Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
NEJMcpc049012
Caricato da
AmberTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
NEJMcpc049012
Caricato da
AmberCopyright:
Formati disponibili
The new england journal of medicine
case records of the massachusetts general hospital
Founded by Richard C. Cabot
Nancy Lee Harris, m.d., Editor
Jo-Anne O. Shepard, m.d., Associate Editor Stacey M. Ellender, Assistant Editor
Sally H. Ebeling, Assistant Editor Christine C. Peters, Assistant Editor
Case 26-2004: A 56-Year-Old Woman
with Cough and a Lung Nodule
Thomas J. Lynch, M.D., Cameron D. Wright, M.D., Noah C. Choi, M.D.,
Suzanne L. Aquino, M.D., and Eugene J. Mark, M.D.
presentation of case
Dr. Jennifer Temel (Medical Oncology): A 56-year-old woman was evaluated in the thoracic From the Departments of Medical Oncol-
oncology clinic for treatment of nonsmall-cell lung cancer. ogy (T.J.L.), Thoracic Surgery (C.D.W.), Radi-
ation Oncology (N.C.C.), Radiology (S.L.A.),
The patient had been in her usual state of good health until three months before and Pathology (E.J.M.), Massachusetts
presentation, when a nonproductive cough developed. During the next two months, General Hospital; and the Departments of
the cough became productive of yellow, blood-tinged sputum. She saw her primary care Medicine (T.J.L.), Surgery (C.D.W.), Radia-
tion Oncology (N.C.C.), Radiology (S.L.A.),
physician, and a chest radiograph revealed a nodule, 2.5 cm in diameter, in the upper and Pathology (E.J.M.), Harvard Medical
lobe of the right lung (Fig. 1A). Computed tomographic (CT) scanning of the thorax School.
identified a 2.5-cm nodule in the right upper lobe, with no enlarged hilar or mediastinal
N Engl J Med 2004;351:809-17.
lymph nodes (Fig. 1B). An abdominal ultrasound examination, a CT scan of the head, Copyright 2004 Massachusetts Medical Society.
and a bone scan showed no abnormalities. A positron-emission tomographic (PET) scan
revealed increased accumulation of fludeoxyglucose F 18 at the apex of the right lung,
at a site corresponding to the primary lesion (Fig. 1C); no other areas of accumulation
were noted.
One month before the patients evaluation in the clinic, bronchoscopy and mediasti-
noscopy were performed in preparation for a thoracotomy and resection of a suspected
bronchogenic carcinoma. Bronchoscopic examination revealed no abnormalities. Medi-
astinoscopy revealed no nodes on the left side but did show a normal-appearing subca-
rinal node and a normal-sized, mobile paratracheal node on the right side. Intraoper-
ative examination of a frozen section of a biopsy specimen of the paratracheal node
showed metastatic nonsmall-cell lung cancer; the subcarinal node was normal. The
thoracotomy was not performed, and the patient was referred to the thoracic oncology
clinic at this hospital.
An aneurysm of the left middle cerebral artery had been repaired three years previ-
ously, and an aneurysm of the right internal carotid artery had been repaired two years
previously. The patient had no neurologic deficits. She had smoked one to two packs of
cigarettes per day for 38 years but had stopped smoking when her cough developed.
She did not drink alcohol. Her only medications were alprazolam as needed for anxiety
and a nicotine patch. She had no family history of lung cancer.
On physical examination, her vital signs were normal and she appeared comfort-
able. There was no palpable lymphadenopathy. The lungs were clear on auscultation.
n engl j med 351;8 www.nejm.org august 19, 2004 809
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
C D
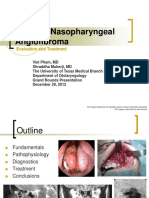
Figure 1. Radiologic Studies.
A chest radiograph shows a 2.5-cm nodule in the right upper lobe (Panel A). A CT scan confirms the presence of a 2.5-cm
nodule in the right upper lobe on lung windows (Panel B). The surrounding lung tissue shows moderate centrilobular em-
physema. A coronal image from a PET scan obtained with the use of fludeoxyglucose F 18 shows increased metabolic ac-
tivity in the upper-lobe nodule (Panel C) and in the right paratracheal (Panel D, arrow) and subcarinal lymph-node regions.
Neurologic examination revealed no abnormali- and mediastinal contours and densities are normal.
ties. Laboratory-test results were normal, except forA CT scan shows a spiculated nodule in the apex of
a slightly elevated level of alkaline phosphatase the right lung (Fig. 1B). There is centrilobular em-
(116 U per liter). physema of the surrounding lung parenchyma.
There is no evidence of enlarged lymph nodes in the
differential diagnosis right hilum or mediastinum.
