Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
The Kerion An Angry Tinea Capitis PB
Caricato da
prajnamitaTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
The Kerion An Angry Tinea Capitis PB
Caricato da
prajnamitaCopyright:
Formati disponibili
Review
The kerion: an angry tinea capitis
Ann M. John1, MD, Robert A. Schwartz1,2, MD, MPH, and Camila K. Janniger1, MD
1
Dermatology, Pathology, Pediatrics, and Abstract
Medicine, Rutgers-New Jersey Medical Tinea capitis has a high incidence with a global changing pathogen distribution, making
School, and 2Rutgers University School of
this condition a public health concern around the world. As the infection is initially
Public Affairs and Administration, Newark,
NJ, USA
asymptomatic, it is easily spread. Moreover, it is present in many fomites, including
hairbrushes, pillows, and bedding. Prompt recognition and treatment is necessary for
Correspondence kerion, an inflammatory subtype characterized by tender boggy plaques with purulent
Robert A. Schwartz, MD, MPH drainage. Kerion is usually associated with infection by zoophilic dermatophytes, although
Professor & Head, Dermatology
other sources have been described. Treatment for this severe form of dermatophytic
185 South Orange Avenue MSB H-576
Rutgers-New Jersey Medical School
infection can be challenging. In addition to the use of topical treatments, oral administration
Newark, NJ 07103 of griseofulvin, terbinafine, itraconazole, or fluconazole is often required. Griseofulvin, the
USA first-line treatment, may not completely eradicate pathogen colonization of the host and
E-mail: raschwartz@gmail.com may contribute to reinfection and prevalence of infective but asymptomatic carriers. This
review highlights new agents that are being evaluated for the treatment of kerion and
Conflicts of Interest: None.
typical tinea capitis, enhanced diagnostic criteria, and a grading system for kerion
doi: 10.1111/ijd.13423 evaluation.
While the incidence has been decreasing in the United States,6
Introduction
it has greatly increased in Europe and other developing
Tinea capitis represents a growing public health concern due to countries.7
changing geographic patterns of infection and high incidence. The development of tinea capitis and kerion in prepubertal age
As one of the most common cutaneous infections in pre-puber- groups is likely due to a lack of sebum secretion. Low sebum pro-
tal children, incidence of infection is high globally, with the duction results in decreased fatty acids and increase in pH of the
World Health Organization claiming it is the second most com- scalp, facilitating colonization and subsequent infection by der-
mon dermatologic infantile infection after pyoderma.1 In the Uni- matophytes. In addition, poor hygiene, playing in sand, crowded
ted States, between 1995 and 2004, the prevalence rates of living conditions, and low socio-economic status have been
tinea capitis were reportedly up to 15%.2,3 A more recent study
Table 1 Geographic distribution of pathogens causing tinea
in the United States determined a carriage rate of 6.6%. Infec-
capitis
tion rates at participating schools ranged from 0% to 19.4%,
with black children demonstrating the highest rate of infection
Location Pathogen
(12.9%).2 Infection is associated with poor hygiene and low
socio-economic status. Adding to the epidemic are three fac- Southern Europe M. canis
tors: late recognition of suspicious lesions, an incubation period Central Europe M. canis, T. verrucosum, T. mentagrophytes,
of a few weeks in which patients are contagious but asymp- T. violaceum
Eastern Europe M. canis, M. audounii, T. violaceum
tomatic, and transmission from household pets.4 Prompt treat-
United Kingdom, M. canis, T. verrucosum, T. mentagrophytes,
ment of an inflammatory subtype, the kerion, is necessary to
France T. violaceum
preclude permanent scarring and alopecia. However, current United States T. tonsurans
treatment may not completely eradicate pathogens. Canada T. mentagrophytes, M. canis
Mexico M. canis, T. tonsurans
Caribbean T. tonsurans, M. canis
Etiology India, Pakistan T. violaceum
China T. violaceum, T. mentagrophytes
Tinea capitis can be caused by any dermatophyte, except Middle East M. canis, T. violaceum, T. schoenleinii,
Epidermophyton floccosum and Trichophyton concentricum. T. verrucosum
The most commonly implicated dermatophytes are of the Western Africa Microsporum audouinii, T. soudanense,
T. yaoundei
Trichophyton and Microsporum genera. The list of causative
Eastern Africa T. schoenleinii
pathogens based on geographic area is shown in Table 1.5 1
ª 2016 The International Society of Dermatology International Journal of Dermatology 2016
2 Review The kerion: an angry tinea capitis John, Schwartz, and Janniger
associated with the development of tinea.8 In particular, kerion is
Clinical presentation
mostly associated with infection by zoophilic dermatophytes.9
Tinea capitis is easily spread from the infected and often asymp- Clinical presentation can be subdivided into two subtypes:
tomatic carrier to others, making family epidemics very common. inflammatory and non-inflammatory. Cervical and suboccipital
Spores of Trichophyton spp. have been cultured from diverse lymphadenopathy are commonly found and may serve as a
sources, including combs, hats, and pillows. Practices such as diagnostic clue.17 Non-inflammatory presentation is character-
the use of oils, frequency of hair washing, and tight braiding, have ized by scaling, a seborrheic form, and loss of hair. The ecto-
not shown to increase the risk of infection.6 thrix pattern commonly causes the non-inflammatory clinical
presentation, with circumscribed patches of alopecia due to
destroyed cuticles. The gray patch presentation is an ectothrix
Epidemiology
Microsporum infection with patchy circular alopecia and scal-
Tinea capitis most commonly infects children between 3 and ing. The black dot presentation is caused by an endothrix Tri-
7 years of age. Infants and adults are rarely affected. Reports chophyton infection, which causes breakage of the hair shaft
of infection in infants are usually related to the use of broad- at the scalp, leaving behind black dots. The diffuse scale pre-
spectrum antibiotics and immunosuppression.10 Some studies sentation is characterized by dandruff-like scaling of the
have shown no gender predilection,11 while others report an scalp.7
increased prevalence among boys,12 and others report the high- The inflammatory subtype is characterized by tender plaques
est prevalence among African–American girls.2,6 Short hair is covered with broken hairs and pustules. This subtype can be
associated with higher incidence because fungal spores can further divided into the pustular form, favus, Majocchi granu-
