Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
SICH Mgmt2
Caricato da
Lennon Ponta-oyCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
SICH Mgmt2
Caricato da
Lennon Ponta-oyCopyright:
Formati disponibili
Open Access Review
Current management of spontaneous
intracerebral haemorrhage
Cyrus K Dastur, Wengui Yu
To cite: Dastur CK, Yu W. ABSTRACT prevention with antihypertensive medication
Current management of Intracerebral haemorrhage (ICH) is the most is likely the most effective strategy to reduce
spontaneous intracerebral devastating and disabling type of stroke. Uncontrolled
haemorrhage. Stroke and
the burden of ICH. Although only account-
hypertension (HTN) is the most common cause of ing for 1015% of all stroke in the USA,
Vascular Neurology 2017;00:
e000047. doi:10.1136/svn-
spontaneous ICH. Recent advances in neuroimaging, ICH causes a disproportionately high level of
organised stroke care, dedicated Neuro-ICUs, medical
2016-000047 morbidity and mortality.7 In 2010 alone,
and surgical management have improved the
62.8 million disability-associated life-years
management of ICH. Early airway protection, control of
malignant HTN, urgent reversal of coagulopathy and (DALY) were lost compared with 39.4 million
Received 10 October 2016 DALYs lost due to ischaemic stroke. Despite
Accepted 8 November 2016 surgical intervention may increase the chance of
survival for patients with severe ICH. Intensive lowering age-standardised mortality rates from ICH
of systolic blood pressure to <140 mm Hg is proven decreasing by over 25% over the last 15 years,
safe by two recent randomised trials. Transfusion of 3.2 million deaths were attributed to ICH vs
platelets in patients on antiplatelet therapy is not 3.3 million deaths from ischaemic stroke in
indicated unless the patient is scheduled for surgical 2013 alone.7
evacuation of haematoma. In patients with small Population-based studies suggest that the
haematoma without significant mass effect, there is no majority of patients with small ICH are
indication for routine use of mannitol or hypertonic
readily survivable with good medical care.8
saline (HTS). However, for patients with large ICH
(volume > 30 cbic centmetre) or symptomatic
For patients with large ICH, comprehensive
perihaematoma oedema, it may be beneficial to keep multidisciplinary care is essential to minimise
serum sodium level at 140150 mEq/L for 710 days morbidity and mortality. Multiple studies
to minimise oedema expansion and mass effect. have shown that caring for patients with ICH
Mannitol and HTS can be used emergently for in dedicated neurological intensive care
worsening cerebral oedema, elevated intracranial units by a specialised neurocritical care team
pressure (ICP) or pending herniation. HTS should be results in signicantly reduced length of stay
administered via central line as continuous infusion and mortality.911 In recent years, numerous
(3%) or bolus (23.4%). Ventriculostomy is indicated clinical trials have examined various medical
for patients with severe intraventricular haemorrhage, and surgical options for ICH. This review will
hydrocephalus or elevated ICP. Patients with large
summarise the advances in the evaluation
cerebellar or temporal ICH may benefit from emergent
haematoma evacuation. It is important to start
and management of ICH.
intermittent pneumatic compression devices at the time
of admission and subcutaneous unfractionated heparin
in stable patients within 48 hours of admission for CLASSIFICATION
prophylaxis of venous thromboembolism. There is no Spontaneous ICH is dened as intraparench-
benefit for seizure prophylaxis or aggressive ymal bleeding in the absence of trauma or
management of fever or hyperglycaemia. Early surgery. Common risk factors for spontan-
aggressive comprehensive care may improve survival eous ICH include HTN, age, history of heavy
and functional recovery. alcohol, methamphetamine or cocaine use,
education at less than a high school level
and genetic alleles associated with cerebral
INTRODUCTION amyloid.3 4 1214
Intracerebral haemorrhage (ICH) affects Spontaneous ICH can be classied as either
>1 million people annually worldwide and is primary or secondary depending on the
the deadliest and most disabling type of underlying cause. Primary ICH accounts for
Department of Neurology, stroke.1 2 Uncontrolled hypertension (HTN) 7080% of cases and is due to spontaneous
University of California Irvine, is the most common risk factor for spontan- rupture of small vessels damaged by HTN or
Irvine, California, USA
eous ICH.3 4 The incidence of ICH is higher amyloid angiopathy. Primary ICH is also clas-
Correspondence to in Asians, partly due to limited primary care sied by location as lobar versus non-lobar
Dr Wengui Yu; wyu@uci.edu for HTN and non-compliance.5 6 Primary and supratentorial versus infratentorial.15
Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047 1
Copyright 2017 by BMJ Publishing Group Ltd.
Open Access
and size of the ICH but also intraventricular extension,
mass effect, hydrocephalus and early signs of herniation.
Haematoma volume can be estimated on head CT
using the ABC/2 method, where A is maximal haema-
toma diameter on the axial slice with largest haematoma
area, B is maximal haematoma diameter perpendicular
to A and C is the number of CT slices with haematoma
multiplied by slice thickness (ignoring slices with <25%
of haematoma area compared with the reference
slice).21 22 This method of haematoma volume calcula-
tion, while variable between examiners, has been shown
to be effective for clinical decision-making.17 22
MRI can be as sensitive as CT in determining the pres-
ence of haemorrhage, but rarely offers additional infor-
mation in the acute setting. The time and transportation
required for MRI can be detrimental due to a high risk
of deterioration during the rst few hours. Delayed MRI
is better utilised as an adjunct tool to aid in determin-
ation of the underlying cause of the ICH (such as CAA,
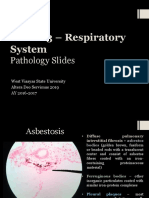
Figure 1 Typical locations of hypertensive ICH are putamen cavernoma and tumour).16
(A), thalamus (B), subcortical white matter (C), pons (D) and CT angiogram is very sensitive for identifying associated
cerebellum (E). Thalamic and subcortical haemorrhages often vascular abnormalities and contrast extravasation as spot
extend into ventricles (B and C). CAA, drug abuse or vascular sign.23 Contrast extravasation during angiography is asso-
anomaly often causes lobar haemorrhage (F). ICH, ciated with ongoing bleeding and increased mortality. The
intracerebral haemorrhage; CAA, cerebral amyloid angiopathy. risk of contrast extravasation is increased with extreme
HTN, depressed consciousness and large haemorrhages. A
Lobar ICH is commonly the result of cerebral amyloid newer technique for determining haematoma expansion,
angiopathy (CAA).14 Amyloid deposition in small-sized to the leakage sign, has higher sensitivity and specicity for
medium-sized cortical perforators may lead to the haematoma expansion than the spot sign, and showed a
rupture of these vessels, resulting in asymptomatic micro- signicant association with poor outcomes.24 However, the
haemorrhages or symptomatic lobar haemorrhages.14 requirement for an additional CT scan and greater radi-
Non-lobar ICH is most often the result of long-standing ation exposure may limit its clinical utility.
