Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Use of Laser in General Dental Practice
Caricato da
Myat NyanCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Use of Laser in General Dental Practice
Caricato da
Myat NyanCopyright:
Formati disponibili
Vol. 21, No.
1, January 2014
Review Article
Use of lasers in
everyday dental practice
Verica Pavlic1, Tijana Adamovic2, Myat Nyan3
1 Department of Periodontology and Oral is collimated, monochromatic and coherent
Medicine, Institute of Dentistry, Banja Luka, Bosnia (Ishikawa et al, 2009). These basic characteristics
are making advantageus biologic properties of
and Herzegovina
lasers, namely possibility to perform treatment
2 Department of Periodontology and Oral options beyond those available via conventional
Medicine, Medical faculty, University of Banja Luka, techniques.
Bosnia and Herzegovina
Lasers, in general, consist of an active
3 Department of Prosthodontics, University of medium and a pumping source enclosed in
Dental Medicine, Yangon, Myanmar
optical cavity. Based on the active lasing medium,
it can be divided on gas, a solid state crystal lasers,
Corresponding author:
diode, excimer and dye lasers (Table 1). Further,
lasers can be divided according to their maximum
Verica Pavlic, DDS, PhD
Department of Periodontology and Oral Medicine, output energy level on soft lasers (low output)
and hard lasers (high output) (Aoki et al., 2008).
Institute of Dentistry,
The specific interaction between laser light and
Zdrave Korde 4, 78000 Banja Luka
biological tissue is determined by the wavelength
Bosnia and Herzegovina
of the laser. Because of monochromacity of laser
Tel/fax: +387 66 769-844
energy, different laser wavelengths have different
E-mail address: dr.vericapavlic@gmail.com
absorption coefficients when in contact with
Abstract
dental tissue. Because human dental tissues are
composed of a combination of water, apatite
Since the development of the ruby laser by crystal, blood and tissue pigment, the dentist must
Maiman in 1960, it has been efficiently used for choose the best wavelength of laser for each and
diagnostics, surgery and therapeutic applications every treatment. For soft tissue treatment, dentist
in dentistry. With expansion in future application can use any dental laser regardless of wavelength,
of lasers in modern dentistry, it is expected that because all dental lasers are absorbed by one or
number of potential laser users will continue more of the soft tissue components. For hard tissue
to grow. Therefore, the aim of this review is to surgery, however, the only lasers to be selected are
present some of the wide range of possible dental from erbium family (Er:YAG and Er,Cr:YSGG), since
treatment options, which can be successfully they can easily ablate layers of calcified tissue
accomplished employing lasers, either used alone without any thermal effects.
or in combination with conventional therapy
approaches.
Low-level laser irradiation (LLLI; lowlevel laser therapy-LLLT, photo-bio-modulation)
Key words/terms: laser, dental lasers, lasers in is considered to be a certain amount of energy
dentistry
that scatters and penetrates into the surrounding
tissues and cells simultaneously during high-level
Introduction
laser irradiation (Fig. 1). Recently, laser systems with
Laser is an acronym for "Light Amplification power and energy densities below the destructive
by Stimulated Emission of Radiation". The first level have been introduced (pure LLLI). LLLI
device, ruby laser, was created in 1960 by Maiman causes analgesia and cell/tissue biostimulation
and since then it has been efficiently used for (e.g. increase of systemic microcirculation and
diagnostics, surgery and therapeutic applications tissue oxygenation, cell metabolism and/or tissue
in dentistry (Brighton et al., 1997). Laser light regeneration and potential tissue healing) without
Myanmar Dental Journal
any thermal damage. Even though several theories
have been proposed, the exact underlying
mechanism by which LLLT impairs tissue healing
and pain attenuation is still unknown (Ohshiro &
Calderhead, 1991; Kreisler et al., 2004; Ando et al.,
1996).
Lasers are successfully used in surgical
(ablative) and non-ablative (LLLT) manner. In
ablative manner lasers are used to remove as
much of oral tissue as possible. Patients are feeling
mild warmth on the targeted place; therefore in
most of the cases anesthesia is required prior to
irradiation, as a part of surgical procedure (Pavlic
& Vujic-Aleksic, 2013). One of the biggest concerns
in ablative manner is laser-related hazard-plume
(having a potential for carrying viral particles). In
contrast to ablative lasers, LLLT is non-destructive,
non-thermal and pain free procedure, which
usually does not require anesthesia and do not
carry any potential of plume hazard to the surgeon
and personnel. Further, it does not produce visual
effects of thermal damage to the oral mucosa such
as ablation, coagulation, vaporization or erythema
(Pavlic & Vujic-Aleksic, 2013).
