Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
TMH PBS Presentation
Caricato da
candiddreams0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
45 visualizzazioni61 pagineTMH proceedings 2010-2011,pdf
Copyright
© © All Rights Reserved
Formati disponibili
PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoTMH proceedings 2010-2011,pdf
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PDF, TXT o leggi online su Scribd
0 valutazioniIl 0% ha trovato utile questo documento (0 voti)
45 visualizzazioni61 pagineTMH PBS Presentation
Caricato da
candiddreamsTMH proceedings 2010-2011,pdf
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 61
Dr Pankhi Dutta MD, DM (haematopathology)
Consultant Haematopathologist, SevenHills Hospital, Mumbai
Frequently performed lab test
Very simple
Very informative
Requirements- a microscope, Romanowsky
stain , a microscopist!
PHYSICIANS REQUEST
Clinical situations like
anemia with jaundice,
unexplained unconjugated
hyperbilirubinemia , etc
Previous abnormal CBC /
PS report
LAB INITIATED
Abnormal CBC
Flagging
Clinical details (rarely)
Evaluation of anemia
Authenticating
thrombocytopenia/thrombocytosis
Diagnosis of abnormal cells (blasts, lymphoma
cells)
Infections like malaria, babesia, microfilaria, etc.
Others, Howell-Jolly bodies (asplenia),etc.
Is diagnostic on many
occasions
Gives vital clues for further
work up
Essential in some situations
where automated analyzer
fails due to interferences
Collection (venepuncture)
Smear preparation- wedge technique/
automated
Staining- manual/ automated
Many people involved, need stringency at
every step!
EDTA samples (within 1 hr of collection)
Many smears may be prepared
No EDTA artefacts if made early
Prevents platelet clumping
No need to prepare smears immediately
Direct smears
No EDTA artefacts at all,
but, stress on the phlebotomist
Wedge technique (most commonly used)
Too large drop- too thick smear
Too small drop- too thin smear
Too much pressure- WBCs disrupted
Too slow push- accentuated WBC tailing
Angle adjustment for anemia/polycythemia
Greasy slide- irregular streaky film
Romanowsky stain (polychrome methylene
blue and eosin)
Mixture of acidic and basic components
Differential stainingsubtle distinctions
Examples
Leishmans, Jenner, Giemsa, May-Grunwald-
Giemsa, Wrights, Wright-Giemsa, Jenner-
Giemsa, Azure B-EosinY, etc.
WBCs poorly fixed and /or refractile shiny
blotches on RBCs-
too much water in slide/methanol/stain
water absorbed from humidity on to
slide/stain.
dry slides quickly, keep stain in tightly closed
bottles, use anhydrous methanol.
RBCs too gray, WBCs too dark, etc- stain is
too alkaline/prolonged staining/under
rinsing/heparin sample
RBCs too pale, WBCs barely visible- stain too
acidic/over rinsing/under staining
Stain debris/ppt- filter stain, do not allow
staining solution to dry over slide
Stain precipitate/debris
Tailing (all WBCs collected at the tail)
Refractile edges on RBCs (excess water on slide)
All cells appear spherocytic (flattened out cells
without central pallor)
EDTA artefacts
Nuclear lobulations,
degeneration, pyknosis,
rupture.
Cytoplasmic granulation,
vacuolization.
RBC changes
Citrate-immediately
EDTA- after 2 hours
A. Narasimha et al,
Indian J Haematol Blood
Transfus 24
Polychromasia
Agglutination/rouleaux
Poikilocytes, spherocytes, blister cells
Parasites
Degree of cytopenia/cytosis (tailing)
Rare blast (thick/ thin slide, distorted WBCs)
Inclusions
CAN LEAD TO SERIOUS MISTAKES!!
Automation may partially overcome such
problems
Set of rules are defined on an analyzer which
initiates automatic slide preparation
e.g., HST-N (Sysmex) : combination of
(A) analyzer with
(B) automatic slide preparation and staining and
(C) cell identification unit
Macroscopic view- quality of slide (spreading & staining)
10x view-quality of slide, cellular distribution, area
selection, microfilariae, rouleaux, platelet
aggregates/clumps.
