Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Gastroenterolgy Reference Guide PDF
Caricato da
bibicul1958Titolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Gastroenterolgy Reference Guide PDF
Caricato da
bibicul1958Copyright:
Formati disponibili
GASTROENTEROLOGY
REFERENCE GUIDE
I
Gastroenterology
Reference Guide
57152-01 6/27/07 8:22 AM Page I
ACKNOWLEDGEMENTS:
Clinical review and editing was provided by George
Pavlou, M.D. of Laneve, Bellardini, Kosc, and Pavlou.
Text development, overall composition, and project
direction were accomplished by Patricia Vendely,
MSMT, ASCP of Quest Diagnostics Medical
Information Department.
II
Gastroenterology
Reference Guide
57152-01 6/27/07 8:22 AM Page II
PART 1. GASTROENTEROLOGY DISEASES:
SUMMARY INFORMATION
CHAPTER 1. NUTRITIONAL AND
MALABSORPTION DISORDERS
1 Section 1. Celiac Disease
10 Section 2. Food Allergies
15 Section 3. Lactose Intolerance
20 Section 4. Irritable Bowel Syndrome
CHAPTER 2. ESOPHAGEAL DISORDERS
27 Section 1. Gastroesophageal Reflux Disease
32 Section 2. Barretts Esophagus
35 Section 3. Esophageal Cancer
CHAPTER 3. STOMACH DISORDERS
43 Section 1. Peptic Ulcer Disease
(Helicobacter pylori Infection)
54 Section 2. Gastric Cancer
CHAPTER 4. GASTROENTERITIS
63 Introduction
64 Section 1. Bacterial Gastroenteritis
71 Section 2. Viral Gastroenteritis
75 Section 3. Parasitic Gastroenteritis
CHAPTER 5. INFLAMMATORY INTESTINAL
DISORDERS
81 Section 1. Diverticular Disease
86 Section 2. Inflammatory Bowel Disease
(Ulcerative Colitis and Crohns Disease)
96 Section 3. Microscopic Colitis (Collagenous
and Lymphocytic Colitis)
CHAPTER 6. COLORECTAL CANCER
99 Overview
CHAPTER 7. LIVER DISORDERS
115 Section 1. Hepatitis
127 Section 2. Primary Biliary Cirrhosis
133 Section 3. Liver Cancer
III
Gastroenterology
Reference Guide
TABLE OF CONTENTS
57152-01 6/27/07 8:22 AM Page III
IV
Gastroenterology
Reference Guide
57152-01 6/27/07 8:22 AM Page IV
Part 2. Gastroenterology Test Listing
Please refer to the printed Directory of Services to find information
about relevant tests. Alternatively, test information can be found
online at http://www.questdiagnostics.com/hcp/qtim/testMenuSearch.do.
Part 3. Test Application and Interpretation
Please refer to the printed Test Selection and Interpretation Guide
or to the online version available at http://www.questdiagnostics.com/
hcp/intguide/hcp_ig_main.html.
PART 1.
GASTROENTEROLOGY
DISEASES:
SUMMARY INFORMATION
V
Gastroenterology
Reference Guide
P
a
r
t
1
.
G
a
s
t
r
o
e
n
t
e
r
o
l
o
g
y
D
i
s
e
a
s
e
s
:
S
u
m
m
a
r
y
I
n
f
o
r
m
a
t
i
o
n
57152-01 6/27/07 8:22 AM Page V
VI
Gastroenterology
Reference Guide
57152-01 6/27/07 8:22 AM Page VI
SECTION 1. CELIAC DISEASE
OVERVIEW
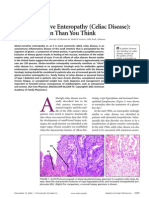
Celiac disease is caused by an immune response to
gluten in genetically susceptible individuals. Gluten is
a generic term for the storage proteins that are
found in grains (gliadin in wheat, secalin in rye,
hordein in barley, avenin in oats). Patients who have
an immune response to gluten may develop partial to
complete villous atrophy of the small intestine, crypt
hyperplasia, and lymphocytic infiltration of the
epithelium and lamina propria.
Onset of celiac disease may occur at any age from
infancy to adulthood. If left untreated, celiac disease
may be accompanied by progression of villous
atrophy and development of other autoimmune
diseases (eg, thyroid disease and insulin-dependent
diabetes mellitus), osteoporosis, and neoplasia,
including T-cell lymphoma and adenocarcinoma of
the small intestine.
Dermatitis Herpetiformis (DH)
1
DH is a related disorder in that it too is caused by
gluten sensitivity. DH manifests as an intensely pruritic
papulovesicular skin disease that affects the extensor
surfaces of the limbs and trunk and back of the scalp.
Onset is usually in the second to fourth decades of life.
The spectrum of histopathologic changes in DH
resembles the spectrum of changes seen in the small
intestine of patients with celiac disease. About 10% to
20% of patients with DH have symptoms of
malabsorption, about 20% have atypical symptoms,
and the remainder have silent celiac disease.
2
1
Gastroenterology
Reference Guide
CHAPTER 1. NUTRITIONAL AND
MALABSORPTION DISORDERS
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 1
DH Diagnosis
Diagnosis of DH requires a skin biopsy and direct
immunofluorescence staining, which reveals the
accumulation of granular IgA and C3 deposits in the
dermal papillary tips. Note that the abnormal
deposits of IgA are found in apparently normal skin
near the lesions, but may not be found in the lesions
themselves. Biopsies should be taken accordingly.
DH Treatment and Prognosis
Strict adherence to a gluten-free diet usually results
in symptom resolution. Dapsone can be prescribed to
relieve symptoms.
PREVALENCE
Estimated prevalence of celiac disease in the United
States is 1:133 people (roughly 1% of the US
population or 3 million Americans), which is much
greater than previous estimates.
3,4
Celiac disease may also occur in patients with Down
syndrome, Turner syndrome, Williams syndrome,
and selective IgA deficiency.
2
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
Table 1. Populations with an Increased Prevalence of Celiac
Disease
4
Population Prevalence (%)
First-degree relatives of individuals with biopsy-proven 4 -12
celiac disease
Second-degree relatives of individuals with biopsy-proven Undetermined
celiac disease
People with type 1 diabetes mellitus 3 - 8
People with Down syndrome 5 -12
57152-01 6/27/07 8:22 AM Page 2
SYMPTOMS
Clinical symptoms of celiac disease in adults and
children vary widely and depend on the extent of
intestinal damage and the duration of nutrient
malabsorption. Depletion of a single nutrient may be
the only symptom, often manifested as iron or folate
deficiency, osteomalacia, and edema from protein
loss. Secondary conditions may occur without
gastrointestinal symptoms. Nearly 50% of patients
may be asymptomatic (silent celiac disease).
DIAGNOSIS AND LABORATORY TESTING
Prompt diagnosis is important, as the disease can
stunt growth and development in children and lead
3
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
Table 2. Symptoms of Celiac Disease
Amenorrhea
Anemia
Bone-related symptoms:
Pain and fractures
Osteoporosis
Osteopenia
Osteomalacia (vitamin
D depletion)
Edema (due to
hypoalbuminemia)
Electrolyte depletion
Excessive appetite
Fatigue: lack of energy/
general weakness
Growth-related symptoms:
Delayed puberty
Short stature
Hyperparathyroidism
Infertility and miscarriages
Neurological changes
(peripheral neuropathy,
ataxia)
Night blindness (due to
vitamin A depletion)
Mouth sores or cracked
lips
Muscle cramping,
especially in the hands
and legs
Reduced padding on the
feet and buttocks
Smooth tongue
Tooth enamel defects
Very dry skin
Weight loss
Abdominal cramping/
distention
Chronic diarrhea*
Abdominal pain
Foul stools
Vomiting (in children)
Secondary Malabsorption-Related
Manifestations
Primary Gastrointestinal
Symptoms
*Diarrhea lasting >4 weeks.
57152-01 6/27/07 8:22 AM Page 3
to autoimmune diseases and other complications.
Presumptive diagnosis of celiac disease is based upon
a combination of symptoms, positive serology, and
biopsy of the small intestine.
4
Serologic assays can be
used to help identify patients who require biopsy and
should be performed while the patient is on a gluten-
containing diet. Diagnosis is confirmed when
symptoms resolve subsequent to a gluten-free diet. A
demonstration of normalized histology following a
gluten-free diet is no longer required for a definitive
diagnosis of celiac disease unless the patient was
asymptomatic at the time of initial diagnosis (ie,
diagnosis was based solely on biopsy and serology).
Testing should be considered for patients with
4
:
Autoimmune disease (thyroiditis, type 1 diabetes
mellitus)
Cerebellar ataxia
Delayed puberty
Dental enamel hypoplasia
Infertility
Iron-deficiency anemia
Irritable bowel syndrome
Recurrent fetal loss
Peripheral neuropathy
Persistent aphthous stomatitis
Short stature
Unexplained gastrointestinal symptoms
Unexplained transaminase elevations
Celiac disease prevalence is increased in the following
and testing may be considered in selected patients
4
:
Down syndrome
First- and second-degree relatives with celiac disease
Type 1 diabetes mellitus
4
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 4
Turner syndrome
Williams syndrome
Serology
Tissue transglutaminase (tTG; IgA) antibody is an
excellent first-line marker, with high sensitivity and
specificity in untreated individuals.
5
The endomysial
antibody (EMA; IgA) assay has high specificity for
celiac disease and is usually used to confirm positive
IgA anti-tTG results. It should also be considered in
cases in which the IgA anti-tTG result is negative but
clinical suspicion remains high. The IgG anti-tTG is
usually performed when the total IgA is low. Some
patients with limited villous atrophy have been
reported to lack EMA and tTG antibodies, and
testing for IgA antigliadin antibody (AGA) may help
detect celiac disease in such patients.
6
Total serum
IgA is measured to identify selective IgA deficiency,
present in about 2% to 10% of celiac disease patients.
Such patients would have negative results on IgA
anti-tTG and EMA assays but may have positive IgG
anti-tTG results. Because levels of anti-tTG and EMA
tend to wane in the absence of gluten ingestion,
these markers are useful to monitor adherence to a
gluten-free diet. Tests can be performed individually
or as a comprehensive panel.
Biopsy
4,7
Biopsy of the proximal small bowel is indicated in
individuals with a positive celiac disease antibody test
and for those whose symptoms and other laboratory
tests indicate malabsorption. Multiple biopsies should
be obtained from the descending part of the
duodenum or beyond (as histologic changes may be
focal). The pathology report should specify the
degree of crypt hyperplasia and villous atrophy as
5
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 5
well as the number of intraepithelial lymphocytes.
Some degree of villous atrophy (Marsh type 3) is
considered necessary for a positive biopsy.
4
Patients
with silent, atypical, or occult celiac disease and those
who have DH may exhibit normal or mild villous
atrophy; thus, histopathology may not be diagnostic.
An infiltrative change with crypt hyperplasia (Marsh
type 2) is consistent with celiac disease, but not
diagnostic.
7
Hyperplasia alone (Marsh type 1) is not
specific for celiac disease. In patients with Marsh type
1 or 2, positive serology strengthens the diagnosis.
HLA typing, repeat biopsy and/or serology, and a
trial of gluten-free diet may be helpful when the
diagnosis is still in question.
7
Genetic Markers
When serology and biopsy results are indeterminate,
HLA haplotype testing can be helpful by stratifying
an individual into a low- or high-risk category.
4
Greater than 97% of people with celiac disease have
the DQ2 and/or DQ8 variant; thus, an individual
who lacks both is highly unlikely to have celiac
disease. However, since about 40% of the general
population carry these variants, presence of the
variant(s) is not diagnostic of celiac disease.
3
TREATMENT
Strict adherence to a gluten-free diet is the only
treatment for celiac disease and DH. A gluten-free
diet is defined by the National Institutes of Health as
one that excludes wheat, rye, and barley.
4
The gluten-
free diet recommendations of the Celiac Sprue
Association also exclude spelt, Kamut
'
, and oats.
While the information on oats is inconclusive, it
should also be excluded due to the potential for
gluten contamination during processing.
4
6
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 6
PROGNOSIS
Strict adherence to a gluten-free diet usually results
in prompt symptom resolution. In most cases, the
small intestine heals and returns to normal function.
Rarely, people with celiac disease have refractory
disease and continue to have symptoms even after
theyve eliminated gluten from their diet. Others may
develop refractory sprue after an initial, often
lengthy, improvement on gluten-free diet. Some
people with refractory disease have collagenous
sprue in which a layer of collagen-like material is
seen below the basement membrane.
3
Treatment
with immunosuppressive agents may help, though
the prognosis is poor.
8
The most significant complication of celiac
disease is development of gastrointestinal and
nongastrointestinal cancers, enteropathy associated
T-cell lymphoma (EATL), and other lymphomas. A
gluten-free diet may diminish the risk of developing
lymphoma.
4
A lymphoma should be suspected in
patients whose disease was previously controlled by
a gluten-free diet and in other patients with
refractory disease.
3,9
The all-cause mortality for
patients with celiac disease is twice that of controls.
4
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Dietetic Association (ADA) Dietary
Support Coalition
Internet: http://www.eatright.org/Public
7
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 7
Association of Gastrointestinal Motility Disorders
Inc. (AGMD)
Phone: 781-861-3874
Internet: http://www.agmd-gimotility.org
Celiac Disease Foundation (CDF)
Phone: 818-990-2354
Internet: http://www.celiac.org
Celiac Sprue Association/USA Inc.
Phone: 877-CSA-4-CSA (272-4272)
Internet: http://www.csaceliacs.org
Digestive Disease National Coalition
Phone: 202-544-7497
Internet: http://www.ddnc.org
Gluten Intolerance Group of North America (GIG)
Phone: 206-246-6652
Internet: http://www.gluten.net
Intestinal Disease Foundation
Phone: 877-587-9606
Internet: http://www.intestinalfoundation.org
National Digestive Diseases Information
Clearinghouse
Phone: 800-891-5389
Internet: http://digestive.niddk.nih.gov/ddiseases/
pubs/celiac/index.htm
National Foundation for Celiac Awareness
Phone: 215-325-1306
Internet: http://www.celiacawareness.org
8
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 8
REFERENCES
1. Yancey KB, Lawley TJ. Immunologically mediated skin diseases. In: Kasper
DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds.
Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-
Hill; 2005:311-318.
2. Zone JJ. Skin manifestations of celiac disease. Gastroenterology.
2005;128:S87-S91.
3. Binder HJ. Disorders of absorption. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1763-1776.
4. National Institutes of Health. NIH Consensus Development Conference
Statement on Celiac Disease [June 28-30, 2004]. Available at:
http://consensus.nih.gov/2004/2004CeliacDisease118html.htm.
Accessed October 18, 2006.
5. Farrell RJ, Kelly CP. Diagnosis of celiac sprue. Am J Gastroenterol.
2001;96:3237-3246.
6. Green PH, Jabri B. Coeliac disease. Lancet. 2003;362:383-391.
7. Hill ID, Dirks MH, Liptak GS, et al. Guideline for the diagnosis and
treatment of celiac disease in children: recommendations of the North
American Society for Pediatric Gastroenterology, Hepatology and
Nutrition. J Pediatr Gastroenterol Nutr. 2005;40:1-19.
8. Murray JA. The widening spectrum of celiac disease. Am J Clin Nutrition.
1999;69:354-365. Available at: http://www.ajcn.org/cgi/content/full/
69/3/354. Accessed October 13, 2005.
9. Celiac disease [MedicineNet website]. Available at:
http://www.medicinenet.com/celiac_disease/page11.htm. Accessed
October 13, 2005.
9
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 9
SECTION 2. FOOD ALLERGIES
OVERVIEW
Food allergy is an immunologically based
hypersensitivity to 1 or more foods. Sensitization may
occur from ingestion of the substance, from
breathing in proteins that are similar to the ones in
the food(s), or through the skin when the barrier
function is impaired. This hypersensitivity can involve
multiple clinical syndromes and may result in severe
and sometime fatal anaphylaxis upon second and
subsequent exposures to the particular food(s).
Symptoms can manifest locally in the GI tract or in
remote organs.
Food allergy can manifest as: 1) an immediate,
anaphylactic, fixed reaction (typical IgE mediated) or
2) a delayed, chronic, cyclic reaction. The symptom
severity of the latter is related to both the quantity
and frequency of food ingested.
Food allergies occur in people of all ages, though the
patterns differ in adults versus children. Children
sometimes outgrow their allergies (especially to milk,
egg, soy, and wheat); adults do not. Allergies to
peanuts, tree nuts, fish, and shellfish are usually
enduring.
Food allergies should be differentiated from other
reactions to foods, including food intolerance and
food idiosyncrasy. These adverse reactions to a food
or additive involve difficulty with the digestion or
metabolism of the substance and are generally
localized, temporary, and rarely life threatening.
10
Gastroenterology
Reference Guide
IgE (Immunoglobin E)
Also known as reagin, or
reaginic antibody, antigen-
specific IgE is 1 of 5 classes
of human immunoglobins. It
interacts with mast cells and
eosinophils to protect the
host against invading
parasites. The same
antibody-cell combination is
also responsible for
immediate hypersensitivity
allergic reactions such as
hay fever, asthma, hives, and
anaphylaxis.
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 10
PREVALENCE
Food allergies are relatively uncommon, affecting 2%
to 5% of the general population.
1
They occur more
often in children (~8%) than in adults (~2%).
1
People at risk for food allergies include those with a
personal or family history of allergies, especially food
allergies. Environmental factors (eg, exposure to
tobacco smoke) may also be involved.
PREVENTION
The American Academy of Pediatrics provides the
following recommendations
1
to prevent development
of a food allergy:
Continuation of breastfeeding for 1st year of the
infants life
Supplement breastfeeding with hypoallergenic
formulas if infant at risk
Avoidance of peanuts and tree nuts and, possibly,
eggs, cows milk, and fish while breastfeeding
Introduce solid foods only after 5 months of age in
high-risk infants
Delay feeding infants dairy products until 1 year of
age, eggs until 2 years, and peanuts, nuts, and fish
until 3 years
The effectiveness of these recommendations,
however, is not yet proven.
1
SYMPTOMS
Symptoms may be mild or severe and may develop
gradually or progress rapidly to life-threatening
anaphylaxis. Symptoms may involve the skin,
gastrointestinal tract, respiratory system, vascular system,
11
Gastroenterology
Reference Guide
Common Causes of Allergic
Food Reactions
The most common causes of
allergic food reactions in
children and adults include:
Eggs (hen)
Milk (cow)
Soy
Wheat
Fish
Fruit
Shellfish (shrimp,
lobster, crab)
Vegetables
Peanuts
Tree Nuts (walnut,
cashew, Brazil,
pistachio)
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
Children
Adults
All
57152-01 6/27/07 8:22 AM Page 11
or the larynx. Anaphylactic reactions occur more
commonly in response to milk, eggs, peanuts, tree nuts,
fish, and shellfish than in response to other allergens.
Symptoms may include the following:
Anaphylaxis (urticaria and angioedema [flushing],
bronchospasm)
Rhinoconjunctivitis (nasal congestion, runny nose,
sneezing)
Edema of lips, tongue, palate, throat (difficulty
swallowing)
Asthma (bronchospasm: difficulty breathing,
shortness of breath, wheezing)
Hypotension (light-headed, fainting)
Nausea, abdominal pain, vomiting, diarrhea
Atopic dermatitis (eczema, hives, rash, itching)
DIAGNOSIS AND LABORATORY TESTING
Diagnosis begins with a relevant history and physical,
focusing on:
List of suspect foods
Quantity of food consumed prior to reaction
Repeatability of reaction to particular food
Time between exposure (eg, ingestion or
inhalation) and reaction
Symptoms (type and duration)
Examination of target organ systems
When the history and physical are consistent with an
IgE-related allergy, the next step is usually food-specific
IgE testing to determine the presence or absence of
an IgE-mediated immune reaction to the suspected
food(s). A positive food-specific IgE test is considered
diagnostic when consistent with the patients history. If
a positive IgE test is not consistent with the history,
either an oral food challenge (see below) or a trial
12
Gastroenterology
Reference Guide
Food-specific IgE Tests
Traditionally, food-specific
IgE skin tests were
performed to diagnose or
rule out IgE mediated food
allergies. Percutaneous skin
tests (PSTs) are
recommended over
intracutaneous skin tests
because intracutaneous
tests are overly sensitive,
and thus have a high rate of
false-positive results, and
are associated with risk of
anaphylaxis and death.
Food-specific IgE serum
tests have roughly the same
sensitivity and specificity as
the skin tests and
consequently have the same
clinical application. Serum
tests are especially useful
when the patient has a
history of a life-threatening
reaction or a medical
condition that prevents
accurate skin testing (eg,
extensive atopic dermatitis
or dermatographism) and
when the patient is known to
have a nonreactive
histamine control or is
known to be pregnant.
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 12
elimination diet is the recommended next step
depending on whether the symptoms are episodic or
chronic, respectively.
1
In a trial elimination diet,
suspected foods are eliminated from the patients diet
for several weeks and then gradually reintroduced one
at a time while the patient is observed for signs of an
allergic reaction.
If the IgE test is negative, further evaluation using a
double blind, placebo controlled food challenge may
be warranted. The patient swallows capsules that
contain either the suspected food or a placebo. A
third party keeps records of the capsules contents
and thus enables the patient and the physician to
judge reactions objectively.
TREATMENT
Dietary avoidance of the implicated food is the
primary treatment. However, vague or inaccurate
labeling or cross-contamination may result in
accidental exposure to the implicated food. If an
anaphylactic reaction results, epinephrine should be
administered (injected).
Individuals subject to anaphylactic reactions should
carry injectable epinephrine.
PROGNOSIS
Prognosis is excellent when dietary avoidance is
successful. However, individuals subject to
anaphylactic reactions should always carry injectable
epinephrine for emergency use.
In some cases, dietary avoidance may lead to future
tolerance, or partial tolerance, of the food.
13
Gastroenterology
Reference Guide
Radioimmunoassay
procedures
(radioallergosorbent test
[RAST]) are no longer used.
Current methods use a food-
specific allergen bound to a
solid phase to detect IgE in
the patients serum. World
Health Organization-based
standards are used to
quantify results, which are
reported in kIU/L.
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 13
Additionally, children often outgrow their allergy to
substances such as milk, eggs, and wheat.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
FDA Center for Food Safety and Applied Nutrition
Information About Food Allergies
Internet: http://www.cfsan.fda.gov/~dms/
wh-alrgy.html
US Food and Drug Administration
5600 Fishers Lane
Rockville, MD 20857-0001
Phone: (888) INFO-FDA (463-6332)
National Institute of Allergy and Infectious Diseases
Phone: 301-496-5717
Internet: http://www.niaid.nih.gov
NIAID Office of Communications and Public
Liaison
6610 Rockledge Drive, MSC 6612
Bethesda, MD 20892-6612
The Food Allergy & Anaphylaxis Network
Phone: 800-929-4040
Internet: http://www.foodallergy.org
REFERENCE
1. American College of Allergy, Asthma, and Immunology. Food allergy: a
practice parameter. Ann Allergy Asthma Immunol. 2006;96(Suppl 2):S1-S68.
14
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 14
SECTION 3. LACTOSE INTOLERANCE
OVERVIEW
Lactose intolerance results from a deficiency in
lactase. Individuals who are deficient in this enzyme
cannot adequately digest lactose, a carbohydrate
present in dairy products. Undigested lactose
osmotically attracts water, leading to diarrhea.
Furthermore, bacteria in the intestines ferment the
lactose, producing gas, which leads to bloating and
abdominal pain.
Primary Lactose Intolerance
Although lactase disappears following the postnatal
period in most animals, it is retained in some human
ethnic groups and lost in others. Symptoms develop
as lactase disappears, usually in the adolescent or
adult years. Such individuals are deemed to have
primary lactose intolerance, an inherited condition
in which lactase is decreased or absent while other
digestive enzymes are not. Other aspects of intestinal
absorption are usually normal. The amount of dairy
products that can be consumed asymptomatically
depends on the degree of lactase deficiency; many
people are asymptomatic.
Secondary Lactose Intolerance
Secondary lactase deficiency stems from disorders
that damage the small-bowel mucosa (eg, celiac
sprue, tropical sprue, and intestinal infection). Other
digestive enzymes may be deficient, and the patient
may have difficulty absorbing many nutrients.
Resolution of the underlying disorder can lead to
resolution of the lactase deficiency.
15
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 15
Congenital Lactose Intolerance
Rarely, infants will be born without lactase. The
condition may be either secondary and temporary
due to premature birth or primary and permanent.
PREVALENCE
Since gradual loss of the lactase enzyme is a normal
process, many people are affected. The enzymatic
loss is more pronounced in African Americans
(>85%), Asian Americans (>90%), Hispanics (~80%)
and Native Americans (>50%).
1,2
In white people of
Northern European descent, however, less than 20%
are affected.
