Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Rheumatology 2014 Ruiz Arruza 1470 6
Caricato da
juanabCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Rheumatology 2014 Ruiz Arruza 1470 6
Caricato da
juanabCopyright:
Formati disponibili
RHEUMATOLOGY
Rheumatology 2014;53:14701476
doi:10.1093/rheumatology/keu148
Advance Access publication 27 March 2014
Original article
Glucocorticoids and irreversible damage in patients
with systemic lupus erythematosus
Ioana Ruiz-Arruza1, Amaia Ugarte1, Ivan Cabezas-Rodriguez1,
Jose-Alejandro Medina1, Miguel-Angel Moran1 and Guillermo Ruiz-Irastorza1
Abstract
Objective. The aim of this study was to analyse the relationship between glucocorticoids and damage
accrual in SLE.
CLINICAL
SCIENCE
Results. By the fifth year, 188 patients (82%) had been treated with prednisone. Eighty-seven patients
(37.8%) had accrued damage at 5 years. Patients with damage at year 5 had received a higher mean daily
prednisone-4 dose (10.4 vs 6 mg/day, P < 0.001). The mean daily prednisone-4 dose was higher in
patients accruing glucocorticoid-attributable damage (11 vs 7 mg/day, P = 0.04). Patients taking mediumhigh doses of prednisone-4 had a higher risk of accruing damage than those taking no prednisone
[adjusted odds ratio (OR) 5.39, 95% CI 1.59, 18.27]. Patients taking mediumhigh doses of prednisone-4
were more likely to develop glucocorticoid-related damage than those on no prednisone (adjusted OR 9.9,
95% CI 1.1, 84). No differences were seen between patients on low doses and those on no prednisone.
The cumulative dose of i.v. methylprednisolone-4 was not associated with global or glucocorticoid-related
damage.
Conclusion. Prednisone causes damage in SLE. Doses <7.5 mg/day and methylprednisolone pulses are
not associated with damage accrual.
Key words: systemic lupus erythematosus, prednisone, methylprednisolone, glucocorticoids, avascular osteonecrosis, osteoporosis, diabetes mellitus, cataract.
Introduction
SLE is a complex disease with a wide clinical spectrum.
Despite the advent of new drugs, glucocorticoids remain
the most used therapy for lupus [1]. High doses of prednisone, usually 1 mg/kg/day, are recommended for severe
1
Autoimmune Diseases Research Unit, Department of Internal
Medicine, Biocruces Health Research Institute, Hospital Universitario
Cruces, University of the Basque Country, Bizkaia, The Basque
Country, Spain.
Submitted 7 October 2013; revised version accepted
13 February 2014.
Correspondence to: Guillermo Ruiz-Irastorza, Servicio de Medicina
Interna, Hospital Universitario Cruces, 48903 Bizkaia, Spain.
E-mail: r.irastorza@euskaltel.net
SLE manifestations, however, such recommendations
are not evidence based [2, 3].
Recent studies have identified different dosedependent mechanisms of action of glucocorticoids [2].
The genomic pathway is almost completely saturated at
doses of prednisone >30 mg/day [2]. This pathway, more
specifically the mechanism known as transactivation, is
responsible for most glucocorticoid-related adverse effects. In lupus, glucocorticoids have been related to
damage accrual [46]. On the other hand, non-genomic
pathways, with more potent and less toxic effects,
become active at doses >100 mg/day [3].
Indirect data suggest that lower doses of prednisone
can be used in lupus patients, with pulse methylprednisolone therapy constituting a good option in acute
! The Author 2014. Published by Oxford University Press on behalf of the British Society for Rheumatology. All rights reserved. For Permissions, please email: journals.permissions@oup.com
Downloaded from http://rheumatology.oxfordjournals.org/ by guest on October 22, 2014
Methods. We report an observational cohort study including 230 patients with SLE enrolled at diagnosis
with 5 years of follow-up. Damage was calculated using the SLICC damage index. Glucocorticoid-related
damage was defined as avascular osteonecrosis, osteoporotic fractures, diabetes mellitus or cataracts.
Prednisone doses were calculated at the end of the fourth year of follow-up (prednisone-4). A categorical
prednisone-4 variable was constructed: no prednisone, 47.5 mg/day (low dose), >7.5 mg/day (mediumhigh dose). The relationship between methylprednisolone pulses and damage was also tested.
Glucocorticoids and irreversible damage in patients with SLE
situations [3, 79]. Clinical and pharmacological studies
suggest that a safe cut-off for prednisone doses could
be around 7.5 mg/day, the limit between low and
medium dose [2, 5]. However, more data are needed in
order to confirm these observations.
This study aimed to analyse the relation between treatment with oral prednisone and damage accrual, both general and domain specific, during the first 5 years of the
disease course as measured by the SLICC damage index
(SDI) [10, 11]. As a secondary objective, we studied the
effects on damage of i.v. pulses of methylprednisolone.
Patients and methods
Patients
Prednisone cumulative doses were calculated from the
information contained in our database, completed with
data from the medical notes if needed. The mean dose
in two consecutive visits was calculated and multiplied by
the period of time between them. The cumulative dose
was obtained in this way and calculated on a yearly basis.
For the purposes of this study we used the dose of
prednisone received by the end of the fourth year of
follow-up (hence denominated prednisone-4), just before
the point when damage at 5 years could be first counted.
