Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
JR 6
Caricato da
Yuni Purnama SariCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
JR 6
Caricato da
Yuni Purnama SariCopyright:
Formati disponibili
Cesarean Delivery: Original Research
Prophylactic Negative Pressure Wound
Therapy and Wound Complication After
Cesarean Delivery in Women With Class II or
III Obesity
A Randomized Controlled Trial
Downloaded from https://journals.lww.com/greenjournal by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3tjcLwhL8g9bZhhig7WeJvpXMcGkffmpkCgxIkNX8Hm0= on 10/09/2018
Kristina A. Wihbey, MD, Ellen M. Joyce, MD, Zachary T. Spalding, MD, Hayley J. Jones, MD,
Todd A. MacKenzie, PhD, Rebecca H. Evans, MD, June L. Fung, PhD, Marlene B. Goldman, MS, ScD,
and Elisabeth Erekson, MD, MPH
OBJECTIVE: To compare the occurrence of superficial months, an interim analysis for futility was conducted
surgical site infections in obese women using prophy- and the decision was made to halt the study.
lactic negative pressure therapy with standard dressings RESULTS: Women were recruited between January 5,
after cesarean delivery. 2015, and January 7, 2017, from two sites. The mean BMI
Methods: We conducted a randomized controlled, non- on admission was 44.9 (68) for the prophylactic negative
blinded, two-center study of prophylactic negative pres- wound therapy group and 43.4 (67) for the standard dress-
sure therapy compared with standard surgical dressings ing group. There were no differences in the occurrence of
placed at the time of primary closure at cesarean delivery observed superficial surgical site infections between
in obese women with body mass indexes (BMI) of 35 or women using prophylactic negative pressure wound ther-
higher (ie, class II and III obesity). Our primary outcome apy (12/80 [15%]) compared with women who received the
was occurrence of a superficial surgical site infection. We standard dressing (8/81 [10%], P5.35, relative risk 1.52, 95%
assumed a superficial surgical site infection occurrence CI 0.66–3.52). There were no differences in the occurrence
rate of 20% and intended to recruit 400 women. of composite wound complications between women using
However, after low enrollment of 166 women over 24 prophylactic negative pressure wound therapy (25/80
[31%]) compared with women who received the standard
From the Departments of Obstetrics and Gynecology and Biomedical Data dressing (24/81 [30%], P5.87).
Science and the Dartmouth Institute for Health Policy and Clinical Practice, the
Geisel School of Medicine at Dartmouth, Lebanon, New Hampshire.
CONCLUSION: In this randomized controlled trial that
did not achieve full anticipated enrollment, we did not
The devices used in this study were provided by an unrestricted research grant
from KCI Medical (San Antonio, Texas). KCI Medical had no role in the study observe a decrease in superficial surgical site infections
design, data collection, or data analysis. Final results of the study were shared after cesarean delivery in obese women with the use of
with the company before manuscript submission; however, the investigators were prophylactic negative pressure wound therapy.
not bound to incorporate KCI’s comments. The authors’ decision as to what the
manuscript contained was final. CLINICAL TRIAL REGISTRATION: ClinicalTrials.gov,
Each author has indicated that he or she has met the journal’s requirements for NCT02390401.
authorship. (Obstet Gynecol 2018;132:377–84)
Received February 6, 2018. Received in revised form May 4, 2018. Accepted May DOI: 10.1097/AOG.0000000000002744
15, 2018.
Corresponding author: Kristina A. Wihbey, MD, Department of Obstetrics and
Gynecology, The Geisel School of Medicine at Dartmouth, 189 N Main Street,
Concord, NH 03301; email: kwihbey@crhc.org.
T he prevalence of obesity (defined as body mass
index [BMI, calculated as weight (kg)/[height
(m)]2] 30 or higher) continues to increase, affecting
Financial Disclosure
The authors did not report any potential conflicts of interest. approximately 40% of adult females in the United
© 2018 by the American College of Obstetricians and Gynecologists. Published
States according to Centers for Disease Control and
by Wolters Kluwer Health, Inc. All rights reserved. Prevention 2013–2014 statistics.1 Obesity has a signif-
ISSN: 0029-7844/18 icant effect on many aspects of pregnancy, including
VOL. 132, NO. 2, AUGUST 2018 OBSTETRICS & GYNECOLOGY 377
Copyright ª by the American College of Obstetricians
and Gynecologists. Published by Wolters Kluwer Health, Inc.
Unauthorized reproduction of this article is prohibited.
increased need for cesarean delivery. In addition, obe- Control and Prevention using prophylactic negative
sity is a well-recognized risk factor for the develop- pressure wound therapy compared with standard
ment of postoperative surgical site infections and dressings after cesarean delivery.
other wound complication.2,3 In the late 1990s, Tran
et al4 found a 9.8% surgical site infection rate among MATERIALS AND METHODS
obese women after cesarean delivery with risk of We conducted a randomized controlled, nonblinded,
infection doubling for every five-unit increment of multicenter study of prophylactic negative pressure
BMI. wound therapy compared with standard surgical
Prophylactic negative pressure wound therapy dressings placed at the time of primary closure in
as a means of reducing wound infection has been a cesarean delivery. Institutional review board
explored as primary dressings in the orthopedic and approval was obtained from the Dartmouth Commit-
cardiothoracic fields, but limited data have been tee for the Protection of Human Subjects on April 21,
published in the peer-reviewed literature report on 2015 (#00005211) and from the Southern New
use with abdominal incisions. Two meta-analyses Hampshire Medical Center Clinical Trials Office
recently combined published peer-reviewed manu- (#2015-01). This trial was registered with clinical-
scripts, meeting abstracts, and data published on trials.gov (Clinical Trial Registration:
intranet websites to determine the effectiveness of NCT02390401). Women were recruited and con-
prophylactic negative pressure wound therapy at sented to participate in this study before the onset of
the time of cesarean delivery.5,6 Unfortunately, active labor during any routine prenatal visit or inpa-
these two meta-analyses reported conflicting data tient admission.
on the effectiveness of prophylactic negative Women were recruited from two hospitals,
pressure. Dartmouth-Hitchcock Medical Center (a rural tertiary
Therefore, the objective of this randomized con- care center with a level III neonatal intensive care
trolled trial was to compare the occurrence of unit) and Southern New Hampshire Medical Center
superficial surgical site infections in women with class (a community-based hospital with a level II neonatal
II or III obesity as defined by the Centers for Disease intensive care unit).
