Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Sexual Reproduction in Humans
Caricato da
Jeanelle Albert0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
123 visualizzazioni77 pagineAbout Sexual Reproduction In Humans for A level
Copyright
© © All Rights Reserved
Formati disponibili
PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoAbout Sexual Reproduction In Humans for A level
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
123 visualizzazioni77 pagineSexual Reproduction in Humans
Caricato da
Jeanelle AlbertAbout Sexual Reproduction In Humans for A level
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 77
Sexual Reproduction in Humans
Hormones of Reproduction
Sex Hormones
Males: androgens (ex: testosterone)
Females: estrogens and progesterone
Function:
-Development of the reproductive organs
-Function of the reproductive organs
-Sexual behavior and drives
-Growth and development of many other organs and
tissues
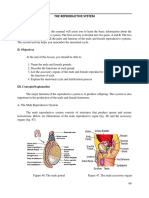
Male Reproductive System
The Testis
Spermatogenesis
Spermatogenesis
70 days for production = 107 per gram
Germinal epithelial cells spermatogonia
primary spermatocytes meiosis secondary
spermatocytes spermatids.
Sertoli / nurse cells = mechanical support,
protection, nourishment
In lumen spermatids mature to form
spermatozoa. - Spermiogenesis
Spermiogenesis
Spermiogenesis is the process in which
spermatids develop into sperm. The
spermatids lose excess cytoplasm and form a
tail, becoming motile sperm
SPERMIOGENESIS
Sperm
SPERM
Sperm
Sperm have 3 major regions
Head contains DNA and hydrolytic enzymes that
allow the sperm to penetrate and enter the egg
Midpiece contains mitochondria spiraled around
filaments
Tail a typical flagellum produced by a
centriole
Hormonal control
Pituitary FSH and LH
FSH stimulates development of
spermatozoa.
LH stimulates development of testosterone.
Also called interstitial cell stimulating
hormone ICSH.
Testosterone is responsible for development
of secondary sexual characteristics
Testosterone
Synthesized from cholesterol
Necessary for fetal development of male external genitalia
Increased levels of testosterone at puberty are responsible for
further growth of male genitalia and for the development and
maintenance of male secondary sex characteristics
Stimulates protein synthesis and accounts for the greater muscular
development of the male
Is the basis of libido in both males and females
Stimulates development of male secondary sexual characteristics
including:
-Appearance of pubic, axillary, and facial hair
-Enhanced growth of the chest and deepening of the voice
-Skin thickens and becomes oily
-Bones grow and increase in density
-Skeletal muscles increase in size and mass
The hypothalamus releases gonadotropin-
releasing hormone (GnRH).
GnRH stimulates the anterior pituitary to secrete
FSH and LH.
FSH causes Sertoli cells to release androgen-
binding protein (ABP).
LH stimulates interstitial (Leydig) cells to release
testosterone.
ABP binding of testosterone enhances
spermatogenesis.
Feedback inhibition on the hypothalamus and
pituitary results from rising levels of testosterone
and increased production of inhibin.
Questions
How come some males are more effeminate
than others?
How long can sperm be stored for in the
human male?
Female Reproductive System
Functions
Labia Majora large and fleshy. Enclose and
protect the external parts. Contains sweat and oil
secreting glands.
Labia minora located just inside labia majora.
Surround the vaginal and urethral openings.
Bartholins glands glands located beside vaginal
opening. Secrete mucus for lubrication during
intercourse.
Clitoris small, sensitive protrusion comparable
to penis in males. Can be stimulated and become
erect. Located at apex of labia minora. Covered
by fold of skin called prepuce similar to foreskin
as in penis.
Vagina canal which joins the cervix to the
outside of the body. Birth canal.
Uterus hollow pear shaped organ comprising
cervix and corpus. Corpus is site of development
of the foetus. Made of endometrium,
myometrium and perimetrium.
Fallopian tubes oviducts. Narrow tubes
attached to upper part of uterus. Serve as tunnels
for ova. Site of fertilisation. Contain cilia which
sweep the fertilised egg to the uterus.
Ovaries small oval shaped structures which
produce ova and hormones.
