Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
06819211
Caricato da
sreenathreddyCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
06819211
Caricato da
sreenathreddyCopyright:
Formati disponibili
IEEE Transactions on Ultrasonics, Ferroelectrics, and Frequency Control ,
vol. 61, no. 6,
June
2014
955
Discrimination of Breast Microcalcifications
Using a Strain-Compounding Technique
with Ultrasound Speckle Factor Imaging
Yin-Yin Liao, Chia-Hui Li, Po-Hsiang Tsui, Chien-Cheng Chang, Wen-Hung Kuo, King-Jen Chang,
and Chih-Kuang Yeh, Senior Member, IEEE
AbstractThe usefulness of breast ultrasound could be extended by improving the detection of microcalcifications by
being able to detect and enhance microcalcifications while simultaneously eliminating hyperechoic spots (e.g., speckle noise
and fibrocystic changes) that can be mistaken for microcalcifications (i.e., false microcalcifications). This study investigated
the use of a strain-compounding technique with speckle factor
(SF) imaging to analyze the degree of scatterer redistributions in breast tissues under strain conditions for identifying
microcalcifications and false microcalcifications. The efficacy
of the proposed method was tested by collecting raw data of
ultrasound backscattered signals from 26 lesions at BI-RADS
category 4 or 5 with suspicious microcalcifications. The different strain conditions were created by applying manual compression to deform the breast lesion. For each region in which
microcalcifications were suspected, estimates of the SNR of
the strain-compounding B-scan images and estimates of the
mean SF (SFavg) in the strain-compounding SF images were
calculated. Compared with microcalcifications, the severity
of speckle of the false microcalcifications would be easily degraded under compressive strain conditions. The results demonstrated that the SNR estimates in the strain-compounding
B-scan images for microcalcifications and false microcalcifications were 5.22 1.04 (mean standard deviation) and 4.62
1.09, respectively; the corresponding SFavg estimates in the
strain-compounding SF images were 0.47 0.10 and 0.22
0.10 (p < 0.01). The mean area under the receiver operating
characteristic curve using the SNR estimate was 0.71, whereas
that using the SFavg estimate was 0.94. These findings indicate
that the strain-compounding SF imaging method is more effective at discriminating between microcalcifications and false
microcalcifications.
I. Introduction
icrocalcifications are tiny deposits of calcium
oxalate or calcium hydroxyapatite within the breast
Manuscript received December 25, 2013; accepted March 25, 2014.
The authors acknowledge the National Science Council of Taiwan (grant
101-2221-E-007-035-MY3) and the National Tsing Hua University
(grants 102N2046E1 and 102N2745E1) for their support.
Y.-Y. Liao, C.-H. Li, and C.-K. Yeh are with the Department of Biomedical Engineering and Environmental Sciences, National Tsing Hua
University, Hsinchu, Taiwan (e-mail: ckyeh@mx.nthu.edu.tw).
P.-H. Tsui is with the Department of Medical Imaging and Radiological Sciences, College of Medicine, Chang Gung University, Taoyuan,
Taiwan, and the Institute for Radiological Research, Chang Gung University, Taoyuan, Taiwan.
C.-C. Chang is with the Institute of Applied Mechanics, National Taiwan University, Taipei, Taiwan.
W.-H. Kuo and K.-J. Chang are with the Department of Surgery,
National Taiwan University Hospital, Taipei, Taiwan.
K.-J. Chang is also with the Department of Surgery, Cheng Ching
General Hospital, Taichung, Taiwan.
DOI http://dx.doi.org/10.1109/TUFFC.2014.2991
08853010
tissue that constitute the main diagnostic feature in early
breast cancers [1]. Mammography has a high sensitivity
but a low specificity for detecting breast microcalcifications [2]. Mammographically detected clustered microcalcifications have a size of about 100m or greater [3]. The
dense breast tissues, and especially in younger women,
cause suspicious regions to be almost invisible, and yield
a misdiagnosis rate for detection of breast cancers as high
as 15% to 25% [4]. In addition, dense tissues can easily be
misinterpreted as microcalcifications [5], [6]. Although the
scanning resolution of ultrasound imaging is lower than
the that of mammography, the use of mammography is
often complemented with ultrasound because ultrasound
can penetrate dense tissues to detect microcalcifications,
and thereby identify early breast cancers within dense
breasts [7][9].
However, the rates of false-negative and false-positive
results have been high when using ultrasound to detect
microcalcifications [10]. It is known that the amplitude
reflection coefficient of microcalcifications in tissue is close
to 0.9, and they frequently manifest as a bright point reflector in ultrasound B-scan images [10]. There is a limit to the physical size of microcalcifications detected by
ultrasound which is dependent on the spatial resolution
of ultrasound imaging. Microcalcification visualization is
also influenced by many factors, including speckle patterns
and display parameters [10][12]. Moreover, speckle noise
or some types of anatomical structures such as Coopers
ligaments or fibrocystic changes could be mistaken for microcalcifications, because they usually cause hyperechoic
signals with shadowing effects [13][16]. Several investigations have described these false-positive microcalcification signals as false microcalcifications. To eliminate the
false detection of microcalcifications, physicians always
alter the scan angle or compress the breast [17], [18]. If
a hyperechoic signal with a shadowing effect disappears
by transducer compression or angulation, it is probably
caused by refractive shadowing related to a Coopers ligament or speckle interference.
The described characteristics imply that combining information from multiple images obtained under different
states could be useful in discriminating between true and
false microcalcifications. Compounding refers to additively combining multiple ultrasound images obtained from
different apertures or frequency bands into a single image
(e.g., spatial compounding or frequency compounding),
which could suppress the artifacts such as speckle interfer-
2014 IEEE
956
IEEE Transactions on Ultrasonics, Ferroelectrics, and Frequency Control ,
ence and acoustic shadowing [19], [20]. However, the spatial resolution is lower for such compounding techniques
because the full aperture or full bandwidth is not used.
A strain-compounding imaging technique was recently
proposed for speckle noise reduction that degraded the
spatial resolution less [21][23]. This technique is based
on combining multiple images obtained under different
strain conditions, where the different strain states can be
created by acoustic-radiation-force excitation or applying
manual external compression. The papers by Anderson et
al. [10], [24] discuss the detectability of microcalcifications
in a speckle background and analyze the efficacy of spatial
and frequency compounding in the detection of microcalcifications. Those authors found that these compounding
methods improve the visualization of microcalcifications
by only a small degree because of the small effects that
such methods have on the amplitudes of signals associated with the microcalcifications. This suggests that the
detectability of microcalcifications should be significantly
advanced by a more comprehensive characterization of
their acoustic properties in vivo.
