Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
ACS Chart
Caricato da
Joey TingTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
ACS Chart
Caricato da
Joey TingCopyright:
Formati disponibili
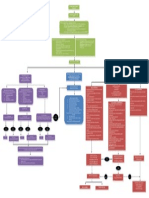
Emergency department/CCU guidelines for the management of acute coronary syndromes
ACS THERAPY ALGORITHM
Commence oxygen and ECG monitoring Insert a cannula and obtain 12-lead ECG Pain relief Blood tests Give aspirin 150-300 mg unless already given or contraindicated
Symptoms consistent with ACS
High-risk NSTEACS
Presentation with clinical features consistent with ACS and any of:
Note: All patients with ACS should be provided with a written chest pain action plan, and referred to comprehensive ongoing prevention and cardiac rehabilitation services.
Repetitive or prolonged (>10 minutes) ongoing chest pain/discomfort Elevation of at least 1 cardiac biomarker (troponin or CK-MB) Persistent or dynamic ST depression 0.5 mm or new T wave inversion 2 mm Transient ST segment elevation (0.5 mm) in more than 2 contiguous leads Haemodynamic compromise: systolic blood pressure <90 mmHg, cool peripheries, diaphoresis, Killip class >1 and/or new onset mitral regurgitation Sustained ventricular tachycardia Syncope LV systolic dysfunction (LVEF <40%) Prior PCI within 6 months or prior CABG surgery Presence of known diabetes (with typical symptoms of ACS) Chronic kidney disease estimated GFR <60 mL/ min (with typical symptoms of ACS)
Admit to coronary care or other high dependency unit and treat with aggressive medical management
Immediate ECG
PCI or CABG
Refer for angiography
Doctor to see patient within 10 minutes of arrival
(national triage category 2)
Continue to monitor: Does patient meet indications for reperfusion therapy?
Medical therapy
chest pain serial ECG cardiac markers
Persistent ST elevation 1mm in 2 contiguous limb leads; or ST elevation 2mm in 2 contiguous chest leads; or New left bundle branch block pattern
NO
Re-evaluate and risk stratify (+/- cardiology consult)
YES
Symptom onset
Intermediate-risk NSTEACS
Presentation with clinical features consistent with ACS and any of:
<1 hour ago
PCI available within 1 hour?
1-3 hours ago
PCI available within 90 minutes?
3-12 hours ago
PCI available within 90 minutes (onsite); or 2 hours (offsite, including transport time)?
Chest pain or discomfort within past 48 hours that occurred at rest, or was repetitive or prolonged (but currently resolved) Age >65 years Known CHD: Prior MI with LVEF 40% or known coronary lesion >50% stenosed No high risk ECG changes (see above) Two or more of: known hypertension, family history, active smoking or hyperlipidaemia Presence of known diabetes (with atypical symptoms of ACS) Chronic kidney disease estimated GFR <60 mL/min (with atypical symptoms of ACS) Prior aspirin use
YES
+
Stress test (e.g. exercise ECG)
YES
NO Fibrinolysis
(unless contraindicated*)
YES
NO Fibrinolysis
(unless contraindicated*)
YES
NO Fibrinolysis
(unless contraindicated*)
Recurrent ischaemia or elevated troponin at follow up testing
NO
PCI
PCI
PCI
Patients in whom brinolysis is contraindicated, or with ongoing symptoms or instability, should be transferred for PCI
AND NOT meeting the criteria for high-risk NSTEACS
Note: Reperfusion not routinely recommended in asymptomatic and haemodynamically stable patients who present more than 12 hours from symptom onset.
