Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Schwartz Chapter 35 Abdominal Wall, Omentum, Mesentery and Retroperitonium
Caricato da
Rem AlfelorCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Schwartz Chapter 35 Abdominal Wall, Omentum, Mesentery and Retroperitonium
Caricato da
Rem AlfelorCopyright:
Formati disponibili
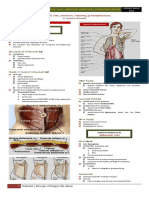
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
KEY POINTS leading edges of these structures develop into the rectus abdominis muscles,
Defects of the complex process of abdominal wall development in the fetus can eventually meet in the midline of the anterior abdominal wall
occur in several ways resulting in muscle fibers of the RECTUS ABDOMINIS
persistent midgut herniation arranged vertically
OMPHALOCELE encased within an aponeurotic sheath
GASTROSCHISIS anterior and posterior layers of which are fused in the midline at the
vitelline duct remnant abnormalities LINEA ALBA
MECKEL'S DIVERTICULUM has insertions on the symphysis pubis and pubic bones, anteroinferior
VITELLINE DUCT FISTULA OR CYST aspects of the fifth and sixth ribs, seventh costal cartilages and the xiphoid
management of rectus sheath hematomas consists of process
reversal of any anticoagulation or coagulopathy lateral border assumes a convex shape that gives rise to the surface
observation landmark of the LINEA SEMILUNARIS
unless either hemodynamic instability or enlargement necessitates usually are three tendinous intersections or inscriptions that cross the rectus
surgical evacuation muscles:
Incisional hernias of the anterior abdominal wall may occur in up to 1020% of level of the xiphoid process
prior abdominal operations of all types. level of the umbilicus
Primary suture repair of abdominal wall incisional hernias is associated with one halfway between the xiphoid process and the umbilicus
unacceptably high incidence of hernia recurrence
Prompted the wide use of prosthetic mesh materials for hernia repair.
Laparoscopic incisional hernia repair offers important advantages over open
repairs including
reduced pain medication use
earlier return to normal function
possibly superior protection from hernia recurrence
SCLEROSING MESENTERITIS
poorly understood mesenteric process
characterized by variable degrees of inflammation and fibrosis within
mesenteric tissues of the small and large bowel
Frequently requires surgical biopsy to rule out neoplasm and to establish The three muscular layers of the abdominal wall lateral to the rectus abdominis are
the external oblique, internal oblique, and transversus abdominis muscles, shown
the correct diagnosis.
here on the low abdomen, where the lower margin of the external oblique reflects
RETROPERITONEAL FIBROSIS posteriorly as the inguinal ligament.
primary or secondary fibroproliferative process in the retroperitoneum
Characterized by distortion of retroperitoneal structures, including the Lateral to the rectus sheath are three muscular layers with oblique fiber
ureters and inferior vena cava. orientations relative to one another
Treatment may include layers are derived from the laterally migrating mesodermal tissues during
ureterolysis or ureteral stenting the sixth to seventh week of fetal development, before fusion of the
Medical therapies such as corticosteroids or Tamoxifen. developing rectus abdominis muscles in the midline
EXTERNAL OBLIQUE MUSCLE
ABDOMINAL WALL Runs inferiorly and medially
arising from the margins of the lowest eight ribs and costal
cartilages
Originates laterally on the latissimus dorsi, serratus anterior
muscles and iliac crest.
Medially it forms a tendinous aponeurosis, which is contiguous with
the anterior rectus sheath
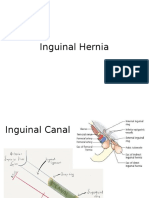
INGUINAL LIGAMENT
inferior-most edge of the external oblique aponeurosis
reflected posteriorly in the area between the anterior superior
iliac spine and pubic tubercle
INTERNAL OBLIQUE MUSCLE
lies immediately deep to the external oblique muscle
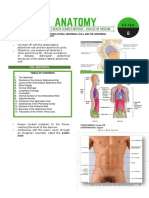
Anterior abdominal wall. The LINEA ALBA is the midline aponeurotic demarcation between the
arises from the lateral aspect of the inguinal ligament, the iliac crest,
bellies of the rectus abdominis muscles. The rectus abdominis muscle and its tendinous and the thoracolumbar fascia
intersections on the left are shown deep to the reflected anterior rectus sheath. Segmental fibers course superiorly and medially and form a tendinous
cutaneous nerve branches also are shown. aponeurosis that contributes components to both the anterior and
posterior rectus sheath
defined lower medial and inferior-most fibers of the internal oblique course
superiorly by the costal margins may fuse with the lower fibers of the TRANSVERSUS ABDOMINIS
inferiorly by the symphysis pubis and pelvic bones muscle
Posteriorly by the vertebral column. conjoined area
serves to support and protect abdominal and retroperitoneal structures inferior-most fibers of the internal oblique muscle are contiguous
complex muscular functions enable twisting and flexing motions of the trunk with the cremasteric muscle in the inguinal canal
mesodermal in origin critical significance in the management of inguinal hernia
develops as bilateral migrating sheets that originate in the paravertebral TRANSVERSUS ABDOMINIS MUSCLE
region and envelop the future abdominal area deepest of the three lateral muscles
By: Rem Alfelor Page 1 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
Runs transversely from the bilateral lowest six ribs, the lumbosacral motor nerves to the rectus muscles, the internal oblique muscles, and the
fascia, and the iliac crest to the lateral border of the rectus transversus abdominis muscles run from the anterior rami of spinal nerves
abdominis musculoaponeurotic structures. at the T6 TO T12 LEVELS
complexities of the anterior and posterior aspects of the rectus sheath are best overlying skin is innervated by afferent branches of the T4 TO L1 NERVE
understood in their relationship to the ARCUATE LINE (SEMICIRCULAR LINE ROOTS, with the nerve roots of T10 subserving sensation of the skin
OF DOUGLAS) around the umbilicus
lies roughly at the level of the anterior superior iliac spines
Above the arcuate line
ANTERIOR RECTUS SHEATH is formed by the external oblique
aponeurosis and external lamina of the internal oblique aponeurosis
POSTERIOR RECTUS SHEATH is formed by the internal lamina of
the internal oblique aponeurosis, transversus abdominis
aponeurosis and transversalis fascia
Below the arcuate line
anterior rectus sheath is formed by the external oblique
aponeurosis, laminae of the internal oblique aponeurosis, and the
transversus abdominis aponeurosis
no aponeurotic posterior covering of this lower portion of the rectus
muscles, although the transversalis fascia remains a contiguous
structure on the posterior aspect of the abdominal wall
Dermatomal sensory innervation of the abdominal wall.
Physiology
Rectus muscles, the external oblique muscles, and the internal oblique muscles
work as a unit to flex the trunk anteriorly or laterally.
Rotation of the trunk is achieved by the contraction of the external oblique
muscle and the contralateral internal oblique muscle.
All four muscle groups (i.e., rectus muscles, external oblique muscles,
internal oblique muscles, and transversus abdominis muscles) are involved
in raising intra-abdominal pressure.
If the diaphragm is relaxed when the abdominal musculature is contracted, the
pressure exerted by the abdominal muscles results in expiration of air from the
lungs or a cough if this contraction is forceful
Cross-sectional anatomy of the abdominal wall above and below the arcuate line of Douglas. The
lower right abdominal wall segment shows clearly the absence of an aponeurotic covering of the
Abdominal muscles are the primary muscles of expiration.
posterior aspect of the rectus abdominis muscle inferior to the arcuate line. Superior to the arcuate If the diaphragm is contracted when the abdominal musculature is contracted
line, there are both internal oblique and transversus abdominis aponeurotic contributions to the (VALSALVA MANEUVER)
posterior rectus sheath. Increased abdominal pressure aids in processes such as micturition,
defecation, and childbirth.
majority of the blood supply to the muscles of the anterior abdominal wall is
derived from the SUPERIOR AND INFERIOR EPIGASTRIC ARTERIES Abdominal Anatomy and Surgical Incisions
SUPERIOR EPIGASTRIC ARTERY arises from the internal thoracic Various anterior abdominal wall incisions for exposure
artery of peritoneal structures. A, Midline incision; B,
INFERIOR EPIGASTRIC ARTERY arises from the external iliac artery. paramedian incision; C, right subcostal incision
and "saber slash" extension to costal margin (dashed
collateral network of branches of the SUBCOSTAL AND LUMBAR ARTERIES line); D, bilateral subcostal (also bucket handle,
also contributes to the abdominal wall blood supply chevron, gable) incision, and "Mercedes Benz"
Lymphatic drainage of the abdominal wall is predominantly to the major nodal extension (dashed line); E, b and Weir extension
basins in the SUPERFICIAL INGUINAL AND AXILLARY AREAS. (dashed line); F, McBurney incision; G, transverse
incision and extension across midline (dashed line);
and H, Pfannenstiel incision.
