Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
38 Acne
Caricato da
DianAndikaTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
38 Acne
Caricato da
DianAndikaCopyright:
Formati disponibili
Acne: Etiopathogenesis and its management
ISSN: 2394-0026 (P)
ISSN: 2394-0034 (O)
Review Article
Acne: Etiopathogenesis and its management
Usha Kataria1*, Dinesh Chhillar2
1
Department of Dermatology, BPS Government Medical College forr Women, Khanpur Kalan,
Sonepat, Haryana, India
2
Department of Forensic Medicine,
Medicine Pt. BDS PGIMS, Rohtak, India
*
Corresponding author email: ushachillar@gmail.com
How to cite this article: Usha Kataria,
Kataria Dinesh Chhillar. Acne: Etiopathogenesis and its management.
management
IAIM, 2015; 2(5): 225-231.
Available online at www.iaimjournal.com
Received on: 22-03-2015
Accepted on: 15-04-2015
Abstract
Acne vulgaris is one of the commonest skin disorders, which dermatologists have to treat, mainly
affect adolescents, though it may present at any age. Acne is chronic inflammatory disease of
pilosebaceous units. Clinically it can present as seborrhea, comedones,
comedones, erythematous papules,
pustules and nodules. In recent years, due to better understanding of the etiopathogenesis of acne,
new therapeutic modalities are designed. The purpose of this article is to review the
etiopathogenesis and treatment options available
available with us in the present scenario.
Key words
Acne vulgaris, Pilosebaceous units,
nits, Seborrhea, Comedones.
Comedones
Introduction
Acne vulgaris is a most common skin disorder of
the pilosebaceous unit [1]. It is generally
characterized
by
seborrhea,
comedone
formation, inflammatory lesions and increased
colonization
by
propionibacterium
spp.
staphylococcus spp. and yeast of malassezia spp.
within the follicular canal [2]. It is common
enough to be called
d a physiological process.
Ninety percent of female and male individuals
experience some degree of acne between
puberty and thirty years of age. It is better
regarded as a disease due to its inflammatory
component
and
physical,
psycho
psycho-social
morbidity and is therefore, in need of systematic
and rational treatment. The disorder can cause
significant emotional distress and physical
scarring if untreated. Underestimating its
importance is of serious consequences [3].
Definition
A precise definition of acne vulgaris is difficult to
frame it can be defined as a chronic, self
limiting, inflammatory disease of pilosebaceous
unit, manifesting generally in adolescence with
pleomorphic lesions like comedones, papules,
nodules and cysts. Extensive scarring can occur
[4].
International Archives of Integrated Medicine, Vol. 2, Issue 5, May, 2015.
Copy right 2015,, IAIM, All Rights Reserved.
Page 225
Acne: Etiopathogenesis and its management
Etiopathogenesis of acne
Acne vulgaris is multifactorial in origin involving
both endogenous and exogenous factors. There
are four primary pathogenic factors, which
interact in a complex manner to produce acne
lesions [5].
Increased sebum production by the
sebaceous gland.
Alteration in the keratinization process.
Follicular
colonization
by
propionibacterium spp.
Release of inflammatory mediators into
the skin.
Others contributing factors include hormonal
influences from
m estrogen and androgens, such
as DHEAS (dehydro-epiandrosterone
epiandrosterone sulfate),
which increases sebum production in
prepubescent children, leading to acne [6, 7].
Seborrhea (increase in sebum secretion) and
sebaceous gland hypertrophy and hyperplasia
are the hallmarks of acne [8]. The changes in the
quality of sebum may cause irritation of the duct
epithelium. It is found that high levels of
squalene and wax esters are found in sebum of
acne patients [9]. Lowered levels of linoleic acid
in sebum can lead to acne
ne vulgaris by promoting
the accumulation of cornified cells [10, 11].
Ductal hypercornification is seen histologically
as microcomedones, which are initial Lesions of
acne. The stimulus to the hyperkeratosis of duct
epithelium may be androgens, or it may
ma be
irritating effect of sebaceous lipids as they pass
through the duct. The acceleration in the rate of
sebum secretion or its composition may irritate
the infundibular keratinocytes, leading to
release of inflammatory substance like IL-1,
IL
this in turn causes reduction of sebaceous
linoleic acid and 5-reductase
reductase enzyme levels.
These changes lead to induction of follicular
hyperkeratosis [12]. Comedogenesis occurs
when abnormally desquamating corneocytes
ISSN: 2394-0026 (P)
ISSN: 2394-0034 (O)
accumulate within the sebaceous follicle and
form a keratinous plug [13]. It blocks the
follicular ostium at the skin surface; it becomes
visible as closed comedone (white head). An
open comedone (black head) occurs if the
follicular ostium dilates and filled with debris.