Recently, the Nakagami distribution was considered as
a general model to describe backscattered signals exhibiting varying statistics, including those associated with
pre-Rayleigh, Rayleigh, and post-Rayleigh distributions,
which are dependent on the density, arrangement, phase,
and other properties of scatterers in tissues [25], [26]. Our
previous study showed that the existence of microcalcifications resulted in one specific case of pre-Rayleigh statistics for the envelope, and the Nakagami parameter (m)
was used to detect and classify microcalcifications [27].
However, some research has reported that the presence of
resolvable strong scatterers (i.e., the existence of microcalcifications) led to different average powers from each
cluster, constituting a scenario which was not part of the
Nakagami scattering regime [28], [29]. The speckle factor (SF) given by Shankar [29] was the inverse of the m
in a peculiar case in which clusters had identical powers,
but this peculiar case did not correspond to the existence
of microcalcifications. Nevertheless, Shankar performed
simulations showing that even when the Nakagami distribution was not the right fit for the envelope signal from
tissues containing microcalcifications, the SF still provided useful information [29]. The presence of microcalcification-like regions in B-scan images was characterized by
the existence of extremely bright spots and high variations
in intensity, leading to high levels of speckle (i.e., high SF
values). However, the study presented by Shankar did not
focus on the detection of actual microcalcifications within
the breast lesions using ultrasound.
The objective of this study is to apply the strain-compounding method to SF imaging to discriminate between
microcalcifications and false microcalcifications. The method involves combining the compounding of multiple images and SF imaging to provide information corresponding
with the speckle characteristics of tissues. In this study, in
vitro experiments were introduced to confirm the feasibility of the strain-compounding SF image in identifying the
vol. 61, no. 6,
June
2014
relative contribution of scattering from microcalcifications
within the soft and hard phantoms after scatterers were
redistributed as a result of mechanical deformations. In
the ultrasound-based Breast Imaging Reporting and Data
System (BI-RADS) classification, lesions with suspicious
microcalcifications are always classified as category 4 or
5. Therefore, clinical data were obtained from 26 breast
lesions (20 and 6 at BI-RADS categories 4 and 5, respectively) that had been subjected to histological work-up.
This paper is organized as follows. Section II introduces
the materials and methods for constructing the straincompounding SF image, and describes how different strain
conditions were created by manual compression. Section
III presents the results obtained in phantom experiments
and clinical tests to reveal the capabilities of the straincompounding B-scan image and the strain-compounding
SF image; the performances of these two types of straincompounding images in identifying microcalcifications and
false microcalcifications are evaluated by receiver operating characteristic (ROC) curve. Section V discusses the
potential of the strain-compounding SF image in breast
ultrasound.
II. Materials and Methods
A. Phantom Experiments
Two types of 60 40 40mm phantoms, each with
a 1-mm-diameter cluster of calcium hydroxyapatite particles embedded in the soft and hard inclusions, were
produced to mimic clustered microcalcifications within
the soft (e.g., benign tumor) and hard (e.g., malignancy)
breast tumors, respectively. Calcium hydroxyapatite has
been considered to be the main chemical composition of
the microcalcifications within the breast tumors [30]. Table I lists the compositions, scatterer density, and Youngs
modulus of the phantoms. The phantom was comprised of
agarose (Ultrapure Agarose, Invitrogen, Carlsbad, CA),
distilled deionized water, and 75-m glass beads (59200U, Supelco, Bellefonte, PA). A homogeneous gel of agarose
and distilled deionized water was produced by raising the
temperature of the solution to 100C before adding glass
beads. The mixture was then poured into the phantom
container and rotated until it had cooled and congealed.
The scatterer density (D) in the container, which is defined as the number of scatterers per cubic millimeter, can
be estimated to be [31]
D=
mg
4
r 3
3
, (1)
where mg, r, and correspond to the mass, radius, and
density of glass beads, respectively, and denotes the total
volume of the solution in the container. Then, the phantoms with various scatterer densities were made by adding
different weights of glass beads. According to the previous
study [32], the scatterer density in the phantom of greater
liao et al.: discrimination of breast microcalcifications using a strain-compounding technique
957
TABLE I. Compositions of the Three Types of Material Included in Phantoms Designed to Simulate
the Scatterer and Elasticity Characteristics of Tissues.
Material
Background
Soft inclusion
Hard inclusion
Ultrapure
agarose
(g)
Distilled
deionized water
(mL)
Glass
beads
(g)
Scatterer
density
(scatterers/mm3)
0.75
0.075
0.15
100
10
10
1.81
0.09
0.09
32
16
16
Calcium
hydroxyapatite
particles
None
1-mm-diameter cluster
1-mm-diameter cluster
Youngs
modulus
(mean std kPa)
43.4 2.2
48.7 1.6
135.2 6.3
or comparable to 32 scatterers/mm3 tended to be fully developed in statistics, leading to the Rayleigh distribution.
In this study, each phantom background (32 scatterers/
mm3) corresponded to global backscattered statistics of
a Rayleigh distribution, and the backscattered statistics
of the inclusions (16 scatterers/mm3) were closer to preRayleigh distributions.
Ultrasound images of the phantom were acquired using
a portable ultrasound scanner (model 3000, Terason, Burlington, MA), with the wideband linear-array transducer
operating at a central frequency of 7.5MHz. Moreover,
the pulse length of the incident wave was approximately
0.9mm, the axial resolution was 0.4mm, and the lateral
resolution was 0.6mm. Insana et al. [33] reported that
stiff scatterers (e.g., glass beads) in the phantom redistributed but did not individually deform during limited compression, and the number density of scatterers remained
constant. They used an engineering strain = (L0 L)/
L0 as that resulting from the compressive stress applied.
L0 was the initial sample height along the compression
axis and L was the instantaneous height. Consequently,
the compressive strain () should be smaller than 0.2 to
ensure sample integrity for scattering measurements, and
the number density of scatterers remained constant with
the estimate because the phantom volume was conserved
under deformation [33]. In this study, the linear transducer was attached to a 3-axis motion stage to provide
a uniform stress distribution, and it was pressed into the
top surface a distance of 10% of the total height of the
phantom (i.e., 4mm) with the bottom surface held fixed,
which corresponded to the applied value of 0.1. A multiple compression strategy was employed in the phantom.
Approximately 75 sequential B-scan images were acquired
in 3s. Each scan line was demodulated using the Hilbert
transform to obtain the envelope image, and the B-scan
image was obtained based on the logarithm-compressed
envelope image with a dynamic range of 40dB. The pixel
size of the B-scan image was 0.09mm.
ages were identified by a physician with more than 20
years of clinical experience. These lesions were categorized
based on the BI-RADS as category 4A (suspicious malignancy with low likelihood) in seven cases, category 4B
(suspicious malignancy with intermediate likelihood) in
five cases, category 4C (suspicious malignancy with moderate likelihood) in eight cases, and category 5 (highly
suggestive of malignancy) in six cases. The final assessments were performed by mammography and ultrasoundguided core biopsy. Note that the positions captured by
ultrasound and punched by core biopsy were the same.