Fig. 1. Flow diagram.
Wihbey. Prophylactic Negative Pressure Wound Therapy. Obstet Gynecol 2018.
378 Wihbey et al Prophylactic Negative Pressure Wound Therapy OBSTETRICS & GYNECOLOGY
Copyright ª by the American College of Obstetricians
and Gynecologists. Published by Wolters Kluwer Health, Inc.
Unauthorized reproduction of this article is prohibited.
Women were eligible for inclusion if they under- Table 1. Demographics and Characteristics of
went cesarean delivery for a viable neonate and their Participating Women
BMI on admission to the labor and delivery floor was
35 or higher. All women undergoing cesarean deliv- NPWT Standard
Dressing Dressing
ery were eligible for inclusion. Women were ap- Characteristic (n580) (n586)
proached only for participation and consent in this
study before active labor Additionally, women who Site
were younger than 18 years old, did not speak A 64 (80) 72 (84)
B 16 (20) 14 (16)
English, had an allergy to silver or adhesives products,
Maternal characteristics
or who had a skin incision that would not fit the Maternal age (y) 31.066 30.265
device or standard dressing (eg, “T” skin incision) Race
were excluded. White 76 (99) 81 (99)
Abdominal preparation for cesarean delivery was Black 1 (1) 0 (0.0)
Other 0 (0) 1 (1)
performed with 2% chlorhexidine alcohol solution.
Ethnicity
All women received intravenous antibiotics before Hispanic 2 (2) 0 (0)
skin incision consistent with American College of Parity
Obstetricians and Gynecologists’ guidelines7 with the 1 20 (25) 34 (40)
majority of women receiving cefazolin or clindamycin 2 37 (46) 23 (27)
3 18 (23) 23 (27)
with gentamicin if allergic. Surgical techniques were
4 or more 5 (6) 6 (7)
left to the discretion of the surgeon. Women were Gestational age (wk)
discharged postoperatively by the primary team, usu- 28 or less 1 (1) 3 (3)
ally on the third or fourth postoperative day, irrespec- Greater than 28–37 21 (29) 17 (22)
tive of study assignment. All women were scheduled Greater than 37–42 51 (70) 59 (74)
Greater than 42 0 (0) 0 (0)
to return for a wound assessment on postoperative
Multiple gestation 4 (5) 5 (6)
day 5–7. Prior cesarean deliveries
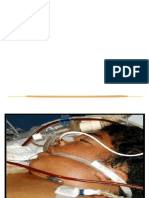
If randomized to prophylactic negative pressure 0 38 (48) 44 (51)
wound therapy, the device was applied at the time of 1 33 (41) 30 (35)
primary skin closure at cesarean delivery. It was 2 7 (9) 11 (13)
3 or more 2 (3) 1 (1)
placed over the closed surgical incision under sterile
BMI (kg/m2) 44.968 43.467
conditions and was removed between postoperative BMI category (kg/m2)
day 5 and 7 at the time of incision check. 35–40 30 (38) 31 (38)
The standard dressing after cesarean delivery was Higher than 40 to 50 31 (39) 40 (49)
also applied using a sterile technique. If subcuticular Higher than 50 19 (24) 15 (19)
Preoperative hct (%) 30.4610 31.369
closure was used, sterile slim adhesive strips (also
Preoperative anemia (hct less than 58 (73) 54 (63)
known as Steri-Strips) were applied. For both sub- 36%)
cuticular and staple closure, the dressing consisted of Antenatal steroids 8 (10) 11 (13)
a sterile nonadherent wound dressing (also known as Diabetes mellitus
Telfa), a sterile gauze, and a waterproof transparent Type I diabetes mellitus 1 (1) 1 (1)
Type II diabetes mellitus 9 (12) 4 (5)
adhesive dressing (also known as Tegaderm). The
Gestational diabetes mellitus 11 (15) 20 (25)
standard dressing was removed on postoperative day Hypertension
2. Chronic hypertension 6 (8) 4 (5)
A randomization program (www.randomization. Gestational hypertension 6 (8) 3 (4)
com, Alberta, Canada) was used to generate sealed Preeclampsia with severe features 6 (8) 9 (11)
Current smoker 14 (18) 13 (15)
opaque envelopes with study assignment. Women
were randomized at the conclusion of the cesarean NPWT, prophylactic negative pressure wound therapy; BMI, body
mass index; hct, hematocrit.
delivery, during skin closure, when the envelopes Data are n (%) or mean6SD.
were opened by a circulating operating room nurse.
Two randomization strata were created using per-
muted blocks with varying block sizes for women with Our primary outcome was occurrence of super-
BMIs from 35 to less than 40 and women with BMIs ficial surgical site infection, defined according to
of 40 or higher and for each site to ensure equal dis- Centers for Disease Control and Prevention criteria8
tribution of study allocation across these two separate as infection involving only the skin or subcutaneous
BMI categories and sites. tissue occurring within 30 days of surgery with at least
VOL. 132, NO. 2, AUGUST 2018 Wihbey et al Prophylactic Negative Pressure Wound Therapy 379
Copyright ª by the American College of Obstetricians
and Gynecologists. Published by Wolters Kluwer Health, Inc.
Unauthorized reproduction of this article is prohibited.