It is widely accepted that propionibacterium
propi
species (P. acne, P. granulosum) etc. are a major
factor in the pathogenesis of acne. P. acne is a
common skin resident and one of the major
components of the microbial flora of the
pilosebaceous follicle [14]. These resident
bacteria produce more lipases which are
responsible for hydrolysis of triglycerides to free
fatty
acids
contributing
to
follicular
hyperkeratosis and even rupture of follicle [15].
Inflammatory process is a key component of
acne which largely accounts for its morbidity
and sequlae. Perifollicular T-- cells are involved in
the immunological events in genetically
predisposed
individuals,
initiating
comedogenesis through release of IL-1
IL [16]. In
addition, ductal corneocytes also produce IL-2,
IL
IL-8 and TNF- which contribute to
inflammation.
Androgens increase sebum
secretion and also cause sebaceous gland
hyperplasia [17]. Estrogen, on the other hand,
suppresses sebaceous gland activity [18]. There
is a negative relationship between acne severity
and serum sex hormone binding
bindi globulin (SHBG)
levels. Peripheral hyper-androgenism
androgenism in many
cases may correlate with severity of acne in
women, and can guide appropriate hormone
therapy [19].
A hot and humid climate aggravates acne due to
increased sweating causing ductal hydration.
hydrati
Emotional stress also plays a significant role in
the aggravation of the pre-existing
pre
acne [20].
External application of oils, pomades, and other
comedogenic chemicals cause acneiform
eruptions [21].
International Archives of Integrated Medicine, Vol. 2, Issue 5, May, 2015.
Copy right 2015,, IAIM, All Rights Reserved.
Page 226
Acne: Etiopathogenesis and its management
A high glycemic diet induces hyper-insulinemia
hyper
which
h results in androgen synthesis, similar to
poly cystic ovarian disease (PCOD) [22]. Diet
induced hyper-insulinemia
insulinemia also increases level of
IGF-1
1 (Insulin Like growth factor) and reduce IGF
binding proteins. The increased free IGF-1
IGF level
results in unregulated
lated growth of follicular
epithelium, increased sebum production and
synthesis of androgens from gonads [22].
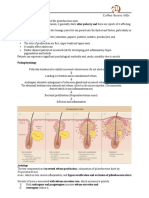
Sequence of events
The microcomedones are the first subclinical
lesion. It is caused by blockage of the sebaceous
canal due to altered keratinization leading to
retention of sebum and initiation of an
inflammatory process. An increase in the
microbial flora increases inflammation (papules
and pustule formation). Further retention of
sebum leads to rupture of sebaceous gland and
spreads the sebum in the dermis resulting in
nodule formation. Confluence of affected glands
results in accumulation of pus, fluid and cyst
formation. A scar results when
en such cysts heal
after rupture or absorption of fluid [4].
The severity of acne can be graded on clinical
grounds as under [4].
Grade 1 (mild): Comedones,
omedones, occasional
papules.
Grade 2 (moderate): Comedones,
omedones, many
papules, few pustules.
Grade 3 (severe): Predominantly
pustules, nodules and abscesses.
Grade 4 (cystic): Mainly
ainly cysts or abscess,
widespread scarring.
The grading is arbitrary and is used as one of the
parameters for treatment and follow up.
Management of acne vulgaris patients [4]
General measures.
Specific measure.
ISSN: 2394-0026 (P)
ISSN: 2394-0034 (O)
General measures
Eliminate stress by reassurance.
Counseling of the patient regarding
nature of illness, treatment modalities
and its outcome.
Advice to avoid scratching of lesions.
Assess the endocrinal status and
premenstrual flares.
Advise to avoid the use of acnegenic
drugs, oils, pomades and heavy
cosmetics.
Balanced diet should be advised. Avoid
high glycemic diet.
Regular washing of face with soap and
water.
Specific measures
The general principles of treatment
treat
are based
upon four strategies that may be combined
according to the clinical aspect of acne patient.
Decreasing the sebaceous gland
secretion.
Correcting the ductal hypercornification.
Decreasing P. acne population and
associated flora.
Producing an anti-inflammatory
inflammatory effect.
Keep in mind one treatment does not fit all
[23].
Topical therapy
Numerous topical preparations are in use for
their anti-comedogenic,
comedogenic, anti-seborrheic
anti
and
antibacterial properties.
Topical Retinoids
Various topical retinoid
d preparations
preparation available
are
Tretinoin: 0.025%, 0.05%, 0.1% gel
/cream.
Isotretinoin: 0.05% gel.
Adaplene: 0.03%, 0.1% gel.
Tazarotene: 0.1%and 0.05% gel.
International Archives of Integrated Medicine, Vol. 2, Issue 5, May, 2015.
Copy right 2015,, IAIM, All Rights Reserved.