40x view- WBC total count estimation, WBC DC, RBC
morphology
100x- WBC-DC, no. & morphology of platelets, finer
details like basophilic stippling & Auer rods, parasites like
malaria, etc.
CLINICAL SITUATION TO BE KEPT IN MIND
Very distinctive PBS (HS, HE, SEAO, HPP)
(Osmotic fragility- non-specific)
SICKLE CELLS ARE DISTINCT BETA-THALLASSEMIA
MEGALOBLASTIC
Vit B12, folate def.
Macro-ovalocytes
Hypersegmented polys
Increased RDW
Fragmented cells, HJ
bodies, Cabots ring, etc.
NON-MEGALOBLASTIC
Liver disease (+target
cells), aplastic anemia,
reticulocytosis
(polychromasia),
hypothyroidism, MDS, etc
Not oval shaped
RDW is a useful
parameter
Raised RDW- IDA
Normal or slightly
raised- beta-thal trait
Iron Deficiency
Thal Trait
HS (Coombs ve, young age)
AIHA (Coombs +ve)
HDN
Post transfusion
Osmotic fragility
(non-specific)
Bite cells- arcuate
defects
Blister cells-vacuoles
or thin areas at
periphery
Oxidant damage
G6PD test, Heinz body
test, etc may help.
Microangiopathic HA
TTP, HUS
HELLP
DIC
March hemoglobinuria
Schistocytes,
reticulocytosis, raised
LDH, other clinical
features.
FRC flagging!
RBC Fragments
RBC Fragments
Pathological
Haemolysis, MPNs,
severe sepsis, b.m.
metastases (leuco-
erythroblastic PS)
May interfere with
automated TLC
Correction of TLC
No. NRBCs / 100 WBCs
NRBCs
NRBCs
BS
Heavy metals, P5N def,
sideroblastic A,
hemoglobinopathies,
thalassemia.
HJ bodies
Asplenia/hyposplenia,
severe haemolyis,
megaloblastic anaemia
PBS - first clue to their presence
Morphology helps to differentiate malignant vs non-
malignant condns. (e.g., IM vs ALL)
Diagnostic morphology- e.gAuer rods in
AML, Hairy cells, etc.
APML and Burkitts lymphoma/leukemia are medical
emergencies, typical PBF allows start of therapy.
Morphologic basis for sophisticated tests like FCM, PCR.
Buffy coat preparations for leucopenic samples
Infectious
mononucleosis
Benign, self limited.
Generalised
lymphadenopathy/
hepatosplenomegaly
Lymphocytosis
Atypical T cells in PS
Hypolobulated nuclei
Pseudo-Pelger cells
MDS
Medical emergency
Hypergranular
promyelocytes
Faggot cells
PS characteristic
PML:RARa transcript
diagnostic
Mature B cell
Medium sized
Oval/indented nucleus
Ground glass
chromatin
Absent nucleoli
Abundant, pale blue
cytoplasm, hairy
projections
TRAP +ve
Platelet clumps
EDTA induced agglutination
Platelet satellitism
Giant / large platelets
Peripheral blood film examination &
manual count is helpful.
Optical / antibody based methods- useful
Harris syndrome
( MPV >10fl, normal
platelet fn, variable
thrombocytopenia)
J Thromb Haemost 2005,
Am J Med 2002
MDS, MPN,recovering
bone marrow
BS, MH anomaly
Microcytic RBC
Giant PLT
Babesia Trypanosmes
MALARIA
PS examination gold
standard
Species identification
Parasite load (PF)
pH (7.2) of staining solution
crucial.
Smear review- increases manual work,
reduces TAT & productivity
Need to reduce smear review rate without
risk of missing anything significant
Different labs different criteria
Criteria depend upon patient population,
type of analyser in use, etc.
