Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
PEDIAPrelims - Care of The Newborn 2
Caricato da
RenatoCosmeGalvanJuniorTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
PEDIAPrelims - Care of The Newborn 2
Caricato da
RenatoCosmeGalvanJuniorCopyright:
Formati disponibili
AUFMED
ANTHROPOMETRIC MEASUREMENTS
Weight
-average: 3000g
-LBW= below 2500 gms; regardless of AOG
Length
- average: 50cm
-techniques: using tape measure
(supine with legs extended)
- crown to rump
- head to heel
Head Circumference (HC):
- average: 35cm
- technique: using tape measure
- from the most prominent part of the
OCCIPUT to just above the EYEBROWS
- 1/3 the size of an adults head
- disproportionately LARGE for its body
- HC should be = or 2cm > CC
Chest Circumeference (CC):
- 30 to 33cm
- Technique: using tape measure
- from the lower edge of the SCAPULAS to
directly over the NIPPLE LINE anteriorly
- CC should be = of <2cm than HC
SKIN
NURSERY CARE CONSIDERATIONS
Under natural light
Assess for:
- color
- hair distribution
- Turgor/ testure
- pigmentation/ birthmarks
- other skin marks
Skin Color
Velvety smooth and puffy esp. at the legs, dorsal
aspects of hands and feet and in the scrotum of
labia
Pinkish red (light skinned) to pinkish brown to
yellow (dark skinned)
Ruddy or reddish due to increased RBC
concentration and decreased subQ tissues
especially premature infants
Acrocyanosis
Bluish discoloration of palms of hands and soles
of feet
Due to immature peripheral circulation
Exacerbated by cold temperatures
Normal within 1st 24 hours
Dr. Rodolfo Ng | June 25, 2015 | Pediatrics
CARE OF THE NEWBORN II
Pallor/ Cyanosis
May indicate hypothermia, infection (usually non
specific in newborns), anemia, hypoglycemia,
cardiac, respiratory or neurological problems
Usually when we extract blood from prematures,
we take note of the amount of blood extracted
Jaundice
50% full term and 80% preterm visibly jaundiced
by 3-5 days
Common among Chinese newborns
Physiologic Jaundice
- noted after 24-48 hours of life
- Term: peak 3-4 days and disappear 7-10
days
- Preterm: peark 5th and gone 2 weeks
- due to immaturity of liver
Pathologic Jaundice
- occurs on the 1st 24 hours of life
- BIlirubin increases >0.5 mg/dl/hr
- peak bilirubin >12mg/dl term and >15mg/dl
in preterm during the first week of life
- hepatosplenomegaly and anemia
- clinical jaundice persisting >1 week (term)
and > 2 weeks (preterm)
*Ask the mother what the color of the urine is
because usually babies are red after birth.
Breastfeeding jaundice
Early onset of jaundice within the first 3-4 days
Also called exaggerated jaundice, lack of
breastmilk jaundice
Factors: oral administration of water of glucose
water, inadequate nursing and decreased stool
output
Rx: continuous breastfeeding; no complementary
feedings
Breast Milk Jaundice
Later onset of jaundice occurring towards the end
of the 1st week and persisting for 3 weeks to 3
months
Cause: unknown, unknown constituent in
breastmilk
Dx by exclusion
Rx: stop breastfeeding x 2-3 days
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 1 of 10
Reassure the mother that the jaundice is not
because of breastfeeding
Phototherapy (eyes and sex organs should be
covered to prevent damage)
BIRTHMARKS
1. Mongolian Spots
- Blue-green or gray pigmentation
- Lower back, sacrum & buttocks
- Disappears by 4 years of age
Meconium Staining
Over the skin, fingernails and umbilical cord
Due to passage of meconium in utero due to fetal
hypoxia
Passage of meconium due to asphyxia in baby <
34 week gestation is UNUSUAL
The baby was in a state of hypoxia and
underwent fetal distress.