The lesion sizes ranged from 1 to 3.5cm. Finally, the database contained 14 microcalcifications within malignant
tumors, 4 microcalcifications within benign tumors, and
8 benign lesions without microcalcifications. Thus, there
were 8 cases of false-positive findings in detecting microcalcifications using ultrasound, and they were denoted as
false microcalcifications in this study.
Several studies have stated that microcalcifications are
mostly useful in detecting intraductal or small invasive
cancers smaller than 5mm [34]. Typical benign microcalcifications may vary in size from 2 to 4mm, and microcalcifications suggestive of malignancy are usually smaller
than 1mm [35]. In addition, according to the previous
studies [36], [37], microcalcifications ranging from 1 to
2mm in diameter could be detected by 7.5MHz ultrasound. The diameter sizes of the clustered microcalcifications included in this study ranged from 0.8 to 3mm. The
correlations between the associated ultrasound findings
and the histological findings of all cases are summarized in
Table II. The experimental procedure and image-acquisition protocol were the same as those used in the phantom
experiments. Manual compression by the experienced physician was applied to the target lesion at a relatively constant velocity and the compression depth was 5 to 8mm.
A sequence of images was acquired within 3s.
B. In Vivo Application: Clinical Data
Fig. 1 shows a schematic diagram of the four stages
involved in the strain-compounding B-scan imaging method: 1) compression using an external force; 2) in-plane
motion estimation by speckle tracking; 3) correction for
in-plane motion; and 4) incoherent image addition [22].
The manual compression used to induce different strain
conditions deformed the object and caused the scatterers
to move in three dimensions. Accurate speckle tracking
requires a strong correlation between two images, whereas
To assess the clinical efficiency of the proposed method,
we collected breast image data from the National Taiwan
University Hospital, and obtained informed consent from
the associated patients. Subjects having breast masses
with suspicious microcalcifications using breast ultrasound
were included in the study. The 26 microcalcification-like
regions associated with breast lesions in the B-scan im-
C. Strain-Compounding B-Scan Imaging
958
IEEE Transactions on Ultrasonics, Ferroelectrics, and Frequency Control ,
vol. 61, no. 6,
June
2014
TABLE II. Correlations Between Ultrasound Findings and Histological Findings of 26 Lesions.
Ultrasound-based
BI-RADS category
Microcalcifications
False
microcalcifications
4A
4B
4C
3
8
2
0
5
Total
6
18
0
8
a weak correlation is required for effective speckle reduction. Therefore, the compression was performed in multiple small increments. It was important to investigate the
degree of speckle correlation under different strain conditions to develop an optimal strategy and to understand
the performance of the strain-compounding B-scan imaging method[23].
The correlation coefficient between the reference Bscan image (uncompressed image) and the B-scan image
obtained under a different strain condition (i.e., comparison image) was calculated. In these images, we manually
defined a rectangular ROI that included the entire lesion
and its margins, because the correlation coefficient depended on the size of the ROI. Then, the correlation coefficient as a function of the applied strain was used to
determine the probabilistic speckle decorrelation, which
was obtained when the correlation coefficients decreased
monotonically to their minimum values. Note that using
Biopsy results
Fibroadenoma (5)
Fibroepithelial lesion (1)
Fibrocystic disease (1)
Fibroadenoma (5)
Invasive ductal carcinoma (6)
Ductal carcinoma in situ (1)
Intraductal papillary carcinoma (1)
Invasive ductal carcinoma (6)
five compounded frames was sufficient to reduce the appearance of speckle and to maximize the contrast resolution in the compound B-scan imaging method [38], [39].
Therefore, five frames were compounded in the acquisition
sequence that had produced probabilistic speckle decorrelation. The block sum pyramid algorithm (BSP) and the
multilevel block-matching algorithm were combined and
referred to as the multilevel BSP algorithm, which had
excellent computational performance for two-dimensional
speckle tracking in B-scan images to obtain the in-plane
displacement map (i.e., where the scatterers move to) [40].
The acquired displacement maps were then used to correct the pixel coordinates of the five compounded frames.
Finally, the strain-compounding B-scan image could be
obtained by combining the five frames that had been spatially corrected.
The degree of speckle reduction for the B-scan images
was quantified by calculating the speckle SNRas
SNR =
target
, (2)
target
where and are the mean and standard deviations of
the amplitude, respectively; these values were estimated in
the target using the manually contoured regions.
D. Strain-Compounding Speckle Factor (SF) Imaging
The probability density function of the ultrasound
backscattered-signal power Z under the Nakagami statistical model is given by[26]
f (z ) =
m mz m 1
m
exp z U (z ), (3)
(m) m
where z corresponds to the possible values for random
variable Z of the backscattered-signal powers, and ()
and U() are the gamma and unit step functions, respectively. The average power is given by . The Nakagami
parameter m associated with the Nakagami distribution
can be obtained from
Fig. 1. Schematic diagram of the strain-compounding technique.
m =
2
. (4)
(Z )2
liao et al.: discrimination of breast microcalcifications using a strain-compounding technique
959
Fig. 2. Flowchart summarizing the strain-compounding SF imaging method used in this study. The steps involved in in-plane motion correction are
indicated by solid arrows; dashed arrows indicate the steps involved in strain-compounding SF imaging.
Then, the SF is defined as[29]
SF =
Z 2
var(Z )
1 =
, (5)
Z 2
Z 2
where denotes the statistical average and var () is the
variance. The m is bounded by the lower limit of 1/2. The
SF becomes 1/m, and it was the quantitative measure of
the severity of the speckle[29].
One previous study demonstrated that the optimal sliding window size for constructing the Nakagami parameter
image was a square with a side length equal to three times
the pulse length of the incident ultrasound [32]. Such a
window size provided both stable estimations of the m and
an acceptable imaging resolution. Consequently, a sliding
window size of 2.7 2.7mm was applied in the following constructions of the SF image. The SF image was
constructed from the SF map, which was obtained using a sliding window within the envelope image to collect
the local backscattered-signal powers for estimation of the
SF based on the first and second moments of the power.
Then, the SF estimate was assigned as the new pixel value
located in the center of the window at each position in
the image. The SF image was normalized, and a rainbow
color scale was applied to emphasize the information in
the image.
The process followed was similar to that used in the
strain-compounding B-scan imaging method. To correctly compound five SF images obtained in the acquisition
sequence, the in-plane displacement fields acquired from
the five B-scan images were used to spatially correct the
corresponding envelope images. The corrected envelope
images were used to form the SF images, and these SF
images were additively combined to create the strain-compounding SF image. The basic flowchart summarizing the
procedure employed in this study is shown in Fig. 2. Additionally, we estimated the average of the SF (SFavg) values
within the manually contoured areas in the SF images.