Low-risk NSTEACS
Presentation with clinical features consistent with ACS without intermediate or high risk features e.g.: Appropriate period of observation Discharge with urgent cardiac follow-up (on upgraded medical therapy)
* Contraindications for brinolysis
Absolute:
Relative:
Active bleeding or bleeding diathesis (excluding menses) Signicant closed head or facial trauma within 3 months Suspected aortic dissection Any prior intracranial haemorrhage Ischaemic stroke within 3 months Known structural cerebral vascular lesion Known malignant intracranial neoplasm
Current use of anticoagulants Noncompressible vascular punctures Recent major surgery (<3 weeks) Traumatic or prolonged (>10 min) CPR Recent internal bleeding (within 4 weeks) Active peptic ulcer
History of chronic, severe, poorly controlled hypertension Severe uncontrolled hypertension on presentation (systolic >180 mmHg or diastolic >110 mmHg) Ischaemic stroke >3 months ago, dementia or known intracranial abnormality (not covered in absolute contraindications) Pregnancy
Onset of anginal symptoms within the last month; or Worsening in severity or frequency of angina; or Lowering in anginal threshold
Based on the National Heart Foundation of Australia/Cardiac Society of Australia and New Zealand Guidelines for the management of acute coronary syndromes 2006. (Aroney CN, Aylward P, Kelly A-M, Chew DPB, Clune E. National Heart Foundation of Australia & Cardiac Society of Australia and New Zealand. Guidelines for the Management of Acute Coronary Syndromes 2006. Med J Aust 2006 ; 184 ; S1-S32). See guidelines for references and further details. April 2006 National Heart Foundation of Australia PP-587 ABN 98 008 419 761
Potrebbero piacerti anche
- 12 Hours: Continue To Monitor: High-Risk NSTEACSDocumento1 pagina12 Hours: Continue To Monitor: High-Risk NSTEACSMeita ReligiaNessuna valutazione finora
- Acute Surgical Topics: An Infographic GuideDa EverandAcute Surgical Topics: An Infographic GuideNessuna valutazione finora
- Cme Acs 2. Stemi (Izzah)Documento36 pagineCme Acs 2. Stemi (Izzah)Hakimah K. SuhaimiNessuna valutazione finora
- ELECTROCARDIOGRAPHY IN ISCHEMIC HEART DISEASEDa EverandELECTROCARDIOGRAPHY IN ISCHEMIC HEART DISEASENessuna valutazione finora
- Acs (Acute Coronary Syndrome)Documento54 pagineAcs (Acute Coronary Syndrome)xiaou123100% (1)
- Tatalaksana Sindrom Koroner Akut Dengan Elevasi Segmen STDocumento77 pagineTatalaksana Sindrom Koroner Akut Dengan Elevasi Segmen STQueenta SariNessuna valutazione finora
- MRCP(UK) and MRCP(I) Part II 200 CasesDa EverandMRCP(UK) and MRCP(I) Part II 200 CasesNessuna valutazione finora
- Acute Coronary Syndrome: Dr. Suhaemi, SPPD, FinasimDocumento65 pagineAcute Coronary Syndrome: Dr. Suhaemi, SPPD, FinasimshintadeviiNessuna valutazione finora
- Acutecoronary Syndrome: Dr. Suhaemi, SPPD, FinasimDocumento65 pagineAcutecoronary Syndrome: Dr. Suhaemi, SPPD, FinasimpuspayafelliNessuna valutazione finora
- St-Segment Elevation Myocardial Infarction: PGI Barrantes, Lloyd DanielDocumento28 pagineSt-Segment Elevation Myocardial Infarction: PGI Barrantes, Lloyd DanielLloyd Daniel BarrantesNessuna valutazione finora
- Acute Coronary Syndrome: Rich Derby, LT Col, USAF MGMC Family Practice ProgramDocumento56 pagineAcute Coronary Syndrome: Rich Derby, LT Col, USAF MGMC Family Practice ProgramSabilul Huda100% (1)
