Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Pulp Revascularization of A Necrotic Infected Immature Permanent Tooth: Case Report and Review of The Literature
Caricato da
Riad BachoTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Pulp Revascularization of A Necrotic Infected Immature Permanent Tooth: Case Report and Review of The Literature
Caricato da
Riad BachoCopyright:
Formati disponibili
PEDIATRIC DENTISTRY
V 29 / NO 1
JAN / FEB 07
Case Report
Pulp Revascularization of a Necrotic Infected Immature Permanent Tooth: Case Report and Review of the Literature
Blayne Thibodeau, DMD, MS1 Martin Trope DMD2
Abstract: The purpose of this report was to present the case of a patient wherein revascularization of the necrotic infected pulp space of an immature permanent
maxillary central incisor tooth was induced in vivo by stimulation of a blood clot from the periapical tissues into the canal space. This was achieved after disinfection of the canal space with a topical antibiotic paste followed by a blood clot scaffold induced from the periapical tissues. This treatment approach offers clinicians great potential to avoid the need for traditional apexication with calcium hydroxide or the need to achieve an articial apical barrier with mineral trioxide aggregate. Furthermore, this treatment approach can help rescue infected immature teeth by physiologically strengthening the root walls. (Pediatr Dent 2007;29:47-50)
KEYWORDS: PULP REVASCULARIZATION, PULP THERAPY, APEXIFICATION
Pulpal necrosis of an immature tooth secondary to caries or trauma poses many potential complications. The traditional techniques of chemomechanical instrumentation and disinfection of the root canal system used in mature teeth are limited by the anatomy of the immature tooth. It is dicult to instrument immature canal spaces with conventional endodontic techniques. The open apex is dicult or impossible to seal with conventional root lling methods because of the absence of an apical stop. Furthermore, the arrested development of the dentinal walls at the time of pulp necrosis leaves a weak tooth with thin dentinal walls that are susceptible to fracture. Root reinforcement techniques for immature, thin-walled teeth are available. They can make root canal re-treatment dicult or even impossible, however, if the need arises in the future.1 Finally, the traditional treatment of immature teeth with necrotic pulps and apical periodontitis involves long-term application of Ca(OH)2 (calcium hydroxide) to induce apexication. Andreasen and others have shown that long-term Ca(OH)2 treatment may leave the tooth even weaker and more susceptible to fracture, emphasizing the need for an improved treatment technique.2
Dr. Thibodeau is currently an endodontist in private practice in Hamilton and St. Catharines, Ontario, Canada, and was formerly a resident in the Department of Endodontics, University of North Carolina School of Dentistry, Chapel Hill, NC; and 2Dr. Trope is JB Freedland Professor, Department of Endodontics, University of North Carolina School of Dentistry. Correspond with Dr. Thibodeau at blaynethibodeau@gmail.com
1
Studies on traumatic injuries to immature teeth show promise for revascularization of the root canal system.3,4 Under such a scenario, the uninfected necrotic pulp may act as a scaold for the ingrowth of new tissue. The key factor for the success of this process in necrotic, infected, immature teeth is disinfection of the root canal system, since it is theorized to be essential to create an environment conducive to revascularization of the root canal system.5,6 Various combinations of topical antibiotics have the ability to disinfect carious dentin and necrotic, infected root canals. One combination that is eective against the bacteria commonly found in infected root canals is the use of: (1) ciprooxacin; (2) metronidazole; and (3) cefaclor.7 By application of a treatment protocol using this combination, it is expected that necrotic infected immature teeth can be rendered to the same starting point as avulsed immature teeth with necrotic but uninfected pulps (ie, a severed vascular supply secondary to avulsion). If this approach is successful, revascularization of the pulp space may be a predictable outcome in disinfected, necrotic, immature teeth. A bacteria-free canal is a prerequisite for tissue regeneration, but tissue will not grow into an empty space.8,9 Rather, a scaold is essential to aid the ingrowth of new tissue into the canal space. Induction of a blood clot, with its constituent growth and dierentiation factors10,11 from the periapical tissues, may act as a scaold for the ingrowth of new tissue in the disinfected necrotic immature toothnot unlike uninfected necrotic pulp does in an avulsion scenario. The blood clot consists of cross-linked brin. It serves as a pathway for the migration of cells,12,13 including macrophages and bro-
PULP REVASCULARIZ ATION IN A NECROTIC TOOTH
47
PEDIATRIC DENTISTRY
V 29 / NO 1
JAN / FEB 07
blasts from the periapical area. A blood clot, however, not only consists of an inactive scaold. Its cells contain many growth and dierentiation factors important in the woundhealing process.10,11,14 Human periapical granulation tissue also contains osteogenic cells.14 Three case reports show that it is possible to use disinfection protocols in vivo for the treatment of immature human teeth with necrotic pulps.15-17 These reports on necrotic premolar teeth in 11- to 13-year-olds show continued root formation after the canals were disinfected with various antibiotic pastes. The purpose of this case report was to add another example to the body of dental literature supporting this treatment modality as a mainstream treatment option for necrotic, infected, immature permanent teeth.
