Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Aortic Dissection
Caricato da
andreaDescrizione originale:
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
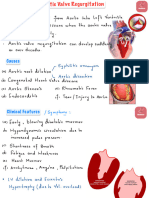
Aortic Dissection
Caricato da
andreaCopyright:
Formati disponibili
the most common catastrophe of the aorta
defn 2-3Xs more common than rupture of the abdominal aorta
1. bloods: Classification:
(i) Stanford classification:
- leukocytosis may be present - type A involves the ascending aorta
- Cr is elevated if dissection involves the renal arteries - type B does not involve the ascending aorta
- Trop is elevated if dissection has caused myocardial ischaemia (ii) DeBakey classification
- decreased Hb suggests leak or rupture - type I involves ascending aorta, arch & descending aorta
- a -ve D-dimer makes diagnosis very unlikely - type II is confined to the arch
- X-match - type III is confined to the descending aorta distal to the left subclavian artery
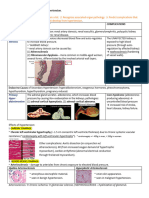
Pathophysiology:
2. imaging: aetiology - breakdown of collagen, elastin and smooth muscle (cystic medial necrosis) occurs
with aging, occlusive atherosclerosis of the vasavasorum & Marfan syndrome
(i) plain radiography
- mediastinal widening of greater than 8cm on AP chest radiograph Risk factors:
- blunted aortic knuckle (i) CT disorders (Marfans, Ehlers-Danlos, adult polycystic kidney disease)
- ring sign (displacement of aorta >5mm past calcified intima is specific) (ii) vascular disease risk factors (smoking, hypertension, dylipidaemia)
- left apical cap (iii) structural anomalies (bicuspid aortic valve, coarctation)
- tracheal deviation (iv) pregnancy increases risk
- deviation of the left mainstem bronchus (v) syphillus
- oesophageal deviation (vi) recent cardiac catherisation increases risk of iatrogenic dissection
- loss of paratracheal stripe investigation
(ii) CT aortogram 1. chest pain is the most frequent presenting complaint:
- advantages are that it details the anatomy and helps surgical planning - may be ripping or tearing in nature
- pain may migrate
- disadvantages are transport of unstable patient out of ED, need for
contrast often with impaired renal function
aortic - chest pain is of sudden onset (a key feature in distinguishing it from ischaemic pain)
dissection - maximal at onset
- location of pain may indicate where the dissection arises (anterior chest pain is
(iii) echocardiography
- TTE is good for evaluating AR and tamponade; it is less senstive than CT [created by associated with anterior dissection & may result in part from coronary occlusion;
- TOE is advantageous because patient does not need to be transported jaw or neck pain occurs with extension into the great vessels; interscapular pain
& because it detects involvement of the coronaries, AR & tamponade; it Paul Young occurs with dissection of the descending aorta)
can give false positives and false negatives due to fact upper ascending
02/10/07] symptoms 2. other presenting symptoms include:
aorta and arch may not be well visualised - neurological symptoms
- syncope
(iv) MRI and angiography - altered mental status
- limb paraesthesias, pain or weakness
3. ECG: - dyspnoea (from tracheobronchial compression)
- ST elevation occurs with coronary involvement - dysphagia (from oesophageal compression)
- right coronary dissects most commonly - orthopnoea
- flank pain if the renal artery is involved
- dyspnoea and haemoptusis if the dissection ruptures into the pleura
1. Oxygen & large bore iv access
2. Pain relief
3. Initiate aggressive management of heart rate 1. Blood pressure:
