Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
SURGPATH - 2.1 The Gastrointestinal Tract (Robbins) - Table
Caricato da
Angela CaguitlaTitolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
SURGPATH - 2.1 The Gastrointestinal Tract (Robbins) - Table
Caricato da
Angela CaguitlaCopyright:
Formati disponibili
II.
1 Gastrointestinal Tract
Robbins
A. ANATOMIC ANOMALIES DISEASE ETIOLOGY Atresia CHD Other GIT malformations Fistula GERD, Caustric burns, Radiotherapy Congenital, Scleroderma Congenital Long-standing reflux esophagitis Chronic graft-vs.-host disease congenital heart disease, neurologic problems, GU or other GI malformations Aspiration, suffocation from food, pneumonia, fluid & electrolyte imbalance
I.
THE ESOPHAGUS MORPHOLOGY Portion of esophagus is replaced by thin, noncanalized cord, with blind pouches above and below the atretic segment Connection between the esophagus and the trachea or a mainstem bronchus
CLINICAL MANIFESTATIONS
Incompatible with life
Stenosis
Episodic dysphagia
Esophageal wall fibrous thickening
Mucosal webs
Plummer-Vinson Syndrome: Cheilosis, glossitis, iron deficiency anemia Episodic dysphagia
UPPER esophageal muscosal overgrowths
Esophageal rings
Episodic dysphagia
LOWER esophageal muscosal overgrowths A ring: if above the gastroesophageal junction B or Schatzki ring: if at the gastroesophageal juction Muscularis propria hypertrophy
B. LESIONS ASSOCIATED WITH MOTOR DYSFUNCTION DISEASE ETIOLOGY CLINICAL MANIFESTATIONS inhibitory neuron dysfunction degeneration of CNS or peripheral nerves (DM, amyloidosis, cancer) protozoal (Toxoplasma) infection of esophageal myenteric plexus of nerves. Progressive dysphagia Aperistalsis Nocturnal regurgitation and aspiration of undigested food. COMPLICATIONS Inc risk of SCC (~5%). Candida esophagitis. Aspiration pneumonia. Airway obstruction.
MORPHOLOGY
Achalasia
Proximal esophageal dilation Thickened or thinned muscular walls Regurgitation with mucosal dage
Secondary Achalasia
Chagas disease Disorders of the vagal dorsal motor nuclei (polio, surgical ablation) Diabetic autonomic neuropathy Infiltrative disorders (malignancy, amyloidosis, sarcoidosis) Crura (muscles) of diaphragm and the esophagus are not close enough. COMPLICATIONS ulceration with bleeding & perforation. Rolling hernias can have strangulation & obstruction.
Hiatal Hernia
unknown. Rolling hernias can be secondary to surgery.
Sliding (axial): Shortened esophagus Traction of upper stomach into thorax Bell-like dilation of stomach w/in the thoracic cavity Paraesophageal (rolling): Cardia of stomach dissects into the thorax adjacent to the esophagus Outpouchings of the alimentary tract containing one or more wall layers
Diverticula Zenker Diverticulum disordered cricopharyngeal motor function Dysphagia, food regurgitation, mass in the neck Aspiration with pneumonia
UPPER esophagus
From 2015 2B edited by Anj. Anne. How. Jerro. Mark. Joseph. Tin
Page 1 of 8
Traction Diverticulum Epiphrenic Diverticulum Lacerations (Mallory-Weiss Syndrome) Boerhaave Syndrome Esophageal Varices
congenital or result of motor dysfunction discoordination of peristalsis & lower sphincter relaxation Episodes of excessive vomiting Failure of LES relaxation Alcohol Large amounts of alcohol Portal hypertension 90% of patients with alcoholic cirrhosis have esophageal varices. Schistosomiasis
asymptomatic Nocturnal regurgitation of massive amounts of fluid no symptoms until rupture with hematemesis 90% chance of recurrence Massive hematemesis Inflammation Residual ulcer Mediastinitis Peritonitis
Mid-esophageal Just above lower esophageal sphincter longitudinal tears across the esophagogastric junction or in the upper stomach are mucosal or sometimes entirely through the wall with perforation. Pressure rupture of the esophagus just above the diaphragm Tortuous, dilated veins in distal esophageal submucosa/mucosa. Irregular luminal protrusion of overlying mucosa Superficial ulceration, inflammation, adherent blood clots
C. ESOPHAGITIS DISEASE Reflux Esophagitis
ETIOLOGY
CLINICAL MANIFESTATIONS In adults Dysphagia Heartburn Regurgitation of gastric contents in the mouth Hematemesis Melena Stricture or Barrett esophagus
MORPHOLOGY
antireflux mechanisms Sliding hiatal hernias Delayed gastric emptying and gastric volume the esophageal mucosa
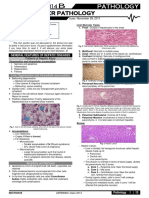
Hyperemia and edema Thickened basal zone & thinning of superficial epithelial layers Neutrophil or eosinophil infiltration Superficial necrosis and ulceration with adherent inflammatory exudate
Barrett Esophagus
long-standing gastroesophageal reflux disease (GERD).
