Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Worksheets On The Following Aspects of A Quality Improvement Project
Caricato da
Anonymous FgT04krgymTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Worksheets On The Following Aspects of A Quality Improvement Project
Caricato da
Anonymous FgT04krgymCopyright:
Formati disponibili
School of Nursing
Saint Louis University
Worksheets on the following aspects of a quality improvement project:
Worksheet A Identifying Areas for Improvement
Worksheet B Forming a Team
Worksheet C Team Meeting Notes
Worksheet D Goal Setting
Worksheet E Current Process Analysis
Worksheet F Root-cause Analysis
Worksheet G Fishbone Diagram
Worksheet H Process Improvement Plan
Worksheet I Implementation Strategy
Worksheet J Pilot-Testing
Worksheet K Pilot-Test Evaluation
Worksheet L Ongoing Monitoring
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing Saint
Louis University
WORKSHEET A:
Identifying Areas for Improvement
1. Select one question, issue, or perceived problem to examine further. (You may use the
institutions checklist, policy or manual of operating procedures if applicable)
Example1: Does the institution routinely ask all patients upon admission/readmission if they have pain?
Example 2: Is nursing intervention X effective in reducing falls in confused patients ?
Example 3: What information do patients watchers need to know to increase compliance in following
hospital visiting hours?
Example 4: Why dont ICU nurses regularly check IV sites at the start of shift?
Question: What are factors affecting communication between nurse and patient?
Randomly select five (or more) records (or other data sources, depending on the question) to review.
Determine a question that will be asked:
Example1: Was this patient asked about their pain upon admission/readmission? Where in chart
X was pain asked to Patient A?
Example2: Did the staff nurse perform nursing intervention X in patient Y?
Example 3: Is information X explained during admission? Who should communicate information
X to patients watchers on admission?
Example 4: Does the chart tell how many times were IV sites regularly checked?
How long were call lights answered within X minutes?
Question:____________________________________________________________
____________________________________________________________________
2. Collect data:
Data can help you separate what you think is happening from what is really happening.
Data will establish a baseline so you can measure improvement.
Data will help you avoid putting solutions in place that will not solve the problem.
Record findings here:
Case # Yes No
1
2
3
4
5
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing Saint
Louis University
WORKSHEET B:
3. If data is not readily available from medical records, what sources did you use to collect your
data, and what at steps did you take to collect this data?
______________________________________________________________________________
____ _____________________________________________________________________
_____________________________________________________________________
Forming a Team
A team is identified as a small number of people with complimentary skills that are committed
to a common purpose and hold themselves mutually accountable.
A. Identify team members who will work on this project
a. Teams should have 3-4 members that will plan, implement, and evaluate their work.
b. If you already have a team, make sure that they include appropriate members related to
the topic chosen for improvement.
c. Involve staff from different shifts, units and departments.
Name Position Alternates:
B. Identify time and place for short weekly meetings (no more than 30 minutes)
a. Team does not have to meet at same time and place each week.
b. Meetings can be more or less frequent as needed. Post meeting schedule in a place
accessible to all team members, where appropriate:
Meeting # Date Time Place
Team Meeting Notes
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing Saint
Louis University
WORKSHEET C:
Team Meeting Notes Team
Members:
Team Start Date:
Team Goal: ______
Date Main points of discussion Next step Person responsible Due by:
Goal Setting
A goal is a clear statement of the intended improvement and how it is to be measured.
Use your goal statement to stay focused, to establish boundaries for what is and is not included
in your teams work.
Post your goal where it is visible at every team meeting (or recite this before start of meeting)
Write a goal for improvement:
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing Saint
Louis University
WORKSHEET D:
Your goal should:
o Answer the question, What do you want to accomplish? o Be measurable.
o Be short so that everyone can remember it.
Does not include how you will achieve goal.
o May include a beginning and end date.
o Your goal may be taken directly from an item on the institutions checklists. Example:
Increase number of care plans that provide for medication on a regular schedule (e.g.,
around the clock), not just PRN, (for patients with daily pain) from 50% to 75% over the
next two months.
STATE YOUR GOAL/AIM:
Current Process Analysis
A process is a series of activities or steps that is meant to achieve a particular result.
When defining a process, think about staff roles in the process, the tools or materials staff use,
and the flow of activities.
Everything is a process, whether it is admitting a patient, serving meals, assessing pain, or
managing a nursing unit. The ultimate goal of defining a process is identifying problems in the
current process.
Have the team identify and define every step in the current process that the facility has chosen to
improve:
Tips:
Take time to brainstorm and listen to every team member.