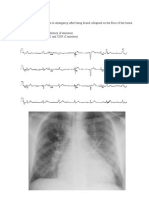
Case description A 9-year-old Caucasian boy was seen in the endodontic emergency clinic at the University of North Carolina School of Dentistry, Chapel Hill, NC, for evaluation and treatment of a maxillary anterior swelling in association with his permanent maxillary right central incisor (Figure 1). The tooth did not respond to cold testing with CO2 ice, although responses to percussion, palpation, and probing pocket depths were all within normal limits vs adjacent and contralateral teeth. The tooth was diagnosed with a necrotic pulp; and an acute apical abscess was treated by incision for drainage. The dental history disclosed that the patient had suered dental trauma nearly 2 years previously, sustaining a complicated crown fracture of his permanent maxillary right central incisor. The tooth was treated with a Cvek pulpotomy approximately 48 hours after the accident, but no rubber dam isolation was possible due to only partial eruption of the patients maxillary anterior teeth at that time. The patient maintained infrequent follow-up appointments after treatment for the initial dental trauma until he presented with the anterior maxillary swelling. At a subsequent appointment after the incision for
Figure 1. Preoperative radiograph showing open apex associated with necrotic pulp.
drainage was made, the tooth was disinfected with Betadine (10% Povidone Iodine Topical Solution, Purdue Products, Stamford, Conn) under local anesthesia and rubber dam isolation. Access was made to the pulp space where a necrotic pulp was conrmed clinically. The canal was not instrumented in the normal manner, but instead was irrigated copiously with 1.25% sodium hypochlorite (NaOCl) and dried with sterile paper points. A creamy paste of equal proportions of metronidazole (Shionogi and Co, Ltd, Osaka, Japan), ciprooxacin (Bayer, Leverkusen, Germany), and cefaclor (Shionogi and Co, Ltd) mixed with sterile water was applied to the canal space with a lentulo spiral in a slow-speed handpiece. The paste was tamped down in the canal space using the blunt ends of sterile paper points. The access cavity was closed with cotton pellets and intermediate restorative material (IRM; Dentsply Caulk, Milford, Del). The patient was asymptomatic when he returned for further treatment 11 weeks later. Under local anesthesia and rubber dam isolation disinfected with Betadine, the tooth was reaccessed. The antibiotic paste was intact in the canal space and was irrigated away using 10 mL of 1.25% NaOCl and 10 mL of sterile water to make space for a blood clot. No instrumentation of the canal space was performed. The apical tissues beyond the connes of the root canal were stimulated with a sterile endodontic le to induce bleeding into the canal space. Approximately 15 minutes were allowed for the blood clot to reach a level that approximated the cementoenamel junction. White mineral trioxide aggregate, MTA (Dentsply Tulsa Dental, Johnson City, Tenn) was mixed with sterile water and applied over the blood clot. A cotton pellet moist with sterile water was placed over the MTA and left protected by the rubber dam. After approximately 1 hour, the moist cotton pellet was removed from the MTA. The MTA exhibited a rm/hard set. The existing unesthetic composite restoration was removed from the tooths crown and an acid etch composite restoration was used to build up the tooths mesio-inciso-faciopalatal surfaces under rubber dam isolation to enhance the immediate seal of the canal space (Figure 2a). At the 3-month follow-up evaluation, the patient was asymptomatic. Compared with his adjacent and contralateral teeth, his right central incisor was within normal limits regarding: (1) percussion; (2) palpation; and (3) pocket probing depths. It was nonresponsive to stimulation with CO2 ice. Radiographic evaluation showed diuse radiopacities within the connes of the canal space. The patient returned for another follow-up assessment 6 months from the time of the blood clot induction. He remained asymptomatic, with normal responses to: (1) percussion; (2) palpation; (3) pocket probing depths; and (4) mobility. The tooth remained nonresponsive to CO2 ice. Radiographic evaluation disclosed signicant apical development of the tooth as well as a
48
PULP REVASCULARIZ ATION IN A NECROTIC TOOTH
PEDIATRIC DENTISTRY
V 29 / NO 1
JAN / FEB 07
greater number of radiopacities within the canal space. Follow-up evaluation at 9.5 months from the time of induction of the blood clot revealed similar clinical ndings: normal responses to percussion, palpation, pocket probing depths, and mobility, with a lack of response to both CO2 and electric pulp testing (EPT). Radiographic examination revealed: 1. continued apical development and closure; and 2. radiopacities within the canal space associated with a. partial pulp canal obliteration; and b. narrowing of the canal space. One year from the time of blood clot induction, the tooth remained asymptomaticwith normal responses to percussion and palpation and normal periodontal probing depths and mobility, but no response to CO2 or EPT. Radiographs revealed normal periapical structures with continued root development and calcication of the canal space (Figure 2b).
