Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
LWBK836 Ch117 p1265-1278
Caricato da
metasoniko81Titolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
LWBK836 Ch117 p1265-1278
Caricato da
metasoniko81Copyright:
Formati disponibili
CHAPTER
117 Scott J. Luhmann
David L. Skaggs
Role of Halo Traction and
Halo-Femoral Traction in Paralytic/
Neuromuscular Scoliosis
INTRODUCTION uity.3,10 In addition to the expected halo-related complications
and traction-related complications, this form of traction, due to
Axial traction to correct spinal deformity is not a new concept; the need for extended bed rest and the presence of a distal
in fact, the first applications were reported in ancient Hindu traction pin in the appendicular skeleton, has had complica-
mythological epics (3500 to 1800 BC).11 Traction for spinal tions in up to 81% of patients, consisting of dislocations of the
deformity correction fell into disfavor due to the production of hip, deep vein thrombosis, extremity fractures after traction
spinal cord injury and paraplegia created by the application of removal, peripheral nerve traction injuries, paraplegia, and
excessive distraction to the spine. Over the last few decades, pressure sores.3,10,14 Because of the high rate of complications,
with refinement in the knowledge of spinal anatomy and bio- these two types of traction have fallen out of common use; how-
mechanics, the concept of controlled axial traction has regained ever, this method has been advocated for use intraoperatively.
attention with the use of the Harrington outrigger, Cotrel trac- A second method of distal fixation was the use of pelvic fixa-
tion, and halo traction. This chapter will outline the three most tion via half pins or small wires. With pelvic fixation, the most
commonly applied techniques of spinal traction currently in common complication is pelvic pin site infections/loosening,
use: preoperative halo-gravity traction, intraoperative halo- but unique to this method of fixation are the complications of
femoral traction (IHFT), and the internal distraction tech- peritoneal penetration and/or perforation of the intestine,20
nique (Table 117.1). ischemic necrosis of odontoid process, cranial neuropraxias,
hip contractures, and superior mesenteric artery syndrome.
Lastly, long-term pathologic changes of the cervical spine have
PREOPERATIVE HALO-GRAVITY been reported in more than 50% of patients.21 The main rea-
TRACTION son for these unique complications in the cervical spine is the
ability to exert high, long-term traction when the pelvis is used
Spinal traction takes advantage of the viscoelastic properties of as an anchor point.
the spinal column. After traction application, an immediate ini- With evolution in spine instrumentation, from Harrington
tial correction occurs and is likely due to the elasticity (or stiff- rods to third-generation Cotrel--Dubousset instrumentation,
ness) of tissues and is then secondarily followed by a creep the need for routine preoperative traction has declined. Despite
phase, in which most of the correction is achieved. In the 1960s, the overall decline in the use of preoperative traction, halo-
Cotrel reintroduced the use of preoperative traction, utilizing gravity traction has become more popular and has been shown
a pelvic sling with a head halter, to improve the overall spinal to be effective in the treatment of complicated spinal deformi-
correction at the time of surgery and to minimize neurologic ties.8,15 As opposed to the other methods mentioned, this alter-
deficits. The approach was routinely used in many centers in native technique uses the patients body weight as a counter-
the 1960s and 1970s but lost favor after several centers demon- force to the halo traction. The patient can not only use the
strated no benefit for this type of preoperative traction when traction in bed but also can ambulate with the use of a modi-
used prior to surgery with Harrington instrumentation. Since fied walker or wheelchair. In addition, the individual can par-
that time four other general techniques of preoperative axial ticipate in a physiotherapy program (Fig. 117.1) to improve
spinal traction have been reported: halo-femoral, halo-pelvic, pulmonary function and overall fitness. This traction can be
halo-tibial, and halo-gravity.3,9,10,15,16,20 used before a single-stage anterior or posterior fusion and also
The addition of a distal femoral or tibial traction pin into between stages of circumferential spine fusions.23
one or both legs permits a high level of distraction to be The strengths/weakness and indications and contraindica-
applied. Correction of coronal spine deformities has been tions for this method of traction are listed in Tables 117.2 and
reported to be 41% to 57% with 53% correction of pelvic obliq- 117.3. The impact of traction on pulmonary function deserves
1265
LWBK836_Ch117_p1265-1278.indd 1265 8/25/11 10:06:21 PM
1266 Section X Paralytic Deformity
TABLE 117.1 Strengths and Weaknesses of Traction
Strengths Weaknesses
Preoperative halo gravity 1. Permits gradual application of traction 1. Requires weeks or months of continuous, daily
2. Correction while patient is awake treatment
3. Low risk of neurologic problems 2. Pin site issues
3. Contraindicated for cervical and occipitocervical
instability
Intraoperative halo femoral 1. Preoperative hospitalization unnecessary 1. Additional operative time for halo application and
2. Can easily adjust traction force to achieve traction pin insertion with scarring
desired correction 2. Contraindicated for cervical or occipitocervical
3. Improves pelvic obliquity instability
4. Decreases operative time 3. Relative contraindication with kyphotic deformity
Internal distraction 1. No external force application 1. Shorter-term application of traction; less stress
relaxation and creep
further comment. In severe scoliosis and kyphoscoliosis, poor problems.15 The technique of halo application and its care
pulmonary function is, in part, due to the restrictive spinal appear deceptively simple; however, there are many pitfalls one
deformity. With the application of halo-gravity traction, pulmo- can encounter. The most common complication is pin loosen-
nary function has been demonstrated to improve signifi- ing, occurring up to 87% of the time.6,10,15,16 Anterior pins
cantly.15--17 Pulmonary function tests (PFTs) obtained during loosen most commonly and, in the absence of infection, can be
preoperative traction can be helpful in documenting improve- retightened by advancing one to two revolutions. If this does not
ments in pulmonary function and should be considered in the tighten then the pin should be removed and shifted to another
timing of surgical intervention. The other less obvious issue is location. If the pin advances too far, intracranial penetration
the positive impact on the patients overall medical cardiopul- can occur in up to 4% of patients.6,7 Secondary brain abscesses
monary fitness, above the obvious quantitative improvement in have been reported after intracranial pin penetration.
PFTs and nutritional status.18 Another common pin site--related complications reported
are superficial and deep infections, which occur in 39% to 59%
of children.6,10,15,16 Superficial infections are much more com-
COMPLICATIONS AND MANAGEMENT
mon than deep infections and are not typically associated with
Complications with the use of halo-gravity traction can be bro- pin loosening. Treatment typically consists of a short course of
ken down into halo-related complications and traction-related oral antibiotics (7 days of cephalexin) with or without pin
removal. However, deep infections or persistent superficial
infections require pin removal, irrigation and debridement of
the pin site, placement of a new pin site, and intravenous anti-
biotics. Other less common pin site complications are superior
migration of the halo due to inappropriate position above the
equator of the cranium, skin necrosis, anterior pin site scar-
ring, pin site pain, and injury to the supraorbital nerve.6,7
Traction-related complications appear to be related to the
duration of traction and the amount of traction applied to the
spine. Excessively fast correction of scoliosis and kyphoscoliosis
increases the risk of neurologic injury. This risk is increased
with the presence of intraspinal anomalies or previous spinal
surgery. MacEwen et al reported six cases of preoperative para-
plegia related halo-femoral or halo-pelvic traction.12 One of the
more common problems are cranial nerve palsies, which have
been reported for the trochlear (IV), abducens (VI), glossopha-
ryngeal (IX), vagus (X), and hypoglossal (XII) nerves both as
isolated and combined deficits.12,24 Of the cranial nerve inju-
ries, the most common palsy is the loss of lateral gaze secondary
to traction on cranial nerve VI.2,10,12,24 The usual course of cra-
nial nerve palsy is resolution within 6 to 10 weeks of
onset.2,12,24
CLINICAL EVIDENCE
Several clinical reports have demonstrated the safety and effi-
cacy of halo-gravity traction. Rinella et al reported a retrospec-
tive analysis of 33 patients who had preoperative halo-gravity
Figure 117.1. Patient on treadmill in traction setup. traction prior to posterior spinal fusion for severe coronal and
LWBK836_Ch117_p1265-1278.indd 1266 8/25/11 10:06:21 PM
Chapter 117 Role of Halo Traction and Halo-Femoral Traction in Paralytic/Neuromuscular Scoliosis 1267
TABLE 117.2 Strengths and Weakness of Halo-Gravity Traction
Strengths Weaknesses
Noninvasive technique Pin site problems
Traction performed on awake, alert patient permits early detection of Requires traction be applied through occipitocervical junction
neurological symptoms (i.e., cranial nerve weakness or deficits) and cervical spine
Most effective on more cephalad deformities (i.e., cervical, Less effective on thoracolumbar and lumbar deformities
cervicothoracic, proximal thoracic)
Effective for gradual correction of sagittal and coronal plane deformities Less effective for patients with increased tone or spasticity
Improves truncal alignment by centering the head over the pelvis Requires intellectually and behaviorally competent individual
Low rate of complications Typically requires inpatient hospital treatment; challenges of
Overall patient tolerance coverage of treatment by third-party payers.