high blood pressure resulting in lipohyalinosis of small Repeat imaging study should be considered for evalu-
perforating arteries of the basal ganglia, thalamus, pons ation of any acute deterioration in the neurological
and cerebellum, leading to deep haemorrhages, often examination or for follow-up of any underlying lesion or
with extension into the ventricles.12 15 The most common vascular anomaly.
locations of hypertensive ICH are the putamen, thal-
amus, subcortical white matter, pons and cerebellum
(gure 1). EMERGENT INTERVENTION
Secondary ICH is associated with a number of con- ICH is a medical emergency requiring urgent therapy
genital and acquired conditions such as vascular malfor- given that >20% of patients experience a decrease of 2
mations, tumours, coagulation disorders, use of or more points in their Glasgow Coma Scale (GCS) after
anticoagulants and thrombolytic agents, cerebral vascu- their initial assessment by Emergency Medical Services
litis, drug abuse and cerebral venous thrombosis.3 16 17 (EMS).25 In addition, 1523% of patients have haema-
toma expansion and neurological decline in the rst
several hours.25 26
EARLY DIAGNOSIS Stabilisation of airway, breathing and circulation
ICH should be suspected in any patient with severe (ABCs) is essential for preventing secondary injury from
headache, vomiting, elevated systolic blood pressures or hypoxaemia, HTN and haematoma expansion.
decreased level of consciousness.16 Rapid diagnosis is Intubation for airway protection is indicated in patient
crucial for appropriate care and better functional out- with GCS 8 or signicant respiratory distress. Patient
comes. Early deterioration in the rst few hours after with a decreased level of consciousness from intraventri-
initial onset is common, from haematoma expansion cular haemorrhage with hydrocephalus, mass effect or
and from secondary injury.1820 In addition to a prompt brainstem herniation should receive ventriculostomy,
clinical history and neurological examination, rapid neu- hyperosmolar therapy with mannitol 0.51 g/kg or
roimaging with a non-contrast head CT is highly sensi- hypertonic saline (HTS) infusion. The Emergency
tive and specic for ICH and is the key to early Department (ED) algorithm for early diagnosis and
diagnosis.21 22 CT scan will reveal not only the location emergent intervention is shown in gure 2.
2 Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047
Open Access
Figure 2 The ED algorithm for early diagnosis and emergent intervention. ICH, intracerebral haemorrhage.
Management of HTN events (9.0% vs 4.0%, p=0.002) in the intensive treat-
Patients with ICH very often present with signicantly ment than the standard treatment group.31 Of note, the
elevated blood pressure. Elevated systolic blood pressure mean minimum SBPs of the two groups during the rst
(SBP) is associated with haematoma expansion, neuro- 2 hours were 128.916 and 141.114.8 mm Hg, respect-
logical deterioration and poor outcomes after ICH.2729 ively, which were much lower than 150 and 164 mm Hg
In the past, there was concern about perihaematomal achieved in the INTERACT-2 trial. The much lower
ischaemia from aggressive early blood pressure reduc- minimum SBPs in the intensive treatment group in the
tion. Recent studies showed no evidence of ischaemia in ATACH II trial might explain the higher incidence of
the perihaematoma zone.28 29 Two large phase III, multi- adverse renal events.31
centre, prospective randomised controlled trials have Given the ndings from INTERACT-2 trial, the 2015
showed that early lowering of SBP to <140 mm Hg is safe update to the AHA/ASA Guidelines for the
without signicant adversary effects.30 31 The Management of Spontaneous ICH recommend that for
INTERACT-2 trial comparing early lowering of SBP to patients presenting with SBP between 150 and 200,
<140 mm Hg with <180 mm Hg showed no increase in acute lowering of SBP to 140 mm Hg is safe and may be
adverse events in the aggressive treatment group.30 effective for improving functional outcome.20 The
There was no signicant difference in death or severe optimum target for patients presenting with SBP
disability at 90 days. An ordinal analysis of modied >220 mm Hg is less clear, though aggressive blood pres-
Rankin scores indicated improved functional outcomes sure reduction with continuous antihypertensive drug
with intensive lowering of blood pressure. The intravenous infusion and frequent monitoring is reason-
Antihypertensive Treatment of Acute Cerebral able. Any clinical deterioration in association with
Hemorrhage (ATACH) II trial used intravenous nicardi- aggressive reduction of blood pressure should lead to a
pine within 3 hours of ICH onset to target SBP reassessment of the target blood pressure.20
140 mm Hg versus SBP 180 mm Hg.31 Participant Intravenous calcium channel blockers (eg, nicardi-
enrolment was suspended at 1000 patients in September pine) and -blockers (eg, labetalol) are the treatment of
2015. There was no signicant difference in the primary choice for early BP reduction, given their short half-life
end points of death or disability at 90 days. The study, and ease of titration.32 Nitrates should be avoided given
however, showed a higher incidence of adverse renal potential for cerebral vasodilation and elevated
Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047 3
Open Access
intracranial pressure (ICP). Oral antihypertensive agents 3-factor products currently available in the USA are
need to be started as soon as possible to control resistant Prolnine SD (Grifols Biologicals, Los Angeles,
HTN and facilitate the transition of care from ICU to California, USA) and Bebulin VH (Baxter Healthcare
long-term management. Arterial line placement is Corporation, Westlake Village, California, USA). Kcentra
recommended to optimise blood pressure monitoring (Beriplex outside the USA) is the rst 4-factor PCC indi-
and medication titration. The guidelines for resistant cated for warfarin reversal in adults during acute major
HTN recommend angiotensin converting enzyme inhibi- bleeding or a need for urgent surgery.
tors (ACE-I) or angiotensin receptor blockers (ARB), PCC is preferred over FFP due to more rapid correc-
calcium channel blocker (CCB) and a thiazide-like diur- tion of INR, lower volume and risk of infection, pulmon-
etic at maximal tolerated doses as an optimal triplets ary oedema, Transfusion-Related Acute Lung Injury
formula.32 The CCB and ACE-I or ARB are widely (TRALI) and Transfusion Associated Cardiac Overload
accepted as the rst-line and second-line drugs for resist- (TACO). If repeat INR 1560 min after PCC administra-
ant patients, but the choice of the third-line and fourth- tion shows continued INR elevation above 1.4, consider
line antihypertensive agents varies greatly in real-world further correction with 24 units FFP. Recombinant
practice. Thiazide may cause hyponatraemia and worsen Factor VIIa (rFVIIa) has been associated with relatively
cerebral oedema in patients with large haemorrhage or high thrombosis rates and should only be considered in
mass effect. It should be used with caution. In a recent patients who will not accept blood products (eg,
randomised trial, spironolactone was shown to be very Jehovahs witness).
