Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Cardio-Vascular Disease: Mitral Stenosis & Mitral Regurgitation
Caricato da
yulia silvi0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
57 visualizzazioni25 paginejhijok
Titolo originale
mitralstenosis-160629184855 (2)
Copyright
© © All Rights Reserved
Formati disponibili
PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentojhijok
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
57 visualizzazioni25 pagineCardio-Vascular Disease: Mitral Stenosis & Mitral Regurgitation
Caricato da
yulia silvijhijok
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 25
Cardio-Vascular Disease
Mitral Stenosis & Mitral Regurgitation
Dr. Deepak K. Gupta
Valvular Heart Diseases
• Mitral stenosis
• Mitral regurgitation
• Aortic stenosis
• Aortic regurgitation
• Tricuspid stenosis
• Tricuspid regurgitation
• Pulmonic stenosis
• Pulmonic regurgitation
Mitral Stenosis
• Almost always rheumatic in
origin
– although in older people it can be
caused by heavy calcification
– also a rare form of congenital MS
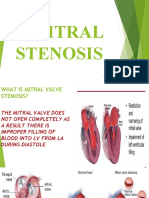
• Mitral valve orifice slowly gets
diminished (5 cm2 - 1 cm2 )
– Progressive fibrosis,
– Calcification of the valve leaflets
– Fusion of the cusps and
subvalvular apparatus.
Aetiology and Pathophysiology
• The flow of blood from LA to LV is restricted
and left atrial pressure rises,
• Leading to pulmonary venous congestion and
breathlessness.
• There is dilatation and hypertrophy of the LA,
• And left ventricular filling becomes more
dependent on left atrial contraction.
Aetiology and Pathophysiology
• Situation which increases heart rate or cardiac
output like pregnancy and exercise – poorly
tolerated
– shortens diastole and produces a further rise in left
atrial pressure
• Atrial fibrillation - progressive dilatation of the LA
• Pulmonary oedema - accompanying tachycardia
and loss of atrial contraction
• All these lead to marked haemodynamic
deterioration
Clinical features: Symptom
• Patients usually remain asymptomatic until the stenosis is <
2 cm2
• Breathlessness - Reduced lung compliance, due to chronic
pulmonary venous congestion
• Fatigue - low cardiac output
– Exercise tolerance typically diminishes very slowly over many
years
• Oedema, ascites (right heart failure)
• Palpitation (atrial fibrillation)
• Haemoptysis (pulmonary congestion, pulmonary embolism)
• Cough (pulmonary congestion)
• Chest pain (pulmonary hypertension)
• Thromboembolic complications (e.g. stroke, ischaemic limb)
Clinical features: Signs
• Atrial fibrillation
• Mitral facies (calcification)
• Auscultation
– Loud first heart sound (S1),
– Opening snap: may be audible and move closer to S2
with increase in severity
– Mid-diastolic murmur: Turbulent flow produces
characteristic low pitched
– accentuated by exercise
– inaudible if the valve is heavily calcified.
• Crepitations, pulmonary oedema, effusions (raised
pulmonary capillary pressure)
Investigations
• ECG
– P mitrale or atrial
fibrillation
– Right ventricular
hypertrophy: tall R
waves in V1–V3
• Chest x-ray
– Enlarged LA and
appendage
– Signs of pulmonary
venous congestion
Investigations
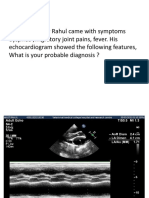
• Echo -
– Thickened immobile cusps
– Reduced valve area
– Reduced rate of diastolic filling of LV
– Enlarged LA
• Doppler echocardiography - definitive evaluation
– Pressure gradient across mitral valve
– Pulmonary artery pressure
– Left ventricular function
• Cardiac catheterisation - assessment of coexisting
conditions.
