Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Managing Mental Illness in Patients From CALD Backgrounds: Psychiatry
Caricato da
1234chocoTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Managing Mental Illness in Patients From CALD Backgrounds: Psychiatry
Caricato da
1234chocoCopyright:
Formati disponibili
Psychiatry CLINICAL PRACTICE
Managing mental illness
in patients from CALD
backgrounds
Litza A Kiropoulos, BEd-Sc, BSc (Hons) Psych, MClinPsych, PhD (Psych), is a Research Fellow,
Department of General Practice, Monash University, Victoria. litza.kiropoulos@med.monash.edu.au
Grant Blashki, MD, FRACGP, is Senior Research Fellow, Department of General Practice, Monash University, Victoria,
and Honorary Senior Lecturer, Health Services Research Department, Institute of Psychiatry, Kings College London.
Steven Klimidis, BSc (Hons) Psych, PhD (ClinPsych), is Associate Professor and Research Co-ordinator, Centre for
International Mental Health, University of Melbourne and Victorian Transcultural Psychiatry Unit, Victoria.
BACKGROUND
Australian general practitioners are often the first point of call for people seeking
mental health care including those from culturally and linguistically diverse (CALD)
backgrounds, some of whom may be more at risk of having a mental illness but are
failing to access the appropriate mental health care.
OBJECTIVE
This article is intended to assist GPs in the recognition, diagnosis and management
of mental illness in patients from CALD backgrounds by providing current research
evidence and presenting some practical recommendations. More attention is paid to the
larger CALD populations such as the southern European and Asian communities, and
does not deal with indigenous Australians.
DISCUSSION
There is an increasing call for GPs to have a key role in the detection, diagnosis and
management of mental illness, including for patients from CALD backgrounds. Effective
care requires that GPs are aware of, and understand how culture may influence
recognition, diagnosis and management of mental illness in this group of patients.
significant proportion of Australias
population consists of people from culturally
and linguistically diverse (CALD) backgrounds.
According to the Australian 2001 Census,
28% of the Australian population were born
overseas; 15% in a non-English speaking
country (Table 1). 1 Notably, older persons
from CALD are becoming a substantial
subgroup among the Australian population;
by 2026 it is projected that one in four
people aged 70 years and over will be from
a CALD background.2 These figures will have
significant implications for general practice
as general practitioners are often the first
point of contact for people requiring mental
health care. However, even though census
data has indicated that 15% of the Australian
population is from a CALD background, only
7% of encounters with GPs were recorded
for CALD people in a national survey of GP-
patient encounters. 3 These consultations
were less likely to involve a psychological
or social problem than patients from an
English speaking background.3 Research also
suggests that people from CALD backgrounds
often prefer to consult with GPs who are of
the same ethnic background or who speak
the same primary language as themselves.4
Research regarding differences in rates of
mental illness in CALD populations compared
with their Australian born counterparts has
been equivocal. The National Health and
Wellbeing Survey found little difference
in rates of affective and anxiety disorders
between people from CALD backgrounds
and Anglo-Australians 5 (although the study
excluded those who could not speak English
sufficiently well to complete the interviews).
However, more recent Australian studies
employing culturally sensitive research
methodology (ie. interview in participant's
own language) have shown that people from
CALD backgrounds have higher levels of
depression and anxiety than their AngloAustralian counterparts. 4,6 The discrepancy
between the low level of GP consultations
involving social and psychological problems
found in CALD populations, and higher
rates of mental illness noted in some
Reprinted from Australian Family Physician Vol. 34, No. 4, April 2005 4 259
Clinical practice: Managing mental illness in patients from CALD backgrounds
CALD populations, have been attributed
to a number of factors related to the
presentation of illness by the patient and
the underdetection, misdiagnosis and
management of mental illness by GPs.
What is culture?
Culture has been defined as a shared
learned behavior transmitted from one
generation to another for purposes of
individual and societal growth, adjustment
and adaptation.7 It is represented externally
as artefacts, roles, and institutions, and
internally as values, beliefs, attitudes and
biological functioning. 7 The term 'culture'
also refers to the shared heritage and social
distinctiveness of the multiplicity of the
ethnic components within a community.
However, it is important to note that it is
impossible to generalise characteristics of
a particular culture to all members of that
group, as not all members subscribe to the
values, beliefs or behaviours common to that
group and members have different levels of
acculturation to mainstream culture.8
Presentation, detection and
diagnosis of mental illness
The influence of culture
Mental illness in different cultures constitutes
different forms of social reality 9 and
needs to be understood within the cultural
context. Cultural factors shape mental illness
including how it is understood and explained,
its experience and manifestation, and its
course and epidemiology.10,11 Some factors
influenced by culture affecting the GP-patient
interaction include: somatisation, explanatory
models, perception of the GP by the
patient, the patients social context, stigma
associated with mental illness, language
difficulties, the GP setting, the role of family
and other social networks and expectations
of medication and religious beliefs.
