Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Robbin and Cotran Pathologic Basis of Disease: Jesly Charlies
Caricato da
Jesly CharliesTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Robbin and Cotran Pathologic Basis of Disease: Jesly Charlies
Caricato da
Jesly CharliesCopyright:
Formati disponibili
ROBBIN AND COTRAN PATHOLOGIC BASIS OF DISEASE Jesly Charlies
BACTERIAL, PARASITIC, AND HELMINTHIC INFECTIONS
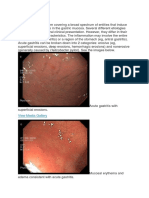
Extrahepatic bacterial infections, particularly sepsis, can induce mild hepatic inflammation and varying degrees of hepatocellular
cholestasis. The latter effect is attributable to the effects of pro-inflammatory cytokines released by Kupffer cells and endothelial cells,
in response to circulating endotoxin. Several bacteria can infect the liver directly, including Staphylococcus aureus in the setting of
toxic shock syndrome, Salmonella typhi in the setting of typhoid fever, and T. pallidum in secondary or tertiary syphilis. Alternatively,
bacteria may proliferate in a biliary tree especially when outflow is compromised by partial or complete obstruction. The intra-biliary
bacterial composition reflects the gut flora, and the severe acute inflammatory response within the intrahepatic biliary tree is called
ascending cholangitis.
Parasitic and helminthic infections are major causes of morbidity worldwide, and the liver is frequently involved ( Chapter 8 ). These
diseases include malaria, schistosomiasis, strongyloidiasis, cryptosporidiosis, leishmaniasis, echinococcosis, and infections by the
liver flukes Fasciola hepatica and Clonorchis sinensis.
Liver abscesses, a form of liver infection that is common in developing countries, deserve special mention. They are usually caused by
echinococcal and amebic infections ( Chapter 8 ), and less commonly, by other protozoal and helminthic organisms. In developed
countries liver abscesses are uncommon; the incidence of amebic infections is low and is usually present in immigrants from endemic
regions. Most such abscesses are pyogenic, representing a complication of a bacterial infection elsewhere. The organisms reach the
liver by (1) the portal vein, (2) arterial supply, (3) ascending infection in the biliary tract (ascending cholangitis), (4) direct invasion of
the liver from a nearby source, or (5) a penetrating injury. The majority of hepatic abscesses used to result from portal spread of intra-
abdominal infections (e.g., appendicitis, diverticulitis, colitis). With improved management of these conditions, spread now occurs
primarily through the biliary tree or the arterial supply in patients suffering from some form of immune deficiency (e.g., old age with
debilitating disease, immunosuppression, or cancer chemotherapy with marrow failure). In these settings, abscesses may develop
without a primary focus elsewhere.
Liver abscesses are associated with fever and, in many instances, right upper quadrant pain and tender hepatomegaly. Jaundice may
result from extrahepatic biliary obstruction. Although antibiotic therapy may control smaller lesions, surgical drainage is often
necessary for the larger lesions. Because diagnosis is frequently delayed since the patients are elderly and have serious coexistent
disease, the mortality rate of patients with large liver abscesses ranges from 30% to 90%. With early recognition and management as
many as 80% of patients can survive. In the case of echinococcal cysts, rupture of this cyst has severe clinical consequences, including
systemic spread of the organism and resultant shock from massive immune response.
