Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Coronary Artery Bypass Grafting
Caricato da
RickCohenCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Coronary Artery Bypass Grafting
Caricato da
RickCohenCopyright:
Formati disponibili
11/7/2014
Coronary Artery Bypass Grafting
CoronaryArteryBypassGrafting
Author:RHBilal,MBBS,MRCSChiefEditor:RichardALange,MDmore...
Updated:Apr4,2014
PracticeEssentials
Coronaryarterybypassgrafting(CABG)isperformedforpatientswithcoronaryarterydisease(CAD)toimprove
qualityoflifeandreducecardiacrelatedmortality.
Indications
ClassIindicationsforCABGfromtheAmericanCollegeofCardiology(ACC)andtheAmericanHeartAssociation
(AHA)areasfollows[1,2]:
Leftmaincoronaryarterystenosis>50%
StenosisofproximalLADandproximalcircumflex>70%
3vesseldiseaseinasymptomaticpatientsorthosewithmildorstableangina
3vesseldiseasewithproximalLADstenosisinpatientswithpoorleftventricular(LV)function
1or2vesseldiseaseandalargeareaofviablemyocardiuminhighriskareainpatientswithstableangina
>70%proximalLADstenosiswitheitherejectionfraction<50%ordemonstrableischemiaonnoninvasive
testing
OtherindicationsforCABGincludethefollowing:
Disablingangina(ClassI)
OngoingischemiainthesettingofanonSTsegmentelevationMIthatisunresponsivetomedicaltherapy
(ClassI)
Poorleftventricularfunctionbutwithviable,nonfunctioningmyocardiumabovetheanatomicdefectthatcan
berevascularized
CABGmaybeperformedasanemergencyprocedureinthecontextofanSTsegmentelevationMI(STEMI)in
caseswhereithasnotbeenpossibletoperformpercutaneouscoronaryintervention(PCI)orwherePCIhasfailed
andthereispersistentpainandischemiathreateningasignificantareaofmyocardiumdespitemedicaltherapy.
Contraindications
CABGisnotconsideredappropriateinasymptomaticpatientswhoareatalowriskofMIordeath.Patientswhowill
experiencelittlebenefitfromcoronaryrevascularizationarealsoexcluded.
Althoughadvancedageisnotacontraindication,CABGislesscommonlyperformedintheelderly.Becauseelderly
patientshaveashorterlifeexpectancy,CABGmaynotnecessarilyprolongsurvival.Thesepatientsarealsomore
likelytoexperienceperioperativecomplicationsafterCABG.
Preproceduralevaluation
BeforeCABG,thepatientsmedicalhistoryshouldbecarefullyexaminedforfactorsthatmightpredisposeto
complications,suchasthefollowing:
RecentMI
Previouscardiacsurgeryorchestradiation
Conditionspredisposingtobleeding
Renaldysfunction
CerebrovasculardiseaseincludingcarotidbruitsandTIA
Electrolytedisturbancesthatmightpredisposethepatienttodysrhythmias
Infection,includingurinarytractinfectionanddentalabscesses
Respiratoryfunction,includingthepresenceofCOPDorinfection[3]
Routinepreoperativeinvestigationsincludethefollowing[3]:
Fullbloodcount(abnormalitiescorrected)
Clottingscreen
Creatinineandelectrolytes(abnormalitiescorrectedanddiscussedwiththeanesthetist)
Liverfunctiontests
ScreeningformethicillinresistantStaphylococcusaureus
Chestradiography
ECG
Echocardiographyorventriculography(toassessLVfunction)
Coronaryangiography(todefinetheextentandlocationofCAD)
Premedication
Theaimsofpremedicationaretominimizemyocardialoxygendemandsbyreducingheartrateandsystemicarterial
pressureandtoimprovemyocardialbloodflowwithvasodilators.Drugsthatshouldbecontinueduptothetimeof
surgeryareasfollows:
Betablockers,calciumchannelblockers,andnitrates
Aspirin
http://emedicine.medscape.com/article/1893992-overview
1/9
11/7/2014
Coronary Artery Bypass Grafting
Agentsgivenareasfollows:
Temazepamimmediatelypreoperatively
Midazolam,asmallIVdoseintheoperatingroombeforearteriallineinsertion
Eachpatientshouldbecrossmatchedwith2unitsofblood(forsimplecases)or6unitsofblood,freshfrozen
plasma,andplatelets(forcomplexcases).[3,4,5]Tranexamicacid(bolus1gbeforesurgicalincisionfollowedbyan
infusionof400mg/hrduringsurgery)maybeconsideredtoreducepostoperativemediastinalbleedingandblood
product(ie,redbloodcellandfreshfrozenplasma)use[6]
Anesthesia
Cardiacsurgerymakesuseofthefollowing2formsofneuraxialblockade:
Intrathecalopioidinfusion
Thoracicepiduralanesthesia(generallyalowdoselocalanesthetic/opioidinfusion)
Monitoring
Inadditiontothestandardanestheticmonitoring(ECG,pulseoximetry,nasopharyngealtemperature,urineoutput,
gasanalysis),specificmonitoringrequirementsforcardiacsurgeryincludethefollowing:
Invasivebloodpressure
Centralvenousaccess
Transesophagealechocardiography(TEE)
Neurologicmonitoring
Technique
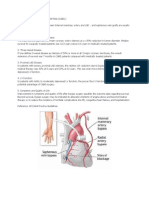
Sitesfromwhichtheconduitcanbeharvestedincludethefollowing:
Saphenousvein
Radialartery
Leftinternalthoracic(mammary)artery(LITA)
Rightinternalthoracic(mammary)artery(RITA)
Rightgastroepiploicartery
Inferiorepigastricartery
Splenicartery
TheusualincisionforCABGisamidlinesternotomy,althoughananteriorthoracotomyforbypassoftheLADor
lateralthoracotomyformarginalvesselsmaybeusedwhenanoffpumpprocedureisbeingperformed.
Cardiopulmonarybypass,cardioplegicarrest,andplacementofgraftfollows.
AlternativeapproachestoCABGincludethefollowing:
OffpumpCABG
TotallyendoscopicCABG
Hybridtechnique(bypassplusstenting
Imagelibrary
Mediansternotomy
Background
Coronaryarterybypassgrafting(CABG)isperformedforpatientswithcoronaryarterydisease(CAD)toimprove
qualityoflifeandreducecardiacrelatedmortality.CADistheleadingcauseofmortalityintheUnitedStates,
Europe,andAustralia.[7]Additionally,itisthemostcommoncauseofheartfailure.[8]
CABGwasintroducedinthe1960swiththeaimofofferingsymptomaticrelief,improvedqualityoflife,andincreased
lifeexpectancytopatientswithCAD.[9,10]Bythe1970s,CABGwasfoundtoincreasesurvivalratesinpatientswith
multivesseldiseaseandleftmaindiseasewhencomparedwithmedicaltherapy.[11]
Despitetheseinitialpositiveresults,theEuropeanCoronarySurgeryStudyconductedinthe1970sindicatedthatthe
significantimprovementin5yearsurvivalrateswithCABGwasnotapparentinthesubsequent5years.[12]
Nonetheless,CABGbecamearoutineoperationinpatientswithCAD.