2a
2b
the tooth against future fracture. Even if the tissue in the canal space undergoes necrosis and subsequent infection at a later time, the prognosis for conventional endodontic therapy would be much better than had it been attempted with the open apex.18 If the progressive calcication of the root canal space continues to complete pulp canal obliteration, vitality will likely be maintained.19,20 If necrosis occurs, modern endodontic techniques utilizing the surgical operating microscope make treatment of such teeth more feasible than in the past. Case selection is important in this treatment protocol. It should be encouraged and promoted for clinicians faced with pulp necrosis with an immature apex that is open greater than 1 mm in a mesiodistal dimension radiographically. The size of the apical opening must be sucient to allow ingrowth of vital tissue. Kling3 suggested that an apical opening greater than 1 mm mesiodistally was associated with successful revascularization of avulsed permanent teeth, while no revascularization occurred in teeth with a smaller apical opening. The materials required for this protocol can be obtained from any pharmacy, and the treatment procedures themselves are less challenging than the more traditional techniques of treating pulpless teeth with open apices. If the attempted revascularization procedure fails, the traditional options of treatment remain, including long-term Ca(OH)2 apexication or MTA apexication followed by a conventional root lling. This case demonstrates that revascularization of necrotic infected root canal systems is possible in vivo. The traditional techniques for treatment of such teethincluding induction of a hard tissue barrier via Ca(OH)2 apexication or an articial hard tissue barrier of MTA without further physiological development of the root walls and apexmay one day be replaced if revascularization is shown to be predictable in controlled research models.
Acknowledgments The authors wish to acknowledge the assistance of Dr. Shizuko Yamauchi for her help with the Japanese translations, Dr. Bill Vann for his thorough review of the manuscript, and Warren (Mac) McCollum for his expertise in editing the photographs and radiographs.
Figure 2a: Postoperative radiograph after clot induction and direct restoration. Figure 2b: Radiograph at 12.5-month follow-up showing continued radicular wall thickening, apical closure, and narrowing of the canal space.
Discussion This case underscores the potential for revascularization of necrotic, infected root canal spaces with some form of vital tissue. Whether the new vital tissue is truly pulp or pulp-like is of little consequence, as long as there is continued development of the root canal walls and apex, which strengthens
References 1. Katebzadeh N, Dalton BC, Trope M. Strengthening immature teeth during and after apexification. J Endod 1998;24:256-9. 2. Andreasen JO, Farik B, Munksgaard EC. Long-term calcium hydroxide as a root canal dressing may increase risk of root fracture. Dent Traumatol 2002;18:134-7. 3. Kling M, Cvek M, Mejare I. Rate and predictability of pulp revascularization in therapeutically reimplanted permanent incisors. Endod Dent Traumatol 1986;2:83-9.
