Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Pathoma Ch06 WBC
Caricato da
kikocornholio0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
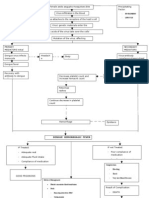
61 visualizzazioni16 pagineHematopoiesis occurs via the stepwise maturation of CD34+ hematopoietic stem cells which can differentiate into myeloid or lymphoid stem cells. Myeloid stem cells can mature into red blood cells, granulocytes, monocytes, or megakaryocytes. Lymphoid stem cells can mature into B or T lymphocytes. Neutropenia refers to a decreased number of circulating neutrophils and can result from chemotherapy, infection, or aplastic anemia. Acute leukemia is defined as over 20% blasts in the bone marrow and is classified as either acute lymphoblastic leukemia (ALL) or acute myelogenous leukemia (AML) based on the phenotype of the
Descrizione originale:
Pathoma Ch06 WBC flashcard notes
Copyright
© © All Rights Reserved
Formati disponibili
TXT, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoHematopoiesis occurs via the stepwise maturation of CD34+ hematopoietic stem cells which can differentiate into myeloid or lymphoid stem cells. Myeloid stem cells can mature into red blood cells, granulocytes, monocytes, or megakaryocytes. Lymphoid stem cells can mature into B or T lymphocytes. Neutropenia refers to a decreased number of circulating neutrophils and can result from chemotherapy, infection, or aplastic anemia. Acute leukemia is defined as over 20% blasts in the bone marrow and is classified as either acute lymphoblastic leukemia (ALL) or acute myelogenous leukemia (AML) based on the phenotype of the
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato TXT, PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
61 visualizzazioni16 paginePathoma Ch06 WBC
Caricato da
kikocornholioHematopoiesis occurs via the stepwise maturation of CD34+ hematopoietic stem cells which can differentiate into myeloid or lymphoid stem cells. Myeloid stem cells can mature into red blood cells, granulocytes, monocytes, or megakaryocytes. Lymphoid stem cells can mature into B or T lymphocytes. Neutropenia refers to a decreased number of circulating neutrophils and can result from chemotherapy, infection, or aplastic anemia. Acute leukemia is defined as over 20% blasts in the bone marrow and is classified as either acute lymphoblastic leukemia (ALL) or acute myelogenous leukemia (AML) based on the phenotype of the
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato TXT, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 16
Hematopoiesis occurs via a stepwise maturation of CD-{{c1::34}}+ hematopoietic stem
cells PathomaWBC WBC
The CD34+ hematopoietic stem cell may differentiate into a {{c1::myeloid}} or
{{c2::lymphoid}} stem cell PathomaWBC WBC
Myeloid stem cells may differentiate into {{c1::erythroblasts}}, which mature into
RBCs PathomaWBC WBC
Myeloid stem cells may differentiate into {{c1::myeloblasts}}, which mature into
granulocytes e.g. neutrophils, basophils, eosinophils PathomaWBC WBC
Myeloid stem cells may differentiate into {{c1::monoblasts}}, which mature into
monocytes PathomaWBC WBC
Myeloid stem cells may differentiate into {{c1::megakaryoblasts}}, which mature
into megakaryocytes PathomaWBC WBC
Lymphoid stem cells may differentiate into {{c1::B lymphoblasts}}, which mature
into naive B cells and then plasma cells PathomaWBC WBC
Lymphoid stem cells may differentiate into {{c1::T lymphoblasts}}, which mature
into naive T cells and then CD4+/CD8+ T cells PathomaWBC WBC
A normal WBC count is approximately {{c1::5}} - {{c1::10}} K/μL PathomaWBC
WBC
A low WBC count (< 5K) is called {{c1::leukopenia}} PathomaWBC WBC
A high WBC count (> 10K) is called {{c1::leukocytosis}} PathomaWBC WBC
{{c1::Neutropenia}} refers to a decreased number of circulating neutrophils
absolute neutrophil count < 1500 cells/mm3 PathomaWBC WBC
Neutropenia may result from drug toxicity, especially {{c1::chemotherapy}} damage
to stem cells results in decreased production of WBCs, especially neutrophils
PathomaWBC WBC
Neutropenia may result from severe {{c1::infection (e.g. gram-negative sepsis)}}
inceased movement of neutrophils into tissues results in decreased
circulating neutrophils PathomaWBC WBC
In addition to drugs and infection, neutropenia also occurs with {{c1::aplastic}}
anemia, SLE, and radiation PathomaWBC WBC
What treatments (2) are used to boost granulocyte production and thus decrease risk
of infection in neutropenic patients? {{c1::GM-CSF or G-CSF}} severe infections
typically occur when < 500 cells/mm3 PathomaWBC WBC
{{c1::Lymphopenia}} refers to a decreased number of circulating lymphocytes
PathomaWBC WBC
Lymphopenia may be caused by {{c1::immunodeficiency}} (e.g. HIV, DiGeorge syndrome,
SCID) PathomaWBC WBC
Lymphopenia may occur due to a high {{c1::cortisol}} state, which induces apoptosis
of lymphocytes e.g. exogenous corticosteroids or Cushing syndrome PathomaWBC
S2B3 WBC
What is the effect of corticosteroids on lymphocyte levels? {{c1::Decreased
(lymphopenia)}} PathomaWBC S2B3 WBC
Lymphopenia may occur due to {{c1::autoimmune}} destruction (e.g. SLE)
PathomaWBC WBC
Lymphopenia may occur with whole body {{c1::radiation}} lymphopenia is the
earliest change to emerge after whole body radiation PathomaWBC WBC
Which type of WBC is the most sensitive to radiation? {{c1::Lymphocytes}}
PathomaWBC WBC
{{c1::Eosinopenia}} refers to a decreased number of circulating eosinophils
absolute eosinophil count < 30 cells/mm3 PathomaWBC WBC
What is the effect of corticosteroids on eosinophil levels? {{c1::Decreased
(eosinopenia)}} also seen with Cushing syndrome; corticosteroids sequester
eosinophils in lymph nodes PathomaWBC S2B3 WBC
{{c1::Neutrophilia}} refers to an increased number of circulating neutrophils
PathomaWBC WBC
A {{c1::left}} shift is an increase in neutrophil precursors, such as band cells
and metamyelocytes, in peripheral blood PathomaWBC WBC
Left shifts are usually seen with neutrophilia in the acute response to
{{c1::bacterial infection}} or {{c2::tissue necrosis}} PathomaWBC WBC
When a left shift is seen with immature RBCs it is called a
{{c1::leukoerythroblastic}} reaction occurs with severe anemia (physiologic
response) or marrow response (e.g. fibrosis, tumor taking up space in marrow)
PathomaWBC WBC
Immature neutrophils (e.g. left shift) are characterized by decreased {{c1::Fc}}
receptors (CD-{{c2::16}}) therefore immature neutrophils don't function as well
PathomaWBC WBC
What is the effect of corticosteroids on neutrophil levels? {{c1::Increased
(neutrophilia)}} high cortisol state impairs leukocyte adhesion, leading to
release of marginated pool of neutrophils PathomaWBC S2B3 WBC
Monocytosis (increased monocytes) is seen with chronic {{c1::inflammatory}} states
and {{c2::malignancy}} PathomaWBC WBC
{{c1::Lymphocytosis}} refers to an increased number of circulating lymphocytes
PathomaWBC WBC
Lymphocytosis often occurs in response to {{c1::viral}} infections T
lymphocytes undergo hyperplasia in response to virally infected cells PathomaWBC
WBC
What bacteria causes lymphocytosis via production of lymphocytosis-promoting
factor? {{c1::Bordetella pertussis}} blocks circulating lymphocytes from
leaving the blood to enter the lymph node PathomaWBC WBC
Infectious mononucleosis most commonly occurs due to an {{c1::EBV}} infection
PathomaWBC WBC
Infectious mononucleosis less commonly occurs due to a {{c1::CMV}} infection
PathomaWBC WBC
"Epstein-Barr virus (EBV) is transmitted by {{c1::saliva (""kissing disease"")}}"
PathomaWBC WBC
What demographic (age group) is associated with infectious mononucleosis due to EBV
infection? {{c1::Teenagers}} PathomaWBC WBC
Epstein-Barr virus (EBV) primarily infects the {{c1::oropharynx}}, {{c2::liver}},
and {{c3::B cells}} causes pharyngitis, hepatitis with hepatomegaly, and
elevated liver enzymes PathomaWBC WBC
EBV infection results in lymphocytosis comprised of reactive CD{{c1::8}}+ T cells
PathomaWBC WBC
The CD8+ T-cell response in infectious mononucleosis leads to lymphadenopathy,
especially in the {{c1::posterior cervical}} nodes PathomaWBC WBC
The lymphadenopathy seen with infectious mononucleosis is due to T-cell hyperplasia
in the lymph node {{c1::paracortex}} PathomaWBC WBC
The CD8+ T-cell response in EBV infection leads to {{c1::spleno}}-megaly
PathomaWBC WBC
The splenomegaly seen with infectious mononucleosis is due to T-cell hyperplasia in
the {{c1::periarterial lymphatic sheath (PALS)}} of the spleen PathomaWBC
WBC
What abnormal cell (seen on blood smear) is associated with infectious
mononucleosis? {{c1::Atypical lymphocytes (reactive CD8+ T-cells)}}
PathomaWBC WBC
What test is used to screen for infectious mononucleosis? {{c1::Monospot test}}
PathomaWBC WBC
The {{c2::monospot}} test detects IgM {{c1::heterophile}} antibodies that cross-
react with horse or sheep RBCs usually turns positive within 1 week after EBV
infection; may be negative with infectious mononucleosis due to CMV PathomaWBC
WBC
A {{c2::negative}} monospot test with symptoms of infectious mononucleosis suggests
{{c1::CMV}} infection PathomaWBC WBC
A definitive diagnosis of infectious mononucleosis is made by serologic testing for
