Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Adhf NCP
Caricato da
kristine keen buan0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
943 visualizzazioni3 pagineThe patient presented with shortness of breath, fatigue, and anxiety related to congestive heart failure. On examination, the patient had distant heart sounds, crackles, edema, and decreased oxygen saturation. The nursing diagnosis was ineffective breathing pattern related to decreased lung expansion from pulmonary congestion. The plan was for the patient to demonstrate improved breathing techniques and decrease respiratory rate with nursing interventions over 8 hours. Goals were met as breathing and vital signs improved with rest, positioning, relaxation techniques,
Descrizione originale:
NCP for acute decompensated heart failure
Titolo originale
ADHF-NCP
Copyright
© © All Rights Reserved
Formati disponibili
DOCX, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoThe patient presented with shortness of breath, fatigue, and anxiety related to congestive heart failure. On examination, the patient had distant heart sounds, crackles, edema, and decreased oxygen saturation. The nursing diagnosis was ineffective breathing pattern related to decreased lung expansion from pulmonary congestion. The plan was for the patient to demonstrate improved breathing techniques and decrease respiratory rate with nursing interventions over 8 hours. Goals were met as breathing and vital signs improved with rest, positioning, relaxation techniques,
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato DOCX, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
943 visualizzazioni3 pagineAdhf NCP
Caricato da
kristine keen buanThe patient presented with shortness of breath, fatigue, and anxiety related to congestive heart failure. On examination, the patient had distant heart sounds, crackles, edema, and decreased oxygen saturation. The nursing diagnosis was ineffective breathing pattern related to decreased lung expansion from pulmonary congestion. The plan was for the patient to demonstrate improved breathing techniques and decrease respiratory rate with nursing interventions over 8 hours. Goals were met as breathing and vital signs improved with rest, positioning, relaxation techniques,
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato DOCX, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 3
ASSESSMENT NSG. DIAGNOSIS PLANNING NSG.
INTERVENTION RATIONALE EVALUATION
SUBJECTIVE: Independent STG:
Ineffective breathing STG: After 1hr of nursing Note heart sounds. S1 and S2 may be weak After 1 hr. of nursing
“Is very anxious pattern related to fatigue intervention the patient because of diminished intervention the patient
and ask, “Am I and decreased lung will be able demonstrate 3 pumping action. Gallop was able to demonstrate 3
going to die?” expansion and pulmonary out of 5 procedures to rythms are common(S3 out 5 ways to improve
Denies pain but congestion secondary to improve breathing pattern and S4), produced as breathing pattern.
says that he feels CHF. blood flows into
like he cannot get LTG: After 8hrs of nursing noncompliant chambers. GOAL MET
enough air intervention the Patient’s
Says that his heart respiratory pattern will Palpate peripheral pulses ↓CO may be reflected in LTG:
feels like it is decrease from 34 to 28 diminished radial, After 8 hrs. of nursing
“running away” cpm without exertion. popliteal, dorsalis pedis, intervention the patient’s
After being and post tibial pulses respiratory pattern was
weighed, he decreased from 34-28
reports, “that is Monitor BP In advanced HF, the body cpm without exertion.
more than I may no longer be able to
usually weigh” compensate, and GOAL MET
Reports that he is profound hypotension may
so exhausted he occur.
can’t eat or drink
by himself Inspect for pallor or Pallor is indicative of
Objective Data cyanosis diminished peripheral
Height: 175 cm perfusion secondary to
Weight: 95.5kg inadequate CO,
Temp: 37.6 vasoconstriction, and
HR: 34 anemia. Cyanosis may
118bpm develop in refractory HF.
BP: 90/60 Dependent area are often
blue or mottled as venous
Distant S1, S2,
congestion increases.
S3, S4 present,
Monitor UO Kidneys respond to
PMI at 6th ICS and
reduced CO by retaining
faint water and sodium
(+) atrial fibrillation Note changes in May indicate inadequate
sensorium, lethargy, cerebral perfuaion
with ventricular
confusion, disorientation, secondary to decreased
rate of 132pbm anxiety, and depression CO.