International consensus group for hematology
review ISLH, 2002 ( Dr. Berend Houwen)
Laid down rules for action following automated
CBC including smear review
Rules tested in 15 labs (13,298 samples)
Data analysed, rules refined, 43 rules laid down
Guidelines for individual laboratories
Morphology
Red cell 2+/moderate/>
Platelet morph (giant
forms) at 2+/>
Platelet clumps at >
rare
Toxic granulation at
2+/>
Vacuoles at 2+/>
Abnormal cell types
Blast>/=1
Meta>2
Myelo/promyelo>/=2
Atypical lymph>5
NRBC>/=1
Plasma cells >/=1
Rule no Parameter Primary And/or Action
1 neonate 1
st
sample Slide review
10 MCV <75fl or >105fl Specimen
<24hrs old
Slide review
15 RDW >22 1
st
time Slide review
16 NoWBC
diff/incomplete
Manual diff &
slide review
7 Platelet <100 or >1000 1
st
time Slide review
flagged normal Analyser
Routine
technician
? Abnormal RBCs
? Atypical mononuclear
WBCs
Common RBC abnormality
Granulocyte left shift
Atyipcal (variant) lymphocytes
normoblasts
Sr. technician
? Blasts
? Organisms
Myelocytes
Plasma cells
Dohle bodies
Targets
Auer rods
Physician
Diagnostic
cells
Report Report Report Report
Examiner
Differentiation
PBS examination-simple but important test
Is diagnostic on many occasions
Gives clues for further workup
Optimum quality slides, a must
PBS examination + parameters on analyzers =
maximum information
Fully automated solutions can
standardize slide preparation and staining
increase TAT of labs
Judicious use of slide review criteria-
reduces slide reviewrate
and also avoids any risk to patients
MORPHOLOGY TRAINING REMAINS ESSENTIAL
(even in days of automation!!)
Potrebbero piacerti anche
- Fusion Tech ActDocumento74 pagineFusion Tech ActrahulrsinghNessuna valutazione finora
- Understanding PancytopeniaDocumento68 pagineUnderstanding PancytopeniaThaveeshaLindsayWhiteNessuna valutazione finora
- Combined Set of Kaplan 900 and High Frequency Words PDFDocumento17 pagineCombined Set of Kaplan 900 and High Frequency Words PDFcandiddreams100% (2)
- Pragmatic Marketing FrameworkDocumento2 paginePragmatic Marketing FrameworkohgenryNessuna valutazione finora
- G10 ICT Lesson1 - Types and Parts of ComputerDocumento4 pagineG10 ICT Lesson1 - Types and Parts of ComputerJOHN RIMMON TAQUISO0% (1)
- PBS examination provides vital hematological insightsDocumento40 paginePBS examination provides vital hematological insightsaustin_doc2rNessuna valutazione finora
- Peripheral Smear Examination PDFDocumento91 paginePeripheral Smear Examination PDFtufis02Nessuna valutazione finora
- Hematology Review: by Felicia Magee Tardy, M.S., MT (Ascp)Documento52 pagineHematology Review: by Felicia Magee Tardy, M.S., MT (Ascp)Reen LeenNessuna valutazione finora
- Ana IfDocumento101 pagineAna Ifshrikrishnapathlab100% (1)
- Peripheral Smear Review: Diagnostic Aid for Blood DisordersTITLEDocumento31 paginePeripheral Smear Review: Diagnostic Aid for Blood DisordersTITLEDaniel McFarlandNessuna valutazione finora
- Body Fluid Analysis in Clinical LabDocumento52 pagineBody Fluid Analysis in Clinical Labmrcool995Nessuna valutazione finora
- Abnormal Blood Film Practical (DR Nazirah)Documento22 pagineAbnormal Blood Film Practical (DR Nazirah)RUDOLF YUSON BM20110052Nessuna valutazione finora