the EBV {{c1::viral capsid}} antigen PathomaWBC WBC
Infectious mononucleosis is associated with increased risk for {{c1::splenic}}
rupture PathomaWBC WBC
Patients with infectious mononucleosis are advised to avoid {{c1::contact sports}}
for one month due to risk of splenic rupture PathomaWBC WBC
Infectious {{c3::mononucleosis}} patients develop a {{c1::rash}} if exposed to
{{c2::ampicillin}} PathomaWBC WBC
Epstein-Barr virus (EBV) remains dormant in {{c1::B}} cells, which increases risk
for {{c2::lymphoma}}, especially if immunodeficiency develops (e.g. HIV)
PathomaWBC WBC
Acute leukemia is defined as a neoplastic proliferation of blasts {{c1::> 20}}% in
the bone marrow PathomaWBC WBC acute_leukemia
Acute leukemia may present acutely with symptoms of {{c1::anemia}},
{{c2::thrombocytopenia}}, and/or {{c3::neutropenia}} e.g. fatigue, bleeding,
infection PathomaWBC WBC acute_leukemia
Acute leukemias are typically associated with {{c1::increased}} circulating WBCs
rare cases present with normal or decreased WBCs PathomaWBC WBC
acute_leukemia
"The blasts seen in acute leukemia are {{c2::large}} (size), immature cells, often
with ""punched out"" {{c1::nucleoli}}" acute_leukemia PathomaWBC WBC
Acute leukemia is subdivided into {{c1::ALL}} or {{c1::AML}} based on the phenotype
of the blasts PathomaWBC WBC acute_leukemia
ALL is a neoplastic accumulation of {{c1::lymphoblasts}} (>20%) in the bone marrow
i.e. acute lymphoblastic leukemia PathomaWBC WBC acute_leukemia
{{c2::Lympho}}-blasts are characterized by positive nuclear staining for
{{c1::TdT}}, which is a {{c3::DNA polymerase}} marker of pre-T and pre-B cells;
absent in myeloid blasts and mature blasts PathomaWBC WBC acute_leukemia
What demographic (age group) is most commonly associated with acute lymphoblastic
leukemia (ALL)? {{c1::Children}} PathomaWBC WBC acute_leukemia
{{c3::Acute lymphoblastic}} leukemia is associated with {{c1::Down}} syndrome;
usually arises {{c2::after}} the age of 5 years PathomaWBC WBC acute_leukemia
Acute lymphoblastic leukemia is subclassified into {{c1::B}}-ALL and {{c1::T}}-ALL
based on surface markers PathomaWBC WBC acute_leukemia
Which type of ALL (B- or T-ALL) is the most common? {{c1::B-ALL}}
PathomaWBC WBC acute_leukemia
B-ALL is usually characterized by lymphoblasts (TdT+) that express CD-{{c1::10}},
CD-{{c1::19}}, and CD-{{c1::20}} CD10 is a marker of pre-B cells; negative in T-
ALL PathomaWBC WBC acute_leukemia
B-ALL has a(n) {{c1::excellent}} response to chemotherapy PathomaWBC WBC
acute_leukemia
Treatment of B-ALL requires prophylaxis to the {{c1::scrotum}} and {{c2::CSF}}
chemotherapy doesn't pass the blood-brain or blood-testis barrier
PathomaWBC WBC acute_leukemia
B-ALL with t({{c3::12}};{{c3::21}}) has a {{c1::good}} prognosis and is more
commonly seen in {{c2::children}} PathomaWBC WBC acute_leukemia
B-ALL with t({{c3::9}};{{c3::22}}) has a {{c1::poor}} prognosis and is more
commonly seen in {{c2::adults}} (age group) Philadelphia+ ALL acute_leukemia
PathomaWBC WBC
T-ALL is characterized by lymphoblasts (TdT+) that express markers ranging from CD-
{{c1::2}} to CD-{{c1::8}} PathomaWBC WBC acute_leukemia
Do the lymphoblasts in T-ALL express CD10? {{c1::No}} important distinguishing
feature from B-ALL PathomaWBC WBC acute_leukemia
{{c3::T}}-ALL usually presents in {{c1::teenagers}} (age group) as a
{{c2::mediastinal}} mass, thus it is often referred to as acute lymphoblastic
lymphoma presents with: - lymphadenopathy - mediastinal mass (thymus and often
associated with pleural effusions) - SVC-like syndrome - tracheal obstruction
(difficulty breathing) acute_leukemia BGedit EXPANSION fa2018 PathomaWBC WBC
AML is a neoplastic accumulation of {{c1::myeloblasts}} (>20%) in the bone marrow
i.e. acute myelogenous leukemia PathomaWBC WBC acute_leukemia
{{c2::Myelo}}-blasts are usually characterized by positive cytoplasmic staining for
{{c1::myeloperoxidase (MPO)}} PathomaWBC WBC acute_leukemia
Myeloblasts may have crystal aggregates of {{c2::MPO}}, which are seen on blood
smear as {{c1::Auer rods}} "described as ""azurophilic, needle-shaped
cytoplasmic inclusions""" PathomaWBC WBC acute_leukemia
Acute myeloid leukemia (AML) most commonly arises in {{c1::older adults (median
onset 65 years)}} PathomaWBC WBC acute_leukemia
One subtype of AML is {{c1::acute promyelocytic leukemia (APL)}}, which is
characterized by t({{c2::15}};{{c2::17}}) formally known as M3 AML PathomaWBC
WBC acute_leukemia cancer
The t(15;17) translocation seen in acute promyelocytic leukemia results in
disruption of the {{c1::retinoic acid}} receptor on chromosome 17 RAR
disruption blocks maturation and promyelocytes (blasts) accumulate PathomaWBC
WBC acute_leukemia cancer
The abnormal promyelocytes seen in APML contain numerous primary granules that
increase risk for {{c1::DIC}} Auer rods can activate coagulation cascade; DIC is
common presentation acute_leukemia PathomaWBC WBC
Acute promyelocytic leukemia is treated with {{c1::all-trans-retinoic acid
(ATRA)}}, a vitamin A derivative binds the altered receptor and causes the
blasts to mature PathomaWBC WBC acute_leukemia cancer
All-trans-retinoic acid binds the altered retinoic acid receptor in APL and causes
blasts to {{c1::mature}} PathomaWBC WBC acute_leukemia
One subtype of AML is acute {{c1::monocytic}} leukemia, which presents with
proliferation of monoblasts PathomaWBC WBC acute_leukemia
Do the monoblasts seen in acute monocytic leukemia typically contain
myeloperoxidase (MPO)? {{c1::No}} PathomaWBC WBC acute_leukemia
In acute {{c2::monocytic}} leukemia, blasts characteristically infiltrate the
{{c1::gums}} PathomaWBC WBC acute_leukemia
One subtype of AML is acute {{c1::megakaryoblastic}} leukemia, which presents with
proliferation of megakaryoblasts PathomaWBC WBC acute_leukemia
Do the megakaryoblasts seen in acute megakaryoblastic leukemia typically contain
myeloperoxidase (MPO)? {{c1::No}} PathomaWBC WBC acute_leukemia
{{c3::Acute megakaryoblastic}} leukemia is associated with {{c1::Down}} syndrome;
usually arises {{c2::before}} the age of 5 PathomaWBC WBC acute_leukemia
AML may arise from pre-existing {{c1::myelodysplastic}} syndromes
myelodysplastic syndromes are stem-cell disorders involving ineffective
hematopoiesis; results in defects in cell maturation of all nonlymphoid lineages
PathomaWBC WBC acute_leukemia
Risk factors for acute myeloid leukemia include prior exposure to
{{c1::alkylating}} chemotherapy and {{c2::radiation}} PathomaWBC WBC
acute_leukemia
Myelodysplastic syndromes usually present with increased blasts {{c1::< 20}}%
causes cytopenias and a hypercellular bone marrow acute_leukemia
PathomaWBC WBC
Myelodysplastic syndromes rarely may progress to {{c1::acute myeloid}} leukemia
most patients die from infection or bleeding before the myelodysplastic
syndrome progresses PathomaWBC WBC acute_leukemia
Myelodysplastic syndromes are caused by {{c1::de novo mutations}} or environmental
exposure (e.g. radiation, benzene, chemotherapy) myelodysplastic syndromes are
stem-cell disorders involving ineffective hematopoiesis PathomaWBC WBC
acute_leukemia
{{c3::Myelodysplastic}} syndromes may be associated with a {{c1::Pseudo-Pelger-
Huet}} anomaly, which are neutrophils with {{c2::bilobed}} nuclei
PathomaWBC WBC acute_leukemia
Pseudo-Pelger Huet anomaly is typically seen after {{c1::chemotherapy}}
PathomaWBC WBC acute_leukemia
{{c1::Chronic}} leukemia (acute or chronic) is a neoplastic proliferation of mature
circulating lymphocytes thus causing a high WBC count PathomaWBC WBC
chronic_leukemia
Chronic leukemia is usually insidious in onset and seen in {{c1::older adults}}
(age group) PathomaWBC WBC chronic_leukemia
{{c2::Chronic lymphocytic}} leukemia is a neoplastic proliferation of naive
{{c3::B}} cells that co-express CD-{{c1::5}} and CD-{{c1::20}} PathomaWBC
WBC chronic_leukemia
What is the most common leukemia in adults? {{c1::Chronic lymphocytic leukemia
(CLL)}} chronic_leukemia PathomaWBC WBC
{{c2::Chronic lymphocytic}} leukemia is associated with {{c1::smudge}} cells and
increased lymphocytes on blood smear PathomaWBC WBC chronic_leukemia
{{c2::Chronic lymphocytic}} leukemia commonly involves lymph nodes, leading to
generalized lymphadenopathy; thus called {{c1::small lymphocytic}} lymphoma
typically asymptomatic with slow progression PathomaWBC WBC
chronic_leukemia
One complication of chronic lymphocytic leukemia is {{c1::hypogammaglobulinemia}},
which predisposes to infection PathomaWBC WBC chronic_leukemia
What is the most common cause of death in patients with chronic lymphocytic
leukemia? {{c1::Infection (due to hypogammaglobulenemia)}} PathomaWBC WBC
chronic_leukemia
One complication of chronic lymphocytic leukemia is {{c1::autoimmune hemolytic}}
anemia Autoimmune hemolytic anemia is one of the most common causes of
acquired hemolytic anemia. It is diagnosed by the detection of antibodies against
the patient's RBCs via the direct Coombs test. This patient has typical lab values
of hemolytic anemia, including elevated LDH, increased indirect bilirubin, and low
haptoglobin levels. Autoimmune hemolytic anemia can be idiopathic, virally induced,
SLE-induced, the result of an adverse drug reaction, and a result of lymphomas.