E. Statistical Assessment
The respective performances of using the strain-compounding B-scan and strain-compounding SF imaging
methods to discriminate microcalcifications and false mi-
crocalcifications were evaluated using the ROC curves and
tests based on Students t-test [41]. A difference was assumed to be statistically significant when its probability
value was less than 0.05. The area under the ROC curve
(Az) was an effective way of comparing the diagnostic efficiency, and it was independent of the decision cut-off
point, eliminating the influence of the cut-off point on
sensitivity and specificity values.
III. Results
A. Phantom Experiments
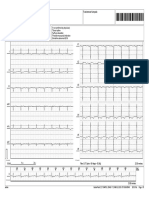
Figs. 3(a) and 4(a) show the reference B-scan images
of the phantoms consisting of hard and soft inclusions
(delineated by white circles) associated with microcalcifications (denoted by arrows), respectively. The two inclusions corresponded to the hypoechoic signals, and the
microcalcification regions showed hyperechoic signals with
shadowing effects. The strain-compounding B-scan images
of the phantoms are shown in Figs. 3(b) and 4(b). The
measurements were performed on six separate phantoms
(three with hard inclusions and three with soft inclusions).
The SNR estimates were 5.32 0.51dB (mean standard deviation) and 5.50 0.33dB for microcalcifications
within the hard (n = 3) and soft (n = 3) inclusions in the
reference B-scan images, respectively, and the corresponding SNR estimates for the strain-compounding B-scan images were 5.40 0.45dB and 6.91 0.73dB.
The microcalcifications within the hard inclusion in the
reference and strain-compounding SF images are shown
in Figs. 3(c) and 3(d), respectively. Figs. 4(c) and 4(d)
show the soft inclusion with microcalcifications in the reference and strain-compounding SF images, respectively.
To find the SF value distributions of microcalcifications
embedded in the inclusions, regions that simultaneously
included microcalcifications and the surrounding inclusion
were selected to analyze the histograms of the SF estimates. Figs. 3(e) and 3(f) show the SF value histograms
of microcalcifications within the hard inclusion in the reference and strain-compounding SF images, respectively.
The histograms for the reference and strain-compounding
SF images contained two peaks; the one at 0.2 to 0.4 was
960
IEEE Transactions on Ultrasonics, Ferroelectrics, and Frequency Control ,
Fig. 3. Different types of images of a phantom containing a hard inclusion with clustered microcalcifications: (a) reference B-scan image,
(b) strain-compounding B-scan image, (c) reference SF image, and (d)
strain-compounding SF image. White circles delineate the hard inclusion, and the arrows indicate the microcalcifications. Histograms for the
ROI in (e) the reference SF image and (f) the strain-compounding SF
image. The dashed rectangle encompasses most of the SF values corresponding to the microcalcifications.
caused by microcalcifications, as indicated by the dashed
rectangles. This phenomenon was also observed in the soft
inclusion with microcalcifications [see dashed rectangles
in Figs. 4(e) and 4(f)]. We estimated the SFavg within the
microcalcification areas in the SF images: this was 0.42
0.02 and 0.65 0.01 for the hard and soft inclusions in
the reference SF images, and 0.43 0.02 and 0.66 0.01
in the strain-compounding SF images.
B. Clinical Applications
Figs. 5 and 6 represent images of an invasive ductal carcinoma with microcalcifications and a fibroadenoma with
false microcalcifications, respectively. Microcalcifications
and false microcalcifications are indicated by arrows, and
appear as hyperechoes in the reference B-scan images, as
seen in Figs. 5(a) and 6(a). The corresponding strain-compounding B-scan images are respectively shown in Figs.
5(b) and 6(b). Figs. 5(c) and 5(d) respectively show mi-
vol. 61, no. 6,
June
2014
Fig. 4. Different types of images of a phantom containing a soft inclusion
with clustered microcalcifications: (a) reference B-scan image, (b) straincompounding B-scan image, (c), reference SF image, and (d) straincompounding SF image. White circles delineate the hard inclusion, and
the arrows indicate the microcalcifications. Histograms for the ROI in
(e) the reference SF image and (f) the strain-compounding SF image.
The dashed rectangle encompasses most of the SF values corresponding
to the microcalcifications.
crocalcifications in the reference and strain-compounding
SF images. The tumor boundaries (delineated by white
lines) were manually determined by the experienced physician for analysis of the histograms. The histograms of
microcalcifications were similar in the reference SF image
and the strain-compounding SF image [see dashed rectangles in Figs. 5(e) and 5(f)]. Compared with the cases
of microcalcifications, the histograms in the cases of false
microcalcifications were changed after the compounding
process, as shown in Figs. 6(c)6(f).
To differentiate microcalcifications from false microcalcifications, the SNR and SFavg estimates were calculated
by determining the regions containing suspicious microcalcifications in the B-scan and SF images, respectively.
Fig. 7 shows box plots for the distributions of SNR and
SFavg estimates for microcalcifications (n = 18) and false
microcalcifications (n = 8). The SNR estimates for microcalcifications in the reference and strain-compounding
liao et al.: discrimination of breast microcalcifications using a strain-compounding technique
Fig. 5. Different types of images of an invasive ductal carcinoma associated with microcalcifications (arrows): (a) reference B-scan image,
(b) strain-compounding B-scan image, (c) reference SF image, and (d)
strain-compounding SF image. The white line delineating the tumor
contour was manually tracked by the physician. Histograms are shown
for the tumor region in (e) the reference SF image and (f) the straincompounding SF image. The dashed rectangle encompasses most of the
SF values corresponding to the microcalcifications.
B-scan images were 4.73 0.69dB and 5.22 1.04dB,
respectively; the corresponding values for false microcalcifications were 4.58 0.56dB and 4.62 1.09dB. The
SFavg values for microcalcifications in the reference and
strain-compounding SF images were 0.41 0.11 and 0.47
0.10, respectively; the corresponding estimates for false
microcalcifications were 0.30 0.16 and 0.22 0.10. We
found that the SFavg values differed significantly between
the cases of microcalcifications and false microcalcifications (p < 0.05 for reference SF image, p < 0.01 for straincompounding SF image).