Indications
CABGisperformedforbothsymptomaticandprognosticreasons.IndicationsforCABGhavebeenclassifiedbythe
AmericanCollegeofCardiology(ACC)andtheAmericanHeartAssociation(AHA)accordingtothelevelofevidence
supportingtheusefulnessandefficacyoftheprocedure[1,2]:
http://emedicine.medscape.com/article/1893992-overview
2/9
11/7/2014
Coronary Artery Bypass Grafting
ClassIConditionsforwhichthereisevidenceand/orgeneralagreementthatagivenprocedureortreatment
isusefulandeffective
ClassIIConditionsforwhichthereisconflictingevidenceand/oradivergenceofopinionaboutthe
usefulnessorefficacyofaprocedureortreatment
ClassIIaWeightofevidenceoropinionisinfavorofusefulnessorefficacy
ClassIIbUsefulnessorefficacyislesswellestablishedbyevidenceoropinion
ClassIIIConditionsforwhichthereisevidenceand/orgeneralagreementthattheprocedure/treatmentis
notusefuloreffective,andinsomecasesitmaybeharmful
IndicationsforCABGasdetailedbytheACCandtheAHA[1,2]arelistedinTable1below.
Table1.ACC/AHAIndicationsforCoronaryArteryBypassGrafting(OpenTableinanewwindow)
Indication
Asymptomatic
orMild
Angina
StableAngina
Unstable
Angina/
NSTEMI
PoorLeft
Ventricular
Function
Leftmainstenosis>50% ClassI
ClassI
ClassI
ClassI
StenosisofproximalLAD ClassI
andproximalcircumflex
>70%
ClassI
ClassI
ClassI
3vesseldisease
ClassI
ClassI
2vesseldisease
ClassIifthereislargeareaofviable
myocardiuminhighriskarea
ClassI,with
proximalLAD
stenosis
ClassIIb
ClassIIaifthereismoderateviablearea
andischemia
With>70%proximalLAD ClassIIa
stenosis
InvolvingproximalLAD
ClassIwitheitherejectionfraction<
50%ordemonstrableischemiaon
noninvasivetesting
ClassIIa
ClassIifthereislargeareaofviable
myocardiuminhighriskarea
ClassIIb
ClassI
ClassIIb
1vesseldisease
ClassIIa,ifthereisviablemoderatearea
andischemia
With>70%proximalLAD ClassIIa
stenosis
InvolvingproximalLAD
ClassIIa
ClassIIa
ClassIIb
ACC=AmericanCollegeofCardiologyAHA=AmericanHeartAssociationLAD=leftanteriordescending
(artery)NSTEMI=nonSTsegmentelevationmyocardialinfarction.
OtherindicationsforCABGincludethefollowing:
Disablingangina(ClassI)
OngoingischemiainthesettingofanonSTsegmentelevationmyocardialinfarctionthatisunresponsiveto
medicaltherapy(ClassI)
Poorleftventricularfunctionbutwithviable,nonfunctioningmyocardiumabovetheanatomicaldefectthatcan
berevascularized
CABGmaybeperformedasanemergencyprocedureinthecontextofanSTsegmentelevationmyocardial
infarction(STEMI)incaseswhereithasnotbeenpossibletoperformpercutaneouscoronaryintervention(PCI)or
wherethisprocedurehasfailedandthereispersistentpainandischemiathreateningasignificantareaof
myocardiumdespitemedicaltherapy.
OtherindicationsforCABGinthesettingofSTEMIareventricularseptaldefectrelatedtomyocardialinfarction,
papillarymusclerupture,freewallrupture,ventricularpseudoaneurysm,lifethreateningventriculararrhythmias,and
cardiogenicshock.
Table2belowshowstherecommendationsfortreatmentofpatientswithacuteheartfailureinthesettingofacute
myocardialinfarction(AMI).
Table2.TreatmentRecommendationsforPatientswithAcuteHeartFailureinSettingofAcuteMyocardialInfarction
(OpenTableinanewwindow)
Classof
levelof
Recommendation Evidence
PatientswithNSTEACSorSTEMIandunstablehemodynamicsshould
immediatelybetransferredforinvasiveevaluationandtargetvessel
revascularization
ClassI
Immediatereperfusionisindicatedinacuteheartfailurewithongoingischemia
ClassI
http://emedicine.medscape.com/article/1893992-overview
3/9
11/7/2014
Coronary Artery Bypass Grafting
EchocardiographyshouldbeperformedtoassessLVfunctionandexclude
mechanicalcomplications
ClassI
Emergencyangiographyandrevascularizationofallcriticallynarrowedarteriesby
PCI/CABGasappropriateisindicatedinpatientsincardiogenicshock
ClassI
IABPinsertionisrecommendedinpatientswithhemodynamicinstability
(particularlythoseincardiogenicshockandwithmechanicalcomplications)
ClassI
SurgeryformechanicalcomplicationsofAMIshouldbeperformedassoonas
possiblewithpersistenthemodynamicdeteriorationdespiteIABP
ClassI
EmergencysurgeryafterfailureofPCIorfibrinolysisisindicatedonlyinpatients
withpersistenthemodynamicinstabilityorlifethreateningventriculararrhythmia
duetoextensiveischemia(leftmainorsevere3vesseldisease)
ClassI
Ifpatientcontinuestodeterioratewithoutadequatecardiacoutputtopreventend
organfailure,temporarymechanicalassistance(surgicalimplantationof
LVAD/BiVAD)shouldbeconsidered
ClassIIa
Routineuseofpercutaneouscentrifugalpumpsisnotrecommended
ClassIII
AMI=acutemyocardialinfarctionBiVAD=biventricularassistdeviceCABG=coronaryarterybypassgrafting
IABP=intraaorticballoonpumpLV=leftventricleLVAD=leftventricularassistdeviceNSTEACS=nonST
segmentelevationacutecoronarysyndromePCI=percutaneouscoronaryinterventionSTEMI=STsegment
elevationmyocardialinfarction.
Specialrecommendationsinpatientswithcomorbiditiesarepresentedinthetablesbelow.
Table3.SpecificTreatmentRecommendationsforCoronaryArteryDiseaseinPatientswithMildtoModerate
ChronicKidneyDisease(OpenTableinanewwindow)
Recommendation
levelof
Evidence
CABGshouldbeconsidered,ratherthanPCI,whenextentofCADjustifiessurgical ClassIIa
approach,patientsriskprofileisacceptable,andlifeexpectancyisreasonable
OffpumpCABGmaybeconsideredratherthanonpumpCABG
ClassIIb
ForPCI,diseaseelutingstentmaybeconsidered,ratherthanbaremetalstent
ClassIIb
CABG=coronaryarterybypassgraftingCAD=coronaryarterydiseasePCI=percutaneouscoronary
intervention.