Table 2. Intrapartum and Intraoperative Characteristics of Participating Women
Intrapartum Event NPWT Dressing (n580) Standard Dressing (n586)
Reason for admission to labor and delivery
Spontaneous labor 51 (65) 54 (65)
Induction of labor 18 (23) 22 (27)
Scheduled cesarean delivery 9 (12) 7 (8)
Duration of rupture of membranes (min) 2116407 2266440
Duration of rupture of membranes (h)
Less than 18 74 (93) 76 (88)
18 or more 6 (8) 10 (12)
Chorioamnionitis 1 (1) 0 (0)
Intraoperative variables
Operative time (incision to stop, min) 82.3625 80.4623
Type of anesthesia
Spinal–epidural 71 (89) 79 (93)
General 9 (11) 6 (7)
Skin incision
Pfannenstiel 55 (86.0) 68 (93.2)
Vertical midline 9 (14) 5 (7)
Skin closure
Subcuticular 58 (91) 67 (93)
Staples 6 (9) 5 (7)
Estimated blood loss (mL) 9366253 9666318
Postpartum hemorrhage (greater than 1,000 mL) 38 (48) 39 (45)
Intraoperative blood transfusion 0 (0) 3 (4)
Maternal procedures with delivery
Tubal ligation 29 (36) 21 (24)
Peripartum hysterectomy 0 (0) 0 (0)
NPWT, prophylactic negative pressure wound therapy.
Data are n (%) or mean6SD.
one of the following: 1) purulent drainage from the distributions were used as appropriate. We first com-
wound or 2) organism identified by culture or wound pleted an observed outcome analysis based on
deliberately opened by the surgeon. Patients also observed outcomes for the women who completed
needed to have at least one of the following symp- their 1-week postoperative incision check. We then
toms: pain, swelling, or erythema. Our secondary calculated an unadjusted relative risk and 95% CI for
outcome was a composite wound complication, the primary outcome. We then completed a second
including superficial, deep, or organ-space surgical outcome analysis for all women who were random-
site infection; wound dehiscence; seroma; or hema- ized and received their intended treatment despite
toma that occurred within 30 days of surgery. Other lack of follow-up at the 5- to 7- day incision check
secondary outcomes included 30-day readmission, by imputing missing data. We assumed that all
30-day reoperation, and need for antibiotic treatment women who were lost to follow-up had developed
for any reason (eg, mastitis, urinary tract infection, superficial surgical site infections. For the secondary
pyelonephritis). We also examined length of stay outcome of composite wound complication, we
after cesarean delivery and rates of breastfeeding at assumed that complications that would not require
discharge this seems to have been erroneously dupli- readmission happened (eg, seroma, hematoma, or
cated. We had already stated this earlier in the text. wound dehiscence) and we assumed that complica-
Additional outcomes were determined by chart tions that would generally require inpatient readmis-
review. sion did not happen (eg, deep surgical site infections
Standard statistical methods such as frequency or organ-space surgical site infections). Finally, we
distributions and measures of central tendency were conducted two subgroup analyses of women with
used to evaluate the demographic and clinical BMIs of 40 to 50 and BMIs of 50 or higher to see
characteristics of the participants. Pearson x2, Fisher whether these groups had differences in superficial
exact test, and Student t test for parametric distrib- surgical site infections not observed in the larger
uted variables and Kruskal-Wallis for nonparametric cohort.
380 Wihbey et al Prophylactic Negative Pressure Wound Therapy OBSTETRICS & GYNECOLOGY
Copyright ª by the American College of Obstetricians
and Gynecologists. Published by Wolters Kluwer Health, Inc.
Unauthorized reproduction of this article is prohibited.
Table 3. Occurrence of Postoperative Complications
Intention-to-Treat Observed Assumed Superficial SSI if
Outcomes Lost to Follow-up
NPWT Dressing Standard Dressing Standard Dressing
Complication (n580) (n581) P (n586) P
Superficial SSI 12 (15) 8 (10) .35 13 (15) .98
Composite wound complication 25 (31) 24 (30) .87 29 (34) .73
Deep SSI 0 (0) 0 (0) — 0 (0) —
Organ SSI 1 (1) 4 (5) .37 4 (5) .37
Seroma 7 (9) 6 (7) .78 11 (13) .46
Hematoma 2 (3) 4 (5) .68 9 (11) .06
Wound dehiscence 14 (18) 13 (16) .84 13 (15) .83
Readmission 3 (4) 5 (6) .72 5 (6) .72
Reoperation 1 (1) 1 (1) 1.00 1 (1) 1.00
Antibiotic treatment
SSI (superficial, deep, organ- 14 (18) 10 (12) .39 17 (20) 1.00
space)
UTI 1 (1) 2 (3) 1.00 7 (8) .17
Pyelonephritis 0 (0.0) 0 (0) 5 (6) .06
Mastitis 0 (0) 0 (0) 5 (6) .06
Hospital length of stay (d) 3.2 (3–4) 3.2 (2–4) .51 3.2 (2–4) .51
Breastfeeding at discharge 52 (65) 63 (73) .31 63 (73) .31
SSI, surgical site infection; NPWT, negative pressure wound therapy; UTI, urinary tract infection.
Data are n (%) or median (interquartile range) unless otherwise specified.
Composite wound complication includes superficial SSI, deep SSI, organ-space SSI, seroma, hematoma, or wound dehiscence. If lost to
follow-up, women were assumed to have developed superficial SSI, seroma, and hematoma. Conditions that required hospitalization
(eg, deep SSI, organ-space SSI, and wound dehiscence) were assumed not to have occurred in women lost to follow-up.