- CardiovascularDocumento23 pagineCardiovascularzacks nyirongoNessuna valutazione finora
- NSTEMIDocumento29 pagineNSTEMIGeanina CreangaNessuna valutazione finora
- Chest Pain Protocol in EDDocumento3 pagineChest Pain Protocol in EDshahidchaudharyNessuna valutazione finora
- Tatalaksana Sindrom Koroner Akut Dengan Elevasi Segmen ST: Saharman Leman, Rony Y SyarifDocumento77 pagineTatalaksana Sindrom Koroner Akut Dengan Elevasi Segmen ST: Saharman Leman, Rony Y SyarifSigit_Rokhmadi100% (1)
- Osce Notes - Myocardial InfarctionDocumento10 pagineOsce Notes - Myocardial InfarctionmmmalcampoNessuna valutazione finora
- Angina and MIDocumento68 pagineAngina and MIAndrassy Twinkle AlineaNessuna valutazione finora
- Algo FibrinolyticDocumento2 pagineAlgo FibrinolyticBobo SmithyNessuna valutazione finora
- Lapkas PP (STEMI)Documento68 pagineLapkas PP (STEMI)KurbulNessuna valutazione finora
- Perfusion, Class 11 ReviewedDocumento45 paginePerfusion, Class 11 ReviewedMelissa GPNessuna valutazione finora
- 11-Acs2 StemiDocumento33 pagine11-Acs2 Stemiمحمد بن الصادقNessuna valutazione finora
- Contraindications For Thrombolytic Therapy in STEMI - 2017Documento1 paginaContraindications For Thrombolytic Therapy in STEMI - 2017Dr. Muha. Hasan Mahbub-Ur-RahmanNessuna valutazione finora
- ReferatDocumento50 pagineReferatvnNessuna valutazione finora
- Stephen Wijayanto: 405110198 Group 12Documento88 pagineStephen Wijayanto: 405110198 Group 12yinvilllNessuna valutazione finora
- Present To Mam: Sajida Zahoor Presented byDocumento35 paginePresent To Mam: Sajida Zahoor Presented byM RazzaqNessuna valutazione finora
- ACS (Dr. Thamrin 2015)Documento43 pagineACS (Dr. Thamrin 2015)ok sogatenNessuna valutazione finora
- Differences BTW ACS, Stable AnginaDocumento7 pagineDifferences BTW ACS, Stable AnginaCarmenhNessuna valutazione finora
- Cardio BBDocumento73 pagineCardio BBايات عبدالرحمنNessuna valutazione finora
- Protocol 13: Chest Pain: A&E DoctorDocumento4 pagineProtocol 13: Chest Pain: A&E DoctorVanessa HermioneNessuna valutazione finora
- P ('t':'3', 'I':'669636497') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Documento56 pagineP ('t':'3', 'I':'669636497') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Muna NadiNessuna valutazione finora
- ACS (Dr. Thamrin 2015)Documento43 pagineACS (Dr. Thamrin 2015)Budianto Aj Ganteng DeweNessuna valutazione finora
- Acs TrombolitikDocumento55 pagineAcs TrombolitikDiana IswardhaniNessuna valutazione finora
- Acut Coronary Syndrome: Joko Sutrisno, S.Kep, NsDocumento54 pagineAcut Coronary Syndrome: Joko Sutrisno, S.Kep, NsJokoSutrisnoNessuna valutazione finora
- Acute Coronary Syndromes 2015Documento26 pagineAcute Coronary Syndromes 2015prototypeallhellNessuna valutazione finora
- Tony Cross CDU Low Risk ACS Proforma - V3.212 Review Due June 2014Documento4 pagineTony Cross CDU Low Risk ACS Proforma - V3.212 Review Due June 2014ED@HEFTNessuna valutazione finora
- Approach To Acute Coronary SyndromeDocumento25 pagineApproach To Acute Coronary Syndromeزكريا الحسناتNessuna valutazione finora
- Vasovagal Reflex SyndromeDocumento19 pagineVasovagal Reflex SyndromeJalalludin AnNessuna valutazione finora
- Acute Coronary Syndrome EditedDocumento38 pagineAcute Coronary Syndrome EditedSurgicalgownNessuna valutazione finora
