Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Management of Flabby Ridges Using Liquid Supported Denture PDF
Caricato da
mujtabaDescrizione originale:
Titolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Management of Flabby Ridges Using Liquid Supported Denture PDF
Caricato da
mujtabaCopyright:
Formati disponibili
J Adv Prosthodont 2011;3:43-6
CASE REPORT
DOI:10.4047/jap.2011.3.1.43
Management of flabby ridges using
liquid supported denture: a case report
Nandita Nitin Keni*, BDS, Meena Ajay Aras, MDS, Vidya Chitre, MDS
Department of Prosthodontics, Goa Dental College & Hospital, Bambolim-Goa-India, Panaji, India
Flabby ridges commonly occur in edentulous patients. Inadequate retention and stability of a complete denture are the often encountered problems in these patients. A liquid supported denture due to its flexible tissue surface allows better distribution of stress and hence provides an
alternate treatment modality in such cases. This case report presents the use of a liquid supported denture in a patient with completely edentulous maxillary arch with flabby tissue in anterior region opposing a partially edentulous mandibular arch. [J Adv Prosthodont 2011;3:43-6]
KEY WORDS. Liquid supported denture, Flabby ridges, Flexible tissue surface
INTRODUCTION
Fibrousorflabbyridge is a superficial area of mobile
soft tissue affecting the maxillary or mandibular alveolar
ridges. It can be developed when hyperplastic soft tissue
replaces the alveolar bone and is a common finding, particularly in long term denture wearers.1 Such ridges are reported
to be caused due to trauma from denture bases.2 In the edentulous patient, it is found more commonly in the anterior
region.3-5
Histologically, flabby ridges are composed of hyperplastic
mucosal tissue and loosely arranged fibrous connective tissue
and dense collagenised connective tissue. In the soft tissue, a
great amount of metaplastic cartilage and/or bone are observable.6
Prosthetic rehabilitation in these patients can be challenging.
Major problems encountered in these patients are loss of
stability and inadequate retention of the dentures. These
problems occur because of the easily distorted flabby tissue during impression taking. Treatment options for these patient
s
include surgery, implant retained prosthesis or conventional
prosthodontics without surgical intervention.1 Treatment
modality has to be chosen depending on patient
s state of health
and need, extent of flabby tissue, financial capacity and skill
of the dentist. In most situations, surgical intervention or
use of implants is not possible and conservative manage-
Corresponding author: Nandita Nitin Keni
GDCH, Department of Prosthodontics, Goa Dental College and Hospital,
Bambolim-goa-India, India
Tel. + 09823088402: e-mail, nandita.keni@gmail.com
Received January 20, 2011 / Last Revison February 21, 2011 / Accepted March 7, 2011
ment is the treatment of choice.
In 1961, Chase7 introduced the use of elastic impression material to relieve traumatised tissue. But this can be only a temporary provision. Moreover, it might easily derive candidal
growth. In a flabby ridge condition, an ideal denture should be
able to withstand masticatory forces and have flexible tissue
surface to reduce stress concentration and trauma on the
underlying tissues.8 A liquid supported denture can hence
be a solution for this problem.
This case report describes the use of a liquid supported
denture in a patient with completely edentulous maxillary arch
with flabby tissue in anterior region opposing a partially
edentulous mandibular arch.
CASE REPORT
A 52 year old female patient reported to Goa dental college
and hospital (GDCH) for replacement of missing teeth. The
patient had a history of wearing a maxillary complete denture
for 5 years. Her chief complaint was the poor fit of the denture
and it felt loose while eating. She was also using denture adhesive. Missing mandibular teeth were not replaced by any
prosthetic treatment. By intraoral examination, a completely
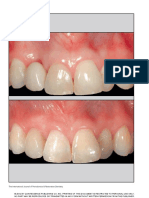
edentulous maxillary arch with flabby tissue existing in the anterior region (Fig. 1) and a partially edentulous mandibular
arch (Kennedy
s Class II) were observed (Fig. 2).