effective for patients with resistant HTN.33 Direct thrombin inhibitors (DTIs; eg, dabigatran, arga-
Spironolactone and -/-antagonists can be used as the troban and bivalirudin) have signicantly less risk of
third and fourth agents to maintain BP control while ICH than vitamin K antagonists. However, haemorrhages
weaning off intravenous agents. During acute phase, do occur and reversal of coagulopathy is indicated if
patients may have resistant HTN due to sympathetic patient presents within 35 half-lives of drug exposure
surge. A few weeks later, they may require fewer medica- (or beyond in patient with renal insufciency).
tions and be at risk of hypotension unless the doses of Idarucizumab (5 g intravenous divided into two doses),
medications are adjusted promptly.16 a specic neutralising monoclonal antibody fragment
for dabigatran, is recommended in cases of haemor-
rhage associated with dabigatran.36 If idarucizumab is
REVERSAL OF COAGULOPATHIES not available, or if the haemorrhage is associated with a
Coagulopathy, whether medication-induced or due to a DTI other than dabigatran, 4-factor PCC (50 units/kg)
systemic disease process, is associated with haematoma or activated PCC (50 units/kg) is recommended.
expansion, and increased risk of poor outcome and Haemodialysis can also be considered in patients with
death.34 Approximately 1220% of patients presenting dabigatran-associated ICH and renal insufciency, espe-
with ICH are taking oral anticoagulants. Though acute cially if continued haemorrhage despite rst-line
reversal of coagulopathy has not been clearly shown to therapies.
be benecial in large randomised trials, rapid correction For patients taking Factor Xa inhibitors (eg, rivaroxa-
of coagulopathy should be considered in any potentially ban, apixaban and edoxaban), 4-factor PCC (50 units/
salvageable patient. kg) or activated PCC (50 units/kg) is recommended if
In December 2015, the Neurocritical Care Society the haemorrhage occurred within 35 half-lives of drug
together with the Society of Critical Care Medicine pub- exposure (or in context of liver failure). If presenting
lished guidelines for the reversal of antithrombotic within 2 hours of drug exposure, activated charcoal can
agents in patients with ICH.35 Whenever ICH is diag- be administrated to prevent further drug absorption.
nosed, any antithrombotic agent should be immediately Laboratory testing is unlikely to be helpful in guiding
discontinued. The method of reversal will depend on treatment for these patients; therefore, reversal should
the agent used. be guided by bleeding (major or intracranial) instead.
For all patients taking vitamin K antagonists (eg, war- Andexanet alfa is a recombinant modied factor Xa that
farin), vitamin K 10 mg and 3-factor or 4-factor pro- can bind and reverse oral and parenteral factor Xa inhi-
thrombin complex concentrates (PCCs) should be bitors, including rivaroxaban, apixaban and edoxaban,
administered intravenously for patients with INR 1.4. and low-molecular-weight heparin.37 It has not been
PCC is an inactivated concentrate of factors II, IX and approved by the FDA for clinical use.
X, with variable amounts of factor VII. Variation in The guidelines for reversing warfarin and novel oral
factor VII concentrations in PCC has led to their classi- anticoagulants (NOAC) coagulopathies in patients with
cation as either 3- or 4-factor. Unlike serum-containing symptomatic ICH are shown in gure 3.
products such as fresh frozen plasma (FFP), PCCs are Reversal of unfractionated heparin is recommended
lyophilised and can be reconstituted quickly for timely for patients who develop ICH while on heparin infusion.
administration. In addition, the concentration of vitamin Reversal of prophylactic subcutaneous heparin should
K-dependent clotting factors is 25 times higher than only be considered if activated partial thormboplastin
plasma and can reverse coagulopathy quickly. The two time (aPTT) is signicantly prolonged in setting of new
4 Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047
Open Access
Figure 3 The guidelines for reversing warfarin and NOAC coagulopathies in patients with symptomatic ICH. ICH, intracerebral
haemorrhage.
haemorrhage. Intravenous protamine (1 mg per every platelet function testing, haemorrhage volume or neuro-
100 units of heparin given in past 23 hours, maximum logical examination. In a multicentre, open-label rando-
50 mg) should be utilised and repeated at half of the mised trial at 60 hospitals in the Netherlands, UK and
initial dose if repeat aPTT remains elevated. France, 190 patients with ICH on antiplatelet therapy
Reversal of low-molecular-weight heparin (low molecular for at least 7 days prior to ICH were randomly assigned
weight heparin (LMWH); eg, enoxaparin, dalteparin, to platelet transfusion and standard care. Platelet trans-
nadroparin and tinzaparin) is also recommended only if fusion seems inferior to standard care for patients taking
receiving therapeutic doses, rather than prophylactic doses. antiplatelet therapy before ICH.38
For enoxaparin administered within past 8 hours, 1 mg of Platelet transfusion should be considered for patients
protamine per every 1 mg of enoxaparin should be admi- with aspirin- or adenosine diphosphate receptor (ADP)
nistered. If enoxaparin given 812 hours, 0.5 mg of protam- inhibitor-associated ICH who will undergo a neurosurgi-
ine per every 1 mg of enoxaparin should be administered. cal procedure. Platelet function testing prior to platelet
For the reversal of dalteparin, nadroparin and tinzaparin, transfusion should be performed if possible and timely
dose 1 mg per every 100 anti-Xa units of LMWH, up to results available. If platelet function is within normal
maximum 50 mg. This can be repeated at half of the initial limits or patient has documented antiplatelet resistance,
dose if continued bleeding or patient has renal insuf- platelet transfusion should be avoided. Platelet transfu-
ciency. rFVIIa is generally not recommended, but can be sion is not recommended for non-steroidal anti-inam-
considered if protamine contraindicated. matory drugs (NSAIDs) or glycoprotein (GP) IIb/IIA
Heparinoids (eg, danaparoid) are not available in the inhibitor-related ICH. Desmopressin (ddAVP) (0.4 g/
USA, but are used in other countries. In ex vivo studies, kg intravenous once) can be considered in ICH asso-
danaparoid was not reversed with protamine, PCC, ciated with cyclooxygenase (COX) inhibitors or ADP
aPCC or FFP; therefore, these agents are not recom- receptor inhibitors.35
mended for reversal in patients with ICH. rFVIIa
(90 g/kg intravenous once) has shown some efcacy Management of intraventricular haemorrhage and
and therefore is recommended instead. hydrocephalus
For thrombolytic (eg, recombinant tissue plasminogen Intraventricular haemorrhage (IVH) occurs in up to
activator (rtPA)) reversal, 10 units of cryoprecipitate may 45% of patients with ICH. It is associated with lower
be considered. If the level of brinogen is <150 mg/dL GCS and an independent predictor of poor outcome.39
post cryoprecipitate use, consider additional cryoprecipi- External ventricular drain (EVD) placement should be
tate administration. If cryoprecipitate is contraindicated considered in any patient with GCS 8, signicant IVH,
or unavailable, an antibrinolytic agent (tranexamic hydrocephalus or evidence of transtentorial hernia-
acid 1015 mg/kg intravenous or -aminocaproic acid tion.20 Elevated ICP (>20 mm Hg) should be treated
45 g intravenous) can be considered. with hyperosmolar therapy (HTS and/or mannitol),
For patients taking antiplatelet agents (eg, aspirin, clo- cerebrospinal uid drainage or sedation, though none
pidogrel and abciximab), platelet transfusion is not of these therapies has been shown to improve
recommended routinely, regardless of antiplatelet agent, outcomes.12
Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047 5
Open Access
Apart from clotting the cerebral aqueduct leading to treatment and may lead to upward herniation and
obstructive hydrocephalus, intraventricular blood and its further neurological decline.12 27 Select patients with
breakdown products cause inammation of the epen- large lobar ICH or temporal lobe haemorrhage may also
dymal layer and subependymal brain tissue. In addition, benet from emergent haematoma evacuation.