Permits improvement of pulmonary function
Eventual instrumentation and fusion easier due to lesser degree of spinal
deformity
sagittal plane deformities.15 Mean preoperative coronal curve be given to obtaining magnetic resonance imaging (MRI) of
magnitude was 84, which improved 46% down to 46, and entire neuraxis prior to traction for severe spinal deformity.
mean thoracic kyphosis decreased 33. The mean increase in The placement of the halo is done in the operating room
spinal length, as measured by the distance from C7 to S1 under deep sedation or general anesthesia, which minimizes
increased 6.3 cm. There were no permanent neurologic com- patient movement and pain/distress (Fig. 117.2). In patients
plications. There were seven halo-related problems: four cases with small or misshapen craniums placement of the halo can be
of halo pin loosening requiring replacement, one infected pin challenging, hence a full complement of sizes and pin configu-
site, one case of nystagmus, and one case of nausea and vomit- rations must be available. Placement of the halo must be just
ing. Sink et al reported a review of 19 patients with severe sco- above the eyebrows and earlobes, which in most patients will
liosis whose pretreatment coronal Cobb was 83.16 Traction was put the halo caudal to equator of cranium, which will prevent
utilized for a mean 13 weeks (6 to 28 weeks) with an improve- cranial migration of halo. The ring should be no greater than
ment of the coronal Cobb to 55 (35% improvement). Trunk 1 cm away from the skin to minimize cantilevering of the pins
decompensation improved in all patients, and the average on the ring, and there should be no contact of the ring with the
increase in trunk height was 5.3 cm. Janus et al reported on 20 ear as skin necrosis is a possible complication. The anterior
osteogenesis imperfecta patients treated with preoperative pins are positioned over the lateral one third of eyebrows to
halo-gravity traction. Mean prehalo Cobb of 78 decreased to avoid the supraorbital and supratrochlear nerves and frontal
53 prior to surgery (32% improvement).9 These three reports sinus. More lateral pin placement risks injury to the temporal
did not document any permanent neurologic complications artery and thin temporal bone. If patient has undergone previ-
and concluded that preoperative halo-gravity traction improves ous hydrocephalus surgery, one should look for the subcutane-
trunk balance and coronal and sagittal alignment in children ous ventricular shunt tubing prior to halo application. The pos-
with severe spinal deformity. terior pins should be placed across halo on opposite side of
DESCRIPTION OF TECHNIQUE
Prior to the initiation of halo-gravity traction a thorough neu-
rological assessment is essential, not only to identify any find-
ings suggestive of an intraspinal anomaly but also to establish a
baseline to which neurological examination during the trac-
tion treatment can be compared. Strong consideration should
Indications and
TABLE 117.3 Contraindications of
Halo-Gravity Traction
Indications Contraindications
Severe scoliosis or kyphoscoliosis Occipitocervical or cervical
Previously failed spinal fusion instability
surgery
Significant truncal
decompensation
Poor pulmonary function due to
restrictive spinal deformity Figure 117.2. Application of halo under anesthesia in the operat-
ing room.
LWBK836_Ch117_p1265-1278.indd 1267 8/25/11 10:06:22 PM
1268 Section X Paralytic Deformity
anterior pins, typically behind the upper, outer region of the
earlobe.
Typically four or six pins (two anteriorly, and two or four
pins posteriorly) are sufficient for most patients. In patients
with a lower traction weight goal (20% total body weight),
shorter planned traction length (i.e., 4 weeks), normal bone
mass and quality, and older age (>11 years) four pins are usu-
ally sufficient. However, the age at which it is safer to shift
between four pins and multiple pins (six to eight) has not been
established.6,13 After identification of the appropriate number
and placement of the pins, the pins are advanced sequentially
from finger- tightness to the final tension in 2 inch/lbs incre-
ments. Usually pin insertion torque of 6 to 8 inch/lbs is ade-
quate in older patients, less in younger children (i.e., 4 inch/
lbs), and only to finger tightness or 2 inch/lbs in infants/tod-
dlers.13 Extreme care must be exercised with loose pins, and in
general retightening pins after 24 to 48 hours is not recom-
mended due to the risk of cranial penetration. If there is a
symptomatic loose pin, removing the symptomatic pin and
placing a pin in a new site nearby should be considered.
Once the halo is applied, the traction is applied through
either a rope/pulley/weight apparatus or a scale device (Figs.
117.3 and 117.4). Approximately 3 to 5 lbs of traction is initially
applied immediately after the halo is applied. The traction
weight is then increased in a scheduled fashion (1 to 3 lbs/d)
until the desired weight goal is achieved. For most patients, the
goal should be between 30% and 45% of body weight (Figs.
117.5A to D). If the patient is at high risk for development of a Figure 117.4. Traction setup utilizing scale as used by Texas
neurological deficit due to existing myelopathy, severe spinal Scottish Rite Hospital. (Courtesy of Dan Sucato, MD).
deformity (i.e., kyphoscoliosis), or multiple previous spine sur-
geries, then a slower rate of weight increase is recommended.
Typically, the goal is for the younger, smaller patients to be almost levitating off their chairs with minimal contact of their
buttocks with the chair.15,16 By doing so, the maximal amount of
force can be applied to the spinal deformity. Traction is applied
for a minimum of 12 hours a day, and the weight is decreased
to 50% to 75% at bedtime, mainly to decrease the proximal
migration of the patient in bed. The pin sites are treated by
shower cleansing without any direct cleaning of the pin sites
with hydrogen peroxide, Betadine, or other topical solution or
ointment.
Neurological assessment is performed every 8 hours. Cranial
nerve assessment (especially abducens) and neurologic exami-
nation of the upper and lower extremities (motor and sensory
examinations) should be performed by the nursing staff and
any changes should be immediately reported. Physiotherapists
should work with these patients on a daily basis to assist in
mobilization with the use of walkers and adapted treadmills,
which provide continuous traction (Fig. 117.1). The traction
apparatus on treadmill permits the patient to exercise, improv-
ing pulmonary function and increasing patients aerobic fitness
while limiting the effect of osteoporosis, which has plagued
other forms of preoperative traction methods. The duration of
preoperative traction is 2 to 12 weeks depending on overall
patient health, medical comorbidities, and the response of the
curves to traction. Extended courses of traction (8 to 12 weeks)
are often performed to optimize pulmonary function and nutri-
tion (and not only to improve curve correction).
PEARLS AND PITFALLS
1. The anterior halo pins should be placed over the lateral one
Figure 117.3. Traction setup with weights on walker. third of the eyebrows to avoid the supraorbital nerve. The
LWBK836_Ch117_p1265-1278.indd 1268 8/25/11 10:06:23 PM
Chapter 117 Role of Halo Traction and Halo-Femoral Traction in Paralytic/Neuromuscular Scoliosis 1269
A B C
D E F
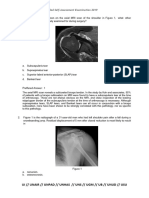
Figure 117.5. A 9-year-old boy status post multiple previous anterior and posterior thoracic fusions with
postoperative progression to severe kyphoscoliosis with 263 of combined coronal and sagittal deformity.
(A and B) Pretraction erect anteroposterior and lateral radiographs. (C and D) After 25 lbs traction demon-
strating a 20% overall improvement of deformity (263 pretraction to 211 in traction). (E, and F) 2 years
after posterior spinal fusion.
LWBK836_Ch117_p1265-1278.indd 1269 8/25/11 10:06:24 PM
1270 Section X Paralytic Deformity
posterior pins should be placed directly opposite to the ante-
Strengths and Weaknesses of
rior pins. All pins should be placed below the equator of skull
TABLE 117.4 Intraoperative Halo-Femoral
to prevent superior migration of halo during traction.
