Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Imaging Features of Inflammatory Breast Disorders: A Pictorial Essay
Caricato da
seruniallisaaslimTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Imaging Features of Inflammatory Breast Disorders: A Pictorial Essay
Caricato da
seruniallisaaslimCopyright:
Formati disponibili
Pictorial Essay | Breast Imaging
https://doi.org/10.3348/kjr.2018.19.1.5
pISSN 1229-6929 · eISSN 2005-8330
Korean J Radiol 2018;19(1):5-14
Imaging Features of Inflammatory Breast Disorders:
A Pictorial Essay
Po Wey Leong, MBBS, MMED, FRCR1, Niketa Chandrakant Chotai, MBBS, FRCR1,
Supriya Kulkarni, MD, DMRD, DNB, ABR2
1
Department of Diagnostic Radiology, Tan Tock Seng Hospital, Jalan Tan Tock Seng 308433, Singapore; 2Princess Margaret Hospital, Department of
Medical Imaging, Toronto, ON M5G 2M9, Canada
Inflammatory breast disorders include a wide array of underlying causes, ranging from common benign infection, non-
infectious inflammation and inflammation resulting from underlying breast malignancy. Because it is at times difficult to
distinguish mastitis and breast cancer based on clinical features, awareness of detailed imaging features may be helpful for
better management of inflammatory breast disorders. Therefore, this pictorial essay intends to demonstrate radiologic
findings of a variety of inflammatory breast disorders, using selected cases with mammography, ultrasound and magnetic
resonance images.
Keywords: Breast; Inflammation; Cancer; Ultrasound; Mammography; Magnetic resonance imaging
INTRODUCTION dilemma. Failure to respond to antibiotic therapy is usually
an indication for a biopsy to rule out underlying malignancy
Mastitis refers to inflammation of the breast parenchyma, (1, 3, 4). This pictorial essay illustrates a variety of common
often presenting with pain, heat and redness that may and uncommon inflammatory breast conditions encountered
be a debilitating illness with prolonged morbidity (1). at a busy breast imaging center.
It may also present with a wide array of other non-
specific symptoms, that may lead to delayed diagnosis Radiological Signs of Breast Inflammation
and inappropriate treatment (2). Broadly, inflammatory
disorders of the breast can be divided into three categories: The breast is a superficial organ and often inflammation
infectious mastitis, non-infectious mastitis and mastitis would involve the overlying skin. Features of cellulitis
related to underlying malignancy (1, 3). Clinical and such as skin thickening and subcutaneous edema should
radiological features of benign mastitis commonly overlap be noted. Radiological imaging is more advantageous than
with breast malignancies, further adding to the diagnostic clinical examination in evaluating skin thickening as it
allows accurate delineation of its extent, measurement and
Received February 14, 2017; accepted after revision July 18, 2017.
comparison to surrounding skin and contralateral breast (1).
Corresponding author: Po Wey Leong, MBBS, MMED, FRCR,
Diagnostic Radiology, Tan Tock Seng Hospital, Singapore 11 Jalan Subcutaneous edema is easily evaluated using Doppler US,
Tan Tock Seng, Singapore 308433, Singapore. revealing diffuse increase in thickening and echogenicity
• Tel: 65 97380529 • Fax: 65 6357 8158/8159 of the subcutaneous tissue and later accumulation of fluid
• E-mail: powey@hotmail.com
This is an Open Access article distributed under the terms of in the subcutaneous tissue (Fig. 1A). On mammogram,
the Creative Commons Attribution Non-Commercial License subcutaneous edema manifests as diffuse increase in breast
(http://creativecommons.org/licenses/by-nc/4.0) which permits density or increased interstitial markings (5).
unrestricted non-commercial use, distribution, and reproduction in
any medium, provided the original work is properly cited.
Hyperemia (increased vascularity) of the breast tissue
Copyright © 2018 The Korean Society of Radiology 5
Leong et al.
A B
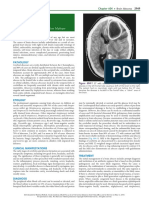
Fig. 1. Pueperal Mastitis in 29-year-old female.
A. Ultrasound reveals features of subcutaneous edema with skin thickening with increase in echogenicity of subcutaneous tissue. Fluid is observed
as intervening hypoechoic lines (white arrows) in subcutaneous tissue. B. Ultrasound with color Doppler also reveals ill-defined hypoechoic fluid
collection with heterogeneous content within site of inflammation. Hyperemia of subcutaneous tissue surrounding collection is noted.
A B
Fig. 2. Reactive versus malignant lymphadenopathy.
A. Ultrasound of right axilla in 33-year-old female with large right breast abscess reveals enlarged lymph node with smooth thickening of cortex.
Normal fatty hilum and reniform configuration is preserved. These are features of benign reactive lymph node. B. Ultrasound of right axilla in
52-year-old female, with painful right breast mass and palpable right axillary nodes. Lymph nodes reveal bulky cortex (white arrows) and loss of
normal fatty hilum (black arrow), features that are more worrisome for malignant involvement. Ultrasound-guided biopsy of node was conducted
and diagnosis of lymphoma was made.
is another sign of inflammation. This can be evaluated collections within the site of inflammation. These commonly
using Doppler US, revealing increased arterial and venous demonstrate hypoechoic and heterogeneous content and
structures (1) (Fig. 1B). Lactiferous duct abnormalities may show irregularly thickened walls. Collections may
such as duct dilatation, thickened walls and presence fistulate into the skin or intra-mammary ducts (1).
of contents within the ducts should be investigated as Breast inflammation may involve the axillary lymph nodes
some inflammatory conditions are related to lactiferous and cause reactive enlargement. Differentiating benign
duct involvement. One should also notice possible fluid reactive lymphadenopathy from malignant lymphadenopathy
6 Korean J Radiol 19(1), Jan/Feb 2018 kjronline.org
Inflammatory Breast Disorders: A Pictorial Essay
A B
Fig. 3. Infected galactocele in 32-year-old lactating female presenting with right breast swelling and pain.