2011 The Korean Academy of Prosthodontics
This is an Open Access article distributed under the terms of the Creative Commons
Attribution Non-Commercial License (http://creativecommons.org/licenses/bync/3.0) which permits unrestricted non-commercial use, distribution, and reproduction
in any medium, provided the original work is properly cited.
43
Management of flabby ridges using liquid supported denture: a case report
Fig. 1. Intraoral view of maxillary arch.
Fig. 3. 1 mm thick sheet placed on the invested
master cast prior to packing.
Keeping the various challenges associated with the case, clinical steps and treatment plan was modified to suit the patient
s
need. It was decided to give a maxillary complete denture (liquid supported) opposing a mandibular cast partial denture.
Primary impressions were made with alginate (Zelgan,
Dentsply/caulk). On the maxillary cast, a special tray was made
with two posterior handles. Border molding was performed by
using low fusing impression compound (Aslate, India) and medium body addition silicone wash impression (Aquasil,
Dentsply/caulk) was made. The flabby tissue was marked in
the mouth and transferred on the tray. This area on the tray was
cut to form a window to expose the flabby tissue. It was
recorded in rest position by injecting light body addition silicone material (Aquasil, Dentsply/caulk).
For the mandibular impressions, a cast framework replacing
the missing teeth was tried and adjusted. An altered cast
impression technique was used to get the master cast. Jaw relations were recorded. Face bow transfer was made and casts were
mounted. Teeth were set and the try in procedure of the
44
Keni NN et al.
Fig. 2. Intraoral view of mandibular arch.
Fig. 4. 1 mm thick sheet being removed from the processed
denture at recall appointment.
waxed denture was done.
The upper denture design was modified to make a liquid supported denture. Lower cast partial denture was acrylised
using conventional procedure.
Steps in fabricating a liquid supported denture:1) Vaccum heat pressed polyethylene sheet of 1 mm thickness
was adapted on the master cast. The sheet was made 2 mm short
of the sulcus and was not extended in the PPS area. This sheet
was incorporated in the denture at the time of packing (Fig. 3).
Upper complete Denture (with 1 mm thick sheet) and lower cast partial denture were then delivered after making
occlusal adjustments. The patient was recalled after 2 weeks
to convert the denture into a liquid supported one. This was done
to check the comfort level of the patient to the polyethylene sheet.
2) At recall appointment, the 1 mm thick sheet which was used
as a spacer was removed from the denture (Fig. 4). Due to
removal of the sheet crevices were formed all along the denture borders. These crevices were helpful in final placement
of 0.5 mm thick sheet. An addition silicone putty impression
J Adv Prosthodont 2011;3:43-6
Management of flabby ridges using liquid supported denture: a case report
Keni NN et al.
Fig. 7. Intra oral view with upper and lower dentures.
Fig. 5. Stone cast poured from the putty impression to mark the
exact junction of polyethylene sheet.
Fig. 6. Upper liquid supported complete denture and lower cast partial
denture.
Fig. 8. Schematic representation of the cross sectional view of the
upper denture with polyethylene sheet and glycerin.
was made of the tissue surface of the denture and cast was made
of it (Fig. 5). This was done to record the exact junction of the
sheet to the denture. On this cast a 0.5 mm thick polyethylene
sheet was vacuum pressed which was used in place of 1mm thick
sheet creating a 0.5 mm space.
3) The polyethylene sheet was cut using the putty index as
guide. The borders of the 0.5 mm thick sheet were placed in
the crevice formed due to removal of 1mm thick sheet.
Cynoacrylate adhesive and autopolymerising acrylic resin
were used to seal the borders and prevent escape of liquid.
4) The space created due to the replacement of a 1 mm thick
sheet with a 0.5 mm thick sheet was filled with glycerine. This
was done by making two holes in the buccal flange area of the
denture and injecting glycerine through these holes and
checking the vertical dimensions simultaneously. The holes were
sealed using self cure acrylic resin.