To date, laser dentistry is still not fully
incorporated in everyday dentistry, mainly due to
the high costs of laser devices. With expansion in
future application of lasers in modern dentistry,
it is expected that specific laser technologies will
become an essential component of contemporary
dental practice with increased number of potential
laser users. Therefore, the aim of this review is
not intended to be a comprehensive literature
review but rather presentation of possible dental
treatment options, which can be successfully
accomplished employing lasers, either used alone
or in combination with conventional therapy
approaches.
Lasers in periodontology
Lasers are used in periodontology as
a treatment modality for soft and hard tissue
surgery as well as non-surgical treatment that
have been proven by a wide range of researchers.
Lasers (CO2, diode, Nd:YAG lasers), which are
used for treatment of soft tissues (frenectomy,
gingivectomy, gingivoplasty) can ablate oral
soft tissues easily and promote hemostasis by
coagulating and occluding small blood vessels
instantly, making surgical area clearly visible
and bloodless. Further, surgery done by lasers
reduces pain, swelling and wound contraction.
But since periodontium is made from hard and
soft tissues, recently introduced erbium lasers left
the possibility to treats both, soft and hard tissues,
without major thermal damages (Aoki et al., 2008;
2000). Therefore, erbium lasers are considered the
most promising laser devices in periodontology.
Frenectomy
Labial frenulums are occasionally
inadequate in size or location, leading to functional
and esthetic limitations. Laser frenectomy can be
successfully done by any dental laser regardless
of wavelength and with significant reduction of
surgical time in comparison with conventional
surgery. Laser frenectomy does not require
anesthesia prior to surgery, reduces pain and
bleeding during surgery, avoids the need of
suturing and special postoperative care (PiSnchez et al., 2012).
Gingivectomy/Gingivoplasty (soft tissue crown
lengthening)
Laser gingivoplasty or gingivectomy can
be successfully performed for the excision of the
soft-tissue wall of the periodontal pocket, for
elimination of suprabony pockets after adequate
initial preparation, for easy access in the presence
of suprabony pockets and in case of gingival
overgrowths, either asymmetrical or unesthetic
(Shankar et al. 2013).
Non-surgical periodontal therapy
Periodontitis is chronic inflammatory
disease caused by bacterial infection, that in later
stages involves progressive loss of alveolar bone,
and if left untreated can lead to subsequent tooth
loss. Some of the advantages of employing erbium
lasers include: successful calculus removal, its
bactericidal and detoxifying effects, reducing of
inflammation and faster healing of periodontal
pockets through elimination of bacteria (Moritz
et al., 1998), resulting in better therapy outcome,
such as reduction of periodontal pocket depth and
clinical attachment level gain (Aoki et al., 2008).
Water irrigation during Er:YAG laser irradiation is
considered essential to eliminate thermal sideeffects on the root surface. In most of the cases,
lasers are described as an adjunct to rather than a
replacement for conventional therapy (mechanical
debridement).
Regenerative periodontal surgery
Periodontal therapy is characterized
by debridement of root surface and successful
removing of diseased granulated tissue from
the bone defect, correction of the alveolar bone
and surgical field disinfection. For this purpose,
Er:YAG laser is considered optimal due to ability
to vaporize bone tissue efficiently without major
thermal side effects (Ishikawa et al., 2000-2009;
Aoki et al, 2008). Recently, American Academy of
Periodontology concluded that the Er:YAG laser
Vol. 21, No. 1, January 2014
demonstrated the best application of laser use
directly on hard tissue, leaving the least thermal
damage and creating a surface that suggest
biocompatibility for soft tissue attachment. Studies
have demonstrated the ability of the Er:YAG laser
to remove lipopolysaccharides from root surfaces,
facilitate removal of the smear layer after root
planning and remove calculus and cementum
(Research, Science and Therapy Committee of
the American Academy of Periodontology, 2002).
Further, recently introduced dual-wavelength
technique (CO2 and Er:YAG lasers) left the
possibility to use the most beneficial characteristics
of both laser systems (Er:YAG for debridement
and disinfection and CO2 for de-epithelization) in
tremendous promise in regenerative periodontal
surgery.
of wavelength (diode, Er:YAG, Nd:YAG, CO2), mainly
due to abilities to speed up the wound healing
process and cause significant analgesia while
reducing the number of recurrences. Lasers are
used in non-contact mode at the distance of 5-6
mm from herpetic lesions. It is particularly useful
for elderly patients, due to the low frequency of
side effects (Schindl &, Neumann, 1999).