PULP REVASCULARIZ ATION IN A NECROTIC TOOTH
49
PEDIATRIC DENTISTRY
V 29 / NO 1
JAN / FEB 07
4. Yanpiset K, Trope M. Pulp revascularization of replanted immature dog teeth After dierent treatment methods. Endod Dent Traumatol 2000;16:211-7. 5. Kakehashi S, Stanley HR, Fitzgerald RJ. The eects of surgical exposures of dental pulps in germ-free and conventional laboratory rats. Oral Surg Oral Med Oral Pathol 1965;20:340-9. 6. Sundqvist G. Bacteriologic Studies of Necrotic Pulps. Umea, Sweden: The University of Umea; 1976. 7. Sato T, Hoshino E, Uematsu H, Noda T. In vitro antimicrobial susceptibility to combinations of drugs on bacteria from carious and endodontic lesions of human deciduous teeth. Oral Microbiol Immunol 1993;8:172-6. 8. Torneck CD. Reaction of rat connective tissue to polyethylene tube implants. I. Oral Surg Oral Med Oral Pathol 1966;21:379-87. 9. Torneck CD. Reaction of rat connective tissue to polyethylene tube implants. II. Oral Surg Oral Med Oral Pathol 1967;24:674-83. 10. Marx RE. Platelet-rich plasma: Evidence to support its use. J Oral Maxillofac Surg 2004;62:489-96. 11. Freymiller EG, Aghaloo TL. Platelet-rich plasma: Ready Or not? J Oral Maxillofac Surg 2004;62:484-8. 12. Harrison JW, Jurosky KA. Wound healing in the tissues of the periodontium following periradicular surgery. I. The incisional wound. J Endod 1991;17:425-35.
13. Harrison JW, Jurosky KA. Wound healing in the tissues of the periodontium following periradicular surgery. 2. The dissectional wound. J Endod 1991;17:544-52. 14. Maeda H, Wada N, Nakamuta H, Akamine A . Human periapical granulation tissue contains osteogenic cells. Cell Tissue Res 2004;315:203-8. 15. Rule DC, Winter GB. Root growth and apical repair subsequent to pulpal necrosis in children. Br Dent J 1966;120:586-90. 16. Iwaya SI, Ikawa M, Kubota M. Revascularization of an immature permanent tooth with apical periodontitis and sinus tract. Dent Traumatol 2001;17:185-7. 17. Banchs F, Trope M. Revascularization of immature permanent teeth with apical periodontitis: New treatment protocol? J Endod 2004;30:196-200. 18. Cvek M. Prognosis of luxated nonvital maxillary incisors treated with calcium hydroxide and lled with gutta-percha: A retrospective clinical study. Endod Dent Traumatol 1992;8:45-55. 19. Robertson A. Pulp survival and hard tissue formation subsequent to dental trauma. A clinical and histological study of uncomplicated crown fractures and luxation injuries. Swed Dent J 1997;125(suppl):1-65. 20. Robertson A. A retrospective evaluation of patients with uncomplicated crown fractures and luxation injuries. Endod Dental Traumatol 1998;14:245-56.
50
PULP REVASCULARIZ ATION IN A NECROTIC TOOTH
Potrebbero piacerti anche
- Regenerative Endodontic Treatment (Revascularization)Documento4 pagineRegenerative Endodontic Treatment (Revascularization)barcimNessuna valutazione finora
- Minimally Invasive Approaches in Endodontic PracticeDa EverandMinimally Invasive Approaches in Endodontic PracticeGianluca PlotinoNessuna valutazione finora
- Abstract and Key WordsDocumento10 pagineAbstract and Key WordsAliyah SaraswatiNessuna valutazione finora
- Regenerative EndodonticsDocumento46 pagineRegenerative EndodonticsShameena KnNessuna valutazione finora
- Challenges in Regenerative Endodontics: A Case SeriesDocumento6 pagineChallenges in Regenerative Endodontics: A Case SeriesDr.O.R.GANESAMURTHINessuna valutazione finora
- Regenerative Endodontics Barriers and Strategies For Clinical Translation 2012 Dental Clinics of North AmericaDocumento11 pagineRegenerative Endodontics Barriers and Strategies For Clinical Translation 2012 Dental Clinics of North AmericaCaioSelaimenNessuna valutazione finora
- Single Visit Apexification with MTA and Biodentin for Immature TeethDocumento10 pagineSingle Visit Apexification with MTA and Biodentin for Immature TeethShreya KediaNessuna valutazione finora
