Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
3 DC 3
Caricato da
astutikTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
3 DC 3
Caricato da
astutikCopyright:
Formati disponibili
Feature
Use of Ventilator Bundle
and Staff Education to
Decrease Ventilator-
Associated Pneumonia in
Intensive Care Patients
Maria Parisi, RN, MSc, PhD
Vasiliki Gerovasili, MD, PhD
Stavros Dimopoulos, MD, PhD
Efstathia Kampisiouli, RN, MSc
Christina Goga, MD
Efstathia Perivolioti, MD, PhD
Athina Argyropoulou, MD, PhD
Christina Routsi, MD, PhD
Sotirios Tsiodras, MD, PhD
Serafeim Nanas, MD, PhD
Background Ventilator-associated pneumonia (VAP), one of the most common hospital-acquired infec-
tions, has a high mortality rate.
Objectives To evaluate the incidence of VAP in a multidisciplinary intensive care unit and to examine
the effects of the implementation of ventilator bundles and staff education on its incidence.
Methods A 24-month-long before/after study was conducted, divided into baseline, intervention, and
postintervention periods. VAP incidence and rate, the microbiological profile, duration of mechanical
ventilation, and length of stay in the intensive care unit were recorded and compared between the periods.
Results Of 1097 patients evaluated, 362 met the inclusion criteria. The baseline VAP rate was 21.6 per
1000 ventilator days. During the postintervention period, it decreased to 11.6 per 1000 ventilator days
(P = .01). Length of stay in the intensive care unit decreased from 36 to 27 days (P = .04), and duration of
mechanical ventilation decreased from 26 to 21 days (P = .06).
Conclusions VAP incidence was high in a general intensive care unit in a Greek hospital. However,
implementation of a ventilator bundle and staff education has decreased both VAP incidence and length
of stay in the unit. (Critical Care Nurse. 2016;36[5]:e1-e7)
V
entilator-associated pneumonia (VAP) is one of the most common hospital-acquired infections.
It is a form of nosocomial pneumonia that occurs in patients undergoing mechanical ventilation
for longer than 48 hours.1 Recently reported VAP rates range from 1 to 4 cases per 1000 ventilator
days in industrialized countries and up to 13 cases per 1000 ventilator days in developing countries.2
VAP is the most serious health care–associated infection and is the leading cause of morbidity and
©2016 American Association of Critical-Care Nurses doi: http://dx.doi.org/10.4037/ccn2016520
www.ccnonline.org CriticalCareNurse Vol 36, No. 5, OCTOBER 2016 e1
Downloaded from http://ccn.aacnjournals.org/ by AACN on October 27, 2017
mortality from device-associated infections, especially Among several identified sources for VAP among
in the intensive care unit (ICU).1 Attributable mortality ICU patients, contamination of the ventilator circuit has
rate estimates vary from 10% to 65%,3 with a mean of been recognized. Such contamination can be prevented
about 30%.2 Furthermore, VAP has long been recognized by the institution of appropriate infection control mea-
as a cause of prolonged ICU stays and increased hospital sures including use of a ventilator-specific bundle.18
costs. An increase of 7 to 9 days in ICU stay has been In the present study, we aimed to evaluate the inci-
reported for a patient with VAP,4 and Kollef et al5 reported dence of VAP in a general ICU and hypothesized that
in 2012 that the cost per patient increases by US$40 000 the implementation of a specific VAP prevention bundle
when the patient has VAP. Finally, VAP accounts for 50% together with a staff education strategy would be effective
of antibiotics used in the ICU.6 in reducing the incidence of VAP in critically ill patients.
The Institute for Healthcare Improvement, during its It is the first time that such a hypothesis has been applied
“100 000 Lives Campaign,” designated the prevention in an ICU in Greece, a country with a very high preva-
of VAP as 1 of 6 interventions that would significantly lence of nosocomial multidrug-resistant pathogens.19
contribute to improved patient care and reduction in
avoidable hospital deaths.7 Evidence-based guidelines for Methods
preventing nosocomial pneumonia have been published Setting and Study Design
by the Centers for Disease Control and Prevention for The study took place in a closed, multidisciplinary
more than 30 years8 and have contributed to a reduced ICU with a total capacity of 30 beds. It was staffed with
incidence of VAP.9 Researchers in several studies10-14 have board-certified intensivists and had both a residency and
reported a a fellowship program. The nurse to patient ratio during
VAP: one of the most common hospital reduced VAP the study period was 1 to 3 during the day and up to 1 to
infections, with a high mortality rate. rate with the 4 during the night. A prospective, intervention study
implementa- consisting of 3 phases was conducted: phase 1 was a
tion of the VAP bundle and the use of similar care bun- baseline period (14 months), phase 2 was an interven-
dles. However, some discordance remains regarding tion/education period (40 days), and phase 3 was a
specific bundle components,15,16 and some researchers postintervention period (8.5 months). The total dura-
have argued against the use of VAP bundles.17 tion of the study was 24 months.
For all patients included in the study, several param-
Authors eters were recorded in a specific structured form, includ-
Maria Parisi is a high-dependency unit nurse, Vasiliki Gerovasili is ing personal medical history, demographics, and comorbid
a pulmonologist, Efstathia Kampisiouli is a nursing specialization conditions. The Acute Physiology and Chronic Health
manager and surgical nurse specialist, Christina Goga is a pulmon-
ologist, Christina Routsi is an associate professor of intensive care Evaluation (APACHE) II severity score20 and Simplified
medicine, and Serafeim Nanas is a professor of intensive care medi- Acute Physiology Score (SAPS) III21 were calculated
cine, First Department of Critical Care, National and Kapodistrian
University of Athens, Evangelismos Hospital, Athens, Greece. for all patients on the day of admission. Causes of ICU
admission were classified as respiratory failure, neuro-
Stavros Dimopoulos is an internal medicine-intensive care medi-
cine specialist, John Farman Intensive Care Unit, Addenbrookes logical disease, cardiovascular disease, neurotrauma,
Cambridge University Hospital, Cambridge, United Kingdom. multiple injury, sepsis, and gastrointestinal disease.