the clot also causes inammation and brosis of the
arachnoid granulations, leading to delayed communicat-
MANAGEMENT OF PERIHAEMATOMA OEDEMA
ing hydrocephalus. Intraventricular brinolysis with rtPA
Perihaematomal oedema (PHE) develops within the
was an emerging therapy for clearing IVH as soon as
rst few days after ICH and may cause elevated ICP,
possible. It was shown to clear IVH without increasing
mass effect, midline shift and brain herniation.48 49 50
perihaemorrhagic oedema.40 Recently, a large, phase III,
The degree and growth of PHE are strongly related to
multicentre, randomised, placebo controlled clinical
the size of haematoma.48 Data from several clinical trials
trial evaluating the use of intraventricular tPA adminis-
indicate that the absolute increase in PHE during the
tration in patients with IVH has completed enrolment.
rst 2472 hours was associated with worse functional
The preliminary results of the Clot Lysis: Evaluating
outcomes at 90 days after ICH.49 50
Accelerated Resolution of Intraventricular Hemorrhage
Patients with asymptomatic PHE require no specic treat-
III (CLEAR III) trial showed no outcome benet.
ment except maintaining a normal sodium goal. There is
Subgroup analysis showed reduced mortality in patients
no indication for routine use of osmotic agents, such as
with large IVH (2016 International Stroke Conference
mannitol or HTS, in most patients with small ICH.
Press Release18 February 2016).
However, mannitol and HTS are the rst-line medical
therapies for patients with symptomatic cerebral oedema
and elevated ICP. Mannitol is an osmotic diuretic. It
SURGICAL INTERVENTION
increases water excretion by the kidneys and reduces
The International Surgical Trial in Intracerebral
cerebral oedema and ICP. HTS increases plasma osmo-
Hemorrhage (ISTICH) and the subsequent STICH II
larity and the ow of excess water from cerebral tissue to
demonstrated no benet for early haematoma evacu-
the blood via the osmotic gradient.
ation in patients with supratentorial ICH.41 42 Subgroup
In a small retrospective study, treatment with 23.4% of
analysis shows a small survival benet in patients with
HTS was associated with rapid reversal of transtentorial
supercial lobar haemorrhages without signicant
herniation and reduced ICP.51 Early continuous infusion
improvement in functional outcomes.
of 3% of HTS for sodium goal of 145155 mmol/L was
Utilisation of minimally invasive techniques for clot
associated with less cerebral oedema and ICP crisis
evacuation, however, may be promising.43 In a clinical
(>20 mm Hg for > 20 min or new anisocoria) than his-
trial performed in China a decade ago, 377 patients
torical control (n=64).52 A meta-analysis performed in
with basal ganglia ICH were randomised to treatment
2011 showed that HTS is slightly more effective than
with minimally invasive craniopuncture and needle
mannitol for the treatment of elevated ICP.53 A recent
aspiration versus conservative treatment.44 The study
analysis of the INTERACT2 data showed that mannitol
showed a signicant improvement in neurological func-
seems safe, but might not improve outcome in patients
tion at 2 weeks and 3 months without mortality benet.
with acute ICH.54
The Minimally-Invasive Surgery plus rtPA for
In real-world practice, the patients medical history
Intracerebral Hemorrhage Evacuation (MISTIE) phase
and the side effect proles of mannitol and HTS may be
II trial evaluated the utilisation of stereotactic clot cath-
the major factors for choosing an osmotic agent for an
eterisation and intermittent dosing of rtPA to facilitate
individual patient. For example, patients with congestive
clot breakdown and aspiration.45 It showed a trend
heart failure should receive a bolus of mannitol or
towards improved outcomes in the surgical patients com-
23.4% of HTS, whereas continuous infusion of 3% of
pared with the medically managed patients. The
HTS can be used for patients with dehydration or
ongoing MISTIE III trial has added a Stereotactic
decreased urine output.
CT-guided Endoscopic Surgery arm. Preliminary data
Of note, Minimally Invasive Surgery Plus tPA for ICH
showed that the newer trans-sylvian, transinsular
Evacuation (MISTIE) II study revealed signicant associ-
minimal invasive approaches may yield better results due
ation of haematoma removal and oedema reduction in
to relative sparing of cortical function.46 47 Randomised
the surgical group.45 Additional study is warranted to
controlled studies are required to evaluate their clinical
show the effect on outcomes.
benet.
