Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
161 FTP
Caricato da
BayuAdjieDescrizione originale:
Titolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
161 FTP
Caricato da
BayuAdjieCopyright:
Formati disponibili
GENITAL PROBLEMS
31
TRENDS IN UROLOGY & MENS HEALTH OCTOBER/NOVEMBER 2010 www.trendsinurology.com
Testicular torsion: a
urological emergency
T
orsion of the testis is a urological
emergency occurring in approximately
17 per cent of acute scrotal presentations.
It can occur at any age, but accounts for
90 per cent of acute testicular pain in
adolescent males between the ages of 13
and 21.
PATHOPHYSIOLOGY
Torsion occurs when an excessively mobile
testis rotates on its cord structures,
impairing venous return, which leads to
venous congestion and oedema. This
results in reduced arterial blood inflow,
with subsequent ischaemia and infarction
of the testis if left uncorrected.
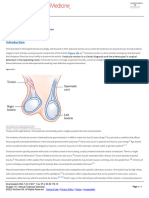
Testicular torsion may be divided into two
main types, depending on the anatomical
details of the axis of torsion. An
intravaginal torsion (Figure 1a), by far the
most frequent in adolescent boys, occurs
when the axis of rotation is within the
tunica vaginalis. In comparison, an
extravaginal torsion (Figure 1b) occurs
due to the tunica vaginalis having an
abnormally long attachment to the testis.
Testicular torsion is an emergency that all
health professionals should be aware of. The
authors outline the presentation, differential
diagnosis and need for rapid management.
Figure 1. Classification of types of testicular torsion: (a) intravaginal
torsion; (b) extravaginal torsion; (c) torsion due to long mesorchium
NIYUKTA THAKARE, KIERAN J. OFLYNN AND IAN PEARCE
Miss N. Thakare, MRCS, Clinical Fellow, Department of Urology,
Manchester Royal Infirmary; Mr K.J. OFlynn, FRCS, FRCSI(Urol),
Consultant Urological Surgeon, Department of Urology, Hope Hospital,
Salford; Mr I. Pearce, FRCS(Urol), Consultant Urological Surgeon,
Department of Urology, Manchester Royal Infirmary, Manchester
Thus the rotation is external to the tunica
vaginalis, which itself is also torted. This
variety of testicular torsion occurs mainly
in children. Males with a horizontal lie to
their testes, the so-called bell-clapper
deformity are more prone to developing
testicular torsion. This anatomical variant
arises as a result of the manner in which
the tunica vaginalis is reflected on the
testis and is bilateral in nature, thus
explaining the risk of subsequent
contralateral torsion in patients who have
experienced a testicular torsion. Testicular
torsion may also occur due to a long
mesorchium, often associated with
cryptorchidism (Figure 1c).
Recent studies have identified cold
ambient temperature and increased
humidity as risk factors for developing
testicular torsion.
1
The exact
pathophysiology of this is unknown.
PRESENTATION
While there may have been preceding
trauma to the genitals, this is not always
a
Twisted
cord
Tunica vaginalis
Mesorchium
b c
GENITAL PROBLEMS
32
www.trendsinurology.com TRENDS IN UROLOGY & MENS HEALTH OCTOBER/NOVEMBER 2010
the case and a significant number of
patients will present having been woken
from sleep with acute unilateral testicular
pain. Vomiting is not uncommon and one
should be cautious of right iliac fossa pain
mimicking appendicitis, especially in
children, who are notoriously poor at
localising pain. It is easy to miss the
diagnosis of testicular torsion in such
patients, particularly during the early phase
of presentation.
The duration of pain is of the utmost
importance it is almost always less than 24
hours in the presence of torsion, and usually
much less. Absence of infective symptoms
and signs such as dysuria, frequency and
pyrexia should increase suspicion, and the
aware patient will often be able to give
assurance as to previously normal testes with
an absence of palpable abnormalities.
Most patients with acute testicular pain
will present directly to the accident-and-
emergency unit, but where primary care is
the initial port of call, immediate referral to
the on-call urological team is mandatory.
On examination, the hemiscrotum in
question will be slightly swollen and
flushed. The testis may lie horizontally,
although this is not a universal feature.