1,2
SYMPTOMS
Not all people with lactose intolerance are
symptomatic since development of symptoms
depends on the degree of lactase deficiency and the
amount of dairy products consumed, the speed at
which the stomach and small intestines are emptied,
and use of antibiotics that affect intestinal microflora.
Those who are symptomatic may have:
Bloating
Abdominal pain or cramps
Diarrhea
Flatulence
Nausea
Symptom onset is about 30 minutes to 2 hours after
eating or drinking foods containing lactose. Severity
varies depending on the amount of lactose each
individual can tolerate.
16
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 16
DIAGNOSIS AND LABORATORY TESTING
Diagnosis begins with a review of symptoms, medical
history, and physical exam. If lactose intolerance is
then suspected, several tests can be used to support
the diagnosis.
Fecal pH
Acidic stool (low pH) is associated with carbohydrate
malabsorption; this test is not specific for lactose
intolerance, however, so follow-up testing is needed.
Lactose Breath Test
The amount of exhaled hydrogen is measured before
and after ingesting 50 g of lactose. The amount of
hydrogen exhaled increases in affected patients
subsequent to bacterial fermentation of the lactose.
Gas, including hydrogen, is released during
fermentation, absorbed into the bloodstream, and
carried to the lungs, from which it is expelled.
Sensitivity and specificity for lactose intolerance are
above 95%.
2
Lactose Challenge
Blood glucose is measured before and after the
patient ingests a lactose load (1.0 to 1.5 g/kg body
weight).
2
Affected patients develop symptoms and
have only a minimal rise in glucose level. This test is
less specific than the breath test.
2
Therapeutic Trial
The patient eliminates dairy products from his/her
diet for a period of time prior to undergoing a
lactose challenge (eg, 1 quart of milk). If symptoms
17
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 17
abate during the period of abstinence and return
with the lactose challenge, a presumptive diagnosis of
lactose intolerance is made.
If symptoms persist while the patient is on a strict
lactose deficient diet, inflammatory bowel disease
should be suspected since the symptoms of these
disorders are similar.
TREATMENT
There is no cure for lactose intolerance but ingesting
either limited amounts or no dairy products can
prevent symptoms. Small amounts of milk (<12 oz per
day) or yogurt are well tolerated in some patients.
Lactase supplements are available in tablet or liquid
form and may facilitate lactose digestion in some
patients. Calcium supplements should be considered
for those restricting their intake of dairy foods.
PROGNOSIS
Prognosis is excellent. A carefully chosen diet is the
key to reducing symptoms and protecting future
health.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Dietetic Association (ADA)
120 South Riverside Plaza, Suite 2000
Chicago, IL 60606-6995
Phone: 800- 366-1655 or 800-877-1600
Internet: http://www.eatright.org
18
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 18
International Foundation for Functional
Gastrointestinal Disorders (IFFGD)
PO Box 170864
Milwaukee, WI 53217-8076
Phone: 888-964-2001
Email: iffgd@iffgd.org
Internet: http://www.aboutibs.org
http://www.iffgd.org
REFERENCES
1. Binder HJ. Disorders of absorption. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1763-1776.
2. Gastrointestinal disorders. In: Beers MH, Porter RS, Jones TV, Kaplin JL,
Berkwits M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed.
Merck Publishing Group; 2006. Available at: http://www.merck.com/
mmpe/sec02/ch017/ch017c.html?qt=lactose%20intolerance&alt=sh.
Accessed November 15, 2006.
19
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 19
SECTION 4. IRRITABLE BOWEL SYNDROME
OVERVIEW
Irritable bowel syndrome (IBS), sometimes referred
to as spastic colon, is an intestinal motility disorder
that interferes with normal function of the colon. IBS
manifests with abdominal pain or discomfort,
constipation, diarrhea, or both. Usually either
constipation or diarrhea is predominant in an
individual patient. Structural abnormalities are
absent. The colon can be more sensitive and reactive
than usual to certain foods and stress. While IBS
causes a great deal of discomfort and distress, it does
not damage the intestines or lead to any serious
complications.
Most patients (70%) have mild disease while others
(25%) have disease of moderate severity. The
remainder (5%) have severe disease.
1,2
ETIOLOGY
The cause of IBS is not clear. There appears to be a
complex interaction between genetics, the
environment, psychosocial factors (eg, life stress,
psychologic state, coping mechanisms, social
support), and physiology (eg, gut motility, visceral
hypersensitivity). Symptoms may occur following
gastrointestinal infection, increased fat or alcohol
intake, traveling, vigorous physical activity, or
psychologic stress.
PREVALENCE
IBS is a relatively common disorder that affects 10%
to 20% of people in the United States.
2
The disorder
occurs twice as often in women than in men,
2
and
20
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 20
80% of those with severe symptoms are women.
1
Prevalence is similar in whites and African
Americans, but may be lower in Hispanics.
2
Patients
usually first present in the third to fifth decades of
life.
2
SYMPTOMS
Symptoms usually occur during the day, but not at
night. They are episodic, lasting an average of 5 days
and may occur several times a month.
2
Periods of
constipation may be followed by a period of diarrhea.
Symptoms wax and wane over the years.
2
Symptoms of IBS include:
Abdominal pain, often relieved by defecation or
passing of gas
Bloating
Perceived flatulence
Constipation and/or diarrhea due to altered rate of
stool movement through the intestinal tract
Mucus in the stool
Sensation of incomplete evacuation after defecation
Rectal urgency and/or incontinence
Dyspepsia
Heartburn
Nausea, vomiting
If the above symptoms occur without pain, alternative
diagnoses should be sought.
Factors that exacerbate IBS symptoms include:
Eating, especially when rapid; especially lipids
Emotional/psychiatric stress
Premenstrual and menstrual phases
Particular foods (patient specific)
21
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 21
DIAGNOSIS AND LABORATORY TESTING
Diagnosis is primarily based on clinical features and
exclusion of other disorders and thus begins with a
complete medical history and physical examination.
The Rome III diagnostic criteria (Table 1) define the
disorder.
When a patient meets the Rome criteria but presents
with alarm signs (ie, those suggesting another
diagnosis) (Table 2), further testing is
recommended. If alarm signs are absent, another
diagnosis is rarely made and further testing may not
be warranted. Diagnostic algorithms are presented in
references 4 and 2 for the primary care physician
and gastroenterologist, respectively.
The following diagnostic tests may be employed,
depending on a particular patients situation:
Complete blood count (CBC)
Hemoccult (stool blood test)
Sedimentation rate (ESR)
Serum chemistries
TSH
Ova and parasites (O&P)
Colonoscopy or sigmoidoscopy
Endomysial and tissue transglutaminase IgA
antibodies to rule out celiac sprue
22
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
Table 1. Rome III Diagnostic Criteria
1-3
At least 3 months, which need not be consecutive, in the
preceding 6 months of abdominal discomfort or pain
associated with 2 of the following 3 features:
1. Relieved by defecation
2. Onset associated with a change in frequency of stool
3. Onset associated with a change in form (appearance) of
stool
57152-01 6/27/07 8:22 AM Page 22
Fecal lactoferrin to rule out inflammatory bowel
disorder
H. pylori test to rule out peptic ulcer disease
Hydrogen breath test or therapeutic trial to rule
out lactose intolerance
Therapeutic trials for constipation (fiber or osmotic
laxative), diarrhea (loperamide, diphenoxylate-
atropine, cholestyramine), pain/gas/bloating
(anticholinergic, antidepressant, psychologic
treatment)
Imaging studies (GI tract, gallbladder)
TREATMENT
Therapy varies depending on the type of symptoms
(eg, predominant constipation vs diarrhea) and their
severity and on the presence of psychosocial
problems. All patients should be educated about the
disorder. Regular physical activity helps alleviate stress
and improve bowel function.
Some patients may benefit from dietary changes if
certain substances exacerbate symptoms. These
23
Gastroenterology
Reference Guide
Differentiating IBS and
Inflammatory Bowel
Disorder (IBD)
Patients with IBD may
develop rectal bleeding and
permanent intestinal
damage. Additionally, they
frequently require long-term
steroid therapy and
immunosuppressive agents.
Consequently, distinguishing
IBS from IBD is critical for
patient management.
Fecal Lactoferrin
Increased in active IBD
Not increased in IBS
86% sensitive and 100%
specific in distinguishing
IBD from IBS
5
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
Table 2. Primary Features Suggesting Non-IBS
Diagnosis
Absence of concurrent psychosocial symptoms
Family history of colon cancer or inflammatory bowel disease
Onset at an older age
Persistent diarrhea after a 48-hour fast
Presence of nocturnal diarrhea or steatorrheal stools
Progressive course of disease
Vomiting
Weight loss
Anemia
Increased sedimentation rate
Leukocytes or blood in stool
Stool volume >200 to 300 mL/d
57152-01 6/27/07 8:22 AM Page 23
substances may include fatty foods, beans and other
gas-producing foods (eg, apples, grape juice,
bananas, nuts, raisins, cabbage), alcohol, caffeine,
and lactose. High fiber diets and stool bulking agents
may be helpful in some but not others; data
regarding efficacy is controversial. Certain types of
sugar (eg, sorbitol, mannitol, fructose) might also be
problematic for some patients.
Medications may include the following:
Antispasmodics (anticholinergics) for pain and
bloating
Antidiarrheal agents (loperamide [Imodium
'
],
diphenoxylate, cholestyramine)
Osmotic laxatives (milk of magnesia, sorbitol,
polyethylene glycol) for constipation
Antidepressants (eg, tricyclics, selective serotonin
reuptake inhibitors [SSRIs])
5-HT
3
receptor antagonists (cilansetron) for
diarrhea and pain
5-HT
4
receptor agonists (tegaserod) for
constipation
Biofeedback, acupuncture, yoga, and meditation may
help some patients.
PROGNOSIS
IBS is a lifelong condition with exacerbations and
remissions, but most people can control their
symptoms with diet, stress management, and
medication. For others, IBS can be severe and
disabling.
24
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 24
RESOURCES
Association of Gastrointestinal Motility Disorders
(AGMD)
11 North Street
Lexington, MA 02420
Phone: 781-861-3874
Email: AGMDInc@aol.com
Internet: http://www.agmd-gimotility.org
International Foundation for Functional
Gastrointestinal Disorders (IFFGD)
PO Box 170864
Milwaukee, WI 53217-8076
Phone: 888-964-2001
Email: iffgd@iffgd.org
Internet: http://www.aboutibs.org
http://www.iffgd.org
REFERENCES CITED
1. Owyang C. Irritable bowel syndrome. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1789-1793.
2. Drossman DA, Camilleri M, Mayer EA, et al. AGA technical review on
irritable bowel syndrome. Gastroenterology. 2002;123:2108-2131.
3. Drossman D. The launching of Rome III. Available at:
http://www.romecriteria.org/launch.pdf#search=%22Rome%20Criteria
%20III%20IBS%22. Accessed: September 22, 2006.
4. Fass R, Longstreth G, Pimentel M, et al. Evidence- and consensus-based
practice guidelines for the diagnosis of irritable bowel syndrome. Arch
Intern Med. 2001;161:2081-2088.
5. Kane SV, Sandborn WJ, Rufo PA, et al. Fecal lactoferrin is a sensitive and
specific marker in identifying intestinal inflammation. Am J Gastroenterol.
2003;98:1309-1314.
ADDITIONAL REFERENCE
1. Irritable bowel syndrome (IBS). In: Beers MH, Porter RS, Jones TV,
Kaplin JL, Berkwits M, eds. The Merck Manual of Diagnosis and Therapy.
18th ed. Merck Publishing Group; 2006. Available at: http://
www.merck.com/mmpe/sec02/ch008/ch008e.html?qt=inflammatory%20
bowel%20syndrome&alt=sh. Accessed November 16, 2006.
25
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 25
26
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
1
:
N
u
t
r
i
t
i
o
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 26
SECTION 1. GASTROESOPHAGEAL REFLUX
DISEASE
OVERVIEW
Gastroesophageal reflux disease (GERD) is a highly
variable chronic condition that is characterized by
periodic episodes of gastroesophageal reflux,
classically accompanied by heartburn. Incompetent
barriers at the gastroesophageal junction enable the
backflow of gastric acid and other gastric contents
into the esophagus, pharynx, larynx, and
tracheobronchial tree, which in turn causes the
symptoms of GERD. Over time, the acid may damage
the lining of the esophagus. Untreated, GERD can
progress to esophagitis. Severe reflux esophagitis can
be complicated by Barretts esophagus, a risk factor
for cancer.
ETIOLOGY
Reflux occurs when the pressure gradient between
the lower esophageal sphincter (LES) and the
stomach is either lost or inadequate. This may be due
to unexplained muscle weakness or loss of tone in
the LES as well as a myriad of other causes such as
myopathy, pregnancy, smoking, and medications, to
name a few. Ineffectiveness of the diaphragmatic
crural muscle can also set the stage for GERD.
Factors that may contribute to reflux include:
Increase in gastric volume (eg, after meals)
Increase in proximity of gastric contents to the
gastroesophageal junction as occurs when lying or
bending down or with a hiatal hernia
27
Gastroenterology
Reference Guide
CHAPTER 2. ESOPHAGEAL DISORDERS
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 27
Increase in gastric pressure caused by obesity,
pregnancy, tight clothing, and ascites
Ingestion of certain substances including alcohol,
caffeine, carbonated beverages, fatty foods,
chocolate, and mint
PREVALENCE
The published prevalence figures vary depending on
the source; however, one thing is clear: GERD is
relatively common. It may affect as many as 40% of
adults in the United States.
1-3
SYMPTOMS
The most common symptoms include:
Regurgitation of gastric contents (sour material)
into the mouth
Heartburn (burning sensation due to irritation of
the esophagus by acidic gastric contents)
Less common symptoms include:
Chronic cough
Bronchoconstriction
Pharyngitis
Laryngitis
Bronchitis
Pneumonia
Morning hoarseness
Wheezing (asthma)
Angina-like or atypical chest pain
Dysphagia
Some patients are asymptomatic and do not seek
treatment until severe complications occur.
28
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 28
Infants may also present with irritability, vomiting,
and anorexia.
DIAGNOSIS AND LABORATORY TESTING
Most people with GERD can be diagnosed based on
their symptoms. Diagnostic tests (Table 1) may be
helpful for patients who have either no response or
inadequate response to treatment and those with
evidence of complications.
TREATMENT
The goals of treatment are to provide symptom relief,
heal erosive esophagitis, and prevent further
complications. Table 2 details therapeutic options.
PROGNOSIS
Treatment is usually effective in suppressing acid
reflux and heartburn. Standard doses of PPI therapy
can heal esophageal erosion within 8 weeks in about
29
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
Table 1. Diagnostic Tests for GERD
1,2,4
Test Purpose
Barium esophagram (ie, barium Diagnose peptic stricture or esophageal ulcer;
swallow radiograph, an X-ray study relatively low sensitivity and specificity
of the esophagus) compared with endoscopy
Endoscopy with biopsy, if indicated Diagnose erosive esophagitis, peptic stricture,
ulcer, Barretts esophagus, or adenocarcinoma
Esophageal pH (ie, ambulatory Document and quantitate acid reflux in
reflux monitoring) symptomatic patients who are unresponsive to
treatment and have an unremarkable
endoscopy
Esophageal manometry Ensure accurate placement of pH probes (see
(motility study) above); determine degree of competence of
the LES and esophageal motor function prior
to surgical treatment
57152-01 6/27/07 8:22 AM Page 29
30
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
Table 2. GERD Therapy
1,2,4
Lifestyle changes* Weight reduction, if indicated
Elevate head while sleeping (4-6 inches)
Avoid tobacco, fatty foods, coffee, alcohol, chocolate, mint,
orange juice
Avoid certain medications (eg, anticholinergics, smooth-
muscle relaxants, calcium channel blockers)
Avoid large fluid intake with meals
Avoid eating within 2 to 3 hours of bedtime
Avoid tight clothing
Medications Antacids
o Useful in mild cases
o Available over-the-counter
o Include: Alka-Seltzer
'
, Maalox
'
, Mylanta
'
, Pepto-Bismol
'
,
Rolaids
'
, Tums
'
Proton pump inhibitors (PPI)
o Acid suppressor (provides symptomatic relief and heals
esophagitis)
o Include: Prilosec
'
, Prevacid
'
, Nexium
'
, Protonix
'
,
Aciphex
'
)
H2 receptor blocking agents
o Acid suppressor (provides symptomatic relief and heals
esophagitis)
o Less effective than PPIs, but may be useful in less severe
cases
o Include: Tagamet HB
'
, Pepcid AC
'
, Axid AR
'
, Zantac 75
'
)
Promotility agents
o Used in conjunction with acid suppressor for selected
patients
o Side effects are common
o Include: metoclopramide, bethanechol, cisapride,
domperidone tegaserod, baclofen
Surgery Fundoplication (gastric fundus is wrapped around the LES to
increase LES pressure)
Endoscopic therapy Radiofrequency application (eg, Stretta
'
)
Endoscopic sewing techniques
*Of uncertain efficacy.
4
57152-01 6/27/07 8:22 AM Page 30
90% of patients.
1
Therapy may have to be prescribed
long-term, however, to keep symptoms from
returning. In untreated or refractory patients, GERD
may cause serious complications:
Reflux esophagitis occurs when acid, pepsin, and
bile damage the mucosa.
o Mild esophagitis is characterized by infiltration of
the mucosa with eosinophils or granulocytes,
basal cell hyperplasia, and elongation of dermal
pegs.
o Erosive esophagitis involves more severe mucosal
damage that can result in esophageal bleeding
ulcers.
Peptic stricture occurs when fibrosis causes
constriction of the lumen (frequency: ~10% of
untreated cases).
Barretts esophagus, a rare premalignant condition,
occurs in some patients with erosive esophagitis.
REFERENCES
1. Goyal RK. Diseases of the esophagus. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1739-1746.
2. Gastroesophageal reflux disease (GERD). In: Beers MH, Porter RS, Jones
TV, Kaplin JL, Berkwits M, eds. The Merck Manual of Diagnosis and
Therapy. 18th ed. Merck Publishing Group; 2006. Available at:
http://www.merck.com/mmpe/sec02/ch012/ch012f.html?qt=gerd&alt=
sh. Accessed November 21, 2006.
3. Delaney BC. Review article: prevalence and epidemiology of
gastrooesophageal reflux disease. Aliment Pharmacol Ther. 2004;20(Suppl
8):2-4.
4. DeVault KR, Castell DO. Updated guidelines for the diagnosis and
treatment of gastroesophageal reflux disease. Am J Gastroenterol.
2005;100:190-200.
31
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 31
SECTION 2. BARRETTS ESOPHAGUS
OVERVIEW
The American College of Gastroenterology (ACG)
defines Barretts esophagus as a change in the
esophageal epithelium of any length that can be
recognized at endoscopy and is confirmed to have
intestinal metaplasia by biopsy of the tubular
esophagus and excludes intestinal metaplasia of the
cardia.
1
Barretts esophagus is characterized by replacement
(metaplasia) of esophageal squamous epithelium with
columnar epithelium during healing of acute
esophagitis. Columnar epithelium is more resistant to
damage by acid and pepsin than is squamous
epithelium. Short-segment Barretts (<2-3 cm in
length) appears to be less severe than long-segment
Barretts (>2-3 cm). The metaplasia in both, however,
can lead to dysplasia and esophageal adenocarcinoma.
ETIOLOGY
Barretts esophagus is a complication of severe reflux
esophagitis, which is a complication, in turn, of
gastroesophageal reflux disease (GERD) (see
Chapter 2, Section 1).
PREVALENCE
About 0.5% of people develop long-segment Barretts
while about 15% develop short-segment Barretts.
2
The
disorder occurs more frequently in white men than in
women or in men of other ethnicities. Prevalence
increases with increasing age. More importantly,
Barretts esophagus is most prevalent in those who
have chronic (10 years) GERD symptoms.
1
32
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 32
SYMPTOMS
Most people with Barretts esophagus have symptoms
of GERD; some people, however, are asymptomatic.
There are no clinical symptoms that differentiate
people who have GERD without Barretts esophagus
from those who have GERD with Barretts esophagus.
DIAGNOSIS AND LABORATORY TESTING
Since people with chronic GERD symptoms are more
likely to have Barretts esophagus, the ACG
recommends upper endoscopy for such patients after
reflux symptoms are controlled with therapy.
1
Biopsy
of abnormal esophageal mucosa should then be
taken to document intestinal metaplasia (eg,
replacement of squamous epithelium by columnar
epithelium) and to detect dysplasia, which is the first
step in the neoplastic process.
1
TREATMENT
When active esophagitis is present, patients are
treated with acid suppression therapy and, possibly,
with surgery. Although such treatment can control
GERD symptoms and maintain a healed mucosa, it
does not reduce the grade of Barretts esophagus nor
eliminate the risk of cancer.
Endoscopic surveillance (Table 1) is instituted to
monitor the patient for dysplasia and early
adenocarcinoma. Endoscopic mucosal resection
(esophagectomy) may be advisable for patients with
multifocal dysplasia and/or mucosal irregularity.
1
Such an approach may prevent frank cancer and the
associated risk of metastasis.
33
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:22 AM Page 33
Other treatments include photodynamic therapy and
surgical esophagectomy.
PROGNOSIS
Control of GERD symptoms and periodic monitoring
of patients with Barretts esophagus, followed by
surgical resection when clinically indicated, is the
best hope of survival for these patients.
REFERENCES
1. Sampliner RE and the Practice Parameters Committee of the American
College of Gastroenterology. Updated guidelines for the diagnosis,
surveillance, and therapy of Barretts esophagus. Am J Gastroenterol.
2002;97:1888-1895.
2. Goyal RK. Diseases of the esophagus. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1739-1746.
34
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
Table 1. Endoscopic Surveillance of Patients with
Barretts Esophagus
1
Degree of Dysplasia Surveillance
No dysplasia* Endoscopy at 3-year interval
Low-grade Endoscopy and biopsy yearly until
dysplasia no longer detected
High-grade, focal Endoscopy and biopsy every
3 months
*On 2 consecutive endoscopies with biopsy.
57152-01 6/27/07 8:22 AM Page 34
SECTION 3. ESOPHAGEAL CANCER
OVERVIEW
Cancer of the esophagus is a lethal cancer as
evidenced by the equivalence between the yearly
number of cases diagnosed and the number of
deaths.
1
Esophageal cancers are either squamous cell
carcinomas or adenocarcinomas. Squamous cell
esophageal carcinoma arises in squamous cells lining
the esophagus and usually occurs in the upper
(cervical) and middle part of the esophagus.
Adenocarcinoma usually develops in the glandular
tissue in the lower (distal) part of the esophagus.
Adenocarcinomas account for more than 50% of all
esophageal cancers.
2
RISK FACTORS
Risk factors associated with esophageal carcinoma are
listed in Table 1. Alcohol and tobacco use are the
strongest risk factors for squamous cell disease, while
35
Gastroenterology
Reference Guide
Esophageal Cancers
2
15% occur in the cervical
esophagus
35% occur in the mid-
esophagus
50% occur in the lower
esophagus
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
Squamous cell
Alcohol consumption (excess)* Fanconis anemia
Cigarette smoking* Ingestion of nitrites or lye
Chronic achalasia Obesity
Diet deficient in molybdenum, zinc, Plummer-Vinson or Paterson-Kelly
vitamin A syndrome
Esophageal irradiation Tylosis (congenital hyperkeratosis and
Extremely hot tea (long-term ingestion) pitting of palms and soles)
Adenocarcinoma
Barretts esophagus Cigarette smoking
Chronic GERD Obesity
GERD, gastroesophageal reflux disease.
*Risk increases with increasing use; these 2 factors increase risk synergistically.
Table 1. Esophageal Carcinoma Risk Factors
2,3
57152-01 6/27/07 8:22 AM Page 35
Barretts esophagus is the strongest risk factor for
adenocarinoma.
PREVALENCE
The American Cancer Society estimates there will be
14,550 new cases and 13,770 deaths from esophageal
cancer in the United States in 2006.
1
It affects more
African Americans than whites and approximately 3
times as many men as women.
2,3
Most cases occur in
older people (ie, 65-74 years of age).
3
SYMPTOMS
In the early stages of esophageal cancer, patients are
asymptomatic. Symptoms usually do not manifest
until the disease is incurable. The first 2 symptoms
listed in Table 2 are classic and affect most patients.
Patients have difficulty swallowing solid food when
first presenting with dysphagia. As the disease
progresses, the patient will have difficulty swallowing
semi-solid foods and, finally, liquids (including
saliva). Weight loss occurs in 75% of patients.
3
SCREENING
General population screening is not recommended
for either type of esophageal cancer; however, the
American Gastroenterological Association (AGA)
36
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
Progressive dysphagia
Weight loss
Aspiration pneumonia
Cough
Gastrointestinal bleeding
Hiccups
Hoarseness
Pain in the chest or back
Pain when swallowing
Regurgitation
Vocal cord paralysis
Vomiting
Table 2. Symptoms of Esophageal Carcinoma
57152-01 6/27/07 8:22 AM Page 36
supports endoscopic screening for a subgroup of
patients with gastroesophageal reflux disease
(GERD).