A. Mammogram of right breast in mediolateral oblique projection shows well-defined predominantly lucent mass with some opaque material
within (white arrow). This appearance is in keeping with presence of both lucent fat and dense proteinaceous content (milk and inflammatory
cells). B. Ultrasound demonstrates large collection in right breast with heterogeneous cystic-solid content. This lesion was aspirated which
yielded milk content and inflammatory cells. No malignant cell was observed. Subsequent follow-up ultrasound examinations reveal gradual
resolution of this lesion.
based on imaging features alone can be challenging. therapy, in which case histological sampling should be
Benign reactive lymph nodes generally demonstrate smooth conducted (1, 3, 8).
thickening of the cortices with preservation of normal fatty
hilum (Fig. 2A). In contrast, tumor involved lymph nodes Infected Galactocele
tend to demonstrate irregular cortical thickening with loss Galactoceles are the most common lesions in lactating
or replacement of the fatty hilum (1, 3) (Fig. 2B). women. Milk is retained and stagnant when breast-feeding
is stopped, causing ductal dilatation and development
Infectious Mastitis of cysts or galactoceles. Infection is a relative common
complication of galactoceles (8). Galactoceles will appear
Acute Puerperal Mastitis similar to abscesses but follow a ductal distribution (3).
Mastitis that occurs during lactation is termed puerperal Diagnosis is made based on an appropriate clinical picture
mastitis. This is the most common form of mastitis and (i.e., history of recent lactation) and aspiration of mixed
usually occurs from infection with Staphylococcus aureus milky and purulent material from the cyst (8) (Fig. 3).
or Streptococcus bacteria. This may lead to reduced milk
production and is a common reason for mothers to stop Non-Puerperal Subareolar Mastitis
breast feeding (6). Infection often arises from disruption Non-puerperal subareolar mastitis and breast abscess,
to the skin surface of the nipple areolar complex and milk also known as Zuska’s disease is an uncommon and
stasis is a risk factor for infection (7). Most patients will recurring disease strongly linked to cigarette smoking (2,
respond to antibiotic treatment, but a small percentage 9) (Fig. 4). It frequently affects middle-age females in
may develop abscess collections, that may complicate their 40s but may affect a wide range of ages (mid-teens-
treatment and require further drainage. Ultrasound is useful 80s) and may even be observed in males (2) (Fig. 5). This
for detecting these collections (Fig. 1B). Although rare, is caused by squamous metaplasia and proliferation of the
one should always keep in mind the possibility of cancer epithelium in the lactiferious ducts, causing obstruction
in puerperal mastitis that does not respond to antibiotic and secretory stasis leading to abscess formation. They
kjronline.org Korean J Radiol 19(1), Jan/Feb 2018 7
Leong et al.
A B
C
Fig. 4. Non-pueperal subareolar abscess in 49-year-old female with history of smoking. This patient presented with palpable
retroareolar lump in right breast.
A. Mammogram of right breast in mediolateral oblique projections reveals retro-areolar opacity (black arrow). B. Ultrasound reveals retro-areolar
collection with increased peripheral vascularity in right breast. C. T2 weighted and post-contrast T1-weighted MR imaging shows cystic lesion in
subareolar region of right breast on T2-weighted image (white arrow). This also demonstrates rim enhancement on post-contrast T1-weighted
image (black arrow). Repeat ultrasound study conducted three months later reveals slightly smaller but persistent subareolar collection. This
lesion was biopsied and inflammatory cells were seen. No malignant cells were obtained.
present as recurring abscesses, often with fistulous tracks In some cases, it may occur in patients with pre-existing
extending to the skin near the periareolar region (1, 2, conditions such as diabetes and rheumatoid arthritis.
10). Initial infections are usually caused by Staphylococcus Staphylococcus aureus is the most common pathogen. These
bacteria. Subsequent recurring episodes of infection may abscesses typically respond well to antibiotic treatment and
be caused by mixed flora of bacteria, including anaerobes, drainage, and they tend not to recur (10).
and can be more complicated to treat with higher rates Peripheral breast abscesses may also occur in
of recurrence. Radiological features of subareolar mastitis patients with pre-existing cystic breast conditions, with
and inflammatory breast carcinoma may be similar (2). If superimposed infection of breast cyst (1). Patients may
clinically suspected, biopsy should be conducted to exclude present with a painful palpable lump in the breast. Typical
presence of malignancy. features of a infected breast cysts include thickening of the
cyst wall, increased peripheral vascularity and presence of
Peripheral Non-Puerperal Breast Abscesses echogenic debris within the cyst (1, 3) (Fig. 6).
Peripheral breast abscesses usually occur in older women.
8 Korean J Radiol 19(1), Jan/Feb 2018 kjronline.org
Inflammatory Breast Disorders: A Pictorial Essay
Post-Procedural Infections presents as a unilateral solitary hard breast lump, that
Infections following invasive procedures such as breast may turn into an abscess, form fistulas or ulcerate into
surgery or biopsy are a relatively common cause of breast the skin. Less commonly, tuberculosis of the breast can
infection. Diagnosis is usually straightforward with the present as a multifocal disseminated disease with multiple
appropriate clinical history (1) (Fig. 7). communicating abscesses and discharging sinuses (Fig.
8). A rare sclerosing type, of which excessive fibrosis is a
Rare Forms of Infectious Mastitis dominant feature, has also been described, in which the
Uncommon microorganisms such as mycobacterium whole breast is hard with nipple retraction. Diagnosis is
tuberculosis, salmonella and fungi may also infect the usually conformed on tissue sampling and detection of acid-
breast. Tuberculosis of the breast is a rare extra-pulmonary fast bacilli on Ziehl-Neelsen stain or by culture (9, 11, 12).
manifestation of tuberculosis infection. It most commonly
A B C
Fig. 5. Subaerolar abscess in 49-year-old male, presenting with left breast pain and swelling.