Table4.SpecificTreatmentRecommendationsforCoronaryArteryDiseaseinDiabeticPatients(OpenTableina
newwindow)
Recommendation
levelof
Evidence
InpatientspresentingwithSTEMI,primaryPCIispreferredoverfibrinolysisifitcan ClassI
beperformedwithinrecommendedtimelimits
InstablepatientswithextensiveCAD,revascularizationisindicatedtoimprove
MACCEfreesurvival
ClassI
Useofdrugelutingstentisrecommendedinordertoreducerestenosisandrepeat ClassI
targetvesselrevascularization
Inpatientsonmetformin,renalfunctionshouldbecarefullymonitoredafter
coronaryangiography/PCI
ClassI
CABGshouldbeconsidered,ratherthanPCI,whenextentofCADjustifiessurgical ClassIIa
approach(especiallymultivesseldisease)andpatientsriskprofileisacceptable
InpatientswithknownrenalfailureundergoingPCI,metforminmaybestopped48
hoursbeforeprocedure
ClassIIb
Systematicuseofglucoseinsulinpotassiumindiabeticpatientsundergoing
revascularizationisnotindicated
ClassIII
CABG=coronaryarterybypassgraftingCAD=coronaryarterydiseaseGIK=glucoseinsulinpotassium
MACCE=majoradversecardiacandcerebraleventPCI=percutaneouscoronaryinterventionSTEMI=ST
segmentelevationmyocardialinfarction.
Table5.RecommendationsforCombiningValveSurgeryandCoronaryArteryBypassGrafting(OpenTableina
newwindow)
Recommendation
levelof
Evidence
CABGisrecommendedinpatientswithprimaryindicationforaortic/mitralvalve
surgeryandcoronaryarterystenosis=70%
ClassI
CABGshouldbeconsideredinpatientswithprimaryindicationforaortic/mitral
valvesurgeryandcoronaryarterystenosis5070%
ClassIIa
MitralvalvesurgeryisindicatedinpatientswithprimaryindicationforCABGand
severeischemicmitralregurgitationandEF>30%a
ClassI
Mitralvalvesurgeryshouldbeconsideredinpatientswithprimaryindicationfor
CABGandmoderateischemicmitralregurgitation,providedthatvalverepairis
feasibleandperformedbyexperiencedoperators
ClassIIa
Aorticvalvesurgeryshouldbeconsideredinpatientswithprimaryindicationfor
ClassIIa
Incombinationwithvalvesurgery:
IncombinationwithCABG:
http://emedicine.medscape.com/article/1893992-overview
4/9
11/7/2014
Coronary Artery Bypass Grafting
CABGandmoderateaorticstenosis(meangradient3050mmHg,Dopplervelocity
34m/sec,orheavilycalcifiedaorticvalveevenwithDopplervelocity2.53m/sec)
aDefinitionofseveremitralregurgitationisathttp://www.escardio.org/guidelines.
CABG=coronaryarterybypassgraftingEF=ejectionfraction.
Table6.CarotidRevascularizationinPatientsScheduledforCoronaryArteryBypassGrafting(OpenTableinanew
window)
Recommendation
levelof
Evidence
CEAorCASshouldbeperformedonlybyteamswithdemonstrated30day
combineddeathstrokeratesof<3%inpatientswithoutpreviousneurologic
symptomsand<6%inpatientswithpreviousneurologicsymptoms
ClassI
Indicationforcarotidrevascularizationshouldbeindividualizedafterdiscussionby
multidisciplinaryteam,includingneurologist
ClassI
Timingofprocedures(synchronousorstaged)shouldbedictatedbylocalexpertise ClassI
andclinicalpresentation,withmostsymptomaticterritorytargetedfirst
InpatientswithpreviousTIA/nondisablingstroke:
Carotidrevascularizationisrecommendedfor7099%carotidstenosis
ClassI
Carotidrevascularizationmaybeconsideredfor5069%carotidstenosisinmen
withsymptoms<6months
ClassIIb
Carotidrevascularizationisnotrecommendedifcarotidstenosis<50%inmenand ClassIII
<70%inwomen
InpatientswithnopreviousTIA/stroke:
Carotidrevascularizationmaybeconsideredinmenwithbilateral7099%carotid
stenosisor7099%carotidstenosisandcontralateralocclusion
ClassIIb
Carotidrevascularizationisnotrecommendedinwomenorpatientswithlife
expectancy<5years
ClassIII
CAS=carotidarterystentingCEA=carotidendarterectomyTIA=transientischemicattack.
Table7.ManagementofPatientswithAssociatedCoronaryandPeripheralArterialDisease(OpenTableinanew
window)
Recommendation
levelof
Evidence
InpatientswithunstableCAD,vascularsurgeryispostponedandCADtreatedfirst, ClassI
exceptwhenvascularsurgerycannotbedelayedbecauseoflifethreatening
condition
Betablockersandstatinsareindicatedpreoperativelyandcontinued
postoperativelyinpatientswithknownCADwhoarescheduledforhighrisk
vascularsurgery.
ClassI
ChoicebetweenCABGandPCIshouldbeindividualizedandassessedbyheart
teaminlightofpatternsofCAD,PAD,comorbidity,andclinicalpresentation
ClassI
Prophylacticmyocardialrevascularizationbeforehighriskvascularsurgerymaybe ClassIIb
consideredinstablepatientsiftheyhavepersistentsignsofextensiveischemicor
highcardiacrisk
CABG=coronaryarterybypassgraftingCAD=coronaryarterydiseasePAD=peripheralarterialdiseasePCI=
percutaneouscoronaryintervention.
Table8.ManagementofPatientswithRenalArteryStenosis(OpenTableinanewwindow)
Recommendation
levelof
Evidence
Functionalassessmentofrenalarterystenosisseverityusingpressuregradient
measurementsmaybeusefulinselectinghypertensivepatientswhobenefitfrom
renalarterystenting
ClassIIb
Routinerenalarterystentingtopreventdeteriorationofrenalfunctionisnot
recommended
ClassIII
Table9.RecommendationsforPatientswithChronicHeartFailureandSystolicLeftVentricularDysfunction
(EjectionFraction=35%),PresentingPredominantlywithAnginaSymptoms(OpenTableinanewwindow)
CABGisrecommendedforthefollowing:
Recommendation
levelof
Evidence
ClassI
Significantleftmainstenosis
Leftmainequivalent(proximalstenosisofbothleftanteriordescendingand
leftcircumflex)
Proximalleftanteriordescendingstenosiswith2or3vesseldisease
http://emedicine.medscape.com/article/1893992-overview
5/9
11/7/2014
Coronary Artery Bypass Grafting
CABGwithsurgicalventricularreconstructionmaybeconsideredinpatientswith
LVESVindex=60mL/m2andscarredleftanteriordescendingterritory
ClassIIb
PCImaybeconsideredinpresenceofviablemyocardiumifanatomyissuitable
ClassIIb
CABG=coronaryarterybypassgraftingLVESV=leftventricularendsystolicvolumePCI=percutaneous
coronaryintervention.