The Ovary
Are the primary female reproductive organs
Produce female gametes (ova)
Secrete female sex hormones (estrogen and
progesterone)
Have ovarian follicles embedded in the ovary
cortex are ovarian follicles; each follicle
consists of an immature egg called an oocyte
The Ovary
Oogenesis
Begins before birth and completed after fertilisation
Germinal epithelial cells give rise to primordial germ
cells.
Primordial cells divide mitotically to form oogonia.
Oogonia divide by mitosis to form primary oocytes.
They stay at prophase of meiosis I until ovulation. They
are enclosed by the membrana granulosa to form
primordial follicles.
Although 2 x 106 follicles are present before birth only
450 will develop to secondary oocytes and be released
during ovulation.
Oogenesis
At puberty the release of FSH stimulates about 20 primordial follicles to
develop to a primary follicle and complete meiosis I. However only one
of these grows while the others undergo follicular atresia.
The wall/membrana granulosa proliferates to produce the theca externa
(fibrous layer ) and theca interna (vascular layer). The granulosa cells
secrete a fluid to form the antrum.
Just before ovulation, the primary oocyte (2n) contained in the primary
follicle by meiosis = secondary oocyte (n) and first polar body.
Further growth of the theca occurs as well as that of the antrum. This is
called a graafian follicle. Meiosis II begins but stops at metaphase.
At fertilisation the secondary oocyte completes meiosis II to form an
ovum and 2nd polar body.
Polar bodies eventually degenerate.
The Graafian Follicle
In the Ovary
Primordial follicle one layer of squamous like
follicle cells surrounds the oocyte
Primary follicle two or more layers of cuboidal
granulosa cells enclose the oocyte
Graafian follicle secondary follicle at its most
mature stage that bulges from the surface of the
ovary.
Ovulation ejection of the oocyte from the
ripening follicle.
Corpus luteum ruptured follicle after ovulation
The Ovarian Cycle
Is a Monthly series of events associated with the
maturation of an egg
There are 3 phases:
1. Follicular Phase
Period of follicle growth (days 114)
The primordial follicle, directed by the oocyte,
becomes a primary follicle
The primary follicle becomes a secondary follicle
Theca, folliculi and granulosa cells produce
estrogens
The secondary follicle becomes a mature
vesicular follicle (Graafian follicle)
2. Ovulation
Occurs midcycle
Occurs when the ovary wall ruptures and
expels the secondary oocyte
Mittelschmerz a twinge of pain sometimes
felt at ovulation
1-2% of ovulations release more than one
secondary oocyte, which if fertilized, results in
fraternal twins
3. Luteal Phase
After ovulation, the ruptured follicle collapses,
granulosa cells enlarge, and along with internal
thecal cells, form the corpus luteum.
The corpus luteum secretes progesterone and
estrogen
If pregnancy does not occur, the corpus luteum
degenerates in 10 days, leaving a scar (corpus
albicans)
If pregnancy does occur, the corpus luteum
produces hormones until the placenta takes over
that role (at about 3 months)
FSH development of primary follicles which
contain primary oocytes. One continues to grow
the others undergo follicular atresia.
Membrana granulosa proliferate to give
membrana externa and membrana interna.
Antrum develops within follicle.
LH stimulate theca to produce oestradiol which
decreases FSH production.
LH maintains development of the follicle into a
Graafian follicle.
During ovulation LH decreases. Prolactin =
corpus luteum = progesterone + oestrogen.
The Uterus
Is a hollow, thick-walled organ that consists of Body major portion of the
uterus
Fundus rounded region superior to the entrance of the uterine tubes
Cervix narrow outlet that protrudes into the vagina
Functions of the uterus
Receives, retains, and nourishes the fertilized egg
Uterine wall is composed of 3 layers:
1. Perimetrium outermost serous layer; the visceral peritoneum
2.Myometrium middle layer; interlacing layers of smooth muscle
3. Endometrium mucosal lining of the uterine cavity. Inner layer allows
for implantation of a fertilized egg. Sloughs off if no pregnancy occurs
(menses). Has numerous uterine glands that change in length as the
endometrial thickness changes
Uterine Cycle
Three phases
- Menstrual Phase: shedding of the epithelial
lining of the endometrium.
- Proliferative phase: thickening of the
endometrium. Coincides with the follicular
phase of the ovarian cycle.
