Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
StemCell - NCI
Caricato da
ripjojonCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
StemCell - NCI
Caricato da
ripjojonCopyright:
Formati disponibili
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Developed by: Donna Kerrigan, M.S. Kathryn Hollen Jeanne Kelly Brian Hollen Discusses how bone marrow produces bloodforming stem cells that include starter immune cells. When diseases like cancer or its treatment damage these hematopoietic cells, transplanting healthy stem cells from marrow, peripheral blood, or other sources can help some patients. Clarifies how antigens that mark cells as self or nonself are critical determinants of transplant success. Explains autologous, syngeneic, and allogeneic transplants as well as tissue typing.
The art in this tutorial is copyrighted and may not be reused for commercial gain. Please do not remove the NCI logo or the copyright mark from any slide. These tutorials may be copied only if they are distributed free of charge for educational purposes.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Stem Cells
Fertilized egg
(1 day)
Blastocyst
(5 to 6 days) Inner cell mass
(14 to 16 days)
Gastrula
Outer cell mass
Endoderm
Pancreas Liver Thyroid Lung Bladder Urethra
(internal layer)
Mesoderm
(middle layer)
Bone marrow Skeletal, smooth and cardiac muscle Heart and blood vessels Kidney tubules
Ectoderm
Skin Neurons Pituitary gland Eyes Ears
(external layer)
Stem cells are immature body cells that act like starter dough because they can make identical copies of themselves. This keeps a constant supply of starter cells ready to mature within several distinct tissue layers--internal, middle, or external--in response to the bodys needs. Stem cells mature within these layers, replacing aging or damaged cells in their respective body tissues. Once they mature, stem cells lose the ability to duplicate themselves.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Blood Stem Cells
Bone graft Marrow Bone Monocyte Hematopoietic stem cell Multipotential stem cell Myeloid progenitor Neutrophil cell Platelets Lymphoid progenitor cell T lymphocyte Dendritic cell Megakaryocyte Eosinophil Erythrocytes Basophil
B lymphocyte Natural killer cell
R
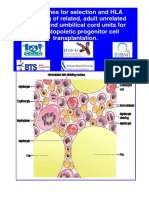
Blood stem cells, known as hematopoietic stem cells, reside primarily in marrow, the spongy interior of bones. These starter cells resupply three types of blood cells: erythrocytes, commonly known as red blood cells; platelets, also called the blood-clotting cells; and leukocytes, the white blood cells of the immune system. When the body needs to replace red blood cells, platelets for blood clotting, or immune cells, stem cells located in the bone marrow mature in a process called hematopoiesis. Hematopoiesis goes on constantly in the human body, but certain conditions call for increased activity. For example, when a person moves to a high altitude or attempts to recover from serious bleeding, increased numbers of stem cells must move from the bone marrow into the bloodstream.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
From Bone Marrow to the Bloodstream
Circulating blood Thymus Lymph nodes Spleen Bone marrow
B lymphocyte
To thymus, tonsils, and lymphoid organs From thymus
T lymphocyte Hematopoietic stem cell Erythrocytes
1 in blood for every 100 in marrow
R
Immune cells--also called white blood cells or lymphocytes--leave the bone marrow while still immature, and they migrate through the bloodstream on their way to the thymus and other lymphoid organs. During their journey, they mature into specialized T or B cells of the immune system. Other blood components, like red blood cells, completely mature in the bone marrow before being released into the blood. In general, at any given moment, there is one blood stem cell circulating in a persons bloodstream for every 100 present in bone marrow. Although it is not precisely understood how the body signals for more blood stem cells to move out of the marrow, scientists are studying some factors that seem to increase the rate of release.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Blood Stem Cell Transplants: When?