access the scalp more easily.6 A recent study also demon- loma, mycetoma, and kerion. The pustular form is associated
strated a higher risk of kerion development in rural populations with a patchy alopecia and scattered pustules or low-grade folli-
compared to suburban populations, perhaps due to greater con- culitis. Favus presents with erythema around hair follicles and
tact with animals. This study postulated that a greater incidence cicatricial alopecia. Eventually, scutula, or yellow-crusted cup-
in boys is related to their increased contact with farm animals shape lesions, form with hair loss and scarring. Favus may also
compared to girls.10 involve the skin and nails.17 Majocchi granuloma is character-
In addition to children, there are several other groups that ized by papular, pustular, or nodular lesions on the limbs or
are at greater risk of developing tinea capitis and kerion. These face. Mycetoma is characterized by nodular lesions overlying
include people with diabetes, anemia, and immunosuppression erythematous and scaly plaques, sinus tracts with purulent drai-
due to leukemia, organ transplant, and the use of immunosup- nage, and pseudoalopecia.18
pressants. The use of immunosuppressants may interfere with Kerion is commonly confused with bacterial abscesses due
hair production and shaft strength, allowing for colonization by to the purulent drainage. It presents as a painful, crusty carbun-
fungi.13 Of note, tinea infections are not as common in patients cle-like boggy plaque that requires early diagnosis to prevent
with HIV, likely because of increased colonization with Malasse- bacterial superinfection, folliculitis, and permanent alopecia
zia, thus competitively inhibiting the colonization of dermato- (Figs 1 and 2). It usually occurs as a solitary lesion, most com-
phytes.14 Chronic users of topical or systemic corticosteroids monly in the occipital area of the scalp,19 although it can occur
may be more likely to develop infection. Women undergoing as multiple lesions. It has been reported to occur in other sites,
major hormonal changes, including during pregnancy and including the beard, eyebrow, and vulva.20–22 The course of ker-
menopause, may also be more prone to infection because of ion begins with dermatophytic folliculitis and a dry lesion with
reduced sebum excretion.15 In fact, the majority of adults with scaling and short hairs. Development of kerion depends on the
tinea capitis are women, likely due to periods of hormonal type of pathogen as well as the host immune status. Erythema,
changes, greater exposure to children, and increased visits to tenderness, and inflammation rapidly follow the initial lesions.
the hairdresser.16 Short hairs are eventually expelled and within 8 weeks, the
infection usually resolves. Dermatophytid reactions, which are
immunological reactions caused by infection or inflammation,
Classification
commonly occur. The reaction can be localized or generalized
Infection with tinea capitis can be classified into three patterns: and often presents as eczematous lesions with papules, scaly
endothrix; ectothrix; and endothrix favosa. The endothrix pattern patches, vesicles, and pustules. Classically, these present as
is characterized by fungal spores dwelling within the hair shaft, the “ear sign,” in which erythematous papules and scaling are
thus allowing the cortex to remain intact. The ectothrix pattern found overlying the helix, antihelix, and retroauricular regions.
of infection involves fungal spores attaching to the surface of Several studies have demonstrated a high rate of association of
the hair shaft, allowing for cuticle destruction. Endothrix favosa dermatophytid reactions and kerion. In one study, 68% of
is characterized by the presence of hyphae and air bubbles patients with kerion had an accompanying dermatophytid reac-
within the hair shaft.17 tion. These reactions tend to occur at the height of the infection
International Journal of Dermatology 2016 ª 2016 The International Society of Dermatology
John, Schwartz, and Janniger The kerion: an angry tinea capitis Review 3
Table 2 Major and minor features suggestive of kerion
Major criteria Minor criteria
Tenderness to palpation Dermatophytid reaction
Alopecia surrounding the lesion Regional lymphadenopathy
Numerous pustules and purulent Short hairs on dermoscopy
drainage Boggy plaques
Scaling at the lesion Clear dermarcation of
borders
Overlying erythema
Pruritus
stages. There are four types of histopathological patterns asso-
ciated with kerion. First, suppurative folliculitis is characterized
by a perifollicular inflammatory infiltrate with spongiosis and infil-
trates of neutrophils, lymphocytes, and plasma cells. Most hair
follicles are in the catagen stage. The second pattern is suppu-
rative folliculitis with suppurative dermatitis. This pattern is char-
acterized by a perifollicular and perivascular infiltrate of
neutrophils with edema in the papillary dermis. Hair follicles are
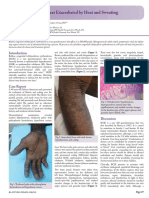
Figure 1 Clinical example of kerion. Note the alopecia surrounding in the catagen or telogen stage with few disrupted follicles. The
the lesion as well as pustules and purulent drainage over multiple third pattern is suppurative folliculitis with suppurative and gran-
lesions
ulomatous dermatitis, which is characterized by an infiltrate of
neutrophils, lymphocytes, and plasma cells, and a granuloma-
tous reaction. There is a decreased number of hair follicles.
Finally, the fourth pattern is suppurative and granulomatous der-
matitis with fibrosing dermatitis. In this pattern, there is an
inflammatory infiltrate of neutrophils, lymphocytes, and plasma
cells, with granuloma formation, increased number of collagen
fibers, and absent hair follicles consistent with scarring alopecia.
The latter two patterns have negative periodic acid-Schiff
stains.18
Diagnosis
Tinea capitis is often misdiagnosed, thus delaying proper treat-
ment and allowing spread of infection. There are no established
Figure 2 Clinical example of alopecia following infection clinical guidelines for kerion, and it is often confused with a bac-
terial infection. We propose major and minor diagnostic criteria
and therefore directly before or after initiation of antifungal ther- for kerion (Table 2). If these criteria are present, a dermatology
apy.19 Therapy should not be discontinued. consult should be requested before surgically manipulating the
site or labeling the infection origin as bacterial. In addition, we
devised a grading system for kerion to ease communication
Histopathology
between practitioners about the severity of the lesion (Table 3).