chronic_leukemia PathomaWBC WBC
{{c2::Chronic lymphocytic}} leukemia may transform into {{c1::diffuse, large B-cell
lymphoma (DLBCL)}} via the {{c3::Richter}} transformation PathomaWBC WBC
chronic_leukemia
Transformation of CLL into diffuse, large B-cell lymphoma presents clinically as an
{{c1::enlarging}} lymph node or spleen PathomaWBC WBC chronic_leukemia
{{c1::Hairy cell}} leukemia is a neoplastic proliferation of mature {{c2::B}} cells
characterized by hairy cytoplasmic processes PathomaWBC WBC
chronic_leukemia
The cells in {{c2::hairy cell}} leukemia stain positive for {{c1::tartrate-
resistant acid phosphatase (TRAP)}} positive TRAP stain has been largely replaced
with flow cytometry PathomaWBC WBC chronic_leukemia
Positive TRAP stain for diagnosis of hairy cell leukemia has been largely replaced
with {{c1::flow cytometry}} PathomaWBC WBC chronic_leukemia
Patients with hairy cell leukemia typically present with massive
{{c1::splenomegaly}} due to expansion of the {{c2::red}} pulp PathomaWBC
WBC chronic_leukemia
"{{c2::Hairy cell}} leukemia causes marrow fibrosis, which results in a ""{{c1::dry
tap}}"" on bone marrow aspiration" PathomaWBC WBC chronic_leukemia
Does hairy cell leukemia typically present with lymphadenopathy? {{c1::No}}
PathomaWBC WBC chronic_leukemia
Hairy cell leukemia has an excellent response to {{c1::cladribine (2-CDA)}}, which
is an adenosine deaminase inhibitor causes adenosine to accumulate to toxic levels
in neoplastic B cells PathomaWBC WBC chronic_leukemia
In addition to cladribine (2-CDA), hairy cell leukemia may also be treated with
{{c1::pentostatin}} PathomaWBC WBC chronic_leukemia
What demographic is associated with hairy cell leukemia? {{c1::Adult males}}
PathomaWBC WBC chronic_leukemia
Adult T-cell leukemia/lymphoma (ATLL) is a neoplastic proliferation of mature
{{c1::CD4+ T}} cells PathomaWBC WBC chronic_leukemia
{{c2::Adult T-cell}} leukemia/lymphoma is caused by the {{c1::HTLV-1}} virus human
T-cell leukemia virus 1 PathomaWBC WBC chronic_leukemia
The HTLV-1 virus (cause of ATLL) is associated with {{c1::IV drug}} users
PathomaWBC WBC chronic_leukemia
What regions are most commonly affected by adult T-cell leukemia/lymphoma?
{{c1::Japan}}, {{c2::West Africa}}, and the {{c3::Caribbean}} PathomaWBC
WBC chronic_leukemia
Adult T-cell leukemia/lymphoma may present with {{c1::cutaneous lesions (rash)}}
due to skin infiltration also may have generalized lymphadenopathy with
hepatosplenomegaly PathomaWBC WBC chronic_leukemia
{{c3::Adult T-cell}} leukemia/lymphoma may present with {{c1::lytic (punched-out)}}
{{c2::bone}} lesions and hypercalcemia must distinguish from multiple myeloma,
which does not cause a rash PathomaWBC WBC chronic_leukemia
How can adult T-cell leukemia/lymphoma be distinguished from multiple myeloma?
{{c1::ATLL causes a rash}} both may present with lytic bone lesions and
hypercalcemia PathomaWBC WBC chronic_leukemia
Mycosis fungoides is a neoplastic proliferation of mature {{c1::CD4+ T}} cells
PathomaWBC WBC chronic_leukemia
Mycosis fungoides typically presents in adults with {{c1::skin}} patches/plaques
cutaneous T-cell lymphoma PathomaWBC WBC chronic_leukemia
The aggregates of neoplastic cells in the epidermis seen with mycosis fungoides are
called {{c1::Pautrier microabscesses}} PathomaWBC WBC chronic_leukemia
Mycosis fungoides may spread to involve the blood, producing {{c1::Sezary}}
syndrome (T-cell leukemia) PathomaWBC WBC chronic_leukemia
{{c2::Sezary}} syndrome is characterized by atypical CD4+ cells with
{{c1::cerebriform}} nuclei seen on blood smear Sezary syndrome is a progression of
mycosis fungoides PathomaWBC WBC chronic_leukemia
{{c1::Myeloproliferative}} disorders are neoplastic proliferations of mature cells
of myeloid lineage cells of all myeloid lineages may be increased; classified
based on the dominant cell produced MyeloproliferativeDisorders PathomaWBC WBC
Myeloproliferative disorders most commonly present in {{c1::late adulthood (50 - 60
years old)}} (age group) MyeloproliferativeDisorders PathomaWBC WBC
Myeloproliferative disorders may cause {{c1::hyperuricemia}} and {{c2::gout}} due
to high turnover of cells nuclear degradation leads to increased purine
degradation, which produces uric acid MyeloproliferativeDisorders PathomaWBC
WBC
Myeloproliferative disorders may progress to marrow {{c1::fibrosis}} or transform
to acute leukemia MyeloproliferativeDisorders PathomaWBC WBC
Chronic myeloproliferative disorders (except CML) are associated with {{c1::V617F
JAK2}} mutations JAK2 (Janus Kinase 2) is a cytoplasmic tyrosine kinase located on
chromosome 9 - mutations result in myeloid progenitors developing a
hypersensitivity to growth stimulating cytokines - this results in unregulated
myeloproliferation; cells have more growth and longer survival BGedit
Boards&Beyond EXPANSION MyeloproliferativeDisorders PathomaWBC Uworld WBC
{{c1::Chronic myeloid}} leukemia is a neoplastic proliferation of mature myeloid
cells, especially {{c2::granulocytes}} and their precursorsbasophils are
characteristically increased MyeloproliferativeDisorders PathomaWBC WBC cancer
{{c2::Chronic myeloid}} leukemia is defined by the t({{c1::9}};{{c1::22}})
translocation Philadelphia chromosome; rarely associated with ALL
MyeloproliferativeDisorders PathomaWBC WBC cancer
The t({{c3::9}};{{c3::22}}) translocation generates a {{c1::BCR}}-{{c1::ABL}}
fusion protein with increased {{c2::tyrosine kinase}} activity the t(9;22)
translocation is known as the Philadelphia chromosome MyeloproliferativeDisorders
PathomaWBC WBC cancer
Chronic myeloid leukemia responds well to tyrosine kinase inhibitors, such as
{{c1::imatinib}} Other Bcr-Abl inhibitors include other oral agents like
Dasatinib, Nilotinib; used for treatment in chronic phase (not curative), expensive
but minimal side effects bone marrow transplant is often used after treatment
failure BGedit EXPANSION MyeloproliferativeDisorders PathomaWBC WBC fa2018
Chronic myeloid leukemia commonly results in {{c1::spleno}}-megaly
MyeloproliferativeDisorders PathomaWBC WBC cancer
"An enlarging {{c1::spleen}} in CML suggests progression to accelerated disease
(""blast crisis"")" transformation to acute leukemia usually follows shortly
thereafter MyeloproliferativeDisorders PathomaWBC WBC
CML may transform to acute {{c1::myeloid}} leukemia (2/3rd of cases)
MyeloproliferativeDisorders PathomaWBC WBC
CML may transform to acute {{c1::lymphoid}} leukemia (1/3rd of transformations)
mutation in CML is in hematopoietic stem cells, thus it is possibly to
develop ALL from CML MyeloproliferativeDisorders PathomaWBC WBC
CML is distinguished from a leukemoid reaction (benign neutrophilia) by presence of
increased {{c1::basophils}} basophils are absent with leukemoid reaction;
additionally bone marrow in leukemoid is normal / hypercellular with increased
bands / early mature neutrophil precursors VS increased immature cells BGedit
EXPANSION MyeloproliferativeDisorders PathomaWBC Uworld WBC
CML is distinguished from a leukemoid reaction (benign neutrophilia) by a
{{c2::negative}} {{c1::leukocyte alkaline phosphatase (LAP)}} stain granulocytes
in leukemoid reaction are LAP positive MyeloproliferativeDisorders PathomaWBC
WBC
{{c1::Polycythemia vera}} is a neoplastic proliferation of mature myeloid cells,
especially {{c2::red blood}} cells - granulocytes and platelets are also increased
- aka primary polycythemia BGedit EXPANSION MyeloproliferativeDisorders
PathomaWBC WBC fa2018
Polycythemia vera is a form of {{c1::primary}} polycythemia (primary or secondary)
Caused by a V617F JAK2 mutation causing myeloid progenitors to become
hypersensitive to cytokine growth stimuli --> myeloproliferation BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
Polycythemia vera may present with symptoms of {{c1::hyperviscosity}} of the blood
(e.g. blurry vision, headache) Increased RBCs results in increased blood
viscosity - this increases the resistance of the vasculature --> rise in blood
pressure; high blood pressure is transmitted to the CNS - increased viscosity
(increased RBCs) results in increased stasis resulting in episodic blood clots in
vessels of extremities (also due to increased platelet count) BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
Polycythemia vera increases risk of venous {{c1::thrombosis}} e.g. hepatic vein
(Budd-Chiari syndrome), portal vein, DVT, and dural sinus thrombosis is the leading
cause of morbidity and mortality in these patients BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
Polycythemia vera rarely may cause {{c1::erythromelalgia}}, which is characterized
by severe, burning pain and red-blood discoloration due to episodic blood clots
in vessels of the extremities BGedit EXPANSION MyeloproliferativeDisorders
PathomaWBC WBC fa2018
{{c2::Polycythemia vera}} classically presents with intense {{c1::itching}},
especially after a hot shower - aka Aquagenic pruritis; due to histamine release
from increased mast cells - patients often present with facial plethora (red, puffy
skin) BGedit EXPANSION MyeloproliferativeDisorders PathomaWBC WBC fa2018
The 1st line treatment for polycythemia vera is {{c1::phlebotomy}}; second-line
therapy is {{c2::hydroxyurea}} without treatment, death usually occurs within
one year BGedit EXPANSION MyeloproliferativeDisorders PathomaWBC WBC fa2018
Patients with polycythemia vera may take low-dose {{c1::aspirin}} to decrease risk
of thrombosis - this is <300 mg/day of Aspirin - however, patients with
polycythemia are at an increased risk of Gout (due to high turnover); and low dose
aspirin (75 mg - 2 g) inhibits OAT channels which transport uric acid into proximal
tubule cells from blood; risk exacerbating gout BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
Polycythemia vera is characterized by {{c1::increased}} plasma volume increased
plasma volume manifests with: - hypertension and increased bleeding (due to
engorged vessels) - facial plethora (red puffy skin) - large retinal veins on
fundoscopy, visual disturbances (increased ICP transmitted through optic nerve
meninges) - headache (stretching of meninges) BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
Polycythemia vera is characterized by {{c1::significantly increased}} RBC mass
- 20 g/dL Hgb (normal is 15); increased HCT (60%) BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
Polycythemia vera is characterized by {{c1::decreased}} EPOdue to negative feedback
suppressing renal EPO production; important distinguishing feature from secondary
polycythemia BGedit EXPANSION MyeloproliferativeDisorders PathomaWBC WBC
fa2018
Relative polycythemia is characterized by {{c1::decreased}} plasma volume e.g.