Finally the upper liquid supported denture was delivered (Fig.
6-8). Denture care instructions were given to the patient.
Patient was told to clean the tissue surface using soft cloth. Recall
appointments were scheduled at 1 day, 1 week, 1 month and
3 months. At 1 week appointment, patient complained of
floating feeling. But, at 3 months recall appointment, patient
was comfortably using the denture. The denture was well maintained.
J Adv Prosthodont 2011;3:43-6
DISCUSSION
Major problems associated with this case were the presence
of flabby tissue in maxillary arch (anterior portion) and the presence of natural dentitions in the opposing arch causes
unfavourable distribution of forces that can cause unfavourable
tissue changes. These problems were solved by modifying the
impression procedures and by fabricating upper liquid supported
denture.
Liquid supported denture is based on the theory that when
the force applied on the denture is absent, the base assumes its
preshaped form that is the one during processing. But under
masticatory load, the base adapts to the modified form of mucosa
due to hydrodynamics of the liquid improving support, retention and stability.9 There will also be optimal stress distribu45
Management of flabby ridges using liquid supported denture: a case report
tion of masticatory forces over a larger area which reduces tissue overloading.9 Prevention of soreness and increased comfort level are other advantages of the liquid supported denture.9,10
In this case, polyethylene thermoplastic clear sheet (Biostar
vaccum forming machine, Scheu-dental, Germany) was used
because of its softness, flexibility and biocompatibility.
Glycerin was used because it is clear, viscous, and biocompatible
and also has been used as a vehicle in liquid medications.
CONCLUSION
Fibrous ridges pose a prosthodontic challenge for the
achievement of stable and retentive dental prostheses. Surgical
removal of the fibrous tissue and implant retained prostheses
may not be possible to be used in all cases. Considering
conventional prosthodontics, the use of liquid supported denture can further improve the patient
s acceptance due to more
uniform distribution of forces and due to the improved comfort level.
46
Keni NN et al.
REFERENCES
1. Crawford RW, Walmsley AD. A review of prosthodontic management of fibrous ridges. Br Dent J 2005;199:715-9.
2. Kelly E. Changes caused by a mandibular removable partial denture opposing a maxillary complete denture. J Prosthet Dent
2003;90:213-9.
3. Carlsson GE. Clinical morbidity and sequelae of treatment
with complete dentures. J Prosthet Dent 1998;79:17-23.
4. Zarb GA, Bolender CL, Carlsson GE. Boucher's prosthodontic
treatment for edentulous patients. 11th ed. London; ST. Louis;
Mosby; 1997. p. 36.
5. Basker RM, Davenport JC. Prosthetic treatment of the edentulous patient. 4th ed. Blackwell; Oxford; 2002. p. 286-9.
m H, Kahnberg KE. Metaplastic formation
6. Magnusson BC, Engstro
of bone and chondroid in flabby ridges. Br J Oral Maxillofac Surg
1986;24:300-5.
7. Chase WW. Tissue conditioning utilizing dynamic adaptive stress.
J Prosthet Dent 1961;11:804-15.
8. Kakade D, Athavale S, Shingote S, Dammani B. Liquid-supported
denture: a gentle option. J Indian Prosthodont Soc 2007;7:359.
9. Davidson CL, Boere G. Liquid-supported dentures. Part I:
Theoretical and technical considerations. J Prosthet Dent
1990;63:303-6.
10. Boere G, de Koomen H, Davidson CL. Liquid-supported dentures. Part II: Clinical study, a preliminary report. J Prosthet Dent
1990;63:434-6.