Histologic analysis is useful in culture-negative patients. As While the grade of the lesion does not change treatment, it may
most cases of kerion are culture negative, histopathology usu- be helpful in determining treatment response and prognosis. In
ally reveals fungal spores surrounding the hair follicle and addition, it would be of interest to determine risk factors that
hyphae within the hair shaft. Inflammatory infiltrate is found in correlate to the grade of lesion, e.g., if immunosuppression pre-
the dermis, and giant cell reaction may occur due to follicular disposes an individual to a higher-grade lesion.
destruction.17 In addition, a periodic acid-Schiff stain can be A culture for fungi is the gold standard to confirm the diagno-
used to confirm diagnosis. sis. A simple method that has demonstrated good efficacy is
Kerion is specifically characterized by neutrophilic and granu- the hairbrush culture method.23 After obtaining a sample of hair,
lomatous infiltrates in the early stages and fibrotic scar in later hair and scalp scale, or scalp brushings, the sample is placed
ª 2016 The International Society of Dermatology International Journal of Dermatology 2016
4 Review The kerion: an angry tinea capitis John, Schwartz, and Janniger
Table 3 Grading of kerion lesions Table 4 Differential diagnoses of kerion and tinea capitis
Grade Characteristics Diagnosis Differentiating features
1 A few pustules overlying erythematous plaque; most hairs in Alopecia areata No epidermal changes; exclamation point hairs; no
catagen phase but still intact; histology shows suppurative crusting, inflammation, or pustules
folliculitis Atopic dermatitis Personal or family history of asthma, hay fever,
2 Pustules and papules overlying erythematous plaque; scaling at sensitive skin; usually no lymphadenopathy; usually
the periphery of plaque; few disrupted hair follicles; histology no alopecia
show suppurative folliculitis with suppurative dermatitis Bacterial scalp Plucking hair produces pain; usually no alopecia
3 Pustules, papules, scaling, and erythema present; vesicles may abscess
be present; clear patches of alopecia; histology shows Psoriasis Family history of psoriasis; gray or silver scale; other
suppurative folliculitis with suppurative and granulomatous systemic involvement
dermatitis; negative PAS stain Seborrheic Greasy scale; usually no alopecia and
4 Pustules, scaling, and erythema present; permanent patches of dermatitis lymphadenopathy
alopecia with scarring; histology shows suppurative and Trichotillomania No scaling; hairs are varying lengths
granulomatous dermatitis with fibrosing dermatitis; negative
PAS stain
A more recent method of diagnosis is the use of real-time
PAS, periodic acid-Schiff. polymerase chain reaction (PCR) test or PCR reverse-line blot
assays to detect T. tonsurans ribosomal DNA in fluid used to
in Sabouraud liquid medium or dermatophyte test medium. At rinse the patient’s hairbrush. This test takes 5 h.23
least one plate should also include cycloheximide–chloram-
phenicol to prevent mold growth and bacterial contamination
Differential diagnosis
that may suggest false findings. Using a cytobrush, which is a
sterile tool with softer bristles, improves sample quality and min- The differential diagnosis of kerion is vast. This complication of
imizes discomfort. Cultures often require 2 weeks of growth untreated tinea capitis should be distinguished from diagnoses
before examination. With Trichophyton verrucosum, cultures with differentiating features listed in Table 4.29 Kerion may be
should be incubated for 3 weeks. Other culture methods include confused with dissecting cellulitis, which is characterized by ten-
growth on rice grains, urease test, and hair perforation test.24 der, suppurative nodules that produce draining sinus tracts and
Of note, patients with kerion have a high false-negative culture scarring. Unlike tinea capitis, dissecting cellulitis usually occurs
rate with conventional methods of sampling, likely because the in African American adults as a deep lesion. It is important to
sample represents the inflammatory response. Therefore, gauze perform cultures and swabs to confirm fungal infections in
swabs or use of a moistened bacterial swab from the pustular cases of atypical presentation.30
area in addition to directly pressing the agar plate on to the ker-
ion may yield more positive cultures.7 Samples should also be
Treatment
examined under a microscope using 10–30% potassium hydrox-
ide with or without calcofluor. For any case of tinea capitis, systemic antifungal agents are
Dermoscopic examination of tinea capitis is increasingly indicated as topical agents will not penetrate the hair shaft.7
becoming a quicker and faster method of diagnosis. Comma However, use of topical agents is being assessed, as described
hair is a classic finding, seen in both endothrix and ectothrix below. Griseofulvin is the first-line treatment for tinea capitis
patterns of infection.25 Corkscrew hair is also a classic finding, since 1958.31 Eight weeks of treatment are necessary for
observed in dark-skinned patients. Less specific findings include Microsporum infections, and 12–18 weeks of treatment are nec-
black dots, broken hair, pigtail hair, and zigzag hairs.25 More essary for Trichophyton.32,33 It should be avoided in pregnant
recently, bar code-like hair has been reported in the ectothrix patients. It is also contraindicated in patients with lupus erythe-
pattern of infection.26 Dermoscopic examination is particularly matosus, porphyria, and severe liver disease. One study
important in differentiating tinea capitis from alopecia areata. reported that griseofulvin does not eradicate Trichophyton in
Specific trichoscopic findings of alopecia areata include yellow most infected children but simply causes symptom resolution.
dots, exclamation mark hairs, and short vellus hair.27 Antiseptic As such, persistent infection and spread of infection may
precautions with the use of a film between the dermoscope and occur.34
lesion should be employed to minimize spread of infection. Newer agents, including terbinafine, itraconazole, and flu-
Wood lamp examination is useful if the infection is caused by conazole, are equally effective according to recent clinical trials.
Microsporum canis, which exhibits green fluorescence under In addition, the newer antifungal agents are more concentrated
the light, or tinea capitis favosa, which exhibits faint blue in the hair and therefore may provide fungicidal concentrations
fluorescence. However, Trichophyton infections, except for even after treatment is completed, allowing for shorter treatment
T. schoenleinii, do not fluoresce.28 duration and lower rates of reinfection. Terbinafine is a
International Journal of Dermatology 2016 ª 2016 The International Society of Dermatology
John, Schwartz, and Janniger The kerion: an angry tinea capitis Review 5
fungicidal drug that acts on the cell membrane. A meta-analysis
Prevention
of randomized clinical trials did not demonstrate significant dif-
ference in efficacy of terbinafine compared to griseofulvin.35 In Prevention of epidemic spread of tinea capitis requires patient
addition, terbinafine requires 2–4 weeks of treatment for Tri- education about proper hygiene techniques and prompt treat-
chophyton infections.36 A newer granule formation of terbinafine ment. One study provided patients with a video, emphasizing
that can be sprinkled on food is approved for use in the United frequent cleaning and washing of rooms and training clothes,
States. However, the cost is high in developing countries, pre- immediate showering after sports practice, and recognition and
cluding its use. It is not recommended for the treatment of immediate reporting of lesions. The video resulted in a signifi-
Microsporum infection. Side effects include gastrointestinal dis- cant decrease in culture-positive rates.23 In addition, patients
comfort and rashes. should be informed to restrain from sharing hairbrushes, combs,
Itraconazole is a fungistatic and fungicidal drug, depending hats, dress-up clothes, and other hair accessories with siblings
on its tissue concentration. Treatment duration is between 2 or classmates who are infected. Additional hand washing should
and 4 weeks. It is shown to have comparable efficacy to griseo- be emphasized. Blankets and bedding should be changed daily
fulvin and terbinafine.37,38 It is also available in the liquid form to prevent spread. Curtains should be washed regularly.