Somatisation
Cultural variations have been noted in the
expression and presentation of mental
illness in general practice.12 Patients from
some CALD backgrounds who have a mental
illness may present more often to their
GP with somatic rather than psychological
symptoms. 1315 This has been termed
somatisation and can be understood as
a culturally appropriate way of expressing
discomfort in many cultures. 13,16,17 For
example, CALD patients might complain to a
GP of somatic symptoms such as insomnia,
headaches, lethargy, abdominal, muscular,
back and joint pains, rather than low mood
or negative thoughts.15,18
Explanatory models
Detection of mental illness in general
p r a c t i c e c a n b e i n f l u e n c e d by t h e
patients conceptualisation of the illness
experience or their explanatory model.19 An
explanatory model relates to the meaning
of illness, specifically, what constitutes
the views of causes, important symptoms,
course, consequences, and treatments or
remedies.20 All aspects of the explanatory
model are influenced and shaped by culture
and social factors such as socioeconomic
status and education, 21 and can influence
help seeking, compliance with treatment
and patient satisfaction.22
Cultural variation in explanatory models is
particularly relevant to causal attributions of
mental illness. For example, psychosomatic
causation is widely accepted by southern
Europeans for anxiety or depression. 23
Indeed, in much of Italian and Greek culture
nerves or nervous breakdowns are not
highly stigmatised but are viewed instead as
common, often minor, afflictions.23 The typical
treatment of nerves may include prayer,
efforts to adopt a better attitude or seek a
change in the social or physical environment.23
Additionally, causal beliefs about mental
illness in older people of southern European
cultures have included witchcraft, demonic
forces and supernatural explanations,
especially in females of low socioeconomic
status and low educational levels, and those
that migrated from rural areas.24 Therefore,
GP consultations with patients from CALD
backgrounds may require a negotiation of
explanatory models where differences in
belief systems are acknowledged and
260 3Reprinted from Australian Family Physician Vol. 34, No. 4, April 2005
Table 1. Australian 2001 census data:
birthplace by country for NESB*
Country
% NESB
population
Italy
1.15
Vietnam
0.82
China
0.70
Greece
0.61
Germany
0.57
Philippines
0.55
India
0.50
Netherlands
0.44
Malaysia
0.41
Lebanon
0.38
Poland
0.30
Yugoslavia
0.29
Sri Lanka
0.28
Croatia
0.27
Indonesia
0.25
Malta
0.24
Fiji
0.23
FYROM**
0.23
Republic of South Korea
0.20
Singapore
0.18
Egypt
0.17
Turkey
0.16
France
0.09
Born elsewhere overseas*** 3.70
* non-English speaking background
** Former Yugoslav Republic of Macedonia
*** born elsewhere overseas (includes
inadequately described, at sea, not elsewhere
classified)
respected. Questions around the patients
view of mental illness will elicit information
about their explanatory model. Table 2
provides questions that can be used by GPs
to elicit CALD patients explanatory models
based on Kleinmans20 original concepts of
health and sickness and the Short Explanatory
Model Interview (SEMI).25
Perception of the GP
Patients from CALD backgrounds may have
different expectations, concerns, meanings
and values about GPs, and may view the GP as
the expert on physical illness. They may think
their role as patient is to present and describe
their physical illness; in part this may explain
the high rate of somatic presentations to GPs.
Clinical practice: Managing mental illness in patients from CALD backgrounds
It may also explain why emotional, social and
psychological difficulties are less often reported
to a GP, as the problem may not be considered
relevant or appropriate to report to a GP.20,26
Some studies suggest that different
communication styles in patients from
CALD backgrounds may be characterised
by a less direct and assertive manner. 27
This may explain why patients sometimes
readily agree with the treatment plan (in
order to please the physician) but do not
comply. Other studies suggest that patients
from CALD backgrounds may expect a
more authoritarian GP in the patient-doctor
relationship, often resulting in passive
acceptance of treatment and low demand
for education about medication.28
Patients social context
Mental illness may be strongly influenced
by adverse social circumstances and may
alert the GP to the possibility of a mental
illness.29,30 For example, factors affecting the
clinical presentation may include the political
context of arrival, reasons for migration (eg.
refugee, economic), level of contact with the
Table 2. Eliciting explanatory models of illness in CALD patients
Nature and causes of the problem
When did you first notice that there was a problem?
Why do you think that the problem began when it did?
What do you call this problem? What is its name?
How long ago did you first notice these problems?
What do you think caused this problem?
Do you think that this problem is an illness?
Australian majority group, level of exposure to
high risk industries, and lower postmigration
employment status relative to education.
Recent adverse life events (>1 in the past
year) could be seen as a reliable indicator of
mental illness in CALD patients, in addition
to multiple visits to the GP (>10 visits per
year). Therefore, those patients from CALD
backgrounds who have had recent adverse
life events or who attend the GP frequently,
warrant particular attention regarding their
psychological wellbeing.
Patients from CALD backgrounds are also
more likely to present to the GP at a later stage
of their mental illness, tolerating a great deal
of emotional and psychological distress before
seeking professional assistance.13 Patients may
consult a GP after having consulted a number
of other culturally appropriate healers, or may
be using other culturally sanctioned remedies
and rituals for their mental health.13
Stigma
Important symptoms of the problem
What do you think are the most troublesome aspects of this problem?