Radiation
X
No blood stem cell production
Chemo
In patients with blood cancers such as myeloma, leukemia, or lymphoma, the chemotherapy and radiation that kill malignant cells also kill healthy marrow and its resident blood stem cells. Whether the cancer begins in the marrow itself or in lymphoid or other organs, anticancer treatment can deplete much of the bodys reserve of blood-forming stem cells. Even patients with noncancerous blood diseases can develop a shortage of blood stem cells, as occurs in lifethreatening anemias or immune disorders. In all these cases, a blood stem cell transplant can restore normal hematopoiesis. Hematopoietic or blood stem cell transplants are also called bone marrow transplants or peripheral blood stem cell transplants, depending upon the location of stem cell collection.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Stem Cells from Self to the Rescue
Stem cells are collected from patient
Patient receives chemotherapy or radiation
Self-donated stem cells are re-infused into patient
R
To minimize any damage to blood stem cells from cancer treatment, these stem cells from the bone marrow are removed and preserved before patients receive chemotherapy. The stem cells are then re-infused into the patient after chemotherapy where they migrate to the bone marrow and begin producing new blood cells. Patients with multiple myeloma as well as non-Hodgkins and Hodgkins lymphoma may be offered this approach as part of their treatment.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Stem Cells from Donor to the Rescue
Patient receives chemotherapy or radiation
Stem cells are collected from donor
Stem cells are infused into patient, where they migrate to bone marrow
R
Once collected, stem cells are usually infused immediately into the patient, where they migrate to the bone marrow and settle in or engraft. Once there, stem cells can repopulate the bloodstream with normal red blood cells and immune cells that rescue the patient. For some cancer types, this feat is curative. Alternatively, stem cells are harvested from a donor source and cryopreserved, which means they are frozen in liquid nitrogen. At some later time, they are thawed and infused into a patient.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Not Just Any Blood Stem Cells Will Do
Self
Non-self
The success of a blood stem cell transplant relies upon the interactions of markers on the surface of all body cells, including the immune cells of both the patient and the donor. Normally, all cells within the patients body coexist peacefully in a state known as self-tolerance because all bear the same self marker proteins. These proteins are also called antigens because, should they be introduced into a new environment, they are capable of stimulating a powerful immune reaction. This is what occurs when a blood stem cell preparation with non-self antigens is transplanted into a patient whose self antigens are very different.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Host vs. Graft/Graft vs. Host
Host versus graft reaction
Graft versus host reaction
Donated blood stem cell transplants bring with them their own distinctive self antigens. The immune system of the patient, who is called a host, senses that these antigens are unmatched or non-self. This prompts the patients immune cells to attack the donated (transplanted) cells, which are called a graft, and this assault can lead to the patients rejection of the transplant (host vs. graft). More often, though, some mature donor immune cells that are mixed in among the transplanted blood stem cells recognize the antigens on the patients body cells (host) as non-self. This causes the transplant to attack the patients tissues and organs. The result is graft vs. host disease, which can be very serious.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Tissue Typing Matches Donors to Patients
Patient Autologous Donor Related donor Allogeneic Donor
Patient No conflict: all marker molecules match Syngeneic Donor
Patient Conflict: only some marker molecules match Allogeneic Donor
Patient Identical twin donor Unrelated donor
Patient
= matches to patient
Success in transplanting blood stem cells depends on finding a compatible match of the antigens on donors cells and tissues with those on the patients. In most cases, this means finding sets that are slightly different, but not too different. Donors need not be related to the patient, but they must have a reasonable amount of compatibility. A blood test known as tissue typing is used to find good matches. When patients donate their own stem cells (autologous), self antigens meet self antigens and there is enough similarity to lessen the risk of immune cell warfare. The same advantages are associated with syngeneic (from identical twin) transplants, although few patients have identical twins. In most cases, the transplant is allogeneic, meaning the blood-forming stem cells come from a non-self donor. These transplants will contain antigens that are somewhat like--but not identical to--those of the patient.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
10
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Many Names for the Self Antigens
Body cell Blood cell (leukocyte)
=
Major histocompatibility complex (MHC) proteins (self markers) Human leukocyte antigens (HLAs) (self markers)
R