- Secretory phase: progesterone from corpus
luteum maintains the lining of the uterus.
The Menstrual Cycle
A 28 day cycle (approximately) which involves
the ovarian and uterine cycles.
Four main phases: 1. menstruation day 1
2. follicular phase day 7
3. ovulation day 14
4. luteal phase day 21
Fertilisation
https://www.youtube.com/watch?v=_5OvgQ
W6FG4
Click on the above link or copy and paste it
into the URL browser to view this video. It is
quite explicit so there was no need for me to
add many slides on this topic.
Development of Foetus
Diary of human development
Week 0
Egg is fertilised in the
fallopian tube.
Week 1
Embryo becomes
attached to the
lining of the uterus
(womb).
Week 2
Foetus eyes begin
to develop. Its
legs and arms are
tiny bumps.
Week 6
Foetus begins to look
like a human. Ears,
hands and feet begin
to grow. Heart begins
to beat.
Week 10
Foetus fingers and
toes grow. It can
move its arms and
legs a little it can
swallow and frown.
Week 14
It is possible to
determine the
foetuss sex.
Week 18
Foetus has hair,
eyebrows. Doctors
can hear the
heartbeat. Mother
begins to feel its
kicks.
Week 26
Foetus opens its eyes.
Week 30
If born now, the
baby could live
with special care.
Week 34
Baby has
grown a lot of
fat in the last
4 weeks, to
keep it warm
when it is
born.
Week 38 - 40
Baby is born.
The placenta
The zygote divides as
it passes to the uterus
and becomes and
embryo.
The embryo implants
in the thick lining of
the uterus.
The placenta
Finger like extensions
called villi project
from the embryo into
the lining of the
uterus eventually
forming the placenta.
The placenta
The embryo develops
into a foetus attached
to the placenta by the
umbilical cord.
The placenta
An artery and a vein
run through the
umbilical cord and
connect the foetus
blood system to the
placenta.
The placenta
The foetus blood
system IS NOT
DIRECTLY CONNECTED
to the blood system of
the mother.
The placenta
The exchange of
oxygen, food and
wastes between the
mother and foetus
depends on diffusion
across the thin wall of
the placenta.
The placenta
Harmful substances
such as nicotine,
alcohol, drugs and
virus can also pass
across the placenta
from the mother to
the foetus.
Potrebbero piacerti anche
- Biodiversity and Its ImportanceDocumento25 pagineBiodiversity and Its ImportanceJeanelle AlbertNessuna valutazione finora
- Interactions in EcosystemsDocumento42 pagineInteractions in EcosystemsJeanelle AlbertNessuna valutazione finora
- Father's Love LetterDocumento10 pagineFather's Love LetterJeanelle AlbertNessuna valutazione finora
- Sexual Reproduction in HumansDocumento77 pagineSexual Reproduction in HumansJeanelle AlbertNessuna valutazione finora
- Topik 6 Impact of Human Activities On Environmental QualityDocumento35 pagineTopik 6 Impact of Human Activities On Environmental Qualitysushant980Nessuna valutazione finora
- WaterDocumento32 pagineWaterJeanelle AlbertNessuna valutazione finora
- HomeostasisDocumento68 pagineHomeostasisJeanelle AlbertNessuna valutazione finora
- Sexual Reproduction in Flowering PlantsDocumento49 pagineSexual Reproduction in Flowering PlantsJeanelle AlbertNessuna valutazione finora
- Human and Cultural Development Via The ArtsDocumento4 pagineHuman and Cultural Development Via The ArtsJeanelle AlbertNessuna valutazione finora
- Cancer Class ProjectDocumento26 pagineCancer Class ProjectJeanelle AlbertNessuna valutazione finora
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5783)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (119)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Biology GlossaryDocumento12 pagineBiology GlossaryShivali AntinNessuna valutazione finora