(+)crackles, Monitor oxygen saturation Provides information
↓breath sounds and ABGs. regarding the heart’s
ability to perfuse distal
RLL, +(frothy tubules with oxygenated
blood-tinged blood.
sputum) Encourage patient of rest Reduces cardiac workload
SpO2- 82% on and assist with all and minimizes myocardial
activities oxygen consumption
room air
(+) bowel sounds Assist the patient in Allows for better chest
assuming a high fowler’s expansion, thereby
Hepatomegaly position improving pulmonary
(4cm below costal capacity.
margin) Assist patient to use Identifies increased work
Bilateral JVD relaxation techniques of breathing
1+ peripheral Weigh patient daily and Body weight is a sensitive
compare to previous indicator of fluid balance
pulses and (+)
weights and an increase indicates
peripheral edema fluid volume excess.
Dependent:
Administer supplemental Increases available
oxygen as indicated oxygen for myocardial
uptake to combat effects
of hypoxia
Administer medications as To improve patient
indicated. condition
Interdependent:
Monitor laboratory results For early detection on
abnormal changes in body
function.
Potrebbero piacerti anche
- NCP 1Documento1 paginaNCP 1hsiriaNessuna valutazione finora
- NCP Acitivity IntoleranceDocumento3 pagineNCP Acitivity IntolerancegizelleNessuna valutazione finora
- NCPDocumento2 pagineNCPsphinx809100% (2)
- Nursing Care Plan: Date/ Time Assessment Nursing Diagnosis Planning Intervention Evaluatio NDocumento2 pagineNursing Care Plan: Date/ Time Assessment Nursing Diagnosis Planning Intervention Evaluatio NnananaNessuna valutazione finora
- Assessment Objectives: "Masakit Lagi Yung Lalamunan NyaDocumento3 pagineAssessment Objectives: "Masakit Lagi Yung Lalamunan Nyaangel_pearl413100% (2)
- Gastrectomy NCP IBPDocumento3 pagineGastrectomy NCP IBPKevin T. Katada100% (1)
- NCP HemoDocumento2 pagineNCP HemoJigs HechNessuna valutazione finora
- Risk For InfectionDocumento1 paginaRisk For InfectionEuanne OrellanoNessuna valutazione finora
- Ineffective Breathing Pattern As Evidenced by Use of Accessory Muscles and Episodes of DyspneaDocumento3 pagineIneffective Breathing Pattern As Evidenced by Use of Accessory Muscles and Episodes of DyspneaNiel MinatozakiNessuna valutazione finora
- 6 Pleural Effusion Nursing Care PlansDocumento7 pagine6 Pleural Effusion Nursing Care PlansShaina Fe RabaneraNessuna valutazione finora
- NCPDocumento11 pagineNCPPatricia VasquezNessuna valutazione finora
- NCPDocumento9 pagineNCPTracy Camille EscobarNessuna valutazione finora
- Fluid Volume DeficitDocumento2 pagineFluid Volume DeficitRuby AnneNessuna valutazione finora
- Goboy - Risk For Infection NCPDocumento3 pagineGoboy - Risk For Infection NCPLouise GermaineNessuna valutazione finora
- NCP HemothoraxDocumento3 pagineNCP Hemothoraxroseonabreeze0% (2)
- NCPDocumento2 pagineNCPDidith AbanNessuna valutazione finora
- Final NCP LeptospirosisDocumento6 pagineFinal NCP LeptospirosisKeith Austin100% (1)
- NCPDocumento4 pagineNCPMark Benedict Ocampo VelardeNessuna valutazione finora
- NURSING CARE PLAN Problem Body Weakness Nursing Diagnosis Impaired PhysicalDocumento1 paginaNURSING CARE PLAN Problem Body Weakness Nursing Diagnosis Impaired Physicalmitchie riveraNessuna valutazione finora
- NCP Acute PainDocumento3 pagineNCP Acute PainSheene Lysethea Sioteco AguilosNessuna valutazione finora