with fewer side effects. However, it has several drug interac- Screening of children and staff at schools has also been pro-
tions with warfarin, antihistamine, antipsychotics, anxiolytics, posed to prevent epidemics.
digoxin, cyclosporine, and simvastatin and must be used cau- Children who are receiving appropriate treatment are
tiously in patients taking multiple medications.7 Fluconazole allowed to return to school. However, all family members
serves as a valid alternative; it is present in the liquid and rectal should be screened and treated if necessary to prevent recur-
forms, persists for several weeks after administration, and must rence. Asymptomatic carriers with high fungal spore load
only be given once weekly. Multiple studies have demonstrated should be treated with oral drugs. In patients with low spore
that fluconazole is comparable to griseofulvin in terms of use, load, topical treatment can be used with repeat tests to ensure
side effects, compliance, and efficacy.39–41 However, its high clearance.48
cost limits its use. Voriconazole shows greater activity against
pathogens than griseofulvin does, but its high cost and adverse
Conclusion
effects are often prohibitive.42
The use of topical squalamine, a natural aminosterol isolated Kerion is a subset of inflammatory tinea capitis that can result
from dogfish shark, has also been reported. While this drug in permanent alopecia and scarring. Prompt recognition and
does not cause complete eradication of fungi, it provides partial treatment is desirable. We have delineated features suggestive
clinical response with some hair growth in areas of the lesion. It of this diagnosis as well as a grading system. Diagnosis
is suggested to be used as an adjuvant therapy to decrease includes culture, dermoscopic examination, Wood’s lamp exami-
treatment duration and increase compliance.43 In addition, use nation, or PCR testing. Treatment requires the use of oral anti-
of 1% or 2.5% selenium sulfide, 2% ketoconazole, 1–2% zinc fungal agents with adjuvant topical treatments to prevent the
pyrithione, and 2.5% povidone iodine shampoos may reduce spread of infection. As tinea capitis remains a public health con-
transmission if used within the first 2 weeks of infection.44,45 cern, patients should be educated on preventative measures
Use of prednisone during the first week of infection may allevi- and lesion appearance, particularly of the angry subtype, the
ate pain and swelling accompanying inflammatory subtypes.46 kerion.
Kerion must be treated emergently with griseofulvin, as fail-
ure to treat can lead to permanent scarring and alopecia. Terbi-
Questions (answers provided after
nafine should only be used if Trichophyton is documented as
references)
the cause of infection. Other treatments, including itraconazole
pulsed therapy, show an initial improvement followed by recur- 1 Risk factors for the development of tinea capitis include all of
rent and worse lesions.47 It is important that surgical drainage the following except:
of kerion is not performed, despite the similarities with bacterial a Prepubertal age
abscesses. In addition, treatment with steroids has not been b Low socio-economic status
shown to reduce scarring or confer long-term advantages but c Tight hair braiding
may reduce itching and pain.46 d Rural living conditions
Patients should be monitored every 14 d starting with the 2 Of the following groups of immunosuppressed patients, which
fourth week of treatment to determine treatment response.17 are least likely to develop tinea capitis infections?
Post-treatment clearance of infection should be verified with cul- a Patients with HIV
ture. For infections with no signs of clinical improvement, the b Chronic steroid users
treatment regimen should be altered by increasing the dose or c Patients with leukemia
changing the agent. d Organ transplant patients
ª 2016 The International Society of Dermatology International Journal of Dermatology 2016
6 Review The kerion: an angry tinea capitis John, Schwartz, and Janniger
3 True or False: Patients with dermatophytid reactions should 6 Mirmirani P, Tucker LY. Epidemiologic trends in pediatric
undergo discontinuation of current treatment with continuation tinea capitis: a population-based study from Kaiser
only after resolution of the reaction. Permanente Northern California. J Am Acad Dermatol 2013;
69: 916–921.
4 How is the presentation of kerion different from that of
7 Fuller LC, Barton RC, Mohd Mustapa MF, et al. British
bacterial abscesses?
Association of Dermatologists’ guidelines for the
a Presence of purulent drainage management of tinea capitis 2014. Br J Dermatol 2014; 171:
b Accompanying tenderness 454–463.
c Presence of alopecia 8 Pires CA, Cruz NF, Lobato AM, et al. Clinical,
5 What is the gold standard of culture for diagnosis in kerion? epidemiological, and therapeutic profile of dermatophytosis.
a Culture growth on rice grains An Bras Dermatol 2014; 89: 259–264.
9 Larralde M, Gomar B, Boggio P, et al. Neonatal kerion
b Hairbrush culture method
Celsi: report of three cases. Pediatr Dermatol 2010; 27:
c Urease test
361–363.
d Hair perforation test 10 Zaraa I, Hawilo A, Aounallah A, et al. Inflammatory tinea
6 Findings of kerion on dermoscopy include all of the following capitis: a 12-year study and a review of the literature.
except: Mycoses 2013; 56: 110–116.
a Comma hairs 11 Laude TA, Shah BR, Lynfield Y. Tinea capitis in Brooklyn.
b Corkscrew hairs Am J Dis Child 1982; 136: 1047–1050.
12 Suh DC, Friedlander SF, Raut M, et al. Tinea capitis in the
c Zigzag hairs
United States: diagnosis, treatment, and costs. J Am Acad
d Exclamation mark hairs
Dermatol 2006; 55: 1111–1112.
7 What is the first-line treatment of kerion? 13 Mao L, Zhang L, Li H, et al. Pathogenic fungus
a Terbinafine Microsporum canis activates the NLRP3 inflammasome.
b Griseofulvin Infect Immun 2014; 82: 882–892.
c Itraconazole 14 Narang K, Pahwa M, Ramesh V. Tinea capitis in the form of
d Fluconazole concentric rings in an HIV positive adult on antiretroviral
treatment. Indian J Dermatol 2012; 57: 288–290.