This can be verified by observation of the
contralateral testis, which will have a
similar lie. The testis may also be high
riding (higher in position) compared with
its counterpart (Figure 2). While both of
these are useful clinical findings, neither is
pathognomonic, nor can their absence
exclude the diagnosis.
Palpation of the testis will reveal exquisite
tenderness. Elevation of the testis with the
patient in a supine position may worsen
the pain (Prehns sign). This may be a
useful sign to differentiate the diagnosis
from epididymo-orchitis, in which the pain
gets better with elevation. Absence of the
cremasteric reflex is the most useful
diagnostic indicator, with a sensitivity
approaching 100 per cent.
For some patients testicular torsion does
not present as an acute event usually
those with bell-clapper testes, suffering
from intermittent testicular torsion. These
patients typically present to primary care
complaining of acute, severe unilateral
testicular pain, which typically resolves
itself within minutes to hours. It is
uncommon to see such a patient in the
acute setting, and hence the diagnosis
is based upon a high index of suspicion.
If such a diagnosis is thought likely, a
urological referral should be made on a
semi-urgent basis for consideration of
bilateral testicular fixation (orchidopexy).
DIFFERENTIAL DIAGNOSIS
Torsion of testicular appendages
The hydatid of Morgagni is a common
testicular appendage embryologically
derived from the Mllerian
(paramesonephric) duct, whereas the
appendix epididymis is a remnant of the
mesonephric (Wolffian) duct. Torsion of
these structures is most common in a
younger age group than testicular torsion,
2
but must be kept in mind in all young men
presenting with an acute scrotum. The
presentation is similar to that of testicular
torsion, but on examination the scrotum,
whilst tender, does not display the degree
of erythema associated with testicular
torsion, nor is the testicular lie abnormal.
The blue dot sign may be present in the
upper half of the hemiscrotum where the
infarcted hydatid is visible through
tightened skin. However, it may be difficult
to visualise, and in its absence the
diagnosis may still be made if scrotal
tenderness is isolated to a hard nodule at
the upper pole of the testis.
If the patient presents to primary care, he
should be urgently referred to the on-call
urological team for further assessment.
Once testicular torsion is excluded, which
in many cases may be at the time of scrotal
surgical exploration, management consists
of either conservative treatment with
non-steroidal anti-inflammatory drugs or
surgical intervention in the form of scrotal
exploration and diathermy to the
appendage. This offers a much more rapid
resolution of the pain.
Epididymitis
In adult men, epididymitis is more common
than torsion,
2
but the latter must be
considered as delayed diagnosis may result
in testicular loss.
The patient typically presents with rapidly
progressive scrotal pain and swelling,
which radiates up the spermatic cord and
to the lower abdomen. The overlying skin
Most patients with acute testicular pain will present
directly to the accident-and-emergency unit, but where
primary care is the initial port of call, immediate
referral to the on-call urological team is mandatory
Figure 2. Clinical presentation of testicular
torsion with high-riding testis (courtesy of
Manchester Royal Infirmary Department of
Urology)
may be erythematous and the
inflammatory process may give rise to a
reactive secondary hydrocele. A midstream
urine culture should be routinely
performed to identify a urinary tract
infection. If the patient complains of
urethral discharge, a Gram stain should
be sent, which may reveal the presence
of intracellular diplococci (Neisseria
gonorrhoeae). If only white cells are
seen, the most likely diagnosis is non-
gonococcal urethritis.
If epididymo-orchitis does not resolve
within two weeks, the patient should be
referred for urgent urological assessment
for suspected testicular cancer.
3
Men over
the age of 50 years in whom a diagnosis of
epididymitis is suspected and proven
should be referred for routine urological
review to exclude any predisposing factors
to urinary tract infection, such as bladder
outflow obstruction or structural
abnormalities.
4
Other causes
Less common conditions to be considered
in the differential diagnosis of torsion
include trauma, hernia, hydrocele and
testicular tumour. Vasculitis due to
Henoch-Schnlein purpura may also
present as an acute scrotum.