Removal of drug-induced gingival hyperplasia
bullous disease of the skin and mucosa that leads
to flaccid blisters and painful multiple erosions.
Lasers (ablative/non-ablative) can be used either
alone or combined with conventional treatment
modalities, such as topical corticosteroids
(Bhardwaj et al., 2010). When used in low-level
mode, CO2 and/or diode lasers are reported
beneficial in therapy of PV lesions (Minicucci et al.,
2012).
Oral lichen planus/ Premalignant lesions
Oral lichen planus (OLP) is chronic
immunologic mucocutaneous inflammatory
disease of oral mucosa. CO2 laser is proven to be
useful and effective in fast and easy ablation of OLP
lesion, with no need for suturing. Further, faster
healing process was uneventful with minimal
post-operative discomfort, minimal pain, swelling
Lasers in oral surgery, oral pathology and oral or bleeding and without visible scarring. Also, LLLT
namely for biostimulation and analgesia of painful
medicine
OLP lesions was suggested (Pavlic & Vujic-Aleksic,
The fields of oral surgery, oral pathology 2013).
and oral medicine are having a great benefit from
laser use. We can also successfully combined use of Pemphigus Vulgaris
laser with conventional techniques.
Pemphigus vulgaris is an autoimmune
Hyperplastic gingiva usually occur
secondary to use of anti-hypertensive drugs (e.g.
calcium channel blockers), anticonvulsants and
immunosuppressant (e.g. cyclosporine). Even
though any laser wavelength can be used to
successfully ablate gingival tissue and accomplish
this procedure, CO2 laser with excellent coagulative
abilities is consider optimal (Muralikrishna et al.,
Pericoronitis
2013).
Treatment of recurrent aphthous stomatitis
Recurrent aphthous stomatitis (RAS)
is described as multifactor immunologic
inflammatory lesion in the oral cavity, characterized
by painful, recurrent single/multiple shallow
ulcerations of mucosal tissues. In the treatment of
painful RAS lesions, lasers are successfully used in
surgical (ablative) and non-ablative (LLLT) manner.
In ablative manner, any laser is used to remove as
much of necrotic RAS tissue as possible, including
the inflamed halo around the aphthae (Colvard &
Kuo, 1991). When employing LLLT, scanning over
RAS lesion at the distance of 5-7 mm (circular
motion) for about 5-10 seconds is suggested (Zand
et al., 2012).
Treatment of herpetic lesions
Pericoronitis is inflammation of the soft
tissues surrounding the crown of a partially erupted
tooth. Since it is primarily bacterial infection, use
of lasers is considered beneficial in inflamed tissue
removal compared to scalpel, namely due to
documented bactericidal effects of lasers (Sezer et
al., 2012).
Gingival abscess
Gingival abscess is caused by infection
from microbial plaque, trauma and foreign body
impaction. The laser instrument (Er:YAG laser,
diode) is placed at the height of the fluctant
mass and an incision is quickly made down to the
bone, causing immediate drainage. That is usually
resulted in resolution of the abscess and clinical
wound healing within approximately 2 to 3 weeks
(Prasad et al., 2011).
Herpetic lesions are characterized with
painful ulcerative erosions caused by herpes Biopsy
simplex virus type 1 (HSV-1). Treatment of herpetic
Lasers can be a useful treatment modality
lesions can be accomplished with LLLT regardless
Myanmar Dental Journal
for excisional biopsies of benign soft tissue
lesions in the oral cavity. After local anesthesia is
administered, the lesion is outlined with the diode,
Nd:YAG, Er:YAG, Er:YSGG, or CO2 laser for incision
of entire lesion, as well as some normal tissue
surrounding the lesion (Bornstein et al., 2005).
Since lasers will have peripheral thermal effect, it is
recommended to enlarge the surgical incision, at
least to around 0.5 mm in circumference, in order
to make a histological diagnosis free from doubt or
uncertainty. Biopsy sites are generally left to heal
with no sutures (secondary intent).