A. Mammogram of both breasts in mediolateral oblique projections demonstrates left breast retro-areolar opacity (white arrow). Prominent left
axillary node is also seen (black arrow). B. Ultrasound of left breast with color Doppler reveals hypoechoic collection in left subareolar region
with echogenic internal debris and increased peripheral vascularity. Ultrasound guided tru-cut biopsy of this lesion was conducted which yielded
inflammatory cells. No malignant cells were observed. C. Post contrast T1 weighted fat saturated MR imaging of both breasts in axial plane
reveals subareolar rim-enhancing collection in left breast (white arrow). Fistulous tract extending to skin surface was also noted (black arrow).
A B C
Fig. 6. Peripheral breast abscesses from infected cysts in 38-year-old non-lactating female, presenting with painful lumps in
right breast.
A. Mammogram of right breast reveals several partial circumscribed masses (black arrows), predominantly in upper half of right breast. B.
Ultrasound of right breast reveals cysts with thickened walls and internal echogenic material. C. T1-weighted post contrast fat saturated MR
imaging of breasts reveal presence of several cysts in upper half of right breast with thickened enhancing walls (black arrows). SAG = sagittal,
TRV = transverse
kjronline.org Korean J Radiol 19(1), Jan/Feb 2018 9
Leong et al.
A B
Fig. 7. Post-procedural breast infections.
A. Post nipple-piercing breast abscess. This is immunocompromised 20-year-old female who presented with left breast swelling and pain post
nipple piercing. Ultrasound image of left breast with color Doppler shows hypoechoic collection with heterogeneous content and increased
peripheral vascularity. B. Abscess post mastectomy with insertion of tissue expander. This 62-year-old female experienced pain, redness and
swelling after mastectomy with insertion of tissue expander. Ultrasound image of affected right breast reveals thick walled, lobulated collection
situated posterior to tissue expander (white arrow). Aspiration of this lesion yielded inflammatory cells. No sign of malignant cells was observed.
A B C
Fig. 8. Tuberculosis mastitis in 33-year-old female with chronic discharging sinuses in left breast.
A. Mammogram of left breast demonstrates partially circumscribed masses in left breast (white arrows). B. Ultrasound of left breast reveals
collections (black arrow) with fistulous tracts to skin surface (white arrow). C. T1-weighted fat saturated MR imaging of left breast in sagittal
plane shows rim-enhancing collections (black arrow) with fistulous tracts to skin surface (white arrow). US-guided biopsy of these lesions
revealed presence of acid-fast bacilli, in keeping with diagnosis of tuberculous mastitis. Chest radiograph was also conducted for this patient.
However it did not reveal any sign of infection.
10 Korean J Radiol 19(1), Jan/Feb 2018 kjronline.org
Inflammatory Breast Disorders: A Pictorial Essay
Infected Skin Lesions echogenicity, reflecting varying internal contents (Fig. 9).
Skin lesions such as epidermal inclusion cysts or There may be presence of a tract extending to the skin
sebaceous cysts can be infected. Radiological investigations surface (13). Inflammatory changes may extend into the
reveal dermal lesion, often well circumscribed with mixed surrounding subcutaneous tissue or even into the breast
parenchyma (1).
Non-Infectious Mastitis
Idiopathic Granulomatous Mastitis
This is a rare form of mastitis that usually occurs in
young women within a few years following childbirth (1,
3). Its clinical and radiological presentation mimics breast
malignancy (7). It may present with a palpable lump, or
a more diffuse involvement of the breast (Fig. 10). This is
usually accompanied with lymphadenopathy. In some cases,
aseptic abscesses can develop, that may form sinus tracts
with the overlying skin. Diagnosis is usually confirmed on
histology, which demonstrates well-formed non-caseating
granulomata with epithelioid macrophages and Langhans-
type multinucleated giant cells (1, 3, 9).
Fig. 9. Infected sebaceous cyst in 59-year-old female with
painful left breast lump. Ultrasound of left breast with color Xanthogranulomatous Mastitis
Doppler reveals hypoechoic lesion within dermis with surrounding Xanthogranulomas are usually well-circumscribed
increased vascularity (white arrow). No deep extension of this lesion
is observed. Surrounding skin is thickened. cutaneous nodules or indurated plaques that occur
A B
Fig. 10. Chronic granulomatous mastitis in 40-year-old female with long standing right breast pain and swelling.
A. Mammogram of breasts in mediolateral oblique projection shows ill-defined mass in upper half of right breast (white arrow). There is also
enlarged right axillary node (black arrow). B. Ultrasound examination reveals lobulated heterogeneously hypoechoic lesion in upper half of right
breast. This lesion has imaging features that are suspicious for malignancy and ultrasound guided biopsy was conducted. Histological diagnosis
of chronic granulomatous mastitis was made.
kjronline.org Korean J Radiol 19(1), Jan/Feb 2018 11
Leong et al.
elsewhere in the body, with predilection for the periorbital periductal mastitis, is a benign inflammatory disease of
area. Extra-cutaneous involvement is rare; involvement of the breast that may present with nipple discharge and
the breast is even more uncommon. Imaging findings in the nipple retraction, which mimics malignancy. On ultrasound,
breast are variable (Fig. 11). These lesions are characterized dilated ducts are noted with echogenic material within
on histology by the presence of multi-nucleated giant cells, (debris) and surrounding increased vascularity (Fig. 12A).
lipid-laden macrophages (also called xanthoma cells or On mammography, inspissated calcified intra-ductal content
foamy histiocytes) and cholesterol crystals (12, 14). will show up as large rod-like branching calcifications
radiating from the nipple (3, 9) (Fig. 12B).