PET scanning of the thorax with the use of
Dr. Suzanne L. Aquino: The chest radiograph obtained fludeoxyglucose F 18 shows increased uptake of
at the other hospital shows an ill-defined, 2.5-cm this radioactive agent in the nodule in the right
nodule in the right upper lobe (Fig. 1A). The hilar upper lobe (Fig. 1C) a finding that suggests the
810 n engl j med 351;8 www.nejm.org august 19 , 2004
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts general hospital
presence of a malignant tumor. Although it was a spiculated, solitary pulmonary nodule, as revealed
not noted at the time, in retrospect it is apparent on a PET scan. Given these factors, the chance that
that there was an increase in fludeoxyglucose F 18 her diagnosis was lung cancer was greater than 90
uptake in the right paratracheal and subcarinal percent.
lymph-node regions (Fig. 1D) a finding that sug- There are pitfalls for the surgeon in the preoper-
gests metastatic disease in the lymph nodes. There ative assessment of mediastinal lymph nodes. Small
are no other areas of increased fludeoxyglucose F 18 nodes that are considered benign according to CT
uptake. This scanning technique has a sensitivity of criteria can be microscopically positive for cancer,
92 to 95 percent and a specificity of 88 to 90 percent and large nodes are sometimes only inflammatory.
for detecting cancer in pulmonary nodules.1-3 False Enlarged nodes that are pathologically benign are
negative results may occur in slowly growing tu- found most commonly when there is an obstructive
mors, such as bronchioloalveolar carcinomas4 and pneumonia caused by a tumor in the bronchus,
carcinoid tumors,5 and in nodules less than 1 cm in usually a squamous-cell cancer. In contrast, large
diameter. Any nodule that shows increased uptake nodes with peripheral lung lesions almost always
of fludeoxyglucose F 18 should be considered po- contain cancer. If both the CT scans and the PET
tentially neoplastic, and a biopsy should be per- scans are read as negative, it is highly likely that the
formed. Nodules without increased metabolic ac- nodes will be negative for cancer. If either set of
tivity should be followed with repeated radiography scans is positive (or if both are), it is necessary to
to ensure that their size remains stable. sample the lymph nodes to obtain a tissue-based
Because PET scanning performed with the use diagnosis. The uncertainty is highlighted in this
of fludeoxyglucose F 18 measures the rate of me- case, since the retrospective interpretation of the
tabolism, other diseases with increased metabolism PET scan suggested that both the right paratracheal
can resemble cancer, especially if the lesions have a and the subcarinal nodes were positive but on biop-
nodular appearance. This explains the slightly lower sy only the paratracheal node was positive. To as-
specificity of the technique for detecting a malig- certain whether a patient is a candidate for preoper-
nant condition.1-3 False positive interpretations ative chemotherapy or radiotherapy, invasive staging
may occur with granulomas, pneumonias, and in- of the mediastinum must be performed.
flammatory lesions such as rheumatoid nodules.6-9 Since this patients PET scan was originally read
Since the detection of abnormal lymph nodes on as showing no evidence of metastasis, we planned
CT scans is based purely on size, a small lymph a one-day operation consisting of surgical staging of
node involved with tumor would be interpreted as the mediastinum with a mediastinoscopy, and if the
benign if it was less than 1 cm in diameter. PET findings were negative, a thoracotomy. Most nodal
scanning performed with fludeoxyglucose F 18 has groups that are important in lung cancer14,15
improved the radiologic staging of lung cancer, with the paratracheal, subcarinal, and tracheobronchial
a sensitivity of 91 percent, a specificity of 86 percent, angle nodes can be readily accessed by a medi-
and negative and positive predictive values of 95 astinoscopy. Nodes on the left side of the aortic
percent and 74 percent, respectively.10-13 As with arch (para-aortic and subaortic) are accessed by an
the detection of a primary tumor, the major limita- anterior mediastinotomy, which can be done at the
tions are false positive findings in lymph nodes same time. It is now possible, when necessary, to
affected by other diseases, such as silicosis or gran- access the inferior mediastinal nodes by endoscopic
ulomatous diseases. Therefore, to confirm the pres- fine-needle aspiration guided by ultrasonography.
ence of cancer, most experts recommend biopsy of The staging of lung cancer is based on the size
any lymph nodes that show increased fludeoxyglu- of the tumor (T1 through T4), the location and num-
cose F 18 uptake. ber of positive lymph nodes (N0 through N3), and
Dr. Thomas J. Lynch: Dr. Wright, can you tell us the absence or presence of distant metastases (M0
about your surgical approach for this patient? or M1). This patient has a tumor that is T1 (diame-
Dr. Cameron D. Wright: In this clinical setting, I ter, <3 cm, without invasion of the pleura), N2 (in-
thought the most likely diagnosis preoperatively volvement of ipsilateral, mediastinal, and subcari-
was nonsmall-cell lung cancer. She was of the ap- nal lymph nodes), and M0 (no distant metastases).
propriate age (older than 55 years), had a history of Lung cancer is also staged as IA or IB, IIA or IIB,
smoking, had no history of previous inflammatory IIIA or IIIB, or IV, depending on the combination of
lung illness, and had emphysema, hemoptysis, and TNM findings. This patients tumor is considered
n engl j med 351;8 www.nejm.org august 19, 2004 811
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
locally advanced (stage IIIA). The expected one-year
and five-year survival rates for this patient are 64 A
percent and 23 percent, respectively.16
There are several prognostic factors in stage N2
lung cancer, but the most important consideration
is whether enlarged mediastinal nodes are seen ei-
ther on a standard posterior-anterior radiograph or
on a CT scan; these clinically positive nodes are also
known as clinical N2 disease. Patients with such
nodes who undergo surgical resection and postop-
erative adjuvant treatment have a five-year survival
rate of only 5 percent, as compared with patients
B
whose lymph nodes are positive but not enlarged
(five-year survival rate, 20 to 30 percent).17,18 Other
poor prognostic variables include the involvement
of nodes at multiple sites and extracapsular growth
of tumor in the lymph node.