Aesthetic crown lengthening
The part of the tooth that is seen above the
gum is called the clinical crown. When not enough
of the clinical crown is showing, the gum must be
Detection of caries
moved up the root to expose more tooth. This is
A major diagnostic application of low called crown lengthening and is successfully done
power lasers is the detection of caries, using with any laser, regardless of wavelength (Shankar
fluorescence elicited from hydroxyapatite or from et al., 2013).
bacterial by-products. Laser fluorescence is an
effective method for detecting and quantifying Laser-activated tooth whitening
incipient occlusal and cervical carious lesions and
Laser dental bleaching, also known as
with further refinement could be used in the same
laser tooth whitening is a common procedure in
manner for proximal lesions.
general dentistry, in which a hydrogen peroxide
(bleaching) solution applied to the tooth surface
Class I-V restorations
is activated by laser energy, which speeds up of
Many wavelengths of laser are available the whitening process (Mohammadi et al., 2011).
today, but not all are to be used for cavity So far, lasers of different wavelengths had been
preparation and removal of carious tissues. The used for laser-driven whitening (Ar, diode, Er:YAG)
erbium lasers (Er:YAG and Er;Cr:YSGG) in tooth without temperature increase (Sari et al., 2013).
preparation are considered optimal minimal Additionally, common complaint following teeth
invasive approach, since they are highly absorbed whitening- teeth and gingival sensitivity was less
in water and, to a lesser extent, in hydroxyapatite. followed by lasers (Mohammadi et al., 2011; Sari et
They remove caries in enamel and dentine by al., 2013).
ablation, without effects of temperature rise
on the pulp and without the risk of micro- and Lasers in endodontics
macro-fractures that have been observed with
conventional rotating instruments. Some of the Desensitization/dentin hypersensitivity
benefits of laser use during cavity preparation
Dentinal hypersensitivity is one of the most
include: restricted or no need for anesthesia, common complaints in clinical dental practice.
selective and precise ablation of only decayed However, since it is subjective complaint, objective
tooth structure (leaving surrounding healthy evaluation of laser efficiency is a very difficult issue
structure), smear layer free cavity walls, cavity walls (Blatz, 2012). To date, clinical studies suggested
with a higher acid resistance resulting in a better safe and effective use of lasers in ablative (Nd:YAG,
protection against secondary decay, sterilization CO2) and non-ablative mode (diode, CO2, Nd:YAG,
and disinfection, and most of all, high patients He-Ne).
acceptance (children and adults), and enhanced
comfort (less pain, no heat or vibration). Use of Root canal disinfection
lasers is having disadvantages, too. For example,
The use of lasers in aiding root canal
erbium lasers can't be used to remove metallic and
disinfection is more promising than in root canal
porcelain restorations (Olivi & Genovese, 2011).
preparation. Nd:YAG, Er:YAG, CO2 and diode
Lasers in aesthetic dentistry
lasers are able to disinfect and decontaminate
the treated tissues by destroying aerobic and
Gingival melanin hyperpigmentation and gingival anaerobic bacteria. Energy can be used directly or
discoloration removal
can be combined with a photosensitive chemical
Melanin hyperpigmentation often occurs that, when bound to microorganisms, may be
in the gingiva as a result of an abnormal deposition activated by low-energy laser light to essentially
Lasers in operative dentistry
of melanin. Gingival discoloration (metal tattoo) is
iatrogenic discoloration of gingival tissue caused by
metal particles (silver sulfate, tin sulfate and pieces
of iron) that were embedded into the connective
tissue during metal abutment preparation (3).
Depigmentation by laser (Nd:YAG, Er:YAG, diode
and CO2 laser) is demonstrated in vivo and
clinically to be effective and safe therapy approach
with uneventful healing and no repigmentation
(Aoki et al., 2008; Murthy et al., 2012).
Vol. 21, No. 1, January 2014
kill the microorganism (Photodynamic TherapyPDT). Currently many in vitro and in vivo studies
suggested the antibacterial efficacy of high-power
laser (Nd:YAG, Ho:YAG, Er:YAG, Er;Cr:YSGG) in root
canals (Mohammadi, 2009; Cheng et al., 2012). Any
laser wavelength can disinfect a root canal system.
However, dentist must think of other endodontic
treatment steps, when selecting the most
appropriate laser wavelength to be employed.
Canal shaping/ Obturation of the root canal
Proper shaping of the root canal helps
remove organic tissue and facilitate canal
irrigation and obturation. In root canal treatment,
lasers may be used to remove the dental pulp
and organic debris, and to modify the dentinal
walls by inducing melting and resolidification
cycles resulting in the enlargement the walls of
the root canal system. Once the preparation is
completed, the root canal is obturated, and the
laser (Nd:YAG, Er;Cr:YSGG, Er:YAG) may be used
to soften and mold the obturating material to the
prepared root canal system. Laser irradiation from
apical to coronal surface in a continuous circling
fashion is considered optimal technique. With the
development of thinner, more flexible and durable
laser fibres, laser applications in endodontics have
increased (Mohammadi, 2009).