At the time of study initiation (April 2015), based infection, as predicted in the original sample size
on the current literature, we assumed an occurrence of calculation (20% superficial surgical site infection in
superficial surgical site infection of 20% of obese women with standard dressing and 10% in women
women undergoing cesarean delivery.4,9,10 We deter- with prophylactic negative pressure wound therapy),
mined that 400 women (200 prophylactic negative our study’s power to detect a difference between the
pressure wound therapy, 200 standard dressing) two interventions would be 29% at completion of
would need to be recruited to have an 80% power enrollment of our 400 participants. If we assumed that
to detect a 50% decrease in superficial surgical site the primary outcome in the remaining 244 women
infection (assuming P,.05). We anticipated that would be the same as prevalence observed in the first
enrollment across the two sites would take 24 months. 166 women who had already completed the study,
At the completion of the anticipated 2 years of our study’s power to detect a difference between the
recruitment, 166 women out of a planned 400 (42%) two interventions would be less than 0.1%. Therefore,
had been enrolled in the study. This was likely the the determination of the data safety monitoring board
result of the limitations of women’s ability to return was that continued enrollment to original recruitment
for device removal and incision evaluation 5–7 days targets was futile and the recommendation was made
after delivery (many had been transported to the ter- to halt further enrollment and disseminate our
findings.
tiary recruiting site and lived a long distance from this
site). As a result of this low enrollment, the study’s
data safety monitoring board recommended an RESULTS
unplanned interim analysis with futility calculation Women were recruited between January 5, 2015, and
to determine whether the study should continue. January 7, 2017. A total of 166 women were random-
We anticipated that to reach our original recruit- ized, 163 received their allocated treatment, and 161
ment goals, we would need to continue our study for (80 prophylactic negative pressure wound therapy and
34 additional months. If we assumed that observed 81 standard dressing) returned for their postoperative
outcomes in the remaining 244 women would wound assessment approximately 1 week after cesar-
develop the primary outcome, superficial surgical site ean delivery (Fig. 1). The two randomization groups
VOL. 132, NO. 2, AUGUST 2018 Wihbey et al Prophylactic Negative Pressure Wound Therapy 381
Copyright ª by the American College of Obstetricians
and Gynecologists. Published by Wolters Kluwer Health, Inc.
Unauthorized reproduction of this article is prohibited.
Table 4. Demographics and Clinical Characteristics of Women With Superficial Surgical Site Infection After
Cesarean Delivery (N5161)
Characteristic Superficial SSI (n520) No Superficial SSI (n5141) P
Group .32
Prophylactic negative pressure wound therapy 12 (60) 68 (48)
Standard dressing 8 (40) 73 (51)
Site .09
A 19 (95) 112 (79)
B 1 (5) 29 (21)
Maternal characteristics
Maternal age (y) 31.066 30.766 .85
Race .24
White 19 (95) 133 (99)
Black 1 (5) 0 (0)
Other 0 (0) 1 (1)
Ethnicity .23
Hispanic 1 (5) 1 (1)
Parity .66
1 9 (45) 43 (31)
2 6 (30) 53 (38)
3 4 (20) 36 (26)
4 or more 1 (5) 9 (6)
Gestational age (wk) .87
28 or less 0 (0) 4 (3)
Greater than 28–37 5 (28) 32 (25)
Greater than 37–42 13 (72) 93 (72)
Greater than 42 0 (0) 0 (0)
Gestational age (d) 261621 260624 .82
Prior cesarean deliveries .03
0 16 (80) 66 (47)
1 2 (10) 57 (40)
2 2 (10) 16 (11)
3 or more 0 (0) 2 (1)
BMI (kg/m2) 46.968 43.567 .06
BMI category (kg/m2) .02
35–40 3 (15) 58 (41)
Higher than 40 17 (85) 83 (59)
Preoperative serum hct (%) 34.866 30.2610 .04
Preoperative anemia (serum hct less than 36%) 9 (45) 101 (72) .02
Antenatal steroids 4 (20) 15 (11) .26
Diabetes mellitus .63
Type I diabetes mellitus 0 (0) 2 (2)
Type II diabetes mellitus 3 (16) 10 (8)
Gestation diabetes mellitus 3 (16) 27 (21)
Hypertension
Chronic hypertension 2 (10) 8 (6) .36
Gestational hypertension 1 (5) 8 (6) 1.00
Preeclampsia with severe features 2 (10) 13 (9) 1.00
Current smoker 3 (15) 23 (16) 1.00
Labor
Reason for admission labor and delivery .79
Spontaneous labor 12 (67) 83 (67)
Induction of labor 5 (28) 27 (22)
Scheduled cesarean delivery 1 (6) 14 (11)
Duration of rupture of membranes (min) 2726457 216 (425) .59
Duration of rupture of membranes (h) 1.00
Less than 18 18 (90) 127 (90)
18 or more 2 (10) 14 (10)
Chorioamnionitis present at the time of delivery 0 (0) 1 (1) 1.00
(continued )
382 Wihbey et al Prophylactic Negative Pressure Wound Therapy OBSTETRICS & GYNECOLOGY
Copyright ª by the American College of Obstetricians
and Gynecologists. Published by Wolters Kluwer Health, Inc.
Unauthorized reproduction of this article is prohibited.
Table 4. Demographics and Clinical Characteristics of Women With Superficial Surgical Site Infection After
Cesarean Delivery (N5161) (continued )
Characteristic Superficial SSI (n520) No Superficial SSI (n5141) P
Intraoperative variables
Fetal weight (g) 3,19261,088 3,1796971 .96
1-min Apgar score 6.563 7.262 .15
5-min Apgar score 8.661 8.461 .61
Operative time (min) 86.3628 80.7624 .33
Type of anesthesia .10
Spinal–epidural 16 (80) 129 (92)
General 4 (20) 11 (8)
Skin incision .21
Pfannenstiel 19 (100) 100 (89)
Vertical midline 0 (0) 13 (12)
Skin closure 1.00
Subcuticular 18 (95) 103 (92)
Staples 1 (5) 9 (8)
Estimated blood loss (mL) 9556309 9496289 .93
Postpartum hemorrhage (greater than 1,000 mL) 9 (45) 65 (46) 1.00
Intraoperative blood transfusion 0 (0) 3 (2) 1.00
Concomitant procedures 1.00
Tubal ligation 6 (30) 42 (30)
Peripartum hysterectomy 0 (0) 0 (0)
SSI, surgical site infection; BMI, body mass index; hct, hematocrit.