Table10.RecommendationsforPatientswithChronicHeartFailureandSystolicLeftVentricularDysfunction
(EjectionFraction=35%),PresentingPredominantlywithHeartFailureSymptoms(NoorMildAngina:Canadian
CardiovascularSociety12)(OpenTableinanewwindow)
levelof
Evidence
Recommendation
LVaneurysmectomyduringCABGisindicatedinpatientswithlargeLV
aneurysm
ClassI
CABGshouldbeconsideredinpresenceofviablemyocardium,irrespectiveof ClassIIa
LVESV
CABGwithSVRmaybeconsideredinpatientswithscarredLADterritory
ClassIIb
PCImaybeconsideredinpresenceofviablemyocardiumifanatomyis
suitable
ClassIIb
Revascularizationinabsenceofevidenceofmyocardialviabilityisnot
recommended
ClassIII
CABG=coronaryarterybypassgraftingLAD=leftanteriordescending(artery)LV=leftventricleLVESV=left
ventricularendsystolicvolumePCI=percutaneouscoronaryinterventionSVR=surgicalventricular
reconstruction.
Contraindications
CABGcarriesariskofmorbidityandmortalityandisthereforenotconsideredappropriateinasymptomaticpatients
whoareatalowriskofmyocardialinfarctionordeath.Patientswhowillexperiencelittlebenefitfromcoronary
revascularizationarealsoexcluded.
CABGisperformedinelderlypatientsforsymptomaticrelief.However,althoughageisnotacontraindication,CABG
islesscommonlyperformedinthisgroupofpatients.Becauseelderlypatientshaveashorterlifeexpectancy,CABG
maynotnecessarilyprolongsurvival.Thesepatientsarealsomorelikelytoexperienceperioperativecomplications
afterCABG.
TechnicalConsiderations
Bestpractices
EitherveinsorarteriesmaybeusedasconduitsforCABG.Thegreatandsmallsaphenousveinsarethemost
commonlyusedveingrafts,andtheinternalthoracic(mammary)arteryisthemostcommonlyusedartery.
Thedisadvantageofsaphenousveingraftsistheirdecliningpatencywithtime:1020%areoccluded1yearafter
surgerybecauseoftechnicalerrors,thrombosis,andintimalhyperplasia.Another12%ofveingraftsoccludeevery
yearfrom15yearsaftersurgery,and45%occludeeveryyearfrom610yearsaftersurgery.Veingraftocclusion
thatoccurs1ormoreyearsafterCABGisduetoveingraftatherosclerosis.At10yearsaftersurgery,only5060%
ofsaphenousveingraftsarepatent,andonlyhalfofthesearefreeofangiographicatherosclerosis.
Unlikesaphenousveingrafts,internalthoracicarterygraftsexhibitstablepatencyovertime.At10years,morethan
90%ofinternalthoracicarterygraftsarepatent.Theleftinternalthoracicarteryshouldbetheconduitusedwhenthe
leftanteriorcoronaryarteryisbypassed.
TechnicalrecommendationsforCABGarepresentedinTable11below.
Table11.TechnicalRecommendationsforCoronaryArteryBypassGrafting(OpenTableinanewwindow)
Recommendation
levelof
Evidence
Proceduresshouldbeperformedinhospitalstructureandbyteamspecializedin
cardiacsurgery,usingwrittenprotocols
ClassI
ArterialgraftingtoLADsystemisindicated
ClassI
CompleterevascularizationwitharterialgraftingtononLADcoronarysystemis
indicatedinpatientswithreasonablelifeexpectancy
ClassI
Minimizationofaorticmanipulationisrecommended
ClassI
Graftevaluationisrecommendedbeforedeparturefromoperatingtheater
ClassI
LAD=leftanteriordescending(artery).
Procedureplanning
Theformationofaheartteamenablesabalancedmultidisciplinarydecisionmakingprocess(seeTable12below).
Theinformedconsentprocessshouldbeseenasanopportunitytoenhanceobjectivedecisionmakingratherthan
solelyasalegalrequirement.Itisvitaltobeawarethatfactorssuchassex,race,availability,technicalskills,local
results,referralpatterns,andpatientpreferencemayaffectthedecisionmakingprocessindependentofclinical
findings.
Table12.MultidisciplinaryDecisionPathways,PatientInformedConsent,andTimingofIntervention(OpenTablein
anewwindow)
http://emedicine.medscape.com/article/1893992-overview
6/9
11/7/2014
Coronary Artery Bypass Grafting
AcuteCoronarySyndrome
Shock
Stable
Multivessel
Disease
Stable
with
Indication
forAdHoc
PCI
STEMI
NSTEACS
OtherACS
Multidisciplinary Not
decisionmaking mandatory
Notmandatory
Notrequired
forculprit
lesionbut
requiredfor
nonculprit
vessel(s)
Required
Required
According
to
predefined
protocols
Informed
consent
Oralwitnessed
informedconsent
maybesufficient
unlesswritten
consentislegally
required
Written
informed
consenta(if
timepermits)
Written
informed
consenta
Written
informed
consenta
Written
informed
consenta
Timeto
Emergency: Emergency:No
revascularization Nodelay
delay
Urgency:
Within24hif
possibleand
nolaterthan
72h
Urgency:Time Elective:No
constraints
time
apply
constraints
Elective:
Notime
constraints
Procedure
Proceedwith
interventionon
basisofbest
evidence/
availability
nonculprit
lesionstreated
accordingto
institutional
protocol
Proceedwith
interventionon
basisofbest
evidence/
availability
nonculprit
lesionstreated
accordingto
institutional
protocol
Proceed
with
intervention
according
to
institutional
protocol
definedby
localheart
team
Oral
witnessed
informed
consentor
family
consentif
possible
without
delay
Proceed
with
intervention
onbasisof
best
evidence/
availability
Proceedwith
interventionon
basisofbest
evidence/availability
Planmost
appropriate
intervention,
allowing
enoughtime
from
diagnostic
catheterization
tointervention
aMaynotapplytocountriesthatlegallydonotaskforwritteninformedconsent,althoughEuropeanSocietyof
CardiologyandEuropeanAssociationforCardiothoracicSurgerystronglyadvocatedocumentationofpatient
consentforallrevascularizationprocedures.
ACS=acutecoronarysyndromeNSTEACS=nonSTsegmentelevationacutecoronarysyndromePCI=
percutaneouscoronaryinterventionSTEMI=STsegmentelevationmyocardialinfarction.
Additionalinputfromgeneralpractitioners,anesthesiologists,geriatricians,andintensivistsmaybeneeded.
Hospitalswithoutasurgicalcardiacunitorwithinterventionalcardiologistsworkinginanambulatorysettingshould
refertostandardevidencebasedprotocolsdevisedincollaborationwithexpertinterventioncardiologistsorcardiac
surgeonsorshouldseektheopinionsofthesephysiciansforcomplexcases.Consensusonthebest
revascularizationtreatmentshouldbedocumented.Standardprotocolsthatareinaccordancewithcurrent
guidelinesmaybeusedtoobviateindividualcasereviewofeachdiagnosticangiogram.
