Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
En V16n2a07
Caricato da
amarisantiTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
En V16n2a07
Caricato da
amarisantiCopyright:
Formati disponibili
Int. Arch. Otorhinolaryngol. 2012;16(2):195-200.
DOI: 10.7162/S1809-97772012000200007
Original Article
Treatment of retroauricular keloids: Revision of cases treated at the ENT service
of HC/UFPR
Tratamento de queloide retroauricular: Reviso dos casos tratados no servio de
otorrinolaringologia do HC/UFPR
Bettina Carvalho1, Annelyse Cristine Ballin2, Renata Vecentin Becker3, Talita Beithum Ribeiro3, Juliana Benthien Cavichiolo1,
Carlos Roberto Ballin4, Marcos Mocellin5.
1) Graduation in Medicine by UFPR /Federal University of Parana State, Brazil . Resident Doctor for Otolaryngology Service of HC/UFPR - Clinics Hospital/ Federal University
of Parana State in Brazil.
2) ENT by ABORL/Brazilian Association of Otolaryngology and Cervicofacial Surgery. Otolaryngologist Doctor.
3) Academic of Medicine from UFPR/Federal University of Parana State, Brazil.
4) Master of Surgery by UFPR/Federal University of Parana State, Brazil. Responsible for the Skull Maxillofacial Surgery Sector of Otolaryngology Service of HC/UFPR
- Clinics Hospital/ Federal University of Parana State in Brazil.
5) Ph.D. in Otolaryngology by Escola Paulista de Medicina (Medicine School of So Paulo State), Brazil (1986). Entitled Professor at Universidade Federal do Paran /
Federal University at Parana State, Doctor-in-Chief for Otolaryngology Service from HC/UFPR - Clinics Hospital/ Federal University of Parana State, Brazil.
Institution:
Hospital de Clinicas da UFPR.
Curitiba / PR Brazil.
Mailing address: Bettina Carvalho - General Carneiro Street, 181 - Centro, Curitiba / PR - Brazil - Zip-code: 80060-900 E-mail: bettinacarvalho@yahoo.com.br
Article received in July 14, 2011. Article approved in September 19, 2011.
SUMMARY
RESUMO
Introduction: Keloids are benign tumors arising from abnormal
healing of the skin, and there are several procedures available
for their treatment.
Objective: The objective of this study was to evaluate the
outcomes of patients undergoing treatment of keloids after
ear, nose, and throat (ENT) surgeries at our service center.
Method: We conducted thorough, retrospective and prospective
analysis of records of patients undergoing treatment of
retroauricular keloids at our center.
Results: Nine patients were evaluated, and 6 underwent
resection and adjuvant beta-therapy, 2 underwent resection
with local application of corticosteroids, and only 1 underwent
resection without adjuvant therapy. There was no recurrence
of keloids in patients that were treated with beta-therapy in the
early postoperative period. One patient had relapsed despite
corticosteroid administration and late beta-therapy.
Discussion: Several techniques have been used for the
treatment of retroauricular keloids, and beta-therapy is thought
to yield the best results, followed by the use of intralesional
corticosteroids.
Conclusion: Treatment of retroauricular keloids remains a
challenge. While new techniques are being developed,
resection followed by early beta-therapy is still the best treatment
option.
Keywords: keloid, treatment outcome, ear.
Introduo: Queloides so tumores benignos resultantes de
cicatrizao anmala da pele, sendo que existem diversos
procedimentos disponveis para o seu tratamento.
Objetivo: O objetivo deste trabalho avaliar os resultados de
pacientes submetidos a tratamento de queloides
retroauriculares aps cirurgias otorrinolgicas em nosso servio.
Mtodo: Estudo retrospectivo e prospectivo, atravs de anlise de pronturios, dos pacientes submetidos a tratamento de
queloides retroauriculares em nosso servio.
Resultados: Nove pacientes foram avaliados, sendo que 6
foram submetidos a resseco e betaterapia adjuvante, 2 foram submetidos a resseco mais aplicao de corticoide local,
1 foi submetido apenas a resseco sem terapia adjuvante.
No houve recidiva nos casos tratados com betaterapia no
ps-operatrio precoce, 1 paciente apresentou recidiva mesmo com corticoterapia e betaterapia tardia.