Prematures do not pass meconium
Lanugo
Found after 20 weeks of gestation on the entire
body except the palms and soles
Fine downy hair that covers the shoulders, back
and upper arms
NURSERY CARE CONSIDERATIONS
More mature, less lanugo
May diappear within 2 weeks
Preterm: woolly patches of lanugo on skin and
head
Post term: parchment-like skin without lanugo
Vernix Caseosa
Protective cheesy-like, gray-white fatty substance
FT: skin folds under the arms and in the groin
under the scrotum or in the labia
Nursing considerations:
-Use baby oil
-DO NOT attempt to remove vigorously
2. Strawberry Marks
- Nevus Vasculosus or Capillary Hemangioma
- Dark red, raised lobulated tumor
- Head, neck trunk & extremities
- After 7 to 9 years of age
3. Large Capillary Hemangioma
4. Cavernous Hemangioma
It is helpful if you do not totally remove especially
for prematures
Post matures usually look paranoid
Desquamation
Dryness/ peeling of the skin
Usually occure after 24-36 hours
Marked scalliness and desquamation=
signs of postmaturity
Milia
Multiple, yellow or pearly white papules
approx. 1 mm wide
Due to enlarged or clogged sebaceous
gland
Usually found on the nose, chin, cheeks,
eyebrows and forehead
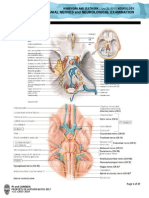
5. Sturge-Weber Syndrome
- A sporadic vascular disorder and
- Consists of a constellation of symptoms and
signs including:
facial capillary malformation (port-wine
stain)
abnormal blood vessels of the brain
(leptomeningeal angioma)
abnormal blood vessels of the eye
leading to glaucoma
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 2 of 10
Patients present with seizures, hemiparesis,
stroke-like episodes, headaches, and
developmental delay
Port-wine stain (nevus flamneus) involving
the forehead and upper lip, glaucoma and
contralateral jacksonian seizures
6. Kasabach-Merritt Syndrome
- Association of a giant hemangioma with
localized intravascular coagulation causing
thrombocytopenia and hypofibrinogenemia
- The site of the hemangioma is obvious, but
retroperitoneal and intraabdominal
hemangiomas may require body imaging for
detection
- Inside the hemangioma there is platelet
trapping and activation of coagulation, with
fibrinogen consumption and generation of
fibrin(ogen) degradation products.
Arteriovenous malformation within the lesions
can cause heart failure
- Peripheral blood smear shows
microangiopathic changes
- Cavernous hemangioma
- Thrombocytopenia
- Microangiopathic changes in RBC (detected
thru peripheral blood smear)
OTHER SKIN MARKS
1. Mottling
- Cutis marmorata
- Reticulated pattern of constricted capillaries
and venules due to vasomotor instability in
immature infants
- Bluish mottling or marbling of skin in
response to chilling, stress or overstimulation
- *Infection of blood/sepsis may also manifest
as mottling in newborns
2. Erythema Toxicum
- Newborn rash; urticaria of newborn;
eosinophil rash (because eosinophils are
present upon examination of lesion under the
microscope)
- Small, white, yellow, or pink to red popular
rash
- Trunk, face and extremities
- Within 48 hrs.
- May be mistaken for septic spots. Careful
examination must be done to prevent
unnecessary administration of antibiotics.
- Suspect allergic or hypersensitivity reaction
3. Petechiae
- Pinpoint hemorrhages on skin
- Due to increased vascular pressure, infection
or thrombocytopenia
- Within 48 hrs.
- *Petechiae do not disappear after blanching
- *May result from mechanical causes such as
cordcoil and pressure during delivery.