Peri-implantitis
Peri-implantitis
is
defined
as
a
localized lesion involving bone loss around
an osseointegrated implant that can induce a
breakdown of the implant-supporting bone. The
main goals of the treatment of peri-implantitis are
elimination of the peri-implant inflammation and
stabilization of the bony attachment. Recently, in
vitro and clinical studies supported use of some
lasers in reduction of bacteria from contaminated
gingiva and peri-implant pockets. For this purpose
Er:YAG, diode and CO2 lasers seem to be safe
and effective, while it has been demonstrated
that Nd:YAG laser use is contraindicated since it
can damage titanium surface of dental implants.
On the other side, Er:YAG lasers could not be
recommended in treatment of ailing implants,
since the laser beam can penetrate the material.
Further, concern regarding use of lasers is the heat
generated at the titanium implant surface and/or
peri-implant bone while diode and CO2 lasers are
used (Aoki et al., 2008; Schwarz et al., 2007).
Lasers in Fixed Prosthodontics
Gingival retraction
Accurate recording of finish line is a very
important parameter for taking the impression
and successful prognosis of indirectly fabricated
Apicoectomy
restorations. Soft tissue lasers can be used as a
Apicoectomy is a surgical root canal substitute to conventional retraction techniques,
procedure whereby the apex of a tooths root because they cause less bleeding and require less
is trimmed and removed. Recently, an Er:YAG working time (Krishna et al., 2013).
laser has attracted attention because of the
possibility of cutting hard tissues with extremely Recontouring of the gingival margin and bone for
small thermal effects. Laser clinical application crown lengthening
for apicoectomy has many advantages including
This is a periodontal procedure in which
absence of discomfort and vibration, less chance gingival and osseous tissue is removed in order to
for contamination of the surgical site, and reduced expose more clinical tooth structure (Lowe, 2006).
risk of trauma to adjacent tissue (Komori et al., An osseous crown-lengthening procedure is
1997).
required to enhance the appearance of a patients
Lasers in implantology
Lasers are widely used to cut gingival tissue
(even without anesthesia) and expose the implant
body for the placement of suprastructure during
the second phase of implant surgery. Use of lasers
will improve hemostasis, enhance wound healing
once abutments are placed and most importantly
it will cause less patient discomfort during the
operative and postoperative period (pain and
edema). Furthermore, in vivo and clinical studies
demonstrated benefits of Er:YAG laser by preparing
fixture holes in bone tissue for successful implant
osseointegration with less mechanical stress to the
bone during surgery (Aoki et al., 2008; Schwarz et
al., 2007).
smile, prevent violation of the biologic width,
and/or provide sufficient tooth structure for the
placement of dental restorations. The erbium lasers
allow the clinician to offer the patient a minimally
invasive alternative to conventional treatment,
which is known to have many adverse side effects.
Hemostasis, stable postoperative margins and
less collateral tissue damage are just some of the
benefits of use of lasers. Above all, patients can see
results of our work immediately, which is highly
appreciated (Lowe, 2006).
Lasers in Removable Prosthodontics
The success of removable complete
and partial dentures mainly depends on the
preoperative evaluation of the supporting
Myanmar Dental Journal
hard and soft tissue structures and their proper
preparation. Lasers can be applied in many preprosthetic surgeries. Stability, retention, function,
and aesthetics of removable prostheses may be
enhanced by proper laser manipulation of the soft
tissues and underlying osseous structure.
1.
Tuberosity reduction
2.
Torus reduction
3.
Soft tissue modification
4.
Treatment of epulis fissuratum
5.
Treatment of denture stomatitis
6.
Residual ridge modification
7.
Laser application in dental laboratory,
such as laser welding of cast metal denture
components, laser scanning of prepared cast for
CAD-CAM fabrication (Punia et al., 2012).
Discussion
10
produce results that are not possible with current
methods. Further, available literature does not
give any strong evidence-based superiority of
lasers upon conventional methods. Therefore,
more comparative clinical studies should be
performed to find the optimal power settings for
safe irradiation, without any harmful effects on the
surrounding tissue in order to clarify the benefits
of lasers upon conventional therapy. Only then, we
will be able to support lasers widespread use in
everyday dental practice.
References
Ando Y, Aoki A, Watanabe H, Ishikawa I. Bactericidal
effect of erbium YAG laser on periodontopathic
bacteria. Lasers Surg Med 1996;19:190-200.