8 True or False: Children with kerion should be allowed to
15 Mansur AT, Artunkal S, Ener B. Tinea capitis in an adult
return to school after completion of treatment.
patient under treatment with trastuzumab. Mycoses 2011;
9 Major diagnostic criteria of kerion include all of the following 54: e609–e10.
except: 16 Takwale A, Agarwal S, Holmes SC, et al. Tinea capitis in
a Tenderness to palpation two elderly women: transmission at the hairdresser. Br J
b Purulent drainage Dermatol 2001; 144: 898–900.
c Boggy plaque 17 Ramos-e-Silva M, Pirmez R. Red face revisited: disorders of
hair growth and the pilosebaceous unit. Clin Dermatol 2014;
d Scaling of lesion
32: 784–799.
10 True or False: Prevention of epidemic spread of tinea capitis
18 Isa-Isa R, Arenas R, Isa M. Inflammatory tinea capitis:
requires patient education about proper hygiene techniques and kerion, dermatophytic granuloma, and mycetoma. Clin
prompt treatment. Dermatol 2010; 28: 133–136.
19 Topaloglu Demir F, Karadag AS. Are dermatophytid
reactions in patients with kerion celsi much more common
References than previously thought? A prospective study Pediatr
Dermatol 2015; 32: 635–640.
1 Kechia FA, Kouoto EA, Nkoa T, et al. Epidemiology of tinea
20 Shreberk-Hassidim R, Ramot Y, et al. Kerion celsi of the
capitis among school-age children in Meiganga, Cameroon.
vulva: an unusual location. J Mycol Med 2014; 24: 359–360.
J Mycol Med 2014; 24: 129–134.
21 Pinto V, Marinaccio M, Serrati A, et al. [Kerion of the vulva.
2 Abdel-Rahman SM, Farrand N, Schuenemann E, et al. The
Report of a case and review of the literature]. Minerva
prevalence of infections with Trichophyton tonsurans in
Ginecol 1993; 45: 501–505.
schoolchildren: the CAPITIS study. Pediatrics 2010; 125:
22 Annabel M, Hubert L, Jacques C, et al. [Treatment of 2
966–973.
cases of kerions with griseofulvin and oral steroids]. Arch
3 Panackal AA, Halpern EF, Watson AJ. Cutaneous fungal
Pediatr 2009; 16: 1464–1466.
infections in the United States: analysis of the
23 Hiruma J, Ogawa Y, Hiruma M. Trichophyton tonsurans
National Ambulatory Medical Care Survey (NAMCS) and
infection in Japan: epidemiology, clinical features, diagnosis
National Hospital Ambulatory Medical Care Survey
and infection control. J Dermatol 2015; 42: 245–249.
(NHAMCS), 1995-2004. Int J Dermatol 2009; 48: 704–712.
24 Chadeganipour M, Mohammadi R, Shadzi S. A 10-year
4 Monod M, Fratti M, Mignon B, et al. [Dermatophytes
study of dermatophytoses in Isfahan, Iran. J Clin Lab Anal
transmitted by pets and cattle]. Rev Med Suisse 2014; 10:
2016; 30: 103–107.
749–753.
25 Slowinska M, Rudnicka L, Schwartz RA, et al. Comma
5 Rebollo N, Lopez-Barcenas AP, Arenas R. [Tinea capitis].
hairs: a dermatoscopic marker for tinea capitis: a rapid
Actas Dermosifiliogr 2008; 99: 91–100.
International Journal of Dermatology 2016 ª 2016 The International Society of Dermatology
John, Schwartz, and Janniger The kerion: an angry tinea capitis Review 7
diagnostic method. J Am Acad Dermatol 2008; 59(Suppl. 5): Microsporum canis tinea capitis? Drugs Exp Clin Res 2005;
S77–S79. 31(Suppl.): 11–15.
26 Wang HH, Lin YT. Bar code-like hair: dermoscopic marker 39 Shemer A, Plotnik IB, Davidovici B, et al. Treatment of tinea
of tinea capitis and tinea of the eyebrow. J Am Acad capitis – griseofulvin versus fluconazole – a comparative
Dermatol 2015; 72(Suppl. 1): S41–S42. study. J Dtsch Dermatol Ges 2013; 11: 737–742.
27 El-Taweel AE, El-Esawy F, Abdel-Salam O. 40 Foster KW, Friedlander SF, Panzer H, et al. A randomized
Different trichoscopic features of tinea capitis and alopecia controlled trial assessing the efficacy of fluconazole in the
areata in pediatric patients. Dermatol Res Pract 2014; 2014: treatment of pediatric tinea capitis. J Am Acad Dermatol
848763. 2005; 53: 798–809.
28 Castelo-Soccio L. Diagnosis and management of alopecia in 41 Valari M, Iordanidou A, Raftopoulou A, et al. Fluconazole
children. Pediatr Clin North Am 2014; 61: 427–442. in the treatment of pediatric tinea capitis caused by
29 Trovato MJ, Schwartz RA, Janniger CK. Tinea capitis: Microsporum canis. Drugs Exp Clin Res 2002; 28: 161–
current concepts in clinical practice. Cutis 2006; 77: 93–99. 164.
30 Miletta NR, Schwartz C, Sperling L. Tinea capitis mimicking 42 Ghannoum M, Isham N, Sheehan D. Voriconazole
dissecting cellulitis of the scalp: a histopathologic pitfall susceptibilities of dermatophyte isolates obtained from a
when evaluating alopecia in the post-pubertal patient. worldwide tinea capitis clinical trial. J Clin Microbiol 2006;
J Cutan Pathol 2014; 41: 2–4. 44: 2579–2580.
31 Oranje AP, de Waard-van der Spek FB. Recent 43 Coulibaly O, Thera MA, Kone AK, et al. A double-blind
developments in the management of common childhood randomized placebo-controlled clinical trial of squalamine
skin infections. J Infect 2015; 71(Suppl. 1): S76–79. ointment for tinea capitis treatment. Mycopathologia 2015;
32 Gupta AK, Cooper EA, Bowen JE. Meta-analysis: 179: 187–193.
griseofulvin efficacy in the treatment of tinea capitis. J Drugs 44 Dastghaib L, Azizzadeh M, Jafari P. Therapeutic options for
Dermatol 2008; 7: 369–372. the treatment of tinea capitis: griseofulvin versus
33 Lorch Dauk KC, Comrov E, Blumer JL, et al. Tinea capitis: fluconazole. J Dermatolog Treat 2005; 16: 43–46.
predictive value of symptoms and time to cure with 45 Gan VN, Petruska M, Ginsburg CM. Epidemiology and
griseofulvin treatment. Clin Pediatr 2010; 49: 280–286. treatment of tinea capitis: ketoconazole vs. griseofulvin.