4. Ecchymosis
- Bruises
- As a result of rupture of blood vessels
- May appear over the presenting part as a
result of trauma during delivery
- May also indicate infection or bleeding
problems
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 3 of 10
5. Harlequin Sign
- When on side, dependent side turns red and
upper side/half turns pale
- Due to gravity and vasomotor instability or
immature circulation
- Clowns Suit
*At birth, it is possible that there is no more
posterior fontanel present due to early
closure/overlapping of sutures
- Bulging or sunken
Sutures
- Overriding or separated
Head lag
- Common when pulling newborn to a sitting
position
- When prone, NB should be able to lift the
head slightly and turn head from side to side
1. Caput Succeedaneum
- Swelling of soft tissues of scalp
- Due to pressure
- Crosses the suture lines
- Presenting part
2. Cephalhematoma
- Subperiosteal hemorrhage with collection of
blood
- Due to rupture of capillaries as a result of
trauma
- Does not cross suture lines
6. Caf-au-lait spots
- Tan or light brown macules or patches
- No pathologic significance, if <3cm in length
and <6 in number
- If >3 or 6 = Cutaneous neurofribromatosis
Molding
Overlapping of skull bones
Due to compression during labor and delivery
Disappears in a few days
HEAD
Forceps Marks
U-shaped bruising usually on the cheeks after
forceps delivery
What to Assess:
For symmetry, shape, swelling, movement
- Soft, pliable, moves easily
Measure HC; HC = or > CC
Fontanelles soft spot
- Anterior fontanel closes between
months
- Posterior fontanel closes at 2 months
Craniotabes
Localized softening of the cranial bones
Can be indented by pressure of fingers
MOST common among 1st born babies,
pathological in older children (consider possibility
of metabolic dosorders)
Caused by pressure of the fetal skull against the
mothers pelvic bone in utero
9-18
Craniosynostosis
Premature closure of the fontanelles
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 4 of 10
FACE, EYES, EARS, NOSE, MOUTH
What to Assess:
Facial movement and symmetry
Symmetry, size, shape, and spacing of eyes,
nose, and ears
Eyes
-
Ears
-
Color: white sclerae; slate gray, brown, or dark
blue; final eye color is acheieved after 6-12
months
Symmetrical
Pupils equally round, reactive to light and
accommodation (PERRLA)
(+) Blink reflex
(+) transient strabismus due to weak EOM,
maybe normal up to 4-5 months of life
Able to move and fixate momentarily
(+) red reflex; if (-), screen for congenital cataract
or retinoblastoma
(+) edema on eyelids related to pressure during
delivery or as effect of medications
(-) tear formation (begins at 2-3 months)
The child may be crossed eyes, normal, within 45 months
At this point in the lecture, Dr.Ng started
enumerating oddities that are physiologic for the
child:
o Anemia (as long as Hgb is not <9)
o Alopecia (usually at the area of the
External occipital protuberance)
o Anorexia (usually until 10 months)
o Hyperactivity (usually at 1 to 4 years old)
o Strabismus (4 to 5 months)
soft and pliable, with firm cartilage
Pinna should be at the level of outer canthus of
the eye
(+) low set ears : assess for renal or
chromosomal abnormalities (eg Trisomy 21)
May be congested and hear well after a few days
Accessory tragus : remnant of the 1st branchial
arch
Congenital preauricular sinus : ends blindly;
may be a risk for infection and therefore requires
closure via surgery
Mouth
Pink, moist gums
Intact soft and hard palates with (+) Epsteins
pearls
Uvula at midline
Tongue moves freely, symmetrical with short
frenulum
(+) extrusion and gag reflexes
(+) bronchial sounds
(+) breast engorgement : subsides after 2 weeks
(+) edema and prominence of nipples
(+) accessory nipples
(+) witch milk
ABDOMEN
Umbilical Cord
2 arteries and 1 vein [AVA]
2 vessels (1 artery and 1 vein only) : assess for
risk of congenital renal malformation or genetic
disorder eg Trisomy 18
Gradually falls of by the 7th to 10th days
Delayed sloughing : assess for infection, disorde
of granulocyte formation (rare)
DAILY CORD CARE:
o Keep cord dry and clean, clamped for
security