2. Initial traction weight should be between 3 and 5 lbs and Traction
then increased sequentially.
Strengths Weaknesses
3. Frequent nursing neurological assessments (every 8 hours)
are necessary. Effective on all types of Necessity of supraorbital and
4. Pin site problems occur; the most common pin site compli- neuromuscular patients distal femoral pins with
cations are superficial infections, which can be treated with regardless of diagnosis secondary scarring
oral antibiotics. Improves truncal alignment by Requires traction be applied
5. One should exercise caution when retightening pins to pre- centering the head over the through occipitocervical
pelvis junction and cervical spine
vent intracranial pin placement.
Effective on all deformities Requires 15 min of additional
6. Neurological problems most commonly are cranial nerve
regardless of location time preincision to place
and temporary. halo- and distal femoral
7. Preoperative halo-gravity traction can be a useful tool in the traction pin
treatment of severe scoliosis and kyphoscoliosis with a low Corrects pelvic obliquity Risk of intracranial placement
rate of temporary complications. of halo pins due to
osteopenic cranium
Eventual instrumentation and
INTRAOPERATIVE HALO-FEMORAL fusion easier due to lesser
TRACTION degree of spinal deformity
Low rate of complications
No need for preoperative
As mentioned in the previous section, the use of preoperative
traction
halo-femoral/pelvic/tibial traction has been shown to have an
Patients head can hang free in
unacceptably high complication.3,10,14 Despite this, the tech- traction eliminating any
nique has shown to be effective in preoperatively correcting pressure over the eyes
coronal deformities (41% to 57%) and pelvic obliquity (up to
53%).3,10 By using this method intraoperatively, one can avoid
the problems associated with long-term traction yet gain the
benefits of direct axial traction during the surgical procedure. COMPLICATIONS AND MANAGEMENT
In nonambulatory neuromuscular scoliosis (i.e., cerebral
palsy, spinal muscle atrophy, myelomeningocele, muscular dys- Little information exists on complications of IHFT. Since the
trophy), progressive scoliosis with long, sweeping thoracolum- traction is applied for only one surgical procedure, complica-
bar curves can cause significant pelvic obliquity, which can cre- tions related to extended traction are not experienced (i.e., pin
ate sitting imbalance and, more problematically, recalcitrant site or traction pin infection, pin loosening, etc.). Theoreti-
pressure sores and pain. This problem is potentiated by abnor- cally, it is possible with the distal femoral traction pin to injure
mal protective skin sensation and the typically low muscle mass. the distal femoral physis, posterior neurovascular structures,
The goal of surgical treatment of this population is different and to create an iatrogenic femur fracture; however, these com-
than for the idiopathic scoliosis patients, specifically to correct plications have not been reported in published reports of
the pelvic obliquity and to obtain, and maintain, a painless, IHFT.
well-balanced spine above the pelvis. Hence, the aim is to estab-
lish a good sitting balance. Most reports on the surgical treat- CLINICAL EVIDENCE
ment of neuromuscular scoliosis (myelomeningocele, cerebral
palsy, Duchennes muscular dystrophy) recommend correction Takeshita et al reported a retrospective case-control study com-
of the pelvic obliquity and fusion to the sacrum when sitting paring outcomes of neuromuscular patients undergoing spine
imbalance is severe.1,23 fusion with and without IHFT.19 In the control group (n = 20),
The strengths/weakness and indications/contraindications the mean preoperative pelvic obliquity was 17, which improved
for this method of traction are listed in Tables 117.4 and 117.5. to 7 postoperatively (52%). The mean preoperative pelvic
The major challenge in the surgical correction of neuromuscu- obliquity in the halo-femoral traction group (n = 20) was 26,
lar scoliosis is how to obtain spinal correction and, secondarily, which improved to 6 postoperatively (78% improvement); a
how to maintain this alignment during the postoperative
period. Osteopenia is a common problem, which, when pres-
ent, poses challenges in how to obtain spinal correction. In Indications and
those patients with large, stiff curves, the addition of an ante- Contraindications of
rior release increased curve flexibility and permitted better cor- TABLE 117.5 Intraoperative Halo-Femoral
rection. The use of IHFT allows direct skeletal traction and cor- Traction
rection of the spinal deformity and pelvic obliquity (Fig. 117.6).
During the surgical procedure, most, if not all, of the correc- Indications Contraindications
tion is obtained by the IHFT obviating the need for significant
spinal implant manipulation for correction. By offloading the Nonambulatory Occipitocervical or cervical instability
neuromuscular Significant kyphosis or kyphoscoliosis
implants, the chance of loosening and losing fixation at the
scoliosis
bone--implant interface is lessened.
LWBK836_Ch117_p1265-1278.indd 1270 8/25/11 10:06:26 PM
Chapter 117 Role of Halo Traction and Halo-Femoral Traction in Paralytic/Neuromuscular Scoliosis 1271
A B C
Figure 117.6. A 14-year-old boy with spastic quadriplegic cerebral palsy with pain and sit-
ting problems due to scoliosis and pelvic obliquity. (A and B) Preoperative upright anteroposte-
rior and lateral radiographs with 97 lumbar curve and severe pelvic obliquity. (C and D) 1 year
postoperative upright radiographs after posterior spinal fusion with intraoperative halo-femoral
D
traction but no anterior release. Note level pelvis and good sagittal and coronal spinal balance.
statistically significant difference (p = .001). There were no routine posterior spinal fusion with the next 51 consecutive
reported intraoperative or postoperative halo-femoral traction- patients having IHFT with lower extremity skin traction. The
related complications (i.e., femoral fractures, pin site infec- traction group had shorter operative times (282 minutes vs. 335
tions, pin cutout, etc.) (Figs. 117.6A to D). Vialle et al reported minutes), less intraoperative maneuvers necessary for leveling
on 110 patients with cerebral palsy who underwent posterior the pelvis, better coronal Cobb correction (63% vs. 44%), and
spinal fusion.22 The initial 59 control patients underwent better correction of pelvic obliquity (81% vs. 56%). Direct
LWBK836_Ch117_p1265-1278.indd 1271 8/25/11 10:06:26 PM
1272 Section X Paralytic Deformity
skeletal fixation appears to be optimal (i.e., halo and skeletal
pin fixation) to exert enough axial force to the spine and min-
imizing skin complications.
DESCRIPTION OF TECHNIQUE
The application of the halo frame was described earlier in this
chapter. Similar to the halo, the distal femoral traction pin is
placed during, or immediately after induction of anesthesia to
minimize delay in the start of surgery. The traction pin is inserted
into the femur on the side of the elevated hemipelvis. Typically,
a threaded pin approximately 2 mm or larger is utilized. Smooth
pins may slide medially or laterally during the surgical procedure
and permit the traction bow to apply direct pressure to the skin
and cause skin breakdown. Similarly, larger traction bows are rec-
ommended to minimize the pressure, and the bow may be placed
over the tibial tubercle during the application of traction. Figure 117.8. Intraoperative head-halo positioning permits the
face to be without any pressure as the halo rests on the clear plastic
While the patient is in the supine position, prior to turning
face board.
the patient prone, the pin entry sites are localized just proximal
to the femoral epicondyle. This minimizes the likelihood of iat-
rogenically injuring the distal femoral physis. Medial to lateral In general, the weights should be fairly equal on both sides
placement also minimizes likelihood of an injury to posterior to prevent the patient from migrating cephalad or caudad dur-
neurovascular bundle. The pin can be placed with either a ing surgery. This can be partially countered by placing the
manual hand drill or a power drill and should be placed per- patient into a slight reverse-Trendelenburg position. The halo
pendicular to the long axis of the femur. After securing the and femoral traction pins are removed after the patient has
traction pin to the bow, the ends of the pins should be heavily been placed supine after being moved from operative table.
padded to prevent skin injury to the contralateral limb
(Fig. 117.7). The patient is then placed in the prone position PEARLS AND PITFALLS
on the four- or six-posterior Jackson frame. The traction is then
applied, with 15 lbs on the halo and 15 to 20 lbs on the femoral 1. Avoid placement of traction pin in the proximal tibia to pre-
traction pin (Fig. 117.8). Weight is increased, up to 30 lbs on vent iatrogenic damage to the proximal tibial physis.
the femoral side, until the pelvic obliquity is corrected to a clin- 2. Careful padding of the tip of the traction pins and the trac-
ically level position (Fig. 117.9). This correction of pelvic obliq- tion bow prevents lower extremity skin problems during sur-
uity can be confirmed clinically by palpating the upper margin gery.
of the iliac wings or alternatively can be confirmed radiograph- 3. Although pin cutout in osteoporotic bone is a concern, this
ically. It is important to recheck around the traction pin and has not been demonstrated to occur. The use of lower trac-
bow to ensure that no excessive pressure is present against the tion weights applied through a centrally placed pin lowers
skin medially, laterally, or more importantly over the tibial the likelihood of this from occurring.
tubercle. Unacceptable pressure over the tibial tubercle can be 4. Extreme care should be exercised in individuals without
rectified by placing gel pads or egg crate foam between the neurological diagnoses (e.g., cerebral palsy, spinal muscle
traction bow and the skin and by flexing the knee and placing atrophy, etc.) and in those with severe kyphosis and kyphosco-
more pillows under the legs and feet. liosis deformities. Neurologic deficits are a concern, and the
use of descending tract spinal cord monitoring is essential.