& blood pressure (HR<60-80 & BP <100-120 systolic) treatment - may increase or decrease
4. urgent surgical intervention is indicated for type A dissection - hypotension is an ominous sign and may result from excessive vagal
5. type B dissection may be managed surgically, radiologically or medically tone, cardiac tamponade or hypovolaemia from rupture of dissection
- 20mmHg differential in an independent predictor of aortic dissection
2. Neurological deficits:
- mortality is 1-2% per hour for the first 24-48 hours - peripheral nerve ischaemia can cause numbness & tingling in the extremities
- untreated 33% die in 24hrs, 50% within 48hrs & mortality approaches
signs - hoarseness from recurrent laryngeal nerve compression has been described
disposition - Horners syndrome
75% in patients with undiagnosed ascending aortic dissection 3. SVC syndrome
initial consultation with cardiology & later with cardiothoracic surgeon - may occur from compression of SVC by aorta
4. cardiac tamponade
5. new diastolic murmur
6. assymetrical pulses (carotid, brachial and femoral)
7. findings of haemothorax if ruptures
Potrebbero piacerti anche
- Arterial Diseases 2010Documento25 pagineArterial Diseases 2010viKиҼswAяAи LiиGaMNessuna valutazione finora
- Carotid Artery DiseaseDocumento48 pagineCarotid Artery DiseaseAdeleye John AdebolaNessuna valutazione finora
- Vascular Vascular: Medicine (ST George's Hospital Medical School) Medicine (ST George's Hospital Medical School)Documento7 pagineVascular Vascular: Medicine (ST George's Hospital Medical School) Medicine (ST George's Hospital Medical School)shravaniNessuna valutazione finora
- Thoracic Aortic AneurysmsDocumento4 pagineThoracic Aortic AneurysmsJoan Melissa SomeraNessuna valutazione finora
- Aortic Dissection Gary 2009Documento22 pagineAortic Dissection Gary 2009Ciubuc AndrianNessuna valutazione finora
- Chest Radio 8 Widening of The MediastinumDocumento14 pagineChest Radio 8 Widening of The Mediastinumlonsilord17Nessuna valutazione finora
- 1 AneurysmDocumento5 pagine1 AneurysmAhmed AdelNessuna valutazione finora
- Echocardiography in The Emergency Assessment of Acute Aortic SyndromesDocumento9 pagineEchocardiography in The Emergency Assessment of Acute Aortic SyndromesDumitru GrozaNessuna valutazione finora
- Definition of Stroke: Risk FactorsDocumento12 pagineDefinition of Stroke: Risk FactorsNik Fatnin YusoffNessuna valutazione finora
- Peripheral Vascular Medicine - Dr. Deduyo PDFDocumento14 paginePeripheral Vascular Medicine - Dr. Deduyo PDFMedisina101Nessuna valutazione finora
- Week 10 - Hypertension, Atherosclerosis, ArrhythmiaDocumento14 pagineWeek 10 - Hypertension, Atherosclerosis, Arrhythmiashivani patel100% (1)
- CVD CSDTDocumento3 pagineCVD CSDTrazeebhasssanNessuna valutazione finora
- Differential Diagnosis of StrokeDocumento2 pagineDifferential Diagnosis of StrokeAnonymous 7dsX2F8nNessuna valutazione finora
- Aortic Dimension & The Risk of DissectionDocumento6 pagineAortic Dimension & The Risk of Dissectionraghesh VNessuna valutazione finora
- Rido, Rudini - Disease of Aorta and Trauma To The AortaDocumento114 pagineRido, Rudini - Disease of Aorta and Trauma To The AortaFikriYTNessuna valutazione finora
- Aortic DissectionDocumento49 pagineAortic DissectionAnonymous ZUaUz1wwNessuna valutazione finora
- Aortic Dissection (Schwartz's 11 Ed.) Pathology and Classification Causes and Clinical HX Clinical Manifestations Diagnostic Evaluation TreatmentDocumento3 pagineAortic Dissection (Schwartz's 11 Ed.) Pathology and Classification Causes and Clinical HX Clinical Manifestations Diagnostic Evaluation TreatmentSean Dominique Cruz MaghinayNessuna valutazione finora