o Apply 70% isopropyl alcohol to the cord
with each diaper change and at least 2-3
times a day
o DO NOT cover with diaper
o Note for any signs of bleeding or
drainage from the cord and other
abnormalities
o Avoid use of Povidone Iodine (Betadine) :
due to the high risk of iodine absorption
via he stump, which may alter thyroid
homeostasis
o Children are abdominal breathers, that is
why putting a piece of fabric around their
abdomen may limit their capacity to
breathe
o Children learn to expectorate only at 6-7
years old, younger ages usually vomit
what is meant to be expectorated
Gastro Intestinal Tract
Capacity: 90mL; with rapid intestinal peristalsis (2
to 3 hours)
Bowel sounds (+) within 1-2 hours after birth
Assess for presence of masses, distention,
depression, or protrusion
Abdomen of children are usually globular
(+) scaphoid : Diaphragmatic Hernia
(+) Distention : LGIT obstruction and mass
Anus
-
check for patency (may use the thermometer to
assess patency while measuring temperature
initially)
First stool (Meconium) appears within the initial
24 hours
Meconium is sticky, blackish-green, odorless
material
IMPERFORATE ANUS
o VATER : Vetebral Anomalies; Anal
atresia; TEF; and radial, renal dysplasia
o VACTERL : same as VATER but with (+)
Cardiac and Limb abnormalities
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 5 of 10
TRANSITIONAL STOOL
o Within 2 to 10 days antenatal
o Breastfed infants : golden yellow,
mushy, more frequent (TID/QID) and has
a sweet smell; watery like
o Bottle-fed infants : pale yellow, firm,
less frequent (BID/TID) and has a more
distinct odor
GENITALS
Female
Labia is edematous
Clitoris is enlarged
Pseudomenstruation is possible
Visible hymen tag
Initial voiding within 24 hours
o
o
o
o
o
o
(+) Ortolanis Click & uneven gluteal folds =
CONGENITAL HIP DYSPLASIA
- (+) inward turning of the foot = CLUB FOOT or
TALIPES EQUINOVARUS
- (+) extra digits = POLYDACTYLY
- (+) web fingers = SYNDACTYLY
- OSTEOGENESIS IMPERFECTA
Brittle Bone Disease
Autosomal recessive
Etiology: unknown
Multiple fractures and callus formation
Severe form: stillbirth or early death
If lived beyond infancy, prognosis is good but
potential to be handicapped
Male
-
Prepuce covers the glans penis
o (+) adherent foreskin : Phimosis
Scrotum is edematous
o Enlarged : hernia
Meatus is centrally located
o If Ventral / Dorsal : Hypo / Epispadias
Testes are fully descended
o Undescended : Cryptorchidism
AMBIGUOUS GENITALIA
- The assessment of ambiguous genitalia may be
summarized through the use of the following
parameters:
o U pelvic ultrasound
o G palpable gonads
o L electrolytes: if there is hyponatremia and
hyperkalemia, suspect CONGENITAL ADRENAL
HYPERPLASIA (CAH)
o Y chromosomal studies
o S steroid tests: urine CS & 17-KS: to rule out
CONGENITAL ADRENAL HYPERPLASIA (CAH)
Skin Creases over the Palms and Soles
Ambiguous Genitalia: Note that the clitoris is
enlarged (resembles glans) and the labia are
thickened (resemble scrotum)
Eliciting the ORTOLANIS SIGN
EXTREMITIES
- Flexed, full ROM, symmetrical
- Clenched fists; flat soles
- With 10 fingers and toes in each hand
- Legs bowed
- Even gluteal folds
- (+) Creases on soles of feet
o (-) Creases = PREMATURITY
- Check for hip fractures or dysplasia
CLUBFOOT/TALIPES EQUINOVARUS
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 6 of 10
POLYDACTYLY (Above) and SYNDACTYLY (Below)
OSTEOGENESIS IMPERFECTA
Swallowing Reflex
Occurs spontaneously after sucking and
obtaining fluids
NEVER disappear
Newborn swallows in coordination with
sucking without gagging, coughing or
vomiting
Tonic Neck Reflex/Fencing Reflex
While the baby is falling asleep or sleeping,
gently and quickly turn the head to one side
As the baby faces the left side, the left arm
and leg extend outward while the right arm or
leg flex and vice-versa
Disappears within 3-4 mos
Palmar (Grasping)/Plantar Reflex
Place a finger in the palm of the babys hand,
then place a finger at the base of the toes
Fingers will curl or grasp the examiners
finger and the toes will curl downward
Palmar: fades within 3-4 mos
Plantar: fades within 8 mos
Moro Reflex
Hold baby in a semi sitting position then allow
