Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
T Wave / T Talas
Caricato da
LidianaBeka0%(1)Il 0% ha trovato utile questo documento (1 voto)
288 visualizzazioni14 paginepromene T talasa
Titolo originale
T wave / T talas
Copyright
© © All Rights Reserved
Formati disponibili
DOCX, PDF, TXT o leggi online da Scribd
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentopromene T talasa
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato DOCX, PDF, TXT o leggi online su Scribd
0%(1)Il 0% ha trovato utile questo documento (1 voto)
288 visualizzazioni14 pagineT Wave / T Talas
Caricato da
LidianaBekapromene T talasa
Copyright:
© All Rights Reserved
Formati disponibili
Scarica in formato DOCX, PDF, TXT o leggi online su Scribd
Sei sulla pagina 1di 14
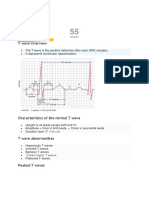
T wave
The T wave is the positive deflection after each QRS complex.
It represents ventricular repolarisation.
Characteristics of the normal T wave
Upright in all leads except aVR and V1
Amplitude < 5mm in limb leads, < 15mm in precordial leads
Duration (see QT interval)
T wave abnormalities
Hyperacute T waves
Inverted T waves
Biphasic T waves
Camel Hump T waves
Flattened T waves
Peaked T waves
Tall, narrow, symmetrically peaked T-waves are characteristically seen in hyperkalaemia.
Peaked T waves due to hyperkalaemia
Hyperacute T waves
Broad, asymmetrically peaked or hyperacute T-waves are seen in the early stages of ST-elevation
MI (STEMI) and often precede the appearance of ST elevation and Q waves. They are also seen
with Prinzmetal angina.
Hyperacute T waves due to anterior STEMI
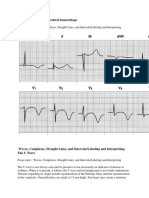
Loss of precordial T-wave balance
Loss of precordial T-wave imbalance occurs when the upright T wave is larger than that in V6. This
is a type of hyperacute T wave.
The normal T wave in V1 is inverted. An upright T wave in V1 is considered
abnormal especially if it is tall (TTV1), and especially if it is new (NTTV1).
This finding indicates a high likelihood of coronary artery disease, and when new
implies acute ischemia.
Inverted T waves
Inverted T waves are seen in the following conditions:
Normal finding in children
Persistent juvenile T wave pattern
Myocardial ischaemia and infarction
Bundle branch block
Ventricular hypertrophy (strain patterns)
Pulmonary embolism
Hypertrophic cardiomyopathy
Raised intracranial pressure
T wave inversion in lead III is a normal variant. New T-wave inversion (compared with prior
ECGs) is always abnormal. Pathological T wave inversion is usually symmetrical and deep
(>3mm).
Paediatric T waves
Inverted T-waves in the right precordial leads (V1-3) are a normal finding in children, representing
the dominance of right ventricular forces.
Normal pattern of T-wave inversions in a 2-year old boy
Persistent Juvenile T-wave Pattern
T-wave inversions in the right precordial leads may persist into adulthood and are most commonly
seen in young Afro-Caribbean women. Persistent juvenile T-waves are asymmetric, shallow
(<3mm) and usually limited to leads V1-3.
Persistent juvenile T-waves in an adult
Myocardial Ischaemia and Infarction
T-wave inversions due to myocardial ischaemia or infarction occur in contiguous leads based on the
anatomical location of the area of ischaemia/infarction:
Inferior = II, III, aVF
Lateral = I, aVL, V5-6
Anterior = V2-6
NOTE:
Dynamic T-wave inversions are seen with acute myocardial ischaemia.
Fixed T-wave inversions are seen following infarction, usually in association with
pathological Q waves.
Inferior T wave inversion due to acute ischaemia
Inferior T wave inversion with Q waves due to prior inferior MI
T wave inversion in the lateral leads due to acute ischaemia
Anterior T wave inversion with Q waves due to recent anterior MI
Bundle Branch Block
Left Bundle Branch Block
Left bundle branch block produces T-wave inversion in the lateral leads I, aVL and V5-6.