Potrebbero piacerti anche
- Gastritis Symptoms, Causes and TreatmentDocumento22 pagineGastritis Symptoms, Causes and TreatmentBîndar CristianNessuna valutazione finora
- Stomach - GastritisDocumento22 pagineStomach - GastritisaimanNessuna valutazione finora
- Peritonitis Clinical UpdateDocumento11 paginePeritonitis Clinical Updatetika tikaNessuna valutazione finora
- Acute Gastritis - Emedicine - 12 Jan 2011Documento8 pagineAcute Gastritis - Emedicine - 12 Jan 2011Melissa KanggrianiNessuna valutazione finora
- A. Overview: I. Intestinal ParasitismDocumento3 pagineA. Overview: I. Intestinal ParasitismSienaNessuna valutazione finora
- Salmonella Infections in Immunocompromised Adults: Melita A. GordonDocumento10 pagineSalmonella Infections in Immunocompromised Adults: Melita A. GordonStefani AtlleNessuna valutazione finora
- Urinary Tract Infection and QuinolonesDocumento49 pagineUrinary Tract Infection and QuinolonesKhanzada ShahzebNessuna valutazione finora
- Escherichia, Klebsiella, Enterobacter, Serratia, Citrobacter, and Proteus: Pathogens and InfectionsDocumento20 pagineEscherichia, Klebsiella, Enterobacter, Serratia, Citrobacter, and Proteus: Pathogens and Infectionsdrpranaykumar5529Nessuna valutazione finora
- PeritonitissDocumento46 paginePeritonitissNinaNessuna valutazione finora
- Liver Abscess: Key PointsDocumento5 pagineLiver Abscess: Key PointsVanadia Nurul MetaNessuna valutazione finora
- Systemic Infections From GiDocumento10 pagineSystemic Infections From GiJake MillerNessuna valutazione finora
- Pa Tho Physiology of Infection DiarrheaDocumento5 paginePa Tho Physiology of Infection DiarrheamisheyableNessuna valutazione finora
- Liver Abscess Causes and SymptomsDocumento6 pagineLiver Abscess Causes and SymptomsKenneth SunicoNessuna valutazione finora
- Pathophysiology of GastritisDocumento2 paginePathophysiology of GastritisFlorsean Mae Sala80% (5)
- Mechanisms of Helminth DiseasesDocumento8 pagineMechanisms of Helminth DiseasesRaihan Zulfiqar HalimNessuna valutazione finora
- Chronic and Acute Infection of TheDocumento6 pagineChronic and Acute Infection of Thecarlos.alberto.palacios.serratNessuna valutazione finora
- S Typhi Has Been A Major Human Pathogen For Thousands of Years, Thriving in Conditions of PoorDocumento11 pagineS Typhi Has Been A Major Human Pathogen For Thousands of Years, Thriving in Conditions of PoorGio Vano NaihonamNessuna valutazione finora
- Microbial TaxonomyDocumento20 pagineMicrobial TaxonomyAfaq AhmadNessuna valutazione finora
- Background TyphoidDocumento21 pagineBackground TyphoidNurmala Rahman LNessuna valutazione finora
- Pathophysiology, Clinical Manifestation and Diagnosis of PeritonitisDocumento6 paginePathophysiology, Clinical Manifestation and Diagnosis of PeritonitisIOSRjournalNessuna valutazione finora
- Background: View Media GalleryDocumento6 pagineBackground: View Media Galleryprayitno tabraniNessuna valutazione finora
- Enteric Gram-Negative Rods (Enterobacteriaceae) : Prepared by Assistant Professor Dr. Khawaja Shakeel AhmedDocumento26 pagineEnteric Gram-Negative Rods (Enterobacteriaceae) : Prepared by Assistant Professor Dr. Khawaja Shakeel AhmedZheemo ArshavinNessuna valutazione finora
- Fever, Jaundice and Hepatitis: It Is Not Always A Viral InfectionDocumento7 pagineFever, Jaundice and Hepatitis: It Is Not Always A Viral Infectionshaznay delacruzNessuna valutazione finora
- Matas 2020Documento9 pagineMatas 2020Aubrey PerezNessuna valutazione finora
- Typhoid Fever - StatPearls - NCBI BookshelfDocumento13 pagineTyphoid Fever - StatPearls - NCBI Bookshelfhasnah shintaNessuna valutazione finora