J Adv Prosthodont 2011;3:43-6
Potrebbero piacerti anche
- Journal Writing PromptsDocumento6 pagineJournal Writing Promptscombination_soupNessuna valutazione finora
- A Practical Guide To Feline DermatologyDocumento292 pagineA Practical Guide To Feline DermatologyclararlvferreiraNessuna valutazione finora
- Prosthodontic Management of Flabby Ridge From Modified Impression To DentureDocumento14 pagineProsthodontic Management of Flabby Ridge From Modified Impression To DenturePhoebe David100% (1)
- The Rule of the 5 Triangles for Immediate ImplantsDocumento12 pagineThe Rule of the 5 Triangles for Immediate ImplantsVikas Aggarwal100% (3)
- Maintenance of Gingival Form Following Implant PlacementDocumento4 pagineMaintenance of Gingival Form Following Implant PlacementRomina BitaNessuna valutazione finora
- Endocrine ChartDocumento7 pagineEndocrine Chartwjg2882Nessuna valutazione finora
- Divine Right - The Leviathans of MinariaDocumento3 pagineDivine Right - The Leviathans of MinariaScribdSucks100% (1)
- Tongue, Speech & Its Prosthodontic ConsiderationDocumento74 pagineTongue, Speech & Its Prosthodontic ConsiderationmujtabaNessuna valutazione finora
- Management Flabby RidgeDocumento4 pagineManagement Flabby RidgeNidya Patricia Sembiring100% (1)
- The Sign of The BeaverDocumento13 pagineThe Sign of The Beaverjuan marcos100% (1)
- Case Report - Complete Denture - 2Documento4 pagineCase Report - Complete Denture - 2Astri Ggamjong Xiao LuNessuna valutazione finora
- Journal Club ProsthodonticsDocumento33 pagineJournal Club ProsthodonticsmujtabaNessuna valutazione finora
- Neutral Zone Technique in Complete DentureDocumento4 pagineNeutral Zone Technique in Complete DenturemujtabaNessuna valutazione finora
- Treatment Planning Single Maxillary Anterior Implants for DentistsDa EverandTreatment Planning Single Maxillary Anterior Implants for DentistsNessuna valutazione finora
- Injertos Aumento RebordeDocumento13 pagineInjertos Aumento Rebordejose miguel perez rodriguez100% (1)
- Mouth Preparation For Removable Dental ProsthesisDocumento64 pagineMouth Preparation For Removable Dental Prosthesismujtaba100% (1)
- of Mouth PreparationDocumento106 pagineof Mouth PreparationDrSweta Gandhi100% (2)
- Preprosthetic SurgeryDocumento4 paginePreprosthetic SurgeryVero AngelNessuna valutazione finora
- The Revolution in Digital Impressioning - ID - DentalaegisDocumento3 pagineThe Revolution in Digital Impressioning - ID - DentalaegismujtabaNessuna valutazione finora
- ECA1 Tests Language Test 7C New2018Documento6 pagineECA1 Tests Language Test 7C New2018Kamila RoguzińskaNessuna valutazione finora
- Sequential Piezocision A Novel Approach To Acelerated Orthodontic TreatmentDocumento11 pagineSequential Piezocision A Novel Approach To Acelerated Orthodontic TreatmentMargareth BritoNessuna valutazione finora
- Passive Voice, Report Text (Kelas 9 SMP)Documento2 paginePassive Voice, Report Text (Kelas 9 SMP)Windarto WindartoNessuna valutazione finora
- Jap 3 43Documento4 pagineJap 3 43AmalorNessuna valutazione finora
- Prosthodontic Rehabilitation of A Patient With Maxillary Flabby Ridge - A Case ReportDocumento4 pagineProsthodontic Rehabilitation of A Patient With Maxillary Flabby Ridge - A Case ReportdedeNessuna valutazione finora
- Padmaja S Dr.Documento4 paginePadmaja S Dr.Dentist HereNessuna valutazione finora