- Dental Pulp Autotransplantation: A New Modality of Endodontic Regenerative Therapy - Follow-Up of 3 Clinical CasesDocumento7 pagineDental Pulp Autotransplantation: A New Modality of Endodontic Regenerative Therapy - Follow-Up of 3 Clinical Casesveena rNessuna valutazione finora
- Apexogenesis of A Symptomatic MolarDocumento5 pagineApexogenesis of A Symptomatic MolarFoysal SirazeeNessuna valutazione finora
- En Do Don TicsDocumento5 pagineEn Do Don TicsAbhinav TalekarNessuna valutazione finora
- Apexogenesis and ApexificationDocumento4 pagineApexogenesis and ApexificationAlandNovrianDwiSaputraNessuna valutazione finora
- Revascularization of Immature Permanent Incisors After Severe Extrusive Luxation InjuryDocumento10 pagineRevascularization of Immature Permanent Incisors After Severe Extrusive Luxation InjuryEduardo CarrielNessuna valutazione finora
- 2012 Histologic Observation of A Human ImmatureDocumento5 pagine2012 Histologic Observation of A Human Immaturebenlaifaoui.amira.2511Nessuna valutazione finora
- ADJALEXU - Volume 43 - Issue 2 - Pages 7-12Documento6 pagineADJALEXU - Volume 43 - Issue 2 - Pages 7-12Belinda SalmaNessuna valutazione finora
- EndoDocumento9 pagineEndorishabh guptaNessuna valutazione finora
- One Step PulpDocumento36 pagineOne Step PulpDR.AMITHBABU.C.BNessuna valutazione finora
- Management of Blunderbuss CanalsDocumento11 pagineManagement of Blunderbuss CanalsNitesh PatilNessuna valutazione finora
- CCR3 11 E7714Documento6 pagineCCR3 11 E7714memo.09navNessuna valutazione finora
- Deciduous Tooth Pulp Autotransplantation For The Regenerative Endodontic Treatment of Permanent Teeth With Pulp Necrosis: A Case SeriesDocumento7 pagineDeciduous Tooth Pulp Autotransplantation For The Regenerative Endodontic Treatment of Permanent Teeth With Pulp Necrosis: A Case SeriesShameena KnNessuna valutazione finora
- Regenerative Treatment of An Immature, Traumatized Tooth With Apical Periodontitis: Report of A CaseDocumento6 pagineRegenerative Treatment of An Immature, Traumatized Tooth With Apical Periodontitis: Report of A CaseLaura ImreNessuna valutazione finora
- Clinical Case Reports - 2023 - Vyver - Apexification of Dens Evaginatus in A Mandibular Premolar A Case ReportDocumento6 pagineClinical Case Reports - 2023 - Vyver - Apexification of Dens Evaginatus in A Mandibular Premolar A Case ReportIqra KhanNessuna valutazione finora
- Regenerative EndodonticsDocumento7 pagineRegenerative EndodonticsEsha AroraNessuna valutazione finora
- Pulpotomy With PRFDocumento8 paginePulpotomy With PRFSai KalyanNessuna valutazione finora
- [International Endodontic Journal 2017-Jul 26 Vol. 51] Nazzal, H_ Kenny, K_ Altimimi, A_ Kang, J_ Duggal, M S - A Prospective Clinical Study of Regenerative Endodontic Treatment of Traumatised Immature Teeth With NeDocumento38 pagine[International Endodontic Journal 2017-Jul 26 Vol. 51] Nazzal, H_ Kenny, K_ Altimimi, A_ Kang, J_ Duggal, M S - A Prospective Clinical Study of Regenerative Endodontic Treatment of Traumatised Immature Teeth With Neكرم الباريNessuna valutazione finora
- Ejpd 2017 1 5Documento5 pagineEjpd 2017 1 5Mariatun Zahro NasutionNessuna valutazione finora
- 3 Badr2016Documento22 pagine3 Badr2016Daniel Espinoza EspinozaNessuna valutazione finora
- Recovery of Pulp Sensibility After the Surgical Management of a Large radicular cystDocumento5 pagineRecovery of Pulp Sensibility After the Surgical Management of a Large radicular cystmeryemeNessuna valutazione finora
- 2016 Dental Pulp Revascularization of Necrotic Permanent Teeth WithDocumento6 pagine2016 Dental Pulp Revascularization of Necrotic Permanent Teeth Withbenlaifaoui.amira.2511Nessuna valutazione finora
- 2nd Gen Platelet Rich ScaffoldDocumento8 pagine2nd Gen Platelet Rich ScaffoldShaliniNessuna valutazione finora
- Banchs Trope JOE 2004Documento5 pagineBanchs Trope JOE 2004digdouw100% (1)
- Management of Teeth With Persistent Apical Periodontitis After Root Canal Treatment Using Regenerative Endodontic TherapyDocumento6 pagineManagement of Teeth With Persistent Apical Periodontitis After Root Canal Treatment Using Regenerative Endodontic TherapyPaulina ÁlvarezNessuna valutazione finora