The absolute amount (in milligrams) obtained was transformed into the average daily dose (mg/day) by dividing
by the total number of days of follow-up (1461.6 days in 4
years).
In addition, a categorical variable, the prednisone-4
dose categories, was created according to the classification by Buttgereit et al. [2], based on the degree of saturation of the different glucocorticoid receptors implicated
in the genomic and non-genomic pathways. The average
daily prednisone dose was thus divided into low dose
(47.5 mg/day), medium dose (430 mg/day) and high
dose (>30 mg/day), however, given the small number of
patients on a high average daily dose of prednisone-4
(n = 5), medium and high categories were grouped for
the purposes of this study. Thus there were three prednisone-4 dose categories: no prednisone, low dose and
mediumhigh dose. The same categorical variable was
created for the average dose of prednisone received up
to the end of the first year (prednisone-1 dose categories).
This variable was used as a surrogate of prednisone-4 and
was only used for the time-dependent analysis (see next
section). Finally, the total dose of i.v. methylprednisolone
in 4 years was also calculated.
Statistical analysis
Damage and activity evaluation
Damage was calculated using the SDI [10]. The first SDI
score was calculated 6 months after the diagnosis of SLE,
as per definition. Damage at this point was designated as
early damage. SDI scores were then calculated on a
yearly basis. The following damage-related variables
were used for the analysis: any damage at 5 years (yes/
no categorical variable), SDI absolute score at 5 years
(SDI-5) and SDI variation between baseline and 5 years
(SDI 15), the latter accounting for new damage.
According to the definition of irreversible damage, SDI
scores can never decrease over time [10].
In order to analyse specific damage attributable to
glucocorticoids, the following SDI subcategories were selected: avascular osteonecrosis, osteoporotic fractures,
diabetes mellitus and cataracts. Cardiovascular damage
domains were not chosen, given the potential influence of
clinical and therapeutic variables other than glucocorticoids. Patients with early damage in any of these domains
(n = 5) were excluded from this subanalysis. In order to
adjust for lupus activity we used the mean SLEDAI
score [13] during years 14.
www.rheumatology.oxfordjournals.org
Descriptive data were generated, using percentages,
means and S.D.s. Univariate comparisons were made
using chi-square test, Fishers exact test or non-paired
Students t-test, as appropriate. Linear regression was
used to test the associations between SDI-5, SDI 15
and prednisone-4 dose. To analyse the relationship of
these final variables and prednisone-4 dose categories,
analysis of variance (ANOVA) with Bonferronis post hoc
analysis was used.
The associations between the average daily prednisone-4 dose and both SDI-5 and SDI 15 were adjusted
by means of multiple linear regression for variables potentially related to irreversible damage [1417]: gender, age
at SLE diagnosis, calendar year of diagnosis, mean
SLEDAI, presence of early damage, presence of proliferative LN and months on antimalarials by the fifth year of
follow-up. The same adjusting variables were used to test
the association of any damage accrual at year 5 with
prednisone-4 dose categories by means of logistic regression. In order to study the effect of i.v. pulses of methylprednisolone on damage accrual, the same analyses
with the same adjusting variables were made using the
1471
Downloaded from http://rheumatology.oxfordjournals.org/ by guest on October 22, 2014
All patients were included in the longitudinal LupusCruces cohort at the Autoimmune Diseases Research
Unit, Hospital Universitario Cruces, University of the
Basque Country. All patients joining the cohort met four
ACR criteria [12]. Patients are routinely assessed every
36 months unless clinical status requires more frequent
visits. Patients on long-term remission are seen on a
yearly basis. At each visit, clinical, laboratory and treatment data are incorporated into our database. All patients
joining the Lupus-Cruces cohort gave informed consent.
The local institutional review board of the Hospital
Universitario Cruces approved the study in compliance
with the Declaration of Helsinki. Among the 305 patients
included in the cohort at the time of this study, 53 patients
were excluded because their follow-up was <5 years and
22 patients because data were insufficient to calculate the
cumulative prednisone dose, most of them because the
diagnosis was made in other centres. Thus the final
number of patients included in the study was 230.
Assessment of glucocorticoid use
Ioana Ruiz-Arruza et al.
TABLE 1 Demographic and clinical variables at baseline
206/230 (90)
228/230 (99)
35.75 (15)
139/230 (60)
120/230 (5)
73/230 (32)
29/230 (13)
41/230 (18)
33/230 (14)
60/230 (26)
45/230 (20)
26/230 (11)
12/230 (5)
18/230 (8)
41/208 (19)*
28/230 (12)
50/230 (22)
6/230 (3)
0.23 (0.54)
8.07 (5.9)
2.16 (3.3)
SDI: SLICC damage index. aMissing data in 22 patients.
total methylprednisolone dose in 4 years instead of prednisone-4 variables.
With regard to the association of prednisone-4 dose category and the development of glucocorticoid-attributed
damage at 5 years, adjustment was made by gender,
age at diagnosis, calendar year of diagnosis, aPL and
months on calcium plus vitamin D by the end of the fourth
year, all potentially influencing the risk of osteoporotic
fractures, osteonecrosis, cataracts and/or diabetes
mellitus [3].