- Infections of the Urinary Tract (UTIsDocumento4 pagineInfections of the Urinary Tract (UTIsfifa nasrul ummahNessuna valutazione finora
- UntitledDocumento15 pagineUntitledDagmawi BahiruNessuna valutazione finora
- Diseases of Liver: FocalDocumento7 pagineDiseases of Liver: FocalIsak ShatikaNessuna valutazione finora
- Parasitic Infections of the Kidney & Urinary TractDocumento39 pagineParasitic Infections of the Kidney & Urinary TractDaud ParluhutanNessuna valutazione finora
- Disentri AmoebaDocumento11 pagineDisentri AmoebaFranklin L. Sinanu100% (1)
- Thyfoid Fever: A Diagnostic ChallengeDocumento36 pagineThyfoid Fever: A Diagnostic ChallengeYogie DjNessuna valutazione finora
- PeritonitisDocumento5 paginePeritonitisdnllkzaNessuna valutazione finora
- Chap01 PDFDocumento3 pagineChap01 PDFaldiansyahraufNessuna valutazione finora
- PeritonitisDocumento36 paginePeritonitisbrnardNessuna valutazione finora
- Intra AbdominalDocumento20 pagineIntra Abdominalbest batiNessuna valutazione finora
- Yersinia Enterocolitica Infection GuideDocumento19 pagineYersinia Enterocolitica Infection GuideLaura Anghel-MocanuNessuna valutazione finora
- Food Poisoning A 2013 Comprehensive Review Articles Articles Medical Toxicology Expert Witness Forensic Toxicology - DRDocumento1 paginaFood Poisoning A 2013 Comprehensive Review Articles Articles Medical Toxicology Expert Witness Forensic Toxicology - DRBahirahNessuna valutazione finora
- Typhoid FeverDocumento14 pagineTyphoid FeverJames Cojab SacalNessuna valutazione finora
- Typhoid DiseaseDocumento28 pagineTyphoid DiseaseSaba Parvin Haque100% (1)
- Chapter 47 - Infective Syndromes of Hepatobiliary SystemDocumento37 pagineChapter 47 - Infective Syndromes of Hepatobiliary SystemKevil LoriyaNessuna valutazione finora
- Gastritis Definition: Gastritis Can Be An Acute orDocumento46 pagineGastritis Definition: Gastritis Can Be An Acute orOdey BeekNessuna valutazione finora
- Primary PeritonitisDocumento6 paginePrimary Peritonitisdietho666Nessuna valutazione finora
- Typhoid FeverDocumento13 pagineTyphoid FeverFajar NarakusumaNessuna valutazione finora
- TB Case HistoryDocumento4 pagineTB Case HistoryMarisa PetersonNessuna valutazione finora
- Gastrointestinal Tract Changes in HIV PathogenesisDocumento4 pagineGastrointestinal Tract Changes in HIV PathogenesisnikkennnNessuna valutazione finora
- E. Coli InfectionsDocumento18 pagineE. Coli InfectionsLaura Anghel-MocanuNessuna valutazione finora
- CURS ENGLEZA Boli InfectioaseDocumento246 pagineCURS ENGLEZA Boli InfectioaseKiran LetrangeNessuna valutazione finora
- Intestinal Infections: Overview: Table 1Documento14 pagineIntestinal Infections: Overview: Table 1HokeNessuna valutazione finora
- Manejo en Colangitis Aguda - Libro XDocumento4 pagineManejo en Colangitis Aguda - Libro XRodrigo MartinezNessuna valutazione finora
- Salmonellosis: Enterica Serovar Typhi) - Less Commonly It Caused by Salmonella Paratyphi (A, BDocumento5 pagineSalmonellosis: Enterica Serovar Typhi) - Less Commonly It Caused by Salmonella Paratyphi (A, BmarcusNessuna valutazione finora
- Typhoid Fever PDFDocumento14 pagineTyphoid Fever PDFginstarNessuna valutazione finora
- Microbiology 2Documento4 pagineMicrobiology 2Michael Delage Jr.Nessuna valutazione finora
- Project 101Documento70 pagineProject 101Joanne Bernadette AguilarNessuna valutazione finora
- Female Urinary Tract Infections in Clinical PracticeDa EverandFemale Urinary Tract Infections in Clinical PracticeBob YangNessuna valutazione finora
- Contagious Diseases: The Science, History, and Future of Epidemics. From Ancient Plagues to Modern Pandemics, How to Stay Ahead of a Global Health CrisisDa EverandContagious Diseases: The Science, History, and Future of Epidemics. From Ancient Plagues to Modern Pandemics, How to Stay Ahead of a Global Health CrisisNessuna valutazione finora