Which symptoms trouble you most?
Development and course of problem
How did the problem develop with time up to now?
How do you think this problem may develop and progress over time in the future?
Do you think the condition would become worse, improve or stay the same, or come
and go over time?
Severity and consequences of the problem
How serious do you think this problem is?
What are the most and least troublesome aspects of the problem?
What are the main difficulties your problem has caused you? How does the problem
affect your relationships, work/study, family role and responsibilities, attending to
your daily needs?
Treatment and help seeking for problem
Is there a particular way that people in your culture/ethnic group deal with this type
of problem? What is usually done?
Is this relevant to do in your case?
What do you think will be effective to help with this problem in your case?
What do you think you can do to help with this problem?
How do you think I can help with this problem?
(If medicine is asked for) Do you think the medicine will cure the problem or just help
control it? How quickly do you expect the medicine to do this?
The stigma associated with having a mental
illness may be particularly strong in some
CALD populations and this affects symptom
disclosure and help seeking behaviour. This may
be one of the explanations for presentation with
somatic symptoms as these may be viewed
as more socially benign than a psychological
problem.31,32 Depressive symptoms may be
seen as socially disadvantageous, and in some
cultures may interfere with marriage prospects,
diminish social status, and compromise the
self esteem required to perform effectively in
society.31,32
Language difficulties
Language preferences affect selection of GPs
by people from CALD backgrounds with
recent surveys showing that 39.5% of nonEnglish speaking patient consultations were
where the GP consulted in a language other
than English,3 and 78% of CALD patients
with poor English proficiency attended
bilingual GPs.4 For nonbilingual GPs, a trained
interpreter should be used to ensure a
meaning orientated translation. Interpreters
are available through the Translating and
Interpreting Service (www.immi.gov.au/tis/) or
Reprinted from Australian Family Physician Vol. 34, No. 4, April 2005 4 261
Clinical practice: Managing mental illness in patients from CALD backgrounds
VITS (www.vits.com.au/services/interpreting.
htm). Using an interpreter will help avoid
mistranslations of biomedical concepts and
errors of omission. An interpreter is preferred
over a family member as the patient may
not want to disclose information in front of
family and/or the family member may add
their own interpretations.
General practice setting
Underdetection of mental illness in general
practice is a complex issue that may be
exacerbated by difficulties in eliciting a
psychiatric history from CALD patients.33 For
example, GPs have been shown to diagnose
CALD patients using more limited indicators of
depression (ie. depressed appearance, sleep
disturbance, weight and appetite changes)
and are more likely to detect more severe
mental illness in general practice.33 Therefore
GPs need to be alert to the early signs of
emotional difficulties in CALD patients.
Role of family and friends
In many cultures, family members and close
friends play a key role in the patients health
care and often accompany the patient,
especially if they have limited English skills.
The GP needs to make sure that the patient
has explicitly given permission for any
discussions that might violate the patients
confidentiality. Where strong collectivistic
values typify the culture, the GP should be
aware that they may be negotiating treatment
with the entire family even if they are not
present. Acknowledging the importance of
other family members and accommodating
their views of the treatment is often essential
to adherence to the treatment plan.
Pharmacological management
N o n c o m p l i a n c e w i t h p s y ch o t r o p i c
medications appears to be more problematic
and prevalent in some nonwestern
cultures. 34 In recent years, research has
found significant differences among ethnic
groups in their response and propensity
to side effects of medications related to
genotypic variations in drug metabolising
isoenzymes. 3537 These differences lead to
variability in pharmacokinetics (ie. absorption,
distribution, metabolism and excretion) and
pharmacodynamics (ie. drug response to
psychotropic agents).38 Metabolism is regarded
as the most significant factor in determining
inter-individual and inter-ethnic differences.39,40
While a detailed description of these
differences is beyond the scope of this article,
GPs should consider variable metabolism
between ethnic groups before prescribing
psychotropics such as antidepressants,
benzodiazepines or antipsychotic medications.
Expectations of medications
Expectations of drug effects are strongly
influenced by a patients cultural origin. For
example, in some studies, patients from a
CALD background are more likely to have
negative attitudes toward medications and to
have poorer medication adherence.34 In some
studies, Chinese patients commonly perceived
that western medicines were more potent and
had greater adverse side effects than herbal
or traditional therapies.41 In another study
examining the side effects of lithium in Chinese
patients, although the actual side effect profile
was similar to caucasians, Chinese patients
showed more concern about fatigue and
drowsiness and were less concerned about
polydipsia and polyuria as such side effects
were regarded as a way of removing toxins
from the body.28 A further study found that
even though Chinese patients expected
western medicines to act quickly, they did not
expect them to treat the underlying condition.42
Religious beliefs
Religious beliefs may also affect compliance
with medication in people from CALD
backgrounds. For example, changes in intake
time and dosing of medication by some Muslim
patients during Ramadan have been found,
often without seeking GP advice.43 As efficacy
and toxicity of psychotropic medications can
vary depending on the time of administration
and their interaction with food intake, GPs
must consider religious beliefs when advising
patients. This is even more relevant for drugs
with a narrow therapeutic index as the risk of
toxicity or side effects are higher.43
262 3Reprinted from Australian Family Physician Vol. 34, No. 4, April 2005
Referral
General practitioners are the most common
referral source to specialist mental health
services for people experiencing a mental
illness and studies suggest that people from
CALD backgrounds are accessing specialist
mental health services at a lower rate compared
to the Australian born population.4 General
practitioners should familiarise themselves with
bilingual mental health professionals and ethnospecific services where they can refer CALD
patients or receive specific advice regarding
assessment and treatment.
