Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Detect Pleural Effusion with Simple Auscultatory Percussion
Caricato da
Diego Ortecho0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
31 visualizzazioni4 pagineThis document describes a study that assesses a new physical examination technique called auscultatory percussion (AP) for detecting pleural effusions. The study involved 293 inpatients, 118 with radiographic evidence of pleural fluid and 175 controls. Using AP, examiners were able to detect a fluid level in 113/118 patients with effusions, but none in controls, demonstrating high sensitivity (96%) and specificity (100%) of AP for detecting pleural fluid. AP is a simple, non-invasive technique that can detect as little as 50mL of pleural fluid and may help diagnose effusions unsuspected by other physical exams or chest x-rays.
Descrizione originale:
Titolo originale
Bf 02600204
Copyright
© © All Rights Reserved
Formati disponibili
PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoThis document describes a study that assesses a new physical examination technique called auscultatory percussion (AP) for detecting pleural effusions. The study involved 293 inpatients, 118 with radiographic evidence of pleural fluid and 175 controls. Using AP, examiners were able to detect a fluid level in 113/118 patients with effusions, but none in controls, demonstrating high sensitivity (96%) and specificity (100%) of AP for detecting pleural fluid. AP is a simple, non-invasive technique that can detect as little as 50mL of pleural fluid and may help diagnose effusions unsuspected by other physical exams or chest x-rays.
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
31 visualizzazioni4 pagineDetect Pleural Effusion with Simple Auscultatory Percussion
Caricato da
Diego OrtechoThis document describes a study that assesses a new physical examination technique called auscultatory percussion (AP) for detecting pleural effusions. The study involved 293 inpatients, 118 with radiographic evidence of pleural fluid and 175 controls. Using AP, examiners were able to detect a fluid level in 113/118 patients with effusions, but none in controls, demonstrating high sensitivity (96%) and specificity (100%) of AP for detecting pleural fluid. AP is a simple, non-invasive technique that can detect as little as 50mL of pleural fluid and may help diagnose effusions unsuspected by other physical exams or chest x-rays.
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 4
Auscultatory Percussion:
A Simple Met hod t o Detect Pleural Effusion
JOHN R. GUARINO, MD, JOE C. GUARINO, PhD, PE
Objective: To assess a new technique for the detection of f'ree pleural
fluid.
Design: 118 consecutive inpatients wi t h radiologic evidence of free
pleural fluid and a control group of 175 randomly selected inpatients
were examined over a three-year period in a prospective blind study
by auscultatory percussion (AP) for evidence of pleural effusion. The
cutoff in the percussion not e by AP is strikingly loud and sharp at the
fluid level and allows precise delineation of even minimal amounts of
pleural fluid. The fluid level was measured in reference to the last rib.
The criterion for detection of pleural effusion by AP was a demon-
strable horizontal fluid level at the sound cutoff across the posterior
hemithorax above the last rib that shifted with lateral tilt.
Setting: A general medical and surgical university-affiliated teaching
Veterans Affairs hospital.
Patients~participants: All inpatients were eligible. Ready availability
of examiners was essential. Rotating third- and fourth-year medical
students, residents, and senior staff members participated.
Interventions: None.
Maj or results: 113 of the 118 patients with radiologic evidence of
pleural effusion had a distinct horizontal fluid level above t he last rib
that shifted with lateral tilt (sensitivity = 95.8% ). None of the 175
control patients examined at random showed evidence of pleural ef-
fusion by AP examination, which was confirmed by chest radiography
(specificity = 100% ). Nine of the 175 patients wi t hout radiologic
evidence of pleural effusion had elevated diaphragms that simulated
a fluid level in the examination by AP. Each of the nine patients,
however, had no shift in the level with lateral tilt. Subpulmonic ef-
fusions were readily displaced and identified by this met hod of AP.
Conclusions: Examination by AP is highly sensitive and specific for
the detection of free pleural fluid, even in the presence of obesity,
thickened pleura, lung masses, pneumonia, and associated lung disease.
The examination correlates closely with standard and lateral decubitus
chest radiography. Pleural effusion unsuspected by conventional means
of physical examination and undetectable by standard chest radiog-
raphy can readily be det ect ed by the met hod of AP. The examination
is easy to do and is particularly suited to enhance det ect i on of pleural
effusion. As little as 50 mL of free pleural fluid can be detected.