The process must be understood and documented.
Make each step in process very specific.
Use one post-it note, index card, or scrap piece of paper for each step in the process.
Lay out each step, move steps, add and remove steps until team agrees on final process.
If the problem is that a process does not exist (for example, there is no current process to
screen for pain upon admission and readmission), then identify the related processes
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing Saint
Louis University
WORKSHEET E:
(for example, the process for admission and readmission.)
If process is different for different shifts, identify each individual process.
Example: Process for making buttered toast
Step Process
1 Check to see if there is bread, butter, knife, and toaster.
2 If supplies are missing, go to the store and purchase them.
3 Check to see if the toaster is plugged in if not, plug in the toaster.
4 Check setting on toaster adjust to darker or lighter as preferred.
5 Put a slice of bread in toaster.
6 Turn toaster on.
7 Wait for bread to toast.
8 When toast is ready, remove from toaster and put on plate.
9 Use knife to cut pat of butter.
10 Use knife to spread butter on toast.
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Current Process Analysis
Team discussion
Evaluate your current process as you define it:
1. What policies and procedures do we have in place for this process?
2. What forms do we use?
3. How does our physical environment support or hinder this process?
4. What/Who are the staff involved in this process?
5. What part of this process does not work?
6. Do we duplicate any work unnecessarily?
7. Are there any delays in the process? Why?
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Continue asking questions that are important in learning more about this process.
When you discover a problem in your current process, continue to Worksheet F: Root-Cause
Analysis, to determine the root cause(s) of the problem.
WORKSHEET F:
Root-Cause Analysis
The root cause analysis allows you to identify the root of the problem you discover in
your process - where and why the problem exists.
You can then make decisions based on data rather than hunches, and look for lasting
solutions rather than relying on quick fixes and band-aid approaches.
1. Begin with brainstorming:
a. All factors of the problem are considered. We dont assess for pain because
b. Once all factors are listed and developed, they should be categorized.
c. Then you can create a cause and effect diagram, such as a Fishbone Diagram
(explained below).
d. General categories for causes are: Environment, Equipment, People, Methods
(Processes) and Materials.
2. The Fishbone Diagram
a. The cause and effect diagram (Fishbone) starts with the problem at the head of the fish.
b. Under each general category of the Fishbone, answer the question, why? in regards to
the problem identified.
c. Once the Fishbone Diagram is completed, the various causes are discussed to determine
the root of the problem or the real reasons why the problem exists. It is from the
result of this discussion that the focus for the improvement plan begins.
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
WORKSHEET G:
Fishbone Diagram
Goal:
_____________________________________________________________________________________
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Worksheet H:
Process Improvement Plan
Identify a manageable change based on the outcome of root-cause analysis. What will we do/change to
address the root of the problem?
1. Identify criteria that will help evaluate potential solutions to the problem, such as:
Cost
Potential facility/resident/staff benefits
How easy it would be to implement
2. Brainstorm all potential solutions before rejecting any ideas.
Use this space for brainstorming
3. Evaluate a few solutions listed above. Dont be afraid to combine ideas. Come to a team
consensus on the best solution to test.
Consensus means that each team member can live with the solution.
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Worksheet I:
4. Write consensus decision on one process change or improvement to make:
_____________________________________________________________
_____________________________________________________________
_____________________________________________________________
Implementation Strategy
Identifies how we will accomplish change.
Planning will help coordinate the activity of the team.
The implementation strategy includes how the change will be communicated, implemented, and
evaluated.
1. Create an implementation strategy that incorporates the following questions:
a. What is the change?
b. Why has the team suggested this change? What is the goal?
c. Who will be involved in the change? Are there other staff members who may be
affected by this change?
d. Where will the change take place? Remember to start small.
e. When will the change be made (start date)?
f. When will it be evaluated (evaluation date)?
g. How will it be evaluated how will we know if we can expand this change to other
areas?
2. Implementation Strategy:
______________________________________________________________________
______________________________________________________________________
______________________________________________________________________
______________________________________________________________________
______________________________________________________________________
______________________________________________________________________
______________________________________________________________________
______________________________________________________________________
______________________________________________________________________
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Worksheet J:
Communication is the key! Share the answers to the above questions with the staff who will be
involved in making the change. Talk about the change positively. Ask for feedback on how to
implement the proposed change.
Pilot Testing
Pilot testing gives your team a chance to see how to implement a change on a small-scale.
Pilot testing can also give your team some early results, to see if the change you make has any
impact.
The team has a role to play in helping to implement any change that is recommended.
What can the team do to make the change happen?