Discusso: diversas tcnicas tem sido utilizadas para tratamento dos queloides retroauriculares, sendo que a betaterapia
considerada a com melhores resultados, seguida pela utilizao de corticoides intralesionais.
Concluso: o tratamento dos queloides retroauriculares continua um desafio. Enquanto novas tcnicas no so desenvolvidas, a resseco seguida de betaterapia precoce ainda a
melhor opo.
Palavras-chave: queloide, teraputica, orelha.
Int. Arch. Otorhinolaryngol., So Paulo - Brazil, v.16, n.2, p. 195-200, Apr/May/June - 2012.
195
Treatment of retroauricular keloids: Revision of cases treated at the ENT service of HC/UFPR.
INTRODUCTION
Keloids are benign fibrous tumors (1) that emerge
as reactions to abnormal skin healing. Keloids develop due
to the response of connective tissue to trauma and
inflammation, burns, piercing, or surgeries in areas of high
tension in the body, in predisposed individuals (1, 2).
Keloids may occur at any age regardless of gender;
however, they tend to occur more frequently in individuals
between 10 and 30 years of age. There is a higher
prevalence in patients with dark skin and in the areas of the
ear, shoulder, and chest (3).
The keloid appears as a thick and smooth (2) scar that
extends beyond the original wound and may cause increased
tension on the skin, leading to local deformation (3). Keloids
usually start to grow within the first year after the trauma
occurs, and they rarely regress on their own (2). The main
symptoms associated with keloids are tingling, burning, and
itching, leading to functional changes and discomfort (1).
At the cellular level, the characteristics of keloids
include uncontrolled synthesis and deposition of excessive
collagen and glycoproteins (2). It has been demonstrated
that keloids are composed of polyclonal fibroblasts that are
intrinsically normal, but exhibit abnormal responses to
extracellular signals, thus resulting in excessive collagen
production and decreased degradation of fibrotic scar
tissue (1).
Differential diagnosis of keloids is made with
hypertrophic scars, which are scars confined to the margins
of the original wound and often show spontaneous regression
(2). This distinction is very important, as these entities
require different treatment strategies.
Carvalho et al.
A chart review was performed for patients
undergoing treatment of retroauricular keloids in the
otorhinolaryngology service center, during the period of
2006 to 2009, and we prospectively evaluated patients
undergoing keloid resection in 2010, with a protocol and
evaluation of photos (pre- and postoperative).
We evaluated the type of surgery that resulted in
the keloid, surgery for keloid resection, postoperative
adjuvant treatments (beta-therapy or intralesional application
of corticosteroids), number of recurrences and reoperations,
characteristics of the recurrence (presence of redness,
telangiectasia, coloring, and size of the scar), associated
symptoms (pain and itching), and patient satisfaction
about the outcome.
RESULTS
We evaluated 9 patients (13 ears), aged between 9
and 27 years, including 6 men and 3 women.
Four patients developed keloids after otoplasty, 2
after tympanoplasty, 1 after mastoidectomy, 1 after surgical
correction of a congenital malformation (preauricular sinus),
and 1 after a surgery that was performed at another
institution (and thus cannot be described).
Patients underwent 6 sessions of beta-therapy at the
Erasto Gaertner Hospital, and 2 patients had started taking
corticosteroids and received beta-therapy late.
Two patients received only local corticosteroids
(betamethasone 3mg, Celestone soluspan), and 1 patient
did not undergo adjuvant therapy since the keloid was very
small.
The retroauricular approach is widely used in
otolaryngology, both in middle ear surgery (tympanoplasty,
tympanomastoidectomy) or in the external ear (otoplasty)
for either functional or purely aesthetic outcomes; this
approach may result in a potential site of origin of keloids
due to creating an area of high skin tension.
After the use of adjuvant therapies, we maintained
the use of triamcinolone ointment 1 mg (Oncilom ) with
massage, for approximately 2 months.
The objective of this study was to assess the
epidemiology of patients with keloids (age, sex, skin color,
procedure that led to the keloid) and the results of patients
undergoing treatment of keloids after ear, nose, and throat
(ENT) surgeries at our service center.
The surgical technique is illustrated in Figure 4. The
surgery was performed as follows: local anesthesia by
infiltration of lidocaine 2% + aadrenaline 1:50,000, marking
the margins of the keloid scar with gentian violet, creating
a spindle-shaped incision, peeling the scar in layers, creating
a sliding flap, hemostasis, suturing, and simple surgical
wound dressing.