However, because the t-test did not take into account
of the variation of samples, a comparison of the validity
of the two estimates (i.e., SNR and SFavg) in discriminating between microcalcifications and false microcalcifications, using ROC analysis, is illustrated in Fig. 8. The
diagnostic efficiency was best for the SFavg estimates in
the strain-compounding SF images, with an accuracy of
88.5%, a sensitivity of 83.3%, and a specificity of 100.0%,
961
Fig. 6. Different types of images of a fibroadenoma associated with false
microcalcifications (arrows): (a) reference B-scan image, (b) strain-compounding B-scan image, (c) reference SF image, and (d) strain-compounding SF image. The white line delineating the tumor contour was
manually tracked by the physician. Histograms are shown for the tumor
region in (e) the reference SF image and (f) the strain-compounding SF
image. The dashed rectangle encompasses most of the SF values corresponding to the false microcalcifications.
as indicated in Table III. The positive (PPV) and negative
predictive values (NPV) were 72.7% and 100.0%, respectively. Moreover, the mean Az obtained by the SNR estimate in the strain-compounding B-scan image was 0.71,
with a 95% confidence interval of 0.47 to 0.94, and that
obtained by the SFavg estimate in the strain-compounding
SF image was 0.94, with a 95% confidence interval of 0.82
to 1.00. This difference was demonstrated by comparing
the Az values. The ability in distinguishing microcalcifications from false microcalcifications differed significantly
between the SNR and the SFavg estimates (p < 0.05);
namely, the classification performance was significantly
better for the strain-compounding SF imaging method
than for the strain-compounding B-scan imaging method.
IV. Discussion
Improvements in the ability to detect microcalcifications would extend the usefulness of breast ultrasound.
962
IEEE Transactions on Ultrasonics, Ferroelectrics, and Frequency Control ,
vol. 61, no. 6,
June
2014
Fig. 8. ROC curves for when using the SNR estimates and the SFavg
estimates to classify microcalcifications and false microcalcifications.
Fig. 7. Box plots showing the distributions (a) of the SNR estimates
for the B-scan images and (b) of the SFavg estimates for the SF images
for microcalcifications and false microcalcifications. Box plots indicate
the median value (bold line), 25th to 75th percentiles (box), and the
data range (whiskers). An asterisk indicates p < 0.05; double asterisks
indicate p < 0.01.
For this it is necessary to detect and enhance microcalcifications while simultaneously eliminating other hyperechoic spots that can result in false microcalcifications.
The strain-compounding technique was used in this study
to improve the discrimination of microcalcifications and
false microcalcifications because the uncertainty associated with working on a single image can be reduced by
combining multiple images obtained under different strain
conditions. Applying the strain-compounding technique
to the B-scan and SF images can have different physical meanings. The strain-compounding B-scan image de-
scribes the similarity and correlation of the pixels among
multiple compounded B-scan images, reflecting the variation in the structural echogenicity of tissues under different strain conditions. The effect on speckle reduction for
the strain-compounding B-scan image could be minimal
because of the effect such a method had on the amplitudes
of signals associated with the microcalcifications, resulting in a small degree of the improvement for identifying
microcalcifications (i.e., the SNR estimates for microcalcifications in the reference and strain-compounding B-scan
images were 4.73 0.69dB and 5.22 1.04dB, respectively). On the other hand, the strain-compounding SF
image displays the statistical distribution of the backscattered signals in tissues, which is determined by the correlation and similarity of the statistical moments of powers
within a scattering medium among multiple compounded
SF images. The severity of speckle of the false microcalcifications would be easily degraded under compressive
strain conditions compared with that of microcalcifications. That might be one of the reasons why compounding
reduced the SFavg values of the false microcalcifications
while the actual microcalcifications withstood the effects
of compounding and stayed where they were, improving
their visibility in the strain-compounding SF images.
TABLE III. Performances of the SNR and the SFavg Estimates Assessed by Their Accuracy, Specificity, Sensitivity,
Positive Predictive Value (PPV), Negative Predictive Value (NPV), and Az Value in Classifying
Microcalcifications and False Microcalcifications.
Classifier performance
parameter
Accuracy (%)
Sensitivity (%)
Specificity (%)
PPV (%)
NPV (%)
Az (mean standard error)
Az (95% confidence interval)
SNR estimates
in reference
B-scan images
SNR estimates in
strain-compounding
B-scan images
57.7
44.4
87.5
41.2
88.9
0.60 0.12
0.340.85
65.4
87.5
55.6
90.9
46.7
0.71 0.12
0.470.94
SFavg estimates
in reference
SF images
76.9
83.3
62.5
62.5
83.3
0.72 0.12
0.490.95
SFavg estimates in
strain-compounding
SF images
88.5
83.3
100.0
72.7
100.0
0.94 0.06
0.821.00
liao et al.: discrimination of breast microcalcifications using a strain-compounding technique
In the present study, we only considered cases with
clearly developed tumor masses. In other words, the strain
compounding technique with SF imaging was applied to
breast B-scan images with clear tumor boundaries. The
SFavg estimate for strain-compounding SF imaging distinguished all false microcalcifications among eight lesions at
BI-RADS category 4A or 4B on conventional ultrasound
(see Table II), and thus can give physicians the opportunity to downgrade from BI-RADS category 4 to category
3 in these cases. These effects could be more important in
such cases than the cases of suspicious microcalcifications
within highly malignant masses on ultrasound.
Several imaging techniques have been proposed for assisting the detection of microcalcifications in ultrasound
imaging. For instance, the elastography image, which reflects the tissue stiffness, has been used to classify benign
and malignant lesions associated with microcalcifications
[42], and vibro-acoustography has been applied in tissue
elasticity imaging to detect breast microcalcifications [43],
[44]. However, the extent of microcalcifications within the
lesion cannot be identified and evaluated by elastography.
Moreover, implementing vibro-acoustography for clinical
applications requires a hydrophone to receive ultrasound
backscattered signals during scanning. The strain-compounding SF imaging method proposed herein can visualize microcalcifications using a commercial ultrasound
system, but its ability to detect microcalcifications still
depends on their size, distribution, form, and density.
V. Conclusions
In conclusion, the measurements of strain-compounding
SF images in breast tissues can be used to distinguish the
relative contribution of scattering from microcalcifications
versus false microcalcifications after scatterers were redistributed as a result of mechanical deformations. However,
the manual ROI should be close to the size of microcalcifications and larger than the SF image resolution. There
will be variation from person to person and that is the
reason for difficult putting a specific value of SFavg in the
strain-compounding SF image for classification. Besides,
this method would be limited by adopting the unfitting
statistical model (i.e., Nakagami model), estimating error in the moment-based method, and the manual compression conditions. Recently, the McKay density model
presented by Shankar [29] was utilized to retain all the
scattering conditions contained in the Nakagami model
and to include the specific condition caused by the existence of microcalcifications. It is certain that validating
the McKay model in clinical tissue characterization will
become an important issue in future work. In addition,
the ultrasound transducer can be mounted on a positioner
controlled by a three-dimensional stepping motor to reduce operator dependence. Further research is being done
to advance this imaging technique with the McKay density for fitting physical descriptions and clinical applications simultaneously.
963
References
[1] A. P. Dhawan, Y. Chitre, and C. Kaiser-Bonasso, Analysis of mammographic microcalcifications using gray-level image structure features, IEEE Trans. Med. Imaging, vol. 15, no. 3, pp. 246259, 1996.