Page 227
Acne: Etiopathogenesis and its management
Mechanisms of action include restoration of the
disturbed keratinization, increase in cell
turnover and regulation of prostaglandin
synthesis. Topical retinoids reduce the number
and formation of precursor lesions; reduce
mature comedones and inflammatory lesions.
The main adverse effect with these agents is
primary irritant dermatitis which can present as
erythema, scaling, and burning sensation and
can vary depending on the skin type, sensitivity
and formulation [24].
Benzoyl Peroxide: It is as effective as
topical retinoids and used in gel, cream
or lotion in a strength varying from 2.5
to 10%. It is a broad-spectrum
broad
antimicrobial agent effective via its
oxidizing activity. It has antianti
inflammatory,
keratolytic
and
comedolytic activities. It is indicated in
mild to moderate acne. Its main side
effects are excessive dryness, irritation,
allergic contact dermatitis and bleaching
of clothes, hair and bed linen [25].
Topical antibiotics: These are used in
inflammatory
acne.
Topical
erythromycin and clindamycin are the
most popularr [26], used in 1-4%
1
formulation either alone or in
combination with benzoyl peroxide or
adaplene. Side effects are minor
including erythema, peeling, itching,
dryness, burning and development of
resistance.
Other topical agents are mentioned as
below.
Azelaic
zelaic acid available 1010
20% cream and effective in
inflammatory
and
comedonal acne [27, 28].
Salicylic acid used as
comedolytic agent, but is
less potent then topical
retinoid [29].
ISSN: 2394-0026 (P)
ISSN: 2394-0034 (O)
Lactic acid is found useful in
reducing acne lesions [30].
Tea-tree
tree oil 5% [31]
Picolinic acid gel 10% [32]
Dapsone gel 5% [33]
Topical 5-fluorouracil
5
[34]
Systemic therapy
Tetracyclines [35]
Tetracyclines
etracyclines - 500mg - 1gm
per day.
Doxycycline - 50-200mg per
day.
Minocycline - 50-200mg per
day.
Lymecycline - 150-300mg
per day.
Sulpha drugs [36]
Cotrimoxazoles (80 mg
trimethoprim + 400 mg
sulphamethoxazole).
Dapsone 50 200 mg per
day.
Macrolides [36]
Erythromycin 250-500 mg
qid
Azithromycin 500 mg once
a day for three days in a
week
Hormonal therapy [37]
Estrogen ethynyl estradiol
30
micro
gm
with
progesterone.
Antiandrogens: Cyproterone
acetate 50-200 mg,
Spironolactone 50-100 mg
per day
Corticosteroids:
Prednisolone
rednisolone 2.5-5 mg per
day [38].
Oral zinc therapy 200 mg per day [39].
Oral retinoids - isotretinoin 0.1-2
0.1
mg
per kg per day [40].
International Archives of Integrated Medicine, Vol. 2, Issue 5, May, 2015.
Copy right 2015,, IAIM, All Rights Reserved.
Page 228
Acne: Etiopathogenesis and its management
Phototherapy the efficacy of UV
radiation in acne is because of presence
of porphyrins in p-acne
acne [41].
Chemical peeling with 10-50%
50% glycolic acid or
10-30
30 % salicylic acid leads to significant
resolution
olution of comedones, papules and pustules.
Repeated glycolic acid peeling is necessary for
acne scars and cystic lesions [42].
Conclusion
Various
arious topical and systemic drugs are available
to treat acne. A summary of the approach to
treatment of acne as perr the severity is as
follows [43].
A. Mild involvement (only comedones )
benzoyl peroxide gel
salicylic acid as cleanser
azelaic acid
B. Mild to moderate involvement (comedone ,
few papules and or pustules)
benzoyl peroxide gel or
topical retinoids and
topical antibiotics.
C. Moderate to severe involvement (many
inflammatory papules , pustules , 1-2
1
nodules and or scarring)
Oral antibiotics
Sebostatic agent - hormonal
therapy, Isotretinoin.
D. Cystic acne (more than 2 nodules, cysts
abscess, scar)
Aspiration
n of the cysts and
intra-lesional
lesional steroid and
Systemic antibiotics and
Dapsone or sebostatic agent
Adjunctive
therapy
comedone
expression,
chemical
peels,
micro
microderma-abrasion.
abrasion.
Laser
aser and light therapy blue light, UV light,
light pulsed
dye laser.
ISSN: 2394-0026 (P)
ISSN: 2394-0034 (O)
Acne surgery
sur
- draining of
cysts and punch grafts for
scars, skin resurfacing with
laser, cryosurgery, dermaderma
abrasion and fillers.
References
1.
2.
3.
4.
5.
6.
7.
8.
Leyden J J. Therapy for Acne vulgaris.