In adults may lead to adenocarcinoma
Gross: irregular circumferential band of red, velvety mucosa at the gastroesophageal junction, with linear streaks or patches of similar mucosa in the distal esophagus Microscopic: Normal squamous mucosa of distal esophagus replaced by metaplastic intestinal-like columnar epithelium
Infectious and Chemical Esophagitis
Causes: Prolonged gastric intubation Ingestion of irritants: alcohol corrosive acids or alkalis, excessive hot fluids, smoking Bacteria, viral (Herpesvirus, CMV) or fungal (candidiasis, mucormycosis, aspergillosis) infection Uremia, Chemo- or radiotherapy, Graft-vs-host disease, Autoimmune diseases, Chron disease Systemic desquamative disorders (pemphigoid, epidermolysis bullosa)
A. CONGENITAL ANOMALIES DISEASE ETIOLOGY Pancreatic heterotopia Diaphragmatic Hernia Weakness of the diaphragm
II.
THE STOMACH MORPHOLOGY In the gastric muscle wall
CLINICAL MANIFESTATIONS
Fatal if with respiratory impairment with pulmonary hypoplasia Male to female ratio 4:1
In utero displacement of the stomach cephalad Hypertrophy or hyperplasia of pyloric muscularis propria Visible peristalsis Palpable firm ovoid mass Gross: edema and hyperaemia, acute hemorrhagic erosive gastritis Microscopic: neutrophil invasion, erosion
Pyloric Stenosis B. GASTRITIS NSAIDs, EtOH, tobacco, stress, uremia, chemotherapy, ischemia, radiation, systemic infections.
Acute Gastritis
Chronic Gastritis
H. pylori colonization of mucosa EtOH, tobacco, post-surgical, obstruction, Crohn disease
Gross: reddened, boggy, coarse-textured mucosa Histologically: Lymphocyte and plasma cell infiltrate in lamina propria Intraepithelial neutrophilic infil8s Mucosal gland atrophy Metaplasia of surface columnar epithelium to intestinal-type Dysplasia in long standing C. Gastritis
I.5 The Thyroid Gland (Robbins)
Page 2 of 8
C. PEPTIC ULCER DISEASE Epigastric gnawing, burning, or aching pain, worse at night and 1-3 hrs after meals. Nausea, vomiting, bloating, belching, weight loss COMPLICATIONS: Hemorrhage, perforation, peritonitis, scarring
Peptic Ulcer
exposure to acid and peptic juices
Gross: sharply punched-out defect with overhanging mucosal borders; smooth, clean ulcer bases Microscopic: necrotic debris; granulation tissue; deep scarring
Acute Gastric Ulceration
Severe stress shock, extensive burns, sever trauma (Curling ulcers) ICP (Cushing ulcers) NSAIDs
Acute gastric erosions or ulcers
Ulcers less than 1cm in diameter Ulcer base is brown (blood)
D. MISCELLANEOUS CONDITIONS Gastric outlet obstruction (pyloric stenosis, tumors) Gastric and intestinal atony (ileus) Phytobezoar trichobezoar (hairball) Heavy eosinophilic infiltration of the mucosa or submucosa Idiopathic; Allergy Hypoalbuminemia risk for PUD Protein-losing enteropathy TGF- overexpression (?) Hypochlorydia Hypoproteinemia Hyperchlorydia Excessive gastrin secrxn Gastrinoma (ZollingerEllison) In portal hypertension
Gastric Dilation
Rarely, gastric rupture
Bezoars Eosinophilic gastritis Hypertrophic Gastropathy Menetrier disease Hypertrophichypersecretory gastropathy Gastric Gland hyperplasia Gastric Varices
Luminal concretions
Hyperplasia of mucosal epithelial of gastric rugal folds Hyperplasia of surface mucous (foveolar) cells Fundic gland atrophy Hyperplasia of parietal and chief cells (fundic glands) Parietal cell hyperplasia Occurs near the gastroesophageal junction
Hyperchlorydia
III.