dehydration, burns, prolonged vomiting, diarrhea, diuretics, dengue hemorrhagic
fever BGedit EXPANSION MyeloproliferativeDisorders PathomaWBC Uworld WBC fa2018
Relative polycythemia is characterized by {{c1::normal}} RBC mass - important
distinguishing feature from other causes of polycythemia (erythrocytosis) - this is
where the term hemoconcentration comes from, as decreased plasma volume + normal
RBC mass results in increased concentration of RBC BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC Uworld WBC fa2018
Relative polycythemia is characterized by {{c1::normal}} EPO - aka
Hemoconcentration, thus normal amount of oxygenated RBCs, thus no hypoxemia (and no
rise in EPO) BGedit EXPANSION MyeloproliferativeDisorders PathomaWBC WBC
fa2018
Which form of polycythemia is associated with dehydration and burns? {{c1::Relative
polycythemia (relative erythrocytosis / hemoconcentration)}} Also associated
with: - prolonged vomiting - excessive diuretic use / chronic diuretic use -
prolonged diarrhea - dengue hemorrhagic fever BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
Appropriate absolute polycythemia is characterized by {{c1::increased}} RBC mass
Here, hypoxemia is leading to an appropriate response of the kidneys to make
more EPO --> more RBCs are produced BGedit EXPANSION MyeloproliferativeDisorders
PathomaWBC WBC fa2018
Appropriate absolute polycythemia is characterized by {{c1::increased}} EPO -
Here, hypoxemia is leading to an appropriate response of the kidneys to make more
EPO --> more RBCs are produced - important distinguishing feature from polycythemia
vera BGedit EXPANSION MyeloproliferativeDisorders PathomaWBC WBC fa2018
{{c2::Appropriate}} absolute polycythemia is characterized by {{c1::decreased}} O2
saturation - this is because patients have developed more vehicles for O2, thus
the blood isn't saturated as much - important distinguishing feature from
inappropriate absolute polycythemia BGedit EXPANSION MyeloproliferativeDisorders
PathomaWBC WBC fa2018
Which form of polycythemia is associated with lung disease (ex. COPD / obstructive
sleep apnea), congenital heart disease, high altitude, and low birth weight?
{{c1::Appropriate absolute polycythemia (appropriate secondary erythrocytosis)}}
all etiologies are associated with hypoxia BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC Uworld WBC fa2018
Inappropriate absolute polycythemia is characterized by {{c1::increased}} RBC mass
This is caused by a paraneoplastic secretion of EPO: BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
Inappropriate absolute polycythemia is characterized by {{c1::increased}} EPO
important distinguishing feature from polycythemia vera BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC WBC fa2018
{{c2::Inappropriate}} absolute polycythemia is characterized by {{c1::normal}} O2
saturation important distinguishing feature from appropriate absolute polycythemia
(appropriate secondary erythrocytosis) BGedit EXPANSION
MyeloproliferativeDisorders PathomaWBC Uworld WBC fa2018
Which form of polycythemia is associated with ectopic EPO production (e.g.
malignancy, hydronephrosis & renal cysts) or exogenous EPO? {{c1::Inappropriate
absolute polycythemia (innapropriate secondary erythrocytosis)}} - Thus can also
see this in athletes who are blood doping - hydronephosis results in a
microcirculatory insult to the kidney, acting on itself to generating increase
hypoxia at the peritubular capillary interstitium (to which fibroblasts respond and
secrete EPO) BGedit EXPANSION MyeloproliferativeDisorders PathomaWBC Uworld
WBC fa2018
{{c1::Essential thrombocythemia (ET)}} is a neoplastic proliferation of mature
myeloid cells, especially {{c2::platelets}} RBCs and granulocytes may also be
increased MyeloproliferativeDisorders PathomaWBC WBC
Blood smear of essential {{c1::thrombocythemia}} shows markedly increased number of
platelets, which may be large or abnormally formed
MyeloproliferativeDisorders PathomaWBC WBC
Symptoms of essential thrombocythemia are related to an increased risk of
{{c1::bleeding}} and/or {{c2::thrombosis}} depends on whether platelets are
functional or non-functional; erythromelalgia may also occur
MyeloproliferativeDisorders PathomaWBC WBC
Are patients with essential thrombocythemia (ET) at risk for marrow fibrosis and/or
acute leukemia? {{c1::No (rare)}} MyeloproliferativeDisorders PathomaWBC
WBC
Does essential thrombocythemia (ET) present with significant risk for hyperuricemia
and gout? {{c1::No}} platelets don't have a nucleus, therefore purine
degradation and uric acid are not increased MyeloproliferativeDisorders
PathomaWBC WBC
{{c1::Myelofibrosis}} is a neoplastic proliferation of mature myeloid cells,
especially {{c2::megakaryocytes}} MyeloproliferativeDisorders PathomaWBC
WBC
In myelofibrosis, megakaryocytes produce excess {{c1::platelet-derived growth
factor (PDGF)}}, causing marrow fibrosis MyeloproliferativeDisorders
PathomaWBC WBC
Myelofibrosis is often associated with massive {{c1::splenomegaly}} due to
extramedullary hematopoiesis MyeloproliferativeDisorders PathomaWBC WBC
Myelofibrosis is characterized by a {{c1::leukoerythroblastic}} smear (increased
nucleated RBCs and immature granulocytes) secondary to extramedullary hematopoiesis
(spleen cannot prevent immature cells from entering blood as well as bone marrow)
MyeloproliferativeDisorders PathomaWBC WBC
Myelofibrosis causes increased risk of infection, thrombosis, and bleeding due to
{{c1::pancytopenia}} spleen is unable to fully compensate for poor hematopoiesis
by bone marrow MyeloproliferativeDisorders PathomaWBC WBC
"What pathologic RBC is associated with myelofibrosis? {{c1::""Tear drop"" cells
(dacrocyte)}}" MyeloproliferativeDisorders PathomaWBC WBC
Polycythemia vera is characterized by {{c1::increased}} WBCs
MyeloproliferativeDisorders PathomaWBC WBC
Polycythemia vera is characterized by {{c1::increased}} platelets
MyeloproliferativeDisorders PathomaWBC WBC
Is polycythemia vera associated with JAK2 mutations? {{c1::Yes}}
MyeloproliferativeDisorders PathomaWBC WBC
Is essential thrombocythemia associated with JAK2 mutations? {{c1::Yes (30-50%)}}
MyeloproliferativeDisorders PathomaWBC WBC
Is myelofibrosis associated with JAK2 mutations? {{c1::Yes (30-50%)}}
MyeloproliferativeDisorders PathomaWBC WBC
Is chronic myeloid leukemia associated with JAK2 mutations? {{c1::No (associated
with Philadelphia chromosome)}} MyeloproliferativeDisorders PathomaWBC
WBC cancer
{{c1::Lymphadenopathy (LAD)}} refers to enlarged lymph nodes PathomaWBC
WBC lymphoma
{{c1::Painful}} lymphadenopathy (painful or painless) is usually seen in lymph
nodes that are draining a region of acute infection e.g. acute lymphadenitis
PathomaWBC WBC lymphoma
{{c1::Painless}} lymphadenopathy (painful or painless) can be seen with chronic
inflammation, metastatic carcinoma, or lymphoma PathomaWBC WBC lymphoma
Proliferation of the B cell compartment of lymph nodes causes {{c1::follicular}}
hyperplasia (e.g. rheumatoid arthritis, early stages of HIV infection) follicles
are located in the cortex (C) PathomaWBC WBC lymphoma
Proliferation of the T cell compartment of lymph nodes causes {{c1::paracortex}}
hyperplasia (e.g. viral infections) PathomaWBC WBC lymphoma
Hyperplasia of sinus histiocytes is seen in lymph nodes that are draining a tissue
with {{c1::cancer}} circled areas in the medulla (m) PathomaWBC WBC lymphoma
{{c1::Lymphomas}} (leukemias or lymphomas) are neoplastic proliferations of
lymphoid cells that form a mass may arise in a lymph node or in extranodal
tissue PathomaWBC WBC lymphoma
Lymphoma is divided into {{c1::non-Hodgkin}} (60%) and {{c1::Hodgkin}} lymphoma
(40%) PathomaWBC WBC lymphoma
{{c1::Follicular}} lymphoma is a neoplastic proliferation of small B cells (CD20+)
that form follicle-like nodules PathomaWBC WBC cancer lymphoma
What form of non-Hodgkin lymphoma is seen in the image below? {{c1::Follicular
lymphoma}} PathomaWBC WBC cancer lymphoma
Follicular lymphoma typically presents in {{c1::late adulthood}} (age group)
PathomaWBC WBC cancer lymphoma
"{{c2::Follicular}} lymphoma is characterized by painless ""{{c1::waxing and
waning}}"" lymphadenopathy" "Has an persistent indolent course and ""waxes /
wanes"" for years; these patients typically DO NOT have B symptoms not all patients
require treatment, and this is difficult to cure" BGedit EXPANSION PathomaWBC
Uworld WBC lymphoma
{{c2::Follicular}} lymphoma is driven by a t({{c1::14}};{{c1::18}}) translocation
BCL2 on chromosome 18 translocates to the Ig heavy chain locus on chromosome
14 PathomaWBC WBC cancer lymphoma
What chromosome is BCL2 located on? {{c1::Chromosome 18}} PathomaWBC WBC
cancer lymphoma
What chromosome is Ig heavy chain located on? {{c1::Chromosome 14}}
PathomaWBC WBC lymphoma
The Ig heavy chain genes on chromosome 14 are {{c1::constitutively}} expressed
thus when other genes are translocated next to this heavy chain region, they
are overexpressed PathomaWBC WBC lymphoma
The t({{c3::14}},{{c3::18}}) translocation results in overexpression of
{{c1::Bcl2}}, resulting in inhibition of {{c2::apoptosis}} BCL2 gene is
constitutively active (follicular lymphoma) PathomaWBC WBC cancer lymphoma
Treatment of follicular lymphoma is reserved for symptomatic patients and involves
low-dose chemotherapy or {{c1::rituximab}} (anti-CD20 antibody) PathomaWBC
WBC cancer lymphoma
Follicular lymphoma may progress to {{c1::diffuse, large B-cell}} lymphoma, which
presents as an enlarging lymph node PathomaWBC WBC cancer lymphoma
Follicular lymphoma is distinguished from reactive follicular hyperplasia by
{{c1::disruption}} of normal lymph node architecture follicles take over entire
lymph node; lymph node architecture is maintained in follicular hyperplasia BGedit
Boards&Beyond EXPANSION PathomaWBC Uworld WBC lymphoma
Follicular lymphoma is distinguished from reactive follicular hyperplasia by lack
of {{c1::tingible body macrophages}} in germinal centers tingible body
macrophages are present in follicular hyperplasia (white spaces on right) vs.