Efstathia Perivolioti is a consultant and Athina Argyropoulou is a The patients were monitored until ICU discharge (due
consultant and director, Department of Clinical Microbiology, to improvement or death) or up to a maximum of 30 days.
Evangelismos Hospital, Athens, Greece.
Inclusion criteria were intubation up to 12 hours
Sotirios Tsiodras is an associate professor of medicine and infec- before ICU admission or within 48 hours of ICU admis-
tious diseases, University of Athens Medical School, 4th Depart-
ment of Internal Medicine, Attikon University Hospital, Athens, sion. Patients who were excluded were those under 18
Greece. years of age or pregnant, those transferred from another
Corresponding author: Vasiliki Gerovasili, MD, PhD, Evangelismos Hospital, 45-47 hospital’s ICU, those who had been treated in an ICU
Ipsilantou Street, 10676, Athens, Greece (e-mail: a.icusn@gmail.com).
for more than 48 hours during the preceding 90 days,
To purchase electronic or print reprints, contact the American Association of Critical-
Care Nurses, 101 Columbia, Aliso Viejo, CA 92656. Phone, (800) 899-1712 or those with less than 48 hours in the ICU, and those
(949) 362-2050 (ext 532); fax, (949) 362-2049; e-mail, reprints@aacn.org. with a diagnosis of brain death.
e2 CriticalCareNurse Vol 36, No. 5, OCTOBER 2016 www.ccnonline.org
Downloaded from http://ccn.aacnjournals.org/ by AACN on October 27, 2017
The diagnosis of VAP was made by the supervising were recorded by the investigators of the protocol. At the
physician according to the guidelines. Specifically, the same time, checklists were placed in the ICU in order to
presence of a new infiltrate on the chest radiograph and monitor the implementation of the VAP bundle. These
2 of 3 clinical criteria (leukocytosis, purulent secretions, checklists were completed by medical and nursing staff
fever),22 together with tracheobronchial secretions, con- of the ICU and were handed over to the protocol investi-
firmed the occurrence of VAP for the physician. Also, the gators for further processing. Adherence to the 4 elements
Clinical Pulmonary Infection Score23 was calculated, and of the basic VAP bundle was monitored during the base-
a score greater than 6 was used to verify the diagnosis. line and intervention periods. A point for adherence to
The study was approved by the ethics committee of the VAP bundle was given if at least 3 of the 4 elements
Evangelismos Hospital, and written informed consent of the bundle were followed on most cases.
was provided by the patients’ relatives.
Main Outcome
Baseline Period The main surveillance outcomes were VAP density
During the baseline period, systematic recording of (events per 1000 mechanical ventilator days) and ICU
all VAP cases was recorded on structured forms accord- length of stay.
ing to the aforementioned criteria. A database of all cases
was constructed with all pertinent epidemiological and Performance Feedback
clinical and laboratory parameters. The investigators received feedback on their perfor-
mance every 2 weeks during the postintervention period.
Intervention Period Charts showing the rates of compliance with the imple-
Following the baseline period, the research team mentation of the basic VAP bundle were presented to the
focused on the intervention and education. Specifically: ICU doctors and head nurses. Future actions were dis-
• A specialized leaflet was distributed to the staff that cussed in these meetings. Staff members present during
emphasized the frequency of VAP in the ICU and the feedback meetings were responsible for the commu-
the relevant risk factors. Lectures were given to nication of the results to all other interested parties.
the medical staff and the heads of the nursing staff,
focusing on the same topics, by 2 specialized nurses, Microbiology Profile
every 2 weeks for 3 months. The total number of Tracheobronchial and oropharyngeal cultures were
people who attended the sessions was more than 20. obtained at admission, after 48 hours, and after 7 days
• The ICU patients’ data cards were modified to of mechanical ventilation. Tracheobronchial samples for
include the basic VAP prevention bundle (elevation culture were obtained through the endotracheal tube
of the head of the bed, daily “sedation vacations” with aspiration by inserting a sterile catheter connected
and assessment of readiness to extubate, peptic to an aspiration device into the airway. The aspirated
ulcer disease prophylaxis, and deep venous throm- secretion was placed in a sterile container directly through
bosis prophylaxis).24-26 the circuit of the aspiration system. These samples were
• A sodium bicarbonate–based oral hygiene protocol used to determine the main pathogen causing the VAP.
was implemented by using special, single-use tooth-
brushes twice daily for 40 days. Statistical Analysis
• Posters were placed in the ICU outlining the cor- Continuous variables are presented as mean (stan-
rect hand hygiene procedure during the staff ’s con- dard deviation) or median (interquartile range), and
tact with the patients. categorical variables are presented as frequencies and
proportions. All variables were tested for normal distri-
Process Surveillance bution. Group means of continuous variables were
An 8.5-month period followed, where the recording compared by using an independent t test or the Mann-
of VAP cases resumed. In parallel, the implementation Whitney test (for distributions that were not normal),
of infection control measures was monitored, at random and categorical variables were compared by using a
time intervals, at least 3 times per week. Parameters χ2 test. The effectiveness of the intervention (ventilator
www.ccnonline.org CriticalCareNurse Vol 36, No. 5, OCTOBER 2016 e3
Downloaded from http://ccn.aacnjournals.org/ by AACN on October 27, 2017
bundles/staff education strategy) was assessed with a
Cox hazard regression analysis model. The lowest level Total number of
for statistical significance was chosen as P less than .05. patients admitted
to the intensive care
unit (N = 1097)
Results Patients excluded
(n = 735)
During the 2-year study period, a total of 1097
patients were admitted to the ICU and were prospec- Patients enrolled
tively evaluated. Of those patients, 362 met the inclusion (n = 362)
criteria and composed the study cohort (Figure 1). The
mean age of the study population was 56 (SD, 19) years,
Patients with
and 68% of them were male. Table 1 shows the baseline ventilator-associated
characteristics of the patients studied. The age and sex pneumonia (n = 74)
of the participants did not differ significantly from before
to after the intervention. The APACHE II score was higher Figure 1 Summary of patients’ sample.