A. CONGENITAL ANOMALIES DISEASE ETIOLOGY Meckel Diverticulum Congenital Aganglionic Megacolon\ (Hirschsprung Disease) Acquired Megacolon Diarrhea
SMALL AND LARGE INTESTINES CLINICAL MANIFESTATIONS MORPHOLOGY Blind pouch leading off the alimentary tract, lined by mucosa and communicating with the gut lumen Absence of ganglion cells and ganglia in muscle wall and submucosa of affected segment (usu. Rectum)
Arrested (proximal to distal) migration of neural crest cells into the gut Assoc with Down syndrome
Male female ratio 4:1 Neonatal failure to pass meconium or abdominal distention Risk: perforation, sepsis, enterocolitis
Occur in Chagas disease, bowel obstruction, inflammatory bowel disease, and psychosomatic disorders
B. ENTEROCOLITIS >250 gm daily stool production with 70%-90% water Dysentery low volume painful diarrhea Secretory Net intestinal fluid secretion >500 mL/day; isotonic with plasma; diarrhea Osmotic >500 mL stool/day; osmotic gap diarrhea Malabsorption Voluminous, bulky stools w/ excess fat and osmolality Exudative Purulent bloody stools diseases Infectious Enterocolitis Rotavirus; Calicivirus (Norwalk/Norwalk-like Acute illness: 1-7 days Viral Entercolitis virus, Sapporo-like Diarrhea, anorexia, fever, virus); headache Enteric adenoviruses; Astroviruses
I.5 The Thyroid Gland (Robbins)
persists during fasting
Shortened villi lamina propria inflammation enterocyte amage (brush border loss & cytoplasmic vascuolization crypt hyperplasia
Page 3 of 8
Ingestion of preformed Bacterial Enterocolitis Infection w/ enteric
Antibiotic Clostridium difficile toxin Associated Colitis overgrowth after (Pseudomem-branous antibiotic therapy Colitis) Parasitic Nematodes, Cestodes, Enterocolitis Protozoa Immature gut immunity Onset of oral feeding Necrotizing Bacterial colonization Entercolitis Mucosal injury Impaired intestinal blood flow Collagenous Colitis Autoimmune disease, sprue Miscellaneous Intestinal Inflammatory Disorders AIDS-associated HIV diarrheal illness Lymphocytic Colitis Transplantation Drug-induced interstinal injury Radiation enterocolitis Neutropenic colitis (Typhlitis) Diversion colitis Colitis cystic profunda solitary rectal ulcer syndrome C. MALABSORPTION SYNDROME Defects in: Intraluminal digestion Terminal digestion Transepithelial transport NSAID
Explosive diarrhea & abd pain Hrs-days incubation; diarrhea; dehydration; dysentery Yersinial & mycobacterial infections Right colon plaquelike adhesion of fibrinopurulent necrotic, grayyellow debris and mucus to the damaged colonic mucosa
In low-birth-weight or premature neonates Mild diarrhea to fulminant illness with gangrene, perforation, sepsis, shock Chronic watery diarrhea with abdominal pain
Mucosal edema, hemorrhage, necrosis in terminal ileum and proximal colon or entire gut Patches of bandlike collagen under the surface epithelium Intraepithelial infiltrates of lymphocytes In mucosal epithelium Mild lymphocytic infiltrate Crypt epithelial cell apoptosis Focal ulceration Mucosal inflammation
Inflammatory diarrhea Bone marrow transplant Enterostomy Inadequate nutrition Acute inflammatory destruction of the cecal region Chronic lymphoplasmacytic inflammation Lymphoid follicular hyperplasia Acute angulation of anterior rectal shelf Mechanical abrasion Distorted, cystically dilated glands surrounded by proliferating smooth muscle cells
Rectal bleeding Mucosal discharge
MALABSORPTION SYDROME
Celiac Disease
Gluten in wheat, oat, barley, rye
Tropical Travel or habitation (Postinfectious) Sprue exposure
Whipple Disease
Tropheryma whippelii
Lactase Deficiency Abetalipoproteinemia Cannot synthesize apolipoprotein B
Diarrhea, flatus, pain, weight loss, bulky,frothy,greasy stools Anemia, bleeding Ostopenia, tetany Amenorrhea, impotence, infertility, hyperparathyroidism Purpura and petechiae, edema, dermatitis Peripheral neuropathy Diarrhea, flatulence, weight loss, fatgue marked atrophy of villi Antibodies to tissue elongated regenerative crypts transglutaminase and surface epithelial damage with gliadin intraepithelial lymphocytes Dermatitis herpetiformis exuberant lamina propria chronic COMPLICATIONS: iron inflammation and vitamin deficiencies; risk for GI lymphoma Villous blunting Abundant lymphocytes and eosinophils in lamina propria Diarrhea, steatorrhea, malabsorption, abdominal mucosa becomes laden w/ cramps, distention, fever, distended macrophages in the weight loss, migratory lamina propria arthritis, heart disease (+) PAS In whites and males Diarrhea; malabsorption No abnormalities of mucosa Failure to thrive, diarrhea, steatorrea, neurologic and Lipid vacuolation liver disorders, retinitis Burr cells pigmentosa