Clinically, this patients disease was N0 because
no enlarged nodes were seen on routine radio-
graphs. Because the intraoperative frozen section
showed a positive node, I thought she might bene-
fit from preoperative chemoradiotherapy, so I elect-
ed not to proceed with the planned thoracotomy. Figure 2. Lymph-Node Biopsy Specimen (Hematoxylin
and Eosin).
pathological discussion There are nests of carcinoma cells (Panel A) adjacent to
fibrotic tissue. At higher magnification the cells are large,
Dr. Eugene J. Mark: The right paratracheal lymph- with no glandular or squamous differentiation (Panel B).
node specimen from mediastinoscopy was submit-
ted for analysis; it consisted mostly of metastatic
large-cell carcinoma (Fig. 2A). The cells had large,
pleomorphic nuclei, and several cells had very large Table 1. Standard Histologic Classification of Lung
nucleoli with clumped chromatin and prominent Cancer and Its Variants.
nucleoli. There was no gland formation or keratini-
Squamous-cell carcinoma
zation to indicate adenocarcinoma or squamous- Papillary
cell carcinoma (Fig. 2B). The subcarinal node did Small-cell
not contain tumor cells. Basaloid
Adenocarcinoma
The standard histologic classification of the com- Acinar
mon carcinomas of the lung is shown in Table 1. Papillary
This patient had an undifferentiated large-cell carci- Bronchioloalveolar
Solid with mucus
noma. The role of the pathologist in the evaluation
Large-cell carcinoma
of carcinomas of the lung is given in Table 2.19-21 Neuroendocrine
The histologic type should conform to the standard Clear-cell
classification. The grade is often given but has not Lymphoepithelial
Rhabdoid
proved to be an independent factor in prognosis.
Small-cell carcinoma
The most important issue is the staging, which in-
cludes an assessment of the size of the tumor, the
relationship of the tumor to the pleura, the pres-
ence or absence of lymph-node metastases, and the a metastasis (Table 3). The most commonly used
adequacy of resection margins, particularly at the markers are thyroid transcription factor 22,23 and
bronchus. cytokeratins of various molecular weights. Thyroid
Immunopathological markers are sometimes transcription factor is largely restricted to lung and
useful in distinguishing a primary lung cancer from thyroid cancer. The expression of cytokeratins of
812 n engl j med 351;8 www.nejm.org august 19 , 2004
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts general hospital
Table 2. Pathological Considerations in the Diagnosis Table 3. Immunopathological Markers of Cancer.
of Lung Cancer.
Marker Expression
Histologic classification
Keratin (broad spectrum) All carcinomas
Histologic grade (optional)
Stage of tumor Carcinoembryonic antigen Adenocarcinoma
Size of primary tumor Keratins 7 and 20 Lung cancer (positive for keratin 7);
Extent of pleural invasion gastrointestinal cancer (positive
Status of lymph nodes for keratin 20)
Status of resection margins
Thyroid transcription factor 1 Lung and thyroid cancers
Investigational variables
Cellular reaction Calretinin and WT-1 Mesothelioma
Blood-vessel or lymphatic invasion CA 19-9 Pancreatic cancer
Effects of therapy Estrogen and progesterone receptors Breast cancer
Prostate-specific antigen Prostate cancer
Neuroendocrine markers (neuron- Small-cell carcinoma
various molecular weights in tumors mirrors that of specific enolase, synaptophysin,
the normal epithelium that the tumor arises from chromogranin)
or differentiates toward, and is useful in the diag-
nosis of metastases from the gastrointestinal tract
as well as the distinction of carcinomas of the lung these patients the disease can be cured by surgery,
from diffuse malignant mesothelioma. but the majority die from metastatic cancer. Strate-
gies that incorporate systemic chemotherapy offer
discussion of management the best chance of controlling distant metastatic
disease in both clinical N2 and minimal N2 lung
Dr. Lynch: In summary, this 56-year-old woman has cancer. A key question that we faced in the manage-
nonsmall-cell lung cancer, with clinical stage N0 ment of this case was how to optimally incorporate
or N1 disease and pathological stage N2 disease systemic chemotherapy and radiotherapy into her
a combination that is sometimes called minimal N2 treatment: Should they be given after surgery (adju-
disease. What is the optimal approach to care for vant) or before surgery (neoadjuvant)?
this patient? Before 2003, the role of adjuvant chemotherapy
Treatment of stage IIIA nonsmall-cell lung for completely resected lung cancer, with or with-
cancer is one of the most controversial topics in the out positive lymph nodes, was unclear. Four years
management of lung cancer. The most important ago, when treatment decisions for this patient were
initial distinction is to classify the disease as either being made, the data available did not support its
clinical N2 or clinical N1 or N0. Currently, oncolo- use. A 1995 meta-analysis found that cisplatin-
gists use the presence of lymph nodes on CT scans based adjuvant chemotherapy was associated with
or chest radiographs as the criterion for clinical N2 a 5 percent improvement in overall survival, but the
disease. A question for the near future is whether number of patients treated was too small to allow
PET scanning will change the preoperative staging an assessment of statistical significance.26 A study
classification. I suspect that patients whose disease in which the combination of cisplatin, etoposide,
is considered positive on the basis of PET scanning and radiotherapy was compared to radiotherapy
and negative on the basis of CT scanning will have alone after complete resection of stage II or III non
a prognosis that is somewhere between that of pa- small-cell lung cancer27 failed to show a benefit
tients with clinical N2 disease and minimal N2 dis- from adjuvant chemoradiotherapy.