after the intervention, although the SAPS III did not
differ from before to after the intervention. During the per 1000 ventilator days (P = .01). A decrease in VAP
intervention period, the percentage of patients with neu- incidence from 23.4 to 15.4 per 100 patients was
rological disease was lower. Adherence to the basic VAP recorded. Also, there was a reduction in duration of
bundle improved significantly from 13% to 28% after mechanical ventilation in the postintervention period
the intervention (P = .02). for patients with VAP. However, these last 2 differences
Outcome measures before and after the intervention were not statistically significant (P = .06). The median
period for the patients with VAP are presented in Table number of days of mechanical ventilation before VAP
2. The total number of VAP cases recorded was 74, and appearance was 6 days (interquartile range, 4-15 days)
the VAP density was reduced from 21.6 to 11.6 events before the intervention and 7 days (interquartile range,
Table 1 Baseline characteristics of patients (n = 362) before and after the intervention period
Before intervention After intervention
Patient data (n = 226) (n = 136) P
Age, median (interquartile range), y 59 (41-73) 58 (42-72) .84
Male sex, No. (%) of patients 160 (71) 87 (64) .18
APACHE II score on admission, mean (SD) 15 (7) 17 (6) .04
SAPS III on admission, mean (SD) 58 (16) 59 (14) .67
Mortality, % 35 41 .24
Admitted to ICU from, No. (%) of patients .006
Emergency department 55 (24) 46 (34)
Surgery 94 (42) 32 (24)
Hospital general care area 68 (30) 50 (37)
Other hospital 9 (4) 8 (6)
Cause of ICU admission,a No. (%) of patients
Respiratory failure 53 (23) 32 (24) .10
Neurological disease 49 (22) 47 (35) .007
Cardiovascular disease 28 (12) 8 (6) .05
Neurotrauma 40 (18) 21 (15) .60
Multiple injury 21 (9) 16 (12) .50
Sepsis 15 (7) 4 (3) .13
Gastrointestinal disease 22 (10) 7 (5) .12
Meningitis 2 (1) 2 (1) .60
Peritonitis 5 (2) 2 (1) .60
Abbreviations: APACHE, Acute Physiology and Chronic Health Evaluation; ICU, intensive care unit; SAPS, Simplified Acute Physiology Score.
a
Sum of causes is more than 100% because some patients had more than 1 cause of admission.
e4 CriticalCareNurse Vol 36, No. 5, OCTOBER 2016 www.ccnonline.org
Downloaded from http://ccn.aacnjournals.org/ by AACN on October 27, 2017
Table 2 Outcome measures for the 74 patients with ventilator-associated pneumonia (VAP)
before and after the intervention period
Outcome measures Before intervention After intervention P
No. of VAP cases 53 21
Days of mechanical ventilation, mean (SD) 26 (16) 21 (8) .06
Days of mechanical ventilation before VAP, median (95% CI) 6 (3-11) 7 (4.5-9.5) .40
VAP incidence (per 100 patients), median (95% CI) 23.4 (17.9-29) 15.4 (9.4-21.5) .06
VAP density (events/1000 ventilator days), median (95% CI) 21.6 (16.2-28.3) 11.6 (7.2-17.8) .01
Days in intensive care unit, mean (SD) 36 (19) 27 (14) .04
Mortality, % 34 33 .10
6-19 days) after the intervention (P = .40). Finally, the
mean ICU length of stay for VAP patients was 36 days 1.0
(SD, 19 days) before the intervention period, and it
Proportion of patients without VAP
decreased to 27 days (SD, 14 days) after the interven- 0.9
tion (P = .04).
Figure 2 shows the time in days until VAP before and 0.8
after the intervention period. The microorganism profile
0.7
of the VAP cases is presented in Table 3, based on the
analysis of sputum samples taken from the patients.
0.6
The microbiological profile did not differ before and
after the intervention period. 0.5
Discussion 0.4
We undertook for the first time in our hospital a 0 5 10 15 20 25
prospective protocol for intervention, education, and Days of mechanical ventilation
surveillance on VAP. We have demonstrated a reduction Intervention
in VAP density from 21.6 events to 11.6 events per 1000 Before After
ventilator days.
Two more positive outcomes of the present study Figure 2 Distribution of days of mechanical ventilation
until ventilator-associated pneumonia (VAP) before and
were the statistically significant decrease (P = .04) in after intervention.
the mean ICU length of stay from 36 to 27 days and
the tendency for a reduction in the mean duration of
mechanical ventilation from 26 to 21 days. These 2
Table 3 Microorganism profile of ventilator-associated
parameters are important both for patients and finan- pneumonia in the participating intensive care units by
cially because both are associated with an increased number of isolated pathogens
number of complications and higher mortality rates. No. of isolated
On the other hand, a considerable cost is associated Isolated microorganisms pathogens
with extended ICU stay and the development of VAP. Acinetobacter baumanii 40
The implementation of a VAP-specific bundle can also Pseudomonas aeruginosa 7
contribute to an overall decrease in patients’ costs. Staphylococcus aureus 10
Researchers have estimated that the mean extra cost Klebsiella pneumoniae 16
for a hospital-acquired infection was between US$2255 Candida albicans 24
and US$5000, making it a very important financial Escherichia coli 1
factor. 27,28 As with other studies,29 no difference in Total 98
mortality was apparent after the intervention.
www.ccnonline.org CriticalCareNurse Vol 36, No. 5, OCTOBER 2016 e5
Downloaded from http://ccn.aacnjournals.org/ by AACN on October 27, 2017
In order to induce pneumonia, the potentially patho- indicate that this measure is effective, so we suggest that
genic microorganisms must reach the lower part of the it be performed on a regular basis.
respiratory system. The most probable cause of such A relatively small chance of a Hawthorne effect is also
infection is aspiration from the oral cavity.30 Hospital- possible, as the study was unblinded. However, the staff
ized patients have high concentrations of oropharyngeal was informed of the study during the observation period
and tracheobroncheal colonization from gram-negative as well as during the intervention period, thus minimiz-
bacilli.30 Subglottic concentrations of these secretions, ing the probability of a Hawthorne effect.