D. IDIOPATHIC INFLAMMATORY BOWEL DISEASE DISEASE ETIOLOGY CLINICAL MANIFESTATIONS Intermittent attacks of diarrhea, Genetic fever, abdominal pain, anorexia, Infectious weight loss Chron Disease Mucosal integrity Migratory polyarthritis, sacroiliitis, Abnormal host ankylosing spondylitis, erythema immunoreactivity nodosum, uveitis, cholangitis,
I.5 The Thyroid Gland (Robbins)
MORPHOLOGY Non-caseating sarcoid-like granulomas Transmural inflammation Goblet cell population Maintenance of gladular architecture Skip lesions
Page 4 of 8
Ulcerative Colitis
amyloidosis COMPLICATIONS: fistulas, malabsorption, malnutrition, protein-losing enteropathy Risk: bowel cancer Intermittent attacks of bloody mucoid diarrhea;abd pain Toxic megacolon Migratory polyarthritis, , sacroiliitis, ankylosing spondylitis, erythema nodosum, uveitis, cholangitis Risk: carcinoma
cobblestone appearance aphthous ulcers Chrronic mucosal damage; fibrosis; dysplasia Non-granulomatous No skip lesions Mucosa reddened, granular or friable iwth inflammatory pseudopolyps and easy bleeding
E. VASCULAR DISORDERS DISEASE ETIOLOGY
CLINICAL MANIFESTATIONS
Ischemic Bowel Disease
Arterial thrombosis Arterial embolism Venous thrombosis Nonocclusive ischemia
Severe abdominal pain Bloody diarrhea Gross melena Nausea Vomiting Bloating Abdominal wall rigidity
MORPHOLOGY Mucosal infarction: patchy mucosal hemorrhage Mural infarction: complete mucosal necrosis Transmural infarction: sudden and total occlusion of major vasculature; gangrene, peforation Venous thrombosis: acute mesenteric venous occlusion Chronic ischemia: mucosal inflammation, ulceration, fibrosis, stricture Tortuous abnormal dilations of submucosal veins to lamina propria of cecum or ascending colon
Angiodysplasia
Hemorrhoids
Constipation Venous stasis during pregnancy Cirrhosis (portal HPN) Usu asymptomatic Cramping, abd discomfort, constipation COMPLICATION: pericolic abscesses, sinus tracts, peritonitis CLINICAL MANIFESTATIONS
Variceal dilations of anal and perianal submucosal venous plexi
Diverticular Disease
Focal bowel wall weakness
Multi flask-like outpouchings
F. INTESTINAL OBSTRUCTION DISEASE ETIOLOGY Peritoneal wall weakness or defect
MORPHOLOGY Hernia sac Incarceration
Hernias
Adhesions
Peritonitis following surgery, infection, endometriosis, radiation Children rotaviral vaccination or infection Adults tumor
Complications: internal herniation; obstruction; strangulation
Fibrous bridging between viscera Telescoping of one intestinal segment into immediately distal segment
Intussusception Volvolus
Obstruction and infarction
Twisting of a bowel loop about its mesenteric vascular base
IV. APPENDIX
Obstruction of appendicial lumen by fecalith, calculus, intraluminal pressure ischemia bacterial invasion Periumbilical pain migrating to RLQ Nausea or vomiting Abdominal tenderness Mild fever Leukocytosis >15,000 cells/mm3
Acute Appendicitis
Early: scant appendicial wall neutrophil exudates congestion of subserosal vessels perivascular neutrophil emigration Advanced/Acute suppurative: Severe neutrophilic infiltration Fibrinopurulent serosal exudates Luminal abscess formation Ulceration Suppurative necrosis Dilation of appendiceal lumen by mucinous secretions Peritoneum distended Tenaceious semisolid, mucinproducing anaplastic
Page 5 of 8
Mucocele Pseudomyxoma peritonei
Innocuous obstruction with inspissated mucus Mucin secreting adenomas Adenocarcinoma
I.5 The Thyroid Gland (Robbins)
adenocarcinoma cells
V. PERITONEUM
A. INFLAMMATION DISEASE ETIOLOGY Appendicitis, peptic ulcer, cholecystitis, diverticulitis, bowel strangulation, acute salpingitis, abd trauma, peritoneal dialysis, nephritic syndrome, cirrhosis CLINICAL MANIFESTATIONS MORPHOLOGY Peritoneal membranes dull and gray; exudates and frank suppuration Localized abscesses Tuberculous peritonitis exudates studded with minute pale granulomas
1. Peritoneal Infection
Can resolve spontaneously or with therapy
2. Sclerosing Retroperitoni tis
Methydergide use Fibrosing disorders (carcinoid tumors, sclerosing cholangitis, Riedel fibrosing thyroiditis)
Hydronephrosis
Dense infiltrative fibrosing overgrowth of retroperitoneal tissues Lymphocyte, plasma cell, neutrophil infiltrate
3. Mesenteric Cysts
Arise from sequestered lymphatic channels, pinched-off enteric diverticula of developing foregut or hindgut, developmental cysts of urogenital orgin, pancreatic pseudocyts, or walled-off infections