The scientific name for self antigens is major histocompatibility complex (MHC) proteins, and each person bears a unique set. To make matters even more confusing, when these MHC proteins mark the surface of immune cells called leukocytes, the antigens are dubbed human leukocyte antigens (HLAs). Since leukocytes are the cells used for tissue typing, HLAs are what clinicians use to find reasonable matches for their patients. Whether called MHC proteins or HLAs, all are the same thing--self antigens. Technicians remove human leukocytes from the blood of potential donors and determine what HLA markers are present.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
11
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Haplotypes: Passing on Genes for Self Antigens
Sample Haplotype: Chromosome 6
HLA alleles
DP DQ DR B C A
400
Many Varieties of MHC Self Genes
395 323 195
No. of possible alleles at this locus
100 75 50 25 0
89 45 19 DP DP DQ 20 DQ DR 2 DR B
93
Genes for self antigens are passed on from one generation to the next in a clump called a haplotype. A haplotype is a combination of genes--HLA alleles, for example--that are located closely together on the same chromosome and tend to be inherited together as a package deal. Alleles are genes that come in many varieties, all of which function reasonably well at making the related protein.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
12
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
6 Major Genes: 10,000 Antigens
Paternal chromosome 6 HLA genes Maternal chromosome 6 HLA genes
6 major genes D D D B C A
6 major genes D D D B C A
Paternal leukocyte
Maternal leukocyte
2 (of 6) major human leukocyte antigens* * are MHC proteins
2 (of 6) major human leukocyte antigens*
R
Six important genes for human leukocyte antigens are contributed by each parent. So each person inherits a double set of six major genes that produce six major corresponding antigens, HLA-A, B, -C, -DP, -DQ, and -DR. Since as many as 20 varieties exist for each of these HLA-producing genes in different individuals, the total possible human leukocyte antigens that can mark self and trigger an immune response number about 10,000!
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
13
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Three Most Important Antigens
400
Many Varieties of MHC Self Genes
395 323 195
No. of possible alleles at this locus
100 75 50 25 0
89 45 19 DP DP DQ 20 DQ DR 2 DR B
93
3 most important antigens for tissue matching
DR A
Leukocyte
DQ
DP
Human leukocyte antigens (MHC proteins)
Some donor self antigens are more antigenic than others, which means they are better at triggering an unwanted immune reaction in the transplant patient. By studying successful cases of blood stem cell transplantations, doctors have identified the three most important antigens to match when choosing non-self donors for a transplant. Matching these helps to minimize the chances of graft vs. host or host vs. graft attacks. The antigens are HLA-A, HLA-B, and HLA-DR.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
14
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
A Clinical Match
HLA-B HLA-DR HLA-A HLA-A HLA-B HLA-DR HLA-A HLA-B HLA-DR HLA-A HLA-B HLA-DR
Haplotype 1
Haplotype 3
Haplotype 2
Haplotype 4
Sperm
Ovum
Child A (patient)
Child B
Child C a perfect match
Child D
Child E (donor)
R
An ideal 6:6 antigen match, known as a clinical match, means that both sets of the three most important inherited human leukocyte antigens in the donor match perfectly with those on the body (and immune) cells in the patient. Below, only Child E would serve as a 6:6 clinically matched donor for Child A; one sibling is a total mismatch; the other siblings and both parents would be haplo-identical because only one of their two inherited haplotypes matches Child A.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
15
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Some Haplotypes Occur More Often
2530% chance 4050% chance
5060% chance
>90% chance
Because certain haplotypes are inherited among siblings more frequently than expected merely by chance, there is a 25-30 percent probability of finding a 6:6 match within a family. If one antigen is mismatched, it is a 5:6 match, which clinicians will accept because it increases the odds of finding a donor. When doctors accept a 4:6 match, the likelihood of finding a donor increases even more. As the number of HLA antigen matches decreases among donors and recipients, the chances of finding a donor increase: Antigen match Percent chance of finding a donor: 6-antigen match 25-30% 5-antigen match 40-50% 4-antigen match 50-60% 3-antigen match >90%
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
16
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Sometimes a 3-Antigen Match Is Necessary
3-antigen match
More than 90 percent of patients can find a haplo-identical donor if they are willing to accept a 3antigen match. Sometimes this is medically necessary, as when severely ill patients cannot wait the several months it may take to find a 4-, 5-, or 6-antigen matched donor. Patients accepting a 3antigen haplo-identical match also accept a serious risk of suffering an immune cell attack on their tissues by the transplant (graft vs. host disease), or of having their body reject the transplant (host vs. graft).