AdhocPCIisatherapeuticinterventionalprocedurethatisperformeddirectlyafterthediagnosticprocedurerather
thanduringadifferentsession.Althoughitisconvenientandoftencosteffective,itisnotdesirableforallcases
somepatientsmaybeincategoriesforwhichCABGisthemostsuitablechoice.Theanatomiccriteriaandclinical
factorsthatdeterminewhetherapatientcanorcannotbetreatedbymeansofadhocPCIshouldbedefinedby
institutionalprotocolsdesignedbytheheartteam.
Complicationprevention
CerebrovascularcomplicationsareamajorcauseofmorbidityafterCABG.Themaincausesofthesecomplications
arehypoperfusionorembolicevents.Accordingly,itisimportanttomaintainadequatemeanarterialpressuresasa
prophylacticmeasureagainsthypoperfusion,althoughthereislittlethatcanbedonetoprotectthepatientfrom
embolicevents.
Outcomes
Inametaanalysisof8randomizedstudiesthatincludedatotalof3612adultpatientswithdiabetesandmultivessel
CAD,treatmentwithCABGsignificantlyreducedtheriskofallcausemortalityby33%at5years,ascomparedwith
PCI.ThisrelativeriskreductiondidnotdiffersignificantlywhenpatientswhounderwentCABGwerecomparedwith
subgroupsofpatientswhoreceivedeitherbaremetalstentsordrugelutingstents.[13,14]
ContributorInformationandDisclosures
Author
RHBilal,MBBS,MRCSSpecialistRegistrarinCardiothoracicSurgery,NorthWestCardiothoracicRotation,UK
RHBilal,MBBS,MRCSisamemberofthefollowingmedicalsocieties:BritishMedicalAssociation
Disclosure:Nothingtodisclose.
http://emedicine.medscape.com/article/1893992-overview
7/9
11/7/2014
Coronary Artery Bypass Grafting
Coauthor(s)
SarahMahmoodUniversityofLiverpoolFacultyofMedicine,UK
Disclosure:Nothingtodisclose.
MahvashZamanUniversityofLiverpoolFacultyofMedicine,UK
Disclosure:Nothingtodisclose.
BridieRO'NeillUniversityofManchester,UK
Disclosure:Nothingtodisclose.
DumborLaatehNgaage,MBBS,MS,FRCSED,FWACS,FETCS,FRCS(CTh)ConsultantCardiothoracic
Surgeon,BlackpoolVictoriaHospital,UK
Disclosure:Nothingtodisclose.
AndrewJDuncan,MBChB,FRCS(CTh)ConsultantCardiothoracicSurgeon,LancashireCardiacCentre,
VictoriaHospital,UK
Disclosure:Nothingtodisclose.
ChiefEditor
RichardALange,MDProfessorandExecutiveViceChairman,DepartmentofMedicine,Director,Officeof
EducationalPrograms,UniversityofTexasHealthScienceCenteratSanAntonio
RichardALange,MDisamemberofthefollowingmedicalsocieties:AlphaOmegaAlpha,AmericanCollegeof
Cardiology,AmericanHeartAssociation,andAssociationofSubspecialtyProfessors
Disclosure:Nothingtodisclose.
AdditionalContributors
MaryLWindle,PharmDAdjunctAssociateProfessor,UniversityofNebraskaMedicalCenterCollegeof
PharmacyEditorinChief,MedscapeDrugReference
Disclosure:Nothingtodisclose.
Acknowledgments
MedscapeReferencethanksDaleKMueller,MD,forassistancewiththevideocontributiontothisarticle.Dr
MuellerisClinicalAssociateProfessorofSurgery,SectionChief,DepartmentofSurgery,UniversityofIllinois
CollegeofMedicineCoMedicalDirector,ThoracicCenterofExcellence,ViceChair,Departmentof
CardiovascularMedicineandSurgery,OSFStFrancisMedicalCenterandDirector,AdultECMO,Cardiovascular
andThoracicSurgeon,HeartCareMidwest,SC.
References
1. [BestEvidence][Guideline]HillisLD,SmithPK,AndersonJL,BittlJA,BridgesCR,ByrneJG,etal.2011
ACCF/AHAGuidelineforCoronaryArteryBypassGraftSurgery:AReportoftheAmericanCollegeof
CardiologyFoundation/AmericanHeartAssociationTaskForceonPracticeGuidelines.Circulation.Nov7
2011[Medline].
2. EagleKA,GuytonRA,DavidoffR,EdwardsFH,EwyGA,GardnerTJ.ACC/AHA2004guidelineupdatefor
coronaryarterybypassgraftsurgery:summaryarticle:areportoftheAmericanCollegeof
Cardiology/AmericanHeartAssociationTaskForceonPracticeGuidelines(CommitteetoUpdatethe1999
GuidelinesforCoronaryArteryBypassGraftSurgery).Circulation.Aug312004110(9):116876.[Medline].
3. ChikweJ,BeddowE,GlenvilleB.CardiothoracicSurgery.Oxford:OxfordUniversityPress2006.
4. MackayJH,ArrowsmithJE.CoreTopicsinCardiacAnaesthesia.Cambridge:CambridgeUniversityPress
2007.
5. GothardJ,KelleherA,HaxbyE.Cardiovascularandthoracicanaesthesia.Edinburgh:Butterworth
Heinemann2004.
6. WangG,XieG,JiangT,WangY,WangW,JiH,etal.TranexamicAcidreducesbloodlossafteroffpump
coronarysurgery:aprospective,randomized,doubleblind,placebocontrolledstudy.AnesthAnalg.Aug
2012115(2):23943.[Medline].
7. WorldHealthOrganisation.WHOGlobalInfobase.Availableathttps://apps.who.int/infobase/Mortality.aspx.
Accessed10/03/2011.
8. GheorghiadeM,BonowRO.ChronicheartfailureintheUnitedStates:amanifestationofcoronaryartery
disease.Circulation.Jan27199897(3):2829.[Medline].
9. vanDomburgRT,KappeteinAP,BogersAJ.Theclinicaloutcomeaftercoronarybypasssurgery:a30year
followupstudy.EurHeartJ.Feb200930(4):4538.[Medline].
10. KonstantinovIE.Thefirstcoronaryarterybypassoperationandforgottenpioneers.AnnThoracSurg.Nov
199764(5):15223.[Medline].
11. ElevenyearsurvivalintheVeteransAdministrationrandomizedtrialofcoronarybypasssurgeryforstable
angina.TheVeteransAdministrationCoronaryArteryBypassSurgeryCooperativeStudyGroup.NEnglJ
Med.Nov221984311(21):13339.[Medline].
12. VarnauskasE.TwelveyearfollowupofsurvivalintherandomizedEuropeanCoronarySurgeryStudy.N
EnglJMed.Aug111988319(6):3327.[Medline].
http://emedicine.medscape.com/article/1893992-overview
8/9
11/7/2014
Coronary Artery Bypass Grafting
13. VermaS,FarkouhME,YanagawaB,etal.Comparisonofcoronaryarterybypasssurgeryand
percutaneouscoronaryinterventioninpatientswithdiabetes:Ametaanalysisofrandomizedcontrolled
trials.TheLancet.Availableathttp://www.thelancet.com/journals/landia/article/PIIS22138587(13)70089
5/abstract.AccessedSeptember13,2013.