Figure 117.9. Intraoperative positioning of patients with 20 lbs of
Figure 117.7. Intraoperative demonstration of lower extremity traction weight applied to halo and 20 lbs to the distal femoral trac-
positioning with right distal femoral traction pin in place. tion bow.
LWBK836_Ch117_p1265-1278.indd 1272 8/25/11 10:06:28 PM
Chapter 117 Role of Halo Traction and Halo-Femoral Traction in Paralytic/Neuromuscular Scoliosis 1273
TABLE 117.6 Strengths and Weaknesses of Internal Distraction Technique
Strengths Weaknesses
Effective on all types of patients regardless of diagnosis Does not automatically center the head over the pelvis
Applicable regardless of cervical spine instability (traction is not Distraction is acutely applied . . . does not permit secondary
applied through occipitocervical junction or cervical spine) viscoelastic improvement in deformity
Effective on thoracolumbar deformities Requires additional time and dissection to place TIDR anchors
Corrects pelvic obliquity Dorsally placed kyphosis-producing distractive technique. Need
accurate neuromonitoring
Eventual instrumentation and fusion easier due to lesser degree of Increased risk of deep infection for two-stage approach
spinal deformity
Low rate of complications
No need for preoperative traction
Avoids scarring and complications associated with halos and distal
traction pin
Gradual correction applied during surgery in many obviate need for
anterior release
Direct axial traction force applied to spine
TEMPORARY INTERNAL DISTRACTION the use of TIDR in a staged fashion (1 or 2 weeks later from the
primary surgery). However, Buchowski et al reported no neuro-
The use of temporary intraoperative distraction rods (TIDRs) logic complications or wound infections with this technique.4
for the correction of severe scoliosis was initially utilized during Another concern is compromising spine fixation points, such
the development of Harrington instrumentation by the use of as pedicle screws, when used for TIDR end points. To minimize
an outrigger, which could be applied intraoperatively. This con- this problem, avoid using pedicle screws as the cephalad fixa-
cept has recently regained interest as an alternative to preop- tion points for the TIDR construct and use ribs instead. The
erative halo-gravity or IHFT.4 The indication for TIDR is severe caudal fixation points are typically pedicle screws or the iliac
spinal deformity of the thoracic and lumbar spine, including wing. If pedicle screws are used then using two or three linked
severe pelvic obliquity. In general, in most instances in which pedicle screw that are not at the end of the construct will not
halo traction is considered for a thoracic or lumbar spinal compromise fixation at the lowest instrumented level.
deformity, a temporary rod may be also be considered. The
only absolute requirement is the presence of sufficient tempo-
CLINICAL EVIDENCE
rary bony fixation points in which to anchor the rods near the
top and bottom of the deformity. Anchor points may include Buchowski et al reviewed 10 patients, from 2 institutions, whose
the spine, pelvis, or ribs. This technique can be utilized in situ- surgical treatment utilized TIDR to improve the surgical out-
ation with cervical problems (i.e., deformity or instability) or comes of posterior spinal fusion for severe, complex rigid sco-
distal deformity (i.e., hip flexion deformity). The strengths/ liosis.4 All patients in this series had contraindications to
weakness and indications/contraindications for this method of traditional halo-gravity traction due to cervical instability,
traction are listed in Tables 117.6 and 117.7. kyphosis, or stenosis. All patients underwent primary posterior
release with six undergoing concomitant anterior release. Four
COMPLICATIONS AND MANAGEMENT of the patients had one surgical procedure (one distraction)
with six patients having staged treatment (two distractions).
At present, there is little information on complications with this Mean preoperative curve size was 104, mean distractive correc-
technique. The risk of wound infection is likely increased with tion was 53% (mean 49), and mean postoperative curve size
was 20 (80% improvement).
Indications and
TABLE 117.7 Contraindications of
DESCRIPTION OF TECHNIQUE
Internal Distraction
As opposed to the other two methods of traction, TIDR may be
Indications Contraindications performed in a two-stage fashion with the first stage consisting
of spinal releases (posterior or combined anterior/posterior)
Severe spinal deformity Lack of adequate fixation points for
(thoracolumbar) TIDR
and TIDR placement.4,5 Because of the recovery time between
Pelvic obliquity Inability to tolerate two-stage TIDR the two stages, it is imperative to maximize the chances of
due to medical comorbidities or returning to the operating room for completion of the surgical
poor nutritional status. plan. Preoperative medical evaluation (such as pulmonary, car-
Inability to neuromonitor the spinal diac, neurological) can be helpful depending on the patients
cord function during TIDR underlying medical condition. In addition to the routine pre-
Rigid kyphosis or kyphoscoliosis operative plain radiographic imaging (upright anteroposterior
Spinal cord abnormalities (syrinx, and lateral views and right and left supine side bending), trac-
diastematomyelia, tethered cord) tion films are particularly helpful in predicting the amount of
LWBK836_Ch117_p1265-1278.indd 1273 8/25/11 10:06:32 PM
1274 Section X Paralytic Deformity
correction possible with TIDR. A general rule of thumb is that
the TIDR usually leads to greater correction of the deformity
than that demonstrated on traction radiograph, and if the cor-
onal curve improves more than 50%, then TIDR (or external
traction) is likely unnecessary. Because of the application of a
distraction force across the deformity, we recommend an MRI
of entire spine to evaluate for intraspinal abnormalities. Spinal
cord monitoring of the upper and lower extremities with soma-
tosensory-evoked potentials and neurogenic mixed--evoked or
transcranial motor--evoked potentials are absolutely necessary.
Preoperative planning should include evaluation of the
bony anchor points for the temporary rod. A basic principle in
choosing anchor points for the temporary rod is to expect that
these anchors will plow through bone a bit, compromising the Figure 117.10. The up-going hooks can be placed suprape-
riosteal as the neurovascular bundle present caudal to the ribs will
holding power of the final anchor. Thus, one should not plan
typically slide anterior to the rib during distraction.
to use the temporary anchors as permanent anchors at either
end vertebrae of the final construct. For example, pedicle
screws will plow upwards in the upper thoracic spine during
their use in securing a temporary rod, so these compromised
general, the apex of the iliac crest appears to be the best place
pedicles should not be used as end vertebrae anchor points in
(Fig. 117.12). If the anchor is lateral to the apex, then the
the final implant. Selection of the cephalad and caudal TIDR
anchor point may slip further laterally. In small children, the
sites is recommended to be one to two level above and below
lateral-cephalad iliac anchor location may be too small to accept
the most inclined vertebra (end Cobb vertebra), respectively.
an iliac screw, so an S hook is likely the best option for these
The upper portion of the rod is generally attached to the
patients.
ribs or the spine. When attaching to ribs, standard large spinal
One of the real advantages of the temporary rod technique
laminar hooks are used on two ribs to disperse the loads (Figs.
is that an anterior release is generally not needed, because cor-
117.7 and 117.8). An advantage of applying the temporary rod
rection through posterior surgery is generally sufficient.
to the ribs rather than the spine is that the spine is then left
However, if a surgeon chooses to perform an apical anterior
unobstructed to placement of the permanent rod while actively
release, this would be done before placement of the temporary
applying distraction to the ribs. A disadvantage of ribs as an
rod. Buchowski et al recommend a one-stage TIDR surgical
anchor point is that one cannot push quite as hard on ribs com-
procedure for most spinal deformities, reserving the two-stage
pared with the spine. If one chooses to use the spine as an
surgery for the most severe deformities. If two stages are
upper anchor point, hooks are generally preferable to pedicle
planned, the interval between the first and second surgical
screws for two reasons: most importantly, when pushing upwards
stage is typically a 1-week period, which appears adequate to
on thoracic pedicle screws, plowing through the bone occurs
more easily than when pushing downwards, thus it is easy to
ruin the pedicle screw site as a permanent fixation point; in
addition, up-going infralaminar or transverse process hooks
permit easier seating of the rod into the hook.