- Hematology Peripheral Blood SmearDocumento7 pagineHematology Peripheral Blood SmearJosephine Armanne AluyenNessuna valutazione finora
- 6 Microscopic Examination of UrineDocumento116 pagine6 Microscopic Examination of Urineaddine061421Nessuna valutazione finora
- ABC of CBCDocumento102 pagineABC of CBCFaaiq ShahNessuna valutazione finora
- Acute Lymphoid Leukemia (Airway Management)Documento48 pagineAcute Lymphoid Leukemia (Airway Management)Ankita SamantaNessuna valutazione finora
- Hematology 1Documento28 pagineHematology 1체리고은Nessuna valutazione finora
- DR Bambang - Anemia OverviewDocumento263 pagineDR Bambang - Anemia OverviewOkta Dwi Kusuma AyuNessuna valutazione finora
- WaloDocumento67 pagineWaloyepNessuna valutazione finora
- Acute Lymphoid Leukemia (Case Presentation)Documento48 pagineAcute Lymphoid Leukemia (Case Presentation)NEILVEL KNessuna valutazione finora
- Lab Activity No. 5 - Slide PresentationDocumento24 pagineLab Activity No. 5 - Slide PresentationChelsea Padilla Delos ReyesNessuna valutazione finora
- Abnormalities of Haematopoiesis and Blood DisordersDocumento51 pagineAbnormalities of Haematopoiesis and Blood DisordersRenad AlharbiNessuna valutazione finora
- Full Blood PictureDocumento29 pagineFull Blood PictureKesavanVeera100% (1)
- Tutori - Anemia MhsDocumento38 pagineTutori - Anemia Mhszaky ariandyNessuna valutazione finora
- AUB - Microscopic Analysis of UrineDocumento4 pagineAUB - Microscopic Analysis of UrineJeanne Rodiño100% (1)
- Quizni AnnieDocumento4 pagineQuizni AnnieJake Cormanes PeraltaNessuna valutazione finora
- Metastaze MedulareDocumento40 pagineMetastaze MedulareIrina StamateNessuna valutazione finora
- Anaemia Comprehensive by DR SarmaDocumento99 pagineAnaemia Comprehensive by DR SarmakyawswakyawswaNessuna valutazione finora
- FBC Analysers and FBC InterpretationDocumento63 pagineFBC Analysers and FBC InterpretationNikkole PhalulaNessuna valutazione finora
- MUST To KNOW in HematologyDocumento45 pagineMUST To KNOW in HematologyDen100% (4)
- University of Al-Ameed College of Medicine: Hematopathology Lecture PlanDocumento226 pagineUniversity of Al-Ameed College of Medicine: Hematopathology Lecture PlanYousif AlaaNessuna valutazione finora
- Red Blood Cell Morphology: A Seminar on RBC AbnormalitiesDocumento11 pagineRed Blood Cell Morphology: A Seminar on RBC AbnormalitiesChabNessuna valutazione finora
- Dr. Sailendra Nayak Assistant Professor MedicineDocumento49 pagineDr. Sailendra Nayak Assistant Professor MedicineAishwarya JeeNessuna valutazione finora
- 21 Anaemia and PancytopeniaDocumento42 pagine21 Anaemia and PancytopeniaLeon Hui MingNessuna valutazione finora
- 1.clinicolab Diagnosis PleuPeritEFFUSIONS016Documento23 pagine1.clinicolab Diagnosis PleuPeritEFFUSIONS016Elena CărăvanNessuna valutazione finora
- Normal Hematolymphoid TissuesDocumento182 pagineNormal Hematolymphoid TissuescandiddreamsNessuna valutazione finora
- Congenital Hemolytic Anemia GuideDocumento37 pagineCongenital Hemolytic Anemia GuideSomendra Mohan ShuklaNessuna valutazione finora
- Anemia Workshop1Documento80 pagineAnemia Workshop1api-3762917Nessuna valutazione finora
- 3 PracticalDocumento47 pagine3 PracticalT NNessuna valutazione finora