- Supplement The Base To Complement The Crown: Localized Ridge Augmentation Using Connective Tissue GraftDocumento5 pagineSupplement The Base To Complement The Crown: Localized Ridge Augmentation Using Connective Tissue GraftBianca DimofteNessuna valutazione finora
- Fabrication of Conventional Complete Dentures For A Left Segmental MandibulectomyDocumento4 pagineFabrication of Conventional Complete Dentures For A Left Segmental MandibulectomyIndrani DasNessuna valutazione finora
- CR2 CocktailManagement KhusbooMishraDocumento6 pagineCR2 CocktailManagement KhusbooMishradella sainNessuna valutazione finora
- DR RituDocumento4 pagineDR RitubhupendraNessuna valutazione finora
- Loss of Anterior Interdental Tissue SolutionsDocumento5 pagineLoss of Anterior Interdental Tissue Solutionsjinny1_0Nessuna valutazione finora
- Crid2014 658790Documento6 pagineCrid2014 658790paula catanaNessuna valutazione finora
- Point of CareDocumento6 paginePoint of Carepbo4Nessuna valutazione finora
- Article 009Documento9 pagineArticle 009MedstudNessuna valutazione finora
- Post-Prosthetic Surgery: Using Complete Denture Prosthesis For Propriotous Outcome During VestibuloplastyDocumento3 paginePost-Prosthetic Surgery: Using Complete Denture Prosthesis For Propriotous Outcome During VestibuloplastyInternational Journal of Innovative Science and Research TechnologyNessuna valutazione finora
- Unconventional Complete Dentures: Innovative Approach in ProsthodonticsDocumento10 pagineUnconventional Complete Dentures: Innovative Approach in ProsthodonticsAastha DuaNessuna valutazione finora
- Gingival Mask: A Case Report On Enhancing Smiles: ASE EportDocumento3 pagineGingival Mask: A Case Report On Enhancing Smiles: ASE EportLouis HutahaeanNessuna valutazione finora
- Gingival Mask A Case Report On Enhancing SmilesDocumento3 pagineGingival Mask A Case Report On Enhancing SmilesLouis HutahaeanNessuna valutazione finora
- Windowimpressiontechnique 2018Documento5 pagineWindowimpressiontechnique 2018Winda KhosasiNessuna valutazione finora
- COMPLETE DENTURES PREPARATION OF THE MOUTHDocumento12 pagineCOMPLETE DENTURES PREPARATION OF THE MOUTHShreyans DamadeNessuna valutazione finora
- Ecde 10 00327Documento8 pagineEcde 10 00327Erisa BllakajNessuna valutazione finora
- Liquid-Supported Denture-A Boon To Flabby RidgesDocumento4 pagineLiquid-Supported Denture-A Boon To Flabby RidgesTarak ChavadaNessuna valutazione finora
- Soft Tissues Remodeling Technique As A N PDFDocumento12 pagineSoft Tissues Remodeling Technique As A N PDFjorgeNessuna valutazione finora
- A Prosthodontic Rehabilitation of A Partial Maxillectomy Patient With Hollow Bulb ObturatorDocumento4 pagineA Prosthodontic Rehabilitation of A Partial Maxillectomy Patient With Hollow Bulb ObturatorDentist HereNessuna valutazione finora
- RETHINKING FERRULEDocumento7 pagineRETHINKING FERRULEpoojaNessuna valutazione finora
- Prosthodontic Management of Compromised Ridges and SituationsDocumento8 pagineProsthodontic Management of Compromised Ridges and SituationsTiwi SitompulNessuna valutazione finora
- 3 (1) 11 14Documento4 pagine3 (1) 11 14marcelodentNessuna valutazione finora
- EDI Prandtner 1 PDFDocumento11 pagineEDI Prandtner 1 PDFadriiianaiiioanaNessuna valutazione finora
- Management of Completely Edentulous MaxillaryDocumento4 pagineManagement of Completely Edentulous MaxillaryDeasireeNessuna valutazione finora