We also analysed the time-dependent effects of prednisone on first damage accrual. Therefore patients with
early damage (n = 42) were excluded from this analysis.
The remaining 188 patients were divided into four
groups according to prednisone-1 dose category (no
prednisone, low, medium or high dose). Free-of-damage
cumulative survival rates up to year 5 were calculated for
each dose category and compared by means of the logrank test. A time to first damagedependent Cox regression was built, with prednisone-1 dose category as the
main independent variable and gender, age at diagnosis,
calendar year of diagnosis and mean SLEADI at year 1 as
adjustment variables.
Results
Baseline features and drug therapy during follow-up
Two hundred and thirty patients were included in the
study. Baseline demographic and clinical variables are
shown in Table 1. By the end of the fourth year of
follow-up, 188 patients (82%) had been treated with oral
prednisone. Prednisone-4 variables are shown in Table 2.
During the 4-year follow-up, antimalarials were ever used
by 118 patients (51%), 20 patients (9%) were treated with
1472
Damage
Forty-two patients (18.3%) had early damage. This
number increased to 87 (37.8%) at 5 years. The mean
SDI increased from 0.23 at baseline to 0.62 at year 5
(P < 0.001). The distribution of damage by specific SDI
domain is shown in Table 3.
Prednisone-4 and damage at year 5
Compared with patients with no damage, patients with
any damage at year 5 had received a higher cumulative
prednisone-4 dose (15.3 vs 8.9 g) and a higher mean
daily prednisone-4 dose (10.4 vs 6 mg/day) (P < 0.001
for both comparisons) (Table 4). Statistically significant
associations were found between the average daily
prednisone-4 dose and both SDI-5 (P = 0.001) and SDI
15 (P = 0.02). By the end of year 5, damage was accrued
by 9/42 (21%) patients on no prednisone, 29/96 (30%)
of those on low doses and 49/92 (53%) of those receiving
mediumhigh doses of prednisone-4 (P < 0.001).
Prednisone-4 dose category was statistically related to
both SDI-5 (P = 0.008) and SDI 15 (0.012). In the post
hoc analyses, significant differences for SDI-5 and SDI
15 were seen between no prednisone and mediumhigh
doses (P = 0.013 and 0.02, respectively). Statistical trends
were found between low and mediumhigh doses
(P = 0.07 and P = 0.08, respectively).
Damage attributable to glucocorticoids
Eighteen patients developed new damage attributable to
glucocorticoids: cataracts in 6 patients, osteoporotic fractures in 7 patients, avascular necrosis in 4 patients and
diabetes mellitus in 2 patients. One patient accrued
damage in two domains.
The mean prednisone-4 cumulative dose and the mean
average daily prednisone-4 dose were higher in patients
accruing damage attributable to glucocorticoids compared with those with no damage: 16.4 vs 10.5 g and 11
vs 7 mg/day, respectively (P = 0.04 for both comparisons)
(Table 4). The analysis using prednisone-4 dose category
yielded similar results: damage attributable to glucocorticoids was present in 1/41 (2.5%) patients on no prednisone, in 4/96 (4%) of those on low doses and in 13/88
(15%) of those on mediumhigh doses (P = 0.01).
The four patients who suffered osteonecrosis had
received average daily doses of prednisone > 7.5 mg/day
up to the time of the occurrence of the event (13, 14, 18
and 37 mg/day, respectively). Similar data were seen in six
of seven patients suffering osteoporotic fractures (8.6, 12,
15, 19, 28 and 60 mg/day), with only a 63-year-old woman
receiving a mean dose of 6.2 mg/day over 3 years.
All patients with cataracts also received prednisone at
medium average doses (8.4, 8.6, 10, 13 and 30 mg/day,
respectively) except for a 74-year-old woman who suffered this complication during the first year of follow-up.
www.rheumatology.oxfordjournals.org
Downloaded from http://rheumatology.oxfordjournals.org/ by guest on October 22, 2014
Women, n/N (%)
Caucasian, n/N (%)
Age at SLE diagnosis, mean (S.D.)
Year of diagnosis after 1990, n/N (%)
Anti-DNA antibodies, n/N (%)
Anti-Ro antibodies, n/N (%)
Anti-La antibodies, n/N (%)
Anti-RNP antibodies, n/N (%)
Anti-Sm antibodies, n/N (%)
aPL, n/N (%)
LN, n/N (%)
Class IIIIV LN, n/N (%)
CNS involvement, n/N (%)
APS, n/N (%)
Smoker, n/N (%)
Hypertension, n/N (%)
Hypercholesterolaemia, n/N (%)
Diabetes mellitus, n/N (%)
SDI at 6 months, mean (S.D.)
Maximum SLEDAI in the first year, mean (S.D.)
Minimum SLEDAI in the first year, mean (S.D.)
CYC, 49 patients (21%) ever received AZA, 12 patients
(5%) were treated with MTX and 9 patients (4%) received
MMF.