ease. The increasing use of simultaneously regis- In 2003 and 2004, the results of two larger trials
tered PET and CT may make this distinction more were reported. One trial found that three cycles of
clear.24 platinum-based chemotherapy resulted in a 2 to
For patients with clinical N2 disease, there is 3 percent rate of absolute improvement in overall
wide agreement that surgery alone does not provide survival as compared with surgery alone, a finding
an acceptable cure rate.25 For patients with clinical that did not reach statistical significance; however,
N0 or N1 disease who have pathologically involved the number of patients in this study was not large
N2 nodes, also known as minimal N2 disease, there enough to permit detection of a 5 percent differ-
are several reasonable options. In nearly a third of ence in survival.28 The second trial was the largest
n engl j med 351;8 www.nejm.org august 19, 2004 813
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
randomized trial reported to date for patients with among the other treatments? How can toxic effects
resected lung cancer.29 In this study, more than from radiation be minimized?
1800 patients with stage I, II, or IIIA lung cancer A randomized, phase 3 clinical trial published
were randomly assigned after surgery to either ob- in abstract form in the early 1990s compared pre-
servation or to one of four cisplatin-based chemo- operative chemotherapy plus radiotherapy with che-
therapy regimens. At five years, the overall survival motherapy alone in patients with stage IIIA (N2)
was 44.5 percent in the group that received adju- and IIIB (T4) nonsmall-cell lung cancer.35 The
vant chemotherapy as compared with 40.0 percent response rate, resection rate, and rate of freedom
in the group that did not get adjuvant treatment from progression for preoperative, concurrent che-
a statistically significant difference. This trial was moradiotherapy as compared with chemotherapy
large enough to demonstrate a benefit of the mag- alone were 67 percent versus 44 percent, 52 percent
nitude that is clinically meaningful to patients. versus 31 percent, and 40 percent versus 21 percent,
Thus, for this patient with minimal N2 disease, respectively; all the differences were statistically sig-
surgical resection followed by three or four cycles of nificant. My colleagues and I conducted a phase 2
adjuvant cisplatin-based chemotherapy would be a study in which 42 patients with stage IIIA (N2) non
reasonable treatment option. Had these data been small-cell lung cancer were treated with two courses
available when this patient presented, she would of preoperative cisplatin, vinblastine, and fluo-
have considered this option. rouracil, with concurrent radiation given in two
Trials of neoadjuvant therapy followed by surgery fractions per day, followed by surgery and another
for stage IIIA nonsmall-cell lung cancer have in- course of postoperative chemoradiotherapy.36 The
volved both chemotherapy and combined chemo- tumor could be resected with negative margins in
therapy and radiotherapy strategies. Phase 2 stud- 81 percent of the patients. The overall survival rates
ies of chemotherapy followed by surgery (and often were 66 percent, 37 percent, and 37 percent at two,
postoperative radiotherapy) have reported cure rates three, and five years, respectively. Pathological ex-
of between 15 percent and 20 percent.30,31 This amination of the surgical specimen showed down-
compares favorably with the 5 percent to 9 percent staging of the tumor in 67 percent of the cases. The
survival rate reported for patients with clinical N2 degree of tumor down-staging translated into a sur-
cancer who were treated with surgery alone. How- vival benefit: five-year survival rates after surgery
ever, the comparison is not completely fair, since pa- were 79 percent, 42 percent, and 18 percent for post-
tient selection could result in differences in known operative tumor stages 0 (T0N0) and I (N0), stage
prognostic factors. Two small, randomized trials re- II (N1), and stage IIIA (N2), respectively. The South-
ported in the early 1990s32,33 showed a clear bene- west Oncology Group, in another phase 2 study,
fit associated with chemotherapy followed by sur- used a regimen of cisplatin and etoposide given
gery as compared with surgery alone; however, both concurrently with 45 Gy of radiation, followed by
studies included patients with T3N0 disease, which surgical resection. The five-year survival rate among
probably has biologic features and a pattern of re- patients with stage IIIA (N2) disease was 35 per-
currence that differ from those of N2 disease. A cent.37
larger, randomized trial34 showed a trend toward Thus, the combination of chemotherapy and ra-
improved outcomes with chemotherapy as com- diotherapy has the potential advantage of enhanc-
pared with surgery alone, but the difference did not ing local control while delivering drug doses that
reach statistical significance because of the small can affect distant metastatic spread. Randomized
number of patients in the study. trials of chemotherapy compared with chemora-
Dr. Choi will discuss the use of combined che- diotherapy are needed to determine which strategy
motherapy and radiotherapy followed by surgery for is better before surgical resection.
stage IIIA nonsmall-cell lung cancer. The targeting of radiotherapy has improved
Dr. Noah C. Choi: Important questions in planning during the past 30 years, with the advent of three-
the appropriate multimodality therapy for a patient dimensional conformal radiation, intensity-modu-
such as this with stage IIIA (N2) nonsmall-cell lated radiation, and proton-beam radiation. These
lung cancer include the following: What is the role techniques permit the delivery of radiation to the
of radiotherapy relative to chemotherapy in down- tumor with normal tissue spared, and they allow
staging the tumor so that it can be resected? What the delivery of radiation concurrently with chemo-
is the proper sequence for the use of radiotherapy therapy without undue toxic effects.38,39 At the time
814 n engl j med 351;8 www.nejm.org august 19 , 2004
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts general hospital
this patients care was planned, these techniques
were not standard, and she was treated with a two- A
dimensional technique.
