora
- From Crème Fraîche To Sour Cream: What's The Difference?Documento14 pagineFrom Crème Fraîche To Sour Cream: What's The Difference?Maricel BautistaNessuna valutazione finora