The superior and inferior epigastric
arteries form an anastomosing
network of vessels in and around the
rectus sheath, withcollateralization to
subcostal and lumbar vessels
situated more laterally on the
abdominal wall. Lymphatic drainage
is via axially or inguinal nodal basins.
Incisions for open surgery generally are located in proximity to the principal
operative targets.
L aparoscopic port site incisions might be remote from the site of interest and
are carefully planned based on the anticipated instrument approach angles and
necessary working distances both to the operative site and between ports.
Orientation of the line of any incision may be determined based on
expected quality of exposure
closure considerations, including cosmesis
avoidance of previous incision sites
Innervation of the anterior abdominal wall is segmentally related to specific Simple surgeon preference.
spinal levels In general, the incision for open peritoneal access can be
longitudinal (in or off the midline)
transverse (lateral to or crossing the midline)
By: Rem Alfelor Page 2 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
oblique (directed either upward or downward toward the flank) allantois
majority of nonlaparoscopic procedures on the GI tract, midline incisions are sixth week of development
used because of the flexibility offered by this approach in establishing Abdominal contents grow too large for the abdominal wall to completely
adequate exposure contain and the embryonic midgut herniates into the umbilical cord.
incision in the fused midline aponeurotic tissue (linea alba) is simple outside the confines of the developing abdomen, it undergoes a 270-
Requires no division of skeletal muscle. degree counterclockwise rotation
End of the twelfth week, returns to the abdominal cavity.
PARAMEDIAN INCISIONS
made longitudinally 3 cm off the midline, through the rectus abdominis
sheath structures Defects in abdominal wall closure may lead to OMPHALOCELE or
largely been abandoned in favor of midline or nonlongitudinal access GASTROSCHISIS
methods OMPHALOCELE
Incisions lateral to the midline made with transverse or oblique viscera protrude through an open umbilical ring
orientations may divide the successive muscular layers or bluntly split covered by a sac derived from the amnion
them in the direction of their fibers GASTROSCHISIS
muscle-splitting approach (exemplified by the CLASSIC MCBURNEY INCISION viscera protrude through a defect lateral to the umbilicus
for appendectomy) No sac is present.
May be less destructive to tissue and thus allow healing with less scarring During the third trimester, the vitelline duct regresses.
and tissue distortion but generally offers more limited exposure than other Persistence of a vitelline duct remnant on the ileal border results in
methods. MECKEL'S DIVERTICULUM.
SUBCOSTAL INCISIONS Complete failure of the vitelline duct to regress results in a VITELLINE
on the right (KOCHER INCISION for cholecystectomy) DUCT FISTULA
on the left (for splenectomy) Associated with drainage of small intestine contents from the
Archetypal muscle-dividing incisions that generally result in transection of umbilicus.
some or all of the rectus abdominis muscle fibers and investing If both the intestinal and umbilical ends of the vitelline duct regress into
aponeuroses. fibrous cords, a CENTRAL VITELLINE DUCT
generally are closed in two layers (OMPHALOMESENTERIC) CYST may occur.
more superficial, one incorporates the anterior aponeurotic sheath Persistent vitelline duct remnants between the GI tract and the anterior
of the rectus muscle medially, transitioning to external oblique abdominal wall may be associated with small intestine volvulus in
muscle and aponeurosis more laterally neonates
posterior, deeper layer consists of internal oblique and transversus Vitelline duct fistulas and cysts should be excised along with any
abdominis muscle accompanying fibrous cord.
anatomic considerations are the same for closure of transverse muscle-dividing URACHUS
incisions, either lateral to or crossing the midline Fibromuscular, tubular extension of the allantois that develops with the
PFANNENSTIEL INCISION descent of the bladder to its pelvic position.
used commonly for pelvic procedures Persistence of urachal remnants can result in CYSTS as well as
Distinguished by transverse skin and anterior rectus sheath incisions, FISTULAS to the urinary bladder with drainage of urine from the umbilicus
followed by rectus muscle retraction and longitudinal incision of the Treated by urachal excision and closure of any bladder defect that
peritoneum. may be present.
Irrespective of the incision type, suture apposition of abdominal wall tissues
during closure ideally is accomplished without great tension and with great Acquired Abnormalities
precision RECTUS ABDOMINIS DIASTASIS (or DIASTASIS RECTI)
Must appreciate all necessary anatomic distinctions to minimize the opportunity clinically evident separation of the rectus abdominis muscle pillars
for defective healing. results in a characteristic bulging of the abdominal wall in the epigastrium
In general, it is prudent to make incisions no larger than is necessary to safely sometimes mistaken for a ventral hernia
accomplish the operative goals. midline aponeurosis is intact and no hernia defect is present
LAPAROSCOPIC SURGERY may be
now natural orifice transluminal endoscopic surgery (NOTES) CONGENITAL
owed their development largely to the belief that avoidance of surgical result of a more lateral insertion of the rectus muscles to the ribs
injury to the abdominal wall is of significant benefit to the patient and costochondral junctions
OPEN SURGERY, a variety of devices are available to retract the abdominal ACQUIRED
wall and facilitate peritoneal exposure without subjecting the patient to occurring with advancing age, in obesity, or after pregnancy
excessively large incisions or surgical personnel to exhausting retraction tasks in postpartum setting, rectus diastasis tends to occur in women who are of
e.g. : BOOKWALTER, OMNI-TRACT and THOMPSON RETRACTORS advanced maternal age
BOOKWALTER RETRACTOR multiple or twin pregnancy
use for exposure of peritoneal structures during abdominal surgery deliver a high birth- weight infant
Valuable exposure aids that reduce the physical demands on easily identified on physical examination
personnel in the operating room and allow more complete focus on
visible in the mid epigastrium with Valsalva maneuver
the surgical site of interest.
edges of the rectus abdominis muscle, rigid with voluntary contraction, are
Congenital Abnormalities palpable along the entire length of the bulging area
abdominal wall layers begin to form in the first weeks after conception should not be mistaken for a ventral hernia
Prominent in the early embryonic abdominal wall Computed tomographic (CT) scanning
large central defect through which pass the vitelline provides an accurate means of measuring the distance between the
(OMPHALOMESENTERIC) duct rectus pillars
connects the embryonic and fetal midgut to the yolk sac
By: Rem Alfelor Page 3 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
Differentiate rectus diastasis from a true ventral hernia if clarification is
required.
Surgical correction by application of the broad midline aponeurosis
described for cosmetic indications and for alleviation of impaired
abdominal wall muscular function
introduce the risk of an actual ventral hernia
RECTUS SHEATH HEMATOMA
Terminal branches of the superior and inferior epigastric arteries course deep to
the posterior aspect of the left and right rectus abdominis muscles and enter the
posterior rectus sheath.
Hemorrhage from any of the network of collateralizing vessels within the
rectus sheath and muscles can result in a RECTUS SHEATH
HEMATOMA
History of major or minor blunt trauma may be elicited; less obvious events also
have been reported to cause this condition, such as sudden contraction of the
rectus muscles with coughing, sneezing, or any vigorous physical activity.
Described in the elderly and in those receiving anticoagulation therapy.