together with leakage around the cuff, are the principal
entrance points for pathogens.31 Another source of Conclusion
infection is colonization of gastric tubes and transfer The positive results from the VAP bundle implemen-
of microbes through microaspiration.30 tation in our institution led to the continuation of this
In the light of these considerations, it is not surpris- strategy in our unit. The bundle strategy was relatively
ing that the most important risk factor for VAP that has easy to implement and did not require the purchase of
emerged in several studies is intubation itself.32 Mechan- expensive technologies. Several improvements are con-
ical ventilation increases the risk of pneumonia 6 to 21 sidered for the near future such as the addition of even
times.32 Risk factors for the occurrence of VAP are multi- more prevention measures in the basic VAP bundle that
ple and variable, including prolonged intubation, enteral have been shown to be effective.42-44 CCN
feeding, supine Financial Disclosures
Implementation of a ventilator bundle position, low None reported.
and a staff education protocol was endotracheal
successful. tube pressure, Now that you’ve read the article, create or contribute to an online discussion about
ventilator cir- this topic using eLetters. Just visit www.ccnonline.org and select the article you want
to comment on. In the full-text or PDF view of the article, click “Responses” in the
cuit contamination, male sex, age more than 60 years, middle column and then “Submit a response.”
tracheostomy, neurosurgery, acute respiratory distress
syndrome, multiorgan failure, coma, and reintubation.33
Regular monitoring for the appropriate implementa- References
1. Augustyn B. Ventilator-associated pneumonia: risk factors and preven-
tion of a bundle is necessary. This requires continuous tion. Crit Care Nurse. 2007;27(4):31-40.
2. Tao L, Hu B, Rosenthal VD, et al. Impact of a multidimensional
education for the participating medical and nursing staff approach on ventilator – associated pneumonia rates in a hospital of
and a dedicated person from the infection control team Shanghai: findings on the international nosocomial infection control
consortium. J Crit Care. 2012;27:440-446.
who would be available for the monitoring of compli- 3. Tejerina E, Frutos-Vivar F, Restrepo MI, et al. Incidence, risk factors, and
outcome of ventilator- associated pneumonia. J Crit Care. 2006;21:56-65.
ance. Such monitoring would raise the staff ’s awareness 4. Papadimos TJ, Hensley SJ, Duggan JM, et al. Implementation of the
and would increase their VAP prevention performance.34,35 “FASTHUG” concept decreases the incidence of ventilator – associated
pneumonia in a surgical intensive care unit. Patient Saf Surg. 2008;2(3):1-6.
On the epidemiology level, we found a strong preva- 5. Kollef MH, Hamilton CW, Ernst FR. Economic impact of ventilator-as-
sociated pneumonia in a large matched cohort. Infect Control Hosp
lence of Acinetobacter baumanii. It is stated in literature Epidemiol. 2012;33(3):250-256.
that there is no significant difference in prognosis, 6. Klompas M. Prevention of ventilator associated pneumonia. Expert Rev
Anti Infect Ther. 2010;8(7):791-800.
mortality, and eradication of VAP caused by Acinetobacter 7. Institute for Healthcare Improvement website. http://www.ihi.org
/Engage/Initiatives/Completed/5MillionLivesCampaign/Documents
species compared with VAP caused by other pathogens.36 /Overview%20of%20the%20100K%20Campaign.pdf. Accessed August
However, Acinetobacter infection is associated with pro- 12, 2014.
8. Simmons BP, Wong ES. Guideline for prevention of nosocomial pneu-
longed ventilation, sedation, and nasogastric intubation37 monia. Am J Infect Control. 1983;11:230-244.
9. National Nosocomial Infections Surveillance System. National nosoco-
and with hemodynamic impairment, which is a predic- mial infections surveillance (NNIS) system report, data summary from
tive of poor outcome.38 January 1992 through June 2004, issued October 2004. Am J Infect Con-
trol. 2004;32:470-485.
10. Resar R, Pronovost P, Haraden C, Simmonds T, Rainey T, Nolan T. Using
Limitations a bundle approach to improve ventilator care processes and reduce ven-
tilator associated pneumonia. Jt Comm J Qual Patient Saf. 2005;31:243-248.
Contrary to the other components that were imple- 11. Al-Tawfiq JA, Abed MS. Decreasing ventilator-associated pneumonia in
adult intensive care units using the Institute for healthcare improvement
mented during the entire period of the study, the oral bundle. Am J Infect Control. 2010;38:552-556.
hygiene protocol was applied for a limited number of 12. Marra AR, Cal RG, Silva CV, et al. Successful prevention of ventilator-
associated pneumonia in an intensive care setting. Am J Infect Control.
days because of financial constraints. Numerous studies39-41 2009;37:619-625.
e6 CriticalCareNurse
Vol 36, No. 5, OCTOBER 2016 www.ccnonline.org
Downloaded from http://ccn.aacnjournals.org/ by AACN on October 27, 2017
13. Bird D, Zambuto A, O’Donnell C, et al. Adherence to ventilator-associated 39. Panchabhai TS, Dangayach NS, Krishnan A, Kothari VM, Karnad DR.
pneumonia bundle and incidence of ventilator-associated pneumonia in Oropharyngeal cleansing with 0.2% chlorhexidine for prevention of noso-
the surgical intensive care unit. Arch Surg. 2010;145:465-470. comial pneumonia in critically ill patients. Chest. 2009;135(5):1150-1156.
14. Cocanour CS, Peninger M, Domonoske BD, et al. Decreasing ventilator- 40. Arroliga AC, Pollard CL, Wilde CD, et al. Reduction in the incidence of
associated pneumonia in a trauma ICU. J Trauma. 2006;61:122-129. ventilator-associated pneumonia: a multidisciplinary approach. Resp Care.
15. Rello J, Lode H, Cornaglia G, Masterton R. A european care bundle for 2012;57(5):688-696.
prevention of ventilator-associated pneumonia. Intensive Care Med. 41. Cutler LR, Sluman P. Reducing ventilator associated pneumonia in adult
2010;36:773-780. patients through high standards of oral care: a historical control study.