Glucocorticoids and irreversible damage in patients with SLE
TABLE 2 Treatment with glucocorticoids by the end of year 4
Prednisone-4 ever users, n/N (%)
Cumulative prednisone-4 dose, mean (S.D.), mg
Average prednisone-4 daily dose, mean (S.D.), mg/day
Prednisone-4 dose category, n/N (%)
Prednisone-4 dose category, average daily dose, mean (S.D.), mg/day
No prednisone
Low dose
Medium dose
High dose
No prednisone
Low dose
Medium dose
High dose
Methylprednisolone-4 cumulative dose, mean (S.D.), mg
188/230 (82)
11 322 (11 903)
7.7 (8)
42/230 (18)
96/230 (42)
87/230 (38)
5/230 (2)
0 (0)
3.8 (2.0)
14.0 (5.4)
38.2 (8.4)
164 (629)
Prednisone-4: prednisone at the end of the fourth year of follow-up; methylprednisolone-4: methylprednisolone at the end of
the fourth year of follow-up.
Type of damage
Cardiovascular, n/N (%)
Renal, n/N (%)
Gonadal failure, n/N (%)
Malignancy, n/N (%)
Peripheral vascular, n/N (%)
Diabetes, n/N (%)
Neuropsychiatric, n/N (%)
Gastrointestinal, n/N (%)
Pulmonary, n/N (%)
Ocular, n/N (%)
Skin, n/N (%)
Musculoskeletal, n/N (%)
6 months
7/230
7/230
5/230
4/230
4/230
4/230
3/230
3/230
3/230
2/230
1/230
1/230
(3)
(3)
(2)
(1.7)
(1.7)
(1.7)
(1.3)
(1.3)
(1.3)
(0.9)
(0.4)
(0.4)
5 years
12/230
11/230
6/230
9/230
10/230
6/230
12/230
9/230
9/230
10/230
6/230
14/230
(5.2)
(4.8)
(2.6)
(3.9)
(4.3)
(2.6)
(5.2)
(3.9)
(3.9)
(4.3)
(2.6)
(6)
Only one of the two cases with diabetes was treated with
prednisone, at a mean dose of 45 mg/day.
Multivariable analysis
The effect of the average daily prednisone-4 dose on SDI5 persisted after adjusting for gender, age at diagnosis,
calendar year of diagnosis, mean SLEDAI, presence of
early damage, proliferative nephritis and cumulative
months on antimalarials by year 5 (adjusted R2 = 0.51,
P = 0.009). Similar results were obtained for the dependent
variable SDI 15 (adjusted R2 = 0.14, P = 0.009). Patients
taking mediumhigh doses of prednisone-4 had a higher
risk of accruing damage than those taking no prednisone
[adjusted odds ratio (OR) 5.39, 95% CI 1.59, 18.27]; no
differences were seen between the latter and patients on
low prednisone-4 doses (adjusted OR 1.65, 95% CI 0.53,
5.10) (Table 5).
In damage attributable to glucocorticoids, the mean
daily prednisone-4 dose was a significant independent
predictor after adjusting for gender, age at diagnosis,
www.rheumatology.oxfordjournals.org
cumulative months on vitamin D treatment, aPL positivity
and calendar year of diagnosis (adjusted OR 1.07, 95% CI
1.01, 1.13). Likewise, patients taking mediumhigh doses
accrued damage attributable to glucocorticoids more frequently than patients on no prednisone (adjusted OR 9.9,
95% CI 1.1, 84), while no differences were seen between
patients receiving low doses and those on no prednisone
treatment (adjusted OR 1.7, 95% CI 0.17, 17) (Table 5).
Survival analysis
Among the 188 patients without early damage, 50 patients
(27%) received no prednisone, 43 patients (23%) were
treated with low doses, 81 patients (43%) with medium
doses and 14 patients (7%) with high doses. There was a
significant correlation between prednisone-1 and prednsione-4 dose categories (McNemar test, P < 0.001).
The mean daily dose of prednisone-4 was 1.2, 4.4, 9.5
and 22.1 mg/day, respectively, in patients on no prednisone, low, medium and high prednisone-1 doses
(P < 0.001).
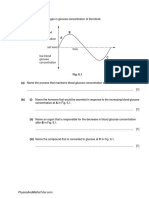
Forty-five patients (24%) accrued damage within the
first 5 years of follow-up. The cumulative free-of-damage
survival in patients treated with no prednisone, low,
medium and high doses was 86%, 73%, 64% and 44%,
respectively (P = 0.008) (Fig. 1). Compared with patients
on no prednisone, a significantly higher risk of accruing
damage was seen among patients treated with high doses
of prednisone-1 [adjusted hazard ratio (HR) 7.2, 95% CI
2.2, 23.1] and a borderline trend among those on medium
doses (adjusted HR 2.4, 95% CI 0.96, 6.2). In contrast, the
risk was not higher for patients treated with low doses of
prednisone-1 (adjusted HR 1.7, 95% CI 0.60, 4.87).
Methylprednisolone and damage
The cumulative dose of i.v. methylprednisolone-4 was not
associated with either the absolute SDI score or the SDI
15 after adjusting for age at SLE diagnosis, calendar year
of diagnosis, gender, mean maximum SLEDAI, presence
of early damage, presence of proliferative LN and months
on antimalarials by the fifth year of follow-up (P = 0.94 in
1473
Downloaded from http://rheumatology.oxfordjournals.org/ by guest on October 22, 2014
TABLE 3 Distribution of damage at first (6 months) and
last (5 years) assessments
Ioana Ruiz-Arruza et al.