Sudden onset of unilateral abdominal pain that may be confused with lateralized ABDOMINAL WALL HERNIAS
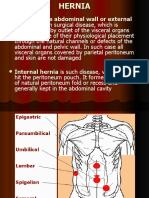
peritoneal disorders such as appendicitis. HERNIAS OF THE ANTERIOR ABDOMINAL WALL or VENTRAL HERNIAS
Below the arcuate line, a hematoma may cross the midline and cause bilateral represent defects in the parietal abdominal wall fascia and muscle through
lower quadrant pain. which intra-abdominal or preperitoneal contents can protrude
History and physical examination alone may be diagnostic. may be
Pain typically increases with contraction of the rectus muscles and a CONGENITAL
tender mass may be palpated ACQUIRED HERNIAS
Ability to appreciate an intra-abdominal mass is ordinarily degraded with develop through slow architectural deterioration of the muscular
contraction of the rectus muscles. aponeuroses or they may develop from failed healing of an anterior
FOTHERGILL'S SIGN abdominal wall incision (INCISIONAL HERNIA)
palpable abdominal mass that remains unchanged with contraction most common finding is a mass or bulge on the anterior abdominal wall, which
of the rectus muscles may increase in size with a Valsalva maneuver
Classically associated with rectus hematoma. May be asymptomatic or cause a considerable degree of discomfort, and
Hemoglobin level and hematocrit should be measured and coagulation studies generally enlarge over time.
should be performed. Physical examination reveals a bulge on the anterior abdominal wall that may
Abdominal ultrasonography reduce spontaneously, with recumbency, or with manual pressure
Show a solid or cystic mass within the abdominal wall depending on the hernia that cannot be reduced is described as INCARCERATED
chronicity of the bleeding. Requires emergent surgical correction.
CT Incarceration of an intestinal segment may be accompanied by
most definitive study to establish the correct diagnosis and to exclude nausea, vomiting, and significant pain
other disorders blood supply to the incarcerated bowel be compromised, the hernia
Magnetic resonance imaging (MRI) also has been used for this purpose is described as STRANGULATED
Specific treatment depends on the severity of the hemorrhage Localized ischemia may lead to infarction and perforation.
Small, unilateral, and stable hematomas may be observed without
patient hospitalization. PRIMARY VENTRAL HERNIAS (NONINCISIONAL)
Bilateral or large hematomas will likely require hospitalization and also termed TRUE VENTRAL HERNIAS
possibly resuscitation More properly named according to their anatomic location.
Need for transfusion or coagulation factor replacement is determined by EPIGASTRIC HERNIAS
the clinical circumstances. located in the midline between the xiphoid process and the
Reversal of warfarin (Coumadin) anticoagulation in the acute setting umbilicus
is frequently, but not always, necessary. generally small, may be multiple
Emergent operative intervention or angiographic embolization at elective repair are usually found to contain omentum or a portion
Required infrequently but may be necessary if hematoma of the falciform ligament
enlargement, free bleeding, or clinical deterioration occur. May be congenital and due to defective midline fusion of developing
Surgical therapy is used in the rare situations of failed angiographic lateral abdominal wall elements.
treatment or hemodynamic instability that precludes any other options. UMBILICAL HERNIAS
Operative goals are evacuation of the hematoma and ligation of any occur at the umbilical ring
bleeding vessel identified. may either be present at birth or develop gradually during the life of
Mortality from this condition is rare but has been reported in elderly the individual
patients requiring surgical treatment. Present in approximately 10 percent of all newborns and are more
common in premature infants.
Most congenital umbilical hernias close spontaneously by age 5
years.
If closure does not occur by this time, elective surgical repair
usually is advised.
Adults with small, asymptomatic umbilical hernias may be followed
clinically.
Surgical treatment is
By: Rem Alfelor Page 4 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
offered associated with a high wound infection risk (20%) and recurrence
if a hernia is observed to enlarge rate of 18.2% at 1 year
if it is associated with symptoms most applicable for the repair of incisional hernias when there are
if incarceration occurs converging needs to
Consist of primary sutured repair or placement of prosthetic a) avoid the use of prosthetic materials
mesh for larger defects (>2 cm) using open or laparoscopic b) Achieve a definitive repair.
methods. Most commonly this occurs in the setting of a contaminated or
SPIGELIAN HERNIAS potentially contaminated surgical field.
occur anywhere along the length of the Spigelian line or zone MESH REPAIR
aponeurotic band of variable width at the lateral border of the Gold standard in the elective management of most incisional hernias.
rectus abdominis Can be categorized according to the way in which the mesh is placed as
most frequent location of these rare hernias is at or slightly above well as its relationship to the abdominal wall fascia.
the level of the arcuate line Mesh placed as an underlay deep to the fascial defect
Not always clinically evident as a bulge and may come to medical (INTRAPERITONEAL OR PREPERITONEAL)
attention because of pain or incarceration. as an interlay either bridging the gap between the defect edges or
Patients with advanced liver disease, ascites, and umbilical hernia require within the abdominal wall musculoaponeurotic layers
special consideration. (INTRAPARIETAL)
Enlargement of the umbilical ring usually occurs in this clinical situation as a as an onlay (superficial to the fascial defect)
result of increased intra-abdominal pressure from uncontrolled ascites Laparoscopic repairs use an intraperitoneal underlay technique.
first line of therapy is can be characterized by type of material, each of which has a specified
aggressive medical correction of the ascites with diuretics density, porosity, and strength
dietary management Can be PROSTHETIC or BIOLOGIC.
paracentesis for tense ascites with respiratory compromise PERMANENT PROSTHETIC MESH implants are made of materials
Hernias usually are filled with ascitic fluid, but omentum or bowel that do not degrade over time
may enter the defect after large-volume paracentesis. ABSORBABLE MESHES are degraded, primarily by hydrolytic
Uncontrolled ascites may lead to skin breakdown on the protuberant hernia and enzyme activity.
eventual ascitic leak, which can predispose the patient to bacterial peritonitis. BIOLOGIC MESH
Patients with refractory ascites may be candidates for transjugular intrahepatic prepared from collagen-rich porcine, bovine, or human
portocaval shunting or eventual liver transplantation. tissues from which all antigenic cellular materials are
Umbilical hernia repair should be deferred until after the ascites is controlled. removed
Mesh materials can be chemically treated to cross-link a
INCISIONAL HERNIAS collagen molecule, which increases strength and durability at
10 to 20% of these patients have been estimated to develop hernias at the the cost of some impairment in host cellular ingrowth.
abdominal incision sites useful in the setting of contaminated or potentially
regarded as a wound healing failure contaminated fields but are very expensive and
cause of incisional hernia in any given case can be difficult to determine, but based on the most recent evidence, do not offer the durability
may all be contributory of permanent prosthetic meshes unless combined with a
primary repair
obesity
Over time, biologic meshderived collagen can be
primary wound healing defects
incorporated into the host tissue, remodeled, and eventually
multiple prior procedures replaced by host collagen.
prior incisional hernias reports show that hernia recurrence rates are excessive in
technical errors during repair this application
occur at sites of defective healing within the approximated incision or at the PROSTHETIC MESHES
suture puncture sites created during the closure, or both Principal advantages of are ease of use, relatively low cost,
most important distinctions in describing surgical management of incisional and durability.
hernias are ABSORBABLE MESHES
primary vs. mesh repair composed of the same materials as polysaccharide-derived
open vs. laparoscopic repair synthetic absorbable suture
Primary repair, even of small hernias (defects <3 cm), is associated with high Provide relatively inexpensive solutions for temporary
reported hernia recurrence rates abdominal wall support in highly contaminated or infected
Identified risk factors for recurrence were fields.
primary suture repair Use leaves patients with recurrent ventral hernias that can be
postoperative wound infection definitively repaired when permitted by improved local wound
prostatism conditions.
surgery for abdominal aortic aneurysm
Primary repair methods for incisional hernia include both simple suture closure
and components separation, and are open procedures.