– Coronary artery disease
– Mitral stenosis and regurgitation
– Pulmonary artery pressure
Management
• Patients with minor symptoms should be
treated medically
• Surgical Management: patient remains
symptomatic despite medical treatment or if
pulmonary hypertension develops
– Balloon valvuloplasty,
– Mitral valvotomy
– Mitral valve replacement
Medical Management
• Systemic embolism: anticoagulants
• Atrial fibrillation: ventricular rate control by
digoxin, β-blockers or rate-limiting calcium
antagonists
• Pulmonary congestion: diuretic therapy
• Antibiotic prophylaxis against infective
endocarditis is no longer routinely recommended
Surgical Management
• Mitral valvuloplasty: treatment of choice if
specific criteria are fulfilled
– Significant symptoms
– Isolated mitral stenosis
– No (or trivial) mitral regurgitation
– Mobile, non-calcified valve/subvalve apparatus on
ech
– LA free of thrombus
Mitral Balloon Valvotomy.A. After transseptal
puncture, the deflated balloon catheter is
advanced across the interatrial septum, then
across the mitral valve and into the left
ventricle. B.-D. The balloon is inflated stepwise
within the mitral orifice
Surgical Management
• Valvoplasty: closed or open mitral valvotomy
are acceptable alternatives
• Valve replacement: substantial mitral reflux or
if the valve is rigid and calcified
• Regular follow up: at 1–2-yearly intervals
because restenosis may occur
Valve replacement
Mitral Regurgitation
• Backflow of blood through a defective
heart valve.
• Any one or more of the five functional
components of the mitral valve apparatus
– Leaflets,
– Annulus,
– Chordae tendineae,
– Papillary muscles,
– Subjacent myocardium
Etiology
• Acute
– Endocarditis
– Papillary muscle rupture (post-MI)
– Trauma
– Chordal rupture/leaflet flail
• Chronic
– Myxomatous (MVP)
– Rheumatic fever
– Endocarditis (healed)
– Mitral annular calcification
– Congenital (cleft, AV canal)
– Hypertrophic obstructive cardiomyopathy (HOCM) with systolic
anterior motion (SAM)
– Ischemic (LV remodeling)
– Dilated cardiomyopathy
– Radiation
Pathophysiology
• Regurgitation into the LA produces LA
dilatation
• But little increase in left atrial pressure if the
regurgitation is chronic
– as the regurgitant flow is accommodated by the
large left atrium
• Acute mitral regurgitation - normal
compliance of the left atrium does not allow
much dilatation
– left atrial pressure rises.
Clinical features
• Symptoms depend on how suddenly the
regurgitation develops
• Chronic: symptom complex that is similar to that
of MS
• Acute: usually presents with acute pulmonary
oedema
• Symptom
– Dyspnoea or Orthopnea (pulmonary venous
congestion)
– Fatigue (low cardiac output)
– Palpitation (atrial fibrillation, increased stroke
volume)
– Oedema, ascites (right heart failure)
Signs
• Atrial fibrillation/flutter
• Cardiomegaly: displaced hyperdynamic apex beat
• Apical pansystolic murmur ± thrill
• Signs of pulmonary venous congestion (crepitations,
pulmonary oedema, effusions)
• Signs of pulmonary hypertension and right heart
failure
• Floppy mitral valve - mid-systolic click
• Prominent third heart sound - sudden rush of blood
back into the dilated left ventricle in early diastole
Investigations
• ECG
– Left atrial hypertrophy (if not in AF)
– Left ventricular hypertrophy
• Chest x-ray
– Enlarged LA
– Enlarged LV
– Pulmonary venous congestion
– Pulmonary oedema (if acute)
Investigations
• Echo
– Dilated LA, LV
– Dynamic LV (unless myocardial dysfunction
predominates)
– Structural abnormalities of mitral valve (e.g. prolapse)
• Doppler: Detects and quantifies regurgitation
• Cardiac catheterisation
– Dilated LA, dilated LV, mitral regurgitation
– Pulmonary hypertension
– Coexisting coronary artery disease
Management
• Mild MR can be treated medically.
– Diuretics
– Vasodilators
– Digoxin if atrial fibrillation is present
– Anticoagulants if atrial fibrillation is present
• Evidence of progressive cardiac enlargement -
early surgical intervention.
– Valvotomy, Valvoplasty and valve replacement.