The caudal anchor points are generally in the lumbar spine
or pelvis. As the pedicles are generally stronger in the lumbar
spine and the direction of force is downwards, the use of two
pedicle screws as a distal anchor point works well. The caudal
TIDR fixation points are commonly pedicle screws in the lum-
bar spine at two or three adjacent levels, so the surgeon should
use the levels a minimum of two above the final caudal level of
the fusion, planning that these screws will likely be suboptimal
for end-construct fixation. In addition, increasing the diameter
of the pedicle screws at the caudal end of the distraction con-
struct improves the fixation in the final fusion construct.
If the caudal TIDR fixation point is to be the pelvis to cor-
rect pelvic obliquity, fixation can be to the sacrum or iliac wing
utilizing an S-shaped hook or to the pelvis with an iliac screw
(Figs. 117.9 and 117.10). If iliac screw fixation is chosen, it is
preferred to place the TIDR iliac screw lateral and proximal to
the site of the definitive iliac screw, as the screw placed for TIDR
is likely to loosen during the distraction. Inserting a longer and
larger diameter screw can additionally improve iliac fixation.
Alternatively an S hook may be placed over the top of the iliac
crest or sacral ala (Fig. 117.11). Regardless of which type of
anchor is chosen, there is a mechanical advantage in correcting
pelvic obliquity if the anchor is placed lateral to the spine. In Figure 117.11. S hook anchor on iliac crest.
LWBK836_Ch117_p1265-1278.indd 1274 8/25/11 10:06:32 PM
Chapter 117 Role of Halo Traction and Halo-Femoral Traction in Paralytic/Neuromuscular Scoliosis 1275
Figure 117.12. The temporary rod (black arrows) is attached to
two ribs at the top, and an iliac screw in the pelvis. Following distrac-
tion and osteotomies, the pelvis is now level, the scoliosis is signifi-
cantly corrected, and the permanent right rod (white arrows) can be
placed while the temporary rod is still in place holding correction. In
this particular case, the entire surgery was done at one stage, as the
temporary rod led to sufficient correction.
achieve the maximal correction from the TIDR construct. At
the second stage the temporary rods are removed, the final
implants are placed, and fusion is performed.
At the time of surgery, the goal is to place the temporary
rod in the spine and begin distraction as early as possible in Figure 117.13. Large lumbar hooks fits well on ribs of moderate
the procedure to take advantage of the viscoelastic nature of to large size children. Hooks are placed just lateral to transverse pro-
the spine (Fig. 117.13). Retensioning of the TIDR constructs cesses, with an upward distraction force.
several times during the surgery permits gradual deformity
correction and lessens acute loading of the distraction con-
amounts of distraction throughout the surgery. For two-stage
struct, which lowers the stresses on the bone--implant inter-
procedures, no bone graft is used at the initial procedure as
face and permits neuromonitoring assessments. After estab-
fusion is not the goal. Closure is challenging at times when sig-
lishing the cephalad and caudal TIDR sites, two rods are
nificant distraction and lengthening has been placed across the
placed (one at each end) and maximally overlapped and con-
spine. Furthermore, the temporary rod usually remains lateral to
nected by a side-to-side connector. Distraction is applied across
these rods via the side-to-side connector. In large curves, it
may be a challenge to get to the anchor points in rods lined
up straight enough for this to occur, but a combination of dis-
traction and rod manipulation is usually sufficient to get the
rods parallel. In cases of extreme deformity, one may need to
apply a very small rod to the upper anchor points and another
very small rod to the lower anchor points with these two rods
connected to a third rod with multiaxial transverse connectors
(Fig. 117.14).
Once the temporary rod has been placed and the distraction
has been applied, one should proceed with subperiosteal dissec-
tion of the remainder of the spine and release of the spine (Figs.
117.15A to I). In most cases, apical osteotomies are indicated for
correction of these severe curves. Placement of the remainder of
the planned spine fixation points is then completed (i.e., pedicle
screws, wires, hooks). One shortcoming of using a temporary rod
is that it is technically difficult to place pedicle screws at the apex
of the deformity on the concave side of the curve. This is because
the temporary rod physically limits how far down one can put his
or her hands to place the pedicle screw in the rotated vertebral
Figure 117.14. Small temporary rods were placed in the upper
and lower anchor points and connected to a temporary rod by two
bodies. This positioning improves over time with further distrac- multiaxial transverse connectors. This type of temporary rod configu-
tion, and pedicle screws that could not be placed initially may be ration is generally too prominent to close soft tissue over but provides
able to be placed later in the surgery following osteotomies and a good start at distraction and aligning the upper and lower anchors
further distraction, or at the second-stage surgery. An essential and should and, which then allows lower-profile rods and connectors
part of this procedure is to apply multiple episodes of small to be placed later in the case.
LWBK836_Ch117_p1265-1278.indd 1275 8/25/11 10:06:34 PM
1276 Section X Paralytic Deformity
A B
Figure 117.15. A 12-year-old
girl with adolescent idiopathic sco-
liosis. (A and B) Preoperative clini-
cal photographs. (C and D)
Preoperative upright radiographs
with main thoracic Cobb measure-
ment of 112. On side bending, the
Cobb measurement was 73 and on
C D
traction view was 67. (continued)
the transverse processes. Raising thick local flaps with the paraspi- encouraged. To allow mobilization following surgery, one should
nal muscles (including the trapezius, latissimus, and rhomboids make sure that sufficient implant stability is obtained at the time
in one thick layer) is often necessary. These large potential dead of the temporary rod application.
spaces should be drained with closed suction drains to lower the
likelihood of hematoma formation, which could become sec-
PEARLS AND PITFALLS
ondarily infected.
In the postoperative management of a two-stage surgery, 1. Avoid using the most proximal and distal fusion levels as
nutrition is a primary concern. The use of total parenteral nutri- fixation points for the temporary rod as some plowing of
tion in these patients immediately following the initial procedure temporary anchors can be expected.
is recommended as it optimizes patients nutritional status. Total 2. Pedicle screws in the upper thoracic vertebrae tend to plow
parenteral nutrition should be continued until adequate regular in a cephalad direction rather easily; for this reason, we gen-
oral intake is demonstrated. Mobilization such as sitting, stand- erally use up-going hooks for cephalad fixation of the tem-
ing, and walking to help avoid pulmonary and other problems is porary rod.
LWBK836_Ch117_p1265-1278.indd 1276 8/25/11 10:06:44 PM
Chapter 117 Role of Halo Traction and Halo-Femoral Traction in Paralytic/Neuromuscular Scoliosis 1277
E F G
H I
Figure 117.15. (Continued) (E) Intraoperative anteroposterior radiograph demonstrating temporary rod
anchored to two ribs on the top left. Distraction caused some derotation of the vertebral bodies, making
placement of the concave apical pedicle screws easier. (F and G) Postoperative radiographs demonstrating
improvement from preoperative Cobb of 112 down to 26. (H and I) Postoperative clinical photographs.
LWBK836_Ch117_p1265-1278.indd 1277 8/25/11 10:06:46 PM
1278 Section X Paralytic Deformity
3. The temporary rod should be placed as early as possible dur- 4. Buchowski JM, Bhatnagar R, Skaggs DL, et al. Temporary internal distraction as an aid to
correction of severe scoliosis. J Bone Joint Surg Am 2006;88:2035--2041.
ing the first surgery, so multiple distractions can be applied 5. Buchowski JM, Skaggs DL, Sponseller PD. Temporary internal distraction as an aid to cor-
to the rods during the procedure as releases and osteoto- rection of severe scoliosis. Surgical technique. J Bone Joint Surg Am 2007;89(Suppl 2):
297--309.
mies are performed.
6. Dormans JP, Criscitiello AA, Drummond DS, et al. Complications in children managed
4. One should be aware of the risk of elevating the left shoul- with immobilization in a halo vest. J Bone Joint Surg Am 1995;77:1370--1373.
der with aggressive distraction. 7. Garfin SR, Botte MJ, Waters RL, et al. Complications in the use of the halo fixation device.