Unlike supratentorial ICH, cerebellar ICH is consid-
ered a neurosurgical emergency and evacuation is SEIZURE PROPHYLAXIS AND TREATMENT
recommended per current guidelines given the high Patient with ICH have up to 16% risk of clinical seizures
morbidity from rapid development of brainstem com- within 1 week, with majority occurring at or near
pression.20 Surgical indications include haematoma size onset.55 56 Lobar ICH with cortical involvement is the
>3 cm in diameter, brainstem compression or hydro- most important risk factor.57 Prospective and population-
cephalus. EVD placement alone is not sufcient based studies have shown no association between clinical
6 Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047
Open Access
seizures and neurological outcome or mortality.58 59 Patients with DVT or PE should be considered for sys-
Between 28% and 31% of patients will have electro- temic anticoagulation depending on stability of the haema-
graphic seizures on continuous electroencephalographic toma, cause of haemorrhage and time since presentation.
monitoring.58 The clinical impact of subclinical seizures If systemic anticoagulation is contraindicated, inferior vena
is unclear. Prophylactic phenytoin usage has been asso- cava lter placement should be considered.20 71
ciated with worse outcomes in several studies.59 60
Continuous EEG monitoring should be considered for
PROGNOSIS
patients with ICH with depressed mental status out of
ICH is the most debilitating and deadly type of stroke. A
proportion to the degree of brain injury. Clinical sei-
number of factors may affect outcome after ICH, includ-
zures should be treated with antiepileptic medications,
ing haematoma volume and location, haematoma
as should electrographic seizures accompanied by
expansion, age, GCS score on presentation, intraventri-
changes in mental status.20
cular extension and anticoagulant use. The ICH score
was developed to predict 30-day mortality rate and func-
GLUCOSE MANAGEMENT tional outcomes at 1 year.72 73 Most patients die from
Hyperglycaemia on admission is associated with worse ICH within the initial hospitalisation due to presumed
morbidity and mortality independent of the presence of poor outcome leading to withdrawal of care.74 None of
diabetes.61 However, tight glucose control with target the existing prediction models, including the ICH score,
glucose 80110 mg/dL increases hypoglycaemia and the is proven reliable. Several studies have shown that with-
risk of morbidity and mortality.62 Care should be taken drawal of support and early care limitations, such as do-
to avoid hyperglycaemia and hypoglycaemia.20 It is rea- not-resuscitate (DNR) orders, within the rst day of hos-
sonable to target glucose level at 100150 mg/dL for pitalisation are an independent predictor of poor
patients with ICH. outcome.7376 This raises concerns for self-fullling
prophecies. Of note, ICH mortality rate in China was
much lower than that in the USA,77 likely due to fewer
FEVER CONTROL withdrawal of life support.
Fever is common after ICH, particularly in patients with The current AHA/ASA guidelines recommend early
intraventricular extension. Sustained fever after ICH is and aggressive care after ICH and postponement of any
an independent prognostic factor for worse outcome.63 new DNR orders until at least the second full day of
However, neither therapeutic hypothermia nor nor- treatment. Patients with pre-existing DNR orders are
mothermia was shown to improve outcome.64 65 In a excluded from this recommendation. However, DNR
retrospective casecontrol study of patients with spontan- status should not limit appropriate medical and surgical
eous ICH having two consecutive fevers 38.3C despite interventions, unless explicitly indicated.20
acetaminophen administration, therapeutic normother-
mia was shown to be associated with increased duration
of sedation, mechanical ventilation and Neuro-ICU CONCLUSIONS
length of stay without discharge outcome benet.65 ICH is a medical emergency with high risk of morbidity
Normothermia or hypothermia should not be used after and mortality. Recent advances in early diagnosis and
ICH except in the setting of clinical trials. neurocritical care have contributed to improved survival.
Continued research into prevention and effective
therapy is pivotal in reducing disease burden and
DEEP VEIN THROMBOSIS PROPHYLAXIS AND TREATMENT improving functional recovery.
There is a signicant risk of venous thromboembolism
Contributors CKD is involved in drafting the work. WY is responsible revising
(VTE) in patients with ICH, with the rate of symptom-
the manuscript critically for important intellectual content.
atic deep vein thrombosis (DVT) at 15%.6670 The inci-
dence of symptomatic pulmonary embolism (PE) is Competing interests None declared.
0.52%.6870 Up to half of the PE are fatal. It is there- Provenance and peer review Commissioned; internally peer reviewed.
fore essential to prevent VTE. Data sharing statement No additional data are available.
Guidelines published by the Neurocritical Care
Open Access This is an Open Access article distributed in accordance with
Society in December 2015 recommend the initiation of the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license,
mechanical VTE prophylaxis, preferably with intermit- which permits others to distribute, remix, adapt, build upon this work non-
tent pneumatic compression (IPC) devices at the time commercially, and license their derivative works on different terms, provided
of admission.20 71 If IPC devices are unavailable, gradu- the original work is properly cited and the use is non-commercial. See: http://
creativecommons.org/licenses/by-nc/4.0/
ated compression stockings (GCS) can be utilised.
Prophylactic doses of subcutaneous unfractionated
heparin or LMWH should be started in patients with REFERENCES
stable haematomas within 48 hours of admission. 1. Qureshi AI, Tuhrim S, Broderick JP, et al. Spontaneous intracerebral
hemorrhage. N Engl J Med 2001;344:145060.
Mechanical VTE prophylaxis should be continued after 2. Flaherty ML, Haverbusch M, Sekar P, et al. Long-term mortality after
initiation of pharmacological prophylaxis. intracerebral hemorrhage. Neurology 2006;66:11826.
Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047 7
Open Access
3. Ariesen MJ, Claus SP, Rinkel GJ, et al. Risk factors for intracerebral 30. Anderson CS, Heeley E, Huang Y, et al. Rapid blood-pressure
hemorrhage in the general population: a systematic review. Stroke lowering in patients with acute intracerebral hemorrhage. N Engl
2003;34:20605. J Med 2013;368:235565.
4. Meretoja A, Strbian D, Putaala J, et al. SMASH-U: a proposal for 31. Qureshi AI, Palesch YY, Barsan WG, et al. Intensive blood-pressure
etiologic classification of intracerebral hemorrhage. Stroke lowering in patients with acute cerebral hemorrhage. N Engl J Med
2012;43:25927. 2016;375:103343.
5. van Asch CJ, Luitse MJ, Rinkel GJ, et al. Incidence, case fatality, 32. Calhoun DA, Jones D, Textor S, et al. Resistant hypertension:
and functional outcome of intracerebral haemorrhage over time, diagnosis, evaluation, and treatment. A scientific statement from the
according to age, sex, and ethnic origin: a systematic review and American Heart Association Professional Education Committee of
meta-analysis. Lancet Neurol 2010;9:16776. the Council for High Blood Pressure Research. Hypertension
6. Feigin VL, Lawes CM, Bennett DA, et al. Worldwide stroke incidence 2008;51:140319.
and early case fatality reported in 56 population-based studies: 33. Williams B, MacDonald TM, Morant S, et al. Spironolactone versus
a systematic review. Lancet Neurol 2009;8:35569. placebo, bisoprolol, and doxazosin to determine the optimal
7. Mozaffarian D, Benjamin EJ, Go AS, et al. Heart disease and stroke treatment for drug-resistant hypertension (PATHWAY-2): a
statistics2016 update a report from the American Heart randomised, double-blind, crossover trial. Lancet 2015;386:205968.