• Repair the valve and restore mitral valve function
by inserting an annuloplasty ring
– overcome annular dilatation
– bring the valve leaflets closer together
THANKS……
Like, share and comment on
https://www.facebook.com/notesdental
http://www.slideshare.net/DeepakKumarGupta2
www.facebook.com/notesdental
www.facebook.com/notesdental
Potrebbero piacerti anche
- ELECTROCARDIOGRAPHY IN ISCHEMIC HEART DISEASEDa EverandELECTROCARDIOGRAPHY IN ISCHEMIC HEART DISEASENessuna valutazione finora
- Valvular Heart Disease. KulDocumento60 pagineValvular Heart Disease. KulIntan Kumalasari RambeNessuna valutazione finora
- Cardiac Tamponade, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDa EverandCardiac Tamponade, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNessuna valutazione finora
- Heart Valve Diseases, A Simple Guide to These ConditionsDa EverandHeart Valve Diseases, A Simple Guide to These ConditionsNessuna valutazione finora
- A Simple Guide to the Heart beats, Related Diseases And Use in Disease DiagnosisDa EverandA Simple Guide to the Heart beats, Related Diseases And Use in Disease DiagnosisValutazione: 5 su 5 stelle5/5 (1)
- Mitral StenosisDocumento17 pagineMitral Stenosispriyanka bhowmikNessuna valutazione finora
- Congestive Heart FailureDocumento86 pagineCongestive Heart FailureNabeel ShahzadNessuna valutazione finora
- MVR CabgDocumento57 pagineMVR CabgRoshani sharmaNessuna valutazione finora
- Aortic StenosisDocumento3 pagineAortic StenosisMaxine BaraquiaNessuna valutazione finora
- Cardiovascular Pathology 1:: Blood VesselsDocumento48 pagineCardiovascular Pathology 1:: Blood VesselsRaiver CadenNessuna valutazione finora
- Jugular Venous Pulse: Madras Medical MissionDocumento53 pagineJugular Venous Pulse: Madras Medical MissionJoshua JayakaranNessuna valutazione finora
- Mitral StenosisDocumento50 pagineMitral Stenosissruthimeena6891Nessuna valutazione finora
- Cardiovascular Disorders: BY: Maximin A. Pomperada, RN, MANDocumento65 pagineCardiovascular Disorders: BY: Maximin A. Pomperada, RN, MANRellie Castro100% (1)
- Valvular Heart Disease 2Documento46 pagineValvular Heart Disease 2Topea BogdanNessuna valutazione finora
- Rheumatic Heart DiseaseDocumento30 pagineRheumatic Heart DiseaseDhiraj PantNessuna valutazione finora
- ECG Master Class-3Documento97 pagineECG Master Class-3Shohag ID CenterNessuna valutazione finora
- BBB EcgDocumento33 pagineBBB EcgLokbre YoasNessuna valutazione finora
- Valvular Heart DiseaseDocumento54 pagineValvular Heart DiseaseKiki RizkyNessuna valutazione finora
- Cardiac Output and Hemodynamic MeasurementDocumento29 pagineCardiac Output and Hemodynamic Measurementdeepa100% (1)
- Slide ShareDocumento53 pagineSlide Sharesamantha_monter3225Nessuna valutazione finora
- Basic Arrythmia AnalysisDocumento60 pagineBasic Arrythmia AnalysisZakky KurniawanNessuna valutazione finora
- Avnrt AvrtDocumento21 pagineAvnrt AvrtRima Rovanne Wenas100% (1)
- Right Heart Catheterization, NicvdDocumento17 pagineRight Heart Catheterization, NicvdNavojit ChowdhuryNessuna valutazione finora
- Mitral RegurgitationDocumento11 pagineMitral RegurgitationAbdur RaqibNessuna valutazione finora
- Hypertensive Crisis: Megat Mohd Azman Bin AdzmiDocumento34 pagineHypertensive Crisis: Megat Mohd Azman Bin AdzmiMegat Mohd Azman AdzmiNessuna valutazione finora
- Pericardial Diseases 3rd Yr BMTDocumento38 paginePericardial Diseases 3rd Yr BMT211941103014100% (1)
- Asthma and CopdDocumento44 pagineAsthma and CopdBeer Dilacshe100% (1)