3
This subgroup consists of white males over
50 years of age. Other high-risk groups that may be
suitable for screening include those with tylosis, lye-
induced strictures, Fanconis anemia, achalasia, and
prior head-and-neck cancer as well as those with
chronic tobacco and alcohol use.
3
SURVEILLANCE
The AGA supports periodic monitoring of patients
with Barretts esophagus.
3
Four-quadrant biopsies of
Barretts mucosa (every 1-2 cm, depending on
degree of dysplasia) may be performed. The AGA
recommendations are similar to those of the
American College of Gastroenterology (Table 3).
Patients with confirmed high-grade dysplasia may be
treated with surgical resection and mucosal ablation
with photodynamic therapy (PDT) to prevent cancer
development.
DIAGNOSIS AND LABORATORY TESTING
During an endoscopic procedure, biopsies are taken
from any suspicious areas. A cytologic examination is
then performed on the tissue. Cytology of tumor
37
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
Degree of Dysplasia AGA Recommendations ACG Recommendations
None 5-year intervals 3-year intervals
Low-grade 1 to 2 year intervals Yearly until dysplasia no
longer detected
High-grade 3-month intervals for 2 years, Every 3 months
then every 6 months
Table 3. Frequency of Monitoring Patients with Barretts Esophagus
3,4
AGA, American Gastroenterological Association; ACG, American College of Gastroenterology.
57152-01 6/27/07 8:22 AM Page 37
brushings may be indicated to complement biopsies.
Inspection of the larynx, trachea, and bronchi, in
addition to the esophagus, may be advisable in
patients with a history of smoking and alcohol use.
Since treatment decisions are based on the stage of
disease, the following procedures should be
considered to assess stage: computed tomography
(CT) of the chest and upper abdomen, endoscopic
ultrasonography (EUS), fine-needle aspiration, and
positron emission tomography (PET).
STAGING
The American Joint Committee on Cancer (AJCC)
has outlined terminology for staging esophageal
38
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
Tumor staging
T0 No evidence of primary tumor
Tis Carcinoma in situ
T1 Tumor invades lamina propria or submucosa
T2 Tumor invades muscularis propria
T3 Tumor invades adventitia
T4 Tumor invades adjacent structures
Nodal staging
N0 No evidence of metastasis to regional lymph nodes
N1 Evidence of metastasis to regional lymph node(s)
Metastasis
M0 No evidence of distant metastasis
M1 Evidence of distant metastasis
M1a Metastasis to celiac nodes (tumor in lower thorax)
M1a Metastasis to cervical nodes (tumor in upper thorax)
M1b Metastasis to nonregional or other nodal groups (tumor in midthorax)
M1b Distant metastasis (tumor in lower esophagus or upper thorax)
X Unable to assess metastasis presence/absence
Table 4. TNM Staging of Esophageal Cancers
3
57152-01 6/27/07 8:22 AM Page 38
cancers (Tables 4 and 5).
3
Tumor staging may be
further divided as shown in Table 6.
TREATMENT
Endoscopic resection is commonly used for
squamous cell cancers confined to the mucosa or
upper third of the submucosa. Endoscopic resection
with or without photodynamic therapy (PDT) is used
to treat adenocarcinomas detected in an early stage
(stages 1 and 2a). Patients with more advanced
disease (stage 2b or 3) might be treated with
radiation and chemotherapy (neoadjuvant therapy)
before undergoing surgery. This helps lower the
stage of the cancer prior to surgical resection,
thereby improving the chance of survival. Patients
39
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
Stage Definition
0 Tis, N0, M0
1 T1, N0, M0
2a T2-3, N0, M0
2b T1-2, N1, M0
3 T3, N1, M0
3 T4, any N, M0
4 Any T, any N, M1
4a Any T, any N, M1a
4b Any T, any N, M1b
Table 5. Definition of Esophageal Cancer Stages
3
T1m T1 confined to the mucosa
T1sm T1 penetrating the submucosa
T1sm1 T1sm in upper third of submucosa
T1sm2 T1sm in middle third of submucosa
T1sm3 T1sm in lower third of submucosa
Table 6. Sub-categorization of T1 Stage
3
57152-01 6/27/07 8:22 AM Page 39
with stage 4 disease are treated with either
radiation/chemotherapy or palliative therapy.
PROGNOSIS
If diagnosed and treated at an early stage, patients
with esophageal cancer have a good chance of 5-year
survival. However, if not diagnosed and treated until
a later stage, prognosis is poor. Thus, screening and
monitoring of high-risk individuals is critical to
management of this cancer.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Cancer Society
Phone: 800-ACS-2345 (227-2345)
Internet: www.cancer.org
Cancer Care, Inc.
Phone: 800-813-HOPE (813-4673) or 212-221-3300
Email: info@cancercare.org
Internet: www.cancercare.org
Cancer Hope Network
Phone: 877-HOPENET (467-3638) or 908-879-4039
(New Jersey Residents)
Email: info@cancerhopenetwork.org
Internet: www.cancerhopenetwork.org
Cancer Information Service (CIS)
Phone: 800-4-CANCER (422-6237)
TTY: 800-332-8615 (for deaf and hard of hearing)
Internet: http://cis.nci.nih.gov/
40
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 40
National Cancer Institute
Phone: 800-422-6237 or 301-496-6631
Internet: www.cancer.gov
www.nci.nih.gov
NCI's Facing Forward Series
Phone: 888-4-CANCER (422-6237)
Internet: www.nci.nih.gov/cancerinfo/
life-after-treatment
National Coalition for Cancer Survivorship
Phone: 877-622-7937 or 301-650-9127
Email: info@canceradvocacy.org
Internet: http://www.canceradvocacy.org
The Cancer Information Network
Internet: www.cancerlinksusa.com/stomach/
index.asp
The Wellness Community Executive Office
Phone: 888-793-WELL (793-9355) or 202-659-9709
Email: help@thewellnesscommunity.org
Internet: www.thewellnesscommunity.org
REFERENCES
1. American Cancer Society. Cancer Facts and Figures 2006. Atlanta:
American Cancer Society; 2005. Available at: http://www.cancer.org/
docroot/STT/stt_0.asp. Accessed November 21, 2006.
2. Mayer RJ. Gastrointestinal tract cancer. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:523-533.
3. Wang KK, Wongkeesong M, Buttar NS. American Gastroenterological
Association technical review on the role of the gastroenterologist in the
management of esophageal carcinoma. Gastroenterology. 2005;128:1471-
1505. Also available at: http://scholar.google.com/scholar?hl=en&lr=&q=
cache:DL2IvPLiS7wJ:www.spg.pt/docspdfs/ AGAesofago.pdf+. Accessed
November 22, 2006.
4. Sampliner RE and the Practice Parameters Committee of the American
College of Gastroenterology. Updated guidelines for the diagnosis,
surveillance, and therapy of Barretts esophagus. Am J Gastroenterol.
2002;97:1888-1895.
41
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 41
42
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
2
:
E
s
o
p
h
a
g
e
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 42
SECTION 1. PEPTIC ULCER DISEASE
(HELICOBACTER PYLORI INFECTION)
OVERVIEW
Peptic ulcer disease (PUD) is characterized by
ulcers within the stomach and/or duodenum. Such
ulcers may be caused by Helicobacter pylori infection,
ingestion of a non-steroidal anti-inflammatory drug
(NSAID), or, rarely, Zollinger-Ellison syndrome.
H pylori accounts for most PUD (~70% of gastric
ulcers and up to 90% of duodenal ulcers).
1
NSAIDs
are the second most common cause of PUD.
Subsequent to the withdrawal of some COX-2
inhibitors (eg, rofecoxib, valdecoxib), NSAID-
induced PUD may be on the rise, especially in the
elderly. Like NSAIDs, COX-2 inhibitors reduce
inflammation, but without irritating the stomach as
do the NSAIDs. With the diminished availability of
the COX-2 inhibitors, doctors must again rely on
NSAIDs to treat inflammatory conditions in spite of
the damaging side effects.
Since H pylori accounts for such a large proportion of
PUD, it will be the focus of the discussion in this
section. H pylori infection is a gram-negative
bacterium that colonizes the stomach. It is suited to
living in a highly acidic environment owing to its
ability to produce urease. Urease stimulates
production of ammonia from urea, and the
ammonia damages the epithelial cells lining the
stomach wall, making it susceptible to gastric acid.
The bodys inflammatory response leads to further
epithelial cell damage, and other enzymes produced
by H pylori damage the mucosa. Damage can lead to
gastritis, PUD, mucosal-associated lymphoid-type
(MALT) lymphoma, and gastric cancer.
43
Gastroenterology
Reference Guide
CHAPTER 3. STOMACH DISORDERS
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 43
Another important factor in H pylori infection is the
ability of the bacterium to move from the antrum of
the stomach to more proximal segments of the
stomach. Location of the bacterium is associated with
clinical disease: antral-predominant infection is most
closely linked with increased acid secretion and
duodenal ulcers, whereas infection primarily in the
body of the stomach (corpus-predominant) is linked
with decreased acid secretion, gastric ulcers, and
development of gastric cancer.
ETIOLOGY AND RISK FACTORS
H pylori is acquired via oral-oral and fecal-oral routes.
Risk of acquiring the infection is associated with:
Poor socioeconomic status
Less education
Birth or residence in a developing country
Domestic overcrowding
Unsanitary living conditions, including unclean
food and water
Exposure to gastric contents of infected individual
(eg, vomit, contaminated endoscope)
Other factors contributing to ulcer development
include NSAIDs, cigarette smoking, and selected
chronic disorders (eg, systemic mastocytosis,
pulmonary disease, renal failure, cirrhosis,
nephrolithiasis, alpha1-antitrypsin deficiency).
Evidence implicating a role for genetic
predisposition, personality type, psychological
stress, certain foods, alcohol, or caffeine is
inconclusive.
44
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 44
PREVALENCE
Acid peptic disorders affect about 4 million people
per year in the United States.
2
This equates to a 10%
to 12% lifetime prevalence of PUD.
2
Overall, about 30% of the U.S. population is
infected with H pylori.
2
Some of these infections are
asymptomatic or mild; not all progress to PUD. H pylori
prevalence increases with increasing age and is more
prevalent in African Americans and Hispanics.
The prevalence of both PUD and H pylori infection is
declining owing to improved sanitation and medical
intervention.
SYMPTOMS
PUD is characterized by dyspepsia. Burning or
gnawing epigastric pain that is worse when fasting
and relieved by eating is common, but not seen in all
patients. Alternatively, the patient may experience an
ill-defined, aching or hunger sensation. Some
patients experience no symptoms until they have a
bleeding ulcer.
In patients with gastric ulcer, pain may be
precipitated, rather than relieved, by eating. Bloating,
nausea, vomiting, and weight loss may also occur and
may suggest more complicated disease.
In patients with duodenal ulcer, patients may awake
with abdominal pain in the middle of the night. They
are more likely to experience relief 2 to 3 hours after
eating or after ingesting an antacid.
Signs of complicated PUD (gastrointestinal bleeding,
perforation, gastric outlet obstruction) include:
45
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 45
Variation in intensity or distribution of abdominal
pain
Consistent pain, not relieved by food or antacid
Pain radiating to the back
Sudden onset of severe, generalized abdominal
pain
Nausea, vomiting
Weight loss
Bloody or black stools
Vomit with appearance of coffee grounds
Anemia
DIAGNOSIS AND MANAGEMENT
Endoscopy enables visualization of the ulcer; it is the
method of choice for definitive diagnosis of PUD,
being preferred over barium radiography.
1
Additionally, endoscopy enables early detection of
gastric cancer and Barretts esophagus. However,
since endoscopy is expensive, other options may be
preferable for managing patients with upper
abdominal pain (dyspepsia). Options include:
Empirical acid suppression
Noninvasive H pylori test followed by endoscopy if
positive
Noninvasive H pylori test followed by eradication
therapy if positive (ie, "test and treat")
Empirical H pylori eradication therapy (no testing)
Early endoscopy
The American Gastroenterological Association
(AGA) recommends H pylori test and treat (followed
by acid suppression if symptoms persist) for patients
with dyspepsia who are <55 years of age and have no
alarm symptoms (eg, weight loss, dysphagia, signs of
blood loss).
3
This approach is cost-effective and may
prevent distal gastric cancer; however, empirical acid
46
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 46
suppression may be a good choice when the
prevalence of H pylori is 10%.
3
For older patients
and those with alarm features, the AGA recommends
early endoscopy.
3
A biopsy should be taken during
endoscopy for H pylori testing. If positive, eradication
therapy can be instituted to reduce the risk of PUD
and gastric cancer.
3
LABORATORY TESTING FOR DIAGNOSIS
Invasive and noninvasive tests are available for H pylori:
Upper gastrointestinal tract biopsy, histologic exam,
rapid urease testing (RUT), and culture
Antibody detection
Antigen detection
Urea breath test (BreathTek
'
UBiT
'
) employing
14
C- or
13
C-urea
When endoscopy is not indicated, the preferred
methods for H pylori testing are the
13
C-urea breath
test and the stool antigen tests, because serology
(antibody detection) is less accurate and does not
differentiate active from resolved infection.
3
When
endoscopy is indicated, histology is the test of choice.
Culture is not very sensitive but may be useful for
antibiotic resistance testing in patients unresponsive
to therapy.
Rationale Against the Use of Serologic Tests
4
Serologic tests are not suitable for diagnosis of H pylori
infection.
They detect the presence of antibodies to H pylori
rather than the bacterium itself.
H pylori antibody levels may persist for years after
eradication of infection (ie, the H pylori bacterium).
47
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 47
Presence of antibody could indicate an active
infection or a resolved, cured infection.
Treating uninfected, cured people
o Is ineffective (ie, no treatment response)
o Contributes to the growing problem of antibiotic
resistance
o Adds needless cost.
Antibody tests are relatively insensitive (ie, more
false-negative test results).
Conversely, urea breath and stool antigen tests can
distinguish between active and resolved infection.
H pylori bacteria must be present to get a positive test
result:
Urea breath test indirectly detects urease produced
by H pylori bacteria.
Stool antigen test uses anti-H pylori antibody to
detect H pylori antigen.
Thus, both urea breath and stool antigen tests can be
used for diagnosis. Moreover, the higher sensitivity
and specificity of these tests lead to even better
performance when prevalence is low. This is
particularly important since the prevalence of H pylori
infection is declining in the U.S.
Urea Breath Test
5
H pylori bacteria produce the enzyme urease which
hydrolyzes urea to produce ammonia and carbon
dioxide (CO
2
). The CO
2
is then exhaled in the
breath and can be measured using an infrared
spectrophotometer. This chemical reaction is the
basis of the UBiT test:
48
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 48
1. An initial, baseline breath sample is tested to
determine the ratio of
13
CO
2
to
12
CO
2
. This ratio will
be low because almost all naturally occurring urea
in the body is
12
C-urea.
2. After the patient ingests
13
C-urea, a synthetic urea
comprised of stable, naturally occurring,
nonradioactive carbon-13, the ratio of
13
CO
2
to
12
CO
2
is determined again.
3. An increased ratio is consistent with the presence
of H pylori bacteria.
Patient Preparation and Sample Collection
The patient should have fasted for a minimum of 1
hour and should have abstained from antimicrobials,
proton pump inhibitors, and bismuth preparations in
the 2 weeks prior.
To collect the first sample, the patient inhales, holds
his/her breath for 4 to 5 seconds, and then exhales
into the bag provided in the sample collection kit.
The patient then drinks, without stopping, all the
13
C-urea solution provided in the kit (powder must
be reconstituted in water). After 15 minutes, during
which there is no eating, drinking, or smoking, the
patient exhales into a second bag using the
procedure detailed above. Both bags should be
capped tightly after collection and stored or
transported at room temperature. The sample should
be tested within 7 days of collection.
Stool Antigen Test
6,7
Stool antigen tests such as HpSA
'
(Meridian
Bioscience) use antibodies to H pylori to determine if
H pylori is present in the stool. Specimens can be
tested immediately, stored for 3 days in the
refrigerator, or frozen. Test results are available
49
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 49
within 5 minutes (point-of-care test) or 90 minutes
(laboratory test) of test initiation.
Table 1 summarizes the laboratory tests for H pylori.
Refer to Part 3, Test Application and Interpretation
50
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
Table 1. Tests Available for Detecting H pylori Infection
CLO, Campylobacter-like organism; PPI, proton pump inhibitor.
*Data represents approximate sensitivity and specificity; not based on side-by-side studies.
Results subject to sampling error.
Test Description Accuracy* Comments
Invasive Tests
Histologic Uses modified Giemsa Sensitivity: Also provides other
exam or silver stain to visualize 80% to 90%
2
histologic information,
H pylori bacteria Specificity: >95%
2
eg, presence/absence of
cancer, etc.
Rapid urease Colorimetric test that Sensitivity: False-negatives caused by
(CLO test) detects urease in biopsy 80% to 95%
2
antibiotics, PPI, or bismuth
specimen Specificity: compounds; suitable for test
95% to 100%
2
of cure
Culture Bacterial growth Sensitivity: Useful to determine
followed by 70% to 80%
8
alternative treatment for
identification and Specificity: 100%
8
nonresponders; expensive;
antibiotic susceptibility slow turnaround time
(if desired)
Non-invasive Tests
Antibody See text Sensitivity: 85%
4
Simple, low cost; no longer
detection Specificity: 79%
4
recommended due to lower
accuracy; not suited for proof
of cure or to differentiate
between active and past
infection
Antigen See text Sensitivity: 93%
4
Useful for diagnosis and
detection Specificity: 93%
4
proof of cure; false-negatives
caused by antibiotics, PPI, or
bismuth compounds
Urea See text Sensitivity: 95%
4
Useful for diagnosis and
breath test Specificity: 96%
4
proof of cure; false-negatives
caused by antibiotics, PPI, or
bismuth compounds
57152-01 6/27/07 8:23 AM Page 50
for additional information on the UBiT and stool
antigen tests.
TREATMENT
Treatment goals include relief of symptoms, healing
of the ulcer, and prevention of recurrence and
complications. Documented eradication of H pylori
infection is associated with substantially decreased
rates of recurrence and complications; thus,
physicians aim for an initial eradication rate of 85%
to 90%.
2
Triple therapy for 7 to 14 days duration is
the typical treatment regimen and may include 2
antibiotics and 1 acid suppressor. The 14-day regimen
is thought to be more efficacious than shorter
regimens.
1,2
Quadruple therapy may be used in
patients who do not respond to triple therapy. Such
patients may have an antibiotic resistant strain. If the
patient still fails to respond, culture and sensitivity
should be considered.
Table 2 lists medications used for H pylori treatment.
LABORATORY TESTING POST THERAPY
H pylori testing is performed 4 or more weeks after
the end of treatment. Such testing is appropriate for:
Patients with a history of ulcer complications
Patients with MALT lymphoma
Patients with early gastric cancer
Patients with recurrent symptoms post-treatment
The urea breath test and the stool antigen test are
the recommended noninvasive tests for confirming
eradication of H pylori. Serologic tests are not suitable
because they cannot distinguish between active and
51
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 51
resolved infection. When endoscopy is indicated, the
rapid urease test results can be used as proof of cure.
PROGNOSIS
Triple therapy is effective in more than 80% of
patients. Once H pylori infection is eradicated, most
patients become symptom-free, and only about 4% to
6% of patients will have recurrent PUD.
2
Therapy can
still be successful when treatment is delayed until
after development of complications (eg, in those who
were previously asymptomatic) as evidenced by
complete remission in >50% of patients with MALT
lymphoma.
2
52
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
Table 2. Medication Options Used for H Pylori Therapy
PPI, proton pump inhibitor.
*Acid suppressor drug class of choice.
Drug Class Action Examples
Antibiotics Eradicate Amoxicillin
H pylori infection Clarithromycin
Metronidazole
Tetracycline
Acid suppressors Relieve symptoms; Antacids (eg, Mylanta
'
, Maalox
'
, Tums
'
,
heal the ulcer Gaviscon
'
)
H2 receptor antagonist (eg, cimetidine,
ranitidine, famotidine, nizatidine)
PPI (eg, omeprazole, lansoprazole,
rabeprazole, pantoprazol, esomeprazole)*
Mucosal Prevent further Bismuth-containing compound
protective damage; heal the (eg, Pepto-Bismol
'
)
agents ulcer Prostaglandin analogue (eg, misoprostol)
Sucralfate
57152-01 6/27/07 8:23 AM Page 52
REFERENCES
1. Talley NJ, Vakil NB, Moayyedi P. American Gastroenterological
Association technical review on the evaluation of dyspepsia.
Gastroenterology. 2005;129:1756-1780.
2. Del Valle J. Peptic ulcer disease and related disorders. In: Kasper DL,
Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds.
Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-
Hill; 2005:1746-1762.
3. Talley NJ for the American Gastroenterological Association. American
Gastroenterological Association medical position statement: evaluation of
dyspepsia. Gastroenterology. 2005:129:1753-1755.
4. Vakil N, Fendrick AM. How to test for Helicobacter pylori in 2005 [review].
Cleve Clin J Med. 2005;72(suppl 2):S8-S13. Also available at:
http://www.ccjm.org/PDFFILES/Vakilsuppl5_05.pdf. Accessed January 5,
2007.
5. BreathTek UBiT [package insert]. Lafayette, Colorado: Meretek
Diagnostics Inc; 2005. Available at: http://meretek.com/downloads/
2215NOV05_cropped.pdf. Accessed January 8, 2007.
6. H pylori Stool Antigen Test Medical Information. Meridian Bioscience
Europe Web site. Available at: http://www.mdeur.com/hpsa-doctor.htm.
Accessed January 8, 2007.
7. Premier Platinum HpSA Plus. Meridian Bioscience Europe Web site.
Available at: http://www.mdeur.com/products/601348.htm. Accessed
January 8, 2007.
8. Meurer LN, Bower DJ. Management of Helicobacter pylori infection. Am
Fam Phys. 2002;65:1327-1336. Available at: http://www.aafp.org/afp/
20020401/1327.html. Accessed January 8, 2007.
53
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 53
SECTION 2. GASTRIC CANCER
OVERVIEW
Gastric cancers include gastric adenocarcinoma (85%
of all gastric cancers), primary gastric lymphoma
(12% to 14%), and nonlymphoid gastric sarcoma (ie,
gastrointestinal stromal tumors [GIST]; 1% to 3%).
1
ETIOLOGY AND RISK FACTORS
The following factors appear to be involved in
development or risk of gastric cancer:
H pylori infection
Familial mutation in the E-cadherin gene
Diet low in fresh fruits and vegetables
Gastric polyps
Ingestion of large amounts of nitrates, commonly
found in dried, smoked, and salted food
High salt intake
Tobacco smoking
Mntriers disease (extreme hypertrophy of gastric
rugal folds)
The following factors are associated with decreased
risk of gastric cancer:
Diet high in vitamin C
Diet high in whole grain foods
Diet high in carotenoids
Diet high in allium compounds
Diet high in green tea
INCIDENCE
The American Cancer Society estimated there would
be about 22,000 new cases of gastric cancer and
54
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 54
11,000 deaths in patients with gastric cancer during
2006.
2
It is the 13th most common cancer, ranking
well below prostate, breast, lung, and colon cancer.
Incidence in distal tumors is declining along with the
declining incidence of H pylori infection, whereas the
incidence of proximal tumors in the cardia is
increasing in the United States (Table 1).
SYMPTOMS
In the early, curable stage of gastric cancer, the
patient is usually asymptomatic. As the tumor
progresses, the patient may have the following:
Upper abdominal discomfort of varying intensity
A feeling of fullness after eating a small amount of
food
Occult blood in the stool
Iron deficiency anemia
Anorexia
Nausea, vomiting (especially in the middle of the
night)
Weight loss
DIAGNOSIS AND LABORATORY TESTING
Evaluation of a symptomatic patient may begin with a
double-contrast barium swallow radiograph, followed
by an esophagogastroduodenoscopy (EGD) if gastric
cancer is not ruled out.
3
Alternatively, evaluation can
55
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
Table 1. Gastric Cancer Site of Origin
1
Location % of All Gastric Cancer
Distal stomach 30
Mid-stomach 20
Proximal third of the stomach 37
Entire stomach 13
57152-01 6/27/07 8:23 AM Page 55
begin with the EGD. Multiple biopsies from
suspicious sites should be taken; diagnosis is based on
microscopic examination of tissue.
Following diagnosis, the patient should be evaluated
further to determine extent of the disease (eg,
presence or absence of lymph node, liver, or lung
metastasis). This workup may include the following:
Computed tomography (CT) scan
Positron emission tomography (PET) scan
Endoscopic ultrasonography (EUS)
Other tests may also be used to evaluate the patient:
Complete blood count (CBC)
Chemistry tests
Coagulation studies
Immunohistochemistry (IHC) tests
The c-kit protein (CD117) test, performed by IHC, is
used to differentiate GISTs from glomus tumors of
the stomach. GISTs are c-kit positive, while glomus
tumors are negative. Additionally, glomus tumors
tend to be positive for smooth muscle actin and
vimentin.