14. O'RiordanM.CABGReducesRiskofDeathvsPCIinDiabeticPatients.Medscape[serialonline].Available
athttp://www.medscape.com/viewarticle/810953.AccessedSeptember23,2013.
15. EuroscoreScoringSystem.Availableathttp://www.euroscore.org/euroscore_scoring.htm.AccessedMarch
24,2011.
16. WardHB,KellyRF.OPCABvsCABG:who,what,when,where?.Chest.Mar2004125(3):8156.[Medline].
17. DeweyTM,MackMJ.MyocardialRevascularizationwithoutCardiopulmonaryBypass.In:CohnL.Cardiac
SurgeryintheAdult.NewYork:McGrawHill2008:633654.
18. ChocronS,VandelP,DurstC,LalucF,KailiD,ChocronM,etal.Antidepressanttherapyinpatients
undergoingcoronaryarterybypassgrafting:theMOTIVCABGtrial.AnnThoracSurg.May
201395(5):160918.[Medline].
19. BrooksM.AntidepressantPriortoBypassMayReducePostopPain.MedscapeMedicalNews.Availableat
http://www.medscape.com/viewarticle/805336.AccessedJune11,2013.
20. ZohrehK,FarahAE,MehrabM,AbbasSO,AlirezaH,SorayaM.Comparisonofcompressionstockingwith
elasticbandageinreducingpostoperativeedemaincoronaryarterybypassgraftpatient.JVascNurs.Dec
200927(4):1036.[Medline].
21. ParolariA,AlamanniF,CannataA,NaliatoM,BonatiL,RubiniP.Offpumpversusonpumpcoronaryartery
bypass:metaanalysisofcurrentlyavailablerandomizedtrials.AnnThoracSurg.Jul200376(1):3740.
[Medline].
22. SongHK,PuskasJD.OffPumpCoronaryArteryBypassSurgery.In:KaiserLR,KronIL,SprayTL.Mastery
ofCardiothoracicSurgery.2nd.Philadelphia:LippincottWilliams&Wilkins.
23. MllerCH,PenningaL,WetterslevJ,SteinbrchelDA,GluudC.Offpumpversusonpumpcoronaryartery
bypassgraftingforischaemicheartdisease.CochraneDatabaseSystRev.Mar1420123:CD007224.
[Medline].
24. BonattiJ,SchachnerT,BonarosN,OhlingerA,DanzmayrM,JonetzkoP.Technicalchallengesintotally
endoscopicroboticcoronaryarterybypassgrafting.JThoracCardiovascSurg.Jan2006131(1):14653.
[Medline].
25. MishraYK,WasirH,SharmaKK,MehtaY,TrehanN.TotallyEndoscopicCoronaryArteryBypassSurgery.
AsianCardiovascThoracAnn.200614:447451.
26. GngoraE,SundtTMIII.MyocardialRevascularizationwithCardiopulmonaryBypass.In:CohnLh.Cardiac
SurgeryintheAdult.3rd.NewYork:McGrawHill2008:599632.[FullText].
27. RoachGW,KanchugerM,ManganoCM,NewmanM,NussmeierN,WolmanR,etal.Adversecerebral
outcomesaftercoronarybypasssurgery.MulticenterStudyofPerioperativeIschemiaResearchGroupand
theIschemiaResearchandEducationFoundationInvestigators.NEnglJMed.Dec191996335(25):1857
63.[Medline].
28. HigginsR,PerezTamayoRA.CoronaryArteryBypassGraftingUsingCardiopulmoaryBypass.In:Kaiser
LR,KronIL,SprayTL.MasteryofCardiothoracicSurgery.2nd.Philadelphia:LippincottWilliams&Wilkins
2007.
29. BuskoM.CABGtrumpsPCIforsurvivalinCADevenwithoutdiabetes.MedscapeMedicalNews[serial
online].December2,2013AccessedDecember17,2013.Availableat
http://www.medscape.com/viewarticle/815245.
30. KatzMH.EvolvingTreatmentOptionsinCoronaryArteryDisease.JAMAInternMed.Dec22013[Medline].
31. SipahiI,AkayMH,DagdelenS,BlitzA,AlhanC.CoronaryArteryBypassGraftingvsPercutaneous
CoronaryInterventionandLongtermMortalityandMorbidityinMultivesselDisease:Metaanalysisof
RandomizedClinicalTrialsoftheArterialGraftingandStentingEra.JAMAInternMed.Dec22013
[Medline].
MedscapeReference2011WebMD,LLC
http://emedicine.medscape.com/article/1893992-overview
9/9
Potrebbero piacerti anche
- Coronary Artery Bypass Graft Report NCM 118Documento23 pagineCoronary Artery Bypass Graft Report NCM 118Vhince Norben PiscoNessuna valutazione finora
- Novel Tools For Hemodynamic Monitoring in Critically Ill Patients With Shock - UpToDateDocumento26 pagineNovel Tools For Hemodynamic Monitoring in Critically Ill Patients With Shock - UpToDateAlex KuliaNessuna valutazione finora
- Mic Cabg Procedure PDFDocumento12 pagineMic Cabg Procedure PDFprofarmah6150Nessuna valutazione finora
- Carpal Tunnel Surgery, Hand Clinics, Volume 18, Issue 2, Pages 211-368 (May 2002)Documento151 pagineCarpal Tunnel Surgery, Hand Clinics, Volume 18, Issue 2, Pages 211-368 (May 2002)alinutza_childNessuna valutazione finora
- Acute MiDocumento61 pagineAcute MiMalueth AnguiNessuna valutazione finora
- 21 - Thyroid Function TestsDocumento2 pagine21 - Thyroid Function Testshamadadodo7Nessuna valutazione finora
- Coronary Artery Bypass Grafting (CABG)Documento1 paginaCoronary Artery Bypass Grafting (CABG)I.m. DanielNessuna valutazione finora
- THROMBOPHLEBITISDocumento50 pagineTHROMBOPHLEBITISmers puno100% (3)
- Powerpoint Presentation For Heart DiseaseDocumento18 paginePowerpoint Presentation For Heart Diseaseapi-301442453100% (1)
- Endometrial Cancer LDocumento26 pagineEndometrial Cancer Lapi-19916399Nessuna valutazione finora
- Omaha System Journal ReadingDocumento4 pagineOmaha System Journal ReadingAya PaquitNessuna valutazione finora
- Hypertensive Emergencies (ESC 2019)Documento10 pagineHypertensive Emergencies (ESC 2019)Glen LazarusNessuna valutazione finora
- Guideline Antibiotic RationalDocumento35 pagineGuideline Antibiotic RationalIstianah EsNessuna valutazione finora
- Understanding Traumatic Brain InjuryDocumento43 pagineUnderstanding Traumatic Brain InjurySilvanaPutriNessuna valutazione finora
- Deep Venous Thrombosis Harrison'sDocumento3 pagineDeep Venous Thrombosis Harrison'sMaria Agustina Sulistyo WulandariNessuna valutazione finora
- Organ Donation in The UKDocumento37 pagineOrgan Donation in The UKKazim AbbasNessuna valutazione finora
- JREC Application FormDocumento7 pagineJREC Application FormKudakwashe MagogoNessuna valutazione finora
- Background of The StudyDocumento4 pagineBackground of The StudyRodelen MarañoNessuna valutazione finora