J Bone Joint Surg Am 1986;68:320--325.
5. Neuromonitoring is essential during the procedure as the 8. Huang MJ, Lenke LG. Scoliosis and severe pelvic obliquity in a patient with cerebral palsy:
spine will be lengthened. surgical treatment utilizing halo-femoral traction. Spine 2001;26:2168--2170.
9. Janus GJ, Finidori G, Englebert RH, et al. Operative treatment of severe scoliosis in osteo-
genesis imperfecta: results of 20 patients after halo traction and posterior spondylodesis
CONCLUSION with instrumentation. Eur Spine J 2000;9:486--491.
10. Kane WJ, Moe JH, Lai CC. Halo-femoral pin distraction in the treatment of scoliosis. J Bone
Joint Surgery [Am] 1967;49:1018--1019.
The goal of surgical management of severe spinal deformities 11. Kumar K. Spinal deformity and axial traction. Spine 1996;21:653--656.
12. MacEwen GD, Bunnell WP, Sriram K. Acute neurological complications in the treatment
is to optimally correct the sagittal and coronal spinal deformity of scoliosis. A report of the Scoliosis Research Society. J Bone Joint Surg Am 1975;57:
in as safe a manner as possible (Fig. 117.15). The three traction 404--408.
13. Mubarak SJ, Camp JF, Vuletich W, et al. Halo application in the infant. J Pediatr Orthop
techniques presented in this chapter have been demonstrated
1989;9:612--614.
to be safe and efficacious tools in the overall surgical treatment. 14. Ransford AO, Manning CW. Complications of halo-pelvic distraction for scoliosis. J Bone
Each technique has its strengths and weaknesses and the sur- Joint Surg [Br] 1975;57:131--138.
15. Rinella A, Lenke LG, Whitaker C, et al. Perioperative halo-gravity traction in the treatment
geon needs to assess the necessity and applicability of adjunc- of severe scoliosis and kyphosis. Spine 2005;30:475--482.
tive traction for each spinal deformity. Continued research is 16. Sink EL, Karol LA, Sanders J, et al. Efficacy of perioperative halo-gravity traction on the
necessary on all three techniques to better delineate the opti- treatment of severe scoliosis in children. J Pediatr Orthop 2001;21:519--524.
17. Swank SM, Lonstein JE, Moe JH, et al. Surgical treatment of adult scoliosis. A review of two
mal indications and technique of traction. Despite the recent hundred and twenty-two cases. J Bone Joint Surg Am 1981;63:268--287.
advances spinal instrumentation, the time-tested method of 18. Swank SM, Winter RB, Moe JH. Scoliosis and cor pulmonale. Spine 1982;7:343--348.
19. Takeshita K, Lenke LG, Bridwell KH, et al. Analysis of patients with nonambulatory neuro-
axial spinal traction continues to have an important role in the
muscular scoliosis surgically treated to the pelvis with intraoperative halo-femoral traction.
treatment of severe spinal deformities. Spine 2006;31:2381--2385.
20. Toledo LC, Toledo CH, MacEwen GD. Halo traction with the circolectric bed in the treat-
ment of severe spinal deformities: a preliminary report. J Pediatr Orthop 1982;2:554--559.
21. Tredwell SJ, OBrien JP. Apophyseal joint degeneration in the cervical spine following halo-
REFERENCES pelvic distraction. Spine 1980;5:497--501.
22. Vialle R, Delecourt C, Morin C. Surgical treatment of scoliosis with pelvic obliquity in
1. Alman BA, Kim HK. Pelvic obliquity after fusion of the spine in Duchenne muscular dys- cerebral palsy: the influence of intraoperative traction. Spine 2006;31:1461--1466.
trophy. J Bone Joint Surg Br 1999;81:821--824. 23. Wild A, Haak H, Kumar M, et al. Is sacral instrumentation mandatory to address pelvic
2. Barsoum WK, Mayerson J, Bell R. Cranial nerve palsy as a complication of operative trac- obliquity in neuromuscular thoracolumbar scoliosis due to myelomeningocele? Spine
tion. Spine 1999;24:585--586. 2001;26:E325--329.
3. Bonnett C, Perry J, Brown JC, et al. Halo-femoral distraction and posterior spine fusion for 24. Wilkins C, MacEwen GD. Cranial nerve injury from halo traction. Clin Orthop 1977;126:
paralytic scoliosis. J Bone Joint Surg Am 1972;54:202. 106--110.
LWBK836_Ch117_p1265-1278.indd 1278 8/25/11 10:06:49 PM
Potrebbero piacerti anche
- CHAPTER 14 - Treatment of Bone Def - 2008 - Surgical Techniques of The ShoulderDocumento11 pagineCHAPTER 14 - Treatment of Bone Def - 2008 - Surgical Techniques of The ShoulderJaime Vázquez ZárateNessuna valutazione finora
- Aaos 2002Documento120 pagineAaos 2002Yusufa ArdyNessuna valutazione finora
- Cervical Disc Replacement NewDocumento17 pagineCervical Disc Replacement NewmarmerosNessuna valutazione finora
- Lower Limb BlocksDocumento5 pagineLower Limb BlocksParvathy R NairNessuna valutazione finora
- Treatment Scapular Winging 2007Documento7 pagineTreatment Scapular Winging 2007YassineNessuna valutazione finora
- Posterior Approaches To The Tibial PlateauDocumento5 paginePosterior Approaches To The Tibial Plateauana starcevicNessuna valutazione finora
- 4 Arthroscopic Bankart Repair With Inferior To Superior Capsular Shift in Lateral Decubitus Position 1723226228Documento6 pagine4 Arthroscopic Bankart Repair With Inferior To Superior Capsular Shift in Lateral Decubitus Position 1723226228César ArveláezNessuna valutazione finora
- Us Peds Regional 2Documento13 pagineUs Peds Regional 2Julio AltamiranoNessuna valutazione finora
- Kne20 25302 v1 Biosure Opt Tg-FinalDocumento16 pagineKne20 25302 v1 Biosure Opt Tg-FinalJuan Martinez Del AngelNessuna valutazione finora
- Whats New Perctaneuous Pelvis FX Surg ClinOrtNAm20Documento8 pagineWhats New Perctaneuous Pelvis FX Surg ClinOrtNAm20Antonio PáezNessuna valutazione finora
- Rehabilitation of Shoulder Impingement Syndrome and Rotator Cuff Injuries: An Evidence-Based ReviewDocumento10 pagineRehabilitation of Shoulder Impingement Syndrome and Rotator Cuff Injuries: An Evidence-Based ReviewEduardo Santana SuárezNessuna valutazione finora
- 1 s2.0 S1058274610003769 MainDocumento9 pagine1 s2.0 S1058274610003769 MainGina Milena Rodriguez SarmientoNessuna valutazione finora
- 19 Haasper Hinged FixatorDocumento4 pagine19 Haasper Hinged FixatorudaysravsNessuna valutazione finora
- An Unusual Case of Elbow Dislocation and A Review of The LiteratureDocumento3 pagineAn Unusual Case of Elbow Dislocation and A Review of The LiteratureNick LasanianosNessuna valutazione finora
- Open Repair of Anterior Shoulder Instability: Michael J. PagnaniDocumento11 pagineOpen Repair of Anterior Shoulder Instability: Michael J. PagnaniJaime Vázquez ZárateNessuna valutazione finora
- Traction : LumbarDocumento10 pagineTraction : LumbarAkshaya MistryNessuna valutazione finora
- Bankarts LesionDocumento6 pagineBankarts Lesionkrissh20Nessuna valutazione finora
- Hip Scope AnchorDocumento9 pagineHip Scope AnchorMarcelo Wiltemburg AlvesNessuna valutazione finora
- Hemivertebra Resection: Surgical ProceduresDocumento10 pagineHemivertebra Resection: Surgical Proceduresmetasoniko81Nessuna valutazione finora
- Aaos2007 Hip Knee PDFDocumento61 pagineAaos2007 Hip Knee PDFHéctor Pando SánchezNessuna valutazione finora
