Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
The New Bone Level Implants - Clinical Rationale For The Development and Current Indications For Daily Practice by Buser
Caricato da
Christian OkaforTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
The New Bone Level Implants - Clinical Rationale For The Development and Current Indications For Daily Practice by Buser
Caricato da
Christian OkaforCopyright:
Formati disponibili
featuring a two-part implant design.
This development
was initiated in the mid-1980s with the design of hollow-
cylinder, hollowscrew and solid-screw implants (Sutter et
al. 1988a; Sutter et al. 1988b). Following several years of
clinical documentation, after the first ITI Consensus
Meeting in 1993, Straumann and the ITI Development
Committee decided to focus further developments mainly
on solid-screw implants, since this specific implant shape
showed excellent clinical performance in patients (Buser
et al. 1997). In consequence, new screw-type implants
were developed alongside the standard screw implant to
comply with increasing demand for optimal treatment of
various well defined clinical situations in partially
edentulous patients.
These addi ti onal i mpl ant types i ncl uded the
di ameter-reduced, wi de-body and wi de-neck
implants. All of these implants had in common a
neck portion with a machined surface of 2.8 mm in
height to locate the implant shoulder close to the
mucosal surface. For esthetic sites, these implant
types were modified and offered as a plus version
wi th a shorter, 1.8 mm machi ned neck
configuration. This esthetic implant line was later
expanded with the narrow-neck and the TE implant
(Figure 1). To improve esthetic outcomes, these
implants featuring a short, 1.8 mm machined neck
had to be inserted with their shoulder close to the
bone crest to allow a submerged or semi-submerged
healing and to avoid a visible metal collar following
restoration (Buser and von Arx 2000; Buser et al.
2004) offering good clinical outcomes (Belser et al.
1998; Giannopoulou et al. 2003).
This implant insertion technique was similar to
standard surgical techniques used for Brnemark-
type i mpl ants, and caused i ncreased bone
The new bone level implants clinical
rationale for the development and
current indications for daily practice
Daniel Buser,
1
Bruno Schmid,
2
Urs C. Belser,
3
David L. Cochran
4
1
Prof. Dr. Daniel Buser
Professor and Chairman of the Department of Oral Surgery and
Stomatology at the University of Berne.
2
Dr. Bruno Schmid
External consultant in the Department of Oral Surgery and
Stomatology at the University of Berne.
3
Prof. Dr. Urs C. Belser
Professor and Head of the Department of Fixed Prosthodontics
and Occlusion, School of Dental Medicine, University of Geneva.
4
Prof. Dr. David L. Cochran, DDS, MS, Ph.D.
Professor and Chairman of the Department of Periodontics at the
University of Texas Health Science Center at San Antonio, Dental
School.
58 INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3
Introduction
The use of osseointegrated dental implants in oral
rehabilitation has become a standard of care in daily
practice. This development was initiated more than 40
years ago in fully edentulous patients (Adell et al. 1981).
Since the mid-1980s, osseointegrated implants have been
increasingly used and documented in partially edentulous
patients (Buser et al. 1990; Lekholm et al. 1994; Buser et
al. 1997; Weber et al. 2000; Behneke et al. 2002). With
the expansion of implant therapy into partially edentulous
patients, implant manufacturers had to modify implant
shapes and components to accommodate implants in
specific clinical situations. The resulting designs were
mainly driven by anatomical considerations related to the
implant itself, whereas prosthetic aspects mainly
influenced the development of implant abutments and
other components.
The Straumann Dental Implant System (Institut
Straumann AG, Basel, Switzerland) is scientifically one of
the best documented implant systems and has been
based to date on tissue level implants (TLI), most of them
Clinical
resorption in the crestal area (Figure 2). Based on
experi mental and cl i ni cal studi es, thi s bone
resorpti on i s much better understood today
(Hammerl e et al . 1996; Cochran et al . 1997;
Hermann et al . 1997). Thi s physi ol ogi c bone
resorpti on amounts to approxi matel y 2 mm
following restoration, which is routinely seen in
radiographs on the mesial and distal aspect of the
i mpl ant (Fi gure 3). Thi s i nterproxi mal bone
resorption does not cause esthetic problems in the
papillary area, as long as the bone height is not
compromised at adjacent teeth (Choquet et al.
2001). Such bone resorption is often termed bone
saucer and is a circumferential phenomenon (Fig.
4) meaning that bone resorption also takes place on
the facial aspect of the implant (Buser et al. 2004;
Grunder et al. 2005). This can cause an esthetic
complication with soft tissue recession on the facial
aspect, if the implant shoulder is positioned too far
apically or too far facially (Buser et al. 2004, Evans
and Chen 2008).