Plasma Cell Mastitis
Plasma cell mastitis, also known as duct ectasia or Diabetic Mastopathy
Diabetic mastopathy is another condition that is
frequently mistaken for carcinoma due to its often
indistinguishable radiological presentation (3, 9). It usually
occurs in patients with longstanding insulin dependent
diabetes. Patients usually present with large, painless, hard
breast masses. Multifocal or bilateral breast involvement is
not uncommon (7). On mammogram, ill-defined masses or
asymmetrical densities can be seen. On ultrasound, diabetic
mastopathy often manifest as ill-defined hypoechoic lesions
with significant posterior acoustic shadowing (12) (Fig.
13). Diagnosis is usually confirmed on histology (3).
Malignant Mastitis
Inflammatory Breast Cancer
Fig. 11. Xanthogranulomatous mastitis in 41-year old female
34 weeks pregnant with pain in upper inner quadrant of
Inflammatory breast cancer is an invasive aggressive
left breast. Hypoechoic well-circumscribed lesion was seen in disease with high rate of metastasis at diagnosis (1).
2:00 position of left breast with surrounding and internal increased Clinical symptoms include palpable tumor, skin erythema,
vascularity. This was thought to be likely related to lactational
changes. However, due to presence of increased vascularity, this lesion edema and warmth, breast enlargement and nipple
was biopsied and histology revealed xanthogranulomatous mastitis. retraction. Some patients may present with breast pain.
A B
Fig. 12. Plasma cell mastitis.
A. Plasma cell mastitis in non-lactating 34-year-old female with pain and swelling in lower half of left breast and nipple discharge. Ultrasound
images of left breast in transverse (image on left) and longitudinal views (image on right) reveal markedly dilated intramammary duct in
retroareolar region with echogenic content and surrounding increased vascularity. Ultrasound-guided biopsy of this duct was conducted to rule
out malignancy, which only yielded inflammatory cells. B. Plasma cell mastitis in asymptomatic 71-year-old female at screening mammogram.
Mammogram of both breasts in mediolateral oblique view shows characteristic large rod-like branching calcifications in both breasts.
12 Korean J Radiol 19(1), Jan/Feb 2018 kjronline.org
Inflammatory Breast Disorders: A Pictorial Essay
Mammographic findings include skin thickening, increased may exhibit similar morphological features such as skin
breast density and trabeculation (15). On ultrasound, thickening, edema and presence of mass lesions or non-
subareolar mastitis tends to show mixed solid-cystic lesions mass like enhancement. Their differences, however, lie in
or collections. However, inflammatory breast cancers are their enhancement characteristics. Masses in inflammatory
more likely to show solid mass lesions. On MR imaging, breast cancer tend to display greater initial enhancement
both inflammatory breast cancers and benign mastitis and more frequent subsequent washout. Lesions in benign
mastitis tend to show a more persistent or plateaued
enhancement pattern. Lesions in benign mastitis also
tend to occur in a subareolar location, whereas malignant
lesions tend to occur either centrally or dorsally within the
breast tissue (2). Any non-lactating patient with mastitis
that does not respond to antibiotic therapy should undergo
biopsy to exclude presence of malignancy (3, 15) (Fig. 14).
CONCLUSION
Inflammatory breast diseases consist of a wide array
of conditions ranging from the benign simple infective
mastitis to breast malignancy. Imaging features of benign
and malignant inflammatory conditions often overlap which
may cause diagnostic confusion and possibly delay proper
treatment. In some cases, correlation with clinical history
and risk factors may be useful. For example, in a case of
a lactating female, with signs of inflammation, benign
mastitis is the most probable diagnosis and treatment can
Fig. 13. Diabetic mastopathy in 29-year-old female with Type be initiated with follow-up imaging to look for resolution.
I diabetes, presenting with palpable lumps in upper outer Complications of breast infection, such as abscess formation
quadrants of both breasts. Ultrasound of upper half of left breast or fistulas should also be sought after. The radiologist
reveals ill-defined heterogeneously hypoechoic area, with posterior
acoustic shadowing. Similar findings were also observed over right should be familiar with the range of common inflammatory
breast. breast conditions and should also be aware of specific
A B C
Fig. 14. Inflammatory breast carcinoma in 43-year-old, presenting with right breast lump, pain and erythema with yellow nipple
discharge and palpable right axillary lymph nodes.
A. Mammogram of both breasts in mediolateral oblique view demonstrates ill-defined opacity on lower half of right breast (black arrows) with
overlying skin thickening (white arrows). B. Ultrasound of right breast reveals heterogeneously hypoechoic, solid-cystic mass with increased
peripheral vascularity. C. Enlarged right axillary node is observed with loss of normal fatty hilum and thickened cortex. US-guided biopsy was
conducted on right breast mass and axillary node. Histology confirms presence of invasive carcinoma with ductal features.
kjronline.org Korean J Radiol 19(1), Jan/Feb 2018 13
Leong et al.
disease patterns such as Zuska’s disease and diabetic las Heras P, et al. Radiologic evaluation of breast disorders
mastopathy. Mastitis that does not resolve or respond to related to pregnancy and lactation. Radiographics 2007;27
Suppl 1:S101-S124
antibiotic therapy should always be further evaluated with
9. Gunawardena RP, Gunawardena D, Metcalf C, Taylor D, Wylie
biopsy to rule out presence of malignancy.