the head and trunk to fall backward to at least
a 30-degree angle
Symmetrically abducts and extends the arms;
fans the fingers out and forms a C with the
thumb and the forefinger; and adducts the
arms to an embracing position & returns to a
relaxed state
Present at birth; complete response at 8
weeks
MOST significant singular reflex indicative of
CNS problem (>6 mos)
Disappears after 4-5 mos
NEUROLOGIC SYSTEM
REFLEXES
o Sucking/Rooting Reflex
Touch the lip, cheek or corner of the mouth
Turns head toward the nipple, opens mouth,
takes hold of the nipple and sucks
Disappears after 3-4 mos up to 1 year
Extrusion Reflex
Anything place on the anterior portion of the
tongue will be spit out
To prevent swallowing of inedible substances
Disappears after 4 months
Disappearance indicates readiness for semisolid to solid foods
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 7 of 10
Startle Reflex
Best elicited if baby is 24 hrs old
Make a loud noise or claps hands
Babys arms adduct while elbows flex with
fists clenched
Disappears within 4 mos
Babinski Reflex
Gently stroke upward along the
lateral aspect of the sole, starting
at the heel of the foot to the ball
of the foot
Dorsiflexion of big toe and
fanning of little toes
Disappears starts a 3 mos to 1
year
Disappearance indicates maturity
of CNS
Stepping/Walking/Dancing Reflex
Hold baby in a standing position
allowing one foot to touch a
surface
Simulates walking by alternately
flexing and extending feet
Disappears after 3-4 mos
Other Nursing Responsibilities:
Identification band
Band registration
Birth record and documentation
NEWBORN SCREENING
The Newborn Screening Reference Center
(NSRC) is an office under the National Institutes
of Health (NIH), University of the Philippines
Manila created under RA 9288 The Newborn
Screening Act of 2004
Performed after 24 hours of life up to 3 days
except for patient in intensive care, must be
tested by 7 days.
o Congenital Hypothyroidism (CH)
o Congenital Adrenal Hyperplasia (CAH)
o Galactosemia (GAL)
o Phenylketonuria
o Glucose-6-Phosphate-Dehydrogenase
Deficiency (G6PD Def)
o Maple Syrup Urine Disease (MSUD)
Infant Care Skills
HOLDING THE BABY
1. Football Hold
2. Cradle Hold
3. Shoulder Hold
Football Hold
Purpose: to carry on one hand free
A holding technique in bathing a baby
Use for small babies
Procedure:
1. Slide forearm under his back
2. Support neck and head with your hand
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 8 of 10
3. Press his arm firmly against your side
4. His head faces you
5. Infants feed tucked under your elbow
Hb E/Beta + Thalassemia
Hb H Disease
Hb H/Constant Spring Disease
Hb Variant/Beta + Thalassemia
Homozygous EE
Sickle Cell Disease (Hb S/C Disease)
Sickle Cell Anemia (Hb S/S Disease)
B. Amino Acid Disorders
Phenylketonuria (PKU)
Variant Hyperphenylalaninemia
Maple Svrup Urine Disease (MSUD)
Cradle Hold
Purpose: used for feeding and cuddling a baby
Procedure:
1. Support head in crook of your arm
2. Encircle the body with your arm
3. Press baby firmly against your side
4. Use other hand to support bottom and
thigh
Shoulder Hold
Purpose: used for burping
Procedure:
1. Draw baby towards your chest with one
forearm
2. Bracing his back and your hand cradling
his head
3. Support your babys bottom and thighs
with your other arm
4. Gently press his head against your
shoulder
C. Organic Acid Disorders
Methylmalonic Acidemia MMA - (Mut0)
Methylmalonic Acidemia MMA - (Mut-)
Beta-Ketothiolase Deficiency (BKT)
Isobutyryl-Coa
Dehydrogenase
Deficiency
(IBDHD)
D. Fatty Acid Oxidation Disorders
Medium
Chain
acyl-Coa
Dehydrogenase
Deficiencv (MCAD Deficiency)
Short Chain acyl-Coa Dehvdrogenase Deficiency
(SCAD Deficiency)
Very Long Chain acyl-Coa Dehydrogenase
Deficiency (VLCAD Deficiency)
Other Fatty Acid Oxidation Disorders
E. Cystic Fibrosis and Related Disorders
Partial BD Deficiency
CFTR-Related Metabolic Syndrome (CRMS)
Cystic Fibrosis
Classical Galactosemia
Duarte Galactosemia (D/G)
Other Disorders
ADDITIONAL INFORMATION
In an article published in the ACTA MEDICA PHILIPPINA
in 2012 authored by UP-Manila Chancellor Carmencita D.