16. Tolentino-DelosReyes AF, Ruppert SD, Shiao SY. Evidence-based prac- Intensive Crit Care Nurs. 2014;30:61-68.
tice: use of the ventilator bundle to prevent ventilator-associated pneu- 42. Blot S, Rello J, Vogelaers D. What is new in the prevention of ventilator-
monia. Am J Crit Care. 2007;16:20-27. associated pneumonia? Curr Opin Pulm Med. 2011;17(3):155-159.
17. Halpern NA, Hale KE, Sepkowitz KA, Pastores SM. A world without 43. Benson S, Johnson A, Petera C. VAP free for 1000 days, it can be done.
ventilator associated pneumonia: time to abandon surveillance and Crit Care Nurs Q. 2013;36(4):421-424.
deconstruct the bundle. Crit Care Med. 2012;40:267-270. 44. Lim KP, Kuo SW, Ko WJ, et al. Efficacy of ventilator-associated pneumonia
18. How-to Guide: Prevent Ventilator-Associated Pneumonia. Cambridge, MA: care bundle for prevention of ventilator-associated pneumonia in the sur-
Institute for Healthcare Improvement; 2012. http://www.ihi.org/resources gical intensive care units of a medical center. J Microbiol Immunol Infect.
/Pages/Tools/HowtoGuidePreventVAP.aspx. Accessed July 14, 2016. 2015;48(3):316-321.
19. European Centre for Disease Prevention and Control. Annual Epidemio-
logical Report 2014: Antimicrobial Resistance and Healthcare-Associated
Infections. Stockholm, Sweden: ECDC; 2015.
20. Knaus WA, Draper EA, Wagner DP, Zimmerman JE. APACHE II: a severity
of disease classification system. Crit Care Med. 1985;13:818-829.
21. Moreno RP, Metnitz PGH, Almeida E, et al. SAPS 3 From the evaluation
of the patient to the evaluation of the intensive care unit. Part 2: Devel-
opment of a prognostic model for hospital mortality at ICU admission.
Intensive Care Med. 2005;31:1345-1355.
22. Chastre J, Fagon JY. Ventilator-associated pneumonia. Am J Respir Crit
Care Med. 2002;165:867-903.
23. Pugin J, Auckenthaler R, Mili N, Janssens JP, Lew PD, Suter PM. Diagnosis
of ventilator-associated pneumonia by bacteriologic analysis of bron-
choscopic and nonbronchoscopic “blind” bronchoalveolar lavage fluid.
Am Rev Respir Dis. 1991;143:1121-1129.
24. Youngquist P, Carroll M, Farber M, et al. Implementing a ventilator bundle
in a community hospital. Jt Comm J Qual Patient Saf. 2007;33(4):219-225.
25. Crunden E, Boyce C, Woodman H, Bray B. An evaluation of the impact
of the ventilator care bundle. Nurs Crit Care. 2005;10(5):242-246.
26. Eom JS, Lee MS, Chun HK, et al. The impact of a ventilator bundle on
preventing ventilator- associated pneumonia: a multicenter study. Am J
Infect Control. 2014;42:34-37.
27. Rosenthal VD, Guzman S, Migone O, Safdar N. The attributable cost
and length of hospital stay because of nosocomial pneumonia in intensive
care units in 3 hospitals in Argentina: a prospective, matched analysis.
Am J Infect Control. 2005;33(3):157-161.
28. Sheng WH, Wang JT, Lu DC, Chie WC, Chen YC, Chang SC. Compara-
tive impact of hospital-acquired infections on medical costs, length of
hospital stay and outcome between community hospitals and medical
centres. J Hosp Infect. 2005;59(3):205-214.
29. Roquilly A, Marret E, Abraham E, Asehnoune K. Pneumonia prevention
to decrease mortality in intensive care unit: a systematic review and meta-
analysis. Clin Infect Dis. 2015;60(1):64-75.
30. Tablan OC, Anderson LJ, Besser R, Bridges C, Hajjeh R. CDC Healthcare
infection control practices advisory committee. Guidelines for prevent-
ing healthcare-associated pneumonia, 2003: Recommendations of CDC
and the healthcare infection control practices advisory committee.
MMWR Recomm Rep. 2004;53(RR-3):1-36.
31. Leong JR, Huang DT. Ventilator-associated pneumonia. Surg Clin North
Am. 2006;86:1409-1429.
32. Mathews PJ, Mathews LM. Reducing the risks of ventilator- associated
infections. Dimens Crit Care Nurs. 2000;19:17-21.
33. Maselli D, Restrepo M. Strategies in the prevention of ventilator-associ-
ated pneumonia. Ther Adv Respir Dis. 2011;5(2):131-141.
34. Ban KO. The effectiveness of an evidence-based nursing care program to
reduce ventilator-associated pneumonia in a Korean ICU. Intensive Crit
Care Nurs. 2011;27:226-232.
35. Caserta RA, Marra AR, Durão MS, et al. A program for sustained
improvement in preventing ventilator associated pneumonia in an
intensive care setting. BMC Infect Dis. 2012;12:234.
36. Di Bonito M, Caiazzo S, Iannazzone M, et al. Prognostic differences
between VAP from Acinetobacter baumanii and VAP from other microor-
ganisms. Transl Med UniSa. 2012;30(3):15-21.
37. El-Saed A, Balkhy HH, Al-Dorzi HM, Khan R, Rishu AH, Arabi YM.
Acinetobacter is the most common pathogen associated with late-onset
and recurrent ventilator-associated pneumonia in an adult intensive
care unit in Saudi Arabia. Int J Infect Dis. 2013;17(9):696-701.