Aoki A, Mizutani K, Takasaki AA, Sasaki KM, Nagai
To date, lasers are offering revolutionary S, Schwarz F, Yoshida I, Eguro T, Zeredo JL, Izumi
advantages in clinical applications for general Y. Current status of clinical laser applications in
dentists in the diagnosis and treatment of patients periodontal therapy. Gen Dent 2008;56:674-87.
in everyday practice. These advantages over Aoki A, Sasaki K, Watanabe H, Ishikawa I. Lasers
conventional instruments include: a completely in non-surgical periodontal therapy. Periodontol
bloodless surgical area/ hemostasis (very important 2000 2004;36:59-97.
in the treatment of highly vascularized lesions and
in the management of patients with infectious Bhardwaj A, Joshi M, Sharma D. Management of
diseases), sterility, the absence of sutures with recalcitrant oral pemphigus vulgaris with CO(2)
good healing by secondary intention, minimal laser - Report of two cases. J Indian Soc Periodontol
postoperative patient discomfort (pain and 2010;14:132-5.
swelling), less mental stress and anxiety (related
to noise, heat and vibration of high speed rotary Blatz MB. Laser therapy may be better than
instrumentation). Even though majority of studies topical desensitizing agents for treating dentin
show the advantages of lasers, some drawbacks hypersensitivity. J Evid Based Dent Pract
and unsolved problems are still present, such as the 2012;12:229-30.
cost of the laser device and the large dimensions
of the systems due to the complexity of the device. Bornstein MM, Winzap-Klin C, Cochran DL, Buser
Usually, dental office requires lasers of different D. The CO2 laser for excisional biopsies of oral
wavelengths to be employed for different dental lesions: a case series study. Int J Periodontics
procedures, since no single laser wavelength is Restorative Dent 2005;25:221-9.
considered capable to optimally treat all dental Brighton CT, Robert MH. Early histologic and
diseases. Also, if used improperly, laser can ultrastructural changes in microvessels of periosteal
pose some risks related to its use. In order to callus. Orthopaedics Trauma 1997;11:244-53.
successfully avoid risks, laser practitioners should
be highly familiar with the characteristics of the Cheng X, Guan S, Lu H, Zhao C, Chen X, Li N, Bai
laser wavelengths and its mode of employment, to Q, Tian Y, Yu Q. Evaluation of the bactericidal effect
receive the proper training to use lasers technology of Nd:YAG, Er:YAG, Er,Cr:YSGG laser radiation, and
safely and effectively, in order to obtain the optimal antimicrobial photodynamic therapy (aPDT) in
results. The oral cavity is very complex anatomical experimentally infected root canals. Lasers Surg
area; therefore any improper use of laser can cause Med 2012;44:824-31.
damage to the very important structures, which
Colvard M, Kuo P. Managing aphthous ulcers: laser
are surrounding targeted place.
treatment applied. J Am Dent Assoc 1991;122:51-3.
Conclusion
Ishikawa I, Aoki A, Takasaki AA, Mizutani K, Sasaki
Even though a considerable body of evidence KM, Izumi Y. Application of lasers in periodontics:
has proven lasers as safe and effective treatment true innovation or myth? Periodontol 2000
modalities, no single laser wavelength is capable 2009;50:90-126.
to completely replace conventional mechanical
instruments with improved clinical results, or to Komori T, Yokoyama K, Takato T, Matsumoto K.
Vol. 21, No. 1, January 2014
Clinical application of the erbium:YAG laser for Murthy MB, Kaur J, Das R. Treatment of gingival
hyperpigmentation with rotary abrasive, scalpel,
apicoectomy. J Endod 1997;23:748-50.
and laser techniques: A case series. J Indian Soc
Kreisler MB, Haj HA, Noroozi N, Willershausen B. Periodontol 2012;16:614-9.
Efficacy of low-level laser therapy in reducing
post-operative pain after endodontic surgery- a Ohshiro T, Calderhead RG. Development of low
randomized double blind clinical study. Int J Oral reactive-level laser therapy and its present status. J
Clin Laser Med Surg 1991;9:267-75.
Maxillofac Surg. 2004;33:38-41.
Krishna Ch V, Gupta N, Reddy KM, Sekhar NC, Aditya Olivi G, Genovese MD. Laser restorative dentistry in
V, Reddy GV. Laser gingival retraction: a quantitative children and adolescents. Eur Arch Paediatr Dent
2011;12:68-78.
assessment. J Clin Diagn Res 2013;7:1787-8.
Lowe RA. Clinical use of the Er,Cr:YSGG laser Pavlic V, Vujic-Aleksic V. Phototherapy approaches
for osseous crown lengthening: redefining the in treatment of oral lichen planus. Photodermatol
standard of care. Pract Proced Aesthet Dent Photoimmunol Photomed 2013
2006;18:2-9.