Padilla entitled Enhancing Case Detection of Selected
Inherited Disorders through Expanded Newborn
Screening in the Philippines, the following disorders
were proposed to be added:
A. Hemoglobinopathies
Alpha-Thalassemia Major
Beta-Thalassemia Major
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 9 of 10
APPENDIX
PI | ARELLANO GAGUI GALVAN PAMINTUAN TIMBANG
PROPERTY OF AUFSOM BATCH 2017
v3.1 s2015-2016
Page 10 of 10
Potrebbero piacerti anche
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Primitive ReflexesDocumento85 paginePrimitive ReflexesBernadette hauw90% (10)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- Reflex Testing Methods For Evaluating CNS DevelopmentDocumento80 pagineReflex Testing Methods For Evaluating CNS DevelopmentTaufik100% (4)
- PATHOPrelims - 1. Surgical Pathology (Introduction)Documento10 paginePATHOPrelims - 1. Surgical Pathology (Introduction)RenatoCosmeGalvanJuniorNessuna valutazione finora
- Cardiac Muscle PhysiologyDocumento4 pagineCardiac Muscle PhysiologyRenatoCosmeGalvanJuniorNessuna valutazione finora
- CPG Cap 2010Documento12 pagineCPG Cap 2010RenatoCosmeGalvanJuniorNessuna valutazione finora
- Statistics ReviewerDocumento3 pagineStatistics ReviewerRenatoCosmeGalvanJunior100% (1)
- PEDIAPrelims - 2. Care of The Newborn 1 (First 24 Hours To Vital Signs)Documento7 paginePEDIAPrelims - 2. Care of The Newborn 1 (First 24 Hours To Vital Signs)RenatoCosmeGalvanJuniorNessuna valutazione finora
- Common Drugs Used in The Out Patient DepartmentDocumento1 paginaCommon Drugs Used in The Out Patient DepartmentRenatoCosmeGalvanJuniorNessuna valutazione finora
- SURGERYFinals - 1. The AppendixDocumento10 pagineSURGERYFinals - 1. The AppendixRenatoCosmeGalvanJuniorNessuna valutazione finora
- NEUROPrelims - History Taking in NeurologyDocumento4 pagineNEUROPrelims - History Taking in NeurologyRenatoCosmeGalvanJuniorNessuna valutazione finora
- Principles of Cancer TreatmentDocumento7 paginePrinciples of Cancer TreatmentRenatoCosmeGalvanJuniorNessuna valutazione finora
- Pediatric Surgery 2 (Respiratory and Gastrointestinal Conditions) PDFDocumento12 paginePediatric Surgery 2 (Respiratory and Gastrointestinal Conditions) PDFRenatoCosmeGalvanJunior100% (1)
- NEUROPrelims - Cranial Nerves and Neurological ExaminationDocumento37 pagineNEUROPrelims - Cranial Nerves and Neurological ExaminationRenatoCosmeGalvanJuniorNessuna valutazione finora
- GYNEPrelims - UrogynecologyDocumento18 pagineGYNEPrelims - UrogynecologyRenatoCosmeGalvanJuniorNessuna valutazione finora
- Pediatric NursingDocumento17 paginePediatric NursingMark Ray A. EspinozaNessuna valutazione finora
- Paediatric Neurology:: Management Practices and Evidence Based PracticesDocumento41 paginePaediatric Neurology:: Management Practices and Evidence Based PracticesNikita ChaubeNessuna valutazione finora