- Caculo Et Al-2013-Journal of Prosthodontics PDFDocumento6 pagineCaculo Et Al-2013-Journal of Prosthodontics PDFArchitNessuna valutazione finora
- New Direct Resilient Relining Material of Denture Base: International Medical Journal (1994) April 2018Documento4 pagineNew Direct Resilient Relining Material of Denture Base: International Medical Journal (1994) April 2018lulukzNessuna valutazione finora
- Pouch Roll Technique For Implant Soft Tissue Augmentation - A Variation of The Modified Roll TechniqueDocumento6 paginePouch Roll Technique For Implant Soft Tissue Augmentation - A Variation of The Modified Roll TechniqueAnthony LiNessuna valutazione finora
- Soft-Tissue Undercuts in Denture PlacementDocumento4 pagineSoft-Tissue Undercuts in Denture Placementdrgayen6042Nessuna valutazione finora
- C01251115Documento5 pagineC01251115agnes herlinaNessuna valutazione finora
- Modified Tray With Mesh Design For The ManagementDocumento4 pagineModified Tray With Mesh Design For The ManagementANessuna valutazione finora
- An 2/2 Implant Overdenture: Case ReportDocumento3 pagineAn 2/2 Implant Overdenture: Case ReportasclepiuspdfsNessuna valutazione finora
- Jpis 42 105Documento5 pagineJpis 42 105Jean Pierre Alcántara VigoNessuna valutazione finora
- Management of The Mucolabial Fold When Developing Impressions For Complete DenturesDocumento6 pagineManagement of The Mucolabial Fold When Developing Impressions For Complete Denturesjinny1_0Nessuna valutazione finora
- Oral Sub-Mucous FibrosisDocumento2 pagineOral Sub-Mucous FibrosisShreyans DamadeNessuna valutazione finora
- CCR3 4 831 PDFDocumento7 pagineCCR3 4 831 PDFArmareality ArmarealityNessuna valutazione finora
- JCDR 8 ZD04Documento3 pagineJCDR 8 ZD04rajaniNessuna valutazione finora
- Print 6Documento5 paginePrint 6hafidh akbarNessuna valutazione finora
- Immediate Denture Advantages and TechniquesDocumento11 pagineImmediate Denture Advantages and TechniquesClaudia AngNessuna valutazione finora
- Adj 12563Documento5 pagineAdj 12563anushiNessuna valutazione finora
- (India) Clinical Management of Highly Resorbed Mandibular Ridge Without Fibrous TissueDocumento5 pagine(India) Clinical Management of Highly Resorbed Mandibular Ridge Without Fibrous TissueTerran ComanderNessuna valutazione finora
- Fabrication and Relining of Dentures With PermanenDocumento5 pagineFabrication and Relining of Dentures With Permanencitra yuliyantiNessuna valutazione finora
- 1457792866immediate DenturesDocumento5 pagine1457792866immediate DenturesegarochmawatiNessuna valutazione finora
- Prosthetic Rehabilitation of Mandibular Defects With Fixed-Removable Partial Denture Prosthesis Using Precision Attachment - A Twin Case ReportDocumento17 pagineProsthetic Rehabilitation of Mandibular Defects With Fixed-Removable Partial Denture Prosthesis Using Precision Attachment - A Twin Case ReportIvy MedNessuna valutazione finora
- Case Report: The Prosthetic Management of A Case of Epulis Fissuratum by A Novel TechniqueDocumento6 pagineCase Report: The Prosthetic Management of A Case of Epulis Fissuratum by A Novel TechniqueMichelle VelezNessuna valutazione finora
- Aumento de Reborde Con Tejido BlandoDocumento8 pagineAumento de Reborde Con Tejido BlandoSilvia SolisNessuna valutazione finora