5
INVESTIGATION
Dipstix urinalysis is the only mandatory
investigation and is typically negative with
testicular torsion. Other investigations such
as full blood count and urea are invariably
normal and time consuming.
The fundamental principle underlying the
management of testicular torsion is that
time is of the essence, with the chance of
testicular survival diminishing as time
progresses. Although occasionally reported,
testicular survival after eight hours of
torsion is extremely unlikely.
6
MANAGEMENT
Once referred for further assessment, if
torsion cannot be excluded, the patient
should undergo urgent surgical
exploration. Radiological investigations are
of questionable value since rapid diagnosis
and prompt scrotal exploration determine
testicular viability in the presence of
torsion. However, the role of Doppler
ultrasound is justifiable if the clinical
picture is doubtful and an experienced
radiologist is available. The presence of
arterial flow on colour Doppler in this
scenario can rule out torsion with an
accuracy of 97 per cent.
Informed consent prior to surgical
exploration should include counselling for
removal or fixation of the affected testis
depending on its viability, and for fixation
of the contralateral testis should the
diagnosis of torsion prove correct. It is
necessary to warn the patient and/or his
parents about the likelihood of an
orchidectomy if the testis is found to be
anything other than viable. The patient
must also be warned that testicular loss
will result in a degree of impaired fertility,
although this will usually be compensated
for by the female partner.
Typically testicular torsion is intravaginal,
ie it occurs within the tunica vaginalis.
Upon delivery of the testis, the twisted
cord is readily apparent and the testis itself
will be of a dark, dusky purple colour, the
intensity of which will be dictated by the
duration of the rotation (Figure 3).
Testicular torsion invariably involves a
rotation towards the midline and can
therefore be reversed by twisting the testis
laterally for the required number of turns.
The testis is then left to pink up as first
GENITAL PROBLEMS
33
TRENDS IN UROLOGY & MENS HEALTH OCTOBER/NOVEMBER 2010 www.trendsinurology.com
KEY POINTS
Testicular torsion is an emergency and requires rapid urological referral
The patient almost always presents with pain of less than 24 hours duration
Differential diagnosis includes torsion of testicular appendages and
epididymitis
Dipstix urinalysis is the only mandatory investigation and is typically negative
If torsion cannot be excluded, the patient should undergo urgent surgical
exploration
Figure 3. Peri-operative photograph of testicular torsion (courtesy of
Manchester Royal Infirmary Department of Urology)
GENITAL PROBLEMS
34
www.trendsinurology.com TRENDS IN UROLOGY & MENS HEALTH OCTOBER/NOVEMBER 2010
the venous congestion and then the
arterial insufficiency is allowed to resolve.
This may require up to 10 minutes wrapped
in a warm saline gauze.
If there is any doubt regarding its viability,
orchidectomy should be performed.
Antisperm antibodies may form if a non-
viable testis or one of doubtful viability is
left within the scrotum and consequently
the fertility of the remaining testis may be
compromised.
7
If the testis is deemed viable, a three-point
testicular fixation should be performed
using non-absorbable suture material. The
contralateral testis should also be fixed to
eliminate the risk of metachronous
contralateral torsion. Orchidopexy is not
indicated in the absence of torsion.
8
Cosmesis may also prove to be an issue for
the patient, but this is a personal thing and
by no means universal. Some patients cope
extremely well with the loss of a testis and
have no negative psychological sequelae.
Others will request the insertion of an
artificial testicular prosthesis. This should be
offered by the initial operating surgeon and
may be performed immediately or at any
stage in the future, as directed by the patient.
CONCLUSION
Testicular torsion is an emergency that all
health professionals should be aware of.
Knowledge of the mode of presentation
and anatomy of the testes is the key to
differentiate torsion from other causes
of acute scrotal pain. When testicular
torsion is suspected, immediate surgical
exploration is mandatory.
REFERENCES
1 Srinivasan AK, Freyle J, Gitlin JS, et al.
Climatic conditions and the risk of testicular
torsion in adolescent males. Urology
2007;178:25858.
2 Ben-Chaim J, Pinthus JH. Testicular torsion.
Eur Urol Update Ser 1998;7:3944.