Lateral T wave inversion due to LBBB
Right Bundle Branch Block
Right bundle branch block produces T-wave inversion in the right precordial leads V1-3.
T-wave inversion in the right precordial leads due to RBBB
Ventricular Hypertrophy
Left Ventricular Hypertrophy
Left ventricular hypertrophy produces T-wave inversion in the lateral leads I, aVL, V5-6 (left
ventricular strain pattern), with a similar morphology to that seen in LBBB.
Lateral T wave inversion due to LVH
Right Ventricular Hypertrophy
Right ventricular hypertrophy produces T-wave inversion in the right precordial leads V1-3 (right
ventricular strain pattern) and also the inferior leads (II, III, aVF).
T wave inversion in the inferior and right precordial leads due to RVH
Pulmonary Embolism
Acute right heart strain (e.g. secondary to massive pulmonary embolism) produces a similar pattern
to RVH, with T-wave inversions in the right precordial (V1-3) and inferior (II, III, aVF) leads.
T wave inversion in the inferior and right precordial leads in a patient with bilateral PEs
Deep T wave inversion in V1-3 with RBBB in a patient with massive PE
Pulmonary embolism may also produce T-wave inversion in lead III as part of the S
I
Q
III
T
III
pattern
(S wave in lead I, Q wave in lead III, T-wave inversion in lead III).
SI QIII TIII pattern in acute PE
Hypertrophic Cardiomyopathy (HOCM)
HOCM is associated with deep T wave inversions in all the precordial leads.
T wave inversion in V1-6 due to HOCM
Raised intracranial pressure
Events causing a sudden rise in ICP (e.g. subarachnoid haemorrhage) produce widespread deep T-
wave inversions with a bizarre morphology.
Widespread deep T wave inversion due to SAH
Biphasic T waves
There are two main causes of biphasic T waves:
Myocardial ischaemia
Hypokalaemia
The two waves go in opposite directions:
Ischaemic T waves go up then down
Hypokalaemic T waves go down then up
Ischaemia
Biphasic T waves due to ischaemia
Hypokalaemia
Biphasic T waves due to hypokalaemia
Wellens Syndrome
Wellens syndrome is a pattern of inverted or biphasic T waves in V2-3 (in patients presenting with
ischaemic chest pain) that is highly specific for critical stenosis of the left anterior descending
artery.
There are two patterns of T-wave abnormality in Wellens syndrome:
Type 1 Wellens T-waves are deeply and symmetrically inverted
Type 2 Wellens T-waves are biphasic, with the initial deflection positive and the
terminal deflection negative
Wellens Type 1
Wellens Type 2
Camel hump T waves
This is a term used by the great ECG lecturer and Emergency Physician Amal Mattu to describe T-
waves that have a double peak or camel hump appearance.
There are two causes for camel hump T waves:
Prominent U waves fused to the end of the T wave, as seen in severe hypokalaemia
Hidden P waves embedded in the T wave, as seen in sinus tachycardia and various
types of heart block
Prominent U waves due to severe hypokalaemia
Hidden P waves in sinus tachycardia
Hidden P waves in marked 1st degree heart block
Hidden P waves in 2nd degree heart block with 2:1 conduction
Flattened T waves
Flattened T waves are a non-specific finding, but may represent ischaemia (if dynamic or in
contiguous leads) or electrolyte abnormality, e.g. hypokalaemia (if generalised).
Ischaemia
Dynamic T-wave flattening due to anterior ischaemia (above). T waves return to normal once the
ischaemia resolves (below).
Dynamic T wave flattening due to anterior ischaemia
T waves return to normal as ischaemia resolves
Hypokalaemia
Note generalised T-wave flattening with prominent U waves in the anterior leads (V2 and V3).