- A Simplified Method For The Fabrication of Obturator:a Case ReportDocumento4 pagineA Simplified Method For The Fabrication of Obturator:a Case ReportinventionjournalsNessuna valutazione finora
- Managing Resorbed Mandibular Ridges with Functional ImpressionsDocumento5 pagineManaging Resorbed Mandibular Ridges with Functional ImpressionsSorabh JainNessuna valutazione finora
- Peri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentDa EverandPeri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentNessuna valutazione finora
- Lingualized Occlusion in RDPDocumento37 pagineLingualized Occlusion in RDPmujtaba100% (1)
- Neutral Zone Technique-JCDocumento43 pagineNeutral Zone Technique-JCmujtaba100% (1)
- Rehabilitation of Glossectomy Cases With Tongue Prosthesis: A Literature ReviewDocumento4 pagineRehabilitation of Glossectomy Cases With Tongue Prosthesis: A Literature ReviewmujtabaNessuna valutazione finora
- The Efficacy of Palatal Augmentation Prostheses For Speech and Swallowing in Patients Undergoing Glossectomy: A Review of The LiteratureDocumento8 pagineThe Efficacy of Palatal Augmentation Prostheses For Speech and Swallowing in Patients Undergoing Glossectomy: A Review of The LiteraturemujtabaNessuna valutazione finora
- Sdarticle PDFDocumento9 pagineSdarticle PDFManjeev GuragainNessuna valutazione finora
- Open Access Scientific ReportsDocumento3 pagineOpen Access Scientific ReportsmujtabaNessuna valutazione finora
- Minor Connectors Rests and Rest Seats in Removable Dental ProsthesisDocumento68 pagineMinor Connectors Rests and Rest Seats in Removable Dental ProsthesismujtabaNessuna valutazione finora
- Okuno 2014Documento4 pagineOkuno 2014mujtabaNessuna valutazione finora
- Meyer 1990Documento3 pagineMeyer 1990mujtabaNessuna valutazione finora
- The Videofluorographic Swallowing StudyDocumento17 pagineThe Videofluorographic Swallowing StudySandra Moiteiro LopesNessuna valutazione finora
- An Alternative Impression Technique For Mobile TeethDocumento25 pagineAn Alternative Impression Technique For Mobile TeethmujtabaNessuna valutazione finora
- Dentoalveolar Distraction Osteogenesis For Rapid Orthodontic Canine RetractionDocumento6 pagineDentoalveolar Distraction Osteogenesis For Rapid Orthodontic Canine RetractionmujtabaNessuna valutazione finora
- Classification of Partially Edentulous ArchesDocumento5 pagineClassification of Partially Edentulous ArchesmujtabaNessuna valutazione finora
- Major Connector in RDPDocumento73 pagineMajor Connector in RDPmujtabaNessuna valutazione finora
- Canine Retraction: A Bracket Systems Comparison of Two PreadjustedDocumento6 pagineCanine Retraction: A Bracket Systems Comparison of Two PreadjustedmujtabaNessuna valutazione finora
- Orbital Prosthesis A Novel Reconstructive Approach 2247 2452.1000653Documento3 pagineOrbital Prosthesis A Novel Reconstructive Approach 2247 2452.1000653mujtabaNessuna valutazione finora
- 3D Digital Scanners - A High-Tech Approach To More Accurate Dental Impressions - ID - DentalaegisDocumento12 pagine3D Digital Scanners - A High-Tech Approach To More Accurate Dental Impressions - ID - DentalaegismujtabaNessuna valutazione finora
- Guide to Managing Flabby Ridges and Hypertrophic TissuesDocumento145 pagineGuide to Managing Flabby Ridges and Hypertrophic TissuesJudy Abbott100% (1)