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
17
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
A Delicate Balance: Graft vs. Tumor/Graft vs. Host
Transplant attacks tumor in patient
Stem cells plus haplo-identical white blood cells
Transplant attacks patient
Cancer cell Cancer cell destroyed
Should I give the patient steroids?
A Delicate Balance
Haplo-identical transplants may provide a possible benefit. They may enable an attack on cancer to occur. A graft vs. tumor or graft vs. leukemia effect occurs when a donors mature immune cells come along with the stem cells in the transplant, and these immune cells recognize and attack as foreign the cancer cells found in the patients body. This phenomenon helps prevent relapse and, in some cancers, can even be curative. To boost this graft vs. tumor effect, patients are sometimes given an infusion of a donors haplo-identical immune cells (white blood cells) along with the stem cell transplant. A risk with haplo-identical transplants is that of enabling an attack on the patients tissues. This can happen when a donors mature immune cells, called T cells, contaminate the stem cell graft. To minimize this risk, researchers sometimes deplete all T cells from the transplant, leaving the graft with stem cells only. While this can minimize the chance of graft vs. host disease, it also reduces the transplants ability to attack any loitering cancer cells. An alternative option is for the doctor to prescribe steroid medications for the patient pre- and post-transplant. This helps to prevent graft vs. host disease, yet leaves T cells available for graft vs. tumor action.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
18
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Success in Matching Varies With Population
Asian 50% North American Caucasian 93%
Japanese 99%
African American 50%
An alternative to a haplo-identical transplant between related individuals is a matched transplant between unrelated individuals. For Japanese patients, because their island geography increases the likelihood of marriage within a limited gene pool, the chances of finding a 6:6 clinical match are better than for patients in larger gene pools. Of course, much depends upon getting enough donors. Like North American Caucasians, African American and Asian patients are part of a large gene pool, but they are under-represented in the donor pool and only have a 50 percent probability of finding a 6:6 clinical match. Among different ethnic groups, the probability of finding a 6:6 match is, from the highest to lowest, Japanese (99%), North American Caucasian (93%), African American and Asian (50%).
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
19
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Preparing Patients for Myeloablative Allogeneic Transplants
Cancer cells destroyed
High-dose radiation and/or High-dose chemotherapy
Lymphocytes destroyed
Before receiving allogeneic transplants--the most common type--patients with blood cancers must undergo a conditioning regimen of high-dose chemotherapy or radiation to kill any resident cancer cells, suppress the patients immune system, and leave a disease-free environment into which healthy new blood stem cells can be infused. Known as myeloablation, the regimen prepares the patient to accept a non-self graft without triggering a severe attack on the patient by the transplant (graft vs. host disease).
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
20
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Preparing Patients for ReducedIntensity Allogeneic Transplants
Before Transplant After Transplant
Immunosuppressant drugs
Sometimes
Low-dose or standard radiation and/or Low-dose or standard chemotherapy
Donors white blood cells
Because many patients are unable to withstand myeloablation, clinical researchers are studying the feasibility of reduced-intensity nonmyeloablative regimens. Before infusing donated bloodforming stem cells, the patient receives low-dose or standard-dose chemotherapy and/or radiation therapy. Afterward, the patient is given immunosuppressant steroid drugs to help prevent the body from rejecting the transplant. Sometimes the patient also receives an infusion of donated immune cells (white blood cells from the same donor who supplied stem cells) to enhance the grafts attack on the patients cancer (graft vs. tumor benefit). This approach is new, so clinical researchers do not have extensive data on its effectiveness. Graft versus host disease sometimes occurs. So far, rates of graft vs. host disease using this approach are similar to those after high-dose conditioning regimens, but the onset is often delayed by weeks and months. Insurance companies and Medicare administrators, who view reduced-intensity transplants as experimental, often do not cover them.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
21