T wave flattening due to hypokalaemia
Potrebbero piacerti anche
- T WaveDocumento15 pagineT WaveKay BristolNessuna valutazione finora
- T WaveDocumento15 pagineT WaveKay BristolNessuna valutazione finora
- ECG NotesDocumento85 pagineECG NotesMalcum TurnbullNessuna valutazione finora
- ECG Master Class-3Documento97 pagineECG Master Class-3Shohag ID CenterNessuna valutazione finora
- ST-T Depression HannaDocumento11 pagineST-T Depression Hannadrimran570Nessuna valutazione finora
- T Wave PDFDocumento6 pagineT Wave PDFgabernNessuna valutazione finora
- УСПDocumento50 pagineУСПAli Aborges Jr.Nessuna valutazione finora
- Wellen EcgDocumento9 pagineWellen EcgElokNessuna valutazione finora
- EkgDocumento3 pagineEkgMihaela GaidurNessuna valutazione finora
- LITFL - Wellens SyndromeDocumento8 pagineLITFL - Wellens Syndromesunil abrahamNessuna valutazione finora
- ST Segment DepressiDocumento16 pagineST Segment Depressiaya405Nessuna valutazione finora
- ECG Master Class-1Documento132 pagineECG Master Class-1Shohag ID Center100% (1)
- ABC of Clinical Electrocardiography - Introduction. II-Basic Terminology - PMCDocumento11 pagineABC of Clinical Electrocardiography - Introduction. II-Basic Terminology - PMCRuban RichardNessuna valutazione finora
- ST Segment DepressiDocumento16 pagineST Segment DepressiHayaNessuna valutazione finora
- 4-Subtle ECG in ACSDocumento20 pagine4-Subtle ECG in ACSyandraNessuna valutazione finora
- Top 100 ECG CasesDocumento212 pagineTop 100 ECG Casessoha.s.tumsa7Nessuna valutazione finora
- Electrocardiograms in The Pediatric EDDocumento69 pagineElectrocardiograms in The Pediatric EDbradsoboNessuna valutazione finora
- Right Ventricular StrainDocumento9 pagineRight Ventricular StrainhasaɴNessuna valutazione finora
- ECG & ArrhythmiasDocumento8 pagineECG & ArrhythmiasDr. SobanNessuna valutazione finora
- ECG Made Easy - An Abnormal LookDocumento46 pagineECG Made Easy - An Abnormal LookabdallahNessuna valutazione finora
- Basic ECG and Arrhythmia FINALDocumento16 pagineBasic ECG and Arrhythmia FINALCharlotte James100% (5)
- TH TH TH THDocumento9 pagineTH TH TH THAlex PengNessuna valutazione finora
- ECG DiscussionDocumento33 pagineECG Discussionyrx8k8j9qyNessuna valutazione finora
- XI. T Wave Abnormalities: Frank G. Yanowitz, MD Professor of Medicine University of Utah School of MedicineDocumento1 paginaXI. T Wave Abnormalities: Frank G. Yanowitz, MD Professor of Medicine University of Utah School of MedicineLwin Maung Maung ThikeNessuna valutazione finora
- ST Segment and T Waves:: Ischemia, Infarction, Drug & Electrolyte EffectsDocumento34 pagineST Segment and T Waves:: Ischemia, Infarction, Drug & Electrolyte EffectsHibba NasserNessuna valutazione finora
- Thinking About Ecgs (Garcia)Documento9 pagineThinking About Ecgs (Garcia)Filip IonescuNessuna valutazione finora
- 15.2. ECG 2 (Chambers Enlargement)Documento149 pagine15.2. ECG 2 (Chambers Enlargement)mirabel IvanaliNessuna valutazione finora
- ECGDocumento6 pagineECGMatthew MackeyNessuna valutazione finora
- Ekg PJKDocumento113 pagineEkg PJKdevipuspaNessuna valutazione finora
- ST - Elevation Myocardial InfarctionDocumento25 pagineST - Elevation Myocardial InfarctionJo CanensNessuna valutazione finora
- ECG Findings: Valvular Heart Disease Cardiomyopathies MyocarditisDocumento30 pagineECG Findings: Valvular Heart Disease Cardiomyopathies MyocarditisensiNessuna valutazione finora
- Wellens SyndromeDocumento4 pagineWellens Syndromeqayyum consultantfpscNessuna valutazione finora