38. Chaari A, Mnif B, Bahloul M, et al. Acinetobacter baumannii ventila-
tor-associated pneumonia: epidemiology, clinical characteristics, and
prognosis factors. Int J Infect Dis. 2013;17(12):1225-1228.
www.ccnonline.org CriticalCareNurse Vol 36, No. 5, OCTOBER 2016 e7
Downloaded from http://ccn.aacnjournals.org/ by AACN on October 27, 2017
Use of Ventilator Bundle and Staff Education to Decrease Ventilator-Associated
Pneumonia in Intensive Care Patients
Maria Parisi, Vasiliki Gerovasili, Stavros Dimopoulos, Efstathia Kampisiouli, Christina Goga, Efstathia
Perivolioti, Athina Argyropoulou, Christina Routsi, Sotirios Tsiodras and Serafeim Nanas
Crit Care Nurse 2016;36 e1-e7 10.4037/ccn2016520
©2016 American Association of Critical-Care Nurses
Published online http://ccn.aacnjournals.org/
Personal use only. For copyright permission information:
http://ccn.aacnjournals.org/cgi/external_ref?link_type=PERMISSIONDIRECT
Subscription Information
http://ccn.aacnjournals.org/subscriptions/
Information for authors
http://ccn.aacnjournals.org/misc/ifora.xhtml
Submit a manuscript
http://www.editorialmanager.com/ccn
Email alerts
http://ccn.aacnjournals.org/subscriptions/etoc.xhtml
Critical Care Nurse is an official peer-reviewed journal of the American Association of Critical-Care Nurses (AACN) published
bimonthly by AACN, 101 Columbia, Aliso Viejo, CA 92656. Telephone: (800) 899-1712, (949) 362-2050, ext. 532. Fax: (949)
362-2049. Copyright ©2016 by AACN. All rights reserved.
Downloaded from http://ccn.aacnjournals.org/ by AACN on October 27, 2017
Potrebbero piacerti anche
- JCDR 10 SC06Documento6 pagineJCDR 10 SC06YANNessuna valutazione finora
- البحث السادس PDFDocumento32 pagineالبحث السادس PDFايمان عمرانNessuna valutazione finora
- Impact Vap Bundle 2017Documento6 pagineImpact Vap Bundle 2017Elisya KharuniawatiNessuna valutazione finora
- Original PapersDocumento8 pagineOriginal PapersLuis NovoaNessuna valutazione finora
- Jurnal Kritis ICU Bundle Vap PneumoniaDocumento6 pagineJurnal Kritis ICU Bundle Vap PneumoniaAdzkia PintaNessuna valutazione finora
- Long-Stay of PICU in SepsisDocumento6 pagineLong-Stay of PICU in SepsisSanti IskandarNessuna valutazione finora
- Vivian I 2010Documento11 pagineVivian I 2010Sumana MahankaliNessuna valutazione finora
- Ventilator Associated Pneumonia: Incidence, Profile and Outcome in Pediatric Intensive Care Unit of Tertiary Care CentreDocumento5 pagineVentilator Associated Pneumonia: Incidence, Profile and Outcome in Pediatric Intensive Care Unit of Tertiary Care CentreJoaquín SosaNessuna valutazione finora
- Ventilator-Associated Pneumonia in Adults in Developing Countries: A Systematic ReviewDocumento8 pagineVentilator-Associated Pneumonia in Adults in Developing Countries: A Systematic Reviewfrisca susdiNessuna valutazione finora
- Insiden Dan Risk Faktor VAP 2013Documento5 pagineInsiden Dan Risk Faktor VAP 2013Yudi Jaya CahyanaNessuna valutazione finora
- Ebn RespiDocumento17 pagineEbn RespilablabkurmNessuna valutazione finora
- Vap PDFDocumento17 pagineVap PDFmardianaNessuna valutazione finora
- Choosing Antibiotic Therapy For Severe Community-Acquired PneumoniaDocumento7 pagineChoosing Antibiotic Therapy For Severe Community-Acquired PneumoniaJuan Sebastian SuarezNessuna valutazione finora
- The Egyptian Journal of Critical Care Medicine: Ahmed Abdelrazik Othman, Mohsen Salah AbdelazimDocumento3 pagineThe Egyptian Journal of Critical Care Medicine: Ahmed Abdelrazik Othman, Mohsen Salah AbdelazimAquardoleo ValentinoNessuna valutazione finora
- Neonatal PneumoniaDocumento8 pagineNeonatal PneumoniaAde Gustina SiahaanNessuna valutazione finora
- Clinical Microbiology and InfectionDocumento6 pagineClinical Microbiology and InfectionAccel XtremeNessuna valutazione finora
- The Clinical Impact of Ventilator-Associated Events - Zhu2015Documento8 pagineThe Clinical Impact of Ventilator-Associated Events - Zhu2015Maxi BoniniNessuna valutazione finora
- Sépsis em Pacientes Neurovascular Focus On Infection and Sepsis in Intensive Care PatientsDocumento3 pagineSépsis em Pacientes Neurovascular Focus On Infection and Sepsis in Intensive Care PatientsEdson MarquesNessuna valutazione finora
- MKV 046Documento5 pagineMKV 046ardhenaNessuna valutazione finora
- A Prospective, Randomized Study of Ventilator-Associated Pneumonia in Patients Using A Closed vs. Open Suction SystemDocumento6 pagineA Prospective, Randomized Study of Ventilator-Associated Pneumonia in Patients Using A Closed vs. Open Suction SystemYur Yenova ChavezNessuna valutazione finora
- Research Paper On Ventilator Associated PneumoniaDocumento8 pagineResearch Paper On Ventilator Associated PneumoniakwbfbzundNessuna valutazione finora
- Candidiasis in PICUDocumento6 pagineCandidiasis in PICUMeirinda HidayantiNessuna valutazione finora
- The Clinical Impact and Preventability of Ventilator-Associated Conditions in Critically Ill Patients Who Are Mechanically Ventilated - Muscedere2013Documento8 pagineThe Clinical Impact and Preventability of Ventilator-Associated Conditions in Critically Ill Patients Who Are Mechanically Ventilated - Muscedere2013Maxi BoniniNessuna valutazione finora
- Comparison of Methicillin-Resistant Community-Acquired and Healthcare-Associated PneumoniaDocumento8 pagineComparison of Methicillin-Resistant Community-Acquired and Healthcare-Associated PneumoniaSuarniNessuna valutazione finora