[2] H. P. Chan, B. Sahiner, K. L. Lam, N. Petrick, M. A. Helvie, M.
M. Goodsitt, and D. D. Adler, Computerized analysis of mammographic microcalcifications in morphological and texture feature
spaces, Med. Phys., vol. 25, no. 10, pp. 20072019, 1998.
[3] M. Ruschin, B. Hemdal, I. Andersson, S. Borjesson, M. Hakansson, M. Bath, A. Grahn, and A. Tingberg, Threshold pixel size
for shape determination of microcalcifications in digital mammography: A pilot study, Radiat. Prot. Dosimetry, vol. 114, no. 13, pp.
415423, 2005.
[4] S. W. Fletcher, W. Black, R. Harris, B. K. Rimer, and S. Shapiro,
Report of the international workshop on screening for breast cancer, J. Natl. Cancer Inst., vol. 85, no. 20, pp. 16441656, 1993.
[5] R. J. Jackman and J. Rodriguez-Soto, Breast microcalcifications:
Retrieval failure at prone stereotactic core and vacuum breast biopsyFrequency, causes, and outcome, Radiology, vol. 239, no. 1,
pp. 6170, 2006.
[6] V. P. Jackson, The role of US in breast imaging, Radiology, vol.
177, no. 2, pp. 305311, 1990.
[7] H. Gufler, C. H. Buitrago-Tllez, H. Madjar, K. H. Allmann, M.
Uhl, and A. Rohr-Reyes, Ultrasound demonstration of mammographically detected microcalcifications, Acta Radiol., vol. 41, no.
3, pp. 217221, 2000.
[8] S. S. Kang, E. Y. Ko, B. K. Han, and J. H. Shin, Breast US in patients who had microcalcifications with low concern of malignancy
on screening mammography, Eur. J. Radiol., vol. 67, no. 2, pp.
285291, 2008.
[9] W. K. Moon, J. G. Im, Y. H. Koh, D. Y. Noh, and I. A. Park, US
of mammographically detected clustered microcalcifications, Radiology, vol. 217, no. 3, pp. 849854, 2000.
[10] M. E. Anderson, M. S. Soo, R. C. Bentley, and G. E. Trahey, The
detection of breast microcalcifications with medical ultrasound, J.
Acoust. Soc. Am., vol. 101, no. 1, pp. 2939, 1997.
[11] N. Kamiyama, Y. Okamura, A. Kakee, and H. Hashimoto, Investigation of ultrasound image processing to improve perceptibility of
microcalcifications, J. Med. Ultrasound, vol. 35, no. 3, pp. 97105,
2008.
[12] W. Teh and A. R. Wilson, The role of ultrasound in breast cancer
screening. A consensus statement by the European Group for Breast
Cancer Screening, Eur. J. Cancer, vol. 34, no. 4, pp. 449450, 1998.
[13] S. Huber, M. Wagner, M. Medl, and H. Czembirek, Real-time spatial compound imaging in breast ultrasound, Ultrasound Med. Biol.,
vol. 28, no. 2, pp. 155163, 2002.
[14] C. M. Sehgal, S. P. Weinstein, P. H. Arger, and E. F. Conant, A
review of breast ultrasound, J. Mammary Gland Biol. Neoplasia,
vol. 11, no. 2, pp. 113123, 2006.
[15] L. Levy, M. Suissa, J. F. Chiche, G. Teman, and B. Martin, BIRADS ultrasonography, Eur. J. Radiol., vol. 61, no. 2, pp. 202211,
2007.
[16] M. B. Kossoff, Ultrasound of the breast, World J. Surg., vol. 24,
no. 2, pp. 143157, 2000.
[17] H. M. Zonderland, The role of ultrasound in the diagnosis of breast
cancer, Semin. Ultrasound CT MR, vol. 21, no. 4, pp. 317324,
2000.
[18] I. Cspedes, J. Ophir, H. Ponnekanti, and N. Maklad, Elastography: Elasticity imaging using ultrasound with application to muscle
and breast in vivo, Ultrason. Imaging, vol. 15, no. 2, pp. 7388,
1993.
[19] V. Behar, D. Adam, and Z. Friedman, A new method of spatial
compounding imaging, Ultrasonics, vol. 41, no. 5, pp. 377384,
2003.
[20] H. D. Cheng, J. Shan, W. Ju, Y. Guo, and L. Zhang, Automated
breast cancer detection and classification using ultrasound images:
A survey, Pattern Recognit., vol. 43, no. 1, pp. 299317, 2010.
[21] M. ODonnell, A. R. Skovoroda, B. M. Shapo, and S. Y. Emelianov,
Internal displacement and strain imaging using ultrasonic speckle
tracking, IEEE Trans. Ultrason. Ferroelectr. Freq. Control, vol. 41,
no. 3, pp. 314325, 1994.
[22] P. C. Li and C. L. Wu, Strain compounding: Spatial resolution and
performance on human images, Ultrasound Med. Biol., vol. 27, no.
11, pp. 15351541, 2001.
964
IEEE Transactions on Ultrasonics, Ferroelectrics, and Frequency Control ,
[23] P. C. Li and M. J. Chen, Strain compounding: A new approach for
speckle reduction, IEEE Trans. Ultrason. Ferroelectr. Freq. Control,
vol. 49, no. 1, pp. 3946, 2002.
[24] M. E. Anderson, M. C. Soo, and G. E. Trahey, Microcalcifications
as elastic scatterers under ultrasound, IEEE Trans. Ultrason. Ferroelectr. Freq. Control, vol. 45, no. 4, pp. 925934, 1998.
[25] P. M. Shankar, J. M. Reid, H. Ortega, C. W. Piccoli, and B. B.
Goldberg, Use of non-Rayleigh statistics for the identification of
tumors in ultrasonic B-scans of the breast, IEEE Trans. Med. Imaging, vol. 12, no. 4, pp. 687692, 1993.
[26] P. M. Shankar, A general statistical model for ultrasonic backscattering from tissues, IEEE Trans. Ultrason. Ferroelectr. Freq. Control, vol. 47, no. 3, pp. 727736, 2000.
[27] Y. Y. Liao, C. H. Li, and C. K. Yeh, An approach based on strain
compounding technique and ultrasound Nakagami imaging for detecting breast microcalcifications, in Proc. IEEE-EMBS Int. Conf.
on Biomedical and Health Informatics, 2012, pp. 515518.
[28] M. Nakagami, The m-distributionA general formula of intensity
distribution of rapid fading, in Statistical Methods in Radio Wave
Propagation, W. C. Hoffman, Ed., Elmsford, NY: Pergamon, 1960.
[29] P. M. Shankar, A statistical model for the ultrasonic backscattered
echo from tissue containing microcalcifications, IEEE Trans. Ultrason. Ferroelectr. Freq. Control, vol. 60, no. 5, pp. 932942, 2013.