- L-R ShuntDocumento88 pagineL-R ShuntnanohaniwiekoNessuna valutazione finora
- Chapter 42 - Sepsis, Septic Shock, and Multiple Organ FailureDocumento15 pagineChapter 42 - Sepsis, Septic Shock, and Multiple Organ FailureWorrawalun FuktongNessuna valutazione finora
- Cardiac CycleDocumento12 pagineCardiac Cycleanupam manu100% (1)
- Ngaji Arrythmia Cordis 3Documento122 pagineNgaji Arrythmia Cordis 3Dhita Dwi NandaNessuna valutazione finora
- FinalDocumento56 pagineFinalvamshidhNessuna valutazione finora
- Valvular Heart DiseaseDocumento10 pagineValvular Heart DiseaseEzyan SyaminNessuna valutazione finora
- Left Ventricular Non-CompactionDocumento20 pagineLeft Ventricular Non-CompactionlawlietNessuna valutazione finora
- Cardiac (Heart) FailureDocumento27 pagineCardiac (Heart) FailureSanthoshi Sadhanaa SankarNessuna valutazione finora
- Properties of Cardiac Muscle and Conducting SystemsDocumento38 pagineProperties of Cardiac Muscle and Conducting Systemsnirilib100% (4)
- Electrolyte DisordersDocumento10 pagineElectrolyte DisordersSlavicaNessuna valutazione finora
- Acute Resp FailureDocumento52 pagineAcute Resp FailureAlex ChiuNessuna valutazione finora
- Anaesthesia and Atrial FibrillationDocumento15 pagineAnaesthesia and Atrial FibrillationNaresh Dhawan100% (1)
- Ecg Pathology 02Documento95 pagineEcg Pathology 02Andi MP Manurung100% (1)
- Electrocardiogram (E.C.G)Documento51 pagineElectrocardiogram (E.C.G)Jamuna PatelNessuna valutazione finora
- Heart Sounds: Mitral Regurgitation Congestive Heart FailureDocumento6 pagineHeart Sounds: Mitral Regurgitation Congestive Heart FailurecindyNessuna valutazione finora
- Aortic RegurgitationDocumento19 pagineAortic RegurgitationsunilgenextNessuna valutazione finora
- TOF Patient EducationDocumento8 pagineTOF Patient EducationMia MiaNessuna valutazione finora
- Mesenteric Ischemia in Dilated CardiomyopathyDocumento30 pagineMesenteric Ischemia in Dilated CardiomyopathyJo AnneNessuna valutazione finora
- ElectrocardiogramDocumento52 pagineElectrocardiogramTuong HoangManhNessuna valutazione finora
- Atrial Septal DefectDocumento12 pagineAtrial Septal DefectNurruhaizi Aizi100% (1)
- Congestive Heart FailureDocumento20 pagineCongestive Heart FailurehuzaifahjusohNessuna valutazione finora
- Cardiac AsthmaDocumento12 pagineCardiac AsthmaNeupane KsabNessuna valutazione finora
- Cardiomyopathy: M Taufik I, MDDocumento28 pagineCardiomyopathy: M Taufik I, MDChi RahmawatiNessuna valutazione finora
- ICP Head InjuryDocumento57 pagineICP Head InjuryWengel RedkissNessuna valutazione finora
- PericarditisDocumento29 paginePericarditisPavin KumarNessuna valutazione finora
- ECG Changes in Drug and Electrolyte AbnormalitiesDocumento28 pagineECG Changes in Drug and Electrolyte AbnormalitiesNachiket Vijay PotdarNessuna valutazione finora
- Right Ventricular Myocardial InfarctionDocumento43 pagineRight Ventricular Myocardial Infarctionrudresh m g0% (2)
- Mitral Valve Prolapse, Flailed Mitral Valve Mitral Annular CalcificationDocumento33 pagineMitral Valve Prolapse, Flailed Mitral Valve Mitral Annular CalcificationcafemedNessuna valutazione finora
- Cardiovascular ExaminationDocumento37 pagineCardiovascular ExaminationmulatumeleseNessuna valutazione finora
- Focal Atrial Tachycardia I: Clinical Features, DiagnosisDocumento10 pagineFocal Atrial Tachycardia I: Clinical Features, Diagnosisapi-26166949Nessuna valutazione finora
- Seminar On Occlusion On 11 May 2022Documento25 pagineSeminar On Occlusion On 11 May 2022Dr Saurav kumar DuttaNessuna valutazione finora