TABLE 4 Average prednisone dose and damage accrual at 5 years
Any damage at year 5
Yes (n = 87) No (n = 143) P-value
Cumulative prednisone-4 dose,
mean (S.D.), g
Average prednisone-4 daily dose,
mean (S.D.), mg/day
Glucocorticoid-related damage at year 5
Yes (n = 18)
No (n = 207)
10.5 (11.5)
15.3 (12.6)
8.9 (10.7)
<0.001
16.4 (10.7)
10.4 (8.6)
6 (7.3)
<0.001
11 (7.4)
7 (7.9)
P-value
0.04
0.04
Prednisone-4: prednisone at the end of the fourth year of follow-up.
TABLE 5 Prednisone dose category and damage accrual at 5 years: multivariable analysis
No prednisone
Low dose
Mediumhigh dose
Glucocorticoid-related
damage at year 5 b, OR (95% CI)
Reference
1.65 (0.53, 5.10)
5.39 (1.59, 18.27)
Reference
1.71 (0.17, 17)
9.9 (1.1, 84)
Adjusted by gender, age at diagnosis, calendar year of diagnosis, mean SLEDAI, presence of early damage, proliferative
nephritis and months on antimalarials at the end of the fourth year. bAdjusted by gender, age at diagnosis, weeks on vitamin D
at the end of fourth year, aPL and calendar year of diagnosis. OR: odds ratio; prednisone-4: prednisone at the end of the
fourth year of follow-up.
both analyses). Likewise, there was no correlation between the cumulative i.v. methylprednisolone-4 and
damage attributable to glucocorticoids, adjusted by sex,
age at diagnosis, months on vitamin D treatment, aPL
positivity and calendar year of diagnosis (adjusted OR
1.0, 95% CI 0.99, 1.001).
FIG. 1 KaplanMeier survival free-of-damage curves
according to prednisone dose received during the first
year of follow-up
Discussion
Our results confirm that prednisone is associated with
damage accrued within the first 5 years following the diagnosis of SLE. A threshold has been identified, since average doses of prednisone >7.5 mg/day were associated
with damage accrual and doses <7.5 mg/day were not.
Irreversible organ damage is a primary outcome in SLE.
It is accrued during the course of lupus, not only caused
by the disease itself, but also by therapy. The SDI, divided
into 38 items grouped in 12 organ systems, quantifies
damage [9] and has been found to be a strong predictor
of mortality [18]. In 2004 we reported that patients in the
Lupus-Cruces cohort with a 1-year SDI >1 had lower
long-term survival rates [19]. Decreased quality of life
and increased economic burden have both been associated with damage [20]. Therefore preventing organ
damage accrual should be one of the main objectives of
lupus therapy, far beyond controlling SLE activity.
The relationship between glucocorticoids and damage
has been investigated by several groups. In 1998 Nossent
et al. [21] analysed the association of damage with corticosteroid therapy in a cohort of 90 Afro-Caribbean patients. The mean SDI scores were similar in corticosteroid
1474
Low dose: 47.5 mg/day; medium dose: 430 mg/day;
high dose: >30 mg/day.
users vs non-users (2.7 vs 2.04, respectively) and patients
who received high prednisone doses did not accrue more
damage than those who did not. The small sample size,
the specific geographic location (Netherlands Antilles) and
the very low survival rates of the cohort (62% at 10 years,
52% at 15 years) made it difficult to generalize these
results.
In 2000, Zonana-Nacach et al. [4] analysed the effect of
glucocorticoids on damage in the Hopkins Lupus Cohort.
www.rheumatology.oxfordjournals.org
Downloaded from http://rheumatology.oxfordjournals.org/ by guest on October 22, 2014
Prednisone-4 dose category
Any damage
at year 5 a, OR (95% CI)
Glucocorticoids and irreversible damage in patients with SLE
www.rheumatology.oxfordjournals.org
analysis of damage associated with methylprednisolone
may be somewhat conditioned by the usual prescription
in our unit of pulses 4500 mg. Thus, whether higher
doses of 1 g can cause damage accrual, as well as
other side effects such as infections [23], cannot be
addressed from our results.
On the other hand, this study has important strengths.
We have analysed not only the presence of damage
accrued as a dichotomized variable, but also quantified
it by using the SDI. For the first time, new damage after
the initial 6-month assessment and new glucocorticoidattributable damage have been used as outcomes in
order to analyse damage accrued after the initiation of
steroid therapy. It is well known that patients with
damage tend to accrue more damage, thus the variable early damage was used to control for this in the
multivariate analyses. Other adjustment variables
were included, such as those related to disease activity/
severity, gender, age, calendar year of diagnosis and
treatment with antimalarials. A number of different variables have been constructed to analyse the effects
of glucocorticoids. A time-dependent analysis using the
surrogate variable average daily prednisone-1 has been
included in order to overcome the potential bias of
damage accrued before the fifth year of follow-up. All
the analyses performed led to the same point: long-term
prednisone at average doses >7.5 mg/day can cause
irreversible organ damage in lupus.