34 Abdel-Rahman SM, Wright KJ, Navarre HC. Griseofulvin Pediatr Infect Dis J 1987; 6: 46–49.
only modestly diminishes persistence of Trichophyton 46 Proudfoot LE, Higgins EM, Morris-Jones R. A retrospective
tonsurans on the scalp of carriers. J Pediatr Pharmacol study of the management of pediatric kerion in
Ther 2009; 14: 94–99. Trichophyton tonsurans infection. Pediatr Dermatol 2011;
35 Gupta AK, Drummond-Main C. Meta-analysis of 28: 655–657.
randomized, controlled trials comparing particular doses of 47 Pranteda G, Muscianese M, Grimaldi M, et al.
griseofulvin and terbinafine for the treatment of tinea capitis. Pharmacological management of pediatric Kerion celsi. Int J
Pediatr Dermatol 2013; 30: 1–6. Immunopathol Pharmacol 2013; 26: 973–976.
36 Fuller LC, Smith CH, Cerio R, et al. A randomized 48 Ilkit M, Demirhindi H. Asymptomatic dermatophyte scalp
comparison of 4 weeks of terbinafine vs. 8 weeks of carriage: laboratory diagnosis, epidemiology and
griseofulvin for the treatment of tinea capitis. Br J Dermatol management. Mycopathologia 2008; 165: 61–71.
2001; 144: 321–327.
37 Ginter-Hanselmayer G, Smolle J, Gupta A. Itraconazole in
the treatment of tinea capitis caused by Microsporum canis:
experience in a large cohort. Pediatr Dermatol 2004; 21: Answers
499–502.
38 Koumantaki-Mathioudaki E, Devliotou-Panagiotidou D, Rallis 1 c; 2 a; 3 False – therapy should not be discontinued; 4 c; 5 b;
E, et al. Is itraconazole the treatment of choice in 6 d; 7 b; 8 True; 9 c; 10 True.
ª 2016 The International Society of Dermatology International Journal of Dermatology 2016
Potrebbero piacerti anche
- Skin Infections, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDa EverandSkin Infections, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNessuna valutazione finora
- Herpes Simplex Virus Recurrent Apthous Stomatitis Oral PathoDocumento35 pagineHerpes Simplex Virus Recurrent Apthous Stomatitis Oral PathoFourthMolar.comNessuna valutazione finora
- Ringworm (Tinea Capitis)Documento15 pagineRingworm (Tinea Capitis)farmasi_hmNessuna valutazione finora
- Skin Manifestations of HIV DiseaseDocumento31 pagineSkin Manifestations of HIV Diseaselovelots1234Nessuna valutazione finora
- The HPV Virus and TypesDocumento8 pagineThe HPV Virus and TypesbournvilleeaterNessuna valutazione finora
- Herpes Zoster (Shingles) : Muhammad Abdullah Dept. of Dermatology DHQ Hospital FaisalabadDocumento26 pagineHerpes Zoster (Shingles) : Muhammad Abdullah Dept. of Dermatology DHQ Hospital FaisalabadwaleedNessuna valutazione finora
- Cutaneous Leishmaniasis: Caused by A Protozoa Called Leishmania PathogenesisDocumento30 pagineCutaneous Leishmaniasis: Caused by A Protozoa Called Leishmania PathogenesisHudh HudNessuna valutazione finora
- Wwa NodosumDocumento21 pagineWwa NodosumMu AbNessuna valutazione finora
- Atopic Dermatitis Practical HCP Guide 2nd Ed 2016Documento12 pagineAtopic Dermatitis Practical HCP Guide 2nd Ed 2016Tia AfelitaNessuna valutazione finora
- Tinea Corporis An Updated ReviewDocumento12 pagineTinea Corporis An Updated ReviewM Ilham FadillahNessuna valutazione finora
- Meningitis in Children 1204809002482509 3Documento48 pagineMeningitis in Children 1204809002482509 3Ali FalihNessuna valutazione finora
- N M To Es: Dr. Wafaa Ezz ElarabDocumento31 pagineN M To Es: Dr. Wafaa Ezz Elarabshoroq zaki100% (1)
- Peds Derm 101 HH HandoutDocumento25 paginePeds Derm 101 HH HandoutzhuorancaiNessuna valutazione finora
- Molluscum Contagiosum Module - PPSXDocumento38 pagineMolluscum Contagiosum Module - PPSXDevy Anggi SitompulNessuna valutazione finora
- 03diffuse Eyelid DiseasesDocumento15 pagine03diffuse Eyelid DiseasesدرالجمانNessuna valutazione finora
- Erythema MultiformeDocumento29 pagineErythema MultiformeSurabhi Sharma100% (1)
- Vasculitis ReviewDocumento132 pagineVasculitis Reviewajmal_rashid@hotmail.com100% (2)
- DermatomycosesDocumento73 pagineDermatomycosessnylstlNessuna valutazione finora
- Molluscum MedscapeDocumento35 pagineMolluscum MedscapeAninditaNessuna valutazione finora
- Classic Childhood ExanthemsDocumento66 pagineClassic Childhood ExanthemsBorzoo Tajdin100% (1)
- VERUCCA VULGARIS PresentationDocumento28 pagineVERUCCA VULGARIS PresentationBrilliantIbnuSina100% (2)
- Pyogenic GranulomaDocumento13 paginePyogenic GranulomaPiyusha SharmaNessuna valutazione finora
- Infectious DermatologyDocumento206 pagineInfectious DermatologyAaron Christian Earl VillosoNessuna valutazione finora
- 7 Bleeding Disorders DR - AlaaDocumento35 pagine7 Bleeding Disorders DR - Alaaaj1998ajNessuna valutazione finora
- Fever With Rash SeminarDocumento98 pagineFever With Rash SeminarSYAZRIANA SUHAIMINessuna valutazione finora
- Erythema NodosumDocumento42 pagineErythema Nodosummedpedshospitalist100% (1)
- Approach in Lymphadenopathy in ChildrenDocumento14 pagineApproach in Lymphadenopathy in Childrennahiry100% (1)
- WoundsDocumento6 pagineWoundsTeddy MuaNessuna valutazione finora
- CMV VirusDocumento8 pagineCMV VirusKalpavriksha1974Nessuna valutazione finora
- Teaching Diagnostic Error Using Problem-Based Learning: A Case of Cellulitis MisdiagnosisDocumento4 pagineTeaching Diagnostic Error Using Problem-Based Learning: A Case of Cellulitis Misdiagnosisvadiningtyas3770Nessuna valutazione finora
- Pertusis TreatmentDocumento20 paginePertusis TreatmentJaipratap SinghNessuna valutazione finora