Association. Circulation 2015;131:e29322. 34. Huhtakangas J, Tetri S, Juvela S, et al. Effect of increased warfarin
8. Zahuranec DB, Gonzales NR, Brown DL, et al. Presentation of use on warfarin-related cerebral hemorrhage: a longitudinal
intracerebral haemorrhage in a community. J Neurol Neurosurg population-based study. Stroke 2011;42:24315.
Psychiatr 2006;77:3404. 35. Frontera JA, Lewin JJ, Rabinstein AA. Guideline for reversal of
9. Diringer MN, Edwards DF. Admission to a neurologic/neurosurgical antithrombotics in intracranial hemorrhage. Neurocrit Care
intensive care unit is associated with reduced mortality rate after 2015;24:646.
intracerebral hemorrhage. Crit Care Med 2001;29:63540. 36. Pollack CV Jr, Reilly PA, Eikelboom J, et al. Idarucizumab for
10. Mirski MA, Chang CW, Cowan R. Impact of a neuroscience intensive dabigatran reversal. N Engl J Med 2015;373:51120.
care unit on neurosurgical patient outcomes and cost of care: 37. Siegal DM, Curnutte JT, Connolly SJ, et al. Andexanet Alfa for the
evidence-based support for an intensivist-directed specialty ICU reversal of factor Xa inhibitor activity. N Engl J Med 2015;373:2413.
model of care. J Neurosurg Anesthesiol 2001;13:8392. 38. Baharoglu MI, Cordonnier C, Al-Shahi Salman R, et al. Platelet
11. Suarez JI, Zaidat OO, Suri MF, et al. Length of stay and mortality in transfusion versus standard care after acute stroke due to
neurocritically ill patients: impact of a specialized neurocritical care spontaneous cerebral haemorrhage associated with antiplatelet
team. Crit Care Med 2004;32:23117. therapy (PATCH): a randomised, open-label, phase 3 trial. Lancet
12. Chan S, Hemphill JC. Critical care management of intracerebral 2016;387:260513.
hemorrhage. Crit Care Clin 2014;30:699717. 39. Hallevi H, Albright KC, Aronowski J, et al. Intraventricular
13. Cai X, Rosand J. The evaluation and management of adult hemorrhage: anatomic relationships and clinical implications.
intracerebral hemorrhage. Semin Neurol 2015;35:63845. Neurology 2008;70:84852.
14. Greenberg SM. Amyloid angiopathy. Neurology 1997;48:291. 40. Volbers B, Wagner I, Willfarth W, et al. Intraventricular fibrinolysis
15. Martini SR, Flaherty ML, Brown WM, et al. Risk factors for does not increase perihemorrhagic edema after intracerebral
intracerebral hemorrhage differ according to hemorrhage location. hemorrhage. Stroke 2013;44:3626.
Neurology 2012;79:227582. 41. Mendelow AD, Gregson BA, Fernandes HM, et al. Early surgery
16. Smith EE, Rosand J, Greenberg SM. Hemorrhagic stroke. versus initial conservative treatment in patients with spontaneous
Neuroimaging Clin N Am 2005;15:25972, ix. supratentorial intracerebral haematomas in the International Surgical
17. Divani AA, Majidi S, Luo X, et al. The ABCs of accurate volumetric Trial in Intracerebral Haemorrhage (STICH): a randomised trial.
measurement of cerebral hematoma. Stroke 2011;42:156974. Lancet 2005;365:38797.
18. Kothari RU, Brott T, Broderick JP, et al. The ABCs of measuring 42. Mendelow AD, Gregson BA, Rowan EN, et al. Early surgery versus
intracerebral hemorrhage volumes. Stroke 1996;27:13045. initial conservative treatment in patients with spontaneous
19. Webb AJS, Ullman NL, Morgan TC, et al. Accuracy of the ABC/2 supratentorial lobar intracerebral haematomas (STICH II): a
score for intracerebral hemorrhage: systematic review and analysis randomised trial. Lancet 2013;382:397408.
of MISTIE, CLEAR-IVH, and CLEAR III. Stroke 2015;46: 43. Dey M, Stadnik A, Awad IA. Spontaneous intracerebral and
24706. intraventricular hemorrhage: advances in minimally invasive surgery
20. Becker KJ, Baxter AB, Bybee HM, et al. Extravasation of and thrombolytic evacuation, and lessons learned in recent trials.
radiographic contrast is an independent predictor of death in primary Neurosurgery 2014;74(Suppl 1):S14250.
intracerebral hemorrhage. Stroke 1999;30:202532. 44. Wang WZ, Jiang B, Liu HM, et al. Minimally invasive craniopuncture
21. Orito K, Hirohata M, Nakamura Y, et al. Leakage sign for primary therapy vs. conservative treatment for spontaneous intracerebral
intracerebral hemorrhage: a novel predictor of hematoma growth. hemorrhage: results from a randomized clinical trial in China. Int
Stroke 2016;47:95863. J Stroke 2009;4:1116.
22. Moon JS, Janjua N, Ahmed S, et al. Prehospital neurologic 45. Mould WA, Carhuapoma JR, Muschelli J, et al. Minimally invasive
deterioration in patients with intracerebral hemorrhage. Crit Care surgery plus recombinant tissue-type plasminogen activator for
Med 2008;36:1725. intracerebral hemorrhage evacuation decreases perihematomal
23. Fan JS, Huang HH, Chen YC, et al. Emergency department edema. Stroke 2013;44:62734.
neurologic deterioration in patients with spontaneous intracerebral 46. Spiotta AM, Fiorella D, Vargas J, et al. Initial multicenter technical
hemorrhage: incidence, predictors, and prognostic significance. experience with the Apollo device for minimally invasive intracerebral
Acad Emerg Med 2012;19:1338. hematoma evacuation. Neurosurgery 2015;11(Suppl 2):24351;
24. Brott T, Broderick J, Kothari R, et al. Early hemorrhage growth in discussion 251.
patients with intracerebral hemorrhage. Stroke 1997;28:15. 47. Przybylowski CJ, Ding D, Starke RM, et al. Endoport-assisted
25. Rodriguez-Luna D, Pieiro S, Rubiera M, et al. Impact of blood surgery for the management of spontaneous intracerebral
pressure changes and course on hematoma growth in acute hemorrhage. J Clin Neurosci 2015;22:172732.
intracerebral hemorrhage. Eur J Neurol 2013;20:127783. 48. Arima H, Wang JG, Huang Y, et al. Significance of perihematomal
26. Hemphill JC III, Greenberg SM, Anderson CS, et al. Guidelines for edema in acute intracerebral hemorrhage: the INTERACT trial.
the management of spontaneous intracerebral hemorrhage. Neurology 2009;73:19638.