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Preparing Donors for Allogeneic Transplants
Growth factor to amplify and mobilize stem cells Stem cells ready for infusion Stem cells ready for infusion
Allogeneic transplant
Blood stem cells are extracted most often from the peripheral blood of donors and occasionally from their bone marrow. Because there are significantly fewer stem cells in peripheral blood than in bone marrow, doctors prepare peripheral blood donors by injecting them with a series of growth factors to move blood stem cells from their marrow into their bloodstream. This increases the blood stem cells concentration 10- to 100-fold in the blood. If stem cells are harvested from bone marrow, the donor is placed under general anesthesia. In a procedure that takes about an hour, marrow is removed through a large needle inserted into the donors pelvic bones, and it is processed to remove blood and bone fragments. After the collection is completed, the donor may be given a transfusion of his or her own red blood cells from units of blood that were self-donated a week earlier.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
22
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Apheresis: Harvesting Stem Cells From Peripheral Blood
Blood-forming stem cells
Whole blood is collected from donor
Whole blood in
Stem cells out
Blood, minus stem cells, is returned to donor
Nurses harvest blood stem cells from a donors peripheral blood using a process called apheresis. This process involves removal of whole blood from the donor. As blood is drawn from the donor, circulating stem cells (and sometimes mature immune cells) are extracted. A centrifuge-type machine then separates the components. The blood itself, minus the stem cells, is returned to the donor. Apheresis requires no anesthesia but can take several hours.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
23
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Preparing Patients for Autologous/Syngeneic Transplants
Autologous: Peripheral Blood
Growth factor to amplify and mobilize stem cells
Syngeneic: Peripheral Blood
Cells for Growth factor infusion to amplify into my and mobilize twin stem cells Identical twin donor
Cells for re-infusion Patient
Like allogeneic donors, patients who donate their own peripheral blood for an autologous stem cell transplant, as well as identical twins making a syngeneic donation, receive injections of growth factor prior to collection by apheresis. This amplifies the number of blood stem cells in the bloodstream. Almost all autologous/syngeneic transplants are now taken from peripheral blood. Of course, the patient will also receive high-dose chemotherapy before his self-donated stem cells are reinfused. Some clinical trials even repeat the procedure twice for these autologous transplants, so high-dose chemotherapy is followed by a self-donated transplant two times. This back-to-back clinical protocol is called a tandem transplant.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
24
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Cord Blood as a Source of Stem Cells
Uterus Umbilical cord Placenta
Umbilical cord
Liver
Primitive stem cells
Placenta
R
The human bodys most primitive stem cells form in the fetal yolk sac and move to the fetal liver before entering the babys bone marrow during the third trimester of pregnancy. When a baby is born, the placenta and umbilical cord still contain a rich supply of immature blood stem cells in the very process of migrating. These stem cells are capable of rebuilding all three types of blood cells in the body (red blood cells, immune cells, and platelets). First used in 1989 to help children with leukemia, cord-blood transplants have since proven themselves effective for adults too.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
25
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Placental and Cord-Blood Stem Cell Transplants
Placenta
Umbilical cord
Stem cells transferred to a new bag
After the birth of the baby, blood is collected into a special blood bag
Cryoprotectant added to minimize damage during freezing
Virus-free, tissue-typed stem cells stored in liquid nitrogen for future transplant
Cord and placental blood are retrieved in a single procedure right after a child is born. Nurses remove the majority of the red blood cells and the plasma (which arent needed for transplant) and concentrate the immune stem cells. Then they add an agent to protect these cells from damage during storage at extremely low temperatures. This helps to assure that enough blood-forming stem cells are cryopreserved successfully for later infusion into a patient.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
26
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Using More Than One Cord-Blood Donor
Cord blood from donor 1 1 2 Cord blood from donor 2
Im in charge!
No, Im in charge!