Key words: auscultatory percussion; pleural effusion; examination of
chest; auscultation of chest; percussion of chest.
J GEN INTERN MED 1994;9;71-74.
PLEURAL EFFUSION i s a f r e q u e n t ma n i f e s t a t i o n o f s e r i o u s
p l e u r o p u l mo n a r y , c a r d i a c , o r e x t r a t h o r a c i c d i s e a s e a n d
n e c e s s i t a t e s s p e c i f i c d i a g n o s i s . Wh e n t h e p a t i e n t is u p -
r i ght , 3 0 0 t o 5 0 0 mL o f f r e e p l e u r a l f l u i d ma y c o l l e c t i n
t h e p o s t e r i o r c o s t o p h r e n i c s u l c u s b u t r e ma i n o b s c u r e d
b y t h e d i a p h r a g m b e f o r e i t b e c o me s d e t e c t a b l e b y t h e
u s u a l me a n s o f p h y s i c a l e x a mi n a t i o n a n d r o e n t g e n o -
g r a p h i c s t u d i e s . 1-3 T h e c o n v e n t i o n a l p h y s i c a l e x a mi -
Received from the University of Washington School of Medicine (JRG),
Seattle, Washington, and the Veterans Affairs Medical Center (JRG,
JCG) and the Department of Engineering, Boise State University (JCG),
Boise, Idaho.
Address correspondence and reprint requests to Dr. Guarino:
Medical Service, VA Medical Center, 500 West Fort Street, Boise, ID
83702.
n a t i o n i n c l u d i n g d u l l n e s s t o p e r c u s s i o n , d i mi n i s h e d b r e a t h
s o u n d s , v o c a l r e s o n a n c e , a n d t a c t i l e f r e mi t u s i s n o t at
al l s e n s i t i v e a n d n o t s u f f i c i e n t l y s p e c i f i c f o r d e t e c t i o n o f
p l e u r a l e f f us i on. T h e s i g n s ma y b e i mp o s s i b l e t o di s t i n-
g u i s h f r o m p l e u r a l t h i c k e n i n g a n d u n d e r l y i n g l u n g dis-.
eas e. T h e y c a n b e a b s e n t i n p a t i e n t s wi t h o b e s i t y , a t h i c k
c h e s t wa l l , o r s ma l l p l e u r a l e f f us i ons . A p h y s i c a l e x a m-
i n a t i o n t h a t i s s i mp l e a n d d i s t i n c t i v e wo u l d b e o f c l i n i c a l
va l ue .
PRINCIPLES
T h e me t h o d i s b a s e d u p o n t h e p r i n c i p l e s o f aus -
c u l t a t o r y p e r c u s s i o n ( AP ) u s e d i n t h e p h y s i c a l e x a mi -
n a t i o n o f t h e c h e s t , h e a d , a n d u r i n a r y b l a d d e r , a n d f o r
t h e d e t e c t i o n o f a s c i t e s . 4- 9 Wh e n t h e p a t i e n t i s e r e c t ,
f r e e p l e u r a l f l u i d g r a v i t a t e s t o t h e b a s e o f t h e l u n g a n d
c r e a t e s a ma r k e d a c o u s t i c i mp e d a n c e mi s ma t c h b e t we e n
a i r - c o n t a i n i n g l u n g a n d t h e f l u i d i n t e r f a c e . T h e p o s t e r i o r
c o s t o p h r e n i c s u l c u s , t h e mo s t d e p e n d e n t p a r t o f t h e
t h o r a c i c c a v i t y , i s a d e e p , r e l a t i v e l y i n c o mp l i a n t s l i t b e -
t we e n t h e c h e s t wa l l a n d t h e b o w o f t h e d i a p h r a g m. I n-
v i t r o e x p e r i me n t s p e r f o r me d i n o u r l a b o r a t o r y wi t h i n-
f l a t e d b a l l o o n s i n c o r p o r a t e d wi t h i n t r a n s p a r e n t p l a s t i c
c o n t a i n e r s s i mi l a r i n s h a p e a n d c a p a c i t y t o t h e p o s t e r i o r
c o s t o p h r e n i c s u l c u s h a v e s h o wn t h a t mi n i ma l f l u i d vol -