Damage caused by glucocorticoids is generally
believed to be the inevitable price to pay for controlling
lupus activity. However, this assumption is based on
custom rather than on solid evidence [3]. In a recent
study by our group, a medium-dose prednisone-based
regime was compared with a high-dose prednisone,
NIH-based protocol for the induction therapy of biopsyproven LN [24]. In the former regimen, prednisone was
rapidly tapered and combined with pulse methylprednisolone, HCQ and CYC. This therapy resulted in an average
prednisone dose at 6 months of 9 mg/day, compared
with 25 mg/day in the high-dose regime. Toxicity was
significantly lower, including metabolic side effects,
osteonecrosis and osteoporotic fractures, and, remarkably, the medium-dose regimen resulted in a more rapid
and sustained renal response, with 100% of patients
eventually achieving complete response vs 70% of patients treated with high doses. Other groups have
reported good response of LN to regimens using doses
of prednisone <20 mg/day [7] or even to oral steroid-free
protocols including rituximab and MMF [25].
Every effort should be made to minimize the unwanted
effects of prednisone without giving up the huge antiinflammatory potential of glucocorticoids. The use of
pulse therapy instead of high oral doses in periods of disease activity, the early association of immunosuppressive
drugs and the universal baseline therapy with HCQ are
simple measures that can contribute to the goal of discontinuing prednisone or, at least, using it at low
doses. We should always keep in mind that one of the
main commitments to our patients is not causing with
1475
Downloaded from http://rheumatology.oxfordjournals.org/ by guest on October 22, 2014
Using a time-dependent model adjusted by gender, race
and age at diagnosis, the cumulative glucocorticoid dose
was associated with specific permanent organ damage:
osteoporotic fractures, avascular necrosis, cataracts, coronary artery disease and diabetes mellitus. A subsequent
analysis showed that the cumulative prednisone dose
maintained the association with osteoporotic fractures,
coronary artery disease and cataracts while the risk of
avascular necrosis and stroke was dependent on high
prednisone doses.
The same group created a weighted model some
years later [5]. The risk of damage accrual increased
with the cumulative prednisone dose, even after adjusting
for multiple variables, including baseline SLE activity.
Such risk tended to increase from the equivalent to 6
mg/day. This study did not analyse specific subtypes of
damage.
In 2003, Gladman et al. [6] studied damage accrual patterns in an inception cohort of 73 patients during the first
15 years of follow-up. They identified SDI domains that
could be related to prednisone use by creating three categories: definitely, possibly or not related. The contribution
of prednisone to damage was lower in early disease,
increasing over time and constituting the highest burden
of damage at 15 years. The musculoskeletal domain
was the most frequently scored domain, followed by the
cardiovascular and neuropsychiatric domains.
Confounding by indication has been claimed as a limitation to attributing damage accrual to glucocorticoids.
However, and despite one isolated link with vertebral fractures [22], methylprednisolone pulses, usually given to
patients with high activity, have not been associated
with increased damage [4], and were not associated in
this study. The inclusion in multivariable models of activity-related variables such as SLEDAI, use of immunosuppressive drugs or specific organ involvement can also
contribute to minimize the influence of confounding by
indication.
This study has a number of limitations. First, this is an
observational cohort study, with treatments prescribed at
the discretion of the attending physicians. Twenty-two patients from the cohort had to be excluded from the study
due to lack of enough data to calculate prednisonerelated variables. Second, our cohort was almost entirely
composed of Caucasians with full access to public health
care, and therefore with a potential better prognosis than
other groups of different ethnic/geographic origin. Indeed,
the mean SDI at the fifth year of follow-up was somewhat
lower in our patients than in those from the Toronto cohort
(0.62 vs 0.8) [8]. Third, we performed an analysis of
damage at 5 years of follow-up, looking for associations
with prednisone received up to that point. However, some
patients accrued damage earlier, with the consequent
miscalculation of the prednisone dose received up to
the time of actual damage accrual. Fourth, we analysed
damage accrued within 5 years after the diagnosis of SLE,
a time of observation that may not be long enough to assess the predictors of damage that might appear later in
the disease course, like cardiovascular domains. Fifth, the
Ioana Ruiz-Arruza et al.
our interventions more harm than the disease we are
aiming to treat.
Rheumatology key messages
Prednisone therapy is associated with damage
accrual in patients with SLE.
. Doses of prednisone <7.5 mg/day do not cause
global or glucocorticoid-related damage in patients
with SLE.
. Methylprednisolone pulses are not related to new
damage accrual in patients with lupus.
.
Acknowledgements
Disclosure statement: The authors have declared no
conflicts of interest.
References
1 Lateef A, Petri M. Unmet medical needs in systemic lupus
erythematosus. Arthritis Res Ther 2012;14(Suppl 4):S4.
2 Buttgereit F, Straub RH, Wehling M, Burmester GR.
Glucocorticoids in the treatment of rheumatic diseases: an
update on the mechanisms of action. Arthritis Rheum
2004;50:340817.
3 Ruiz-Irastorza G, Danza A, Khamashta M. Glucocorticoid
use and abuse in SLE. Rheumatology 2012;51:114553.
4 Zonana-Nacach A, Barr SG, Magder LS, Petri MA.
Damage in systemic lupus erythematosus and its association with corticosteroids. Arthritis Rheum 2000;43:
18018.
5 Thamer M, Hernan MA, Zhang Y, Cotter D, Petri MA.
Prednisone, lupus activity and permanent organ damage.
J Rheumatol 2009;36:5604.
6 Gladman DD, Urowitz MB, Rahman P, Ibanez D, Tam L-S.
Accrual of organ damage over time in patients with systemic lupus erythematosus. J Rheumatol 2003;30:19559.