The New Eng J Med.,
Med. 1997; 1156-62.
Leyden
JJ.
Current
issues
in
antimicrobial therapy for the treatment
of acne. J Eur Dermatol Venereol.,
Venereol.
2001; 15: 51-5.
Koo J. The psycho-social
psycho
impact of
acne: Patients
atients perceptions. J Am Acad
Dermatol., 1995; 32: s26-30.
Tutakne M A, Vaishampayan S S. Acne,
A
Rosacea and perioral dermatitis. In:
Valia R G, Valia A R editors, IADVL text
book of dermatology. Vol 1; 3rd edition;
Bhalani publishing house: 2008; p.
p 83950.
Thiboutot D, Gollnick H, Bettoli V, et al.
Global alliance to improve outcomes in
acne.
New
ew
insights
into
the
management of acne: An update from
the Global Alliance to Improve
Outcomes in Acne group. J Am Acad
Dermatol., 2009; 60: S1-50.
Zaenglein A l, Thiboutot D M. Acne
vulgaris. In: Jorizzo J L, Rapini R P,
Olognia J L, editors. Dermatology. 2nd
edition.. Edinburgh: Elsevier Mosby;
2009.
Cappel M, Mauger D, Thiboutot D.
Correlation between serum levels of
insulin-like
like growth factor-1,
factor
dihydroepiandrosterone sulfate and dihydrodihydro
testosterone and acne lesion counts in
adult women. Arch Dermatol.,
Dermatol. 2005;
141: 333-8.
Pochi P E,, Strauss J S. Sebum
production, causal sebum levels,
International Archives of Integrated Medicine, Vol. 2, Issue 5, May, 2015.
Copy right 2015,, IAIM, All Rights Reserved.
Page 229
Acne: Etiopathogenesis and its management
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
titrable acidity of sebum and urinary
fractional 17 keto steroid excretion in
males with acne. J Invest Dermatol.,
Dermatol.
1964; 43: 383-8.
Kenaar P. Lipolysis
lysis of skin surface lipids
of acne vulgaris patients and healthy
controls. Dermatologica,
Dermatologica 1971; 143:
121-9.
Morello A M, Downing D T, Strauss JS.
Octadecadienoic acids in the skin
surface lipids of acne patients and
normal subjects. J Invest Dermatol.,
Dermatol.
1976; 66: 319-23.
Downing D T, Stewart M E, Wertz P W,
et al. Essential fatty acids and acne. J
Am Acad Dermatol., 1986; 14: 221-5.
Guy R, Kealy T. Modeling the
infundibulum in acne. Dermatology,
Dermatology
1998; 196: 32-7.
Cunliffe W J, Holland D B, Clark S M, et
al. Comedogenesis:
Some
new
aetiological,, clinical and therapeutic
strategies. Br J Dermatol.,
Dermatol. 2000; 142:
1084-91.
Habif T P. Acne, rosacea, and related
disorders, In: Habif T P, Editior. Clinical
dermatology: A color guide to diagnosis
and therapy, 4th editi
ition. Edinburgh:
Mosby; 2004, p.168-70.
70.
Whiteside J A, Voss J G. Incidence and
lipolytic activity of Propionibacterium
acnes and P. granulosum
sum in acne and
normal skin. J Invest Dermatol.,
Dermatol. 1973;
60: 94-7.
Jeremy A H, Holland D B, Roberts S G,
et al. Inflammatory
ory events are
vinvolved in acne lesion
lesio initiation. J
Invest Dermatol., 2003; 121: 20-7.
Pochi P E, Strauss J S. Sebaceous gland
suppression with ethinyloestradiol
ethinyloe
and
diethylstilbestrol. Arch Dermatol.,
Dermatol.
1973; 108: 210-14.
Strauss J S, Kligman A M, Pochi P E. The
effect of androgens and estrogens on
19.
20.
21.
22.
23.
24.
25.
26.
27.
ISSN: 2394-0026 (P)
ISSN: 2394-0034 (O)
human sebaceous glands. J Invest
Dermatol., 1962; 39: 139-55.
Borgia F, Cannavo S, Guarneri F,
Cannavo S P, Vaccare M. Correlation
between endocrinal parameters and
a
acne severity in adult women.
women Acta
Derm Venereol., 2004; 84: 201-04.
Chiu A, Chon S Y, Kimball A B . The
response of skin diseases to stress:
Changes in the severity of acne vulgaris
as affected by examination stress. Arch
Dermatol., 2003; 139: 897-900.
Simpson N B, Cunliffe W J. Disorders of
sebaceous
baceous glands. In: Burns T,
Breathnach S, Cox N, editors. Rooks
Textbook of dermatology. 7th edition.
Oxford: Blackwell Publishing; 2004, p.
43.1-75.