Dr. Lynch: Finally, we need to consider whether
surgery is needed after chemotherapy or chemo-
radiotherapy. In a recent multicenter study, patients
with histologically proven N2 disease were random-
ly assigned to either induction chemoradiotherapy
(cisplatin, etoposide, and 45 Gy of radiation) fol-
lowed by surgery or to chemoradiotherapy alone.40
The initial data indicate that induction chemoradio-
therapy followed by surgery was superior in terms of
the time to progression and the rate of survival at B
five years (38 percent vs. 33 percent). However, the
trial was small and this difference, though potential-
ly clinically meaningful, was not statistically signif-
icant. Both neoadjuvant chemoradiotherapy and
chemoradiotherapy alone offer results that are supe-
rior to those of surgery alone for clinical N2 disease.
In the case under discussion, the decision was
made to administer neoadjuvant chemoradiother-
apy followed by surgery. Today, this strategy might
well still be the treatment of choice, but it would
Figure 3. Specimen of Resected Lung after Chemoradio-
certainly be reasonable to offer treatment with de-
therapy (Hematoxylin and Eosin).
finitive chemoradiotherapy without surgery or to op-
There is necrotic tumor containing cholesterol clefts
erate initially and follow up with adjuvant chemo- (Panel A) adjacent to desmoplastic inflammation and fi-
therapy. brosis. There is emphysema (Panel B) with free-floating
Dr. Temel: Therapy was begun with concurrent fragments of alveolar walls.
chemotherapy and radiation to the tumor region in
the right lung. She was treated with 45 Gy of radia-
tion to the right lung and hilus and the right para- response on radiography, because there can still
tracheal region in 25 fractions over a period of six be microscopic residual disease in either the lymph
weeks. She also received carboplatin at a dose calcu- nodes or lung. Close attention is given to the bron-
lated to result in an area under the concentration chial stump after induction therapy, and it is covered
time curve of 6.0 mg per milliliter per minute in a with a vascularized flap to prevent development of
three-week cycle and paclitaxel at a dose of 50 mg a bronchopleural fistula.
per square meter of body-surface area each week. The surgeon will do a complete mediastinal lym-
The patient had mild nausea, which was well con- phadenectomy, both for therapeutic reasons (to re-
trolled with ondansetron. She had mild esophageal move any residual cancer in the lymph nodes) and
mucositis and alopecia. Restaging studies showed a for restaging. It is preferable not to perform a right
decrease in the size of the mass in the right upper pneumonectomy in patients who have received
lobe from 2.5 cm to 2.0 cm and no evidence of met- induction therapy, because of the possibility of
astatic disease. higher-than-expected postoperative mortality. Pa-
Dr. Wright: After the induction therapy, both tients whose tumors can be removed either by lobec-
pulmonary-function studies and laboratory studies tomy or by left-sided pneumonectomy have a peri-
should be performed to make sure that there is a operative mortality rate similar to that of patients
good functional as well as a hematologic recovery, who have not received preoperative therapy.
which will enable the patient to tolerate surgery. Twelve weeks after this patients initial medias-
Because it usually causes hilar fibrosis, induction tinoscopy, I performed a right thoracotomy, with a
chemoradiotherapy often increases the difficulty of right upper lobectomy and mediastinal lymphade-
subsequent surgery. The surgeon treats the original nectomy.
volume of disease even if there has been a complete Dr. Mark: The lung resected after radiotherapy
n engl j med 351;8 www.nejm.org august 19, 2004 815
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
and chemotherapy contained necrotic tumor; no well 42 months after the diagnosis, overall survival
definitely viable cells remained and there was only in this disease is still poor, and novel approaches
a single focus of possibly viable cells. Cholesterol need to be studied. Future trials in locally advanced
clefts and necrosis were surrounded by inflamma- nonsmall-cell lung cancer will incorporate new
tion and fibrosis (Fig. 3A). Blood vessels were in- molecular agents. A key issue will be the identifica-
flamed with intimal fibrosis, which could have been tion of patients who are likely to benefit from bio-
caused by the cancer itself, by the radiation, or in logic therapy. An example is the recent demonstra-
this case, by both. Free-floating fragments of alve- tion that activating mutations in the epidermal
olar walls in the parenchyma apart from the tumor growth factor receptor predict responses of non
indicated there was emphysema as a consequence small-cell lung cancers to the tyrosine kinase inhib-
of the patients smoking (Fig. 3B). The lymph-node itor, gefitinib.41 Ultimately, a successful care plan
dissection specimens (paratracheal and subcarinal) for a patient with stage IIIA nonsmall-cell lung
had no evidence of cancer cells. cancer will need to include maximal local treat-
Dr. Temel: Two months after the operation, the ment with surgery, radiotherapy, or both in addition
patient received two additional cycles of full-dose to systemic treatment that targets residual micro-
carboplatin and paclitaxel. Forty-two months after scopic tumor.
the completion of therapy, she had no evidence of
recurrent disease. anatomical diagnosis
Dr. Lynch: This patients case illustrates the need
for multidisciplinary management of nonsmall- Large-cell undifferentiated carcinoma of the lung,
cell lung cancer. Although this patient was doing stage IIIA (T1N2M0).