- HEMATOLOGY SECRETS FOR CATS & DOGSDocumento88 pagineHEMATOLOGY SECRETS FOR CATS & DOGSŞtefania MafteiNessuna valutazione finora
- Hyperkalemia How To Recognize and How To ManageDocumento26 pagineHyperkalemia How To Recognize and How To Managedhika2496Nessuna valutazione finora
- 20 CSFDocumento53 pagine20 CSFnivetha26082000Nessuna valutazione finora
- Hematology Review 2021-2Documento142 pagineHematology Review 2021-2Maram AbdullahNessuna valutazione finora
- Laboratory Picture of Patient With Blood Cell DisorderDocumento30 pagineLaboratory Picture of Patient With Blood Cell DisorderMirahNessuna valutazione finora
- A Practical Approach to Diagnosing and Treating AnemiaDocumento99 pagineA Practical Approach to Diagnosing and Treating AnemiaNipun AgrawalNessuna valutazione finora
- Apheresis SemDocumento34 pagineApheresis Semswaraj sharmaNessuna valutazione finora
- Systematic Plan For The Diagnosis of AnaemiaDocumento31 pagineSystematic Plan For The Diagnosis of AnaemiaAriyike OmoobaNessuna valutazione finora
- Love, luck and hematology reviewDocumento5 pagineLove, luck and hematology reviewKarylle HilarioNessuna valutazione finora
- Week 4 - HandoutDocumento4 pagineWeek 4 - Handoutjess waldenNessuna valutazione finora
- Routine Hematology ExaminationDocumento29 pagineRoutine Hematology Examinationgulamg21Nessuna valutazione finora
- Cardiovascular System:The Blood - NSUDocumento47 pagineCardiovascular System:The Blood - NSUGregrodockerNessuna valutazione finora
- Blood Picture; BM; LN-1Documento187 pagineBlood Picture; BM; LN-1Thriyampakan VimalanathanNessuna valutazione finora
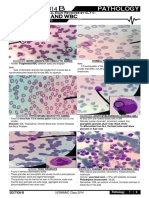
- PATHO Practicals - RBC and WBC Pathology (CLT)Documento2 paginePATHO Practicals - RBC and WBC Pathology (CLT)Miguel Cuevas DolotNessuna valutazione finora
- PansitopeniaDocumento33 paginePansitopeniaBrad WrightNessuna valutazione finora
- Complete Blood Count GuideDocumento20 pagineComplete Blood Count GuideAnastasia100% (1)
- Aplastic Anaemia: DR Sandeep M R Physician Jayanagar General Hospial BangaloreDocumento26 pagineAplastic Anaemia: DR Sandeep M R Physician Jayanagar General Hospial BangaloreSandeep m rNessuna valutazione finora
- Circulatory Anatomy GuideDocumento61 pagineCirculatory Anatomy GuideEshtiey_MegaNessuna valutazione finora
- 1 HemaDocumento35 pagine1 HemaMiaNessuna valutazione finora
- Diagnostic Laboratoric To Anemia: Prof. Dr. Adi Koesoema Aman SPPK (KH) - Dr. Malayana Nasution Mked. Clin - Path. SPPKDocumento41 pagineDiagnostic Laboratoric To Anemia: Prof. Dr. Adi Koesoema Aman SPPK (KH) - Dr. Malayana Nasution Mked. Clin - Path. SPPKrubyniNessuna valutazione finora
- MYELODYSPLASTIC SYNDROME AND MULTIPLE MYELOMADocumento46 pagineMYELODYSPLASTIC SYNDROME AND MULTIPLE MYELOMAdelaNessuna valutazione finora
- RBC and WBC MorphologyDocumento165 pagineRBC and WBC MorphologyZeeshan Yousuf100% (1)
- Fast Facts: Leucemia: Desde la mutación genética inicial hasta el apoyo para la supervivenciaDa EverandFast Facts: Leucemia: Desde la mutación genética inicial hasta el apoyo para la supervivenciaNessuna valutazione finora
- MGCTDocumento11 pagineMGCTcandiddreamsNessuna valutazione finora
- 2010 BaxterDocumento7 pagine2010 BaxtercandiddreamsNessuna valutazione finora