- Antibiotics 10 00608Documento10 pagineAntibiotics 10 00608Marketable StudioNessuna valutazione finora
- International Journal of SurgeryDocumento12 pagineInternational Journal of SurgeryNadya PutriNessuna valutazione finora
- Ventilator-Associated Pneumonia in Paediatric InteDocumento7 pagineVentilator-Associated Pneumonia in Paediatric InteDr tahera noorNessuna valutazione finora
- Klebsiella PDFDocumento4 pagineKlebsiella PDFOscarEduardoNessuna valutazione finora
- The University of Chicago Press The Society For Healthcare Epidemiology of AmericaDocumento11 pagineThe University of Chicago Press The Society For Healthcare Epidemiology of Americaزينب محمد عبدNessuna valutazione finora
- Combes 2007Documento9 pagineCombes 2007RaffaharianggaraNessuna valutazione finora
- 1 s2.0 S0012369221004815 MainDocumento10 pagine1 s2.0 S0012369221004815 Mainkritis ardiansyahNessuna valutazione finora
- 10-Effect of Chest Physical Therapy On Pediatrics Hospitalized With Pneumonia PDFDocumento8 pagine10-Effect of Chest Physical Therapy On Pediatrics Hospitalized With Pneumonia PDFandina100% (1)
- Rapid Training of Healthcare Staff For Protected Cardiopulmonary Resuscitation in The COVID-19 PandemicDocumento3 pagineRapid Training of Healthcare Staff For Protected Cardiopulmonary Resuscitation in The COVID-19 PandemicRicardo BarreraNessuna valutazione finora
- s41598 021 88207 6 PDFDocumento8 pagines41598 021 88207 6 PDFManuel ArenasNessuna valutazione finora
- BJSTR MS Id 006919Documento22 pagineBJSTR MS Id 006919Anz JoyNessuna valutazione finora
- Ventilator Associated Pneumonia in ChildrenDocumento7 pagineVentilator Associated Pneumonia in ChildrendarlingcarvajalduqueNessuna valutazione finora
- Biomedical Journal: SciencedirectDocumento6 pagineBiomedical Journal: SciencedirectFarihah SamarraNessuna valutazione finora
- Incidence and Risk Factors For Ventilator Associated Pneumon 2007 RespiratorDocumento6 pagineIncidence and Risk Factors For Ventilator Associated Pneumon 2007 RespiratorTomasNessuna valutazione finora
- VAP PreventionDocumento8 pagineVAP PreventionstarykNessuna valutazione finora
- Urinary CatheterDocumento22 pagineUrinary Catheterايمان عمرانNessuna valutazione finora
- Changes in Appendicitis Treatment During The COVID-19 PandemicDocumento13 pagineChanges in Appendicitis Treatment During The COVID-19 PandemicCarla GarcíaNessuna valutazione finora
- Triage and Flow Management in Sepsis: Originalresearch Open AccessDocumento8 pagineTriage and Flow Management in Sepsis: Originalresearch Open Accessaktiva25Nessuna valutazione finora
- IndianJMedRes1396814-2632712 071847Documento8 pagineIndianJMedRes1396814-2632712 071847christian hansNessuna valutazione finora
- Recommendations and Guidelines For The Treatment of Pneumonia in TaiwanDocumento28 pagineRecommendations and Guidelines For The Treatment of Pneumonia in TaiwanMaymay DamayNessuna valutazione finora
- The Epidemiology, Antibiotic Resistance and Post-Discharge Course of Peritonsillar Abscesses in London, OntarioDocumento7 pagineThe Epidemiology, Antibiotic Resistance and Post-Discharge Course of Peritonsillar Abscesses in London, OntarioMaharaniNessuna valutazione finora
- Tranilast As An Adjunctive Therapy in Hospitalized Patients With Severe COVID - 19 - A Randomized Controlled TrialDocumento10 pagineTranilast As An Adjunctive Therapy in Hospitalized Patients With Severe COVID - 19 - A Randomized Controlled TrialMax JaksicNessuna valutazione finora
- Intermediate Care Units and Their Role in Medical WardsDocumento2 pagineIntermediate Care Units and Their Role in Medical WardsJHNessuna valutazione finora
- VAP in ICU ReviewDocumento8 pagineVAP in ICU ReviewAdam KurniaNessuna valutazione finora
- Risk Factors of Ventilator-Associated Pneumonia in Critically III PatientsDocumento7 pagineRisk Factors of Ventilator-Associated Pneumonia in Critically III PatientsGladysNessuna valutazione finora
- Risk Factors For Ventilator-Associated Events - Liu 2019Documento6 pagineRisk Factors For Ventilator-Associated Events - Liu 2019Maxi BoniniNessuna valutazione finora
- Outcome of Ventilator-Associated Pneumonia: Impact of Antibiotic Therapy and Other FactorsDocumento6 pagineOutcome of Ventilator-Associated Pneumonia: Impact of Antibiotic Therapy and Other FactorsAnonymous r3ql4y9Nessuna valutazione finora
- Mounier - 2010Documento10 pagineMounier - 2010Cindy KarmilaNessuna valutazione finora
- Lansford 2007Documento6 pagineLansford 2007Danielle Santos RodriguesNessuna valutazione finora
- Clinical Microbiology and Infection: Original ArticleDocumento6 pagineClinical Microbiology and Infection: Original ArticleAkira Masumi100% (1)
- 6887 25815 1 PB PDFDocumento7 pagine6887 25815 1 PB PDFmochkurniawanNessuna valutazione finora
- Ferrer 2008Documento10 pagineFerrer 2008yusNessuna valutazione finora
- Infeccion Nosocomial en UciDocumento7 pagineInfeccion Nosocomial en UciPaul SalazarNessuna valutazione finora
- Ak 2011Documento6 pagineAk 2011bouchra8blsNessuna valutazione finora
- Effect of Procalcitonin-Guided Antibiotic Treatment On Mortality in Acute Respiratory Infections: A Patient Level Meta-AnalysisDocumento36 pagineEffect of Procalcitonin-Guided Antibiotic Treatment On Mortality in Acute Respiratory Infections: A Patient Level Meta-Analysisrista ria ariniNessuna valutazione finora