Cordain L, Linedeburg S, Hurtado M, et
al. Acne vulgaris: A disease of western
civilization. Arch Dermatol.,
Derm
2002; 138:
1584-90.
Longshore S J, Hollandsworth K. Acne
vulgaris: One
ne treatment does not fit all.
Cleve Clin J Med., 2003; 70: 670,6724,677-8.
Jain S. Topicaltretion or adapalene in
acne vulgaris: An overview.
overview J Dermatol
Treat., 2004; 15: 200-7.
200
Mills
ills O H, Jr Kligman A M, Pochi P,
Comite H. Comparing 2.5%, 5% and
10% benzolperoxide: On inflammatory
acne vulgaris. Int J Dermatol.,
Dermatol. 1986; 25:
664-7.
Eady E A, Cove J H, Joanes D N, Cunliffe
W J. Topical antibiotics for the
treatment of acne vulgaris: A critical
evaluation of the literature on their
clinical benefit and comparative
efficacy. J Dermatol Treat.,
Treat. 1990; 1:
215-26.
Cunliffe W J, Holland K T. Clinical and
laboratory studies on treatment with
20% azelaic acid cream for acne. Acta
International Archives of Integrated Medicine, Vol. 2, Issue 5, May, 2015.
Copy right 2015,, IAIM, All Rights Reserved.
Page 230
Acne: Etiopathogenesis and its management
28.
29.
30.
31.
32.
33.
34.
35.
Derm VenerolSuppl
ppl (stockh),
(stockh) 1989;
143: 31-4.
Iraji F, Sadeghinia A, Shahmoradi Z,
Siadat A H, Jooya A. Efficacy of topical
azelaic acid gel in the treatment of
mild- moderate acne vulgaris. Indian J
Dermatol Venereol Leprol.,
Leprol. 2007; 73:
94-6.
Shalita A R. Treatment of mild and
moderate acne vulgaris with salicylic
acid in an alcohol detergent
detergent vehicle.
Cutis, 1981; 28: 556-8,
8, 561.
Garg T, Raman M, Pasricha JS, Verma
KK. Long term topical application of
lactic acid/lactate lotion as a preventive
treatment for acne vulgaris. Indian J
Dermatol Venereol Leprol,
Leprol 2002; 68:
137-9.
Enshaieh S, Jooya A, Sidat A H, Iraji F.
The efficacy of 5% topical tea tree oil
gel in mild to
o moderate acne vulgaris: A
randomized, double--blind placebo
controlled study.. Indian J Dermatol
Venereol Leprol, 2007; 73: 22-5.
Hefferman M P, Nelsoa M M, Anadkat
M J. A pilot study of the safety and
efficacy of picolinic acid gel in the
treatment of acnee vulgaris. Br J
Dermatol., 2007; 136: 548-52.
548
Draelos Z D, Carter E, Maloney J M, et
al.
Two
randomized
studies
demonstrate the efficacy and safety of
dapsone gel, 5%for the treatment of
acne vulgaris. J Am Acad Dermatol.,
Dermatol.
2007; 56: 439.
Milstein H G. 5-Fluorouracil
Fluorouracil as an aid in
the management of acne and melasma.
Jam Acad Dermatol., 1981; 4: 97-8.
Cunliffe W J, Gellnick H P. Acne:
Diagnosis and management. First
Source of support: Nil
36.
37.
38.
39.
40.
41.
42.
43.
ISSN: 2394-0026 (P)
ISSN: 2394-0034 (O)
edition, London: Martin Dermitz ltd;
2001.
Mernadier J, Alirezai M. Systemic
antibiotics for acne. Dermatology, 1998;
196: 135-9.
Redmond G F, Elson W H, Lippman J S,
Hafrisen M F, Jones T M, Jorizzo J L.
Norgestimate and ethinylestradiol in the
treatment of acne vulgaris. A
randomized placebo controlled trial.
Obstet Gynaecol., 1997; 89: 615-22.
Saiohan E M,, Burton J L.
L Sebaceous
gland suppression in female acne
patients by combined glucocortcoid and
oestrogen
trogen treatment. Br J Dermatol.,
Dermatol
1981; 103: 139-42.
Dreno B, Amblerd P, Agache P, et al. Low
doses of zinc gluconate for inflammatory
acne. Acta Derm Venereol.,
Venereol. 1989; 69:
541-3.
Gollnick H, Cunliffe W, Birson D,
D et al.
Management of acne;
acne A report from
global alliance to improve outcome in
acne. J Am Acad Dermatol.,
Dermatol. 2003; 49: S137.
Papageorgiou P, Katsambas A, Chu P.
Photo therapy with blue (415 nm) and
red (660 nm) light in the treatment of
acne vulgaris.Br J Dermatol,
Dermatol 2000; 142:
973-8.