Who
Who will train staff? ________________
Who will update/revise/remove tool, if necessary? ________________
Who will monitor to see if process has changed? ________________
Who will team contact if they need support implementing change? ________________
Who will audit outcome of process change? ________________
Additional team roles:
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Worksheet K:
Indicate here any revisions to the implementation strategy that the team makes during the pilot-test:
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Worksheet K:
Pilot Test Evaluation Worksheet
Evaluating the pilot test allows your team to organize observations that the team has made
through the pilot test.
Evaluation also includes collecting data to check whether the change has helped you reach your
goal.
Ask these evaluation questions at a team meeting, a staff meeting, in an anonymous questionnaire, or
via informal communication with staff.
1. Do we need to reevaluate our initial goal?
2. What is working well? Why?
3. What is not working? Why?
4. What can be done differently?
5. Do we need to revise the materials we are using (if any)?
6. How does staff feel about the change in process?
7. Are residents positively affected by the change in process?
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Pilot Test Evaluation Worksheet
Collect data to evaluate change.
Has the change (in process, in form, etc.) had an impact? The chosen measure for evaluation can be
taken directly from an item on the Hospital Checklist, Manual, Procedure, Policy (if applicable) used to
begin this project.
Example: 5 out of 5 new admissions have completed assessment forms within 24 hours Example: 5 out of
5 call lights received response within X minutes.
Goal: __________________________________________________________________
_______________________________________________________________________
Data source (medical records, staff survey, etc.): _____________________________
Example:
Date Chosen measure for evaluation (i.e., # of cases # of cases with B out of A
assessment for new admission is reviewed positive results (B/A)
completed within 24 hours. See (A) (B)
Hospital Checklists for possible
measures.)
Continue data collection as often as desired during the pilot test.
Results
Dates of pilot test: _______________________________
Did team reach its goal? Yes No
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
Does the team need to revise the process or make changes? Yes No If
yes, what changes? Repeat the pilot-test if necessary.
If no, continue to Worksheet I to design implementation strategy facility-wide. Use Worksheet L
to monitor improvement once a change to the process has been implemented.
Worksheet L:
Ongoing Monitoring
Monitoring the implemented change allows your team to evaluate, on an ongoing basis,
whether or not the implemented change has made an impact on overall care delivery.
Decide who on staff will perform tracking related to the facility-wide implementation.
Decide when this monitoring will be completed (i.e. monthly, bimonthly, quarterly).
Decide on how this data will be collected and evaluated.
Goal:___________________________________________________________________
Ex.: Pain assessments will be completed on all residents within 24 hours after admission.
Date of facility-wide implementation_______________
How will you know if you have achieved implementation?
Ex.: We will know when 10 out of 10 admissions/readmissions this month show that a pain
assessment was completed upon admission/readmission. We will know when __________________
Record findings:
Date # of cases reviewed (A) # of cases with positive B out of A (B/A)
results (B)
Review the following:
1. Based on the data collected, check to see if the process has been implemented 100%. If it has,
continue to monitor as long as the team feels necessary.
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
School of Nursing
Saint Louis University
2. Based on the data collected, check to see if implementation of the new (improved) process has
had an impact on the delivery of care. If it has not, you may wish to explore the following
questions:
a. Has the process been successful on some shifts or units, and not on others? If so, why?
b. Is further staff education needed? In what areas?
c. Does the process need to be revised for facility-wide implementation? If so, plan a pilot
test of some revision to the process. Use these worksheets to plan the pilot test if
necessary.