Development of improved implant designs to
reduce crestal bone resorption
Efforts have been made for years to reduce crestal bone
resorption. One development with scalloped implants did
not fulfill high expectations (Nowzari et al. 2006).
Another development related to the platform switching
concept was accidentally discovered and has heavily
influenced implant dentistry in the past five years (Lazzara
and Porter 2006).
More than six years ago, a task force was established
by Straumann to develop a new bone level implant
based on the platform switching concept. Beside
various Straumann specialists, the working group also
included Urs Belser, Daniel Buser and David Cochran
from the ITI to provide clinical expertise for the
development. After two years of intensive in-vitro
testing of various prototypes, pre-clinical and clinical
studies were initiated to evaluate the new BLI in its
currently available form. Some of these studies have
been published in the meantime confirming the high
potential of this new implant type (Jung et al. 2008;
Buser et al. 2009). It was hypothesized that this
implant offers minimal peri-implant bone resorption
following restoration, which is important for single
tooth implants on the facial aspect, and for adjacent
implants to better maintain the bone level in the
interimplant area. In addition, the location of the
implant platform at the bone level offers the clinical
Figure 1: Straumann tissue level implants with a short 1.8 mm neck
configuration have been mainly utilized in esthetic sites (from left):
The standard plus, the narrow neck and the TE implant.
Figure 2: Implant placement of a standard plus implant in an esthetic
site routinely caused a typical bone saucer in the crestal area which
measures around 2 mm in the vertical direction and at least 1 mm in
the horizontal direction.
INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3 59
Clinical
Clinical Indications of Bone Level Implants
The new BLI has the same endosseous shape as the TE
implant, but with a cut-off neck configuration (Figure 5).
Consequently, a new abutment connection had to be
developed and it took time and effort to find an ideal
solution. Finally, the new CrossFit connection (Figure 6) was
chosen by Straumann, which offers the clinician easy
touch-and-feel handling during impression taking and
abutment insertion. The new BLI is currently available in
three different diameters (Figure 7) and offers a wide range
of prosthetic components. They are not intended to replace
tissue level implants, but to complement them for specific
clinical situations. The selection criteria of when to use
which implant type will vary from clinician to clinician based
on personal preference. Based on the above mentioned
advantages of BLI, it is clear that they will be used
predominantly in esthetic sites, since they help the clinician
to better preserve important peri-implant bone structures in
the crestal area while allowing abutment heights to vary.
Both aspects optimize esthetic outcomes.
An important indication will be the single tooth
replacement following extraction in the esthetic zone.
Thus, this indication was selected for the first clinical study
to evaluate BLI (Figures 8a, b). The prospective case series
study examined BLI with a diameter of 4.1 mm in 20
consecutive patients. The implants were inserted
following an eightweek soft tissue healing period using
the concept of early implant placement and simultaneous
contour augmentation with the GBR technique (Buser et
al. 2008, Buser et al. 2009). Particular emphasis was
placed on the correct three-dimensional positioning in the
mesio-distal, oro-facial and coronoapical direction.
Compared with tissue level implants, BLI are inserted
according to the same basic principles (Buser et al. 2004)
with one exception: BLI are inserted roughly 1 mm more
apically. It is recommended to position the implant
shoulder approximately 3 mm apical to the desired soft
tissue margin at the future implant crown mid-facially
(Figure 8c).
The one-year results showed good to excellent
esthetic treatment outcomes, objectively evaluated with
the esthetic PES (Pink Esthetic Score) and WES (White
Esthetic Score) indices (Belser et al. 2009). Bone loss was
minimal with a mean DIB value of only 0.18 mm. Only
one out of 20 implants showed more than 0.5 mm bone
loss (Figure 9).
At present, most of the two-year follow-up
examinations have been performed, but a few are still
missing. So far, the clinical and radiographic examinations
58 INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3
advantage of selecting the abutment height according
the local soft tissue characteristics and thickness. Thus,
the clinician benefits from a clearly increased
versatility.
Buser et al
Figure 3: Radiographic documentation of a typical bone saucer
around a standard plus implant ten years following implant
placement. The peri-implant bone is in a steady-state.
Figure 4: Diagram illustrating the circumferential bone saucer, which
routinely develops around tissue level implants in esthetic sites.
Critical is the bone resorption on the facial aspects, since this can
cause a mucosal recession.
sites, potential indications for BLI are sites with a
limited mesio-distal space of less than 7 mm in the
premolar area, where a regular neck implant cannot
be utilized. The smaller coronal platform of BLI makes
it possible to avoid the approximal danger zone in
such situations (Figures 12 ad).