4
STAGING
The American Joint Committee on Cancer (AJCC)
has outlined terminology for staging gastric cancers
(Tables 2 and 3).
3
TREATMENT
Selection of treatment regimens depends on the
type of gastric cancer, extent of disease, and
general health of the patient. The National
56
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 56
57
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
Table 2. TNM Staging of Gastric Cancers
3
Tumor staging
T0 No evidence of primary tumor
Tis Carcinoma in situ
T1 Tumor invades lamina propria or submucosa
T2 Tumor invades muscularis propria or subserosa
T2a Tumor invades muscularis propria
T2b Tumor invades subserosa
T3 Tumor penetrates serosa (visceral peritoneum)
T4 Tumor invades adjacent structures
Nodal staging
N0 No evidence of metastasis to regional lymph nodes
N1 Metastasis in 1 to 6 regional lymph node(s)
N2 Metastasis in 7 to 15 regional lymph nodes
N3 Metastasis in >15 regional lymph nodes
Metastasis
M0 No evidence of distant metastasis
M1 Evidence of distant metastasis
Table 3. Definition of Gastric Cancer Stages
3
Stage Definition
0 Tis, N0, M0
Ia T1, N0, M0
Ib T1, T2, M0,
T2a or T2b, N0, M0
II T1, N2, M0
T2a or T2b, N1, M0
T3, N0, M0
IIIa T2a or T2b, N2, M0
T3, N1, M0
T4, N0, M0
IIIb T3, N2, M0
IV T4, N1, 2, or 3, M0
T1, 2, or 3, N3, M0
Any T, any N, M1
57152-01 6/27/07 8:23 AM Page 57
Comprehensive Cancer Network (NCCN)
recommendations for gastric adenocarcinoma are
outlined in Table 4. Components of supportive care
are outlined in Table 5.
PROGNOSIS
Prognosis varies based on the extent of disease
(stage) at time of diagnosis and treatment and the
type of gastric cancer. Patients with early stage cancer
are potentially curable (5-year survival up to 80%);
6
however, only about one-third of patients are
diagnosed when the cancer is in an early stage.
Prognosis for late stage is poor (<15% 5-year survival
rate).
6
Prognosis is much better for patients with primary
gastric lymphoma (eg, MALT lymphoma) than with
adenocarcinoma because antibiotic therapy, aimed at
eradication of H pylori infection, has a 75% response
rate.
1
Surgery, radiation, and chemotherapy may not
even be necessary for these patients. Patients with
localized, high-grade lymphomas who are treated
with surgery have a 40% to 60% 5-year survival rate.
1
58
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
Table 4. NCCN Recommendations for Treatment of Gastric Cancer
5
Patient Characteristics Therapy
Medically fit with stage Surgery: partial (for distal tumors) or
I to III gastric cancer complete (for proximal tumors) gastrectomy
Medically fit with unresectable tumor* Radiation or chemotherapy
Medically unfit with locoregional cancer
Radiotherapy or salvage chemotherapy
Distant metastasis (M1) Salvage therapy
Post surgery, select individuals Adjuvant radiation or chemotherapy
*Evidence of peritoneal or major blood vessel involvement or distant metastasis.
Stage I to III or M0.
Consisting of supportive care, chemotherapy, or clinical trial participation.
57152-01 6/27/07 8:23 AM Page 58
Patients with nonlymphoid gastric sarcoma (eg, GIST)
may also have a better prognosis than those with
adenocarcinoma. About 50% of patients with c-kit
positive GIST tumors respond to imatinib mesylate
(Gleevec
'
) therapy.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Cancer Society
Phone: 800-ACS-2345 (227-2345)
Internet: http://www.cancer.org
Cancer Care, Inc.
Phone: 800-813-HOPE (813-4673) or 212-221-3300
Email: info@cancercare.org
Internet: http://www.cancercare.org
59
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
Table 5. Components of Supportive Care
5
Stent placement, laser surgery, photodynamic therapy,
radiotherapy, surgery, or combination of these*
Surgery, endoscopic therapy, radiotherapy
Nutritional support
PEG tube
Counseling
Pain management
Radiotherapy
Medications
PEG, percutaneous endoscopic gastrostomy.
*For patients with luminal obstruction.
For patients with significant bleeding.
57152-01 6/27/07 8:23 AM Page 59
60
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
Cancer Hope Network
Phone: 877-HOPENET (467-3638) or
908-879-4039 (New Jersey residents)
Email: info@cancerhopenetwork.org
Internet: www.cancerhopenetwork.org
National Cancer Institute
Phone: 800-422-6237 or 301-496-6631
Internet: http://www.cancer.gov
http://www.nci.nih.gov
Cancer Information Service
Building 31, Room 10A16
31 Center Drive, MSC 2580
Bethesda, MD 208922580
NCI's Facing Forward Series
Phone: 888-4-CANCER (422-6237)
Internet: http://www.nci.nih.gov/cancerinfo/
life-after-treatment
National Coalition for Cancer Survivorship
Phone: 877-622-7937 or 301-650-9127
Email: info@canceradvocacy.org
Internet: http://www.canceradvocacy.org
The Cancer Information Network
http://www.cancerlinksusa.com/stomach/index.asp
The Wellness Community Executive Office
Phone: 888-793-WELL (793-9355) or 202-659-9709
Email: help@thewellnesscommunity.org
Internet: http://www.thewellnesscommunity.org
57152-01 6/27/07 8:23 AM Page 60
61
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
REFERENCES CITED
1. Mayer RJ. Gastrointestinal tract cancer. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:523-533.
2. American Cancer Society. Cancer facts and figures 2006 graphs and
figures. Available at: http://www.cancer.org/docroot/MED/content/
MED 1 1 Most-Requested Graphs and Figures 2006.asp. Accessed January
12, 2007.
3. Layke JC, Lopez PP. Gastric cancer: diagnosis and treatment options. Am
Fam Physician. 2004;69:1133-1140.
4. Hwang JH, Rulyak SD, Kimmey MB. American Gastroenterological
Association Institute Technical Review on the management of gastric
subepithelial masses. Gastroenterology. 2006;130:2217-2228.
5. Ajani J, Bekaii-Saab T, DAmico TA, et al. National Comprehensive Cancer
Network clinical practice guidelines in oncology v.1.2006: gastric cancer.
Available at: http://www.nccn.org/professionals/physician gls/PDF/
gastric.pdf. Accessed January 12, 2007.
6. Stomach cancer. In: Beers MH, Porter RS, Jones TV, Kaplin JL, Berkwits
M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck
Publishing Group; 2006. Available at: http://www.merck.com/mmpe/
sec02/ch021/ch021d.html?qt=gastric%20cancer&alt=sh. Accessed
January 12, 2007.
ADDITIONAL REFERENCE
1. Gastric Cancer (PDQ
'
). National Cancer Institute Web site. Available at:
http://www.cancer.gov/cancertopics/pdq/prevention/gastric/
healthprofessional. Accessed January 12, 2007.
57152-01 6/27/07 8:23 AM Page 61
62
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
3
:
S
t
o
m
a
c
h
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 62
63
Gastroenterology
Reference Guide
CHAPTER 4. GASTROENTERITIS
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
INTRODUCTION
Gastroenteritis is an acute inflammation of the
stomach and/or intestinal lining. It can be caused by
bacteria, viruses, parasites, and irritating substances
in food or drinks (eg, capsaicin, found in hot
peppers, or ciguatera found in barracuda, snapper,
jack, and grouper fish). Common symptoms include
loss of appetite, nausea, diarrhea, abdominal pain,
and weakness. Since these symptoms are nonspecific,
gastroenteritis differential diagnosis includes
consideration of drug toxicity and inflammatory
bowel disease as well as the causes just listed.
Gastroenteritis is a very common disease worldwide,
second only to acute respiratory illness.
1
Morbidity
ranges from mild to severe: mild cases may require
no medication, whereas severe cases may be life-
threatening (eg, due to dehydration). Some
infections causing gastroenteritis may become
chronic (>2 weeks duration) and may lead to
malnutrition. Many of these infections are
transmitted via a fecal/oral route (ie, contaminated
water and food, food poisoning). This chapter will
focus on bacterial, viral, and parasitic gastroenteritis.
REFERENCE
1. Butterton JR, Calderwood SB. Acute infectious diarrheal diseases and
bacterial food poisoning. In: Kasper DL, Braunwald E, Fauci AS, Hauser
SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine.
16th ed. New York, NY: McGraw-Hill; 2005:754-759.
57152-01 6/27/07 8:23 AM Page 63
64
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
SECTION 1. BACTERIAL GASTROENTERITIS
OVERVIEW
Bacterial gastroenteritis is caused by food poisoning
(ie, ingestion of contaminated food or water). When
such poisoning occurs in people who have recently
or are traveling in another country, it is termed
Table 1. Bacterial Causes of Gastroenteritis
1
Bacteria Incubation Disease Toxin Transmission Symptoms
Period Duration Producing
Aeromonas Swimming, Sporadic, nonbloody
drinking water diarrhea
Bacillus 1-6 h <12 h Yes, Fried rice, pork Nausea, vomiting,
cereus emetic abdominal cramping
Bacillus 8-16 h Yes, Beef, pork, Abdominal cramping,
cereus entero chicken, watery diarrhea
vanilla sauce
Campylobacter 16-72 h 1 wk Uncooked Fever, headache, myalgia,
jejuni poultry, abdominal cramps, watery
unpasteurized or bloody diarrhea that
milk, infected may include WBCs
pet (eg, reptiles,
dogs, cats)
Clostridium Few d Yes, Fecal-oral, Ranges from none to life-
difficile to 2 mo entero or person-to-person, threatening colitis
cytopathic during or following
antibiotic therapy
Clostridium 8-16 h 24 h Yes, alpha, Meat, poultry, Abdominal cramps,
perfringens beta, or gravy, hash, watery diarrhea
entero stew
Escherichia coli 72-120 h 1 wk Yes Undercooked Bloody diarrhea,
(E coli O157:H7) (Shiga ground beef, abdominal cramps,
(enterohemorrhagic) toxin) unpasteurized milk hemolytic uremic
and juice, water, syndrome (5%-10%
person-to-person of patients)
Escherichia coli 16-72 h ? Developing Watery diarrhea; blood,
(enteroinvasive) countries mucus, and/or WBCs in
stool; fever; cramps
Escherichia coli No Nursery outbreak Watery diarrhea, fever,
(enteropathogenic) vomiting, mucus in stool
57152-01 6/27/07 8:23 AM Page 64
travelers diarrhea. There are many different species
of bacteria that can be involved in bacterial
gastroenteritis (Table 1).
RISK FACTORS
Travel to endemic regions, especially those with
poor sanitation or hygiene
65
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
Table 1. (Continued)
Bacteria Incubation Disease Toxin Transmission Symptoms
Period Duration Producing
Escherichia coli 16-48 h Yes, Contaminated meat, Watery diarrhea,
(enterotoxigenic) entero vegetables, fruit; cramps, nausea
person-to-person
Listeria Uncooked chicken, Fever, diarrhea*
beef, vegetables,
milk, cheese
Salmonella 16-72 h Few d Yes, Uncooked fruits, Nausea, vomiting,
to 1 wk endotoxin vegetables, oysters, diarrhea, fever, malaise,
shellfish, eggs, muscle aches,
poultry, pork, abdominal pain
dairy products,
water, pets (turtles)
Shigella 16-72 h 1 wk Yes Primarily Fever, abdominal
(Shiga person-to-person; cramping, watery
toxin) food (egg salad, diarrhea followed by
vegetables) bloody diarrhea
less commonly
Staphylococcus 2 to 6 h Yes, Custard-filled Nausea, vomiting,
aureus enterotoxin baked goods, abdominal cramps,
canned food, watery diarrhea
processed meat,
potato salad,
ice cream
Vibrio cholerae 16-48 h Yes, Uncooked or Vomiting, watery
entero undercooked food diarrhea with mucus
(eg, shellfish), water
Vibrio 16-72 h Undercooked Diarrhea
parahaemolyticus seafood
Yersinia 16-72 h Pork chitterlings, Fever, abdominal pain,
enterocolitica tofu, milk, water diarrhea
h, hours; wk, weeks; d, days; mo, months; WBC, white blood cell.
*More commonly a cause of meningitis.
57152-01 6/27/07 8:23 AM Page 65
People with lowered immunity
Children in day care centers
Those who are in the hospital or a long-term care
facility (eg, the elderly)
INCIDENCE
Although relatively common, bacterial gastroenteritis
occurs less often than viral gastroenteritis. It occurs
more often in developing countries or regions with
poor sanitation and is more common in the summer
or rainy months. The overall incidence is difficult to
determine because many self-limiting cases are not
reported.
SYMPTOMS
See Table 1 for typical symptoms associated with each
bacterium. These symptoms range from mild to severe.
Severe symptoms such as profuse watery diarrhea (and
the resultant dehydration) can be life threatening.
Complications can occur. For example, enterohem-
orrhagic E coli can lead to hemolytic uremic
syndrome in 5% to 10% of patients.
1
Arthritis may
develop following Campylobacter, Salmonella, Shigella, or
Yersinia infection.
DIAGNOSIS
Diagnostic evaluation begins with a medical history
and physical examination. The patient should be
evaluated for:
Symptom onset, intensity, frequency, duration
Stool characteristics
o Presence or absence of blood
66
Gastroenterology
Reference Guide
Hemolytic Uremic
Syndrome (HUS)
Overview
HUS primarily affects young
children between the ages
of 1 and 10 years. It is a
vascular disorder that may
lead to acute renal failure. It
can occur following a minor
febrile or viral illness (eg,
enterohemorrhagic E coli).
Although there is no
effective treatment, only
10% to 50% of patients
develop chronic renal
disease and <10% of
children die.
2
Symptoms
Fever
Thrombocytopenia
Microangiopathic
hemolytic anemia
Hypertension
Varying degrees of
acute renal failure C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 66
o Presence or absence of leukocytes
o Consistency (bulky vs watery)
Frequency of bowel movements
Quantity of stool
Recent antibiotic use (may raise suspicion of
C difficile infection)
Additionally, the following epidemiologic risk factors
can be considered:
Potential ingestion of contaminated food or water
(especially during a known outbreak)
Travel history
Contact with similarly ill people
Contact with animals and reptiles
Daycare center attendance or employment
Occupation as a food handler or caregiver
Underlying medical conditions likely to predispose
patient to infectious diarrhea (eg, AIDS)
The differential diagnosis should also include
consideration of viral or parasitic gastroenteritis, drug
toxicity, irritable bowel syndrome, inflammatory
bowel disease, appendicitis, cholecystitis, and
ulcerative colitis. Celiac disease, lactose intolerance,
and other forms of malabsorption should be
considered in patients with chronic diarrhea. Table 2
illustrates how specific symptoms can be used to
suggest a possible diagnosis.
A specific diagnosis (ie, identification of the causative
bacterium) is not always necessary to determine the
course of treatment.
LABORATORY TESTING
Laboratory tests may be helpful in selected cases.
These tests include:
67
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 67
Tests for serum electrolyte, blood urea nitrogen
(BUN), and creatinine levels to assess the severity
of disease (ie, dehydration and acid-base balance)
Gram stain
Fecal lactoferrin test to detect the presence of fecal
leukocytes which indicate an inflammatory process;
elevated lactoferrin levels may be associated with
inflammatory bowel disease, C difficile, C jejuni,
enterohemorrhagic or enteroinvasive E coli,
Salmonella, Shigella, V parahaemolyticus, or Y enterocolitica,
and Entamoeba histolytica
Bacterial culture of stool specimens
Shiga toxin EIA to help diagnose Shigella or
enterohemorrhagic E coli (O157:H7) infection
Y enterocolitica antibody
Analysis of suspected food to detect bacterial
presence and/or toxin
68
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
Table 2. Symptom Driven Differential Diagnosis
3
Symptom Possible Cause
Diarrhea of >2 weeks duration Causes of acute diarrhea unlikely
Fever Invasive disease, malaria
Fecal leukocytes, blood, mucus Inflammatory disorder (invasion or cytoxin)
rather than noninflammatory disorder
(enterotoxin)
Bloody stools without leukocytes Enterohemorrhagic E coli
Bulky white stools Small intestine disorder causing malabsorption
Profuse watery diarrhea with Cholera or other toxigenic process
small pieces of mucus
Severe abdominal pain Campylobacter, Shigella, cholera, necrotizing
toxins
Appendicitis-like syndrome Yersinia enterocolitica
Tenesmus* Shigella
Vomiting Toxin-producing bacteria, malaria, intestinal
obstruction
Diarrhea coincident with or C difficile, Salmonella
following antibiotic therapy
*Little stool produced in spite of strong urge to defecate and painful rectal spasms.
57152-01 6/27/07 8:23 AM Page 68
TREATMENT
Most bacterial gastroenteritis cases are mild and self-
limiting; thus, the focus is on bed rest and hydration
rather than on antibiotic therapy. Oral rehydration
solutions (ORS) containing electrolytes and glucose,
rice, or cereal may be prescribed. ORS are often sold
over-the-counter and include, among others, Lytren
'
,
Rehydralyte
'
, and Pedialyte
'
. Sports drinks, soda,
and juice are not recommended because they may
result in additional fluid loss owing to lack of optimal
balance between carbohydrate and sodium
concentrations. If dehydration is severe, intravenous
fluids such as Ringers lactate may be prescribed.
Bismuth subsalicylate, antiperistaltic agents, and
antimicrobial agents may shorten the duration of
symptoms in patients with enterotoxigenic E coli
infection. However, antibiotics that increase the
production of Shiga toxins are contraindicated for
treatment of enterohemorrhagic E coli infection.
Antibiotics are sometimes recommended for patients
with Shigella, V cholerae, or C difficile infection.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Dietetic Association
Phone: 800-366-1655 or 800-877-1600
Internet: http://www.eatright.org
U.S. Department of Agriculture
Meat and Poultry Hotline
Phone: 888-MPHotline (674-6854)
Internet: http://www.usda.gov
69
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 69
US Department of Health and Human Services
Phone: 877-696-6775 or 202-619-0257
Internet: http://www.os.dhhs.gov
US Environmental Protection Agency (EPA)
Phone: 202-272-0167
Internet: http://www.epa.gov
US Food and Drug Administration FDA (HFE-88)
Phone: 888-INFO-FDA (463-6332)
Internet: http://www.fda.gov
Center for Food Safety & Applied Nutrition
Phone: 888-SAFEFOOD (723-3366)
Internet: http://vm.cfsan.fda.gov/list.html
Centers for Disease Control and Prevention (CDC)
Phone: 800-311-3435 or 404-639-3534
Internet: http://www.cdc.gov
Gateway to Government Food Safety Information
Internet: www.FoodSafety.gov
REFERENCES
1. Isada CM, Kasten BL, Goldman MP, Gray LD, Aberg JA. Infectious Diseases
Handbook. 4th ed. Hudson (Cleveland), OH: Lexi-Comp, Inc; 2001.
2. Handin RI. Disorders of the platelet and vessel wall. In: Kasper DL,
Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds.
Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-
Hill; 2005:673-680.
3. Butterton JR, Calderwood SB. Acute infectious diarrheal diseases and
bacterial food poisoning. In: Kasper DL, Braunwald E, Fauci AS, Hauser
SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine.
16th ed. New York, NY: McGraw-Hill; 2005:754-759.
70
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 70
SECTION 2. VIRAL GASTROENTERITIS
OVERVIEW
Viral gastroenteritis, commonly misnamed as
stomach flu, is caused by rotavirus (group A);
caliciviruses, which include norovirus (formerly
Norwalk virus) and sapovirus; astrovirus; and
adenovirus (types 40 and 41). Table 1 details some
characteristics of these viruses. Mortality is a rare
sequelae among healthy young adults, but elderly
persons, particularly those in fragile health, are at
risk of severe dehydration and death.
INCIDENCE
Viral gastroenteritis is a common disease that
occurs more often in winter than other times of the
year in the United States. Unlike bacterial
gastroenteritis, the incidence of viral gastroenteritis
is similar in industrial and developing countries.
Viral gastroenteritis is much more common than
bacterial. Most adults have antibodies to the
Norwalk and related human caliciviruses, and
71
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
Table 1. Characteristics of Gastroenteritis-causing Viruses
1-5
Virus Incubation Disease Primary Population Relative
Period Duration Affected Severity
Rotavirus, Infants: <2 d 3-9 d Children aged 6 mo to 2 y +++
group A Adults: 2-4 d
Norovirus 24-48 h 24-60 h All ages ++
Sapovirus Infants, young children +
Astrovirus 3-4 d 2-4 d Children <5 y +
Adenovirus, types 3-10 d Infants, children <4 y +/++
40 and 41
d, days; mo, months; y, year; h, hours.
57152-01 6/27/07 8:23 AM Page 71
nearly all children are infected with rotavirus by
age 5 years.
TRANSMISSION
Transmission of these viruses is predominantly via a
fecal-oral route. Ingestion of contaminated food or
water, person-to-person contact, vomit, aerosol,
respiratory secretions, and contaminated surfaces or
objects may be involved.
SYMPTOMS
Although patients are sometimes asymptomatic,
nonbloody, noninflammatory, watery diarrhea is
more likely to be manifested. The patient may also
experience nausea, vomiting, abdominal pain, fever,
chills, headache, and myalgia. Severe illness may be
complicated by life-threatening dehydration.
Rotavirus typically causes the most severe illness, but
it may be relatively mild in the neonatal period owing
to maternal antibodies. Severity decreases with each
reinfection. Severity of illness caused by norovirus is
typically less than that caused by rotavirus but greater
than that caused by sapovirus and astrovirus. Severity
of adenovirus infection can be the same as sapovirus
and astrovirus or similar to that caused by norovirus.
DIAGNOSIS
The diagnostic evaluation is essentially the same as
that for bacterial gastroenteritis. If antibiotic therapy
is being considered, laboratory testing should be
used to differentiate viral from bacterial disease
because differentiation based on clinical and
epidemiologic characteristics is difficult. Parasitic
72
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 72
gastroenteritis, drug toxicity, and inflammatory bowel
disease should also be considered.
A specific diagnosis (ie, identification of the causative
organism) is not always necessary to determine the
course of treatment.
LABORATORY TESTING
The following tests are available to confirm a viral
etiology:
Rotavirus antigen detection using enzyme
immunoassay (EIA)
Norovirus RNA detection using reverse-
transcriptase polymerase chain reaction (RT-PCR)
Adenovirus antigen detection using EIA
Adenovirus culture
Stool collection during the 1st week of symptoms
provides the best recovery of rotavirus; however,
viral shedding may continue longer in
immunocompromised patients. Stool specimens for
norovirus testing should be collected within 48 to
72 hours of onset of symptoms for best results;
however, viral recovery can occur up to 2 weeks
after resolution of symptoms.
TREATMENT
Specific antiviral therapy is not available and
generally not required since viral gastroenteritis is
self-limiting. Supportive therapy to prevent or treat
dehydration may be needed, however. For details, see
the section describing treatment of bacterial
gastroenteritis. Antibiotic therapy is contraindicated.
73
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 73
PROGNOSIS
Most people recover from viral gastroenteritis
without any complications. However, viral
gastroenteritis can be serious if severe dehydration
develops.
RESOURCES
Centers for Disease Control and Prevention
Phone: 800-311-3435 or 404-639-3534
Internet: http://www.cdc.gov
REFERENCES
1. Isada CM, Kasten BL, Goldman MP, Gray LD, Aberg JA. Infectious Diseases
Handbook. 4th ed. Hudson (Cleveland), OH: Lexi-Comp, Inc; 2001.
2. Centers for Disease Control. CDC technical fact sheet about noroviruses.
Available at: http://www.cdc.gov/ncidod/dvrd/revb/gastro/noro-
factsheet.pdf. Accessed January 31, 2007.
3. Public Health Agency of Canada. Adenovirus types 40 and 41 material
safety data sheet. Available at: http://www.phac-aspc.gc.ca/msds-ftss/
msds4e.html. Accessed January 31, 2007.
4. Parashar UD, Glass RI. Viral gastroenteritis. In: Kasper DL, Braunwald E,
Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1140-1143.
5. Matsui SM, Greenberg HB. Astroviruses. In: Knipe DM, Howley PM, eds.
Fields Virology. 4th ed. Philadelphia, PA: Lippincott Williams and Wilkins;
2001:875-893.
74
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 74
SECTION 3. PARASITIC GASTROENTERITIS
OVERVIEW
Parasitic gastroenteritis is caused by infection with
Giardia lamblia, Cryptosporidium parvum, Cyclospora
cayetanensis, Isospora belli, Entamoeba histolytica
(amebiasis), and microsporidia (eg, Enterocytozoon
bieneusi, Encephalitozoon intestinalis). Characteristics of
these protozoan parasites are listed in Table 1.