u me s p r o d u c e a d i s p r o p o r t i o n a t e r i s e i n t h e f l u i d l e v e l
t h a t c a n b e p r e c i s e l y d e l i n e a t e d a n d me a s u r e d b y t h e
me t h o d o f AP. I n a n a n e s t h e t i z e d 3 0 - k g s h e e p s u p p o r t e d
u p r i g h t , we d e mo n s t r a t e d t h a t t h e i n t r o d u c t i o n o f o n l y
25 mL o f p h y s i o l o g i c a l s a l i n e s o l u t i o n t h r o u g h a c h e s t
t u b e i n t h e p l e u r a l s p a c e p r o d u c e d a h o r i z o n t a l f l u i d
l e v e l t h a t wa s r e a d i l y d e t e c t e d b y AP. A r i s e i n t h e f l u i d
l e v e l wa s d e l i n e a t e d b y AP wi t h e a c h i n c r e me n t o f 25
mL o f t h e p h y s i o l o g i c a l s a l i n e s o l u t i o n . Wh e n t h e s h e e p
wa s t i l t e d l a t e r a l l y a p p r o x i ma t e l y 35 f r o m t h e p e r p e n -
d i c u l a r t o wa r d t h e s i d e o f i n f u s i o n , t h e f l u i d l e v e l q u i c k l y
s h i f t e d t o t h e d e p e n d e n t s i d e a n d r a i s e d t h e l e v e l a l o n g
t h e l a t e r a l b o r d e r wi t h a s i mu l t a n e o u s f al l i n t h e l e v e l
me d i a l l y .
TECHNIQUE
Wi t h t h e p a t i e n t s i t t i n g o r s t a n d i n g , hi s o r h e r b a c k
f a c i n g t h e e x a mi n e r , t h e u p p e r e d g e o f t h e t we l f t h r i b
i s ma r k e d o n e a c h s i d e o f t h e t h o r a x . Af t e r a p p r o x i l n a t c l y
5 mi n u t e s u p r i g h t , f r e e p l e u r a l f l u i d g r a v i t a t e s t o t h e
b a s e o f t h e l ung. T h e d i a p h r a g ma t i c p i e c e o f t h e s t e t h -
o s c o p e i s p l a c e d p o s t e r i o r l y wi t h i t s u p p e r e d g e ap-
p r o x i ma t e l y 3 c m b e l o w t h e l a s t r i b i n t h e mi d c l a v i c u l a r
71
72 Guarino, Guarino, PLEURAL EFFUSION DETECTION
PATI ENTS AND METHODS
!
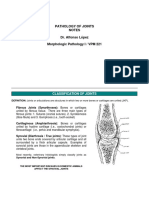
FIGURE 1. Method of auscul t at ory percussion t o detect t he level of
pleural effusion ( a r r o w , l e f t s / d e ) and t o delineate t he paravert ebral t r i angl e
of Grocco ( ar r ow, r i g h t s i d e ) .
line. Direct percussion is applied with the free hand
preferably by finger flicking or with the pulp of a finger,
along three or more parallel lines from the apex of each
hemithorax perpendicularly down toward the base (Fig.
1 ). In the absence of pleural effusion, the percussion
note percei ved t hrough the apposed st et hoscope sounds
dull and remains unchanged, but changes sharply to a
loud note that is striking at the last rib, forming a hor-
izontal baseline across the posterior hemithorax. In the
presence of pleural effusion a similar sharp change to a
loud percussion not e occurs at the interface of air-con-
taining lung and pleural fluid, approximating a horizontal
line across the post eri or hemi t horax clearly above the
baseline at the last rib. In the absence of air in the pleural
space, the fluid level is usually highest laterally towards
the axilla. The distance bet ween the level and the upper
border of the last rib is measured and used as a guide
for thoracentesis and for estimation of fluid volume.