- Patient-Specific Thresholds of Intracranial Pressure in SevereDocumento8 paginePatient-Specific Thresholds of Intracranial Pressure in SevereastutikNessuna valutazione finora
- The Need For Physiotherapy Intervention For Mandibular Condyle Fracture Patients: A Needs AnalysisDocumento4 pagineThe Need For Physiotherapy Intervention For Mandibular Condyle Fracture Patients: A Needs AnalysisastutikNessuna valutazione finora
- Research ArticleDocumento10 pagineResearch ArticleastutikNessuna valutazione finora
- Us 20130296408Documento65 pagineUs 20130296408astutikNessuna valutazione finora
- HEPATITEDocumento49 pagineHEPATITEAeron TamayoNessuna valutazione finora
- Metal-Earth Imbalance.! Treats ANY Tai Yin Problems & ANY Yang Ming Problems!! Wood-Earth Imbalance. !Documento1 paginaMetal-Earth Imbalance.! Treats ANY Tai Yin Problems & ANY Yang Ming Problems!! Wood-Earth Imbalance. !Diego NicoliniNessuna valutazione finora
- Ineffective Health Management Related To Mrs. Gama: Provide The Client Enough Knowledge About The ProblemDocumento5 pagineIneffective Health Management Related To Mrs. Gama: Provide The Client Enough Knowledge About The ProblemAndrea Albester GarinoNessuna valutazione finora
- CELYN H. NATURAL MAPEH LESSON PLAN (MR - Gepitulan)Documento6 pagineCELYN H. NATURAL MAPEH LESSON PLAN (MR - Gepitulan)Celyn NaturalNessuna valutazione finora
- Microsoft PowerPoint - KNUST-LECT-STUDENT MALARIA (Compatibility Mode)Documento9 pagineMicrosoft PowerPoint - KNUST-LECT-STUDENT MALARIA (Compatibility Mode)AnastasiafynnNessuna valutazione finora
- Negative Effects of Technology On Child Development - Carolina PerezDocumento6 pagineNegative Effects of Technology On Child Development - Carolina PerezCarolina PerezNessuna valutazione finora
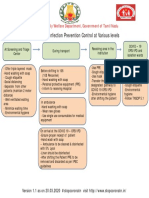
- TNSOP 5.0 Infection Prevention Control at Various Levels PDFDocumento1 paginaTNSOP 5.0 Infection Prevention Control at Various Levels PDFSridhar KrishnamurthiNessuna valutazione finora
- HRM Project ScribdDocumento91 pagineHRM Project ScribdGristy GranaNessuna valutazione finora
- Untitled 2Documento6 pagineUntitled 2tyakimisNessuna valutazione finora
- Introduction To Psychiatry JulitaDocumento30 pagineIntroduction To Psychiatry JulitaBugingo Julita100% (1)
- Tool Box Talk Topic-Workplace Housekeeping & Material StackingDocumento2 pagineTool Box Talk Topic-Workplace Housekeeping & Material StackingSameer PatilNessuna valutazione finora
- Addressing The High Corporate Costs of Back Pain (And Other MSDS) - Spine Research InstituteDocumento2 pagineAddressing The High Corporate Costs of Back Pain (And Other MSDS) - Spine Research InstituteDouglas Nespoli de MelloNessuna valutazione finora
- Chapter 18 Module Mood DisorderDocumento6 pagineChapter 18 Module Mood DisorderCheetah GemmaNessuna valutazione finora
- HealthAndSafetyUpdateSeptember2022 (002) 6Documento1 paginaHealthAndSafetyUpdateSeptember2022 (002) 6magsNessuna valutazione finora
- Unit Ig1: Management of Health and SafetyDocumento15 pagineUnit Ig1: Management of Health and SafetyVikash Kumar RayNessuna valutazione finora
- ESI Clinical Practice Guidelines For The.2Documento24 pagineESI Clinical Practice Guidelines For The.2Phan Ngo Minh TriNessuna valutazione finora
- Sample Socio Economic PlanDocumento9 pagineSample Socio Economic PlanajNessuna valutazione finora
- Symptoms and Signs of Psychiatric Disorders 1 1Documento56 pagineSymptoms and Signs of Psychiatric Disorders 1 1Vaso Talakvadze100% (1)
- III. Nursing Care Plan Nursing Priority No. 1: Ineffective Airway Clearance Related To Excessive Accumulation of Secretions Secondary To PneumoniaDocumento6 pagineIII. Nursing Care Plan Nursing Priority No. 1: Ineffective Airway Clearance Related To Excessive Accumulation of Secretions Secondary To PneumoniaRae Marie Aquino100% (1)
- HCIN-552: Clinical Documentation-Electronic Medical Record SystemsDocumento20 pagineHCIN-552: Clinical Documentation-Electronic Medical Record SystemssNessuna valutazione finora
- Chronic Kidney DiseaseDocumento29 pagineChronic Kidney DiseaseEsayas KebedeNessuna valutazione finora
- Transfer To Definitive Care EcaDocumento40 pagineTransfer To Definitive Care EcaFahrurido Kusbari100% (1)
- First CaseDocumento11 pagineFirst CaseRisha A.MNessuna valutazione finora
- BIRTH CompressedDocumento2 pagineBIRTH CompressedDip PatraNessuna valutazione finora
- Just Another Sebaceous Cyst?: I. Clinical QuestionDocumento3 pagineJust Another Sebaceous Cyst?: I. Clinical QuestionJaessa FelicianoNessuna valutazione finora
- Alternative MedicineDocumento306 pagineAlternative MedicineDamir Brankovic100% (3)
- Unhappy Meals - Michael Pollan - The New York TimesDocumento25 pagineUnhappy Meals - Michael Pollan - The New York TimesBob0% (1)
- Manual of The Medical DepartmentDocumento130 pagineManual of The Medical DepartmentDaryl IrwinNessuna valutazione finora
- Ayurvedic Treatment For Pancreatitis by Vaidya Balendu PrakashDocumento41 pagineAyurvedic Treatment For Pancreatitis by Vaidya Balendu Prakashpadaav100% (1)
- ) Administering Nasogastric Tube or Orogastric Tube FeedingDocumento6 pagine) Administering Nasogastric Tube or Orogastric Tube FeedingJohn Pearl FernandezNessuna valutazione finora