refer enc es
1. Dewan NA, Gupta NC, Redepenning LS, with thyroid cancer. J Nucl Med 1998;39: 18. Suzuki K, Nagai K, Yoshida Y, Nishimu-
Phalen JJ, Frick MP. Diagnostic efficacy of 234-6. ra M, Takahashi K, Nishiwaki Y. The prog-
PET-FDG imaging in solitary pulmonary 10. Pieterman RM, van Putten JWG, Meuze- nosis of surgically resected N2 non-small
nodules: potential role in evaluation and laar JJ, et al. Preoperative staging of non cell lung cancer: the importance of clinical
management. Chest 1993;104:997-1002. small-cell lung cancer with positron-emis- N status. J Thorac Cardiovasc Surg 1999;
2. Gupta NC, Maloof J, Gunel E. Probabil- sion tomography. N Engl J Med 2000;343: 118:145-53.
ity of malignancy in solitary pulmonary nod- 254-61. 19. Gephardt GN, Baker PB. Lung carcino-
ules using fluorine-18-FDG and PET. J Nucl 11. Valk PE, Pounds TR, Hopkins DM, et al. ma surgical pathology report adequacy:
Med 1996;37:943-8. Staging non-small cell lung cancer by a College of American Pathologists Q-Probes
3. Lowe VJ, Fletcher JW, Gobar L, et al. Pro- whole-body positron emission tomograph- study of over 8300 cases from 464 institu-
spective investigation of positron emission ic imaging. Ann Thorac Surg 1995;60:1573- tions. Arch Pathol Lab Med 1996;120:922-7.
tomography in lung nodules. J Clin Oncol 82. 20. Kerr KM, Johnson SK, King G, Kennedy
1998;16:1075-84. 12. Scott WJ, Gobar LS, Terry JD, Dewan MM, Weir J, Jeffrey R. Partial regression in
4. Higashi K, Ueda Y, Seki H, et al. Fluo- NA, Sunderland JJ. Mediastinal lymph node primary carcinoma of the lung: does it oc-
rine-18-FDG PET imaging is negative in staging of non-small-cell lung cancer: a cur? Histopathology 1998;33:55-63.
bronchioloalveolar lung carcinoma. J Nucl prospective comparison of computed to- 21. Recommendations for the reporting of
Med 1998;39:1016-20. mography and positron emission tomogra- resected primary lung carcinomas. Am J
5. Erasmus JJ, McAdams HP, Patz EF Jr, phy. J Thorac Cardiovasc Surg 1996;111: Clin Pathol 1995; 104:371-4.
Coleman RE, Ahuja V, Goodman PC. Evalua- 642-8. 22. Tan D, Li Q, Deeb G, et al. Thyroid tran-
tion of primary pulmonary carcinoid tumors 13. Gupta NC, Tamin WJ, Graeber GG, scription factor-1 expression prevalence and
using FDG PET. AJR Am J Roentgenol 1998; Bishop HA, Hobbs GR. Mediastinal lymph its clinical implications in non-small cell
170:1369-73. node sampling following positron emission lung cancer: a high-throughput tissue mi-
6. Kapucu LO, Metzler CC, Townsend DW, tomography with fluorodeoxyglucose imag- croarray and immunohistochemistry study.
Keenan RJ, Luketich JD. Fluorine-18-fluoro- ing in lung cancer staging. Chest 2001;120: Hum Pathol 2003;34:597-604.
deoxyglucose uptake in pneumonia. J Nucl 521-7. 23. Demarchi LMMF, Reis MM, Palomino
Med 1998;39:1267-9. 14. Martini N, Flehinger BJ, Zaman MB, SAP, et al. Prognostic values of stromal pro-
7. Goo JM, Im JG, Do KH, et al. Pulmonary Beattie EJ Jr. Results of resection in non-oat portion and PCNA, Ki-67, and p53 proteins
tuberculoma evaluated by means of FDG cell carcinoma of the lung with mediastinal in patients with resected adenocarcinoma of
PET: findings in 10 cases. Radiology 2000; lymph node metastases. Ann Surg 1983; the lung. Mod Pathol 2000;13:511-20.
216:117-21. 198:386-97. 24. Lardinois D, Weder W, Hany TF, et al.
8. Gotway MB, Storto ML, Golden JA, 15. Mountain C, Dressler C. Regional lymph Staging of non-small-cell lung cancer with
Reddy GP, Webb WR. Incidental detection node classification for lung cancer staging. integrated positron-emission tomography
of thoracic sarcoidosis on whole-body Chest 1997;111:1718-23. and computed tomography. N Engl J Med
18fluorine-2-fluoro-2-deoxy-glucose posi- 16. Spira A, Ettinger DS. Multidisciplinary 2003;348:2500-7.
tron emission tomography. J Thorac Imag- management of lung cancer. N Engl J Med 25. Andre F, Grunenwald D, Pignon J, et al.
ing 2000;15:201-4. 2004;350:379-92. Survival of patients with resected N2 non-
9. Bakheet SM, Powe J. Fluorine-18-fluo- 17. Martini N, Flehinger BJ. The role of sur- small-cell lung cancer: evidence for a sub-
rodeoxyglucose uptake in rheumatoid ar- gery in N2 lung cancer. Surg Clin North Am classification and implications. J Clin Oncol
thritis-associated lung disease in a patient 1987;67:1037-49. 2000;18:2981-9.