- P Wave With A Broad ( 0.04 Sec or 1 Small Square) and Deeply Negative ( 1 MM) Terminal Part in V1 P Wave Duration 0.12 Sec in Leads I and / or IIDocumento9 pagineP Wave With A Broad ( 0.04 Sec or 1 Small Square) and Deeply Negative ( 1 MM) Terminal Part in V1 P Wave Duration 0.12 Sec in Leads I and / or IIpisbolsagogulamanNessuna valutazione finora
- EKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesDocumento58 pagineEKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesRenn Karlo LindoNessuna valutazione finora
- Lia TrapaidzeDocumento32 pagineLia TrapaidzeShubham TanwarNessuna valutazione finora
- EKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesDocumento58 pagineEKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesDyah Ajeng PratiwiNessuna valutazione finora
- EKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesDocumento58 pagineEKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesWidya Surya AvantiNessuna valutazione finora
- Ekg FastlaneDocumento10 pagineEkg FastlaneAida UzunovicNessuna valutazione finora
- Introduction To ECG: Presenter: Emiacu Kenneth Facilitator: Dr. Ssebuliba MosesDocumento36 pagineIntroduction To ECG: Presenter: Emiacu Kenneth Facilitator: Dr. Ssebuliba MosesNinaNessuna valutazione finora
- Normal Atria: o o o o o o oDocumento5 pagineNormal Atria: o o o o o o oPoetraSyah اولياء 花火Nessuna valutazione finora
- Stemi, Stemi Equivalents and STEMI Mimics: Kyaw Soe WinDocumento114 pagineStemi, Stemi Equivalents and STEMI Mimics: Kyaw Soe WinYoung MilkNessuna valutazione finora
- A Normal Adult 12Documento8 pagineA Normal Adult 12el adikkzNessuna valutazione finora
- 7InitialDraft 4Documento8 pagine7InitialDraft 4pigzeniNessuna valutazione finora
- ECG TerminologyDocumento66 pagineECG TerminologyblndfflNessuna valutazione finora
- ECG NotesDocumento7 pagineECG NotesShams NabeelNessuna valutazione finora
- Physio 4.3-4.5Documento4 paginePhysio 4.3-4.5Raj BulaNessuna valutazione finora
- EKG PJK Co AssDocumento115 pagineEKG PJK Co AsssalmaNessuna valutazione finora
- EKG Interpretation: UNS Cardiovascular Dept Medical Student Lecture SeriesDocumento85 pagineEKG Interpretation: UNS Cardiovascular Dept Medical Student Lecture Seriesandina rosmalianti100% (1)
- T Wave & U WaveDocumento4 pagineT Wave & U WavejthsNessuna valutazione finora
- Stemi'Documento25 pagineStemi'Kaviya RaviNessuna valutazione finora
- 2 ECG HockstadDocumento65 pagine2 ECG HockstadAUH ICUNessuna valutazione finora
- ECG - Doc 09Documento11 pagineECG - Doc 09Rincy RajanNessuna valutazione finora
- EKG+Mastery +ischemia PDFDocumento6 pagineEKG+Mastery +ischemia PDFCatur Ari Intan PuspitasariNessuna valutazione finora
- EKG+Mastery +ischemiaDocumento6 pagineEKG+Mastery +ischemiamoussa medjahedNessuna valutazione finora
- Anterior Myocardial InfarctionDocumento14 pagineAnterior Myocardial InfarctionUtami HandayaniNessuna valutazione finora
- Anatomy, Physiology & Conduction System of The HeartDocumento122 pagineAnatomy, Physiology & Conduction System of The HeartShelly Lavenia Sambodo100% (1)
- Understanding Intracardiac EGMs: A Patient Centered GuideDa EverandUnderstanding Intracardiac EGMs: A Patient Centered GuideNessuna valutazione finora
- EKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookDa EverandEKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookNessuna valutazione finora