Cells from one unit dominate the other; both attack patients immune system
Clinical trials using cord-blood units from two different donors to increase the number of stem cells infused in a single transplant show that cells from one unit may dominate the other, although both can attack the hosts immune system. This phenomenon, which seems to facilitate grafting and boost the rate of hematopoiesis, is the subject of ongoing research.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
27
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
Placental and Cord-Blood Transplants: Pros and Cons
Pros
Lifesaver when there
Cons
1/10 number of cells vs. Longer time for
is no eligible donor (about 2 weeks)
bone marrow transplant transplant to take maternal cell/genetic disease contamination one cord-blood donor
Available quickly Unlikely to harbor
cytomegalovirus
Slight chance of
Adults need more than
For many patients waiting to be matched to a suitable donor, or for those unable to find one, umbilical cord blood is now a readily available, easy-to-store alternative. Even with a 1- or 2antigen mismatch, cord-blood transplants succeed in a greater percent of cases than occurs with equally mismatched bone marrow transplants. This discovery greatly increases the transplant options for minorities who are under-represented in the donor pool. And cord blood is unlikely to harbor a virus called the cytomegalovirus that can cause life-threatening infections and contaminates about 10 percent of marrow donations. On the other hand, there is a slight risk that maternal cells or genetic disease in the child could contaminate the cord-blood donation. And cord transplants contain only about 1/10 of the number of cells that can be harvested from a bone marrow transplant. Another concern is that cord-blood transplants require more time to take in the recipients bone marrow, leaving the patient vulnerable to infection longer.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
28
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
New Development: Stockpiling
Researchers are investigating different ex vivo methods for amplifying and stockpiling hematopoietic stem cells. If successful, these approaches, along with increased use of placentas and umbilical cords as donors, will offer new hope for patients unable to find a close HLA match.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
29
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
When a Blood Stem Cell Transplant Works
Your biopsy was negative, and your immune cells look good!
The newly transplanted cells home to bone marrow, engraft, then begin to produce healthy new blood cells. Peripheral blood stem cells generally restore the bone marrow within about two weeks, but it can take up to five weeks if the stem cells come from the marrow itself. Restoring complete immune function can take several months in autologous transplants, and one to two years in allogeneic transplants. During the patients recovery, doctors can determine whether the cancer has returned by taking blood samples or aspirating small amounts of bone marrow through a needle for biopsy.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
30
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
National Marrow Donor Program Helps Many
Thank you, DONORS!
To begin a search for unrelated donors, oncologists consult the National Marrow Donor Program coordinating center in Minneapolis, MN, a network of international collection and transplant facilities. It maintains a list of more than three million donors, over one million of whom have been fully typed. Potential matches are found in about 70 percent of preliminary searches, although this rate is lower among certain ethnic groups. More extensive tissue typing is then performed to narrow the potential donor pool further. The federally funded nonprofit National Marrow Donor Program can be reached at: http://www.marrow.org. Persons interested in donating blood stem cells and mothers willing to donate cord blood can find nearby collection centers on this Web site. A technician at the center will draw a small blood sample and subject it to tissue typing. This information will be added to the database of potential donors.
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
31
National Cancer Institute
Understanding Cancer and Related Topics
Understanding Blood Stem Cell Transplantation
We would like to hear from you . . . If you have questions about this tutorials content, suggestions for new topics, or other feedback on the Web site, please send an e-mail to kerrigad@mail.nih.gov. If you have questions about this tutorials artwork or want permission to use it, please send an e-mail to beankelly@verizon.net.