- Tissue Response To Dental CariesDocumento24 pagineTissue Response To Dental CariesGabriel Miloiu100% (1)
- 10 1016@j Joen 2019 10 009Documento8 pagine10 1016@j Joen 2019 10 009fatimahNessuna valutazione finora
- Outcome of Revascularization Procedure A Retrospective Case Series PDFDocumento8 pagineOutcome of Revascularization Procedure A Retrospective Case Series PDF吳國豪Nessuna valutazione finora
- Clinical Calcium Hydroxide Paste as a Surface Detoxifying Agent for Infected Dental ImplantsDocumento6 pagineClinical Calcium Hydroxide Paste as a Surface Detoxifying Agent for Infected Dental ImplantsDevvrat SinghNessuna valutazione finora
- Endodontic Retreatment in Case of Failure: Case ReportDocumento3 pagineEndodontic Retreatment in Case of Failure: Case ReportputriraudatulNessuna valutazione finora
- Nonsurgical RetreatmentDocumento4 pagineNonsurgical RetreatmentNia LieantoNessuna valutazione finora
- Copia de Tissue Response To Dental CariesDocumento7 pagineCopia de Tissue Response To Dental Cariesjorefe12Nessuna valutazione finora
- Tooth Autotransplantation As A Treatment Option: Dr. Eddie CK YAUDocumento4 pagineTooth Autotransplantation As A Treatment Option: Dr. Eddie CK YAUHatem Abo RiaNessuna valutazione finora
- Case Report Treatment of A Periodontic-Endodontic Lesion in A Patient With Aggressive PeriodontitisDocumento10 pagineCase Report Treatment of A Periodontic-Endodontic Lesion in A Patient With Aggressive PeriodontitissulistiyaNessuna valutazione finora
- Direct Pulp Capping in Primary Molars: Report of Two CasesDocumento3 pagineDirect Pulp Capping in Primary Molars: Report of Two Casesemie sitorusNessuna valutazione finora
- A Review of The Regenerative Endodontic Treatment ProcedureDocumento9 pagineA Review of The Regenerative Endodontic Treatment ProcedureOmar TalibNessuna valutazione finora
- Delayed Replantation of An Avulsed Permanent Incisor Tooth: Case ReportDocumento4 pagineDelayed Replantation of An Avulsed Permanent Incisor Tooth: Case ReportadiNessuna valutazione finora
- Dahl ApplianceDocumento8 pagineDahl Appliancesarah wilderNessuna valutazione finora
- Apexification ApexogenesisDocumento68 pagineApexification ApexogenesisSarath MohanNessuna valutazione finora
- Full Mouth Rehabilitation of The Patient With Severly Worn Out Dentition A Case Report.Documento5 pagineFull Mouth Rehabilitation of The Patient With Severly Worn Out Dentition A Case Report.sivak_198100% (1)
- Multiple Sites of Pink Spot Resorption in Primary TeethDocumento44 pagineMultiple Sites of Pink Spot Resorption in Primary TeethPrachi MulayNessuna valutazione finora
- Reimplantation of Avulsed Teeth After Dry Storage For One WeekDocumento5 pagineReimplantation of Avulsed Teeth After Dry Storage For One WeekHesti RahayuNessuna valutazione finora
- Management of Recently Traumatized Maxillary Central Incisors by Partial Pulpotomy Using MTA: Case Reports With Two-Year Follow-UpDocumento5 pagineManagement of Recently Traumatized Maxillary Central Incisors by Partial Pulpotomy Using MTA: Case Reports With Two-Year Follow-UpKevin Carmona TomyNessuna valutazione finora
- Influence of Age and Apical Diameter on TheDocumento6 pagineInfluence of Age and Apical Diameter on ThethaynamodtkowskiNessuna valutazione finora
- Trauma 4 Edited2Documento8 pagineTrauma 4 Edited2rushilzbox4701Nessuna valutazione finora
- International Journal of Research in Dentistry: Single Sitting Apexification Treatment With Mta Apical Plugs: A CaseDocumento4 pagineInternational Journal of Research in Dentistry: Single Sitting Apexification Treatment With Mta Apical Plugs: A CaseirfanaNessuna valutazione finora
- AvulsiDocumento10 pagineAvulsiNirma JerabunNessuna valutazione finora
- 1 s2.0 S0099239917312359 MainDocumento6 pagine1 s2.0 S0099239917312359 MainDANTE DELEGUERYNessuna valutazione finora
- Estefan 2016Documento6 pagineEstefan 2016mounica kadaliNessuna valutazione finora