3 Dearnaley D, Huddart R, Horwich A. Regular
review managing testicular cancer. BMJ
2001;322:15838.
4 Luzzi GA, OBrien TS. Acute epididymitis.
BJU Int 2001;87:74755.
5 Ioannides AS, Turnock R. An audit of the
management of the acute scrotum in
children with Henoch-Schonlein purpura.
J R Coll Surg Edinb 2001;46:989.
6 Cummings JM, Boullier JA, Sekhon D, et al.
Adult testicular torsion. J Urol 2002;167:210910.
7 Barsch G, Frank S, Marbeger J, et al.
Testicular torsion: late results with special
regard to fertility and endocrine function.
J Urol 1980;124:3758.
8 Pearce I, Islam S, McIntyre IG, et al.
Suspected testicular torsion: a survey of
clinical practice in Northwest England. J R
Soc Med 2002;94:2479.
FURTHER READING
1 Galejs LE. Diagnosis and treatment of the
acute scrotum. Am Fam Physician
1999;59:81724.
2 Kass EJ, Lundak B. The acute scrotum.
Paed Clin North Am 1997;44:125166.
Potrebbero piacerti anche
- Acute ScrotumDocumento9 pagineAcute ScrotumIsabel ReyNessuna valutazione finora
- Module 1 Acute Scrotum PDFDocumento11 pagineModule 1 Acute Scrotum PDFbayutrihatmajaNessuna valutazione finora
- Acute Scrotum PDFDocumento9 pagineAcute Scrotum PDFJody FelizioNessuna valutazione finora
- M 1: T A S: Odule HE Cute CrotumDocumento10 pagineM 1: T A S: Odule HE Cute CrotumROMANNessuna valutazione finora
- Torsio TestisDocumento55 pagineTorsio TestisAulia RizkiaNessuna valutazione finora
- Chapter 136 Pediatric Urologic and Gynecologic DisordersDocumento12 pagineChapter 136 Pediatric Urologic and Gynecologic Disordersemergency.fumcNessuna valutazione finora
- Testicular Torsion - StatPearls - NCBI BookshelfDocumento6 pagineTesticular Torsion - StatPearls - NCBI Bookshelfwijana410Nessuna valutazione finora
- The Acute ScrotumDocumento9 pagineThe Acute ScrotumAnastasia FebriantiNessuna valutazione finora
- Chapter 151. Manual Testicular DetorsionDocumento7 pagineChapter 151. Manual Testicular DetorsionRichard QiuNessuna valutazione finora
- Bowl in 2017Documento12 pagineBowl in 2017kafosidNessuna valutazione finora
- Acute Scrotum PDFDocumento9 pagineAcute Scrotum PDFthejaskamathNessuna valutazione finora
- Acute Scrotum, Differential DiagnosisDocumento57 pagineAcute Scrotum, Differential DiagnosisRajesh Menon100% (1)
- Escroto AgudoDocumento15 pagineEscroto Agudojuliandavid.chinomeNessuna valutazione finora
- Testicular TorsionDocumento5 pagineTesticular Torsionmohammed agungNessuna valutazione finora
- Acute ScrotumDocumento54 pagineAcute ScrotumIntan Eklesiana NapitupuluNessuna valutazione finora
- Torsio Testis2016Documento6 pagineTorsio Testis2016Patrico Rillah SetiawanNessuna valutazione finora
- Testicular Torsion, Hydrocele & Fournier GangreneDocumento41 pagineTesticular Torsion, Hydrocele & Fournier GangreneNur Insyirah100% (1)
- Testicular Torsion - ClinicalKeyDocumento10 pagineTesticular Torsion - ClinicalKeyWialda Dwi rodyahNessuna valutazione finora
- Mehu108 - U8 - T8 - Afecciones Del Escroto y Contenido3Documento18 pagineMehu108 - U8 - T8 - Afecciones Del Escroto y Contenido3Elaine Alondra Ortiz OrtizNessuna valutazione finora
- Acute Scrotum 231016 PDFDocumento50 pagineAcute Scrotum 231016 PDFDany Dias100% (1)
- Emergency Department Approach To Testicular Torsion: Two Illustrative CasesDocumento5 pagineEmergency Department Approach To Testicular Torsion: Two Illustrative CasesMega MahardikaNessuna valutazione finora