[30] A. S. Haka, K. E. Shafer-Peltier, M. Fitzmaurice, J. Crowe, R. R.
Dasari, and M. S. Feld, Identifying microcalcifications in benign
and malignant breast lesions by probing differences in their chemical
composition using Raman spectroscopy, Cancer Res., vol. 62, no.
18, pp. 53755380, 2002.
[31] P. H. Tsui, C. C. Huang, and S. H. Wang, Use of Nakagami distribution and logarithmic compression in ultrasonic tissue characterization, J. Med. Biol. Eng., vol. 26, no. 2, pp. 6973, 2006.
[32] P. H. Tsui and C. C. Chang, Imaging local scatterer concentrations
by the Nakagami statistical model, Ultrasound Med. Biol., vol. 33,
no. 4, pp. 608619, 2007.
[33] M. F. Insana, T. J. Hall, P. Chaturvedi, and C. Kargel, Ultrasonic
properties of random media under uniaxial loading, J. Acoust. Soc.
Am., vol. 110, no. 6, pp. 32433251, 2001.
[34] A. P. Dhawan, Y. Chitre, and C. Kaiser-Bonasso, Analysis of mammographic microcalcifications using gray-level image structure features, IEEE Trans. Med. Imaging, vol. 15, no. 3, pp. 246259, 1996.
[35] M. Muttarak, P. Kongmebhol, and N. Sukhamwang, Breast calcifications: Which are malignant? Singapore Med. J., vol. 50, no. 9,
pp. 907913, 2009.
[36] V. P. Jackson, E. Kelly-Fry, P. A. Rothschild, R. W. Holden, and S.
A. Clark, Automated breast sonography using a 7.5-MHz PVDF
transducer: Preliminary clinical evaluation, Radiology, vol. 159, no.
3, pp. 679684, 1986.
[37] W. T. Yang, M. Suen, A. Ahuja, and C. Metreweli, In vivo demonstration of microcalcification in breast cancer using high resolution
ultrasound, Br. J. Radiol., vol. 70, no. 835, pp. 685690, 1997.
[38] Y. Y. Liao, C. H. Li, P. H. Tsui, C. C. Chang, W. H. Kuo, K. J.
Chang, and C. K. Yeh, Strain-compounding technique with ultrasound Nakagami imaging for distinguishing between benign and
malignant breast tumors, Med. Phys., vol. 39, no. 5, pp. 23252333,
2012.
[39] R. R. Entrekin, B. A. Porter, H. H. Sillesen, A. D. Wong, P. L.
Cooperberg, and C. H. Fix, Real-time spatial compound imaging:
Application to breast, vascular, and musculoskeletal ultrasound,
Semin. Ultrasound CT MR, vol. 22, no. 1, pp. 5064, 2001.
[40] P. C. Li and W. N. Lee, An efficient speckle tracking algorithm for
ultrasonic imaging, Ultrason. Imaging, vol. 24, no. 4, pp. 215228,
2002.
[41] C. E. Metz, Basic principles of ROC analysis, Semin. Nucl. Med.,
vol. 8, no. 4, pp. 283298, 1978.
[42] N. Cho, W. K. Moon, and J. S. Park, Real-time US elastography
in the differentiation of suspicious microcalcifications on mammography, Eur. Radiol., vol. 19, no. 7, pp. 16211628, 2009.
[43] A. Alizad, M. Fatemi, L. E. Wold, and J. F. Greenleaf, Performance of vibro-acoustography in detecting microcalcifications in
excised human breast tissue: A study of 74 tissue samples, IEEE
Trans. Med. Imaging, vol. 23, no. 3, pp. 307312, 2004.
[44] M. W. Urban, A. Alizad, and M. Fatemi, Vibro-acoustography and
multifrequency image compounding, Ultrasonics, vol. 51, no. 6, pp.
689696, 2011.
vol. 61, no. 6,
June
2014
Yin-Yin Liao was born in 1985 in Taichung, Taiwan. She received her M.S. and Ph.D. degrees in
the Department of Biomedical Engineering and
Environmental Sciences from the National Tsing
Hua University, Hsinchu, Taiwan, in 2009 and
2013, respectively. She worked as a postdoctoral
researcher with the Department of Biomedical Engineering and Environmental Sciences at the National Tsing Hua University in 2013. Her research
interests include computer-aided diagnosis of
breast cancer, ultrasound tissue characterization,
and tissue elasticity imaging.
Chia-Hui Li was born in 1986 in Taipei, Taiwan. She earned her B.E.
degree in the Department of Medical Imaging and Radiological Sciences
from Chang Gung University, Taoyuan, Taiwan, in 2009. She received
her M.S. degree in the Department of Biomedical Engineering and Environmental Sciences from the National Tsing Hua University, Hsinchu,
Taiwan, in 2011. She is currently a radiological technologist in the Department of Obstetrics and Gynecology at the National Taiwan University Hospital, Taipei, Taiwan. Her research interests include breast
ultrasound and ultrasound parametric imaging.
Po-Hsiang Tsui (M09) was born in Taiwan. He
received the B.E., M.S., and Ph.D. degrees in biomedical engineering from Chung Yuan Christian
University, Chung Li, Taiwan, in 2000, 2001, and
2005, respectively. In 2006, he was with the Research Center for Applied Sciences, Academia Sinica, Taipei, Taiwan, for postdoctoral research. In
2010, he joined the Department of Medical Imaging and Radiological Sciences, College of Medicine, Chang Gung University, Taoyuan, Taiwan.
He is currently an Associate Professor and the
Director for the Medical Imaging Research Center, Institute for Radiological Research, Chang Gung University and Hospital. His research interests focus on ultrasound scattering, parametric imaging, and tissue
characterization.
Chien-Cheng Chang received a bachelors degree in chemical engineering from the National
Taiwan University in 1980. In 1982, he was awarded a University Fellowship to do an advanced
graduate study at the University of California,
Berkeley, and he received the Ph.D. degree in applied mathematics in 1985. After that, Dr. Chang
worked at the Lawrence Berkeley National Laboratory (LBNL) as a Research Associate. In 1986,
he went to Minneapolis, holding a Postdoctoral
Fellowship at the Institute for Mathematics and
its Applications. Since 1987, he has been a faculty member at the Institute of Applied Mechanics, National Taiwan University, and currently he
is a Distinguished Professor. From July 2005 to June 2009, Prof. Chang
held a joint appointment in Academia Sinica to establish the Division of
Mechanics and served as its Head in the Research Center for Applied
Sciences. From August 2009 to July 2012, he served as the Director of
the Institute of Applied Mechanics, National Taiwan University. His
fields of research interest include fluid mechanics, multi-scale mechanics,
and biomedical mechanics and engineering.