follicular lymphoma (left) PathomaWBC WBC cancer lymphoma
Follicular lymphoma is distinguished from reactive follicular hyperplasia by
expression of {{c1::Bcl2}} in follicles Bcl2 is not expressed in follicular
hyperplasia to allow for apoptosis during somatic hypermutation PathomaWBC WBC
cancer lymphoma
Follicular lymphoma is distinguished from reactive follicular hyperplasia by
{{c1::mono}}-clonality follicular hyperplasia is polyclonal PathomaWBC WBC
cancer lymphoma
Grade {{c1::1}} follicular lymphoma is characterized by small cleaved cells
smaller cells are more well-differentiated and thus have better prognosis
(lower grade) small cells = centrocytes BGedit EXPANSION PathomaWBC Uworld WBC
lymphoma
Grade {{c1::2}} follicular lymphoma is characterized by a mixture of small cleaved
cells and large noncleaved cells Centrocyte = small cleaved cells Centroblast =
large noncleaved cells BGedit EXPANSION PathomaWBC Uworld WBC lymphoma
Grade {{c1::3}} follicular lymphoma is characterized by large noncleaved cells
large noncleaved cells = centroblasts ( BGedit EXPANSION PathomaWBC Uworld
WBC lymphoma
Is follicular lymphoma typically aggressive or indolent? {{c1::Indolent}}
PathomaWBC WBC cancer lymphoma
{{c1::Mantle cell}} lymphoma is a neoplastic proliferation of small B cells (CD20+)
that expands into the mantle zone PathomaWBC WBC lymphoma
Which region of the lymph node is immediately adjacent to the follicle?
{{c1::Mantle zone}} PathomaWBC WBC lymphoma
What demographic is associated with mantle cell lymphoma? {{c1::Adult males}}
PathomaWBC WBC lymphoma
{{c2::Mantle cell}} lymphoma is driven by a t({{c1::11}};{{c1::14}}) translocation
cyclin D1 on chromosome 11 translocates to the Ig heavy chain locus on
chromosome 14 PathomaWBC WBC cancer lymphoma
What chromosome is cyclin D1 located on? {{c1::Chromosome 11}} PathomaWBC
WBC cancer lymphoma
The t({{c3::11}},{{c3::14}}) translocation results in overexpression of
{{c1::Cyclin D1}}, which promotes the {{c2::G1/S}} transition in the cell cycle,
facilitating neoplastic proliferation seen in mantle cell lymphoma PathomaWBC
WBC cancer lymphoma
Is mantle cell lymphoma typically aggressive or indolent? {{c1::Aggressive}}
typically presents with late-stage disease PathomaWBC WBC lymphoma
{{c1::Marginal zone}} lymphoma is a neoplastic proliferation of small B cells
(CD20+) that expands into the marginal zone PathomaWBC WBC lymphoma
{{c1::Marginal zone}} lymphoma is associated with chronic inflammatory states (e.g.
Hashimoto thyroiditis, Sjogren syndrome, H. pylori gastritis) the marginal zone
is formed by post-germinal center B cells PathomaWBC WBC lymphoma
{{c1::MALToma}} is a form of marginal zone lymphoma in mucosal sites
PathomaWBC WBC lymphoma
Gastric MALTomas may regress with treatment of {{c1::H. pylori}} lymphoma
PathomaWBC WBC
{{c1::Burkitt}} lymphoma is a neoplastic proliferation of intermediate-sized B
cells (CD20+) PathomaWBC WBC cancer lymphoma
Burkitt lymphoma is associated with {{c1::EBV}} infection PathomaWBC WBC
cancer lymphoma
Burkitt lymphoma classically presents as an extranodal mass in a {{c1::child}} or
{{c1::young adult}} (age group) PathomaWBC WBC cancer lymphoma
The {{c2::African}} form of Burkitt lymphoma typically involves the {{c1::jaw}}
PathomaWBC WBC cancer lymphoma
The {{c3::sporadic}} form of Burkitt lymphoma typically involves the {{c1::pelvis}}
or {{c2::abdomen}} PathomaWBC WBC cancer lymphoma
{{c2::Burkitt}} lymphoma is driven by a t({{c1::8}};{{c1::14}}) translocation
c-myc on chromosome 8 translocates to the Ig heavy chain locus on chromosome
14 PathomaWBC WBC cancer lymphoma
What chromosome is c-myc located on? {{c1::Chromosome 8}} PathomaWBC WBC
cancer lymphoma
The t({{c2::8}},{{c2::14}}) translocation results in overexpression of {{c1::c-
myc}}, which promotes growth c-myc gene is constitutively active (Burkitt
lymphoma) PathomaWBC WBC cancer lymphoma
"{{c2::Burkitt}} lymphoma is characterized by a high {{c3::mitotic index}} and
""{{c1::starry-sky}}"" appearance on microscopy" "starry sky appearance due
to: - sheets of lymphocytes (blue sky) - interspersion of ""tingible body""
macrophages (filled with many phagocytized, apoptotic cells in various states of
degradation) [""white stars"" seen in the center] high mitotic index is represented
by high Ki-67 fraction" BGedit EXPANSION NBME120 PathomaWBC Uworld WBC lymphoma
{{c1::Diffuse large B-cell}} lymphoma is a neoplastic proliferation of large B
cells (CD20+) that grow diffusely in sheets - treat with Rituximab - normal
lymph node architecture of the follicle has been obliterated; these cells have
nuclei at least 5 times the size of small lymphocytes BGedit EXPANSION PathomaWBC
Uworld WBC lymphoma
What is the most common form of non-Hodgkin lymphoma? {{c1::Diffuse large B-cell
lmyphoma (DLBCL)}} PathomaWBC WBC cancer lymphoma
Is diffuse large B-cell lymphoma typically aggressive or indolent?