Simple suture approximation of fascial defect edges predictably results in
a suture line under tension
Components separation hernia repair
entails the creation of large subcutaneous flaps lateral to the fascial
defect followed by incision of the external oblique muscles and, if
necessary, incision of the posterior rectus sheath bilaterally
fascial releases allow for primary apposition of the fascia under far
less tension than in simple primary repair
By: Rem Alfelor Page 5 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
Once the area encompassing all fascial defects is defined, a mesh is
fashioned to allow for sufficient overlap (minimum of 3 to 4 cm) under the
healthy abdominal wall.
After insertion into the abdomen, the mesh is fixed into position with
transfascial sutures placed circumferentially around the mesh and spiral
tacks placed according to surgeon preference
transfascial sutures contribute to excessive postoperative pain,
and some surgeons have eliminated them from the technique,
relying solely on spiral tacks for the strength of the repair
Recommended a minimum 5-cm overlap of mesh from defect
edge if transfascial sutures are not used.
OMENTUM
Surgical Anatomy
GREATER OMENTUM AND LESSER OMENTUM
fibro-fatty aprons that provide support, coverage, and protection for peritoneal
contents
begin to develop during the fourth week of gestation
OPEN MESH REPAIR GREATER OMENTUM
Generally requires incision or excision of the previous laparotomy scar, develops from the dorsal mesogastrium, which begins as a double-layered
with care taken to avoid injury to the underlying abdominal contents. structure
peritoneum and hernial sac are then dissected free from the abdominal spleen develops in between the two layers, and later in development the
wall fascia so that at least 3 to 4 cm of fascia is circumferentially exposed two layers fuse, giving rise to the intraperitoneal spleen and the
mesh can then be sutured into place using an underlay, onlay, interlay, gastrosplenic ligament
or "sandwich-style" (both underlay and onlay) method
fused layers then hang from the greater curvature of the stomach and
Most successful method is to extensively develop a preperitoneal space to
drape over the transverse colon, to which their posterior surface becomes
accommodate a large sheet of polypropylene or woven polyester mesh. fixed
Mesh, which is isolated from the peritoneal contents, is then secured to Gastrocolic ligament and the gastrosplenic ligament are those segments
the musculoaponeurotic tissues using interrupted nonabsorbable sutures. of the greater omental apron that connect the named structures.
Tissue ingrowth within the interstices of these mesh types results in dense In the adult, lies in between the anterior abdominal wall and the hollow
attachment to whatever tissues the mesh comes into contact with. viscera, and usually extends into the pelvis to the level of the symphysis
This effect is desirable when the mesh is located in the pubis.
preperitoneal position. LESSER OMENTUM
problems attributed to adherence of peritoneal contents to mesh are known as the HEPATODUODENAL AND HEPATOGASTRIC
chronic pain LIGAMENTS
bowel obstruction develops from the mesoderm of the septum transversum, which connects
fistulization to bowel the embryonic liver to the foregut
Polytetrafluoroethylene (PTFE) common bile duct, portal vein, and hepatic artery are located in the
does not become incorporated into the surrounding tissues inferolateral margin of the lesser omentum
not associated with dense adhesions to the intraperitoneal Also forms the anterior margin of the foramen of Winslow.
structures blood supply to the greater omentum is derived from the RIGHT AND LEFT
Commonly used for intraperitoneal applications. GASTROEPIPLOIC ARTERIES
Irrespective of technique, the recurrence rate after open incisional hernia Venous drainage parallels the arterial supply to a great extent, with the LEFT
repair can be high AND RIGHT GASTROEPIPLOIC VEINS ultimately draining into the portal
LAPAROSCOPIC INCISIONAL HERNIA REPAIR system.
new gold standard for abdominal wall reconstruction for ventral hernia
recurrence rate of only 3.4% Physiology
Secondary to technical errors committed early in the surgeons' omentum tended to wall off areas of infection and limit the spread of
experience that were avoided during the latter cases. intraperitoneal contamination
associated with statistically fewer wound complications, fewer overall termed the omentum the abdominal policeman
complications, and a lower recurrence rate than use of the open technique intrinsic hemostatic characteristics of the omentum
benefits of the minimally invasive technique are achieved by concentration of tissue factor in omentum is over twice the amount per
eliminating the requisite large abdominal incision at a location gram of that found in muscle
where the abdominal wall blood supply has previously been facilitates activation of coagulation at sites of inflammation, ischemia,
compromised infection, or trauma within the peritoneal cavity
Entire undersurface of the abdominal wall can be examined, which Consequent local production of fibrin contributes to the ability of the
often reveals multiple secondary defects that might not otherwise be omentum to adhere to areas of injury or inflammation.
appreciated.
Generally involves laterally placed ports for midline defects and OMENTAL INFARCTION
contralaterally placed ports for lateral defects. Interruption of the blood supply to the omentum
All adhesions to the anterior abdominal wall are divided, with great care rare cause of an acute abdomen
taken not to injure the intestine either directly or with thermal or electrical may be
energy secondary to torsion of the omentum around its vascular pedicle
Contents of the hernial sac are completely reduced, but in contrast to thrombosis or vasculitis of the omental vessels
open repairs, the sac itself is left in situ. Omental venous outflow obstruction.
Diagnosis is most likely to be made in male adults.
By: Rem Alfelor Page 6 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
Depending on the location of the infarcted omental tissue, this disease process In the region of the colon, the dorsal mesentery is known as the
may mimic MESOCOLON.
Appendicitis
Cholecystitis
Diverticulitis
perforated peptic ulcer
ruptured ovarian cyst
Present with localized right lower quadrant, right upper quadrant, or left lower
quadrant pain.
Although a mild degree of nausea may be present, patients do not usually have
concomitant intestinal symptoms.
Physical examination
mild tachycardia and a low-grade fever
Abdominal examination: tender, palpable mass associated with guarding
and rebound tenderness
Either abdominal CT or ultrasonography will show a localized, inflammatory
mass of fat density.
Treatment of depends on which the diagnosis is made
patients who are not toxic and whose abdominal imaging results are
convincing, supportive care is sufficient
many cases are indistinguishable from surgical conditions with immediate
surgical implications, such as appendicitis Anatomic relationships of intestinal mesentery to the retroperitoneum after completion of intestinal
Laparoscopic exploration offers the opportunity to establish an rotation during fetal development. art. = artery; sup. = superior; transv. = transverse.
accurate diagnosis and determine the most appropriate treatment.
Resection of the infarcted tissue results in rapid resolution of symptoms. During embryonic development, after the 270-degree counterclockwise rotation
of the herniated midgut, the reduced mesentery achieves its final fixation state.
OMENTAL CYSTS segments at the duodenum, ascending colon, and descending colon
Cystic lesions of the omentum and mesentery are related disorders, likely become fixed to the retroperitoneum
resulting from either peritoneal inclusions or degeneration of lymphatic small intestine mesentery, transverse colon mesentery and the sigmoid
structures colon mesentery remain mobile
less common than mesenteric cysts Defects in the normal developmental steps of intestinal rotation result in
Present as an asymptomatic abdominal mass or may cause abdominal pain with malrotation disorders.
or without appreciable mass or distention.
Physical examination: reveal a freely mobile intra-abdominal mass.
Mesocolic hernia of
Both CT and abdominal ultrasound reveal a well circumscribed, cystic mass small bowel into a
lesion arising from the greater omentum. retrocolic hernial sac
posterior to the
Treatment involves resection of all symptomatic omental cysts descending colon
Accomplished using laparoscopic techniques. mesentery. Hernias of
this type, as well as
hernias into paraduodenal recesses, result
OMENTAL NEOPLASMS from abnormal fixation of mesenteric
Primary tumors of the omentum are uncommon. structures during the course of intestinal
rotation. a. = artery; v. = vein.
Benign tumors of the omentum include
Lipomas
Myxomas
Desmoid tumors. root of the small intestine mesentery wall normally courses in an oblique
Primary malignant tumors of the omentum are considered mesodermally derived direction, from the left upper quadrant at the ligament of Treitz to the right lower
stromal tumors quadrant at the ileocecal valve and the fixed cecum
associated immunohistochemical characteristics of GI stromal tumors Small and large intestine mesenteries serve as the major pathway for arterial,
(e.g. c-kit immunopositivity) venous, lymphatic, and neural structures coursing to and from the bowel.