In addition, situations with a limited vertical space from
the implant platform to the occlusal plane might be better
suited to BLI.
From a surgical point of view, the utilization of BLI can
be an advantage in osseous defect sites requiring large
augmentation volumes, since the implant has less
volume in the crestal area and facilitates an easier
application of bone fillers and of barrier membrane. This
in turn allows for easier, more tensionfree primary
wound closure (Figures 13aj).
Conclusions
The new bone level implants are a most welcome extension
to the existing tissue level implants of the Straumann
Dental Implant System. The clinical experience of more
than three years clearly confirmed the expected minimal
bone resorption at the implant shoulder in patients with
single tooth replacements. The results of a prospective case
series study also demonstrated favorable esthetic treatment
outcomes as documented by the PES-WES Index. Although
the clinical experience with two adjacent implants in the
anterior maxilla is still limited, the preliminary results are
very promising. Currently, BLIs are clinically tested in
additional indications such as posterior sites with large
58 INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3
indicate good stability of the peri-implant tissues (Figures
8d and 8e). Based on positive clinical experience with
single tooth implants, the indication for BLI was expanded
in mid-2006 for sites with two missing central incisors to
be used for adjacent implant placement. The clinical
experience with roughly 20 patients indicates good bone
stability between the implants (Figures 10 ac), but this is
a preliminary observation and needs to be confirmed by a
mid-term radiographic analysis. In 2008, an additional
indication was addressed, namely the single tooth
replacement in lateral incisor sites in the maxilla utilizing
the 3.3 mm diameter BLI (Figures 11ab). However, no
published data is available yet for the narrow diameter
BLI. Currently, we have also started to use BLI in extended
edentulous spaces in the anterior maxilla with more than
two missing teeth.
In posterior, non-esthetic sites, tissue level implants
continue to be predominantly utilized in daily practice. In
fact, the clinical experience of more than 22 years with
two part tissue level implants has clearly demonstrated
the advantages of a restoration implant interface located
in the vicinity of the soft tissue surface. With this implant
shoulder location, restorative procedures are similar to
conventional crown and bridge prosthetics, and thus easy
to control by the clinician.
In this context, one should mention the design
simplicity of cemented crowns and short-span fixed
dental prostheses (FDP). In addition, the maintenance
of peri-implant tissue health is easy to accomplish by
patients routine oral hygiene measures. In posterior
Buser et al
Figure 5: The new bone level implant has the
same endosseous shape as a TE implant.
Figure 6: Bone level implants are also
characterized by a new abutment connection,
the CrossFitTM connection.
Figure 7: Bone level implants are currently
availableinthreedifferent shapes withdiameters
of 3.3, 4.1, and 4.8 mm(fromleft to right).
bone augmentation procedures or in sites with limited
mesio-distal or vertical space. The next two to three years
will show in which indications BLIs offer particular
advantages or benefits, and thus will be preferred over
tissue level implants.
References
Adell R, Lekholm U, Rockler B, Brnemark P-I (1981). A
15-year study of osseointegrated implants in the treatment
of the edentulous jaw. Int J Oral Surg 10:387-416.
Behneke A, Behneke N, dHoedt B (2002). A 5-year
longitudinal study of the clinical effectiveness of ITI solid-
screw implants in the treatment of mandibular edentulism.
Int J O ral Maxillofac Implants 17:799-810.
Belser UC, Buser D, Hess D, Schmid B, Bernard JP, Lang
NP (1998). Aesthetic implant restorations in partially
58 INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3
Buser et al
Figure 8a: Female patient with a root fracture of tooth 11 and increased
probing depths. The contralateral tooth 21 demonstrates a gingival
recession. Tooth 11 has to be extracted and replaced with an implant
borne crown. The concept of early implant placement will be utilized.
Figure 8b: Status eight weeks following extraction. The extraction
site shows a typical flattening in the middle of the socket.
Figure 8c: Intrasurgical view demonstrating a correct corono-apical
positioning of the implant: Mid-facially, the shoulder is located roughly
3 mm apical to the future mucosal margin of the implant crown. The
peri-implant bone defect is augmented with the GBR technique.
Figure 8d: Clinical status at the two-year follow-up examination. A
pleasing esthetic outcome is noted with stable soft tissues at the
implant-supported crown. Please note a minor incisal step between
the two central incisor crowns indicating a slight growth of the
alveolar process.
Figure 8e: Periapical radiograph at the two-year examination
exhibiting the bone level implant with no crestal bone loss.
58 INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3
edentulous patients-a critical appraisal. Periodontol 2000
17:132-50.