75
Gastroenterology
Reference Guide
Parasite Infective Incubation Disease Transmission Symptoms
Form Period Duration
Cryptosporidium Oocyst 2-14 d 2 wk Fecal-oral, person-to- Watery diarrhea, malaise,
parvum person; water; food; abdominal cramping or pain,
animal-human fever
Cyclospora Oocyst 1 wk 6 wk Fecal-oral [not Intermittent watery diarrhea,
cayetanensis person-to-person]; abdominal cramping,
muscle
water, food aches, anorexia,
fever, nausea, vomiting
Entamoeba Cyst 7-10 d 1-4 wk Contaminated food Asymptomatic (90%);
histolytica or water; fecal-oral abdominal pain; bloody
diarrhea
Giardia Cyst 1-14 d 1-3 wk Contaminated water Asymptomatic (50%);
lamblia or food; fecal-oral; watery diarrhea,
oral-anal sexual abdominal pain,
contact bloating; chronic
malabsorption
Isospora belli Oocyst weeks Contaminated Watery diarrhea, abdominal
food or water cramps, anorexia, weight
loss, occasional fever
Enterocytozoon Spore Chronic Birds Gradual onset of diarrhea,
bieneusi* weight loss, nausea, abdominal
cramps, anorexia
Encephalitozoon Spore Chronic Domestic and Gradual onset of diarrhea,
intestinalis* wild animals weight loss, nausea, abdominal
cramps, anorexia
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
*Opportunistic infections occurring predominantly in immunocompromised patients.
Table 1. Parasitic Causes of Gastroenteritis
1,2
57152-01 6/27/07 8:23 AM Page 75
RISK FACTORS
Travelers to endemic areas (Table 2) and
campers are at risk of parasitic gastroenteritis.
Other risk factors include recent immigration,
institutionalization, and homosexuality. People
with IgA deficiency or diverticulosis are at
increased risk of severe or relapsing giardiasis.
DIAGNOSIS
Diagnosis is frequently based on an ova and parasites
(O&P) test, which includes concentration of a fecal
specimen (via centrifugation) followed by
examination of the concentrate under a microscope.
A trichrome, acid-fast, or other stain may be used to
help visualize and identify the parasite. Other tests
may be appropriate depending on the suspected
organism (Table 3).
Identification of Cyclospora cayetanensis, though
infrequent, is important since treatment is available.
The oocytes are twice as large as Cryptosporidium
oocytes and appear deep red or pink when using an
76
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
Table 2. Geographic Distribution of Protozoan Parasites
1
Parasite Distribution
Cryptosporidium parvum Worldwide
Cyclospora cayetanensis Worldwide, especially in Nepal, Peru, Mexico,
Morocco, India, Pakistan
Entamoeba histolytica Mexico, India, West and South Africa, portions
of Central and South America
Giardia lamblia Worldwide, especially in wilderness and
mountainous areas
Isospora belli Tropical and subtropical climates
Enterocytozoon bieneusi Worldwide
Encephalitozoon intestinalis Worldwide
57152-01 6/27/07 8:23 AM Page 76
acid-fast stain. Nonrefractile hyaline cysts can be seen
using phase microscopy, while neon blue
fluorescence can be seen using ultraviolet
microscopy. Stool specimens, duodenal aspirate, or
small bowel biopsy specimens can be submitted for
testing.
Sensitivity of O&P for diagnosis of Entamoeba
histolytica is 80% to 90% when 3 stool specimens are
examined, each within 20 minutes of collection.
1
Detection of E histolytica antigen, using enzyme
immunoassay (EIA), is 60% to 90% 7 days after
exposure.
1
Sigmoidoscopy or colonoscopy can be
used to differentiate parasitic gastroenteritis from
inflammatory bowel disease in patients with chronic
colitis.
77
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
Table 3. Diagnosis of Parasitic Gastroenteritis
1
DFA, direct immunofluorescence assay; EIA, enzyme immunoassay; O&P, ova and parasites test; UV,
ultraviolet; PCR, polymerase chain reaction.
Parasite Laboratory Tests
Cryptosporidium parvum Acid-fast stain on 2 or more separate samples;
DFA; EIA
Cyclospora cayetanensis O&P, modified acid-fast stain, phase microscopy,
UV microscopy
Entamoeba histolytica O&P, antigen detection, sigmoidoscopy or
colonoscopy
Giardia lamblia O&P with or without staining, duodenal biopsy
aspiration, string test
Isospora belli O&P, acid-fast stain
Enterocytozoon bieneusi Microscopic examination of trichrome-stained
stool smear; other stains may also be used; PCR
(select research laboratories)
Encephalitozoon intestinalis Microscopic examination of trichrome-stained
stool smear; other stains may also be used; PCR
(select research laboratories)
57152-01 6/27/07 8:23 AM Page 77
TREATMENT
Therapeutic regimens employed are listed in Table 4.
Supportive care to prevent or treat dehydration may
be needed. For details, see the section describing
treatment of bacterial gastroenteritis.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
Centers for Disease Control and Prevention /
Division of Parasitic Diseases (CDC /DPD)
Phone: 800-311-3435 or 404-639-3534
Internet: http://www.cdc.gov/ncidod/dpd/
78
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
Table 4. Therapeutic Regimens for Parasitic Gastroenteritis
1,2
Parasite Treatment
Cryptosporidium parvum Supportive care; clarithromycin and nitazoxanide may
be useful, but more studies needed
Cyclospora cayetanensis Drug of choice is co-trimoxazole, a combination of
trimethoprim and sulfamethoxazole (orally for 7 days)
Entamoeba histolytica Metronidazole (3 times/day for 10 days) followed by
diloxanide furoate; alternatively, treat with metronidazole
followed by paromomycin or iodoquinol
Giardia lamblia Many self-resolving, but treatment with metronidazole is
recommended; other options include quinacrine,
tinidazole, and nitazoxanide
Isospora belli Co-trimoxazole (4 times/day); alternatively treat with
sulfadoxine and pyrimethamine or with ciprofloxacin
Enterocytozoon bieneusi Supportive care, albendazole
Encephalitozoon intestinalis Supportive care, albendazole
57152-01 6/27/07 8:23 AM Page 78
REFERENCES
1. Isada CM, Kasten BL, Goldman MP, Gray LD, Aberg JA. Infectious Diseases
Handbook. 4th ed. Hudson (Cleveland), OH: Lexi-Comp, Inc; 2001.
2. DPDx Laboratory identification of parasites of public health concern.
[Centers for Disease Control and Prevention, National Center for
Infectious Diseases, Division of Parasitic Diseases Web site]. Available at:
http://www.dpd.cdc.gov/dpdx/Default.htm. Accessed February 12, 2007.
79
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 79
80
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
4
:
G
a
s
t
r
o
e
n
t
e
r
i
t
i
s
57152-01 6/27/07 8:23 AM Page 80
SECTION 1. DIVERTICULAR DISEASE
OVERVIEW
Diverticular disease includes diverticulosis and
diverticulitis. Diverticulosis is characterized by
diverticula affecting any part of the gastrointestinal
(GI) tract; the sigmoid colon is most commonly
affected, accounting for 95% of cases.
1
False, or
pseudodiverticulum, is the most common type of
diverticulum in the colon; this sac-like projection or
hernia extends through the muscularis propria, but
not all layers of the intestinal wall. True diverticula
contain all layers of the intestinal wall.
Diverticulitis is the most common complication of
diverticulosis. It is characterized by inflammation of
the diverticulum, which is caused by trapped fecal
material. Infection, bleeding, and perforation may
follow.
ETIOLOGY
Diverticula are most likely caused by an increase in
pressure (higher amplitude contraction) within the
GI tract in combination with weak sections of the
wall. Since the sigmoid colon is the narrowest part of
the colon and has the highest pressure between
segments, it is the most likely location for diverticula
formation. A low-fiber diet (low-bulk stool) is thought
to contribute to the increased pressure and is
considered the probable cause of diverticular disease.
Diverticula of the right side of the colon are thought
to be congenital.
1
81
Gastroenterology
Reference Guide
CHAPTER 5. INFLAMMATORY INTESTINAL
DISORDERS
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 81
PREVALENCE
Diverticular disease affects about 50% of people over
the age of 60 in western populations.
2
It is much less
common in underdeveloped countries in which high-
fiber diets are common. It is relatively rare in people
younger than 40 years of age, but prevalence
increases with increasing age thereafter. Although
men usually present at a younger age than women
do, both genders are equally affected.
SYMPTOMS
About 20% of people with diverticulosis develop
symptoms.
2
Primary symptoms include painless rectal
hemorrhage or those associated with diverticulitis.
Patients with diverticulitis may present with:
Fever
Abdominal pain
Nausea
Vomiting
Abdominal distention
Diarrhea or constipation
Anorexia
Diverticulitis complications include abscesses,
peritonitis, pneumaturia, or recurrent urinary tract
infections in patients with a fistula between the
bladder and bowel. Fistulas may also occur in other
adjacent structures such as the small bowel, vagina,
and uterus. Fistulas are uncommon, however,
occurring mostly in patients with recurrent attacks of
diverticulitis.
82
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 82
DIAGNOSIS AND LABORATORY TESTING
Asymptomatic diverticulosis is detected during
procedures (eg, imaging studies, endoscopy, or
colonoscopy) that are performed to evaluate another
ailment or as part of colon cancer screening.
In patients presenting with rectal bleeding,
colonoscopy or mesenteric angiography is used to
localize the site of bleeding. When diverticulitis is
suspected, computed tomography (CT) scan of the
abdomen and pelvis is used. The differential
diagnosis includes irritable bowel sydrome,
appendicitis, and colon or ovarian cancer. To assist in
diagnosis, other procedures such as ultrasonography,
barium enema, and laparoscopy may be employed.
Laboratory tests may show leukocytosis, increased
erythrocyte sedimentation rate (ESR), or increased
C-reactive protein (CRP) levels.
TREATMENT
The asymptomatic patient, diagnosed incidentally, is
treated with a high-fiber (15 to 30 gm/d) diet. Fiber
supplements such as Metamucil
'
, Citrucel
'
, and
Fibercon
'
may be used.
Diverticular bleeding stops spontaneously in the
majority of patients. However, heat or laser
coagulation of vessels can be employed during
colonoscopy for patients with mild to moderate
bleeding. In patients with more extensive bleeding,
coil embolization techniques can be used during
angiography with an 80% success rate.
2
Alternatively,
vasopressin infusion can be used to stop bleeding.
Both procedures are associated with side effects
and/or recurrence.
83
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 83
Diverticulitis should be treated initially with a 7- to
10-day course of antibiotics and bowel rest (nothing
by mouth or a clear liquid diet) until abdominal pain
ceases. This is successful in nearly 75% of cases.
2
Antibiotic choices include trimethoprim/
sulfamethoxazole, ciprofloxacin, metronidazole,
ampicillin, amoxicillin, ceftazidime, and piperacillin.
Surgical resection (segmental or total abdominal
colectomy) is sometimes required; for example,
surgery is offered to patients who have had 2
episodes of diverticular disease and to those who do
not respond rapidly to other therapy. Surgery is also
required for patients with complicated disease (eg,
abscesses, fistulas, obstructed bowel). Segmental
resection is performed more often than total
abdominal colectomy.
PROGNOSIS
Diverticular disease is successfully treated in most
cases. A small percentage will have recurrent disease.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
Digestive Disease National Coalition
507 Capitol Court NE, Suite 200
Washington, DC 20002
Phone: 202-544-7497
National Digestive Diseases Information
Clearinghouse (NDDIC)
Phone: 800-891-5389
Internet: http://digestive.niddk.nih.gov/index.htm
84
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 84
REFERENCES CITED
1. Joffe S, Kachulis A, Horowitz M. Colon, diverticulitis. [EMedicine Web
site]. Available at: http://www.emedicine.com/radio/topic183.htm.
Accessed February 13, 2007.
2. Gearhart SL, Bulkley G. Common diseases of the colon and anorectum
and mesenteric vascular insufficiency. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1795-1803.
ADDITIONAL REFERENCE
Gastrointestinal disorders: diverticular disease. In: Beers MH, Porter RS,
Jones TV, Kaplan JL, Berkwits M, eds. The Merck Manual of Diagnosis and
Therapy. 18th ed. Merck Publishing Group; 2006. Available at:
http://www.merck.com/mmpe/sec02/ch019/ch019a.html. Accessed
February 13, 2007.
85
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 85
SECTION 2. INFLAMMATORY BOWEL
DISEASE (ULCERATIVE COLITIS AND
CROHN'S DISEASE)
OVERVIEW
Inflammatory bowel disease (IBD) is a chronic
inflammation of the intestine characterized by
diarrhea and abdominal pain. There are 2 main
types: ulcerative colitis (UC) and Crohns disease. UC
usually involves the rectum and may extend to part
or all of the large intestine (colon) in a continuous
and contiguous pattern. Damage to the lining of the
intestine is usually limited to the mucosa. Crohns
disease can involve any part of the gastrointestinal
(GI) tract, from the mouth to the anus. Damage
usually affects all layers of the intestine. Moreover,
unlike UC, areas of healthy bowel alternating with
regions of diseased bowel characterize Crohns
disease.
ETIOLOGY AND RISK FACTORS
IBD is an idiopathic disorder in which inflammation
is thought to develop subsequent to interaction
between the patients genetics, physiology, and
environment. In genetically susceptible individuals,
endogenous intestinal microorganisms (normal
flora) may somehow trigger an autoimmune
(inappropriate) response. This response is
exacerbated by environmental factors.
Epidemiology studies show about 10% of IBD
patients have an affected first-degree relative.
1
Prevalence along ethnic lines also indicates a genetic
link: prevalence is highest in those of Jewish ethnicity
and decreases progressively in Caucasian, African-
American, Hispanic, and Asian ethnicities.
1
IBD is
86
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 86
also associated with some inherited disorders (eg,
Turners syndrome, Hermansky-Pudlak syndrome).
1
Gene mapping has identified a genetic link between
3 mutations in the NOD2 gene located on
chromosome 16 and Crohns disease susceptibility.
2
This gene is also called CARD15. Up to 50% of
western Caucasian patients with Crohns disease have
a NOD2/CARD15 mutation.
2
These 3 mutations have
not been found in Chinese or Japanese people with
Crohns disease, though. The 3 NOD2/CARD15
mutations do not appear in patients with other
inflammatory disorders, including UC.
To date, a causative infectious agent has not been
identified. Lifestyle risk factors include cigarette
smoking and oral contraceptive use. Cigarette
smokers are twice as likely to have Crohns disease
than nonsmokers; conversely, smokers are less likely
to have UC than nonsmokers.
1,3
Women who use oral
contraceptives are at increased risk (RR 1.9) of
Crohns disease, but not UC.
1
INCIDENCE
UC incidence in the United States is about
11:100,000, and Crohns disease incidence is about
7:100,000.
1
Additional cases of IBD also occur since
UC and Crohns disease cannot be differentiated in
about 10% of affected people. Such people are said
to have indeterminate colitis.
UC incidence is similar in men and women; however,
Crohns disease occurs more frequently in men.
Onset peaks in people aged 15 to 30 years and in
people aged 60 to 80 years (ie, 2 peak periods).
1
As
discussed previously, incidence is highest in people of
Jewish ethnicity.
87
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 87
SYMPTOMS
Ulcerative Colitis
Symptom severity correlates with the extent of
disease. The patient presents with:
Bloody diarrhea
Rectal urgency
Tenesmus
Rectal bleeding
Passage of mucus
Crampy abdominal pain
In severe disease, the patient may also have:
Fever
Malaise
Anemia
Anorexia
Weight loss
Joint pain
Symptoms may be exacerbated by recent or past
cigarette smoking cessation or nonsteroidal anti-
inflammatory drug use.
Crohns Disease
Characteristic symptoms of Crohns disease include:
Chronic or nocturnal diarrhea
Abdominal pain
Weight loss
Fever
Rectal bleeding
88
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 88
Other symptoms vary depending on the location of
disease within the GI tract:
Anorexia
Nutritional deficiency
Malaise
Nausea
Vomiting
Incontinence
Bowel obstruction
Upper respiratory tract and enteric infections,
cigarette smoking, and use of nonsteroid anti-
inflammatory drugs may exacerbate symptoms.
Extraintestinal manifestations of IBD
IBD may manifest a multitude of extraintestinal
conditions, including:
Skin disorders (eg, erythema nodosum, pyoderma
gangrenosum)
Peripheral arthritis
Ankylosing spondylitis (in HLA-B27 positive
patients)
Sacroiliitis
Ocular inflammation (eg, conjunctivitis, uveitis,
episcleritis)
Hepatic steatosis
Cholelithiasis
Kidney stones
Ureteral obstruction
Fistulas
Thromboembolic disease
89
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 89
DIAGNOSIS AND LABORATORY TESTING
Owing to the non-specific symptoms, the differential
diagnosis of IBD is lengthy. Disorders to be
considered include:
Gastroenteritis/infectious colitis
Ischemic, radiation-induced, medication-induced,
or other inflammatory bowel disease (eg,
lymphocytic or collagenous colitis)
Celiac disease
Irritable bowel syndrome
Neoplasia
Refer to the appropriate sections of this manual to
review tests that may be useful to rule out these
disorders. Additionally, UC differentiation from
Crohns disease may be helpful for: 1) determining
prognosis and cancer risk, 2) medical and surgical
therapy selection, and 3) patient counseling.
4
Features useful for UC differentiation from Crohns
disease are listed in Table 1. Diagnostic tools include
endoscopy, sigmoidoscopy or colonoscopy,
computerized tomography (CT), magnetic resonance
imaging (MRI), and pathology. Laboratory testing is
also employed.
Complete blood count (CBC) to assess leukocytosis
and anemia is helpful in diagnosis and determining
the severity of disease, respectively. Erythrocyte
sedimentation rate (ESR) helps determine the
severity of disease, as do liver function tests. ESR is
also useful to assess a patients response to therapy.
Perinuclear antineutrophil cytoplasmic antibodies
(pANCA) and anti-Saccharomyces cerevisiae antibody
(ASCA) tests can help differentiate UC from Crohns
disease in the majority of patients.
4
90
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 90
TREATMENT
Inducing and maintaining remission of symptoms,
promoting the highest possible quality of life, is the
primary goal of therapy. IBD treatment is selected, in
part, on the basis of anatomic extent and clinical
severity of the acute attack (eg, disease location,
severity, extraintestinal complications).
The American College of Gastroenterology has
recommended treatment for the various categories of
UC severity (Table 2).
4
Patients are treated medically
91
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
Table 1. Differentiating Features of Ulcerative Colitis and Crohns
Disease
1
Feature Ulcerative Colitis Crohns Disease
Fistula +
Cobblestoning mucosa +
Significant small bowel abnormality +
Segmental colitis +
Asymmetric colitis +
Granuloma on biopsy +/
Perianal disease ++
Abdominal mass /+ +
Obstruction /+ ++
Rectal sparing /+ ++
ASCA-positive /+ ++
ANCA-positive ++ /+
Bloody stools + +/
Mucus + +/
Continuous disease + +/
Abnormal terminal ileum +/ +
Systemic symptoms +/ ++
Pain +/ ++
Stricture +/ ++
, not present; +, present; +/, occasionally present; ++, frequently present; /+, rarely present; ANCA,
perinuclear antineutrophil cytoplasmic antibodies, pANCA; ASCA, anti-Saccharomyces cerevisiae antibody.
57152-01 6/27/07 8:23 AM Page 91
with anti-inflammatory drugs (aminosalicylates such
as mesalamine, corticosteroids such as prednisolone),
immunosuppressives (mercaptopurine, azathioprine,
cyclosporine), and antibiotics (metronidazole,
ciprofloxacin). Additionally, the FDA approved use of
infliximab for inducing and maintaining remission in
patients with refractory disease in 2005 and 2006,
respectively. Surgery (partial or total colectomy) is
recommended if there is exsanguinating
hemorrhage, frank perforation, or documented or
strongly suspected carcinoma.
4
Patients with less
severe, but medically intractable disease, may also be
considered for surgery. Surgery is performed within
92
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
Table 2. Ulcerative Colitis Disease Management
4
Disease Criteria for Therapeutic
Severity Classification Options
Mild <4 stools/d with or Distal colitis: topical mesalamine (preferred),
without blood, no systemic oral aminosalicylates, or topical steroids; oral
toxicity, normal ESR prednisone if refractory
Extensive colitis: daily oral sulfasalazine or
aminosalicylate; if refractory, oral steroids
(prednisone); if still refractory,
6-mercaptopurine or azathioprine
The combined use of oral and topical
aminosalicylates is more effective than use of
either alone.
Moderate >4 stools/d with minimal Same as for mild disease
toxicity
Severe >6 bloody stools/d with Hospitalization, daily intravenous steroid (eg,
fever, tachycardia, anemia, hydrocortisone, methylprednisolone); if
or increased ESR refractory, IV cyclosporine (alternatively,
colectomy); consider CMV and C difficile
infection
Fulminant >10 stools/d, continuous Same as for severe disease with addition of
bleeding, toxicity, broad-spectrum antibiotics and small bowel
abdominal tenderness and decompression tube (if small bowel ileus
distension, anemia present), keep NPO, rotate frequently into
requiring blood transfusion, prone or knee-elbow position; if deterioration
and colonic dilation occurs, perform immediate colectomy
IV, intravenous.
57152-01 6/27/07 8:23 AM Page 92
the first 10 years of illness for about half of the
patients with extensive chronic UC.
1
Since patients with UC are at increased risk of colon
cancer, annual or biannual colonoscopy should be
performed in patients who have been affected for >8
to 10 years. Evidence of dysplasia warrants consideration
of colectomy to prevent cancer and metastasis.
The American College of Gastroenterology has
recommended treatment for the various categories
of Crohns disease severity (Table 3).
5
Patients are
treated medically with anti-inflammatory drugs
(aminosalicylates such as mesalamine and
sulfasalazine, corticosteroids such as prednisolone
and budesonide, and infliximab), immunosuppressives
(cyclosporine, tacrolimus), and antibiotics
(metronidazole, ciprofloxacin). Corticosteroids are
contraindicated for long-term maintenance; however
antibiotics can be used. Surgery is recommended to
93
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
Table 3. Crohns Disease Management
5
Disease Criteria for Therapeutic
Severity Classification Options
Mild-moderate Ambulatory, no dehydration, Oral mesalamine, sulfasalazine,
fever, rigor, prostration, metronidazole, or ciprofloxacin
abdominal tenderness, painful
mass, obstruction or >10%
weight loss
Moderate-severe Refractory to treatment for mild- Oral steroid therapy (eg,
moderate disease or presence of prednisone, budesonide),
fever, significant weight loss, antibiotic therapy, percutaneous or
abdominal pain, intermittent surgical drainage of abscess,
nausea or vomiting, or anemia infliximab infusion
Severe-fulminant Symptoms persist despite Hospitalization with percutaneous
outpatient steroid therapy or or surgical drainage of abscesses,
presence of high fever, persistent parenteral corticosteroids,
vomiting, intestinal obstruction, nutritional support, and/or surgery
rebound tenderness, cachexia, as clinically indicated
or abscess
57152-01 6/27/07 8:23 AM Page 93
treat complications or medically refractory disease.
5
Most patients with Crohns disease require surgery at
some point.
1
PROGNOSIS
While IBD is a serious chronic disease, most people
with the illness may continue to lead full, active, and
productive lives, even though they may be
hospitalized from time to time or need to take
medications. In between flare-ups of the disease,
many individuals may be relatively free of symptoms.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
The Crohn's and Colitis Foundation of America
(CCFA)
Phone: 800-932-2423
Internet: http://www.ccfa.org
94
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 94
REFERENCES
1. Friedman S, Blumberg RS. Inflammatory Bowel Disease. In: Kasper DL,
Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds.
Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-
Hill; 2005:1776-1789.
2. Russell RK, Wilson DC, Satsangi J. Unravelling the complex genetics of
inflammatory bowel disease. Arch Dis Child. 2004;89:598-603.
3. Gastrointestinal disorders: inflammatory bowel disease (IBD). In: Beers
MH, Porter RS, Jones TV, Kaplan JL, Berkwits M, eds. The Merck Manual
of Diagnosis and Therapy. 18th ed. Merck Publishing Group; 2006.
Available at: http://www.merck.com/mmpe/sec02/ch018/
ch018a.html?qt=inflammatory%20bowel%20disease&alt=sh. Accessed
February 14, 2007.
4. Kornbluth A, Sachar DB. Ulcerative colitis practice guidelines in adults
(update): American College of Gastroenterology, Practice Parameters
Committee. Am J Gastroenterol. 2004;99:1371-1385.
5. Hanauer SB, Sandborn W and the Practice Parameters Committee of the
American College of Gastroenterology. Management of Crohns disease
in adults. Am J Gastroenterol. 2001;95:635-643.