The results are shown in Table 1 and Figures 1, 2,
and 3.
METHOD
This study was approved by the Ethics Committee
on Human Research of the HC/UFPR.
The beta-therapy was carried out with plates of
Strontium (90Sr). The source of the beta-therapy was a 2cm plate that was packed in a container, as shown in Figure
Int. Arch. Otorhinolaryngol., So Paulo - Brazil, v.16, n.2, p. 195-200, Apr/May/June - 2012.
196
Treatment of retroauricular keloids: Revision of cases treated at the ENT service of HC/UFPR.
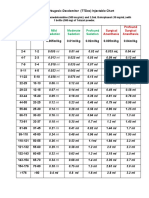
Table 1. Results.
Patient
Previous surgery
1
Bilateral after otoplasty
2
Bilateral after tympanoplasty
3
4
5
6
7
Bilateral after otoplasty
Bilateral after otoplasty
Unilateral after mastoidectomy
Unilateral after tympanoplasty
Unilateral after otoplasty
Unilateral after correction of
congenital malformation
Unilateral
Treatment
Resection + betatherapy + ointment**
Resection + betatherapy + ointment**
Resection unilateral (longer side) + betatherapy
Resection + CTC*** + ointment**
Resection + CTC*** + betatherapy *+ ointment**
Resection + CTC***
Resection + re making of sutures master of Mustard
+ betatherapy
Resection only
Resection + betatherapy + CTC***
Carvalho et al.
Recurrence
no recurrence
no recurrence EL
mild hypertrophy ER
no recurrence
no recurrence
recurrence
no recurrence
no recurrence
no recurrence
no recurrence
* Betatherapy started late (2 months)
** Corticosteroid triamcinolone ointment 1mg (Oncilom )
*** CTC = corticosteroid injection 3mg intralesional betamethasone (Celestone Soluspan)
Figure 1. Case 3: Preoperative (left) and postoperative 3
months (right).
Figure 2. Case 2: Post-operative 3 months.
Figure 3. Case 1: Postoperative 1 year and 1 month.
Figure 4. Surgical procedure - resection of the spindle keloid
retroauricular flap by sliding.
Int. Arch. Otorhinolaryngol., So Paulo - Brazil, v.16, n.2, p. 195-200, Apr/May/June - 2012.
197
Treatment of retroauricular keloids: Revision of cases treated at the ENT service of HC/UFPR.
Carvalho et al.
5. The instructions for use indicate that the board should
stay out of the container only during the treatment period,
the technician must keep as much distance as possible
during the application, and the source of radiation has an
acrylic plate that serves as a barrier to radiation. The patient
is instructed to wash the area to be irradiated and dry the
skin, and not to use any product or application during the
irradiation period. The timing and amount of radiation in
Grays varies with each patient, depending on the extent
of the wound.
DISCUSSION
Keloids are a problem that affects the quality of life
of patients, not only for aesthetic reasons, but also primarily
by the associated symptoms (itching, pain, burning
sensation, and intolerance to some tissues) (4), making it
necessary to utilize an effective, specific treatment approach.
The most common difficulty in treating keloids is
their recurrence after surgical excision. To solve this problem,
various types of adjuvant treatments have been developed.
The various treatment options used to prevent the
recurrence of keloids include continuous pressure after
surgery, application intralesional steroids, use of a carbon
dioxide laser, application of silicone gel, administration of
retinoic acid, covering with silicone gel (1), cryosurgery,
use of chemotherapeutic agents (5-fluorouracil), intralesional
interferon administration, radiation therapy, and others (5).
However, there is no solid evidence that these methods
are effective in prevention of keloid recurrence, and
radiotherapy is the only treatment shown to be effective
in preventing the formation of keloids (1).
It is important to remember that the keloid that is
formed is not radiosensitive, but the fibroblasts in the
recently scarred areas are; therefore, it is necessary to
apply the radiation to the connective tissue in the immediate
postoperative period, during the cellular proliferation and
differentiation stage, and before the fibrotic tissue has
formed (4).
The radiotherapy techniques that are typically
employed include external radiotherapy with superficial
X-rays, brachytherapy with strontium (Sr90) or electron
beams, low-dose brachytherapy (1), high-dose
brachytherapy (6,7), and radiation associated with pre or
postoperative therapy (8).