- Cardiac Rhythm Management Division August 2010: U.S. Product CatalogDocumento71 pagineCardiac Rhythm Management Division August 2010: U.S. Product CatalogAbid KhanNessuna valutazione finora
- BLS ExamDocumento5 pagineBLS ExamAhmed - Sawalha67% (6)
- Stroke: Dr. M.T.M RiffsyDocumento29 pagineStroke: Dr. M.T.M RiffsyTrishenth FonsekaNessuna valutazione finora
- Gore EndoprotesesDocumento4 pagineGore EndoprotesesLivio NakanoNessuna valutazione finora
- Handbook of Intravenous Fluids (Supradip Ghosh)Documento349 pagineHandbook of Intravenous Fluids (Supradip Ghosh)parijat69Nessuna valutazione finora
- Cardiovascular Surgery QuizDocumento4 pagineCardiovascular Surgery Quizjeevan more100% (2)
- Reanimacion CardiopulmonarDocumento15 pagineReanimacion CardiopulmonarVictoriano ValienteNessuna valutazione finora
- Short Learning Topics On Biomedical EquipmentsDocumento37 pagineShort Learning Topics On Biomedical EquipmentsAtif Aslam100% (1)
- Hotel Dpalma, Bandung 16 Maret 2018: Dr. Benny Prasetya PDocumento145 pagineHotel Dpalma, Bandung 16 Maret 2018: Dr. Benny Prasetya PkangheriNessuna valutazione finora
- 1.1 Cardiac Conduction SystemDocumento1 pagina1.1 Cardiac Conduction Systembilqis shabirahNessuna valutazione finora
- CPR MCQ 03Documento21 pagineCPR MCQ 03Ryam Taif100% (1)
- Cardiology MCQDocumento2 pagineCardiology MCQmohamed mowafeyNessuna valutazione finora
- Circulatory System Chapter 8.1 & 8.2 2020Documento61 pagineCirculatory System Chapter 8.1 & 8.2 2020ALEXANDER NYKKO BAYLANNessuna valutazione finora
- Cardio MechDocumento84 pagineCardio MechTim LeeNessuna valutazione finora
- #7assess CV Function Physical ExamDocumento27 pagine#7assess CV Function Physical Examkimberly dedaseNessuna valutazione finora
- Cardioversion and DefibrillationDocumento15 pagineCardioversion and DefibrillationShalini ChanduNessuna valutazione finora
- Hypertension Nursing Care PlanDocumento3 pagineHypertension Nursing Care PlanAsylla PajijiNessuna valutazione finora
- Arrhythmia - WikipediaDocumento76 pagineArrhythmia - WikipediaJamesNessuna valutazione finora
- Circulatory System NotesDocumento6 pagineCirculatory System NotesShayan UzzamanNessuna valutazione finora
- Care of Clients With Cardiovascular DisordersDocumento67 pagineCare of Clients With Cardiovascular DisordersMatt Lao DionelaNessuna valutazione finora
- Vital Signs: Temperature HypothalamusDocumento7 pagineVital Signs: Temperature Hypothalamuscringie214johanesNessuna valutazione finora
- eSP EchoDocumento18 pagineeSP EchoBeck100% (1)
- Arterial Thrombosis by AbrarDocumento20 pagineArterial Thrombosis by AbrarZain HadiNessuna valutazione finora
- Cardiovascular Disorders IIDocumento13 pagineCardiovascular Disorders IIAngel Joy CatalanNessuna valutazione finora
- Mobil-O-Graph PWA Brochure PDFDocumento1 paginaMobil-O-Graph PWA Brochure PDFhyde93Nessuna valutazione finora
- AngiographyDocumento15 pagineAngiographyCrystal AdnalacNessuna valutazione finora
- Anesthesia Management For Pulmonary Hypertension PatientsDocumento18 pagineAnesthesia Management For Pulmonary Hypertension PatientsAliNasrallahNessuna valutazione finora
- NCLEX Review Question in Cardiovascular System Part 7Documento5 pagineNCLEX Review Question in Cardiovascular System Part 7Rochelle Ricafrente100% (2)
- DLL Science-6 Q2 W3Documento6 pagineDLL Science-6 Q2 W3Grea Dela Cruz EdnilaoNessuna valutazione finora
- Catheter Ablationin in AF With CHFDocumento11 pagineCatheter Ablationin in AF With CHFKristian Sudana HartantoNessuna valutazione finora