- Nursing Care PlanDocumento2 pagineNursing Care PlanAldrein GonzalesNessuna valutazione finora
- NCP Activity IntoleranceDocumento5 pagineNCP Activity IntoleranceRea HashimNessuna valutazione finora
- Cholecystectomy Nursing Care Plan: Intraoperative Problem: Risk For AspirationDocumento1 paginaCholecystectomy Nursing Care Plan: Intraoperative Problem: Risk For AspirationJess GoNessuna valutazione finora
- NCP Activity Intolerance Related To Decreased in Oxygen SupplyDocumento3 pagineNCP Activity Intolerance Related To Decreased in Oxygen SupplyKyle Stephen TancioNessuna valutazione finora
- Nursing Care Plan: Pulmonary EbolismDocumento5 pagineNursing Care Plan: Pulmonary EbolismneuronurseNessuna valutazione finora
- Compartment Syndrome NCP (PAIN)Documento2 pagineCompartment Syndrome NCP (PAIN)eunica16Nessuna valutazione finora
- Hyperthermia NCPDocumento2 pagineHyperthermia NCPSian AsadaNessuna valutazione finora
- NCP For COLON Cancer PatientDocumento4 pagineNCP For COLON Cancer PatientCarolina Tardecilla100% (1)
- Nursing Care Plan: Fluid Volume DeficitDocumento2 pagineNursing Care Plan: Fluid Volume DeficitGenEsis CarandangNessuna valutazione finora
- Case Scenario (Pedia)Documento2 pagineCase Scenario (Pedia)Hamima Azis PandapatanNessuna valutazione finora
- NCP: Acute GastroenteritisDocumento3 pagineNCP: Acute GastroenteritishauteanicoleNessuna valutazione finora
- NCP For SVTDocumento6 pagineNCP For SVTRen VillenaNessuna valutazione finora
- NCP - Excess Fluid Volume Related Compromised Regulatory Mechanism (Renal Failure) (Acute Renal Failure)Documento3 pagineNCP - Excess Fluid Volume Related Compromised Regulatory Mechanism (Renal Failure) (Acute Renal Failure)Kian Herrera100% (1)
- Nursingcrib Com NURSING CARE PLAN Hepatitis A PDFDocumento2 pagineNursingcrib Com NURSING CARE PLAN Hepatitis A PDFswapnilazarusNessuna valutazione finora
- Acute Pain Related To Inflammation of Tissues Secondary To AppendicitisDocumento2 pagineAcute Pain Related To Inflammation of Tissues Secondary To AppendicitisRachel SaavedraNessuna valutazione finora
- NCPDocumento3 pagineNCPJezza RequilmeNessuna valutazione finora
- Acute Pain Related To Tissue Trauma and InjuryDocumento4 pagineAcute Pain Related To Tissue Trauma and Injuryprickybiik50% (2)
- Impaired Skin IntegrityDocumento3 pagineImpaired Skin IntegrityAubrey SungaNessuna valutazione finora
- NCP For StrokeDocumento4 pagineNCP For StrokeJASON OGALESCONessuna valutazione finora
- Risk For InjuryDocumento4 pagineRisk For InjuryKatrina Denise TolentinoNessuna valutazione finora
- NCP Lack of KnowledgeDocumento3 pagineNCP Lack of KnowledgeFaye BartianaNessuna valutazione finora
- Assesment Diagnosis Planning Interventio N Rationale EvaluationDocumento2 pagineAssesment Diagnosis Planning Interventio N Rationale EvaluationRenea Joy ArruejoNessuna valutazione finora
- Word Ncp.......... TetanusDocumento3 pagineWord Ncp.......... TetanusYvounne Ananias Bautista RNNessuna valutazione finora
- Nursing Care Plan BalnkDocumento2 pagineNursing Care Plan BalnkKateLayaogNessuna valutazione finora
- Thyroidectomy NCPDocumento3 pagineThyroidectomy NCPKim Enrico Jumarang100% (2)
- Body Weakness NCPDocumento1 paginaBody Weakness NCPtwicetrashNessuna valutazione finora