- John Murtagh's Cautionary Tales PDFDocumento383 pagineJohn Murtagh's Cautionary Tales PDFvistamaniac100% (5)
- BUTRANS-buprenorphine Patch, Extended Release Purdue Pharma LPDocumento64 pagineBUTRANS-buprenorphine Patch, Extended Release Purdue Pharma LPmeiraimNessuna valutazione finora
- Pharmaceuticals 11 00094Documento14 paginePharmaceuticals 11 00094CindyGaniNessuna valutazione finora
- Dracula ScriptDocumento69 pagineDracula Scriptapi-160443830Nessuna valutazione finora
- Endocrine System - LectureDocumento213 pagineEndocrine System - LectureRosita Antiquina Elopre100% (1)
- CHPP 0913 ClarkDocumento7 pagineCHPP 0913 ClarkFarzana AfrinNessuna valutazione finora
- Mosquitoe Repellent Plants Final 31 AugustDocumento48 pagineMosquitoe Repellent Plants Final 31 AugustHomero SilvaNessuna valutazione finora
- Bes More On MiasmDocumento16 pagineBes More On MiasmSatyendra RawatNessuna valutazione finora
- Total Protein SpinreactDocumento1 paginaTotal Protein Spinreactariyan khanNessuna valutazione finora
- Ob 2Documento9 pagineOb 2Danica Chiara Motia100% (1)
- Chemistry in Everyday LifeDocumento398 pagineChemistry in Everyday LifeArsh DhawanNessuna valutazione finora
- Dettol Liquid Antiseptic Disinfected ProposalDocumento7 pagineDettol Liquid Antiseptic Disinfected ProposalabdullahNessuna valutazione finora
- Neonatal Birth InjuriesDocumento22 pagineNeonatal Birth InjuriesPauli Monsálvez ElissaldeNessuna valutazione finora
- New Diagnostic Criteria For Acute Pericarditis A Cardiac MRIDocumento6 pagineNew Diagnostic Criteria For Acute Pericarditis A Cardiac MRIsaNessuna valutazione finora
- Jet Lag PDFDocumento8 pagineJet Lag PDFIan FitzpatrickNessuna valutazione finora
- Synthesis PaperDocumento19 pagineSynthesis Paperapi-330084238Nessuna valutazione finora
- LW Challenge FormDocumento14 pagineLW Challenge Formapi-311321754Nessuna valutazione finora
- Ayurveda PDFDocumento12 pagineAyurveda PDFsanjit0907_982377739Nessuna valutazione finora
- Legal Medicine NotesDocumento61 pagineLegal Medicine NotesJocelyn Yemyem Mantilla VelosoNessuna valutazione finora
- Tanganyika Nacte Past Paper-1Documento116 pagineTanganyika Nacte Past Paper-1Mnawaru KhalfaniNessuna valutazione finora
- Adilah TranskripDocumento1 paginaAdilah Transkripadik_mira893219Nessuna valutazione finora
- 200 Bed Hospital Project ReportDocumento59 pagine200 Bed Hospital Project ReporttonyNessuna valutazione finora
- Biomedical Signal Processing and ControlDocumento6 pagineBiomedical Signal Processing and ControlIntan Alwaystry TobehappyNessuna valutazione finora
- EnVisorA1 User' SGuide enDocumento366 pagineEnVisorA1 User' SGuide enFrank QuitianNessuna valutazione finora
- Anisometropia in Children and Its ProblemDocumento37 pagineAnisometropia in Children and Its ProblemekaNessuna valutazione finora
- ACD/Percepta: Overview of The ModulesDocumento91 pagineACD/Percepta: Overview of The ModulesTinto J AlencherryNessuna valutazione finora
- Procedural Checklist NCM 112 RLE Preparing A Sterile Field Opening A Sterile Pack Adding Items To A Sterile Field Adding Liquids To A Sterile Field Skin PreparationDocumento5 pagineProcedural Checklist NCM 112 RLE Preparing A Sterile Field Opening A Sterile Pack Adding Items To A Sterile Field Adding Liquids To A Sterile Field Skin PreparationAbegail Eliah EstalaneNessuna valutazione finora
- Beneficence and Non-MaleficenceDocumento3 pagineBeneficence and Non-MaleficenceRathin BanerjeeNessuna valutazione finora
- RBC PathologyDocumento7 pagineRBC PathologyKent CruzNessuna valutazione finora