L. Inflammatory breast disease: a pictorial essay with
radiological-pathological correlation. J Med Imaging Radiat
REFERENCES Oncol 2017;61:70-76
10. Trop I, Dugas A, David J, El Khoury M, Boileau JF, Larouche
1. Lepori D. Inflammatory breast disease: The radiologist’s role. N, et al. Breast abscesses: evidence-based algorithms for
Diagn Interv Imaging 2015;96:1045-1064 diagnosis, management, and follow-up. Radiographics
2. Kasales CJ, Han B, Smith JS Jr, Chetlen AL, Kaneda HJ, 2011;31:1683-1699
Shereef S. Nonpuerperal mastitis and subareolar abscess of 11. Baharoon S. Tuberculosis of the breast. Ann Thorac Med
the breast. Am J Roentgenol 2014;202:W133-W139 2008;3:110-114
3. Kamal RM, Hamed ST, Salem DS. Classification of inflammatory 12. Sabaté JM, Clotet M, Gómez A, De Las Heras P, Torrubia S,
breast disorders and step by step diagnosis. Breast J Salinas T. Radiologic evaluation of uncommon inflammatory
2009;15:367-380 and reactive breast disorders. Radiographics 2005;25:411-424
4. Tan H, Li R, Peng W, Liu H, Gu Y, Shen X. Radiological and 13. Gao Y, Slanetz PJ, Eisenberg RL. Echogenic breast masses at
clinical features of adult non-puerperal mastitis. Br J Radiol US: to biopsy or not to biopsy? Radiographics 2013;33:419-
2013;86:20120657 434
5. Kwak JY, Kim EK, Chung SY, You JK, Oh KK, Lee YH, et al. 14. Koo JS, Jung W. Xanthogranulomatous mastitis:
Unilateral breast edema: spectrum of etiologies and imaging clinicopathology and pathological implications. Pathol Int
appearances. Yonsei Med J 2005;46:1-7 2009;59:234-240
6. Michie C, Lockie F, Lynn W. The challenge of mastitis. Arch Dis 15. Yeh ED, Jacene HA, Bellon JR, Nakhlis F, Birdwell RL,
Child 2003;88:818-821 Georgian-Smith D, et al. What radiologists need to know
7. Kim YR, Kim HS, Kim HW. Are irregular hypoechoic breast about diagnosis and treatment of inflammatory breast cancer:
masses on ultrasound always malignancies?: a pictorial essay. a multidisciplinary approach. Radiographics 2013;33:2003-
Korean J Radiol 2015;16:1266-1275 2017
8. Sabate JM, Clotet M, Torrubia S, Gomez A, Guerrero R, de
14 Korean J Radiol 19(1), Jan/Feb 2018 kjronline.org
Potrebbero piacerti anche
- Salivary Gland Cancer: From Diagnosis to Tailored TreatmentDa EverandSalivary Gland Cancer: From Diagnosis to Tailored TreatmentLisa LicitraNessuna valutazione finora
- Lipoma of The Uterine Corpus Exceptional Eventuality Combined With An Ovarian ThecomaDocumento5 pagineLipoma of The Uterine Corpus Exceptional Eventuality Combined With An Ovarian ThecomaAlex HydronNessuna valutazione finora
- Mastitis 2Documento4 pagineMastitis 2lolytofarisaNessuna valutazione finora
- JURNALDocumento4 pagineJURNALsaosaharaNessuna valutazione finora
- EBT in AbdomenDocumento8 pagineEBT in Abdomengiant nitaNessuna valutazione finora
- Male Tuberculous Mastitis: A Rare Entity Case ReportDocumento3 pagineMale Tuberculous Mastitis: A Rare Entity Case ReportlolytofarisaNessuna valutazione finora
- Primary Tuberculosis of Breast in 22 Year Old Female - A Rare Case ReportDocumento5 paginePrimary Tuberculosis of Breast in 22 Year Old Female - A Rare Case ReportInternational Organization of Scientific Research (IOSR)Nessuna valutazione finora
- Lucivero Et Al 2011 Lupus Mastitis in Systemic Lupus Erythematosus A Rare Condition Requiring A Minimally InvasiveDocumento5 pagineLucivero Et Al 2011 Lupus Mastitis in Systemic Lupus Erythematosus A Rare Condition Requiring A Minimally Invasiveruthdaniel6041Nessuna valutazione finora
- S. A. Robertson., 2014Documento13 pagineS. A. Robertson., 2014ajeng hefdeaNessuna valutazione finora
- Why Diagnosing Inflammatory Breast Cancer Is Hard and How To Overcome The Challenges: A Narrative ReviewDocumento10 pagineWhy Diagnosing Inflammatory Breast Cancer Is Hard and How To Overcome The Challenges: A Narrative ReviewMarc BantilanNessuna valutazione finora
- Benign & Malignant Breast Lesions Presented By: Omar Al. Ma'aita Mais Al - Shboul 6 Year, Surgery Course, J.U.S.TDocumento87 pagineBenign & Malignant Breast Lesions Presented By: Omar Al. Ma'aita Mais Al - Shboul 6 Year, Surgery Course, J.U.S.TRussia Al Shboul100% (1)
- Imaging Features and Diagnosis of Tuberculosis of The BreastDocumento6 pagineImaging Features and Diagnosis of Tuberculosis of The Breastdmaja duluuuNessuna valutazione finora
- Faz Zio 2016Documento9 pagineFaz Zio 2016seruniallisaaslimNessuna valutazione finora
- Fam New 4Documento5 pagineFam New 4novaNessuna valutazione finora
- Inflamasi, Abses PayudaraDocumento7 pagineInflamasi, Abses PayudaraIntan PermataNessuna valutazione finora
- Breast PathologyDocumento80 pagineBreast Pathologysymonlangisi354Nessuna valutazione finora
- Mastitis IgmDocumento12 pagineMastitis IgmMariajanNessuna valutazione finora
- Case Report EndometriosisDocumento4 pagineCase Report EndometriosischristinejoanNessuna valutazione finora
- Kamal 2009Documento14 pagineKamal 2009seruniallisaaslimNessuna valutazione finora
- Best-Practice Care Pathway For Improving Management of Mastitis and Breast AbscessDocumento8 pagineBest-Practice Care Pathway For Improving Management of Mastitis and Breast AbscessEgy SeptiansyahNessuna valutazione finora
- Case Report PathoDocumento3 pagineCase Report PathoZak KazNessuna valutazione finora