- Psoriasis and ComorbiditiesDocumento8 paginePsoriasis and ComorbiditiesIvanWinardyNessuna valutazione finora
- CalciphylaxisDocumento2 pagineCalciphylaxisRajiv SinghalNessuna valutazione finora
- Case 17: 28-Year-Old With A Rash - Mr. MoellerDocumento19 pagineCase 17: 28-Year-Old With A Rash - Mr. MoellerJDNessuna valutazione finora
- Ve Siculo Bull Ous DiseasesDocumento73 pagineVe Siculo Bull Ous DiseasesAARYANessuna valutazione finora
- Differential Diagnosis Fever With RashDocumento15 pagineDifferential Diagnosis Fever With RashJeetat OngNessuna valutazione finora
- PediatricsDocumento38 paginePediatricskhanNessuna valutazione finora
- Topical Antibiotics in DermatologyDocumento19 pagineTopical Antibiotics in DermatologyJejem Marandra EmkamasNessuna valutazione finora
- UrticariaDocumento12 pagineUrticarialilyrbrtNessuna valutazione finora
- Connective Tissue DiseasesDocumento54 pagineConnective Tissue DiseasesRatnakar KamathNessuna valutazione finora
- Gilut Herpes ZosteRDocumento24 pagineGilut Herpes ZosteRdimasahadiantoNessuna valutazione finora
- DermatomyositisDocumento26 pagineDermatomyositiszaki100% (1)
- Yeung H Et Al 2012. Patient Reported Reasons For The Discontinuation of Commonly Used Treatments For Moderate To Severe PsoriasisDocumento9 pagineYeung H Et Al 2012. Patient Reported Reasons For The Discontinuation of Commonly Used Treatments For Moderate To Severe PsoriasisAndi MarsaliNessuna valutazione finora
- Atopic DermatitisDocumento10 pagineAtopic DermatitistazzycaNessuna valutazione finora
- Dermatology FinalDocumento16 pagineDermatology FinalMelinda100% (2)
- Bacterial InfectionDocumento41 pagineBacterial InfectionUmmi Rinandari100% (1)
- An Approach To The Patient With ErythrodermaDocumento42 pagineAn Approach To The Patient With ErythrodermaShakilNessuna valutazione finora
- Unit 2 - Physiological Reaction To InjuryDocumento90 pagineUnit 2 - Physiological Reaction To InjuryFabian Chapima100% (1)
- KalsifilaksisDocumento28 pagineKalsifilaksisAnonymous rt6lXkLZNessuna valutazione finora
- Id ModuleDocumento4 pagineId ModuleKumar AdityaNessuna valutazione finora
- Infection UMMP PDFDocumento138 pagineInfection UMMP PDFShafiah Aqilah Mohd JamalNessuna valutazione finora
- Sqweqwesf Erwrewfsdfs Adasd Dhe: Dermnet NZDocumento19 pagineSqweqwesf Erwrewfsdfs Adasd Dhe: Dermnet NZkdwazirNessuna valutazione finora
- JurnalDocumento120 pagineJurnalIman PradanaNessuna valutazione finora
- Psoriasis and Comorbid DeseaseDocumento67 paginePsoriasis and Comorbid DeseaseAl NaifNessuna valutazione finora
- Opportunistic Infections PDFDocumento88 pagineOpportunistic Infections PDFironbuang100% (1)
- Vesiculobullous DiseasesDocumento40 pagineVesiculobullous Diseasessgoeldoc_550661200100% (1)
- Systemic Lupus Erythematosus (SLE)Documento39 pagineSystemic Lupus Erythematosus (SLE)Nadya SabrinaNessuna valutazione finora
- Infections in Pregnancy FinalDocumento67 pagineInfections in Pregnancy FinalkashafNessuna valutazione finora
- 3255 11255 1 PB PDFDocumento4 pagine3255 11255 1 PB PDFArini NurlelaNessuna valutazione finora
- 43861Documento29 pagine43861Min-Joo Esther ParkNessuna valutazione finora
- Referat Refluks Vesikoureter Pada AnakDocumento7 pagineReferat Refluks Vesikoureter Pada AnakprajnamitaNessuna valutazione finora
- Effectiveness of Treatment RegimensDocumento7 pagineEffectiveness of Treatment RegimensprajnamitaNessuna valutazione finora
- Typhoid Intestinal Perforations in Northern GhanaDocumento5 pagineTyphoid Intestinal Perforations in Northern GhanaprajnamitaNessuna valutazione finora
- Typhoid Intestinal Perforations in Northern GhanaDocumento5 pagineTyphoid Intestinal Perforations in Northern GhanaprajnamitaNessuna valutazione finora
- Typhoid Intestinal Perforations in Northern GhanaDocumento7 pagineTyphoid Intestinal Perforations in Northern GhanaprajnamitaNessuna valutazione finora
- Dipake Lamellar Ichthyosis enDocumento6 pagineDipake Lamellar Ichthyosis enprajnamitaNessuna valutazione finora
- Herediter and Acquired Ichthyosis VulgarisDocumento4 pagineHerediter and Acquired Ichthyosis VulgarisprajnamitaNessuna valutazione finora
- 524304Documento5 pagine524304fadhilNessuna valutazione finora
- A Comparison of Continuous Subcutaneous Insulin PDFDocumento8 pagineA Comparison of Continuous Subcutaneous Insulin PDFprajnamitaNessuna valutazione finora
- Emergence of African Species of Dermatophytes in TineaDocumento6 pagineEmergence of African Species of Dermatophytes in TineaprajnamitaNessuna valutazione finora
- A Comparison of Continuous Subcutaneous Insulin PDFDocumento8 pagineA Comparison of Continuous Subcutaneous Insulin PDFprajnamitaNessuna valutazione finora
- Typhoid Intestinal Perforations in Northern GhanaDocumento7 pagineTyphoid Intestinal Perforations in Northern GhanaprajnamitaNessuna valutazione finora
- A Study of Tinea Capitis in ChildrenDocumento4 pagineA Study of Tinea Capitis in ChildrenTantriSaptennoPattiradjawaneNessuna valutazione finora
- Herediter and Acquired Ichthyosis VulgarisDocumento4 pagineHerediter and Acquired Ichthyosis VulgarisprajnamitaNessuna valutazione finora
- Bcie Iktiosis DDDocumento2 pagineBcie Iktiosis DDprajnamitaNessuna valutazione finora
- Dipake Lamellar Ichthyosis enDocumento6 pagineDipake Lamellar Ichthyosis enprajnamitaNessuna valutazione finora