816 n engl j med 351;8 www.nejm.org august 19 , 2004
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts general hospital
26. Non-Small Cell Lung Cancer Collabora- A randomized trial comparing perioperative radiotherapy followed by surgery for stages
tive Group. Chemotherapy in non-small cell chemotherapy and surgery with surgery IIIA (N2) and IIIB (N3) non-small-cell lung
lung cancer: a meta-analysis using updated alone in resectable stage IIIA non-small-cell cancer: mature results of Southwest Oncol-
data on individual patients from 52 random- lung cancer. J Natl Cancer Inst 1994;86:673- ogy Group phase II study 8805. J Clin Oncol
ised clinical trials. BMJ 1995;311:899-909. 80. 1995;13:1880-92.
27. Keller SM, Adak S, Wagner H, et al. 33. Rosell R, Gomez-Codina J, Camps C, et 38. Murshed H, Liu HH, Liao Z, et al. Dose
A randomized trial of postoperative adju- al. A randomized trial comparing preopera- and volume reduction for normal lung us-
vant therapy in patients with completely re- tive chemotherapy plus surgery with surgery ing intensity-modulated radiotherapy for ad-
sected stage II or IIIA nonsmall-cell lung alone in patients with nonsmall-cell lung vanced-stage nonsmall-cell lung cancer.
cancer. N Engl J Med 2000;343:1217-22. cancer. N Engl J Med 1994;330:153-8. Int J Radiat Oncol Biol Phys 2004;58:1258-
28. Scagliotti GV, Fossati R, Torri V, et al. 34. Depierre A, Milleron B, Moro-Sibilot D, 67.
Randomized study of adjuvant chemothera- et al. Preoperative chemotherapy followed 39. Liu HH, Wang X, Dong L, et al. Feasibil-
py for completely resected stage I, II, or IIIA by surgery compared with primary surgery ity of sparing lung and other thoracic struc-
non-small-cell lung cancer. J Natl Cancer in resectable stage I (except T1N0), II, and tures with intensity-modulated radiotherapy
Inst 2003;95:1453-61. IIIa non-small-cell lung cancer. J Clin Oncol for non-small-cell lung cancer. Int J Radiat
29. Arriagada R, Bergman B, Dunant A, et 2002;20:247-53. Oncol Biol Phys 2004;58:1268-79.
al. Cisplatin-based adjuvant chemotherapy 35. Fleck J, Camargo J, Godoy D, et al. 40. Albain KS, Scott CB, Rusch VR, et al.
in patients with completely resected non Chemoradiation therapy alone versus che- Phase III comparison of concurrent chemo-
small-cell lung cancer. N Engl J Med 2004; motherapy alone as a neoadjuvant treatment therapy plus radiotherapy (CT/RT) and CT/
350:351-60. for stage III non-small cell lung cancer: pre- RT followed by surgical resection for stage
30. Elias AD, Skarin AT, Leong T, et al. Neo- liminary report of a phase III, randomized IIIA (pN2) non-small cell lung cancer
adjuvant therapy for surgically staged IIIA trial. Prog Proc Am Soc Clin Oncol 1993;12: (NSCLC): initial results from intergroup trial
N2 non-small cell lung cancer (NSCLC). 333. abstract. 0139 (RTOG 93-09). Prog Proc Am Soc Clin
Lung Cancer 1997;17:147-61. 36. Choi N, Carey RW, Daly W, et al. Poten- Oncol 2003;22:621. abstract.
31. Sugarbaker DJ, Herndon J, Kohman LJ, tial impact on survival of improved tumor 41. Lynch TJ, Bell DW, Sordella R, et al. Acti-
Krasna MJ, Green MR. Results of Cancer downstaging and resection rate by preoper- vating mutations in the epidermal growth
and Leukemia Group B protocol 8935: a mul- ative twice-daily radiation and concurrent factor receptor underlying responsiveness
tiinstitutional phase II trimodality trial for chemotherapy in stage IIIA non-small-cell of nonsmall-cell lung cancer to gefitinib.
stage IIIA (N2) non-small-cell lung cancer. lung cancer. J Clin Oncol 1997;15:712-22. N Engl J Med 2004;350:2129-39.
J Thorac Cardiovasc Surg 1995;109:473-85. 37. Albain K, Rusch VW, Crowley JJ, et al. Copyright 2004 Massachusetts Medical Society.
32. Roth JA, Fossella F, Komaki R, et al. Concurrent cisplatin/etoposide plus chest
35-millimeter slides for the case records
Any reader of the Journal who uses the Case Records of the Massachusetts General Hospital as a medical teaching
exercise or reference material is eligible to receive 35-mm slides, with identifying legends, of the pertinent x-ray films,
electrocardiograms, gross specimens, and photomicrographs of each case. The slides are 2 in. by 2 in., for use with a
standard 35-mm projector. These slides, which illustrate the current cases in the Journal, are mailed from the Department
of Pathology to correspond to the week of publication and may be retained by the subscriber. Each year approximately
250 slides from 40 cases are sent to each subscriber. The cost of the subscription is $450 per year. Application forms for
the current subscription year, which began in January, may be obtained from Lantern Slides Service, Department of
Pathology, Massachusetts General Hospital, Boston, MA 02114 (telephone 617-726-2974).