- SHOULDER INSTABILITY ManagDocumento18 pagineSHOULDER INSTABILITY ManagFarhan JustisiaNessuna valutazione finora
- Bristow Laterjet Protocol PDFDocumento10 pagineBristow Laterjet Protocol PDFVlad FocaNessuna valutazione finora
- Rehabilitation Techniques for Flexor Tendon RepairsDocumento9 pagineRehabilitation Techniques for Flexor Tendon RepairsAzmi FarhadiNessuna valutazione finora
- Percutaneous Medial Collateral Ligament Repair and Posteromedial Corner Repair With Suture Tape AugmentationDocumento5 paginePercutaneous Medial Collateral Ligament Repair and Posteromedial Corner Repair With Suture Tape AugmentationGerson Aldair FariasNessuna valutazione finora
- Reversetotalshoulder Arthroplasty: Early Results of Forty-One Cases and A Review of The LiteratureDocumento11 pagineReversetotalshoulder Arthroplasty: Early Results of Forty-One Cases and A Review of The LiteratureBruno FellipeNessuna valutazione finora
- Aco102 085dDocumento2 pagineAco102 085dDonny HendrawanNessuna valutazione finora
- Approaches For Primary Total Hip ReplacementDocumento6 pagineApproaches For Primary Total Hip ReplacementDebNessuna valutazione finora
- MainDocumento7 pagineMainDeborah SalinasNessuna valutazione finora
- Paper RHB Protesis Reversa 211Documento9 paginePaper RHB Protesis Reversa 211Valentina Alejandra Barros WernerNessuna valutazione finora
- Latissimus Dorsi Tendon Transfer For Massive, Irreparable Posterosuperior Rotator Cuff Tears: Surgical TechniqueDocumento6 pagineLatissimus Dorsi Tendon Transfer For Massive, Irreparable Posterosuperior Rotator Cuff Tears: Surgical TechniquemichellmariottiNessuna valutazione finora
- Luxaciones Cadera 3Documento11 pagineLuxaciones Cadera 3Sammy FarahNessuna valutazione finora
- 19-Chadha Et AlDocumento4 pagine19-Chadha Et AlAzmi FarhadiNessuna valutazione finora
- Postlaminectomy Deformities in The Thoracic and Lumbar SpineDocumento6 paginePostlaminectomy Deformities in The Thoracic and Lumbar Spinemetasoniko81Nessuna valutazione finora
- Aaos 2019Documento283 pagineAaos 2019alealer2708Nessuna valutazione finora
- 10 1097@JSA 0b013e3182393e06Documento8 pagine10 1097@JSA 0b013e3182393e06Dr Abdallah BahaaNessuna valutazione finora
- History and Indications of Lateral Tenodesis in AthletesDocumento5 pagineHistory and Indications of Lateral Tenodesis in Athletesसंदीप गुप्ताNessuna valutazione finora
- 0 1 The Pathophysiology of Shoulder Instability 2800953368Documento8 pagine0 1 The Pathophysiology of Shoulder Instability 2800953368César ArveláezNessuna valutazione finora
- Shoulder Arthroplasty WIC - Dr. LSDocumento56 pagineShoulder Arthroplasty WIC - Dr. LSDifitasari Cipta Perdana100% (1)
- LWBK836 Ch98 p1021-1030Documento10 pagineLWBK836 Ch98 p1021-1030metasoniko81Nessuna valutazione finora
- Rehabilitation After Colles' FractureDocumento4 pagineRehabilitation After Colles' FractureAlexisFotiadisNessuna valutazione finora
- ACL Injuries: Anatomy, Physiology, Biomechanics, and ManagementDocumento17 pagineACL Injuries: Anatomy, Physiology, Biomechanics, and Managementwirdah ulfahaini m.Nessuna valutazione finora
- Surgical Repair and Rehabilitation ProtocolsDocumento28 pagineSurgical Repair and Rehabilitation ProtocolsSiti FahwizaNessuna valutazione finora
- Elastic Bandage Traction Technique For Reduction of Distal Tibial FracturesDocumento4 pagineElastic Bandage Traction Technique For Reduction of Distal Tibial FracturesAlejandro Godoy SaidNessuna valutazione finora
- Tendon Transfers For Lateral Pinch: Albert A. Weiss, MD, and Scott H. Kozin, MDDocumento11 pagineTendon Transfers For Lateral Pinch: Albert A. Weiss, MD, and Scott H. Kozin, MDFernando Martín Arce AlvaNessuna valutazione finora
- Patellar Tendon RupturesDocumento4 paginePatellar Tendon Rupturesmarcelogascon.oNessuna valutazione finora
- 2009 CHAPTER 50 - The Role of The Scapula in RehabilitationDocumento14 pagine2009 CHAPTER 50 - The Role of The Scapula in RehabilitationIsrael Matías Chandia RamírezNessuna valutazione finora
- Manage and Treat Traumatic Knee DislocationsDocumento15 pagineManage and Treat Traumatic Knee DislocationsToño Solano NogueraNessuna valutazione finora
- J Neurosurg Pediatr Article p701Documento4 pagineJ Neurosurg Pediatr Article p701mirmasottNessuna valutazione finora
- 1 s2.0 S1877056811000818 MainDocumento4 pagine1 s2.0 S1877056811000818 MainEvans JohnNessuna valutazione finora
- Article 5Documento10 pagineArticle 5Rangga InktaenNdoek'sNessuna valutazione finora
- Proximal Humerus Fracture Fixation Surgical TechnicDocumento6 pagineProximal Humerus Fracture Fixation Surgical TechnicAdhimas WicaksanaNessuna valutazione finora
- Letters To The Editor: Rationale Behind Twin-Block InclineDocumento1 paginaLetters To The Editor: Rationale Behind Twin-Block InclineHARITHA H.PNessuna valutazione finora
- Vertebral Column Resection For Complex Spinal Deformity: Posterior ApproachDocumento16 pagineVertebral Column Resection For Complex Spinal Deformity: Posterior Approachmetasoniko81Nessuna valutazione finora
- CHAPTER 19 - Mini Open Rota - 2008 - Surgical Techniques of The Shoulder ElbowDocumento7 pagineCHAPTER 19 - Mini Open Rota - 2008 - Surgical Techniques of The Shoulder ElbowJaime Vázquez ZárateNessuna valutazione finora
- Anterior Shoulder Instability A Review of PathoanatomyDocumento8 pagineAnterior Shoulder Instability A Review of PathoanatomyNikita TripthiNessuna valutazione finora
- Dryer1980 1Documento2 pagineDryer1980 1Dr LAUMONERIENessuna valutazione finora
- Elbow Arthritis and Removal of Loose Bodies and SpursDocumento11 pagineElbow Arthritis and Removal of Loose Bodies and SpurspuchioNessuna valutazione finora
- Basic Arthroplasty - Unit 4 - Ext Mech Allograft BurnettDocumento21 pagineBasic Arthroplasty - Unit 4 - Ext Mech Allograft BurnettShu Yang HuNessuna valutazione finora
- Diskinesia Escapular - Tratamiento - Sciascia 2020Documento6 pagineDiskinesia Escapular - Tratamiento - Sciascia 2020Neho TerrasNessuna valutazione finora
- Current Techniques in Canine and Feline NeurosurgeryDa EverandCurrent Techniques in Canine and Feline NeurosurgeryAndy ShoresNessuna valutazione finora
- LWBK836 Ch152 p1617-1621Documento5 pagineLWBK836 Ch152 p1617-1621metasoniko81Nessuna valutazione finora
- LWBK836 Ch146 p1575-1580Documento6 pagineLWBK836 Ch146 p1575-1580metasoniko81Nessuna valutazione finora
- Intradural, Extramedullary Spinal Tumors: BackgroundDocumento9 pagineIntradural, Extramedullary Spinal Tumors: Backgroundmetasoniko81Nessuna valutazione finora
- LWBK836 Ch06 p65-73Documento9 pagineLWBK836 Ch06 p65-73metasoniko81Nessuna valutazione finora
- LWBK836 Ch150 p1598-1607Documento10 pagineLWBK836 Ch150 p1598-1607metasoniko81Nessuna valutazione finora
- LWBK836 Ch154 p1633-1648Documento16 pagineLWBK836 Ch154 p1633-1648metasoniko81Nessuna valutazione finora
- LWBK836 Ch147 p1581-1583Documento3 pagineLWBK836 Ch147 p1581-1583metasoniko81Nessuna valutazione finora