R
NCI Web site: http://cancer.gov/cancertopics/understandingcancer
32
Potrebbero piacerti anche
- Human Electromagnetic Emission in The ELF BandDocumento4 pagineHuman Electromagnetic Emission in The ELF BandbingwazzupNessuna valutazione finora
- JCM 6000 BrochureDocumento15 pagineJCM 6000 BrochureripjojonNessuna valutazione finora
- Jose SilvaDocumento67 pagineJose SilvaLiviu-George Saizescu100% (2)
- Stem Cell Transplant: UnderstandingDocumento24 pagineStem Cell Transplant: Understandingmojimoji00Nessuna valutazione finora
- Insulinom PDFDocumento11 pagineInsulinom PDFverdi33Nessuna valutazione finora
- Blood and Marrow Stem Cell - LLSDocumento56 pagineBlood and Marrow Stem Cell - LLSripjojonNessuna valutazione finora
- Direct Reprogramming of Lymphocites BDocumento23 pagineDirect Reprogramming of Lymphocites BripjojonNessuna valutazione finora
- Survivor Guide To Bone Marrow Transplat PDFDocumento68 pagineSurvivor Guide To Bone Marrow Transplat PDFripjojonNessuna valutazione finora
- Stem Cell Transplant - ACSDocumento32 pagineStem Cell Transplant - ACSripjojon100% (2)
- Astronomybasics Con CelestronDocumento35 pagineAstronomybasics Con CelestroncosmofloydNessuna valutazione finora
- Microsoft Excel 2010 - Training Manual (Beginners)Documento22 pagineMicrosoft Excel 2010 - Training Manual (Beginners)ripjojon50% (2)
- Visible Body ControlsDocumento1 paginaVisible Body Controlsdanhtinh3209Nessuna valutazione finora
- Openerp BookDocumento478 pagineOpenerp Bookjope007Nessuna valutazione finora
- Openerp 61 AccountingDocumento188 pagineOpenerp 61 AccountingFabrizioMaltaDiNapoliNessuna valutazione finora
- HIV Medicine 2005Documento762 pagineHIV Medicine 2005Ionut VrejaNessuna valutazione finora
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (119)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Reelabs Presentation (MotherDocumento79 pagineReelabs Presentation (MotheraashishpoladiaNessuna valutazione finora
- The Thaakat Insider - Summer 2012 EditionDocumento4 pagineThe Thaakat Insider - Summer 2012 EditionthaakatNessuna valutazione finora
- Stem Cell Donor Selection Guidelines V2012 - 13Documento36 pagineStem Cell Donor Selection Guidelines V2012 - 13cristina_zaharia865440Nessuna valutazione finora
- PBL Report ThalassemiaDocumento10 paginePBL Report Thalassemiasarah_amigurlz88100% (2)
- Standardizing SOPs benchmarks cell processing lab performanceDocumento3 pagineStandardizing SOPs benchmarks cell processing lab performanceTejasNessuna valutazione finora
- BTM Report2Community 2010Documento20 pagineBTM Report2Community 2010Vanshika SharmaNessuna valutazione finora
- HLA DictionaryDocumento76 pagineHLA DictionaryNeel MehtaNessuna valutazione finora
- Cord Blood Banking Saves LivesDocumento9 pagineCord Blood Banking Saves LivesGreen AlonsoNessuna valutazione finora
- Simulasi TOEFL Buku EdukasiDocumento28 pagineSimulasi TOEFL Buku EdukasiMuhammad SudrajadNessuna valutazione finora
- Acute Myeloid LeukemiaDocumento15 pagineAcute Myeloid LeukemiaMark Anthony IbayNessuna valutazione finora
- TO E F 4 PRACTICE LISTENING SECTIONDocumento28 pagineTO E F 4 PRACTICE LISTENING SECTIONadindaNessuna valutazione finora
- 1-Bank Soal TOEFLDocumento72 pagine1-Bank Soal TOEFLfadiah19Nessuna valutazione finora
- Storage of Cellular Therapy Products: Issues Related To Duration, Discard and QuarantineDocumento61 pagineStorage of Cellular Therapy Products: Issues Related To Duration, Discard and Quarantinepopatlilo2Nessuna valutazione finora
- Slovenia's 25-year journey to help blood cancer patientsDocumento40 pagineSlovenia's 25-year journey to help blood cancer patientsKlemen JamnikNessuna valutazione finora
- UntitledDocumento295 pagineUntitledoutdash2Nessuna valutazione finora
- Storage of Cellular Therapy Products Presentation Slide Format PDFDocumento61 pagineStorage of Cellular Therapy Products Presentation Slide Format PDFpopatlilo2Nessuna valutazione finora
- Stem Cell Transplant - ACSDocumento32 pagineStem Cell Transplant - ACSripjojon100% (2)
- AABB Sample New Program Business PlanDocumento14 pagineAABB Sample New Program Business Planbiospacecowboy100% (1)
- LDLF Press Release 20012 Swabs For 2012Documento2 pagineLDLF Press Release 20012 Swabs For 2012Luis Danvers Leukemia FundNessuna valutazione finora
- Kisi2 UtsDocumento8 pagineKisi2 Utslulumiftahunnisa29Nessuna valutazione finora