Applying the same t echni que to the hemi t horax op-
posite the effusion, a sharp change to a loud percussi on
note clearly defines the borders of the paravertebral
triangular area of Grocco, 1 whose apex lies along the
spine and whose base ext ends 6 to 10 cm at a right angle
to the spine (Fig. 1). The triangular area can be dull to
conventional percussion but may be difficult to define
with this modality. It is easily and sharply delineated
by AP.
Over a three-year peri od ( 1989- 1992) , 118 con-
secutivc inpatients with pleural effusion recognizable on
chest radiographs and 175 inpatient control subjects
selected at random from the medical and surgical wards,
ranging in age from 32 to 96 years (mean 64 years),
were examined by AP. Ninety percent of the patients
were men. The t echni que was developed and taught at
the bedside by the senior investigator on patients with
and without radiologic evi dence of pleural effusion. Pa-
tients with pleural effusion who were teaching cases for
trainees were not part of the study group. Finger-flicking
percussion was done rapidly and gently at about 5-mm
intervals along three parallel lines that ran perpendic-
ularly from the apex of the hemi t horax to its base. Body
contact with only the tip of the fingernail ensures pre-
cision. The examination was usually compl et ed within
5 minutes and required only minimal skill. When the
patient was maintained in the erect position with the
fluid level at equilibrium, the endpoint of the ausco-
percussive not e was characteristically sharp, loud, and
precise. A common, inexpensive Sprague-Rappaport type
of stethoscope was used in the examination. When the
examiners became proficient and able to identify the
endpoint with eyes closed and with consistent accuracy,
they were asked to examine patients and to mark the
cndpoint in the auscopercussive note. The marked sites
were measured and compared by the examiners. Each
of the 118 inpatients with pleural effusion as well as
each of the 175 randomi zed controls was evaluated by
two to three examiners separately and independently.
In the three-year period, 60 medical students, 15 resi-
dents, and five senior staff members were trained par-
ticipants. The examiners were unaware of the history,
physical, and radiologic findings prior to their evalua-
tion. Which patients had plcural effusion was obtained
from a central source and was known only to the senior
investigator. There was no communi cat i on bet ween the
examiners and the senior investigator during the ex-
amination. All patients had a standard physical exami-
nation and standard post er i or - ant er i or and lateral ra-
diography of the chest upon admission. Lateral decubitus
radiographs were obtained when pleural effusion was
suspected by the radiologist after examining the stan-
dard radiographs. Ultrasonography and comput eri zed
t omography of the chest were done for several patients
unrelated to this study. Patients with a horizontal level
above the last rib in the examination by AP suggestive
of pleural effusion were tilted laterally with support ap-
proximately 35 from the perpendicular, and the ex-
amination was repeated. Corresponding shifts in the level
and changes in the size of the paravertebral triangle of
Grocco in the contralateral lung base were also noted.
To avoid false-positive examinations results, it was
essential to mark the last rib and to keep the upper edge
of the diaphragmatic piece well bel ow this rib. False-
JOURNAL OF GENERAL INTERNAL MEDICINE, Vol ume 9 (February), 1994 73
negative results can occur when patients are examined
too quickly upon arising from recumbency, i.e., before
settling of the pleural fluid. Five minutes upright was
considered sufficient time to establish a fluid level in
nearly all patients wi t h free pleural fluid. With the dia-
phragmatic piece held as described bel ow the last rib,
the location of the diaphragm at the peri phery at end-
inspiration and end-expiration was easily identified by
a sharp cutoff produci ng a suddenly l oud auscopercus-
sive note bel ow and above the last rib, respectively.
RESULTS
All examiners report ed their findings i ndependent l y
to the senior investigator (JRG). One hundred thirteen
of the 118 patients with pleural effusion according to
the standard and lateral decubitus chest radiographs had
a demonstrable fluid level above the last rib accordi ng
to the examination by AP, and a distinct shift in the level
by lateral tilt (sensitivity = 95.8% ). Of note, a backward
tilt produced a distinct rise in the fluid level; conversely,
a forward tilt caused a fall in the level. The five patients
who yielded false-negative findings in the initial exam-
ination by AP had been supine approximately t wo hours.
The fluid level was not discernable until the patients
were upright for 25 to 30 minutes. The chest radiographs
for each patient showed fluid loculation, and subsequent
thoracentesis revealed viscous fluid. Each of the five
patients were re-examined by AP at lO-minute intervals
in the erect position. The sensitivity of the AP test for
pleural effusion may thus increase when the examination
is repeated.