7 Fischer-Betz R, Chehab G, Sander O et al. Renal outcome
in patients with lupus nephritis using a steroid-free regimen of monthly intravenous cyclophosphamide: a prospective observational study. J Rheumatol 2012;39:
21117.
8 Ruiz-Irastorza G, Espinosa G, Frutos MA et al. Diagnosis
and treatment of lupus nephritis. Consensus document
from the systemic auto-immune disease group (GEAS) of
the Spanish Society of Internal Medicine (SEMI) and
Spanish Society of Nephrology (S.E.N.). Nefrologia 2012;
32:S135.
9 Badsha H, Edwards CJ. Intravenous pulses of methylprednisolone for systemic lupus erythematosus. Semin
Arthritis Rheum 2003;32:370377.
10 Gladman D, Ginzler E, Goldsmith C, Fortin P et al. The
development and initial validation of the Systemic Lupus
International Collaborating Clinics/American College
1476
11 Gladman DD, Urowitz MB, Goldsmith C. The reliability of
the Systemic Lupus International Collaborating Clinics/
American College of Rheumatology Damage Index in
patients with systemic lupus erythematosus. Arthritis
Rheum 1997;40:80913.
12 Hochberg MC. Updating the American College of
Rheumatology revised criteria for the classification of
systemic lupus erythematosus [letter]. Arthritis Rheum
1997;40:1725.
13 Gladman DD, Ibanez D, Urowitz MB. SLE Disease Activity
Index 2000. J Rheumatol 2002;29:28891.
14 Molad Y, Gorshtein A, Wysenbeek AJ et al. Protective
effect of hydroxychloroquine in systemic lupus erythematosus. Prospective long-term study of an Israeli cohort.
Lupus 2002;11:35661.
15 Alarcon GS, Roseman JM, McGwin G Jr et al. Systemic
lupus erythematosus in three ethnic groups. XX. Damage
as a predictor of further damage. Rheumatology 2004;43:
2025.
16 Fessler BJ, Alarcon GS, Mcgwin G et al. Systemic lupus
erythematosus in three ethnic groups: XVI. Association of
hydroxychloroquine use with reduced risk of damage
accrual. Arthritis Rheum 2005;52:147380.
17 Petri M, Purvey S, Fang H, Magder LS. Predictors of organ
damage in systemic lupus erythematosus: the Hopkins
Lupus Cohort. Arthritis Rheum 2012;64:40218.
18 Chambers SA, Allen E, Rahman A, Isenberg DA. Damage
and mortality in a group of British patients with systemic
lupus erythematosus followed up for over 10 years.
Rheumatology 2009;48:6735.
19 Ruiz-Irastorza G, Egurbide M-V, Ugalde J, Aguirre C. High
impact of antiphospholipid syndrome on irreversible organ
damage and survival of patients with systemic lupus
erythematosus. Arch Intern Med 2004;164:7782.
20 Meacock R, Dale N, Harrison MJ. The humanistic
and economic burden of systemic lupus erythematosus : a systematic review. Pharmacoeconomics 2013;31:
4961.
21 Nossent JC. SLICC/ACR damage index in Afro-Caribbean
patients with systemic lupus erythematosus: changes in
and relationship to disease activity, corticosteroid therapy
and prognosis. J Rheumatol 1998;25:6549.
22 Bultink IEM, Lems WF, Kostene PJ, Dijkmans BAC,
Voskuyl AE. Prevalence and risk factors for low bone
mineral density and vertebral fractures in patients with
systemic lupus erythematosus. Arthritis Rheum 2005;54:
204450.
23 Kong KO, Badsha H, Lian TY, Edwards CJ, Chng HH.
Low-dose pulse methylprednisolone is an effective
therapy for severe SLE flares. Lupus 2004;13:2123.
24 Ruiz-Irastorza G, Danza A, Perales I et al. Prednisone in
lupus nephritis: how much is enough? Autoimmun Rev
2014;13:20614.
25 Condon MB, Ashby D, Pepper RJ et al. Prospective
observational single-centre cohort study to evaluate the
effectiveness of treating lupus nephritis with rituximab and
mycophenolate mofetil but no oral steroids. Ann Rheum
Dis 2013;72:12806.
www.rheumatology.oxfordjournals.org
Downloaded from http://rheumatology.oxfordjournals.org/ by guest on October 22, 2014
Dr Ruiz-Arruza was supported by a grant from Fundacion
Jesus Gangoiti Barrera.
of Rheumatology damage index for systemic lupus
erythematosus. Arthritis Rheum 1996;39:3639.