Conclusion
General practitioners play a key role in the
detection, diagnosis and management of
CALD patients with mental illness, although
more research is clearly needed. Effective
care requires understanding and awareness
of how culture may affect the patient, GP, and
setting factors. The complex task of managing
mental illness in CALD populations can be
made easier by better understanding of the
patients culture, social and family context,
their explanatory models, their perception of
the GP, and the stigma associated with mental
illness. Additionally, GPs need to be aware of
factors contributing to the variable metabolism
of medications across CALD groups.
Summary of important points
Negotiate explanatory models with
your patient.
Be aware of the stigma that mental
illness may carry in some cultures.
Use interpreters to facilitate the GPpatient interaction.
Involvement of family and friends may
facilitate the GP-patient consultation
and treatment compliance.
Pharmacological effects may differ in
patients from CALD backgrounds.
Conflict of interest: none declared.
References
1.
2.
National Census of Population and Housing Data 2001.
Basic community profile, Australia. Canberra: Australian
Bureau of Statistics, 2001. (ABS Catalogue No. 2001.0).
Gibson D, Braun P, Benham C, Mason F. Projections of
older immigrants: people from culturally and linguistically
diverse backgrounds, 19962026. Canberra: Australian
Clinical practice: Managing mental illness in patients from CALD backgrounds
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
Institute of Health and Welfare, 2001.
Knox SA, Britt H. A comparison of general practice
encounters with patients from English speaking and
non-English speaking backgrounds. Med J Aust
2002;177:98101.
Stuart GW, Klimidis S, Minas IH. The treated prevalence of mental disorder amongst immigrants and the
Australian born: community and primary care rates. Int J
Soc Psychiatry 1998;44:2234.
McLennan W. Mental health and wellbeing: profile of
adults, Australia, 1997. Canberra: Australian Bureau of
Statistics, 1998. (ABS Catalogue No: 4326.0).
Kiropoulos LA, Klimidis S, Minas IH. Depression and
anxiety: a comparison of older aged Greek born immigrants and Anglo Australians in Melbourne. Aust NZ J
Psychiatry 2004;38:71424.
Marsella AJ. Cross-cultural research on severe mental
disorders: issues and findings. Acta Psychiatr Scand
1988;78:722.
Rosenthal D, Ranieri N, Klimidis S. Vietnamese adolescents in Australia: relationships between perceptions of
self and parental values, intergenerational conflict, and
gender dissatisfaction. Int J Psychology 1996;31:8191.
Good B, Kleinman A. Culture and depression: studies in
the anthropology and cross-cultural psychiatry of affect
and disorder. Berkeley: University of California Press,
1985.
Kirmayer LJ. Cultural variations in the clinical presentation of depression and anxiety: implications for diagnosis
and treatment. J Clin Psychiatry 2001;62:228.
Marsella AJ, Kaplan A, Suarez E. Cultural considerations
for understanding, assessing and treating depressive experience and disorder. In: Reinecke MA, Davison MR,
editors. Comparative treatments of depression. New York,
NY: Springer, 2000.
Bhui K, Bhugra D, Goldberg D. Causal explanations of
distress and general practitioners assessments of common
mental disorders among Punjabi and English attendees.
Soc Psychiatry Psychiatr Epidemiol 2002;37:3845.
Chan B, Parker G. Some recommendations to assess
depression in Chinese people in Australasia. Aust NZ J
Psychiatry 2004;38:1417.
Gater R, De Almeida e Sousa B, Barrientos G, et al.
The pathways to psychiatric care: a cross-cultural study.
Psychol Med 1991;21:76174.
Husain N, Creed F, Tomenson B. Adverse social circumstances and depression in people of Pakistani origin in the
UK. Br J Psychiatry 1997;171:4348.
Gureje O, Simon GE, Ustun TB, Goldberg DP.
Somatisation in cross-cultural perspective: a world health
organisation study in primary care. Am J Psychiatry
1997;154:98995.
Comino EJ, Silove D, Manicavasagar V, Harris E, Harris
MF. Agreement in symptoms of anxiety and depression
between patients and the GPs: the influence of ethnicity.
Fam Pract 2001;18:717.
Phan T, Silove D. The influence of culture on psychiatric assessment: the Vietnamese refugee. Psychiatr Serv
1997;48:8690.