- Leiomyosarcoma of The Uterus: A Report of 3 Cases and A Discussion of Its Unusual Clinicopathological AssociationsDocumento11 pagineLeiomyosarcoma of The Uterus: A Report of 3 Cases and A Discussion of Its Unusual Clinicopathological AssociationsFlorina PaulaNessuna valutazione finora
- 245209-Article Text-588493-1-10-20230405Documento7 pagine245209-Article Text-588493-1-10-20230405Reza adi kurniawanNessuna valutazione finora
- Enfermedad de PayetDocumento10 pagineEnfermedad de PayetGabriela Zavaleta CamachoNessuna valutazione finora
- SGL1 - Breast ImagingDocumento93 pagineSGL1 - Breast ImagingDarawan MirzaNessuna valutazione finora
- ABM Protocol #36 PDFDocumento17 pagineABM Protocol #36 PDFRana HassanNessuna valutazione finora
- Jurnal Radiologi 3Documento10 pagineJurnal Radiologi 3Yuni AurraNessuna valutazione finora
- Infections in The Breast - Common Imaging Presentations and MimicsDocumento7 pagineInfections in The Breast - Common Imaging Presentations and MimicsAridayana HalideNessuna valutazione finora
- Treatment of Bbreast InfectionDocumento12 pagineTreatment of Bbreast InfectionThắng NguyễnNessuna valutazione finora
- Accessory Breasts: When To Excise?: The Breast Journal March 2005Documento4 pagineAccessory Breasts: When To Excise?: The Breast Journal March 2005Mirachel AugustNessuna valutazione finora
- Kurtz 2016Documento5 pagineKurtz 2016Stevano PattiasinaNessuna valutazione finora
- Breast Cancer CasebookDocumento15 pagineBreast Cancer CasebookMechelle Bajamunde PenasoNessuna valutazione finora
- Kataria 2012Documento6 pagineKataria 2012jjeongjjangNessuna valutazione finora
- Abdominal Inflammatory Myofibroblastic Tumor: Report On Four Cases and Review of LiteratureDocumento6 pagineAbdominal Inflammatory Myofibroblastic Tumor: Report On Four Cases and Review of LiteratureLisma EkayantiNessuna valutazione finora
- Lymphedema in Survivors of Breast CancerDocumento12 pagineLymphedema in Survivors of Breast CancerAllyson DinizNessuna valutazione finora
- Tabark Radhi - Benign Breast NeoplasmDocumento19 pagineTabark Radhi - Benign Breast NeoplasmAhmed AliNessuna valutazione finora
- Classification and Diagnosis of Endometrial Hyperplasia - UpToDateDocumento24 pagineClassification and Diagnosis of Endometrial Hyperplasia - UpToDatenoor hyNessuna valutazione finora
- Incidental Finding of Uterine Adenomyosis in A Bitch With Reproductive Disorders: A Case ReportDocumento5 pagineIncidental Finding of Uterine Adenomyosis in A Bitch With Reproductive Disorders: A Case ReportAgustina Anggraeni PurnomoNessuna valutazione finora
- Granulomatous Mastitis - A Case ReportDocumento3 pagineGranulomatous Mastitis - A Case ReportqalbiNessuna valutazione finora
- Mandai2012 Article ClinicalManagementOfOvarianEndDocumento17 pagineMandai2012 Article ClinicalManagementOfOvarianEndharyo wiryantoNessuna valutazione finora
- Introduction To Breast DiseasesDocumento10 pagineIntroduction To Breast DiseasessintayehuNessuna valutazione finora
- 12283-Article Text-26421-1-10-20061102Documento2 pagine12283-Article Text-26421-1-10-20061102zacNessuna valutazione finora
- Rosen's Breast Pathology 2 Abnormalies of M Growth and DevelopementDocumento9 pagineRosen's Breast Pathology 2 Abnormalies of M Growth and DevelopementyoussNessuna valutazione finora
- Sinha 2018Documento6 pagineSinha 2018Frank MacíasNessuna valutazione finora
- Gynaecomastia FinalizedDocumento18 pagineGynaecomastia FinalizedAdamNessuna valutazione finora
- Diagnosis in Oncology: UnusualaspectsofbreastcancerDocumento5 pagineDiagnosis in Oncology: UnusualaspectsofbreastcancerLìzeth RamìrezNessuna valutazione finora
- Bmjopen 2021 July 11 7 Inline Supplementary Material 2Documento11 pagineBmjopen 2021 July 11 7 Inline Supplementary Material 2فاطمة الزهراء أسامةNessuna valutazione finora
- A Case of Giant Uterine Fibroid in A Toung WomanDocumento5 pagineA Case of Giant Uterine Fibroid in A Toung WomanTETINOUNessuna valutazione finora
- Manejo Miomas 2021Documento16 pagineManejo Miomas 2021Laura Daniela MurilloNessuna valutazione finora
- Dec24 16 PDFDocumento8 pagineDec24 16 PDFijasrjournalNessuna valutazione finora
- Management Fam 1998Documento5 pagineManagement Fam 1998Envhy WinaNessuna valutazione finora
- MastectomyDocumento11 pagineMastectomyTomi AtmadirjaNessuna valutazione finora
- Breast Implant Associated Anaplastic Large Cell Lymphoma A Case ReportDocumento8 pagineBreast Implant Associated Anaplastic Large Cell Lymphoma A Case ReportAthenaeum Scientific PublishersNessuna valutazione finora
- 43 Ijss Apr Oa43 - 2019Documento5 pagine43 Ijss Apr Oa43 - 2019Evelyn ChacónNessuna valutazione finora
- ANDI DR Louis Jordaan - 2Documento9 pagineANDI DR Louis Jordaan - 2aprooolNessuna valutazione finora
- Pathopysiology of AdenomyosisDocumento11 paginePathopysiology of AdenomyosisVenansius Ratno KurniawanNessuna valutazione finora
- Keywords: Endometrial Polyp, Endometrioma, Ovarian Cyst, Ovarian Dermoid, PelvicDocumento13 pagineKeywords: Endometrial Polyp, Endometrioma, Ovarian Cyst, Ovarian Dermoid, PelvicWarrodNessuna valutazione finora
- Breast and Lung CancerDocumento141 pagineBreast and Lung CancerabdurehmanNessuna valutazione finora
- Skon Cancer Zoe AppalaDocumento15 pagineSkon Cancer Zoe AppalabagasNessuna valutazione finora
- MM in PregnancyDocumento8 pagineMM in PregnancyIrma YasminNessuna valutazione finora
- Lip Balm Nivea - Google SearchDocumento1 paginaLip Balm Nivea - Google SearchseruniallisaaslimNessuna valutazione finora