Potrebbero piacerti anche
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Truth About: Autism in AdultsDocumento35 pagineThe Truth About: Autism in AdultsThe Next Generation of Steel100% (1)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5795)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1091)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Circulatory System Revision WorksheetDocumento4 pagineCirculatory System Revision WorksheetPoulomi Sengupta100% (1)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- 2017 Critical Care Pharmacy Drug Guideline Folder PDFDocumento182 pagine2017 Critical Care Pharmacy Drug Guideline Folder PDFDeniNessuna valutazione finora
- AINSHAMS - Master of DermatologyDocumento84 pagineAINSHAMS - Master of DermatologyMuhammad SammyNessuna valutazione finora
- TF CBTDocumento12 pagineTF CBTBrittany Wright PruittNessuna valutazione finora
- Drug Study AmierDocumento25 pagineDrug Study AmierKabang Moa100% (5)
- Basic Medical Survival SkillsDocumento2 pagineBasic Medical Survival SkillsSaira ZafarNessuna valutazione finora
- Final Health Report PDFDocumento2 pagineFinal Health Report PDFRAHUL SHARMANessuna valutazione finora
- 15 Principles of Management and Prevention of Odontogenic inDocumento24 pagine15 Principles of Management and Prevention of Odontogenic inVukasin VostinicNessuna valutazione finora
- Anemia of Chronic DiseaseDocumento2 pagineAnemia of Chronic DiseasejuanabNessuna valutazione finora
- Nutrition - TPN (Basics)Documento37 pagineNutrition - TPN (Basics)Giorgi BradNessuna valutazione finora
- Ann Rheum Dis 2013 Pope Annrheumdis 2013 203684Documento10 pagineAnn Rheum Dis 2013 Pope Annrheumdis 2013 203684juanabNessuna valutazione finora
- Artrosis 2014Documento8 pagineArtrosis 2014juanabNessuna valutazione finora
- Fiebre Chikungunya - Revisión.Documento24 pagineFiebre Chikungunya - Revisión.juanabNessuna valutazione finora
- Anti CCP, FR, VSG PCRDocumento6 pagineAnti CCP, FR, VSG PCRjuanabNessuna valutazione finora
- Budd-Chiari Syndrome: Phuong L. Doan, MD University of North Carolina Hospitals Morning Report April 22, 2005Documento24 pagineBudd-Chiari Syndrome: Phuong L. Doan, MD University of North Carolina Hospitals Morning Report April 22, 2005juanabNessuna valutazione finora
- STI College of Nursing - Assessment Tool, Drug Study and NCPDocumento2 pagineSTI College of Nursing - Assessment Tool, Drug Study and NCPdjanggo18Nessuna valutazione finora
- Anatomy and Physiology of Peptic UlcerDocumento16 pagineAnatomy and Physiology of Peptic UlcerDrNarayan KR100% (8)
- Case Study 11Documento28 pagineCase Study 11api-301883277Nessuna valutazione finora
- Muscle Weakness and Functional Disability in Patients With Myasthenia GravisDocumento6 pagineMuscle Weakness and Functional Disability in Patients With Myasthenia GravisshodhgangaNessuna valutazione finora
- ODB - Nursing Thera 2 (NLE)Documento2 pagineODB - Nursing Thera 2 (NLE)AP Pride Slear DeveraNessuna valutazione finora
- Biological Molecules 1 QPDocumento10 pagineBiological Molecules 1 QPClinton ChikengezhaNessuna valutazione finora
- Isolasi, Identifikasi Dan Uji Sensitivitas Antibiotik Terhadap Pasteurella Multocida Asal Sapi Yang Dipotong Di Rumah Pemotongan Hewan Oeba KupangDocumento9 pagineIsolasi, Identifikasi Dan Uji Sensitivitas Antibiotik Terhadap Pasteurella Multocida Asal Sapi Yang Dipotong Di Rumah Pemotongan Hewan Oeba KupangSekar ArumNessuna valutazione finora
- Journal of Biontology CarolDocumento1 paginaJournal of Biontology Carolapi-233979066Nessuna valutazione finora
- PSM SeminarDocumento33 paginePSM SeminarSamarth JainNessuna valutazione finora
- Original Article: Specific Learning Disabilities and Psychiatric Comorbidities in School Children in South IndiaDocumento8 pagineOriginal Article: Specific Learning Disabilities and Psychiatric Comorbidities in School Children in South IndiaMarilyn BucahchanNessuna valutazione finora
- Ointment Box OutlineDocumento1 paginaOintment Box OutlineDon Nestor Razon Jr.Nessuna valutazione finora
- Presentation 1Documento23 paginePresentation 1Anonymous HK3LyOqR2g100% (1)
- Tchernof2013 PDFDocumento46 pagineTchernof2013 PDFindahNessuna valutazione finora
- 2018 Article 61Documento11 pagine2018 Article 61gheaastridgayatriNessuna valutazione finora
- Fever With Rash (Peds)Documento13 pagineFever With Rash (Peds)Asish Geiorge100% (1)
- 1 800 805 7837Documento124 pagine1 800 805 7837Same Day STD TestingNessuna valutazione finora
- Appropriate Maximum Phlebotomy Volumes: Neonate, Infant and Pediatric PopulationDocumento2 pagineAppropriate Maximum Phlebotomy Volumes: Neonate, Infant and Pediatric PopulationEthiopia HagereNessuna valutazione finora
- Carcinoma Pancreas: Risk Factors: (A) Demographic FactorsDocumento4 pagineCarcinoma Pancreas: Risk Factors: (A) Demographic FactorsSakthi Annamalai.cNessuna valutazione finora
- The Mental Health Continuum Model: Healthy Reacting Injured ILLDocumento1 paginaThe Mental Health Continuum Model: Healthy Reacting Injured ILLViet Quang NguyenNessuna valutazione finora
- Food ToxicologyDocumento33 pagineFood ToxicologyAhmad HassunNessuna valutazione finora