- Concept Map MI 2Documento1 paginaConcept Map MI 2nicole barcenaNessuna valutazione finora
- Sedation in ICUDocumento14 pagineSedation in ICUIhtesham Ul HaqNessuna valutazione finora
- Ischemic Heart DiseaseDocumento55 pagineIschemic Heart DiseaseAndrassy Twinkle AlineaNessuna valutazione finora
- Management of Stroke MadamDocumento27 pagineManagement of Stroke MadamHanif SumonNessuna valutazione finora
- Murmur EvaluationDocumento4 pagineMurmur EvaluationManjunath GeminiNessuna valutazione finora
- Refkas CondylomaAccuminataDocumento18 pagineRefkas CondylomaAccuminatamichelle1945Nessuna valutazione finora
- Surgical Intervention in Management of Heart Failure: DR Royman Simanjuntak Sp. BTKVDocumento118 pagineSurgical Intervention in Management of Heart Failure: DR Royman Simanjuntak Sp. BTKVEmily RumiaNessuna valutazione finora
- Indications of Cabg: DR Altaf Hussain Jatoi Resident Cardiac Surgery Civil Hospital KarachiDocumento17 pagineIndications of Cabg: DR Altaf Hussain Jatoi Resident Cardiac Surgery Civil Hospital KarachiakhlaqjatoiNessuna valutazione finora
- Surgical Management of Ischemic Heart Disease - An UpdateDocumento48 pagineSurgical Management of Ischemic Heart Disease - An UpdateRezwanul Hoque BulbulNessuna valutazione finora
- Summary 2013 Esc GuidelinesDocumento8 pagineSummary 2013 Esc GuidelinesNick StamatiadisNessuna valutazione finora
- To Stent or Not To Stent in Ischemic Heart Failure - The REVIVED-BCIS2 Trial - AmDocumento2 pagineTo Stent or Not To Stent in Ischemic Heart Failure - The REVIVED-BCIS2 Trial - AmHand SanitizerNessuna valutazione finora
- Circulation 2014 Silvain 918 22Documento6 pagineCirculation 2014 Silvain 918 22aninNessuna valutazione finora
- Surgical Coronary Revascularization Who, What, WhenDocumento68 pagineSurgical Coronary Revascularization Who, What, WhenAlaaGaballaNessuna valutazione finora
- Diagnosis and Management in Peripheral Artery Disease EditedDocumento5 pagineDiagnosis and Management in Peripheral Artery Disease Editedwahyu suparnoNessuna valutazione finora
- Heart Failure AbnetDocumento119 pagineHeart Failure AbnetAbnet WondimuNessuna valutazione finora
- Curs de Chirurgie Cardiaca PT StudentiDocumento86 pagineCurs de Chirurgie Cardiaca PT StudentiLozan GabrielaNessuna valutazione finora
- Cardiac Imaging For Assessing Low-Gradient Severe Aortic StenosisDocumento18 pagineCardiac Imaging For Assessing Low-Gradient Severe Aortic StenosisFilipe PennaNessuna valutazione finora
- Stirrup - Comparison of ESC and ACC:AHA Guidelines For Myocardial RevascularizationDocumento8 pagineStirrup - Comparison of ESC and ACC:AHA Guidelines For Myocardial RevascularizationM. PurnomoNessuna valutazione finora
- Current Management of Rheumatic Valvular Heart DiseaseDocumento23 pagineCurrent Management of Rheumatic Valvular Heart DiseaseirineNessuna valutazione finora
- Aortic StenosisDocumento3 pagineAortic StenosissanchezmNessuna valutazione finora
- Cardiac Surgery Coronary I e IIDocumento43 pagineCardiac Surgery Coronary I e IIFrancisNessuna valutazione finora
- Reverse Tria24 MolDocumento12 pagineReverse Tria24 Molbinh doNessuna valutazione finora
- HF Gui 2013 SD ENDocumento36 pagineHF Gui 2013 SD ENmimuiNessuna valutazione finora
- Diagnostic and Therapeutic Challenges in Patients With Coexistent Chronic Obstructive Pulmonary Disease and Chronic Heart FailureDocumento10 pagineDiagnostic and Therapeutic Challenges in Patients With Coexistent Chronic Obstructive Pulmonary Disease and Chronic Heart FailureLucy Naomi BesitimurNessuna valutazione finora
- Cardiac Valve Replacement SurgeryDocumento25 pagineCardiac Valve Replacement SurgeryJamalul AdilNessuna valutazione finora
- Case-Based Device Therapy for Heart FailureDa EverandCase-Based Device Therapy for Heart FailureUlrika Birgersdotter-GreenNessuna valutazione finora
- Preoreoperative Cardiac AssessmentDocumento71 paginePreoreoperative Cardiac AssessmentHossam atefNessuna valutazione finora
- CH F ManagementDocumento38 pagineCH F ManagementShafid HamzabNessuna valutazione finora
- Strain 3Documento7 pagineStrain 3Mustafa Beyazıt AlkanNessuna valutazione finora
- View Topic Percutaneous Coronary Intervention Overview: December 2014Documento49 pagineView Topic Percutaneous Coronary Intervention Overview: December 2014Siska Prima OlimvianiNessuna valutazione finora
- RANASINGHE Cardiac Function & Disease & AnesthesiaDocumento51 pagineRANASINGHE Cardiac Function & Disease & AnesthesiaDagimNessuna valutazione finora
- Principle and Practice of Cardiac Mechanic For Assessing LV FunctionDocumento33 paginePrinciple and Practice of Cardiac Mechanic For Assessing LV FunctionSofia Kusumadewi100% (1)
- Braunwald: Chronic Coronary Artery DiseaseDocumento122 pagineBraunwald: Chronic Coronary Artery Diseaseusfcards100% (1)
- Atwater 2020Documento6 pagineAtwater 2020Vlada SiricNessuna valutazione finora
- Bibliografia 6Documento7 pagineBibliografia 6mrcristian_17892Nessuna valutazione finora
- Cardiac Resynchronization Therapy and Cardiac Contractility Modulation in Patients With Advanced Heart FailureDocumento8 pagineCardiac Resynchronization Therapy and Cardiac Contractility Modulation in Patients With Advanced Heart FailuresunhaolanNessuna valutazione finora
- CHF Dan CBFDocumento5 pagineCHF Dan CBFRisky Ilona SaputraNessuna valutazione finora
- Cardiac Resynchronisation Therapy For Patients With Heart FailureDocumento5 pagineCardiac Resynchronisation Therapy For Patients With Heart FailureIpar DayNessuna valutazione finora