- LWBK836 Ch151 p1608-1616Documento9 pagineLWBK836 Ch151 p1608-1616metasoniko81Nessuna valutazione finora
- LWBK836 Ch138 p1487-1498Documento12 pagineLWBK836 Ch138 p1487-1498metasoniko81Nessuna valutazione finora
- Primary Malignant Tumors of The Spine: Gregory S. Mcloughlin Daniel M. Sciubba Jean-Paul WolinskyDocumento12 paginePrimary Malignant Tumors of The Spine: Gregory S. Mcloughlin Daniel M. Sciubba Jean-Paul Wolinskymetasoniko81Nessuna valutazione finora
- Intramedullary Spinal Cord Tumors: Clinical PresentationDocumento15 pagineIntramedullary Spinal Cord Tumors: Clinical Presentationmetasoniko81Nessuna valutazione finora
- Spinal Vascular Malformations: Michelle J. Clarke William E. Krauss Mark A. PichelmannDocumento9 pagineSpinal Vascular Malformations: Michelle J. Clarke William E. Krauss Mark A. Pichelmannmetasoniko81Nessuna valutazione finora
- LWBK836 Ch137 p1485-1486Documento2 pagineLWBK836 Ch137 p1485-1486metasoniko81Nessuna valutazione finora
- LWBK836 Ch148 p1584-1590Documento7 pagineLWBK836 Ch148 p1584-1590metasoniko81Nessuna valutazione finora
- LWBK836 Ch140 p1511-1519Documento9 pagineLWBK836 Ch140 p1511-1519metasoniko81Nessuna valutazione finora
- LWBK836 Ch135 p1460-1473Documento14 pagineLWBK836 Ch135 p1460-1473metasoniko81Nessuna valutazione finora
- LWBK836 Ch126 p1355-1376Documento22 pagineLWBK836 Ch126 p1355-1376metasoniko81Nessuna valutazione finora
- LWBK836 Ch132 p1424-1438Documento15 pagineLWBK836 Ch132 p1424-1438metasoniko81Nessuna valutazione finora
- LWBK836 Ch136 p1474-1484Documento11 pagineLWBK836 Ch136 p1474-1484metasoniko81Nessuna valutazione finora
- LWBK836 Ch131 p1411-1423Documento13 pagineLWBK836 Ch131 p1411-1423metasoniko81Nessuna valutazione finora
- LWBK836 Ch125 p1345-1354Documento10 pagineLWBK836 Ch125 p1345-1354metasoniko81Nessuna valutazione finora
- LWBK836 Ch130 p1399-1410Documento12 pagineLWBK836 Ch130 p1399-1410metasoniko81Nessuna valutazione finora
- Anterior Decompression Techniques For Thoracic and Lumbar FracturesDocumento10 pagineAnterior Decompression Techniques For Thoracic and Lumbar Fracturesmetasoniko81Nessuna valutazione finora
- LWBK836 Ch144 p1553-1559Documento7 pagineLWBK836 Ch144 p1553-1559metasoniko81Nessuna valutazione finora
- Postlaminectomy Deformities in The Thoracic and Lumbar SpineDocumento6 paginePostlaminectomy Deformities in The Thoracic and Lumbar Spinemetasoniko81Nessuna valutazione finora
- LWBK836 Ch134 p1449-1459Documento11 pagineLWBK836 Ch134 p1449-1459metasoniko81Nessuna valutazione finora
- LWBK836 Ch127 p1377-1380Documento4 pagineLWBK836 Ch127 p1377-1380metasoniko81Nessuna valutazione finora
- Bone Grafting and Spine FusionDocumento8 pagineBone Grafting and Spine Fusionmetasoniko81Nessuna valutazione finora
- LWBK836 Ch129 p1390-1398Documento9 pagineLWBK836 Ch129 p1390-1398metasoniko81Nessuna valutazione finora
- LWBK836 Ch128 p1381-1389Documento9 pagineLWBK836 Ch128 p1381-1389metasoniko81Nessuna valutazione finora
- AsphyxiaDocumento35 pagineAsphyxiaAna Cristina Montillano100% (1)
- Intravenous Nutrient TherapyDocumento15 pagineIntravenous Nutrient TherapySuresh IndiaNessuna valutazione finora
- Thesis Recovery After Cataract Surgery: Susanna Porela-TiihonenDocumento40 pagineThesis Recovery After Cataract Surgery: Susanna Porela-TiihonenSaskia MediawatiNessuna valutazione finora
- British Homeopathic AssociationDocumento195 pagineBritish Homeopathic AssociationNasarMahmoodNessuna valutazione finora
- Tracheostomy Care GuideDocumento4 pagineTracheostomy Care GuideSuchismita SethiNessuna valutazione finora
- Surgical Site Infections and Hand Hygiene Discharge TeachingDocumento36 pagineSurgical Site Infections and Hand Hygiene Discharge TeachingKhzNessuna valutazione finora
- Case Report on BPH and Heart DiseaseDocumento18 pagineCase Report on BPH and Heart DiseaseAsrarudin HamidNessuna valutazione finora
- Social MedDocumento6 pagineSocial MedIntekhabAtaharNessuna valutazione finora
- Seminar 5 - Thyroid Disease in PregnancyDocumento25 pagineSeminar 5 - Thyroid Disease in PregnancyHakimah K. SuhaimiNessuna valutazione finora
- Lecture Cardio Physiotherapy 1Documento318 pagineLecture Cardio Physiotherapy 1Nurse GhanemNessuna valutazione finora
- Alarm Fatigue: Use of An Evidence-Based Alarm Management StrategyDocumento8 pagineAlarm Fatigue: Use of An Evidence-Based Alarm Management StrategyMister BigglesworthNessuna valutazione finora
- VenesectionDocumento2 pagineVenesectionMorounshayo OshodiNessuna valutazione finora
- Pre - and Post Test Cardiac ArrhythmiasDocumento6 paginePre - and Post Test Cardiac ArrhythmiasEköw Santiago JavierNessuna valutazione finora
- Prolonged Paroxysmal Sympathetic Storming Associated With Spontaneous Subarachnoid HemorrhageDocumento5 pagineProlonged Paroxysmal Sympathetic Storming Associated With Spontaneous Subarachnoid Hemorrhageiri_balNessuna valutazione finora
- Pycnogenol For Cardiovascular Health - V2010Documento12 paginePycnogenol For Cardiovascular Health - V2010LubimOffNessuna valutazione finora
- Risks of Elective Cesarean SectionDocumento11 pagineRisks of Elective Cesarean SectionLutfiAnny Rahman HakimNessuna valutazione finora
- How Framing Influences Human Decision-MakingDocumento4 pagineHow Framing Influences Human Decision-MakingshreyakarNessuna valutazione finora
- LEPROSYDocumento55 pagineLEPROSYGeraldine Marie SalvoNessuna valutazione finora
- Nursing Care Plan Impaired AdjustmentDocumento1 paginaNursing Care Plan Impaired Adjustmentderic100% (2)
- Copd (Chronic Obstructive Pulmonary Disease)Documento5 pagineCopd (Chronic Obstructive Pulmonary Disease)Kirin JoiezNessuna valutazione finora
- Nursing Care Plan - SLHDocumento4 pagineNursing Care Plan - SLHheartyprincess54Nessuna valutazione finora
- Albuterol Sulfate Drug StudyDocumento4 pagineAlbuterol Sulfate Drug StudyFrancis Corpuz100% (1)
- International Journal of Psychophysiology: Helen Beuzeron-Mangina, Constantine A. ManginaDocumento6 pagineInternational Journal of Psychophysiology: Helen Beuzeron-Mangina, Constantine A. ManginaIcaroNessuna valutazione finora
- AyusynkDocumento2 pagineAyusynknahar570Nessuna valutazione finora
- PERFORMANCE EVALUATION CRITERIADocumento4 paginePERFORMANCE EVALUATION CRITERIAmaryNessuna valutazione finora
- Team 2 Presents Vital SignsDocumento44 pagineTeam 2 Presents Vital Signswiwin100% (1)
- A Deprogrammer For Occlusal Analysis and Simplified Accurate Case MountingDocumento7 pagineA Deprogrammer For Occlusal Analysis and Simplified Accurate Case MountingMichael XuNessuna valutazione finora
- Wellington ICU Drug Manual 2013Documento444 pagineWellington ICU Drug Manual 2013khangsiean89Nessuna valutazione finora
- Multiple SclerosisDocumento35 pagineMultiple SclerosisJc SeguiNessuna valutazione finora
- Ahmed Currim's compilation of James Tyler Kent's unpublished workDocumento31 pagineAhmed Currim's compilation of James Tyler Kent's unpublished worksunnyjamiel63% (8)