- Manual of First Aid Professional English: Part 2Da EverandManual of First Aid Professional English: Part 2Nessuna valutazione finora
- Viral Vistas: Insights into Infectious Diseases: The Invisible War: Decoding the Game of Hide and Seek with PathogensDa EverandViral Vistas: Insights into Infectious Diseases: The Invisible War: Decoding the Game of Hide and Seek with PathogensNessuna valutazione finora
- Cats and Toxoplasma: A Comprehensive Guide to Feline ToxoplasmosisDa EverandCats and Toxoplasma: A Comprehensive Guide to Feline ToxoplasmosisNessuna valutazione finora
- The Big Book of Infectious Disease Trivia: Everything You Ever Wanted to Know about the World's Worst Pandemics, Epidemics and DiseasesDa EverandThe Big Book of Infectious Disease Trivia: Everything You Ever Wanted to Know about the World's Worst Pandemics, Epidemics and DiseasesNessuna valutazione finora
- NAFLD HarrisonDocumento2 pagineNAFLD HarrisonJesly CharliesNessuna valutazione finora
- Anat GMBRDocumento3 pagineAnat GMBRJesly CharliesNessuna valutazione finora
- HEPATITIS RobbinDocumento4 pagineHEPATITIS RobbinJesly CharliesNessuna valutazione finora
- NAFLD HarrisonDocumento2 pagineNAFLD HarrisonJesly CharliesNessuna valutazione finora
- Amebiasis HarrisonDocumento5 pagineAmebiasis HarrisonJesly CharliesNessuna valutazione finora
- Nelson JaundiceDocumento7 pagineNelson JaundiceJesly CharliesNessuna valutazione finora
- HCC HarrisonDocumento5 pagineHCC HarrisonJesly CharliesNessuna valutazione finora
- Nelson JaundiceDocumento7 pagineNelson JaundiceJesly CharliesNessuna valutazione finora
- Hepatitis RobbinDocumento4 pagineHepatitis RobbinJesly CharliesNessuna valutazione finora
- Liver Abscesses HarrisonDocumento2 pagineLiver Abscesses HarrisonJesly CharliesNessuna valutazione finora
- The Gallbladder and Extrahepatic Bile Ducts RubinDocumento4 pagineThe Gallbladder and Extrahepatic Bile Ducts RubinJesly CharliesNessuna valutazione finora
- Octreotide for Gastrointestinal Neuroendocrine TumorsDocumento2 pagineOctreotide for Gastrointestinal Neuroendocrine TumorsJesly CharliesNessuna valutazione finora
- The Gallbladder and Extrahepatic Bile Ducts RubinDocumento4 pagineThe Gallbladder and Extrahepatic Bile Ducts RubinJesly CharliesNessuna valutazione finora
- Octreotide for Gastrointestinal Neuroendocrine TumorsDocumento2 pagineOctreotide for Gastrointestinal Neuroendocrine TumorsJesly CharliesNessuna valutazione finora
- Appetite MechanismDocumento2 pagineAppetite MechanismJesly CharliesNessuna valutazione finora
- Alcoholic Liver Disease HarrisonDocumento3 pagineAlcoholic Liver Disease HarrisonJesly Charlies0% (1)
- Amebiasis HarrisonDocumento5 pagineAmebiasis HarrisonJesly CharliesNessuna valutazione finora
- Harrison's Online Chapter 271 Severe Sepsis Septic ShockDocumento9 pagineHarrison's Online Chapter 271 Severe Sepsis Septic ShockJesly CharliesNessuna valutazione finora
- Anatomy of Kidneys, Renal Veins and Suprarenal GlandsDocumento3 pagineAnatomy of Kidneys, Renal Veins and Suprarenal GlandsJesly CharliesNessuna valutazione finora
- Harrison's Online Chapter 272. Cardiogenic Shock and Pulmonary EdemaDocumento7 pagineHarrison's Online Chapter 272. Cardiogenic Shock and Pulmonary EdemaJesly CharliesNessuna valutazione finora
- Pterygium EmedicineDocumento9 paginePterygium EmedicineThomas SmithNessuna valutazione finora
- Aphakia - Essentials of Ophthalmology 2007Documento1 paginaAphakia - Essentials of Ophthalmology 2007Jesly CharliesNessuna valutazione finora
- Retropharyngeal AbscessDocumento3 pagineRetropharyngeal AbscessN NwekeNessuna valutazione finora