The mechanism by which radiation acts is not well
understood, but it is believed that radiation destroys
fibroblasts, which are replaced by cells from the blood
stream that migrate from other tissues (1).
Figure 5. Strontium container plate (betatherapy).
Areas of excessive curvature of the skin can lead to
greater difficulty in the delivery of postoperative radiation.
Furthermore, the compression that is required for handling
and radiating newly operated areas often is not well
tolerated or may lead to damage to the areas that have
been recently sutured. Huhne et al. (9) demonstrated a
technique for postoperative radiotherapy that maintains
the anatomical position of the ear, thus minimizing handling
of the wound while maximizing the radiation dose to the
target area. The external auditory canal is protected with
a cotton ball and a lead shield, and the shell is filled with a
moldable material (bolus Supertuff ), thereby creating a
flat and uniform level for the helix and tragus. Another
material (Superflab) is used to fill the retroauricular space,
thus forming a continuous surface with the propeller and
the antihelical fold. It is estimated that this arrangement
would keep the target areas within 95% of the dose limit
of the electron beam.
At our service center, we send patients who
underwent keloid resection with radiotherapy to the Erastus
Gaertner Hospital (oncology hospital) to undergo
postoperative beta-therapy.
Beta-therapy is accomplished using plates of 90Sr
(Strontium 90 radioisotope) in doses of approximately 30
Gy (Gray = unit of absorbed dose) (4).
According to HOCHMAN et al. (10), combining surgery
with beta-therapy is the best treatment option, especially
when the beta-therapy is administered 24 to 48 hours after
the excision, in order to mitigate fibroplasia.
Our department obtained the best results from betatherapy utilization when it was performed early (1 patients
Int. Arch. Otorhinolaryngol., So Paulo - Brazil, v.16, n.2, p. 195-200, Apr/May/June - 2012.
198
Treatment of retroauricular keloids: Revision of cases treated at the ENT service of HC/UFPR.
beta-therapy was started the same day of surgery) in 4
patients. Only 1 patient received late beta-therapy (2
months after surgery), which resulted in relapse, even with
early corticosteroid administration.
Postoperative percutaneous radiation therapy is
associated with a few side effects, such as darkening of the
skin in the treated area (11), but no serious adverse effects
(such as the emergence of tumors) have been demonstrated,
even in the long term (4,11).
Among the variety of technical aids that are available
for the treatment of keloids, intralesional injection of
corticosteroids (usually triamcinolone) is used for prevention
or treatment of keloids in existing wounds. This
administration may be intraoperative and postoperative,
and has been shown to reduce the rate of recurrence of
keloids (11); according to HOCHMAN et al. (10), it reduces
keloid recurrence to less than 50%.
Bermueller et al. (12) achieved good cosmetic
results and a high degree of patient satisfaction with
resection, preparation of a skin flap, and retroauricular
keloid complete closure with injection of corticosteroids to
prevent formation of ear lobe keloids.
In our department, for the prevention of keloids
after surgery, intralesional corticosteroids are used during
the immediate postoperative period (1 mL per application,
once every 2 weeks, for the first 2 months after surgery).
We use 3-mg betamethasone (Celestone soluspan).
Although we still prefer beta-therapy, corticosteroid
application is an alternative treatment when beta-therapy
is not possible or not desired by the patient. In our study,
4 patients underwent application of corticosteroids after
surgical resection, with good results.
The main side effects of corticosteroid therapy are
local atrophy, depigmentation, and telangiectasia of the
treated scar; although infrequent, some patients may be
adverse to the use of systemic corticosteroids, even with
the intralesional application. LIU and YEMCHA (13) reported
a case of iatrogenic Cushings syndrome that developed
after the use of intralesional injections of triamcinolona for
the treatment of multiple keloids. The authors suggest,
therefore, that physicians consider the dose and number of
injections of intralesional corticosteroids that are necessary
for the treatment of keloids. Taking into account the
potential for recurrence and the aggressiveness of disease,
there may be a need for large volumes and frequency of
injections, which increases the potential of systemic effects;
thus, patients should have their adrenal function monitored
before signs of the syndrome appear.
Carvalho et al.
risk of recurrence depends on local factors that are related
to surgical wounds and on general factors that are related
to the patient. A higher recurrence of keloids is seen in
areas in which the wound is sutured with tension, or there
is postoperative infection and dehiscence of the suture.