Pi-Snchez J, Espaa-Tost AJ, ArnabatMinicucci EM, Miot HA, Barraviera SR, Almeida- Domnguez J, Gay-Escoda C. Comparative study
Lopes L. Low-level laser therapy on the treatment of upper lip frenectomy with the CO2 laser versus
of oral and cutaneous pemphigus vulgaris: case the Er,Cr:YSGG laser. Med Oral Patol Oral Cir Bucal
2012;17:e228-32.
report. Lasers Med Sci 2012;27:1103-6.
Mohammadi Z. Lasers as aids for cleaning, shaping, Prasad S, Monaco EA Jr, Andreana S. Gingival
and obturation of the root canal system. Dent abscess removal using a soft-tissue laser. Dent
Today 2011;30:114-6.
Today 2009;28:81-6.
Mohammadi Z, Palazzi F, Giardino L. Laser Punia V, Lath V, Khandelwal M, Punia SK, Lakhyani
application in tooth bleaching: an update review. R. The Current Status of Laser Applications In
Prosthodontics . NJIRM. 2012; 3(3): 170-175.
Minerva Stomatol 2011;60:167-78.
Moritz A, Schoop U, Goharkhay K, Schauer P, Research, Science and Therapy Committee of the
Doertbudak O, Wernisch J, Sperr W. Treatment of American Academy of Periodontology. Lasers in
periodontal pockets with a diode laser. Lasers Surg periodontics. J Periodontol 2002;73:1231-9.
Med. 1998;22:302-11.
Sari T, Celik G, Usumez A. Temperature rise in pulp
Muralikrishna T, Kalakonda B, Gunupati S, Koppolu and gel during laser-activated bleaching: in vitro.
P. Laser-Assisted Periodontal Management of Lasers Med Sci 2013.
Drug-Induced Gingival Overgrowth under General
Anesthesia: A Viable Option. Case Rep Dent Shankar BS, T R, S NM, Reddy PS, Saritha G, Reddy
JM. Chronic inflammatory gingival overgrowths:
2013;2013:387453.
laser gingivectomy & gingivoplasty. J Int Oral
Health 2013;5:83-7.
11
Myanmar Dental Journal
Schindl A, Neumann R. Low-intensity laser therapy
is an effective treatment for recurrent herpes
simplex infection. Results from a randomized
double-blind placebo-controlled study. J Invest
Dermatol 1999;113:221-3.
Sezer U, Eltas A, Ustn K, Senyurt SZ, Erciyas K,
Aras MH. Effects of low-level laser therapy as an
adjunct to standard therapy in acute pericoronitis,
and its impact on oral health-related quality of life.
Photomed Laser Surg 2012;30:592-7.
Schwarz F, Olivier W, Herten M, Sager M, Chaker
A, Becker J. Influence of implant bed preparation
using an Er:YAG laser on the osseointegration of
titanium implants: a histomorphometrical study in
dogs. J Oral Rehabil 2007;34:273-81
12
Zand N, Fateh M, Ataie-Fashtami L, Djavid GE,
Fatemi SM, Shirkavand A. Promoting wound
healing in minor recurrent aphthous stomatitis
by non-thermal, non-ablative CO2 laser therapy: a
pilot study. Photomed Laser Surg 2012;30:719-23.