- Hasselblad X1D-50c - DxOMarkDocumento8 pagineHasselblad X1D-50c - DxOMarkseruniallisaaslimNessuna valutazione finora
- Calories Needed For A 26 Year Old, 73 KG FemaleDocumento1 paginaCalories Needed For A 26 Year Old, 73 KG FemaleseruniallisaaslimNessuna valutazione finora
- Calories Needed For A 26 Year Old, 95 KG MaleDocumento1 paginaCalories Needed For A 26 Year Old, 95 KG MaleseruniallisaaslimNessuna valutazione finora
- Bridestorycom - Online Wedding MarketplaceDocumento4 pagineBridestorycom - Online Wedding MarketplaceseruniallisaaslimNessuna valutazione finora
- Hygiene: Industrial Hygienist Dental Hygienist Hygiene, ColoradoDocumento40 pagineHygiene: Industrial Hygienist Dental Hygienist Hygiene, ColoradoseruniallisaaslimNessuna valutazione finora
- Calories Needed For A 26 Year Old, 73 KG FemaleDocumento1 paginaCalories Needed For A 26 Year Old, 73 KG FemaleseruniallisaaslimNessuna valutazione finora
- Ubs Gold Bars - Google SearchDocumento1 paginaUbs Gold Bars - Google SearchseruniallisaaslimNessuna valutazione finora
- New Doc 2019-04-29 21.27.27 - 20190429212901Documento1 paginaNew Doc 2019-04-29 21.27.27 - 20190429212901seruniallisaaslimNessuna valutazione finora
- Jurnal DM PDFDocumento5 pagineJurnal DM PDFseruniallisaaslimNessuna valutazione finora
- Mark Twain QuotesDocumento1 paginaMark Twain QuotesBen ChongNessuna valutazione finora
- Mark Twain QuotesDocumento1 paginaMark Twain QuotesBen ChongNessuna valutazione finora
- Jurnal TB PDFDocumento4 pagineJurnal TB PDFseruniallisaaslimNessuna valutazione finora
- Jurnal Ge 4 PDFDocumento3 pagineJurnal Ge 4 PDFseruniallisaaslimNessuna valutazione finora
- Jurnal HTDocumento8 pagineJurnal HTseruniallisaaslimNessuna valutazione finora
- Jurnal Ge 5Documento6 pagineJurnal Ge 5seruniallisaaslimNessuna valutazione finora
- Jurnal TBDocumento4 pagineJurnal TBseruniallisaaslimNessuna valutazione finora
- Jurnal TB 3Documento6 pagineJurnal TB 3seruniallisaaslimNessuna valutazione finora
- Jurnal TB 2Documento7 pagineJurnal TB 2seruniallisaaslimNessuna valutazione finora
- Jurnal HT 2Documento16 pagineJurnal HT 2seruniallisaaslimNessuna valutazione finora
- Jurnal GeDocumento4 pagineJurnal GeseruniallisaaslimNessuna valutazione finora
- Jurnal Ge 5Documento6 pagineJurnal Ge 5seruniallisaaslimNessuna valutazione finora
- Jurnal Ge 4Documento3 pagineJurnal Ge 4seruniallisaaslimNessuna valutazione finora
- Jurnal DMDocumento5 pagineJurnal DMseruniallisaaslimNessuna valutazione finora
- 3 Abses SerebelumDocumento3 pagine3 Abses SerebelumseruniallisaaslimNessuna valutazione finora
- Jurnal Ge 2Documento6 pagineJurnal Ge 2seruniallisaaslimNessuna valutazione finora
- 4 Abses SerebelumDocumento17 pagine4 Abses SerebelumseruniallisaaslimNessuna valutazione finora
- 5 Abses SerebelumDocumento3 pagine5 Abses SerebelumseruniallisaaslimNessuna valutazione finora
- 1a Abses SerebelumDocumento18 pagine1a Abses SerebelumseruniallisaaslimNessuna valutazione finora
- 1 Abses SerebelumDocumento6 pagine1 Abses SerebelumseruniallisaaslimNessuna valutazione finora
- Foundation of Health Care and ServicesDocumento21 pagineFoundation of Health Care and ServicesAnnieska Maceda AldeNessuna valutazione finora
- The Vodka Diet Edit 12.20Documento114 pagineThe Vodka Diet Edit 12.20Late Knight GamingNessuna valutazione finora
- Janu Basti Treatment in AyurvedaDocumento17 pagineJanu Basti Treatment in AyurvedaAP AyurvedaNessuna valutazione finora
- Case Studies Vol 1Documento179 pagineCase Studies Vol 1Kushal Dishnu100% (3)
- Colonoscopy For DummiesDocumento79 pagineColonoscopy For Dummiesmike.krawulski9224100% (3)
- Breast Cancer Facts: What You Need To KnowDocumento2 pagineBreast Cancer Facts: What You Need To KnowDrashua AshuaNessuna valutazione finora
- Study Checklist For Passing NCLEX-RN - AllnursesDocumento2 pagineStudy Checklist For Passing NCLEX-RN - AllnursesbeingfiredNessuna valutazione finora
- Biology Ch. 9Documento55 pagineBiology Ch. 9ddNessuna valutazione finora
- Magsaysay Maritime Corporation vs. National Labor Relations Commission (Second Division), 616 SCRA 362 (2010Documento27 pagineMagsaysay Maritime Corporation vs. National Labor Relations Commission (Second Division), 616 SCRA 362 (2010Mei SuNessuna valutazione finora
- Poet Report: KRAS Testing For Colorectal CancerDocumento9 paginePoet Report: KRAS Testing For Colorectal CancerJohn KentNessuna valutazione finora
- Case PresentationDocumento31 pagineCase PresentationYogaPratayogaMNessuna valutazione finora
- Dresslier Supporting The Leukaemia FoundationDocumento1 paginaDresslier Supporting The Leukaemia FoundationDavroeNessuna valutazione finora
- WHO - Toolkit For Delivering The 5a's and 5R's Brief Tobacco InterventionsDocumento17 pagineWHO - Toolkit For Delivering The 5a's and 5R's Brief Tobacco InterventionsTawangNessuna valutazione finora
- Rough Draft Coffee ConsumptionDocumento5 pagineRough Draft Coffee ConsumptionMariana Cedeño RamosNessuna valutazione finora
- Immunity and Vaccines As Biology Answers AQA OCR EdexcelDocumento3 pagineImmunity and Vaccines As Biology Answers AQA OCR EdexcelShela HuangNessuna valutazione finora
- Frequencies - ListDocumento171 pagineFrequencies - Listparamatman111199100% (3)
- Cap 16 Schwatz - Pyoderma Gangrenosum (PG) : SummaryDocumento2 pagineCap 16 Schwatz - Pyoderma Gangrenosum (PG) : SummaryLuca VaccaroNessuna valutazione finora