95
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 95
SECTION 3. MICROSCOPIC COLITIS:
COLLAGENOUS AND LYMPHOCYTIC
COLITIS
OVERVIEW
Microscopic colitis causes chronic watery diarrhea in
spite of a normal appearing colorectum on
endoscopy. Histologic examination of a biopsy,
however, reveals microscopic inflammation. There
are 2 types of microscopic colitis: collagenous colitis
and lymphocytic colitis.
ETIOLOGY
Although no precise cause has been found for
collagenous colitis or lymphocytic colitis, multiple
etiologic theories exist, including that it is an
autoimmune, infectious, or medication-induced
disease.
PREVALENCE
Collagenous colitis occurs primarily in women
(female to male ratio is 9:1), and the age of onset is
60 to 80 years.
1
People with lymphocytic colitis
present at the same age; however, the disorder affects
women and men equally. Both collagenous and
lymphocytic colitis are rare disorders.
SYMPTOMS
Symptoms of microscopic colitis include:
Chronic, nonbloody, watery diarrhea
Dehydration
Fatigue
96
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 96
Weight loss
Abdominal cramping
Patients may also exhibit signs of malnutrition.
DIAGNOSIS AND LABORATORY TESTING
Microscopic colitis is considered when other, more
common causes of watery diarrhea have been
excluded. Diagnosis is based on histologic
appearance of biopsy specimens acquired during
sigmoidoscopy or colonoscopy. Collagenous colitis
shows increased subepithelial collagen deposition
and intraepithelial lymphocytes. Lymphocytic colitis
shows increased intraepithelial lymphocytes, but no
subepithelial collagen deposition.
TREATMENT
Symptoms may disappear without treatment in about
20% of patients.
2
Avoidance of nonsteroidal anti-
inflammatory drugs (NSAIDS) may be successful in
eliminating symptoms in some patients. A low-fat diet
devoid of caffeine and lactose-containing foods may
be helpful. Medical treatment options including
antidiarrheals, antibiotics, 5-aminosalicylates, steroids,
and immunosuppressants are shown in Table 1.
97
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
Table 1. Medical Treatment Options for
Microscopic Colitis
2
Therapy Options
First line Loperamide (Imodium
'
) or
diphenoxylate/atropine (Lomotil
'
)
Second line Bismuth subsalicylate, mesalamine, or
cholestyramine
Third line Budesonide, prednisone
Fourth line Azathioprine, 6-mercaptopurine
57152-01 6/27/07 8:23 AM Page 97
Surgery may be considered in the few cases
refractory to medical therapy or in patients who
cannot tolerate medical therapy.
PROGNOSIS
Some patients become asymptomatic with no
treatment, while others become asymptomatic after 6
months of treatment. More than 80% of patients will
become asymptomatic within 3 years.
2
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
Digestive Disease National Coalition
507 Capitol Court NE, Suite 200
Washington, DC 20002
Phone: 202-544-7497
National Digestive Diseases Information
Clearinghouse (NDDIC)
Phone: 800-891-5389
Internet: http://digestive.niddk.nih.gov/index.htm
REFERENCES
1. Friedman S, Blumberg RS. Inflammatory Bowel Disease. In: Kasper DL,
Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds.
Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-
Hill; 2005:1776-1789.
2. Goosenberg E, Chaudhary A. Collagenous and lymphocytic colitis.
[EMedicine Web site]. Available at: http://www.emedicine.com/med/
topic1351.htm. Accessed February 14, 2007.
98
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
5
:
I
n
f
l
a
m
m
a
t
o
r
y
I
n
t
e
s
t
i
n
a
l
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 98
OVERVIEW
Colorectal cancer is a common cancer affecting the
colon (large intestine) and/or rectum. It usually
develops from adenomatous polyps; almost all cases
are adenocarcinomas. Colorectal cancer may be
preventable in patients who undergo routine
screening and is often curable when detected early. If
not detected and treated early, colorectal cancer may
metastasize to the regional lymph nodes, liver, lung,
or abdominal peritoneum.
ETIOLOGY AND RISK FACTORS
About three-quarters of colorectal cancer cases result
from environmental factors, diet, and aging. The
remaining 25% of cases are associated with a family
history of colorectal cancer.
1
Risk factors include
2
:
Age (>50 years)
Previous colorectal cancer
Previous colorectal polyps
Inflammatory bowel disease (especially ulcerative
colitis)
Family history of colorectal cancer
Diet high in animal fat (meat and dairy products)
Obesity
Physical inactivity
Cigarette smoking
Heavy alcohol intake
Genetics and Colorectal Cancer
Hereditary colorectal cancer is 1 of 2 types: the rare
familial adenomatous polyposis (FAP) and the less
rare hereditary nonpolyposis colorectal cancer
99
Gastroenterology
Reference Guide
CHAPTER 6. COLORECTAL CANCER
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 99
(HNPCC). FAP is characterized by the presence of
thousands of adenomatous polyps in the large
bowel. Polyps typically develop after puberty but
before age 25 years. If untreated, almost all patients
develop colorectal cancer by the age of 40 years.
FAP is caused by mutations in the adenomatous
polyposis coli (APC) gene. These mutations are
transmitted in an autosomal dominant fashion;
thus, children of an affected parent have a 50%
chance of inheriting FAP. Children should be
routinely screened with proctosigmoidoscopy and,
once the polyps appear, should undergo colectomy
to prevent development of the cancer.
HNPCC, also known as Lynch syndrome, is
transmitted in an autosomal dominant fashion, as is
FAP. Unlike FAP, huge numbers of polyps do not
develop. Cancer usually arises in the proximal large
bowel before the patient is 50 years old. Affected
women may also develop primary ovarian or
endometrial cancer. Microsatellite instability (MSI)
testing can identify individuals who may have
inherited HNPCC. If MSI testing is positive,
identification of a causative mutation confirms the
diagnosis of HNPCC. Such mutations are found in
the MLH1, MSH2, MSH6, or PMS2 genes. Individuals
meeting the Amsterdam criteria (Table 1) or the
Bethesda criteria (Table 2) are suitable for testing.
More often, multiple members of a family will have
colorectal cancer, but no identifiable hereditary
cause can be found. These patients are said to have
familial colorectal cancer.
PREVALENCE
Colorectal cancer is the second leading cause of
cancer death in the United States, with projections of
100
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 100
55,000 deaths and 149,000 new cases (colon: 107,000;
rectum: 42,000) diagnosed in 2006.
2
101
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
3 relatives with an HNPCC-associated tumor*
1 is a first-degree relative of the other 2
2 successive generations affected
1 diagnosed at <50 years of age
FAP should be excluded in the patients with colorectal
cancer
Tumor should be verified by pathologic examination
Table 1. Amsterdam Criteria
3
FAP, familial adenomatous polyposis.
*Endometrial, stomach, ovarian, pancreas, ureter and renal pelvis, biliary
tract, and brain tumors; sebaceous gland adenomas and keratoacanthomas
in Muir-Torre syndrome; and carcinoma of the small bowel.
Colorectal tumors should be tested for MSI in individuals
meeting any of the following:
Colorectal cancer diagnosed at age <50 years
Presence of synchronous colorectal cancers (multiple
cancers 6 months after initial tumor removal),
metachronous colorectal cancer (cancer recurrence >6
months after initial tumor removal), or other HNPCC-
associated tumors*
Colorectal cancer with the MSI-H histology
diagnosed at
age <60 years
Colorectal cancer in 1 first-degree relative with an
HNPCC-related tumor with 1 of the cancers diagnosed
at age <50 years
Colorectal cancer diagnosed in 2 first- or second-degree
relatives with HNPCC-related tumors
Table 2. Bethesda Criteria
4
*Endometrial, stomach, ovarian, pancreas, ureter and renal pelvis, biliary
tract, and brain tumors; sebaceous gland adenomas and keratoacanthomas
in Muir-Torre syndrome; and carcinoma of the small bowel.
Presence of tumor infiltrating lymphocytes, Crohns-like lymphocytic
reaction, mucinous/signet-ring differentiation, or medullary growth
pattern.
57152-01 6/27/07 8:23 AM Page 101
PREVENTION
Screening for colorectal cancer is an important step
in prevention. Removal of polyps found during
screening helps prevent some colorectal cancers
from developing. Additionally, early detection of
colon cancer enables treatment that may cure the
patient.
Although reduction and/or elimination of lifestyle-
based risk factors has not been proven to prevent
colorectal cancer, it is reasonable to recommend such
reduction and/or elimination.
5
Thus, patients should
be counseled to:
Reduce animal fat
Ingest >30 to 35 grams of fiber per day by eating
fruits, vegetables, legumes, and whole grains
5
Avoid obesity
Exercise daily
Stop smoking
Drink alcohol in moderation or not at all
Dietary supplements (eg, folic acid, calcium) and
medications (eg, aspirin, nonsteroidal anti-
inflammatory drugs [NSAIDs], estrogen-replacement
therapy) may reduce risk of colorectal cancer. Their
use to prevent colorectal cancer is not currently
recommended, however.
SYMPTOMS
Symptoms vary based on the location of the cancer
and extent of disease (Table 3).
102
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 102
SCREENING
Screening for colorectal cancer can detect
adenomatous polyps, the precursors of most
colorectal cancers. Removal of these polyps may
prevent cancer from developing. Additionally,
screening can detect colorectal cancer before
outward signs and symptoms are observed. Such early
detection enables treatment that is likely to be
successful in curing the patient.
Screening recommendations vary according to the
individuals risk (Tables 4-6).
103
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
Table 3. Colorectal Cancer Signs and Symptoms
Location Signs and Symptoms
Cecum and ascending Chronic, insidious blood loss leading
(right) colon to fatigue, weakness, unexplained
iron deficiency anemia; occult blood
Transverse and Abdominal cramping, constipation
descending colon and increased stool frequency or
diarrhea, stool streaked or mixed
with blood, focal pain or tenderness
signifying perforation
Rectosigmoid Bloody stools, rectal bleeding,
tenesmus, sensation of incomplete
evacuation, pain
Table 4. Screening Options for Adults of Average
Risk*
6
Annual FOBT or FIT
Flexible sigmoidoscopy every 5 years
Annual FOBT and flexible sigmoidoscopy every 5 years
Double contrast barium enema every 5 years
Colonoscopy every 10 years
FOBT, fecal occult blood test; FIT, fecal immunochemical test.
*Begin screening at age 50 years.
57152-01 6/27/07 8:23 AM Page 103
104
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
Table 5. Screening Recommendations Based on
Personal History
6
History of Screening Recommendation
Inflammatory Consider monitoring with colonoscopy
bowel disease and biopsy beginning 8 to 10 years after
onset
1 to 2 tubular Colonoscopy in 5 years
adenomas (<1 cm)
>3 or advanced Colonoscopy in 3 years; if normal or
adenoma only 1-2 adenomas <1 cm, repeat in
5 years
Colorectal cancer Colonoscopy at diagnosis or 6 months
following surgery if obstructed
preoperatively; repeat in 3 years if
normal; repeat again every 5 years if
normal
Table 6. Screening Recommendations Based on
Family History
6
History of Screening Recommendation
1st degree relative with Screen as for average risk
colorectal cancer or individuals, but start at age 40
adenomatous polyp years
at age >60 years
2 1st degree relatives Colonoscopy every 5 years,
with colorectal cancer or beginning at age 40 years or 10
1st degree relative with years before age of diagnosis in
adenomatous polyps at age affected relative, whichever
60 years occurs earlier
1st degree relative with Colonoscopy every 1-2 years,
HNPCC or carrier of beginning at age 20-25 years or
known MMR gene 10 years before age of diagnosis
mutation in affected relative, whichever
occurs earlier
1st degree relative with FAP Colonoscopy annually
or carrier of known APC beginning at age 10-12 years
gene mutation
MMR, mismatch repair.
57152-01 6/27/07 8:23 AM Page 104
DIAGNOSIS AND LABORATORY TESTING
Colorectal cancer is diagnosed based on histologic
examination of biopsied tissue, which is usually
obtained during sigmoidoscopy or colonoscopy.
Laboratory tests are useful for screening, diagnosis,
selecting therapy, and monitoring patients with
colorectal cancer.
Fecal Occult Blood (FOBT) and Fecal
Immunochemical Tests (FIT)
These tests are non-invasive screening tests
performed on stool samples. Positive results indicate
the presence of blood, which is associated with
colorectal cancer, polyps, trauma, benign tumors,
hemorrhoids, anal fissures, inflammatory bowel
disease, and colonic angiodysplasia. Positive results
should be followed by colonoscopy for a definitive
diagnosis. A negative test means that colorectal
cancer is unlikely; however, a negative test does not
rule out colorectal cancer. Intermittent bleeding or
nonuniform distribution of blood in the stool can
cause negative tests.
Table 7 outlines the differences between these 2 tests.
FIT is considered more specific for colorectal cancer
because diet and medication do not cause false-
positive or false-negative results and because it
measures only the globin portion of the hemoglobin
molecule. Globin does not survive passage from the
upper gastrointestinal (GI) tract, thus ruling out
upper GI causes of blood in the stool (eg, bleeding
esophageal varices, esophagitis, gastritis, peptic
ulcer). In a recent clinical study comparing an FIT
(InSure
'
) with an FOBT, the FIT had a colorectal
cancer true-positive rate of 87.5% vs 54.2% for the
FOBT.
7
105
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 105
Flexible Sigmoidoscopy
Sigmoidoscopy allows inspection of the rectum and
the sigmoid (descending) colon. The patient takes a
laxative the night before and has an enema on the
morning of the test. During the procedure, polyps
and tissue samples (biopsies) can be removed by
inserting tools through the sigmoidoscope. If
adenomatous polyps or colorectal cancer is
diagnosed, a colonoscopy should be performed to
inspect the entire colon.
106
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
Table 7. Differentiating Characteristics of FOBT and FIT
FOBT FIT
Method Oxidation of guaiac by hemoglobin Immunochemistry targeting globin
peroxidase; detects the human and portion of hemoglobin
non-human heme portion of
hemoglobin
Specificity Detects upper* and lower GI Detects lower GI bleeding associated
bleeding with colorectal cancer, adenomas,
polyps, and other lower GI conditions
Patient Avoid ingestion of red meat, some Diet and medication restrictions not
preparation raw fruits, and uncooked vegetables required
for 3 days prior to stool sample
collection; may also need to avoid
non-steroidal anti-inflammatory
drugs, aspirin, and >250 mg/day
vitamin C
Sample Patient defecates into a clean, dry InSure
'
: Toilet water is collected by
collection container (not toilet bowel); patient gently disturbing surface of stool with
smears a portion of the stool on a a supplied brush and then dabbing
slide or card. Patient repeats the water onto a specimen card.
procedure for a total of 3 Patient performs the procedure for a
consecutive bowel movements. total of 2 consecutive bowel
movements.
Other products: 3 consecutive stool
samples as described for FOBT
Examples Hemoccult
'
, Seracult
'
, Coloscreen
'
InSure
'
, HemeSelect
'
, FlexSure
'
*Not associated with colorectal cancer; includes bleeding in the esophagus and stomach.
57152-01 6/27/07 8:23 AM Page 106
Double-Contrast Barium Enema
A double-contrast barium enema is used to optimize
X-rays of the lining of the colon. The patient takes a
laxative the night before and has an enema on the
morning of the test. If positive, this procedure should
be followed by a colonoscopy.
Colonoscopy
Colonoscopy allows inspection of the entire colon
(ascending, transverse, and descending colon) and
the rectum. The patient consumes a clear liquid diet
for 1 to 3 days before the exam. Additionally, the
patient takes a laxative the night before and has an
enema on the morning of the test. During the
procedure, polyps and tissue samples (biopsies) can
be removed by inserting tools through the
colonoscope.
Histologic Exam
Tissue removed from the colon or rectum is
examined under a microscope by a pathologist. This
examination is the only sure way to determine if
cancer is present or not.
MSI, MLH1, MSH2, MSH6
These tests are useful for screening (MSI) and
diagnosis of HNPCC. See Part 3. Test Application
and Interpretation for more information.
Complete Blood Count (CBC)
This laboratory test may be used to determine if
anemia is present. Presence of anemia suggests
chronic bleeding. The patient might need to be
107
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 107
treated for the anemia prior to surgical treatment of
the cancer.
Carcinoembryonic Antigen (CEA)
This laboratory test is used to monitor a patient
being treated for colorectal cancer. An initial,
baseline test is performed before treatment. The
result of this baseline test is then compared with the
result of tests performed during or after treatment. If
the level of CEA increases or stays the same as the
baseline level, the patient is not responding to
treatment and an alternative therapy can be tried. A
decreasing CEA level indicates the patient is
responding to treatment. After successful treatment,
an increasing level means the cancer is recurring.
CEA can detect recurrence before other signs or
symptoms of recurrence are evident.
CA19-9 and CA72-4
These tumor markers might be helpful for the 25%
of patients whose cancer does not produce CEA. If
the patients cancer produces either marker, that
marker can be used in the same manner as CEA.
Additional Procedures
Other procedures such as CT of the abdomen, chest,
and pelvic area may be used to determine if the
cancer has metastasized. Liver function tests may
help evaluate possible liver metastasis. UGT1A1 and
DPYD mutation analysis can be used to predict
toxicity to irinotecan and pyrimidine-based
chemotherapeutic agents (5-fluorouracil,
capecitabine), respectively. UGT1A1 can also be used
to assist in selecting an optimal initial dose of
irinotecan.
108
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 108
STAGING
The American Joint Committee on Cancer (AJCC)
has outlined terminology for staging colorectal
cancers (Tables 8 and 9). The corresponding Dukes
stage is provided in Table 9.
109
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
Table 8. TNM Staging of Colorectal Cancer
8
Tumor staging
T0 No evidence of primary tumor
Tis Carcinoma in situ
T1 Tumor invades submucosa
T2 Tumor invades muscularis propria
T3 Tumor invades subserosa or non-peritonealized pericolic or
perirectal tissues
T4 Tumor invades other organs or structures and/or perforates
visceral peritoneum
Nodal staging
N0 No evidence of metastasis to regional lymph nodes
N1 Metastasis to 1-3 regional lymph nodes
N2 Metastasis to 4 regional lymph nodes
Metastasis
M0 No distant metastasis
M1 Distant metastasis
Table 9. Definition of Colorectal Cancer Stages
8
AJCC Stage Dukes Stage Definition
0 Tis, N0, M0
I A T1 or 2, N0, M0
IIA B T3, N0, M0
IIB B T4, N0, M0
IIIA C T1 or 2, N1, M0
IIIB C T3 or 4, N1, M0
IIIC C Any T, N2, M0
IV Any T, any N, M1
57152-01 6/27/07 8:23 AM Page 109
TREATMENT
Treatment options depend on the stage and
histologic grade (degree of differentiation) as well as
the general health of the patient. Options are
presented in Table 10. Radiation therapy may also be
used for patients with rectal cancer.
9
PROGNOSIS
Early detection and treatment is the key to surviving
colorectal cancer (Table 11). Surgery is often
curative when the tumor has not metastasized.
Additionally, surgical patients rarely (colon) or
infrequently (rectum) need a colostomy.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Society of Colon and Rectal Surgeons
Phone: 847-290-9184
Email: ascrs@fascrs.org
Internet: http://www.fascrs.org
110
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
Table 10. Therapeutic Options for Patients with Colorectal Cancer
1,8,9
Option Comments
Curative Appropriate for nonmetastatic cancers; may include surgical resection
surgery of the tumor or colectomy and removal of regional lymph nodes
Non-curative Appropriate for patients with metastatic disease with GI bleeding or
surgery obstruction; less extensive than curative surgery. Also appropriate to
treat metastatic disease in selected cases
Adjuvant Not indicated for patients with stage I cancer; options include
chemotherapy 5-fluorouracil, leucovorin, oxaliplatin, irinotecan, capecitabine,
bevacizumab, cetuximab, panitumumab
57152-01 6/27/07 8:23 AM Page 110
American Cancer Society
Phone: 800-ACS-2345 (227-2345)
TTY: 866-228-4327
Internet: http://www.cancer.org
Cancer Care, Inc.
Phone: 212-221-3300 or 800-813-HOPE (813-4673)
Email: info@cancercare.org
Internet: http://www.cancercare.org
Cancer Hope Network
Phone: 877- HOPENET (467-3638)or
908-879-4039 (New Jersey residents)
Internet: http://www.cancerhopenetwork.org
Cancer Information Service (CIS)
Phone: 800-4-CANCER (422-6237)
TTY: 800-332-8615
Internet: http://cis.nci.nih.gov
Colon Cancer Alliance (CCA)
Phone: 877-422-2030
Internet: http://www.ccalliance.org
Association of Cancer Online Resources Colon
Cancer Discussion List
Internet: http://www.acor.org/colon.html
111
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
Table 11. Colorectal Cancer Survival Rates
2
Stage at Treatment 5-Year Survival Rate (%)
All 64
Early, localized cancer 90
Regional metastasis* 68
Distant metastasis 10
*Lymph nodes or adjacent organs.
57152-01 6/27/07 8:23 AM Page 111
Colorectal Cancer Network
Phone: 301-879-1500
Email: CCNetwork@colorectal-cancer.net
Internet: http://www.colorectal-cancer.net
American Gastroenterological Association
Foundation for Digestive Health and Nutrition
Phone: 301-222-4002 or 866-337-FDHN (337-3346)
Email: info@fdhn.org
Internet: http://www.fdhn.org
Gilda's Club
Phone: 888-GILDA-4-U (445-3248)
Email: info@gildasclub.org
Internet: http://www.gildasclub.org
National Cancer Institute
Phone: 800-4-CANCER (422-6237) or
301-496-6631
Internet: http://www.nci.nih.gov
NCI's Facing Forward Series
Phone: 888-4-CANCER (422-6237)
Internet: http://www.nci.nih.gov/cancerinfo/
life-after-treatment
National Coalition for Cancer Survivorship
Phone: 877-NCCS-YES (622-7937) or 301-650-9127
Email: info@canceradvocacy.org
Internet: http://www.canceradvocacy.org
The Cancer Information Network
Internet: http://www.cancerlinksusa.com/colorectal/
index.asp
112
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 112
Collaborative Group of the Americas on Inherited
Colorectal Cancer (CGA-ICC)
Phone: 847-290-9184
Internet: http://www.cgaicc.com
United Ostomy Associations of America, Inc.
Phone: 800-826-0826
Email: editor@uoaa.org
Internet: http://www.uoaa.org
The Wellness Community
Phone: 888-793-WELL (793-9355) or 202-659-9709
Email: help@thewellnesscommunity.org
Internet: http://www.thewellnesscommunity.org
REFERENCES CITED
1. Mayer RJ. Gastrointestinal tract cancer. In: Kasper DL, Braunwald E, Fauci
AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of
Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:523-533.
2. American Cancer Society: Cancer facts and figures 2006. Available at:
http://www.cancer.org/downloads/STT/CAFF2006PWSecured.pdf.
Accessed February 15, 2007.
3. Vasen HF, Watson P, Mecklin J-P, et al. New clinical criteria for hereditary
nonpolyposis colorectal cancer (HNPCC, Lynch syndrome) proposed by
the International Collaborative Group on HNPCC. Gastroenterology.
1999;116:1453-1456.
4. Umar A, Boland CR, Terdiman JP, et al. Revised Bethesda guidelines for
hereditary nonpolyposis colorectal cancer (Lynch syndrome) and
microsatellite instability. J Natl Cancer Inst. 2004;96:261-268.
5. American Gastroenterological Association medical position statement:
impact of dietary fiber on colon cancer occurrence. Gastroenterology.
2000;118:1233-1234.
6. Winawer S, Fletcher R, Rex D, et al for the U.S. Multisociety Task Force
on Colorectal Cancer. Colorectal cancer screening and surveillance:
clinical guidelines and rationaleUpdate based on new evidence.
Gastroenterology. 2003;124:544-560.
7. Smith A, Young GP, Cole SR, et al. Comparison of a brush-sampling fecal
immunochemical test for hemoglobin with a sensitive guaiac-based fecal
occult blood test in detection of colorectal neoplasia. Cancer.
2006;107:2152-2159. [This study was funded in part by Enterix Inc.
(through Enterix Australia Pty. Ltd), the manufacturer of InSure FIT.
Enterix is now owned by Quest Diagnostics Incorporated. However,
neither Enterix nor Quest Diagnostics participated in the data analysis or
influenced the conclusions reached by the authors.]
113
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 113
8. Engstrom PF, Benson AB III for the National Comprehensive Cancer
Network
'
. NCCN Clinical Practice Guidelines in Oncology
'
. Colon Cancer,
v.1.2007. Available at: http://www.nccn.org/professionals/physician_gls/
PDF/colon.pdf. Accessed February 20, 2007.
9. Engstrom PF, Benson AB III for the National Comprehensive Cancer
Network
'
. NCCN Clinical Practice Guidelines in Oncology
'
. Rectal Cancer,
v.1.2007. Available at: http://www.nccn.org/professionals/physician_gls/
PDF/rectal.pdf. Accessed February 20, 2007.