Data are n (%) or mean6SD.
were similar in regard to maternal characteristics and there were no differences in the occurrence of observed
intrapartum and intraoperative events (Tables 1 and 2). superficial surgical site infections in women using the
Twelve percent of women (20/161) completing prophylactic negative pressure wound therapy (21%
the 1-week incision check experienced superficial [4/19]) compared with women receiving standard dress-
surgical site infection. There were no statistically ings (20% [3/15], P..99).
significant differences in the occurrence of observed Risk factors for superficial surgical site infection
superficial surgical site infections between women are explored in Table 4. In addition to maternal BMI
using prophylactic negative pressure wound therapy category, number of prior cesarean deliveries and pre-
(12/80 [15%]) compared with women who received operative anemia (serum hematocrit less than 36%)
the standard dressing (8/81 [10%], P5.35; Table 3; were both associated with increased postcesarean
relative risk 1.52, 95% CI 0.66–3.52). Assuming that superficial surgical site infection (Table 4).
all women who were lost to follow-up developed There were no statistically significant differences
superficial surgical site infection, there still would observed for length of stay after delivery and breastfeed-
not have been a statistically significant difference in ing at the time of hospital discharge between women
the occurrence of superficial surgical site infection with prophylactic negative pressure wound therapy and
between groups (12/80 [15%] vs 13/86 [15%], P5.98). standard dressings. Fifteen percent of women (12/80)
There were no significant differences in the occur- with the prophylactic negative pressure wound therapy
rence of composite wound complications between device had it removed early: five women for local skin
women using prophylactic negative pressure wound irritation, six women because the pump stopped work-
therapy (25/80 [31%]) compared with women who ing, and one additional woman requested early removal.
received the standard dressing (24/81 [30%], P5.87).
In a subgroup analysis of the 71 women with BMIs of DISCUSSION
40 to 50, there were no statistically significant differences In this randomized controlled trial, we did not observe
observed in superficial surgical site infections in the a decrease in superficial surgical site infection after
women using the prophylactic negative pressure wound cesarean delivery in obese women with the use of
therapy (7/31 [23%]) compared with women receiving prophylactic negative pressure wound therapy. Even in
standard dressings (7/40 [18%], P5.77). In a subgroup a subgroup analysis of morbidly obese (BMI of 40 to 50)
analysis of the 34 women with BMIs higher than 50, and the most obese women (BMI higher than 50), who
VOL. 132, NO. 2, AUGUST 2018 Wihbey et al Prophylactic Negative Pressure Wound Therapy 383
Copyright ª by the American College of Obstetricians
and Gynecologists. Published by Wolters Kluwer Health, Inc.
Unauthorized reproduction of this article is prohibited.
are considered to be at significantly higher risk of REFERENCES
surgical site infection and wound complication based 1. Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden
on published literature (Tran et al), we did not find CL. Trends in obesity among adults in the United States, 2005
to 2014. JAMA 2016;315:2284–91.
a difference in the occurrence of superficial surgical site
2. El-Chaar D, Finkelstein SA, Tu X, Fell DB, Gaudet L, Sylvain J,
infection with the use of prophylactic negative pressure
et al. The impact of increasing obesity class on obstetrical out-
wound therapy; however, the results of these subgroup comes. J Obstet Gynaecol Can 2013;35:224–33.
analyses are limited by small numbers. 3. Myles TD, Gooch J, Santolaya J. Obesity as an independent risk
Our study was limited by slow enrollment and factor for infectious morbidity in patients who undergo cesarean
therefore failure to reach our planned sample size. delivery. Obstet Gynecol 2002;100:959–64.
The two limiting factors in our enrollment were the 4. Tran TS, Jamulitrat S, Chongsuvivatwong V, Geater A. Risk
factors for postcesarean surgical site infection. Obstet Gynecol
need to consent women before active labor to ensure
2000;95:367–71.
women could give informed consent free from pain
5. Smid MC, Dotters-Katz SK, Grace M, Wright ST, Villers MS,
and the need for patients to return for an incision Hardy-Fairbanks A, et al. Prophylactic negative pressure wound
check 5–7 days after their delivery. As a tertiary cen- therapy for obese women after cesarean delivery: a systematic
ter for a large rural geographic catchment area, many review and meta-analysis. Obstet Gynecol 2017;130:969–78.
women delivering at our facility could not feasibly 6. Yu L, Kronen RJ, Simon LE, Stoll CRT, Colditz GA, Tuuli
return for an incision check after discharge. MG. Prophylactic negative-pressure wound therapy after cesar-
ean is associated with reduced risk of surgical site infection:
In conclusion, we did not observe a statistically a systematic review and meta-analysis. Am J Obstet Gynecol
significant difference in postcesarean superficial surgical 2018;218:200–10.e1.
site infection or composite wound complications 7. Use of prophylactic antibiotics in labor and delivery. Practice
between women who used the prophylactic negative Bulletin No. 120. American College of Obstetricians and Gy-
necologists. Obstet Gynecol 2011;117:1472–83.
pressure wound therapy and women who received
a standard dressing. There is currently a large multi- 8. National Healthcare Safety Network, Centers for Disease Con-
trol and Prevention. Surgical site infection (SSI) event.
centered National Institutes of Health-funded trial (Clin- Available at: http://www.cdc.gov/nhsn/pdfs/pscmanual/
icalTrials.gov Identifier: NCT03009110) to examine the 9pscssicurrent.pdf. Retrieved May 17, 2017.
use of prophylactic negative pressure wound therapy for 9. Leth RA, Uldbjerg N, Nørgaard M, Møller JK, Thomsen RW.
the reduction of wound complications in obese women Obesity, diabetes, and the risk of infections diagnosed in hospital
and post-discharge infections after cesarean section: a prospective
after cesarean delivery with a goal of 2,850 women. cohort study. Acta Obstet Gynecol Scand 2011;90:501–9.
Until the results of this or other trials are published,
10. Alanis MC, Villers MS, Law TL, Steadman EM, Robinson CJ.
we recommend against use of prophylactic negative Complications of cesarean delivery in the massively obese par-
pressure wound therapy after cesarean delivery. turient. Am J Obstet Gynecol 2010;203:271.e1–7.