Wang C M, Haung C L,
L Hu C T, Chan M I.
The effect of glycolic acid on the
treatment of acne in Asian skin.
Dermatological Surgery,
Surgery 1997; 23: 23-8.
Batra RS. Acne. In: Arndt K A, Hsu J T S,
editors. Manual of dermatologic
therapeutics. 7th edition,
ed
Philadelphia:
Lippincott
cott Williams and Wilkims; 2007,
p. 7- 17.
Conflict of interest: None declared.
International Archives of Integrated Medicine, Vol. 2, Issue 5, May, 2015.
Copy right 2015,, IAIM, All Rights Reserved.
Page 231
Potrebbero piacerti anche
- Folliculitis, A Simple Guide To the Condition, Treatment And Related DiseasesDa EverandFolliculitis, A Simple Guide To the Condition, Treatment And Related DiseasesNessuna valutazione finora
- Acne: Etiopathogenesis and Its Management: Usha Kataria, Dinesh ChhillarDocumento7 pagineAcne: Etiopathogenesis and Its Management: Usha Kataria, Dinesh ChhillarBayu Surya DanaNessuna valutazione finora
- Pathogenesis of Acne: Masahiko Toyoda Masaaki MorohashiDocumento2 paginePathogenesis of Acne: Masahiko Toyoda Masaaki Morohashihadi firmanNessuna valutazione finora
- Acne VulgarisDocumento53 pagineAcne VulgarisBahaa Shaaban100% (1)
- A Strategic Review On The Involvement of Receptors, Transcription Factors and Hormones in Acne PathogenesisDocumento13 pagineA Strategic Review On The Involvement of Receptors, Transcription Factors and Hormones in Acne Pathogenesisoctavio oliveiraNessuna valutazione finora
- Artigo FabrociniDocumento13 pagineArtigo FabrociniSuzana PoloncaNessuna valutazione finora
- Article Pathogenesis of AcneDocumento5 pagineArticle Pathogenesis of AcneFajrin Dwi SyaputraNessuna valutazione finora
- Development of Anti-Acne Gel From Herbal ExtractionDocumento8 pagineDevelopment of Anti-Acne Gel From Herbal ExtractionInternational Journal of Innovative Science and Research TechnologyNessuna valutazione finora
- Delivery of Pharmaceutical Agents to Treat Acne: Current Status and PerspectivesDocumento10 pagineDelivery of Pharmaceutical Agents to Treat Acne: Current Status and Perspectivesimroatul ulyaNessuna valutazione finora
- Acne VulgarisDocumento11 pagineAcne VulgariserwinNessuna valutazione finora
- HERBAL PLANTS AND PROPIONIBACTERIUM ACNES - AN OVERVIEWDocumento13 pagineHERBAL PLANTS AND PROPIONIBACTERIUM ACNES - AN OVERVIEWmskchoudhuriNessuna valutazione finora
- TranslateDocumento67 pagineTranslatesriwahyuniNessuna valutazione finora
- Pathogenesis of Acne Vulgaris SimplifiedDocumento5 paginePathogenesis of Acne Vulgaris SimplifiedErena HairunisaNessuna valutazione finora
- Journal Reading Marsya Y. Loppies (201283003) BaruDocumento18 pagineJournal Reading Marsya Y. Loppies (201283003) BaruMarsya Yulinesia LoppiesNessuna valutazione finora
- Acne Vulgaris: Key PointsDocumento6 pagineAcne Vulgaris: Key PointsRafly FairuzNessuna valutazione finora
- Acne, The Skin Microbiome, and Antibiotic Treatment2019Documento10 pagineAcne, The Skin Microbiome, and Antibiotic Treatment2019sara3elena3manolacheNessuna valutazione finora
- New Insights Into The Etiopathogenesis of Seborrheic DermatitisDocumento5 pagineNew Insights Into The Etiopathogenesis of Seborrheic DermatitisnyomanNessuna valutazione finora
- Bab I Pendahuluan 1.1 Latar Belakang: Case Report Session Ini Disusun Untuk Memenuhi Tugas Kepaniteraan KlinikDocumento33 pagineBab I Pendahuluan 1.1 Latar Belakang: Case Report Session Ini Disusun Untuk Memenuhi Tugas Kepaniteraan KlinikNurifnaNessuna valutazione finora
- AcneVulgaris PDFDocumento12 pagineAcneVulgaris PDFMhae LopezNessuna valutazione finora
- Acne and food relation: A naturopathic perspectiveDocumento4 pagineAcne and food relation: A naturopathic perspectiveant beeNessuna valutazione finora
- Bacterial Skin Infections GuideDocumento33 pagineBacterial Skin Infections GuideLucas Victor AlmeidaNessuna valutazione finora
- 547 2094 1 PB PDFDocumento8 pagine547 2094 1 PB PDFYesichaNessuna valutazione finora