ADDITIONAL REFERENCES
1. Colorectal Cancer. In: Beers MH, Porter RS, Jones TV, Kaplan JL, Berkwits
M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck
Publishing Group; 2006. Available at: http://www.merck.com/mmpe/
sec02/ch021/ch021h.html?qt=colorectal%20cancer&alt=sh. Accessed
February 21, 2007.
2. Fecal Occult Blood Test (FOBT). [MedlinePlus Web site]. Available at:
http://www.nlm.nih.gov/medlineplus/ency/article/007008.htm.
Accessed February 21, 2007.
114
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
6
:
C
o
l
o
r
e
c
t
a
l
C
a
n
c
e
r
57152-01 6/27/07 8:23 AM Page 114
SECTION 1. HEPATITIS
OVERVIEW
Hepatitis is characterized by inflammation of the liver
and can be caused by a variety of things, including
viruses, bacteria, alcoholism, autoimmune disease,
medications, and an inherited disorder called
Wilsons disease. Viral hepatitis is relatively common
and can be caused by cytomegalovirus (CMV),
Epstein-Barr virus (EBV), and human
immunodeficiency virus (HIV) as well as by the
hepatitis viruses A, B, C, D, and E. Of these, hepatitis
A, B, and C are the most common, occurring at a
rate of 4.3 per 100,000 individuals in 2004.
1
Hepatitis
C is the most serious of the 3 because the majority of
infections become chronic, it accounts for a
substantial proportion of serious liver disease, and
there is no vaccine for prevention. Viral hepatitis
caused by hepatitis A, B, C, and D will be the focus of
the discussion in this section.
ETIOLOGY
The hepatitis viruses can be transmitted in a variety
of ways (Table 1).
115
Gastroenterology
Reference Guide
CHAPTER 7. LIVER DISORDERS
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 1. Primary Transmission Routes of the Hepatitis Viruses
2
Hepatitis Virus Fecal-oral Parenteral Perinatal Sexual
A X
B X X X
C X X X*
D X X
Bold reflects most common transmission route.
*Possibly, but barrier protection is nevertheless advised.
57152-01 6/27/07 8:23 AM Page 115
RISK FACTORS
Risk factors for transmission of the hepatitis viruses
are listed in Table 2. People with certain disorders
(eg, hemophilia, chronic renal failure, cancer
requiring chemotherapy) are at increased risk for
hepatitis infections transmitted parenterally.
Healthcare workers in hospitals or other institutions
are at increased risk of infections transmitted
parenterally or through a fecal-oral route.
Contaminated needles are a risk for healthcare
workers (accidental needle sticks), for those injecting
drugs of abuse, and for those getting a tattoo or
having acupuncture. Transmission risk increases for
people who travel to endemic areas. Table 3 lists the
most common risk factor for HAV, HBV, and HCV as
reported to the Centers for Disease Control in 2004.
1
116
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 2. Transmission Risk of the Hepatitis Viruses
2
Transmission Route Risk Factors
Fecal-oral Poor personal hygiene
Overcrowding
Contaminated water
Contaminated food (eg, milk, raspberries and strawberries,
shellfish)
Close contact with infected person(s)
Parenteral Repeated blood or blood product transfusions
Contact with bodily fluids (eg, blood) of infected person
Drug abuse (injection with contaminated needles)
Hemodialysis
Organ transplantation
Perinatal HBV infection (including carrier status) during pregnancy
(risk to fetus)
Sexual Hepatitis-infected sex partner
Multiple sex partners
Men having sex with men
57152-01 6/27/07 8:23 AM Page 116
PREVALENCE
The overall prevalence of viral hepatitis attributed to
HAV, HBV, and HCV has decreased in the United
States since 1998.
1
This decrease is due, in part, to
the use of HAV and HBV vaccines and improvements
in the screening of blood donors. Table 4 lists
prevalence statistics for HAV, HBV, and HCV.
PREVENTION
Immunization (passive and active) is used to help
prevent viral hepatitis infection (Table 5). Other
prevention measures include screening blood donors
and implementation of behavioral changes designed
to limit exposure.
117
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 4. Hepatitis Virus Prevalence
1
Prevalence Hepatitis A Hepatitis B Hepatitis C
Estimated new 56,000 60,000 26,000
cases in 2004*
Age-related Similar among all Highest in ages 25 Highest in ages >15 years
age groups to 44 years; lowest
in ages <15 years
Gender-related Similar in males and 1.7 times higher in Slightly higher in males
females except higher males than females than females
in males 35-44 years
of age
Table 3. Most Common Risk Factor for Hepatitis A, B, and C
Infection
1
Hepatitis Virus Most Common Risk Factor
A International travel to endemic area
B Sexual contact
C Drug abuse (injection with contaminated needles)
*Asymptomatic infection and underreporting were taken into account.
57152-01 6/27/07 8:23 AM Page 117
118
Gastroenterology
Reference Guide
Table 5. Immunization for Prevention of Viral Hepatitis
2
Hepatitis Immunization Appropriate Effective
Virus Availability Individuals Period
A Immunoglobulin Individuals in intimate contact* Short term
administered before with an affected person
or up to 2 weeks Children (and their family members)
after exposure and staff at day-care centers with an
infected individual
Travelers to endemic areas if <4
weeks from date of travel
Vaccine Age >2 years 20 years
Children living in area of high
frequency
Day-care center employees
Intravenous drug users
Laboratory (health care) workers
Men having sex with men
Military personnel
Patients requiring frequent doses of
clotting-factor concentrates
Patients with chronic liver disease
(including chronic HCV infection)
Primate handlers
Travelers to endemic areas
B Vaccine Children <18 years of age Unclear;
Health care workers exposed to blood probably 5
Hemodialysis center patients and staff to 10 years
Household and sexual contacts of
HBV carriers
Intravenous drug users
People in endemic areas (living or
travelers)
People with hemophilia
People with multiple sex partners
Prison inmates
Vaccine + HBIG Unvaccinated person exposed to HBV Unclear
(eg, needle stick, sex with affected
person, etc)
Infants born to HBsAg-positive woman
C None
D HBV vaccine Susceptible people Unclear
HBIG, hepatitis B immune globulin.
*Household, sexual, institutional.
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 118
SYMPTOMS
The hepatitis viruses produce clinically similar
illnesses and cannot be differentiated based solely on
the patients presentation. While some patients are
asymptomatic, others experience sudden, intense
symptoms (ie, fulminant disease). Chronic infections
(ie, those of 6 months duration) can progress to
liver cirrhosis and hepatocellular carcinoma.
Symptoms of acute viral hepatitis include:
Anorexia
Nausea
Vomiting
Malaise
Arthralgias
Myalgias
Headache
Fever
Dark urine
Clay-colored stools
Jaundice
Weight loss
Abdominal pain
Symptoms typically appear 2 to 26 weeks after
exposure (Table 6).
119
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 6. Incubation Periods for the Hepatitis
Viruses
2
Hepatitis Virus Incubation Period (weeks)
A 2 to 6
B 4 to 26
C 2 to 23
D 4 to 26
57152-01 6/27/07 8:23 AM Page 119
Patients with chronic viral hepatitis may be
asymptomatic or may have the same symptoms as
those with acute stage disease. Additionally, patients
with chronic viral hepatitis may have:
Fatigue
Ascites
Edema
Bleeding gastroesophageal varices
Hepatic encephalopathy
Coagulopathy
Hypersplenism
Leukocytoclastic vasculitis
Immune-complex glomerulonephritis
Polyarteritis nodosa
Sjgrens syndrome
Lichen planus
Porphyria cutanea tarda
DIAGNOSIS AND LABORATORY TESTING
The differential diagnosis of viral hepatitis includes:
Leptospira, Candida, Brucella, Mycobacteria, and
Pneumocystis infections
Medication- or anesthesia-induced hepatitis
Alcoholism
Cholecystitis
Common duct stone
Ascending cholangitis
Pancreatic cancer
Primary parenchymal liver disease
Certain vascular disorders
Acute fatty liver, cholestasis, eclampsia in a
pregnant patient
Wilsons disease
1
-antitrypsin deficiency
120
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 120
Liver function tests (Table 7), along with clinical
features, help diagnose hepatitis. Liver function tests
are not specific, however. Abnormal results are found
in many conditions. Serologic and molecular tests are
specific for the particular type of viral hepatitis. Table
8 lists tests associated with HAV, HBV, HCV, and
HDV. Tests specific for HEV, CMV, EBV, HIV, herpes
simplex, and coxsackievirus are also available. See
Part 2 and 3 of this manual for test availability, testing
algorithms, and detailed interpretive information.
Liver biopsies are usually not required for diagnosis,
but may be helpful to rule out certain conditions (eg,
alcoholic hepatitis) and assess the extent of disease
(ie, stage of fibrosis) prior to treatment in patients
with chronic hepatitis. HepaScore
is a newly
developed, non-invasive laboratory test that also may
assist with diagnosis and staging of liver fibrosis in
patients with hepatitis C.
TREATMENT
Acute Viral Hepatitis
Antiviral medication is not required for most cases of
acute hepatitis A and B. Since untreated hepatitis C
very often progresses to chronic disease, the decision
to treat hepatitis C with antiviral therapy in the early
121
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 7. Liver Function Test Results in Patients
with Hepatitis
Test Result
Alanine aminotransferase (ALT)
Albumin Normal or
Alkaline phosphatase Normal or
Aspartate aminotransferase (AST)
Bilirubin (total, direct)
57152-01 6/27/07 8:23 AM Page 121
days following onset is dependent on HCV RNA and
ALT levels and the stage of liver fibrosis. Patients are
generally advised to restrict physical activity, eat a
high-calorie diet (primarily in the morning owing to
afternoon nausea), avoid alcoholic drinks, and avoid
medications that may cause cholestasis and those that
are metabolized by the liver. Patients with fulminant
disease require special treatment including
maintenance of fluid balance, circulatory and
respiratory support, control of bleeding and glycemic
state, and restricted protein intake. Laboratory tests
can be used to determine recovery from acute
infection (Table 9).
Chronic Viral Hepatitis
Antiviral therapy (Table 10) is commonly used to
treat chronic viral hepatitis. The goal is to reduce the
viral load (level of viral DNA or RNA in the blood) to
undetectable levels. Thus, viral load testing is an
important tool for monitoring therapy. Additional
indicators of successful therapy are listed in Table 9.
122
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 8. Laboratory Tests for the Differential
Diagnosis of Viral Hepatitis
Viral Hepatitis Type Test Result*
Hepatitis A HAV antibody (IgM) Reactive
Hepatitis B HBV core antibody (IgM) Reactive
HBV surface antigen Reactive
Hepatitis C HCV antibody (EIA) Reactive
HCV antibody (RIBA) Positive
HCV RNA 5 IU/mL
Hepatitis D HDV antibody Reactive
HDV antigen Reactive
*Consistent with type-specific viral hepatitis.
57152-01 6/27/07 8:23 AM Page 122
Genotyping can predict the response to antiviral
therapy. For example, some HBV-associated
mutations diminish response to one medication but
not to another. Thus, knowing the HBV genotype
can help in selecting appropriate medication for an
individual patient. Since the genotype may change
over the course of treatment, periodic monitoring of
non-responders may be helpful.
123
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 9. Indicators of Recovery from Viral Hepatitis
Viral Hepatitis Type Test Result*
Hepatitis A ALT Normal
Hepatitis B HBV envelope antigen Nonreactive
HBV envelope antibody Reactive
HBV surface antigen Nonreactive
HBV DNA Not detected
<100 IU/mL
(<160 copies/mL)
Hepatitis C HCV antibody (RIBA) Negative
HCV RNA Negative
<5 IU/mL
ALT, alanine aminotransferase.
*Consistent with recovery.
Table 10. Antiviral Therapy for Treating Chronic Viral Hepatitis
3
Hepatitis B Hepatitis C* Hepatitis D
Approved Interferon None effective;
Interferon Ribavirin treatment of choice
Lamivudine Pegylated interferon-2a is liver transplantation
Adefovir dipivoxil Pegylated interferon-2b at time of liver failure
Entecavir
Under development
Telbivudine
Clevudine
Emtricitabine
Pegylated interferon
*Pegylated interferon combined with ribavirin is the most effective regimen.
57152-01 6/27/07 8:23 AM Page 123
Patients with HCV genotype 2 or 3 are more likely to
respond to therapy than are patients with HCV
genotype 1. Additionally, patients with genotype 1
require a longer course of treatment.
More detailed information, including test availability,
testing algorithms, and interpretive information can
be found in Part 2 and 3 of this manual.
PROGNOSIS
Most patients with hepatitis A recover from their
infection within 6 months; however, the infection is
fatal in a small percentage of infected people (Table
11). Hepatitis A does not progress to chronic disease,
and patients who recover are immune to recurrent
infection.
Most patients with acute hepatitis B also recover
within 6 months and are immune for life. In those
who do not, the infection is fatal in some and
becomes chronic in others. Patients with chronic
disease may develop hepatocellular carcinoma. Those
who develop a superinfection or coinfection with
hepatitis D also have a poorer prognosis.
Although most patients with hepatitis C develop
chronic disease, their prognosis is relatively good. A
124
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 11. Viral Hepatitis Prognosis
2,3
Viral Mortality Likelihood Likelihood Association with
Hepatitis Rate (%) of Carrier of Chronic Hepatocellular
Type State Disease Carcinoma
A 1 None None No
B 1 to 2 10% (adults) 1%-10% Yes
90% (infants)
C 1 to 5 50%-80% 80%-90% Yes
57152-01 6/27/07 8:23 AM Page 124
small proportion develops serious complications such
as type II cryoglobulinemia and hepatocellular
carcinoma.
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Liver Foundation (ALF)
Phone: 800-GO-LIVER (465-4837) or
888-4HEP-USA (443-7872) or 212-668-1000
Email: info@liverfoundation.org
Internet: http://www.liverfoundation.org
Centers for Disease Control (CDC)
Phone: 800-CDC-INFO (232-6348)
Email: cdcinfo@cdc.gov
Internet: http://www.cdc.gov/ncidod/diseases/
hepatitis/
National Digestive Diseases Information
Clearinghouse (NDICC)
Phone: 800-891-5389
Email: nddic@info.niddk.nih.gov
Internet: http://www.cdc.gov/ncidod/diseases/
hepatitis/
The following links are provided by the American
Liver Foundation:
HCV Advocate
Internet: http://www.hcvadvocate.org/
Hep C Alert
Internet: http://www.hep-c-alert.org/index.htm
125
Gastroenterology
Reference Guide
Hepatitis D Infection
Hepatitis D virus (HDV) can
only infect patients who
have a hepatitis B infection
(ie, no HBV infection, no
HDV infection). There are 2
types of HDV infection:
coinfection and
superinfection. A patient is
said to have HDV
coinfection when the HDV
infection was acquired at
the same time as the HBV
infection. Conversely, a
patient is said to have an
HDV superinfection when
the HDV infection was
acquired after the HBV
infection.
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 125
Hep C Connection
Internet: http://www.hepc-connection.org/
Hepatitis B Foundation
Phone: 215-489-4900
Email: info@hepb.org
Internet: http://www.hepb.org
Hepatitis Foundation International
Phone: 800-891-0707 or 301-622-4200
Email: hfi@comcast.net
Internet: http://www.hepfi.org/
REFERENCES
1. Centers for Disease Control and Prevention. Hepatitis Surveillance Report
No. 61. Atlanta, GA: U.S. Department of Health and Human Services,
Centers for Disease Control and Prevention, 2006. Available at:
http://www.cdc.gov/ncidod/diseases/hepatitis/resource/PDFs/
hep_surveillance_61.pdf. Accessed: February 23, 2007.
2. Dienstag JL, Isselbacher KJ. Acute viral hepatitis. In: Kasper DL,
Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds.
Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-
Hill; 2005:1822-1838.
3. Dienstag JL, Isselbacher KJ. Chronic hepatitis. In: Kasper DL, Braunwald
E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles
of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1844-1855.
126
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 126
SECTION 2. PRIMARY BILIARY CIRRHOSIS
OVERVIEW
Primary biliary cirrhosis (PBC) is characterized by a
slow, progressive destruction of the bile ducts within
the liver, leading to cholestasis (impaired flow of
bile), fibrosis, cirrhosis, and eventual liver failure. In
stage 1, there is chronic inflammation and necrosis of
intrahepatic bile ducts. In stage 2, bile ductules
proliferate; there is infiltration of mononuclear cells
in portal areas; and mild fibrosis may be seen. In
stage 3, there is less inflammatory infiltrate in portal
areas; bile ducts are absent from portal triads; and
there is increased fibrosis. In stage 4, there is biliary
cirrhosis with few remaining bile ducts.
ETIOLOGY AND RISK FACTORS
PBC is thought to be an autoimmune disorder
because it is frequently associated with other
autoimmune disorders (eg, sicca syndrome [dry eyes
and mouth], autoimmune thyroiditis, type 1 diabetes,
rheumatoid arthritis, CREST syndrome, Raynauds
syndrome). Moreover, >90% of patients have an
antimitochondrial antibody (AMA) that is rare in
other forms of liver disease.
1
INCIDENCE/PREVALENCE
PBC occurs most often in women over the age of 20
years.
2
Among patients with symptomatic disease,
90% are women between the ages of 35 and 60
years.
1
127
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 127
SYMPTOMS
About 50% to 60% of patients with PBC are
asymptomatic at time of diagnosis.
2,3
The first sign
may be an abnormal liver function test that is found
during a routine physical or as part of a work-up for
another disorder. Symptomatic patients may have:
Pruritus (itchy skin)
Fatigue
Jaundice
Hyperpigmentation (melanosis)
Hyperlipidemia
Steatorrhea (excessive fat in feces)
Malabsorption of fat-soluble vitamins
Xanthomata (lipid-filled nodule or plaque)
Variceal hemorrhage (portal hypertension)
Ascites
Osteoporosis
Osteomalacia
Finger clubbing
Hepatic insufficiency
DIAGNOSIS AND LABORATORY TESTING
Diagnosis is based on laboratory tests (Table 1),
ultrasound of the liver and biliary tree, and liver
biopsy results. Cholangiography may be needed for
some patients. The differential diagnosis includes
primary sclerosing cholangitis and remediable
extrahepatic biliary tract obstruction.
An otherwise unexplained increase in the alkaline
phosphatase (ALP) level should prompt
consideration of PBC diagnosis. The patient may be
tested for gamma glutamyl transpeptidase (GGT),
conjugated bilirubin, and total cholesterol. An
elevated GGT level confirms liver origin of the
128
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 128
increased ALP. Alkaline phosphatase isoenzymes can
also be used to confirm liver origin. Bilirubin and
cholesterol levels may or may not be elevated
depending on the stage of disease. Bilirubin is usually
elevated in the later stages and suggests a worse
prognosis. Almost all patients (>90%) with PBC have
a positive AMA result.
1,3
An ultrasound is
recommended for patients with evidence of
cholestasis.
2
A liver biopsy may be performed to
confirm the diagnosis, but is not always necessary.
2,3
The most important diagnostic criteria include
increased liver enzymes for >6 months, a positive
AMA result, and compatible liver biopsy (histologic)
findings.
3
If the diagnosis is questionable, other tests
may be performed, including an immunoglobulin
profile and a serum antinuclear antibody (ANA)
test.
2
An elevated IgM fraction is supportive of a PBC
diagnosis, as is a positive ANA test result; however,
these results are not specific for PBC.
129
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 1. Laboratory Test Results Consistent with Primary Biliary
Cirrhosis
2,3
Test Result
Alkaline phosphatase (ALP)
Gamma glutamyl transpeptidase (GGT)
Bilirubin, conjugated or normal
Cholesterol, total or normal
Immunoglobulins IgG: normal
IgM:
IgA: normal or if coincident IgA
deficiency
Antimitochondrial antibody (AMA) Positive, titer 1:40
Antinuclear antibody (ANA) Positive (50% of patients)
57152-01 6/27/07 8:23 AM Page 129
TREATMENT
Two treatments are available for PBC: ursodiol
(ursodeoxycholic acid) and liver transplantation.
Ursodiol therapy (13 to 15 mg/kg/day) slows the
progression of PBC but does not cure it. ALP, GGT,
bilirubin, and cholesterol levels tend to decrease.
Some symptoms may be improved while others are
not. For example, ursodiol has no effect on fatigue or
osteoporosis but has variable effect on pruritus and
portal hypertension. Side effects are rare.
Liver transplantation is an effective therapy:
recurrence is uncommon and, if it does happen, the
progression is very slow. Timing of liver
transplantation is based in part on the Mayo risk
score, which includes consideration of the patients
age, serum albumin and bilirubin levels, edema
score, and prothrombin time test results. The
American Association for the Study of Liver Diseases
recommends transplantation for liver failure and in
some patients with uncontrollable pruritus or severe
osteoporosis.
2
Immunosuppressive therapy is not currently
recommended.
Prior to liver transplantation, symptomatic and
preventative treatment is often employed (Table 2).
PROGNOSIS
Although PBC progresses slowly, people with it do
not live as long as those without it. Progression is
highly variable, taking months to years. However, as
stated above, liver transplantation is very successful.
130
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 130
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Liver Foundation (ALF)
Phone: 800-GO-LIVER (465-4837)or
888-4HEP-USA (443-7872)
Email: info@liverfoundation.org
Internet: http://www.liverfoundation.org
National Digestive Diseases Information
Clearinghouse (NDICC)
Phone: 800-891-5389
Email: nddic@info.niddk.nih.gov
Internet: http://digestive.niddk.nih.gov/ddiseases/
pubs/primarybiliarycirrhosis/index.htm
131
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 2. Management of Primary Biliary Cirrhosis
1,2
Symptom Options
Pruritus Cholestyramine (1st choice)
Rifampicin (2nd line therapy)
Opioid antagonists such as nalmephene
and naltrexone (resistant patients only)
Steatorrhea Low-fat diet
Fat soluble Supplementation with vitamins A, D, E,
vitamin deficiency and K
Portal hypertension Beta blockers with or without nitrates
when varices are visualized endoscopically
Osteoporosis Calcium and vitamin D supplementation
Exercise, smoking cessation
Hormone replacement therapy
Bisphosphonate therapy (eg, alendronate)
57152-01 6/27/07 8:23 AM Page 131
REFERENCES
1. Chung RT, Podolsky DK. Cirrhosis and its complications. In: Kasper DL,
Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds.
Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-
Hill; 2005:1858-1869.
2. Heathcote EJ. Management of primary biliary cirrhosis. The American
Association for the Study of Liver Diseases practice guidelines. Hepatology.
2000;31:1005-1013.
3. Kaplan MM, Gershwin ME. Primary biliary cirrhosis. N Engl J Med.
2005;353:1261-1273.
132
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 132
SECTION 3. LIVER CANCER
OVERVIEW
Primary liver cancer includes hepatocellular
carcinoma (HCC), fibrolamellar carcinoma,
cholangiocarcinoma, and papilla of Vater carcinoma.
Hepatocellular carcinoma is by far the most frequent
of these and will be the focus of discussion in this
section.
Metastatic liver cancer is about 20 times more
frequent than primary liver cancer and ranks second
only to cirrhosis as a cause of fatal liver disease.
1
Primary cancers of the gastrointestinal tract, breast,
and lung are the most common types of cancer that
metastasize to the liver. However, all primary cancers,
except those in the brain, may spread to the liver.
Patients may present with weight loss, anorexia, fever,
sweating, and fatigue. Other symptoms occur in more
advanced stages. Evaluation for liver metastasis
usually occurs before treatment of the primary
cancer. Definitive diagnosis is based on liver biopsy
results following discovery of an elevated alkaline
phosphatase level and/or a mass shown on an
ultrasound, CT, or MRI of the liver. Therapy is usually
palliative. Surgery or systemic chemotherapy may
prolong life in some cases.
ETIOLOGY AND RISK FACTORS
HCC is a complication of cirrhosis and, as such, is
caused by chronic liver disease of any type (Table 1).
In the United States, chronic hepatitis B and C
infections are the greatest risk factors. Hormones
may also play a role since prevalence is greater in
men than in women.
1,2
133
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 133
INCIDENCE
The American Cancer Society estimates there will be
about 19,000 new cases of liver and intrahepatic bile
duct cancer in the United States during 2007.
2
More
than half of these will be in men and more than half
of the estimated 16,800 deaths will also be in men.
2
SYMPTOMS
Patients present with nonspecific symptoms including:
Upper abdominal pain
Anorexia
Weight loss
Malaise
Jaundice
Additionally, a paraneoplastic syndrome may occur
and include:
Erythrocytosis
Hypercalcemia
Hypercholesterolemia
134
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 1. Hepatocellular Carcinoma Risk Factors in
the United States
1
Hepatitis C infection
Hepatitis B infection
Alcoholic liver disease
1-antitrypsin deficiency
Hemochromatosis
Tyrosinemia
Primary biliary cirrhosis
Nonalcoholic steatohepatitis
Environmental carcinogens (eg, thorium dioxide, vinyl
chloride)
57152-01 6/27/07 8:23 AM Page 134
Hypoglycemia
Polymyositis
Porphyria
Dysfibrinogenemia
Cryofibrinogenemia
Vasoactive peptide-associated diarrhea
SCREENING
Screening the general population for HCC is not
recommended; however, the National
Comprehensive Cancer Network (NCCN)
recommends patients at high risk be monitored with
alkaline phosphatase, albumin, alpha-fetoprotein
(AFP), and liver ultrasonography every 3 to 6
months.