Metastatic tumors of the omentum are common Anatomic anomalies of the mesentery related to rotational disorders can lead to
paraduodenal or mesocolic hernias
metastatic ovarian cancer showing the highest preponderance of omental
Can present as chronic or acute intestinal obstruction in children or adults.
involvement.
Malignant tumors of the stomach, small intestine, colon, pancreas, biliary
SCLEROSING MESENTERITIS
tract, uterus, and kidney may also metastasize to the omentum.
also referred to as MESENTERIC PANNICULITIS or MESENTERIC
LIPODYSTROPHY
MESENTERY
chronic inflammatory and fibrotic process that involves a portion of the intestinal
Surgical Anatomy mesentery
Develops from mesenchyme that attaches the foregut, midgut, and hindgut to No gender or race predominance, but the condition is most commonly
the posterior abdominal wall. diagnosed in individuals >50 years of age.
During embryonic maturation, this mesenchyme forms the dorsal mesentery. etiology of this process is unknown
In the region of the stomach, the dorsal mesentery becomes the greater cardinal feature is increased tissue density within the mesentery
omentum localized and associated with a discrete non-neoplastic mesenteric mass or
In the region of the jejunum and ileum the dorsal mesentery becomes the more diffuse
mesentery proper. Sometimes involving large swaths of mesentery without well-defined
borders.
By: Rem Alfelor Page 7 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
Varying relative degrees of fat tissue degeneration, inflammation, and fibrosis on Colchicine
histologic examination, which gives rise to the various terms used to describe Tamoxifen
this condition. cyclophosphamide
MESENTERIC LIPODYSTROPHY
used when the inflammatory and fibrotic components are small MESENTERIC CYSTS
MESENTERIC PANNICULITIS Benign lesions with an incidence of <1 in 100,000.
Signifies an increased inflammatory component with replacement of etiology of such cysts remains unknown, but several theories regarding their
degenerative fatty elements. development have been put forward, including that they are caused by
SCLEROSING MESENTERITIS degeneration of the mesenteric lymphatics
signifies a major fibrotic component Arise as a congenital anomaly.
sometimes referred to as RETRACTILE MESENTERITIS to may be asymptomatic or may cause symptoms of a mass lesion
describe mesenteric retraction and shortening associated with Acute abdominal pain secondary to a mesenteric cyst is generally caused by
scarring rupture or torsion of the cyst or by acute hemorrhage into the cyst
discrete mass may be up to 40 cm in diameter chronic intermittent abdominal pain secondary to compression of adjacent
Typically present with symptoms of a mass lesion. Structures or spontaneous torsion followed by detorsion of the cyst.
Abdominal pain is the most frequent presenting symptom, followed by the Can be the cause of nonspecific symptoms such as anorexia, nausea, vomiting,
presence of a nonpainful mass or, more rarely, intestinal obstruction. fatigue, and weight loss.
Discovered incidentally when imaging studies (most frequently abdominal CT Physical examination: mass lesion that is mobile only from the patient's right to
scanning) are performed for unrelated reasons. left or left to right (Tillaux's sign)
CT of the abdomen In contrast to the findings with omental cysts, this should be freely mobile
verify the presence of a mass lesion or area of the mesentery with a in all directions.
higher density than found in normal mesenteric tis all have been used to evaluate patients with mesenteric cysts
frequently involve the vascular structures in the mesenteric root CT
cannot definitively distinguish sclerosing mesenteritis from a primary or abdominal ultrasound
secondary mesenteric tumor MRI
identification of a "fat ring sign" or hypodense zone around the mass
area has been suggested as a means of distinguishing sclerosing
mesenteritis from lymphoma
presence of a hyperattenuating stripe also has been suggested as a
radiologic finding that would favor a diagnosis of mesenteritis
Computed tomographic coronal section of a
focus of sclerosing mesenteritis at the
mesenteric root, straddling major proximal
branches of the superior mesenteric artery.
The location of the mass restricted surgical
options to biopsy and confirmation of
diagnosis.
Computed tomographic scan of a mesenteric cyst. The unilocular appearance without an
associated solid component strongly suggests the diagnosis of benign cyst.
Computed tomographic scan of sclerosing mesenteritis (mesenteric lipodystrophy). This condition cannot easily be
distinguished from a neoplasm of the mesentery on radiologic study. In this case, the study showed "fatty
mesenteric tumor with involvement of mesenteric vessels," and "mesenteric lipodystrophy" was demonstrated by imaging modalities reveals a cystic structure without a solid component in the
biopsy findings at exploration. The finding of a hyperattenuating stripe around the lesion, as seen in this image, has central abdomen
been associated with the diagnosis of mesenteritis . Structures are generally unilocular but may on occasion be multiple or
multilocular.
Irrespective of the imaging method used, it may be difficult to distinguish
Surgery has been used most frequently to establish a diagnosis and to rule out a
these cystic masses from rare solid mesenteric tumors with cystic
neoplastic process components, such as a cystic stromal tumor or mesothelioma.
extent and location of mesenteric involvement defines options for surgical
intervention MESENTERIC CYSTIC LYMPHANGIOMA
simple biopsy, bowel and mesenteric resection can be considered in cases in
Present as numerous, often large cysts in the setting of abdominal pain.
which it is technically feasible based on mass size and the ability to avoid injury
Can be difficult to treat and almost invariably recur after excision.
to the small intestine blood supply
When symptomatic, SIMPLE MESENTERIC CYSTS are surgically excised
involvement of the vascular structures at the mesenteric root makes
either openly or laparoscopically when feasible.
resection unfeasible
Cyst unroofing or marsupialization is not recommended, because mesenteric
ostomy of some type for fecal diversion in the face of obstruction can be
cysts have a high propensity to recur after drainage alone.
considered
On rare occasion, adjacent mesentery may be densely adherent to the cyst or
use of positron emission tomography with CT scanning
mesenteric vessels must be sacrificed to achieve complete excision
effective in ruling out neoplasia for focal mesenteric masses, which leaves
bowel resection is performed
the sclerosing mesenteritis diagnosis a one of exclusion
process appears to be self-limited
Mesenteric Tumors
May even demonstrate regression if followed with interval imaging studies.
Primary tumors of the mesentery are rare.
Clinical symptoms are very likely to improve without intervention, and therefore
Benign tumors of the mesentery include
aggressive surgical treatments are generally not indicated.
Lipoma
problematic cases that are not amenable to resection because of widespread
mesenteric involvement or unfavorable location cystic lymphangiomas
Medical treatment has been given to alleviate severe symptoms. Desmoid tumors.
Corticosteroids Primary malignant tumors of the mesentery are similar to those described for the
omentum.
By: Rem Alfelor Page 8 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
Liposarcomas may all lead to retroperitoneal infection with or without abscess formation
leiomyosarcomas Retrocecal appendicitis
malignant fibrous histiocytomas perforated duodenal ulcers
lipoblastomas pancreatitis
lymphangiosarcomas diverticulitis
Metastatic small intestine carcinoid in mesenteric lymph nodes may exceed Substantial space and rather nondiscrete boundaries of the retroperitoneum
the bulk of primary disease and compromise blood supply to the bowel. allow some retroperitoneal abscesses to become quite large before diagnosis.
Treatment of mesenteric malignancies involves wide resection of the mass. RETROPERITONEAL ABSCESS
Proximity to the blood supply to the intestine, such resections may be presents with pain, fever, and malaise
technically unfeasible or involve loss of substantial lengths of bowel. Site of the patient's pain may be variable and can include the back, pelvis,
or thighs.
RETROPERITONEUM Clinical findings: tachypnea and tachycardia.
Erythema may be observed around the umbilicus or flank
analogous to the ecchymosis seen in these locations after
massive retroperitoneal hemorrhage (Cullen's sign and Grey
Turner's sign, respectively)
Palpable flank or abdominal mass may be present.