- Heart - PathologyDocumento22 pagineHeart - Pathologyjmosser100% (1)
- Intramural Hematoma: Journal of Cardiothoracic and Vascular AnesthesiaDocumento22 pagineIntramural Hematoma: Journal of Cardiothoracic and Vascular AnesthesiaRomeo GuevaraNessuna valutazione finora
- Vascular Sugergy Questions NasirDocumento19 pagineVascular Sugergy Questions NasirAhmad SobihNessuna valutazione finora
- Aortic Dissection AtfDocumento8 pagineAortic Dissection AtfAmir mohammad moori MohammadiNessuna valutazione finora
- Diseases of The Aorta - Dr. Deduyo PDFDocumento11 pagineDiseases of The Aorta - Dr. Deduyo PDFMedisina101Nessuna valutazione finora
- Cvspa04 Ihd and MiDocumento8 pagineCvspa04 Ihd and MiRobert So JrNessuna valutazione finora
- Z. Tume?: Used To Diagnose Injury After Both Blunt andDocumento3 pagineZ. Tume?: Used To Diagnose Injury After Both Blunt andNyx UlricNessuna valutazione finora
- Mesenteric Ischaemia:: Diffusely DilatedDocumento1 paginaMesenteric Ischaemia:: Diffusely DilatedJason HarryNessuna valutazione finora
- Aortic Dissection AneurysmsDocumento32 pagineAortic Dissection Aneurysmsأبوأحمد الحكيمNessuna valutazione finora
- Cardiovascular Pathology - 029) Peripheral Arterial Disease (Notes)Documento11 pagineCardiovascular Pathology - 029) Peripheral Arterial Disease (Notes)Geraldine HernandezNessuna valutazione finora
- Acute Ischemic Stroke: Etiology, Pathophysiology, Clinical Features, Diagnostics, TreatmentDocumento7 pagineAcute Ischemic Stroke: Etiology, Pathophysiology, Clinical Features, Diagnostics, TreatmentAfrah AbdulNessuna valutazione finora
- E363 FullDocumento4 pagineE363 FullRamadhyanNessuna valutazione finora
- Acute Limb Ischemia SiteDocumento23 pagineAcute Limb Ischemia Sitebenypermadi100% (1)
- Acute Aortic Disecccion Type ADocumento15 pagineAcute Aortic Disecccion Type AAnonymous envUOdVNessuna valutazione finora
- Aortic DissectionDocumento59 pagineAortic DissectionDwi Gunawan Fardhani100% (1)
- Chest TraumaDocumento63 pagineChest Traumatesfayegermame95.tgNessuna valutazione finora
- Overview of NeuroangiographyDocumento9 pagineOverview of Neuroangiographynaren_winv1350Nessuna valutazione finora
- Semiology of Vessels ImagingDocumento52 pagineSemiology of Vessels ImagingSothearith ThenNessuna valutazione finora
- Surgery Reviosn NotesDocumento41 pagineSurgery Reviosn Noteshy7tn100% (1)
- 2 - Vascular InjuryDocumento6 pagine2 - Vascular Injuryمحمد عماد عليNessuna valutazione finora
- Aneurysms Copy 2Documento74 pagineAneurysms Copy 2Konstantin DimitrovNessuna valutazione finora
- Linician Pdate: Acute Aortic DissectionDocumento18 pagineLinician Pdate: Acute Aortic DissectionBagus DikaNessuna valutazione finora
- Acute Limb Ischemia and VasculitisDocumento6 pagineAcute Limb Ischemia and VasculitisnivraeNessuna valutazione finora
- TRP Surgery Study GuideDocumento27 pagineTRP Surgery Study GuidekatNessuna valutazione finora
- (02.19) SU Tumors of The Heart (TG3) - Final - Jan Matthew TolentinoDocumento5 pagine(02.19) SU Tumors of The Heart (TG3) - Final - Jan Matthew TolentinoMikmik DGNessuna valutazione finora
- Medad Note of Orthopedics SpecialityDocumento34 pagineMedad Note of Orthopedics SpecialityAtef FahmyNessuna valutazione finora
- Congenital Heart DefectsDocumento6 pagineCongenital Heart DefectsJohiarra Madanglog TabigneNessuna valutazione finora
- Aortic DissectionDocumento2 pagineAortic DissectionTiffney NesakumarNessuna valutazione finora
- Distal To Ligament of Treitz: CausesDocumento8 pagineDistal To Ligament of Treitz: CausesKiara GovenderNessuna valutazione finora