Potrebbero piacerti anche
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- Lymphatic SystemDocumento12 pagineLymphatic SystemMyat NyanNessuna valutazione finora
- Muscular SystemDocumento2 pagineMuscular SystemMyat NyanNessuna valutazione finora
- Blood and Its ComponentsDocumento8 pagineBlood and Its ComponentsMyat NyanNessuna valutazione finora
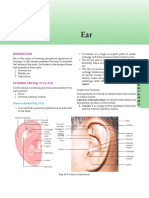
- Pinna or Auricle (Fig. 31.1) : Ssion)Documento12 paginePinna or Auricle (Fig. 31.1) : Ssion)Myat NyanNessuna valutazione finora
- Eye and OrbitDocumento30 pagineEye and OrbitMyat NyanNessuna valutazione finora
- TissuesDocumento8 pagineTissuesMyat NyanNessuna valutazione finora
- Competitive Potential of Skilled LaborDocumento24 pagineCompetitive Potential of Skilled LaborMyat NyanNessuna valutazione finora
- Code of Conduct For DentistryDocumento10 pagineCode of Conduct For DentistryMyat NyanNessuna valutazione finora
- Implantium SurgicalDocumento10 pagineImplantium SurgicalMyat NyanNessuna valutazione finora
- Implantium CatalogDocumento28 pagineImplantium CatalogMyat NyanNessuna valutazione finora
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Cooper - Formal Review of Karla Noles RaDocumento6 pagineCooper - Formal Review of Karla Noles RaMark CooperNessuna valutazione finora
- Ra 9293 Amending Ra 7836Documento2 pagineRa 9293 Amending Ra 7836vonoblesseNessuna valutazione finora
- Acd 1Documento3 pagineAcd 1Kath LeynesNessuna valutazione finora
- Company ProfileDocumento15 pagineCompany ProfileMuhammad Syaqil NgNessuna valutazione finora
- Soil MechDocumento21 pagineSoil MechAhsan AbbasNessuna valutazione finora
- Case Digest 2 S.C. MEGAWORLD CONSTRUCTIONDocumento3 pagineCase Digest 2 S.C. MEGAWORLD CONSTRUCTIONRomualdo CabanesasNessuna valutazione finora
- SwahiliDocumento7 pagineSwahiliMohammedNessuna valutazione finora
- Ap Government Imperial PresidencyDocumento2 pagineAp Government Imperial Presidencyapi-234443616Nessuna valutazione finora
- A Gandhari Version of The Rhinoceros Sutra - Salomon.thieuDocumento29 pagineA Gandhari Version of The Rhinoceros Sutra - Salomon.thieuTRAN NGOCNessuna valutazione finora
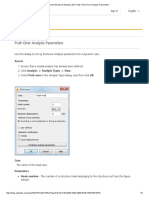
- Robot Structural Analysis 2017 Help - Push Over Analysis ParametersDocumento3 pagineRobot Structural Analysis 2017 Help - Push Over Analysis ParametersJustin MusopoleNessuna valutazione finora
- EXERCISE 1-Passive FormDocumento5 pagineEXERCISE 1-Passive FormMichele LangNessuna valutazione finora
- Global Perspectives Reflective PaperDocumento3 pagineGlobal Perspectives Reflective PaperMoaiz AttiqNessuna valutazione finora
- Dialogue-2: Problem of Our CountryDocumento6 pagineDialogue-2: Problem of Our CountrysiamNessuna valutazione finora
- Projects & Operations: IN: NE Power Systm ImprvmDocumento5 pagineProjects & Operations: IN: NE Power Systm ImprvmGaurang PatelNessuna valutazione finora
- PMAIZMTUSDMDocumento6 paginePMAIZMTUSDMLinh TranNessuna valutazione finora
- Detergent For Auto DishWashing Machine EDocumento5 pagineDetergent For Auto DishWashing Machine EkaltoumNessuna valutazione finora
- The Real World An Introduction To Sociology Test Bank SampleDocumento28 pagineThe Real World An Introduction To Sociology Test Bank SampleMohamed M YusufNessuna valutazione finora
- Apy1 Kinematics Review - 2015 - KeyDocumento13 pagineApy1 Kinematics Review - 2015 - KeyemadNessuna valutazione finora
- Agne Vs Director of LandsDocumento7 pagineAgne Vs Director of LandsLee SomarNessuna valutazione finora
- III Job Order CostingDocumento66 pagineIII Job Order CostingJoshuaGuerrero0% (1)
- A Feasibility/Project Study OnDocumento14 pagineA Feasibility/Project Study OnWilson Domingo LazarteNessuna valutazione finora
- La Lit Review-Jennifer Draper-2-2Documento9 pagineLa Lit Review-Jennifer Draper-2-2api-653567856Nessuna valutazione finora
- Globalization and Challenges To Secondary EducationDocumento46 pagineGlobalization and Challenges To Secondary Educationsollu786_889163149Nessuna valutazione finora
- Airplus CDF3 Technical SpecsDocumento38 pagineAirplus CDF3 Technical Specssadik FreelancerNessuna valutazione finora
- AutoPIPE Tutorial PDFDocumento156 pagineAutoPIPE Tutorial PDFdhaktodesatyajitNessuna valutazione finora
- Theological Differences Between Christianity and IslamDocumento18 pagineTheological Differences Between Christianity and IslamMencari KhadijahNessuna valutazione finora
- Students List - All SectionsDocumento8 pagineStudents List - All SectionsChristian RiveraNessuna valutazione finora
- STD 12 Accountancy1Documento264 pagineSTD 12 Accountancy1Chetan KhonaNessuna valutazione finora
- South WestDocumento1 paginaSouth WestDarren RadonsNessuna valutazione finora
- Jobsheet PMDocumento49 pagineJobsheet PMwindhy fitrianaNessuna valutazione finora