Laboratory evaluation: elevated white blood cell count
CT
diagnostic imaging modality of choice
demonstrate stranding of the retroperitoneal soft tissues and/or a
unilocular or multilocular collection
Computed tomographic scan of a
retroperitoneal abscess complicating
complex, surgically treated
retroperitoneal infection that had
resulted from ampullary perforation at
the time of endoscopic retrograde
cholangiopancreatography. This
Surgical Anatomy pattern of infection may be difficult to
Although ectodermal, mesodermal, and endodermal contributions to the treat and may result in multiple
interventions, such as percutaneous
contents of the retroperitoneum, embryonic mesoderm predominates in the drainage, before resolution.
developing retroperitoneal space.
From the intermediate mesoderm arise the organs of the urinary and genital
systems
lateral plate mesoderm eventually divides into two layers, the parietal layer and
the visceral layer Management of retroperitoneal infections includes
Layers eventually become the pleura, pericardium, peritoneum, and 1) identification and treatment of the underlying condition
retroperitoneum. 2) IV administration of antibiotics
RETROPERITONEUM 3) drainage of all well-defined collections
space between the posterior envelopment of the peritoneum and the unilocular abscesses may be drained percutaneously under CT guidance
posterior body wall Multilocular collections usually require operative intervention for adequate
RETROPERITONEAL SPACE drainage.
bounded superiorly by the diaphragm, posteriorly by the spinal Because of the large size of the retroperitoneal space, patients with
column and iliopsoas muscles, and inferiorly by the levator ani retroperitoneal abscesses usually do not seek treatment until the abscess is
muscles advanced
Although technically bounded anteriorly by the posterior reflection of the Mortality rate for retroperitoneal abscess, even when the abscess is drained,
peritoneum, the anterior border of the retroperitoneum is quite convoluted, has been reported to be as high as 25%, or even higher in rare cases of
extending into the spaces in between the mesenteries of the small and necrotizing fasciitis of the retroperitoneum.
large intestine.
Because of the rigidity of the superior, posterior, and inferior boundaries, RETROPERITONEAL FIBROSIS
and the compliance of the anterior margin, retroperitoneal tumors tend to class of disorders characterized by hyperproliferation of fibrous tissue in the
expand anteriorly toward the peritoneal cavity retroperitoneum
organs and structures that reside within the retroperitoneum may be a
primary disorder as in idiopathic retroperitoneal fibrosis, also known as
Ormond disease
Secondary reaction to an inciting inflammatory process, malignancy, or
medication.
IDIOPATHIC RETROPERITONEAL FIBROSIS
Rare disorder, usually affecting 0.5 in 100,000 patients annually.
Men are twice as likely to be affected as women
Retroperitoneal Infections no predilection for any particular ethnic group
Posterior reflection of the peritoneum limits the spread of most intra-abdominal Primarily affects individuals in the fourth to the sixth decades of life.
infections to the peritoneum. allergic or autoimmune mechanism
Source of retroperitoneal infections is usually an organ contained within or
abutting the retroperitoneum.
By: Rem Alfelor Page 9 of 10
Schwartz Chap 35: Abdominal Wall, Omentum, Mesentery and Retroperitoneum
Circulating antibodies to ceroid, a lipoproteinaceous by-product of palpation of an abdominal or flank mass
vascular atheromatous plaque oxidation, are present in >90% of lower extremity edema (unilateral or bilateral)
patients Diminished lower extremity pulses (unilateral or bilateral).
Early inflammatory reaction involves predominately helper T cells, plasma Laboratory evaluation
cells, and macrophages, but these are subsequently replaced by elevated blood urea nitrogen and/or creatinine level
collagen-synthesizing fibroblasts
erythrocyte sedimentation rate almost always is elevated
Infiltrate is indistinguishable from that seen with periadventitial
imaging modalities
involvement in aortic aneurysmal disease, Riedel's thyroiditis,
sclerosing cholangitis, and Peyronie's disease. ABDOMINAL AND LOWER EXTREMITY ULTRASONOGRAPHY
fibrotic process begins in the retroperitoneum just below the level of the least invasive imaging procedure, but results are technician
renal arteries dependent
Gradually expands, encasing the ureters, inferior vena cava, aorta, useful if iliocaval compressive or renal symptoms predominate
mesenteric vessels, or sympathetic nerves. Lower extremity ultrasonography may show deep vein
Bilateral involvement is noted in 67% of cases. thrombosis
may also occur secondary to a variety of inflammatory conditions or as an Abdominal ultrasonography may identify a mass lesion or
allergic reaction to a medication hydronephrosis.
abdominal aortic aneurysm IV PYELOGRAPHY
Once the diagnostic procedure of choice, but less commonly used
pancreatitis
today.
histoplasmosis
If the ureters are involved, the findings of IV pyelography will include
tuberculosis ureteral compression
actinomycosis ureteral deviation toward the midline
associated with a variety of malignancies, including hydronephrosis
prostate ABDOMINOPELVIC CT WITH ORAL AND IV CONTRAST AGENTS
pancreatic, and gastric cancers imaging procedure of choice
non-Hodgkin's lymphoma Allow the extent of the fibrotic process to be determined.
stromal tumors If renal function is diminished so that the use of IV contrast agents
carcinoid tumors must be avoided, the ability to characterize retroperitoneal tissue
described in association with autoimmune disorders, including planes will be reduced.
ankylosing spondylitis In this case, MRI may be used
systemic lupus erythematosus - signal intensity of the fibrotic process is discrete from
Wegener's granulomatosis that of muscle or fat
polyarteritis nodosa - Generally provides a good assessment of the degree of
iliocaval involvement.
strongest case for a causal relationship between medication and retroperitoneal
Once a mass lesion is identified, biopsy of the mass should be performed to rule
fibrosis is made for METHYSERGIDE
out a retroperitoneal malignancy
Semisynthetic ergot alkaloid used in the treatment of migraine headaches.
Specimen may be obtained using image-guided techniques or a surgical
Other medications that have been linked to retroperitoneal fibrosis include
retroperitoneal biopsy procedure, which may be performed
beta blockers laparoscopically or during open laparotomy.
hydralazine Once malignancy, drug effects, and infectious causes are ruled out, treatment of
methyldopa is instituted.
ENTACAPONE Corticosteroids, with or without surgery, are the mainstay of medical therapy.
inhibits catechol-O-methyltransferase Surgical treatment consists primarily of ureterolysis or ureteral stenting
used as an adjunct with levodopa in the treatment of Parkinson's Required in patients who present with moderate or massive
disease hydronephrosis.
Regresses on discontinuation of these medications. Laparoscopic ureterolysis has been shown to be as efficacious as open
Presenting symptoms depend on the structure or structures affected by the surgery in addressing this problem.
fibrotic process. Patients with iliocaval thrombosis require anticoagulation.
Initially, patients complain of the insidious onset of dull, poorly localized Prednisone is initially administered at a relatively high dose (60 mg every other
abdominal pain. day for 2 months)
Sudden-onset or severe abdominal pain may signify acute Then gradually tapered over the next 2 months.
mesenteric ischemia. Therapeutic efficacy is assessed on the basis of patient symptoms and
Other symptoms of retroperitoneal fibrosis include interval imaging studies.
unilateral leg swelling Used to treat patients who respond poorly to corticosteroids.
intermittent claudication Cyclosporin
oliguria Tamoxifen
hematuria Azathioprine
Dysuria. Overall prognosis in idiopathic retroperitoneal fibrosis is good, with 5-year
Findings on physical examination vary with the retroperitoneal structure survival rates of 90 to 100%.
involved. Because long term recurrences have been described, lifelong follow-up is
Hypertension warranted.