- Module 6 Psy04 InfancyDocumento10 pagineModule 6 Psy04 Infancyairah magraciaNessuna valutazione finora
- New Born ReflexesDocumento40 pagineNew Born ReflexesKarun Prakash100% (1)
- Assessment and Nursing Management Normal NewbornDocumento17 pagineAssessment and Nursing Management Normal NewbornVinay Kp100% (1)
- Typical and Atypical DevelopmentDocumento43 pagineTypical and Atypical DevelopmentJosh PelayoNessuna valutazione finora
- Growth and Development of Newborn To InfancyDocumento54 pagineGrowth and Development of Newborn To Infancymerin sunilNessuna valutazione finora
- Childhood and Adolescence: Voyages in Development, 7e: Chapter 4: Birth and TheDocumento65 pagineChildhood and Adolescence: Voyages in Development, 7e: Chapter 4: Birth and TheNUR HUMAIRA ROSLINessuna valutazione finora
- Newborn NotesDocumento3 pagineNewborn NotesSharlotte EbayNessuna valutazione finora
- Handouts - Module 12Documento7 pagineHandouts - Module 12Kalliste HeartNessuna valutazione finora
- Newborn ScreeningDocumento23 pagineNewborn Screeningloglesb1Nessuna valutazione finora
- Primitive ReflexesDocumento11 paginePrimitive ReflexesFadriani NurdinNessuna valutazione finora
- Primitive Reflex Free GuideDocumento22 paginePrimitive Reflex Free Guideristeacristi100% (2)
- MCN Long Exam 4 1Documento7 pagineMCN Long Exam 4 1bianca molinaNessuna valutazione finora
- Reflexes and Stereotypies WebDocumento36 pagineReflexes and Stereotypies WebBillal HossenNessuna valutazione finora
- Module 12 of Child and Adolescence DevelopmentDocumento3 pagineModule 12 of Child and Adolescence DevelopmentMakki Andre Antonio75% (4)
- Anne Boyer My Common HeartDocumento37 pagineAnne Boyer My Common HeartFederica Bueti100% (2)
- Newborn AssessmentDocumento17 pagineNewborn Assessmentmarycris100% (2)
- A List of ReflexesDocumento2 pagineA List of ReflexesChristlee BersaminaNessuna valutazione finora
- Characteristics of NewbornDocumento28 pagineCharacteristics of NewbornChandu Raj100% (4)
- Approach To A Child With HemiplegiaDocumento5 pagineApproach To A Child With HemiplegiaBeenish IqbalNessuna valutazione finora
- NCP PostnatalDocumento37 pagineNCP PostnatalNadiya Rashid86% (7)
- Newborn ReflexesDocumento41 pagineNewborn ReflexesUmairah Bashir100% (5)
- Newborn RevDocumento14 pagineNewborn RevRuthangela GarciaNessuna valutazione finora
- Leader, Darian - Hands - What We Do With Them and Why-Penguin Books LTD (2016)Documento113 pagineLeader, Darian - Hands - What We Do With Them and Why-Penguin Books LTD (2016)Jorge RodriguezNessuna valutazione finora
- Characteristic of NewbornDocumento9 pagineCharacteristic of NewbornLALRINTLUANGI CHHAKCHHUAKNessuna valutazione finora
- Reflexes in NewbornDocumento7 pagineReflexes in NewbornRayan DakaNessuna valutazione finora
- NCM107 - Chapter 04-Lesson 3 Postpartal CareDocumento22 pagineNCM107 - Chapter 04-Lesson 3 Postpartal CareJosephine LoriaNessuna valutazione finora