{{c1::Aggressive}} PathomaWBC WBC lymphoma
{{c1::Diffuse large B-cell}} lymphoma arises sporadically or from transformation of
low-grade lymphoma (e.g. follicular lymphoma) PathomaWBC WBC cancer
lymphoma
Diffuse large B-cell lymphoma often presents in {{c1::late adulthood}} (age group)
as an enlarging lymph node or an extranodal mass PathomaWBC WBC lymphoma
While diffuse large B-cell lymphoma is usually seen in older adults, {{c1::20}}% of
cases occur in children PathomaWBC WBC lymphoma
Primary CNS lymphoma is most commonly seen in patients with {{c1::AIDS::disease}}
considered an AIDS-defining illness and is the most frequent CNS tumor in
immunosuppressed patients BGedit EXPANSION PathomaWBC Uworld WBC lymphoma
{{c1::Primary CNS}} lymphoma typically presents in adults with confusion, memory
loss, and seizures (variable presentation) PathomaWBC WBC lymphoma
{{c1::Primary CNS}} lymphoma typically presents as a single, solid brain lesion on
MRI may be ring-enhancing in immunocompromised patient; versus multiple ring
enhancing lesions in toxoplasmosis Primary CNS depicted below: Toxo depicted below:
BGedit EXPANSION PathomaWBC WBC fa2018 lymphoma
Primary CNS lymphoma must be distinguished from {{c1::toxoplasmosis}} infection via
CSF analysis or other lab tests single, solid lesion (lymphoma) vs multiple,
ring-enhancing lesions (toxoplasmosis) PathomaWBC WBC lymphoma
{{c2::Hodgkin}} lymphoma is a neoplastic proliferation of {{c1::Reed-Sternberg}}
cells RS cells are necessary but not sufficient for diagnosis of Hodgkin lymphoma
PathomaWBC WBC lymphoma
"{{c2::Reed-Sternberg}} cells are large {{c1::B}} cells with multilobed nuclei and
prominent nucleoli (""owl eye"" appearance)" note: it is a single Reed-Sternberg
cell surrounded by other inflammatory cells (classic for Hodgkin lymphoma) BGedit
EXPANSION PathomaWBC Uworld WBC lymphoma
Reed-Sternberg cells are classically positive for CD-{{c1::15}} and CD-{{c1::30}}
"""2 owl eyes x 15 = 30""" PathomaWBC WBC lymphoma
Reed-Sternberg cells secrete {{c1::cytokines}}, which attract other inflammatory
cells e.g. reactive lymphocytes, plasma cells, macrophages, and eosinophils
PathomaWBC WBC lymphoma
"Reed-Sternberg cells occassionally result in ""{{c1::B}}"" symptoms (fever,
chills, weight loss, night sweats)" due to cytokine production lymphoma
PathomaWBC WBC
The tumors seen in Hodgkin lymphoma are mostly composed of reactive
{{c1::inflammatory}} cells forms the basis for classification of Hodgkin
lymphoma PathomaWBC WBC lymphoma
What is the most common subtype of Hodgkin lymphoma (70%)? {{c1::Nodular
sclerosis}} PathomaWBC WBC lymphoma
What demographic is classically associated with the nodular sclerosis subtype of
Hodgkin lymphoma? {{c1::Young adult females}} PathomaWBC WBC lymphoma
The {{c1::nodular sclerosis}} subtype of Hodgkin lymphoma typically presents as an
enlarging cervical or mediastinal lymph node in a female PathomaWBC WBC
lymphoma
Which subtype of Hodgkin lymphoma is seen in the image below? {{c1::Nodular
sclerosis - Lymph node divided by bands of sclerosis}} PathomaWBC WBC
lymphoma
The {{c2::nodular sclerosis}} subtype of Hodgkin lymphoma is characterized
histologically by presence of Reed-Sternberg cells in {{c1::lake}}-like spaces
(lacunar cells) PathomaWBC WBC lymphoma
Which subtype of Hodgkin lymphoma has the best prognosis? {{c1::Lymphocyte-rich}}
for Hodgkin lymphoma, the more lymphocytes, the better the prognosis
PathomaWBC WBC lymphoma
Which subtype of Hodgkin lymphoma is often associated with abundant eosinophils?
{{c1::Mixed-cellularity}} PathomaWBC WBC lymphoma
Hodgkin lymphoma may present with eosinophilia due to production of {{c1::IL-5}} by
Reed-Sternberg cells (especially mixed cellularity subtype) PathomaWBC WBC
lymphoma
Which subtype of Hodgkin lymphoma is the most aggressive? {{c1::Lymphocyte-
depleted}} PathomaWBC WBC lymphoma
Which subtype of Hodgkin lymphoma is usually seen in the elderly and HIV+
individuals? {{c1::Lymphocyte-depleted}} worst prognosis; for Hodgkin lymphoma,
the more lymphocytes, the better the prognosis PathomaWBC WBC lymphoma
Most subtypes of Hodgkin lymphoma are more common in {{c1::men}} (gender) the
exception being nodular sclerosis subtype PathomaWBC WBC lymphoma
Which type of lymphoma (Hodgkin or non-Hodgkin) is associated with masses composed
of lymphoid cells? {{c1::non-Hodgkin lymphoma}} majority involve B-cells; a few are
of T-cell lineage (e.g. ATLL) PathomaWBC WBC lymphoma
Which type of lymphoma (Hodgkin or non-Hodgkin) is associated with masses composed
of reactive inflammatory cells? {{c1::Hodgkin lymphoma}} PathomaWBC WBC
lymphoma
Which type of lymphoma (Hodgkin or non-Hodgkin) is characterized by contiguous
spread? {{c1::Hodgkin lymphoma}} localized, single group of nodes; rarely
extranodal PathomaWBC WBC lymphoma
Which type of lymphoma (Hodgkin or non-Hodgkin) is characterized by non-contiguous
spread? {{c1::non-Hodgkin lymphoma}} diffuse spread PathomaWBC WBC lymphoma
Which type of lymphoma (Hodgkin or non-Hodgkin) is associated with extranodal
involvement? {{c1::non-Hodgkin lymphoma}} PathomaWBC WBC lymphoma
{{c2::Staging}} is important and the strongest predictor of prognosis for
{{c1::Hodgkin}} lymphoma (Hodgkin or non-Hodgkin) staging is also is used to
guide therapy; many patients have a relatively good prognosis PathomaWBC WBC
lymphoma
{{c1::Radiation}} is the mainstay of treatment for Hodgkin lymphoma
chemotherapeutic regimens can be used ex. ABVD (Doxorubicin (Adriamycin),
Bleomycin, Vinblastine, Dacarbazine) However, if given to the neck, may cause an
iatrogenic hypothyroidism and if near the head can cause an iatrogenic
hypopituitarism BGedit Boards&Beyond EXPANSION PathomaWBC WBC lymphoma
Hodgkin lymphoma has a bimodal distribution: common in {{c1::young adulthood}} and
{{c2::adults > 55 years}} PathomaWBC WBC lymphoma
{{c2::Multiple myeloma}} is a malignant proliferation of {{c3::mono}}-clonal
{{c1::plasma}} cells in the bone marrow PathomaWBC PlasmaCellDisorders WBC
{{c1::Multiple myeloma}} is the most common primary malignancy of bone in people >
40 - 50 years old PathomaWBC PlasmaCellDisorders WBC
What is the most common bone malignancy? {{c1::Metastatic cancer}}
PathomaWBC PlasmaCellDisorders WBC
Multiple myeloma is associated with high serum IL-{{c1::6}}, which stimulates
plasma cell growth and immunoglobulin production PathomaWBC
PlasmaCellDisorders WBC
Multiple myeloma presents with {{c1::lytic (punched-out)}} {{c2::bone}} lesions and
hypercalcemia increases risk for fracture PathomaWBC PlasmaCellDisorders WBC
The bone lesions seen with multiple myeloma are most common in the
{{c1::vertebrae}} and {{c2::skull}} PathomaWBC PlasmaCellDisorders WBC
In multiple myeloma, neoplastic plasma cells produce {{c1::IL-1}}, which stimulates
{{c2::osteoclast}} maturation that will lead to bone resorption "In this role, IL-
1 is known as Osteoclast Activating Factor this results in lytic lesions on x-ray
(""punched out"")" BGedit EXPANSION MedBullets PathomaWBC PlasmaCellDisorders
WBC fa2018
Multiple myeloma is associated with {{c1::elevated}} serum protein due to
increased immunoglobulin production PathomaWBC PlasmaCellDisorders WBC
Multiple myeloma is associated with {{c1::M spike}} on serum protein
electrophoresis (SPEP) M stands for monoclonal; remember that gamma spike
indicates gamma globulin, not IgG specifically PathomaWBC PlasmaCellDisorders WBC
The M spike seen in {{c3::multiple myeloma}} is most commonly due to monoclonal
{{c1::IgG}} (55%) or {{c2::IgA}} (25%) important distinguishing feature from
Waldenstrom macroglobulinemia (typically IgM) PathomaWBC PlasmaCellDisorders WBC
Multiple myeloma is associated with increased risk of {{c1::infection}} due to lack
of {{c2::antigenic}} diversity of monoclonal antibodies PathomaWBC
PlasmaCellDisorders WBC
What is the most common cause of death in multiple myeloma? {{c1::Infection}}
PathomaWBC PlasmaCellDisorders WBC
Multiple myeloma is associated with {{c1::Rouleaux formation}} of RBCs on blood
smear increased serum protein decreases charge between RBCsPathomaWBC
PlasmaCellDisorders WBC
Multiple myeloma may deposit in tissue, causing {{c1::primary (AL)}} amyloidosis
free light chains circulate in serum and deposit in tissue as amyloid light
chain (AL) PathomaWBC PlasmaCellDisorders WBC
{{c3::Multiple myeloma}} is associated with free {{c1::light chain}} excretion in
the urine, known as {{c2::Bence Jones}} proteinuria Kappa light chain increased
PathomaWBC PlasmaCellDisorders WBC
In multiple myeloma, free light chain (Bence Jones protein) may deposit in kidney
tubules, leading to risk for {{c1::renal failure (myeloma kidney)}} these appear
as large, eosinophilic casts composed of Bence-Jones protein in the tubular lumen
PathomaWBC PlasmaCellDisorders WBC
"The signs/symptoms of {{c6::multiple myeloma}} may be remembered with the mnemonic
""CRAB"": C: {{c1::hyperCalcemia}} R: {{c2::Renal involvement}} A: {{c3::Anemia}}
B: {{c4::Bone lytic lesions}} / {{c5::Back pain}}" PathomaWBC
PlasmaCellDisorders WBC
{{c1::Monoclonal gammopathy of undetermined significance (MGUS)}} is an
asymptomatic condition characterized by an M spike on SPEP without other features
of multiple myeloma "i.e. no ""CRAB"" symptoms (multiple myeloma) and no
hyperviscosity symptoms (Waldenstrom macroglobulinemia)" PathomaWBC