- PAD vs. DVTDocumento3 paginePAD vs. DVTKrystel BatinoNessuna valutazione finora
- Pulsating Abdominal MassDocumento9 paginePulsating Abdominal MasshalesNessuna valutazione finora
- Evar 9Documento1 paginaEvar 9Amor KourdouliNessuna valutazione finora
- Surgery II: Congenital Heart DiseaseDocumento10 pagineSurgery II: Congenital Heart DiseaseRea Dominique CabanillaNessuna valutazione finora
- Aortic Valve RegurgitationDocumento3 pagineAortic Valve Regurgitationprakash ramNessuna valutazione finora
- 220pm - Acute Aortic SyndromesDocumento17 pagine220pm - Acute Aortic SyndromesHARBENNessuna valutazione finora
- Talley Sum Up ExaminationDocumento57 pagineTalley Sum Up ExaminationGroup 14Nessuna valutazione finora
- Left Ventricular Diverticulum in Association With Bicuspid Aortic Valve and Pseudocoarctation: Hitherto Unreported AssociationDocumento3 pagineLeft Ventricular Diverticulum in Association With Bicuspid Aortic Valve and Pseudocoarctation: Hitherto Unreported AssociationIsabella María GantivarNessuna valutazione finora
- Imaging of Cardiovascular Thoracic Emergencies Acute Aortic Syndrome and Pulmonary EmbolismDocumento8 pagineImaging of Cardiovascular Thoracic Emergencies Acute Aortic Syndrome and Pulmonary EmbolismAlejandro ColombanoNessuna valutazione finora
- Cardiovascular Dysfunction: (Patent Ductus Arteriosus)Documento6 pagineCardiovascular Dysfunction: (Patent Ductus Arteriosus)Jc MacujaNessuna valutazione finora
- Surgical Recall Vascular SurgeryDocumento28 pagineSurgical Recall Vascular SurgeryAltariaNessuna valutazione finora
- Chapter 41 - Thoracic Outlet Syndrome SynonymsDocumento8 pagineChapter 41 - Thoracic Outlet Syndrome SynonymsPiero Massafra100% (1)
- Correlation of Arterial Blood Gas Measurements With Venous Blood Gas Values in Mechanically Ventilated PatientsDocumento6 pagineCorrelation of Arterial Blood Gas Measurements With Venous Blood Gas Values in Mechanically Ventilated PatientsandreaNessuna valutazione finora
- Acute Renal Failure and CovidDocumento9 pagineAcute Renal Failure and CovidandreaNessuna valutazione finora
- Jaha 121 022694Documento36 pagineJaha 121 022694andreaNessuna valutazione finora
- Prokalsitonin in CovidDocumento22 pagineProkalsitonin in CovidandreaNessuna valutazione finora
- AF PredictorDocumento9 pagineAF PredictorandreaNessuna valutazione finora
- SlideKit STEMI TreatmentDocumento71 pagineSlideKit STEMI TreatmentandreaNessuna valutazione finora
- CardiologyDocumento11 pagineCardiologyandreaNessuna valutazione finora
- Chest PainDocumento13 pagineChest PainandreaNessuna valutazione finora
- Association Between Coronary Dominance and Acute Inferior Myocardial Infarction: A Matched, Case-Control StudyDocumento7 pagineAssociation Between Coronary Dominance and Acute Inferior Myocardial Infarction: A Matched, Case-Control StudyandreaNessuna valutazione finora
- ECG Patterns of Isolated RightDocumento5 pagineECG Patterns of Isolated RightandreaNessuna valutazione finora
- Muchtar Nora Ismail SiregarDocumento15 pagineMuchtar Nora Ismail SiregarandreaNessuna valutazione finora
- Blood Supply of The HeartDocumento1 paginaBlood Supply of The HeartandreaNessuna valutazione finora
- Case PediatriDocumento41 pagineCase PediatriandreaNessuna valutazione finora
- Antenatal Therapy For Fetal Supraventricular TachyarrhythmiasDocumento14 pagineAntenatal Therapy For Fetal Supraventricular TachyarrhythmiasandreaNessuna valutazione finora
- NTSEMI and Unstable Angina ANdreaDocumento17 pagineNTSEMI and Unstable Angina ANdreaandreaNessuna valutazione finora