B. TUMORS Primary tumors Mesothelioma Desmoplastic small round cell tumor Secondary tumors
TUMORS OF THE GASTROINTESTINAL TRACT ESOPHAGUS 1. Benign Tumors: a. Intramural or submucosal: Leiomyoma, fibroma, lipoma, hemangioma, neurofibroma, lymphangioma b. Mucosal (larger than 3cm): Squamous papilloma, Fibrovascular polyp, Inflammatory polyp 2. Malignant Tumors DISEASE ETIOLOGY CLINICAL MANIFESTATIONS MORPHOLOGY Adults older than 50 years Gross: lesions may be polypoid (60%), More often in men and blacks Dietary, exhibit necrotizing excavation (25%), or Dysphagia Lifestyle, diffusely infiltrative (15%) Squamous Cell Obstruction Esophageal Microscopic: tumors well differentiated, Carcinoma Weight loss disorders, with or w/o keratinisation (SCC) Hemorrhage Genetic Begin as in situ gray-white, plaquelike Sepsis Predisposition Respiratory tree fistulas with longitudinally/circumferential aspiration Gross: exophytic nodules to excavated and Patients older than 40, more deeply infiltrative masses Barrett Adenocarcinoma often in men Microscopic: mucin-producing glandular esophagus Symptoms of GERD and SCC tumors with intestinal futures; Diffusely infiltrative signet ring cells
STOMACH 1. Benign Tumors a. Non-Neoplastic Polyps DISEASE ETIOLOGY Hyper-plastic or inflammatory polyps Fundic gland polyps Inflammatory fibroid polyps Hamartomatous polyps Occur with Peutz-Jeghers syndrome or; Juvenile polyposis syndrome Assoc with chronic gastritis
CLINICAL MANIFESTATIONS 90% of gastric polyps
MORPHOLOGY Smooth, sessile or pedunculated Epithelial tubules and cysts interspersed Inflamed stroma Fundic gland dilation Fibroblast proliferation in submucosa with eosinophil infiltrate
Occur with FAP
I.5 The Thyroid Gland (Robbins)
Page 6 of 8
b. Neoplastic Polyps Gastric Adenoma 2. Malignant
Chronic gastritis Genetic polyposis syndrome
40% harbour carcinoma
Proliferative dysplastic epithelium Single, can be sessile or pedunculated
Gastric Carcinoma
Environment; Diet; Smoking; chronic gastritis; autoimmune gastritis; partial gastrectomy H. pylori infection c-KIT gene mutation
Usu. Asymptomatic Weight loss, abdominal painm, anorexia, vomiting, altered bowel habits, dysphagia, anemia, hemorrhage
Gastric mucosa dysplasia Tumors are exophytic, flat, or depressed or excavated (See Lauren classification)
Lymphoma (MALT) Gastrointestinal stromal tumor (GIST) Carcinoid Tumors Schwannomas Lipomas
Solid tumor of the gastric mucosa or wall Tumor cells are either epithelioid or spindle cell shaped Enterochromaffin-like cell tumor
TUMORS OF THE SMALL INTESTINE DISEASE ETIOLOGY Adenomas Adenocarcinoma In Px with familial polyposis syndromes
CLINICAL MANIFESTATIONS Clinically silent unless they obstruct the intestinal lumen or CBD Obstruction (cramping pain, nausea, vomiting), weight loss, bleeding
MORPHOLOGY
Metastatic spread to mesentery, regional lymph nodes, liver
TUMORS OF THE COLON AND RECTUM 1. Benign a. Non-neoplastic polyps DISEASE Hyperplastic polyp ETIOLOGY CLINICAL MANIFESTATIONS 6th decade MORPHOLOGY Nipple like hemispheric protrusions Well-formed mature glands with crowding Focal sporadic hamartomatous malformations of SI and colon mucosa Large polyps, rounded, and pedunculated w/ cystically dialted glands and abundant laminar polyp Sporadic hamartomatous mucosal polyps of SI and colon Large polyps, pedunculated, lobulated with arborizing smooth muscle surrounding normal glands
Juvenile polyp
Children <5yrs
Peutz-Jeghers polyp b. Adenoma (Neoplastic polyps) Tubular adenoma Villous adenoma Tubulovillous adenoma Serrated adenoma 2. Malignant Assoc with MSI
risk for carcinomas
Asyptomatic or may cause occult bleeding with anemia SI adenomas cause obstruction and intusseption
Tubular glands, smooth surface Villous frondlike projections of epithelial surface Mixture of first two Features of both hyperplastic polyp and adenoma
Colorectal Carcinoma (FAP)
APC gene mutation; DNA methylation K-RAS, SMADs, p53, telomerase mutation
Asymptomatic at first Fatigue, weakness, iron deficiency anemia, abd discomfort, progressive bowel obstruction, liver enlargement
Gross: polypoid exophytic mass or annular mass with napkin-ring obstruction Histological: tall, columnar cells with invasion
II.1 The Gastrointestinal Tract (Robbins) - Trans
Page 7 of 8
a. Carcinoid Tumors
Asymptomatic but Sx caused by tumor secretory products