Patients with positive family history and previous history of
recurrent keloids that have failed previous therapies have
a higher risk of recurrence (10,11).
In our study, 1 patient did not undergo adjuvant
therapy, but the keloid was small, showed no recurrence,
and the patient was satisfied with the outcome.
The peak incidence of relapse occurs until around
the 13th month, so patients with keloids should be monitored
for a longer period of time (10). We routinely monitor our
patients for at least 1 year after the completion of treatment.
Although keloids are more common in people of
black ethnicity, all patients that were treated in our
department were classified as Caucasians. According to
HOCHMAN et al. (10), relapse rates show no relationship with
ethnicity, age, or size of the lesion.
At the biochemical level, previous studies
demonstrated increased expression of the cytokine
transforming growth factor beta (TGF-) and its receptors
in fibroblasts from keloid tissue. The TGF- family mediates
physiological growth and promotes cell proliferation, inhibits
apoptosis, induces synthesis of cyclooxygenase-2 (COX2), and promotes tumor growth, invasion, and angiogenesis
by upregulating the secretion of matrix metalloproteinase2 (MMP-2). GAO et al. (14) showed increased expression of
the gene for growth differentiation factor-9 (GDF-9, a
family member of TGF-) in fibroblasts of the peripheral
region of the keloid tissue, which is the area that is
responsible for the growth and invasion of normal tissues.
This result suggests that the fibroblasts that produce a
GDF-9 are responsible for the invasion of peripheral tissue.
ULRICH et al. (15) showed that the formation of
granulation tissue and wound healing depends on an
adequate balance between the synthesis and degradation
of the extracellular matrix, and that an excessive synthesis
or degradation deficiency (or both) can lead to pathological
scarring, including keloids. The enzymes involved in this
process are the matrix metalloproteinases (MMPs), enzymes
that degrade extracellular matrix components, which are
inhibited by tissue inhibitors of metalloproteinases (TIMPs).
The authors indicate that future non-surgical treatments
that reduce the expression of TIMPs and increase that of
MMPs may be effective therapeutic strategies for the
treatment of pathologic scars such as keloids (15).
However, regardless of type of adjuvant used, the
While these future therapeutic approaches may
Int. Arch. Otorhinolaryngol., So Paulo - Brazil, v.16, n.2, p. 195-200, Apr/May/June - 2012.
199
Treatment of retroauricular keloids: Revision of cases treated at the ENT service of HC/UFPR.
prove to be effective, the treatment of keloids, including
retroauricular keloids, remains a challenge.
Carvalho et al.
Yaparpalvi R, Delrowe J, Beitler JJ. Adjuvant high dose
brachytherapy (Ir-192) in the managemente of keloids
which have recurred after surgical excision and external
radiation. Radiotherapy and Oncology. 2004, 73:233236.
CONCLUSION
The treatment of retroauricular keloids presents
many difficulties, either with regard to the treatment of
keloid itself or due to location.
In our department, we obtained the best results
when surgical excision was combined with beta-therapy
that was started soon after surgery.
It is expected that the development of other nonsurgical therapies will facilitate the treatment of retroauricular
keloids and other keloids as well.
BIBLIOGRAPHIC REFERENCES
1. Viani GA, Stefano EJ, Afonso SL, De Fendi LI . Posoperative
strontium-90 brachytherapy in the prevention of keloids:
results and prognostic factors. Int J Radiation Oncology Biol
Phys. 2009, 73(5):15101516.
2. Froelich K, Staudenmaier R, Leinsasse N, Hagen R.
Therapy of auricular keloids: review of different treatmente
modalities and proposal for a therapeutic algorithm. Eur
Arch Otorhinolaryngol. 2007, 264:14971508.
3. Correspondence and Comunication. Use of colchicine to
prevent recurrence of ear keloids. A new approach. Journal
of Plastic, Recontructive and Aesthetic Surgery. 2010, 63:
e650-e652.
4. Oliveira Jr B, Lastoria JC, Pereira HR, Silveira LVA, Oliveira
LP, Stolf HO. Estudo comparativo entre o tratamento
radioterpico com eltrons e betaterapia, aps cirurgia de
quelides. Surgical & Cosmetic Dermatology. 2009, 1(2):5357.