3
High-risk individuals include those with
chronic hepatitis C virus infection. The frequency of
monitoring should increase to every 3 months when
the AFP is rising but the ultrasound remains
negative.
3
It is unclear whether such monitoring
results in detection of HCC at a curable stage.
Others recommend screening every 6 months to 1
year with AFP and ultrasound. The cost-effectiveness
of this strategy is also questionable.
4
DIAGNOSIS AND LABORATORY TESTING
The diagnostic work-up includes a medical history,
physical examination, laboratory tests, imaging
studies, and biopsy.
Laboratory Tests
Laboratory tests include:
AFP
AFP-L3
135
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 135
Des--carboxy prothrombin protein (DCP)
Glypican-3
Complete blood count (CBC) and platelets
Hepatitis screen
Liver function tests, including alanine
aminotransferase (ALT), total protein, albumin,
globulin, alkaline phosphatase, aspartate
aminotransferase (AST), and bilirubin (total,
direct, indirect)
Prothrombin
Blood urea nitrogen (BUN)
Creatinine
Lactate dehydrogenase (LDH)
The first 4 tests listed above are tumor markers that
are used in the diagnosis and management of HCC.
5
AFP is the most widely used of these tumor markers.
It is an oncofetal protein that is elevated in patients
with HCC, cirrhosis, hepatitis, nonseminomatous
germ cell tumors, and other conditions. Levels >500
g/L (ie, >500 ng/mL), however, are highly
suggestive of HCC and occur in 70% to 80% of
patients.
1
Like AFP, each of these tumor markers are elevated
in some patients with HCC as well as in patients with
other conditions. Their sensitivity and specificity for
HCC vary with the population studied and the cut-off
value (ie, reference range) used. Since they are
independent markers, their combined use improves
the diagnostic sensitivity and specificity.
Tumor markers are also important for assessing
prognosis and monitoring therapy. When monitoring
therapy:
A sustained level post therapy indicates residual
disease
136
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 136
Rising levels indicate recurrent and/or progressive
disease
Falling levels indicate therapeutic response
The other tests listed above help assess the liver
reserve and comorbid conditions and are considered
when making management decisions.
Imaging Studies
Imaging studies enable visualization of the tumor and
may include:
Ultrasound
Computed tomography (CT)
Magnetic resonance imaging (MRI)
Hepatic artery angiography
CT and MRI help define the extent and number of
lesions, vascular anatomy, vessel involvement, and
metastasis; this information is considered when
making treatment decisions.
Biopsy
AFP and imaging studies can be sufficient for
diagnosis; however, definitive diagnosis is based on
biopsy and histologic examination. Biopsy is
appropriate for patients with potentially resectable
disease who have:
<400 ng/mL AFP and a non-reactive hepatitis B
surface antigen test result
<4,000 ng/mL AFP and a reactive hepatitis B
surface antigen test result
3
137
Gastroenterology
Reference Guide
AFP-L3
AFP has 3 different forms,
called glycoforms. The AFP-
L1 glycoform is the major
form found in patients with
nonmalignant liver disorders
such as cirrhosis and viral
hepatitis infection. AFP-L2 is
found primarily in yolk-sac
tumors. AFP-L3 is produced
by liver cancer cells; it is the
major glycoform found in
people with HCC. AFP-L3
might therefore be more
specific for HCC than total
AFP measurements and may
help differentiate between
malignant and nonmalignant
liver disease. People with an
increased percentage of
AFP-L3, relative to total AFP,
are at greater risk of HCC.
Additionally, people with
HCC and increased AFP-L3
may have a worse
prognosis.
5
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 137
Additionally, a biopsy sample is used to determine
the histologic grade of the tumor (Table 2).
STAGING
The American Joint Committee on Cancer (AJCC)
has outlined terminology for staging liver cancer
(Tables 3 and 4). Other scoring systems (eg, Cancer
of the Liver Italian Program [CLIP]) can be used for
predicting prognosis for patients with unresectable
tumors.
138
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 2. Histologic Grading of Hepatocellular
Cancer
3
Grade Definition
G1 Well differentiated
G2 Moderately differentiated
G3 Poorly differentiated
G4 Undifferentiated
Table 3. TNM Staging of Liver Cancer
3
Tumor staging
T0 No evidence of primary tumor
T1 Solitary tumor without vascular invasion
T2 Solitary tumor with vascular invasion or multiple
tumors 5 cm
T3 Multiple tumors >5 cm or tumor involving major
branch of portal or hepatic vein
T4 Invasion of adjacent organs other than gallbladder
or perforation of visceral peritoneum
Nodal staging
N0 No evidence of metastasis to regional lymph nodes
N1 Metastasis to regional lymph nodes
Metastasis
M0 No distant metastasis
M1 Distant metastasis
57152-01 6/27/07 8:23 AM Page 138
TREATMENT
Treatment options (Table 5) vary based on the
tumor stage, grade, liver reserve, and comorbid
conditions. Surgery that includes a liver
transplantation is the only cure for HCC. Patients
who are candidates for liver transplantation include
those for whom resection is not an option and who
have the following:
A single tumor 5 cm or 2 to 3 tumors each 3 cm
No macrovascular invasion
No extrahepatic spread to lymph nodes, lungs,
abdominal organs, or bone
139
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
Table 5. Therapeutic Options for Hepatocellular
Cancer
3
Surgical resection with or without ablation
Surgical resection with liver transplantation
Ablation with radiofrequency, alcohol, cryotherapy, or
microwave
Embolization (vessel occlusion) including chemoembolization
or radioembolization
Chemotherapy
Radiation therapy
Palliative therapy (ie, supportive care)
Table 4. Definition of Liver Cancer Stages
3
Stage Definition
I T1, N0, M0
II T2, N0, M0
IIIA T3, N0, M0
IIIB T4, N0, M0
IIIC Any T, N1, M0
IV Any T, any N, M1
57152-01 6/27/07 8:23 AM Page 139
PROGNOSIS
The 5-year survival in liver transplant recipients is as
high as 75%.
3
The 3-year survival for patients
diagnosed before symptoms occur and who receive
surgical resection without a liver transplant is 28%.
1
Most patients diagnosed when symptomatic die
within 3 to 6 months.
1
RESOURCES
National and regional educational and supportive
resources are available. For more information,
contact:
American Cancer Society
Phone: 800-ACS-2345 (227-2345)
TTY: 866-228-4327
Internet: http://www.cancer.org
American Liver Foundation (ALF)
Phone: 800-GO-LIVER (465-4837) or
888-4HEP-USA (443-7872) or 212-668-1000
Email: info@liverfoundation.org
Internet: http://www.liverfoundation.org
Cancer Care, Inc.
Phone: 800-813-HOPE (813-4673) or 212-221-3300
Email: info@cancercare.org
Internet: http://www.cancercare.org
Cancer Hope Network
Phone: 877-HOPENET (467-3638) or
908-879-4039 (New Jersey residents)
Email: info@cancerhopenetwork.org
Internet: http://www.cancerhopenetwork.org
140
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 140
National Cancer Institute
Phone: 800-4-CANCER (422-6237) or 301-496-6631
TTY: 800-332-8615
Email: cancergovstaff@mail.nih.gov
Internet: http://cancer.gov
NCIs Facing Forward Series
Phone: 888-4-CANCER (422-6237)
Internet: www.nci.nih.gov/cancerinfo/life-after-
treatment
National Coalition for Cancer Survivorship
Phone: 877-NCCS-YES (622-7937) or 301-650-9127
Email: info@canceradvocacy.org
Internet: http://www.canceradvocacy.org
The Cancer Information Network
Internet: http://www.cancerlinksusa.com
The Wellness Community Executive Office
Phone: 888-793-WELL (793-9355) or 202-659-9709
Email: help@thewellnesscommunity.org
Internet: http://www.thewellnesscommunity.org
141
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 141
REFERENCES
1. Dienstag JL, Isselbacher KJ. Tumors of the liver and biliary tract. In:
Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL,
eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY:
McGraw-Hill; 2005:533-536.
2. American Cancer Society: Cancer facts and figures 2007. Available at:
http://www.cancer.org/docroot/STT/stt_0.asp. Accessed March 07, 2007.
3. Benson AB III, Curley SA, Sigurdson ER for the National Comprehensive
Cancer Network
'
. NCCN Clinical Practice Guidelines in Oncology
'
.
Hepatobiliary cancers. V.1.2007. Available at: http://www.nccn.org/
professionals/physician_gls/PDF/hepatobiliary.pdf. Accessed March 6,
2007.
4. Daniele B, Bencivenga A, Megna AS, et al. Alpha-fetoprotein and
ultrasonography screening for hepatocellular carcinoma. Gastroenterology.
2004;127(Suppl 1):S108-S112.
5. Zhou L, Liu J, Luo F. Serum tumor markers for detection of
hepatocellular carcinoma. World J Gastroenterol. 2006;12:1175-1181
142
Gastroenterology
Reference Guide
C
h
a
p
t
e
r
7
:
L
i
v
e
r
D
i
s
o
r
d
e
r
s
57152-01 6/27/07 8:23 AM Page 142
Potrebbero piacerti anche
- A Simple Guide to Celiac Disease and Malabsorption DiseasesDa EverandA Simple Guide to Celiac Disease and Malabsorption DiseasesNessuna valutazione finora
- Gastro PDFDocumento304 pagineGastro PDFAri Syuhada PutraNessuna valutazione finora
- Celiac Disease (Updated 4th Edition): A Hidden EpidemicDa EverandCeliac Disease (Updated 4th Edition): A Hidden EpidemicNessuna valutazione finora
- Celiac Disease (Gluten-Sensitive Enteropathy)Documento6 pagineCeliac Disease (Gluten-Sensitive Enteropathy)Cricket Trick & FitnessNessuna valutazione finora
- Gluten-Free Diet in Celiac Disease-ForeverDocumento14 pagineGluten-Free Diet in Celiac Disease-ForeverRadwan AjoNessuna valutazione finora
- Celiac Disease: Mobin Ur RehmanDocumento46 pagineCeliac Disease: Mobin Ur RehmanMobin Ur Rehman KhanNessuna valutazione finora
- A Guide to Diabetes: Symptoms; Causes; Treatment; PreventionDa EverandA Guide to Diabetes: Symptoms; Causes; Treatment; PreventionNessuna valutazione finora
- Celiac Disease FinalDocumento7 pagineCeliac Disease FinalacholineNessuna valutazione finora
- Booklet On Coeliac DiseaseDocumento12 pagineBooklet On Coeliac DiseaseQiliang Liu100% (1)
- Celiac DiseaseDocumento37 pagineCeliac DiseaseTaj lamajed100% (1)
- Celiac Disease Celiac Sprue Gluten SensiDocumento2 pagineCeliac Disease Celiac Sprue Gluten SensiNərmin ŞahverdiyevaNessuna valutazione finora
- Celiac Disease - 2024Documento9 pagineCeliac Disease - 2024khaleelNessuna valutazione finora
- Orphanet Journal of Rare Diseases: Celiac DiseaseDocumento8 pagineOrphanet Journal of Rare Diseases: Celiac DiseaseFauzi NoviaNessuna valutazione finora
- Celiac Disease in Women: Mohamed Kandeel, M.D. Professor of Obstetrics and Gynecology Menofyia University EgyptDocumento19 pagineCeliac Disease in Women: Mohamed Kandeel, M.D. Professor of Obstetrics and Gynecology Menofyia University EgyptMohammad EklakhNessuna valutazione finora
- Non Celiac Enteropathy Level 2 - July 2016Documento7 pagineNon Celiac Enteropathy Level 2 - July 2016احمد ليمونهNessuna valutazione finora
- Celiac Disease: Clinical PracticeDocumento8 pagineCeliac Disease: Clinical PracticeRo RojasNessuna valutazione finora
- Celiac DiseaseDocumento20 pagineCeliac DiseasezaydeeeeNessuna valutazione finora
- C D /G I: Case ReportDocumento3 pagineC D /G I: Case ReportCatalina Mariana MargarintNessuna valutazione finora
- Involuntary Weight Loss (GSH)Documento30 pagineInvoluntary Weight Loss (GSH)Febriliana Mao-maoNessuna valutazione finora
- DC Mais Comum Do Que Se PensaDocumento8 pagineDC Mais Comum Do Que Se PensaMary Jane NascimentoNessuna valutazione finora
- Immunology of Type 1 DiabetesDocumento14 pagineImmunology of Type 1 DiabetesKPRI Bina WaluyaNessuna valutazione finora
- Review Article On Gluten AllergyDocumento4 pagineReview Article On Gluten Allergyfelicsp2001Nessuna valutazione finora
- KNH 413 Diet Instruction Celiac DiseaseDocumento3 pagineKNH 413 Diet Instruction Celiac Diseaseapi-301897220Nessuna valutazione finora
- Involuntary Weight Loss (GSH)Documento39 pagineInvoluntary Weight Loss (GSH)AchmadRizaNessuna valutazione finora
- Gluten IntoleranceDocumento8 pagineGluten IntoleranceSanda Maria CretoiuNessuna valutazione finora
- Dermatitis Herpetiformis CDAC PP 508Documento2 pagineDermatitis Herpetiformis CDAC PP 508D U N I A A N I M ENessuna valutazione finora
- Group 2 Presentation DieteticsDocumento30 pagineGroup 2 Presentation DieteticsEman ZahraNessuna valutazione finora
- Final Manuscript TorresDocumento22 pagineFinal Manuscript Torrescharibel torresNessuna valutazione finora
- Chronic Constipation in A 7-Year-Old Boy: Judy-April Oparaji, MD, RDN, CSP, Theresa Heifert, MDDocumento5 pagineChronic Constipation in A 7-Year-Old Boy: Judy-April Oparaji, MD, RDN, CSP, Theresa Heifert, MDbella friscaamaliaNessuna valutazione finora
- Celiac Disease - Case StudyDocumento29 pagineCeliac Disease - Case StudyRye HanaNessuna valutazione finora
- 05 ConstipationDocumento13 pagine05 ConstipationNatanael NababanNessuna valutazione finora
- 05.diagnosis and Classification of Diabetes Mellitus PDFDocumento6 pagine05.diagnosis and Classification of Diabetes Mellitus PDFEliuth ZamoraNessuna valutazione finora
- Celiac DiseaseDocumento42 pagineCeliac DiseaseTri P BukerNessuna valutazione finora
- Gastroesophagean Reflux DiseaseDocumento13 pagineGastroesophagean Reflux Diseasedenisa malinaNessuna valutazione finora
- Case Study 1Documento10 pagineCase Study 1api-242123281Nessuna valutazione finora
- Celiac DiseaseDocumento35 pagineCeliac DiseaseRye HanaNessuna valutazione finora
- Diabetes MellitusDocumento37 pagineDiabetes MellitusAnu PatelNessuna valutazione finora
- Celiac DiseaseDocumento12 pagineCeliac DiseaseDasagrandhi Chakradhar100% (1)
- NCGS or WIS - J Pediatr 2015Documento7 pagineNCGS or WIS - J Pediatr 2015Fernando Clemente YagoNessuna valutazione finora
- IBD Final11Documento41 pagineIBD Final11abraham debebeNessuna valutazione finora
- Coeliac Disease: John S. Leeds, Andrew D. Hopper, and David S. SandersDocumento14 pagineCoeliac Disease: John S. Leeds, Andrew D. Hopper, and David S. Sandersbdalcin5512Nessuna valutazione finora
- Hepatic ProblemsDocumento29 pagineHepatic ProblemsQing Liang OngNessuna valutazione finora
- The Pathogenesis and Pathophysiology of Type 1 and PDFDocumento12 pagineThe Pathogenesis and Pathophysiology of Type 1 and PDFasmawatiNessuna valutazione finora
- knh411 Celiac DiseaseDocumento11 pagineknh411 Celiac Diseaseapi-301897220100% (1)
- DM Tipe 1 AnakDocumento13 pagineDM Tipe 1 AnakChaira Alkanzi DjeniNessuna valutazione finora
- Celiac Disease: DR Ajeet Kumar Lohana Senior Registrar Gastroenterology AtmcDocumento59 pagineCeliac Disease: DR Ajeet Kumar Lohana Senior Registrar Gastroenterology AtmcAjeet LohanaNessuna valutazione finora
- DM Type 2Documento13 pagineDM Type 2paul vinothNessuna valutazione finora
- Case Study 1-1Documento9 pagineCase Study 1-1api-242226130Nessuna valutazione finora
- The Present and The Future in The Diagnosis and Management of Celiac DiseaseDocumento9 pagineThe Present and The Future in The Diagnosis and Management of Celiac Diseaseمودة المنعميNessuna valutazione finora
- Diabetic Ketoacidosis in Toddler With A Diaper RashDocumento4 pagineDiabetic Ketoacidosis in Toddler With A Diaper RashKarl Angelo MontanoNessuna valutazione finora
- Neonatal CholestasisDocumento13 pagineNeonatal Cholestasisgts999Nessuna valutazione finora
- Crohn's DiseaseDocumento8 pagineCrohn's DiseaseShannen Madrid Tindugan100% (1)
- AJGP 2018 0102 Clinical CoeliacDocumento6 pagineAJGP 2018 0102 Clinical CoeliacAngie Viquez BeitaNessuna valutazione finora
- Diagnosis and Classi Fication of Diabetes Mellitus: Merican Iabetes SsociationDocumento8 pagineDiagnosis and Classi Fication of Diabetes Mellitus: Merican Iabetes SsociationSmeu MirelaNessuna valutazione finora
- Acute Pancreatitis PathoDocumento5 pagineAcute Pancreatitis PathoENessuna valutazione finora
- Celiac Disease: The Right Clinical Information, Right Where It's NeededDocumento42 pagineCeliac Disease: The Right Clinical Information, Right Where It's NeededDragomir SandaNessuna valutazione finora
- Celiac Desease: By: Leila Floresca Esteban BSNIII-BDocumento38 pagineCeliac Desease: By: Leila Floresca Esteban BSNIII-BScarletNessuna valutazione finora
- Celiac DiseaseDocumento15 pagineCeliac DiseaseOsama Edris Hama SamanNessuna valutazione finora
- DSC Reporting CodesDocumento7 pagineDSC Reporting Codesbibicul1958Nessuna valutazione finora
- DSC Technical Note - Contact ID Codes: ALARMCOM (02) 9564 5812 or 1800 252 960Documento2 pagineDSC Technical Note - Contact ID Codes: ALARMCOM (02) 9564 5812 or 1800 252 960bibicul1958Nessuna valutazione finora
- APC Computer Magazine Issue 452 March 2018Documento116 pagineAPC Computer Magazine Issue 452 March 2018bibicul1958Nessuna valutazione finora
- High Frequency Transformer For Switch-Mode Power SupplyDocumento154 pagineHigh Frequency Transformer For Switch-Mode Power Supplybibicul1958Nessuna valutazione finora
- Electronics Assembly Electronics Assembly: Surface Surface Mount Mount Technology Technology SMT: SMTDocumento24 pagineElectronics Assembly Electronics Assembly: Surface Surface Mount Mount Technology Technology SMT: SMTbibicul1958Nessuna valutazione finora
- Canon Fax l120Documento58 pagineCanon Fax l120bibicul1958Nessuna valutazione finora
- Gastrointestinal Physiology 05 RevDocumento62 pagineGastrointestinal Physiology 05 Revbibicul1958Nessuna valutazione finora
- Looking Inside Cells FFFFDocumento19 pagineLooking Inside Cells FFFFbibicul1958Nessuna valutazione finora
- Restoring Factory Hard Drive CapacityDocumento73 pagineRestoring Factory Hard Drive Capacitybibicul1958Nessuna valutazione finora
- Ademco Contact IDDocumento5 pagineAdemco Contact IDbibicul1958Nessuna valutazione finora
- 6 Bit AttenuatorDocumento1 pagina6 Bit Attenuatorbibicul1958Nessuna valutazione finora
- How To Find Business InformationDocumento218 pagineHow To Find Business Informationbibicul1958100% (1)
- Azimuth Steueung - EngDocumento13 pagineAzimuth Steueung - EnglacothNessuna valutazione finora
- IMS Objectives Targets 2Documento2 pagineIMS Objectives Targets 2FaridUddin Ahmed100% (3)
- IEC ShipsDocumento6 pagineIEC ShipsdimitaringNessuna valutazione finora
- Article An Incident and Injury Free Culture Changing The Face of Project Operations Terra117 2Documento6 pagineArticle An Incident and Injury Free Culture Changing The Face of Project Operations Terra117 2nguyenthanhtuan_ecoNessuna valutazione finora
- Gods Omnipresence in The World On Possible MeaninDocumento20 pagineGods Omnipresence in The World On Possible MeaninJoan Amanci Casas MuñozNessuna valutazione finora
- Washing Machine: Service ManualDocumento66 pagineWashing Machine: Service ManualFernando AlmeidaNessuna valutazione finora
- Regions of Alaska PresentationDocumento15 pagineRegions of Alaska Presentationapi-260890532Nessuna valutazione finora
- Classifications of AssessmentsDocumento11 pagineClassifications of AssessmentsClaire CatapangNessuna valutazione finora
- Service Manual: SV01-NHX40AX03-01E NHX4000 MSX-853 Axis Adjustment Procedure of Z-Axis Zero Return PositionDocumento5 pagineService Manual: SV01-NHX40AX03-01E NHX4000 MSX-853 Axis Adjustment Procedure of Z-Axis Zero Return Positionmahdi elmay100% (3)
- Quick Help For EDI SEZ IntegrationDocumento2 pagineQuick Help For EDI SEZ IntegrationsrinivasNessuna valutazione finora
- My Personal Code of Ethics1Documento1 paginaMy Personal Code of Ethics1Princess Angel LucanasNessuna valutazione finora
- Spesifikasi PM710Documento73 pagineSpesifikasi PM710Phan'iphan'Nessuna valutazione finora
- BNF Pos - StockmockDocumento14 pagineBNF Pos - StockmockSatish KumarNessuna valutazione finora
- Ib History Command Term PostersDocumento6 pagineIb History Command Term Postersapi-263601302100% (4)
- Elements of ArtDocumento1 paginaElements of Artsamson8cindy8louNessuna valutazione finora
- Nutrition and CKDDocumento20 pagineNutrition and CKDElisa SalakayNessuna valutazione finora
- Quantitative Methods For Economics and Business Lecture N. 5Documento20 pagineQuantitative Methods For Economics and Business Lecture N. 5ghassen msakenNessuna valutazione finora
- SMR 13 Math 201 SyllabusDocumento2 pagineSMR 13 Math 201 SyllabusFurkan ErisNessuna valutazione finora
- Financial Accounting 2 SummaryDocumento10 pagineFinancial Accounting 2 SummaryChoong Xin WeiNessuna valutazione finora
- German Atv-Dvwk Rules and StandardsDocumento25 pagineGerman Atv-Dvwk Rules and StandardsMehmet Emre Bastopcu100% (1)
- How Drugs Work - Basic Pharmacology For Healthcare ProfessionalsDocumento19 pagineHow Drugs Work - Basic Pharmacology For Healthcare ProfessionalsSebastián Pérez GuerraNessuna valutazione finora
- A Case Study Puga Geothermal System,: OF IndiaDocumento7 pagineA Case Study Puga Geothermal System,: OF IndiaPERIKALA TARUNNessuna valutazione finora
- Jesus Prayer-JoinerDocumento13 pagineJesus Prayer-Joinersleepknot_maggotNessuna valutazione finora
- Chemistry Form 4 Daily Lesson Plan - CompressDocumento3 pagineChemistry Form 4 Daily Lesson Plan - Compressadila ramlonNessuna valutazione finora
- Revenue and Expenditure AuditDocumento38 pagineRevenue and Expenditure AuditPavitra MohanNessuna valutazione finora
- Report On GDP of Top 6 Countries.: Submitted To: Prof. Sunil MadanDocumento5 pagineReport On GDP of Top 6 Countries.: Submitted To: Prof. Sunil MadanAbdullah JamalNessuna valutazione finora
- DarcDocumento9 pagineDarcJunior BermudezNessuna valutazione finora
- LEIA Home Lifts Guide FNLDocumento5 pagineLEIA Home Lifts Guide FNLTejinder SinghNessuna valutazione finora
- Turning PointsDocumento2 pagineTurning Pointsapi-223780825Nessuna valutazione finora
- C - Amarjit Singh So Bhura SinghDocumento5 pagineC - Amarjit Singh So Bhura SinghRohit JindalNessuna valutazione finora