Bhui K, Bhugra D. Explanatory models for mental distress: implications for clinical practice and research. Br J
Psychiatry 2002;181:67.
Kleinman A. Patients and healers in the context of culture.
Berkeley: University of California Press, 1980.
Carillo JEA, Green AR, Betancourt JR. Cross-cultural
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
primary care: a patient based approach. Ann Intern Med
1999;30:82934.
Jacob KS, Bhugra D, Lloyd KR. Common mental disorders, explanatory models and consultation behaviour
among Indian women living in the UK. J R Soc Med
1998;91:6671.
Kirmayer LJ, Young A, Robbins JM. Symptom attribution
in cultural perspective. Can J Psychiatry 1994;39:58495.
Meiser B, Gurr R. Non-English speaking persons perceptions of mental illness and associated needs: an explanatory
study of Arabic-, Greek- and Italian-speaking communities in New South Wales. Health Promotion Journal of
Australia 1996;6:449.
Lloyd KR, Jacob KS, Patel V, St Louis L, Bhugra D,
Mann AH. The development of the Short Explanatory
Model Interview (SEMI) and its use among primary care
attenders with common mental disorders. Psychol Med
1998;28:12317.
Parker G, Gladstone G, Chee KT. Depression in the
planets largest ethnic group: the Chinese. Am J Psychiatry
2001;158:85764.
Gao G, Ting-Toomey S, Gudykunst WB. Chinese
communication processes. In: Bond MH, editor. The
handbook of Chinese psychology. Hong Kong: Oxford
University Press, 1996;28093.
Lee S. Side effects of chronic lithium therapy in Hong
Kong Chinese: an ethnopsychiatric perspective. Cult Med
Psychiatry 1993;17:30120.
Odell SM, Surtees PG, Wainwright NWJ, Commander
MJ, Sashidharan SP. Determinants of general practitioner
recognition of psychological problems on a multi-ethnic
inner-city health district. Br J Psychiatry 1997;171:537
41.
Maginn S, Boardman AP, Craig TKJ, Hadad M, Heath
G, Stott J. The detection of psychological problems by
general practitioners: influence of ethnicity and other
demographic variables. Soc Psychiatry Psychiatr Epidemiol
2004;39:46471.
Bakshi L, Rooney R, ONeill K. Working transculturally
to reduce the stigma surrounding mental illness amongst
non-English speaking background communities: a guide.
Melbourne: Australian Transcultural Mental Health
Network, 1999.
Raguram R, Weiss MG, Channabasavanna SM, Devins
GM. Stigma, depression and somatization in South India.
Am J Psychiatry 1996;153:10439.
Mihalopoulos C, Pirkis J, Naccarella L, Dunt D. The role
of general practitioners and other primary care agencies in
transcultural mental health care. Melbourne: Australian
Transcultural Mental Health Network, 1999.
Li KM, Poland RE, Nakasaki G. Psychopharmacology
and psychobiology of ethnicity. Washington, DC:
American Psychiatric Press, 1993.
Ng C-H, Schweitzer I, Norman T, Easteal S. The emerging role of pharmacogenetics: implications for clinical
psychiatry. Aust NZ J Psychiatry 2004;38:4839.
Matthews HW. Racial, ethnic and gender differences
in response to medicines. Drug Metabol Drug Interact
1995;12:7791.
Pi EH, Gray GE. A cross-cultural perspective on psychopharmacology. Essential Psychopharmacol
1998;2:23359.
Lin K-M. Biological differences in depression and
anxiety across races and ethnic groups. J Clin Psychiatry
2001;62:1319.
39. Sjoqvist F, Borga O, Dahl M-L, Orme MLE.
Fundamentals of clinical pharmacology. In: Speight TM,
Holford NHG, editors. Averys Drug Treatment. 4th ed.
Auckland: Adis International, 1997;173.
40. Poolsup N, Li Wan Po A, Knight TL. Pharmacogenetics
and psychopharmacotherapy. J Clin Phar Ther
2000;25:197220.
41. Lee RP. Perceptions and uses of Chinese medicine
among the Chinese in Hong Kong. Cult Med Psychiatry
1980;4:34575.
42. Owan TC. Southeast Asian mental health: Treatment,
prevention, services, training, and research. Rockville,
MD: National Institute of Mental Health, 1985.
43. Aadil N, Houti IE, Moussamih S. Drug intake during
Ramadan. BMJ 2004;329:77882.