5. Durani P, Bayat A. Levels of evidence for the treatment
of keloid disease. Jouranl of Plastic, Reconstructive and
Aesthetic Surgery. 2008, 61:4-17.
6. Garg MK, Weiss P, Sharma AK, Gorla GR, Jaggernauth W,
7. Veen RE, Kal HB. Postoperative high-dose-rate
brachytherapy in prevention of keloids. Int. J. Radiation
Oncology Biol Phys. 2007, 69(4):12051208.
8. Stahl S, Barnea Y, Weiss J, Zaretski A, Leshem D, Miller
E, Shafir R, Ben-yosef R, Gur E. Treatment of earlobe keloids
by extralesional excision combined with preoperative and
postoperative sandwich radiotherapy. Plastic and
Reconstructive Surgery. January 2010,125(1).
9. Huhn JL, Johnson EL, St Clair W. Adjuvant radiation of
bilateral postauricular keloids: an illustration of technique.
Medical dosimetry 2007, 32(4):278-280.
10. Hochman B, Locali RF, Oliveira LQR, Ferreira LM.
Disfunes cicatriciais hiperproliferaticas: Quelide. Estima.
2004, 4(4):33-39.
11. Ragoowansi R, Cornes PGS, Glees JP, Powell BW, Moss
LH. Ear-lobe keloids: treatment by a protocol of surgical
excision and immediate postoperative adjuvant
radiotherapy. British Journal of Plastic Surgery. 2001, 54:
504-508.
12. Bermueller C, Rettinger G, Keck T. Auricular keloids:
treatment and results. Eur Arch Otorhinolaryngol. 2010,
267:575580.
13. Liu MF, Yencha M. Cushings syndrome secondary to
intralesional steroid injections of multiple keloids.
OtolaryngologyHead and Neck Surgery. 2006, 135:960961.
14. Gao Z, Wu X, Song N, Zhang L, Liu W. Differential
expression of growth differentiation factor-9 in keloids. Burns.
2010.
15. Ulrich D, Ulrich F, Unglaub F, Piatkowski A, Pallua N.
Matrix metalloproteinases and tissue inhibitors of
metalloproteinases in patients with different types of scars
and keloids. Journal of Plastic, Reconstructive & Aesthetic
Surgery. 2010, 63:1015-1021.
Int. Arch. Otorhinolaryngol., So Paulo - Brazil, v.16, n.2, p. 195-200, Apr/May/June - 2012.
200
Potrebbero piacerti anche
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- Post Test 5Documento18 paginePost Test 5amarisanti98% (48)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- Read MeDocumento1 paginaRead MeamarisantiNessuna valutazione finora
- TextDocumento13 pagineTextamarisantiNessuna valutazione finora
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- American Journal of Gastroenterology Volume Issue 2016 (Doi 10.1038/ajg.2016.499) Vanheel, H Carbone, F Valvekens, L Simren, M Tornblom, H Va - Pathophysiological Abnormalities in Functional DDocumento9 pagineAmerican Journal of Gastroenterology Volume Issue 2016 (Doi 10.1038/ajg.2016.499) Vanheel, H Carbone, F Valvekens, L Simren, M Tornblom, H Va - Pathophysiological Abnormalities in Functional DamarisantiNessuna valutazione finora
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Daftar PustakaDocumento6 pagineDaftar PustakaamarisantiNessuna valutazione finora
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- (Neuroscience Education Institute) Insights Into T (BookFi) PDFDocumento22 pagine(Neuroscience Education Institute) Insights Into T (BookFi) PDFamarisantiNessuna valutazione finora
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- Constipation in Children JournalDocumento10 pagineConstipation in Children JournalamarisantiNessuna valutazione finora
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- The Effects of Paracetamol and Parecoxib On Kidney FunctionDocumento7 pagineThe Effects of Paracetamol and Parecoxib On Kidney FunctionamarisantiNessuna valutazione finora
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- Steps of Repertorization - 5e097dab9ad98Documento18 pagineSteps of Repertorization - 5e097dab9ad98Sowjanya JyothsnaNessuna valutazione finora
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- Flip Class Reflection 1Documento3 pagineFlip Class Reflection 1api-301784889Nessuna valutazione finora