Tumors are small, firm, yellow-tan intramural or submucosal masses Fibrosis of muscularis kinking and obstruction Microscopic: islands to sheets of uniform chohesive cells with scant, granular cytoplasm and oval, stippled nuclei (+) for chromogranin and synaptophysin Early lesions: plaquelike mucosal or submucosal expansions Advanced: full mural thickness or polypoid exophytic masses protruding to lumen Microscopic: atypical lymphocytes infiltrate
b. Gastrointestinal Lymphoma c. Mesenchymal Tumors Lipomas GIST Smooth muscle tumors Kaposi Sarcoma (Most common GI mesenchymal tumor)
Amenable to surgical resection; chemoresponsive
Asymptomatic Larger lesions: mucosal ulcerations with bleeding, obstruction, or intusseption
In SI or colon submucosa Spindle shaped ore epitheloid; c-KIT positive Spindle shaped lesions with smooth muscle phenotype Visceral involvement
II.1 The Gastrointestinal Tract (Robbins) - Trans
Page 8 of 8
Potrebbero piacerti anche
- Gastrointestinal PathologyDocumento14 pagineGastrointestinal PathologyRahul ShuklaNessuna valutazione finora
- GASTROINSTINAL TRACT Robbins 8th EditionDocumento4 pagineGASTROINSTINAL TRACT Robbins 8th EditionLim EricNessuna valutazione finora
- Robbins Ch. 20 The Kidney Review QuestionsDocumento10 pagineRobbins Ch. 20 The Kidney Review QuestionsPA2014100% (4)
- Flashcards FinalDocumento272 pagineFlashcards FinalMarie SantoroNessuna valutazione finora
- Endocrine System - Part 1 (Robbins)Documento28 pagineEndocrine System - Part 1 (Robbins)sarguss14100% (2)
- Patho4-6 - Liver (Dr. Dy)Documento13 paginePatho4-6 - Liver (Dr. Dy)miguel cuevas100% (1)
- Lymphomas and Leukemias ChartDocumento2 pagineLymphomas and Leukemias ChartPA2014Nessuna valutazione finora
- Chapter 7 Neoplasia 1 2 Robbins and Cotran Pathologic Basis of Disease PDFDocumento9 pagineChapter 7 Neoplasia 1 2 Robbins and Cotran Pathologic Basis of Disease PDFChethranNessuna valutazione finora
- Ch.1 Baby Robbins OutlineDocumento11 pagineCh.1 Baby Robbins OutlinePA2014100% (3)
- Robbins Pathology Chapter 24 - EndocrineDocumento2 pagineRobbins Pathology Chapter 24 - Endocrinescorpiosphinx79100% (2)
- Robbin's SummariesDocumento98 pagineRobbin's SummariesnopedontsuemepleaseNessuna valutazione finora
- Endocrine PathologyDocumento13 pagineEndocrine Pathologysarguss14100% (1)
- USMLE STEP 1: Microbiology Bug List With Drugs Bugs Drugs: Bacteriology BacteriologyDocumento4 pagineUSMLE STEP 1: Microbiology Bug List With Drugs Bugs Drugs: Bacteriology BacteriologymkhararahNessuna valutazione finora
- Endocrine Pathology p17-32Documento16 pagineEndocrine Pathology p17-32zeroun24Nessuna valutazione finora
- Pharma Super TableDocumento56 paginePharma Super TableMarco Paulo Reyes NaoeNessuna valutazione finora
- Most CommonsDocumento6 pagineMost CommonsBobet ReñaNessuna valutazione finora
- Top 100 Pathology Secrets List W/ NotesDocumento6 pagineTop 100 Pathology Secrets List W/ NotesPA2014100% (4)
- Infectious Disease Pathology p31-55Documento25 pagineInfectious Disease Pathology p31-55zeroun2450% (2)
- Robbins Ch. 18 Liver and Biliary Tract Review QuestionsDocumento12 pagineRobbins Ch. 18 Liver and Biliary Tract Review QuestionsPA2014Nessuna valutazione finora
- Table of Genetic Disorders: Download A Copy of This Study GuideDocumento11 pagineTable of Genetic Disorders: Download A Copy of This Study Guideerica perezNessuna valutazione finora
- High YieldDocumento4 pagineHigh YieldJobelle Fernandez-SantosNessuna valutazione finora
- TOPNOTCH Patho Supplement Handout For Sept 2018 UPDATED May 2018Documento25 pagineTOPNOTCH Patho Supplement Handout For Sept 2018 UPDATED May 2018Waiwit KritayakiranaNessuna valutazione finora
- Lung Head and NeckDocumento26 pagineLung Head and Neckzeroun24100% (2)
- Robbins Ch. 26 Bones Joints and Soft-Tissue Tumors Review QuestionsDocumento7 pagineRobbins Ch. 26 Bones Joints and Soft-Tissue Tumors Review QuestionsPA2014100% (1)
- Heart - PathologyDocumento22 pagineHeart - Pathologyjmosser100% (1)
- Systemic Response To InjuryDocumento5 pagineSystemic Response To InjuryJohn Christopher LucesNessuna valutazione finora
- Microbiology USMLE ReviewDocumento9 pagineMicrobiology USMLE ReviewLaura TapiaNessuna valutazione finora
- Hi Yield Notes in SurgeryDocumento16 pagineHi Yield Notes in SurgeryNiñoTan100% (2)
- Endocrine Gland Hormone(s) Secreted Stimulus Effect of Hormone Inhibition PathologyDocumento3 pagineEndocrine Gland Hormone(s) Secreted Stimulus Effect of Hormone Inhibition PathologySamuelNessuna valutazione finora
- Diseases - BiochemDocumento4 pagineDiseases - BiochemJay FeldmanNessuna valutazione finora
- Free AssociationDocumento10 pagineFree AssociationimorkzoneNessuna valutazione finora
- Gi Pathology - Block 3 ReviewDocumento34 pagineGi Pathology - Block 3 ReviewMatt McGlothlin100% (1)