Belser UC, Grutter L, Vailati F, Bornstein MM, Weber HP,
Buser D (2009). Outcome evaluation of early placed
maxillary anterior single-tooth implants using objective
esthetic criteria. A cross-sectional, retrospective study in 45
patients with a 2-4 year follow-up using pink and white
esthetic scores (PES/WES). J Periodontol 80:140-151.
Buser D, Weber HP, Lang NP (1990). Tissue integration of
non-submerged implants. 1-year results of a prospective
study with 100 ITI hollow-cylinder and hollow-screw
implants. Clin O ral Implants Res 1:33-40.
Buser D, Mericske-Stern R, Bernard JP, Behneke A,
Behneke N, Hirt HP, Belser UC, Lang NP (1997). Long-term
evaluation of non-submerged ITI implants. Part 1: 8-year
life table analysis of a prospective multicenter study with
2359 implants. Clin Oral Implants Res 8:161-72.
Buser D, von Arx T (2000). Surgical procedures in partially
edentulous patients with ITI implants. Clin Oral Implants
Res 11 Suppl 1:83-100.
Buser D, Martin W, Belser UC (2004). Optimizing
esthetics for implant restorations in the anterior maxilla:
anatomic and surgical considerations. Int J Oral Maxillofac
Implants 19 (Suppl):43-61.
Buser D, Chen ST, Weber HP, Belser UC (2008). The
concept of early implant placement following single tooth
extraction in the esthetic zone: Biologic rationale and
surgical procedures. Int J Periodont Rest Dent 28:440-451.
Buser D, Hart C, Bornstein M, Grutter L, Chappuis V,
Belser UC (2009). Early implant placement with
simultaneous GBR following single-tooth extraction in the
esthetic zone: 12-month results of a prospective study with
Buser et al
Figure 9: Radiographic observation at the 12-months examination
of 20 consecutive patients. No or less than 0.25 mm bone loss was
noted in 15 patients. Four patients showed a bone loss of 0.25 and
0.5 mm, whereas one implant (5%) exhibited a bone loss of 0.76 mm
(Buser et al. J Periodontol 80:152, 2009).
Figure 10a: 45-year old female patient with two missing central
incisors caused by traumatic tooth fracture. Both fractured roots are
still in place in the edentulous area. Implant placement with
simultaneous contour augmentation using GBR is planned.
Figure 10b: Clinical status nine months following implant placement
with simultanous GBR. After a soft tissue conditioning phase with
provisional crowns, both implants were restored with full ceramic
crowns. The esthetic outcome, including the central papilla, is pleasing.
Figure 10c: The periapical radiograph at nine months confirms stable
bone crest levels and shows no indication for bone loss around and
between the two implants.
58 INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3
Buser et al
Figure 11c: Clinical status nine months
following implant placement with
simultaneous GBR and restoration with an all-
ceramic crown. The soft tissue esthetic
outcome is pleasing.
Figure 11b: The cone-beam tomography illustrates the single-tooth gap with just 6 mm mesio-
distal space and a reduced crest width of less than 5 mm. This requires a simultaneous contour
augmentation using the GBR technique.
Figure 11d: The periapical radiograph
demonstrates the 3.3 mm bone level implant
with stable peri-implant bone levels.
Figure 11a: Single tooth gap with a missing
lateral incisor in the right maxilla. The mesio-
distal gap size measures roughly 6 mm and
requires a narrow diameter implant.
Figure 12b: The BLI was inserted slightly subcrestally on
the mid-facial aspect. A 2 mm healing cap was inserted.
Figure 12a: Missing first premolar in the mandible with a
reduced mesio-distal gap size of less than 6 mm at the
level of the contact points. Status during insertion of a
bone level implant (BLI 4.1 mm).
Figure 12c: Clinical outcome following
restoration with a single crown, which is
clearly smaller in size than the adjacent
second premolar.
Figure 12d: The periapical radiograph at
five months of follow-up shows no
obvious bone loss around the bone level
implant.
12c 12d
58 INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3
Buser et al
Figure 13a: 60-year old female patient with a
distal extension situation. Status six weeks
following extraction of teeth 35, 36 and 37.
Figure 13b: The periapical radiograph exhibits
the edentulous area in the posterior mandible.
The extraction sockets are clearly visible.
Figure 13c: Status following implant placement
of twobone level implants andinsertionof 2mm
healing caps. The peri-implant bone defects
require local bone augmentation with GBR.
Figure 13d: The defects have been augmented
with locally harvested autogenous bone chips
and DBBM to the level of the healing caps.
Figure 13e: The augmentation material was
covered with a resorbable collagen membrane.
Figure 13f: Implant surgery was completed with
a tensionfree primary wound closure. This is
easier to achieve compared with tissue level
implants, since less volume in the crestal area
needs to be covered.