- A Spectacle With Magnet Retained Eye Prosthesis For Rehabilitation of Orbital DefectDocumento4 pagineA Spectacle With Magnet Retained Eye Prosthesis For Rehabilitation of Orbital DefectIOSRjournalNessuna valutazione finora
- A Hollow Complete Lower DentureDocumento3 pagineA Hollow Complete Lower DenturemujtabaNessuna valutazione finora
- Ocular Prosthesis: Custom Devices for Eye DisfigurementDocumento11 pagineOcular Prosthesis: Custom Devices for Eye DisfigurementManjeevNessuna valutazione finora
- Balanced Semi StaticDocumento14 pagineBalanced Semi StaticRadhika SrivastavaNessuna valutazione finora
- Complete Denture FabricationDocumento14 pagineComplete Denture FabricationmujtabaNessuna valutazione finora
- Shark Teeth IdentificationDocumento3 pagineShark Teeth Identificationkira.arifa.designsNessuna valutazione finora
- Way To Go 8º Pag 88 - 109Documento22 pagineWay To Go 8º Pag 88 - 109Jenny TorresNessuna valutazione finora
- Surgery of Penis & UretraDocumento81 pagineSurgery of Penis & UretraRiris SutrisnoNessuna valutazione finora
- Infertility ACOGDocumento8 pagineInfertility ACOGRifdaNessuna valutazione finora
- Find The Temperature Using CricketsDocumento2 pagineFind The Temperature Using CricketsMoreMoseySpeedNessuna valutazione finora
- Fun Animal Facts for KidsDocumento2 pagineFun Animal Facts for KidsAivy YlananNessuna valutazione finora
- Module Possessive Adj. Lesson 3Documento29 pagineModule Possessive Adj. Lesson 3Lance TuvillaNessuna valutazione finora
- Ecological Terms - 1 PDFDocumento2 pagineEcological Terms - 1 PDFraviNessuna valutazione finora
- The Bishop ScoreDocumento3 pagineThe Bishop ScoreJheanAlphonsineT.MeansNessuna valutazione finora
- EUS教學 (19) 急診超音波在睪丸急症之應用Documento58 pagineEUS教學 (19) 急診超音波在睪丸急症之應用juice119100% (1)
- Shark Finning Report WildaidDocumento16 pagineShark Finning Report WildaidGlobal Wildlife Warriors100% (1)
- Crochet Plush Bunny Neon Amigurumi Free PatternDocumento4 pagineCrochet Plush Bunny Neon Amigurumi Free PatternflechedestructriceNessuna valutazione finora
- Vĩnh Phúc exam prep for grade 11 entrance examDocumento4 pagineVĩnh Phúc exam prep for grade 11 entrance examnguyenmai02185Nessuna valutazione finora
- Economically Feasible Fish Feed For GIFT Tilapia (Oreochromis LankaDocumento31 pagineEconomically Feasible Fish Feed For GIFT Tilapia (Oreochromis Lankasantosh kumarNessuna valutazione finora
- Đề Thi DAKLAK DienanhDocumento14 pagineĐề Thi DAKLAK DienanhWin Trần Điển AnhNessuna valutazione finora
- 0610 s18 QP 23 PDFDocumento16 pagine0610 s18 QP 23 PDFTesterNessuna valutazione finora
- Meat Inspection OrdinanceDocumento7 pagineMeat Inspection OrdinanceAlexander ObongNessuna valutazione finora
- Soal Vocabulary Part 2Documento3 pagineSoal Vocabulary Part 2Sastrawan PelawiNessuna valutazione finora
- How Bravery Helps Us GrowDocumento6 pagineHow Bravery Helps Us GrowNajeehah RohaizadNessuna valutazione finora
- Упражнения На Отработку Притяжательных МестоименийDocumento3 pagineУпражнения На Отработку Притяжательных МестоименийKristinaNessuna valutazione finora
- The Clever BarberDocumento2 pagineThe Clever BarberKHAIRUL NIZAM BIN ZAINALUDIN MoeNessuna valutazione finora
- Reading and Writing Short Vowel Sounds in CVC PatternDocumento4 pagineReading and Writing Short Vowel Sounds in CVC PatterndncblzmNessuna valutazione finora
- PET Masterclass StudentBook PDFDocumento137 paginePET Masterclass StudentBook PDFMiguel Angel Olvera Garcia100% (2)