- 7 Restaurants Worth Visiting in KolkataDocumento5 pagine7 Restaurants Worth Visiting in KolkatacandiddreamsNessuna valutazione finora
- Best Television SeriesDocumento37 pagineBest Television SeriescandiddreamsNessuna valutazione finora
- Meningioma SDocumento10 pagineMeningioma ScandiddreamsNessuna valutazione finora
- NeuroendoDocumento8 pagineNeuroendocandiddreamsNessuna valutazione finora
- Polymorphous Breast CA.Documento6 paginePolymorphous Breast CA.candiddreamsNessuna valutazione finora
- MesotheliomaDocumento7 pagineMesotheliomacandiddreamsNessuna valutazione finora
- Gastric CancerDocumento8 pagineGastric CancercandiddreamsNessuna valutazione finora
- Male Breast CA.Documento6 pagineMale Breast CA.candiddreamsNessuna valutazione finora
- Lung OsteomaDocumento4 pagineLung OsteomacandiddreamsNessuna valutazione finora
- LeiomyomaDocumento3 pagineLeiomyomacandiddreamsNessuna valutazione finora
- Primary Intracranial Leiomyoma: A Case Report and Literature ReviewDocumento3 paginePrimary Intracranial Leiomyoma: A Case Report and Literature ReviewcandiddreamsNessuna valutazione finora
- Hepatic Collision TumourDocumento6 pagineHepatic Collision TumourcandiddreamsNessuna valutazione finora
- Hyperplastic Gastric PolypDocumento5 pagineHyperplastic Gastric PolypcandiddreamsNessuna valutazione finora
- Current Practice of Gleason Grading of Prostate Carcinoma: ReviewarticleDocumento8 pagineCurrent Practice of Gleason Grading of Prostate Carcinoma: ReviewarticlecandiddreamsNessuna valutazione finora
- Statistical Approach in HematologyDocumento33 pagineStatistical Approach in HematologycandiddreamsNessuna valutazione finora
- Eye AstrocytomaDocumento5 pagineEye AstrocytomacandiddreamsNessuna valutazione finora
- Apocrine Breast LesionsDocumento7 pagineApocrine Breast LesionscandiddreamsNessuna valutazione finora
- AtherosclerosisDocumento8 pagineAtherosclerosiscandiddreamsNessuna valutazione finora
- BreastDocumento3 pagineBreastcandiddreamsNessuna valutazione finora
- Statistical Approach in HematologyDocumento33 pagineStatistical Approach in HematologycandiddreamsNessuna valutazione finora
- Validation Cell AnalyzersDocumento45 pagineValidation Cell AnalyzerscandiddreamsNessuna valutazione finora
- Normal Hematolymphoid TissuesDocumento182 pagineNormal Hematolymphoid TissuescandiddreamsNessuna valutazione finora
- Clonality Analysis in Hematolymphoid Malignancies: DR Jay MehtaDocumento65 pagineClonality Analysis in Hematolymphoid Malignancies: DR Jay MehtacandiddreamsNessuna valutazione finora
- Mean Normal Prothombin Time (MNPT)Documento10 pagineMean Normal Prothombin Time (MNPT)candiddreamsNessuna valutazione finora
- MANI Quality Control in Hematology AnalysersDocumento65 pagineMANI Quality Control in Hematology Analyserscandiddreams100% (1)
- Gujral FCMDocumento102 pagineGujral FCMcandiddreamsNessuna valutazione finora
- Perkin Elmer Singapore Distribution CaseDocumento3 paginePerkin Elmer Singapore Distribution CaseJackie Canlas100% (1)
- Curriculum VitaeDocumento8 pagineCurriculum VitaeChristine LuarcaNessuna valutazione finora
- 6 - English-How I Taught My Grandmother To Read and Grammar-Notes&VLDocumento11 pagine6 - English-How I Taught My Grandmother To Read and Grammar-Notes&VLManav100% (2)