Engelbert C. Manuel, RN, MM-IR/ Quality Improvement Worksheets/ 1st sem/2016/v.1
Potrebbero piacerti anche
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- Pdsa 1&2Documento10 paginePdsa 1&2Anonymous FgT04krgymNessuna valutazione finora
- Nurses Use of Time PDFDocumento9 pagineNurses Use of Time PDFAnonymous FgT04krgymNessuna valutazione finora
- Australasian Emergency Nursing Journal: Kelli Innes, Debra Jackson, Virginia Plummer, Doug ElliottDocumento6 pagineAustralasian Emergency Nursing Journal: Kelli Innes, Debra Jackson, Virginia Plummer, Doug ElliottAnonymous FgT04krgymNessuna valutazione finora
- Australasian Emergency Nursing Journal: Kelli Innes, Debra Jackson, Virginia Plummer, Doug ElliottDocumento6 pagineAustralasian Emergency Nursing Journal: Kelli Innes, Debra Jackson, Virginia Plummer, Doug ElliottAnonymous FgT04krgymNessuna valutazione finora
- AJOT HildebrandDocumento10 pagineAJOT HildebrandAnonymous FgT04krgymNessuna valutazione finora
- Australasian Emergency Nursing Journal: Kelli Innes, Debra Jackson, Virginia Plummer, Doug ElliottDocumento6 pagineAustralasian Emergency Nursing Journal: Kelli Innes, Debra Jackson, Virginia Plummer, Doug ElliottAnonymous FgT04krgymNessuna valutazione finora
- Dyosaaaaaaaaa ExaaaamDocumento13 pagineDyosaaaaaaaaa ExaaaamAnonymous FgT04krgymNessuna valutazione finora
- Laboratory Results CasepresDocumento1 paginaLaboratory Results CasepresAnonymous FgT04krgymNessuna valutazione finora
- Objectiv ES Rationa LE: Evaluatio NDocumento3 pagineObjectiv ES Rationa LE: Evaluatio NAnonymous FgT04krgym100% (1)
- Factors Associated With Triage Assignment of Patients Ultimately Diagnosed With Myocardial Infarction 1Documento5 pagineFactors Associated With Triage Assignment of Patients Ultimately Diagnosed With Myocardial Infarction 1Anonymous FgT04krgymNessuna valutazione finora
- Role of District and CommunityDocumento8 pagineRole of District and CommunityAnonymous FgT04krgymNessuna valutazione finora
- The Effect of Access To Contraceptive Services On Injectable Use and Demand For Family Planning in MalawiDocumento12 pagineThe Effect of Access To Contraceptive Services On Injectable Use and Demand For Family Planning in MalawiAnonymous FgT04krgymNessuna valutazione finora
- DOH Health Record TemplateDocumento2 pagineDOH Health Record TemplateAnonymous FgT04krgymNessuna valutazione finora
- Your BibliographyDocumento1 paginaYour BibliographyAnonymous FgT04krgymNessuna valutazione finora
- Sagles, Maria Robelle Anne Pearl M. November 9, 2016 BSN Iv-C1Documento9 pagineSagles, Maria Robelle Anne Pearl M. November 9, 2016 BSN Iv-C1Anonymous FgT04krgymNessuna valutazione finora
- Meta-Analysis of Pain and Stress in Emergency Department PatientsDocumento6 pagineMeta-Analysis of Pain and Stress in Emergency Department PatientsAnonymous FgT04krgymNessuna valutazione finora
- Nurse PT Communication PDFDocumento9 pagineNurse PT Communication PDFAnonymous FgT04krgymNessuna valutazione finora
- Nurses Use of TimeDocumento9 pagineNurses Use of TimeAnonymous FgT04krgymNessuna valutazione finora
- HCAHPS V9.0 Appendix A - Mail Survey Materials (English) March 2014 PDFDocumento18 pagineHCAHPS V9.0 Appendix A - Mail Survey Materials (English) March 2014 PDFAnonymous FgT04krgymNessuna valutazione finora
- Surgery Journ PDFDocumento10 pagineSurgery Journ PDFAnonymous FgT04krgymNessuna valutazione finora
- Meds Coro Ward 2017Documento8 pagineMeds Coro Ward 2017Anonymous FgT04krgymNessuna valutazione finora
- Er JournalDocumento5 pagineEr JournalAnonymous FgT04krgymNessuna valutazione finora
- ER DrugsDocumento22 pagineER DrugsAnonymous FgT04krgymNessuna valutazione finora
- Cardiac MedsDocumento4 pagineCardiac MedsAnonymous FgT04krgymNessuna valutazione finora
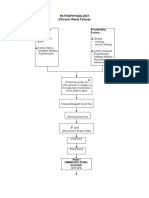
- Pathophysiology (Chronic Renal Failure)Documento3 paginePathophysiology (Chronic Renal Failure)marshmalou86% (7)
- SorryDocumento2 pagineSorryJohann CarrascoNessuna valutazione finora
- CorooDocumento1 paginaCorooAnonymous FgT04krgymNessuna valutazione finora
- NCP Impaired Urinary Elimination CRFDocumento2 pagineNCP Impaired Urinary Elimination CRFAnonymous FgT04krgymNessuna valutazione finora