- Decreased Cardiac Output Related To Decreased Myocardial Contractility Secondary To CardiomyopathyDocumento2 pagineDecreased Cardiac Output Related To Decreased Myocardial Contractility Secondary To CardiomyopathySoniaMarieBalanayNessuna valutazione finora
- Ineffective Breathing PatternDocumento8 pagineIneffective Breathing PatternJansen Arquilita Rivera100% (2)
- NCP For CTTDocumento1 paginaNCP For CTTJen Rhae LimNessuna valutazione finora
- Nursing Care Plan For RabiesDocumento1 paginaNursing Care Plan For RabiesAngel VillamorNessuna valutazione finora
- NCP For Ruptured AppendicitisDocumento2 pagineNCP For Ruptured AppendicitisJansen Arquilita RiveraNessuna valutazione finora
- NCP LatestDocumento6 pagineNCP LatestThirdy AquinoNessuna valutazione finora
- Case Study On Children With Cardiac DisordersDocumento3 pagineCase Study On Children With Cardiac DisordersAlyNessuna valutazione finora
- 2 NCP Chronic Heart FailureDocumento5 pagine2 NCP Chronic Heart FailureLovely CacapitNessuna valutazione finora
- Afib NCPDocumento3 pagineAfib NCPGen RodriguezNessuna valutazione finora
- CHF NCPDocumento8 pagineCHF NCPZy Hallasgo100% (1)
- Diana Kyla A. Punay Bsn-Dash-6: Subjective Data: Short Term: Short TermDocumento3 pagineDiana Kyla A. Punay Bsn-Dash-6: Subjective Data: Short Term: Short TermZoè AshtrönNessuna valutazione finora
- Excess or Deficit in Oxygenation And/or Carbon Dioxide Elimination at The Alveolar-Capillary MembraneDocumento6 pagineExcess or Deficit in Oxygenation And/or Carbon Dioxide Elimination at The Alveolar-Capillary MembraneHazel MiraranNessuna valutazione finora
- Icu 4Documento7 pagineIcu 4GemilleDaphneAndradaNessuna valutazione finora
- AssessmentDocumento2 pagineAssessmentHazel MiraranNessuna valutazione finora
- Inflammation TASK 1. Briefly Discuss The Three Divisions of Immunity and Its Relationship To One AnotherDocumento5 pagineInflammation TASK 1. Briefly Discuss The Three Divisions of Immunity and Its Relationship To One Anotherkristine keen buanNessuna valutazione finora
- Task 1. Concept Analysis and DiagramDocumento4 pagineTask 1. Concept Analysis and Diagramkristine keen buanNessuna valutazione finora
- Acute Pancreatitis Case PresDocumento29 pagineAcute Pancreatitis Case Preskristine keen buanNessuna valutazione finora
- HIS 101-Presidents PDFDocumento12 pagineHIS 101-Presidents PDFkristine keen buanNessuna valutazione finora
- Suici DE: By: Kristine Keen BuanDocumento57 pagineSuici DE: By: Kristine Keen Buankristine keen buanNessuna valutazione finora
- Case Study - Ectopic PregnancyDocumento10 pagineCase Study - Ectopic Pregnancykristine keen buanNessuna valutazione finora
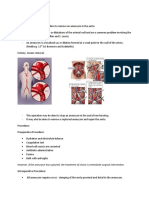
- However, If The Aneurysm Has Ruptured, The Treatment of Choice Is Immediate Surgical InterventionDocumento4 pagineHowever, If The Aneurysm Has Ruptured, The Treatment of Choice Is Immediate Surgical Interventionkristine keen buanNessuna valutazione finora
- HypoglycaemiaDocumento3 pagineHypoglycaemiakristine keen buanNessuna valutazione finora
- Care of The Newborn 1219399928791425 9Documento167 pagineCare of The Newborn 1219399928791425 9kristine keen buanNessuna valutazione finora
- Management of Patientswith Complications From Heart DiseaseDocumento8 pagineManagement of Patientswith Complications From Heart Diseasekristine keen buanNessuna valutazione finora