- CNS Path ChartDocumento10 pagineCNS Path Chartjamesomoore100% (1)
- Liver - RobbinsDocumento25 pagineLiver - Robbinssarguss14100% (2)
- GIT Fully DoneDocumento14 pagineGIT Fully DoneTirtha Taposh100% (1)
- Micro Final Buzz Word CheatsheetDocumento10 pagineMicro Final Buzz Word CheatsheetThesmith FamNessuna valutazione finora
- Pathology of Liver, Biliary, and PancreasDocumento52 paginePathology of Liver, Biliary, and PancreasHassan.shehri100% (11)
- Nephrology ReviewerDocumento3 pagineNephrology ReviewerNix14Nessuna valutazione finora
- Harrison TablesDocumento163 pagineHarrison Tablesfrancieudo1Nessuna valutazione finora
- Gi - PathophysiologyDocumento96 pagineGi - Pathophysiologyjmosser100% (4)
- Patho Robbins Sumary Pereira MDDocumento22 paginePatho Robbins Sumary Pereira MDNicole SarcosNessuna valutazione finora
- Hallmark Findings PDFDocumento4 pagineHallmark Findings PDFGIST (Gujarat Institute of Science & Technology)Nessuna valutazione finora
- Nina Bacteria Chart Medical School Step 1Documento11 pagineNina Bacteria Chart Medical School Step 1M PatelNessuna valutazione finora
- Malassezia Furfur An-An Ap-Ap Naturally Found On The SkinDocumento48 pagineMalassezia Furfur An-An Ap-Ap Naturally Found On The SkinNikki ValerioNessuna valutazione finora
- Board Recall Must ReadDocumento8 pagineBoard Recall Must ReadSarahSalvanNessuna valutazione finora
- UW (Step 1) Renal - Educational Objectives PDFDocumento50 pagineUW (Step 1) Renal - Educational Objectives PDFDrbee10Nessuna valutazione finora
- Patho ReviewDocumento40 paginePatho ReviewCoy Nuñez100% (2)
- Chapter 8 Infectious Diseases Robbins and Cotran Pathologic Basis of DiseaseDocumento12 pagineChapter 8 Infectious Diseases Robbins and Cotran Pathologic Basis of DiseaseArun Nayak86% (7)
- Summary of Pathways Inhibitors/Poisons of The Etc: Cytosol CytosolDocumento6 pagineSummary of Pathways Inhibitors/Poisons of The Etc: Cytosol CytosolBeatrix Graecia Fernandez100% (1)
- Pathology Supplement Handout Nov 2018Documento25 paginePathology Supplement Handout Nov 2018Zak Kaz100% (2)
- Esophagous Stomach Small Intestine PathologyDocumento58 pagineEsophagous Stomach Small Intestine PathologytahaNessuna valutazione finora
- Surgical Disease of The Esophagus: Mahteme Bekele, MD Assistant Professor of SurgeryDocumento72 pagineSurgical Disease of The Esophagus: Mahteme Bekele, MD Assistant Professor of SurgeryBiniamNessuna valutazione finora
- PathologyDocumento28 paginePathologyninja-2001Nessuna valutazione finora
- Upper Gastrointestinal Pathology, Baru 2010Documento59 pagineUpper Gastrointestinal Pathology, Baru 2010adystiNessuna valutazione finora
- 07a. Non Neoplastic Disease of OesophagusDocumento35 pagine07a. Non Neoplastic Disease of Oesophagus21701101016 - Juliana Ayu NugrahaNessuna valutazione finora
- Small and Large IntestinesDocumento44 pagineSmall and Large IntestinespempuladesmondsimfukwelNessuna valutazione finora
- PA GI Tract Skuad Tandingan Elnineno!Documento281 paginePA GI Tract Skuad Tandingan Elnineno!Arsya AliNessuna valutazione finora
- DYSPHAGIA Lecture NotesDocumento84 pagineDYSPHAGIA Lecture Notesmcmak357Nessuna valutazione finora
- GI Stomach PDFDocumento65 pagineGI Stomach PDFBatool SherbiniNessuna valutazione finora
- Gyne 11Documento3 pagineGyne 11Angela CaguitlaNessuna valutazione finora
- Kiwi Market ResearchDocumento1 paginaKiwi Market ResearchAngela CaguitlaNessuna valutazione finora
- 01 - 01 - 2019 or Tech - Teñedo - CsiiDocumento1 pagina01 - 01 - 2019 or Tech - Teñedo - CsiiAngela CaguitlaNessuna valutazione finora
- Hellp 2Documento57 pagineHellp 2Angela CaguitlaNessuna valutazione finora
- GYNECOLOGY - 2.7 B&M Lesions of The CervixDocumento7 pagineGYNECOLOGY - 2.7 B&M Lesions of The CervixAngela CaguitlaNessuna valutazione finora
- GYNECOLOGY - 2.8 B&M Lesions of The OvariesDocumento6 pagineGYNECOLOGY - 2.8 B&M Lesions of The OvariesAngela CaguitlaNessuna valutazione finora
- Clinical Practice Guidelines For The Obstetrician - GynecologistDocumento79 pagineClinical Practice Guidelines For The Obstetrician - GynecologistAngela Caguitla67% (3)
- Management of Bleeding Due To Portal Hypertension - Surgical and MedicalDocumento5 pagineManagement of Bleeding Due To Portal Hypertension - Surgical and MedicalAngela CaguitlaNessuna valutazione finora
- Lab Rep #5 Body FluidsDocumento9 pagineLab Rep #5 Body FluidsAngela CaguitlaNessuna valutazione finora
- Gyne Onco Interns NotesDocumento54 pagineGyne Onco Interns NotesCoy NuñezNessuna valutazione finora