A guideline for healthcare professionals from the American 49. Murthy SB, Moradiya Y, Dawson J, et al. Perihematomal edema and
Heart Association/American Stroke Association. Stroke functional outcomes in intracerebral hemorrhage: influence of
2015;46:203260. hematoma volume and location. Stroke 2015;46:308892.
27. Sakamoto Y, Koga M, Yamagami H, et al. Systolic blood pressure 50. Yang J, Arima H, Wu G, et al. Prognostic significance of
after intravenous antihypertensive treatment and clinical outcomes in perihematomal edema in acute intracerebral hemorrhage: pooled
hyperacute intracerebral hemorrhage: the stroke acute management analysis from the intensive blood pressure reduction in acute
with urgent risk-factor assessment and improvement-intracerebral cerebral hemorrhage trial studies. Stroke 2015;46:100913.
hemorrhage study. Stroke 2013;44:184651. 51. Koenig MA, Bryan M, Lewin JL III, et al. Reversal of transtentorial
28. Zazulia AR, Diringer MN, Videen TO, et al. Hypoperfusion without herniation with hypertonic saline. Neurology 2008;70:10239.
ischemia surrounding acute intracerebral hemorrhage. J Cereb 52. Wagner I, Hauer EM, Staykov D, et al. Effects of continuous
Blood Flow Metab 2001;21:80410. hypertonic saline infusion on perihemorrhagic edema evolution.
29. Butcher KS, Jeerakathil T, Hill M, et al. The intracerebral Stroke 2011;42:15405.
hemorrhage acutely decreasing arterial pressure trial. Stroke 53. Kamel H, Navi BB, Nakagawa K, et al. Hypertonic saline versus
2013;44:6206. mannitol for the treatment of elevated intracranial pressure: a
8 Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047
Open Access
meta-analysis of randomized clinical trials. Crit Care Med 67. Goldstein JN, Fazen LE, Wendell L, et al. Risk of thromboembolism
2011;39:5549. following acute intracerebral hemorrhage. Neurocrit Care
54. Wang X, Arima H, Yang J, et al. Mannitol and outcome in 2009;10:2834.
intracerebral hemorrhage: propensity score and multivariable 68. Gregory PC, Kuhlemeier KV. Prevalence of venous
Intensive Blood Pressure Reduction in Acute Cerebral Hemorrhage thromboembolism in acute hemorrhagic and thromboembolic stroke.
Trial 2 results. Stroke 2015;46:27627. Am J Phys Med Rehabil 2003;82:3649.
55. De Herdt V, Dumont F, Hnon H, et al. Early seizures in 69. Kim KS, Brophy GM. Symptomatic venous thromboembolism:
intracerebral hemorrhage: incidence, associated factors, and incidence and risk factors in patients with spontaneous or
outcome. Neurology 2011;77:1794800. traumatic intracranial hemorrhage. Neurocrit Care 2009;11:
56. Bladin CF, Alexandrov AV, Bellavance A, et al. Seizures after stroke: 2833.
a prospective multicenter study. Arch Neurol 2000;57:161722. 70. Diringer MN, Skolnick BE, Mayer SA, et al. Thromboembolic events
57. Passero S, Rocchi R, Rossi S, et al. Seizures after spontaneous with recombinant activated factor VII in spontaneous intracerebral
supratentorial intracerebral hemorrhage. Epilepsia 2002;43:117580. hemorrhage: results from the factor seven for acute hemorrhagic
58. Mullen MT, Kasner SE, Mess SR. Seizures do not increase stroke (FAST) trial. Stroke 2010;41:4853.
in-hospital mortality after intracerebral hemorrhage in the nationwide 71. Nyquist P, Bautista C, Jichici D, et al. Prophylaxis of venous
inpatient sample. Neurocrit Care 2013;19:1924. thrombosis in neurocritical care patients: an evidence-based
59. Naidech AM, Garg RK, Liebling S, et al. Anticonvulsant use and guidelinea statement for healthcare professionals from the
outcomes after intracerebral hemorrhage. Stroke 2009;40:381015. Neurocritical Care Society. Neurocrit Care 2016;24:
60. Mess SR, Sansing LH, Cucchiara BL, et al. Prophylactic 4760.
antiepileptic drug use is associated with poor outcome following 72. Hemphill JC, Bonovich DC, Besmertis L, et al. The ICH score: a
ICH. Neurocrit Care 2009;11:3844. simple, reliable grading scale for intracerebral hemorrhage. Stroke
61. Passero S, Ciacci G, Ulivelli M. The influence of diabetes and 2001;32:8917.
hyperglycemia on clinical course after intracerebral hemorrhage. 73. Hemphill JC, Farrant M, Neill TA. Prospective validation of the ICH
Neurology 2003;61:13516. Score for 12-month functional outcome. Neurology
62. Finfer S, Chittock DR, Su SY, et al. Intensive versus conventional 2009;73:108894.
glucose control in critically ill patients. N Engl J Med 2009;360:128397. 74. Hemphill JC, Newman J, Zhao S, et al. Hospital usage of early
63. Schwarz S, Hfner K, Aschoff A, et al. Incidence and prognostic do-not-resuscitate orders and outcome after intracerebral
significance of fever following intracerebral hemorrhage. Neurology hemorrhage. Stroke 2004;35:11304.
2000;54:35461. 75. Zahuranec DB, Brown DL, Lisabeth LD, et al. Early care limitations
64. Kollmar R, Staykov D, Drfler A, et al. Hypothermia reduces independently predict mortality after intracerebral hemorrhage.
perihemorrhagic edema after intracerebral hemorrhage. Stroke Neurology 2007;68:16517.
2010;41:16849. 76. Zahuranec DB, Morgenstern LB, Snchez BN, et al.
65. Lord AS, Karinja S, Lantigua H, et al. Therapeutic temperature Do-not-resuscitate orders and predictive models after intracerebral
modulation for fever after intracerebral hemorrhage. Neurocrit Care hemorrhage. Neurology 2010;75:62633.
2014;21:2006. 77. Wang W, Lu J, Wang C, et al. Prognostic value of ICH score and
66. Lacut K, Bressollette L, Le Gal G, et al. Prevention of ICH-GS score in Chinese intracerebral hemorrhage patients:
venousthrombosis in patients with acute intracerebral hemorrhage. analysis from the China National Stroke Registry (CNSR). PLoS
Neurology 2005;65:8659. ONE 2013;8:e77421.