384 Wihbey et al Prophylactic Negative Pressure Wound Therapy OBSTETRICS & GYNECOLOGY
Copyright ª by the American College of Obstetricians
and Gynecologists. Published by Wolters Kluwer Health, Inc.
Unauthorized reproduction of this article is prohibited.
Potrebbero piacerti anche
- IJGM 335893 Effects of Modes and Timings of Delivery On Feto Maternal OuDocumento7 pagineIJGM 335893 Effects of Modes and Timings of Delivery On Feto Maternal OuFred OkelloNessuna valutazione finora
- Cesarean Scar Pregnancy, Incidence, And.26Documento11 pagineCesarean Scar Pregnancy, Incidence, And.26ginogjNessuna valutazione finora
- 05 Hawkins Non Obstetric SurgeryBWpDocumento14 pagine05 Hawkins Non Obstetric SurgeryBWpAita AladianseNessuna valutazione finora
- Pregnancy Associated Breast Changes After.3Documento9 paginePregnancy Associated Breast Changes After.3diego.guerra.smithNessuna valutazione finora
- AmericanDocumento1 paginaAmericanAdzkia_ZRNessuna valutazione finora
- Contoh Presentasi Jurnal Reading ObgynDocumento20 pagineContoh Presentasi Jurnal Reading Obgynbella karinaNessuna valutazione finora
- Ectopico de Cicatriz UterinaDocumento7 pagineEctopico de Cicatriz UterinaNATHALY SARMIENTO ACOSTANessuna valutazione finora
- Negative Pressure Wound Therapy (NPWT) in Breast SurgeryDocumento7 pagineNegative Pressure Wound Therapy (NPWT) in Breast SurgerydokterhelmaNessuna valutazione finora
- 2018-BJOG An International Journal of Obstetrics & GynaecologyDocumento40 pagine2018-BJOG An International Journal of Obstetrics & GynaecologyBagusHibridaNessuna valutazione finora
- 10 Recommendation SC-SibaiDocumento5 pagine10 Recommendation SC-SibaiHervi LaksariNessuna valutazione finora
- Acupuncture and Acupressure in LaborDocumento5 pagineAcupuncture and Acupressure in LaborAstri YuliandiniNessuna valutazione finora
- Literature 3 PDFDocumento1 paginaLiterature 3 PDFVhiena ShittaNessuna valutazione finora
- FinleyDocumento1 paginaFinleyDedi SaputraNessuna valutazione finora
- 10 1089@bfm 2018 0060Documento6 pagine10 1089@bfm 2018 0060rakhelmaharanipybNessuna valutazione finora
- Facchinetti 2005Documento5 pagineFacchinetti 2005Sri HariNessuna valutazione finora
- Direct To Implant Versus Immediate Free Flap.5Documento9 pagineDirect To Implant Versus Immediate Free Flap.5LeiNessuna valutazione finora
- 辅助生殖技术和胎盘介导的不良妊娠结果Obstet GynecolDocumento7 pagine辅助生殖技术和胎盘介导的不良妊娠结果Obstet GynecolchenziendrNessuna valutazione finora
- Journal ObgynDocumento4 pagineJournal ObgynFeby AnggreiniNessuna valutazione finora
- Original Research Articles: Acute Pain SectionDocumento8 pagineOriginal Research Articles: Acute Pain SectionFfNessuna valutazione finora
- Supported By: None.: AbstractsDocumento1 paginaSupported By: None.: AbstractsFerry DimyatiNessuna valutazione finora
- Journal Reading: Advisor: Dr. Ariawan Ditya, SP - OG Arranged byDocumento18 pagineJournal Reading: Advisor: Dr. Ariawan Ditya, SP - OG Arranged bydesti cahyantiNessuna valutazione finora
- UC San Francisco Previously Published Works: TitleDocumento8 pagineUC San Francisco Previously Published Works: TitleluciaNessuna valutazione finora
- Black and Brown Business BrochureDocumento2 pagineBlack and Brown Business BrochureMa. Ferimi Gleam BajadoNessuna valutazione finora
- Nejm 199604183341601Documento6 pagineNejm 199604183341601Simon ReichNessuna valutazione finora
- Deh 001Documento4 pagineDeh 001syid rosyidNessuna valutazione finora
- Marisa - Jurnal - PENGARUH PEMBERIAN TERAPI MUSIK TERHADAP PENURUNAN PDFDocumento7 pagineMarisa - Jurnal - PENGARUH PEMBERIAN TERAPI MUSIK TERHADAP PENURUNAN PDFBrylian TumbolNessuna valutazione finora
- Massagem Perineal em Trabalho de Parto e Prevenção de Trauma Perineal Ensaio Clínico RandomizadoDocumento4 pagineMassagem Perineal em Trabalho de Parto e Prevenção de Trauma Perineal Ensaio Clínico RandomizadoSheila SilvaNessuna valutazione finora
- Successful Conservative Treatment of Microinvasive Cervical Cancer During PregnancyDocumento3 pagineSuccessful Conservative Treatment of Microinvasive Cervical Cancer During PregnancyEres TriasaNessuna valutazione finora
- Abdominal BinderDocumento6 pagineAbdominal BinderyinvilllNessuna valutazione finora
- Poster 2Documento1 paginaPoster 2cringu.ionescuNessuna valutazione finora
- Vaginal Birth After Cesarean: Los Angeles, Californ IaDocumento6 pagineVaginal Birth After Cesarean: Los Angeles, Californ IaRiska PermatasariNessuna valutazione finora
- Comments Fritz Jama EBM2016Documento1 paginaComments Fritz Jama EBM2016Ju ChangNessuna valutazione finora
- Adnexal Masses in Pregnancy: Surgery Compared With ObservationDocumento6 pagineAdnexal Masses in Pregnancy: Surgery Compared With ObservationAgustinus FatollaNessuna valutazione finora
- Ne W Engl and Journal MedicineDocumento9 pagineNe W Engl and Journal MedicinehanifahrafaNessuna valutazione finora
- Made Ayu AsnggrainiDocumento5 pagineMade Ayu AsnggrainiMoh RamliNessuna valutazione finora