Wen-Hung Kuo is currently the attending surgeon in the Department of Surgery, National Taiwan University Hospital, Taipei, Taiwan. His research interests focus on clinical applications of
breast ultrasound.
liao et al.: discrimination of breast microcalcifications using a strain-compounding technique
King-Jen Chang obtained his Ph.D. degree
from the Institute of Clinical Medicine, National
Taiwan University, Taipei, Taiwan in 1982. He is
currently the superintendent of Cheng Ching Hospital (Chung-Kang Branch), Taichung, Taiwan.
His research interests focus on clinical applications of functional ultrasound imaging on breast
diagnosis.
965
Chih-Kuang Yeh was born in 1973 in Taiwan.
He received his B.S. and M.S. degrees in biomedical engineering from Chung-Yuan Christian University, Chung-Li, Taiwan, in 1995, and the National Cheng-Kung University, Tainan, Taiwan, in
1997, and his Ph.D. degree in electrical engineering from the National Taiwan University, Taipei,
Taiwan, in 2004, respectively. He joined Professor
Katherine Ferraras research group at the University of California, Davis as a visiting researcher
from 2003 to 2004. In 2005, he joined the Department of Biomedical Engineering and Environmental Sciences, National
Tsing Hua University, Hsinchu, Taiwan. He now is a professor, and his
current research interests include ultrasound contrast agents and ultrasound theranostics.
Potrebbero piacerti anche
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Mother and Child Hospital DesignDocumento13 pagineMother and Child Hospital DesignNikhil Duggal100% (5)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- 10.1007@978 3 030 26044 6Documento545 pagine10.1007@978 3 030 26044 6Magda CabralesNessuna valutazione finora
- Go All-Datasheet VA20Documento28 pagineGo All-Datasheet VA20CeoĐứcTrường100% (2)
- A Cog Practice Bulletin 175 Ultrasound in PregnancyDocumento16 pagineA Cog Practice Bulletin 175 Ultrasound in Pregnancyansel7Nessuna valutazione finora
- SFGDocumento55 pagineSFGsreenathreddyNessuna valutazione finora
- Block Diagram Reduction TechniquesDocumento27 pagineBlock Diagram Reduction TechniquessreenathreddyNessuna valutazione finora
- AMIE Prospectus 2012Documento16 pagineAMIE Prospectus 2012vinayvpalekarNessuna valutazione finora
- Cramér-Rao Bound For Circular Complex Independent Component Analysis - SpringerDocumento10 pagineCramér-Rao Bound For Circular Complex Independent Component Analysis - SpringersreenathreddyNessuna valutazione finora
- Jawaharlal Nehru Technological University Anantapur AnantapurDocumento2 pagineJawaharlal Nehru Technological University Anantapur AnantapursreenathreddyNessuna valutazione finora
- Digital Signal Processing Lab MannualDocumento37 pagineDigital Signal Processing Lab Mannualsreenathreddy100% (4)
- Emotion Explained Edmund T. RollsDocumento16 pagineEmotion Explained Edmund T. RollsLam Sin WingNessuna valutazione finora
- ItteDocumento3 pagineItteAkram KastiranNessuna valutazione finora
- Dental Accreditation StandardsDocumento66 pagineDental Accreditation Standardsdhir.ankurNessuna valutazione finora
- LOGIQ S8 XDC BrochureDocumento5 pagineLOGIQ S8 XDC BrochureDANIA BWIDANINessuna valutazione finora
- Dicom in Radiotherapy: First, What Is DICOM?Documento4 pagineDicom in Radiotherapy: First, What Is DICOM?Cata CtuNessuna valutazione finora
- Lumbar InstabilityDocumento6 pagineLumbar InstabilityCotta MüllerNessuna valutazione finora
- SYSC 4810: Introduction To Network and Software Security Module 2 AssignmentDocumento13 pagineSYSC 4810: Introduction To Network and Software Security Module 2 AssignmentAmbar MendezNessuna valutazione finora
- Nuclear Medicine Resources ManualDocumento544 pagineNuclear Medicine Resources ManualHend Ayman Azazy100% (2)
- Azhra Naheed Medical CollegeDocumento16 pagineAzhra Naheed Medical CollegeBismillah_2250% (2)
- Philips NMR and MRIDocumento98 paginePhilips NMR and MRItsram90Nessuna valutazione finora
- Final - Specifications of Stereotactic FrameDocumento2 pagineFinal - Specifications of Stereotactic FrameadeshdrNessuna valutazione finora
- 4 SiemensDocumento85 pagine4 SiemensTold Told LeungNessuna valutazione finora
- Musculoskeletal Imaging - The Basics: Dr. Rosy SetiawatiDocumento54 pagineMusculoskeletal Imaging - The Basics: Dr. Rosy SetiawatiNova RizkaNessuna valutazione finora
- MRI Findings of 26 Patients With Parsonage-Turner SyndromeDocumento6 pagineMRI Findings of 26 Patients With Parsonage-Turner SyndromeTopciu Mihaela FeliciaNessuna valutazione finora
- Leiomioma - Miomectomia LaparoscopicaDocumento20 pagineLeiomioma - Miomectomia LaparoscopicaNella SolanoNessuna valutazione finora
- Sodium Bicarbonate - It's Role in Reversing CancerDocumento9 pagineSodium Bicarbonate - It's Role in Reversing CancerDr. Robert. O. Young100% (4)
- Pi Is 0894731714003502Documento33 paginePi Is 0894731714003502eryxspNessuna valutazione finora
- Access All Areas With The: Premium DR Room To GoDocumento8 pagineAccess All Areas With The: Premium DR Room To GoNguyen AnhNessuna valutazione finora
- Chapter IDocumento76 pagineChapter ITine Astrero Martin-HonorioNessuna valutazione finora
- RPTDocumento6 pagineRPTparagkulkarni11Nessuna valutazione finora
- Imaging Features of Pediatric Musculoskeletal Tuberculosis: Pictorial EssayDocumento15 pagineImaging Features of Pediatric Musculoskeletal Tuberculosis: Pictorial EssayMarwin JouleNessuna valutazione finora
- Jaclyn Wanie Resume PDFDocumento2 pagineJaclyn Wanie Resume PDFapi-631931479Nessuna valutazione finora
- Elizabeth Kiger Journal 11Documento3 pagineElizabeth Kiger Journal 11api-556937362Nessuna valutazione finora
- PCPNDT Act Presentation BY: Dr. Advani Asha Special Officer F.W. & M.C.HDocumento134 paginePCPNDT Act Presentation BY: Dr. Advani Asha Special Officer F.W. & M.C.HGaurav M. AdvaniNessuna valutazione finora
- Uk Guidelines SarcomaDocumento21 pagineUk Guidelines Sarcomachu_chiang_3Nessuna valutazione finora
- Jijnasa Vol 9Documento67 pagineJijnasa Vol 9lakshshetty16Nessuna valutazione finora