- Acne More Than Skin DeepDocumento7 pagineAcne More Than Skin DeepImahalimahNessuna valutazione finora
- Acné Vulgaris Nueva Evidencia Sobre Patogenesis y Futuras Modalidad de TratamienytoDocumento10 pagineAcné Vulgaris Nueva Evidencia Sobre Patogenesis y Futuras Modalidad de TratamienytoMaría Fernanda Castro FuentesNessuna valutazione finora
- Therapeutice Agents and Herbs in Topical Application For Acne Treatment PDFDocumento9 pagineTherapeutice Agents and Herbs in Topical Application For Acne Treatment PDFAaron PowersNessuna valutazione finora
- Drug-Induced Acneiform EruptionDocumento10 pagineDrug-Induced Acneiform EruptionIvan KurniadiNessuna valutazione finora
- Acne and Rosacea: AetiologyDocumento7 pagineAcne and Rosacea: AetiologyananNessuna valutazione finora
- Jurnal Kulit JerawatDocumento13 pagineJurnal Kulit JerawatDevana MaelissaNessuna valutazione finora
- Meth Elab Topic N2Documento19 pagineMeth Elab Topic N2Group M1869Nessuna valutazione finora
- Dandruff PDFDocumento8 pagineDandruff PDFArthur ChietraNessuna valutazione finora
- Diaper Rash: Practice EssentialsDocumento17 pagineDiaper Rash: Practice EssentialsXimena MedinaNessuna valutazione finora
- Acne More Than Just Skin Deep: Review Explores Causes and TreatmentDocumento8 pagineAcne More Than Just Skin Deep: Review Explores Causes and TreatmentPRANAY TIWARINessuna valutazione finora
- PH and Acne 2018Documento8 paginePH and Acne 2018Mariana de la VegaNessuna valutazione finora
- Pityriasis Capitis: Causes, Pathophysiology, Current ModalitiesDocumento13 paginePityriasis Capitis: Causes, Pathophysiology, Current ModalitiesShashikant DrShashikant BagadeNessuna valutazione finora
- Sala CunillDocumento13 pagineSala CunillAnak Agung Ayu Ira Kharisma Buana Undiksha 2019Nessuna valutazione finora
- Antimicrobial Activity of GelaDocumento19 pagineAntimicrobial Activity of GelanuriffaniaminNessuna valutazione finora
- Practice Essentials AcneDocumento6 paginePractice Essentials AcneaigoooNessuna valutazione finora
- Microbiome and Probiotics in Acne Vulgaris-A Narrative ReviewDocumento11 pagineMicrobiome and Probiotics in Acne Vulgaris-A Narrative ReviewVanNessuna valutazione finora
- Impetigo - Review : Luciana Baptista Pereira1Documento7 pagineImpetigo - Review : Luciana Baptista Pereira1Edwar RevnoNessuna valutazione finora
- Acne vulgaris pathogenesis and future treatment modalitiesDocumento11 pagineAcne vulgaris pathogenesis and future treatment modalitiesTrustia RizqandaruNessuna valutazione finora
- Title: Skin Microbiome and Acne Vulgaris: Staphylococcus, A New Actor in AcneDocumento18 pagineTitle: Skin Microbiome and Acne Vulgaris: Staphylococcus, A New Actor in Acnehadi firmanNessuna valutazione finora
- Diaper (Napkin) Dermatitis A FoldDocumento6 pagineDiaper (Napkin) Dermatitis A FoldLina Mahayaty SembiringNessuna valutazione finora
- Pathophysiology and Impact of Acne Vulgaris (38 charactersDocumento6 paginePathophysiology and Impact of Acne Vulgaris (38 charactersPrajnamita Manindhya El FarahNessuna valutazione finora
- Acne and Other Common Acneiform DisordersDocumento6 pagineAcne and Other Common Acneiform DisordersSudesna Roy ChowdhuryNessuna valutazione finora
- Tinea Versicolor: Pathophysiology, Etiology in <40 CharsDocumento4 pagineTinea Versicolor: Pathophysiology, Etiology in <40 Charswahyuni taslimNessuna valutazione finora
- An Overview On Medicinal Plants For The TreatmentDocumento8 pagineAn Overview On Medicinal Plants For The TreatmentSEPTIANA SAPUTRINessuna valutazione finora
- Acne Vulgaris New Evidence in Pathogenesis and Future Modalities of TreatmentDocumento11 pagineAcne Vulgaris New Evidence in Pathogenesis and Future Modalities of TreatmentyelsiNessuna valutazione finora
- 22212-Article Text-71095-1-10-20211130Documento5 pagine22212-Article Text-71095-1-10-20211130Chanell Giv,NNessuna valutazione finora