AFP
Correspondence
Email: afp@racgp.org.au
Reprinted from Australian Family Physician Vol. 34, No. 4, April 2005 4 263
Potrebbero piacerti anche
- Mental Health, Intellectual and Developmental Disabilities and the Ageing ProcessDa EverandMental Health, Intellectual and Developmental Disabilities and the Ageing ProcessNessuna valutazione finora
- Outsmart Your Brain The Insider's Guide to Life-Long MemoryDa EverandOutsmart Your Brain The Insider's Guide to Life-Long MemoryNessuna valutazione finora
- A Framework for the Holistic Management of SchizophreniaDa EverandA Framework for the Holistic Management of SchizophreniaNessuna valutazione finora
- The Health Improvement Profile: A manual to promote physical wellbeing in people with severe mental illnessDa EverandThe Health Improvement Profile: A manual to promote physical wellbeing in people with severe mental illnessNessuna valutazione finora
- 0408PP TrujilloDocumento15 pagine0408PP TrujillojaverianaNessuna valutazione finora
- Living with Bipolar: A Guide to Understanding and Managing the DisorderDa EverandLiving with Bipolar: A Guide to Understanding and Managing the DisorderValutazione: 2 su 5 stelle2/5 (1)
- Epidemiology for Canadian Students: Principles, Methods and Critical AppraisalDa EverandEpidemiology for Canadian Students: Principles, Methods and Critical AppraisalValutazione: 1 su 5 stelle1/5 (1)
- Eugenics as a Factor in the Prevention of Mental DiseaseDa EverandEugenics as a Factor in the Prevention of Mental DiseaseNessuna valutazione finora
- The Health Improvement Profile: A manual to promote physical wellbeing in people with severe mental illnessDa EverandThe Health Improvement Profile: A manual to promote physical wellbeing in people with severe mental illnessNessuna valutazione finora
- Breaking the Silence: Shining a Light on Schizoid Personality DisorderDa EverandBreaking the Silence: Shining a Light on Schizoid Personality DisorderNessuna valutazione finora
- Clinician's Guide to Chronic Disease Management of Long Term Conditions, TheDa EverandClinician's Guide to Chronic Disease Management of Long Term Conditions, TheNessuna valutazione finora
- Research Paper Topics On Mental IllnessDocumento6 pagineResearch Paper Topics On Mental Illnesszufehil0l0s2100% (3)
- Nourishing Minds: The Interplay of Eating and Mental HealthDa EverandNourishing Minds: The Interplay of Eating and Mental HealthNessuna valutazione finora
- Cultural Competency in Health PDFDocumento6 pagineCultural Competency in Health PDFMikaela HomukNessuna valutazione finora
- Healing Across Cultures: Pathways to Indigenius Health EquityDa EverandHealing Across Cultures: Pathways to Indigenius Health EquityNessuna valutazione finora
- Fatigue and Dysautonomia: Chronic or Persistent, What's the Difference?Da EverandFatigue and Dysautonomia: Chronic or Persistent, What's the Difference?Nessuna valutazione finora
- Counseling From Within: The Microbiome Mental Health ConnectionDa EverandCounseling From Within: The Microbiome Mental Health ConnectionNessuna valutazione finora
- Killer Diseases, Modern-Day Epidemics: Keys to Stopping Heart Disease, Diabetes, Cancer, and Obesity in Their TracksDa EverandKiller Diseases, Modern-Day Epidemics: Keys to Stopping Heart Disease, Diabetes, Cancer, and Obesity in Their TracksNessuna valutazione finora
- Oppositional Defiant Disorder and Conduct Disorder in ChildrenDa EverandOppositional Defiant Disorder and Conduct Disorder in ChildrenNessuna valutazione finora
- Mental Health Guide: For students, teachers, school psychologists, nurses, social workers, counselors and parents.Da EverandMental Health Guide: For students, teachers, school psychologists, nurses, social workers, counselors and parents.Nessuna valutazione finora
- Chronic Disease and Disability: A Social Worker's GuideDa EverandChronic Disease and Disability: A Social Worker's GuideNessuna valutazione finora
- Social Aspects of The Quality of Life of Persons Suffering From SchizophreniaDocumento11 pagineSocial Aspects of The Quality of Life of Persons Suffering From SchizophreniaFathur RNessuna valutazione finora
- Different Cultures, Similar Struggles: Understanding ADHD in Ethnic CommunitiesDa EverandDifferent Cultures, Similar Struggles: Understanding ADHD in Ethnic CommunitiesNessuna valutazione finora
- The Unraveling Mind: A Guide to Understanding PsychosisDa EverandThe Unraveling Mind: A Guide to Understanding PsychosisNessuna valutazione finora
- Mental health and psicological disturb: What they are and how they workDa EverandMental health and psicological disturb: What they are and how they workNessuna valutazione finora