Figure 13g: Primary soft tissue healing was
uneventful for eight weeks.
Figure 13j: The corresponding radiograph
demonstrates the 10 and 8 mm long BLI
restored with two splinted single crowns. No
bone resorption is visible around both implants.
Figure 13h: The reopening procedure was
performed with a mid-crestal incision and
insertion of longer healing caps. The wound
margins withkeratinizedmucosa were adapted
and secured with interrupted single sutures.
Figure 13i: Clinical status six months post
placement: Both implants were restored with
two splinted single crowns.
58 INTERNATIONAL DENTISTRY SA VOL. 12, NO. 3
Buser et al
submerged implants in the canine mandible. J Periodontol
68:1117-30.
Jung RE, Jones AA, Higginbottom FL, Wilson TG,
Schoolfield J, Buser D, et al. (2008). The influence of non-
matching implant and abutment diameters on radiographic
crestal bone levels in dogs. J Periodontol 79:260-70.
Lazzara RJ, Porter SS (2006). Platform switching: a
new concept in implant dentistry for controlling
postrestorative crestal bone levels. Int J Periodont Rest
Dent 26:9-17.
Lekholm U, van Steenberghe D, Hermann I, Bolender C,
Folmer T, Gunne J (1994). Osseointegrated implants in the
treatment of partially edentulous jaws: A prospective 5-year
multicenter study. Int J Oral Maxillofac Impl 9:627-635.
Nowzari H, Chee W, Y i K , Pak M, Chung WH, Rich S
(2006). Scalloped dental implants: a retrospective analysis
of radiographic and clinical outcomes of 17 NobelPerfect
implants in 6 patients. Clin Implant Dent Relat Res 8:1-10.
Sutter F, Schroeder A, Buser D (1988a). New ITI implant
concept Technical aspects and methods. Quintessenz
39:1875-1890.
Sutter F, Schroeder A, Buser DA (1988b). The new
concept of ITI hollow-cylinder and hollow-screw implants:
Part 1. Engineering and design. Int J Oral Maxillofac
Implants 3:161-72.
Weber HP, Crohin CC, Fiorellini JP (2000). A 5-year
prospective clinical and radiographic study of non-
submerged dental implants. Clin Oral Implants Res
11:144-53.
20 consecutive patients. J Periodontol 80:152-162.
Choquet V, Hermans M, Adriaenssens P, Daelemans P,
Tarnow DP, Malevez C (2001). Clinical and radiographic
evaluation of the papilla level adjacent to single-tooth
dental implants. A retrospective study in the maxillary
anterior region. J Periodontol 72:1364-71.
Cochran DL, Hermann JS, Schenk RK, Higginbottom FL,
Buser D (1997). Biologic width around titanium implants. A
histometric analysis of the implantogingival junction
around unloaded and loaded nonsubmerged implants in
the canine mandible. J Periodontol 68:186-98.
Evans CJD, Chen ST (2008). Esthetic outcomes of
immediate implant placements. Clin Oral Implants Res
19:73-80.
Giannopoulou C, Bernard JP, Buser D, Carrel A, Belser
UC (2003). Effect of intracrevicular restoration margins on
peri-implant health: clinical, biochemical, and microbiologic
findings around esthetic implants up to 9 years. Int J Oral
Maxillofac Implants 18:173-81.
Grunder U, Gracis S, Capelli M (2005). Influence of the
3-D bone-to-implant relationship on esthetics. Int J
Periodontics Restorative Dent 25:113-9.
Hammerle CHF, Brgger U, Burgin W, Lang NP (1996)
The effect of the subcrestal placement of the polished
surface of ITI implants on the marginal soft and hard
tissues. Clin Oral Implants Res 7:111-119.