Dastur CK, Yu W. Stroke and Vascular Neurology 2017;00:e000047. doi:10.1136/svn-2016-000047 9
Potrebbero piacerti anche
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- BFS Case DiscxnDocumento23 pagineBFS Case DiscxnLennon Ponta-oyNessuna valutazione finora
- Tourniquet (Test Procedure)Documento2 pagineTourniquet (Test Procedure)Lennon Ponta-oyNessuna valutazione finora
- Block 13 Patho SlidesDocumento62 pagineBlock 13 Patho SlidesLennon Ponta-oyNessuna valutazione finora
- Ophtha Case ReportDocumento7 pagineOphtha Case ReportLennon Ponta-oyNessuna valutazione finora
- AFE Vs PEDocumento1 paginaAFE Vs PELennon Ponta-oyNessuna valutazione finora
- Clinical Study: Button Battery Foreign Bodies in Children: Hazards, Management, and RecommendationsDocumento8 pagineClinical Study: Button Battery Foreign Bodies in Children: Hazards, Management, and RecommendationsLennon Ponta-oyNessuna valutazione finora
- A Narrative Review of The Management of Nasal Foreign Bodies in Children in General PracticeDocumento8 pagineA Narrative Review of The Management of Nasal Foreign Bodies in Children in General PracticeLennon Ponta-oyNessuna valutazione finora
- SICH MGMTDocumento12 pagineSICH MGMTLennon Ponta-oyNessuna valutazione finora
- A Specific Brain Structural Basis For Individual Differences in Reality MonitoringDocumento2 pagineA Specific Brain Structural Basis For Individual Differences in Reality MonitoringLennon Ponta-oyNessuna valutazione finora
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5795)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1091)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Kwah Dan Diong, 2014Documento1 paginaKwah Dan Diong, 2014heruNessuna valutazione finora
- Vascular DementiaDocumento3 pagineVascular DementiaAkhmad Ulil AlbabNessuna valutazione finora
- Application Form IHCDocumento79 pagineApplication Form IHCGÜENDY HOUSTONNessuna valutazione finora
- Neurorehabilitation 1Documento439 pagineNeurorehabilitation 1Duncan D'AmicoNessuna valutazione finora
- Hypertensive Emergencies Part 1Documento55 pagineHypertensive Emergencies Part 1P100% (1)
- Estenosis Carotidea en Paciente Con Cardiopatía IsquémicaDocumento57 pagineEstenosis Carotidea en Paciente Con Cardiopatía IsquémicaSOLACI - Sociedad Latinoamericana de Cardiología IntervencionistaNessuna valutazione finora
- Effect of Constraint Induced Movement Therapy Versus Motor Relearning Programme To Enhance Upper Limb Motor Function in Stroke Patients: A Quasi Experimental StudyDocumento7 pagineEffect of Constraint Induced Movement Therapy Versus Motor Relearning Programme To Enhance Upper Limb Motor Function in Stroke Patients: A Quasi Experimental StudyInternational Journal of Innovative Science and Research TechnologyNessuna valutazione finora
- Case Study On CVADocumento19 pagineCase Study On CVAmolukas10190% (42)
- Stroke Case StudyDocumento2 pagineStroke Case StudyayeshasadiqamukhtarNessuna valutazione finora
- Prepared By: Floriza P. de Leon, PTRPDocumento10 paginePrepared By: Floriza P. de Leon, PTRPFloriza de Leon100% (1)
- Stroke School Brockville Part 3Documento39 pagineStroke School Brockville Part 3Gautam KhannaNessuna valutazione finora
- The Blood Pressure Solution Ebook 022318Documento14 pagineThe Blood Pressure Solution Ebook 022318Rolando M Tabora100% (2)
- CNS NotesDocumento103 pagineCNS NotesrileyNessuna valutazione finora
- Therapy ManualDocumento52 pagineTherapy ManualcrisNessuna valutazione finora
- "Black Man in A White Coat" IntroductionDocumento8 pagine"Black Man in A White Coat" Introductionwamu8850% (1)
- 2012 Mirror Therapy For Improving Motor Function After StrokeDocumento68 pagine2012 Mirror Therapy For Improving Motor Function After StrokeMarcelo Ortiz Valenzuela100% (1)
- Positioning Patients Cheat SheetDocumento7 paginePositioning Patients Cheat SheetUchi Nurul FauziahNessuna valutazione finora
- Jurnal Kedokteran Dan Kesehatan Indonesia: Risk Factors of Stroke Survivors' Quality of LifeDocumento7 pagineJurnal Kedokteran Dan Kesehatan Indonesia: Risk Factors of Stroke Survivors' Quality of LifeEster YunitaNessuna valutazione finora
- Diagnosis of Vascular Cognitive ImpairmentDocumento17 pagineDiagnosis of Vascular Cognitive ImpairmentInes Strenja LinićNessuna valutazione finora
- Academic Recruitment BrochureDocumento9 pagineAcademic Recruitment BrochureGlenden KhewNessuna valutazione finora
- 1228 HFStroke Altered Neuro 2011Documento74 pagine1228 HFStroke Altered Neuro 2011Cyndy EnterlineNessuna valutazione finora
- Evolution Healing Centre - Lived Experiences of Stroke For Bermuda 2022Documento22 pagineEvolution Healing Centre - Lived Experiences of Stroke For Bermuda 2022BernewsAdminNessuna valutazione finora
- Hemiplegia Resource Book ModifiedDocumento60 pagineHemiplegia Resource Book ModifiedAnonymous czrvb3hNessuna valutazione finora
- Berlin 2014 Vorontsov PDFDocumento53 pagineBerlin 2014 Vorontsov PDFNeagu AndreiNessuna valutazione finora
- Ie CvaDocumento12 pagineIe CvaSteve ColbertNessuna valutazione finora
- Neuro Post TestDocumento6 pagineNeuro Post Testmarlon armamentoNessuna valutazione finora
- Constraint Induced Manual TherapyDocumento165 pagineConstraint Induced Manual TherapyPrabhu Chinna Gounder100% (1)
- CCT - MeaningDocumento10 pagineCCT - Meaningmandeep axonNessuna valutazione finora
- OxfordMedicineLIVETitleList FEB 2018 Batch1Documento288 pagineOxfordMedicineLIVETitleList FEB 2018 Batch1Albert E KastratiNessuna valutazione finora
- 2021 AHA ASA Guideline For The Prevention of Stroke in Patients With Stroke and TIA Clinical UpdateDocumento43 pagine2021 AHA ASA Guideline For The Prevention of Stroke in Patients With Stroke and TIA Clinical Updatejulioel1nico20100% (1)