Each of eight patients in the study suspected to have
subpulmonic effusion by chest radiography, confirmed
by lateral decubitus radiography, had a distinct fluid
level above the last rib in the examination by AP that
shifted with lateral tilt. They were readily identified by
the met hod of AP.
Pleura] effusion was not specifically identified in the
standard conventional physical examinations of the chest
for any of the 118 patients in the admitting examination.
The 175 control patients examined at random included
patients with lung masses, pneumonia, l obect omy, dia-
phragm elevation, and unspecified lung disease. None
had evidence of pleural effusion in the examination by
AP or by chest radiograph.
Nine of the cont rol patients wi t h unilateral dia-
phragmatic elevation visible on the chest radiograph had
a horizontal level above the last rib in the examination
by AP, suggesting pleura] effusion. However, none of
these patients had a shift in the level wi t h lateral tilt,
thus none constituted false-positive AP test results for
pleura] effusion (specificity = 100% ).
The paravertebral triangle of dullness of Grocco was
easily elicited in all patients in this study wi t h unilateral
pleura] effusion and in those patients wi t h unilateral
diaphragmatic elevation. A lateral tilt of 35 toward the
side with effusion quickly obliterated the triangular area
of dullness in the contralateral hemithorax, shifted the
fluid to the dependent side, and raised the fluid level
along the lateral border. The maneuver wi t h a slight
backward tilt facilitated thoracentesis of small effusions
at the post eri or axillary line. Within the triangular area
of dullness of Grocco, breath sounds were diminished
to absent. Muffled e-to-a changes may be elicited, and
distant bronchovesi cul ar breathing coul d be heard in
some patients, suggesting pneumoni c consolidation. The
abnormal findings were quickly obliterated wi t h lateral
tilt toward the side wi t h pleura] effusion, with disap-
pearance of dullness and e-to-a changes, and return of
normal breath sounds.
Diaphragmatic excursions were easily and precisely
identified at the peri phery by AP and normally ranged
from 5 to 6 cm. Of the 118 cases of pleural effusion, 57
were due to malignant neoplasms, 32 to congestive heart
failure, eight to pneumonia, t wo to empyema, five to
acute pancreatitis, t wo to pancreatic abscess, three to
ascites, t wo to nephrot i c syndrome, t wo to traumatic
rib fractures with hemot horax, one to subphrenic ab-
scess, t wo to lung abscess, and t wo to pul monary in-
farctions. Pleural effusion was bilateral in 22 patients,
18 of whom had congestive heart failure.
For all the patients except the five who had viscous
or loculated fluid, the examiners uniformly concurred
100% of the time that the cutoff" in the percussi on not e
was striking and precise at the fluid level. When the
patient was maintained in the erect position with the
fluid level at equilibrium, the endpoi nt in the exami-
nation of the same patient by different examiners varied
by 0.5 cm.
DISCUSSION
Subpulmonic effusions are common and often un-
suspected.-" They simulate an elevated diaphragm in the
chest radiograph and can be difficult to recognize. The
infrapulmonic fluid is quickly displaced by lateral tilt of
the chest and readily identified by the met hod of AP.
Small pleura] effusions obscured in the posterior cos-
t ophreni c sulcus or t oo thin to be recogni zed in the
lateral decubi t us radiograph can bc demonst rat ed in the
examination by AP.