Hermann JS, Cochran DL, Nummikoski PV, Buser D
(1997). Crestal bone changes around titanium implants. A
radiographic evaluation of unloaded nonsubmerged and
Potrebbero piacerti anche
- Forbidden Cures E Book DR SircusDocumento381 pagineForbidden Cures E Book DR Sircusvitaolga7100% (18)
- SFMA Score Sheet PDFDocumento7 pagineSFMA Score Sheet PDFdgclarkeNessuna valutazione finora
- Antipsychotic DrugsDocumento3 pagineAntipsychotic DrugsArtt1975Nessuna valutazione finora
- CBCTDocumento5 pagineCBCTIndahLaraswatiNessuna valutazione finora
- Bone Loss and Patterns of Bone DestructionDocumento5 pagineBone Loss and Patterns of Bone Destructionnimisha kakkadNessuna valutazione finora
- Kayachikitsa Paper 1 PDFDocumento24 pagineKayachikitsa Paper 1 PDFMayura JainNessuna valutazione finora
- Clinical Complications of Dental ImplantsDocumento25 pagineClinical Complications of Dental Implantssmritinarayan100% (1)
- Implant Failure and Their ManagementDocumento61 pagineImplant Failure and Their ManagementDharshiniNessuna valutazione finora
- Maxillofacial Prosthetics Part-1 A Revie PDFDocumento10 pagineMaxillofacial Prosthetics Part-1 A Revie PDFmehak malhotraNessuna valutazione finora
- Hematologic DisordersDocumento30 pagineHematologic DisordersUday Kumar100% (1)
- A New Veneer Technique With Prefabricated Composite Denture Teeth Combined With The "Biologically Oriented Preparation Technique" (BOPT) - A Case Report PDFDocumento14 pagineA New Veneer Technique With Prefabricated Composite Denture Teeth Combined With The "Biologically Oriented Preparation Technique" (BOPT) - A Case Report PDFLinda Garcia PNessuna valutazione finora
- Accuracy of Implant Placement With Computer-Guided SurgeryDocumento15 pagineAccuracy of Implant Placement With Computer-Guided SurgerydentureNessuna valutazione finora
- Titanium in Dentistry Historical Development State of The Art PDFDocumento7 pagineTitanium in Dentistry Historical Development State of The Art PDFPabloNessuna valutazione finora
- Vsip - Info - Anterior Wax Up PDF Free PDFDocumento3 pagineVsip - Info - Anterior Wax Up PDF Free PDFMekideche dental officeNessuna valutazione finora
- Prosthetic Rehabilitation: Part II: Technical ProceduresDocumento31 pagineProsthetic Rehabilitation: Part II: Technical ProceduresDentist HereNessuna valutazione finora
- Analysis of The Socket Bone Wall Dimensions in The Upper Maxilla in Relation To Immediate Implant PlacementDocumento6 pagineAnalysis of The Socket Bone Wall Dimensions in The Upper Maxilla in Relation To Immediate Implant PlacementLeonardo PolitoNessuna valutazione finora
- Atlas of Topographical and Pathotopographical Anatomy of the Head and NeckDa EverandAtlas of Topographical and Pathotopographical Anatomy of the Head and NeckNessuna valutazione finora
- Stoelting Anasthesia and Co Existing Disease PDFDocumento28 pagineStoelting Anasthesia and Co Existing Disease PDFEgidia SetyaNessuna valutazione finora
- Endodontic ArmamentariumDocumento29 pagineEndodontic ArmamentariumAbdulSamiNessuna valutazione finora
- Periodontology 2000 - 2023 - Urban - Minimal Invasiveness in Vertical Ridge AugmentationDocumento19 paginePeriodontology 2000 - 2023 - Urban - Minimal Invasiveness in Vertical Ridge AugmentationLEONARDO ALBERTO CRESPIN ZEPEDANessuna valutazione finora
- Prosthetic Dentistry 1916Documento1.248 pagineProsthetic Dentistry 1916lotusfrog100% (1)
- Analisis Faciales PDFDocumento8 pagineAnalisis Faciales PDFJhon CarlosNessuna valutazione finora
- Contact LensesDocumento22 pagineContact LensesDaniela DaniiNessuna valutazione finora
- Silverman 1971Documento19 pagineSilverman 1971Krupali JainNessuna valutazione finora
- ImpressionDocumento7 pagineImpressionAnnisa Nur AmalaNessuna valutazione finora
- Bone Level ImplantsDocumento9 pagineBone Level Implantshp1903Nessuna valutazione finora
- Prostho IV Slide 3 Impression Making For Complete DenturesDocumento82 pagineProstho IV Slide 3 Impression Making For Complete DenturesBoka BokaNessuna valutazione finora
- Articulation Cast Mounting and Teeth ArrangementDocumento65 pagineArticulation Cast Mounting and Teeth ArrangementMuhammad Shakeel KhawajaNessuna valutazione finora