- Testicular TorsionDocumento18 pagineTesticular TorsionAviZhafira100% (3)
- 1843 1pqu7ccDocumento8 pagine1843 1pqu7ccOttofianus Hewick KalangiNessuna valutazione finora
- Pediatric EmergencyDocumento66 paginePediatric EmergencyWaseem MoukhtarNessuna valutazione finora
- Acutescrotalemergencies: Molly M. Bourke,, Joshua Z. SilverbergDocumento18 pagineAcutescrotalemergencies: Molly M. Bourke,, Joshua Z. SilverbergSebastian ChavesNessuna valutazione finora
- 25 UrologyDocumento47 pagine25 UrologyMahmoud AbuAwadNessuna valutazione finora
- GGGGDocumento18 pagineGGGGfatihahannisahumairaNessuna valutazione finora
- 31 Uro Hydrocele 111211112520 Phpapp02Documento6 pagine31 Uro Hydrocele 111211112520 Phpapp02ppc_20Nessuna valutazione finora
- 8412-Article Text-29472-1-10-20130809Documento8 pagine8412-Article Text-29472-1-10-20130809NenyNessuna valutazione finora
- Urological Science: Jiun-Hung Geng, Chun-Nung HuangDocumento4 pagineUrological Science: Jiun-Hung Geng, Chun-Nung Huangyerich septaNessuna valutazione finora
- Testicular Torsion Fani FinalDocumento31 pagineTesticular Torsion Fani Finalrockblaster80Nessuna valutazione finora
- 0616 SCuDocumento18 pagine0616 SCuYolanda Dwi OktaviyaniNessuna valutazione finora
- Anal Abscess and FistulaDocumento12 pagineAnal Abscess and FistulaGustavoZapataNessuna valutazione finora
- Fracture of The Penis - A ReviewDocumento6 pagineFracture of The Penis - A ReviewNatalindah Jokiem Woecandra T. D.Nessuna valutazione finora
- 13.2 Testicular Torsion - 1 Lecture-TZDocumento29 pagine13.2 Testicular Torsion - 1 Lecture-TZOjambo FlaviaNessuna valutazione finora
- Rhode Island Hospital: Related Emedicine TopicsDocumento6 pagineRhode Island Hospital: Related Emedicine TopicsApril Shane OreiroNessuna valutazione finora
- Pediatric and Adolescent Gynecologic Emergencies 2022Documento16 paginePediatric and Adolescent Gynecologic Emergencies 2022Felipe MayorcaNessuna valutazione finora
- Rectovaginal Fistulae: Bidhan Das, MD Michael Snyder, MDDocumento7 pagineRectovaginal Fistulae: Bidhan Das, MD Michael Snyder, MDNovaNessuna valutazione finora
- 10.1.1.546.6206 BedahDocumento7 pagine10.1.1.546.6206 Bedahfikri hanifNessuna valutazione finora
- 1 ScrotumDocumento7 pagine1 ScrotumMohamed Al-zichrawyNessuna valutazione finora
- Testicular Disorders Freeman 2013Documento56 pagineTesticular Disorders Freeman 2013Evan PermanaNessuna valutazione finora
- Avoiding Common Errors in The Emergency Department-801-1002Documento200 pagineAvoiding Common Errors in The Emergency Department-801-1002Hernando CastrillónNessuna valutazione finora
- Ovarian TorsionDocumento4 pagineOvarian TorsionRiko KuswaraNessuna valutazione finora
- Appendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenDocumento7 pagineAppendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenAndi HairunNessuna valutazione finora
- Acuteurologicalconditions 130121123140 Phpapp01Documento58 pagineAcuteurologicalconditions 130121123140 Phpapp01Dr. NasrumminallahNessuna valutazione finora
- Testicular TorsionDocumento20 pagineTesticular TorsionDarshan SinghNessuna valutazione finora
- Surgery NotesDocumento127 pagineSurgery NotesDawit KimNessuna valutazione finora
- Scrotal SwellingDocumento40 pagineScrotal Swellingeirene simbolonNessuna valutazione finora