Awareness of the triangle of Gr occo has clinical
significance. The abnormal physical findings within the
triangle have been mistaken for pneumoni c consolida-
tion in the physical examination. The mechani sm of
Grocco' s triangle is unclear. TM ~2 The triangular config-
uration of dullness may be due to compressi on of the
contralateral lung by the hydrostatic pressure of the
pleura] effusion. When the patient is upright, compres-
sion of the lung is least at the apex wher e the hydrostatic
pressure is l ow and maximal at the base wher e the hy-
drostatic pressure is high. The triangular area is not vis-
ible in the chest radiographs but is sharply delineated
74 Guarino, Guarino, PLEURAL EFFUSION DETECTION
by AP. The l ack of r adi opaci t y i n an area of what is
t hought t o be compr es s i ve at el ect asi s is confusi ng. How-
ever, it shoul d be not ed t hat t he r adi ogr aphi c fact ors for
def i ni t i on 13 differ f r om t he acoust i c fact ors i nvol ved in
t he t r ansmi ssi on of sound vi brat i on. 7, 14
The mechani s m of AP i nvol ves t he effect on t he
passage of sound vi br at i ons t hr ough di f f er ent medi a. The
t r ansmi ssi on of s ound vi br at i ons depends upon t he dif-
f er ence in t he acoust i c i mpe da nc e val ues be t we e n t he
medi a. The acoust i c i mpedance ( Z) of a mat er i al is t he
pr oduct of t he s ound vel oci t y ( c ) wi t hi n t he par t i cul ar
me di um and t he densi t y ( p) of t he medi um:
Z = c - o.
T h e t r a n s mi s s i o n o f s o u n d f r o m a ma t e r i a l wi t h l o w
a c o u s t i c i mp e d a n c e , i . e. , a i r o r ga s , t o a ma t e r i a l wi t h
hi gh acoust i c i mpedance, i.e., wa t e r or body fluids, is
great l y i nhi bi t ed, per mi t t i ng sharp del i neat i on of t he
boundar y at t he a i r - f l ui d i nt er f ace in t he AP exami na-
tion. Appl i cat i on of t he s t et hos cope conf i nes and pre-
vent s di sper si on of sound vi br at i ons gener at ed by t he
per cussi ve not e and mar kedl y enhances t he pr eci si on
of t he AP exami nat i on.
In cont r ast t o AP, t he r adi ogr aphi c fact ors are chem-
ical and depend upon el ect r on densi t y. The opaci t y of
t he i mage is pr opor t i onal t o t he cube of t he at omi c
numbe r of t he mat eri al .
The AP exami nat i on is cons i der ed a val uabl e sup-
pl ement t o t he convent i onal chest exami nat i on t o det ect
pl eur al effusion. The AP exami nat i on is hi ghl y sensi t i ve
and speci fi c and cor r el at es cl osel y wi t h t he st andard and
l at eral decubi t us chest radi ographi es. Small amount s of
pl eur al fluid may yi el d posi t i ve AP exami nat i on resul t s
in cases wi t h negat i ve r adi ol ogi c findings. Serial AP ex-
ami nat i ons s howi ng a change in t he fluid l evel conf i r m
t he pr es ence of pl eur al effusion. The AP exami nat i on is
especi al l y useful t o al er t t he cl i ni ci an t o t he possi bi l i t y
of uns us pect ed pl eur opul monar y, cardi ac, or syst emi c
disease, and pr ompt s f ur t her st udy and fol l ow-up.
The cooperation and assistance of the Medical, Surgical, and Nursing
Services of the Boise Veterans Affairs Medical Center are gratefully
acknowledged. The authors thank Wayne L. Kirk for his laboratory
assistance and Barry Cusack, MD, for review of the manuscript. They
are especially grateful to Paula Carvalho, MD, for her assistance in the
preparation of the manuscript.
REFERENCES
1. Hinshaw HC, Garland LH. Diseases of the pleura. In: Diseases of
the Chest, 2nd ed. Philadelphia: W. B. Saunders, 1963;592-638.
2. Felson B. The pleura. In: Fundamentals of Chest Roentgenology.
Philadelphia: W. B. Saunders, 1960;183--93.
3. Vladutiu AO. Clinical signs of pleural effusion. In: Pleural Effusion.
Mount Kisco, NY: Futura Publishing Company, 1986;19-67.
4. Guarino JR. Auscultatory percussion: a new aid in the examination
of the chest. Kans Med. 1974;75:193-4.
5. Guarino JR. Auscultatory percussion of the chest. Lancet.
1980;1:1332-4.
6. Guarino JR. Auscultatory percussion of the bladder to detect uri-
nary retention. N Engl J Med. 1981;305:701.
7. Guarino JR. Auscultatory percussion of the head. BMJ.
1982;284:1075- 7.
8. Guarino JR. Auscultatory percussion of the urinary bladder. Arch
Intern Med. 1985;145:1823-5.