- Intentional Living Worksheet - Copyright - Day Designer - Do Not Distribute - 03-17 PDFDocumento1 paginaIntentional Living Worksheet - Copyright - Day Designer - Do Not Distribute - 03-17 PDFCourtney JohnsonNessuna valutazione finora
- Prosthodontic Stents: March 2019Documento28 pagineProsthodontic Stents: March 2019Ahmad WahabNessuna valutazione finora
- J Esthet Restor Dent - 2024 - Esquivel - Timing Implant Provisionalization Decision Making and Systematic WorkflowDocumento10 pagineJ Esthet Restor Dent - 2024 - Esquivel - Timing Implant Provisionalization Decision Making and Systematic WorkflowDANTE DELEGUERYNessuna valutazione finora
- SupportDocumento8 pagineSupportprits_88100% (1)
- Sample Haad QuestionDocumento15 pagineSample Haad QuestionFaith Levi Alecha AlferezNessuna valutazione finora
- Digital WorkflowsDocumento14 pagineDigital Workflowsmoji_puiNessuna valutazione finora
- Semilunar Coronally Repositioned FlapDocumento5 pagineSemilunar Coronally Repositioned FlapTarun Kumar Bhatnagar100% (1)
- 11037Documento4 pagine11037api-309082881Nessuna valutazione finora
- Retainers in FPDDocumento77 pagineRetainers in FPDNiaz Ahammed100% (1)
- Bone Grafting Techniques for Maxillary ImplantsDa EverandBone Grafting Techniques for Maxillary ImplantsNessuna valutazione finora
- Harris1992 The Connective Tissue and Partial Thickness Double Pedicle GraftDocumento10 pagineHarris1992 The Connective Tissue and Partial Thickness Double Pedicle GraftAna Maria Montoya GomezNessuna valutazione finora
- Gallucci (2004) - Immediate Loading With Fixed Screw-Retained Provisional Restorations in Edentulous Jaws, The Pickup Technique.Documento10 pagineGallucci (2004) - Immediate Loading With Fixed Screw-Retained Provisional Restorations in Edentulous Jaws, The Pickup Technique.Antonio González Ruiz0% (1)
- Reconstructive Periodontal SurgeryDocumento38 pagineReconstructive Periodontal SurgeryAlnielJoManlapig100% (1)
- Vertical Jaw Relation in Complete DentureDocumento74 pagineVertical Jaw Relation in Complete DentureLeela GayatriNessuna valutazione finora
- 3D AnalysisDocumento7 pagine3D AnalysisMarllury PabonNessuna valutazione finora
- Hassall 2021Documento6 pagineHassall 2021DhanasriNessuna valutazione finora
- GTC 4 - Impressions & Retraction Cord (PPSG Lectures)Documento34 pagineGTC 4 - Impressions & Retraction Cord (PPSG Lectures)Aisha MutiaraNessuna valutazione finora
- Spear 2008Documento9 pagineSpear 2008IlseNessuna valutazione finora
- 2018 Admixed TechDocumento3 pagine2018 Admixed TechBrijesh MaskeyNessuna valutazione finora
- He History of ArticulatorsDocumento13 pagineHe History of ArticulatorsrekabiNessuna valutazione finora
- Fabrication of Occlusal RimsDocumento4 pagineFabrication of Occlusal RimsHarsha Reddy100% (1)
- 10 1016@j Prosdent 2020 05 007Documento5 pagine10 1016@j Prosdent 2020 05 007Anjali DuttaNessuna valutazione finora
- Precision of Intraoral Digital Dental Impressions With ITero and Extraoral Digitization With The ITero and A Model ScannerDocumento8 paginePrecision of Intraoral Digital Dental Impressions With ITero and Extraoral Digitization With The ITero and A Model ScannerAlex BurdeNessuna valutazione finora
- Alveolar Bone GraftDocumento12 pagineAlveolar Bone Graftanon_620185252Nessuna valutazione finora
- Whale's Tail TechniqueDocumento32 pagineWhale's Tail Techniquevijeta vyasNessuna valutazione finora
- Definition of New Three Dimensional Cephalometric.628Documento5 pagineDefinition of New Three Dimensional Cephalometric.628Hernando Luis Borja ChoisNessuna valutazione finora
- Management of Acquired Maxillary Defects Partially Edentlous PDFDocumento129 pagineManagement of Acquired Maxillary Defects Partially Edentlous PDFRamy Khalifa AshmawyNessuna valutazione finora
- Novel Porcelain Laminate Preparation 2004 PDFDocumento12 pagineNovel Porcelain Laminate Preparation 2004 PDFCarmen Breban Cirțiu100% (1)
- 3D Printing Temporary Crown and Bridge by Temperature Controlled Mask Image Projection StereolithographyDocumento11 pagine3D Printing Temporary Crown and Bridge by Temperature Controlled Mask Image Projection StereolithographyBalavigneshwaran bt18ipf04Nessuna valutazione finora