- Agenda - Biblioteka de Biomarkeri - FINALDocumento1 paginaAgenda - Biblioteka de Biomarkeri - FINALOlteanu Gheorghe-EmilianNessuna valutazione finora
- Toxicology: CH153 Q3 AY2021Documento11 pagineToxicology: CH153 Q3 AY2021Astra BeckettNessuna valutazione finora
- MSDS FluorouracilDocumento3 pagineMSDS FluorouracilRita NascimentoNessuna valutazione finora
- Cancer 2Documento3 pagineCancer 2Charissa Magistrado De LeonNessuna valutazione finora
- Real World Data Applications and Relevance To CA 2023 Seminars in RadiationDocumento12 pagineReal World Data Applications and Relevance To CA 2023 Seminars in RadiationFlavio GuimaraesNessuna valutazione finora
- 2019 Book PrincipleOfNursingInOncologyDocumento454 pagine2019 Book PrincipleOfNursingInOncologyMarNessuna valutazione finora
- Hong Kong Ophthalmological Symposium 2015 Abstract BookDocumento44 pagineHong Kong Ophthalmological Symposium 2015 Abstract BookFaculty.Nessuna valutazione finora
- Final Case Study-Bili (ReVISED)Documento35 pagineFinal Case Study-Bili (ReVISED)malentot100% (1)
- Clinical Presentation, Histopathology, Diagnostic Evaluation, and Staging of Soft Tissue Sarcoma - UpToDateDocumento36 pagineClinical Presentation, Histopathology, Diagnostic Evaluation, and Staging of Soft Tissue Sarcoma - UpToDateKevin AdrianNessuna valutazione finora
- 3011 Pittsburgh Pulverized Coal - 1213Documento3 pagine3011 Pittsburgh Pulverized Coal - 1213abdullah amanullah100% (1)
- Young Fatal Case of Familial Hypercholesterolemia: A Case ReportDocumento2 pagineYoung Fatal Case of Familial Hypercholesterolemia: A Case ReportPeertechz Publications Inc.Nessuna valutazione finora
- NCCC - Melanoma Assessment and Management of Melanoma, 2015Documento886 pagineNCCC - Melanoma Assessment and Management of Melanoma, 2015Anca-Raluca PascuNessuna valutazione finora
- Umbrella SIOPDocumento9 pagineUmbrella SIOPmairaperrenNessuna valutazione finora
- The Obesity Code: Unlocking the Secrets of Weight LossDa EverandThe Obesity Code: Unlocking the Secrets of Weight LossValutazione: 4 su 5 stelle4/5 (6)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDa EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityValutazione: 4 su 5 stelle4/5 (28)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsDa EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNessuna valutazione finora
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDa EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeValutazione: 2 su 5 stelle2/5 (1)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDa EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDValutazione: 5 su 5 stelle5/5 (2)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDa EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionValutazione: 4 su 5 stelle4/5 (404)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDa EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsValutazione: 5 su 5 stelle5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDa EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisValutazione: 4.5 su 5 stelle4.5/5 (42)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDa EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedValutazione: 5 su 5 stelle5/5 (81)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDa EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsValutazione: 3.5 su 5 stelle3.5/5 (3)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisDa EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisValutazione: 4 su 5 stelle4/5 (1)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDa EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityValutazione: 4 su 5 stelle4/5 (3)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDa EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaValutazione: 4.5 su 5 stelle4.5/5 (266)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningDa EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningValutazione: 4 su 5 stelle4/5 (3)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Da EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Nessuna valutazione finora
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisDa EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisValutazione: 3.5 su 5 stelle3.5/5 (2)
- Gut: the new and revised Sunday Times bestsellerDa EverandGut: the new and revised Sunday Times bestsellerValutazione: 4 su 5 stelle4/5 (392)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryDa EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryValutazione: 4 su 5 stelle4/5 (44)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Da EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Valutazione: 4.5 su 5 stelle4.5/5 (110)
- The Marshmallow Test: Mastering Self-ControlDa EverandThe Marshmallow Test: Mastering Self-ControlValutazione: 4.5 su 5 stelle4.5/5 (58)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessDa EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessValutazione: 4.5 su 5 stelle4.5/5 (328)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingDa EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingValutazione: 4 su 5 stelle4/5 (1138)
- Troubled: A Memoir of Foster Care, Family, and Social ClassDa EverandTroubled: A Memoir of Foster Care, Family, and Social ClassValutazione: 4.5 su 5 stelle4.5/5 (27)