- Overcoming The Barrier Treatment of Ichthyosis PDFDocumento5 pagineOvercoming The Barrier Treatment of Ichthyosis PDFprajnamitaNessuna valutazione finora
- 1 SS Skin Cancer - Chapter 1Documento12 pagine1 SS Skin Cancer - Chapter 1Muhammad IqbalNessuna valutazione finora
- Dipake Lamellar Ichthyosis enDocumento6 pagineDipake Lamellar Ichthyosis enprajnamitaNessuna valutazione finora
- Prevalence of Inherited IchthyosisDocumento7 paginePrevalence of Inherited IchthyosisprajnamitaNessuna valutazione finora
- Inherited Nonsyndromic Ichthyoses - An Update On Pathophysiology, Diagnosis and TreatmentDocumento16 pagineInherited Nonsyndromic Ichthyoses - An Update On Pathophysiology, Diagnosis and TreatmentDimas PrajagoptaNessuna valutazione finora
- Prevalence of Inherited IchthyosisDocumento7 paginePrevalence of Inherited IchthyosisprajnamitaNessuna valutazione finora
- Loss of Funtion Filagrin Mutation Caused IVDocumento6 pagineLoss of Funtion Filagrin Mutation Caused IVprajnamitaNessuna valutazione finora
- IchthyosisDocumento154 pagineIchthyosisprajnamitaNessuna valutazione finora
- Bcie Iktiosis DDDocumento2 pagineBcie Iktiosis DDprajnamitaNessuna valutazione finora
- S1 Guidelines For The Diagnosis and Treatment IchthyosisDocumento13 pagineS1 Guidelines For The Diagnosis and Treatment IchthyosisprajnamitaNessuna valutazione finora
- Sumber DD IktiosisDocumento9 pagineSumber DD IktiosisprajnamitaNessuna valutazione finora
- LEGO Group A Strategic and Valuation AnalysisDocumento85 pagineLEGO Group A Strategic and Valuation AnalysisRudmila Ahmed50% (2)
- The Invisible Museum: History and Memory of Morocco, Jewish Life in FezDocumento1 paginaThe Invisible Museum: History and Memory of Morocco, Jewish Life in FezmagnesmuseumNessuna valutazione finora
- XT 125Documento54 pagineXT 125ToniNessuna valutazione finora
- 3 Habits For SuccessDocumento1 pagina3 Habits For SuccesssiveramNessuna valutazione finora
- Operations Management-CP PDFDocumento4 pagineOperations Management-CP PDFrey cedricNessuna valutazione finora
- 21 and 22 Case DigestDocumento3 pagine21 and 22 Case DigestRosalia L. Completano LptNessuna valutazione finora
- Eric Thomas Grissen - The American Technology Awards, or "The Termans"Documento1 paginaEric Thomas Grissen - The American Technology Awards, or "The Termans"Eric Thomas GrissenNessuna valutazione finora
- TRUE/FALSE. Write 'T' If The Statement Is True and 'F' If The Statement Is FalseDocumento44 pagineTRUE/FALSE. Write 'T' If The Statement Is True and 'F' If The Statement Is FalseYukiNessuna valutazione finora
- Review - ChE ThermoDocumento35 pagineReview - ChE ThermoJerome JavierNessuna valutazione finora
- Republic of The Philippines Legal Education BoardDocumento25 pagineRepublic of The Philippines Legal Education BoardPam NolascoNessuna valutazione finora
- Catalogue of Khalsa Darbar Records Vol.1 - Compiled by Sita Ram KohliDocumento180 pagineCatalogue of Khalsa Darbar Records Vol.1 - Compiled by Sita Ram KohliSikhDigitalLibrary100% (1)
- Evolut Pro Mini Product Brochure PDFDocumento8 pagineEvolut Pro Mini Product Brochure PDFBalázs PalcsikNessuna valutazione finora
- Good Governance and Social Responsibility-Module-1-Lesson-3Documento11 pagineGood Governance and Social Responsibility-Module-1-Lesson-3Elyn PasuquinNessuna valutazione finora
- B. Complete The Following Exercise With or Forms of The Indicated VerbsDocumento4 pagineB. Complete The Following Exercise With or Forms of The Indicated VerbsLelyLealGonzalezNessuna valutazione finora
- Critical Evaluation of Biomedical LiteraturesDocumento34 pagineCritical Evaluation of Biomedical LiteraturesPratibha NatarajNessuna valutazione finora
- The City of GodDocumento16 pagineThe City of GodJei Em MonteflorNessuna valutazione finora
- Foods: Ffee AdulterationDocumento11 pagineFoods: Ffee AdulterationJpNessuna valutazione finora
- Botswana Ref Ranges PaperDocumento7 pagineBotswana Ref Ranges PaperMunyaradzi MangwendezaNessuna valutazione finora
- Fundamental of Transport PhenomenaDocumento521 pagineFundamental of Transport Phenomenaneloliver100% (2)
- Portfolio Assignment MaternityDocumento2 paginePortfolio Assignment Maternityapi-319339803100% (1)
- Computer Science Past Papers MCQS SolvedDocumento24 pagineComputer Science Past Papers MCQS SolvedLEGAL AFFAIRS DIVISION100% (1)
- Liddell Hart PDFDocumento5 pagineLiddell Hart PDFMohamed Elkhder100% (1)
- Strama-Ayala Land, Inc.Documento5 pagineStrama-Ayala Land, Inc.Akako MatsumotoNessuna valutazione finora
- Body ImageDocumento7 pagineBody ImageCristie MtzNessuna valutazione finora
- Historical Perspective of Financial Reporting Regulations in MalaysiaDocumento2 pagineHistorical Perspective of Financial Reporting Regulations in Malaysiauglore100% (6)
- Meter BaseDocumento6 pagineMeter BaseCastor JavierNessuna valutazione finora
- Movie ReviewDocumento2 pagineMovie ReviewJohanna Gwenn Taganahan LomaadNessuna valutazione finora
- COPARDocumento21 pagineCOPARLloyd Rafael EstabilloNessuna valutazione finora
- National Geographic Traveller India - July 2016-P2PDocumento104 pagineNational Geographic Traveller India - July 2016-P2PPeter100% (2)
- Administrative Clerk Resume TemplateDocumento2 pagineAdministrative Clerk Resume TemplateManuelNessuna valutazione finora