Slides from individual cases may be obtained at a cost of $35 per case.
n engl j med 351;8 www.nejm.org august 19, 2004 817
The New England Journal of Medicine
Downloaded from nejm.org at UNIVERSITY OF TORONTO on November 2, 2014. For personal use only. No other uses without permission.
Copyright 2004 Massachusetts Medical Society. All rights reserved.
Potrebbero piacerti anche
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- What Is Immunotherapy?Documento19 pagineWhat Is Immunotherapy?Najia ChoudhuryNessuna valutazione finora
- SESAP16 Self AssessmentDocumento280 pagineSESAP16 Self AssessmentKamil Hanna100% (1)
- Modalities of Cancer TreatmentDocumento65 pagineModalities of Cancer TreatmentBspharma 2E100% (1)
- RadiotherapyDocumento60 pagineRadiotherapyAARYANessuna valutazione finora
- Journal Club Presentation On Pancreatic CancerDocumento1 paginaJournal Club Presentation On Pancreatic Cancercusom34Nessuna valutazione finora
- Pillai2016 PDFDocumento35 paginePillai2016 PDFmehak malhotraNessuna valutazione finora
- Overview of The Management of Primary Colon Cancer - UpToDateDocumento30 pagineOverview of The Management of Primary Colon Cancer - UpToDateCaio AmaralNessuna valutazione finora
- E002435 FullDocumento33 pagineE002435 FullAlizaPinkyNessuna valutazione finora
- Dapus CaDocumento3 pagineDapus CaAlif RamadhanNessuna valutazione finora
- Sinonasal Undifferentiated Carcinoma (SNUC) Treatment Outcomes: A ReviewDocumento13 pagineSinonasal Undifferentiated Carcinoma (SNUC) Treatment Outcomes: A ReviewAnonymous VTZ0bL5Od7Nessuna valutazione finora
- Carcinoma of The Cervix 2Documento8 pagineCarcinoma of The Cervix 2api-3705046Nessuna valutazione finora
- CTR Conference BookletDocumento150 pagineCTR Conference BookletAhmad Abu-AyshehNessuna valutazione finora
- NJMS 14 185Documento5 pagineNJMS 14 185Guma KipaNessuna valutazione finora
- Early Postoperative Complications After Oncoplastic Reduction - PMCDocumento14 pagineEarly Postoperative Complications After Oncoplastic Reduction - PMCluis david gomez gonzalezNessuna valutazione finora
- UpdateJul2007 3julDocumento10 pagineUpdateJul2007 3julAnshul SinghNessuna valutazione finora
- Cancer NotesDocumento12 pagineCancer Noteswavezone113Nessuna valutazione finora
- Phyllodes Tumors of The Breast: Natural History, Diagnosis, and TreatmentDocumento7 paginePhyllodes Tumors of The Breast: Natural History, Diagnosis, and TreatmentFrancis BillanesNessuna valutazione finora
- BRAJFEC Guideline Breast CancerDocumento5 pagineBRAJFEC Guideline Breast CancerdidiisafitriNessuna valutazione finora
- Drugs Dosage Nursing Implications: Discharge PlanDocumento2 pagineDrugs Dosage Nursing Implications: Discharge PlanCristina L. JaysonNessuna valutazione finora
- Aromatase Inhibitors For Breast Cancer I PDFDocumento11 pagineAromatase Inhibitors For Breast Cancer I PDFGaro ArslanianNessuna valutazione finora
- 2022 ESMO AC Early Stage NSCLC Perspective Adjuvant Immunotherapy SPDocumento43 pagine2022 ESMO AC Early Stage NSCLC Perspective Adjuvant Immunotherapy SPTowhidul IslamNessuna valutazione finora
- 2005 AHPBA CONGRESS ABSTRACTS—FREE PAPERS AND VIDEOSDocumento100 pagine2005 AHPBA CONGRESS ABSTRACTS—FREE PAPERS AND VIDEOSDrAmmar MagdyNessuna valutazione finora
- ACR In-Service 2007 Exam, Answers, RationalDocumento98 pagineACR In-Service 2007 Exam, Answers, RationalDave FullerNessuna valutazione finora
- Angiofibroma Pic 2012 12 BDocumento55 pagineAngiofibroma Pic 2012 12 Bkhairanifahma100% (1)
- Cholangiocarcinoma 2 Juni 2018Documento40 pagineCholangiocarcinoma 2 Juni 2018Anonymous 1UgsHkUNessuna valutazione finora
- Makalah Bhom 2018 PDFDocumento354 pagineMakalah Bhom 2018 PDFAndrian KHoerul Anwar SiiGogon100% (2)
- ST Gallen 2017 - Early Breast CancerDocumento13 pagineST Gallen 2017 - Early Breast CancerPaulo Cesar Castañeda RuizNessuna valutazione finora
- Paclitaxel-Induced Pneumonitis in PatientsDocumento5 paginePaclitaxel-Induced Pneumonitis in PatientsAndiie ResminNessuna valutazione finora
- The Principles of The Surgical Management of Gastric CancerDocumento5 pagineThe Principles of The Surgical Management of Gastric CancerRobert ChristevenNessuna valutazione finora
- Recto y Ano TraducidoDocumento19 pagineRecto y Ano TraducidoJacqueline GómezNessuna valutazione finora