- Nutritional and Herbal Therapies for Children and Adolescents: A Handbook for Mental Health CliniciansDa EverandNutritional and Herbal Therapies for Children and Adolescents: A Handbook for Mental Health CliniciansNessuna valutazione finora
- Kleinman Culture and DepressionDocumento3 pagineKleinman Culture and DepressionАлександра Курленкова100% (1)
- Understanding Psychological AbnormalityDocumento21 pagineUnderstanding Psychological AbnormalityTitikshaNessuna valutazione finora
- Cholestasis Demystified: Doctor’s Secret GuideDa EverandCholestasis Demystified: Doctor’s Secret GuideNessuna valutazione finora
- Troubled Minds: understanding and treating mental illnessDa EverandTroubled Minds: understanding and treating mental illnessNessuna valutazione finora
- Psychology Assessment - I - M1Documento42 paginePsychology Assessment - I - M1Brinda ChughNessuna valutazione finora
- My Health, My Faith, My Culture: A guide for healthcare practitionersDa EverandMy Health, My Faith, My Culture: A guide for healthcare practitionersNessuna valutazione finora
- Research Paper Mental HealthDocumento5 pagineResearch Paper Mental Healthc9s9h7r7100% (1)
- Depression - Let's TalkDocumento9 pagineDepression - Let's TalkThavam RatnaNessuna valutazione finora
- Understanding Autism Spectrum Disorder: A Book That Every Parent and Teacher Should HaveDa EverandUnderstanding Autism Spectrum Disorder: A Book That Every Parent and Teacher Should HaveNessuna valutazione finora
- The Clinician's Guide to Treating Health Anxiety: Diagnosis, Mechanisms, and Effective TreatmentDa EverandThe Clinician's Guide to Treating Health Anxiety: Diagnosis, Mechanisms, and Effective TreatmentErik Hedman-LagerlöfNessuna valutazione finora
- Gale Researcher Guide for: Clinical and Abnormal PsychologyDa EverandGale Researcher Guide for: Clinical and Abnormal PsychologyNessuna valutazione finora
- Understanding the Many: Navigating Dissociative Identity DisorderDa EverandUnderstanding the Many: Navigating Dissociative Identity DisorderNessuna valutazione finora
- Integrative Medicine for Vulnerable Populations: A Clinical Guide to Working with Chronic and Comorbid Medical Disease, Mental Illness, and AddictionDa EverandIntegrative Medicine for Vulnerable Populations: A Clinical Guide to Working with Chronic and Comorbid Medical Disease, Mental Illness, and AddictionNessuna valutazione finora
- Student'S Having Anxiety & DepressionDocumento10 pagineStudent'S Having Anxiety & DepressionAmie TabiNessuna valutazione finora
- Psychology and Aging: PsychologistsDocumento8 paginePsychology and Aging: PsychologistsThamer SamhaNessuna valutazione finora
- Debat Kel. FitrahDocumento17 pagineDebat Kel. FitrahnurisNessuna valutazione finora
- Experiences of Adolescents Living with Type 1 Diabetes Mellitus Whilst Negotiating with the SocietyDa EverandExperiences of Adolescents Living with Type 1 Diabetes Mellitus Whilst Negotiating with the SocietyNessuna valutazione finora
- A Short Guide To Psychiatric DiagnosisDocumento4 pagineA Short Guide To Psychiatric DiagnosisNaceiraNessuna valutazione finora
- Fairy Tail - Main ThemeDocumento3 pagineFairy Tail - Main Theme1234chocoNessuna valutazione finora
- Code Geass - StoriesDocumento5 pagineCode Geass - Stories1234chocoNessuna valutazione finora
- Mbs Quick Guide: JULY 2020Documento2 pagineMbs Quick Guide: JULY 20201234chocoNessuna valutazione finora
- Topical Steroids (Sep 19) PDFDocumento7 pagineTopical Steroids (Sep 19) PDF1234chocoNessuna valutazione finora
- Doctor Talk: Communication Practice Role PlaysDocumento6 pagineDoctor Talk: Communication Practice Role Plays1234chocoNessuna valutazione finora
- Blue BirdDocumento7 pagineBlue Bird1234chocoNessuna valutazione finora
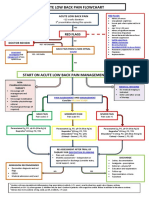
- Acute Low Back Pain Flowchart January 2017Documento1 paginaAcute Low Back Pain Flowchart January 20171234chocoNessuna valutazione finora
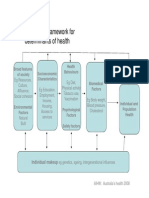
- A Conceptual Framework For HealthDocumento1 paginaA Conceptual Framework For Health1234chocoNessuna valutazione finora
- PBM Module1 MTP Template 0Documento2 paginePBM Module1 MTP Template 01234chocoNessuna valutazione finora
- Language of PreventionDocumento9 pagineLanguage of Prevention1234chocoNessuna valutazione finora
- Blue Card Declaration PDFDocumento1 paginaBlue Card Declaration PDF1234chocoNessuna valutazione finora
- Taking A Social and Cultural HistoryDocumento3 pagineTaking A Social and Cultural History1234chocoNessuna valutazione finora
- Preoperative AssessmentDocumento9 paginePreoperative Assessment1234chocoNessuna valutazione finora
- Acute Post-Op Pain ManagementDocumento4 pagineAcute Post-Op Pain Management1234chocoNessuna valutazione finora