- What Is The Evidence Base For The Efficacies of Different Complete Denture Impression Procedures? A Critical ReviewDocumento16 pagineWhat Is The Evidence Base For The Efficacies of Different Complete Denture Impression Procedures? A Critical ReviewVishal ReddyNessuna valutazione finora
- Periodontal Microsurgery: Home Mcq's Discussions ContactDocumento8 paginePeriodontal Microsurgery: Home Mcq's Discussions Contactdileep9002392Nessuna valutazione finora
- Lingualised Occ RevisitedDocumento5 pagineLingualised Occ RevisitedDrPrachi AgrawalNessuna valutazione finora
- Prosthetic Management of An Existing Transmandibular Implant: A Clinical ReportDocumento5 pagineProsthetic Management of An Existing Transmandibular Implant: A Clinical ReportDragos CiongaruNessuna valutazione finora
- Applied Anatomy Related To Complete Denture-Maxilla MandibleDocumento57 pagineApplied Anatomy Related To Complete Denture-Maxilla MandibleRen Jye ChongNessuna valutazione finora
- Biologic WidthDocumento39 pagineBiologic Widthsharanya chekkarrajNessuna valutazione finora
- A Review of Esthetic Pontic Design OptionsDocumento12 pagineA Review of Esthetic Pontic Design OptionsCristhiane Rodrigues MaryNessuna valutazione finora
- Biomatric Approach For Complete Denture DesignDocumento18 pagineBiomatric Approach For Complete Denture Designفواز نميرNessuna valutazione finora
- Fixed Prosthodontics TerminologyDocumento1 paginaFixed Prosthodontics TerminologyMohammed YousriNessuna valutazione finora
- J Am Dent Assoc 2009 Spear 1160 6Documento8 pagineJ Am Dent Assoc 2009 Spear 1160 6alimordecai945Nessuna valutazione finora
- 1 s2.0 S002239131360030X MainDocumento6 pagine1 s2.0 S002239131360030X MainAmar Bhochhibhoya100% (1)
- Crestal Bone Level Alterations in Implant Therapy: August 2011Documento35 pagineCrestal Bone Level Alterations in Implant Therapy: August 2011Muhammad Shakeel KhawajaNessuna valutazione finora
- Resume 2Documento2 pagineResume 2api-576574115Nessuna valutazione finora
- Acute Abdominal PainDocumento5 pagineAcute Abdominal PainLM Mys100% (1)
- Blood Composition For REPRODUCEDocumento2 pagineBlood Composition For REPRODUCEJasmineNessuna valutazione finora
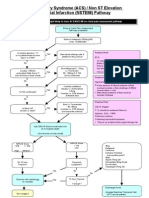
- ACS NSTEMI Clinical PathwayDocumento3 pagineACS NSTEMI Clinical PathwayXtiaRNessuna valutazione finora
- Case Clerking PPP EDDocumento13 pagineCase Clerking PPP EDFiras HashimNessuna valutazione finora
- Cues Nursing Diagnosis Goal Nursing Interventions Rationale EvaluationDocumento3 pagineCues Nursing Diagnosis Goal Nursing Interventions Rationale EvaluationVher SisonNessuna valutazione finora
- HandoutDocumento3 pagineHandoutapi-336657051Nessuna valutazione finora
- A Woman's Curse - ArticleDocumento4 pagineA Woman's Curse - ArticleSarina BacaniNessuna valutazione finora
- Effect of Crew Resource ManagementDocumento10 pagineEffect of Crew Resource ManagementoguzatikNessuna valutazione finora
- Health Assessment in NursingDocumento48 pagineHealth Assessment in NursingCj MayoyoNessuna valutazione finora
- Bayero University Kano: College of Health ScienceDocumento12 pagineBayero University Kano: College of Health ScienceNrs Sani Sule MashiNessuna valutazione finora
- Poster PPT OssnDocumento12 paginePoster PPT OssnShilpa B KNessuna valutazione finora
- Tinetti Assessment GaitDocumento1 paginaTinetti Assessment GaitAlexandru ChivaranNessuna valutazione finora
- Seminar Proposal PTDocumento2 pagineSeminar Proposal PTPeetee MomshieNessuna valutazione finora
- 16Documento198 pagine16sanjeev gaurNessuna valutazione finora
- WarmTouch User Manual Wt5200 UsDocumento34 pagineWarmTouch User Manual Wt5200 Usnobel0001Nessuna valutazione finora
- Pathology Assignment 3Documento3 paginePathology Assignment 3mah_heroNessuna valutazione finora
- ICRP Pub116Documento257 pagineICRP Pub116chibagoNessuna valutazione finora
- Aging and Down Syndrome A Health and Well-Being GuidebookDocumento44 pagineAging and Down Syndrome A Health and Well-Being GuidebookNicoleNessuna valutazione finora
- Saeed Book Bank: Leading Importers, Exporter, Distributors, Booksellers & Publishers of PakistanDocumento15 pagineSaeed Book Bank: Leading Importers, Exporter, Distributors, Booksellers & Publishers of Pakistantalisella50% (2)