PlasmaCellDisorders WBC
Monoclonal gammopathy of underdetermined significance (MGUS) is common in the
{{c1::elderly}} (age group) seen in 5% of 70-year-old individuals PathomaWBC
PlasmaCellDisorders WBC
1-2% of patients with monoclonal gammopathy of underdetermined significance (MGUS)
develop {{c1::multiple myeloma}} per year PathomaWBC PlasmaCellDisorders WBC
{{c1::Waldenstrom macroglobulinemia}} is a B-cell lymphoma with monoclonal IgM
production PathomaWBC PlasmaCellDisorders WBC
Does Waldenstrom macroglobulinemia present with lytic bone lesions? {{c1::No}}
"no ""CRAB"" symptoms; important distinguishing feature from multiple
myeloma" PathomaWBC PlasmaCellDisorders WBC
The M spike seen in {{c2::Waldenstrom macroglobulinemia}} is due to monoclonal
Ig{{c1::M}} important distinguishing feature from multiple myeloma (typically IgG
or IgA) PathomaWBC PlasmaCellDisorders WBC
Waldenstrom macroglobulinemia typically presents with {{c1::visual}} and
{{c2::neurologic}} deficits e.g. retinal hemorrhage, stroke; due to serum
hyperviscosity PathomaWBC PlasmaCellDisorders WBC
Waldenstrom macroglobulinemia is associated with symptoms of {{c1::hyperviscosity}}
(due to large size of IgM pentamer) e.g. Raynaud phenomenom PathomaWBC
PlasmaCellDisorders WBC
Waldenstrom macroglobulinemia may present with {{c1::bleeding}} due to defective
platelet aggregation secondary to viscous serum PathomaWBC
PlasmaCellDisorders WBC
Acute complications of Waldenstrom macroglobulinemia are treated with
{{c1::plasmapheresis}}, which removes IgM from the serum PathomaWBC
PlasmaCellDisorders WBC
Langerhans cells are specialized {{c1::dendritic}} cells predominantly found in
skin LangerhansCellHistiocytosis PathomaWBC WBC
Langerhans cells are derived from bone marrow {{c1::monocytes}}
LangerhansCellHistiocytosis PathomaWBC WBC
Langerhans cells present antigen to naive {{c1::T}} cells
LangerhansCellHistiocytosis PathomaWBC WBC
{{c1::Langerhans cell histiocytosis}} is a neoplastic proliferation of Langerhans
cells LangerhansCellHistiocytosis PathomaWBC WBC
{{c2::Langerhans cell histiocytosis}} is characterized by {{c1::Birbeck (tennis
racket)}} granules on electron microscopy LangerhansCellHistiocytosis
PathomaWBC WBC
Langerhans cells are positive for {{c1::CD1a}} and {{c2::S100}} on
immunohistochemistry LangerhansCellHistiocytosis PathomaWBC WBC
{{c1::S100}} is an immunohistochemical stain that stains cells of neural crest
origin also stains Langerhans cells, dendritic cells, macrophages, and
chondrocytes LangerhansCellHistiocytosis PathomaWBC WBC
Langerhans cell histiocytosis may present as recurrent {{c1::otitis media}} with a
mass involving the mastoid bone LangerhansCellHistiocytosis PathomaWBC
WBC
Do the Langerhans cells in Langerhans cell histiocytosis effectively stimulate
primary T cells via antigen presentation? {{c1::No (functionally immature)}}
LangerhansCellHistiocytosis PathomaWBC WBC
Letterer-Siwe disease is a {{c1::malignant}} proliferation (benign or malignant) of
Langerhans cells Pathoma rules for Langerhans cell histiocytosis: 1. If it
involves names, it is malignant 2. Malignant proliferations involve the skin 3. If
two people named, affects children < 2 years old 4. If three people named, affects
children > 3 years old LangerhansCellHistiocytosis PathomaWBC WBC
Which Langerhans cell histiocytosis presents as skin rash and cystic skeletal
defects? {{c1::Letterer-Siwe disease}} multiple organs may be involved; rapidly
fatal Pathoma rules for Langerhans cell histiocytosis: 1. If it involves names, it
is malignant 2. Malignant proliferations involve the skin 3. If two people named,
affects children < 2 years old 4. If three people named, affects children > 3 years
old LangerhansCellHistiocytosis PathomaWBC WBC
Letterer-Siwe disease is often seen in {{c1::infants < 2 years old}} (age group)
Pathoma rules for Langerhans cell histiocytosis: 1. If it involves names, it
is malignant 2. Malignant proliferations involve the skin 3. If two people named,
affects children < 2 years old 4. If three people named, affects children > 3 years
old LangerhansCellHistiocytosis PathomaWBC WBC
Eosinophilic granuloma is a {{c1::benign}} proliferation (benign or malignant) of
Langerhans cells Pathoma rules for Langerhans cell histiocytosis: 1. If it
involves names, it is malignant 2. Malignant proliferations involve the skin 3. If
two people named, affects children < 2 years old 4. If three people named, affects
children > 3 years old LangerhansCellHistiocytosis PathomaWBC WBC
Which Langerhans cell histiocytosis presents as pathologic fracture with no skin
involvement? {{c1::Eosinophilic granuloma}} Pathoma rules for Langerhans cell
histiocytosis: 1. If it involves names, it is malignant 2. Malignant proliferations
involve the skin 3. If two people named, affects children < 2 years old 4. If three
people named, affects children > 3 years old LangerhansCellHistiocytosis
PathomaWBC WBC
Eosinophilic granuloma is often seen in {{c1::adolescents}} (age group)
Pathoma rules for Langerhans cell histiocytosis: 1. If it involves names, it
is malignant 2. Malignant proliferations involve the skin 3. If two people named,
affects children < 2 years old 4. If three people named, affects children > 3 years
old LangerhansCellHistiocytosis PathomaWBC WBC
Hand-Schuller-Christian disease is a {{c1::malignant}} proliferation (benign or
malignant) of Langerhans cells Pathoma rules for Langerhans cell
histiocytosis: 1. If it involves names, it is malignant 2. Malignant proliferations
involve the skin 3. If two people named, affects children < 2 years old 4. If three
people named, affects children > 3 years old LangerhansCellHistiocytosis
PathomaWBC WBC
Which Langerhans cell histiocytosis presents as scalp rash, lytic skull lesions,
diabetes insipidus, and exopthalmos? {{c1::Hand-Schuller-Christian disease}}
Pathoma rules for Langerhans cell histiocytosis: 1. If it involves names, it
is malignant 2. Malignant proliferations involve the skin 3. If two people named,
affects children < 2 years old 4. If three people named, affects children > 3 years
old LangerhansCellHistiocytosis PathomaWBC WBC
Hand-Schuller-Christian disease is often seen in {{c1::children > 3 years old}}
(age group) Pathoma rules for Langerhans cell histiocytosis: 1. If it involves
names, it is malignant 2. Malignant proliferations involve the skin 3. If two
people named, affects children < 2 years old 4. If three people named, affects
children > 3 years old LangerhansCellHistiocytosis PathomaWBC WBC
{{c1::Acute lymphoblastic}} leukemia is associated with the t(12;21) translocation
specifically the B-ALL subtype PathomaWBC WBC acute_leukemia cancer
The t(9;22) translocation (BCR-ABL) is also known as the {{c1::Philadelphia}}
chromosome most commonly seen in CML; rarely seen with ALL
MyeloproliferativeDisorders PathomaWBC WBC cancer
In multiple myeloma, neoplastic plasma cells produce IL-{{c1::6}} which stimulates
osteoclast activating factor PathomaWBC PlasmaCellDisorders WBC
Hodgkin lymphoma is associated with {{c1::EBV}} infection PathomaWBC WBC
lymphoma
Is primary CNS lymphoma typically a B-cell or T-cell neoplasm? {{c1::B-cell}}
WBC
The pathogenesis of primary CNS lymphoma involves {{c1::EBV}} infection
WBC
Potrebbero piacerti anche
- MyeloproliferativeDocumento9 pagineMyeloproliferativeRashed ShatnawiNessuna valutazione finora
- Deep Vein Thrombosis and Pulmonary Embolism: A guide for practitioners 2/edDa EverandDeep Vein Thrombosis and Pulmonary Embolism: A guide for practitioners 2/edValutazione: 5 su 5 stelle5/5 (1)
- Interpret CBC Test Results and Diagnose Common Blood DisordersDocumento39 pagineInterpret CBC Test Results and Diagnose Common Blood Disorderspido29Nessuna valutazione finora
- Complete Blood CountDocumento10 pagineComplete Blood CountJohn Lee Lorena Gacusan100% (1)
- Acute Lymphoblastic Leukemia (ALL) TreatmentDocumento10 pagineAcute Lymphoblastic Leukemia (ALL) TreatmentAndreea TudurachiNessuna valutazione finora
- Disorders of The Wihte CellsDocumento22 pagineDisorders of The Wihte CellsdoniNessuna valutazione finora
- Acute and Chronic LeukemiasDocumento3 pagineAcute and Chronic Leukemiaskaku100% (2)
- Acute Leukemia: Understanding the Pathogenesis, Diagnosis and ManagementDocumento52 pagineAcute Leukemia: Understanding the Pathogenesis, Diagnosis and ManagementJamilNessuna valutazione finora
- Hem/Onc Lecture 1Documento4 pagineHem/Onc Lecture 1xcupcakex122006Nessuna valutazione finora
- ThrombocytopeniaDocumento4 pagineThrombocytopeniaValerrie NgenoNessuna valutazione finora
- How to Interpret HEMATOLOGY Test ResultsDocumento36 pagineHow to Interpret HEMATOLOGY Test Resultssylvia haryantoNessuna valutazione finora
- Hyperleukocytosis and Leukostasis in Hematologic MalignanciesDocumento17 pagineHyperleukocytosis and Leukostasis in Hematologic MalignanciesAna María Díaz MedinaNessuna valutazione finora
- Complete Blood CountDocumento18 pagineComplete Blood CountNazih MominNessuna valutazione finora
- 2nd Sem - Hema1 - An Overview of Clinical Laboratory HematologyDocumento3 pagine2nd Sem - Hema1 - An Overview of Clinical Laboratory HematologyAisle Malibiran PalerNessuna valutazione finora
- CBC JusselDocumento3 pagineCBC JussellessujmNessuna valutazione finora