- Mdcat Crash Test 1 BiologyDocumento8 pagineMdcat Crash Test 1 BiologyMUHAMMAD NOMAN SALEEMNessuna valutazione finora
- Science test reviewDocumento6 pagineScience test reviewJoan AlfarasNessuna valutazione finora
- Group 3 - PCOS and SD Written OutputDocumento25 pagineGroup 3 - PCOS and SD Written OutputJolly S. SendinNessuna valutazione finora
- Anatomy Physiology of The Male Female Reproductive SystemDocumento17 pagineAnatomy Physiology of The Male Female Reproductive SystemLilian JerotichNessuna valutazione finora
- Charybdis Natator (HERBST, 1794), FROM ESTANCIA, ILOILODocumento37 pagineCharybdis Natator (HERBST, 1794), FROM ESTANCIA, ILOILORey Malvin SG PallominaNessuna valutazione finora
- Animal Science Practice Test QuestionsDocumento17 pagineAnimal Science Practice Test QuestionsJoylyn Troniado100% (1)
- Understanding the Physical and Emotional Changes of AdolescenceDocumento14 pagineUnderstanding the Physical and Emotional Changes of AdolescenceRC SectionNessuna valutazione finora
- K-Klinis Dokter ObsgynDocumento6 pagineK-Klinis Dokter Obsgynadyat89Nessuna valutazione finora
- Science 5Documento81 pagineScience 5Michael Joseph Santos100% (2)
- Adebayo M.O. Care Study On Ovarian CystectomyDocumento47 pagineAdebayo M.O. Care Study On Ovarian CystectomyDamilola Olowolabi AdebayoNessuna valutazione finora
- The Science of Medical Intuition WorkBookDocumento88 pagineThe Science of Medical Intuition WorkBookSo100% (9)
- Feamle Reproductive System PoultryDocumento35 pagineFeamle Reproductive System PoultryGenNessuna valutazione finora
- Quarter3 Week 1: (MELC) : Compose An Argumentative Essay Reference: English 10 Learner's Material - Celebrating DiversityDocumento7 pagineQuarter3 Week 1: (MELC) : Compose An Argumentative Essay Reference: English 10 Learner's Material - Celebrating Diversitymy musicNessuna valutazione finora
- Case Study - CS With BTLDocumento16 pagineCase Study - CS With BTLAJ Roze Holmes100% (2)
- Bio Review MOGCHS G10Documento8 pagineBio Review MOGCHS G10Ayesha Faye MantalaNessuna valutazione finora
- Anatomy and Physiology of Farm AnimalsDocumento157 pagineAnatomy and Physiology of Farm AnimalsOliver Talip100% (1)
- Nicolopoulou-Stamati - Reproductive Health and The EnvironmentDocumento409 pagineNicolopoulou-Stamati - Reproductive Health and The EnvironmentGiorgos PapasakelarisNessuna valutazione finora
- Sample Dessertation, DR NandanDocumento98 pagineSample Dessertation, DR Nandansrilalitha avinashNessuna valutazione finora
- HymenectomyDocumento5 pagineHymenectomyShamaine limNessuna valutazione finora
- ATELERIX Albiventris Reproduction PDFDocumento8 pagineATELERIX Albiventris Reproduction PDFmariaNessuna valutazione finora
- Topic12-Magcamit, Mark Vincent MaciasDocumento8 pagineTopic12-Magcamit, Mark Vincent MaciasHermaphroditiusNessuna valutazione finora
- Ecology and Reproductive Biology of The Senatorial Scallop Chlamys SenatoriaDocumento10 pagineEcology and Reproductive Biology of The Senatorial Scallop Chlamys SenatoriaLaureen ManaloNessuna valutazione finora
- Reproductive System AnatomyDocumento30 pagineReproductive System AnatomyJune PinedaNessuna valutazione finora
- Polycystic Ovary SyndromeDocumento12 paginePolycystic Ovary SyndromeTijana ŠtatkićNessuna valutazione finora
- Part Test For Aipmt 2016Documento18 paginePart Test For Aipmt 2016Apex InstituteNessuna valutazione finora
- PCOS HealingDocumento36 paginePCOS HealingKheyrne Danu100% (1)
- Reproductive and Sexual HealthDocumento8 pagineReproductive and Sexual HealthHappyOwl01100% (3)
- Endocrine SystemDocumento52 pagineEndocrine Systemnurshuhada zainuddinNessuna valutazione finora
- Human reproduction overviewDocumento30 pagineHuman reproduction overviewfirstclassNessuna valutazione finora