- PEDIA 4.1 NephrologyDocumento7 paginePEDIA 4.1 NephrologyAngela CaguitlaNessuna valutazione finora
- CPG POGS Cesarean SectionDocumento65 pagineCPG POGS Cesarean SectionAngela Caguitla100% (4)
- Hyper Parathyroid Ism - PTH ActionDocumento2 pagineHyper Parathyroid Ism - PTH ActionAngela CaguitlaNessuna valutazione finora
- FCM Group3 FilariasisDocumento90 pagineFCM Group3 FilariasisAngela CaguitlaNessuna valutazione finora
- Expt Lipid - Influence of Bile in The Action of LipaseDocumento3 pagineExpt Lipid - Influence of Bile in The Action of LipaseAngela CaguitlaNessuna valutazione finora
- 1.5 (2) Back MusclesDocumento7 pagine1.5 (2) Back MusclesAngela CaguitlaNessuna valutazione finora
- 1.5 DermatomesDocumento2 pagine1.5 DermatomesAngela CaguitlaNessuna valutazione finora
- 2 Dilemma of Inferior TurbinateDocumento17 pagine2 Dilemma of Inferior TurbinateputrivbpNessuna valutazione finora
- Clinical Applications of OrthodonticDocumento405 pagineClinical Applications of Orthodonticamina kaidNessuna valutazione finora
- Family Care Product Policyholder: SHAZIA KHALID (Quotation No. 1)Documento4 pagineFamily Care Product Policyholder: SHAZIA KHALID (Quotation No. 1)Moksh SharmaNessuna valutazione finora
- SPC Marbonor 100 MLDocumento6 pagineSPC Marbonor 100 MLJelena TerzicNessuna valutazione finora
- Ovarian Cysts & Torsion - 0Documento5 pagineOvarian Cysts & Torsion - 0mikonugrihiNessuna valutazione finora
- Sharma Krishna N., Exploration of The History of Physiotherapy (The Scientific Research Journal of India. SRJI Vol-1 No-1 Year 2012)Documento4 pagineSharma Krishna N., Exploration of The History of Physiotherapy (The Scientific Research Journal of India. SRJI Vol-1 No-1 Year 2012)Dr. Krishna N. SharmaNessuna valutazione finora
- Biochemistry - Meaning & ScopeDocumento2 pagineBiochemistry - Meaning & ScopeBasudev GoswamiNessuna valutazione finora
- NCM 109 MidtermDocumento12 pagineNCM 109 MidtermApril Maecy F. DignomoNessuna valutazione finora
- Drugs & Substance AbuseDocumento22 pagineDrugs & Substance AbuseRajaraamanSrinivasNessuna valutazione finora
- 3 LIT208RevH BrainPath-Product-Info FINAL 181003Documento2 pagine3 LIT208RevH BrainPath-Product-Info FINAL 181003Carlos Minino P.Nessuna valutazione finora
- Body Dysmorphic DisorderDocumento6 pagineBody Dysmorphic DisorderAllan DiasNessuna valutazione finora
- A02 419Documento36 pagineA02 419jaimeNessuna valutazione finora
- Acute Zonal Occult Outer Retinopathy A Classification Based On Multimodal ImagingDocumento10 pagineAcute Zonal Occult Outer Retinopathy A Classification Based On Multimodal ImagingStefanieNessuna valutazione finora
- ValiumDocumento12 pagineValiumAnonymous KPhTy0CENessuna valutazione finora
- BSC (N) Iii Year Child Health Nursing: Unit Vi - Management of Behavioural and Social Problems in ChildrenDocumento79 pagineBSC (N) Iii Year Child Health Nursing: Unit Vi - Management of Behavioural and Social Problems in ChildrenERIC ANGEL100% (1)
- PATIENT CASE HPI J.O. Is A 5 Yo Girl Who Is Brought To The PediatricDocumento5 paginePATIENT CASE HPI J.O. Is A 5 Yo Girl Who Is Brought To The PediatricKyla ValenciaNessuna valutazione finora
- Np2 Recalls 4Documento7 pagineNp2 Recalls 4AhrisJeannine EscuadroNessuna valutazione finora
- Underestanding Periods.Documento11 pagineUnderestanding Periods.Counseling BGANessuna valutazione finora
- RCP 2020Documento51 pagineRCP 2020Jose Jhampool Quevedo LealNessuna valutazione finora
- Health 6 - 3rd Quarter FinalDocumento43 pagineHealth 6 - 3rd Quarter Finalmarvin reanzoNessuna valutazione finora
- Psychotic DisordersDocumento52 paginePsychotic DisordersYazan Mahafza100% (1)
- Enteral NutritionDocumento11 pagineEnteral NutritionPablo CauichNessuna valutazione finora
- Gastro POMDocumento63 pagineGastro POMLionell Castillo100% (1)
- Asaftei Sohail 2018Documento7 pagineAsaftei Sohail 2018Ileana StoicaNessuna valutazione finora
- P 6-ScienceDocumento8 pagineP 6-ScienceMonydit santinoNessuna valutazione finora
- Abstract Book INAACCDocumento83 pagineAbstract Book INAACCrodtobingNessuna valutazione finora
- Optimize Your Brain S Cleansing Mechanism 2414Documento9 pagineOptimize Your Brain S Cleansing Mechanism 2414WilberellisNessuna valutazione finora
- GanglionDocumento10 pagineGanglionJunben DelacruzNessuna valutazione finora
- Heart Meridian Acupuncture PointsDocumento9 pagineHeart Meridian Acupuncture Pointsلوليتا وردةNessuna valutazione finora
- CNS Practical - Tutorial, Student VersionDocumento10 pagineCNS Practical - Tutorial, Student VersionDaniel CoyleNessuna valutazione finora