- Adolescent Acne Treatment Options OverviewDocumento3 pagineAdolescent Acne Treatment Options OverviewDesi RatnaningtyasNessuna valutazione finora
- Adolescent Acne Treatment Options OverviewDocumento3 pagineAdolescent Acne Treatment Options OverviewMutiaraDaraNessuna valutazione finora
- Host-Microbiome Interactions and Recent Progress Into Understanding The Biology of Acne VulgarisDocumento17 pagineHost-Microbiome Interactions and Recent Progress Into Understanding The Biology of Acne VulgarisMing XianNessuna valutazione finora
- AcnevulgarisDocumento35 pagineAcnevulgarisMai AmerNessuna valutazione finora
- Chronic Pruritus in The Elderly: Pathophysiology, Diagnosis and ManagementDocumento15 pagineChronic Pruritus in The Elderly: Pathophysiology, Diagnosis and ManagementFersha Syafir RamadhanNessuna valutazione finora
- Propionobacterium Acnes: An Update On Its Role in The Pathogenesis of AcneDocumento3 paginePropionobacterium Acnes: An Update On Its Role in The Pathogenesis of AcneJoebert Gelera GarciaNessuna valutazione finora
- 124-Article Full Text-229-1-10-20210102Documento4 pagine124-Article Full Text-229-1-10-20210102sri karuniaNessuna valutazione finora
- Acne and Related Skin Conditions: Causes and TreatmentsDocumento43 pagineAcne and Related Skin Conditions: Causes and TreatmentsqurataNessuna valutazione finora
- Eukalyptusoel AkneDocumento5 pagineEukalyptusoel AkneAmit SachanNessuna valutazione finora
- The intricacies of vitiligo and recent updates in treatment modalitiesDocumento11 pagineThe intricacies of vitiligo and recent updates in treatment modalitiesMostafa EidNessuna valutazione finora
- Harper's Textbook of Pediatric DermatologyDa EverandHarper's Textbook of Pediatric DermatologyProf. Dr. Alan D. IrvineNessuna valutazione finora
- Acute Perimyocarditis Following mRNA COVIDDocumento1 paginaAcute Perimyocarditis Following mRNA COVIDRamadhan Harya Puja KusumaNessuna valutazione finora
- Happy ChemicalsDocumento43 pagineHappy ChemicalsAkramPal100% (4)
- AntibicDocumento95 pagineAntibicJameston BostreNessuna valutazione finora
- Malaria PDFDocumento36 pagineMalaria PDFRamadhan Harya Puja KusumaNessuna valutazione finora
- 3 SHE New Employee Checklist OtherDocumento4 pagine3 SHE New Employee Checklist OtherRamadhan Harya Puja KusumaNessuna valutazione finora
- DuaneDocumento2 pagineDuaneRamadhan Harya Puja KusumaNessuna valutazione finora
- PT Instructions SuturesDocumento1 paginaPT Instructions SuturesRamadhan Harya Puja KusumaNessuna valutazione finora
- TITLE: Evidence of BetrayalDocumento22 pagineTITLE: Evidence of BetrayalRamadhan Harya Puja KusumaNessuna valutazione finora
- Your Electronic Ticket Receipt PDFDocumento2 pagineYour Electronic Ticket Receipt PDFRamadhan Harya Puja KusumaNessuna valutazione finora
- Antidote Chart 2012 PDFDocumento3 pagineAntidote Chart 2012 PDFRommel IrabagonNessuna valutazione finora
- SH VersusManitol CCM 2011Documento6 pagineSH VersusManitol CCM 2011Ramadhan Harya Puja KusumaNessuna valutazione finora
- RARBGDocumento1 paginaRARBGRamadhan Harya Puja KusumaNessuna valutazione finora
- ICMJE Form For Disclosure of Potential Conflicts of InterestDocumento21 pagineICMJE Form For Disclosure of Potential Conflicts of InterestRamadhan Harya Puja KusumaNessuna valutazione finora
- Antidote Chart 2012 PDFDocumento3 pagineAntidote Chart 2012 PDFRommel IrabagonNessuna valutazione finora
- HPVDocumento32 pagineHPVRamadhan Harya Puja KusumaNessuna valutazione finora
- Fisiologi Ketinggian AklimatisasiDocumento11 pagineFisiologi Ketinggian AklimatisasiRamadhan Harya Puja KusumaNessuna valutazione finora
- PearlingDocumento1 paginaPearlingRamadhan Harya Puja KusumaNessuna valutazione finora
- Daftar PustakaDocumento2 pagineDaftar PustakaRamadhan Harya Puja KusumaNessuna valutazione finora
- EncephalitisDocumento25 pagineEncephalitisAndreas IoannouNessuna valutazione finora