- Acute Coronay Syndrome - BACCDocumento72 pagineAcute Coronay Syndrome - BACCYeyen Devyanti HandokoNessuna valutazione finora
- Nursing Module For Brain StrokeDocumento27 pagineNursing Module For Brain StrokeziadabiakarNessuna valutazione finora
- Topic:: Unstable AnginaDocumento44 pagineTopic:: Unstable AnginaApurba100% (1)
- Acute Coronary Syndrome: Patsadee Nachom MDDocumento58 pagineAcute Coronary Syndrome: Patsadee Nachom MDRachapon OngwibunwongNessuna valutazione finora
- Sindroma Koroner Akut: World Heart Day 29 SEPTEMBER 2021Documento68 pagineSindroma Koroner Akut: World Heart Day 29 SEPTEMBER 2021Dafhina Store100% (1)
- Chart 40-9Documento1 paginaChart 40-9MelissaNessuna valutazione finora
- Unstable AnginaDocumento20 pagineUnstable AnginaMoon AudioNessuna valutazione finora
- Advanced Cardiovascular Life Support (ACLS)Documento73 pagineAdvanced Cardiovascular Life Support (ACLS)maya_fitrianaNessuna valutazione finora
- Stemi Extensive Anterior Onset 12 Hours Killip 2Documento30 pagineStemi Extensive Anterior Onset 12 Hours Killip 2dhinialfiandariNessuna valutazione finora
- Sindrom Koroner AkutDocumento54 pagineSindrom Koroner AkutAfnil FitraNessuna valutazione finora
- ACS LectureDocumento55 pagineACS LectureAyunda AlmiradaniNessuna valutazione finora
- Cardiac Lecture NotesDocumento10 pagineCardiac Lecture NotesKateNessuna valutazione finora
- AcsDocumento20 pagineAcsTitanSeptiansyahNessuna valutazione finora
- Stemi Extensive Anterior Onset 12 Hours Killip 2Documento30 pagineStemi Extensive Anterior Onset 12 Hours Killip 2Nurul Rezki Fitriani AzisNessuna valutazione finora
- ST Segment Elevation Myocardial Infarction (Stemi) : Agus Riansyah C 111 10 335Documento39 pagineST Segment Elevation Myocardial Infarction (Stemi) : Agus Riansyah C 111 10 335Rika Sartyca IlhamNessuna valutazione finora
- Thrombolysis Version 2 0 2015 Final PDFDocumento16 pagineThrombolysis Version 2 0 2015 Final PDFtitisNessuna valutazione finora
- Tata Laksana Sindroma Koroner Akut: Cholid Tri TjahjonoDocumento84 pagineTata Laksana Sindroma Koroner Akut: Cholid Tri TjahjonoVio Alveolita PrimayaniNessuna valutazione finora
- Aula Iamcst - Cm2Documento82 pagineAula Iamcst - Cm2Sofia DiasNessuna valutazione finora
- Main Stroke Protocol - Use For All Suspected Stroke-TIA PatientsDocumento2 pagineMain Stroke Protocol - Use For All Suspected Stroke-TIA PatientsRivulet1Nessuna valutazione finora
- ACS Final DraftDocumento33 pagineACS Final Draftomcm17006Nessuna valutazione finora
- Everyday Situation Prayer For Court of HeavenDocumento9 pagineEveryday Situation Prayer For Court of HeavenJoey Ting100% (2)
- Muscles That Originate OnDocumento7 pagineMuscles That Originate OnJoey TingNessuna valutazione finora
- Visual Field DefectsDocumento3 pagineVisual Field DefectsJoey TingNessuna valutazione finora
- Foods That Nourish YinDocumento2 pagineFoods That Nourish YinJoey TingNessuna valutazione finora
- Guidelines For The Management of Haemoptysis:: Date Produced: November 2003-11-06 Next Revision: February 2012Documento3 pagineGuidelines For The Management of Haemoptysis:: Date Produced: November 2003-11-06 Next Revision: February 2012Joey TingNessuna valutazione finora
- Ijcem0006 0358Documento9 pagineIjcem0006 0358najwaNessuna valutazione finora