- Cyst Decompression ReportDocumento5 pagineCyst Decompression ReportFrederick Alexander TrisnaNessuna valutazione finora
- Kim Regenerative EndodonticsDocumento51 pagineKim Regenerative Endodonticsrasagna reddyNessuna valutazione finora
- Diogenes2017.PDF Regenerative EndoDocumento15 pagineDiogenes2017.PDF Regenerative Endodrmezzo68Nessuna valutazione finora
- Blunt Trauma AbdomenDocumento41 pagineBlunt Trauma AbdomenSanthanu SukumaranNessuna valutazione finora
- OSCE PracticeDocumento8 pagineOSCE PracticeU$er100% (2)
- Nanotechnology Based Drug Delivery System,: "Nanomedicine"Documento10 pagineNanotechnology Based Drug Delivery System,: "Nanomedicine"rohit a bhosaleNessuna valutazione finora
- Fast Track Diagnostics Assays Brochure 0917 FINAL 1800000004342593Documento6 pagineFast Track Diagnostics Assays Brochure 0917 FINAL 1800000004342593Svasthya ManagerNessuna valutazione finora
- Nursing Home Checklist: Basic Information Yes No NotesDocumento9 pagineNursing Home Checklist: Basic Information Yes No NotesHarendra Narayan Singh100% (1)
- Bishop Score of PregnancyDocumento13 pagineBishop Score of PregnancydrvijeypsgNessuna valutazione finora
- Clinical Pharmacology Answers 2022Documento223 pagineClinical Pharmacology Answers 2022nancy voraNessuna valutazione finora
- Nutritional Content and Health Benefits of EggplantDocumento6 pagineNutritional Content and Health Benefits of Eggplantdhanashri pawarNessuna valutazione finora
- Antepartum HemorrhageDocumento3 pagineAntepartum Hemorrhagenur1146Nessuna valutazione finora
- IJMRHS VOl 3 Issue 3 With Cover Page v2Documento272 pagineIJMRHS VOl 3 Issue 3 With Cover Page v2Muhammad ZubairNessuna valutazione finora
- (IU-GADSOP 2018) (A4) First Announcement - Versi ADocumento1 pagina(IU-GADSOP 2018) (A4) First Announcement - Versi AIfah Inayah D'zatrichaNessuna valutazione finora
- The Hall Technique: Food for ThoughtDocumento50 pagineThe Hall Technique: Food for ThoughtMustafa Tambawala100% (1)
- Colorful insights into mental wellnessDocumento4 pagineColorful insights into mental wellnessJonrheym RemegiaNessuna valutazione finora
- Chapter 11 StsDocumento3 pagineChapter 11 StsCute kittyNessuna valutazione finora
- Dr. A. Hazekamp Self-Medication With CannabisDocumento39 pagineDr. A. Hazekamp Self-Medication With CannabisEl'Nelu Weed100% (2)
- 302 RUA - Interview WorksheetDocumento4 pagine302 RUA - Interview WorksheetChristy RobinettNessuna valutazione finora
- Resume William S Tokasz December 2015 For BuffstateDocumento2 pagineResume William S Tokasz December 2015 For Buffstateapi-301347959Nessuna valutazione finora
- DCA-Coalition Insulin GuidelinesDocumento5 pagineDCA-Coalition Insulin GuidelinesNabihah BarirNessuna valutazione finora
- Pathology Item CardDocumento2 paginePathology Item CardBir Mohammad SonetNessuna valutazione finora
- Lifestyle Medicine - The Future of Chronic Disease Management (2) - AnnotatedDocumento19 pagineLifestyle Medicine - The Future of Chronic Disease Management (2) - AnnotatedMaccaRiquelmeNessuna valutazione finora
- ATC 2014 GuidelinesDocumento286 pagineATC 2014 GuidelinesSilvanaMedhatNessuna valutazione finora
- Total Neoadjuvant Therapy in Rectal CancerDocumento9 pagineTotal Neoadjuvant Therapy in Rectal CancerMed MedNessuna valutazione finora
- Literatur A 123Documento5 pagineLiteratur A 123Adis ŠišićNessuna valutazione finora
- Methamphetamine EditedDocumento7 pagineMethamphetamine EditedJohn MainaNessuna valutazione finora
- Orthopedics P - Iv June15 PDFDocumento2 pagineOrthopedics P - Iv June15 PDFPankaj VatsaNessuna valutazione finora
- Barodontalgia 2009Documento6 pagineBarodontalgia 2009Maganti Sai SandeepNessuna valutazione finora
- OBGYN End of Rotation Exam OutlineDocumento35 pagineOBGYN End of Rotation Exam OutlinehevinpatelNessuna valutazione finora
- ValuCare University of Santo Tomas Hospital Plan Coordinators and SpecialistsDocumento2 pagineValuCare University of Santo Tomas Hospital Plan Coordinators and SpecialistsAnonymous HH3c17osNessuna valutazione finora