- Estimated Fetal Weight: Comparison of Clinical Versus Ultrasound EstimateDocumento6 pagineEstimated Fetal Weight: Comparison of Clinical Versus Ultrasound EstimateNadia AyuningtiasNessuna valutazione finora
- 5.-Diu PostplacentaDocumento11 pagine5.-Diu PostplacentaLuz PuentesNessuna valutazione finora
- Randomized Trial of 3 Techniques of Perineal Skin Closure During Second-Degree Perineal Laceration RepairDocumento16 pagineRandomized Trial of 3 Techniques of Perineal Skin Closure During Second-Degree Perineal Laceration RepairDR RISKA WAHYUNessuna valutazione finora
- Balogunrg RGDocumento10 pagineBalogunrg RGPrasetio Kristianto BudionoNessuna valutazione finora
- Marlene Makenzius, Monica Oguttu, Marie Klingberg-Allvin, Kristina Gemzell-Danielsson, Theresa M A Odero, Elisabeth FaxelidDocumento11 pagineMarlene Makenzius, Monica Oguttu, Marie Klingberg-Allvin, Kristina Gemzell-Danielsson, Theresa M A Odero, Elisabeth FaxelidNaserian SalvyNessuna valutazione finora
- Acetaminophen Analgesia in Neonatal Circumcision: The Effect On PainDocumento8 pagineAcetaminophen Analgesia in Neonatal Circumcision: The Effect On PainDaud GultomNessuna valutazione finora
- Cureus 0010 00000003715Documento12 pagineCureus 0010 00000003715widiastrikNessuna valutazione finora
- Epidural Analgesia in Mothers Undergoing Trial of Vaginal Birth After Previous Cesarean Section: A Prospective StudyDocumento7 pagineEpidural Analgesia in Mothers Undergoing Trial of Vaginal Birth After Previous Cesarean Section: A Prospective StudySANessuna valutazione finora
- Medi 96 E8341Documento4 pagineMedi 96 E8341Mi GleveNessuna valutazione finora
- Teknik Penaganan NyeriDocumento8 pagineTeknik Penaganan NyeriSulis SipinNessuna valutazione finora
- 976 FullDocumento6 pagine976 FullazifadewiatasyaNessuna valutazione finora
- Journal Medicine: The New EnglandDocumento7 pagineJournal Medicine: The New EnglandSyifarNessuna valutazione finora
- Grob Man 2018Documento11 pagineGrob Man 2018Ervan SuryaNessuna valutazione finora
- Perception of Caesarean Section Among PRDocumento7 paginePerception of Caesarean Section Among PRogunwoleisrael1Nessuna valutazione finora
- Combination Analgesia For Neonatal Circumcision A Randomized Controlled TrialDocumento10 pagineCombination Analgesia For Neonatal Circumcision A Randomized Controlled TrialHanny ArdianNessuna valutazione finora
- Routine Antibiotics For BreastConservingDocumento1 paginaRoutine Antibiotics For BreastConservingQuennie Abellon QuimanNessuna valutazione finora
- E002622 FullDocumento10 pagineE002622 FullUsee TvNessuna valutazione finora
- Xiao 等。 - 2018 - Application of Fluorescein Sodium in Breast CancerDocumento7 pagineXiao 等。 - 2018 - Application of Fluorescein Sodium in Breast CancerYouPingLiNessuna valutazione finora
- Eliminating Breast Surgery For Invasive Cancer.12Documento8 pagineEliminating Breast Surgery For Invasive Cancer.12Oncología CdsNessuna valutazione finora
- 0315 DVTDocumento28 pagine0315 DVTGavin TexeirraNessuna valutazione finora
- Effect of Misoprostol With and Without Evening Primrose On Induction of Missed AbortionDocumento9 pagineEffect of Misoprostol With and Without Evening Primrose On Induction of Missed AbortionmozhganNessuna valutazione finora
- Comparison of The Pregnancy Outcomes Between The Medical and Surgical Treatments in Tubal Ectopi PregnancyDocumento4 pagineComparison of The Pregnancy Outcomes Between The Medical and Surgical Treatments in Tubal Ectopi PregnancyYullytia Galaksi MharyatiNessuna valutazione finora
- A Case Study: Prescriptive Exercise Intervention After Bilateral MastectomiesDocumento5 pagineA Case Study: Prescriptive Exercise Intervention After Bilateral MastectomiesPaul GumbocNessuna valutazione finora
- A Case Study: Prescriptive Exercise Intervention After Bilateral MastectomiesDocumento5 pagineA Case Study: Prescriptive Exercise Intervention After Bilateral MastectomiesPaul GumbocNessuna valutazione finora
- WHO Dengue Guidelines 2013Documento160 pagineWHO Dengue Guidelines 2013Jason MirasolNessuna valutazione finora
- Gomes Wses 15Documento6 pagineGomes Wses 15Rara Aulia IINessuna valutazione finora
- DR Leonar, DENGUE PIN PAPDI 2019Documento51 pagineDR Leonar, DENGUE PIN PAPDI 2019Yuni Purnama SariNessuna valutazione finora
- Oftalmologi Indonesia. Vol.6 (2) : 92-103.: Daftar PustakaDocumento1 paginaOftalmologi Indonesia. Vol.6 (2) : 92-103.: Daftar PustakaYuni Purnama SariNessuna valutazione finora
- JR 4Documento9 pagineJR 4Yuni Purnama SariNessuna valutazione finora
- Oftalmologi Indonesia. Vol.6 (2) : 92-103.: Daftar PustakaDocumento1 paginaOftalmologi Indonesia. Vol.6 (2) : 92-103.: Daftar PustakaYuni Purnama SariNessuna valutazione finora
- JR 1Documento10 pagineJR 1Yuni Purnama SariNessuna valutazione finora
- JR 3Documento10 pagineJR 3Yuni Purnama SariNessuna valutazione finora
- JR 5Documento10 pagineJR 5Yuni Purnama SariNessuna valutazione finora
- JR 2Documento5 pagineJR 2Yuni Purnama SariNessuna valutazione finora
- JRDocumento10 pagineJRYuni Purnama SariNessuna valutazione finora