- 2018 ESC-EACTS Guidelines On Myocardial RevascularizationDocumento96 pagine2018 ESC-EACTS Guidelines On Myocardial RevascularizationTony Miguel Saba SabaNessuna valutazione finora
- Fractional Flow ReserveDocumento44 pagineFractional Flow Reserveusfcards100% (2)
- Nejmcp 2023658Documento9 pagineNejmcp 2023658bbraitsilvaNessuna valutazione finora
- Electrocardiography Basics: Dr. Nagula PraveenDocumento90 pagineElectrocardiography Basics: Dr. Nagula PraveenhendranatjNessuna valutazione finora
- Cardiomiopatia Hipertrofica 2016 PDFDocumento25 pagineCardiomiopatia Hipertrofica 2016 PDFBlanca Herrera MoralesNessuna valutazione finora
- Pendidikan Pasien Cath LabDocumento10 paginePendidikan Pasien Cath LabAgnesthesiaNessuna valutazione finora
- Congestive Heart Failure Nursing CareDocumento20 pagineCongestive Heart Failure Nursing Careminikompo100% (1)
- Ecg NotesDocumento35 pagineEcg NotesDanielle100% (1)
- Coils Embolization Use For Coronary Procedures - Cathet Cardio Intervent - 2023 - LohDocumento13 pagineCoils Embolization Use For Coronary Procedures - Cathet Cardio Intervent - 2023 - LohEvandro Martins FilhoNessuna valutazione finora
- Afya PresentationDocumento82 pagineAfya PresentationrebeccaNessuna valutazione finora
- Estenosis AórticaDocumento11 pagineEstenosis AórticaFamilia Morales JuradoNessuna valutazione finora
- What Is Cardiomyopathy?Documento11 pagineWhat Is Cardiomyopathy?ImmanuelNessuna valutazione finora
- Critical Care Goals and ObjectivesDocumento28 pagineCritical Care Goals and ObjectivesjyothiNessuna valutazione finora
- Myocardia IschemiaDocumento114 pagineMyocardia Ischemiasara rababahNessuna valutazione finora
- ACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)Documento11 pagineACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)김민길100% (2)
- The Main Applications of The ECG Nursing Lecture NotesDocumento19 pagineThe Main Applications of The ECG Nursing Lecture NotesMaria Rowena O. SalvoNessuna valutazione finora
- CPG Unstable AnginaDocumento58 pagineCPG Unstable AnginaAmir HassenNessuna valutazione finora
- Amiodarone Guideline For Use and MonitoringDocumento8 pagineAmiodarone Guideline For Use and MonitoringTania NicolaescuNessuna valutazione finora
- (02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle LiuDocumento18 pagine(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle LiuMikmik DGNessuna valutazione finora
- ECG Apib PDFDocumento68 pagineECG Apib PDFArthur KakarekoNessuna valutazione finora
- Cardiac SurgeryDocumento35 pagineCardiac SurgeryxxxNessuna valutazione finora
- Chapter 34 - Test QuestionsDocumento9 pagineChapter 34 - Test Questionsfriendofnurse100% (4)
- Acute Coronary SyndromesDocumento47 pagineAcute Coronary SyndromeshorosuNessuna valutazione finora
- Pharmacotherapy of ArrythmiasDocumento68 paginePharmacotherapy of ArrythmiasABREHAM BUKULONessuna valutazione finora
- Echocardiography Juni 2018Documento1 paginaEchocardiography Juni 2018Prima Agung LNessuna valutazione finora
- Update ACLSDocumento64 pagineUpdate ACLSVenansius Ratno KurniawanNessuna valutazione finora
- Coronary Artery DiseaseDocumento30 pagineCoronary Artery DiseaseDaniel Doddy Darmawan Wea100% (1)
- Jurnal Coronary Artery FistulaDocumento3 pagineJurnal Coronary Artery FistulaRistinyaUnuyNessuna valutazione finora
- 1 Part I CPR Q&ADocumento54 pagine1 Part I CPR Q&AYousaf LallarNessuna valutazione finora