- Leukemia Lymphoma Skin Cancer - RubioDocumento22 pagineLeukemia Lymphoma Skin Cancer - Rubiochristian pulmonesNessuna valutazione finora
- Haematopathology 3:: Leucocytosis/LeucopeniaDocumento113 pagineHaematopathology 3:: Leucocytosis/LeucopeniaarwaNessuna valutazione finora
- Leukocyte Classification and Differential CountDocumento37 pagineLeukocyte Classification and Differential CountHend HamedNessuna valutazione finora
- Casos Clinicos de Hematopatología IiDocumento5 pagineCasos Clinicos de Hematopatología IiRicardo LaraNessuna valutazione finora
- Hemostasis Disorders in LeukemiaDocumento14 pagineHemostasis Disorders in LeukemiaNurul HidayahNessuna valutazione finora
- 1 Hematology TestDocumento48 pagine1 Hematology TestAhmed YassinNessuna valutazione finora
- CBC Test Results and InterpretationDocumento9 pagineCBC Test Results and InterpretationamiosaNessuna valutazione finora
- Hematology - 2013 SDDDocumento17 pagineHematology - 2013 SDDOrlan Defensor BalanoNessuna valutazione finora
- Complete Blood CountDocumento10 pagineComplete Blood CountGenevang Seaweeds100% (1)
- What Is LeukopeniaDocumento8 pagineWhat Is LeukopeniaMustafa AlmasoudiNessuna valutazione finora
- Complete blood count guide for screening disordersDocumento22 pagineComplete blood count guide for screening disordersSerious LeoNessuna valutazione finora
- Thrombocytopenia & TTP GuideDocumento17 pagineThrombocytopenia & TTP GuidemohNessuna valutazione finora
- BloodDocumento30 pagineBloodOm HabibaNessuna valutazione finora
- Hematology Review 2021-2Documento142 pagineHematology Review 2021-2Maram AbdullahNessuna valutazione finora
- LabDocumento28 pagineLabChamCham AquinoNessuna valutazione finora
- Hyperleukocytosis and leukostasis in hematologic malignanciesDocumento13 pagineHyperleukocytosis and leukostasis in hematologic malignanciesIGD RSKDNessuna valutazione finora
- Hyperleukocytosis and Leukostasis in Hematologic MalignanciesDocumento9 pagineHyperleukocytosis and Leukostasis in Hematologic Malignanciessoclose1200Nessuna valutazione finora
- Good AfternoonDocumento18 pagineGood Afternoonmathurarun2000Nessuna valutazione finora
- Med Surg Chapters 19 - 20 Hematologic Functions and Disorders PPT and QuestionsDocumento36 pagineMed Surg Chapters 19 - 20 Hematologic Functions and Disorders PPT and QuestionsAshley100% (1)
- Hematology IIDocumento26 pagineHematology IIpieterinpretoria391Nessuna valutazione finora
- C B C I: Omplete Lood Ount NterpretationsDocumento44 pagineC B C I: Omplete Lood Ount NterpretationsridhoniNessuna valutazione finora
- 3rd CBC & Blood IndicesDocumento65 pagine3rd CBC & Blood Indicesso mohamedNessuna valutazione finora
- Chronic Lymphocytic CLLDocumento14 pagineChronic Lymphocytic CLLPamy AbellaNessuna valutazione finora
- Pathoma - Leukopenia and LeucocytosisDocumento9 paginePathoma - Leukopenia and Leucocytosissubbuhc100% (1)
- Haematological Tests: Jhanvi Ka Patel Rool No. 09Documento21 pagineHaematological Tests: Jhanvi Ka Patel Rool No. 09Aditya PatelNessuna valutazione finora
- CBC test components and resultsDocumento4 pagineCBC test components and resultsGenefer AlmeliaNessuna valutazione finora
- Pancytopenia: Reduced RBC, WBC and Platelet DefinitionDocumento2 paginePancytopenia: Reduced RBC, WBC and Platelet DefinitionsalyasaaNessuna valutazione finora
- Practical Hematology Lab: CBC ParametersDocumento27 paginePractical Hematology Lab: CBC ParametersDiane-Richie PezLoNessuna valutazione finora
- CBC 150106153749 Conversion Gate02Documento44 pagineCBC 150106153749 Conversion Gate02KhetanNessuna valutazione finora
- CBC Analysis & Types of AnemiaDocumento19 pagineCBC Analysis & Types of AnemiarayevieNessuna valutazione finora
- Complete Blood CountDocumento19 pagineComplete Blood CountIrene Andriani Halim100% (1)
- Chronic Myeloid Leukemia (CML) Is A Form of Leukemia CharacterizedDocumento4 pagineChronic Myeloid Leukemia (CML) Is A Form of Leukemia CharacterizedbassamhematolNessuna valutazione finora
- Hematology: Complete Blood Count and Differential CountDocumento12 pagineHematology: Complete Blood Count and Differential CountimperiouxxNessuna valutazione finora
- HEMADocumento3 pagineHEMAFlorence Mae RoselNessuna valutazione finora
- Hema RecallDocumento11 pagineHema Recallmkct111100% (1)
- Lab Final Exam ReviewDocumento59 pagineLab Final Exam ReviewManju ShreeNessuna valutazione finora
- MK Hematology-LeukemiasDocumento35 pagineMK Hematology-LeukemiasMoses Jr KazevuNessuna valutazione finora
- Complete Blood Count: Performed To Provide An Overview of A Patient's General Health StatusDocumento4 pagineComplete Blood Count: Performed To Provide An Overview of A Patient's General Health StatusRaprnaNessuna valutazione finora
- Information From MicrographsDocumento4 pagineInformation From MicrographsOjambo FlaviaNessuna valutazione finora
- Answers - Haematological Malignancies Digital Images QuizDocumento4 pagineAnswers - Haematological Malignancies Digital Images Quizcande casanasNessuna valutazione finora
- Acute LeukemiasDocumento48 pagineAcute LeukemiaslaibaNessuna valutazione finora
- Heme-Onc Anki QDocumento41 pagineHeme-Onc Anki Qjhk0428Nessuna valutazione finora
- Pathoma Ch04 HemeDocumento16 paginePathoma Ch04 HemekikocornholioNessuna valutazione finora
- Zanki Pathoma RBCDocumento29 pagineZanki Pathoma RBCkikocornholioNessuna valutazione finora
- ImunoDocumento66 pagineImunokikocornholioNessuna valutazione finora
- ImunoDocumento66 pagineImunokikocornholioNessuna valutazione finora
- Zanki MicroDocumento584 pagineZanki MicrokikocornholioNessuna valutazione finora
- Superparamagnetism: Limits and ApplicationsDocumento7 pagineSuperparamagnetism: Limits and ApplicationsNguyen VuNessuna valutazione finora
- Tema 3 - Inmune Responses To ImplantsDocumento18 pagineTema 3 - Inmune Responses To ImplantsIsrael GonzálezNessuna valutazione finora
- Stages of CancerDocumento9 pagineStages of CancerAlisha SharanNessuna valutazione finora
- Understanding Nodular PrurigoDocumento5 pagineUnderstanding Nodular Prurigoranz ibonkNessuna valutazione finora
- Syllabus-Neuroscience 10 Neuroscience in 21st Century-2012FallDocumento4 pagineSyllabus-Neuroscience 10 Neuroscience in 21st Century-2012FallJerikko Timm AgatepNessuna valutazione finora
- Cancer Detection by GraphologyDocumento5 pagineCancer Detection by GraphologyEndy Mulio100% (1)
- Vitamin K: Wallflower Sister of The FamousDocumento3 pagineVitamin K: Wallflower Sister of The FamousbisanpaNessuna valutazione finora
- Biochemistry of The Eye, 2ed. 2003Documento331 pagineBiochemistry of The Eye, 2ed. 2003Vuqar100% (3)
- Rheumatoid ArthritisDocumento38 pagineRheumatoid ArthritisOlga GoryachevaNessuna valutazione finora
- The Immune System and Immunity: By: Princess Nhoor A. AgcongDocumento24 pagineThe Immune System and Immunity: By: Princess Nhoor A. AgcongCess Abad AgcongNessuna valutazione finora
- Water BugggssDocumento20 pagineWater BugggssShayna Evangelista Del ValleNessuna valutazione finora
- Pathophysio DHF EDITEDDocumento3 paginePathophysio DHF EDITEDricmichael100% (1)
- CFP Report 2022 IvaDocumento265 pagineCFP Report 2022 IvaИва АрифајNessuna valutazione finora
- Functions of Blood and ComponentsDocumento15 pagineFunctions of Blood and ComponentsayuNessuna valutazione finora
- Causes and prevention of cancerDocumento4 pagineCauses and prevention of cancerosamaNessuna valutazione finora
- Characteristics and Classification of NeoplasmsDocumento31 pagineCharacteristics and Classification of Neoplasmsjpanay100% (1)
- About Inflammation and InfectionDocumento2 pagineAbout Inflammation and InfectionHAZRULNessuna valutazione finora
- Reproductive Physiology: The Development of GonadsDocumento113 pagineReproductive Physiology: The Development of GonadsWonze WossendresNessuna valutazione finora
- Criminal Behavior Genre DraftDocumento6 pagineCriminal Behavior Genre Draftapi-309159739Nessuna valutazione finora
- NCP For Ectopic PregnancyDocumento4 pagineNCP For Ectopic PregnancyClarissa_Dante_735850% (4)
- Molecular Networking As A Drug Discovery, Drug Metabolism, and Precision Medicine StrategyDocumento12 pagineMolecular Networking As A Drug Discovery, Drug Metabolism, and Precision Medicine StrategySam SonNessuna valutazione finora
- Chloroquine Diphosphate Salt (C6628) - Product Information SheetDocumento1 paginaChloroquine Diphosphate Salt (C6628) - Product Information SheetSigma-Aldrich100% (2)
- A Network Analysis of COVID-19 mRNA Vaccine Patents: ModernaDocumento3 pagineA Network Analysis of COVID-19 mRNA Vaccine Patents: ModernaMatthieu BecquartNessuna valutazione finora
- 3a ReproductionDocumento25 pagine3a ReproductionThaarvena Retina100% (1)
- Hepatitis C Virus Encoded Antigen DetectionDocumento25 pagineHepatitis C Virus Encoded Antigen DetectionPrasanth GovindanNessuna valutazione finora
- CH 5 SaladinDocumento95 pagineCH 5 Saladinalphabennydelta4468100% (1)
- FC Ophth (SA) Regulations 18-3-2019Documento27 pagineFC Ophth (SA) Regulations 18-3-2019RichardNessuna valutazione finora
- The Variability in The Fungal Ribosomal DNA (Korabecna, 2007)Documento6 pagineThe Variability in The Fungal Ribosomal DNA (Korabecna, 2007)annisa pramestiNessuna valutazione finora
- Transport of Oxygen and Carbon DioxideDocumento39 pagineTransport of Oxygen and Carbon DioxideJayballabh KumarNessuna valutazione finora