- CardiologyDocumento102 pagineCardiologyashrafholailNessuna valutazione finora
- Interpreting The Athlete's ECGDocumento10 pagineInterpreting The Athlete's ECGVaniaAlmiraNessuna valutazione finora
- Syntax Score and Its Relation To Lipoprotein A - LP (A) and Extended Lipid Parameters in Non-Diabetic Patients With Acute Coronary Syndrome Having Age Below 55 YearsDocumento7 pagineSyntax Score and Its Relation To Lipoprotein A - LP (A) and Extended Lipid Parameters in Non-Diabetic Patients With Acute Coronary Syndrome Having Age Below 55 YearsPremier PublishersNessuna valutazione finora
- Vimal PAD - SlidesDocumento53 pagineVimal PAD - SlidesVimal NishadNessuna valutazione finora
- Essential Jazz Ear Training Exercises - The Jazz Guitar Blog PDFDocumento6 pagineEssential Jazz Ear Training Exercises - The Jazz Guitar Blog PDFRickCohenNessuna valutazione finora
- SAUNA - Rhonda PatrickDocumento33 pagineSAUNA - Rhonda PatrickRickCohen100% (1)
- P4 GuitarDocumento20 pagineP4 GuitarLea Pav100% (1)
- Folk Music Trivia QuizesDocumento161 pagineFolk Music Trivia QuizesRickCohenNessuna valutazione finora
- (FITNESS) The New Aerobics - Dr. Kenneth CooperDocumento191 pagine(FITNESS) The New Aerobics - Dr. Kenneth CoopercoltsiversNessuna valutazione finora
- The Habits of MusicianshipDocumento15 pagineThe Habits of MusicianshipRickCohenNessuna valutazione finora
- Five Ways To Know Yourself - Shinzen Young, 2011Documento183 pagineFive Ways To Know Yourself - Shinzen Young, 2011Raj Narayanan67% (3)
- Guitar-Tabs-Rock-Guitar-Secrets Book PDFDocumento180 pagineGuitar-Tabs-Rock-Guitar-Secrets Book PDFSmart Bodies100% (10)
- An Introductory in Elementary Number TheoryDocumento171 pagineAn Introductory in Elementary Number TheoryHAMZAHSEQUATIONNessuna valutazione finora
- Heart AttackDocumento4 pagineHeart AttackMirella Lereleré100% (1)
- Bartoszko 2018Documento9 pagineBartoszko 2018Rian AprizaNessuna valutazione finora
- IndianJAnaesth607451-4566018 124100 PDFDocumento7 pagineIndianJAnaesth607451-4566018 124100 PDFhartoNessuna valutazione finora
- NSG 210 Study GuideDocumento25 pagineNSG 210 Study GuideyasserNessuna valutazione finora
- Lakunar and Outcome StrokeDocumento11 pagineLakunar and Outcome StrokesitialimahNessuna valutazione finora
- Pneumothorax and Pneumomediastinum: Dr. Emad EfatDocumento89 paginePneumothorax and Pneumomediastinum: Dr. Emad Efatinterna MANADONessuna valutazione finora
- Glucovance Tablet Salut Selaput 500 mg-5 MG - Metformin Hidroklorida-Glibenclaminde - DKL1715809217C1 - 2021 - 0Documento16 pagineGlucovance Tablet Salut Selaput 500 mg-5 MG - Metformin Hidroklorida-Glibenclaminde - DKL1715809217C1 - 2021 - 0Felesia MissyNessuna valutazione finora
- Dobutamine HydrochlorideDocumento16 pagineDobutamine HydrochlorideSepri Dwi Arista DasliyNessuna valutazione finora
- اسئلة تمريض شاملDocumento116 pagineاسئلة تمريض شاملAmin TahaNessuna valutazione finora
- E Cart MedicationsDocumento12 pagineE Cart Medicationsbalong1219Nessuna valutazione finora
- Q A 1Documento48 pagineQ A 1ChannelGNessuna valutazione finora
- Health Education - HypertensionDocumento10 pagineHealth Education - Hypertensionmohamad dildar100% (1)
- Anatomy of The Cardiovascular SystemDocumento75 pagineAnatomy of The Cardiovascular SystemM RazzaqNessuna valutazione finora
- Periodontics يرﻛﺷ ﺎﮭﻣ د: Periodontal management of medically compromised patientsDocumento8 paginePeriodontics يرﻛﺷ ﺎﮭﻣ د: Periodontal management of medically compromised patientsYehya Al KhashabNessuna valutazione finora
- Step 2 Medicine (UA) 2023 - Attempt Review6Documento60 pagineStep 2 Medicine (UA) 2023 - Attempt Review6berdaderagaNessuna valutazione finora
- Cholesterol Tri FoldDocumento2 pagineCholesterol Tri FoldJake PetrykowskiNessuna valutazione finora
- Side Effects of Drugs - Annual 33 - J. Aronson (Elsevier, 2011) WWDocumento1.122 pagineSide Effects of Drugs - Annual 33 - J. Aronson (Elsevier, 2011) WWAndrei E. HawayNessuna valutazione finora
- 2011 Cardiovascular Disease Prevention in WomenDocumento20 pagine2011 Cardiovascular Disease Prevention in WomenRafi UllahNessuna valutazione finora
- Myocarditis NEJM 2022Documento13 pagineMyocarditis NEJM 2022Πάνος ΣταγήςNessuna valutazione finora
- What Is Junk FoodDocumento8 pagineWhat Is Junk FoodMuhammad AdeelNessuna valutazione finora
- Medicine NuggetsDocumento12 pagineMedicine NuggetsFiaz medicoNessuna valutazione finora
- Dr. Nagula Praveen, MD, DMDocumento79 pagineDr. Nagula Praveen, MD, DMDr. RajibNessuna valutazione finora
- Thesis Statement Heart DiseaseDocumento7 pagineThesis Statement Heart Diseasexgkeiiygg100% (2)
- High Dose Vs Low Dose Statin in MaceDocumento9 pagineHigh Dose Vs Low Dose Statin in MaceErvan ZuhriNessuna valutazione finora
- Unstable Angina With Underlying DyslipidaemiaDocumento9 pagineUnstable Angina With Underlying DyslipidaemiaAiman ArifinNessuna valutazione finora
- 2013 ExamDocumento32 pagine2013 ExamJohn M. HemsworthNessuna valutazione finora
- CH17 Cardiac Surgery in The Adult 5th Edition 2018Documento26 pagineCH17 Cardiac Surgery in The Adult 5th Edition 2018ChengShiun ShiueNessuna valutazione finora
- Final Pathology PDFDocumento294 pagineFinal Pathology PDFabdeljelile100% (1)
- Case Study 29Documento2 pagineCase Study 29Edna MooreNessuna valutazione finora
- Science: Quarter 1, WK 2 - Module 2Documento31 pagineScience: Quarter 1, WK 2 - Module 2Andres Boni85% (13)