9. Guarino JR. Auscultatory percussion to detect ascites. N Engl J
Med. 1986;315:1555.
10. Grocco P. Brevi note de semiiotica fisica. Rev crit di clin reed.
Firenze. 1902;3:274.
11. Major HR, Delp MH. Inspection, palpation and percussion of the
chest. In: Physical Diagnosis, 6th ed. Philadelphia: W. B. Saunders,
1962;103-29.
12. SapiraJD. The chest. In: The Art and Science of Bedside Diagnosis.
Baltimore: Urban & Schwarzenberg, 1990;245-81.
13. Peterson HO, Kieffer SA. Neuroradiology. In: Baker AB, Baker LH
(eds): Clinical Neurology. Hagerstown, MD: Harper and Row,
1980;257-90.
14. TonndorfJ. Physics of sound. In: Paperella M, Shumrick D (eds).
Otolaryngology. Philadelphia: W. B. Saunders, 1973;214-60.
Potrebbero piacerti anche
- Tocmj 5 85Documento5 pagineTocmj 5 85Diego OrtechoNessuna valutazione finora
- Impact of Prepregnant Body Mass IndexDocumento8 pagineImpact of Prepregnant Body Mass IndexDiego OrtechoNessuna valutazione finora
- J 1468-3083 2006 02023 XDocumento14 pagineJ 1468-3083 2006 02023 XDiego OrtechoNessuna valutazione finora
- Interview With Lawrence Weed, MDDocumento6 pagineInterview With Lawrence Weed, MDDiego OrtechoNessuna valutazione finora
- Clin Infect Dis. 2008 Moellering 1032 7Documento6 pagineClin Infect Dis. 2008 Moellering 1032 7Diego OrtechoNessuna valutazione finora
- Clin Infect Dis. 2002 Stevens S93 S100Documento8 pagineClin Infect Dis. 2002 Stevens S93 S100Diego OrtechoNessuna valutazione finora
- s80 FullDocumento3 pagines80 FullDiego OrtechoNessuna valutazione finora
- Pharmacokinetic Characteristics of Antimicrobials and Optimal Treatment of UrosepsisDocumento15 paginePharmacokinetic Characteristics of Antimicrobials and Optimal Treatment of UrosepsisDiego OrtechoNessuna valutazione finora
- The Uses and Limitations of The Fetal Biophysical Profile.Documento18 pagineThe Uses and Limitations of The Fetal Biophysical Profile.Diego Ortecho100% (1)
- Singh Et AlDocumento9 pagineSingh Et AlDiego OrtechoNessuna valutazione finora
- 378 FullDocumento3 pagine378 FullDiego OrtechoNessuna valutazione finora
- A Llega To 441161Documento6 pagineA Llega To 441161Diego OrtechoNessuna valutazione finora
- Hemolysis of Blood Samples Has No Significant Impact On The Results of Pharmacokinetic DataDocumento4 pagineHemolysis of Blood Samples Has No Significant Impact On The Results of Pharmacokinetic DataDiego OrtechoNessuna valutazione finora
- Effect of in Vitro Hemolysis On Chemical Values For SerumDocumento5 pagineEffect of in Vitro Hemolysis On Chemical Values For SerumDiego OrtechoNessuna valutazione finora
- 1947 FullDocumento2 pagine1947 FullDiego OrtechoNessuna valutazione finora
- Blood 1985 Cazzola 935 9Documento6 pagineBlood 1985 Cazzola 935 9Diego OrtechoNessuna valutazione finora
- Pbio 0050018Documento2 paginePbio 0050018Diego OrtechoNessuna valutazione finora
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (890)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (587)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (265)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (119)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Not Eligible As No Experience of Teaching and ResearchDocumento5 pagineNot Eligible As No Experience of Teaching and ResearchVasanth Kumar AllaNessuna valutazione finora
- Uttar Pradesh Empanelment List for Minilap 2018-19Documento19 pagineUttar Pradesh Empanelment List for Minilap 2018-19Vijay KumarNessuna valutazione finora