- Congenital SyphilisDocumento22 pagineCongenital SyphilisJuliana MariaNessuna valutazione finora
- Advantage and DisadvantageDocumento5 pagineAdvantage and Disadvantageحسين يوسفNessuna valutazione finora
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDa EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionValutazione: 4 su 5 stelle4/5 (402)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingDa EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingValutazione: 5 su 5 stelle5/5 (4)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDa EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityValutazione: 4 su 5 stelle4/5 (13)
- The Happiness Trap: How to Stop Struggling and Start LivingDa EverandThe Happiness Trap: How to Stop Struggling and Start LivingValutazione: 4 su 5 stelle4/5 (1)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDa EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNessuna valutazione finora
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDa EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsValutazione: 3.5 su 5 stelle3.5/5 (3)
- The Obesity Code: Unlocking the Secrets of Weight LossDa EverandThe Obesity Code: Unlocking the Secrets of Weight LossValutazione: 5 su 5 stelle5/5 (3)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDa EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedValutazione: 5 su 5 stelle5/5 (78)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisDa EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisValutazione: 4 su 5 stelle4/5 (1)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDa EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityValutazione: 3.5 su 5 stelle3.5/5 (2)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDa EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsNessuna valutazione finora
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsDa EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsValutazione: 4.5 su 5 stelle4.5/5 (169)
- The Ultimate Guide To Memory Improvement TechniquesDa EverandThe Ultimate Guide To Memory Improvement TechniquesValutazione: 5 su 5 stelle5/5 (34)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsDa EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNessuna valutazione finora
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingDa EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingValutazione: 3.5 su 5 stelle3.5/5 (31)
- Techniques Exercises And Tricks For Memory ImprovementDa EverandTechniques Exercises And Tricks For Memory ImprovementValutazione: 4.5 su 5 stelle4.5/5 (40)
- Summary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisDa EverandSummary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisValutazione: 5 su 5 stelle5/5 (3)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Da EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Valutazione: 4.5 su 5 stelle4.5/5 (110)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDa EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeDa EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeValutazione: 4.5 su 5 stelle4.5/5 (253)
- Secure Love: Create a Relationship That Lasts a LifetimeDa EverandSecure Love: Create a Relationship That Lasts a LifetimeValutazione: 5 su 5 stelle5/5 (17)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessDa EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessValutazione: 4.5 su 5 stelle4.5/5 (327)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryDa EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryValutazione: 4 su 5 stelle4/5 (44)

























![[International Endodontic Journal 2017-Jul 26 Vol. 51] Nazzal, H_ Kenny, K_ Altimimi, A_ Kang, J_ Duggal, M S - A Prospective Clinical Study of Regenerative Endodontic Treatment of Traumatised Immature Teeth With Ne](https://imgv2-1-f.scribdassets.com/img/document/649306081/149x198/6cdc9cdd33/1685435519?v=1)