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Overview of Nephrotic SyndromeDocumento19 pagineOverview of Nephrotic Syndromefarmasi_hm100% (1)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Clotting Concept Analysis Diagram and ExplanationDocumento2 pagineClotting Concept Analysis Diagram and ExplanationJulius Haynes100% (1)
- Nutritional DiseasesDocumento30 pagineNutritional DiseasesSwara SawantNessuna valutazione finora
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- SimMan 3G BrochureDocumento8 pagineSimMan 3G BrochureDemuel Dee L. BertoNessuna valutazione finora
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- OT Relevance RMTDocumento12 pagineOT Relevance RMTFredy RamoneNessuna valutazione finora
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- ORAL DIAG Q&A DentistryDocumento46 pagineORAL DIAG Q&A DentistryTJ OberioNessuna valutazione finora
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- Threats of Vector-Borne Zoonotic Disease in Europe: Dogs, Drosophilids, and Oriental Eye WormDocumento3 pagineThreats of Vector-Borne Zoonotic Disease in Europe: Dogs, Drosophilids, and Oriental Eye WormGustavo AndresNessuna valutazione finora
- Programmed Postoperative Physiotherapy May Improve Functional Outcomes in Pneumonectomy Patients of Rare Causes Case SeriesDocumento7 pagineProgrammed Postoperative Physiotherapy May Improve Functional Outcomes in Pneumonectomy Patients of Rare Causes Case SeriesAtu KaushalNessuna valutazione finora
- Malpractice CaseDocumento4 pagineMalpractice CaseAr-jay JubaneNessuna valutazione finora
- The Gut Microbiota in Anxiety and Depression - A Systematic Review (Simpson Et Al, 2020)Documento18 pagineThe Gut Microbiota in Anxiety and Depression - A Systematic Review (Simpson Et Al, 2020)GokushimakNessuna valutazione finora
- CancerDocumento70 pagineCancerapi-3735995100% (1)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- Suspected Preeclampsia AlgorithmDocumento1 paginaSuspected Preeclampsia Algorithmmisstina.19876007100% (1)
- People Running PowerPoint TemplatesDocumento16 paginePeople Running PowerPoint TemplatesPutri Aulia AmaraNessuna valutazione finora
- Farmakologi Cns Stimulants DrugsDocumento15 pagineFarmakologi Cns Stimulants DrugsRifqiNessuna valutazione finora
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- RL2 CCR Book March-2021-P117-118Documento2 pagineRL2 CCR Book March-2021-P117-118Judah ObengNessuna valutazione finora
- African Swine FeverDocumento4 pagineAfrican Swine FeverJamaicah PattungNessuna valutazione finora
- Efficacy of Unani Formulation in Infertility Among Obese Women: A Clinical StudyDocumento10 pagineEfficacy of Unani Formulation in Infertility Among Obese Women: A Clinical StudyWaseem AhmedNessuna valutazione finora
- McqepilipsyDocumento3 pagineMcqepilipsyNguyen Anh TuanNessuna valutazione finora
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Notes: Generally, What Are They?Documento10 pagineNotes: Generally, What Are They?Yusril MarhaenNessuna valutazione finora
- Pricelist 13 Juli 2020Documento21 paginePricelist 13 Juli 2020Achmad Sya'idNessuna valutazione finora
- BRO-ZEDEX RANGE Knowledge ExpressDocumento7 pagineBRO-ZEDEX RANGE Knowledge Expressamit khairnarNessuna valutazione finora
- Daftar Isi FormulariumDocumento9 pagineDaftar Isi FormulariumNilam atika sariNessuna valutazione finora
- TTDexDocumento2 pagineTTDexSparKY NIghtcoreNessuna valutazione finora
- Chronic Renal FailureDocumento1 paginaChronic Renal Failurejj_cuttingedges100% (2)
- Renal Calculi: Ahmednagar Homoeopathic Medical College & Hospital AhmednagarDocumento15 pagineRenal Calculi: Ahmednagar Homoeopathic Medical College & Hospital AhmednagarSuhas IngaleNessuna valutazione finora
- PHAR 400 Pharmacology I Master 1-3-21Documento5 paginePHAR 400 Pharmacology I Master 1-3-21Zahid Bashir BhattiNessuna valutazione finora
- 0 Small FoundationsDocumento9 pagine0 Small FoundationsFrancesc Xavier Bofill De RosNessuna valutazione finora
- GDS Scale PDFDocumento2 pagineGDS Scale PDFDiyah RahmawatiNessuna valutazione finora
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)