- Drug StudyDocumento5 pagineDrug StudyAnonymous FgT04krgymNessuna valutazione finora
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Mext Gsaps 2021.09 Ma Applicationguide EngDocumento34 pagineMext Gsaps 2021.09 Ma Applicationguide EngabidafifaNessuna valutazione finora
- Louis Braille Lesson Plan Nancy Romero From Day 1-8Documento20 pagineLouis Braille Lesson Plan Nancy Romero From Day 1-8api-337275999Nessuna valutazione finora
- Faci ModuleDocumento158 pagineFaci ModuleRizza Manabat PacheoNessuna valutazione finora
- General Mathematics: Quarter 2 - Module 3: Solving Problems Involving Simple and Compound InterestDocumento34 pagineGeneral Mathematics: Quarter 2 - Module 3: Solving Problems Involving Simple and Compound InterestLovely Joy Valdez50% (2)
- Aspillaga, Kayechel Mae P. (EDUC 106)Documento3 pagineAspillaga, Kayechel Mae P. (EDUC 106)Kayechel Mae AspillagaNessuna valutazione finora
- Leadership TheoriesDocumento24 pagineLeadership TheoriesNorazela HamadanNessuna valutazione finora
- Running Head: CASE STUDY 1Documento16 pagineRunning Head: CASE STUDY 1api-401897362100% (1)
- A1 Writing Assessment 6 Deciding On What To Write About PDFDocumento3 pagineA1 Writing Assessment 6 Deciding On What To Write About PDFAndrea JimenezNessuna valutazione finora
- Biographical DataDocumento3 pagineBiographical DataAko Si Vern ÖNessuna valutazione finora
- English: ObjectivesDocumento6 pagineEnglish: ObjectivesJessi HerediaNessuna valutazione finora
- Isabelle Stengers and The Dramatization of PhilosophyDocumento154 pagineIsabelle Stengers and The Dramatization of Philosophybethânia ZanattaNessuna valutazione finora
- KDP Mentor Training Course SummaryDocumento2 pagineKDP Mentor Training Course SummaryJohnNessuna valutazione finora
- The Norton Anthology of British Literature, Vol. C (9: Krummell@calpoly - EduDocumento4 pagineThe Norton Anthology of British Literature, Vol. C (9: Krummell@calpoly - Eduapi-327282816Nessuna valutazione finora
- Importance of EnglishDocumento1 paginaImportance of EnglishsushilmohantyNessuna valutazione finora
- Memoriam Nabia AbbottDocumento3 pagineMemoriam Nabia AbbottHanif EL-AinNessuna valutazione finora
- DLL - English 5 - Q3 - W1Documento7 pagineDLL - English 5 - Q3 - W1Jayson PamintuanNessuna valutazione finora
- Arkeologi Islam NusantaraDocumento4 pagineArkeologi Islam NusantaraMuhammad Ma'ruf AsyhariNessuna valutazione finora
- The Islamia University of Bahawalpur: Part-IDocumento27 pagineThe Islamia University of Bahawalpur: Part-IubillNessuna valutazione finora
- NDSW TrustDocumento5 pagineNDSW Trustndsw trustNessuna valutazione finora
- Nursing Final DraftDocumento2 pagineNursing Final Draftapi-272895943Nessuna valutazione finora
- Daily Lesson Log Template SampleDocumento5 pagineDaily Lesson Log Template SampleNonie Beth CervantesNessuna valutazione finora
- 1 Epoka University FEAS Thesis Guide Line Ed A 13 December v1-SODocumento14 pagine1 Epoka University FEAS Thesis Guide Line Ed A 13 December v1-SORiada JadaNessuna valutazione finora
- Nikki Chwatt ResumeDocumento1 paginaNikki Chwatt ResumeNikki ChwattNessuna valutazione finora
- Weekly Learning Plan (WLP) : Department of Education Division of Rizal San Isidro Senior High SchoolDocumento8 pagineWeekly Learning Plan (WLP) : Department of Education Division of Rizal San Isidro Senior High SchoolJohnMar TomNessuna valutazione finora
- Allotment of SeatsCAPR-I - EN6141 For Rajarshi Shahu.Documento36 pagineAllotment of SeatsCAPR-I - EN6141 For Rajarshi Shahu.mohammed ameenNessuna valutazione finora
- Final ProjectDocumento32 pagineFinal Projectapi-340985028Nessuna valutazione finora
- Walter's Resume (Powerpoint Version)Documento12 pagineWalter's Resume (Powerpoint Version)Walter SteppNessuna valutazione finora
- Plato - An Ancient Philosopher-1 PDFDocumento21 paginePlato - An Ancient Philosopher-1 PDFAli ZohaibNessuna valutazione finora
- Kenya Registered NgosDocumento604 pagineKenya Registered NgosfoundationsNessuna valutazione finora
- Haycroft - Pillars of Pronunciation (IH2010)Documento6 pagineHaycroft - Pillars of Pronunciation (IH2010)Karolina CiNessuna valutazione finora