By: Rem Alfelor Page 10 of 10
Potrebbero piacerti anche
- Ruba Ali - Home Base GuideDocumento173 pagineRuba Ali - Home Base GuideShahenda El-MenshawyNessuna valutazione finora
- HLTAAP001 - Horia RevisedDocumento74 pagineHLTAAP001 - Horia RevisedYouYou Tube80% (5)
- Inguinal Hernias Lecture by Wilfredo Tayag, M.D, FPCS Schwartz Principle of Surgery 10 EditionDocumento9 pagineInguinal Hernias Lecture by Wilfredo Tayag, M.D, FPCS Schwartz Principle of Surgery 10 EditionMarlon molano100% (9)
- Serial Sections of 10 MM Pig EmbryoDocumento41 pagineSerial Sections of 10 MM Pig EmbryoChristalie Bea FernandezNessuna valutazione finora
- Strong CurvesDocumento2 pagineStrong CurvesCarmine100% (1)
- Schwartz UrologyDocumento10 pagineSchwartz UrologyRem Alfelor100% (1)
- Os 206: Pe of The Abdomen - ©spcabellera, Upcm Class 2021Documento4 pagineOs 206: Pe of The Abdomen - ©spcabellera, Upcm Class 2021Ronneil BilbaoNessuna valutazione finora
- Head and Neck SchwartzDocumento10 pagineHead and Neck Schwartz2013SecBNessuna valutazione finora
- Basic Emergency Skills in Trauma Part 3 - Penetrating Abdoninal Injury - Dr. Oliver BelarmaDocumento3 pagineBasic Emergency Skills in Trauma Part 3 - Penetrating Abdoninal Injury - Dr. Oliver BelarmaRaquel ReyesNessuna valutazione finora
- Schwartz Chapter 33 SpleenDocumento20 pagineSchwartz Chapter 33 SpleenGay Solas Epalan100% (1)
- OB Williams Chap 2 Maternal AnatomyDocumento7 pagineOB Williams Chap 2 Maternal AnatomyRem Alfelor0% (1)
- OB Williams Chap 2 Maternal AnatomyDocumento7 pagineOB Williams Chap 2 Maternal AnatomyRem Alfelor0% (1)
- OB Williams Chap 2 Maternal PhysiologyDocumento9 pagineOB Williams Chap 2 Maternal PhysiologyRem Alfelor100% (2)
- Progressive Muscle Relaxation Script PDFDocumento3 pagineProgressive Muscle Relaxation Script PDFRayNessuna valutazione finora
- 8.anterior GuidanceDocumento15 pagine8.anterior GuidanceVikas AggarwalNessuna valutazione finora
- Core Knowledge in Orthopaedics - SpineDocumento330 pagineCore Knowledge in Orthopaedics - Spinedexx12780% (5)
- Abdominal Wall, Omentum, Mesentery and RetroperitoneumDocumento8 pagineAbdominal Wall, Omentum, Mesentery and RetroperitoneumRae Marie AquinoNessuna valutazione finora
- GYNE 4.04 Pelvic Organ DisordersDocumento7 pagineGYNE 4.04 Pelvic Organ DisordersGray SnellNessuna valutazione finora
- 0.6 Surgery Trans PDFDocumento17 pagine0.6 Surgery Trans PDFJoy ManzanoNessuna valutazione finora
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Documento13 pagineSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101Nessuna valutazione finora
- Schwartz Cpap 16 Skin and Subcutaneous TissueDocumento16 pagineSchwartz Cpap 16 Skin and Subcutaneous TissueRem AlfelorNessuna valutazione finora
- Operative Procedures: 1130 SRB's Manual of SurgeryDocumento1 paginaOperative Procedures: 1130 SRB's Manual of SurgerymadhuNessuna valutazione finora
- 4.2 Abdominal Wall Hernia (Jerome Villacorta's Conflicted Copy 2014-03-22)Documento7 pagine4.2 Abdominal Wall Hernia (Jerome Villacorta's Conflicted Copy 2014-03-22)Miguel C. DolotNessuna valutazione finora
- Abdominal Access TechniquesDocumento7 pagineAbdominal Access TechniquesdrmarcsNessuna valutazione finora
- Gastrectomy 1Documento86 pagineGastrectomy 1Mysnow OpalNessuna valutazione finora
- Operative Surgery ManualDocumento273 pagineOperative Surgery Manualvikeshramkelawon8422100% (1)
- 1.40 (Surgery) GIT Surgical Diseases - Diagnostics - Obesity ManagementDocumento10 pagine1.40 (Surgery) GIT Surgical Diseases - Diagnostics - Obesity ManagementLeo Mari Go LimNessuna valutazione finora
- Chapter Summary - PANCREAS Final (Schwartz) PDFDocumento19 pagineChapter Summary - PANCREAS Final (Schwartz) PDFMiguel Cuevas DolotNessuna valutazione finora
- Open Inguinal Hernia RepairDocumento6 pagineOpen Inguinal Hernia RepairKris TejereroNessuna valutazione finora
- Bowel AnastomosisDocumento30 pagineBowel AnastomosismrashaiedehNessuna valutazione finora
- HEAD AND NECK 1.robbins & Cotran Pathologic Basis of Disease ReviewerDocumento14 pagineHEAD AND NECK 1.robbins & Cotran Pathologic Basis of Disease ReviewerSeff Causapin100% (1)
- 5 General Principles in TraumaDocumento10 pagine5 General Principles in TraumaMyrtle Yvonne RagubNessuna valutazione finora
- Surgery EntranceDocumento352 pagineSurgery EntranceDipesh Shrestha100% (1)
- Topic - Diaphragmatic HerniasDocumento13 pagineTopic - Diaphragmatic HerniasOlga CerlatNessuna valutazione finora
- Surgery BreastDocumento11 pagineSurgery BreastLady ElocinNessuna valutazione finora
- Maternal AnatomyDocumento9 pagineMaternal AnatomyAika Agudilla100% (2)
- IncisionalDocumento50 pagineIncisionalelsayedsalemNessuna valutazione finora
- Phyllodes TumorDocumento20 paginePhyllodes TumorManuela KarinaaNessuna valutazione finora
- Pelvic AnatomyDocumento0 paginePelvic AnatomyAlynne De Luna PascuaNessuna valutazione finora
- 3 Surgery - Mediastinum and PleuraDocumento6 pagine3 Surgery - Mediastinum and PleuraCassey Koi FarmNessuna valutazione finora
- Salivary Gland 2001 01Documento36 pagineSalivary Gland 2001 01theibban89Nessuna valutazione finora
- Abdominal Wall Edited WordDocumento13 pagineAbdominal Wall Edited WordKennie RamirezNessuna valutazione finora
- Surgery Trans 2a - Fluid and Electrolyte Management of The Surgical PatientDocumento14 pagineSurgery Trans 2a - Fluid and Electrolyte Management of The Surgical PatientJoan Caacbay De GuzmanNessuna valutazione finora
- LEC 15.1 - Abdominal HerniasDocumento37 pagineLEC 15.1 - Abdominal HerniasTudor CorneaNessuna valutazione finora
- Peptic UlcerDocumento4 paginePeptic UlcerEris Abdul AzizNessuna valutazione finora
- Inguinal HerniaDocumento15 pagineInguinal HerniaTessa LaiNessuna valutazione finora
- Pancreatic Cancer: Aziz Ahmad, MD Surgical Oncology Mills-Peninsula Hospital April 23, 2011Documento18 paginePancreatic Cancer: Aziz Ahmad, MD Surgical Oncology Mills-Peninsula Hospital April 23, 2011mywifenoor1983Nessuna valutazione finora
- SURGERY Lecture 3 - Abdominal Hernia (Dr. Mendoza)Documento12 pagineSURGERY Lecture 3 - Abdominal Hernia (Dr. Mendoza)Medisina101100% (1)
- Benign Gynecologic LesionsDocumento103 pagineBenign Gynecologic Lesions201286% (7)
- Breast CancerDocumento32 pagineBreast Cancerjames garcia100% (1)
- 0.7 Surgery Trans PDFDocumento29 pagine0.7 Surgery Trans PDFJoy ManzanoNessuna valutazione finora
- Pulmonary PathologyDocumento6 paginePulmonary PathologyjamesjaanNessuna valutazione finora
- Surgery ReviewDocumento12 pagineSurgery ReviewJo AnneNessuna valutazione finora
- Schwartz's Hemostasis, Surgical BleedingDocumento33 pagineSchwartz's Hemostasis, Surgical BleedingArifHidayat100% (4)