- Disorders of Testicles & ScrotumDocumento10 pagineDisorders of Testicles & ScrotumAli SafaaNessuna valutazione finora
- Emergencia UrologicaDocumento13 pagineEmergencia UrologicaEduardo DV MunizNessuna valutazione finora
- Emergency Management of Penile Conditions - Our Institute ExperienceDocumento6 pagineEmergency Management of Penile Conditions - Our Institute ExperienceIJAR JOURNALNessuna valutazione finora
- Bladder Diverticulum and SepsisDocumento4 pagineBladder Diverticulum and SepsisInternational Medical PublisherNessuna valutazione finora
- Scrotal MassesDocumento19 pagineScrotal MassesJohnNessuna valutazione finora
- Scrotal Swelling2Documento26 pagineScrotal Swelling2bigtemptationNessuna valutazione finora
- 2017 Pediatric Testicular TorsionDocumento12 pagine2017 Pediatric Testicular TorsionVladimir BasurtoNessuna valutazione finora
- Ou Sumber4Documento14 pagineOu Sumber4AnggaNessuna valutazione finora
- Torsio Omentum 1Documento5 pagineTorsio Omentum 1prabowoaji12Nessuna valutazione finora
- Acute Scrotum: DR - Ameer Alaraji College of Medicine, Fabms, FJMC, High Speciality in UrologyDocumento63 pagineAcute Scrotum: DR - Ameer Alaraji College of Medicine, Fabms, FJMC, High Speciality in UrologyHaider Nadhem AL-rubaiNessuna valutazione finora
- Textbook of Urgent Care Management: Chapter 39, Ensuring Patient SafetyDa EverandTextbook of Urgent Care Management: Chapter 39, Ensuring Patient SafetyNessuna valutazione finora
- Acute Cough (Bronchitis) : 2011 UpdateDocumento4 pagineAcute Cough (Bronchitis) : 2011 UpdatecorsaruNessuna valutazione finora
- Gastroenteritis:: Diarrhea & DehydrationDocumento26 pagineGastroenteritis:: Diarrhea & DehydrationcorsaruNessuna valutazione finora
- BronchitisDocumento3 pagineBronchitiscorsaruNessuna valutazione finora
- C C W - B C - T M: U R T I (P, Urti, S, B) : (1) PharyngitisDocumento5 pagineC C W - B C - T M: U R T I (P, Urti, S, B) : (1) PharyngitiscorsaruNessuna valutazione finora
- Dyspepsia Management Guidelines: PrefaceDocumento9 pagineDyspepsia Management Guidelines: PrefacecorsaruNessuna valutazione finora
- Urticaria: Evaluation and Treatment: Paul Schaefer, MD, PHD, University of Toledo College of Medicine, Toledo, OhioDocumento7 pagineUrticaria: Evaluation and Treatment: Paul Schaefer, MD, PHD, University of Toledo College of Medicine, Toledo, OhiocorsaruNessuna valutazione finora
- Diarrhoea Audit KDRS1 - VanceDocumento1 paginaDiarrhoea Audit KDRS1 - VancecorsaruNessuna valutazione finora
- Acute GastroenteritisDocumento9 pagineAcute GastroenteritiscorsaruNessuna valutazione finora
- Epididymitis: (Epididymo-Orchitis)Documento4 pagineEpididymitis: (Epididymo-Orchitis)corsaruNessuna valutazione finora
- Presentation 3Documento30 paginePresentation 3corsaruNessuna valutazione finora
- Bladder InjuryDocumento7 pagineBladder InjurycorsaruNessuna valutazione finora
- SJS12002 62Documento5 pagineSJS12002 62corsaruNessuna valutazione finora
- Rupture of The Pubic Symphysis: Diagnosis, Treatment and Clinical OutcomeDocumento3 pagineRupture of The Pubic Symphysis: Diagnosis, Treatment and Clinical OutcomecorsaruNessuna valutazione finora
- Ankle FractureDocumento11 pagineAnkle FracturecorsaruNessuna valutazione finora
- Trauma Vesica LDocumento2 pagineTrauma Vesica LcorsaruNessuna valutazione finora