- 2 - Pizeo Electric SensorDocumento33 pagine2 - Pizeo Electric SensorNesamaniNessuna valutazione finora
- Starters Flash CardsDocumento28 pagineStarters Flash CardsNara GarridoNessuna valutazione finora
- Chemrite SP 200Documento3 pagineChemrite SP 200ghazanfarNessuna valutazione finora
- On How To Design A Low Voltage SwitchboardDocumento11 pagineOn How To Design A Low Voltage SwitchboardsabeerNessuna valutazione finora
- Oral Rehydration SolutionDocumento22 pagineOral Rehydration SolutionAlkaNessuna valutazione finora
- Qualitative Tests Organic NotesDocumento5 pagineQualitative Tests Organic NotesAdorned. pearlNessuna valutazione finora
- 3 14 Revision Guide Organic SynthesisDocumento6 pagine3 14 Revision Guide Organic SynthesisCin D NgNessuna valutazione finora
- Sampoong Department Store - A Literary Critique (Mimetic Theory)Documento2 pagineSampoong Department Store - A Literary Critique (Mimetic Theory)Ron Marc CaneteNessuna valutazione finora
- Material: Safety Data SheetDocumento3 pagineMaterial: Safety Data SheetMichael JoudalNessuna valutazione finora
- G.R. No. 94523 ST - Theresita's Academy vs. NLRCDocumento3 pagineG.R. No. 94523 ST - Theresita's Academy vs. NLRCyetyetNessuna valutazione finora
- KL 4 Unit 6 TestDocumento3 pagineKL 4 Unit 6 TestMaciej Koififg0% (1)
- ESR 2538 ChemofastDocumento14 pagineESR 2538 ChemofastEduardo Antonio Duran SepulvedaNessuna valutazione finora
- CASE 721F TIER 4 WHEEL LOADER Operator's Manual PDFDocumento17 pagineCASE 721F TIER 4 WHEEL LOADER Operator's Manual PDFfjskedmmsme0% (4)
- EE2401 Power System Operation and ControlDocumento93 pagineEE2401 Power System Operation and ControlPrasanth GovindarajNessuna valutazione finora
- Report Text: General ClassificationDocumento7 pagineReport Text: General Classificationrisky armala syahraniNessuna valutazione finora
- OBESITY - Cayce Health DatabaseDocumento4 pagineOBESITY - Cayce Health Databasewcwjr55Nessuna valutazione finora
- Internationalresidential Code 2009 Edition Fuel Gas SectionDocumento49 pagineInternationalresidential Code 2009 Edition Fuel Gas SectionZarex BorjaNessuna valutazione finora
- Alternative ObligationsDocumento42 pagineAlternative ObligationsJanella Gail FerrerNessuna valutazione finora
- PYMS Is A Reliable Malnutrition Screening ToolsDocumento8 paginePYMS Is A Reliable Malnutrition Screening ToolsRika LedyNessuna valutazione finora
- Course Weekly Schedule Health Science TheoryDocumento6 pagineCourse Weekly Schedule Health Science Theoryapi-466810096Nessuna valutazione finora
- DIP Lecture1Documento12 pagineDIP Lecture1Manish SandilyaNessuna valutazione finora
- Science 7 - Q2 - M7Documento16 pagineScience 7 - Q2 - M7RAMOS ERLYN P.Nessuna valutazione finora
- The Human Body: An Orientation: Part ADocumento10 pagineThe Human Body: An Orientation: Part ARoi Christoffer Jocson PeraltaNessuna valutazione finora
- Ne XT ProtDocumento2 pagineNe XT Protwilliam919Nessuna valutazione finora
- Chemistry DemosDocumento170 pagineChemistry DemosStacey BensonNessuna valutazione finora
- Governance StructureDocumento1 paginaGovernance StructureJoydip MukhopadhyayNessuna valutazione finora
- TCM Reach TrucksDocumento5 pagineTCM Reach TrucksMuhammad SohailNessuna valutazione finora
- Ams - 4640-C63000 Aluminium Nickel MNDocumento3 pagineAms - 4640-C63000 Aluminium Nickel MNOrnella MancinelliNessuna valutazione finora