- Prenatal Screening Test (AUS) PDFDocumento24 paginePrenatal Screening Test (AUS) PDFshirley_ling_15Nessuna valutazione finora
- Barrett's Esophagus: Identifying The Squamocolumnar (SC) and Gastroesophageal (GE) Junctions EndoscopicallyDocumento10 pagineBarrett's Esophagus: Identifying The Squamocolumnar (SC) and Gastroesophageal (GE) Junctions Endoscopically1234chocoNessuna valutazione finora
- Facilities Strategic Asset Management Plan TemplateDocumento85 pagineFacilities Strategic Asset Management Plan Templateoli mohamedNessuna valutazione finora
- Honey ProcessingDocumento5 pagineHoney Processingvenkatrao_gvNessuna valutazione finora
- Group 1 Reviewer Social LegislationDocumento5 pagineGroup 1 Reviewer Social Legislationxsar_xNessuna valutazione finora
- SPE-199498-MS Reuse of Produced Water in The Oil and Gas IndustryDocumento10 pagineSPE-199498-MS Reuse of Produced Water in The Oil and Gas Industry叶芊Nessuna valutazione finora
- University of Engineering & Management, Jaipur: (A) Production (B) Quality (C) Product Planning (D) All of The AboveDocumento4 pagineUniversity of Engineering & Management, Jaipur: (A) Production (B) Quality (C) Product Planning (D) All of The AboveSupriyo BiswasNessuna valutazione finora
- Surat Textile MillsDocumento3 pagineSurat Textile MillsShyam J VyasNessuna valutazione finora
- E F Eng l1 l2 Si 011Documento2 pagineE F Eng l1 l2 Si 011Simona ButeNessuna valutazione finora
- 6977 - Read and Answer The WorksheetDocumento1 pagina6977 - Read and Answer The Worksheetmohamad aliNessuna valutazione finora
- Posthumanism Cyborgs and Interconnected Bodies by Jon BaileyDocumento59 paginePosthumanism Cyborgs and Interconnected Bodies by Jon BaileyDavid García MonteroNessuna valutazione finora
- WIKADocumento10 pagineWIKAPatnubay B TiamsonNessuna valutazione finora
- Lunch Hour Meetings: Kiwanis Mission:: - Officers & Directors, 2018-2019Documento2 pagineLunch Hour Meetings: Kiwanis Mission:: - Officers & Directors, 2018-2019Kiwanis Club of WaycrossNessuna valutazione finora
- Task Performance Valeros Roeul GDocumento6 pagineTask Performance Valeros Roeul GAnthony Gili100% (3)
- COSL Brochure 2023Documento18 pagineCOSL Brochure 2023DaniloNessuna valutazione finora
- Modul9 VPNDocumento34 pagineModul9 VPNDadang AbdurochmanNessuna valutazione finora
- United States Court of Appeals, Third CircuitDocumento8 pagineUnited States Court of Appeals, Third CircuitScribd Government DocsNessuna valutazione finora
- Anglicisms in TranslationDocumento63 pagineAnglicisms in TranslationZhuka GumbaridzeNessuna valutazione finora
- God's Word in Holy Citadel New Jerusalem" Monastery, Glodeni - Romania, Redactor Note. Translated by I.ADocumento6 pagineGod's Word in Holy Citadel New Jerusalem" Monastery, Glodeni - Romania, Redactor Note. Translated by I.Abillydean_enNessuna valutazione finora
- Operations Management Final Exam Solutions CourseraDocumento2 pagineOperations Management Final Exam Solutions Courseratheswingineer0% (5)
- Jesus Hold My Hand EbDocumento2 pagineJesus Hold My Hand EbGregg100% (3)
- Accountancy Service Requirements of Micro, Small, and Medium Enterprises in The PhilippinesDocumento10 pagineAccountancy Service Requirements of Micro, Small, and Medium Enterprises in The PhilippinesJEROME ORILLOSANessuna valutazione finora
- Company Profile RadioDocumento8 pagineCompany Profile RadioselviNessuna valutazione finora
- Listening Fill in The Gaps and ExercisesDocumento4 pagineListening Fill in The Gaps and ExercisesAdriano CamargoNessuna valutazione finora
- Industrial Cpmplus Enterprise Connectivity Collaborative Production ManagementDocumento8 pagineIndustrial Cpmplus Enterprise Connectivity Collaborative Production ManagementEng Ahmad Bk AlbakheetNessuna valutazione finora
- RulesDocumento508 pagineRulesGiovanni MonteiroNessuna valutazione finora
- 61 Point MeditationDocumento16 pagine61 Point MeditationVarshaSutrave100% (1)
- 1 Intro To Society, Community and EducationDocumento29 pagine1 Intro To Society, Community and EducationMaria Michelle A. Helar100% (1)
- Explained - How To Read Q1 GDP Data - Explained News, The Indian ExpressDocumento11 pagineExplained - How To Read Q1 GDP Data - Explained News, The Indian ExpresshabeebNessuna valutazione finora
- Surge Protectionfor ACMachineryDocumento8 pagineSurge Protectionfor ACMachineryvyroreiNessuna valutazione finora
- Research On Goat Nutrition and Management in Mediterranean Middle East and Adjacent Arab Countries IDocumento20 pagineResearch On Goat Nutrition and Management in Mediterranean Middle East and Adjacent Arab Countries IDebraj DattaNessuna valutazione finora
- Kangaroo High Build Zinc Phosphate PrimerDocumento2 pagineKangaroo High Build Zinc Phosphate PrimerChoice OrganoNessuna valutazione finora