- Morning Report: Supervisor: Dr. Rusdhy A.H., SP - OG Medical StudentsDocumento8 pagineMorning Report: Supervisor: Dr. Rusdhy A.H., SP - OG Medical StudentsEra MoetzNessuna valutazione finora
- Biofeedback 2000x-Pert Hardware ManualDocumento45 pagineBiofeedback 2000x-Pert Hardware ManualNery BorgesNessuna valutazione finora
- Fracture of Shoulder and Upper Arm S42Documento9 pagineFracture of Shoulder and Upper Arm S42yunitaNessuna valutazione finora
- 3-Gmc Claim Form HDFC ErgoDocumento3 pagine3-Gmc Claim Form HDFC ErgoDT worldNessuna valutazione finora
- Anatomy & Physiology Unit 1Documento29 pagineAnatomy & Physiology Unit 1Priyanjali SainiNessuna valutazione finora
- Raasn October NewsletterDocumento6 pagineRaasn October Newsletterapi-231055558Nessuna valutazione finora
- All PackageRates (ABPMJAY) PDFDocumento300 pagineAll PackageRates (ABPMJAY) PDFSumit Soni0% (1)
- Unani Product List PDFDocumento109 pagineUnani Product List PDFAK50% (2)
- Ruppels Manual of Pulmonary Function Testing 11th EditionDocumento61 pagineRuppels Manual of Pulmonary Function Testing 11th Editiondanny.johnson566100% (43)
- Author 'S Accepted ManuscriptDocumento24 pagineAuthor 'S Accepted ManuscriptAgal BimaNessuna valutazione finora
- LHPCDocumento23 pagineLHPCChristine AzmiNessuna valutazione finora
- The Performance Wellness SeminarDocumento8 pagineThe Performance Wellness SeminarMirelaAlexandraNessuna valutazione finora
- PACS Basics PDFDocumento6 paginePACS Basics PDFBalaji BalasubramanianNessuna valutazione finora
- The Antimicrobial ActivitiesDocumento4 pagineThe Antimicrobial ActivitiesromalfioNessuna valutazione finora
- Hospital Requirement-FinalDocumento9 pagineHospital Requirement-FinalPrasanna Ramasamy100% (1)
- Callyspongia SP Callyspongia SP: Identification of Antioxidant Compounds in The Sponge The SpongeDocumento7 pagineCallyspongia SP Callyspongia SP: Identification of Antioxidant Compounds in The Sponge The SpongeZulfajriNessuna valutazione finora
- Sido Muncul Value Chain - Final10112021Documento16 pagineSido Muncul Value Chain - Final10112021Hezekiah PardedeNessuna valutazione finora
- TRIKATUDocumento5 pagineTRIKATUAngshuman DuttaNessuna valutazione finora
- Microbiology Case Study Pneumonia EpidemidimiologyDocumento4 pagineMicrobiology Case Study Pneumonia EpidemidimiologyArguend0Nessuna valutazione finora
- Psych 2012123115115620Documento6 paginePsych 2012123115115620Rara QamaraNessuna valutazione finora
- Autoimmune Mash - Up FinalDocumento38 pagineAutoimmune Mash - Up Finalapi-546809761Nessuna valutazione finora
- Operative Hand InstrumentsDocumento22 pagineOperative Hand InstrumentsSharad Banker50% (2)
- Autonomic Control of The Heart Cardiovascular Reflexes Student Version (7) - 2Documento27 pagineAutonomic Control of The Heart Cardiovascular Reflexes Student Version (7) - 2Mohammed MoghavelehNessuna valutazione finora
- Pest ControlDocumento8 paginePest ControlFirst Last100% (1)
- What Are Thrombosed External Hemorrhoids?Documento3 pagineWhat Are Thrombosed External Hemorrhoids?Hanine HassanNessuna valutazione finora
- Welcome To The Celestial Biolabs LimitedDocumento8 pagineWelcome To The Celestial Biolabs LimitedsaahilsinghiNessuna valutazione finora
- Pathfinder 2nd Edition House Rules Compendium - GM BinderDocumento119 paginePathfinder 2nd Edition House Rules Compendium - GM BinderBrandon PaulNessuna valutazione finora
- Felicias Resume 1Documento1 paginaFelicias Resume 1api-357153848Nessuna valutazione finora
- Teaching Plan About Conjunctivitis: Haemophilus InfluenzaeDocumento3 pagineTeaching Plan About Conjunctivitis: Haemophilus InfluenzaeJanaica Juan100% (1)