- Bhaktisiddhanta Appearance DayDocumento5 pagineBhaktisiddhanta Appearance DaySanjeev NambalateNessuna valutazione finora
- Prayer BuddyDocumento42 paginePrayer BuddyJoribelle AranteNessuna valutazione finora
- Contemporary Philippine Arts From The RegionsDocumento29 pagineContemporary Philippine Arts From The RegionsDina Ilagan50% (2)
- Literature ReviewDocumento4 pagineLiterature Reviewapi-549241187Nessuna valutazione finora
- Introduction To Vitamin C, (Chemistry STPM)Documento2 pagineIntroduction To Vitamin C, (Chemistry STPM)NarmeenNirmaNessuna valutazione finora
- Endocrine Hypothyroidism HyperthyroidismDocumento16 pagineEndocrine Hypothyroidism HyperthyroidismJeel MohtaNessuna valutazione finora
- New Text DocumentDocumento8 pagineNew Text DocumentDhaniNessuna valutazione finora
- People vs. Abad SantosDocumento2 paginePeople vs. Abad SantosTrixie PeraltaNessuna valutazione finora
- The Other Side of Love AutosavedDocumento17 pagineThe Other Side of Love AutosavedPatrick EdrosoloNessuna valutazione finora
- VIII MKL Duet I Etap 2018 Angielski Arkusz Dla PiszącegoDocumento5 pagineVIII MKL Duet I Etap 2018 Angielski Arkusz Dla PiszącegoKamilNessuna valutazione finora
- PallavaDocumento24 paginePallavaAzeez FathulNessuna valutazione finora
- Bible Study RisksDocumento6 pagineBible Study RisksVincentNessuna valutazione finora
- Librarianship and Professional Ethics: Understanding Standards for Library ProfessionalsDocumento12 pagineLibrarianship and Professional Ethics: Understanding Standards for Library ProfessionalsHALLNessuna valutazione finora
- Simple Past Tense The Elves and The Shoemaker Short-Story-Learnenglishteam - ComDocumento1 paginaSimple Past Tense The Elves and The Shoemaker Short-Story-Learnenglishteam - ComgokagokaNessuna valutazione finora
- Homework WatergateDocumento8 pagineHomework Watergateaapsujtif100% (1)
- Think Like An EconomistDocumento34 pagineThink Like An EconomistDiv-yuh BothraNessuna valutazione finora
- Circumstances Which Aggravate Criminal Liability People vs. Barcela GR No. 208760 April 23, 2014 FactsDocumento8 pagineCircumstances Which Aggravate Criminal Liability People vs. Barcela GR No. 208760 April 23, 2014 FactsJerome ArañezNessuna valutazione finora
- Debt Recovery Management of SBIDocumento128 pagineDebt Recovery Management of SBIpranjalamishra100% (6)
- Discuss in Details With Appropriate Examples What Factors Could Lead To Sympatric and Allopatric SpeciationDocumento5 pagineDiscuss in Details With Appropriate Examples What Factors Could Lead To Sympatric and Allopatric SpeciationKhairul ShahmiNessuna valutazione finora
- Telesure Mock 8Documento13 pagineTelesure Mock 8Letlhogonolo RatselaneNessuna valutazione finora
- Leading a Community Through Integrity and CourageDocumento2 pagineLeading a Community Through Integrity and CourageGretchen VenturaNessuna valutazione finora
- The Ontological Argument.: A Basic IntroductionDocumento12 pagineThe Ontological Argument.: A Basic IntroductionJas PalNessuna valutazione finora
- Narasimha EngDocumento33 pagineNarasimha EngSachin SinghNessuna valutazione finora
- Kurukshetra English August '17Documento60 pagineKurukshetra English August '17amit2688Nessuna valutazione finora