- American Society For Biochemistry and Molecular BiologyDocumento23 pagineAmerican Society For Biochemistry and Molecular BiologyShishui UchihaNessuna valutazione finora
- Psychology All Case Studies PDFDocumento54 paginePsychology All Case Studies PDFArmeen AmirNessuna valutazione finora
- How to prepare your Asil for fightingDocumento16 pagineHow to prepare your Asil for fightingcinna01Nessuna valutazione finora
- Zingiber Officinale MonographDocumento5 pagineZingiber Officinale Monographc_j_bhattNessuna valutazione finora
- Cerebrolysin in Patients With Hemorrhagic StrokeDocumento7 pagineCerebrolysin in Patients With Hemorrhagic StrokeZeynep Emirhan ŞenyüzNessuna valutazione finora
- Atlas de Acupuntura (Ingles)Documento16 pagineAtlas de Acupuntura (Ingles)Medicina Tradicional China - Grupo LeNessuna valutazione finora
- Smell & TasteDocumento4 pagineSmell & Tasteminji_DNessuna valutazione finora
- Aj. Chulaporn-Bosutinib-Search Engine and Study EndpointsDocumento5 pagineAj. Chulaporn-Bosutinib-Search Engine and Study EndpointsCalm Phurit SenachaiNessuna valutazione finora
- Pathology of JointsDocumento13 paginePathology of JointswobblegobbleNessuna valutazione finora
- Training of Top US Distance SwimmersDocumento45 pagineTraining of Top US Distance SwimmersMel HarbourNessuna valutazione finora
- Types of Casts and Their IndicationsDocumento3 pagineTypes of Casts and Their IndicationsPhylum ChordataNessuna valutazione finora
- Isolating Staphylococcus SPDocumento4 pagineIsolating Staphylococcus SPHani HairullaNessuna valutazione finora
- Treatment of Class III Malocclusion: The Key Role of The Occlusal PlaneDocumento9 pagineTreatment of Class III Malocclusion: The Key Role of The Occlusal PlaneFabian BarretoNessuna valutazione finora
- AnupanaDocumento60 pagineAnupanaVaidya Nur50% (4)
- Adime Due 10 29Documento3 pagineAdime Due 10 29api-437192216Nessuna valutazione finora
- Bell's PalsyDocumento12 pagineBell's PalsyMercy nafulaNessuna valutazione finora
- A Devoted SonDocumento1 paginaA Devoted SonAnkur MaheshwariNessuna valutazione finora
- Showtime - Smilf 1x01 (Pilot)Documento36 pagineShowtime - Smilf 1x01 (Pilot)Vishnu SinhaNessuna valutazione finora
- Sample IQ TestDocumento34 pagineSample IQ TestResIpsa LoquitorNessuna valutazione finora
- Sample 20715Documento16 pagineSample 20715Sachin KumarNessuna valutazione finora
- The Hypothesis and Assumptions of The StudyDocumento12 pagineThe Hypothesis and Assumptions of The StudyMaria Arlene67% (3)
- Emergency Welfare FormDocumento2 pagineEmergency Welfare FormKristopher HarperNessuna valutazione finora
- Caliber - L: Expandable Lateral Lumbar Interbody Fusion DeviceDocumento6 pagineCaliber - L: Expandable Lateral Lumbar Interbody Fusion DeviceBobNessuna valutazione finora
- Asymptomatic BacteriuriaDocumento23 pagineAsymptomatic BacteriuriaSabita PaudelNessuna valutazione finora
- ASPEN Pocket Cards - Guidelines For The Provision and Assessment of Nutrition Support Therapy in The Pediatric Critically Ill Patient-1Documento12 pagineASPEN Pocket Cards - Guidelines For The Provision and Assessment of Nutrition Support Therapy in The Pediatric Critically Ill Patient-1Ceren KamalıNessuna valutazione finora
- JAPAN-Flag-Standard Medical Chest MAR 2018 (Req)Documento10 pagineJAPAN-Flag-Standard Medical Chest MAR 2018 (Req)shishir kumarNessuna valutazione finora
- De Gruchys Clinical Haematology PDFDocumento1 paginaDe Gruchys Clinical Haematology PDFShivanshi K0% (1)
- Framingham Risk Score SaDocumento8 pagineFramingham Risk Score Saapi-301624030Nessuna valutazione finora