- 05 - 203perkembangan Terkini Diagnosis Dan Penatalaksanaan Imflammatory Bowel Disease PDFDocumento6 pagine05 - 203perkembangan Terkini Diagnosis Dan Penatalaksanaan Imflammatory Bowel Disease PDFrisda aulia putriNessuna valutazione finora
- JR 7Documento8 pagineJR 7Yuni Purnama SariNessuna valutazione finora
- 05 - 203perkembangan Terkini Diagnosis Dan Penatalaksanaan Imflammatory Bowel DiseaseDocumento10 pagine05 - 203perkembangan Terkini Diagnosis Dan Penatalaksanaan Imflammatory Bowel DiseaseYuni Purnama SariNessuna valutazione finora
- Concept of Man Health and IllnessDocumento3 pagineConcept of Man Health and IllnessChristian Shane BejeranoNessuna valutazione finora
- Certificate of Level 1 Training Paediatrics 2021Documento15 pagineCertificate of Level 1 Training Paediatrics 2021Jehangir AllamNessuna valutazione finora
- Reporter Issue 765Documento32 pagineReporter Issue 765backbackNessuna valutazione finora
- National Guideline For Ipc in Hse Dental and Orthodontic ServicesDocumento125 pagineNational Guideline For Ipc in Hse Dental and Orthodontic ServicesSimona BugaciuNessuna valutazione finora
- Role of Statistics in HealthcareDocumento4 pagineRole of Statistics in HealthcareSumita ChatterjeeNessuna valutazione finora
- Community Assessment Ebi Paper - GaDocumento7 pagineCommunity Assessment Ebi Paper - Gaapi-542442476Nessuna valutazione finora
- Complications of Brain Tumors and Their TreatmentDocumento18 pagineComplications of Brain Tumors and Their TreatmentBenedictus Yudha BaskaraNessuna valutazione finora
- Screening For Speech and Language DelayDocumento173 pagineScreening For Speech and Language DelayEdi Hendri MNessuna valutazione finora
- Apollo-Annual Report 2016 PDFDocumento143 pagineApollo-Annual Report 2016 PDFShriniket PatilNessuna valutazione finora
- Epidemiology Lecture 7mmDocumento29 pagineEpidemiology Lecture 7mmSherif AliNessuna valutazione finora
- The Nursing Shortage and Its Effect On Patient CareDocumento7 pagineThe Nursing Shortage and Its Effect On Patient Careapi-641842901Nessuna valutazione finora
- Vision 2015: Medical Council of IndiaDocumento60 pagineVision 2015: Medical Council of IndiaAli Hyder SyedNessuna valutazione finora
- Fundamentals of Nursing NCLEX Practice Quiz 2 (30 Items) : About Privacy Disclaimer ContactDocumento26 pagineFundamentals of Nursing NCLEX Practice Quiz 2 (30 Items) : About Privacy Disclaimer ContactAkia Cayasan BayaNessuna valutazione finora
- Indonesian Policy On HIV/AIDS: 1. HIV Infection in IndonesiaDocumento8 pagineIndonesian Policy On HIV/AIDS: 1. HIV Infection in IndonesiadebbyanggitamsNessuna valutazione finora
- Full Download Gordis Epidemiology 6th Edition Celentano Test BankDocumento34 pagineFull Download Gordis Epidemiology 6th Edition Celentano Test Bankjamboolflexuous.el624100% (37)
- Final 2009 Treatment Technical Report1Documento169 pagineFinal 2009 Treatment Technical Report1Agung GinanjarNessuna valutazione finora
- DLP in Health 10 Global Health InitiativesDocumento10 pagineDLP in Health 10 Global Health InitiativesJoshua MaravillasNessuna valutazione finora
- MAN and His Basic Human NeedsDocumento22 pagineMAN and His Basic Human NeedsKathleen RagudoNessuna valutazione finora
- Chapter 2 Chn2Documento26 pagineChapter 2 Chn2Jahara Aiko PandapatanNessuna valutazione finora
- Practice Bulletin ACOG Antibiotic Prophylaxis For LabourDocumento12 paginePractice Bulletin ACOG Antibiotic Prophylaxis For LabourLorenzo TzuNessuna valutazione finora
- Sick Individuals and Sick Population by Rose. GDocumento7 pagineSick Individuals and Sick Population by Rose. GTate SimbaNessuna valutazione finora
- Chapter 4Documento25 pagineChapter 4missy23pap100% (1)
- Unit Roles and Responsibilities of Community Health Nursing PersonnelDocumento17 pagineUnit Roles and Responsibilities of Community Health Nursing PersonnelExperiencologistNessuna valutazione finora
- Aids OrdinanceDocumento20 pagineAids Ordinancesecdiv2021Nessuna valutazione finora
- National Health PolicyDocumento84 pagineNational Health PolicyPriya SharmaNessuna valutazione finora
- AVC Management I Long PDFDocumento32 pagineAVC Management I Long PDFvasarhely imolaNessuna valutazione finora
- Analysis of Veterinary Service Delivery in Uganda An Application of The Process Net-Map ToolDocumento25 pagineAnalysis of Veterinary Service Delivery in Uganda An Application of The Process Net-Map ToolKYALIGONZA GEOFREYNessuna valutazione finora
- Fundamentals of Canadian Nursing Concepts Process and Practice Canadian 3rd Edition Kozier Test BankDocumento19 pagineFundamentals of Canadian Nursing Concepts Process and Practice Canadian 3rd Edition Kozier Test Bankoxheartpanch07mce100% (22)
- BODYATTACK 96 Choreography BookletDocumento33 pagineBODYATTACK 96 Choreography BookletSusanaNessuna valutazione finora
- School-Based Oral Health Promotion and Prevention ProgramDocumento30 pagineSchool-Based Oral Health Promotion and Prevention ProgramAshraf Ali Smadi100% (6)