- C 10 + 11 GALLBLADDER AND BILIARY TRACT Part1Documento45 pagineC 10 + 11 GALLBLADDER AND BILIARY TRACT Part1mikaaa00050% (2)
- Omphalocelevsgastroschisis 160810122732Documento23 pagineOmphalocelevsgastroschisis 160810122732LNICCOLAIO100% (1)
- Surgery II - Pancreas 2014Documento20 pagineSurgery II - Pancreas 2014Medisina101Nessuna valutazione finora
- Breast CancerDocumento4 pagineBreast CancerMaikka IlaganNessuna valutazione finora
- GYNE 4.06-Benign and Malignant Lesions of UterusDocumento7 pagineGYNE 4.06-Benign and Malignant Lesions of UterusGray SnellNessuna valutazione finora
- Bile Duct InjuryDocumento62 pagineBile Duct InjuryShashidhara Puttaraj100% (1)
- Excision of Preauricular Pits and SinusesDocumento7 pagineExcision of Preauricular Pits and SinusesHNessuna valutazione finora
- GIT Fully DoneDocumento14 pagineGIT Fully DoneTirtha Taposh100% (1)
- Gestroresectional SyndromesDocumento18 pagineGestroresectional SyndromesAna CotomanNessuna valutazione finora
- 2014-06-03-Anterior Abdominal Wall Slides PDFDocumento18 pagine2014-06-03-Anterior Abdominal Wall Slides PDFGrigore PopaNessuna valutazione finora
- Inguinal Region AnatomyDocumento6 pagineInguinal Region AnatomysimonaNessuna valutazione finora
- Anatomy of The Anterior Abdominal Wall & Groin PDFDocumento4 pagineAnatomy of The Anterior Abdominal Wall & Groin PDFmoetazNessuna valutazione finora
- Peretul AbdominalDocumento9 paginePeretul AbdominalBotond LukacsNessuna valutazione finora
- Anatomy - B. Rabischong - GRDocumento20 pagineAnatomy - B. Rabischong - GRAnonymous UHnQSkxLBDNessuna valutazione finora
- Chapter 2 Maternal AnatomyDocumento9 pagineChapter 2 Maternal AnatomyRem Alfelor100% (2)
- POST-TEST Mock Written Diplomate ExaminationDocumento62 paginePOST-TEST Mock Written Diplomate ExaminationRem AlfelorNessuna valutazione finora
- Chap 8 Prenatal CareDocumento9 pagineChap 8 Prenatal CareRem AlfelorNessuna valutazione finora
- Chapter 2 Maternal AnatomyDocumento9 pagineChapter 2 Maternal AnatomyRem Alfelor100% (2)
- Chapter 4 Maternal PhysiologyDocumento12 pagineChapter 4 Maternal PhysiologyRem AlfelorNessuna valutazione finora
- Chapter 3 Congenital Genitourinary AbnormalitiesDocumento4 pagineChapter 3 Congenital Genitourinary AbnormalitiesRem AlfelorNessuna valutazione finora
- Psychiatric History and Mental Status ExaminationDocumento6 paginePsychiatric History and Mental Status ExaminationRem AlfelorNessuna valutazione finora
- Case 01 - Maternal PhysiologyDocumento5 pagineCase 01 - Maternal PhysiologyRem AlfelorNessuna valutazione finora
- Community Medicine Cavite ReportDocumento46 pagineCommunity Medicine Cavite ReportRem AlfelorNessuna valutazione finora
- Retinoblastoma QuizDocumento1 paginaRetinoblastoma QuizRem AlfelorNessuna valutazione finora
- Generalities of Blood and Its ElementsDocumento3 pagineGeneralities of Blood and Its ElementsRem AlfelorNessuna valutazione finora
- Ent Case Report Acute Otitis Media Stage IIIDocumento12 pagineEnt Case Report Acute Otitis Media Stage IIIRem Alfelor100% (1)
- Comprehensive Gynecology Uterine BleedingDocumento7 pagineComprehensive Gynecology Uterine BleedingRem AlfelorNessuna valutazione finora
- Diagnosis TopisDocumento101 pagineDiagnosis TopisGita Nur SiwiNessuna valutazione finora
- Hamstrings - Mechanics, Injury and Rehabilitation. Christopher NorrisDocumento9 pagineHamstrings - Mechanics, Injury and Rehabilitation. Christopher NorrisPascu MariusNessuna valutazione finora
- Curvy Workout EbDocumento2 pagineCurvy Workout Ebsuz8585Nessuna valutazione finora
- Tallgren1972 PDFDocumento13 pagineTallgren1972 PDFgermanpuig100% (1)
- Chapter 8 Muscular Analysis of Upper Extremity ExercisesDocumento20 pagineChapter 8 Muscular Analysis of Upper Extremity ExercisesAya AmerNessuna valutazione finora
- Chapter04 Massage TechniquesDocumento40 pagineChapter04 Massage TechniquesRonn LlaveNessuna valutazione finora
- Cinahl Rotator Cuff InjuriesDocumento11 pagineCinahl Rotator Cuff InjurieslizardbeeNessuna valutazione finora
- Body Systems Chart System Illustration Structures Function: DigestiveDocumento3 pagineBody Systems Chart System Illustration Structures Function: DigestiveMicaela DNessuna valutazione finora
- Ortho MCQs Quastions 1Documento192 pagineOrtho MCQs Quastions 1Nofouz MaswadaNessuna valutazione finora
- Chapter 12 VocabDocumento2 pagineChapter 12 VocabwdsfNessuna valutazione finora
- Attune Knee Single Use Instrument SetDocumento72 pagineAttune Knee Single Use Instrument SetJason100% (2)
- Anatomy and Physiology (Respiratory System)Documento3 pagineAnatomy and Physiology (Respiratory System)Kirstin del CarmenNessuna valutazione finora
- Orthodontic Treatment of A Severe Combined Anterior and Posterior Open Bite Case, Involving AnkylosisDocumento8 pagineOrthodontic Treatment of A Severe Combined Anterior and Posterior Open Bite Case, Involving Ankylosisgifar ihsanNessuna valutazione finora
- Anatomy of The Lower LimbDocumento3 pagineAnatomy of The Lower LimbRayNessuna valutazione finora
- The Oral Cavity Lecture NotesDocumento6 pagineThe Oral Cavity Lecture NotesFarizan hasyim Hari prathamaNessuna valutazione finora
- Skeletal System ReviewerDocumento4 pagineSkeletal System ReviewerMadelle Capending DebutonNessuna valutazione finora
- Calipers - Lower ExtremityDocumento40 pagineCalipers - Lower ExtremityNivetha RavikumarNessuna valutazione finora
- Design and Fabrication of A Full Denture With Shorthened Dental Arch and Flat Ridge in MandibularDocumento10 pagineDesign and Fabrication of A Full Denture With Shorthened Dental Arch and Flat Ridge in MandibulardinaNessuna valutazione finora
- An Electromyographic Analysis of Trunk and Hip Extensor Muscles During Bridging Exercises - Effect of Voluntary Control of The Pelvic TiltDocumento3 pagineAn Electromyographic Analysis of Trunk and Hip Extensor Muscles During Bridging Exercises - Effect of Voluntary Control of The Pelvic TiltNicolás ManonniNessuna valutazione finora
- Treatment of An Ankylosed Central Incisor by Single Tooth Dento-Osseous Osteotomy and A Simple Distraction DeviceDocumento9 pagineTreatment of An Ankylosed Central Incisor by Single Tooth Dento-Osseous Osteotomy and A Simple Distraction DeviceJuan Carlos MeloNessuna valutazione finora
- PrinciplesofOsteopathicMedicine PDFDocumento5 paginePrinciplesofOsteopathicMedicine PDFsuso73Nessuna valutazione finora
- 8th Icse Endocrine & TransportDocumento2 pagine8th Icse Endocrine & TransportManoj BhatiaNessuna valutazione finora
- 6 WHO Standard Acupuncture Point Locations in The Westernpart 6Documento30 pagine6 WHO Standard Acupuncture Point Locations in The Westernpart 6Virgil Anma100% (1)