- Goat Production Handbook WEBDocumento100 pagineGoat Production Handbook WEBAakritee100% (1)
- HemoroidDocumento2 pagineHemoroidvivianmtNessuna valutazione finora
- Acute Colonic Diverticulitis - Medical Management - UpToDateDocumento30 pagineAcute Colonic Diverticulitis - Medical Management - UpToDateJulieth QuinteroNessuna valutazione finora
- Lecture 5Documento3 pagineLecture 5Shakil MahmodNessuna valutazione finora
- Sa CelulitisDocumento19 pagineSa CelulitisJulio Ramos EliasNessuna valutazione finora
- SURGERY B - Physical Examination of Surgical Patient: ObjectivesDocumento28 pagineSURGERY B - Physical Examination of Surgical Patient: Objectivesstar220498Nessuna valutazione finora
- Meconium Aspiration SyndromeDocumento7 pagineMeconium Aspiration SyndromeAi Niech Inoel100% (1)
- Template EbcrDocumento7 pagineTemplate EbcrNoraNessuna valutazione finora
- Bacterial Infections and ManagementDocumento3 pagineBacterial Infections and ManagementRobert Francis DikioNessuna valutazione finora
- HONORARY New Article For 32-34Documento3 pagineHONORARY New Article For 32-34Ramesh BeniwalNessuna valutazione finora
- 06-Systematic Review of Perforated Appendicitis and PhlegmonDocumento7 pagine06-Systematic Review of Perforated Appendicitis and PhlegmonTo MarNessuna valutazione finora
- 13 - Surgical InfectionsDocumento26 pagine13 - Surgical InfectionsEma KhalilNessuna valutazione finora
- Rotational Flap Closure of 1st and 5nth Met HeadDocumento8 pagineRotational Flap Closure of 1st and 5nth Met HeadleahbayNessuna valutazione finora
- Preseptal Cellulitis GuideDocumento19 paginePreseptal Cellulitis GuideCharles AlonzoNessuna valutazione finora
- Hitachi Hydraulic Excavator Ex1900 6 Parts Catalog p18k 1 3Documento22 pagineHitachi Hydraulic Excavator Ex1900 6 Parts Catalog p18k 1 3mskimberlymclaughlin080893cprNessuna valutazione finora
- Surgical Drains. What The Resident Needs To KnowDocumento8 pagineSurgical Drains. What The Resident Needs To Knowginoahnna33Nessuna valutazione finora
- Renal Infections: Abscesses, Xanthogranulomatous Pyelonephritis and Emphysematous PyelonephritisDocumento45 pagineRenal Infections: Abscesses, Xanthogranulomatous Pyelonephritis and Emphysematous PyelonephritisIber Coutiño100% (1)
- l8 Management of Perianal Pain and ConditionsDocumento51 paginel8 Management of Perianal Pain and ConditionsMohd Johari Mohd ShafuwanNessuna valutazione finora
- Lung Abscess in ChildrenDocumento9 pagineLung Abscess in ChildrenCaballero X CaballeroNessuna valutazione finora
- Preseptal cellulitis guide under 40 charactersDocumento18 paginePreseptal cellulitis guide under 40 charactersMario Mendoza TorresNessuna valutazione finora
- Javier1 ThemapDocumento1 paginaJavier1 Themapapi-253216868Nessuna valutazione finora
- Phil. Court Rules Tuberculosis Not Work-Related for SeamanDocumento10 paginePhil. Court Rules Tuberculosis Not Work-Related for SeamanJB AndesNessuna valutazione finora
- Everything About DogsDocumento326 pagineEverything About Dogstobiasaxo5653100% (1)
- CAFL EnglishDocumento21 pagineCAFL Englishredtruck99Nessuna valutazione finora
- ICD 9 CM Drainage of Facial AbscessesDocumento2 pagineICD 9 CM Drainage of Facial Abscessesnoerrekmed_816409184Nessuna valutazione finora
- Adolphe Didier MesmerismDocumento40 pagineAdolphe Didier MesmerismAren RoukemaNessuna valutazione finora
- EmpyemaDocumento52 pagineEmpyemaDivara Syauta100% (3)
- Boushra Rahman Postpartum InfectionDocumento1 paginaBoushra Rahman Postpartum InfectionClinica GinecologicaNessuna valutazione finora
- SDCEP MADP Consultation DraftDocumento58 pagineSDCEP MADP Consultation DraftLisa Pramitha SNessuna valutazione finora